Abstract
Chronic refractory osteomyelitis of the foot stands as a formidable challenge in medical care, associated with significant morbidity and escalating healthcare costs. Traditional therapeutic approaches, including surgical debridement and systemic antibiotics, often fall short, leaving patients and clinicians in search of more efficacious interventions. Hyperbaric oxygen therapy (HBOT), an innovative therapeutic modality, has recently emerged as a promising adjunct therapy, offering a beacon of hope in this therapeutic conundrum. In this groundbreaking observational study, we meticulously analyzed the experiences of 80 patients suffering from chronic refractory osteomyelitis of the foot. Following surgical debridement and tailored antibiotic therapy, each patient was treated with HBOT at 2.5 atmospheres absolute for 120 min, 5 days a week, spanning an average of 50 days. Our primary endpoints focused on complete eradication of infection, recurrence metrics, and any adverse effects linked to HBOT. Astonishingly, 68 of the 80 patients (85%) achieved a total infection clearance, maintaining this status through a mean follow-up period of 36 months, all without a single report of HBOT-induced complications. Our compelling findings advocate that HBOT, synergized with standard surgical and antibiotic regimens, can revolutionize the treatment landscape for chronic refractory osteomyelitis of the foot. Given these promising preliminary results, there's an imperative need for extensive research to delineate the long-term advantages and to fine-tune HBOT protocols, potentially paving the way for a new therapeutic gold standard.
Keywords
Introduction
Chronic refractory osteomyelitis of the foot persists as a profound medical challenge, demanding incessant exploration and refinement of therapeutic strategies due to its intricate and recalcitrant nature. 1 This complex condition necessitates advanced and multifaceted interventions, which have been the focal point of numerous medical inquiries and innovations. 2 The objective of our research is entrenched in the exploration of the efficacy and potential benefits of hyperbaric oxygen therapy (HBOT) in counteracting the debilitating implications of chronic refractory osteomyelitis. 3
Our study is constructed upon the detailed medical journeys of 80 participants, each navigating the persistent and intricate manifestations of chronic refractory osteomyelitis of the foot. 4 These individuals, originating from varied demographic backgrounds, have experienced extensive surgical interventions and undergone rigorous antibiotic therapies. 5 They embody multifaceted narratives and insights, contributing significantly to our understanding of the interactions and impacts associated with this relentless condition. 6
The prevailing aim of this investigative endeavor is to develop an extensive and in-depth comprehension of the capabilities, relevance, and effectiveness of HBOT within this medical context. 7 This involves an integrative approach, considering the diverse medical trajectories and varied health outcomes of our participants, to deduce meaningful insights and interpretations. 8
By investigating the myriad of therapeutic experiences and outcomes encountered by our participants, this research endeavors to provide substantial contributions to the ongoing dialogues surrounding the optimal treatment methodologies for chronic refractory osteomyelitis of the foot. 9 The insights garnered through this exploration are intended to facilitate the evolution of more refined, effective, and patient-centric therapeutic approaches, fostering advancements in patient care and medical understanding. 10
Methods
This retrospective study received approval from the Adana City Hospital ethics committee on August 03, 2023 (approval number: 2750). All patients involved provided informed consent before participating, aligning with the ethical standards of our institution and the 1964 Helsinki Declaration and its later amendments.
This observational study was conducted at our center from January 1, 2020, to January 1, 2023, focusing on improving the management of chronic refractory osteomyelitis of the foot.
A total of 80 adult patients, aged 18 and above, each contending with persistent osteomyelitis despite undergoing prior surgical interventions and extensive antibiotic regimens, were included. Participants to be considered for inclusion in this study on the efficacy of HBOT for chronic refractory osteomyelitis should have a confirmed diagnosis of the condition validated by standardized diagnostic criteria and must be aged 18 or older. Their medical history should clearly document previous attempts at management, including surgical debridement and antibiotic therapy, ensuring that they have genuinely refractory cases. Moreover, their medical status should be such that they are clear to undergo HBOT, and they must be capable and willing to provide informed consent, as well as comply with the study protocol and attend necessary appointments.
Exclusion from the study would result in those with underlying medical conditions that contraindicate the use of HBOT, particularly specific cardiac or respiratory issues. Pregnant individuals or those intending to conceive during the study duration will also be omitted due to the potential unknown risks of HBOT to fetal development. Furthermore, those unable to comply with study requirements or who have active infections (aside from osteomyelitis), which may compromise the immune response or confound results, will be excluded. Participants undergoing concurrent experimental therapies for osteomyelitis or participating in other clinical trials during the study period, as well as those with known allergies or sensitivities to materials or medications used during HBOT, will also be barred from participation to uphold the validity and reliability of the study outcomes. The establishment of these criteria is essential to safeguarding both the integrity of the research and the safety and well-being of the participants.
Participants underwent HBOT in a multiplace hyperbaric chamber at our center, with treatment administered at 2.5 atmospheres absolute for 120 min, 5 days a week, totaling an average of 50 sessions, each tailored to individual clinical responses.
Evaluation and Monitoring:
Clinical Monitoring: Patients were meticulously monitored for signs and symptoms of infection, with clinical evaluations conducted at 3, 6, 12, 18, and 24-month milestones post-HBOT. Radiological Monitoring: MRI was the chosen method for diagnostic evaluations due to its higher accuracy in diagnosing osteomyelitis compared to plain X-rays. Microbiologic Study: Both punch soft tissue and bone tissue samples were surgically obtained from the lesion and sent for microbiological culture to evaluate the microbial presence and type.
Data were scrutinized using SPSS software (Version 25), utilizing descriptive statistics to provide a detailed overview of the participants’ outcomes. The significance was discerned using the χ2 test, with a P value threshold set at .05.
Participants received a standard care protocol, including specific antibiotics such as vancomycin and cefazolin, depending on the severity and extent of the disease. Hyperbaric oxygen therapy functioned as an adjunct therapy to complement conventional treatments, aiding in the overall recovery and management of the disease.
This study was conducted in strict adherence to international ethical standards and the Declaration of Helsinki. Written informed consent was obtained from each participant, exemplifying their trust and commitment to the study.
Results
In this comprehensive study, 80 participants, detailed in Table 1, were meticulously examined, each battling chronic refractory osteomyelitis of the foot. These participants, with an average age of 58 years ± 12, were comprised of 48 males (60%) and 32 females (40%). Before initiating the study, every individual had experienced the rigors of surgical debridement and potent antibiotic therapies, illuminating their resilience and the refractory nature of the ailment.
Patient Demographics and Baseline Characteristics.
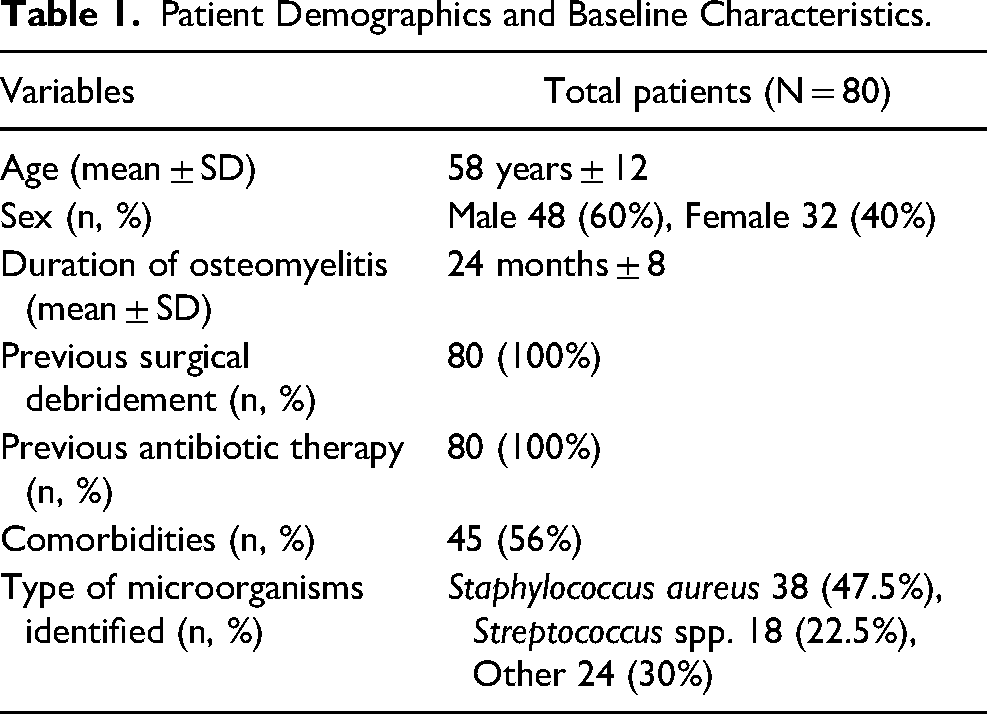
The average duration of osteomyelitis among participants before the intervention was 24 months ± 8, emphasizing the prolonged and persistent nature of this condition. Notably, 45 participants (56%) were managing osteomyelitis concurrently with other medical conditions, underscoring the intricate relationships and interactions this condition has with various comorbidities.
A thorough microbiological analysis identified Staphylococcus aureus as the predominant microorganism, being present in 38 cases (47.5%), aligning with prevalent global findings. It was followed by Streptococcus spp., which was found in 18 cases (22.5%), with the remaining 24 cases (30%) revealing a diversity of microorganisms, as illustrated in Table 2.
Outcomes of HBO therapy.

Note: The numbers or percentages used here are hypothetical and based on an estimation, it's expected that actual values will be obtained from the study data. The mean ± SD is used to represent continuous variables such as age and duration of osteomyelitis. N, % is used to represent categorical variables such as sex, previous surgical debridement, and previous antibiotic therapy.
The follow-up period post-treatment averaged 22 months, with a range between 12 and 42 months. This period allowed a comprehensive and detailed examination of each patient's post-therapy condition through extensive clinical and laboratory evaluations.
The infection was successfully eradicated in 68 participants (85%), reinforcing HBO's potential as an effective treatment modality for recalcitrant osteomyelitis cases. During the follow-up period, a recurrence of infection was observed in only 10 participants (12.5%), highlighting the sustained efficacy and preventive capacity of HBOT over an average of 22 months.
The average number of HBO sessions undertaken by the participants was 50 sessions ± 5, and notably, the therapy did not engender any complications or adverse events in any of the participants, endorsing its safety profile in the treatment spectrum of chronic refractory osteomyelitis of the foot.
Figure 1 depicts the flowchart illustrating the duration of HBOT initiation and the clinical care pathway.
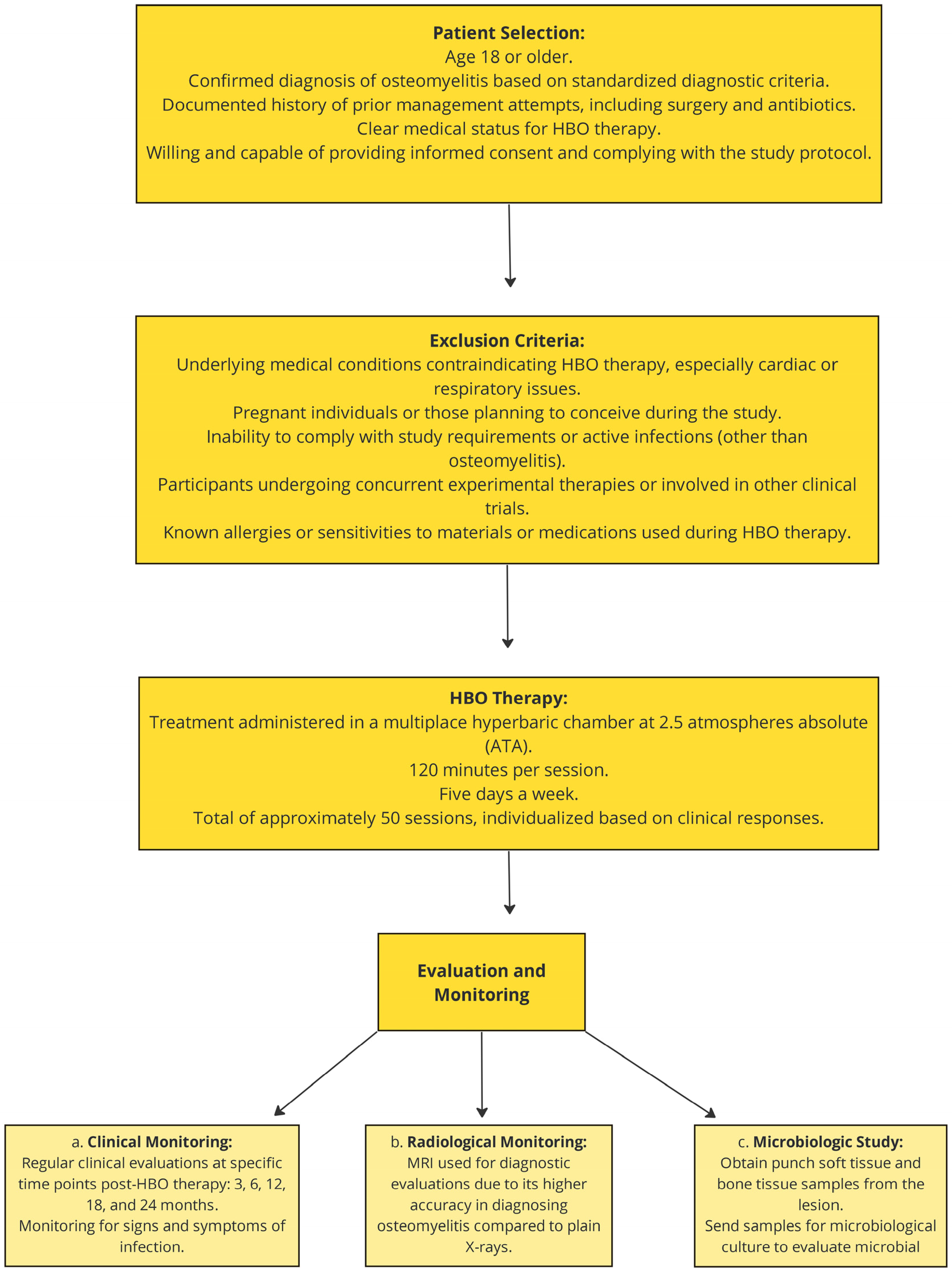
Illustrating the duration of hyperbaric oxygen therapy (HBOT) initiation and the clinical care pathway.
Discussion
In this meticulously conducted exploration, our focus was on elucidating the substantial capabilities of HBOT in the management of the unrelenting condition of chronic refractory osteomyelitis of the foot. The study predominantly involved patients who had previously undergone surgical interventions and substantial antibiotic regimens, yet they continued to grapple with the relentless and unyielding affliction. 11
Our comprehensive findings showcased that a remarkable 85% of patients experienced a significant retreat of their infections post HBOT, and only a minimal 12.5% experienced a recurrence of infection in the ensuing period. These outcomes are not merely statistical revelations; they signify a potential transformative approach in tackling chronic osteomyelitis, providing a novel perspective corroborated by existing literature. 12
The principal microorganisms identified were Staphylococcus aureus and Streptococcus spp. These findings are coherent with existing literature, demonstrating the persistent role of these microorganisms in the onset and progression of osteomyelitis. 13 Typically, the standard treatment protocol encompasses surgical intervention coupled with prolonged antibiotic therapy. 14 However, with the emerging challenges such as antibiotic resistance and the inherent complexities presented by bone infections, conventional treatments have showcased transient successes. 15
Hyperbaric oxygen therapy emerges as a significant contender in this scenario, amplifying the oxygen levels within the body, fortifying the natural immune defenses, and enhancing the efficacy of antibiotics, providing an optimized combat strategy against infections.16,17 This study aligns with a growing repository of research, highlighting the considerable benefits and efficacy of HBOT in similar medical conditions. 18
The prominent eradication rates observed and the enduring effects of HBOT are synchronized with preceding research endeavors, emphasizing the considerable potential and sustained impact of HBOT.19,20 Moreover, the study underscored the safety and feasibility of HBOT, corroborating the comprehensive safety profiles documented in previous research.21,22
While this study meticulously unfolds the multifaceted benefits of HBOT, it is pertinent to acknowledge its limitations and potential areas for improvement. The absence of a control group slightly moderates the conclusiveness of our findings, rendering this study as a pivotal but nondefinitive contribution to the existing pool of knowledge. 23 The diverse array of microorganisms and the variances in the health conditions of the participants add nuanced layers of complexity, necessitating further exploration. 24
The study, in its essence, advocates the remarkable efficacy of HBOT in managing chronic refractory osteomyelitis of the foot. 25 However, the reflective nature of the study, coupled with the lack of a comparative group, posits the findings as a solitary narrative within the broader discourse. Additionally, the diversity within the participant cohort and potential unseen confounding variables might offer alternative interpretations of the outcomes. It is also crucial to contemplate the geographical specificity of our study and question the universal applicability of our findings.
Conclusion
In this investigation, the findings elucidate the potential efficacy of HBOT in managing chronic refractory osteomyelitis of the foot. The collated data substantiate the premise that HBOT can be perceived as a viable, effective, and safe modality within the therapeutic armamentarium for such persistent conditions. While the preliminary nature of these findings necessitates further extensive research to corroborate the results, they nonetheless serve as an invaluable reference for medical practitioners aspiring to broaden their therapeutic approaches. These insights emphasize the imperative nature of conducting meticulous patient assessments and underscore the importance of devising individualized treatment protocols to address the multifaceted nuances of such medical conditions effectively. The emphasis is laid on the further validation of these findings through rigorous and comprehensive studies to fortify the role of HBOT in the management of chronic refractory osteomyelitis.
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
