Abstract
Hypothesis. Anthocyanins possess well-known biological effects and suppress DNA damage induced by therapeutic topoisomerase poisons. Our study focusses on the modulatory effects of anthocyanidins—malvidin (MAL) and pelargonidin (PEL)—on topoisomerase II poison mitoxantrone (MXT)-induced cytotoxicity and genotoxicity in in vitro and in vivo conditions. Study design. HepG2 cells were treated with MXT (1-10 µM), MAL (10-100 µM,) and PEL (5-640 µM) to determine cell viability. Further, experiments on cytotoxicity and apoptosis induction by single agents or combinations were performed. In vitro and in vivo antigenotoxic effect of MAL/PEL against MXT was evaluated in human lymphocytes and mouse bone marrow cells. Methods. Cytotoxicity of test agents and apoptosis induction in HepG2 cells was assessed by MTT assay, trypan blue dye exclusion assay and Hoechst 33258 staining. Antigenotoxic effects of MAL/PEL against MXT were assessed in co-treated human lymphocytes and bone marrow from mice that received MXT intraperitoneally 30 minutes post MAL/PEL oral administration Results. Dose-dependent cytotoxicity was observed with all 3 test agents in HepG2 cells. Highest test concentration of 100 µM MAL, 640 µM PEL, and 10 µM MXT decreased HepG2 cell viability by 80%, 30%, and 90%, respectively. The combination of 1 µM MXT + 80 µM MAL reduced cell viability better than single agents. MAL/PEL treatment significantly reduced MXT-induced genotoxicity in human lymphocytes and micronuclei formation in mice. Conclusion. Combination of MAL/PEL with lower doses of MXT, especially MAL+MXT increases the cytotoxicity in cancer cells. In addition, MXT treatment with MAL/PEL reduced MXT-induced genotoxicity and protected normal cells during chemotherapy.
Introduction
Cancer being the second main cause of deaths in the world, research over the past decade has been aiming to improve the current strategies of chemotherapy for better outcomes. 1 Consistent epidemiological studies have shown that consumption of bioactive compounds isolated from grains, fruits, and vegetables strongly reduced the incidence and risk of several chronic diseases, including cancer.2-4 Thus, owing to the enhanced health benefits of nutraceuticals (use of chemicals from food as medicine) several studies have been carried out for their effective application in chemoprevention.5,6 In addition, conventional chemotherapy induced drug resistance and disease relapse in several cases, including breast, lung, liver, colon and prostate cancers 7-9 With increasing evidences on the cytotoxic potential of plant-derived compounds and continuous efforts to improve patient survival, combination therapy is expected to provide effective inhibition of carcinogenesis, with limited side effects.10-12
Anthocyanins are one of several phytochemicals that are being extensively studied for beneficial effects during combination therapy.13-15 Anthocyanins are the most abundant flavonoid compounds that confer bright colors to fruits and vegetables and possess antioxidant and anti-inflammatory properties.16,17 Of the 6 common anthocyanidins found in higher plants, the present study focuses on the analysis of chemopreventive activity of malvidin (MAL) and pelargonidin (PEL) either alone or in combination with mitoxantrone (MXT) in cancer cells and their protective effect against MXT-induced genotoxicity in normal cells. MAL, abundantly present in berries and occurring attached to a sugar moiety, is responsible for the blue-red color and has been proved to have antioxidant, antidiabetic, and anti-inflammatory activities.18,19 PEL is the red color–producing anthocyanidin found in fruits especially pomegranate and is known to possess estrogenic activity. 20
Topoisomerase inhibitors form a major class of antineoplastic agents consistently used in the therapy regimens of various cancers. 21 MXT is a topoisomerase II–targeting anthracenedione that efficiently works against acute leukemia, non-Hodgkin’s lymphoma, breast, liver, lung, prostate, and bladder cancer. 22 Although MXT has been known to produce considerably fewer side effects, such as cardiotoxicity than doxorubicin, 23 drug resistance is a major drawback observed in treated cases. 24 In addition, the high-dose regimen induces genetic damage in cells, which might be a cause for secondary cancers. 25 Studies have also shown selective antiproliferative potential of anthocyanins against cancer cells compared to normal cells, where normal cells are minimally or completely unaffected.26,27 Thus, coadministration of anthocyanins, especially MAL or PEL with MXT, might be an effective strategy to reduce genotoxicity in normal cells and enhance antitumor efficacy as a combination therapy providing a low-dose, multitargeted approach with high antineoplastic efficacy, warranting better outcome with minimal side effects.28,29
The results of the present study showed that MAL with low doses of MXT, than PEL in combination or as single-agent treatment, efficiently killed hepatocellular carcinoma cells and also that MAL/PEL + low doses of MXT potentially reduced MXT-induced in vitro and in vivo genotoxicity.
Materials and Methods
Chemicals and Drugs
The phytochemicals malvidin chloride (CAS no. 643-84-5), pelargonidin chloride (CAS no. 134-04-3; purity ≥95%) and chemotherapeutic drug mitoxantrone dihydrochloride (CAS no. 90476-82-3; purity ≥97%) were obtained from Sigma-Aldrich, Germany. All other chemicals used in the study were of analytical grade.
Cell Line
Human hepatocellular carcinoma cell line, HepG2 was procured from National Centre for Cell Sciences, Pune, India and cultured in DMEM (Himedia, India) containing 10% heat-inactivated fetal bovine serum (Gibco, USA), 100 units/mL penicillin G, 100 mg/mL streptomycin (Himedia, India), 2 mM glutamine (Gibco, USA), 25 mM HEPES, and 2 mM sodium bicarbonate at a cell density of 1 to 3 × 106 cells/mL. Cells growing in the exponential phase were harvested at 80% to 90% confluency and subsequently used for experiments under standard conditions (37°C in 5% CO2 with 95% humidity) in an Eppendorf–New Brunswick Galaxy CO2 incubator. Cells were grown up to 3 passages before the treatments.
Animals
All the experiments were carried out with male Swiss albino mice, which were 12 to 14 weeks old, weighing 30 to 36 g. These animals were bred in the university animal house and maintained at 25°C ± 2°C on the standard mouse diet and water ad libitum in accordance with guidelines from Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA). Approval for this work was obtained from the university animal ethical committee (IAEC-JNU 5/2011).
Preliminary Analysis of in Vitro Cytotoxic Activity
The dose- and time-dependent cytotoxic activity of MAL, PEL, and MXT in experimental cells was measured using the MTT assay. Briefly, HepG2 cells were plated at a density of 1 × 104 cells/well on a 96-well plate with 100 µL medium/well. Following 24 hours of incubation and attachment, the cells were treated with MAL (10-100 µM), PEL (5-640 µM), and MXT (1-10 µM). After different treatment periods, cell viability was analyzed by MTT assay to compare the ability of metabolically active cells to reduce tetrazolium salt to colored formazan compounds. MTT (Sigma, MO) at a final concentration of 5 mg/mL was added to each well and incubated for 4 hours at 37°C in 5% CO2. After 4 hours, dimethyl sulfoxide (DMSO) was added to each well to solubilize formed formazan. Optical density was measured at 570 nm with 650 nm as reference filter using an iMark microtitre plate reader (BioRad, USA). All the experiments were performed in triplicate.
Cotreatment and Trypan Blue Dye Exclusion Assay
For evaluating the combinatorial effect of experimental compounds in inducing cytotoxicity, cancer cells were treated with anthocyanins and chemotherapeutic drug as single agents or in combinations of low and high concentrations for a period of 24 hours, and cell viability was assessed using trypan blue dye exclusion assay. 0.4% trypan blue was added to the treated cells. After 5 minutes, cells were loaded into a hematocytometer and counted based on dye uptake. Cells with damaged membrane appeared blue because of the accumulation of dye and were counted as dead. Live cells maintained cell membrane integrity and did not take up the dye. The number of viable cells was calculated as a percentage of the total cell population.
Morphological Assessment by Phase Contrast Microscopy
Exponentially growing cells were seeded on 24-well plates at a density of 5 × 104 cells/mL/well. After 24 hours, the cells were treated with specified concentrations of anthocyanins and chemotherapeutic drug as single agents and combinations. At the end of the experimental period, digital photographs were taken visualizing the treated cells under a phase contrast inverted microscope (TS100-F, Nikon, Japan) to assess their morphology.
Detection of Apoptosis by Hoechst 33258 Staining
The ability and extent of apoptosis induction by experimental compounds as single agents and combinations was assessed by staining cells with Hoechst 33258. Briefly, after the experimental period, cells were trypsinized and washed twice with PBS (phosphate-buffered saline, pH 7.4); 100 µL of cell suspension was stained with Hoechst 33258 (10 µg/mL) for 20 minutes, and the characteristic apoptotic morphological changes, chromatin condensation, and fragmentation were observed under a fluorescent microscope (Eclipse 80i, Nikon, Japan).
Human Peripheral Blood Lymphocyte Culture
To determine the protective effect of the anthocyanins against MXT-induced genomic instability in non-tumorigenic cells, human peripheral blood lymphocytes were cultured and treated with specific concentrations of experimental drugs as mentioned above. Briefly, blood samples were collected in heparin-coated tubes from healthy donors. Lymphocytes were isolated from the blood using Histopaque (Sigma) and were cultured in a humidified incubator (37°C, 5% CO2) in RPMI-1640 supplemented with 20% FBS, 200 mM
Mitotic Index (MI) and Chromosomal Aberration (CA) Assay
To determine the MI, after incubation for a specific period with experimental drugs, the cultured lymphocytes were centrifuged at 300g for 15 minutes, washed with ice cold PBS (pH 7.4), and resuspended in 6 mL of prewarmed hypotonic solution (0.075 M KCl) and kept at 37°C for 10 to 15 minutes. Cells were then centrifuged and fixed in Carnoy’s fixative (methanol:acetic acid, 3:1). The slides were prepared and stained with 4% Giemsa for 8 to 10 minutes. The frequency of mitotic cells per culture condition was determined by tallying the number of mitotic cells out of a population of 1000 consecutive cells, ignoring broken cells, clumped cells, and cellular debris. For the analysis of CA induced, the experimental cells were treated with colchicine and then harvested and fixed as mentioned above. Slides were prepared by dropping 3 to 5 drops of the fixed cell suspension on a clean slide and air dried. The slides were stained with Giemsa. For each treatment, 100 well-spread metaphases were analyzed to detect the presence of CAs.
Treatment of Mice With Anthocyanidins and MXT
MAL (1 or 2 mg/kg b.w.) and PEL (5 or 10 mg/kg b.w) were dissolved in double-distilled water and administered to mice by gavage (10 mL/kg b.w.). MXT (6 mg/kg b.w) was dissolved in distilled water and injected intraperitoneally (10 mL/kg b.w.), 30 minutes after the administration of MAL/PEL. The control animals received the same volume of distilled water. Depending on the body weight (b.w.) of the animals, volume administered varied, so as to match the doses. The doses of anthocyanins for in vivo studies were chosen as described previously. 31
Bone Marrow Micronucleus Test
After treatment with specific concentrations of MAL, PEL, and MXT, mice were sacrificed by cervical dislocation; bone marrow cells from the femur were collected in tubes containing FBS, and genotoxic effects were evaluated by the mouse bone marrow micronucleus test according to Schmid. 32 The dose for in vivo analysis was fixed based on the in vitro results and previous literature. Slides were prepared and stained with May-Grünwald and Giemsa stain. A total of 2000 polychromatic erythrocytes (PCEs) were scored per animal per slide to determine the frequency of micronucleated PCEs (MnPCEs).
Statistical Analysis
The results are presented as mean ± SD of replicate analyses of independent experiments. Statistical analyses were carried out using ANOVA by GraphPad Ver 5.03 statistical software and Microsoft Excel. Differences at P < .05 or less were considered statistically significant.
Results
Dose and Time Determination for Combination Treatment
The experimental cells were treated with different doses of MAL, PEL, and MXT to determine the ideal concentration that could produce cytotoxicity in HepG2 cells. Our results show that there was a prominent dose-dependent decrease in cell viability when treated with MAL for 24 hours. Figure 1A shows that approximately 60% and 80% cytotoxicity was induced at concentrations of 40 and 100 µM (highest dose used for the study) of MAL, respectively. PEL induced only 30% cytotoxicity even at the maximum concentration of 640 µM (Figure 1B) used in the study for all 3 time periods (24, 48, and 72 hours). The chemotherapeutic drug MXT produced a dose-dependent decrease in cell viability. Approximately, 50% cytotoxicity was induced at 2 µM, and almost 90% cell killing was observed at the highest dose of MXT used for the study (10 µM). There was no significant time-dependent difference in the cytotoxicity (Figure 1C). Based on our observation, the doses for further investigation into the combinatorial cytotoxic effect of MAL+MXT and PEL+MXT, and antigenotoxic effects of MAL and PEL against MXT-induced genotoxicity in experimental cells were chosen to be 40, 80, and 1 µM for MAL, PEL, and MXT respectively for a time period of 24 hours.

Dose- and time-dependent cytotoxic effects of (A) MAL (0-100 µM), (B) PEL (0-640 µM), and (C) MXT (0-10 µM) on HepG2 cells. Data expressed as mean ± SD of 3 independent experiments.
Combinatorial Effect of MAL, PEL, and MXT on HepG2 Cytotoxicity and Apoptosis Induction
After cotreatment with combinations of MAL, PEL, and MXT, the ratio of viable cells was analyzed. All treated cells had significant decrease in cell count when compared with untreated control cells. We observed that 1 µM MXT + 40 µM MAL and 1 µM MXT + 80 µM MAL reduced cell viability by 70% and 80%, respectively, whereas only 40% to 60% cell death was induced when they were used as single agents (Figure 2). The cotreatment of MXT+PEL did not produce significant cytotoxicity when compared with MXT alone or MXT+MAL (data not shown). Our results of cotreatment show that 1 µM MXT was sufficient enough to induce around 70% to 80% cytotoxicity when combined with MAL, whereas twice the concentration of MXT (2 µM) was able to induce only ~50% cell death when used alone. There was no statistically significant increase in cytotoxicity when the cotreatment groups were compared.
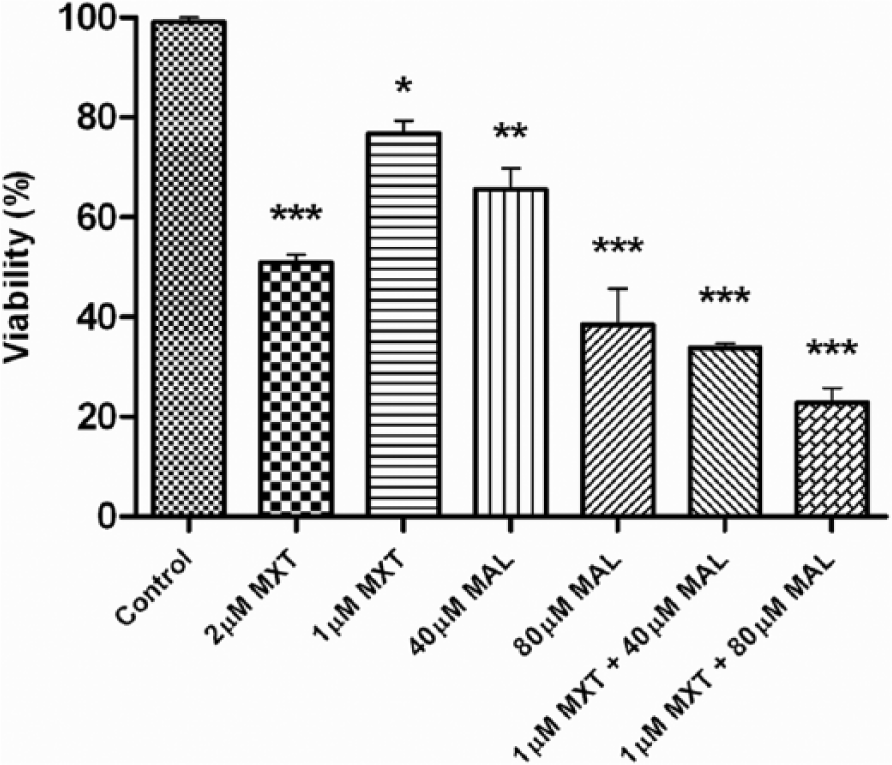
Effect of MAL and MXT on cell viability in combination treatment. Data expressed as mean ± SD of 3 independent experiments. *P < .05, **P < .01, ***P < .001 compared with control.
Morphological assessment of treated cells by phase contrast microscopy showed that control cells formed a complete monolayer with robust epithelial morphology (Figure 3A), whereas treated cells exhibited cell shrinkage and detachment of cells from the monolayer, indicating the occurrence of apoptosis (Figures 3B-3G).

Morphological assessment by phase contrast microscopy of HepG2 cells treated with (A) control, (B) 2 µM MXT, (C) 1 µM MXT, (D) 40 µM MAL, (E) 80 µM MAL, (F) 1 µM MXT+40 µM MAL, and (G) 1 µM MXT+80 µM MAL. Magnification: 100×.
The changes in the nuclear morphology to determine the extent of apoptosis induction in the experimental cells as evidenced by Hoechst 33258 staining showed that the control cells had intact nuclei (Figure 4A), whereas all the treated cells had nuclear changes with varying degrees of apoptotic features (Figures 4B-4G). Apoptosis induction is characterized by chromatin condensation, fragmentation of nuclear material, membrane blebbing, and formation of apoptotic bodies. We found that there was no significant difference in the number of apoptotic cells within the cotreated cells. However, cells treated with 1 µM MTX+40 µM MAL and 1 µM MTX+80 µM MAL had increased fluorescence (Figures 4F and 4G) when compared with cells treated with single agents, showing increased chromatin condensation marking severe apoptosis induction.

Hoechst 33258–stained HepG2 cells treated with (A) control, (B) 2 µM MXT, (C) 1 µM MXT, (D) 40 µM MAL, (E) 80 µM MAL, (F) 1 µM MXT+40 µM MAL, and (G) 1 µM MXT+80 µM MAL. Magnification: 100×. Yellow arrows indicate apoptotic features such as increased fluorescence, chromatin condensation and apoptotic bodies.
Effect of Cotreatment on Normal Cells
To analyze the genoprotective nature of MAL and PEL against MXT in normal cells, human peripheral blood lymphocytes were treated with the same doses and combinations of MAL, PEL, and MXT as HepG2 cells. Figures 5A and 6A show the MIs of treated lymphocytes. We observed that 2 µM MXT greatly reduced the doubling potential of cells when compared with untreated control cells, and cells treated with 1 µM MXT had ~25% to 30% MI. Cotreatment with MXT+MAL reduced the MI of cells similar to MXT alone, whereas it was comparatively higher in cells treated with MAL alone (Figure 5A). MXT+PEL treatment showed a higher MI than MXT treatment alone (Figure 6A). PEL treatment as a single agent did not show any change when compared with the control.

Mitotic index (A) and frequency of chromosomal aberrations (B) in human blood lymphocytes after treatment with MAL and MXT as single agents or in combination. Data expressed as mean ± SD of 3 independent experiments. **P < .01, ***P < .001 compared with control.

Mitotic index (A) and frequency of chromosomal aberrations (B) in human blood lymphocytes after treatment with PEL and MXT as single agents or in combination. Data expressed as mean ± SD of 3 independent experiments. *P < .05, **P < .01, ***P < .001 compared with control.
The protective effect of cotreatment at the chromosomal level was analyzed by calculating the number of abnormal metaphases and total number of CAs, such as breaks, gaps, and dicentrics. Analysis of single-agent treatment showed that 2 µM MXT and 1 µM MXT produced ~48% and 39% cells with CA, respectively, whereas the number of cells with CA after MAL or PEL treatment was not significant. Cotreatment of MXT with MAL/PEL greatly reduced the number of cells with CA to half the percentage when treated with MXT alone (Figures 5B and 6B). Also, 1 µM MXT+40 µM MAL, 1 µM MXT+80 µM MAL, 1 µM MXT+40 µM PEL, and 1 µM MXT+80 µM PEL reduced the incidence to 25%, 32%, 16%, and 20%, respectively.
In Vivo Genoprotective Activity
Analysis of the protective effect of MAL and PEL against MXT-induced genotoxicity was evaluated by micronuclei assay. It was observed that there was a significant dose-dependent increase in percentage of MnPCEs in all MXT-treated animals when compared with control (Figure 7). As concentrations of MXT (2-8 mg/kg b.w. ) used for the study had a significant impact on the genome integrity, 6 mg/kg b.w. was chosen for further analysis during combination studies. The frequency of MnPCEs was found to be maximum in MXT-alone treated animals, whereas there was a statistically insignificant incidence at the higher doses of MAL (2 mg/kg b.w.) and PEL (10 mg/kg b.w.) treatments used in the study when compared with the control. A dose-dependent reduction in the level of genotoxicity was observed in the combined treatment. MXT (6 mg/kg b.w.) with PEL (5 mg/kg b.w.), and PEL (10 mg/kg b.wt) treatment reduced the frequency of MnPCEs to ~40% and 45.5%, respectively, when compared with the control (Figure 8). There was no significant variation between the combined treatment animals. MXT+MAL (1 mg/kg b.w.) treatment reduced the MnPCE incidence to ~38% when compared with MXT-treated animals (Figure 9). Thus, our results show that minimal doses of MAL (1 and 2 mg/kg b.w.) greatly reduced drug-induced genotoxicity when compared with minimal dose of PEL (5 mg/kg b.w.).
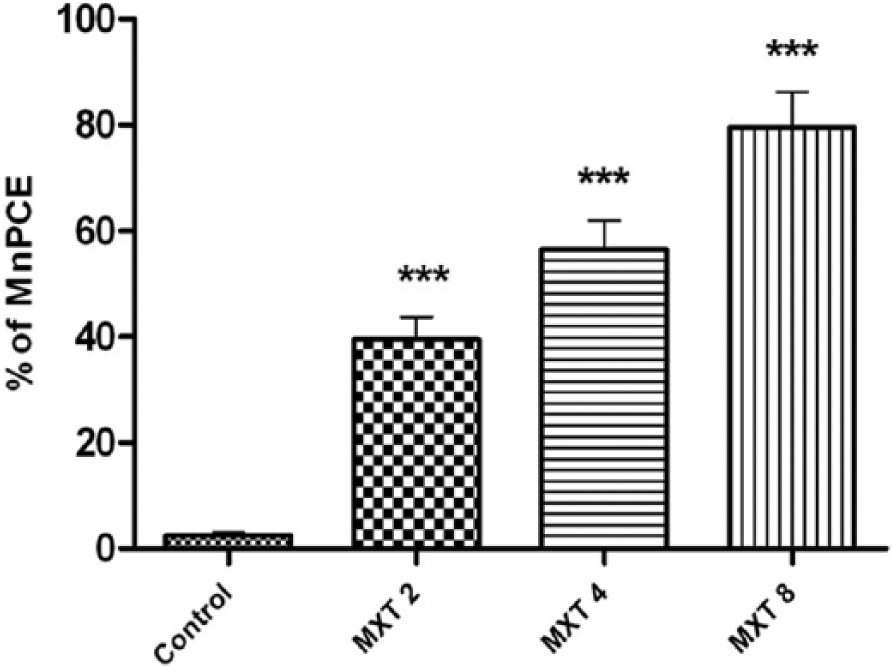
Frequency of MnPCEs/2000 PCEs from bone marrow of experimental animals treated with MXT at different doses. Data are expressed as mean ± SD of 3 independent experiments. ***P < .001 compared with control.

Frequency of MnPCEs/2000 PCEs from bone marrow of experimental animals treated with PEL and MXT as single agents or combination. Data are expressed as mean ± SD of 3 independent experiments. **P < .01, ***P < .001 compared with control.

Frequency of MnPCEs/2000 PCEs from bone marrow of experimental animals treated with MAL and MXT as single agents or combination. Data expressed as mean ± SD of 3 independent experiments. ***P < .001 compared with control.
Discussion
Anthocyanins have been widely studied in recent times because they are expected to be more than just plant colors because of their unravalled medicinal properties. Among the anthocyanins, MAL and PEL have been proved to possess chemopreventive potential in several reports. However, their potential cytotoxic and genoprotective activities when given in combination with standard drugs are yet to be elucidated. In the current study, MAL produced significant death of experimental cells, whereas PEL was not cytotoxic. Similar results have been obtained in our previous study involving HL-60 33 and several other studies on cell lines such as MCF-7, AGS, and HCT-116. 15 The variation in the cytotoxic effect might be attributed to the change in the functional groups, and the low sensitivity of HepG2 cells to PEL can also be a result of their selective responsiveness to the estrogenic activity of PEL. 34 MXT induced cell death at all 3 time points in the experimental cells at doses similar to that in previous reports.35,36 Identification and analysis of compounds that produce effective cell killing at minimal doses is essential to prevent the deleterious side effects. From the preliminary cytotoxicity assessment, the doses of anthocyanins to be used for further studies were chosen as 40 µM for MAL and 80 µM for PEL for combination treatment with MXT.
Combination therapy has been gaining more importance because of its benefits such as limited side effects, decreased chemoresistance, and improved toxicity to cancer cells; anthocyanins have also been shown to have anticancer activity as single agents, 37 targeting several mechanisms such as reactive oxygen species generation (ROS), activation of inflammatory mediators, induction of apoptotic proteins, and inhibition of matrix metalloproteases. However, this work serves as a pilot study for the use of MAL and PEL in combination with MXT to enhance the cytotoxicity in HepG2. The dose of MXT needed for effective killing of cancer cells in combination was reduced to 50% of the required concentration when administered as a single agent. This reduction in dose may be attributed to the synergistic or additive effect of MAL and PEL when coadministered with MXT. Similar synergistic activities have been observed in several other phytochemicals when given as combinations of epicatechin, tea polyphenols, curcumin, and other flavonoids.38,39 The reduction in the dose of MXT used might prevent acquired drug resistance induced during high-dose administration.40,41
The results of the study also show successful activation of apoptosis in the experimental cells subjected to combination treatment, as evidenced by Hoechst staining. Studies have shown that extracts rich in anthocyanins such as blueberry extract and red wine inhibited the growth of several cell lines by the activation of apoptosis, specifically modulating the expression levels of Bax/Bcl-2, caspases, ERK, mitochondrial membrane potential along with increased ROS generation.18,42-44 However, elucidation of the exact mechanism that is responsible for cancer cell toxicity during cotreatment of MAL or PEL with MXT is necessary to understand the alteration in the cellular physiology and assessment of any deleterious effects that might be produced.
The ROS thus, expected to be generated by combination treatment might interact with the macromolecules of surrounding normal cells and in turn induce genotoxicity with subsequent alterations in cell cycle and development of secondary cancers. Huber et al 45 have shown that DNA damage induced in the cells of the microenvironment in prostate cancer might lead to secondary cancers. In addition, MXT treatment led to the development of myelodysplastic syndrome characterized by deregulation of apoptosis, dysplastic features in hematopoietic precursors, and peripheral blood cytopenias that increased risk for transformation to acute leukemia. 46 Analysis of the effect of combination therapy on normal cells in in vitro conditions has shown that there is no significant increase in the MI of cells between MXT alone and in combination treatment with MAL, whereas there is a very distinct reduction in the incidence of CAs in MAL+MXT treatment. PEL+MXT treatment in cells showed a slight increase in the MI and lower genoprotective effect when compared with MAL+MXT, proving that MAL cotreatment with MXT gives an additive effect in inducing chemopreventive and genoprotective function relative to single agents. Circulating tumor cells generally exhibited a biologically aggressive cancer phenotype, accompanied by selective resistance to chemotherapy. 47 The introduction of combination therapy involving MXT + anthocyanidins can effectively reduce the aggressiveness of cancer and its progression.
The in vivo assessment of combination treatment of PEL/MAL with MXT also showed that the anthocyanidins under study greatly reduced the frequency of micronucleated cells, thereby reducing the chances of therapy-induced cancer development and drug resistance. The reduction in genotoxicity after MAL/PEL treatment was similar to that of the effect observed in our previous study on combinatorial treatments of anthocyanidins with cyclophosphamide. 31 This study thus confirms the genoprotective activity of specific anthocyanins MAL and PEL that could be effectively used to enhance the existing methods of chemotherapy, especially combination treatment with topoisomerase inhibitors for improved patient survival.
Conclusion
It is well known that anthocyanins have the potential to normalize several physiological activities in disease conditions. However, lack of knowledge on synergistic interactions, predictable combinations, and their clinical outcomes prevent the use of these plant-derived compounds in therapy regimens. The present study thus proposes the primary idea of utilizing a combination of anthocyanins and chemotherapeutic drugs, especially MAL/PEL+MXT, which ensures cancer cell killing along with the protection of genome integrity in normal cells. Our study has focused on the application of specific anthocyanins in combination with specific chemotherapeutic drugs. However, further analysis on the molecular mechanisms orchestrated during such combination treatments might help in the development and analysis of several other combinations of phytochemicals with conventional therapeutic agents and enhance current therapy strategies, minimizing or nullifying the side effects, if any.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr.KPK Thank the Department of Science and Technology (SERB), & University Grants Commission [UGC F. No. 37-109/2009 (SR)]. Dr.SKA thank Department of Science and Technology(PURSE). N.K. thank the University Grants commission for the Meritorious Research Fellowship. S.D. thank Lady Tata Memorial Trust for financial assistance.
