Abstract
Since the 1980s, survivorship for persons with spinal cord injury/disease (SCI/D) has significantly improved; however, life expectancy remains lower than the general population due to secondary health conditions (SHCs) that lead to decreased function and death. This study explored (1) facilitators and barriers to engaging in self-management (SM) for persons with SCI/D and (2) stakeholder perspectives on potential SM program components and content for intervention development. Around 38 participants with SCI/D responded to this cross-sectional study and needs assessment conducted at the University of Missouri, Columbia. Responses were analyzed to determine descriptive statistics. Participants indicated barriers to SM include transportation/distance, presence of SHCs, and a lack of local resources. Participants noted that virtual SM programs with strong psychological health/coping components were preferred. These findings should guide the development of an SM program tailored to SCI/D to reduce the prevalence and impact of SHC on the SCI/D population.
Plain Language Summary
Persons with Spinal Cord Injury/Disease (SCI/D) experience secondary health conditions to a higher degree than the general population which impacts their function, quality of life, and lifespan. The factors that limit or support participation in self-management behaviors and programs were explored and we asked people with SCI/D what they would want out of a self-management program tailored to their needs. Results showed that virtual programs with a both group and individual sessions with a strong mental health component were preferred.
Introduction
Mortality in the first 2 years for individuals with spinal cord injury/disease (SCI/D) has improved 40% in the last three decades due to focus on improving acute medical intervention (DiMarco & Dawson, 2014). Meaning there are a substantial percentage of individuals who survive their initial injury but require ongoing care and support at the community level to prevent secondary health conditions (SHCs) that are significantly associated with the cause of premature death for this population (Cao et al., 2019; Strauss et al., 2006). For this reason, the focus of care must shift from acute intervention to the utilization of rehabilitation and community programs for the 294,000 people living in the United States with SCI/D (National Spinal Cord Injury Statistical Center [NSCISC], 2020).
Each year, the number of people returning to their communities and managing chronic SCI increases as an estimated 17,000 people in the United States survive a new SCI/D (NSCISC, 2020). And though these individuals with SCI/D are often discharged from inpatient settings back to the community, the medical complications and associated costs persist due to limited ability for these individuals to manage the chronic symptoms of their condition (Conti et al., 2020; May et al., 2006). This not only poses health risks but is also an incredible financial burden on the individual, their family, and the health care industry as whole.
For example, in the first year of injury, the medical costs for a 25-year-old person with high tetraplegia (C1–C4) averages $1,129,302, and for each subsequent year, another $196,107 for an average lifetime cost of $5,010,748 (NSCISC, 2020). Re-hospitalization due to SHCs is a major contributor to these yearly costs and interrupt community participation (Krause & Saunders, 2011; Scott et al., 2004). The re-hospitalization rate for persons with SCI/D is approximately 30% every subsequent year after injury, with the average length of stay per hospital visit of 19 days (NSCISC, 2020). These chronic and prevalent SHCs put a burden on a person’s ability to engage in self-care, social participation, maintain employment, and participate consistently in community living (Krause & Saunders, 2011).
The length of time since injury, age at time of injury, etiology, and biological sex does not affect the likelihood of experiencing secondary health complications, such as pressure ulcers, spasms, pain, urinary tract infections (UTIs), bowel dysfunction, circulation issues, and sexual dysfunction (New, 2016). According to prior research, persons with tetraplegic injuries, higher body mass, traumatic lesions, complete lesions, and aging with SCI/D are the greatest risk factors for secondary conditions, such as UTIs, pressure sores, respiratory complications, and pain (Haisma et al., 2007; Richards et al., 2004). The presence of these SHCs leads to decreased life expectancy, as well as the rising cost of health management for the person with a spinal cord injury (Krause & Saunders, 2011). The secondary conditions persons with SCI/D experience are well documented, preventable, and treatable and have a significant impact on independence and quality of life. These data highlight the lack of health management skills following injury and acute intervention for individuals with SCI. One factor likely impacting this is the reduced number of days of inpatient care a person has following their injury; during which they learn the critical knowledge and skills for maintaining their health when returning to the community. Since the 1970s, the average hospital length of stay for this population has decreased from 24 days to 11 days, and subsequently, rehabilitation length of stay has been reduced to a third from 98 to 31 days according to current data (NSCISC, 2020). During which, in a 1-week span of inpatient rehabilitation patients with SCI are only spending an average of 14% of that time (Whiteneck et al., 2011) with therapy where they are most likely to be learning the skills necessary for self-care and management. Owing to the decreased length of stay, individuals are unable to adequately learn the content and skills needed to successfully manage their health at the community level (Conti et al., 2020). Furthermore, more recent studies quantifying rehabilitation at the community level for persons with neurological disorders have concluded that the amount of rehabilitation currently being provided at the community level is likely insufficient to improve functional performance and quality of life (Saumur et al., 2022). Therefore, it is timely and plausible that a community-based self-management (SM) program would be beneficial to address these ongoing needs for persons with SCI/D.
SM is a proven intervention approach to help individuals learn to manage chronic conditions for numerous lifelong diagnoses such as stroke, diabetes, multiple sclerosis, cancer, chronic obstructive pulmonary disorder, and others (Ory et al., 2013). There is a significant amount of evidence that SM approaches can improve performance in activities of daily living, improve quality of life, lower rates of depression, decrease emergency department visits, decrease hospitalization, and even improve physical functioning (Brody et al., 2002; Jones & Riazi, 2011; Ory et al., 2013; Wolf et al., 2017). Although health care professions use elements of SM education within acute care and rehabilitation hospitals, there has been little formal program development for individuals with SCI. In spite of education and improved content knowledge within the rehabilitation setting, evidence shows that poor health problem-solving remains for people with spinal cord injuries postdischarge (May et al., 2006). This suggests that further development of SM programs could enhance the SCI/D populations’ ability to manage their health within the community for optimal prevention and care of SHCs. While current programs exist, their success within the SCI/D population has been limited.
An example of a gold-standard SM program for chronic conditions is the Stanford Chronic Disease Self-Management Program (CDSMP) (Lorig et al., 2001). The CDSMP has evidentiary validity and success in decreasing the prevalence of secondary conditions resulting in subsequent medical care; for example, findings show reduced emergency department visits for participants at 12 months postintervention (Ory et al., 2013). Although traditional SM programs, like the CDSMP, have been used with individuals diagnosed with chronic neurological conditions and have been proven to improve health outcomes in other populations; satisfaction, attrition, and outcomes for these programs within the SCI population is low (Allin et al., 2018; Hirsche et al., 2011; Lorig et al., 2001). Few SCI/D SM programs have been established and reported in literature.
A lifestyle redesign study to address pressure ulcers for persons with SCI/D was reported in 2017; however, the results of its efficacy were inconclusive (Carlson et al., 2019). Another study implemented a telehealth voice-automated response system, “CareCall” that addressed pressure ulcers, health care utilization, and depression through weekly phone calls via an automated system. While the depression scores improved at the 6 month follow-up, no significant improvements in health care utilization or pressure sore development were noted (Houlihan et al., 2013). The findings of these studies suggest that designing a new SCI/D SM that is successful in reducing SHCs and improving SM skills requires further investigation to identify the unique considerations for this population that could better inform program development. Therefore, it is imperative to consider the facilitators and barriers to engagement in SM programs for the SCI population.
Qualitative studies have suggested that funding, accessibility, psychological health, physical limitations (including the presence of secondary conditions), and caregiver support can be barriers to engaging in SM programs (Munce et al., 2014). In addition, the importance of mood and psychological health of both the participant and their caregiver (if required) plays a significant role in a person’s motivation and ability to engage in an SM program effectively (Munce et al., 2014). In addition, persons with SCI/D have also reported what facilitators improve their motivation and engagement in these programs.
Preliminary evidence supports that SCI/D participants have greater engagement when information is presented from a peer or trusted health professional and when health information is discussed with peers or in groups (Allin et al., 2018). One study implemented a two-part inpatient education group workshop to prevent pressure ulcers. Almost 75% of their intervention group had a pressure ulcer in the 12 months prior. The study found that following the therapeutic patient education, the incidence of pressure sores reduced to 30% in the following 12 months (Robineau et al., 2019). Persons with spinal cord injuries have also suggested that multimedia, interactive, and telehealth platforms are preferred (Newman et al., 2019). In addition, a telehealth modal structured program may be beneficial for this population to account for the potential lack of transportation, psychological factors, and physical barriers to engagement. While much is known about potential SM needs for individuals with SCI/D, these factors need to be further explored in the context of developing a tailored SM program for individuals with SCI/D.
The overall objective of this study was to evaluate the facilitators and barriers to participation in an SCI/D SM program for the community-dwelling individual with SCI/D. In addition, the objective of this study was to explore health care needs to inform the content of a potential SCI/D-tailored SM program. The long-term goal is to develop an SM program for the spinal cord–injured person to improve health and participation in the community.
Methods
Research Design
This was a cross-sectional quantitative study with participants with SCI/D (n = 38) who were living in the community conducted at the University of Missouri and administered online via REDcap. Participants were asked to respond to the Spinal Cord Injury Self-Management (SCISM) Survey to explore facilitators and barriers to SM for individuals with SCI/D and complete a needs assessment related to SM program delivery and content. The SCISM Survey was designed based on current literature by the Principal Investigator, an SCI occupational therapist and PhD candidate, to better understand stakeholder perceptions of facilitators and barriers to SCI/D SM using principles from participatory design. The Institutional Review Board of the University of Missouri, Columbia, reviewed and approved this study. Informed consent was obtained from all participants in this study.
Participants and Recruitment
A convenience sample of individuals with SCI/D was recruited via email, social media, flyers, and word of mouth primarily from the University of Missouri Health Care System. Participants were included in the study if they met the following criteria: 18 years of age or older, a diagnosis of SCI (traumatic or nontraumatic), willingness to respond in English, and living in the community with or without caregiver assistance. Exclusion criteria included persons living in skilled nursing or assisted living facilities.
Measures
Demographic Questionnaire
Basic demographic information was gathered from the individuals with SCI/D as well as a brief health history, level of injury, injury etiology, and years since injury.
SCISM Survey
This survey was constructed for this study to reflect and expand on the findings of previous research that explored facilitators and barriers for individuals with SCI/D to participate in SM programs (Allin et al., 2018; Munce et al., 2014). The survey included five domains with 56 Likert-type-scale items covering a range of topics such as ability, accessibility, transportation, motivation, psychological factors, activities and health, presence of SHCs, and interest. Statements were structured to be rated on a 9-point Likert-type Scale (1 = Strongly Disagree, 5 = Neutral, 9 = Strongly Agree). A free-text response option, “Please elaborate on and/or discuss any other barriers or facilitators in regards to [domain] that were not mentioned above.” was also included within each domain to give opportunity for participants to identify facilitators and/or barriers that may not have been covered by the survey items (see Supplemental Appendix A).
SCISM Survey Domains
Survey items were categorized by domains to reflect common themes appearing across current literature (Allin et al., 2018; Conti et al., 2020; Hirsche et al., 2011; Munce et al., 2014). The domains are as follows: (1) Ability: items pertaining to an individual’s ability to engage in health management activities and attend appointments in relation to resources, time, physical assistance, and perceived personal or family burden; (2) Accessibility: items referring to persons with SCI/Ds’ ability to access and use resources such as technology, brick and mortar health care establishments, and community resources with or without assistance; (3) Motivation: items addressing facilitators and barriers to motivation for persons with SCI/D regarding SM and SM behaviors; (4) Activities and Health: items related to specific common SHCs experienced because of SCI/D and the impact of these SHC on daily life; and finally, (5) Interest: items gauging interest in a potential SM program for persons with SCI/D (see Supplemental Appendix A).
SCISM Needs Assessment
Finally, participants were asked to complete a needs assessment by ranking six potential SM program components and 10 topics from most (1) to least (6, 10) important (see Supplemental Appendix A).
Administration and Scoring
The SCISM Survey was administered via REDCap, a secure site for managing surveys and databases. Participants were given a link to access the consent form and online survey to complete on their own. Participants also had the option to complete over the phone with the PI if it was their preference or due to accessibility issues. Prior to administration, the survey was reviewed by clinical occupational therapists, physical therapists, and a clinical psychologist.
Statistical Analyses
All data were cleaned and checked for accuracy, and all statistical procedures were performed using IBM SPSS v27 (IBM Corp., 2020). Incomplete survey responses were included to the extent that they were appropriate for specific survey items for analysis. Frequencies and percentages were calculated for demographic data. Descriptive analyses were conducted to determine item averages and standard deviations by SCISM survey domains. Free-text responses were not formally analyzed and were included only to provide further insight for interpretation of quantitative values.
Results
Participant Demographics
Participants (n = 38) were primarily white (89.5%) males (63.2%) with an average age of 47.2 years. The majority had quadriplegic injuries (52.6%) and were 10+ years out from their initial injury (39.5%). The majority (84.2%) also reported either having received or currently receiving inpatient or outpatient therapy related to their SCI/D. Most participants (65.8%) also indicated they did have a caregiver. Refer to Table 1 Participant Demographics for further details.
Demographics.
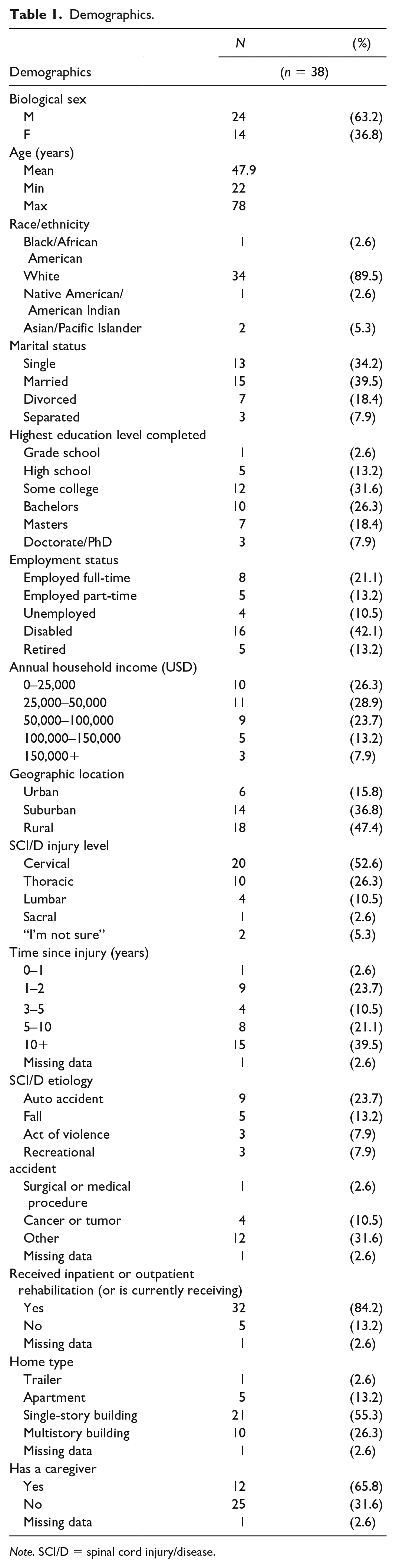
Note. SCI/D = spinal cord injury/disease.
Survey Results
Thirty-eight participants completed the SCISM Survey and 87% of these participants (n = 33) completed the Needs Assessment. Items from the SCISM Survey with means greater than 6.00 and lower than 4.00 are reported in two figures for ease of readability (see Figures 1 and 2). In addition, participants had the ability to leave free-text comments within each of the domains to provide further insight to their responses as well as to address any additional information that may not have been included in the survey items that they felt were pertinent.
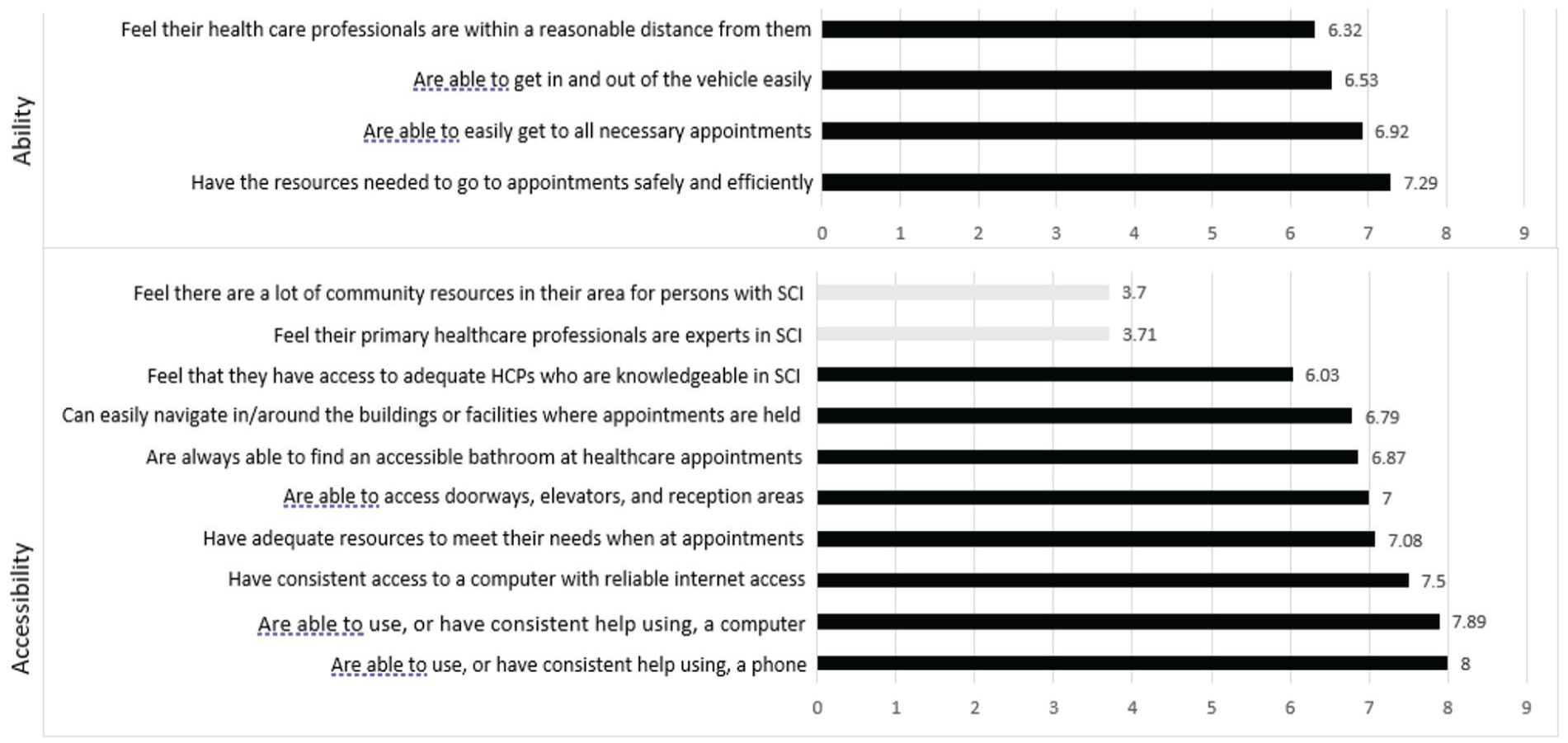
SCISM Survey Results Ability and Accessibility.
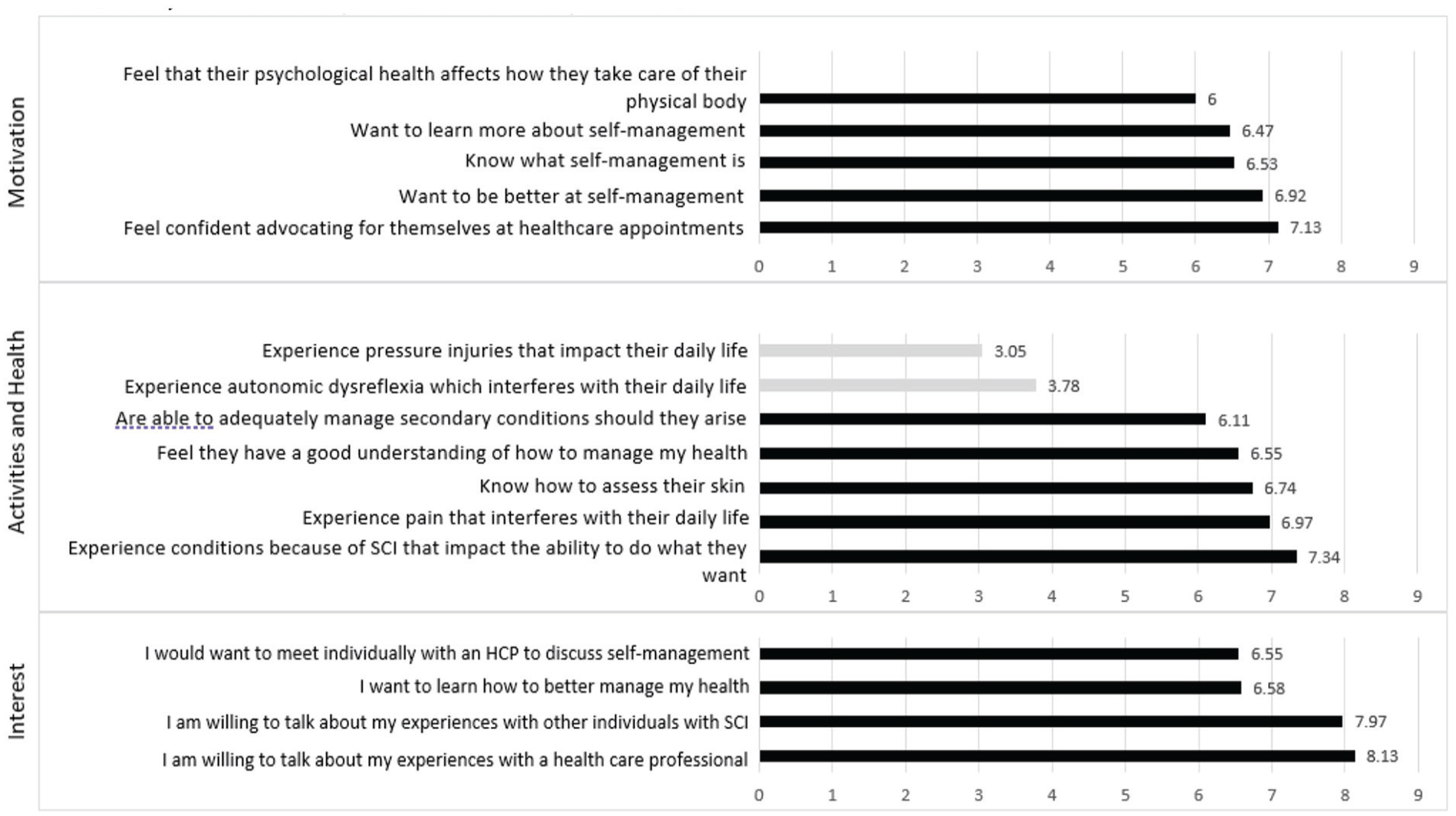
SCISM Survey Results, Motivation, Activities and Health, and Interest.
Ability
Participants agreed (M = 7.29, SD = 2.3) that they have the resources needed to go to appointments safely and efficiently and that they can easily get to all necessary appointments (M = 6.92, SD = 2.20) and that health care providers are within a reasonable distance (M = 6.32, SD = 2.81) from them. However, participants also left comments about the impact of inclement weather, transportation costs, lack of local specialists, appointment availability, increased pain from riding in vehicles, and risks to their skin during long duration car rides to appointments as barriers. No items in this domain fell below a mean rating of 5.00 which was a “neutral” response (Figure 1).
Accessibility
The majority of patients agreed that they have access to and are able to consistently use a phone, computer, and have reliable internet access (M = 8.00, SD = 1.86; M = 7.89, SD = 1.78; M = 7.50, SD = 2.22, respectively). They also reported that can access doorways, elevators, reception areas (M = 7.00, SD = 2.46) and that their health care providers have adequate resources to meet their needs while there (M = 7.08, SD = 1.99). However, participants did not agree that there are a lot of community resources in their area for persons with SCI/D (M = 3.70, SD = 2.37), that their primary health care professionals (HCPs) are experts in SCI/D (M = 3.71, SD = 2.32), or that their health care providers understand the unique needs of persons with SCI/D (M = 4.82, SD = 2.72). Participants also left several comments about lack of accessible parking at health care appointments, inadequate appointment length, and lack of help or care for persons with SCI/D both in health care and in the community (Figure 1).
Motivation
Most participants agreed that they felt confident in advocating for themselves at health care appointments (M = 7.13, SD = 2.41) but that they also want to be better at SM (M = 6.92, SD = 2.05). Few, however, agreed that they learned about SM from HCPs (M = 4.95, SD = 2.78) despite knowing what SM is (M = 6.53, SD = 2.71). When asked to respond to statements regarding psychological health and coping, participants did not agree that they were less likely to attend appointments when feeling anxious or depressed (M = 4.47, SD = 3.37) or that they felt anxious when meeting new people (M = 4.34, SD = 2.90). Despite this, several comments were left which noted lack of social support, fatigue, chronic pain, and psychological health affected their life and behaviors. For instance, some participants stated that depression led to lack of pressure relief, sleeping through catheterization times, forgetting to take meds, and feeling like they do not have the will to live anymore since their injury but are only living for the sake of their families (Figure 2).
Activities and Health
Participants agreed that they experienced conditions because of SCI/D that impact the ability to do what they want (M = 7.34, SD = 2.13) including pain (M = 6.97, SD = 2.57). Participants agreed least that persons with SCI/D experience pressure injuries or pressure ulcers that impact their daily life (M = 3.05, SD = 2.86) yet 60% of free-text comments which mentioned SHC left by participants for this domain discussed how the presence of pressure injuries impacted their ability to work, attend class, have “impacted [their] life the most” has made them “immobile” and that they felt they were never informed about how to “deal with” pressure wounds (Figure 2).
Interest
No item’s average in this domain fell below neutral (M = 5.00). Participants overwhelmingly agreed (M = 8.13, SD = 1.80) that they are willing to talk about their experiences with HCPs and others with SCI/D (M = 7.97, SD = 1.90). They also agreed that they want to learn how to better manage their health (M = 6.58, SD = 2.50) and that they would want to meet individually with an HCP (M = 6.55, SD = 2.30). Participants expressed in the free-text section that they would want SM programs for SCI to include exercise programs for persons with SCI/D, sexual functioning after SCI/D, and incomplete SCI/D support. Some concerns expressed included time commitment, not feeling like doctors [HCP] understand their situation, posttraumatic stress disorder (PTSD), and anxiety making it hard for them to meet other people despite wanting to, and risks to their skin if participation involved traveling a long distance from home. However, participants also expressed that a SM program would help them feel less alone and that their “cries of help” were heard (Figure 2).
Needs Assessment
Participants rated having virtual meetings as the most important component of an SM program (M = 3.03, SD = 1.73) followed by group discussion (M = 3.17, SD = 1.56), and being easily accessible (M = 3.23, SD = 1.83). The least important component as ranked by participants was caregiver involvement (M = 4.41, SD = 1.71; Table 2).
Needs Assessment.
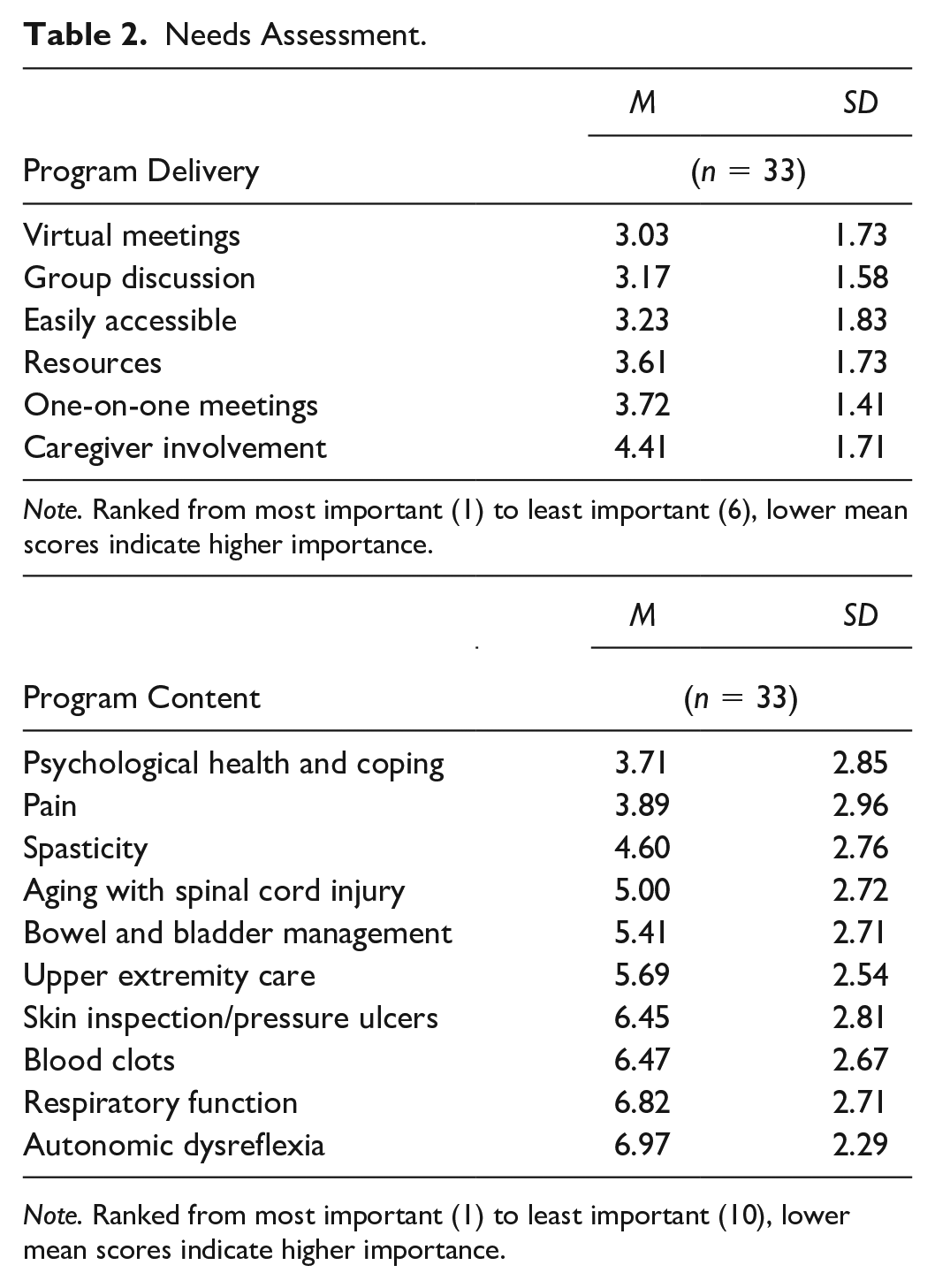
Note. Ranked from most important (1) to least important (10), lower mean scores indicate higher importance.
Participants were also asked to rank potential program topics from most (1) to least important (10). Participants indicated that psychological health and coping was most important (M = 3.71, SD = 2.85) followed by pain (M = 3.89, SD = 2.99), spasticity (M = 4.60, SD = 2.76), and aging with SCI (M = 5.00, SD = 2.72). Respiratory function and autonomic dysreflexia were the topics rated as least important (M = 6.82, SD = 2.71; M = 6.97, SD = 2.29, respectively; Table 2).
Discussion
Participants’ responses indicated interest in SM programs tailored to SCI/D needs and highlighted some of the integral aspects they expect of such a program, as well as what barriers currently exist that limit their participation. One of which being transportation and lack of local specialists or health care resources for those with SCI/D. A potential solution for this is the adoption of a community-based telehealth intervention.
Telehealth has been an emerging practice area in occupational therapy for more than a decade (Estes, 2017). However, during the COVID-19 pandemic, telehealth interventions were swiftly adopted across the globe in various practice settings due to the pressing need for immediate solutions for patients to safely access care (Kichloo et al., 2020; Signal et al., 2020). Owing to this, the health care system has become more open and accustomed to using telehealth practices and has begun to refine their use which makes it an ideal option for an SM program for the SCI/D population (Kichloo et al., 2020). As participants noted, there were often concerns or health risks involved with traveling to health care appointments, and many indicated that their SCI/D providers were a far distance from where they lived. Acquiring accessible transportation may be an additional barrier for persons with SCI/D whose socioeconomic status may have been impacted by the onset of their injury due to loss of employment. Many participants also indicated that they did not know or have friends with SCI/D. The adoption of a virtual program, however, opens the potential for persons with SCI/D to engage with HCPs and peers in health-related tasks, like an SM program, from home where they are more likely to have adequate resources, necessary adaptations, and support to engage successfully. Telehealth delivery also eliminates the barrier of transportation for sufficient participation.
Signal et al. (2020) compiled information related to telehealth adoption in neurologic populations and found that provider assumptions that telehealth would not be preferred or successful with their patients was often incorrect. This could explain why “Virtual Meetings” was ranked the highest in the Needs Assessment. To adequately meet this need however, several factors should be considered to increase success: technology selection, clearly designed protocols in the case of adverse events, guides for technology use, and participant technology training before beginning treatment or intervention (Signal et al., 2020). Signal et al. (2020) also highlights important considerations during telehealth implementation to increase engagement and therapeutic success. Participants indicated that for an SM program, they would like to engage with both a HCP and others with SCI/D. The success of which relies on participant ability to engage with both the HCP facilitating the program and other members. Research indicates that while initial rapport may take longer to establish, the quality of the therapeutic relationship and maintaining it via telehealth remains unchanged from the provider perspective (Signal et al., 2020).
Owing to the heterogeneity of injury within SCI/D, lived experiences vary greatly, which could explain why the topics of autonomic dysreflexia and respiratory function were rated the least important as they affect those with higher-level injuries more significantly. However, there are still common threads such as facing similar SHCs or barriers they experience due to injury. Results from the Needs Assessment indicate which of these shared experiences are most important to address within a tailored SM program. Psychological health and coping was ranked most highly which is consistent with literature as persons with SCI/D are at higher risk of anxiety, depression, alcohol dependency, dementia, and psychological multimorbidity (Sandalic et al., 2022).
It is known that the presence of mental health disorders is also correlated with negative health behaviors, increased risk for SHC, and increased burden for both the individual with SCI/D and caregiver(s) (Conti et al., 2019). This was echoed in several survey items and free-text responses that discussed the impact poor mental health had on their physical health. Any tailored SM program for this population, therefore, must include a strong mental health component which acts as a thread throughout the remaining content areas covered. This could be achieved using theoretical frameworks such as the theory of Psychosocial Adaptation to Chronic Illness and Disability (PA-CID) (Livneh, 2022).
The PA-CID approaches the process of psychological health to chronic illness and disability with a three-part model, each of which incorporates context, medical and psychological status, and intra/inter/extra personal factors including functional performance (Livneh, 2022). This theory ties in well with the aim and scope of occupational therapy SM interventions to affect the underlying psychological mechanisms while integrating the importance of contextual and environmental factors that result in decreased functional performance, independence, and quality of life within the community.
Limitations
There are several limitations to note with this study. The first being a relatively modest sample size, which may reflect limitations in recruitment strategy. Most recruitment was via online communication which could have disproportionately excluded participation from persons of low socioeconomic status, which can be exacerbated by the onset of SCI/D due to loss of employment. It also could have disproportionately excluded those with higher-level SCI/D injuries with less access to adaptive technology and/or caregiver support. Also, participants who responded to this survey did not reflect wider SCI/D population statistics in terms of race and ethnicity with 89.5% of participants identifying as white compared to the national SCI/D population which is 58.9% white (NSCISC, 2020). This is most likely a result of the sample majority being from a localized region in the Midwest which impacts generalizability of the findings.
Conclusion
Despite improved initial survivorship after SCI/D, SHC are prevalent and often preventable issues within the SCI/D community which lead to increased health costs, premature death, and decreased functional performance within the community. Gold standard SM programs have been trialed with limited success within the SCI/D population, which points to the need for an SCI/D-tailored SM program. Based on these findings, telehealth implementation, addressing psychological health and coping, and group discussions with other persons with SCI/D could reduce barriers to SCI/D engagement in SM programs and have the potential to improve the success of these programs within the SCI/D population.
Implications and Next Steps
Using the responses from this survey, next steps include the development of a tailored SM program for the SCI/D population to be trialed via telehealth with a strong psychological health component. This study highlighted the critical need for a community-based SM program for persons with SCI to reduce the presence and severity of SHCs impacting functional performance, health and well-being, quality of life, and community participation. Stakeholders in this study indicated that an SCI-tailored SM program should incorporate both group and one-on-one meetings to address SM. This telehealth intervention however should use frameworks such as Rhon et al.’s (2022). Template for the Intervention Description and Replication (TIDieR) throughout the development and trial phase to ensure that replicability is achievable. With a growing network of telehealth practices and national profession organizational support, occupational therapists are well-equipped to implement such interventions which target the underlying mechanisms and barriers to successful SM for the SCI/D population and incorporate the necessary contextual factors which impact functional performance within the community.
Supplemental Material
sj-docx-1-otj-10.1177_15394492231183627 – Supplemental material for Needs Assessment of Self-Management for Individuals With Chronic Spinal Cord Injury/Disease
Supplemental material, sj-docx-1-otj-10.1177_15394492231183627 for Needs Assessment of Self-Management for Individuals With Chronic Spinal Cord Injury/Disease by Bridget Kraus and Timothy J. Wolf in OTJR: Occupational Therapy Journal of Research
Footnotes
Acknowledgements
The authors thank our participants for their time and input in completing this study. B.K. also thanks the University of Missouri-Columbia, Department of Occupational Therapy, Tim Wolf, Rachel Proffitt, Bill Janes, Stephanie Reid-Arndt, and Anne Sales for their consistent mentorship, expertise, and support while in the pursuit of this study and beyond.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was approved as exempt by the Institutional Review Board at the University of Missouri (IRB # 2061503). Funding for Open Access publishing is supported by the University of Missouri Spinal Cord Injuries/Disease Research Program.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
