Abstract
Objective
To evaluate the therapeutic effect of Traditional Chinese Medicine (TCM), specifically Fuzheng Qingdu (FZQD) therapy, on the survival time of metastatic GC patients.
Patients and Methods
Databases of medical records of 6 hospitals showed that 432 patients with stage IV GC were enrolled from March 1, 2012 to October 31, 2020. Propensity score matching (PSM) was used to reduce the bias caused by confounding factors in the comparison between the TCM and the non-TCM users. We used a Cox multivariate regression model to compare the hazard ratio (HR) value for mortality risk, and Kaplan-Meier survival curve for the survival time of GC patients
Results
The same number of subjects from the non-TCM group were matched with 122 TCM-treated patients after PSM to evaluate their overall survival (OS) and progression-free survival (PFS). Median time of OS of TCM and non-TCM users were 16.53 and 9.10 months, respectively. TCM and non-TCM groups demonstrated a 1-year survival rate of 68.5% and 34.5%, 2-year survival rate of 28.6% and 3.5%, and 3-year survival rate of 17.8% and 0.0%, respectively. A statistical difference exists in OS between the 2 groups (χ2 = 33.39 and P < .0001). The PFS of TCM users was also longer than that of non-TCM users (χ2 = 4.95 and P = 0.026). Notably, Chinese herbal decoction, Shenmai and compound Kushen injections were commonly used for FZQD therapy.
Conclusion
This propensity-matched study showed that FZQD therapy could improve the survival of metastatic GC patients.
Keywords
Graphical Abstract
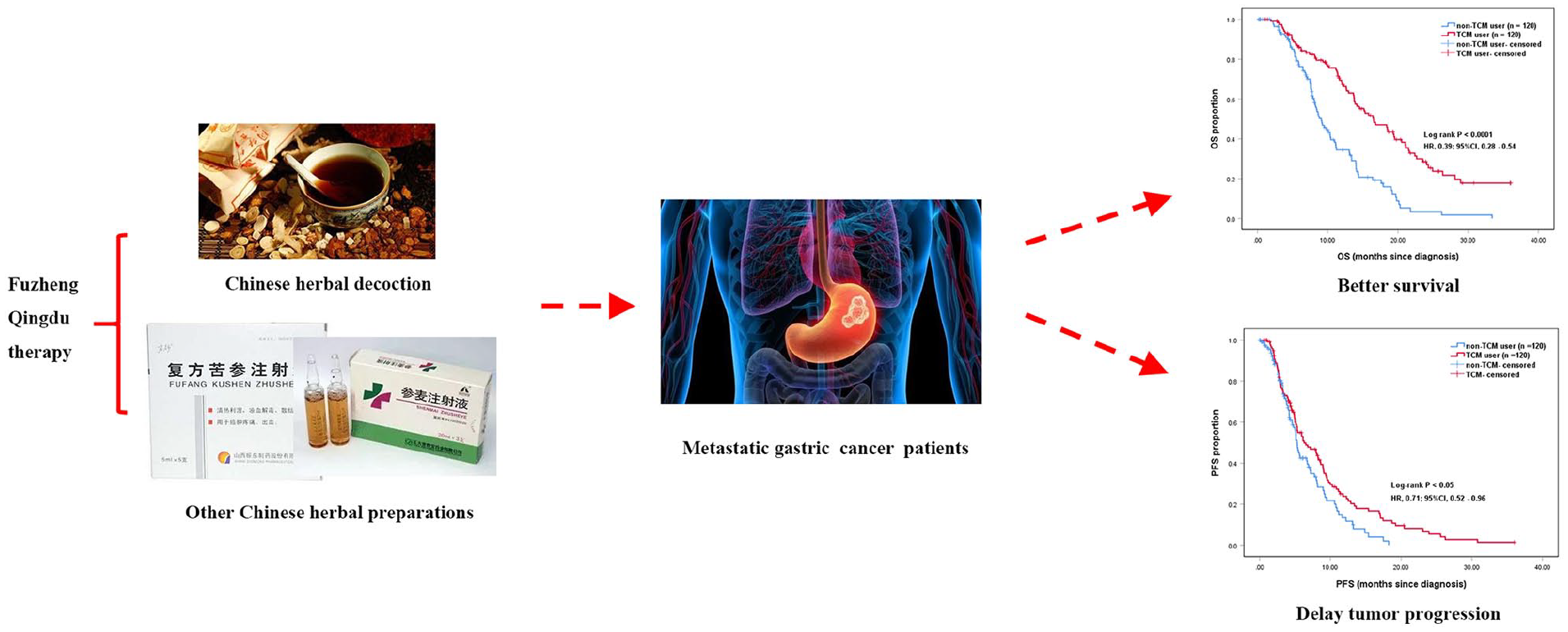
Introduction
Gastric carcinoma (GC) is the third most common cause of cancer-related deaths worldwide. 1 The latest world cancer report reached 478 508 new and 373 789 death cases of gastric cancer from China in 2020, with both values ranking third among the total new and death cancer cases, respectively. 2 Thus, China has been suffering from high incidence and mortality of GC. Curative surgery is the principal treatment for GC patients, but most patients with advanced GC do not have the chance for an operation. Metastatic GC is an advanced tumor that demonstrates poor prognosis. Chemotherapy is the principal treatment for improving the survival of patients.3,4 However, the 5-year OS of metastatic GC patients is still unsatisfactory. Research 5 demonstrated that the median OS of GC patients with liver metastasis is less than 8 months. Besides, many patients with metastatic GC may refuse or give up chemotherapy due to its side effects. 6 Thus, an increasing number of GC patients have been searching for other treatments to prolong their survival time. 7
Traditional Chinese medicine (TCM) is a complementary and alternative treatment in China that plays an important role in reducing adverse effects caused by other therapies, improving quality of life, and prolonging the overall survival (OS) of patients with GC. 8 Fuzheng Qingdu (FZQD) therapies, based on the TCM pathogenesis of GC formation, namely “spleen deficiency and toxic gathering,” have been used by GC patients in Yangzhou for a long time. However, there is no research to explore the effect of FZQD therapy on the survival of GC patients. Chinese herbal preparations (CHPs) are various Chinese herbal forms such as decoctions, tablets, injections, and capsules, which are made from Chinese herbals and their extracts. Chinese herbal decoctions (CHD) are a traditional type of CHP, which are obtained by decocting herbs in water and removing the dregs, or soaking herb granules in boiling water. As an important part of FZQD therapies, CHDs, and other CHPs have also been widely used by GC patients. Systematic reviews and meta-analysis have confirmed that CHPs, such as Brucea javanica oil emulsion 9 injection, can improve clinical efficacy of chemotherapy, and relieve adverse drug reactions for patients with GC. However, most of these studies are single-center clinical trials with small sample sizes and fail to specifically target prolonged survival of metastatic GC patients. Meanwhile, investigations on the relationship between FZQD therapy and prognosis of metastatic GC are limited. Therefore, we performed a multicenter propensity-matched study to explore the effects of FZQD therapy on the survival of metastatic GC.
Materials and Methods
Study Population and Selection Criteria
In this multicenter study, the baseline survey of was performed from March 1, 2012 to October 31, 2020 among the patients with stage IV GC, who were enrolled from 6 local hospitals in Yangzhou. Inclusion criteria were as follows: (1) gastric cancer confirmed by cytological or histological diagnosis; (2) diagnosed with clinical TNM stage IV gastric cancer, based on the 2018 International Union Against Cancer/American Joint Committee on Cancer (UICC/AJCC) staging of gastric cancer (UICC, 2018); (3) aged 18 to 75 years. Exclusion criteria were as follows: (1) patients with other types of primary tumor; (2) patients with incomplete key clinical data, (3) patients with other stages of gastric cancer; (4) patients with serious comorbidities including the obstruction of digestive tract and gastrointestinal bleeding, and (5) patients using TCM treatment after tumor progression. According to treatment type, patients included in this study were classified into 2 groups. Patients accepting more than 2 weeks of FZQD herbs after diagnosis of GC, were divided into TCM group. Patients not accepting any TCM treatment were assigned to the non-TCM group. Both groups of patients received one or more conventional treatments, such as palliative surgery, radiotherapy, chemotherapy, symptomatic relief, and supportive treatments. Notably, since some patients just started to seek for TCM treatment when their disease progressed, they belong to TCM group in the OS evaluation, but belong to the non-TCM group in the evaluation of progression-free survival (PFS). Propensity score matching (PSM) of 1:1 was performed in this study using a logistic regression model wherein all baseline characteristics, such as age, gender, TNM stage, and therapy strategy, were included to reduce the bias caused by confounding factors and allow a fair comparison between TCM and non-TCM users.
Study Variables
Patient baseline data were divided into demographic and clinical characteristics. Demographic data includes age, gender, diabetes, hypertension, coronary artery disease, KPS or PS, family history of GC, history of smoking, and history of alcohol use, which were measured or evaluated at the time of diagnosis. Tumor conditions including location, pathology, tissue differentiation, HER-2 expression, resection margin, blood vessel invasion, nerve invasion, adjacent tissue invasion and metastasis site, and treatment type were classified into clinical variables. FZQD herbs could be divided into Fuzheng and Qingdu categories. Fuzheng herbs have various functions to regulate physical fitness, such as spleen-invigorating, Qi-replenishing, blood-nourishing, Yang-increasing, Yin-replenishing, and kidney-nourishing. Qingdu herbs also had various functions such as detoxifying, resolving phlegm, removing dampness, promoting blood circulation, or digesting food. The primary evaluation indicator of this study was OS of GC patients, with the observation time from the date of diagnosis to the date of the patient’s death or December 31, 2020. The date of death was determined from the database maintained by the Yangzhou Municipal Center for Disease Control and Prevention of Cancer Patient Registration System. The secondary indicator was PFS of GC patients, with the observation time from the date of diagnosis to the date of disease progression or December 31, 2020. The judgment of disease progression was based on Response Evaluation Criteria in Solid Tumors (RECIST 1.0). 10
Statistical Analysis
The statistical analyses were performed using SPSS 26.0 (IBM Corp.; Armonk, NY, United States). P values <.05 were considered statistically significant. Qualitative data were compared using the χ2 test or Fisher’s exact test. Quantitative data consistent with the normal distribution were analyzed by t-test, while non-normally distributed data were analyzed with the Wilcoxon test. Log-rank test and multivariate Cox proportional hazard regression analyses were used to assess the independent risk factors that affect OS and PFS of GC patients. The cumulative OS rates were calculated by the Kaplan–Meier method and the survival curves were compared via the log-rank test. The time-dependent Cox proportional hazard model was used to assess immortal time bias.
Ethics Approval and Consent
The study was approved by the Ethics Committee for Clinical Medical Research of Yangzhou Hospital of Traditional Chinese Medicine. The researchers only collected the clinical data of patients, did not interfere with the treatment plan of the patients, and did their best to protect the information provided by the patients from leaking personal privacy, which was in compliance with the Declaration of Helsinki.
Results
Participant Selection
Our study enrolled 2136 patients with GC from 6 local hospitals. According to the inclusion and exclusion criteria, 147 and 285 patients were chosen from TCM and non-TCM groups to evaluate the OS and PFS. We matched 122 patients who received TCM treatment with the same number of subjects from the comparison group according to their propensity score to evaluate the OS and PFS. The flow diagram of recruitment of participants for this propensity-matched study is shown in Figure 1. The composition of participants from 6 local hospitals before and after PSM are presented in Figure 2.

The flow diagram of recruitment of participants for this propensity-matched study.

Composition of patients included from different hospitals before and after PSM to evaluate OS and PFS.
Patient Characteristics
Demographic characteristics of patients selected to evaluate the OS showed a statistical difference in history of smoking (P = .024), and history of alcohol use (P = .037) between TCM and non-TCM groups (Supplemental Table S1). Clinical characteristics of tissue differentiation (P = .013), blood vessel invasion (P < .0001), and nerve invasion (P = .032) were significantly different between the 2 groups. TCM users exhibited a high ratio of palliative surgery (P = .026) and apatinib therapy (P = .008) in terms of treatment type. Minimal or no heterogeneity of baseline, including demographic and clinical characteristics, was observed between the 2 groups after PSM (Figure 3 and Supplemental Table S1).
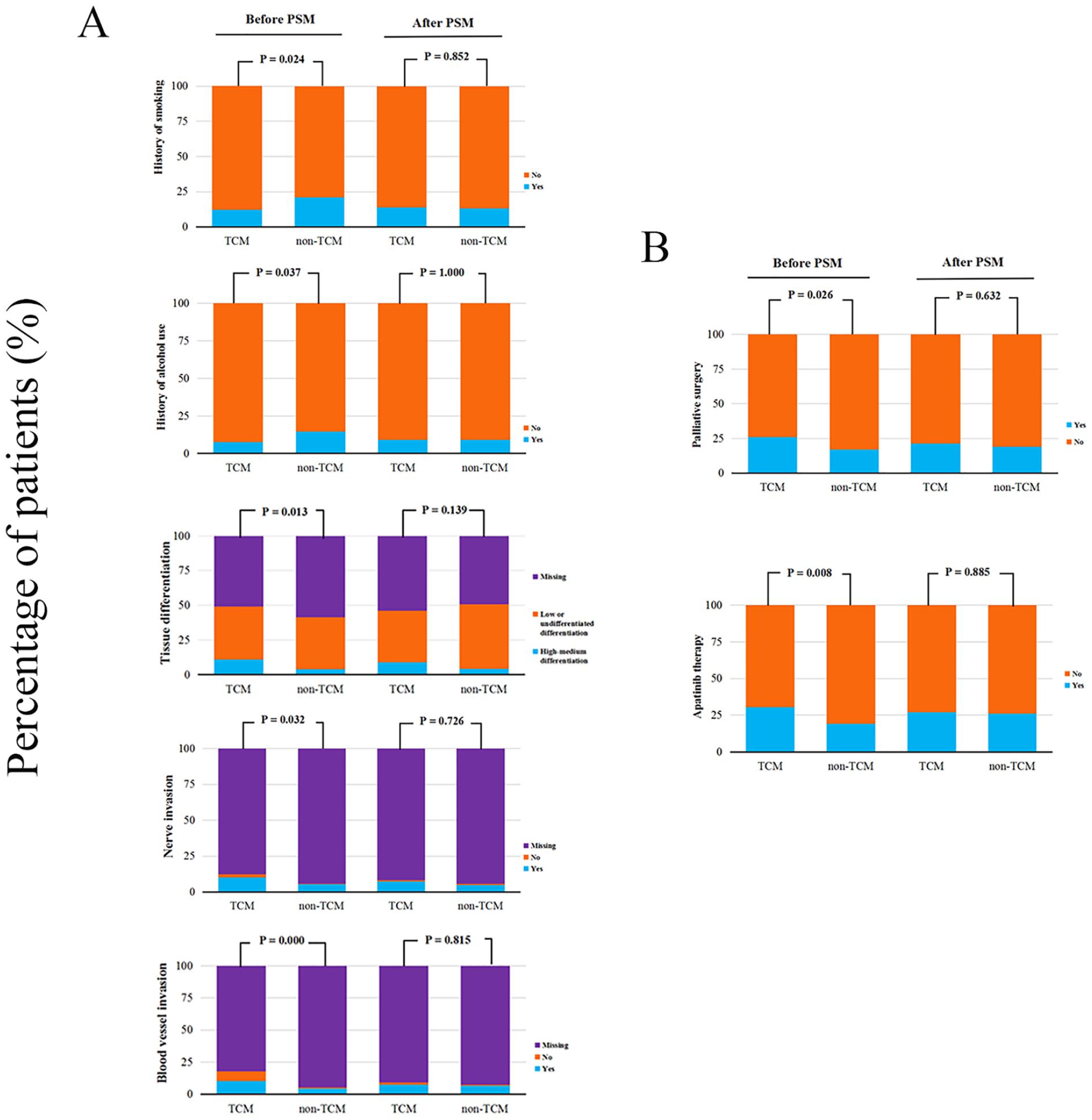
Characteristic changes of patients before and after PSM. (A) Demographic and clinical characteristics including history of smoking, history of alcohol use, tissue differentiation, blood vessel invasion, and nerve invasion. (B) Treatment types including palliative surgery and apatinib therapy.
Analysis of Prognostic Factors
Multiple potential confounders, including age, gender, diabetes, hypertension, coronary artery disease, KPS or PS, tumor location, pathology, tissue differentiation, HER-2 expression, resection margin, blood vessel invasion, nerve invasion, adjacent tissue invasion, distant metastases, and treatment types, might affect the prognosis of patients. The multivariate Cox proportional-hazard model was used to analyze effects of these confounders on the OS in GC patients. The results showed the following independent protective factors (Table 1): “distant metastases—lung” (adjusted HR = 0.24, 95% confidence interval [CI]: 0.07-0.85, and P = .027), palliative surgery (adjusted HR = 0.50, 95% CI: 0.32-0.78, and P = .002), chemotherapy (adjusted HR = 0.46, 95% CI: 0.27-0.76, and P = .002), radiotherapy (adjusted HR = 0.66, 95% CI: 0.44-0.98, and P = .038), anti-tumor immunotherapy (adjusted HR = 0.50, 95% CI: 0.26-0.98, and P = .042),and TCM treatment (adjusted HR = 0.40, 95% CI: 0.30-0.55, and P < .0001), while “tumor location—others” (adjusted HR = 2.25, 95% CI: 1.20-4.23, and P = .012) was an independent risk factor. TCM treatment showed the maximum protective effect after multivariate correction.
Factors Associated With Overall Survival of GC Patients.

Abbreviations: GC, gastric carcinoma; HR, hazard ratio; CI, confidence interval; TCM, traditional Chinese medicine; KPS, Karnofsky performance status; PS, Performance status.
Age, gender, diabetes, hypertension, coronary artery disease, KPS or PS, tumor location, pathology, tissue differentiation, HER-2 expression, resection margin, blood vessel invasion, nerve invasion, adjacent tissue invasion, distant metastases, and treatment type are adjusted using a Cox proportional hazard regression model.
The Effect of TCM Treatment on Survival
The effect of TCM treatment on survival before and after PSM
Median times of OS of TCM and non-TCM users before PSM were 16.80 (95% CI: 14.00-19.60) and 9.80 (95% CI: 8.76-10.84) months, respectively. One, 2-, and 3-year survival rates of TCM and non-TCM groups were 70.7% and 37.9%, 30.2% and 6.7%, and 14.3% and 1.8%, respectively (Figure 4). A significant difference was observed between the 2 groups (χ2 = 40.67 and P < .0001) (Figure 5a). The median times of PFS of TCM and non-TCM users were 7.97 (95% CI: 5.95-9.99) and 5.50 (95% CI: 4.41-6.59) months, respectively. The log-rank analysis also showed that the median time of PFS in the TCM group is significantly longer than that of the non-TCM group (χ2 = 5.20 and P = .023) (Figure 5b).

Milestone OS rate between TCM and non-TCM user groups before and after PSM.
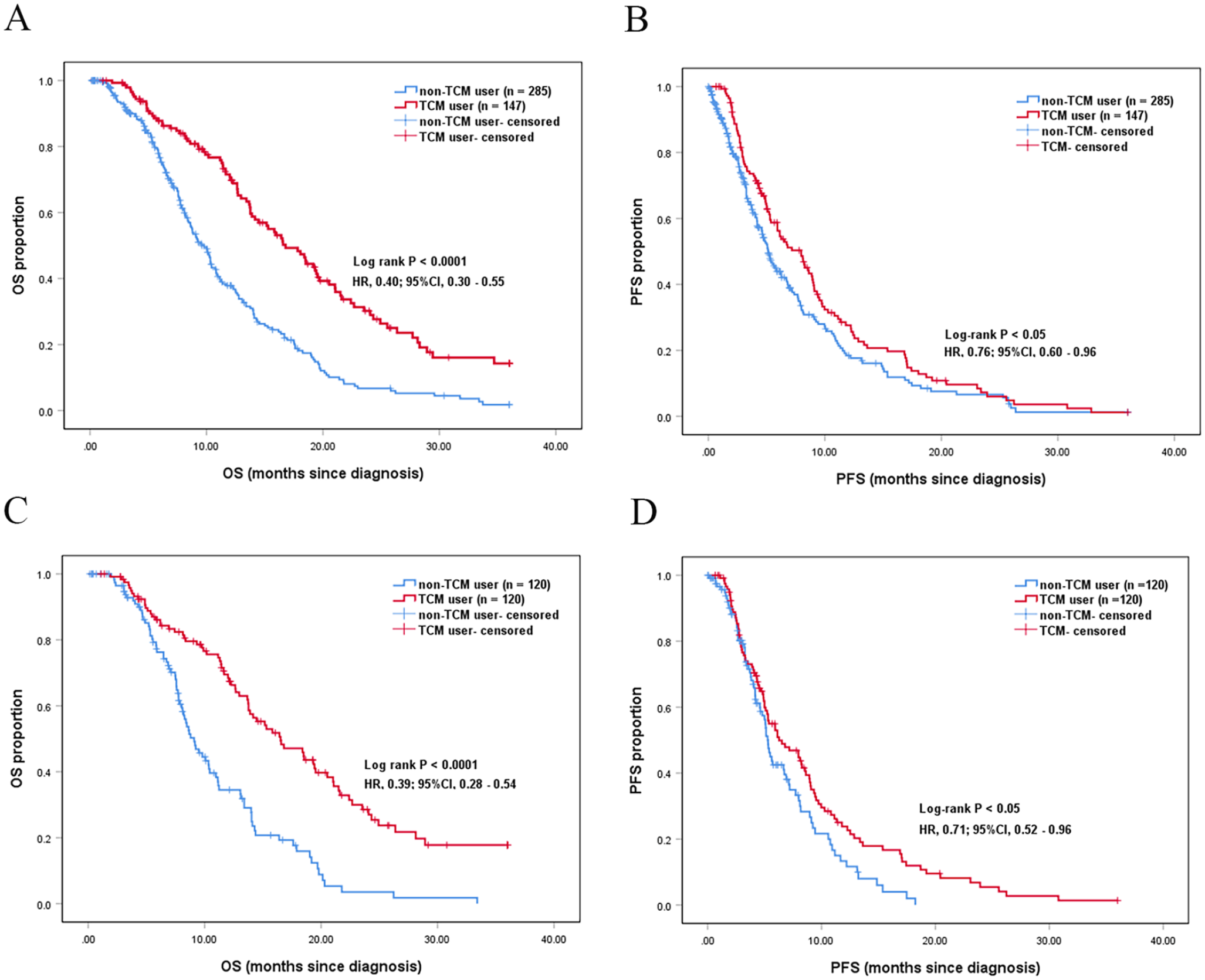
OS and PFS between TCM and non-TCM users in patients with GC. (A and B) OS and PFS between TCM users and non-TCM users before PSM. (C and D) OS and PFS between TCM users and non-TCM users after PSM.
The median time of OS for TCM and non-TCM users after PSM were 16.53 (95% CI: 12.69-20.37) and 9.10 (95% CI: 7.76-10.44) months, respectively. One, 2-, and 3-year survival rates of TCM and non-TCM groups were 68.5% and 34.5%, 28.6% and 3.5%, and 17.8% and 0.0%, respectively (Figure 4). The 2 groups demonstrated a significant difference (χ2 = 33.39 and P < .0001) (Figure 5c). The median times of PFS for TCM and non-TCM users were 6.53 (95% CI: 4.25-8.81) and 5.33 (95% CI: 4.78-5.88) months, respectively. The log-rank analysis showed that the median time of PFS of the TCM group was significantly longer than that of the non-TCM group (χ2 = 4.95 and P = .026) (Figure 5d).
Landmark analysis
Since all the patients of the TCM group started to use Chinese medicine within 4 months after GC diagnosis, we set 4 months as an index date in landmark analysis to assess immortal time bias. Before the landmark, there was no significant difference in OS (χ2 = 0.44 and P = .508) and PFS (χ2 = 1.52 and P = .217) between the 2 groups (Figure 6). After the landmark, the median times of OS for TCM and non-TCM users after PSM were 18.40 (95% CI: 15.13-21.67) and 9.50 (95% CI: 7.93-11.07) months, respectively. The 2 groups demonstrated a significant difference (χ2 = 36.34 and P < .0001) (Figure 6a). The median times of PFS for TCM and non-TCM users were 7.97 (95% CI: 6.06-9.88) and 5.40 (95% CI: 4.85-5.95) months, respectively. The log-rank analysis showed that the median time of PFS of the TCM group was significantly longer than that of the non-TCM group (χ2 = 6.04 and P = .014) (Figure 6b).

Landmark analysis in OS and PFS between TCM and non-TCM users for patients with GC. (A) Landmark analysis in OS between TCM users and non-TCM users. (B) Landmark analysis in PFS between TCM users and non-TCM users.
Subgroup analysis
Additionally, the effects of the TCM treatment on the OS of GC patients in different subgroups were evaluated. The results showed that TCM users exhibited better prognostic outcome than non-TCM users for GC patients with liver metastases (χ2 = 18.80 and P < .0001). Prognostic outcome was not statistically different between TCM and non-TCM groups for GC patients with distant metastases of the lung and bone. Additionally, TCM users presented significantly lower mortality than non-TCM users regardless of categories of smoking abuse, tumor location, palliative surgery, chemotherapy, radiotherapy, and anti-tumor immunotherapy (P < .05) (Table 2).
Mortality Risk of Non-TCM and TCM Users in Different Subgroups of GC Patients.

Abbreviations: GC, gastric carcinoma; CI, confidence interval; TCM, traditional Chinese medicine; mOS, median overall survival.
Comparison of Mortality Risk in GC Patients With Different Use Time of TCM Treatment
TCM users were classified into 4 subgroups according to the use time of TCM treatment, namely, <6 months, 6 to 12 months, and >12 months groups. The multivariate Cox proportional-hazard model demonstrated that the adjusted mortality risk of TCM users in each subgroup administered with TCM for more than 6 months after PSM was lower than that of patients in other subgroups (P < .05). Therefore, longer administration of TCM treatment indicates more benefits to survival (Figure 7 and Supplemental Table S2).
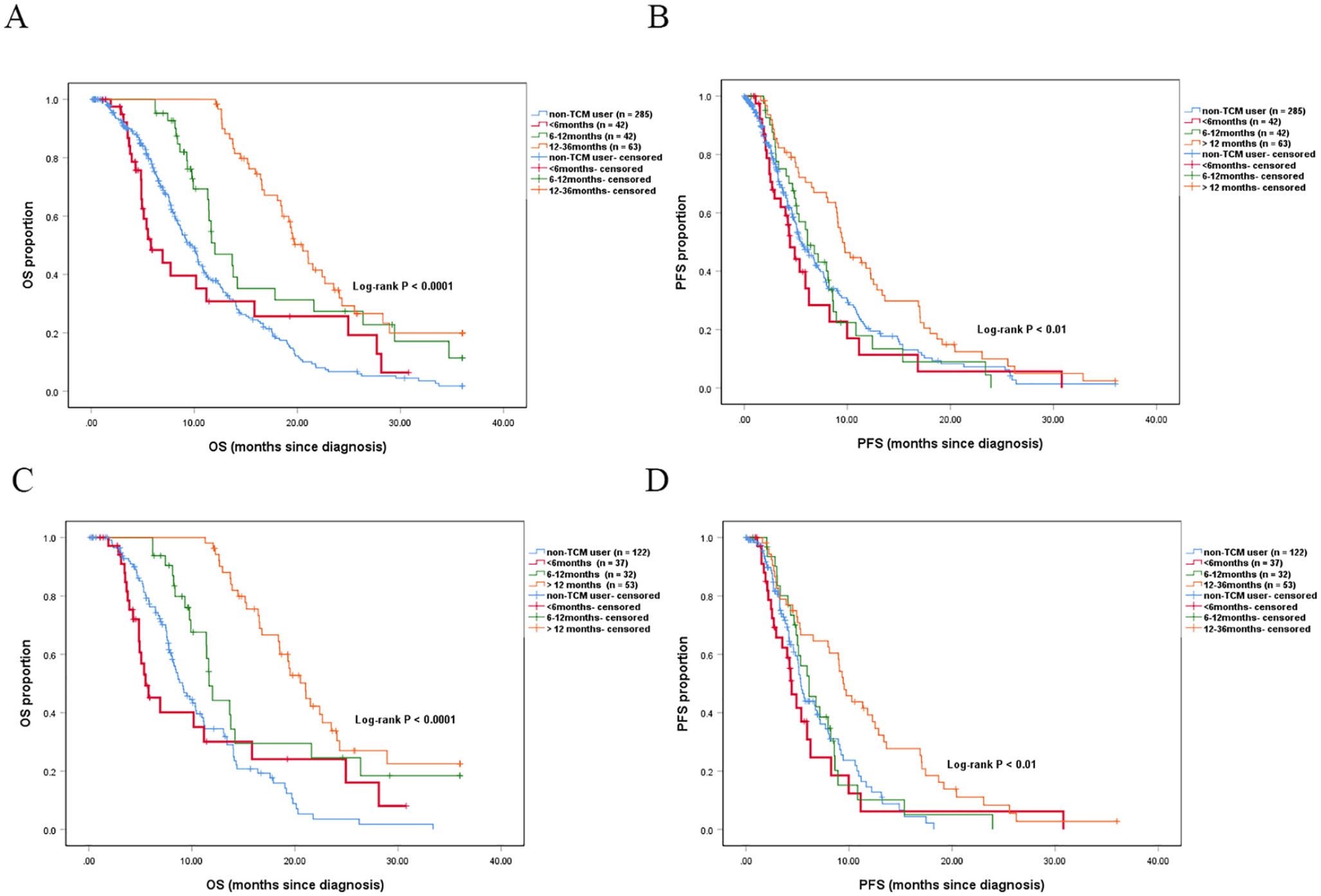
OS and PFS for different use time of TCM treatment. (A and B) OS and PFS for different administration periods of TCM before PSM. (C and D) OS and PFS for different administration periods of TCM after PSM.
TCM Treatment Types
TCM treatment in our study mainly consisted of CHDs and other CHPs. According to the TCM theory, single herbs of the CHDs could usually divided into 2 categories, namely Fuzheng herbs, and Qingdu herbs. Further analysis determined the 20 most commonly prescribed Chinese herbs (Table 3). Other CHP treatments included oral Chinese patent medicine and intravenous injections. We listed the ten most commonly used CHPs (Table 4), which were all approved by the State Food and Drug Administration of China. The national medicine permission numbers of Fufang Shenqi Shiyi Wei granule and Aidi, Brucea javanica oil emulsion, Kangai, sodium cantharidinate, Shenmai, Shenqi Fuzheng, compound Kushen, Lentinan, and Danshen injections were Z10980002, Z52020236, Z21021715, Z20026868, H52020601, Z13020887, Z19990065, Z14021231, H20030131, and Z51021303, respectively. Ingredients, functional classification, administration method, and dosage of CHPs were listed in Supplemental Table S3.
The Most Commonly Prescribed Herbs Used by Patients With Gastric Cancer.

Risk of Overall Survival According to the Use of Common TCM Treatments Among Patients With Gastric Carcinoma.

Abbreviations: GC, gastric carcinoma; CI, confidence interval; TCM, traditional Chinese medicine; Results are expressed as hazard ratios (95% confidence intervals).
Crude HR represents relative hazard ratio.
Adjusted HR represents multivariate-adjusted hazard ratio: age, gender, diabetes, hypertension, coronary artery disease, KPS or PS, tumor location, pathology, tissue differentiation, HER-2 expression, resection margin, blood vessel invasion, nerve invasion, adjacent tissue invasion, distant metastases, and treatment type are adjusted using a Cox proportional hazard regression model.
Comparison of Mortality Risk in GC Patients With Different Types of TCM Treatment
As shown in Table 4, analysis of proportions of TCM treatment in this study revealed that CHD, Shenmai injection, and compound Kushen injection were the top 3 commonly used therapies, with a proportion of 69.67%, 36.07%, and 31.15%, which yielded an adjusted three-year mortality risk of 0.27 (95% CI: 0.15-0.48), 0.23 (95% CI: 0.13-0.42), and 0.30 (95% CI: 0.15-0.58), respectively, in GC patients. Additionally, except for Shenqi Fuzheng and Brucea Javanica oil emulsion injections, other CHPs in this study also improved the survival of the patients.
Discussion
Metastatic GC patients usually do not have the opportunity to get radical surgery. Carefully selected patients could benefit from surgery, which may significantly improve their overall survival. 11 Our prognostic analysis also demonstrated that palliative surgery is an independent protective factor for the survival of metastatic GC patients. Chemotherapy is now widely used as the standard treatment for stage IV GC patients.3,4 The recommended chemotherapy first-line regimen, including fluorouracil drugs plus platinum or taxane drugs, can control disease progression to some extent, but its effect is unsatisfactory in terms of prolonging survival of GC patients.12 -14 Although chemotherapy was also proved to be an independent protective factor for the survival of GC patients in our study, it also produces various adverse drug actions, such as gastrointestinal reaction, marrow suppression, and neurotoxicity. 6 Given the limitations of conventional treatments, many advanced patients kept seeking for other therapies. In China, TCM therapies are widely accepted as an important alternative intervention in the treatment of all kinds of malignant tumors. Studies have demonstrated that TCM treatment can enhance clinical efficacy and reduce adverse effects for patients with various cancers, such as liver, 15 and lung 16 cancers. Besides, an increasing number of evaluations on the clinical efficacy of TCM therapies in the treatment of GC have been conducted in recent years. A retrospective clinical analysis 8 revealed that TCM treatment combined with chemotherapy can improve the survival and quality of life of GC patients at stage IV. Two studies have shown that TCM can prolong the OS of GC patients after surgery and adjuvant Chemotherapy.7,17 Further research found that TCM treatment based on the therapy of “Jianpi Bushen” can improve the clinical efficacy of chemotherapy on GC patients. 18 Pharmacological experiments 19 proved that TCM treatment can exert anti-tumor effects through multiple mechanisms, including cell cycle arrest, inhibition of telomerase activity, promotion of mitochondrial apoptosis pathway, interference with angiogenesis, inhibition of cell migration and invasion, and regulation of the expression of adhesion molecules.
Although 3 studies7,8,17 have demonstrated that TCM treatment can improve the survival of GC patients, most of the GC cases were from Taiwan and did not illustrate the effect of TCM therapies on the GC patients at specific TNM stage, especially metastatic patients after palliative surgery. Additionally, the effects of different TCM treatment types on the OS and PFS of GC patients remain to be confirmed. Our study was the first to examine the clinical effects of TCM, especially FZQD therapy, on the PFS and OS of metastatic GC patients including those with palliative surgery. Prognostic analysis showed that TCM treatment is the primary protective factor for the survival of stage IV GC patients. Since there are other factors, such as age, gender, performance status, tumor location, blood vessel invasion of tumor, treatment types that could affect the prognosis of gastric cancer, 20 in order to reduce the bias caused by confounding factors, we performed 1:1 PSM for the baseline data of patients. The cumulative OS and PFS of TCM users were still statistically longer than those of non-TCM users after PSM. The results also showed a significant protective effect of TCM with 34.0%, 25.1%, and 17.8% improvements of 1-year, 2-year, and 3-year survival rates, respectively in all GC patients. Since the so-called lag time to treatment might affect the HR value for mortality risk, 21 we conducted a landmark analysis to reduce the immortal time bias. The results showed that the median time of OS and PFS of the TCM group were still significantly longer than that of the non-TCM group after the landmark. Besides, subgroup analysis suggested that TCM therapy is suitable for GC patients with liver metastases. In all subgroups of smoking abuse, tumor location, palliative surgery, chemotherapy, radiotherapy, and anti-tumor immunotherapy, TCM users presented significantly lower mortality than non-TCM users. Additionally, further analysis showed that the mortality risk is halved in GC patients who received TCM treatment for more than 6 months compared to those with TCM treatment for less than 6 months. The result indicated that a longer TCM treatment period might lead to a stronger protective effect.
Finally, we found that CHD was the most commonly used TCM treatment type, which was associated with a 8.5% reduction in death events. We further determined the twenty most commonly prescribed Chinese herbs from the CHDs and divided the herbs into Fuzheng and Qingdu categories, of which the main components are spleen-invigorating and detoxifying herbs, respectively. Many TCM physicians thought that spleen-deficiency and cancer-toxin is the main pathogenesis of GC formation, and GC toxin is mainly composed of phlegm, moisture, blood stasis, food accumulation and Qi stagnation, Qingdu herbs could detoxifying, resolving phlegm, removing dampness, promoting blood circulation, or digesting food, 22 Additionally, we found the summarized herbs were the main components of some classic Chinese herbal formulas, such as Huo-Po-Xia-Ling-Tang, Xiang-Sha-Liu-Jun-Zi-Tang, and Shen-Ling-Bai-Zhu-San, which were similar to some reports.7,17 Besides, the identified herbs and their extracted substances also exhibited anti-tumor activities. For example, the extract of Astragalus membranaceus (Fisch.) Bunge shows multiple functions, such as immunomodulation, antiproliferation, and attenuation of adverse effects induced by cytotoxic therapy. 23 Glycyrrhizic acid extracted from Glycyrrhiza uralensis Fisch. can induce apoptosis in human GC KATO III and human promyelocytic leukemia HL-60 cells. 24 Overall, the herbs identified in our study may provide useful information for further clinical trials and pharmacological experiments against GC in the future. Taken together, our study might provide useful evidence for the clinical application of CHD decoctions against GC. However, further related pharmacological experiments need to be carried out in the future.
Additionally, we also identified the 2 most commonly used CHPs other than CHDs, namely Shenmai and compound Kushen injections, which were associated with 3.76% and 6.51%, respectively reduction in death events. Studies have also confirmed that the 2 injections could reduce adverse effects of other therapies, and demonstrated multiple antitumor functions, such as tumor blood vessel normalization, apoptosis promotion, and metabolic regulation. For example, Shenmai injection could inhibit myocardial excessive autophagy through regulating the expression of miR-30a/Beclin 1 and alleviate the myocardial injury induced by doxorubicin, 25 and enhance drug delivery and anti-tumor effect by promoting tumor vessel normalization. 26 Experiments have proved that compound Kushen injection induced apoptosis of cancer cells through multiple pathways. 27 Metabolomics results indicated that the anti-tumor effect of compound Kushen injection on liver cancer might be involved in multiple metabolic pathways. 28 Other CHP injections, such as Aidi, 29 sodium cantharidinate, 30 and Brucea javanica oil emulsion, 31 injections, showed anticancer abilities. Shenqi Shiyi Wei granule, as an oral administration of CHP, was also used widely by the metastatic GC patients, but its pharmacodynamic mechanism and clinical efficacy have not been reported.
Notably, this study presents certain limitations. First, many differences were observed in baseline characteristics of patients between TCM and non-TCM groups in this multicenter propensity-matched study. Although patients were matched basis on their PS core, estimated using the demographic and clinical characteristics, hypertension and adjacent tissue invasion of tumor between the 2 groups still were demonstrated to be slightly different. Additionally, baseline heterogeneity between the 2 groups was inevitable because of the incomplete information of GC patients. Thus, prospective randomized controlled trials are still needed to verify the effects of CHPs on the survival of metastatic GC patients. Second, since some death events missed the cause of death, we cannot confirm the effect of TCM treatment on GC-related survival. Third, long-term surviving patients are more likely to get a long period of TCM treatment than those with shorter survival time. So the correlation between the anti-tumor effect of TCM treatment and the usage time needs to be further confirmed by future studies. Fourth, the CHDs were made based on the different experience of TCM physicians, which makes it difficult to detect the effectiveness of commonly used CHDs. Finally, our study did not involve the influences of TCM treatment on other TNM stages of GC. Therefore, the effects of CHDs and other CHPs on the survival of GC with other TNM stages need to be further investigated.
Conclusion
This study showed that TCM treatment may prolong the OS and PFS of metastatic GC patients, especially those with liver metastases. TCM treatment consisting of CHD, Shenmai injection, and compound Kushen injection for more than 6 months may be the optimal regimen for achieving improved survival benefits.
Supplemental Material
sj-docx-1-ict-10.1177_15347354211058464 – Supplemental material for Effect of Fuzheng Qingdu Therapy for Metastatic Gastric Cancer is Associated With Improved Survival: A Multicenter Propensity-Matched Study
Supplemental material, sj-docx-1-ict-10.1177_15347354211058464 for Effect of Fuzheng Qingdu Therapy for Metastatic Gastric Cancer is Associated With Improved Survival: A Multicenter Propensity-Matched Study by Chao Hou, Die Yang, Yusen Zhang, Yifei Li, Zhengfei He, Xiaojun Dai, Qingyun Lu, Shanshan Wang, Xiaochun Zhang and Yanqing Liu in Integrative Cancer Therapies
Supplemental Material
sj-docx-2-ict-10.1177_15347354211058464 – Supplemental material for Effect of Fuzheng Qingdu Therapy for Metastatic Gastric Cancer is Associated With Improved Survival: A Multicenter Propensity-Matched Study
Supplemental material, sj-docx-2-ict-10.1177_15347354211058464 for Effect of Fuzheng Qingdu Therapy for Metastatic Gastric Cancer is Associated With Improved Survival: A Multicenter Propensity-Matched Study by Chao Hou, Die Yang, Yusen Zhang, Yifei Li, Zhengfei He, Xiaojun Dai, Qingyun Lu, Shanshan Wang, Xiaochun Zhang and Yanqing Liu in Integrative Cancer Therapies
Supplemental Material
sj-docx-3-ict-10.1177_15347354211058464 – Supplemental material for Effect of Fuzheng Qingdu Therapy for Metastatic Gastric Cancer is Associated With Improved Survival: A Multicenter Propensity-Matched Study
Supplemental material, sj-docx-3-ict-10.1177_15347354211058464 for Effect of Fuzheng Qingdu Therapy for Metastatic Gastric Cancer is Associated With Improved Survival: A Multicenter Propensity-Matched Study by Chao Hou, Die Yang, Yusen Zhang, Yifei Li, Zhengfei He, Xiaojun Dai, Qingyun Lu, Shanshan Wang, Xiaochun Zhang and Yanqing Liu in Integrative Cancer Therapies
Footnotes
Acknowledgements
The authors are grateful to the medical records department of Yangzhou First People’s Hospital, Subei People’s Hospital, Yangzhou Hospital of Traditional Chinese Medicine, Gaoyou Hospital of Traditional Chinese Medicine, Jiangdu District Hospital of Traditional Chinese Medicine, Yizheng District Hospital of Traditional Chinese Medicine and Yangzhou Municipal Center for Disease Control and Prevention for their data support.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Natural Science Foundation of Jiangsu Province (No. BK20180277), China Postdoctoral Science Foundation (No.137070586), Beijing Hisco Clinical Oncology Research Fund (No.Y-L2020-0043), the Second Traditional Chinese Medicine Leadership Training Foundation of Jiangsu Province (Clinical Study on Prevention and Treatment of Postoperative Recurrence and Metastasis of Gastric Cancer Based on “Fuzheng Qingdu” Syndrome ).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
