Abstract
Introduction
Hematopoietic stem cell transplantation (HSCT) has become a well-established treatment for hematologic disorders. Since its introduction in 1957, HSCT techniques have improved, resulting in increased survival rates mainly due to a reduction in organ damage and decreases in infection and severe acute graft-versus-host disease (GVHD).1,2 In most high-risk acute leukemia patients, HSCT is the only treatment that offers the prospect of long-term survival. This prospect, however, is still dismal, and some studies suggest that 3-year overall survival in such patients is less than 20%. 3 Relapse is still the main cause of death, and together with infections and GVHD, it accounts for 65% to 70% of all posttransplantation mortality. 4
A number of avenues have been explored to address these causes of mortality. T-cell-depleted and CD34+-“enriched” grafts entail higher economic costs but are still commonly used.5,6 These options tend to increase rates of engraftment while decreasing the rate of GVHD, but they also result in prolonged immune reconstitution, putting patients at higher risk of infection and relapse. Recent research has shone a spotlight on natural killer (NK) cells and γδ T cells, which might be helpful in the fight against viral infections and may improve graft-versus-leukemia responses. 7 Along this same line of reasoning, recent graft manipulation approaches include the depletion of CD19+ and αβ T cells.8,9 These techniques emphasize the key role that immunoregulation likely plays in necessary improvements in post-HSCT mortality rates.
We wondered whether the immunoregulatory properties attributed to some Chinese herbal medicines (CHM) could curtail these mortality rates. Many cell line and animal model studies have demonstrated that some CHM exert favorable effects on the immune system. For instance, extracts of Angelica sinensis (dang gui) have been shown to induce the activation and proliferation of γδ T cells; 10 Astragalus membranaceus (huang qi) can both prompt the proliferation of and mitigate the effects of immunosuppressive agents on bone marrow CD34+ cells. 11 Epidemiological studies have shown that there are correlations between prolonged survival times and the use of CHM among leukemia patients.12-14 Although few such studies have been published in peer-reviewed journals, a handful of clinical studies have been conducted in China regarding the use of CHM in post-HSCT leukemia patients, and these have achieved positive results. 15
Due to the poor prognosis of high-risk leukemia HSCT patients and the seemingly positive potential of CHM, we employed a more rigorous clinical study to evaluate the efficacy of this treatment. We obtained blood samples from patients to measure the influence of CHM on immune reconstitution. Various methodological and logistical aspects of the trial posed new challenges to our group, and we were therefore motivated to perform a feasibility study.
Methods
Chinese Herbal Formulation
Following a review of existing studies and in combination with our own clinical knowledge, 15 we chose to use the CHM formulation Sheng-Yu-Tang (聖愈湯, SYT; Table 1), which was administered without a personalized diagnosis. This formula is fairly simple (6 ingredients) and is composed of herbs that have been extensively studied. Moreover, and as explained in our previous publication, this formula embodies the core treatment strategy that seems to be ideal in the vast majority of post-HSCT patients from a Chinese medicine perspective. 15
Constituents of the Sheng-Yu-Tang Formulation as Produced by Sun Ten Pharmaceutical a .

This product is registered with the Taiwanese Ministry of Health and Welfare under serial number 047770.
Inclusion and Exclusion Criteria
Patients should be (1) ≥20 years of age; (2) diagnosed with acute lymphocytic leukemia, acute myeloid leukemia, or myelodysplastic syndrome; and (3) eligible for allogeneic blood stem cell transplantation in accordance with the criteria of the local institution and the attending physician. Patients must also agree to comply with all study requirements. Patients should be excluded from the trial if they receive CHM from other sources.
Design
Patients were enrolled by signing a consent form prior to transplantation. Three months following transplantation, upon consent, patients were allocated to the SYT group. Patients who were not interested in taking SYT were allocated to the control group. Both groups continued to receive standard biomedical care from their oncologist. Patients allocated to the treatment group were to receive a batch of SYT once each month for a duration of 6 months. Peripheral blood samples were collected and analyzed on a monthly basis.
Sample Size and Statistical Analysis
Estimations of power size were performed using the “diggle.linear.power” of the “longpower” package of R Version 3.4.0 (R Core Team, 2015). A general estimation equation (GEE) model with a normal distribution, identity function, and unstructured working correlation matrix structure was used on selected outcomes of the patients followed in the study. We estimate that a minimum of 10 patients in each group would be required for achieving statistical significance. According to our preliminary results (described below), although none of the patients dropped out of the trial, the mortality rate was roughly 38%, and only 33% of patients who commenced herbal treatment persisted for >30 days. We therefore estimate that the recruitment of 50 patients in each group (n = 100) should be sufficient for a randomized controlled trial. The data from patients receiving SYT for 30 days or less who then cease its use for any reason should be excluded from analysis. Similarly, data of patients from the control group who expire prior to the 4 month posttransplantation time point should be excluded from analysis. The remaining data should be analyzed according to an intention-to-treat approach.
Outcome Measures
The main outcome measured in this study is the immune reconstitution rate of key cell populations, which is measured using flow cytometry with peripheral blood samples. If possible, records of minimal residual disease (MRD) from bone marrow aspirations and the occurrence rate of opportunistic infections, hospitalization frequency, and relapse rates should be obtained and considered secondary outcome measures. An additional secondary outcome measure is the EORTC QLQ-C30 questionnaire.
For immune reconstitution, other than CD4+ and CD8+ T cells, the following cell compartments are to be analyzed.
NK Cells
NK cells are among the first population of cells to recuperate following transplantation and play an important role as first-line response against viral infections. 16 First NK subset to recover express CD56brightCD16− and are derived from hematopoietic CD34+ cells, which give rise to CD56dimCD16+, which have cytotoxic capabilities. These are found mostly in peripheral blood. 17 Furthermore, NK cell transfusions following HSCT have been shown in some groups to reduce the relapse of acute myeloid leukemia, decrease GVHD, and improve engraftment and the overall survival. 18
T Regulatory Cells
The incidence of either MRD+ or relapse in patients with a high frequency of CD4+CD25−CD69+ T cells (>7%) has been reported to be significantly higher than that of patients with a low frequency of CD4+CD25−CD69+ T cells at +60 days, +90 days, and +270 days after transplant. 19 Also, in vitro and animal models have shown that the increase of donor CD4+CD25+ T regulatory cells can suppress the early expansion of alloreactive T cells—a hallmark of acute GVHD. 20 Clinical studies that have adopted this treatment principle have shown that infusion of donor T regulatory cells can prevent GVHD while favoring the reconstitution of regular T cells. 21
γδ T Cells
Gamma delta T cells have been described as a link between the adaptive and innate immune responses, because it has already been shown that γδ T cell reconstitution is associated with fewer infections and improved event-free survival after hematopoietic stem cell transplantation.22,23
B Cells
Naïve B cells are the first B cell subset to return to their normal values, approximately 6 months posttransplantation. The counts of memory B cells, however, might be low for up to 2 years post-HSCT. 24 Delayed B cell reconstitution has been associated with GVHD, and impaired immunoglobulin gene rearrangement render HSCT patients susceptible to various bacteria and viruses.25,26
Dendritic Cells
In peripheral blood stem cell transplantations, it has been shown that there is a relationship between a low dendritic cell count in the first 3 to 4 months following transplant, and disease relapse, acute GVHD, and death. 27
Flow Cytometry
Approximately 5 mL of peripheral blood should be collected in heparin tubes (BD Biosciences, San Jose, CA, USA) and placed on a rotary plate overnight at 10 rpm. Peripheral blood mononuclear cells (PBMC) can be isolated from whole blood using Ficoll-Paque PLUS (GE Healthcare Life Sciences, Uppsala, Sweden). To induce cytokine production, cells should be stimulated with paramethoxyamphetamine (50 ng/mL; Sigma-Aldrich, St Louis, MO, USA), ionomycin (500 ng/mL; Sigma-Aldrich, St Louis, MO, USA), and GolgiStop (1:1000; BD Biosciences, San Jose, CA, USA) for 5 hours. The following antibodies may be used: Foxp3, CD11c (BD Bioscience, Franklin Lakes, NJ, USA), IFN-γ, CD8 (Beckman Coulter, Mississauga, ON, Canada), CD3, CD4, CD45RA, CD62L, T cell receptor (TCR) γ/δ, CD56, CD16, CD19, CD27, IgD, CD14, CD25, and IL-17 (Biolegend, San Diego, CA, USA).
Enzyme-Linked Immunosorbent Assay
PBMC obtained from patients were seeded (2 × 106) in 96-well rounded-bottom plates using Iscove’s Modified Dulbecco’s Medium containing 5% fetal bovine serum (Gibco, MA, USA) at 37°C and 5% CO2. Cells were co-cultured for 24 and 48 hours with SYT (50, 100, and 200 µg/mL), paramethoxyamphetamine 50 ng/mL (Sigma-Aldrich), and ionomycin 500 ng/mL (Sigma-Aldrich). The concentrations of IL-2, TNF-α, and IFN-γ were measured using the appropriate ELISA (enzyme-linked immunosorbent assay) kits (BD Biosciences, San Jose, CA, USA) as per manufacturer’s instructions.
Safety
No adverse events related to SYT occurred in our pilot study. In a future protocol, all adverse events are to be recorded regardless of the possible association to herbal treatment. Herbal treatment is to be discontinued if either the attending oncologist or the trial investigator believes that the patient may be at risk of harm, including disability, hospitalization, or death.
Preliminary Results
Patients
Patients from the Division of Hematology and Oncology of the China Medical University Hospital were consecutively enrolled in the trial from September 1, 2015, onwards. The study protocol was approved by the Institutional Review Board of the China Medical University Hospital (DMR-105-005), and all participants provided informed consent. The trial protocol was made public on clincaltrials.gov (identifier NCT02580071).
Chinese Herbal Formulation
Granulated SYT was purchased from the Sun Ten Pharmaceutical Co, Ltd, Taiwan (product license #047770) and packaged as 90 portions per batch. Patients received 1 batch per month and were instructed to take 1 portion (4.2 g) 3 times a day. Before enrollment, patients were explained that they were expected to take SYT for 6 months.
Clinical Experiences
We recruited 18 patients in a nonrandomized consecutive manner since November 2015 until May 2017 (Table 2). Our goals have been to test the feasibility of the proposed protocol and to assess the compliance rate of patients and the adequacy of our inclusion and exclusion criteria, among other factors, with the intention of building on these insights to conduct a more comprehensive randomized trial. 28
Patient Characteristics.
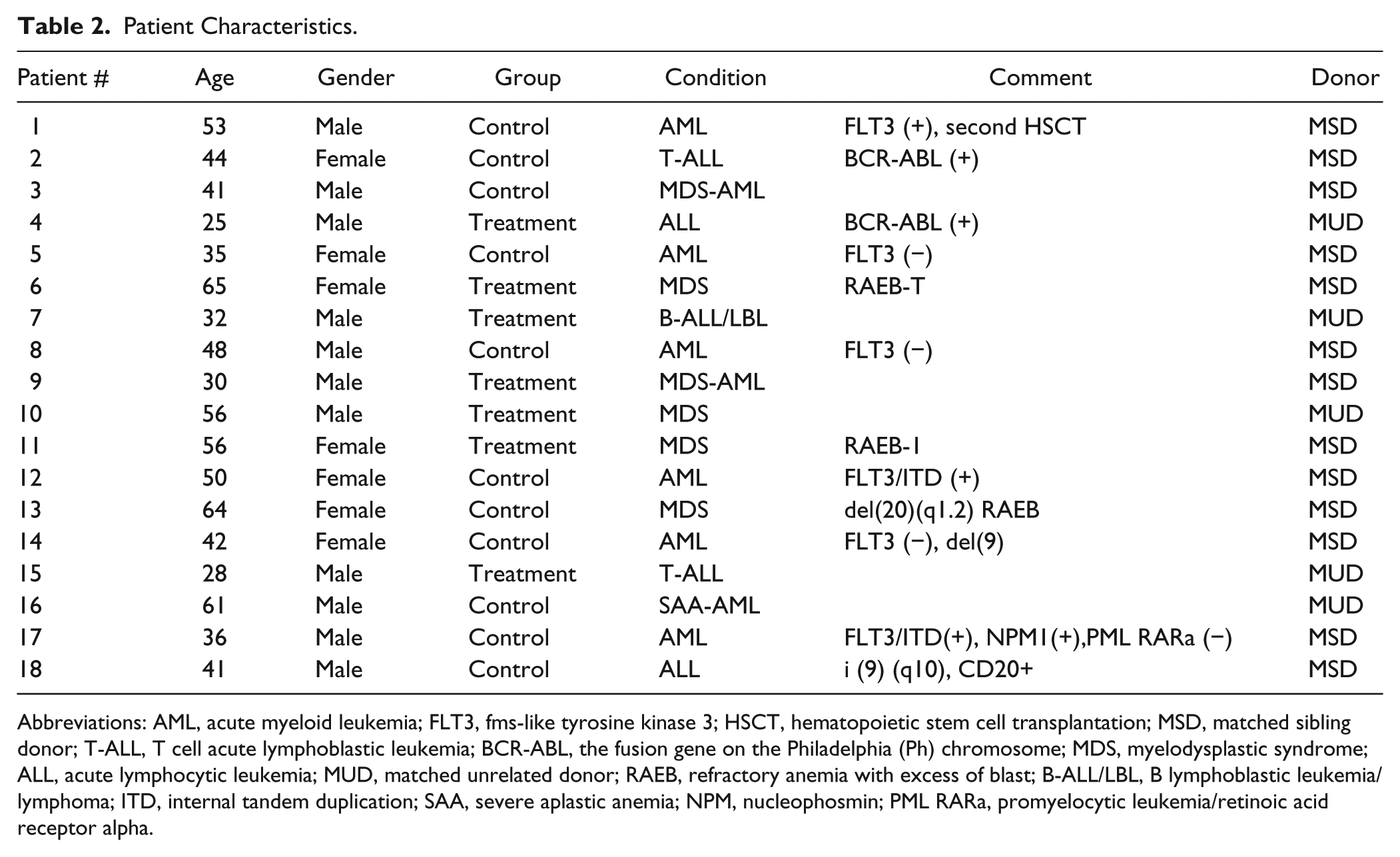
Abbreviations: AML, acute myeloid leukemia; FLT3, fms-like tyrosine kinase 3; HSCT, hematopoietic stem cell transplantation; MSD, matched sibling donor; T-ALL, T cell acute lymphoblastic leukemia; BCR-ABL, the fusion gene on the Philadelphia (Ph) chromosome; MDS, myelodysplastic syndrome; ALL, acute lymphocytic leukemia; MUD, matched unrelated donor; RAEB, refractory anemia with excess of blast; B-ALL/LBL, B lymphoblastic leukemia/lymphoma; ITD, internal tandem duplication; SAA, severe aplastic anemia; NPM, nucleophosmin; PML RARa, promyelocytic leukemia/retinoic acid receptor alpha.
Of the 7 patients who were assigned to receive SYT, only 2 continued for >30 days. Reasons for discontinuation included persistent leukopenia, herpes zoster, and relapse. We were aware of at least 2 other patients enrolled in the trial who did not receive SYT but sought CHM treatment elsewhere.
Despite the small sample size and the inability to demonstrate efficacy or effectiveness through statistical means, we analyzed our preliminary data. These data demonstrate the feasibility of the methods applied here to distinguish differences in the immune reconstitution of both trial groups (Figures 1 and 2).
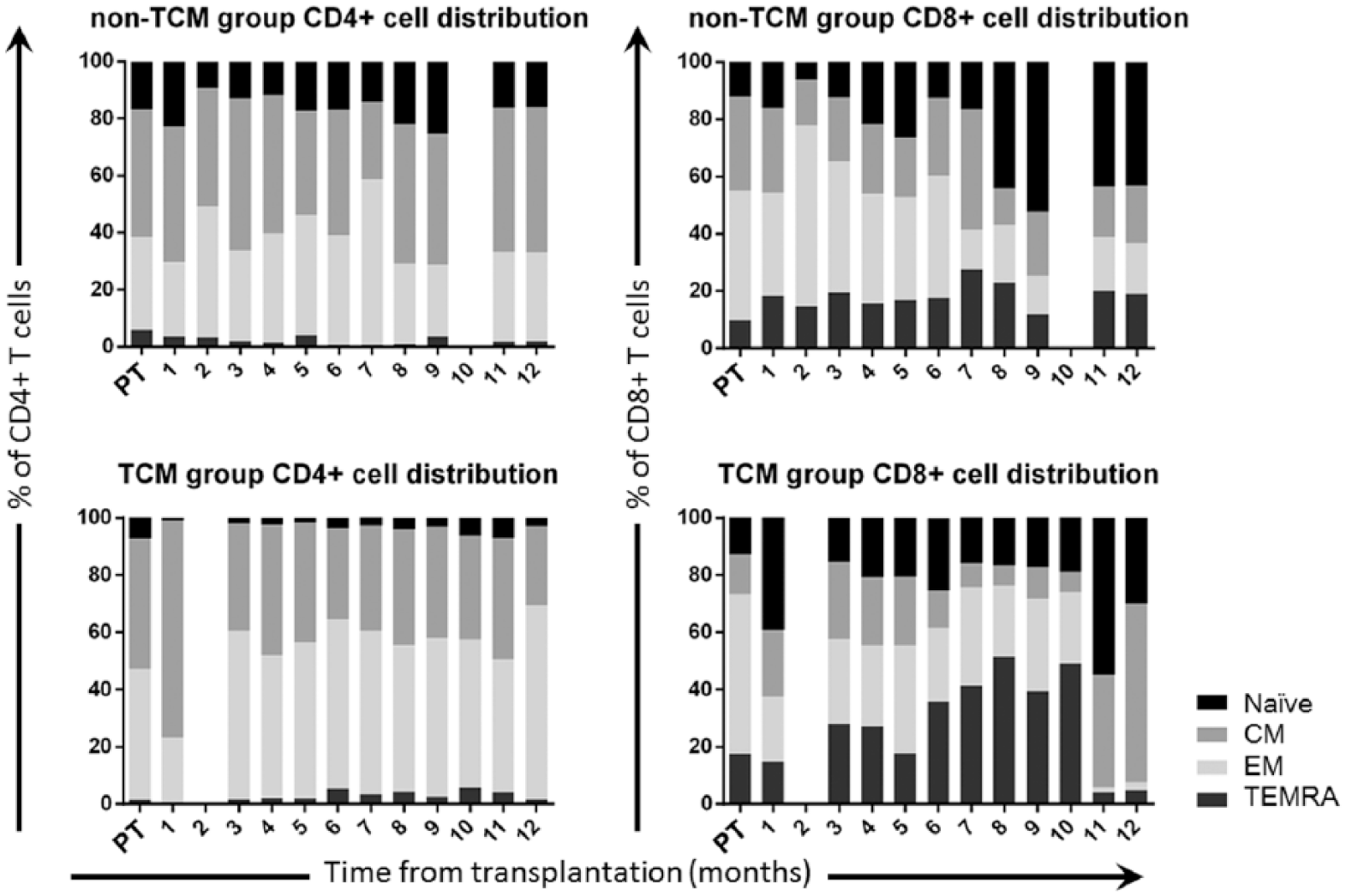
Average differences in immune reconstitution of CD4+ and CD8+ T cells. Patient sample size of current data is insufficient to draw conclusions; however, these data demonstrate the possible contribution of this type of analysis. There is, for example, a distinct difference in relative proportion of CD4+ naïve cells and CD8+ terminally differentiated cells, between the 2 groups. Missing columns represent time points at which no samples were collected from any patients.
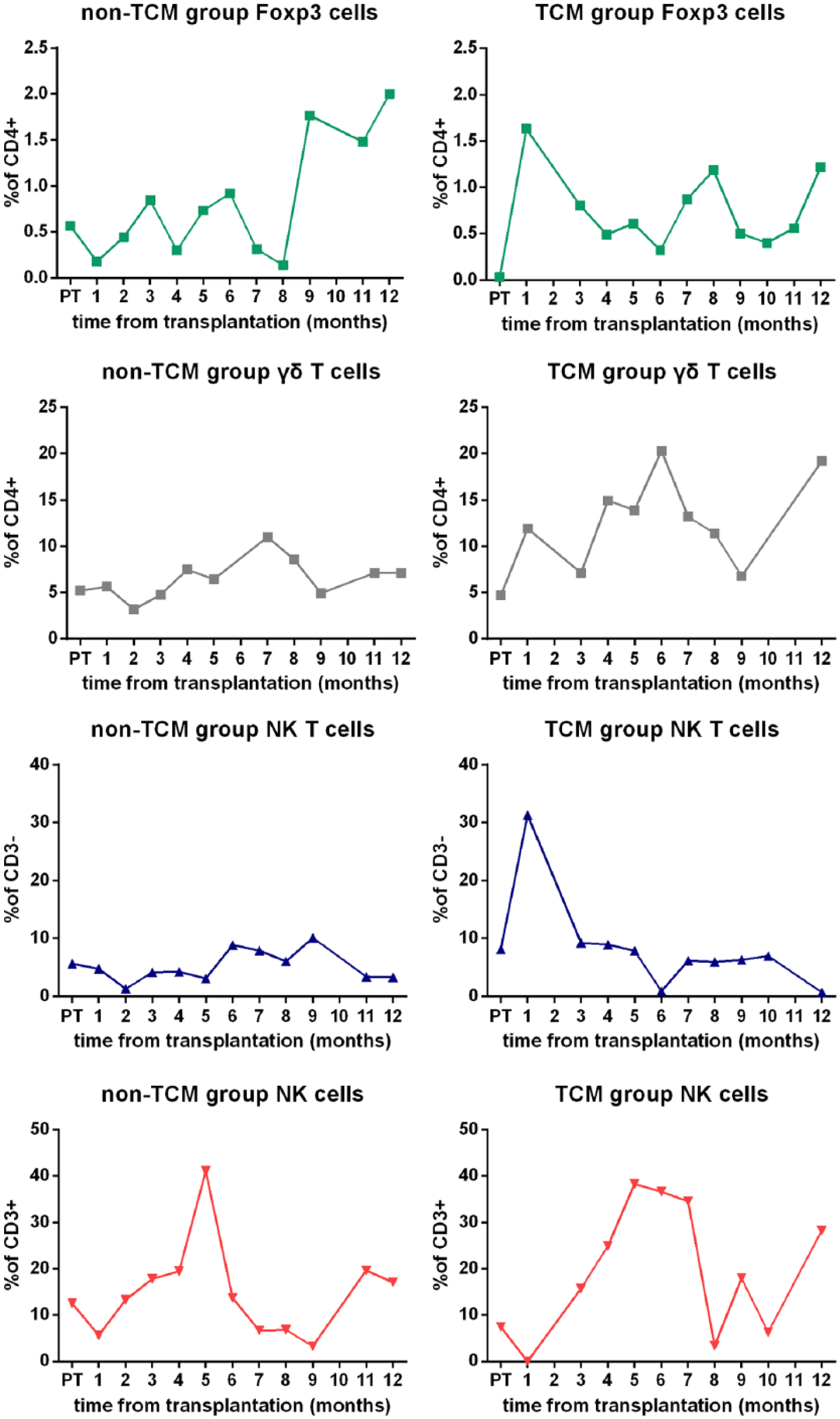
Immune reconstitution of various other cell compartments. Because there is no certain way to predict in advance which, if any, subset of cells will be affected by Sheng-Yu-Tang, it would be preferable to track the reconstitution of as many cell compartments as possible.
We also studied the in vitro effects of SYT on patient unsorted PBMC with regard to the secretion of IL-2, IFN-γ, and TNF-α, which are representative cytokines of the TH1 subset that are known to be directly related to graft-versus-leukemia and GVHD (Figure 3). 29 Due to the small sample size of measurements, we did not achieve statistical significance, and the only distinguishable trend was a decrease in TNF-α. GVHD is a result of the interplay between multiple types of cell components and cytokines, but TNF-α plays a central role, and its reduction is known to decrease the symptoms of GVHD.30,31 Whether this implies that SYT may mitigate GVHD requires further investigation. This type of in vitro examination should be considered exploratory as it is unlikely that a simple increase or decrease in a single signaling factor is predictive of the clinical outcome. IL-2, for example, may induce the proliferation of T cells, exacerbating post-HSCT on one hand and inducing immunosuppression via T regulatory cells on the other.32-34 This assay is thus not defined as an outcome measure, though it might provide complementary insight to other observations from the trial.

Secretion of IL-2, TNF-α, and IFN-γ by peripheral blood mononuclear cells obtained from 7 patients, following in vitro co-culture with Sheng-Yu-Tang. None of the differences between any 2 columns reached significance level; however, a possible trend may be observed in the concentration levels of TNF-α.
Discussion
Mortality was not chosen as a primary outcome measure for this study for a number of reasons. First, the prognoses of affected patients vary widely according to numerous factors, such as severity of disease, gender, genetic and molecular abnormalities, as well as donor type (ie, familial relationships and HLA-matching). 35 No data that we know of suggest different rates of immune reconstitution according to disease, and other recently published studies have excluded the consideration of these factors in their study design.36,37 Second, as most deaths occur within the first 2 years of HSCT, measuring mortality would require an additional year of follow-up. Measurement of immune reconstitution allows for the simultaneous assessment of multiple factors and offers insights concerning the possible mechanisms of action of the intervention.
No consensus exists regarding the ideal sampling rate for measurement of long-term immune reconstitution. In the protocol described above, we obtained peripheral blood samples from patients monthly, over the course of 1 year. Currently, we believe that 6 samples over the course of 1 year should be adequate, and other recently published studies have also followed this protocol (Figure 4). 36 With regard to the inclusion criteria, we originally intended this study to focus on patients with acute leukemia. However, since the total number of patients that undergo allo-HSCT is limited, we suggest a revision of this condition to open the trial to all patients undergoing allo-HSCT. As noted above, different disease diagnoses should have no effect on the rate of immune reconstitution.

Suggested design for future controlled trial. One-hundred patients are to be randomized to control or treatment group, 3 months following transplantation. Peripheral blood samples will be obtained at months 1, 2, 3, 6, 9, and 12 (noted in figure by the blood vial).
While designing this study, we were uncertain about the appropriate monetary incentive to use to motivate patients to enroll. We found that many patients were indifferent toward this incentive and that the backing of the respective attending oncologist was the most crucial factor for enrollment. This is understandable in light of the decisions and repercussions these patients face. The processing of blood samples together with the monetary incentive for patients per sample constituted a major portion of the resources required for this study, and their revision directly relates to the feasibility of a larger trial.
In its acute form, GVHD commonly presents within the first 100 days post-HSCT. In all trials we reviewed that were conducted in China, herbal treatment was administered during this period. To avoid unnecessary risk, the initiation of herbal treatment in this protocol was defined as 3 months following transplantation. Herbal treatment should be discontinued in the case of manifestation of moderate to severe chronic GVHD per the assessment of the attending oncologist. In our preliminary trial, patients were offered to continue receiving herbal medicine after the alleviation of GVHD if they were able to complete the treatment course prior to the 1-year posttransplantation time point. We believe future trial protocols should adopt this option.
Chronic kidney disease (CKD) should be acknowledged twice in the context of an allo-HSCT clinical study design. Decline in renal function is common among post-HSCT patients and may progress into CKD. Incidence rates of CKD among studies are highly variable, with values ranging from 13% to 66%.38,39 The main implication of post-HSCT renal damage is the due diligence that should be exercised when administering herbal medicine. Basic research demonstrates that Rehmannia glutinosa and the combination of Astragalus membranaceus and Angelica sinensis—constituents of SYT—may actually exert a renoprotective effect. However, until further evidence is collected, it is impossible to rule out potentially deleterious drug interactions.40,41 In our preliminary study, we determined that the administration of SYT to patients would be reassessed in cases where the glomerular filtration rate dropped below 50 mL/min/1.73 m2 or if serum creatinine levels rose to double that of baseline. Adequate consideration should also be given to patients with pretransplantation kidney disorders. Abnormal renal function is considered a major risk factor for HSCT. However, collective experience and practices among institutions may strongly vary.42,43 Although renal function does not appear in the above-mentioned inclusion/exclusion criteria, these should be explicitly defined in cooperation with the oncologists participating in the trial, in order to avoid the occurrence of selection bias and survivorship bias.
Conclusion
The results of this pilot study suggest that a larger and more rigorous trial is feasible. Revisions to the inclusion criteria, immune reconstitution sampling rate, and monetary incentive to patients should make for a more manageable protocol.
Footnotes
Authors’ Note
If any reader is interested in individual participant data that underlie the results reported in this article, the authors have no objection to share these, after de-identification, and requests will be considered on request.
Author Contributions
Drafting of manuscript: TF. Study design: TF, TTC, and HRY. Data collection and analysis: TF. Statistical analyses: JHC. Critical revision of the manuscript for intellectual content: TF, TTC, and HRY.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by China Medical University under the Aim for Top University Plan of the Ministry of Education, Taiwan. This study was also supported in part by China Medical University Hospital, Taiwan (DMR-105-005) and the Taiwan Ministry of Health and Welfare Clinical Trial and Research Center of Excellence (MOHW106-TDU-B-212-113004). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the article.
