Abstract
Diabetic foot ulcer represents the primary cause of hospital admissions, amputations, and mortality in diabetic patients. The development of diabetic foot ulcers is influenced by peripheral neuropathy, infection, and ischemia, with diabetes contributing to peripheral artery disease. Free tissue transfer combined with revascularisation of the lower extremity provides the potential opportunity for limb salvage in individuals with lower extremity defects due to critical limb ischemia and diabetic foot.
Keywords
Introduction
Diabetic foot ulcer is a worldwide issue with significant economic consequences for patients, families, and society. Diabetic foot complications are the primary cause of hospital admission, amputation, and mortality in patients with diabetes, accounting for 40% to 70% of all lower-extremity amputations. 1 It results from varying extents of peripheral neuropathy, infection, and ischemia. In addition, diabetes contributes to the development of peripheral artery disease (PAD) through the interplay of hemodynamic, neuro-hormonal, and metabolic factors (Figure 1).
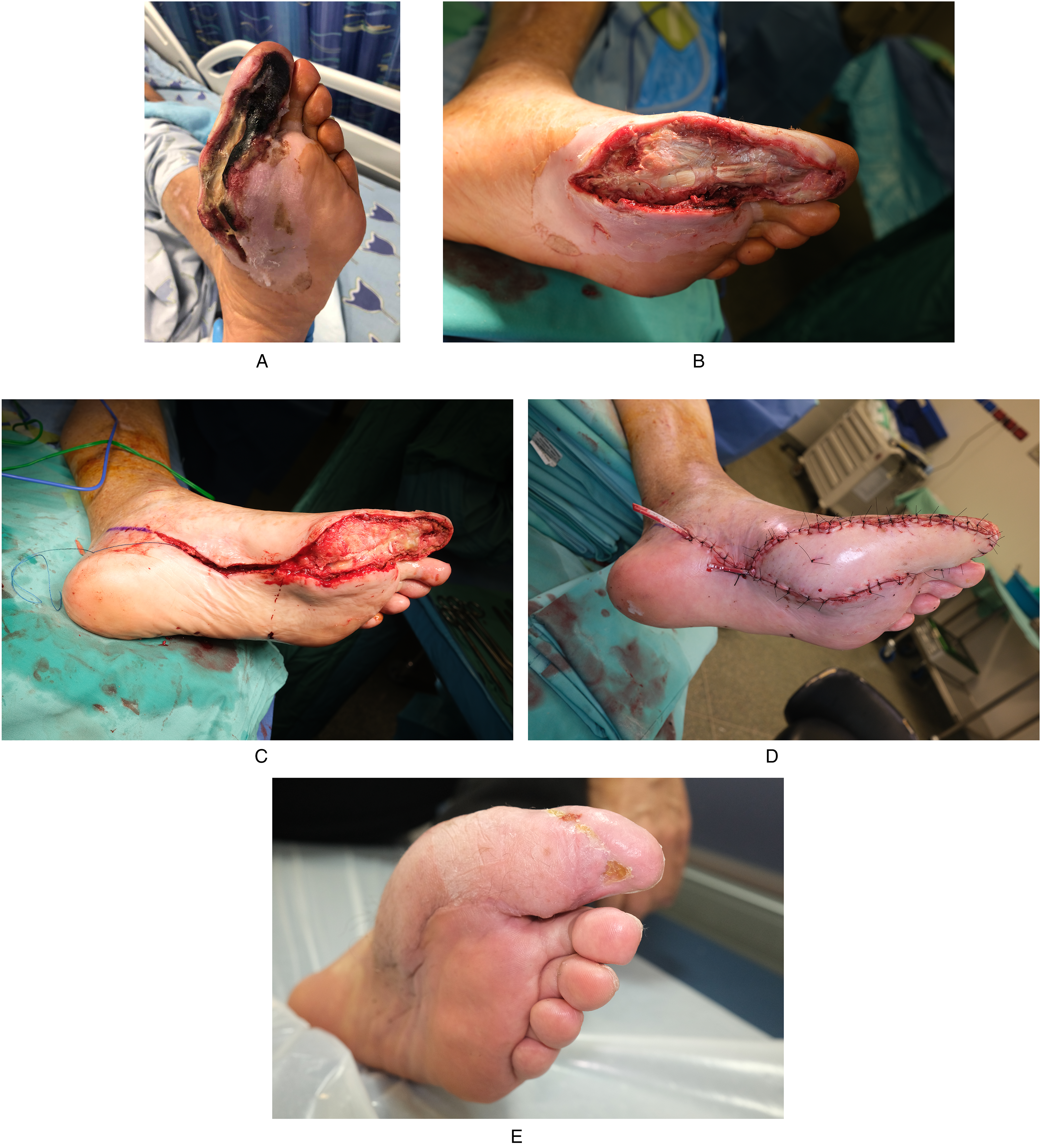
(A) A 72-year-old male diabetic patient presented with infection and ischemia of the first toe (Lt Foot).
These patients have a high mortality rate after amputation, ranging from 39% to 80% at 5 years. 1 With the introduction of a multidisciplinary approach and increased focus on reconstruction, the aim and result of management have shifted from major amputation to limb salvage. 2
Considerations in Diabetic Foot Reconstruction
Wound debridement is the first and a major step to limit the spread of acute infection and lead to the salvage of the diabetic foot.3,4 A delay in surgical debridement increases the risk of a more proximal level of amputation, while in a deep tissue infection, systemic antibiotic therapy administration in the absence of extensive surgical debridement is insufficient for limb salvage. 5 Following infection control and stabilizing the blood glucose levels, maximizing the flow to the feet sets the foundation for reconstruction and an increased salvage rate, especially since ischemia has been reported to be at least a contributing factor in 90% of diabetics undergoing major amputation. 6
Although the indications for major amputation still exist and are often caused by multiple factors such as systemic sepsis, major tissue loss, significant comorbid factors, poor patient compliance, and non-reconstructable peripheral vascular disease, the goal remains to salvage the limb under good clinical judgment. 7 A nonhealing ulcer itself should not be considered an indication for amputation but be explored to solve the pathology behind it.
In the reconstruction of diabetic foot ulcers, many potential surgical options are available. These include healing by secondary intention, skin grafts, local flaps, pedicled flaps, and free tissue transfer.
The reconstruction should preserve the length of the limb by minimizing the amputation. The preservation of leg length decreases energy expenditure and aids ambulation by providing a suitable contour with a durability permitting normal ambulation with or without appropriate prosthesis and orthosis.
In the absence of exposed vital structures, wounds such as potentially contaminated or irregular can be left to heal by secondary intention through the application of daily dressing changes, wound healing adjuncts, Hyperbaric Oxygen treatment and/or Negative pressure wound therapy. Delayed primary closure is easier to accomplish when tissue edema and induration have resolved. An adequate soft-tissue envelope can also be created by removing underlying bone. This occurs in partial foot amputations where just enough bone is removed to facilitate delayed primary closure. For example, when amputating a necrotic toe, preservation of the bony structure is important for preventing the collapse of adjacent digits into the amputated space. In these cases, fillet flap coverage is often offered. 8
Split-thickness skin graft is the simplest of all coverage techniques and can be used to close most foot and ankle wounds. The only prerequisite is wound with a bed of healthy granulation tissue. Skin grafts are contraindicated in wounds with exposed bone, tendon and joints where the vascularity may not be sufficient to promote granulation tissue. Local flaps may be useful for small defects, because they only need to be of sufficient size to cover the exposed tendon, bone, or joint. The rest of the wound can then be covered with a simple skin graft. This combination of limited local flap and skin graft frequently obviates the need of larger pedicled or free flaps. If correctly designed, a local flap can also improve the surgical exposure of the underlying tissue if corrective surgery has to be performed. 9
For moderate defects, pedicled flaps are often necessary. However, when reconstructing diabetic foot with reduced vascular flow, the use of local flaps may breach the distal flow of the small collateral vessels which may play an important role for distal circulation. Also, the angiosome affected by ischemia must be weighed since a Poor design of a local flap in the territory of that angiosome may lead to the expansion of defect size and may cause of new progression of the ischemic wound. 10
For these reasons, Free flaps may be ideal. 11 Microvascular free tissue transfer promotes healing by covering various defects with well-vascularized tissue, providing supplementary blood flow to ischemic zones, contributing to venous drainage in regions of venous insufficiency, and may promote faster inosculation. 12 Although free flap reconstruction in diabetic patients makes both the treatment and the healing process more complex, reconstruction rather than amputating above the ankle improves the quality of life and significantly increases the resultant 5-year survival rate. 13 Free tissue transfer combined with revascularization to overcome critical limb ischemia (CLI) and diabetic foot infection have been common choices over the last few decades and have led to a high rate of limb salvage and good long-term prognosis.1,14,15
Preoperative Work-Up and Vascular Intervention
Having adequate flow to the region of reconstruction is most essential before microsurgery reconstruction. We believe that the most important factor for the success of microsurgical reconstruction may be the perfusion of the recipient vessel.
In our surgical algorithm, all patients considered for microsurgical reconstruction undergo a noninvasive computerized tomography (CT) angiogram or an invasive angiogram to evaluate the vascular status. The CT angiogram provides information regarding the general vascular anatomy of the lower extremity and shows artherosclerotic changes in vessels. The overview is important as collateral vessels may be the main trunk to the distal limb. Without this information, one may elevate the flap harvesting the main arterial source to the distal limb and cause limb ischemia. If vascular status is in doubt, then revascularization by angioplasty or bypass surgery is referred. In the preoperative work-up, potential recipient vessel sites are examined and marked around the ulceration with ultrasound color duplex. The flow is considered adequate if the flow velocity measured in the target anastomotic site is 15 to 20 cm/s or more, as most of the perforator flaps have a flow velocity greater than 20 cm/s for the perforating artery. 3
When looking for recipient vessels, three main options are considered. The first is a spared segment of a major vessel. In this case, an end-to-side anastomosis is warranted as the distal flow can be vital to tissue survival beyond the point of anastomosis. For this same reason, an occlusion in the anastomosis could be catastrophic and lead to extensive necrosis and the need for amputation. The second option is to look for branches originating from this major vessel. When a side branch is found with adequate flow, it may allow an end-to-end anastomosis to the flap's pedicle with a smaller effect on the vascularity of the foot. Frequently, the use of small branches will require meticulous anastomosis as the diameter will be smaller than 0.8 mm, requiring a supermicrosurgery approach. In these cases, the branch will have a good pulse if there is reasonable flow from the major artery. If the major artery is totally collapsed because of the progression of the pathologic change leading to severe calcification, the branches from the major artery become useless despite the small arteries being spared from calcification. The third option is any small perforating vessels from either in the defect or the adjacent angiosome territory. With this approach, even patients with poor vascular flow from the major vessels and advanced ischemia can be given the opportunity for reconstruction, if a small artery with an adequate pulse can be found. Following successful recanalization, the diversity of suitable recipient vessels may increase, leaving the surgeon with more options to choose from, as there is usually an increase in flow velocity of 15% to 50% for the small recipient artery after endovascular procedures. 16 This improvement may shift a vessel with a marginal flow to an adequate flow. It should be noted that when considering using recanalized vessels as recipients, flap failure and secondary amputation rates after diabetic foot reconstruction with a free flap differed with the severity of the vessel status before angioplasty. Partially occluded vessels showed results comparable to intact vessels, while totally occluded had higher failure rates. However, even with higher failure rates, an acceptable rate of extremity salvage can be obtained, with the combined patient survival and limb salvage rate of 76.2% at 1, 3, and 5 years. 17
Surgical Technique for Diabetic Foot Reconstruction with a Free Flap
Debridement is performed according to the angiosome principle, respecting the territory belonging to the involved occluded artery segment. During debridement, pulsatile arteries are marked. Any artery in the operative field that presents a good pulsatile flow can be used as a recipient vessel since it is a good indicator of sufficient arterial circulation in the anastomotic site.
In most cases, a named artery is used for its rapid accessibility. In our practice, end-to-side anastomosis is most often used since all efforts are made to preserve the distal flow to the foot and to avoid injury to the collateral vessels that may be crucial for perfusion. Other considerations regarding the choice of the recipient vessel include the flap to be used, the method, and the site of microvascular anastomosis. Flap selection and recipient vessel selection affect each other reciprocally. The major determinants have to do with positional convenience and the surgeon's preference. 18 A contingent recipient vessel must always be anticipated since diabetic patients have a high prevalence of vascular calcifications. These calcifications may occur even in the absence of significant vascular disease, especially in the presence of diabetic neuropathy. 19 If there are no pulsating small arteries in the lesion, the search for an adequate recipient artery is extended to the adjacent healthy angiosome territory. Once a pulsatile perforator or small artery is found, it is dissected and preserved. For the recipient veins, there is no preference over superficial or deep veins. Easily available veins found during debridement are mostly used. If not, the vena comitantes of the most adjacent main vessel can be used even if it is not the recipient vessel.
Because of the superficiality of this approach, usually there is no need for a flap with a long pedicle. Since these patients have poor vascular state, reconstruction in many cases is considered a one-chance procedure since if a recanalized vessel reconstruction fails, patients are referred to amputation. In cases of failure, if perforator flaps are used for reconstruction, there is minimal added morbidity. Nor does it significantly delay the progression to amputation.
Timing of Flap Surgery After Vascular Intervention
Although intact flow can be observed immediately after percutaneous transluminal angioplasty (PTA), the lumen of the vessel can rapidly reocclude by narrowing or by thrombosis caused by the intimal injury of the PTA or free flap surgery. Previous reports indicate that target vessel restenosis occurs in up to 70% at 3 months20,21 and up to 83% of isolated below-the-knee arteries in diabetic patients within 1 year.21,22 Nevertheless, despite these significant re-occlusion rates, studies on the impact of tibial patency on clinical outcomes have indicated that even with the inevitable re-occlusion of the recanalized vessel, no significant differences in clinical outcomes were observed in an interval of 12, 24, and 36 months between bypass treated patients that showed much higher patency rates compared to angioplasty-treated patients. 23 These findings were used to define the tide-over concept predicated on the assumption that increased perfusion is mandatory for ulcer healing in CLI but not thereafter for maintaining skin integrity. For this same reason, reconstruction is scheduled as early as possible to remain within the therapeutic window of improved perfusion and the optimal setting for wound healing. However, in the severe ischemic patients, following vascular intervention, patients are at a higher risk of suffering from reperfusion injury or aggravated overt infection and may need further debridement before reconstruction. 3 In our recent study, the duration between angioplasty and reconstruction was an average of 18.8 days. 17 In cases of open vascular intervention, reconstruction should take place at the same time if possible, especially if the bypass is done using a vein, since the resistance in the graft will rise with time. If reconstruction is not possible at the time of intervention, we advise waiting for stabilization of the graft.
Vascular Intervention Following Free Flap Reconstruction
When a flap begins to fail, the likely causes must be identified and rectified. The majority of the complications are related to vascular compromise that necessitates urgent re-exploration, and for most cases, postoperative PTA for flap salvage is not routinely recommended under usual circumstances. However, in these extremely challenging cases, when there is low doubt for intraoperative technical or anastomosis failure, PTA could be an alternative, since intraoperative spasm or thrombosis of the recipient artery can occur, and unless resolved, may lead to flap failure. 24
The Role of Free Flap Reconstruction in Establishing Tissue Perfusion—“The Nutrient Flap”
The concept of a nutrient flap delivering and increasing perfusion in an ischemic area was first proposed in 1989. 25 Following this principle, a free flap serves as a source of supplementary blood flow to ischemic tissues and induces a capillary network. Evidence of a new capillary connection being established between the nutrient flap and the ischemic region was provided more recently by Tanaka et al. 26 Typically when the flap reestablishes the flow after microsurgery, the free flap transcutaneous partial pressure of oxygen level, measured with a Clark-type measuring electrode probe, can be as low as 10 mm Hg in the first few days, whereas the surrounding normal tissue is around 50 mm Hg, creating an oxygen gradient that allows inosculation and angiogenesis to occur into the flap. By nourishing the ischemic limb, local conditions are improved enough to allow the free flap to survive, even when the pedicle is occluded. 27 In ischemic limbs, following revascularization, the initial process may be the same with transcutaneous partial pressure of oxygen level reaching over 40 mm Hg after PTA. However, the oxygen content of the surrounding tissue usually starts to decline after 3 to 4 weeks, despite the angioplasty. 28 In our recent study, we observed that transcutaneous partial pressure of oxygen levels was significantly higher in patients that following PTA were reconstructed with a free flap compared to patients with transmetatarsal amputation or ray amputation that were able to heal by either primary or local flap closure. The patients that underwent free flap surgery were able to not only sustain the increased oxygen tension level after PTA but also augment it, further supporting the idea of the nutrient flap. Therefore, in the free flap group, one can assume that the tissue oxygen level will start to decline on the surrounding tissue as well. At some point, the pressure gradient between the flap and the surrounding tissue will flip, and ultimately a "reverse angiogenesis" will occur from the flap to the surrounding tissue, and the transcutaneous partial pressure of oxygen level of the surrounding tissue will rise instead of fall, as seen in the non-free flap group. A recent case report by Seo et al 29 supports this concept, where they describe a patient in whom there was a change in the direction of blood flow in a distal bypass graft following microsurgical reconstruction with a Latissimus dorsi free flap in an ischemic lower limb.
Conclusion
The management of diabetic foot complications has evolved towards a greater emphasis on limb salvage rather than major amputation, thanks to advancements in reconstructive techniques and multidisciplinary approaches. Microvascular free tissue transfer combined with revascularization of the lower extremity provides the potential opportunity for limb salvage in individuals with lower extremity defects due to CLI. Preoperative work-up and thorough vascular intervention are essential steps in achieving successful outcomes in free flap reconstruction. The careful selection of recipient vessels and timely reconstruction after vascular intervention contribute to the improved survival of the reconstructed limb. The concept of the “nutrient flap” has further highlighted the potential benefits of free flap reconstruction in establishing tissue perfusion and supporting wound healing in ischemic limbs.
While the challenges remain, the utilization of free flaps for diabetic foot reconstruction offers a promising avenue to enhance limb salvage rates and ultimately improve the quality of life for diabetic patients.
Supplemental Material
Supplemental Material
Supplemental Material
Supplemental Material
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
