Abstract
Introduction. There is epidemiological evidence that Jia-Wei-Xiao-Yao-San (JWXYS) is the most common Chinese medicine decoction coprescribed with tamoxifen (Tam) when breast cancer is treated by hormonal therapy. However, whether there is interaction between JWXYS and Tam remains to be clarified. The aim of this study was to investigate the in vitro and in vivo effects of JWXYS on human breast cancer MCF-7 cells treated with Tam. Methods. In vitro cultured MCF-7 cells were cotreated with JWXYS and Tam. This was followed by MTT ([4,5-cimethylthiazol-2-yl]- 2,5-diphenyl tetrazolium bromide) assays and cell cycle analysis to assess cell proliferation; Western blot analysis was used to analyze the expression of various proteins involved in growth-related signal pathways. In addition, immunohistochemistry was used to detect autophagy among the cancer cells. In vivo analysis used female athymic nude mice implanted with MCF-7 cells; these mice were randomly assigned to 6 groups. All mice were killed humanely after 21 days of treatment; body weight, tumor volume, and tumor weight were then measured. Results. JWXYS was not cytotoxic to MCF-7 cells, based on the fact that there were no statistically significant changes between the JWXYS + Tam groups and the Tam-alone group in cell numbers, cell cycle progression, and cell proliferation signals, the latter including the expression levels of AKT, ERK, P38, p27(Kip1), and light chain (LC3)-I, II. Furthermore, using the MCF-7 xenograft mouse model, there were no significant changes between the JWXYS (1.3-3.9 gm/kg) + Tam groups and the Tam-alone group in terms of tumor weight and the protein expression levels of AKT, ERK, P38, and p27 (Kip1). However, there was a significant decrease in LC3-II protein expression with the low-dose JWXYS + Tam group but not with the middle- or high-dose JWXYS + Tam groups compared with the Tam-alone group. Conclusion. Based on in vitro studies and in vivo functional studies, there is no obvious interaction between JWXYS and Tam. However, the presence of interference at the molecular level in relation to LC3-II expression provides important information and may affect treatment strategies when physicians have patients with estrogen receptor-α(+) or progesterone receptor(+) breast cancers.
Introduction
Breast cancer is the most common cause of cancer-related mortality among women worldwide, 1 and the incidence has been increasing in Asia.2,3 It ranks as having the highest incidence and the fourth highest mortality rate among female cancers in Taiwan.4,5 Although many therapeutic advances have been developed for breast cancer, endocrine therapies that target estrogen receptor-α (ER) activity (tamoxifen [Tam])6-8 remain important adjuvant treatments after surgery for breast cancer. Hormonal therapy with Tam for 5 years has resulted in a significant reduction of 34% in the annual breast cancer death rate, with an absolute reduction in mortality at 15 years of 9.2%. 9
There is consensus that hormone therapies may cause certain adverse effects, such as hot flushes, cancer-related fatigue, joint pain, and insomnia, among breast cancer patients. Hot flushes occur in up to 80% of women who receive Tam treatment, and up to 45% of them grade this symptom as severe; this reduces their quality of life and affects patient compliance during hormonal therapy. In addition, hot flushes have become a common reason for coadministration of Tam and other drugs.6,10 Despite the fact that there are standard guidelines for cancer treatments in modern medicine, the use of complementary and alternative medicine (CAM) has become popular among oncology patients over recent decades.11,12 Breast cancer patients tend to use CAM therapies more frequently than those with other types of cancer, and the prevalence rate ranges from 28% to 97%.13,14 Recent studies have demonstrated that CAM, when used as a complementary therapy, has fewer side effects when relieving symptoms and improving quality of life.5,15 In Taiwan, more than one-third of breast cancer patients have used traditional Chinese medicine (TCM) at least once, and more than 80% of TCM users chose to use a Chinese herbal product (CHP) for the adjuvant management of their breast cancer.16,17 Unfortunately, many of the individuals who use such herbal remedies to alleviate their discomfort, including patients in Taiwan, are not aware of the potential adverse effects of such combinations—namely, herb-drug interactions, which might counteract the effects of hormonal therapy. 18
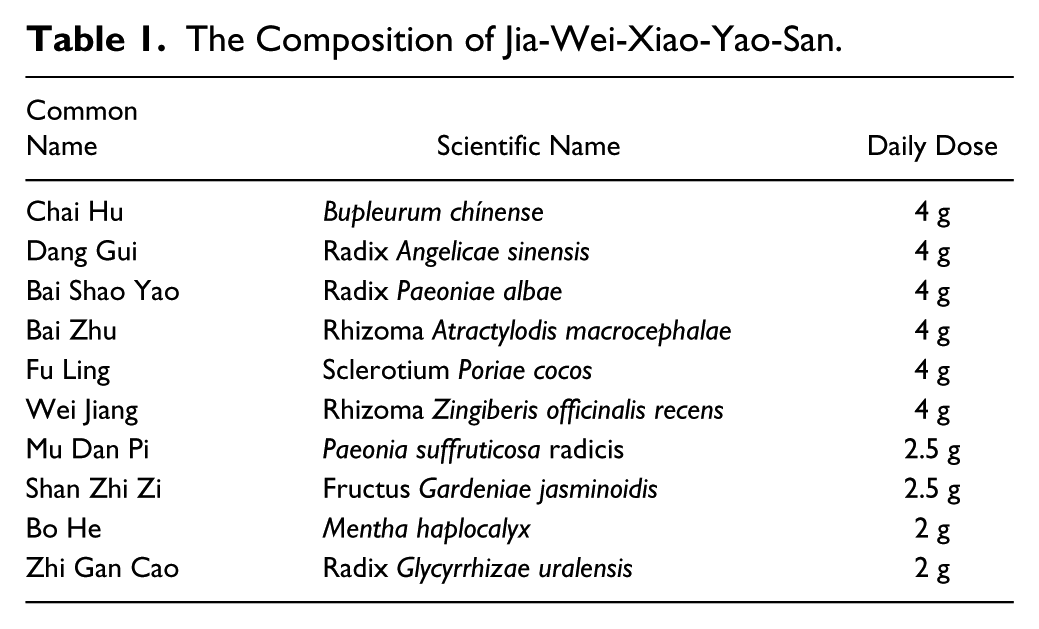
Jia-Wei-Xiao-Yao-San (JWXYS) is a very common Chinese herbal formula that has been used by Chinese for thousands of years. JWXYS consists of Radix Bupleuri, Radix Angelicae sinensis, Radix Paeoniae alba, Rhizoma Atractylodis macrocephalae, Poria, Rhizoma Zingiberis preparata, Cortex Moutan, Fructus Gardeniae, Herba Menthae, and Radix Glycyrrhizae preaparata (Table 1). The indication for JWXYS use is stagnation of the “Liver qi with blood deficiency,” and it is mostly used to treat symptoms such as anxiety, anorexia, night sweating, headache, dry eyes, hot flushes, palpitations, and irregular menstruation.19-23
The Composition of Jia-Wei-Xiao-Yao-San.
Based on data obtained from the National Health Insurance database (NHIRD) in Taiwan, JWXYS is the most commonly prescribed formula by TCM doctors when treating breast cancer patients (Table 2). In addition, JWXYS is also the leading formula coprescribed with Tam when breast cancer is treated using hormonal therapy (Table 2). However, whether there is herb-drug interaction between JWXYS and Tam remains to be clarified.
The Top 10 Most Used Herbal Formulas (HFs) for Breast Cancer in Taiwan. a

Chinese herbal medications and frequency of prescriptions in 2009.
Our previous in vitro and in vivo studies have demonstrated that Si-Wu-Tang (SWT) and its active constituents are able to stimulate mammary duct cell proliferation by modulating human epidermal growth factor receptor 2 (HER-2), PI3K/AKT, and MAPK signaling and that there is a positive feedback on HER-2 gene expression. 24 In addition, ferulic acid, an active compound in SWT, stimulates cell proliferation by MCF-7 cells in an ER-dependent manner in vitro. 25 Furthermore, SWT was found to be able to reverse in vivo various Tam-induced antiproliferative effects among the Tam + SWT–treated group compared with the Tam-only treated group, such as tumor weight and tumor volume, as well as increasing ER-α and N-cadherin expression. Because there has been no report showing the possible herb-drug interaction between JWXYS and Tam up to now, the aim of the present study was to investigate the effects of JWXYS, both in vitro and in vivo, on human breast cancer MCF-7 cells that were treated with Tam.
Methods
Ethics Statement
We obtained ethical approval for this study from the institutional review board (IRB) of the Chang Gung Memorial Foundation (CGMF) as a pure observational cross-sectional study (IRB No. 99-3502B). All information used in this study was acquired from the database of the NHIRD, which comprised medical records of the whole of daily clinical practice. Because we retrieved the data anonymously for analysis, it was found that informed consent was not needed under the approval of the IRB of the CGMF.
This animal study was carried out in strict accordance with the recommendations in the Guide for the Care and Use of Laboratory Animals of the National Institutes of Health. The protocol was approved by the Institutional Animal Care and Use Committee of National Yang-Ming University (Permit Number: 1011209). All surgery was performed under sodium pentobarbital anesthesia, and all efforts were made to minimize suffering. 26
The CHP Prescription Database
TCM treatments in Taiwan are reimbursed by the National Health Insurance. All claimed outpatient data sets were obtained from NHIRD for the year 2009 (January 2009 to December 2009); they contain visit date, medical service facility, specialty, patient gender, date of birth, and 3 major diagnoses based on the International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM). 27 The coverage of the National Health Insurance is very high, and therefore, performing a nationwide prescription analysis is feasible when this highly digitized database is used.
Participant Selection
To identify breast cancer patients, TCM visits with at least 1 diagnosis of breast cancer (ICD-9 codes: 174.0-174.9) were extracted from the NHIRD. The CHP prescriptions for each visit were then also extracted to create a prescription database. The whole process of this study was monitored by the IRB of the CGMF (No. 99-3502B). Visits involving acupuncture, massage, or traumatology were excluded for reasons of possible confounding effects on the CHP data set.28,29
Cell Line and Reagents
The human breast cancer cell line MCF-7 (ER+, HER2-low) was obtained from the Food Industry Research and Development Institute (Taiwan, ROC). The cell line is routinely screened for the absence of mycoplasma contamination. It was maintained on Dulbecco’s Modified Eagle’s Medium supplemented with 10% fetal bovine serum, 2 mM
Preparation of JWXYS Extract
JWXYS is composed of Radix Bupleuri, Radix Angelicae sinensis, Radix Paeoniae alba, Rhizoma Atractylodis macrocephalae, Poria, Rhizoma Zingiberis preparata, Cortex Moutan, Fructus Gardeniae, Herba Menthae, and Radix Glycyrrhizae preaparata. The preparation of the JWXYS extract (denoted as JWXYS here) followed the standard procedures used when making a composition for patients. The herbeous material was extracted by a Good Manufacturing Practice company (Sun Ten Pharmaceutical Co, Ltd). The final preparation was stored at −20°C until use. The quality control of the herbs was monitored by high-performance liquid chromatography (Figure 1). 30

High-performance liquid chromatography for Jia-Wei-Xiao-Yao-San. The peak flow showed the index components, including albiflorin, paeonol, glycyrrhizin, cinnamic acid, geniposide, and paeoniflorin.
Cell Viability Assay by (4,5-Cimethylthiazol-2-yl)-2,5-Diphenyl Tetrazolium Bromide (MTT)
After MCF-7 cells had been seeded overnight, they were pretreated with Tam and/or different doses (0, 0.1, 0.3, 1, 3, and 10 µg/mL) of JWXYS for 48 and 72 hours. This was followed by counting of cell numbers using the MTT method, and the results were double-checked using the trypan blue exclusion assay.
Luciferase Reporter Assay for ERBB2 and ESR1 Gene Expressions
To investigate the effects of JWXYS on ERBB2 and ESR1 gene expressions, a pGL2 luciferase reporter vector containing the human HER2 (ERBB2 luciferase: RDB no. 2839, RIKEN BioResource Center, Ibaraki, Japan) promoter and a pGL4 luciferase reporter vector containing the human ERα (ESR1 luciferase: RDB no. 7528) promoter were constructed and individually transfected into MCF-7 cells. The transfection procedure was performed using the manufacturer’s recommended protocol as described in the “T-Pro non-liposome transfection reagent II (T-Pro NTRII)” transfection kit (T-Pro Biotechnology, JT97-N002). In brief, 2 µg plasmid DNA and 6 µL reagent II were mixed with Opti-MEM individually at room temperature (RT) for 20 minutes. Each mixture was added to individual plates of cells for 24 hours. The transfection efficiency was about 90%. In addition, Promega’s Renilla Luciferase Assay System (Promega Corp, WI) was used for reporter quantification in the mammalian cells. The data are presented as a relative optical density ratio—namely, specific luciferase/Renilla luciferase ratio.
Cell Cycle Analysis
After MCF-7 cells were seeded for 24 hours, they were treated with 0.1% fetal bovine serum overnight, which was followed by pretreatment with different doses (0, 1, and 3 µg/mL) of JWXYS for 30 minutes. The cells were then treated with Tam (0, 2.5, 5 µg/mL) for another 24 hours, and their cell cycle profile was analyzed by DNA flow cytometry. The DNA contents of the cells were used to classify the cells into presynthetic growth phase (G0/G1), S-phase, and postsynthetic/mitotic growth phase (G2+M). The proliferative capacity of the cells was defined as the S+G2/M phase fraction.
Western Blot Analysis
Before Western blot analysis of tumor tissue, samples were obtained from MCF-7–implanted nude mice; this tumor tissue was homogenized using lysis buffer (400 µL), and then, the tissue homogenate was washed twice with cold phosphate-buffered saline (PBS) containing 1 mmol/L Na3VO4, pH 7.4. To carry out the Western blot analysis of either cultured MCF-7 cells or tissue homogenate, samples were lysed in a buffer containing 150 mmol/L KCl, 10 mM Tris, pH 7.4, 1% Triton X-100, and protease inhibitor cocktail (CompleteMini, Roche, Mannheim, Germany). The protein concentrations in the cell homogenates were measured as described previously. 31 Samples consisting of 30 to 50 µg of protein were then separated on 10% sodium dodecyl sulfate polyacrylamide gels by electrophoresis and then transferred to a polyvinylidene difluoride membrane (Millipore, Bedford, MA). The membrane was blocked with 5% bovine serum albumin and probed with specific primary antibodies—namely, anti-phospho-p27 (Kip1; pThr187, LifeSpan BioSciences Inc, Seattle, WA), anti-ERα (Stressgen Biotechnologies Inc, Victoria, BC, Canada), anti-phospho-AKT 1/2/3 (Ser473, Cell Signaling Technology, Beverly, MA), anti-AKT (Cell Signaling Technology), anti-phospho-ERK1/2 (Thr202/ Tyr204, Cell Signaling Technology), anti-ERK1/2 (Cell Signaling Technology), anti-phospho-p38 (Thr180/Tyr182, Cell Signaling Technology, Inc, Danvers, MA), anti-p38 (Cell Signaling Technology), anti–light chain (LC)3 (Cell Signaling Technology), anti-α-tubulin (AbFrontier, Seoul, Korea), and anti-β-actin (AbFrontier, Seoul, Korea). The immunoreactive bands were visualized using enhanced chemiluminescence detection reagents (Thermo Scientific, Bremen, Germany) and quantified by multigauge software analysis (Fuji Photo Film Co, Ltd, Tokyo, Japan).
Immunohistochemistry Staining for Autophagy
MCF-7 cells were cultured overnight, which was followed by treatment with different doses (0, 1, and 3 µg/mL) of JWXYS for 30 minutes and then Tam (0, 2.5, and 5 µg/mL) for another 24 hours. After these treatments, the cultured cells were fixed in 4% paraformaldehyde for 5 minutes. The cultured slides were treated with 0.4% Triton X 100 for 5 minutes, blocked in 2% bovine serum albumin for 1 hour, washed with PBS, and then treated with anti-LC3-I, II antibody (rabbit anti-LC3-I, II IgG, 1:400; Sigma-Aldrich) for 1.5 hours at RT, which was followed by goat anti-rabbit IgG conjugated with FITC (1:40; Sigma-Aldrich) at RT for 1 hr. After rinsing with PBS, the cultured cells were mounted and examined using fluorescence microscopy.
Assessment of In Vivo Growth Interaction Between JWXYS and Tam
A group of 6-week-old female homozygous inbred BALB/c-nu+/nu+ athymic mice were purchased from the National Laboratory Animal Center (Taipei, Taiwan, ROC). The animals were given ad libitum access to food and water under the regulations of the animal care committee of National Yang-Ming University. They were maintained in a specific pathogen-free environment with a 12-hour light-dark cycle at 22°C to 24°C and 50% humidity. MCF-7–implanted nude mice were obtained by the subcutaneous injection of MCF-7 cells (2 × 106 cells/50 µL/site + Matrigel 0.2 mL) into the dorsal aspect of the animals. 32 The mice were then randomly assigned to 6 groups. These were the vehicle group (300 µL sterile water, oral, 2 days), estradiol group (5.5 × 10−7 mole/g, subcutaneously, 3 days), Tam group (4.6 mg/kg, oral, 2 days), low-dose JWXYS (1.3 g/kg, oral, 2 days) + Tam group, middle-dose JWXYS (2.6 g/kg, oral, 2 days) + Tam group, and high-dose JWXYS (3.9 g/kg, oral, 2 days) + Tam group. The middle dose of JWXYS (2.6 g/kg) + Tam was the most similar to the situation in humans. The E2 group was used as a positive control for this study. All mice were killed humanely after 21 days of treatment.
To evaluate any possible interference that JWXYS and/or Tam might have on mice metabolism, the body weight of the mice, tumor size, and tumor volume were measured twice weekly. The tumor volume in mm3 was calculated using the following formula: Tumor volume = [(Width)2 × Length]/2. After 21 days of treatment, the mice were killed humanely under adequate anesthesia, and the tumor sizes were recorded. Furthermore, the implanted tumors on the dorsal aspect of the mice were removed and fixed in 4% formaldehyde for pathological examination. Any remaining tissue was stored in liquid nitrogen for further analysis.
Statistics
For the human study, the software package ASIQ 12.5.7 (Sybase Inc, Dublin, CA) was used for data processing, and association rule mining was applied to analyze the prescription patterns. The association rule mining technique was originally designed to help identify which groups or sets of items are likely to be purchased together in a supermarket and has been applied successfully to determine the combination patterns of CHP in previous studies.28,29
For the in vitro and in vivo studies, the results are expressed as the mean ± standard error of the mean. Differences between group means were compared using repeated-measures 1-way ANOVA, followed by Dunnett’s post hoc test or the unpaired t test. Statistical comparisons between 2 independent variables were determined by 2-way ANOVA followed by Dunnett’s post hoc test. A P value <.05 was considered statistically significant, and all results were compared against the vehicle group.
Results
NHIRD Data Analysis
The software package ASIQ 12.5.7 (Sybase Inc) was applied to process the data and to apply association rule mining in order to analyze the patients’ prescription patterns. Based on data obtained from NHIRD for Taiwan, JWXYS is the most commonly prescribed formula given by TCM doctors to patients who are being treated for breast cancer (Table 2). In addition, JWXYS is also the leading formula coprescribed with Tam when breast cancer is being treated by hormonal therapy (Table 2). However, whether a herb-drug interaction between JWXYS and Tam occurs remains unclear.
Effects of JWXYS on Cell Viability
To study the possible cytotoxic effect of JWXYS, MCF-7 cells were seeded overnight, pretreated with different doses (0, 0.1, 0.3, 1, 3, and 10 µg/mL) of JWXYS, and then evaluated by MTT assay. The result showed that there was negligible cell toxicity when JWXYS was used to treat MCF-7 cells (Figure 2A).
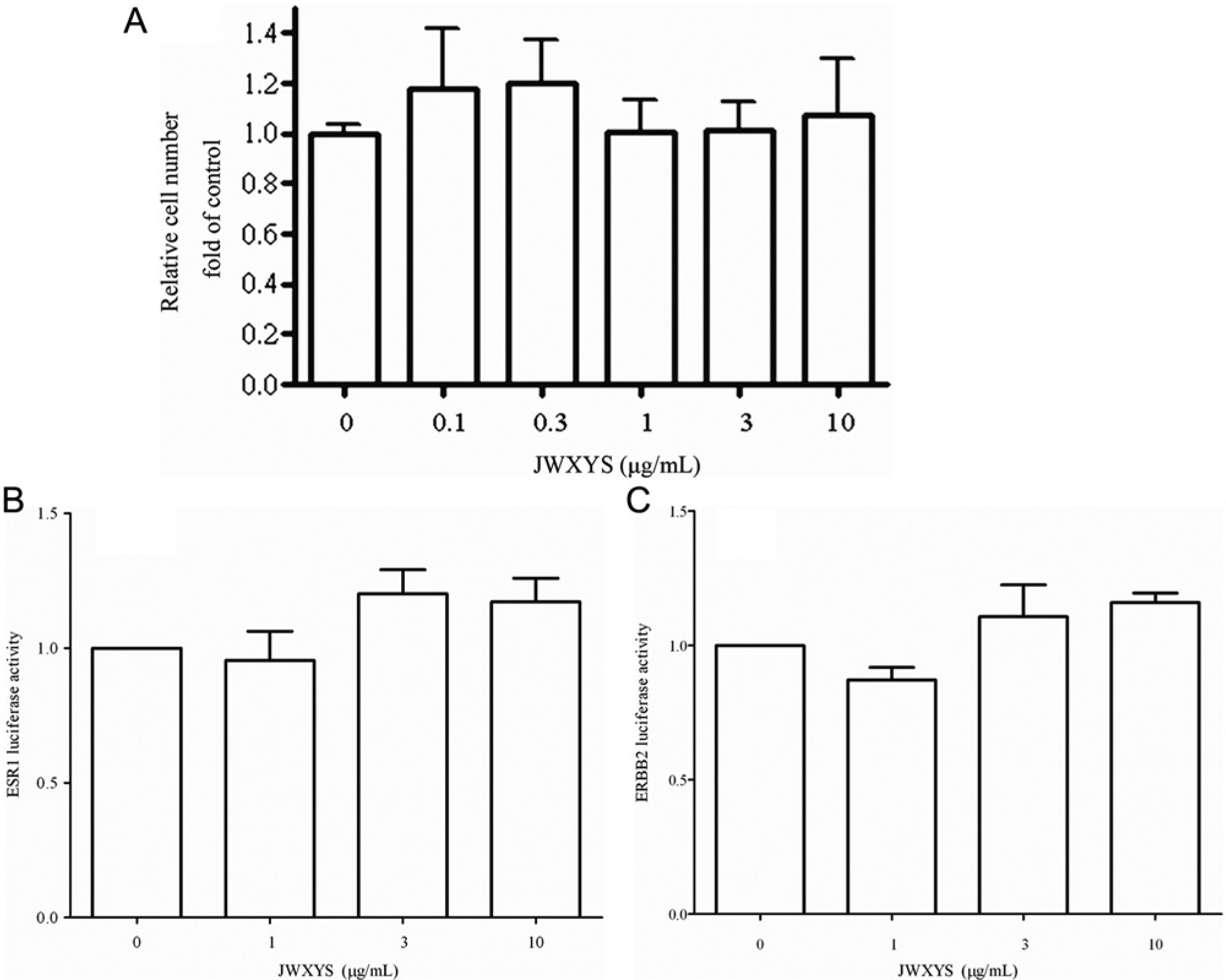
Effects of JWXYS on cell growth and ESR1, ERBB2 luciferase reporter assay in tamoxifen-treated MCF-7 breast cancer cells in vitro. There was no concentration-dependent increase in cytotoxicity among tamoxifen-treated MCF-7 breast cancer cells (A). Using the MCF-7 cell line as in the in vitro model, the effects of JWXYS extract were assessed by trypan blue dye exclusion assay and DNA flow cytometry. The pGL3 luciferase reporter vectors containing the human ERα and HER-2 promoter were constructed and transfected to human breast cancer MCF-7 cells. The herb-modulated ERα and HER-2 gene expression were evaluated by the luciferase reporter assay. The result showed that there was no significant increase in ESR1and ERBB2 luciferase activity on (1, 3, and 10 µg/mL) JWXYS (B, C).
Effects of JWXYS on ERBB2 and ESR1 as Assessed by Luciferase Reporter Assay
To investigate the effects JWXYS on ERBB2 and ESR1 gene expression, luciferase reporter vectors containing the human HER2 or the human ESR1 promoters were transiently transfected into MCF-7 cells. This was followed by treatment with different doses of JWXYS, and the results are presented as the luciferase/Renilla luciferase ratio. The results showed that the specific activities of ESR1 for the vehicle, JWXYS (1 µg/mL), JWXYS (3 µg/mL) and JWXYS (10 µg/mL) groups were 1.0, 0.872 ± 0.162, 1.107 ± 0.115 and 1.160 ± 0.137, respectively. In a similar manner, the specific ERBB2 activities for the vehicle, JWXYS (1 µg/mL), JWXYS (3 µg/mL) and JWXYS (10 µg/mL) groups were 1.0, 0.955 ± 0.057, 1.201 ± 0.158 and 1.171 ± 0.050, respectively. These findings indicate that there were no significant changes in ESR1 and ERBB2 luciferase activity when cells were treated with low, medium, or high levels of JWXYS (1, 3, 10 µg/mL) compared with the vehicle group (Figures 2B and 2C).
Effects of JWXYS on the Cell Growth of Tamoxifen-Treated MCF-7 Cells In Vitro
To investigate the possibility of interference between JWXYS and Tam, MCF-7 cells were cotreated with the 2 drugs, and this was followed by cell counting and cell cycle analysis by DNA flow cytometry. The results showed that there were no significant changes in cell growth, either in terms of cell number (Figures 3A and 3B) or in terms of cell cycle analysis (Figures 3C and 3D) between the JWXYS + Tam groups and the Tam-alone group.

MTT assay of herb-drug interaction in tamoxifen-treated MCF-7 cells (48 and 72 hours). There was no concentration-dependent increase in cytotoxicity among tamoxifen-treated MCF-7 cells (A, B). Cell cycle analysis showed no concentration-dependent increase in cytotoxicity among tamoxifen-treated MCF-7 cells (C). Flow cytometry of herb-drug interaction in tamoxifen-treated MCF-7 cells is shown. There was no significant change of cell cycle on the herb-drug interference between JWXYS and tamoxifen in vitro (D).
Effects of JWXYS on Growth-Related Signaling Pathways in Tam-Treated MCF-7 Cells In Vitro
When analyzed by Western blotting, there were no significant changes in various growth-related signals, such as ERK, P38, and P27Kip1, between the JWXYS + Tam groups and the Tam alone group.(Figures 4A-4D).
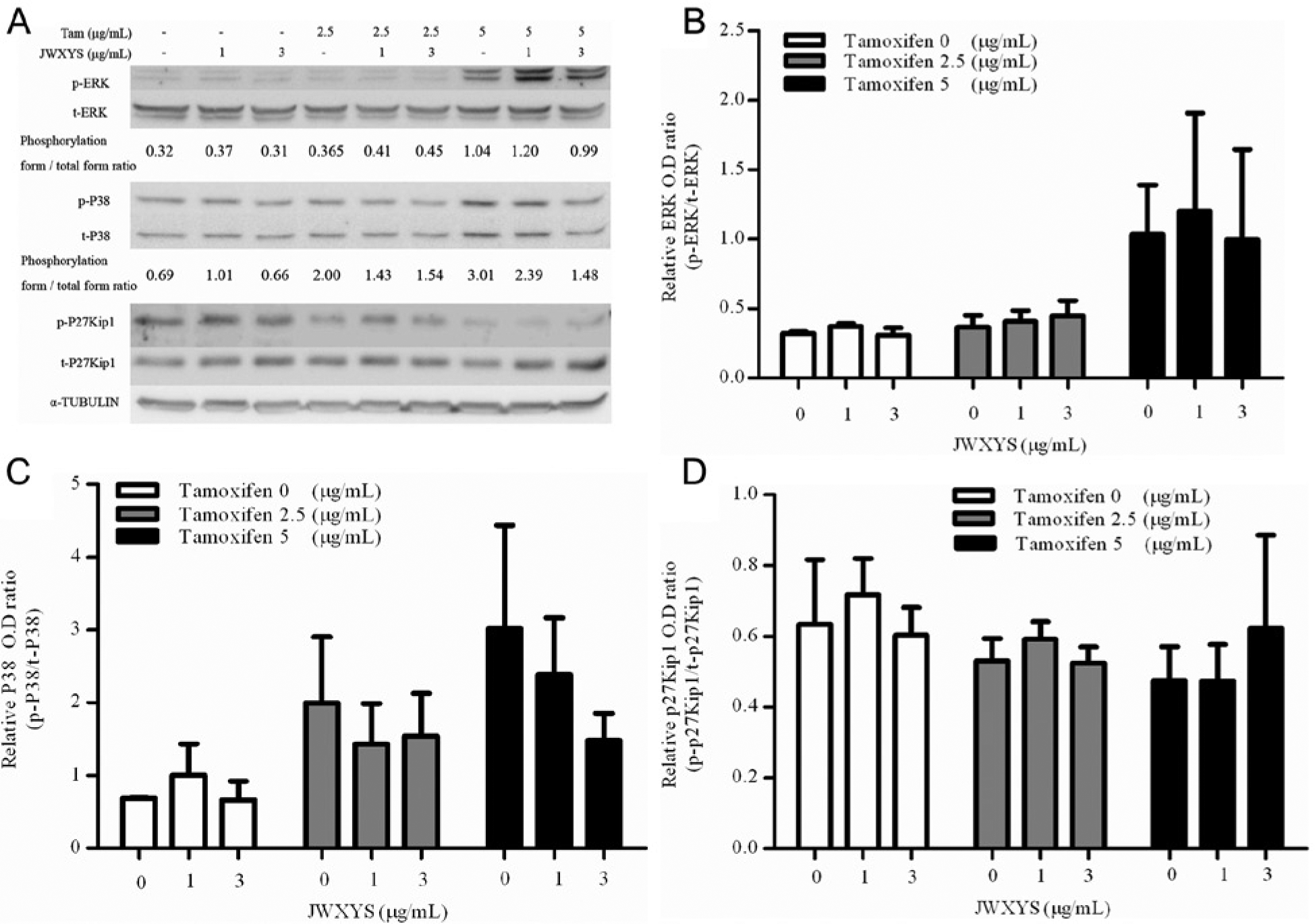
Effects of JWXYS on the signaling pathways in tamoxifen-treated MCF-7 breast cancer cells in vitro (A). When analyzed by Western blot, JWXYS treatment for 4 hours did not increase the protein expression of ERK, P38, and p27(Kip1) compared with tamoxifen treatment alone (B, C, and D).
Effects of JWXYS on Autophagy in Tam-Treated MCF-7 Cells In Vitro
Because Tam is a strong inducer of autophagy, it was important to elucidate the effects of herb-drug interaction by JWXYS on Tam-induced autophagy. This was done by examining the protein expression of microtubule-associated protein 1A/1B-LC3 (I, II) by immunofluorescence (Figure 5A) and Western blotting (Figures 5B and 5C) across the various groups. The results showed that there were no significant changes in LC3-I, LC3-II protein expression and the ratio of LC3-II to LC3-I, neither qualitatively nor quantitatively, between the various JWXYS + Tam groups and the Tam-alone group.

Herb-drug interaction on tamoxifen induces autophagy in MCF-7 breast cancer cells in vitro. The greenish coating on the cells indicates that tamoxifen induces autophagy (A). When analyzed by Western blot, JWXYS treatment did not significantly increase the protein expression compared with tamoxifen treatment alone (B, C).
Effects of JWXYS on Tam-Treated MCF-7–Implanted Athymic Nude Mice
To verify the in vitro findings whereby there seemed to be no JWXYS-Tam interference, MCF-7–implanted nude mice were used to study JWXYS-Tam interference in vivo. The results showed that there were no significant changes in body weight across the various groups (Figure 6A). After examining the tumors excised from the mice by microscopy (Figure 6B) as well as by tumor weight (Figure 6C) and tumor volume (Figure 6D), it was found that there was no significant change in tumor weight and tumor volume when the JWXYS + Tam groups were compared with the Tam-alone group.

Effects of JWXYS in tamoxifen-treated MCF-7–implanted athymic nude mice: parameters evaluated include body weight (A), microscopic examinations for tumors (B), tumor weight (C), and tumor volume (D). Results were expressed as the mean ± standard error of the mean. Differences between groups were compared using repeated-measures 1-way ANOVA followed by an unpaired t test.
Effects of JWXYS on Protein Expression in Tam-Treated MCF-7–Implanted Athymic Nude Mice
Using Western blot analysis, it was found that the protein expression of AKT, ERK, and P38 using the MCF-7-transferred nude mice model showed no significant changes in the JWXYS + Tam groups compared with the Tam-alone group (Figure 7A).

Effects of JWXYS on signaling pathways in MCF-7–implanted nude mice. There were 6 groups—namely, vehicle, E2, Tam, JWXYS(1.3 g/kg) + Tam, JWXYS (2.6 g/kg) + Tam, and JWXYS (3.9 g/kg) + Tam. There was no significant change in the protein expression of AKT, ERK, and P38 in the JWXYS + Tam groups compared with the vehicle and Tam groups (A). Herb-drug interaction on tamoxifen induces autophagy in MCF-7–implanted athymic nude mice. There was a significant increase in the protein expression of light chain (LC)3-II in the Tam and JWXYS (3.9 g/kg) + Tam groups compared with the vehicle group. But there was also a significant decrease in the protein expression of LC3-II in the JWXYS (1.3 g/kg) + Tam groups compared with the Tam group (B, C).
Effects of JWXYS on LC3-II Expression in Tam-Treated MCF-7–Implanted Athymic Nude Mice
When Western blot analysis was performed on Tam-treated MCF-7–implanted tumor tissue samples, the results showed that there was a significant decrease in LC3-II protein expression at a low dose (1.3 g/kg) of JWXYS but neither at the middle dose (2.6 g/kg) nor the high dose (3.9 g/kg) of JWXYS in the JWXYS + Tam groups compared with the Tam-alone group (Figures 7B and 7C).
Discussion
JWXYS, which is the most commonly prescribed Chinese medicine among breast cancer patients, is the leading formula coprescribed with Tam in order to alleviate the discomfort felt by patients who are receiving hormonal therapy.16,33,34 This study is the first to provide evidence as to whether JWXYS interacts with Tam either in vitro or in vivo. Accumulating evidence suggests that many patients, including those with cancer, concurrently take prescription drugs with herbal supplements and that, in some cases, this may have a negative effect on the patients because of pharmacodynamic and pharmacokinetic herb-drug interactions. 35 The prevalence of TCM use by health care providers and the interest in their use by patients outside of China continues to rise annually, especially within the field of oncology. 22 The use of TCM as an adjuvant cancer therapy has been reported to enhance the efficacy of both chemotherapy and radiotherapy as well as helping reduce adverse effects of these 2 approaches to treatment. 4 There is consensus that hormone therapies may cause certain adverse effects, such as hot flushes, cancer-related fatigue, joint pain, and insomnia, among breast cancer patients. Hot flushes occur in up to 80% of women who receive Tam treatment, and up to 45% of them grade this symptom as severe; this reduces their quality of life and affects patient compliance during hormonal therapy. JWXYS is the core formula for the treatment of breast cancer. First recorded 4 centuries ago, JWXYS was developed to cure anxiety, irritability, depression, and hot flushes in women who were suffering from menstrual disorders, which can also be considered as common adverse effects of breast cancer therapy. 36 Based on the above findings on the most used formula (Table 2) and on the most common symptoms reported by breast cancer patients,36,37 there is the advantage of cotreatment of JWXYS with Tam prescription.
The cyclin-dependent kinase (CDK) inhibitor p27 (KIP1) plays a key role in the growth and development of the mammary epithelium and in breast cancer. In normal cells, p27 inhibits nuclear CDK activity and is thus considered a tumor suppressor. 38 Recent studies have shown that p27 (KIP1) is a predictive factor for Tam treatment response in both premenopausal and postmenopausal breast cancer patients.39,40 In contrast to other tumor suppressor proteins, p27 expression levels in tumor cells are frequently regulated by ubiquitin-dependent proteolysis, which in turn is controlled by phosphorylation of p27 at a conserved threonine (T187), which facilitates polyubiquitylation of p27. This then prevents binding to its critical cellular targets, such as the cyclin E and A/CDK2 complexes. In addition, the phosphorylation of p27 by AKT and SRC kinases at either T157 (AKT) or Y74/88 (SRC) induces cellular mislocalization or functional inactivation, which disable p27 as a tumor suppressor protein.41,42 Our previous study showed that SWT, a popular herbal decoction used to modulate the menstruation cycle in women, is able to decrease, in a dose-dependent manner, trastuzumab-induced cytotoxicity in HER2 (+) cell lines, such as SK-BR-3 and BT-474, by increasing phosphorylation of p27 (Kip1) and of the antiapoptosis protein P38. 43 However, Si-Su-Tang is not a herbal product commonly used in breast cancer patients. In contrast, JWXYS is the leading formula coprescribed with Tam in Taiwan. The results of the present study have shown that there seem to be no significant changes in the protein expression of p27 (Kip1) among the JWXYS + Tam groups compared with the Tam-alone group. In addition, P38 MAPK has been shown to play an important role in regulating cell growth and to have antiapoptotic ability; this has been shown to occur not only in T lymphocytes 44 and smooth muscle cells 45 but also in cancer cells. 46 Similar to the finding for p27 (Kip1), the protein expression of P38, both in vitro and in vivo, showed no significant differences between the JWXYS + Tam groups and Tam-alone group. Taken together, these results suggests that an obvious herb-drug interaction between JWXYS and Tam in relation to either p27 (Kip1) or P38-related signal transduction is absent.
Autophagy, one type of programmed cell death, is induced when cells are deprived of nutrients, hormones, and energy; the mechanisms involved are mainly associated with the (PI3K)–AKT–mTOR signaling pathway. Microtubule-associated protein 1A/1B-LC3 is a soluble protein with a molecular mass of approximately 17 kDa that is distributed ubiquitously in mammalian tissues and cultured cells. During autophagy, a cytosolic form of LC3 (LC3-I) is conjugated to phosphatidylethanolamine to form a LC3-phosphatidylethanolamine conjugate (LC3-II), which is then recruited to the membrane of autophagosomal cells. Because LC3-II in the autolysosomal lumen is able to be degraded, lysosomal turnover of the autophagosomal marker, as detected by immunoblotting or immunofluorescence, has become a reliable method for monitoring autophagy-related processes, including autophagic cell death. 47 Using Tam and JWXYS as cotreatments, our results demonstrated that no changes could be detected by immunofluorescence when the JWXYS-Tam groups and the Tam-alone group were compared.
Tam, an antagonist of the estrogen receptor, seems to be able to prolong the survival rate for ER(+) breast cancer patients. Tam is generally known as a strong autophagy inducer, and the drug is known to stimulate autophagy by increasing the intracellular level of ceramide, which, in turn, inhibits mTOR activation. To our knowledge, very little information is available on the effects of herbal remedies on autophagy in cancer cells. Our findings show that no definitive JWXYS-Tam interaction could be identified by either the in vitro or the in vivo parts of the present study. Nevertheless, the fact that JWXYS at a low dose (1.3 g/kg), but neither at middle (2.6 g/kg) nor at high (3.9 g/kg) doses, does attenuate LC3-II expression in Tam-treated MCF-7–implanted tumors suggests that there may still be some herb-drug interactions at a molecular level. In Figure 7, there was a significant increase seen in the protein expression of LC3-II in the Tam and JWXYS (3.9 g/kg) + Tam groups compared with the vehicle group. Also in Figure 6B, a decrease in MCF-7 breast cancer cells can be seen in the JWXYS (3.9 g/kg) + Tam group similar to the Tam group. These indicate that JWXYS (3.9 g/kg) might exert a synergistic anticancer effect, but a large-scale in vivo or human study is mandatory to elucidate the possible synergistic anticancer effects of JWXYS.
There is an increasing trend whereby patients are concomitantly coprescribed drugs and food supplements but without being informed of the possibility of food-drug interaction. The use of warfarin as a drug is a good example; this is because the number of drugs that have been reported to interact with warfarin continues to expand. A recent clinical report has suggested that these types of interactions can be classified into potentiation, inhibition, and no effect, whereas the severity of interaction can be defined as major, moderate, minor, and nonclinical. 48 Unfortunately, little is known about the incidence and consequences of such interactions between modern medicines and TCM. A tentative herb-drug interaction can be postulated based on 4 possibilities: these are (1) detected and identified at the molecular level, (2) identified using a functional study, (3) identified using an animal study, and (4) found to occur in a clinical study. Interaction between Ginkgo biloba and aspirin as well as the interaction between warfarin and Danshen can be regarded as clinical interactions.
Conclusion
In summary, based on in vitro studies as well as in vivo functional studies, there seem to be no obvious interactions between JWXYS and Tam. However, the attenuation of LC3-II expression in Tam-treated MCF-7–implanted tumors at a low dose of treatment with JWXYS suggests that interference may be present at a molecular level. As more breast cancer patients seek to use traditional Chinese medicine as a complementary and alternative treatment method, doctors need to pay increasing attention to the possibility of herb-drug interactions. However, further evidence in humans using epidemiological studies and large-scale clinical data sets are needed.
Footnotes
Acknowledgements
The luciferase reporter vectors, RDB no. 2839 and RDB no. 7528, use in this study were deposited by Dr Masatoshi Tagawa at Chiba Cancer Center and Gene Engineering Division of RIKEN BioResource Center, respectively. These 2 clones were provided by the RIKEN BRC through the National Bio-Resource Project of the Ministry of Education, Culture, Sports, Science, and Technology (MEXT), Japan. This work was assisted by the Division of Experimental Surgery, Department of Surgery, Taipei Veterans General Hospital.
Authors’ Note
Jen-Hwey Chiu and Jir-You Wang designed the experiments, performed data analysis and statistics, and drafted the manuscript. Jiun-Liang Chen, Nattanant Noomhorm, Hui-Ju Liu, and Wen-Chi Chang participated in the design of the experiments and carried out the in vivo and in vitro experiments. Ling-Ming Tseng participated in the study design and helped with the data analysis. Che-Sheng Wen, Chun-Ju Chang, Wei-Shone Chen, and Yi-Ming Shyr helped with the data analysis and statistics. All authors read and approved the final manuscript. Ling-Ming Tseng and Jen-Hwey Chiu have contributed equally to this work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by grants from Taipei Veterans General Hospital (V101C-022), Cheng-Hsin and Yang-Ming project (102F218C04), Ministry of Health and Welfare (Center of Excellence for Cancer Research at Taipei Veterans General Hospital phase II), and Chang-Gung Memorial Hospital (PMRPG3A0031). We are in debt to Miss Pei-Wen Chen, Yu-Tzu Huang, and Che-Sheng Wen for their technical assistance.
