Abstract
Purpose:
This study aimed to identify determinants that promote the initiation and maintenance of complete decongestive therapy (CDT) as well as effective strategies for mitigating barriers to self-management of lymphedema among breast cancer survivors.
Methods:
A descriptive and qualitative design was used. In-depth interviews were conducted with 13 breast cancer survivors who were managing breast cancer-related lymphedema. Interviews were transcribed verbatim. An iterative descriptive data analysis method was employed to examine the data, compare codes, challenge interpretations, and inductively identify themes.
Results:
A realization that lymphedema requires daily self-management was the primary determinant leading breast cancer survivors to initiate CDT self-management. The determinants for maintaining daily CDT self-management included the perceived effectiveness of CDT, being willing to assume accountability, and perceived efficacy to undertake CDT. Developing strategies to integrate CDT regimens into daily life is key to maintaining CDT self-management of lymphedema. Three core concepts mediate initiation and maintenance of CDT self-management: understanding lymphedema as a chronic condition that can be managed with CDT self-management, being worried about lymphedema exacerbation, and having support from patient peers and family.
Conclusions:
Interventions should be tailored to promote the initiation and maintenance of CDT self-management. While clinicians provided knowledge-based and clinical skills-based information, patient peers provided daily life examples, and real-life implementation strategies for CDT self-management. Ongoing patient-provider and patient-peer communication functioned as effective support for maintaining CDT self-management. Reliable and realistic methods of symptom self-assessment are important for maintaining CDT at home.
Introduction
More than 18 million cancer survivors are living in the United States. That number continues to grow, and is projected to top 22.5 million by 2032. 1 There are approximately 4.1 million breast cancer survivors in the United States, with a 90% 5-year relative survival rate. 2 With the growing number of survivors and the shortage of healthcare specialists, the long-term demands for survivorship care are a substantial burden for individuals and healthcare systems.3,4 Cancer and cancer treatment cause side effects, and long-term effects on survivors can differ significantly from person to person, necessitating a patient-centered approach to caring for cancer survivors. 5
Lymphedema is a major late and chronic effect of breast cancer treatment, most commonly resulting from removal of the lymph nodes and damage to the lymphatic system from surgery and radiation. 6 Lymphedema can develop at any time following cancer treatment. Conservative estimates indicate lymphedema occurs in 20% to 40% of breast cancer survivors. 7 The disruption of lymph drainage leads to chronic swelling, pain, heaviness, and decreased range of motion in the upper limbs.8,9 The chronic symptoms and distress of lymphedema affect an individual’s physical functioning, self-esteem, and social activities, and leads to poor quality of life (QOL).10,11 Complete decongestive therapy (CDT), considered the gold standard of non-surgical care, reduces volume of swelling limbs, controls infection, and manages fibrosis, thereby improving functioning and QOL. 12 CDT consists of daily manual lymphatic drainage, application of compression bandages and garments, remedial exercise, and skincare. CDT requires daily self-management practices throughout the survival years.13,14 Patients frequently visit lymphedema therapists for CDT and apply bandages for at least 23 hours every day during an 8-week intensive phase before transitioning to the maintenance phase of routine CDT self-management at home. 13
Self-management of lymphedema creates significant challenges for survivors hoping to return to their normal routines.15 -17 Lymphedema self-management adherence is not optimal.18,19 Inconsistent management often leads to dysfunction, serious complications, and poor QOL.12,15 Barriers to lymphedema self-management are associated with a lack of lymphedema education and support, a lack of support for emotional regulation and self-efficacy, limited access to medical resources, and a lack of workplace and societal understanding and support.15,20 Family caregivers’ support is associated with improved functioning and QOL of lymphedema patients, 21 though studies examining how caregivers coordinate home care of lymphedema among cancer survivors are limited. Survivors with a recent diagnosis of lymphedema are more likely to report challenges performing CDT than those who have been managing lymphedema for decades.20,22,23 Balancing self-management and other daily tasks (eg, working) is essential in the adherence of lymphedema self-management.15,24,25
Self-management involves treating patients as partners in their own care, which is central to patient-centered care and a key component in the Chronic Care Model (CCM).26 -28 Patient activation, a key indicator of self-management in the CCM, is defined as the patient being ready, willing, and able to engage in health behavior change and management of their health. 29 Patient activation is strongly related to a broad range of patient health and utilization outcomes, such as addressing unhealthy behaviors, reducing hospitalization incidence, and lower medical costs.30 -32 A growing body of literature indicates that activated patients make more effective use of resources and are more likely to engage in positive health behaviors than their peers. 33
The barriers and behavioral determinants associated with patient initiation and maintenance of lymphedema self-management are not fully understood. Behavioral determinants reference factors that influence behavior change, such as knowledge, attitudes, values, skills, etc. This study aimed to identify behavioral determinants that promote the initiation and maintenance of complete decongestive therapy (CDT) as well as effective strategies for mitigating barriers to self-management of lymphedema among breast cancer survivors.
Methods
Design
We used a descriptive and qualitative approach that acknowledges various shared experiences of individuals and human interactions.34,35 This method allowed breast cancer survivors to describe their experiences of initiating and maintaining CDT self-management of lymphedema. This study was approved by the Institutional Review Board at a public university in the Midwest region of the United States.
Participants and Recruitment
We utilized a purposive and maximum variability sampling method to recruit participants who had a broader range of experiences with CDT self-management of lymphedema. Interviews with breast cancer survivors with lymphedema at different stages of CDT self-management (eg, those who had just started learning self-management, those who had managed lymphedema for 1 year, and those living with lymphedema for over a decade) allowed for detailed explications of determinants for initiating and maintaining CDT self-management. Inclusion criteria were women who (1) were diagnosed with lymphedema following breast cancer treatment, (2) were more than 6 months beyond the surgery, (3) were introduced to CDT self-management by a lymphedema therapist, (4) were willing and able to participate in face-to-face interviews, and (5) were able to speak English. Study flyers were posted at breast cancer support groups, survivors’ events, and local lymphedema clinics in a Midwestern United States city. Eligible and interested patients were instructed to contact the first author through email and phone; those meeting the inclusion criteria were invited to participate.
Data Collection
An investigator-developed, structured survey was created and administered to each participant in person, which was followed by a 60-minute face-to-face interview. The pre-interview survey includes demographic information (eg, age, education, occupation, social support, etc.) and clinical information (eg, breast cancer survival time, date of lymphedema diagnosis, symptoms, etc.). The level of social support was measured using a 5-point Likert scale, which included “no support or potential support is available,” “given or potentially available from family and friends (above average),” and “much support is either given or is available from family and friends (high degree).” The face-to-face interview involved questions focusing on participants’ experience of CDT self-management and coping strategies. Thematic saturation of coding categories occurred after 13 interviews. 34 Interviews were conducted by the first author and audio-recorded. A reflective journal and field notes were maintained throughout the course of the study to document any unusual observations, confusion, and possible bias during the data collection process.
Data Analysis
Demographic and clinical data were summarized using descriptive statistics (median, percentage). Each interview was transcribed verbatim and proofread by one researcher (YS). A 7-step descriptive data analysis method was used to examine transcripts, compare codes, challenge interpretations, and develop themes inductively.35 -38 The steps included: (1) reading the transcripts multiple times to develop an overall understanding of the text, (2) 3 researchers (YS, MRF, YJ) working as a group to identify key quotations and discuss key codes related to the research question, (3) integrating the coded quotations into one document and checking the accuracy of the codes and quotations, (4) thoroughly analyzing coded quotations to identify major themes and subthemes by collating key quotations for each research question, (5) 3 researchers (YS, MRF, YJ) working as a group to review themes and engaging in active dialog to resolve discrepancies, (6) reviewing the transcripts and validating the structure of themes alongside interviews, and (7) researchers (YS, MRF, YJ, AL) discussing and reaching consensus on each aspect of the data analysis. A web-based software, Dedoose Version 7.0.23, 39 was used to perform the analysis.
Rigor and Trustworthiness
To ensure the study’s rigor, we applied Lincoln and Guba’s 40 4 criteria: credibility, transferability, dependability, and confirmability. We conducted reflective journals, field notes, and verbatim transcriptions and checked transcripts’ accuracy against recordings to establish credibility. Detailed descriptions from participants provided transferability. The emergence of similar data from different participants supported the reliability and dependability of the data. Member checking, interrater reliability, and consensus regarding results among researchers supported confirmability.
Results
Participant Characteristics
Thirteen breast cancer survivors who were diagnosed with lymphedema were enrolled in this study. The time-since-diagnosis of lymphedema ranged from 1 month to 25 years. The majority (12/13, 92%) of the participants resided in the central Midwest of the United States. All participants were employed at the time they initiated CDT self-management, and about 77% had employer-based medical insurance. About half lived with a partner and reported having social support. Table 1 presents the participants’ demographic and clinical characteristics.
Demographic and Clinical Characteristics (N = 13).
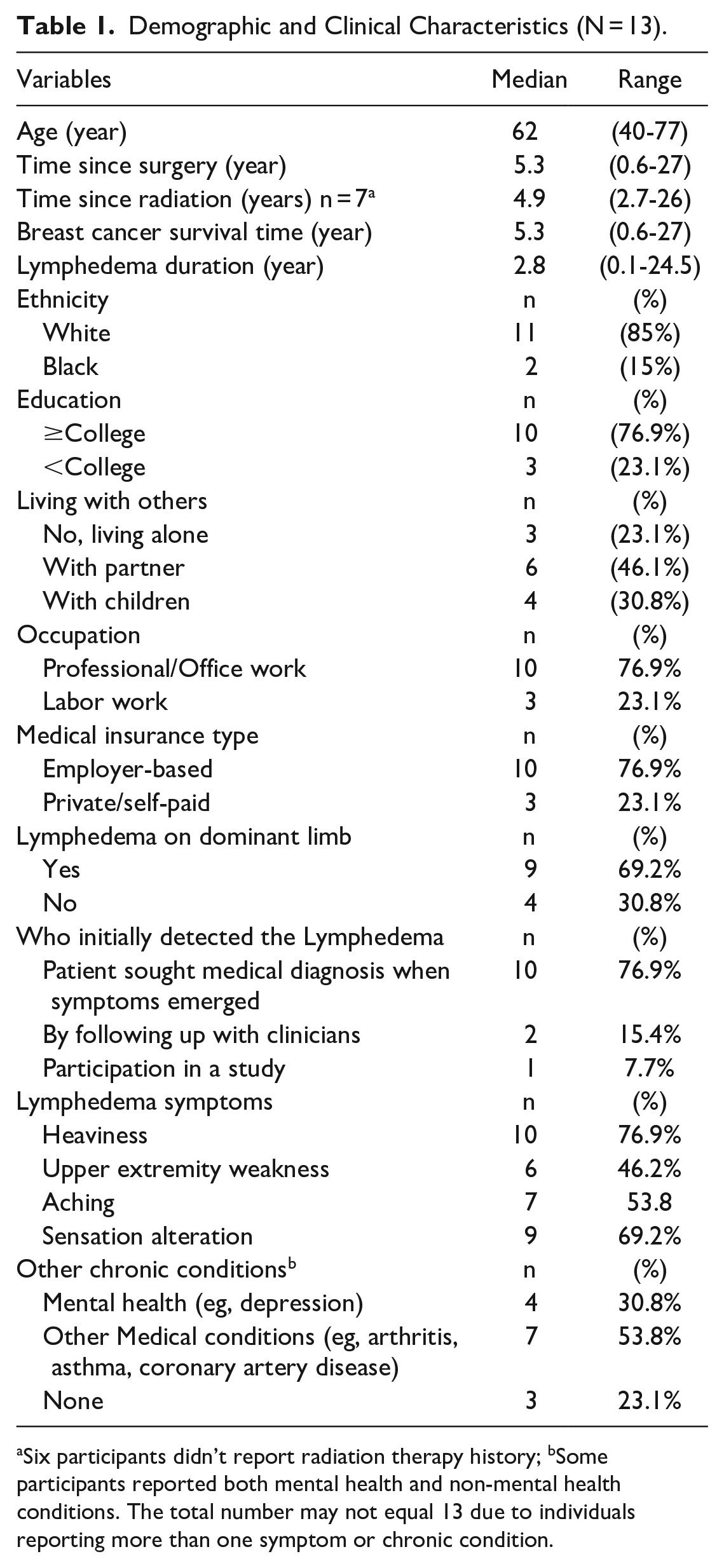
Six participants didn’t report radiation therapy history; bSome participants reported both mental health and non-mental health conditions. The total number may not equal 13 due to individuals reporting more than one symptom or chronic condition.
Findings
Several essential themes emerged that reflected determinants of CDT self-management of lymphedema (Table 2). A realization that lymphedema requires daily CDT self-management was the primary determinant leading breast cancer survivors to initiate CDT self-management. The determinants for maintaining daily CDT self-management included the perceived effectiveness of CDT, being willing to assume accountability, and perceived efficacy to undertake CDT. Developing strategies to integrate CDT regimens into daily life is key to maintaining CDT self-management. Three core concepts mediate initiating and maintaining CDT self-management: understanding lymphedema as a chronic condition that can be managed with CDT, being worried about lymphedema exacerbation, and having support from patient peers and family (Figure 1).
Themes and Representative Quotes.

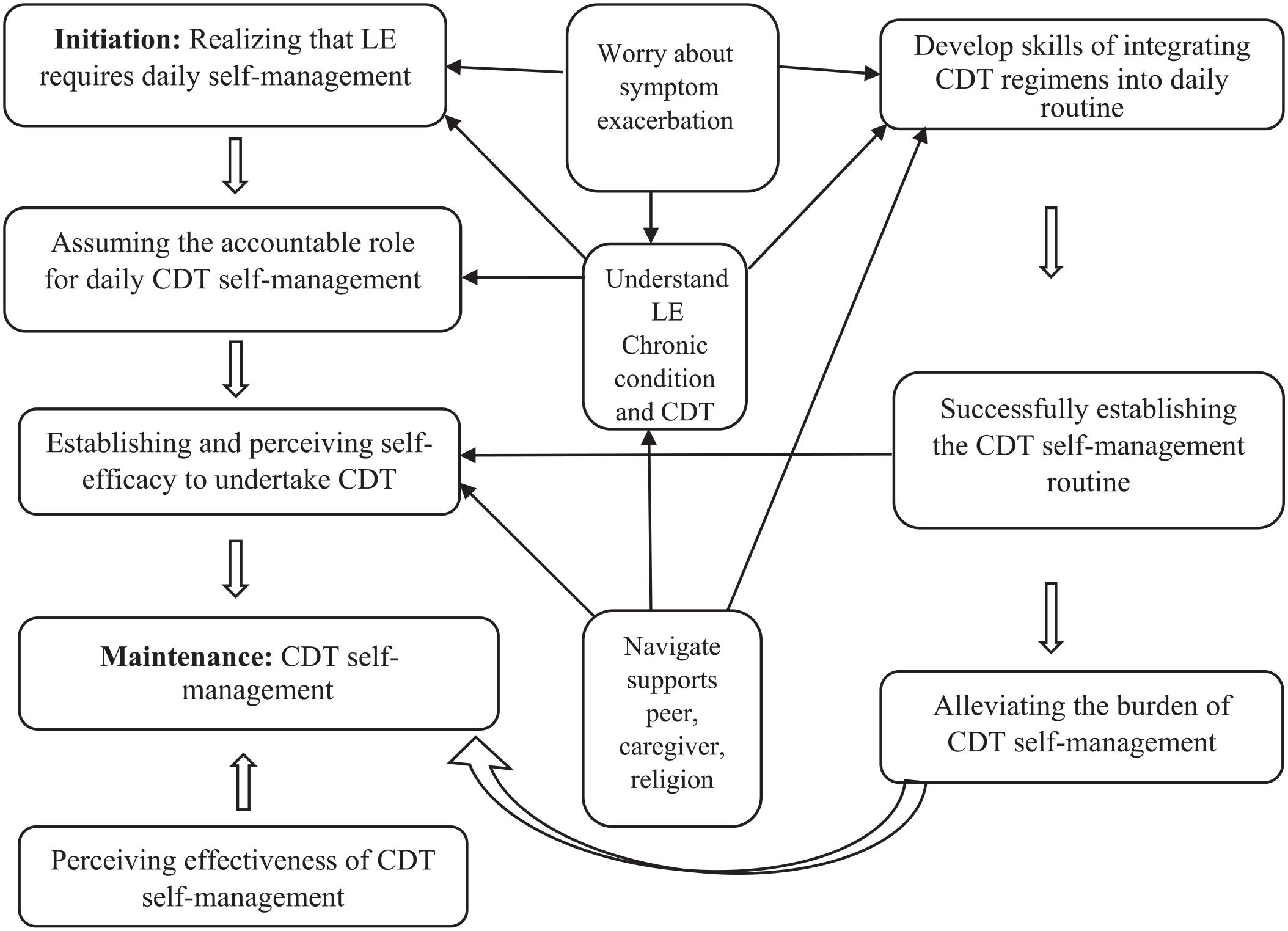
Concept map of the determinants of initiating and maintaining lymphedema self-management.
Determinants for Initiating CDT Self-Management
A realization that lymphedema requires daily CDT self-management was the primary determinant leading breast cancer survivors to initiate CDT self-management
Participants understood the necessity of self-management when they accepted that lymphedema is a chronic condition that was “not going away” and must be managed consistently. “I’ve learned to adapt to the fact that I have lymphedema. And it’s just a constant thing I have to make myself daily aware of. It’s not going away. It’s like if a person has kidney problems or if a person has high blood pressure or if a person has Crohn’s disease. I had cancer, something that I had to deal with” (8). Understanding the importance of daily lymphedema self-management occurred when women experienced the negative consequences of not performing self-management and suffered function impairment and distressing symptoms. One participant (10) shared she thought “it’s not really that big of deal” when first diagnosed with lymphedema, and only realized the importance of self-management as symptoms progressed and became “completely life invasive.” Quite a few participants (1, 2, 6, 8, 9, 10, 12, 13) perceived that lymphedema impaired their functioning at work and in social activities, which was one of their cues to initiate self-management. As the symptoms progressed, their understanding of self-management grew. One said, “when I’m having more problems, I just become more aware of what I am doing” (Participant 8). For example, some participants (5, 6, 8) who experienced cellulitis, one of the most serious complications of lymphedema, reported worrying about lymphedema “going out of control,” which is frightening if “don’t know how to handle it.” They were more cautious and diligent in CDT skin care and infection control.
Determinants for Maintaining CDT Self-Management
The determinants for maintaining daily CDT self-management included the perceived effectiveness of CDT, being willing to assume accountability, and perceived self-efficacy to undertake CDT. Developing strategies to integrate CDT regimens into daily life is key to maintaining CDT self-management. Three core concepts mediate initiation and maintenance of lymphedema CDT self-management: understanding lymphedema as a chronic condition that can be managed with CDT, being worried about lymphedema exacerbation, and having support from patient peers and family caregivers.
Perceiving the effectiveness of CDT self-management in mitigating distressing symptoms and improving functions was essential in maintaining daily self-management
One participant said, “They (compression bandages) help me. If I would wear mine a little bit more often, I would probably do better myself” (Participant 9). Perceiving the effectiveness of lymphedema self-management could outweigh the discomfort and inconvenience of performing self-management. Though she (9) feels “smothered most of the times” and would prefer not to wear the bandages, she did so “because they do help.” Others were willing to tolerate the heaviness of the garments “as long as it keeps the swelling down” (12). Eventually, participants realized self-management was important to functioning normally. For example, 2 participants (8 and 10) stated they “struggle to function” when they did not perform self-management, which convinced them that they needed to wear compression sleeves and practice manual drainage.
For survivors with newly diagnosed lymphedema, lack of understanding that self-management needs time to show results led to discouragement and inconsistent CDT self-management. One participant who had just started CDT was disappointed when she did not see outcomes: “I would wake up feeling kind of defeated, like I’ve done this all day long and my arm still was bad” (13). While patients with recent diagnoses were discouraged by not seeing immediate changes, long-term patients were frustrated by the intermittency of symptoms and would discontinue self-management until visible threats returned. A participant (6) who had lymphedema for 2 decades would “give up on the wraps and say ‘I’m just not gonna worry about it’” when the swelling came back, only starting CDT self-management when serious complications (infections) occurred. Importantly, participants expressed the challenges of monitoring the progression of lymphedema at home, which affected their motivation in maintaining CDT self-management. “I don’t know if they are really working” (1). One participant (7) suggested that getting “a baseline check of the arm” would be important to know if the lymphedema had progressed or not.
Assuming accountability for daily CDT self-management was the foundation for establishing self-efficacy and maintaining CDT self-management
Survivors who had activated and sustained self-management behavior understood the importance of assuming accountability for their self-management. As one participant said, “It’s just something that I had to deal with and learn to deal with it. We have to educate ourselves and look after ourselves. We can’t expect somebody else to do it for us” (8). Their realization that they had to assume accountability was based on their understanding of lymphedema’s chronic nature and what self-management requires. One participant said, “you have to take care of yourself. You can’t just ignore it and hope it will all go away cause it’s not going to” (3). When survivors assumed accountability in self-management, they started to consciously prioritize it: “This is part of my job right now is taking care of my health. And because I treated it that way, it was so much easier to deal with” (5).
Perceived self-efficacy leads to adherence to CDT self-management
A good understanding of CDT and obtaining peer and family support were essential for breast cancer survivors in developing self-efficacy in CDT self-management. Some participants reported being exhausted by large amounts of information and intimidated by the complexity of lymphedema self-management, especially participants who were newly diagnosed (2, 12, 13). Survivors expressed a need to be guided during this transition to help convince themselves that they could conduct CDT on their own. They felt that knowing both the short-term and long-term commitments of lymphedema self-management would ease their fears. Participants were intimidated by the prospect of wearing compression bandages 23 hours a day, but found it was “helpful to understand the scheme of things” (13), in particular the fact that it is only the intensive phase of CDT that “is very aggressive and (involves) wrapping a lot.”
Survivors who activated self-management usually came to believe “I can do it” through different avenues. Some stated that clinician’s explanations of therapy relieved their fears and anxiety about lymphedema self-management. Many participants (1, 3, 4, 5, 7, 13) gained confidence by communicating with peers in the survivorship group. A participant (13) stated, “When I started listening to other people’s stories, I could take it much better.” She felt that her peers’ experiences were valuable to her and provided practical strategies for incorporating lymphedema self-management into daily life. “You have to see the perspective of everybody’s dealing with something. Talking about what it is, how it fits into your life, how I deal with this.” These practical tips were seen as complementing the more structured information provided by clinics. “If your clinician you can’t understand, maybe you should talk to other people and say, ‘this is what Jen did, here how I was before, here are my measurements after, here’s what I did could help. (Participant 13).” Relationships with peers not only helped her develop implementation strategies but supported her mental preparation as she came to understand “the scheme of things” when initiating lymphedema self-management. Family members such as partner, parents, and close friends were important sources of support for CDT self-management, including providing assistance with CDT bandaging, taking over other responsibilities (eg, housekeeping, walking dogs), and giving emotional support and motivation. Family support was identified as extremely helpful, especially in the early stages of learning lymphedema self-management and during the intensive phase of CDT therapy. However, family support was only reported as available to less than half of the interviewed participants. Two participants (9, 12) also relied on their religious beliefs “for strength.”
Developing strategies to integrate CDT regimens into daily life is key to maintaining CDT self-management
Participants built skills and creatively integrated lymphedema self-management behaviors into daily activities, which helped them successfully establish a self-management routine and reduce the burdens of self-management. Participants who successfully integrated self-management into their daily lives often improved their time-management and organizational skills and developed strategies for adapting lymphedema self-management appliances to different activities. One participant (13) restructured her day to manage lymphedema by showering in the morning instead of the evening, thus allowing a longer block of time for wearing compression bandages. She assigned self-management tasks to several slots throughout the day to allow self-management activities while keeping up with other responsibilities.
Scheduling CDT self-management activities around other tasks was used by quite a few participants in developing routines. For example, an office clerk said, “Every morning when I get up, I go through all of them (the CDT element). And during the day, I will do the stretching, lean and different exercises trying to keep things moving. At work too sometimes, I stretch. Periodically through the day” (1). A fitness instructor rescheduled her classes to the early morning to allow her affected arm to be compression bandaged for the rest of the day (8). A teacher also used lunch breaks for rebandaging (11). A hospital technician kept a compression sleeve in her back-pocket and put it on when she had breaks at work (4). And a businesswomen tailored her workday around lymphedema self-management and completed CDT exercises during breaks (10).
Some survivors found ways to accommodate lymphedema appliances in different situations during the day. An ornithologist shared, “I prefer my nighttime sleeve on when I’m working just because it has more cushion. If I’m writing, then I need to put on my customized sleeve, so I can type. If I’m just doing like point and click the type of stuff, I can have the nighttime sleeve on. And if I’m working out, I wear the ones that for more active” (5). Similarly, one participant wore less-bulky compression sleeves to work and used bandaging when at home (13).
Once a routine was established and self-management became a part of daily life, participants found the burdens of self-management lightened considerably. One participant said, “It takes some time. But I think once you get used to it, it just becomes part of your routine. Once you do things so many times, it just becomes a habit. Like in the morning I got up, I put my sleeve on. It wasn’t even something I had to consciously think about, where in the beginning it was like I gotta put my sleeve on” (3). A participant who had managed her lymphedema for 2 decades considered the compression garments as part of her regular clothing when she dressed (4).
Discussion
This study presents the determinants for the initiation and maintenance of CDT self-management. Realizing that lymphedema needed daily self-management was the primary determinant for breast cancer survivors to initiate CDT. The determinants for maintaining daily CDT self-management included perceiving the effectiveness of self-management, assuming accountability and perceived self-efficacy to undertake the necessary activities of CDT. Developing strategies to incorporate CDT regimens into daily life was the key to maintaining CDT self-management. Three key concepts mediate initiating and maintaining CDT: understanding that lymphedema is a chronic condition, being worried about lymphedema exacerbation, and navigating support from patient peers and family.
Mediate Concepts of Initiating and Maintaining CDT Self-Management
The findings of the study provided a foundation for conceptualizing the CDT self-management model, as shown in Figure 1. Three key concepts mediate the initiation and maintenance of lymphedema self-management: understanding that lymphedema is a chronic condition, being worried about lymphedema exacerbation, and navigating support from patient peers and family caregivers. Understanding lymphedema is “not going away” as a chronic condition is the first step for accepting the need for long-term management of lymphedema and assuming the accountable role for self-management. Accepting the fact that lymphedema “is not going away” and needs long-term care, survivors assumed their responsibility for lymphedema self-management. Thus, the rationale of “not going away” is the basis for survivors to initiate lymphedema self-management and actively develop the skills and routine for the care. Once they assume responsibility, the self-efficacy of CDT self-management improves. Personal worries caused by lymphedema influence an individual’s perceived priority of lymphedema self-management. Worrying about the worsening of symptoms, they started taking lymphedema self-management seriously, and “to do everything” (eg, developing CDT self-management skills) they can “try to keep it from progressing.” With the symptoms out of control, survivors even feel frightened if “they don’t know how to handle (manage) it.” Support from patient peers and family caregivers promotes understanding of the “scheme” of the CDT self-practice, enhances an individual’s self-efficacy, and facilitates their skill development of integrating CDT self-management into daily routines. Once people developed skills and routines, maintaining CDT self-management became less burdensome. With lessened symptoms, participants realized CDT self-management was important to functioning normally and were motivated to continue the practice. Participants’ quotations from Table 2 support the mediate concepts.
CDT Self-Management Education
Our findings suggest that a person’s understanding and acceptance of their chronic illness are predictors of self-management behavior. A lack of understanding that lymphedema is “not going away” could prevent survivors from recognizing the importance of: their own involvement in lymphedema self-management, having realistic expectations of outcomes, and establishing self-management habits. The findings validate studies reporting that survivors who are more knowledgeable of and confident with lymphedema management tend to have better adherence and patient outcomes. 41 These findings mirror several concepts from the health belief model, 42 which is used to promote healthy behaviors in individuals with various chronic conditions.43 -45 These cognitive determinants represent areas for educational intervention. 46
Support for the Initiation and Maintenance of CDT Self-Management
Communication with patient peers was identified by our participants as an important determinant for establishing and enhancing self-efficacy in CDT self-management of lymphedema. This implies that self-management information and training could also be effectively delivered by other patients and community members, who are valuable health care resources and whose involvement can lead to better patient outcomes.47,48 As noted, clinicians provided more clinical information, while patient peers provided live demonstrations, real-life implementation strategies, and mutual motivation. A clinician-peer-support model may provide a valuable motivation for patient activation of self-management. Additionally, our findings also validate that relationships with family caregivers are important factors when identifying barriers to survivors’ self-management of lymphedema. 49 Patient-family caregiver dyadic coping positively influenced the patient’s self-efficacy and promoted activation of the patient’s self-management of their chronic illness.31,50 More studies are needed to assess the coordination of multiple caregivers in all aspects of lymphedema home care.
Person-Centered Initiation of CDT Self-Management
Managing treatment complications, such as lymphedema, is often one of many works or cancer survivors.4,51 In this study, some survivors successfully transitioned to a new normal; that is, they practiced self-management while maintaining other life functions, including job and family responsibilities, which allowed for higher life satisfaction and better self-management. Survivors reported that only receiving printed information, which is the practice at most clinics, was insufficient education in lymphedema self-management.15,18 Beyond technique support, survivors also seek support with regulating negative emotions.15,18,25 Some research has suggested that self-management of chronic illness centers the person with the condition. 52 Previous unsuccessful interventions were found to have lacked individualized support and failed to engage patients. 46
Maintaining CDT Self-Management Through Habit Formation
Integrating self-management practice into a person’s daily life enhances a person’s self-efficacy in maintaining CDT self-management. Once the CDT self-management became a lifestyle, its burden lightened. Studies have examined the relevance of habit formation to health and demonstrated that once an action becomes a habit, the requirement for conscious motivation is reduced.53,54 Our findings suggest survivors need more practical support with integrating self-management into daily life and forming new habits, which allows them to maintain other important aspects of their lives.
CDT Self-Management Follow-Up Care and Symptom Assessment at Home
Although the newly diagnosed patients in this analysis were struggling to master CDT self-management techniques and fit time-consuming tasks into their busy schedules, long-term patients were trying to maintain motivation and adjust self-management to their ever-changing lives. 25 Studies indicated that follow-up education about lymphedema treatment and risk-reduction activities would have facilitated consistent intervention for survivors’ lymphedema. 18 Ongoing assessments of barriers to CDT self-management and targeting initiation strategies to individuals at different stages of CDT self-management journey are necessary. 55 It is essential to further identify reliable and feasible methods/technologies of volume measurement and lymphedema symptom assessment at home. Recent trends have included attempts to administer lifestyle medical care via telehealth and mhealth, which appear to be less burdensome and preferable for cancer survivors when compared to standard follow-up visits. 56 This innovation is promising for follow-up care among survivors with lymphedema.
Limitations and Strengths
This is a qualitative study with the goal of obtaining a deeper understanding of the phenomenon instead of generalization. 34 Findings may be approached with caution because participants were from a single Midwestern city. Studies of populations in different geographic areas and ethnicities have been conducted. This qualitative study yielded rich data that provided valuable information for developing targeted interventions in supporting lymphedema self-management.
Conclusion
This study examined determinants to initiate and maintain CDT self-management of lymphedema. The findings highlight the importance of the patient’s understanding of lymphedema as a chronic condition and assuming accountability for their life-long CDT self-management of lymphedema. Interventions should be tailored to promote the initiation and maintenance of CDT self-management. While clinicians provided knowledge-based and clinical skills-based information, patient peers provided daily life examples and real-life implementation strategies for CDT self-management. Ongoing patient-provider and patient-peer communication functioned as effective support for maintaining CDT self-management. Reliable and realistic methods of symptom self-assessment are important for maintaining CDT at home.
Footnotes
Author Contributions
Conception and design: Yuanlu Sun, Mei R. Fu;
Collection and assembly of data: Yuanlu Sun;
Data analysis and interpretation: Yuanlu Sun, Mei R. Fu;
Manuscript Drafting: Yuanlu Sun, Mei R Fu;
Manuscript revision and editing: Yuanlu Sun, Mei R. Fu, Yun Jiang; Amy Little
Final approval of manuscript: All authors.
Availability of data and material
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The data collected through the study approved by University of Missouri Institutional Research Board (IRB# 2003958). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent/Consent for Publication
Informed consent was obtained from all individual participants included in the study. Participants were informed of data publication in the consent. Individual participant was not identifiable from reported results.
