Abstract
Introduction
Radiofrequency ablation (RFA), as one type of local treatment modality, challenges surgery for hepatocellular carcinoma (HCC) <3 cm and is currently widely used owing to its safety, effectiveness, minimal invasiveness, and shorter hospitalization1,2; however, several cases of rapid and aggressive recurrence of HCC after RFA have been reported.3,4 Our team previously demonstrated the pro-metastatic effects of insufficient RFA in a HCC orthotopic nude mice model, 5 and the underlying molecular mechanism might be that insufficient RFA induced epithelial-mesenchymal transition (EMT) through activated β-catenin signaling in residual HCCLM3 cancer.
There are also many other studies about the explanation of enhanced metastasis potential in residual cancer after RFA. Kong et al reported that hyperthermia might play an important role in the rapid growth of residual HCC after RFA by promoting angiogenesis of residual cancer via HIF-1a/VEGFA. 6 Yoshida et al demonstrated that suboptimal RFA accelerated HCC growth and spread by transiently inducing a cellular phenotype that was EMT-like and which was also more aggressive. 7 Directing our focus onto the respective mechanism to produce possible interventional measures and improve the efficacy of RFA on HCC patients is necessary.
Interferon-α (IFN-α), which initially was discovered for its antiviral activity, belongs to the group subtype 1. It also has a series of other biological properties including antitumor and immune regulation activity. 8 IFN-α also showed remarkable efficacy in treatment of HCC; several studies have also demonstrated the encouraging efficacy of IFN-α monotherapy or IFN-α-based combination therapy for HCC.9,10 Wang et al verified that high-dose and long-term therapy with IFN-α inhibited tumor growth and recurrence in nude mice bearing HCC xenografts with high metastatic potential. 11 In a randomized controlled trial, Lo et al reported that adjuvant interferon therapy showed a trend for survival benefit for postoperative hepatitis B-related HCC patients, especially in those with pTNM stage III/IVA tumors. 12 These findings were also consistent with the outcome of our previous randomized control trial, which showed that 18 months of postoperative IFN-α treatment delayed recurrence and prolonged patient survival. 13
Songyou Yin (SYY) is a traditional Chinese medicine (TCM) and contains 5 herbal compounds. Our team’s previous study verified the effectiveness of treatment of HCC in vivo and in vitro.14-16 SYY effectively inhibited tumor growth, metastasis, and prolonged survival in nude mice models. Moreover, regarding resistance to chemotherapy, SYY enhanced HCC sensitivity to oxaliplatin through inhibition of stemness or reverse EMT. Based on the above-mentioned evidence, we proposed the hypothesis that SYY could play a role in minimizing the pro-metastatic effects of insufficient RFA in HCC, particularly when combined with IFN-α.
For the rapid progression of residual HCC after RFA, we first attempted to use combinational therapy (IFN-α and SYY) as one of the new approaches in orthotopic nude mice models. The aim of the present study was to explore whether combined therapy displays an advantage over the monotherapy of each drug and to explore their respective potential mechanisms.
Materials and Methods
Cell Line and Animals
The HCCLM3-G with stable green fluorescent protein (GFP) expression (which had a high metastatic potential 17 ) was used in the present study. The cells were maintained in Dulbecco’s modified Eagle’s medium (DMEM; Gibco BRL, Rockville, MD) with 10% fetal bovine serum (Life Technologies, Carlsbad, CA), 100 mg/mL penicillin G at 37°C in a humidified atmosphere containing 5% CO2. Male athymic BALB/c nu/nu mice, weighing ~20 g at 4 to 6 weeks of age, were obtained from SLAC Laboratory Animal Co Ltd, Shanghai, China. All mice were maintained under specific pathogen-free conditions. All animal protocols were approved by the Ethical Committee on Animal Experiments of Animal Care Committee of Fudan University, Shanghai, China.
Characterization and Preparation of Herbal Extracts
The Chinese herbal medicine formula, SYY, a dietary component, is authorized by the Chinese State Food and Drug Administration (Grant No. G20070160). The mixture includes 5 Chinese medicinal herbal extracts and has a fingerprint in the following proportions (w/w): Salvia miltiorrhiza Bge, 14.3%; Astragalus membranaceus Bge, 14.3%; Lycium barbarum L, 23.8%; Crataegus pinnatifida Bge, 23.8%; and Trionyx sinensis Wiegmann, 23.8% (all from China). The fingerprint and protocol of preparation have previously been reported. 18 The SYY used in this study was produced by Shanghai Fang Xin Pharmaceutical Technology Co Ltd (Shanghai, China).
Establishment of Insufficient RFA Orthotopic Nude Mouse Model
According to the method developed by our institute, the human HCC orthotopic nude mouse models with HCCLM3-G cells were established. 19 The HCC orthotopic nude mice model has been established in our liver cancer institute for about 20 years, and most technicians are able to master this technique skillfully. The success rate of this animal model is close to 100%. Two weeks later, a total of 64 nude mice received the insufficient RFA intervention, and the specific operation detail referred to in our previous description. 5
Drug Treatments for Insufficient RFA Nude Mice Models
Twenty-four hours after insufficient RFA, 64 nude mice bearing orthotopic xenografts were randomly divided into the control group, IFN-α group, SYY group, and the IFN-α + SYY group. The IFN-α group mice were treated with subcutaneous injection daily with 0.1 mL IFN-α (Sinogen, Kexing Bioproduct Company Ltd, Shenzhen, China) at a dose of 7.5 × 106 U/kg/day, and orally with 0.1 mL distilled water; the SYY group mice were treated with subcutaneous injection with 0.1 mL (0.9%) normal saline (NS) and orally with 0.1 mL SYY (8.4 g/kg/day) every day. The IFN-α + SYY group mice were treated with subcutaneous injection with 0.1 mL IFN-α at a dose of 7.5 × 106 U/kg/day and orally with 0.1 mL SYY (8.4g/kg/day) every day; the control group mice were treated with 0.1 mL (0.9%) NS and 0.1 mL distilled water in the same method as the other groups. Five weeks after the initial treatment, 6 mice from each of the groups were sacrificed to evaluate tumor growth and metastasis. The largest (a) and smallest (b) tumor diameters were measured, and the tumor size was calculated as follows: Tumor volume (mm3) = a (mm) × b (mm) × b (mm)/2. 11 The lungs were excised, and the images of the GFP-positive metastatic foci were obtained (MZ205; Leica, Wetzlar, Germany). The lung tissues were sectioned serially, and hematoxylin-eosin staining was performed to confirm the above-mentioned results. The remaining mice from each group were kept for survival analysis.
Quantitative Real-Time Polymerase Chain Reaction Analysis
Total RNA was extracted from tumor tissues of each group and was reversely transcribed using a Prime Script RT reagents kit (TaKaRa Bio Inc, Shiga, Japan). Messenger RNA expression was determined by real-time polymerase chain reaction using SYBR Premix Ex Taq II (TaKaRa). The primers used for the amplification of human genes were as follows: Snail, 5′-TGCAGGACTCTAATCCAAGTTTACC-3′ (forward), 5′-GTGGGATGGCTGCCAGC-3′ (reverse); Slug, 5′-GGTCAAGAAGCATTTCAAC-3′ (forward), 5′-CTGAGCCACTGTGGTCCTTG-3′ (reverse).
Western Blot Assay
The Western blotting procedures used are described elsewhere. 20 Primary antibodies used included the following: anti-E-cadherin, anti-N-cadherin, anti-β-catenin (Abcam, Cambridge, MA), and anti-β-actin (Boster, Wuhan, China).
Immunohistochemistry
Paraffin-embedded tumor tissues were cut into standard 6-µm sections. Immunohistochemistry staining of CD31, VEGF, E-cadherin, N-cadherin, β-catenin, and MMP2 (1:100; Abcam) was performed using a standard protocol. 21 The integrated optical density or area of positive staining/total area was quantified by Image-Pro Plus software (Media Cybernetics Inc, Bethesda, MD).
Statistical Analysis
Data were analyzed by SPSS 20.0 (SPSS Inc, Chicago, IL) using Student’s t test, analyses of variance, and Kaplan-Meier method (log-rank test). All continuous variables were expressed as means ± SD or means ± SEM. P < .05 was considered statistically significant.
Results
Combined Therapy of IFN-α and SYY Attenuated Growth of Residual Cancer After Insufficient RFA and Prolonged Survival
To explore the effects of IFN-α and SYY on tumor growth in vivo, we examined the nodules formed in the residual cancers of nude mice treated with RFA or SYY alone or combined. Mice were sacrificed 5 weeks after oral perfusion, and the residual cancers were harvested. Both the control and intervention therapy groups were observed for tumor formation. The experimental results indicated that the mice that received either IFN-α or SYY showed decelerated growth of residual tumors in neoplastic colonies and possessed a decreased ratio of tumorigenic area to total area. Moreover, we found that the combination of SYY and IFN-α effectively inhibited the growth of residual cancer to the maximum extent among the 4 groups (1409.42 ± 558.56 mm3 vs 5784.17 ± 2453.46 mm3, P < .01); in addition, the volume of residual cancer in the intervention group of IFN-α alone was also less than compared with the control group (2817.17 ± 801.08 mm3 vs 5784.17 ± 2453.46 mm3, P < .05), while the group of SYY alone showed no statistically significant difference from the control group (4770.42 ± 819.95 mm3 vs 5784.17 ± 2453.46 mm3, P = .36; Figure 1A). Next, we assessed the correlation between the therapy regimens and survival prognosis using the data of a cohort of mice. The survival curve confirmed that each intervention group could prolong the survival time of mice compared with the control (P < .001), and that the combined therapy group demonstrated an extreme maximal survival time compared with other groups (68.60 ± 3.17 vs 81.70 ± 4.57, P < 0.001; Figure 1B).

Combined therapy of IFN-α and SYY suppressed growth of residual cancer after insufficient RFA and increased survival time. (A) Tumor volumes in different groups. The right bar demonstrated that either IFN-α or SYY was able to decelerate the growth of residual tumors originated from HCCLM3 with high metastatic potential after insufficient RFA, and the IFN-α co-treatment with SYY could extremely attenuate the growth of residual cancer among these groups (P < .01). (B) Log-rank survival analysis of the 4 groups, *P < .05, **P < .05, #P < .01, compared with the control group.
Combined Therapy Effectively Limited Lung Metastasis After Insufficient RFA
In our previous study, we demonstrated that insufficient RFA significantly promoted lung metastasis; thus, we opted to assess the value of combined therapy in inhibiting lung metastasis after insufficient RFA. Compared with the control group, the single IFN-α or SYY therapeutic group displayed a slight decrease in lung metastasis, while the lung metastasis rate of the combined therapy group was significantly decreased after insufficient RFA through the GFP-positive metastatic foci (P < .05; Figure 2A). The results of hematoxylin-eosin–stained lung tissues also revealed that the number of lung metastasis foci in each drug treatment group was significantly less than the control group; it was especially lower in the combined therapy group (P < .05; Figure 2B).

Combined therapy effectively decreased lung metastasis after insufficient RFA. (A) Combination with IFN-α and SYY resulted in reduced pulmonary metastasis in fluorescence (white arrows indicate pulmonary metastasis foci). (B) Confirmation of the presence of pulmonary metastasis by H&E staining (black arrow indicates metastasis node), comparison of pulmonary metastasis among the 4 groups (Right panel).
Combined Therapy Decreased Microvessel Density of Residual Cancer
The growth of tumor and the development of metastasis depends on angiogenesis, which is the adequate structure for blood supply. 22 As a highly vascularized tumor, angiogenesis plays a vital role in the origination, development, and metastasis of HCC. VEGF is overexpressed in HCC and correlates with poorer clinical outcomes. This suggests that VEGF-mediated signaling is fundamental in HCC pathogenesis, and that it may be a therapeutic target. 23 Many antiangiogenic agents are currently being tested for the treatment of HCC. IFN-α itself, or in combination with other cytokines, also was verified to have a significant effect on inhibition of angiogenesis.11,24 In the present study, we tested the effect of IFN-α on the metastatic potential of residual cancer, and especially when combined with SYY, assessed whether it exerted a greater role. Based on the immunohistochemical and statistical analysis of the residual cancer tissue, the expression level of CD31, a surface marker of neovascular endothelial cells, was detected in different groups. Subsequently, the significantly decreased expression was tested in the combined therapy group compared with the single drug groups (Figure 3A). We further analyzed the expression of VEGF after drug treatment, and the research results showed significantly attenuated expression of VEGF in the combined therapy group (Figure 3B). The above-mentioned data demonstrated the combined therapy could effectively weaken the angiogenesis of residual cancer after insufficient RFA.

The combination treatment of IFN-α and SYY could effectively restrain the angiogenesis of residual cancer. The expression of CD31 (A) and VEGF (B) was displayed in the intervention groups and control group, respectively; the bar on the right revealed that combined treatment significantly limited the expression of CD31 and VEGF in protein level compared with the control, and the group of SYY alone showed no statistically significant difference from the control in both expression of CD31 and VEGF.
Combined Therapy Reversed EMT of Residual Cancer
Since EMT is closely related to cancer invasiveness and metastasis, we examined whether combined therapy can affect the expression of EMT-related genes. The immunohistochemical analysis unveiled that compared with the control, the E-cadherin expression was remarkably upregulated in the intervention group of single SYY or IFN-α; furthermore, it was particularly higher in the combined therapy group. In contrast, the alternative EMT marker N-cadherin demonstrated an inverse trend (Figure 4A). Moreover, Western blot analysis also showed that combined therapy resulted in decreased expression of N-cadherin and an upregulation of E-cadherin (Figure 4B). Consistent with the above-mentioned results, the expression of Slug and Snail, which are considered as transcription factors of EMT and are related to metastasis, were also clearly downregulated in the combined therapy group compared with the control group (P < .05). Meanwhile, the single drug intervention groups demonstrated a slight decrease but showed no significant difference (P > .05; Figure 4C).

The combination treatment could reverse EMT of residual cancer. (A) Immunohistochemical analysis unveiled that E-cadherin expression was significantly elevated in the combined therapy group, compared with the control. In contrast to E-cadherin, the expression of N-cadherin in residual cancer tissue was extremely limited in the combined therapy group. (B) Western blot showed the changes of EMT markers in therapy groups and control group were consistent with immunohistochemical analysis data (eg, upregulation of E-cadherin and downregulation of N-cadherin). (C) RT-PCR showed the expression of transcription factors Snail and Slug were significantly attenuated at the mRNA level in combined therapy group (P < .05).
Combined Therapy Dampens the Activation of β-Catenin and MMP2
In our previous study, we observed the activation of β-catenin signaling of residual cancer induced by insufficient RFA. 5 To explore whether combined therapy can effectively attenuate this physiological process, immunohistochemical staining analysis was used to test the expression of β-catenin in tissue samples regarding their protein levels. As shown in Figure 5A and B, the expression of β-catenin was inhibited significantly by combined therapy compared with individual use alone. Increasing evidence shows that MMPs play a key role in tumor metastasis and angiogenesis. MMP2 and MMP9 are the major MMPs verified to be involved in tumor angiogenesis. 25 Therefore, we tested the expression of MMP2 and MMP9 in residual cancer tissue to explore whether both factors participated in the neovascularization modulation. The results revealed that MMP2, not MMP9, had significantly decreased expression affected by combined treatment (Figure 5C). These evidences verified that MMP2 might play a role to some extent in the antimetastatic process of combined therapy.
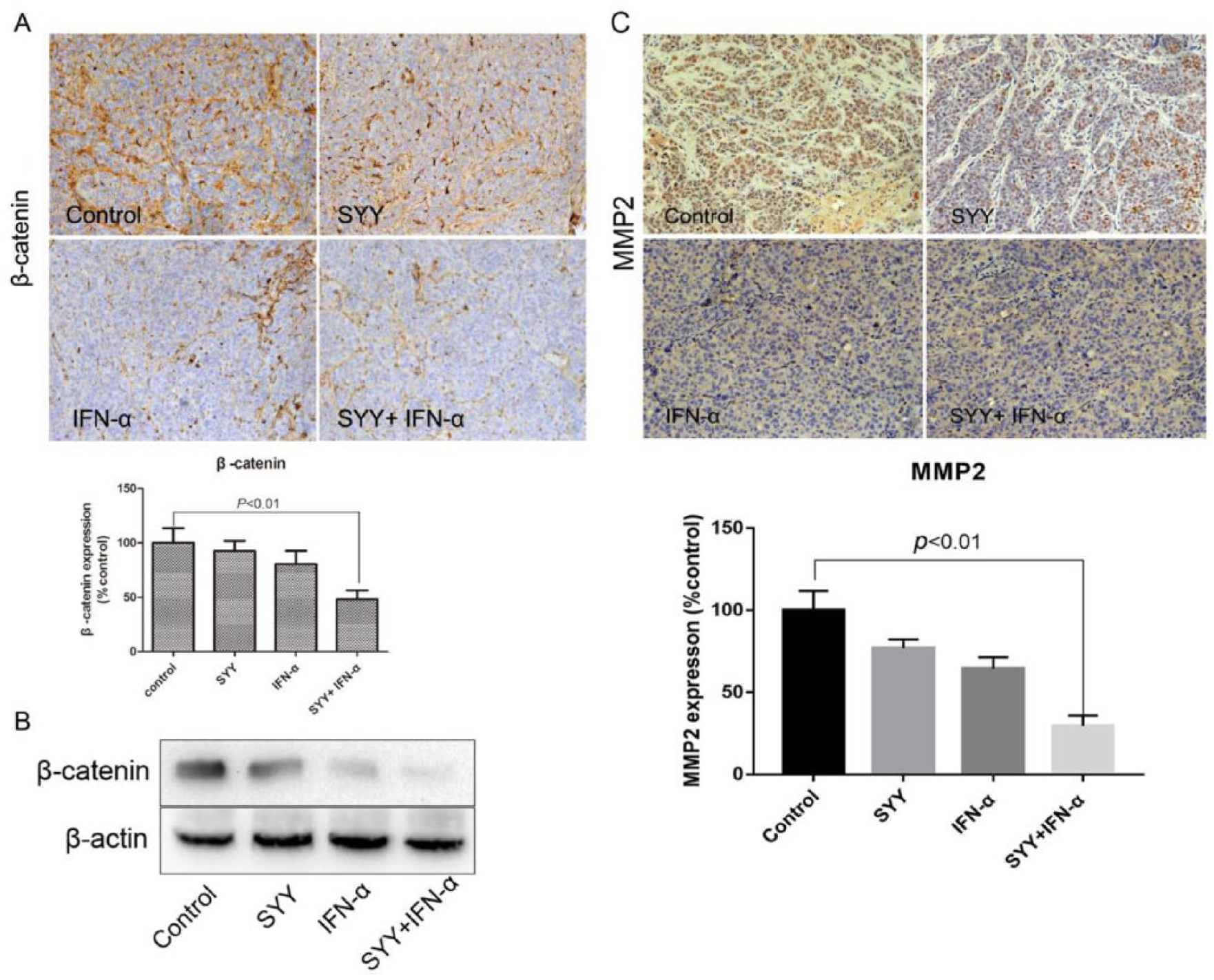
Combined therapy limited the activation of β-catenin and MMP2. (A) Immunohistochemistry revealed that β-catenin expression was extremely decreased in combined therapy group compared with the control (P < .01). (B) Western blot analysis also demonstrated the significantly attenuated expression of β-catenin in combined therapy group. (C) Immunohistochemical analysis exhibited a similar trend as β-catenin, in that combined treatment could suppress the enhanced expression of MMP2.
Discussion
As an important part of Chinese culture, TCM has played an indelible role in safeguarding and protecting the health of Chinese people in the past thousands of years. Chinese herbal medicine is the most common modality of TCM. 26 Herbal medicine was used to treat malignancies for centuries, and recent studies revealed the anticancer mechanism including apoptosis promotion, inhibition of angiogenesis, and modulation of cancer stem cells.27,28 SYY is a traditional Chinese herbal medicine, and its effective antitumor activity has been verified in previous studies conducted by our team.14,15,18,28,29
There are the remnants of HCC in some cases after RFA, and especially when the tumor is larger, or the tumor is adjacent to large blood vessels, the proportion of tumor remnants is higher. The presence of residual HCC can easily lead to postoperative local recurrence, and further affects long-term prognosis.30,31 In our previous study, the results were consistent with the above-mentioned research conclusion, and it further demonstrated that heat intervention might reduce EMT, which could result in enhanced invasiveness and metastatic ability of residual cancer. 5
To our knowledge, SYY exerted inhibition of molecular changes consistent with EMT in oxaliplatin-treated tumor tissues and cell lines. 28 Meanwhile, correlative randomized clinical trials verified that postoperative IFN-α treatment can postpone recurrence and improve overall survival in patients after curative resection of hepatitis B–related HCC.12,13 Whether SYY can inhibit the metastasis of residual cancer after insufficient RFA, particularly when combined with IFN-α, is a question yet to be answered.
In the current study, the results indicated that the combined therapy of SYY and IFN-α could prominently decrease residual cancer volume and prolong the survival time of nude mice. More important, combined treatment could effectively suppress pulmonary metastasis. Meanwhile, the use of SYY and IFN-α alone also exhibited antitumor activity. What was the underlying mechanism of antitumor effects induced by combined therapy? Mounting evidence has identified a significant correlation between EMT and invasiveness in various types of tumor.32,33 Our previous work pointed out that EMT is the main approach that enhances metastasis of residual cancer. For this reason, we focused our attention on EMT. The experimental results displayed downregulation of N-cadherin and upregulation of E-cadherin in protein levels. Moreover, the study revealed decreased mRNA expression of EMT transcription factors Snail and Slug, which were examined by real-time polymerase chain reaction in xenografts, respectively. These data revealed that combined therapy might limit the metastasis of residual cancer through attenuating EMT.
As a key factor in the Wnt/β-catenin signal pathway, β-catenin plays an important role in HCC progression, phenotype changes, and metastasis.34-36 Mutations involving the Wnt/β-catenin pathway appear to be one of the most frequent genetic events that contribute to liver carcinogenesis and progression. 36 Moreover, the correlation between β-catenin signaling and EMT has been examined in several research studies. Yang et al suggested that downregulation of miR-3127-5p promoted EMT by activating the Wnt/FZD4/β-catenin signaling pathway and might represent a therapeutic target for non–small cell lung cancer metastasis. 37 Another study also proved that Frizzled 7 (FZD7), a member of Frizzled family, promoted EMT and stemness via activating the canonical Wnt/β-catenin pathway in gastric cancer. 38 The finding of our previous study was that insufficient RFA promoted EMT of residual cancer via activating β-catenin, which was consistent with other studies. Meanwhile, the data of the current research revealed that combined therapy extremely reduced the overexpression of β-catenin in protein level of tissue samples. The above-mentioned results suggested suppression of β-catenin signaling might be an important approach of blocking EMT of residual cancer cells by the combined therapy.
As we know, there are many factors that affect the development and metastasis of tumors, and angiogenesis plays an important role in the progression and metastasis of HCC, which is a type of tumor with an enriched blood supply.39,40 We thus examined whether combined therapy could dampen the neovascularization of residual cancer. Immunohistochemical analysis showed that the microvessel density was the lowest in the combined therapy group compared with others. Angiogenesis related cytokines, such as VEGF, HGF, and MMP2, were involved in this neovascularization process. 41 The immunohistochemical analysis further verified that the expression of MMP2 was significantly downregulated in the combined therapy group. The current study findings prompted us to the idea that attenuating angiogenesis of residual cancer might be another way to restrain invasiveness by combined therapy.
To our knowledge, this is the first report to apply the combination of Chinese and Western medicine to interfere with residual cancer tissue after insufficient RFA. Fortunately, we have obtained a positive result. Although there is a long distance from its clinical application, it also provides an option for adjuvant treatment after RFA for the HCC patients. The core idea of TCM is to treat the human body as an organic whole; while the overall concept and the syndrome differentiation are its main characteristics, and this is the difference from Western medicine. In the present study, the potential mechanism of combined therapy also requires further exploration to provide more experimental and theoretical basis for the clinical application of this combined method.
Conclusion
The combined therapy of SYY and IFN-α demonstrated enhanced effects on suppressing growth and distant metastasis of liver cancer by restraining the EMT induced by activated β-catenin; the effect is superior to SYY or IFN-α use alone. Although the herbal compound SYY and IFN-α belong to Chinese medicine and Western medicine, respectively, the combined application of both exerts a stronger antitumor effect. This may also contribute to some ideas for the treatment of liver cancer by integrating traditional Chinese and Western medicine. To understand whether this model is beneficial for patients suffering from HCC requires further clinical trials in the future.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by National Natural Science Foundation of China (grant number: 81372314).
