Abstract
Acute limb ischemia (ALI) is the sudden onset of decreased blood supply to the extremities and carries a poor prognosis for the affected limb and survival. A rare but well-recognized embolic etiology is a paradoxical embolism, the translocation of a thrombus from venous to arterial circulation through an intracardiac communication, most commonly a patent foramen ovale. The presentation of ALI secondary to a PFO-mediated paradoxical embolism is most often accompanied by combinations of deep vein thrombosis (DVT), pulmonary embolism (PE), and an acute cerebral or visceral ischemia. We present the first documented case of a Rutherford class I ALI secondary to a PFO-mediated paradoxical embolism, ipsilateral DVT, and PE in a 29-year-old female who was surgically managed for her disabling claudication rather than limb salvage. The overlapping presentation of a viable ALI and ipsilateral DVT created a challenging clinical diagnosis. Our review of the literature on PFO-mediated paradoxical emboli involved 43 reports including 51 patients with various arterial thromboses; 19 of these cases involved lower extremity ALI. This case report is the first case to date that demonstrates a paradoxical embolism causing acute lower extremity ischemia with ipsilateral DVT and no additional limb/visceral ischemia to suggest the diagnosis of ALI. We also highlight the role that quality of life plays in vascular surgical decision-making, extending ALI management goals to not only reducing mortality and major amputations, but also improving quality of life.
Keywords
Introduction
Paradoxical embolism refers to the translocation of a thrombus from the venous circulation to arterial circulation through an intracardiac communication, most commonly a patent foramen ovale (PFO). 1 (15–35)% of the adult population have PFO’s and paradoxical emboli most commonly manifest as cerebrovascular accidents, although acute limb ischemia is a much rarer but well-recognized manifestation.2,3 We present the case of a 29-year-old female with a left popliteal vein thrombosis (a deep vein thrombosis (DVT)), sub-massive pulmonary embolism (PE), and concurrent Rutherford grade I acute limb ischemia (ALI), which was due to thromboembolism to the left popliteal artery and tibioperoneal trunk through a previously silent PFO. The patient’s DVT presentation overlapped with her Rutherford grade I ALI, rendering the clinical presentation of her ischemic leg complex and inconspicuous. There were no additional acute limbs or viscera on presentation that suggested an arterial thromboembolic event, which commonly occurs in paradoxical emboli.4–7 Initially, a non-surgical strategy was employed because the patient’s leg was viable and there was an increased perioperative risk of morbidity and mortality from her heavy PE burden. However, the patient quickly developed disabling claudication, present on short-distance ambulation, so a multidisciplinary decision was made for a surgical thrombectomy to improve this young patient’s quality of life as opposed to limb salvage.
This case report: 1) adds to the existing scarce literature on lower extremity ALI secondary to paradoxical emboli; 2) recommends a high index of suspicion for paradoxical embolism in young patients with PFO’s and an unknown embolic source, particularly in the face of overlapping clinical features of a viable ALI with ipsilateral DVT; 3) presents the first case of a paradoxical embolism causing acute lower extremity ischemia with ipsilateral DVT and no concurrent arterial ischemia to clinically corroborate the diagnosis; and 4) highlights the vital role that patient characteristics and quality of life plays in vascular surgical decision-making.
Case Report
This is a case of a 29-year-old female with a history of recurrent pulmonary emboli (post-partum, post-flight), obesity (BMI 50.7), stable hypothyroidism, bipolar disorder on lithium, obstructive sleep apnea, asthma, active cigarette smoking, and daily marijuana use. The patient’s father had a PFO with DVT, PE, and a stroke. The patient’s grandmother suffered from a stroke and other undocumented clotting events. There is a family history of miscarriages.
Since her first pulmonary embolism (PE) six years ago, she was placed on lifelong anticoagulation therapy with warfarin and later rivaroxaban 20 mg daily. She was recently admitted for an incarcerated umbilical hernia repair, for which she discontinued her rivaroxaban three days pre-operatively. For the duration of those three days, she declined receiving unfractionated heparin or other forms of anti-coagulation. Although she began to notice intermittent mild left leg cramping, she did not seek any medical attention. She resumed her rivaroxaban on discharge. Six weeks post-operatively, she presented to the emergency department (ED) complaining of mild shortness of breath. She was discharged with a 5-day course of prednisone and puffers. She returned to the ED the following day with new left leg pain and swelling. Venous doppler ultrasound demonstrated a small non-occlusive thrombus in the left popliteal vein spanning 3.5 cm (Figure 1). Unfortunately, the patient left against medical advice and ran out of her rivaroxaban for two days, until she returned to the ED with worsening chest discomfort and lower left leg pain with numbness/paresthesia. She was dyspneic, tachycardic, tachypneic, and hypoxic, saturating at 87% on room air which worsened with exertion. (A) gray-scale duplex ultrasonography of the left popliteal vein with a 3.5 cm thrombus (indicated by the red arrow); (B) color duplex ultrasonography of the same 3.5 cm non-occlusive thrombus as a filling defect indicated by the red arrow.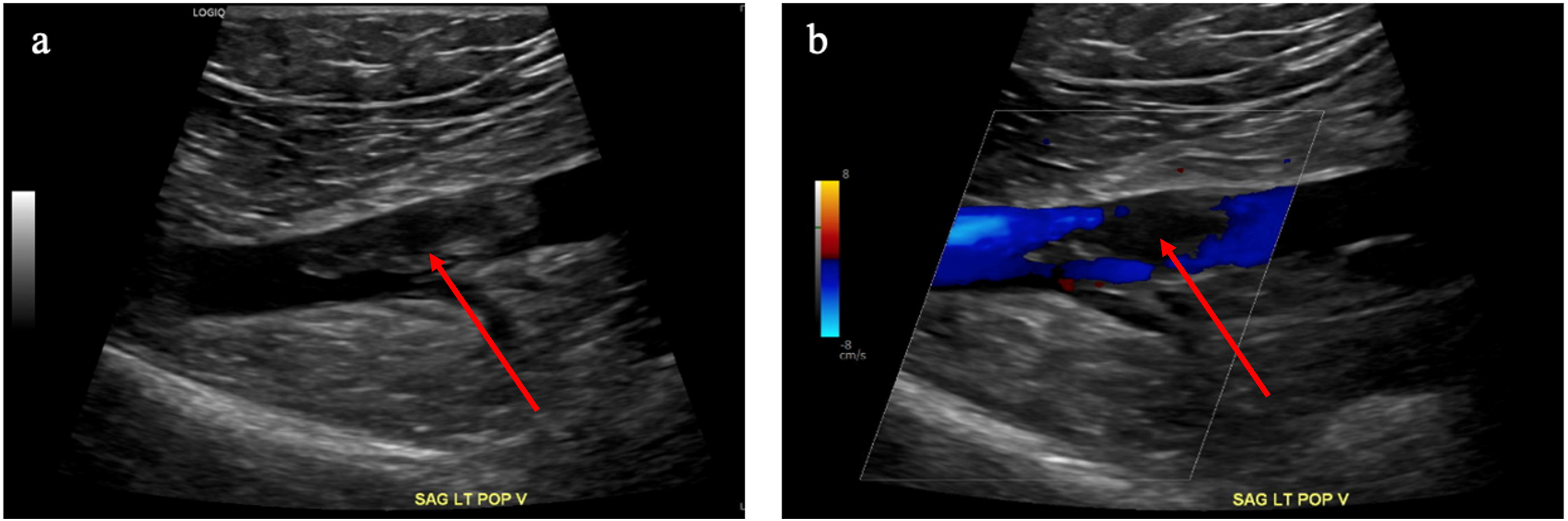
Given her symptoms, a CT pulmonary angiography was done, which demonstrated sub-massive bilateral PE’s (Figure 2). She was placed on intravenous (IV) heparin infusion and later transferred to the intensive care unit for close monitoring of her poor cardiopulmonary status. A transthoracic echocardiogram demonstrated right ventricular dysfunction and a PFO with right to left shunting via agitated saline contrast injection, and measuring 1.75 cm. A cardioembolic workup consisting of an electrocardiogram, echocardiogram, and Holter monitor was negative. A hypercoagulable workup was negative for anti-phospholipid antibody syndrome and no abnormalities in Protein C, Protein S, or antithrombin III. (A) Computed Tomography Pulmonary Angiography coronal section demonstrating a left main pulmonary artery embolus (red circle); (B) (A) sagittal section demonstrating the left main pulmonary artery cross-section with luminal embolus (red circle); (C) (A) coronal section demonstrating a right main pulmonary artery embolus (red arrows).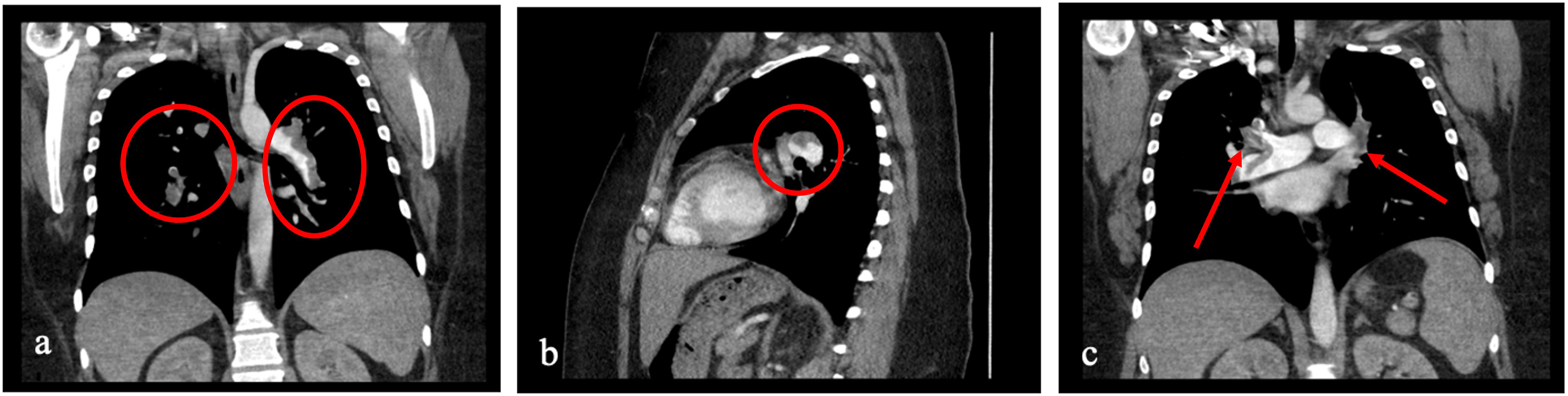
The Vascular Surgery service was consulted to evaluate her leg pain. The patient’s physical examination was remarkable for left calf tenderness on palpation as well as mild numbness/paresthesia to the left foot. There was no motor dysfunction and pedal pulses were palpable bilaterally. Clinically, the patient’s symptoms were in keeping with a DVT, especially given her PE, recent anticoagulation discontinuation, and history of recurrent (venous thromboembolic events (VTEs). However, computed tomography (CT) angiography examining the patient’s lower extremity vessels demonstrated an occlusion of the left popliteal artery and tibioperoneal trunk over a length of approximately 15 cm, with reconstitution and three vessel runoff (Figure 3). There was abundant collateralization visualized on CT. There was also a short segment occlusion of the left profunda femoris artery spanning 4 cm immediately upstream of the second perforating artery (Figure 3(E)). An angiogram was also completed, confirming the findings of the CT (Video 1). Despite her risk factors (smoking, elevated BMI), significant atherosclerosis was not noted on her peripheral vessels. Given the physical examination findings and investigations, it is highly likely that her ischemia was acute-on-chronic. The patient was classified as Rutherford I ALI and remained on heparin for 7 days. Operative management was recommended against initially, as her leg was viable and she had an increased perioperative risk of morbidity and mortality secondary to heavy pulmonary embolus burden. (A) CT angiogram axial section above the level of the distal SFA/popliteal occlusion; (B) coronal section demonstrating the popliteal artery before occlusion; (C) axial section at the level of the popliteal occlusion, with evidence of the patient’s ipsilateral DVT (red arrow); (D) coronal section at the level of the popliteal occlusion, again with evidence of the patient’s ipsilateral DVT (red arrow); (E) axial section of the profunda femoris arteries, within a 4 cm occlusion of the left profunda femoris artery (red arrow) just superior to the second perforating artery; (F) axial section demonstrating distal reconstitution and three-vessel runoff to the left ischemic leg.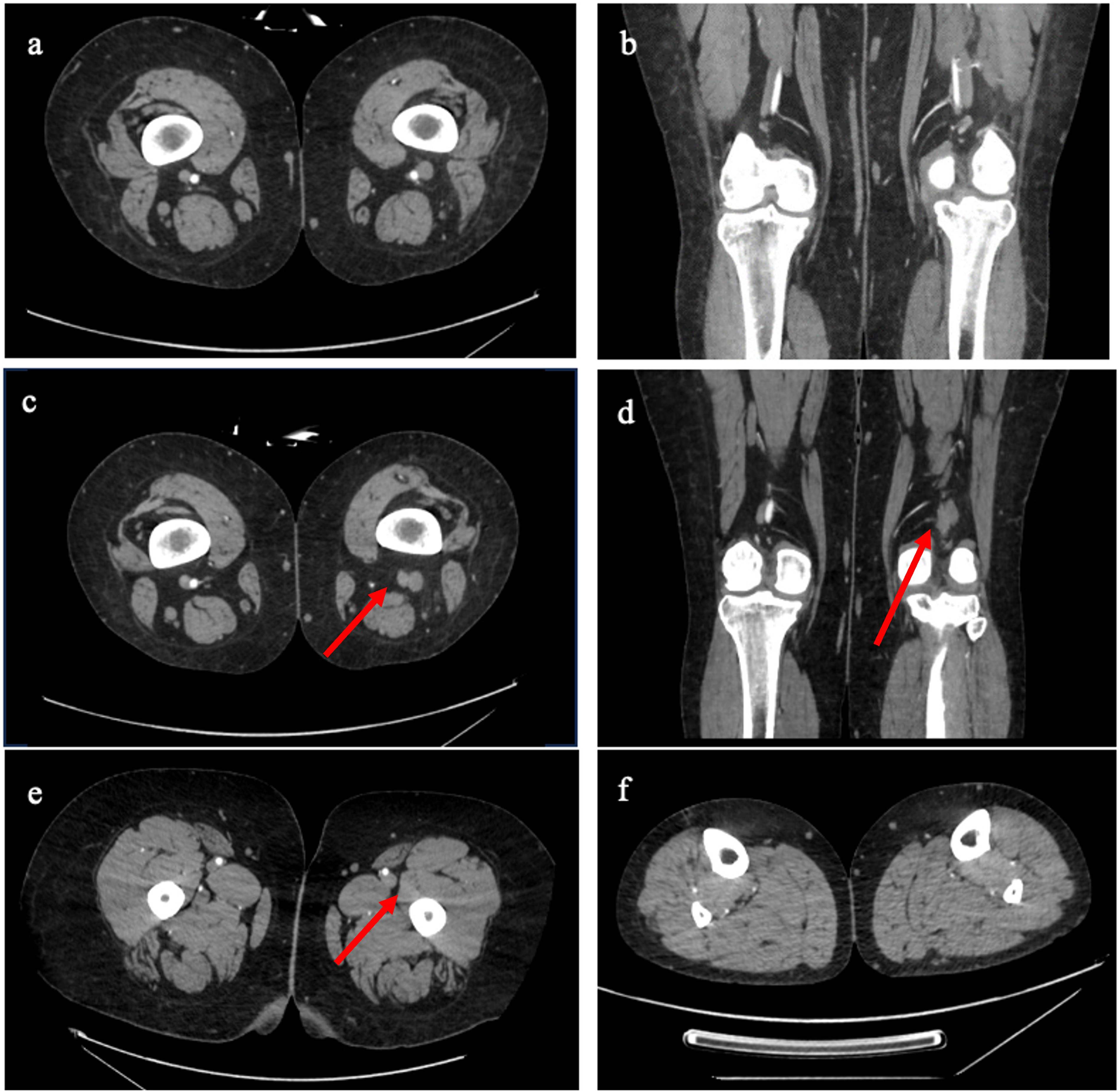
After 7 days of anti-coagulation, and during the same admission, the patient’s left leg symptoms worsened, with ascension of numbness/paresthesia above the ankle. The patient had no symptoms or signs of compartment syndrome and there were no motor deficits or tissue loss. Importantly, she was left with severe short-distance claudication, which was worst in her left hamstring. From a vascular surgical perspective, the patient was left with significant vasculogenic claudication secondary to a paradoxical embolism mediated by her PFO. Her limb was not immediately threatened, and her ALI was classified a Rutherford grade I. However, given her young age and marked disabling claudication, the decision was later made to revascularize with a popliteal artery embolectomy to improve her walking ability and quality of life. This decision was made in light of the increased cardiopulmonary morbidity and mortality associated with her heavy PE clot burden.
The patient was given general anesthetic, and a radial artery pressure monitoring line was inserted. A medial left thigh incision was made to expose the distal superficial femoral artery (SFA). After IV heparin was administered, a transverse arteriotomy was made and several passes of a #4 Fogarty catheter were made distally to 60 cm, obtaining abundant fresh homogenous dark red clot. There was adequate back-bleeding following the embolectomy. No clot was retrieved with proximal insertion of the Fogarty catheter and there was adequate arterial inflow. Strong palpable pulses were felt in the distal SFA and excellent quality biphasic doppler signals were audible on her hyperemic foot. A flat Blake drain was placed deep into the incision and was later removed. The patient tolerated the procedure well. She was discharged in stable condition on warfarin and will follow up with her local thrombosis clinic on an outpatient basis to determine her long-term anti-coagulation plan. She was also referred to Interventional Cardiology to further review options for the closure of her PFO.
Discussion
Characteristics of Case Reports to Date of Lower Extremity acute Limb Ischemia Secondary to Paradoxical Embolism Mediated by a Patent Foramen Ovale. ALI, acute Limb Ischemia; PE, Pulmonary Embolism; DVT, Deep Vein Thrombosis.
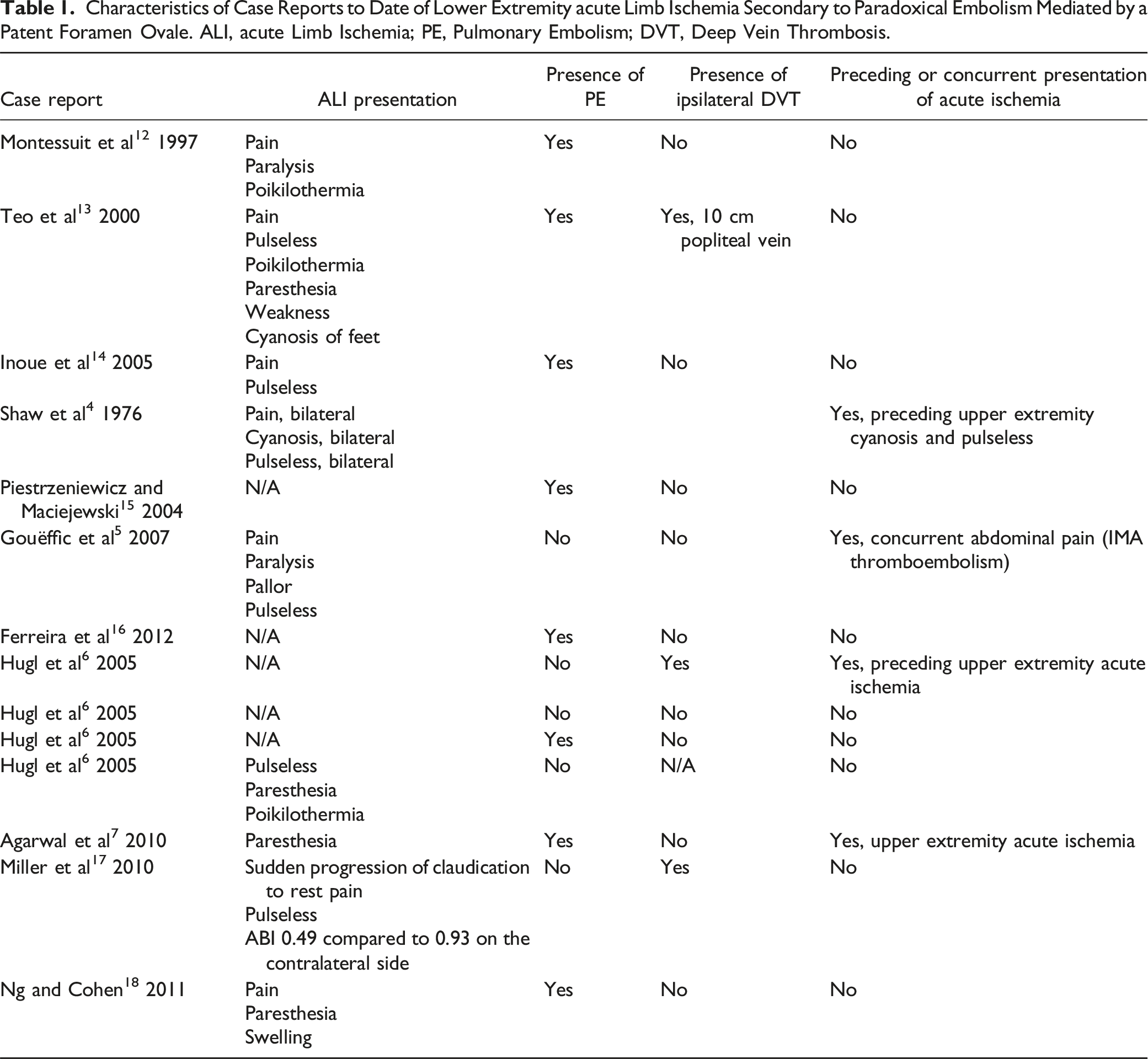
The management of ALI begins with anticoagulation (unfractionated heparin unless contraindicated) and appropriate analgesia. 19 Rutherford class I may require only medical therapy with anticoagulation; however, factors that influence treatment beyond the Rutherford classification include the duration of ALI, location and cause of ALI, the presence or absence of underlying atherosclerotic disease, and the patient’s medical condition. 9 This case highlights another vitally important factor: the patient’s quality of life. Factors pointing against the patient’s surgical revascularization included: 1) a Rutherford classification deeming her leg viable; 2) a CT angiogram displaying abundant collateralization and three vessel run-off; and 3) a heavy pulmonary clot burden increasing her perioperative morbidity and mortality risk. However, these factors were weighed against the patient’s young age and potential natural history of several decades of disabling claudication. This claudication can severely affect the patient’s quality of life and potentially deter the patient from adequate exercise and mobility, further increasing her baseline high risk of VTEs. While not used for this specific case, it is important to mention the potential applicability of percutaneous mechanical thrombectomy devices for treating leg ischemia. A device, such as ROTAREX S (Straub Medical, HI, USA), can be considered for treating acute lower limb arterial embolism. Furthermore, an inferior vena cava filter was considered for this patient, but the interventional radiology specialists deemed the patient to not be a good candidate for one.
Conclusion
In summary, the clinical diagnosis of paradoxical embolism causing ALI can be challenging, especially with an ipsilateral DVT and no additional ischemic limbs or viscera that point to an arterial ischemic event. This is an interesting case, with an isolated Rutherford class I ALI and ipsilateral DVT. Additionally, a patient’s quality of life should be evaluated and seriously considered in the vascular surgical decision-making process, in addition to limb prognosis (i.e., Rutherford classification), the location and cause of ALI, the presence of atherosclerotic disease, and the patient’s medical condition.
Supplemental Material
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
