Abstract
Keywords
Introduction
It is well documented that Indigenous people in Australia, Canada, New Zealand, and the United States consistently experience substantial inequities in cancer outcomes in comparison with their non-Indigenous counterparts, in terms of increased incidence,1-3 poorer prospects of treatment,2-4 and higher mortality rates.1-3,5 Current evidence suggests that these disparities are attributable to a range of factors, including, but not limited to, later stage at diagnosis, lower treatment compliance, lower cancer screening rates, and social deprivation.3,6
Cancer ‘patients’ are increasingly using traditional and complementary medicine (T&CM) in addition to conventional medical treatments, such as chemotherapy or radiation therapy, to both cure and cope with their cancer diagnosis.7,8 A recent systematic review 7 reported a combined prevalence of 40% for current complementary medicine (CM) use in 152 studies, from across 18 countries, which included more than 65 000 cancer patients. Horneber et al 7 also reported that CM use had increased over time from approximately 25% in the 1970s to more than 32% in the 1990s and to 49% post-2000. Cancer patients’ disclosure of their use of T&CM to health care providers is important to assess any potential treatment interactions.9-12
Indigenous people tend to view health from a holistic perspective that incorporates physical, cultural and spiritual wellbeing and this underpins their care-seeking behaviors.6,13 The use of traditional medicine (TM) (eg, singing/chanting, bush medicine, traditional healers, and external remedies) is part of Indigenous culture, continuing traditions and lore. 13 TM is often used to enhance overall well-being through reconnection to land, spiritual, and ancestral roots.6,13 Traditional healers provide spiritual and social support that is equally as important as the botanically based herbal remedies. 13 To date there has been no comprehensive review of T&CM among Indigenous cancer patients and this manuscript aims to address this gap.
Methods
Eligibility Criteria
TM and CM 14 include a broad range of practices, technologies, products, knowledge systems, and approaches to preventing and/or treating illness and/or promoting well-being, which are not historically associated with the conventional medical profession or medical curriculum. 15 While TM refers to health care indigenous to the local culture of users (including examples such as herbal medicines and practices provided by traditional healers who are usually unregulated and operate outside the publicly funded health care system), CM refers to health care, both self-administered or practitioner-led, which is often exotic to the culture of users (examples include massage, chiropractic, and Western herbal medicine). 14 As these definitions suggest there may well be temporal and geographical fluidity whereby the definition of a particular health care practice can be considered TM or CM depending on the context of use and users. 16 However, despite these possible variations of context both TM and CM in the vast majority of cases are largely defined by their continuing provision and use beyond the routine focus of conventional medical practice. 14
Indigenous populations eligible for inclusion in this review were from Australia (Aboriginal and Torres Strait Islander), Canada (Aboriginal, First Nations, Inuit, or Métis), New Zealand (Māori), or the United States (American Indian, Native American, Alaskan Native, American Samoan, Eskimo, and Native Hawaiian). These countries were included because of their shared history of colonization and disproportionally worse health in Indigenous populations.1,3 In this review, we respectfully refer to Indigenous people in these 4 countries as “Indigenous” while acknowledging that they comprise many diverse groups with distinct languages, beliefs, and cultural practices.
Search Strategy
The search originally aimed to identify peer reviewed literature reporting new empirical data from qualitative or quantitative studies examining T&CM use for 1 of 5 chronic diseases (cancer, cardiovascular disease, kidney disease, diabetes type 2, or respiratory disease) in adult (18 years and older) Indigenous populations from Australia, Canada, New Zealand, and the United States. As approximately half of all records were unique to cancer at the end of our search, this review focuses on cancer only; however, the flowchart (Figure 1) and search terms (Table 1) depict the screening of studies for all 5 diseases. We required full records of original research that were published in a peer-reviewed journal from 2000 onward, excluding (a) books or book chapters, commentaries, literature reviews, editorials, poster abstracts, and dissertations; (b) published languages other than English; and (c) efficacy studies (as we are interested in T&CM use).

Study selection and PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) flow diagram.
Free-Text Terms for All Databases and Controlled Vocabulary for CINAHL.

Abbreviations: CINAHL, Cumulative Index to Nursing and Allied Health Literature; CM, complementary medicine; TM, traditional medicine.
We searched AMED, AltHealthWatch, CINAHL, EMBASE, PsychINFO, and PubMed for records published between January 2000 and October 2017 (the year 2000 was chosen because of changes in complementary medicine and service systems that might limit the applicability of studies prior to this date). Keywords included using free-text terms representing (a) Indigenous populations from and residing in Australia, Canada, New Zealand, and the United States; (b) common chronic conditions among Indigenous populations (ie, cancer, diabetes, heart disease, kidney disease, respiratory disease); and (c) terms used previously for CM, 9 which included TM terms (Table 1). In addition, we searched the reference lists of articles that had previously conducted systematic literature reviews on similar topics to ours.
Review Process
The systematic review process was guided by the Cochrane Collaboration 17 and the Centre for Reviews and Dissemination 18 and the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines 19 as outlined in Figure 1.
After removing duplicates, AG and SL independently examined titles and abstracts using Covidence systematic review software. 20 Articles not meeting eligibility criteria were excluded. All retrieved full-text articles were independently assessed by AG and SL and the reasons for excluding articles were documented and discrepancies were resolved by consensus. Extraction of data in qualitative studies was conducted via the Joanna Briggs Institute’s method of qualitative research synthesis (meta-aggregation) as it avoids reinterpreting data and attempts to accurately and reliably present the findings of included studies consistent with the intent of the original authors. 21 AG and SL independently piloted this approach 21 to achieve consensus on interpretation and data extraction. AG and SL then proceeded with double independent extraction of findings, categories and synthesised findings from qualitative studies. Extraction discrepancies were documented and discrepancies were resolved by consensus.
Quality Appraisal of Studies
The methodological quality of each publication was assessed by AG and SL using separate tools for quantitative and qualitative studies. Quality assessment for the quantitative studies was conducted using the Newcastle-Ottawa Scale (NOS) modified for prevalence studies 22 and a 6-item critical appraisal tool was used for the qualitative studies developed by Kuper et al. 23
The NOS scale authors report that the scale has face/content validity and interrater reliability. 24 The modified NOS produce a rating out of 5. It assesses the representativeness of the sample, the sample size adequacy, nonresponse, measurement of variables and the quality of the descriptive statistics reporting. Consistent with Cochrane guidance, 17 we made minor adaptions to the NOS to fit the specifics of our review question. Specifically, we altered the first NOS item to score studies on variability in remoteness, socioeconomic status, gender, and age. In addition, we modified the fourth NOS item to represent our topic of interest, T&CM, by keeping the validated measurement tool and adding the need for a T&CM definition.
The Kuper et al 23 quality assessment tool for qualitative studies produces a rating out of 6. The 6 questions cover: sampling, data collection, data analysis, transferability, ethical issues, and reflexivity and the overall clarity of the study. AG and SL piloted the measures, introducing half marks for items that had 2-part questions and agreed upon a scoring system based on our research question. Furthermore, studies with no ethnic breakdown reported, received a reduced score, as we were unable to distinguish Indigenous from non-Indigenous participants.
Ethics
Ethical approval was not required for this systematic literature review.
Results
Of the 794 records retrieved, 195 duplicates were removed and 599 records were screened by title and abstract. An additional 9 records were identified through checking the reference lists. Of the 608 abstracts considered for inclusion, 96 full-text articles were assessed for eligibility, and 40 records were subsequently considered eligible for inclusion. Of these records, 21 were cancer-related, and as such other chronic conditions were excluded (see Figure 1).
Characteristics of the Included Articles
The 21 articles represented 18 individual studies: 3 were conducted in Australia,25-29 4 in Canada,30-33 3 in New Zealand,34-36 and 8 in the United States.37-45 Most were qualitative,26-33,35-42,44,45 (n = 15, 83%), including 2 case studies,32,38 and all 3 quantitative studies were cross-sectional.25,34,43 All quantitative studies assessed TM as a subset of CM, where the qualitative studies differed in their focus, with 10 (75%) exclusively examining TM and/or TM healers; 2 from Australia, 4 from the United States, 3 from Canada, and 1 from New Zealand.
Most studies included participants from urban/accessible areas (n = 6; 33%), or rural areas (n = 8; 44%) and were conducted in a range of clinical and community settings. Most studies contained solely Indigenous participants (n = 13; 72%) and females (83.9%). Sample sizes varied extensively, with single clinical case studies, 126 in the largest qualitative study and 248 in the largest quantitative study; with both samples 100% Indigenous. For those studies that reported cancer type (n = 15; 83%), most included participants with breast cancer (40.5%), followed by digestive organ cancers (14.2%) and lung cancer (12.7%).
Of the quantitative studies, only the Australian study exclusively sampled an Indigenous population (from Queensland, a state of Australia), whereas the others sampled small (n = 26) and moderately sized (n = 129) Indigenous subgroups. Seven of 15 qualitative studies investigated TM and/or CM use exclusively, with 2 of these 7 being case studies. Four qualitative articles intentionally reported on TM and/or CM as a subset of a broader focus, often indicated by mention of these practices only in the abstract. Seven qualitative studies referred to TM and/or CM in a section of the results not devoted to their use.
Using the modified Newcastle-Ottawa scoring guide, 24 the overall scores assigned to each quantitative study out of a possible score of 5 was 4.5, 3.5 and 0.5 (see Table 2). Using the quality assessment tool of Kuper et al 23 for qualitative studies, we assigned the 15 studies scores ranging from 1 to 5.5 (mean = 3.41) out of 6 possible points (see Table 3).
Characteristics of Included Quantitative Studies.

Abbreviations: NIB, no Indigenous breakdown; NR, not reported; HP, health professional(s); T&CM, traditional and complementary medicine.
Characteristics of Included Qualitative Studies.
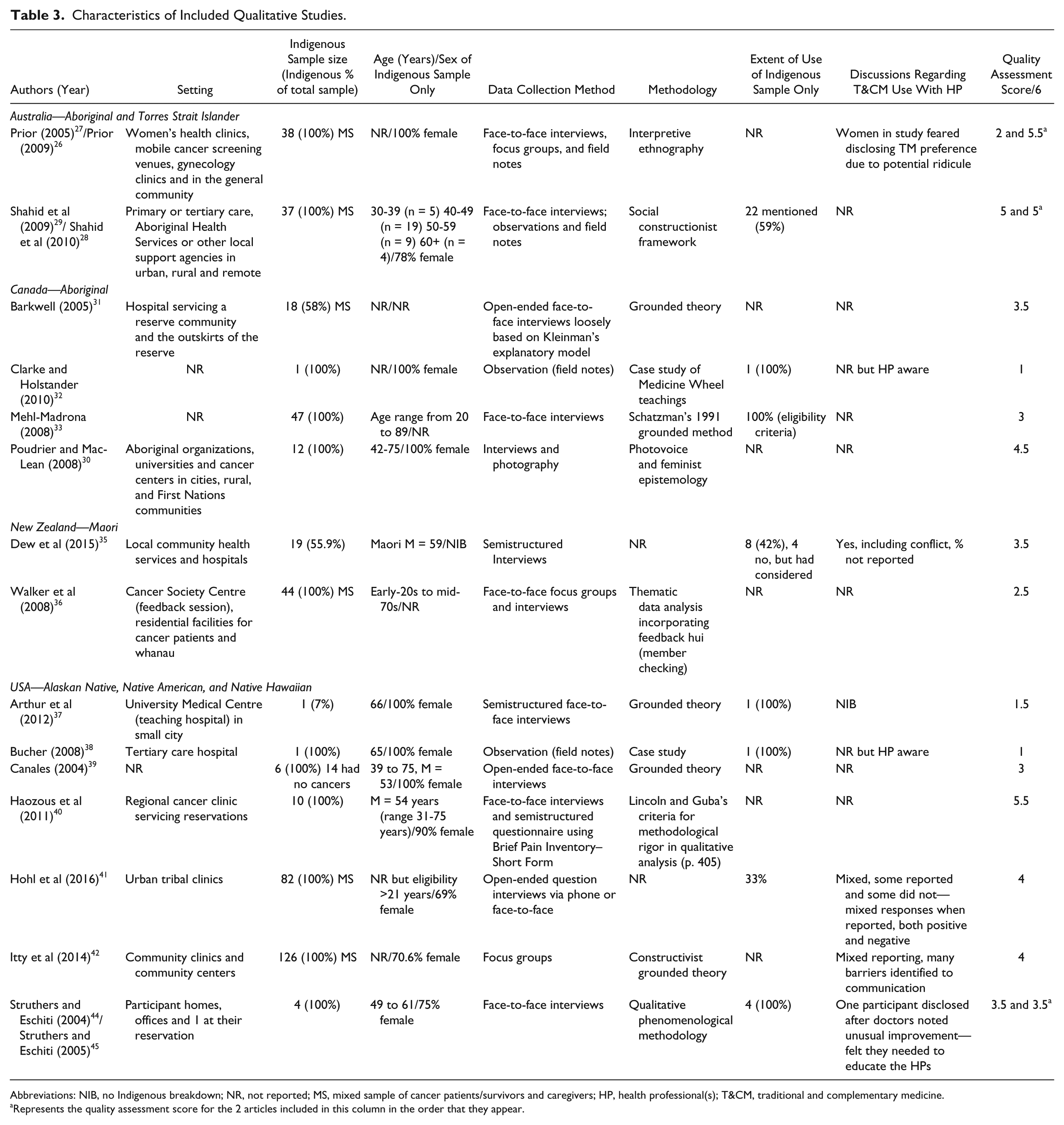
Abbreviations: NIB, no Indigenous breakdown; NR, not reported; MS, mixed sample of cancer patients/survivors and caregivers; HP, health professional(s); T&CM, traditional and complementary medicine.
Represents the quality assessment score for the 2 articles included in this column in the order that they appear.
Quantitative Study Findings
Three quantitative studies were conducted, one each in Australia, 25 New Zealand, 34 and the United States. 43 Two studies focused exclusively on T&CM,34,43 and one reported T&CM use within a broader study not focused on T&CM use. 25 One study included broad terms to assess T&CM use (eg, “traditional Indigenous practitioner,” “complementary medicine practitioner,” and “relaxation/meditation class”) 25 while the other 2 assessed specific therapies.34,43 Across the 3 studies, T&CM use ranged from 19% to 57.7%—with Maori reporting the highest use and Indigenous Australians the lowest (note: we are only reporting on the Indigenous populations reported in these studies). Two studies did not provide reasons for T&CM use by Indigenous status.34,43 However, Adams and colleagues 25 found all users employed T&CM for support with their cancer; however, the specific areas of support were not identified. This Australian study also identified those patients with an education level of high-school or above were more likely to consult a CM practitioner than those with education levels less than high school (P = .015). 25
Qualitative Study Findings
Fifteen qualitative studies were conducted: 2 Australian,26-29 4 Canadian,30-33 2 New Zealand,35,36 and 7 United States studies.37-42,44,45 Following meta-aggregation, thematic analysis revealed 4 broad themes: (a) perceived efficacy and benefits of T&CM, (b) integrating T&CM with conventional treatments, (c) T&CM use as connection to culture, and (d) impact of health professionals’ views of T&CM (Table 4).
Findings Summary of Main Themes Identified via Meta-Aggregation.

Abbreviation: T&CM, traditional and complementary medicine.
Perceived Efficacy and Benefits of T&CM
The terms used to describe efficacy and benefits of T&CM are often ambiguous, such as believing in it,
40
healing,30,33,40,45 and protection.
41
Three studies reported patients’ belief in T&CM as a cancer treatment,35,44,45 with 2 studies reporting patients’ belief that efficacy depends on the strength of their confidence in T&CM.28,29 The reported benefits of T&CM included: helping to cope; stress relief; cleansing and strengthening the body; increasing strength, energy, healing and recovery; and improving well-being.26-29,33,38,40,41,44,45 . . . it’s a bush or root that you boil it up, but there is something in it that is good for insides, just as a cleanser. Makes all your body organs healthy and strong, it gets rid of all your internal stress
28
The exclusive use of TM during palliation was associated with “reconnection to land, ancestral and spiritual roots that enhanced the person’s overall well-being”; TM was used to reduce side effects of chemotherapy, including weight and appetite loss. 38 For many patients, TM was described as a highly valued Indigenous way of healing that was attributed to health improvements.28,30,40,44 TM was said to work best when patients are diagnosed early, believe in the value of TM, and have a strong desire to fight cancer. 44 Some participants had safety concerns about TM—citing the paucity of evidence relating to efficacy, the lack of prescription information and previous experiences of allergic reactions or interactions with other medications.28,35
Integrating T&CM With Conventional Treatments
Most participants used T&CM alongside conventional cancer treatments,28,35-39,42,44 while a minority replaced conventional treatments with TM.
28
Some participants used TM for curing their cancer,28,30,44 some for healing and coping, and others to prevent recurrence,
39
while some used it only as a last resort.28,35 One participant speaks of fully integrating the 2: In between having my surgery, convalescing, and coming back home, they had done ceremonies to heal me.
44
One participant explains why some people rely solely on TM: I know a couple of people who chose the bush medicine once they read up about chemotherapy . . . they took their chances with the bush medicine, and they are still going. It’s either the quality of life or being sick from the chemo, that’s what they weighed up.
28
Integrating TM and conventional medicine was common for some participants and this flowed naturally into their cancer treatment.28,39,44 Some participants used T&CM on recommendation from community members or after seeing others benefit. 28 Some decided against using conventional treatments in order to stay with family and community or due to their care responsibilities. 28
T&CM Use as Connection to Culture
Evidence that Indigenous cancer patients employ alternative health paradigms when using TM is consistent with Indigenous holistic conceptions of health.28,36,37,39,42,44 TM was associated with spirituality in all Indigenous cultures and the practice of TM with holistic healing.28,36,37,39,42,44 Prior and colleagues argued that TM usage is an active choice that fits with Indigenous cultural values
26
and offers Indigenous patients a safe place for healing that is free of racism.
30
Some participants expressed distrust and opposition to conventional treatment: I said, “No, I’m not going that way. I’m going to stay with the rongoa”. The Māori herbal way.
35
The role of TM in maintaining family and community connections was an important coping mechanism for participants; particularly given the common shame and stigma associated with a cancer diagnosis.28,40,42 The communal nature of many TM therapies encourage connection between patients, family, and community.26,28,30,35,38,40,42,44 Many participants desired to use TM,28,35,42,44 however, reported barriers facing urban participants included distance from traditional healers who are predominantly in remote and rural areas,28,35,42,44 uncertainty about accessing TM,28,35 lack of connection to Indigenous culture, and a preference for conventional medicines.
Indigenous Australians spoke of cancer being caused by spiritual forces associated with “payback”
28
and TM was seen as essential in countering such forces.
28
For some, TM ensured a peaceful passage into the afterlife.32,38 Shahid and colleagues
28
stated that many Aboriginal Australians were brought up on missions with strong Christian beliefs that associated TM with paganism: We didn’t use traditional medicine or anything like that. Because we are not traditional Aboriginal, and our family was Christian based, and so . . . We put our trust on God.
28
Impact of Health Professionals’ Views of T&CM
When conventional healthcare providers respected and had knowledge of TM, Indigenous patients’ satisfaction reportedly increased,28,39,41 and they had confidence and trust in conventional medical services.28,39 Participants who used CM and/or TM were reportedly more actively engaged in their treatment plans.26,37
Most studies found that health professionals had little understanding of traditional beliefs and values of Indigenous cultures,26-30,36,39,41,44 which negatively affected communication and patients satisfaction.29,36 Some authors argue that culture and spirituality is central to healing and argue that TM could improve cancer outcomes.28,44 Health professionals need to counter “white man’s authority”
27
in health care and better “negotiate a balance between the different cultural paradigms.”
26
TM use had variable support from health professionals and there was a perceived lack of respect for TM, which arguably hinders patient-provider communication, reducing the likelihood of patients disclosing their T&CM use. Some participants felt belittled in their choice to use TM,35,39,41 as one participant describes: I tried to (discuss traditional medicine with providers). They didn’t take the things I said seriously.
41
While a minority of health professionals were openly accepting of TM, some participants reported some of their health care providers were personally interested in TM, but reluctant to openly discuss it, as it is generally disapproved of in conventional healthcare settings. 41
Discussion
This systematic review reports on the use of T&CM by Indigenous cancer patients in Australia, Canada, New Zealand, and the United States. We identified 21 journal articles25-45 from 18 studies that inform understandings of usage of T&CM across all 4 countries.
Most of the articles in this review were qualitative, with 7 investigating T&CM use exclusively.28,32,33,37,38,44,45 Two32,38 of these were case studies; 4 articles reported TM and/or CM use as a component of a broader study (eg, a study on quality of life)29,35,39,40; and the remainder made some reference to T&CM use within their results.26,27,30,31,36,41,42
The number of quantitative studies was small. All explicitly focused on TM and/or CM use, but only 1 Australian study exclusively sampled an Indigenous population (Queensland, a state of Australia), 25 whereas the others sampled34,43 Indigenous people as a subgroup. The estimated extent of T&CM use in the quantitative articles varied from 19% in Indigenous Australians, 25 58% in Maori in NZ 34 and 29.8% in Native Hawaiians. 43 The Australian study may have produced the lowest estimate because of the limitations of having only 5 options for reporting the type of T&CM used in a structured questionnaire, which would miss some types of T&CM. In contrast, the US study 43 and the NZ study 34 collected much more detailed T&CM information asking 21 and 19 questions, respectively. The estimate of T&CM in Native Hawaiians may be lower relative to the New Zealand study as the study collected data pre-2000, which yields lower estimates relative to studies conducted in the year 2000 or after. 7 It is known that restricting CM use to certain categories or treatments reduces estimates, 7 and makes comparisons difficult. Therefore, the use of consistent definitions and measurements are recommended using standardized and validated tools such as the International Complementary and Alternative Medicine Questionnaire (I-CAM-Q). 46 While standardization is critical improving overall understanding of the types and prevalence of T&CM use among Indigenous people, the validity of such tools to measure the diversity of TM is often questioned. 47 It has been previously reported that when evaluating CM use in ethnically diverse populations, ethnic-specific modalities should be recognized 7 ; this should also include TM.
High heterogeneity was observed in the quantitative studies, which is consistent with the 2012 systematic review and meta-analysis of CM use in non-Indigenous cancer patients that reported estimates ranging between nine and 88%. 7 These disparate estimates speak to the importance of consistency in survey methods. In light of this, we advocate following the recommendations of Horneber and colleagues’ review 7 to improve the relevance, reliability, validity, and reporting of future surveys assessing CM use in cancer patients. These recommendations relate to improvements in the conduct and reporting of future surveys of CM use in cancer patients, and specify 10 quality criteria, with recommendations on how these criteria should be fulfilled and reported.
It is evident from the current thematic analysis that Indigenous populations perceive T&CM as more than just a treatment for physical symptoms, and a cure for cancer. Indigenous people who use T&CM also do so as intrinsic to their wider belief system as a means of maintaining connections with family and community. 13 Similarly, Iwasaki et al 48 found that Indigenous people in Canada used T&CM as a means to impart spirituality, which they see as sacred and fundamental to their lives; in particular to their ability to cope and heal from their diabetes. 48 It is important that health professionals recognize this and be respectful when engaging in conversations about T&CM use. This also speaks to the importance of creating safe spaces in health services to make patients feel comfortable discussing T&CM and disclosing its use. The importance of open and effective patient-clinician communication is paramount to assessing the potential risks and benefits associated with the use of T&CM in the cancer setting.49,50 Indeed, effective, safe, and coordinated care for Indigenous cancer patients relies on shared open decision making and communication across patients, communities, and health care providers. Therefore, it is important for health professionals and policymakers to ensure that the care afforded to Indigenous cancer patients is culturally relevant, safe, effective, and optimal wherever and as much as possible.
Future research in this area would benefit from addressing some of the questions not addressed in the current review. In particular, studies looking at predictors of T&CM use in Indigenous populations. For instance, does the use of T&CM have an impact on the time taken to seek Western medical treatments for cancer? What are Indigenous people’s perceptions and beliefs regarding the ability for T&CM to prevent or cure cancer; does this impact or prompt T&CM use? Its questions like these that will help to form a clearer understanding about the potential motivations and predictors of T&CM use in Indigenous populations. Furthermore, there is a clear lack of research focused on determining the actual percentages of Indigenous people from Australia, Canada, New Zealand, and the United States that are using T&CM either alongside or instead of conventional cancer treatments. Without accurate quantitative data in this area, we are not able to show the significance of this phenomenon.
Conclusion
The current review identified wide variations in the estimates of T&CM use among Indigenous cancer patients, perhaps due to methodological variety across studies. This review highlights the importance of understanding the cultural beliefs of Indigenous people with cancer about the effectiveness and safety of T&CM, and in providing clinical information known about the T&CM treatments to enable Indigenous people to make informed choices. These findings are also a reminder of the importance of reflexivity when working with Indigenous populations, to recognise and set aside health professionals’ own backgrounds, positions, perspectives, paradigms, experiences, and biases, which have an impact on attitudes to T&CM use and patient-practitioner relations. The review results highlight a critical need for further research investigating T&CM use, decision-making and information seeking among Indigenous cancer patients, to help inform health practitioners and policy makers on how to create culturally relevant, safe, effective, and optimal care for Indigenous cancer patients wherever and as much as possible.
Footnotes
Acknowledgements
We would like to acknowledge the contributions of Abbey Diaz, Bronwyn Morris, Lisa Whop, and Suzanne Moore, who provided support and guidance throughout the research process to Alana Gall.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was undertaken under the auspices of the Centre of Research Excellence in Discovering Indigenous Strategies to improve Cancer Outcomes Via Engagement, Research Translation and Training (DISCOVER-TT CRE, funded by the National Health and Medical Research Council #1041111), and the Strategic Research Partnership to improve Cancer control for Indigenous Australians (STREP Ca-CIndA, funded through Cancer Council NSW (SRP 13-01) with supplementary funding from Cancer Council WA). We also acknowledge the ongoing support of the Lowitja Institute, Australia’s National Institute for Aboriginal and Torres Strait Islander Health Research. GG was supported by an NHMRC Early Career Fellowship (#1105399). JA was supported by an ARC Professorial Future Fellowship (#FT140100195). The views expressed in this publication are those of the authors and do not necessarily reflect the views of the funding agencies.
