Abstract
Purpose:
Health utility, which is a measure of patient-reported outcome (PRO), has recently been used in health-related quality of life for patients with various cancers. However, the relationship between health utility and the physical function and of patients undergoing pleurectomy/decortication (P/D) as surgical treatment for malignant pleural mesothelioma (MPM) has not been reported in the perioperative and convalescent phases. This study aimed to evaluate the perioperative and postoperative health utility of patients undergoing P/D for MPM at one year postoperatively and to examine the relationship with physical function.
Methods:
We included patients underwent P/D. Grip strength, knee extension strength, 6-minute walk distance (6MWD), forced vital capacity (FVC), and forced expiratory volume in one second (FEV1) were measured to assess physical function, and the Short-Form Six-Dimension (SF-6D) was completed to assess health utility. These assessments were performed preoperatively, postoperatively, and one year postoperatively. Statistical analysis was performed using one-way analysis of variance for comparison of pre and postoperative and one year mean values.
Results:
There were 24 subjects (23 males, 65.5±8.3 year). SF-6D, 6MWD, FVC, and FEV1 values one year operatively improved significantly compared with postoperative. Additionally, SF-6D was correlated with 6MWD.
Conclusion:
Health utility were also correlated with exercise capacity.
Keywords
Introduction
Malignant pleural mesothelioma (MPM) is a rare, aggressive, and devastating disease of the thoracic cavity associated with asbestos exposure. In recent years, the incidence of MPM has been rising and, although the use of asbestos has been prohibited in 55 countries, it is not expected to decrease until 2030. 1 Different treatment strategies such as resection, chemotherapy, radiotherapy, and immune-therapy have been used in various combinations for treating MPM, and in the context of multimodality therapy, curative-intent surgery has been associated with improved survival.2-4 In MPM, surgical resection includes either extrapleural pneumonectomy (EPP) or radical or extended pleurectomy/decortication (P/D). EPP is defined as an en bloc removal of the lung, parietal and visceral pleurae, diaphragm, and pericardium. Radical or extended P/D includes resection of the parietal and visceral pleurae with or without removal of the diaphragm and/or pericardium if involved with tumors, but it always preserves the underlying lung.5,6 P/D is theoretically less radical than EPP and is associated with less perioperative mortality/morbidity and postoperative deterioration of cardiopulmonary function. 7 Most clinicians now agree that P/D, the lung-sparing resection strategy for MPM, is recommended for cancer-directed surgery for MPM. 5
For patient preferences to be effectively used in the delivery of health care, it is important that patients be able to formulate and express preferences, and these preferences be made known to the clinician at the time of care, and these statements meaningfully inform care activities. 8 Health-related quality of life (HRQOL) is an important factor for determining the overall health status of a population. Quality-adjusted life-years (QALYs) is a measure of health status that incorporates both quantity and QOL. One QALY is equivalent to 1 year of life in perfect health. QALYs are fundamental for understanding the population burden of disease and the cost-effectiveness of disease treatment. QALYs are estimated using health utility weights, where 1 is equivalent to perfect health, and 0 is the worst possible state of health.9,10
Previous studies have recently reported that health utility has been used for analyzing various diseases.11-20 In contrast, there are previous studies on lung cancer, where health utility for patients with non-small cell lung cancer after surgery have been studied, 21 but there are no studies evaluating the health utility of MPM patients undergoing P/D.
Thus, this study aimed to assess the health utility and physical function before, after, and 1 year after P/D in MPM patients, and to assess how health utility and physical function are affected by the response to surgery.
Methods
Design
This was a prospective observational study. The study was approved by the Hyogo College of Medicine Institutional Committee on Human Research (approval number: 1690, April 8th 2014). Written informed consent was obtained from all participants.
Demographic, Clinical, and Diagnostic Data
The following data were extracted from the medical records of each patient: age, sex, disease stage at surgery, affected side, time from confirmed diagnosis (from initial diagnosis to operation), and cycles of chemotherapy received prior to P/D. Anthropometric, muscle strength, submaximal exercise capacity, and health utility data were measured during physical examination before and after the procedure. All other data were collected during physical examination before and after the procedure. Preoperative assessments were performed the day before or 2 days before surgery, and postoperative assessments were performed approximately 3 weeks after surgery. Convalescent phases assessments were performed 1 year after surgery.
Participants
Twenty-four MPM patients who underwent P/D between September 2014 and April 2019 were recruited from Hyogo College of Medicine Hospital, Nishinomiya, Japan. Before the surgery, patients were assessed for handgrip and knee-extensor strength, submaximal exercise capacity based on 6-minute walking distance (6MWD), forced vital capacity (FVC), forced expiratory volume in 1 second (FEV1), and HRQOL using the Medical Outcome Study Questionnaire SF-36.
Physiotherapy
Physiotherapy was promptly commenced the day after the surgery. Early rehabilitation was initiated with mobilization (such as sitting, standing, and walking) in the intensive care unit or high-care unit 5 to 6 times a week. After discharge, there was no rehabilitation intervention.
Measurements
Anthropometric measurements
Height (in cm) and weight (in kg) were measured with a wall-mounted stadiometer and a body composition analyzer (BC-118D; Tanita Co., Ltd., Tokyo, Japan), respectively. Body mass index (BMI) was calculated by dividing the body weight (in kg) by the height (in m) squared.
Handgrip strength
A standard adjustable-handle dynamometer (T.K.K. 5101; TAKEI Scientific instruments Co. Ltd., Niigata, Japan) was used for measuring handgrip strength as the index of upper-limb muscle strength and was set at the second grip position for all patients. Grip strength was measured with the same handgrip dynamometer, and the examination was performed by the same physical therapist. Attention was paid to a possible Valsalva effect, and the grip strength of both the hands was measured. The measured data were used as the index of handgrip strength (kilogram-force [kgf]).
Knee extensor muscle strength
Hand-held dynamometers (HHD; μ-tas MT1; ANIMA Co., Tokyo, Japan) were used for measuring knee extensor muscle strength as an index of lower-limb muscle strength. In all sessions, a HHD equipped with a stabilizing belt that the tester held was used when applying resistance. The HHD was used in the manual mode using kgf units. A previous study showed that the intraclass correlation coefficients (ICC) was .98 with a belt and .04 without a belt. 22 In a reliability test-retest of the belt-restrained HHD, ICCs ranged from .94 to .96. 23 Knee extension force was tested in a sitting position with the knee flexed at approximately 90°. The dynamometer was applied just proximal to the malleoli. The maximum force during 10 seconds of effort was recorded in kgf. The HHD was reset to kgf at the start of each measurement. Two measurements were conducted for each leg, and the higher value of the 2 measurements was selected for analysis.
Submaximal exercise capacity
Submaximal exercise capacity was assessed using the 6MWD measured according to the American Thoracic Society guidelines. 24 Patients walked up and down a 20-m corridor for 6 minutes at their own pace. They were encouraged to cover as much distance as possible but were permitted to rest as required and to continue walking as soon as they felt able to or to stop if they experienced symptoms of dyspnea or leg pain. 25 The following data were collected and analyzed: distance after 6 minutes (in m), duration (in minutes), and heart rate at initiation and 6 minutes. 26
Pulmonary function
Pulmonary function was assessed with spirometry (Minato Autospiro AS-302; Minato Medical Science Co., Ltd., Osaka, Japan) and was measured according to the American Thoracic Society guidelines. 27 FVC and FEV1 were expressed in liters.
Health-related quality of life and health utility
HRQOL was assessed with the SF-36 by the direct questioning of participants. Thus, those who were too confused or too dysphasic to answer were excluded. This self-administered questionnaire has been widely used and validated in the Japanese general population 28 and in patients who underwent P/D. The SF-36 assesses physical and mental health components in 8 domains: physical functioning (PF), physical role functioning (RP), bodily pain (BP), general health perceptions, vitality (VT), social role functioning (SF), emotional role functioning, and mental health (MH). The SF-36 measures the multidimensional properties of HRQOL on a scale of 0–100, with higher scores indicating better HRQOL. Health utility was assessed using the Short-Form Six-Dimension (SF-6D). The SF-6D measures the strength of preference for a particular health state and are represented as a number between 0 and 1, with 0 equivalent to death and 1 equivalent to being alive for a year in perfect health. After patients were assessed with the SF-36, the scores were converted to mean SF-6D utility scores by iHope International Co. Ltd. (Kyoto, Japan) based on techniques used in previous reports.29-31
Statistical Analyses
Data are summarized as mean ± standard deviation or median with interquartile range. Repeated-measure analysis of variance was used for comparing continuous data (body weight, handgrip, knee extensor muscle strength, 6MWD, FVC, FEV1, and preoperative, postoperative, and 1-year postoperative values of the SF-6D). The correlation between physical function (body weight, handgrip strength, knee extensor muscle strength, 6MWD, FVC, and FEV1) and the SF-6D were analyzed using Pearson’s correlation coefficient. Statistical analyses were performed with SPSS 17.0J (IBM, Tokyo, Japan). A P-value of <.05 was considered statistically significant.
Results
The demographic and diagnostic data for the cohort are summarized in Table 1. Twenty-four patients with MPM (23 men) underwent P/D between September 2014 and April 2019. The disease stage at surgery was stage I MPM in 18 patients (75%), stage II MPM in 3 patients (12.5%), and stage III MPM in 3 patients (12.5%). The median time from confirmed diagnosis was 5 months (range, 3–6 months). The number of chemotherapy cycles received before P/D was 3 in all patients.
Patient Baseline Data (n = 24).

Data are provided as mean (SD), median (range), or n (percent).
Physiological Variables
The body weight, muscle strength, and submaximal exercise capacity data of patients are summarized in Table 2. The postoperative body weight was significantly lower than preoperative values (P = .002). The body weight at 1 year postoperatively was higher than postoperative values and lower than preoperative values; however, these differences were non-significant. For muscle strength values (handgrip and knee extension), postoperative values after surgery were lower than preoperative values, whereas values 1-year post-surgery were higher than postoperative values and lower than preoperative values; however, all the noted differences were non-significant. The postoperative submaximal exercise capacity was significantly lower than the preoperative (P < .001) and 1-year postoperative (P < .001) values. No significant difference was observed between 1-year postoperative and preoperative submaximal exercise capacities (P = .949).
Body Weight, Strength, Submaximal Exercise Capacity and Lung Function of Patients.
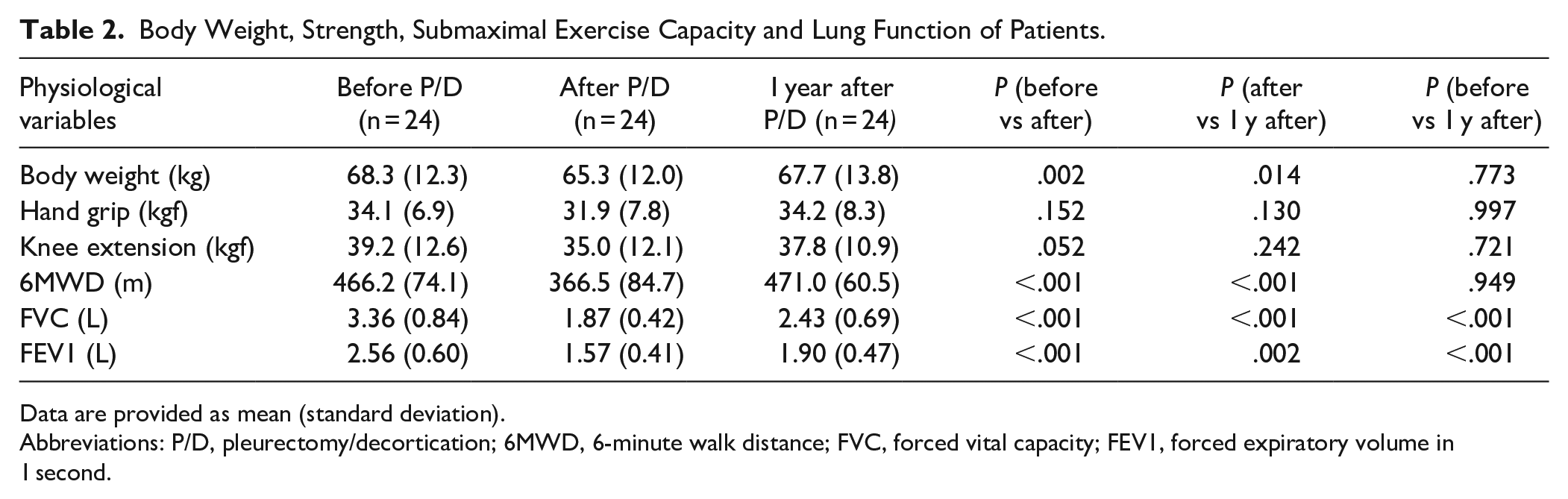
Data are provided as mean (standard deviation).
Abbreviations: P/D, pleurectomy/decortication; 6MWD, 6-minute walk distance; FVC, forced vital capacity; FEV1, forced expiratory volume in 1 second.
Pulmonary Function
The pulmonary function data are summarized in Table 2. Postoperative FVC and FEV1 were significantly lower than preoperative values (both P < .001). FVC and FEV1 at 1-year postoperatively were significantly lower than preoperative values (both P < .001). FVC and FEV1 at 1-year postoperatively were significantly higher than preoperative values (both P < .001).
Health-Related Quality of Life
HRQOL data are summarized in Table 3. Postoperative PF, BP, GH, VT, SF, MH, and physical component summary scores decreased significantly relative to the preoperative values, while changes in scores in other domains were not statistically significant. Significant increases were noted at 1-year postoperatively in the PF, BP, GH, VT, SF, MH, physical component summary scores, and mental component summary scores than the postoperative period, whereas changes in the scores in other domains were not statistically significant. There was no significant difference in domain scores between the preoperative and 1-year postoperative period.
Health-Related Quality of Life and Health Utility of Patients.

Data are provided as mean (SD).
Abbreviations: P/D, pleurectomy/decortications; SF-36, short form 36. Higher scores indicate better quality of life; domain scores range from 0 to 100; SF-6D, Short-Form Six-Dimension. Higher scores indicate better utility; domain scores range from 0 to 1.
Health Utility
Health utility data are summarized in Table 3. Postoperative values decreased significantly relative to preoperative values. Significant increases were noted at 1-year postoperatively relative to the postoperative period. There was no significant difference between the preoperative and 1-year postoperative period.
Correlations Between Health Utility and Physical Function
Correlations between health utility and physical function with respect to the differences between these values in the preoperative, postoperative, and 1-year postoperative periods are presented in Table 4. Regarding the difference between the preoperative and 1-year postoperative values, 6MWD correlated with SF-6D.
Correlations Between Health Utility and Physical Function.

Statistical analysis was performed using Pearson’s correlation coefficient.
Abbreviations: Δ, delta represents the difference in preoperation, postoperation, and 1 year after operation; Knee ext, knee extension; 6MWD, 6-minute walk distance; FVC, forced vital capacity; FEV1, forced expiratory volume in 1 second; SF-6D, Short-Form Six-Dimension.
P < .05.
Discussion
This is the first study to report health utilities of MPM patients who underwent P/D. Our results showed that patients who underwent P/D surgery had a significantly lower postoperative health utility than preoperative health utility. However, 1 year later, their health utility markedly improved compared to their postoperative values. Additionally, these patients had a significantly lower postoperative body weight, exercise capacity, and lung function than their preoperative values. Moreover, 1 year later, their health utility showed marked improvement compared to their postoperative values. Correlations were found between health utility and exercise capacity, considering the differences between the preoperative, postoperative, and 1-year postoperative values.
EPP patients had a significantly reduced pulmonary function compared to P/D patients. Ambrogi et al32,33 evaluated 29 consecutive patients who underwent neoadjuvant chemotherapy, EPP, and adjuvant radiation. An extensive list of quality of life (QOL) measurements was reported at baseline and post-surgery for approximately 3 years of follow-up. Although lung and cardiac functions were stable at 6 months, they significantly deteriorated at 12 months. Pain, dyspnea, cough, and fever initially improved at 3 months post-surgery but deteriorated again at 12 months. The 36-item Short Form (SF-36), a 36-item survey of physical and mental health summary scores, improved across all domains at 3 months, but only the physical QOL domains remained above baseline at 12 months. Similar results were obtained using the St. George respiratory questionnaire. Rena and Casadio 34 studied 77 patients with stage I or II mesothelioma, where 40 patients underwent EPP and 37 underwent P/D. The EORTC QLQ (The European Organization for Research and Treatment of Cancer Quality of Life Questionnaire) C30 questionnaire was administered at baseline and 6 and 12 months post-surgery, and both procedures resulted in significant impairment of all EORTC C30 variables at 6 months. Soysal et al 35 reported QOL symptoms at baseline and 6-month follow-up from 100 consecutive patients who underwent P/D or partial pleurectomy over a 19-year period. At 6 months, 71% of patients reported decreased chest pain, 40% had decreased cough, 37% had decreased dyspnea, and 30% reported decreased chest constriction.
Previously, we reported that in patients undergoing P/D, postoperative 6MWD, FVC, and FEV1 were significantly lower than their preoperative values in the acute phase. 36 However, at 1 year after surgery, 6MWD improved to the same degree as before surgery. 37 This could be because P/D preserves the lung parenchyma and does not markedly disrupt the patient’s daily activities. Many patients continue MPM management while working, so their levels of daily activities are maintained.
In our study, SF-6D was used as an easily obtainable measure of health utility. SF-6D responses were then given a preference-based utility tariff using the parsimonious consistent model, which allowed for the estimation of QALYs owing to morbidity. However, there are few reports of quality of life during and after treatment in the acute phase after P/D.35,38 In our study, SF-6D values deteriorated after P/D. However, 1 year after surgery, SF-6D values improved to preoperative levels. In a previous study, physical components tended to improve more than mental components of patients at 12 months following EPP. 32 A previous study reported that QOL was significantly associated with exercise capacity at 1 year after P/D. 37 Concerning HRQOL, previous findings suggest that P/D has a greater effect on the mental component than on the physical component in the convalescent phase. 37
Study Limitations
This study has a few limitations. First, this was not an interventional study; therefore, causality could not be estimated for the effects of rehabilitation interventions (such as prehabilitation) on the outcomes measured in our study. Second, in the present study, patients with recurrent malignant mesothelioma were not included, which may have caused selection bias. Third, the factors of poor pulmonary function of patients pre and postoperatively were not investigated. Persistent poor pulmonary function after P/D is an ongoing problem in MPM patients. To explain the factors of poor pulmonary function, a multivariate analysis needs to be performed in a future study. Fourth, this study did not consider the effect of chemotherapy on HRQOL and could not be compared with the effect of P/D on HRQOL. Finally, in the present study, we were unable to correct for correlations between multiple measurements in the same patient when determining correlations between physical function and health utility values. In future studies, we are considering the use of mixed models to solve these problems.
Clinical Implications
For MPM patients, exercise tolerance and health utility were shown to be related. Physicians, nurses, and rehabilitation staff should note these findings, which may provide insight into the development of customized rehabilitation strategies in the convalescent phase for MPM patients who undergo P/D.
Conclusions
The aim of the current study was to assess the health utility and physical function before, after, and 1 year after P/D in MPM patients, and to assess how health utility and physical function are affected by the response to surgery. In conclusion, patients with MPM who underwent P/D demonstrated improved health utility and physical function when compared with their postoperative values in the convalescent phase.
Footnotes
Acknowledgements
The authors are grateful to the study participants and the physiotherapists at the Rehabilitation Department and surgeons at the Department of Thoracic Surgery of the Hyogo College of Medicine Hospital.
Author Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Takashi Tanaka, Shinichiro Morishita, Masaki Hashimoto, Toru Nakamichi, Yuki Uchiyama, Seiki Hasegawa, and Kazuhisa Domen. The first draft of the manuscript was written by Takashi Tanaka and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the Hyogo College of Medicine Institutional Committee on Human Research (approval number: 1690).
Consent to Participate
Written informed consent was obtained from all participants.
Consent for Publication
Written informed consent was obtained from all participants.
Availability of Data and Materials
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
