Abstract
Objective:
We aimed to investigate the effects of exercise, monitored and managed using smart bracelets, on body composition, and quality of life in breast cancer survivors.
Methods:
A before-and-after study was conducted in 109 patients who were in the recovery phase of breast cancer and attended the Breast Surgery Department of the Cancer Hospital of Fudan University up to December 2017. Patients were advised to adhere to at least 150 minutes of moderate-intensity exercise per week, and a smart bracelet was issued to each participant to record their daily exercise data for 3 months. Bioelectrical impedance analysis was used to observe the effects of short-term unsupervised exercise intervention on body composition in patients recovering from breast cancer. Patients completed the Functional Assessment of Cancer Therapy-Breast to assess health-related quality of life.
Results:
Weight, body mass index (BMI), body fat mass (BFM), fat mass index (FMI), percent body fat (PBF), arm circumference (AC), arm muscle circumference (AMC), and visceral fat area (VFA) were lower than baseline after exercising for 3 months based on data from the wearable devices (P < .05).
Conclusion:
In this study, we demonstrated that short-term exercise may be beneficial for postoperative breast cancer survivors. A wearable device could help patients track physical data easily and promote a healthier and more positive life.
Introduction
Breast cancer is one of the most common malignancies in women. According to the latest global cancer statistics published in 2018, the morbidity (24.2%) and mortality (15%) of breast cancer were the highest among all female cancer cases. 1 In the past 30 years, the morbidity and mortality of breast cancer in China have also been increasing year by year. The incidence of female breast cancer in China was 19.2% in 2018, and 367 900 people were diagnosed with breast cancer, which ranked fourth for the number of female cancer deaths. Although the incidence of breast cancer in China is low compared to other countries, it has increased by 20% to 30% over the past 30 years, with annual increases of 3% to 5%, far exceeding the global average increase (1.5%). Such increases in frequency are due to the westernization of the diet, excessive intake of red meat and processed meat products, and poor lifestyle habits such as a sedentary lifestyle and lack of exercise.2,3
In recent years, there has been increasing interest in prognostic risk factors for breast cancer patients. Currently, evidence-based medicine suggests that the age at diagnosis, tumor size, tumor tissue grade, presence of lymph node metastases, and the presence of positive estrogen receptors affect patient prognosis. 4 With the continuous exploration of newer surgical approaches and chemotherapeutic agents, the lifestyle of breast cancer patients has gradually become the focus of research. Several randomized trials have followed healthy women and breast cancer patients and found that personal lifestyle factors such as dietary structure, weight change, and exercise can have an impact on patient prognosis. 5 Obesity and being overweight are closely related to the occurrence and prognosis of many cancers. Appropriate exercise can reduce body weight, decrease the secretion of androgens and estrogens in the body, reduce the risk of breast cancer recurrence, and improve patients’ quality of life.6,7 In addition, exercise also influences metabolism and improves prognosis by reducing the inflammatory response and insulin resistance in the body. 5 Supervised exercise, which forces patients to exercise at fixed times and places, has provided a good influence on cancer patients. 8 Frequency, duration, and intensity of exercise could be in good control under the supervision of experienced trainers, but the choices of exercise are limited, making the program less pleasurable, which may lead to poor patient compliance. 9 Some recent studies showed unsupervised exercise has better adherence than supervised, with exercise freed from times and places. 10 However, current clinical studies related to cancer prognosis mainly intervene, detect, and collect data from patients through telephone follow-up, and the data lack objectivity, accuracy, and continuity makes it difficult to promote the findings on a large scale. 11
In the context of rapid technological development, wearable devices represented by smart bracelets are now widely used. They can objectively and continuously monitor and record real-time data such as physical activity, energy consumption, and sleep quality of the wearer, allowing users to more conveniently understand their own health status, adjust their lifestyle in a timely manner, and prevent or reduce the potential risk of disease occurrence. Smart bracelets are mainly used in the management of patients with chronic diseases such as diabetes, cardiovascular diseases, stroke, and early functional recovery after surgery.12,13 Currently, there are dozens of studies that have used smart bracelets as main components of an intervention for cancer survivors. Most of them have claimed wearable technology with exercise programs could increase physical activity of cancer survivors, but a few pilot studies have focused on the influences on cancer survivors’ body composition.8,14-16 The aim of the present study was to investigate the effects of unsupervised exercise, based on smart bracelet monitoring, on the body composition and quality of life of breast cancer survivors.
Materials and Methods
Study Subjects
One hundred and nine breast cancer survivors in Fudan University Shanghai Cancer Center were selected for this study from November 8, 2017 to March 22, 2018. The study was approved by the Hospital Ethics Committees (registration number: 1711178-7).
Inclusion criteria: (1) age 18 to 65 years; (2) stage I to III breast cancer, more than 1 year after surgery; (3) major treatment completed (including surgery, radiotherapy, chemotherapy, excluding endocrine therapy); (4) possession of a smartphone with Bluetooth function and proficient in using WeChat to request medication dispensing on the platform; and (5) voluntary participation and commitment to wearing the smart bracelet continuously for at least 3 months.
Exclusion criteria: (1) breast cancer patients with distant metastases; (2) women who were breastfeeding or pregnant; (3) serious mental disorder or drug abuse; (4) physical lesions that affect normal exercise, such as fractures, limb disabilities, and severe rheumatoid arthritis; (5) prior participation in other planned exercise programs; (6) respondents with the Godin Leisure-Time Exercise Questionnaire (GLTEQ) scores greater than 90; (7) inability to connect to the YanKang e-follow-up, the full-course management platform; and (8) patients who could not commit to wearing the bracelet continuously.
Study Method
A smart bracelet (Mi Band 2, developed by Huami Technology Company and based on the Amazon health cloud data services) was issued to each participant, and patients were instructed on how to properly use them. According to the 2017 Lifestyle Guidelines for Breast Cancer Patients of the Women’s Health Branch of the Chinese Society of Preventive Medicine, 17 a healthy lifestyle manual was designed and distributed, and patients were advised to adhere to at least 150 minutes of moderate-to-vigorous physical activities (MVPAs) per week, such as walking, cycling and running (5 times per week, 30 minutes each time). Due to the limitations of bracelet recording, we had to suggest that patients do walking and running during the program. The 30-minute moderate-intensity (4.5 MET) exercise calorie consumption value was calculated based on the patient’s own body weight and set as the daily exercise target. Before the program beginning, face to face exercise education was provided to each participant by a professional trainer. Each participant was able to monitor their daily calorie consumption in real time using the smart bracelet and feedback their feelings, such as feeling stronger than before or not and emotional feelings, by telephone follow-up every 2 weeks.
Observation Indicators
Main Observation Indices
Body composition analysis
Each patient’s body composition was measured 1 day before and 90 days after wearing the smart bracelet, to observe whether short-term exercise had an effect on each index of body composition. The measurements were performed using a segmental multi-frequency bioelectrical impedance analysis (SMFBIA) analyzer (Inbody S10, Biospace Co.). The patient was checked in lying position and the electrodes were attached to the ankles for leg measurement and thumbs and middle fingers for arm measurement. All the patients fasted 2 hours before the measurement. The measurements included body fat mass (BFM), fat-free mass (FFM), skeletal muscle (SM), mineral content, and so on. BMI of each breast cancer patient was calculated before and after wearing the smart bracelet using the formula: BMI = body mass (kg)/[height (m2)].
Fat mass index (FMI) and fat-free mass index (FFMI) were calculated as follows: FMI = FM (kg)/[height (m2)]; FFMI = FFM (kg)/[height (m2)].
Smart bracelet data analysis
The data recorded by the smart bracelet worn by the patients included daily walking and running steps, time, distance, and calories consumed. The data were stored in the band for up to 30 days and, once linked to the app (Mi Fit), they were synchronized to the user’s account. Patients could get access to the data from the app (Mi Fit) synchronized with the equipment. Prior authorization was obtained from each participant to access their daily statistics through the health management system (Shanghai Ruochu Information Technology Co., Ltd.).
Secondary Observables (Quality-of-Life Assessment)
Each patient’s quality of life was evaluated using the Functional Assessment of Cancer Therapy-Breast (FACT-B), 18 developed by the Center for End Results Research and Education in the United States. The scale consists of 5 main categories: physical wellbeing (PWB), social/family wellbeing (SWB), emotional wellbeing (EWB), functional wellbeing (FWB), and additional concerns about breast cancer (BCS). The scales were in the form of questionnaires to be completed by the patients, who were administered the questionnaires before and after 3 months of wearing the smart bracelet.
Statistical Analysis
SPSS 21.0 software was used for statistical analysis of the data. Measurements conforming to a normal distribution were expressed as
Results
In total, 109 patients were enrolled in this study and completed the initial data assessment. All patients received modified radical mastectomy, including 99 patients receiving both chemotherapy and radiotherapy and 10 patients receiving only chemotherapy; 3 patients did not complete the questionnaire after 90 days and 2 patients refused to have their data assessed again. Data recorded by the bracelets for a total of 91 patients were obtained through the health management system, and data were not successfully obtained for another 13 patients due to account privileges.
Baseline Characteristics of the Participants
The average age of the 91 women recovering from breast cancer was 48.59 ± 8.04 years. There were 41 patients with stage I breast cancer, 47 patients with stage II, and 3 patients with stage III. Among these study subjects, 23.1% of the patients were obese or overweight (BMI >23.9 kg/m2) (Table 1).
Characteristics of Study Samples.

Abbreviations: BMI, body mass index; ER, estrogen receptor; PR, progesterone receptor; HER-2, human epidermal growth factor-2.
Analysis of Bracelet Exercise Data
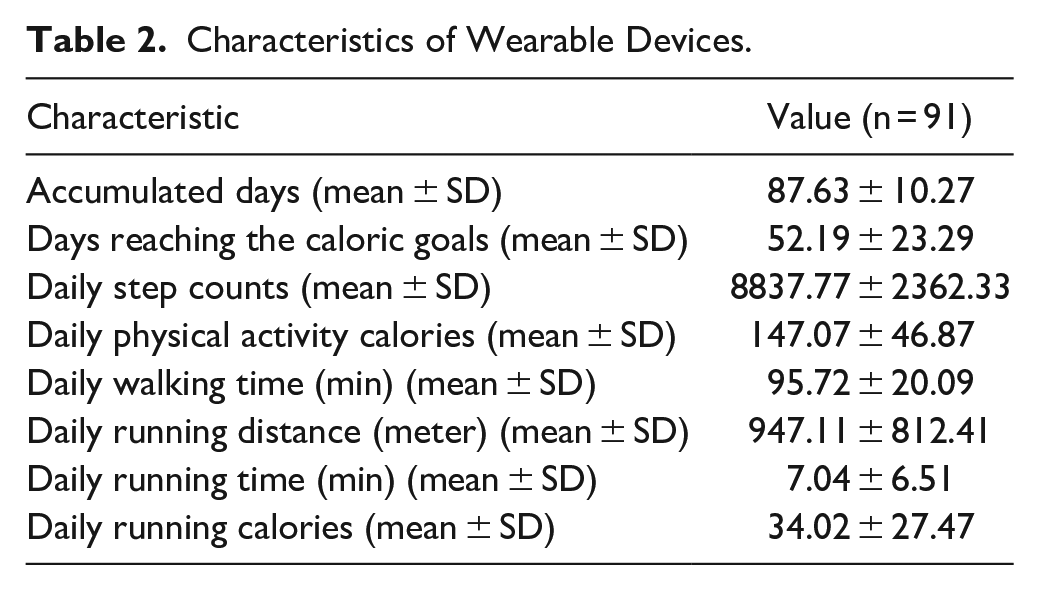
A total of 91 breast cancer survivors walked 8837.77 ± 2362.33 steps per day. The daily walking time was 95.72 ± 20.09 minutes, the daily calorie consumption was 147.07 ± 46.87 kcal, and the number of days that reached the calorie goal was 52.19 ± 23.29 days (Table 2).
Characteristics of Wearable Devices.
Changes in Body Composition Before and After Short-Term Exercise in Breast Cancer Survivors
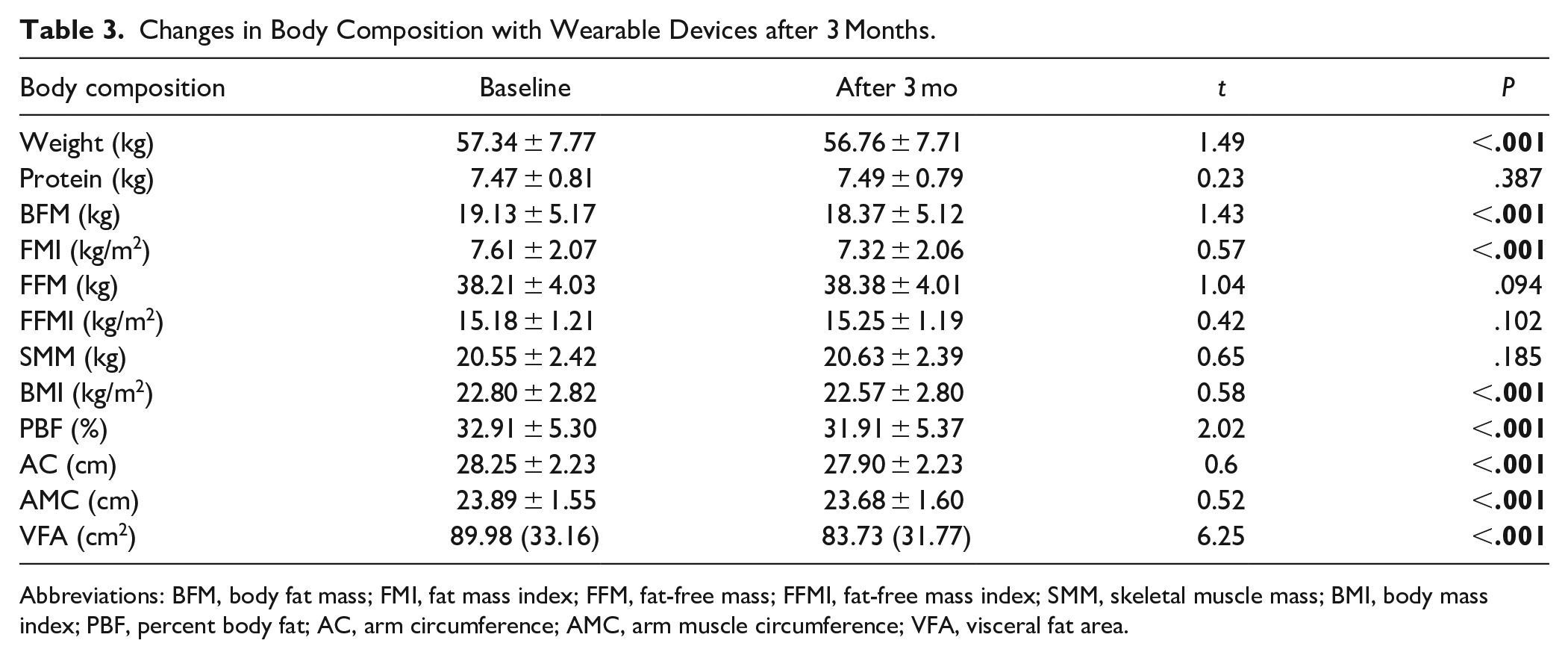
After 3 months of monitoring with the smart bracelet, patients had different degrees of changes in body composition indexes. Body mass, BMI, BFM, FMI, PBF, AC, AMC, and VFA were significantly lower than 3 months before, and the differences were statistically significant (P < .05), as shown in Table 3. Patients’ protein content, FFM, FFMI, and SMM were slightly increased compared with 3 months before, but the differences were not statistically significant (P ≥ .05).
Changes in Body Composition with Wearable Devices after 3 Months.
Abbreviations: BFM, body fat mass; FMI, fat mass index; FFM, fat-free mass; FFMI, fat-free mass index; SMM, skeletal muscle mass; BMI, body mass index; PBF, percent body fat; AC, arm circumference; AMC, arm muscle circumference; VFA, visceral fat area.
Changes in Quality of Life Before and After Short-Term Exercise in Breast Cancer Survivors
The independent sample t-test was applied to compare the total FACT-B scale and scores of each category before and after 3 months of exercise in breast cancer survivors. The results showed that there was a significant difference (P < .05) in the scores of the additional concerns category, which improved after exercise compared to before exercise. However, the remaining categories and total scores were not significantly different with P ≥ .05 (Table 4).
Changes in FACT-B of Study Samples after 3 months.

Correlation Analysis Between the Exercise Bracelet Recording Index and Each Index of Body Composition
The results (Table 5) showed that the average walking time correlated with the changes in BFM, PBF, and FMI, and longer walking times were associated with lower BFM, PBF, and FMI values; the average running calories consumption correlated with FFM, and when more running calories were burned, the FFM was higher.
Correlation Analysis Between the Exercise Bracelet Recording Index and Each Index of Body Composition.
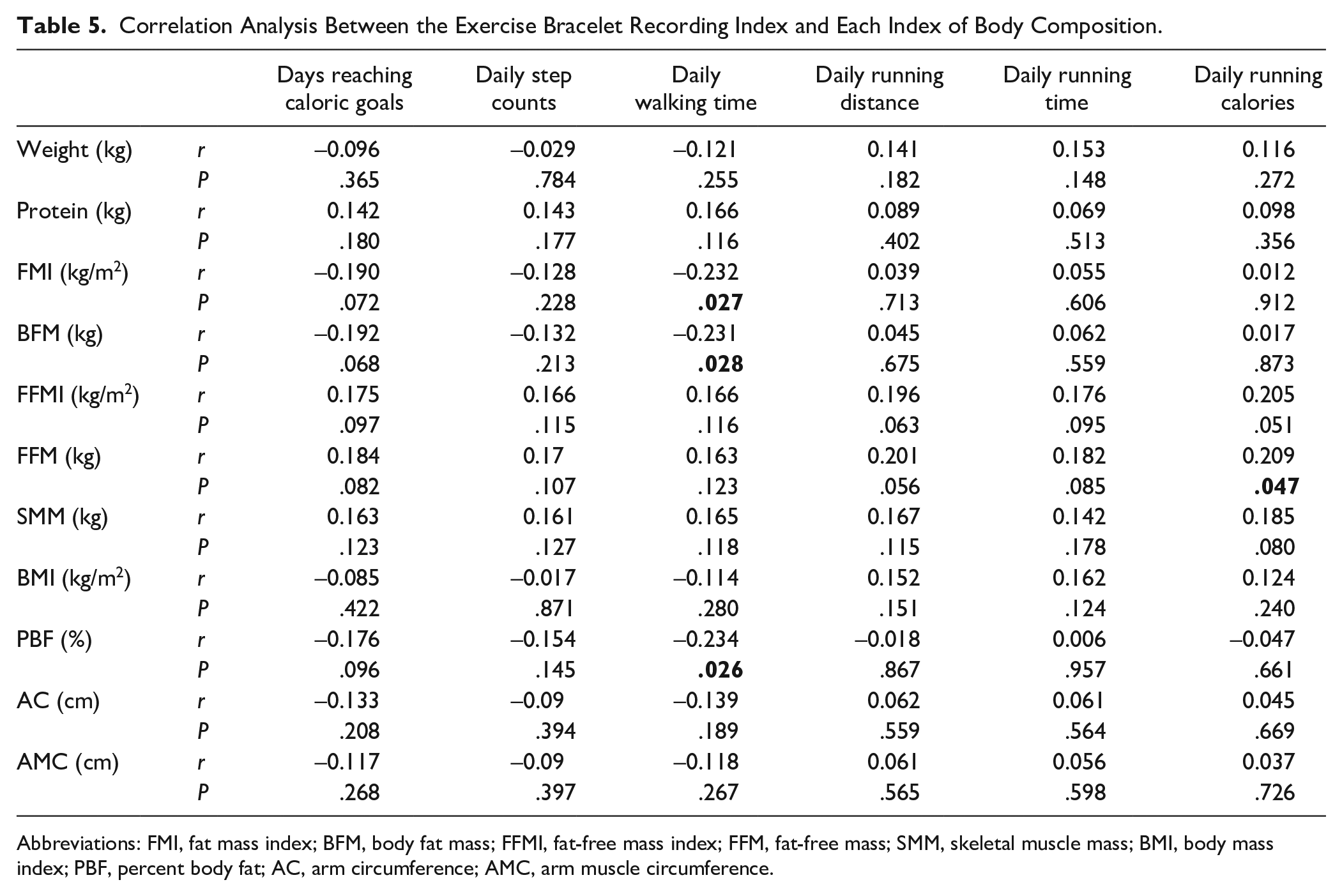
Abbreviations: FMI, fat mass index; BFM, body fat mass; FFMI, fat-free mass index; FFM, fat-free mass; SMM, skeletal muscle mass; BMI, body mass index; PBF, percent body fat; AC, arm circumference; AMC, arm muscle circumference.
Discussion
Breast cancer, a public health issue of global concern, seriously threatens the quality of life of women. The 5-year relative survival rate of breast cancer patients in China is about 82% (81.0%-83.0%), which is lower than that of developed countries such as the United States of America (≥90%). 19 Studies have found that the lifestyle of cancer patients is closely related to the occurrence and prognosis of cancer.5-7 In this study, we intended to monitor patients’ daily exercise through the wearing of a smart bracelet to assess whether short-term exercise could help improve the body composition and quality of life of breast cancer survivors. The results of the study indicated that short-term exercise could significantly improve body composition and reduce body fat in breast cancer survivors, but there was no significant improvement in quality-of-life scores.
The composition of the human body mainly consists of 2 parts: adipose tissue and lean body tissue, of which lean body tissue includes water, protein, muscle, and other substances. Adipose tissue is the main energy storage site in the body, and also participates in regulating neuroendocrine function and autoimmunity by secreting hormones and cytokines such as leptin, tumor necrosis factor (TNF)-α, and interleukin (IL)-6. Excessive accumulation of adipose tissue in the body may induce metabolic syndromes such as metabolic inflammatory response, diabetes, and cardiovascular diseases. 20 Freedman et al indicated that breast cancer patients in stages I to III showed a significant increase in body fat after adjuvant chemotherapy. 21 This may be related to the fact that the drugs used by patients during their treatment can lead to some degree of lean body mass loss. Thus, it is important to start an intervention on breast cancer survivors as soon as possible.
With the continuous improvement of medical technology, the survival period of cancer patients has been extended, and ways to improve the quality of life have become a key concern for cancer patients. Exercise, as a safe and effective life intervention, has been widely used in the rehabilitation treatment of cancer patients. The Guidelines for Exercise for Cancer Survivors published by The America College of Sports Medicine (ACSM) states that cancer patients should avoid sedentary activities and should perform no less than 150 minutes of moderate intensity or 75 minutes of high intensity aerobic exercise per week. 22 Our current study suggested that breast cancer survivors showed improvement in body composition after a 3-month unsupervised short-term exercise intervention, and in particular, obesity-related indicators were significantly lower than before. Thomas et al found that aerobic and resistance exercises could reduce BFM and BMI, thus, alleviating the side effects of endocrine therapy. 23 Kim et al suggested that exercise not only improved the motor function of the shoulder joint in breast cancer patients, but also reduced the levels of breast cancer recurrence markers. 24 Moreover, most of the patients completed this program and provided positive feedback, such as being more energetic and stronger, from telephone follow-up every 2 weeks. Cornette et al showed aerobic capacity of breast cancer survivors was increased after 6 months of unsupervised exercise. 25 Thus, it is clear that regular exercise can improve the body composition of breast cancer patients and assist their recovery. Similarly, unsupervised exercise may also improve other aspects of physical condition of patients, which should be measured in further studies.
Quality of life is an important outcome indicator of tumor recovery. The use of scales to detect and evaluate the health status of tumor patients helps physicians to have a more comprehensive understanding of the patient’s treatment so that the treatment plan can be adjusted in a timely manner.26,27 Studies have indicated that lower quality of life is one of the important risk factors affecting prognosis. 28 Exercise can effectively improve the quality of life of breast cancer patients. 29 We found that only the additional concerns category score improved significantly after short-term exercise compared to before exercise, and there were no statistically significant differences in the remaining category scores. Christina et al conducted experiments involving aerobic and resistance exercise for 6 months in breast cancer patients, and the results showed that moderate-intensity aerobic and resistance exercises significantly improved the quality of life of patients. 30 Schmidt et al found the same significant improvement in quality of life after 12 weeks of resistance exercise in patients with breast cancer. 31 This suggested that short-term low-intensity walking may not improve the quality of life of breast cancer patients. Therefore, based on the available evidence, improving the quality of life of patients may require moderate-intensity aerobic or resistance exercise.
Exercise as an intervention applied to the lives of breast cancer survivors requires continuous and objective monitoring and assessment of the amount of exercise, so it is important to quantify the amount of exercise. Traditionally, exercise interventions for cancer rehabilitation patients have mostly used pedometers as a self-monitoring tool, but pedometers can only record a single activity and do not allow for 24-hour dynamic monitoring. 32 Smart bracelets can provide real-time feedback and cues, and when connected to a mobile application, users can monitor their exercise through uploaded data which can even effectively promote increased exercise. A study by Brigid et al. found that giving patients a smart bracelet significantly increased their moderate-intensity exercise and significantly decreased the amount of time spent sitting compared to the control group; thus, resulting in healthier and more active patients. 33 The present study found that mean walking time was negatively correlated with BFM, PBF, and FMI, while mean running calorie consumption was positively correlated with FFM. A study from the USA found that after giving participants a smart bracelet for 1 academic year, overweight women had significantly lower body fat levels than before. 34 This suggests that we can focus on daily walking time and increase it appropriately for breast cancer survivors with excessive body fat content. For patients with less muscle mass in the recovery phase, protein supplementation can be added along with moderate-intensity exercise to increase daily calorie consumption. 35 However, as patients’ compliance and length of time wearing the bracelet varies, and some do not even wear bracelets every day, further studies with a large population are recommended to investigate the significance of our findings.
In conclusion, short-term exercise intervention could improve the body composition of breast cancer patients, but it did not significantly improve their quality of life, which may be related to exercise intensity and exercise mode. Wearing a smart bracelet allowed patients to monitor exercise more conveniently and adjust exercise time and exercise mode according to their own condition in real time, so that the lifestyle of patients during cancer recovery became healthier and more active. Further studies should involve more indicators, especially biomarkers such as leptins, TNF-α and C-reactive protein, and should assess lifestyle at the beginning of the program as well as account for the energy intake during the program. In additionally, research is also needed on the accuracy, effectiveness, and practicality of smart bracelets for monitoring exercise and improving the compliance of breast cancer recovery patients wearing bracelets.
Footnotes
Author Contributions
Liuqing Xu drafted and revised the manuscript. Changming Zhou analyzed and interpreted the data. Yiqun Ling designed the study and critically reviewed the manuscript. Huiping Ding, Qiong Wang, Yan Wu, Yong Qian, Bingqin He, and Tianhao Ni collected the data. All authors approved the final version of manuscript submitted for publication.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the Fudan University Shanghai Cancer Center Ethics Committee (Approval Number: 1711178-7).
