Abstract
Research suggests Cognitive Behavioural Therapy (CBT) is an effective intervention for tinnitus-related distress in typically developing adults. However, there is no specific evidence that CBT is effective for tinnitus distress in people with a learning disability (LD), or information regarding potential adaptations. This quasi-experimental single case study aimed to test the hypothesis that CBT would reduce tinnitus distress in a person with an LD. Quantitative and qualitative data showed significant reductions in self-reported tinnitus-related annoyance, sadness, interference with valued activities and sleep disturbance. All tinnitus distress-related measures except perceived loudness showed statistically significant improvement, with interference with valued activities showing the largest effect size, Ruscio’s A = 0.99, 95% CI [0.91, 0.99], p = .0026. Adaptations included use of visual and sensory aids, and inclusion of parental thoughts, feelings and behaviours as treatment targets. This study offers support for the efficacy of CBT for treating tinnitus distress in people with LD, and for the efficacy of carer-supported CBT in this population.
Theoretical and Research Basis for Treatment
Tinnitus is characterised by unwanted perception of sound unrelated to external stimuli. Various factors are associated with tinnitus onset, including head injuries, exposure to loud noise and medical treatments such as chemotherapy (Dille et al., 2010). Tinnitus affects 14% of adults globally (Jarach et al., 2022). However, only 10-20% of tinnitus sufferers experience distress (Baguley et al., 2012). Indeed, self-reported tinnitus-related distress correlates only weakly with psychoacoustic measures of loudness (Adamchic et al., 2012), leading to an emphasis on psychological models of tinnitus distress.
According to McKenna et al. (2014) cognitive model of tinnitus, overly negative appraisals of tinnitus amplify distress and physiological arousal. This drives selective attention, hypervigilant monitoring and safety-seeking behaviours that increase perceptions of tinnitus intensity and frequency, further compounding negative appraisals. National Institute for Health and Care Excellence (2020) recommend Cognitive Behavioural Therapy (CBT) for the treatment of tinnitus-related distress, as well as amplification devices if tinnitus occurs in the context of hearing loss. National Institute for Health and Care Excellence (2020) guidelines do not recommend other proposed treatments for tinnitus, due to a lack of robust evidence for sound therapy and neuromodulation, and due to evidence of adverse effects in the case of betahistine. A Cochrane review of CBT interventions for tinnitus including 28 studies found a medium effect size for CBT compared with no intervention in terms of tinnitus-related impact on quality of life, a large effect compared with audiological care and tinnitus retraining therapy, and a small effect compared with active controls such as relaxation training and psychoeducation (Fuller et al., 2020), suggesting CBT is an effective intervention for tinnitus-related distress.
However, these studies focused on typically developing people, meaning there is no specific evidence that CBT is effective for tinnitus distress in people with a learning disability (LD). Indeed, to the authors’ knowledge, no single case studies have evaluated CBT for tinnitus distress in people with LD. Historically, behavioural and medication-based interventions were predominant for people with LD (Vereenooghe & Langdon, 2013) due to widespread beliefs that cognitive deficits precluded engagement with cognitive approaches (Bütz et al., 2000). However, subsequent research indicates people with mild to moderate LD can deploy or develop skills crucial to CBT engagement, including linking events with emotions (Oathamshaw & Haddock, 2006) and distinguishing thoughts, feelings and behaviours (Sams et al., 2006). Indeed, McGillivray & Kershaw (2015) found combined cognitive and behavioural strategies delivered superior long-term improvement for adults with a mild LD experiencing depression compared with only behavioural or only cognitive strategies. A meta-analysis (Graser et al., 2022) and systematic review (Fynn et al., 2023) have indicated that CBT is effective for treating depression and anxiety respectively in people with LD.
For people with LD, National Institute for Health and Care Excellence (2016) advises utilising guidelines for specific mental health problems, with adaptations made to suit the person’s preferences, understanding, needs and strengths, as well as involving family members to support treatment. The most common adaptations to CBT for people with LD included adapting activities, including using visual worksheets to enhance generalisation, consideration of developmental level, simplification, adaptation of language, and, crucially, the involvement of caregivers (Routledge Surley & Dagnan, 2019).
Involving caregivers may be particularly important given the role of parental factors in the aetiology of mental health difficulties such as anxiety (Murray et al., 2009). Anxiety may be transmitted from parent to child via modelling (Gerull & Rapee, 2002), information transfer (Hadwin et al., 2006) and parenting style, particularly parental control (DiBartolo & Helt, 2007).
Parental control comprises two components: overinvolvement and autonomy-granting (McLeod et al., 2007). Overinvolvement concerns the impeding of emotional independence and autonomy, and encouraging of dependence on the parent (Barber, 1996). Autonomy-granting concerns the encouraging of a child’s decision making and input on problem-solving (Bumpus et al., 2001). A meta-analysis (McLeod et al., 2007) of associations between parenting and child anxiety found a medium effect of .23 for overinvolvement and a large effect of −.42 for autonomy granting. An experimental study (Thirlwall & Creswell, 2010) found that greater maternal controlling behaviours led to children predicting poorer performance before giving a speech, and less satisfaction with their performance after the speech. As such, reducing overinvolvement and enhancing autonomy-granting parental behaviours may be an important target for intervention, particularly with LD populations (Jahoda et al., 2009).
Stallard, 2009 identifies four roles parents may play in CBT for young people: facilitator, co-clinician, co-client and client. As ‘facilitator’, parents ensure attendance and may at times attend themselves to understand the treatment rationale. As ‘co-clinician’, parents engage in treatment alongside their child to bolster utilisation of skills and promote generalisation. As a client or co-client, parental factors become a treatment focus, such as the interaction between parent and child thoughts, feelings and behaviours. These roles may shift throughout treatment (Creswell et al., 2013; Siddaway et al., 2014).
Similarly, in CBT with LD populations, caregivers can support clients in developing and generalising skills, but also by stepping back to facilitate autonomy (Jahoda et al., 2009). Jahoda et al. (2009) suggest caregivers can help scaffold skill development within and between sessions. Yet scaffolding must also sit within a dialectic dance between support-giving and autonomy-granting. Jahoda et al. (2009) highlight the role of others’ reactions in the development of one’s sense of self. This underscores the importance of cultivating opportunities outside therapy for people with LD to implement new learning autonomously, and, crucially, to have this autonomy acknowledged and reflected back to them.
There is a lack of research evaluating CBT for tinnitus in LD populations. As such, this single-case quasi-experimental study aimed to test whether CBT with parental involvement would reduce tinnitus distress in a person with an LD.
Case Introduction
Jane is a Caucasian woman in her early twenties with a mild to moderate LD and hearing impairment. Jane is able to communicate verbally, but experiences challenges with information processing and comprehending complex questions, and requires time to express herself verbally. She also struggles with memory, such as retaining skills she has learned. She lives with her parents and younger brother and attends adult learning courses at a local college. Jane is able to attend to her basic needs independently such as toileting and eating, but requires support with more complex tasks such as preparing food. She was referred to a community LD service by her social worker for support managing distress related to her tinnitus. An initial psychology screening noted Jane and her mother both experienced anxiety, with Jane’s mother reporting she was currently receiving therapeutic support for her own anxiety. Following the screening, Jane was placed on the waiting list for psychological therapy for tinnitus. When weekly therapy commenced, Jane requested that her mother, Liz, attend all appointments to support her and facilitate communication. Both Jane and Liz provided written informed consent for this case study to be written up and published. Their names have been changed to preserve anonymity.
Presenting Complaints
Jane described tinnitus as a high-pitched buzzing noise which often kept her awake at night, meaning she sometimes missed college due to tiredness. She said tinnitus was intensified both by silence and loud noise. As such, she said it stopped her doing things she wanted to do, such as going to concerts, and made college difficult if the classroom was noisy. She said tinnitus made her feel sad and annoyed. Liz and Jane reported using numerous coping strategies for tinnitus, including noise machines, audiobooks, saying a mantra, wiggling body parts, looking at happy pictures on keyrings, and Liz stroking Jane’s head. These were largely guided by Liz, who would go into Jane’s room at night when she heard Jane wake up. They said these coping strategies helped slightly, but felt they had become largely ineffective. They both reported being worried by tinnitus and its potential to cause Jane distress, impede sleep and preclude college attendance the next day.
History
As a toddler, Jane underwent surgery, chemotherapy and radiotherapy treatment for a brain tumour. Jane and her mother reported this was a difficult time for the whole family, with frequent trips to the hospital. Jane was left with impaired speech, cognition, memory and co-ordination, low energy levels, hearing damage requiring hearing aids, and she subsequently developed tinnitus (of which there was no previous evidence). Jane’s mother reported that psychological support for tinnitus was sought seven years earlier from a mainstream child and adolescent mental health service, but said this support was not granted due to Jane’s learning disability.
Jane was currently receiving hormone treatment for early menopause, which was causing periodic headaches. She received considerable support in daily living from her parents, particularly her mother. Jane had a large extended family, which she and her mother said had been very supportive at various times, including a family member who also experienced tinnitus, and as such was particularly understanding of Jane’s difficulties.
Assessment
Assessment was conducted across an introductory meeting, at which idiosyncratic tinnitus measures were developed, and four assessment sessions. These included reviews of symptoms and existing coping strategies, development of a genogram and identification of treatment goals. Treatment goals agreed with Jane and Liz focused on reducing tinnitus distress as reflected in the idiosyncratic measures, namely: annoyance, sadness, interference with valued activities and sleep disturbance.
Based on the assessment, it was hypothesised that adapted CBT for tinnitus would reduce Liz’ tinnitus-related distress (sadness, annoyance, interference with valued activities and sleep disturbance). More specific hypotheses guided treatment, but could not be tested statistically due to the AB design and integrated treatment package with components introduced concurrently. Specifically, it was predicted that: (a) reducing Jane and Liz’s worry about tinnitus would reduce perceived frequency and loudness of tinnitus and tinnitus distress; (b) increasing Jane’s self-efficacy in tinnitus coping would reduce the perceived loudness and functional and emotional impact of tinnitus.
Measures
Idiosyncratic tinnitus measures were developed collaboratively to measure targets of change that were most salient to Jane (Morley, 2018). Measures tracked perceived tinnitus loudness (henceforth referred to as ‘loudness’) tinnitus-related emotional distress (henceforth ‘annoying’ and ‘sad’), impact on valued activities (‘stops me doing’) and tinnitus-related sleep disturbance (‘sleep’). As such, the idiosyncratic measures reflected the core CBT principles underpinning CBT for tinnitus, i.e. that emotional and behavioural responses can change—typically via cognitive mediation—without the aversive stimulus changing in itself (McKenna et al., 2014). The content also reflected psychometrically validated tinnitus measures (e.g. Newman et al., 1996).
Questions used Jane’s language, and sought to track multiple targets for change, but without being burdensome to administer repeatedly. The measures used a ten-point scale with visual and verbal anchors (see Figure 1). Idiosyncratic tinnitus measure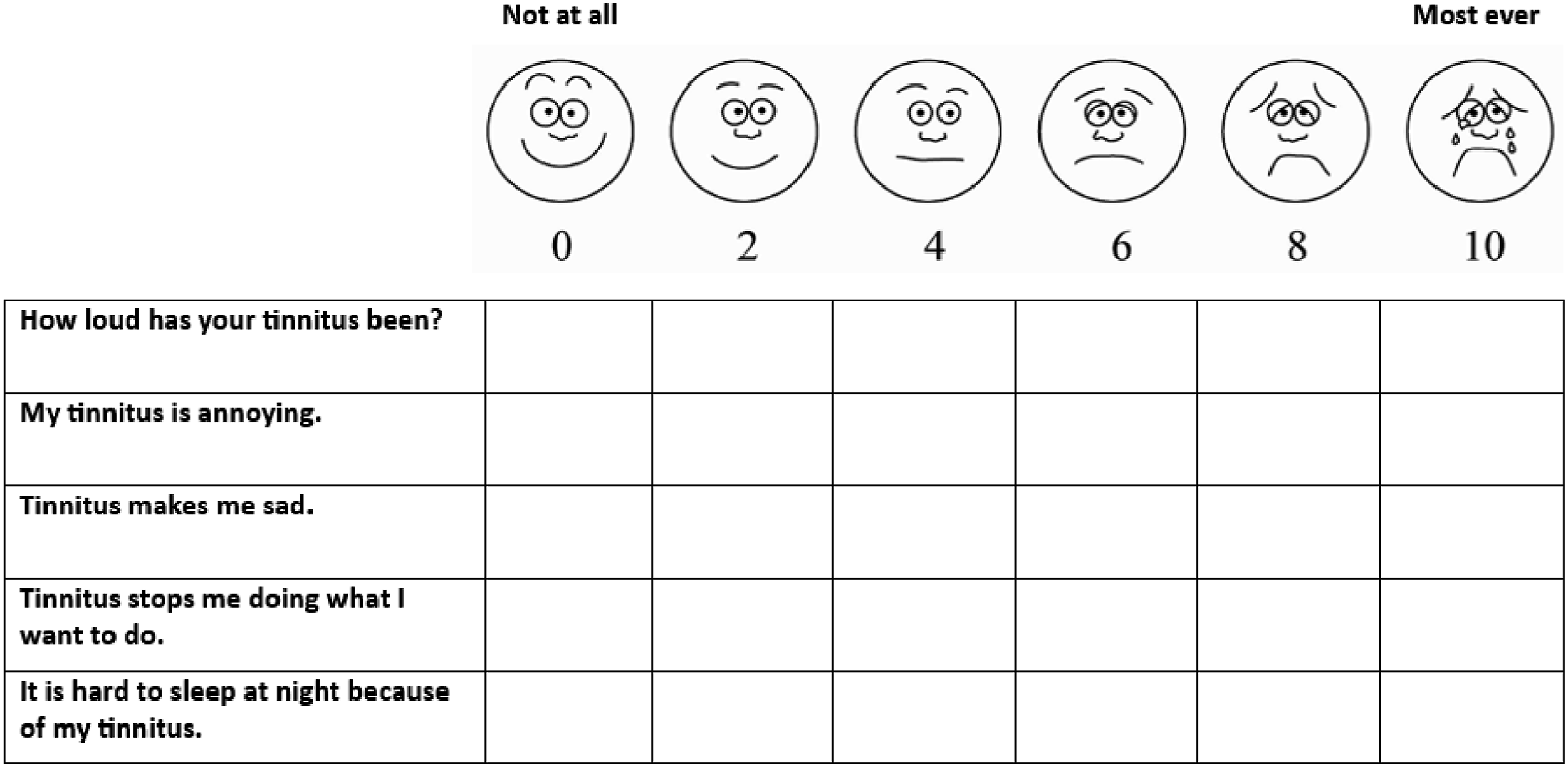
Design
A single case AB design was used, with A representing the pre-treatment baseline phase, and B representing the intervention phase. This is considered a quasi-experimental design, because treatment components are not manipulated systematically, nor is treatment withdrawn and reintroduced (Barlow et al., 2009).
Originally three baseline measures were planned. However, due to lack of baseline stability, this was extended to five (Barlow et al., 2009). This aligns with What Works Clearinghouse guidelines (Kratochwill et al., 2013) recommending a minimum of five data points per phase. Measures were administered at the start of weekly treatment sessions by the therapist and primary author. Three follow-up measures were planned, one, three and six months after the end of treatment.
Data Analysis
Data were analysed using the R package ‘SCED’ (Hussey, 2018). As single case data typically violate parametric assumptions, for each tinnitus measure non-parametric effect sizes were calculated: Ruscio’s A (Ruscio, 2008) and median difference between conditions. p values were calculated with non-parametric permutation tests. Ruscio’s A represents the probability that a score randomly selected from phase B is superior to a score randomly selected from phase A (P(B>A)) (Ruscio, 2008). Hedge’s g was calculated for illustrative purposes, although its parametric assumptions were violated. Bootstrapped 95% confidence intervals were calculated.
For each tinnitus score, baseline trends were examined via visual inspection (see Figure 7) and calculation of standardised beta linear regression coefficients (see Table 2). There was evidence of baseline trends for ‘annoying’, ‘sad’ and ‘stops me doing’. For ‘annoying’ and ‘sad’, trends indicated deterioration, while the ‘stops me doing’ trend indicated improvement. Baseline trends —particularly improvement-pose a threat to validity due to the potential confound of natural improvement (Barlow et al., 2009). However, due to ethical issues in delaying treatment (Morley, 2018), treatment commenced after five baseline measures. Baseline trends were not systematic across measures, and there was no evidence of baseline trend when the five tinnitus measures were combined: α = .944, standardised beta = .1 (see Table 2). However, results should be interpreted cautiously.
Case Conceptualization
Cognitive behavioural models of tinnitus are intrapersonal (e.g. McKenna et al., 2014), but usually focus less on interpersonal factors, which are particularly important to consider when working with people with LD (Jahoda et al., 2009). As such, case conceptualisation drew on McKenna et al. (2014) cognitive behavioural model of tinnitus distress, as well as Halldorsson et al. (2019) model of child anxiety which incorporates parental thoughts, feelings and behaviours.
A typical nighttime example of tinnitus distress was formulated (see Figure 2). In the example, Jane reported that she would often wake at 4.30am, and listen out for tinnitus with hypervigilance, worrying that it would be bad, upsetting and sleep-disrupting. This fuelled anxiety, and she subsequently noticed tinnitus. This pattern is consistent with research findings indicating significant associations between catastrophising, fear of tinnitus, increased attention toward tinnitus, and diminished quality of life (Cima et al., 2011). It also reflects research linking physiological arousal, stress appraisal (Heinecke et al., 2008) and emotional status (Mazurek et al., 2012) with tinnitus distress and sleep disturbance (Wallhäusser-Franke et al., 2013). Intrapersonal formulation of tinnitus distress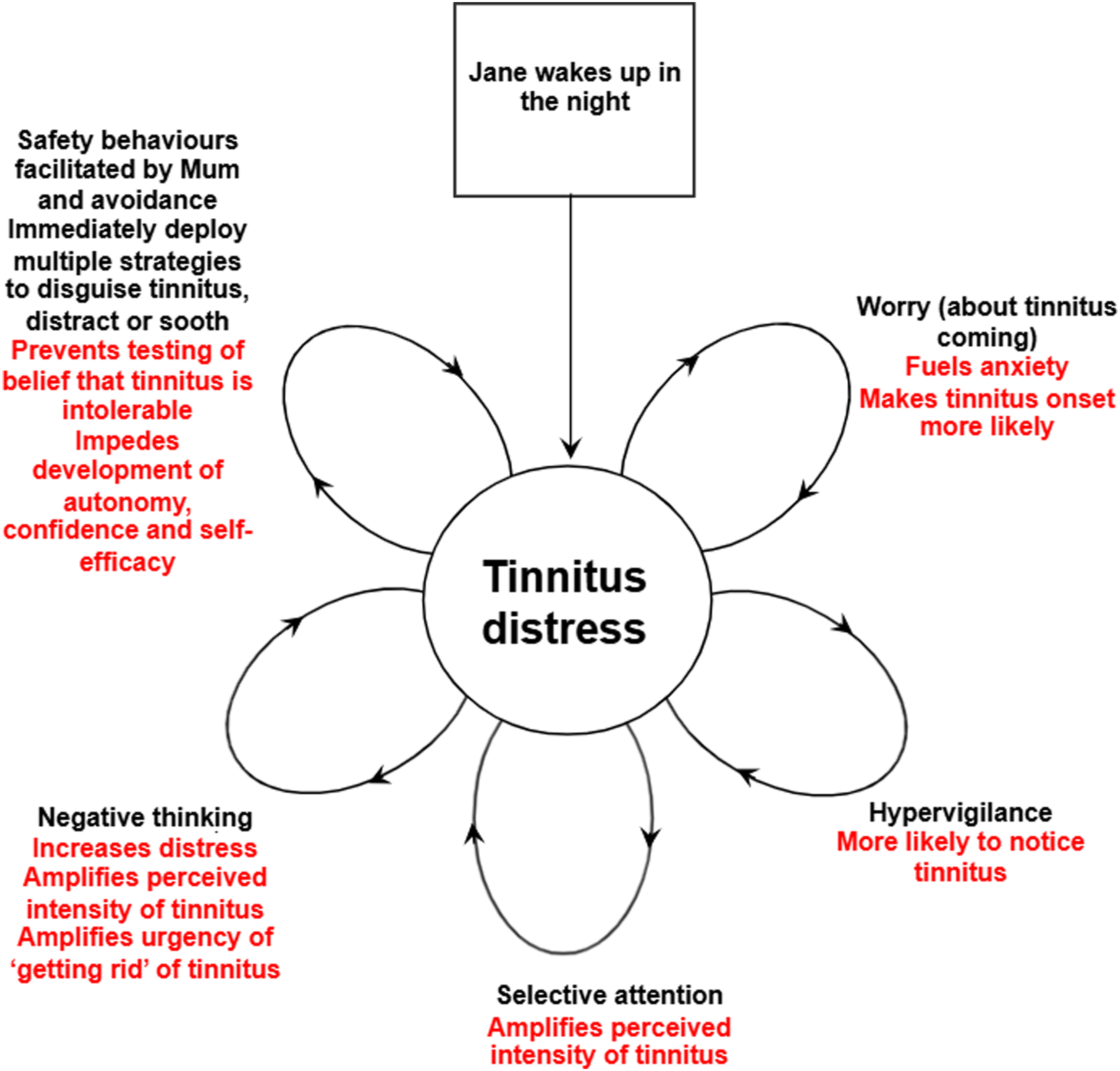
Further catastrophising ensued, including thoughts that tinnitus will impede sleep and college attendance, fuelling further arousal, less likelihood of sleeping, and emotional distress, including frustration and anxiety. At Liz’s instigation, Jane conducted multiple strategies driven by the shared belief, “we’ve got to get rid of tinnitus”, which inadvertently increased focus on tinnitus, reinforced and prevented the testing of beliefs that tinnitus is intolerable, and meant that next time Jane awoke, catastrophic predictions about tinnitus would ensue again, generating a vicious cycle (McKenna et al., 2014).
Drawing on Halldorsson et al. (2019) model of child anxiety, a side-by-side formulation was developed, conceptualising how Jane and Liz’s thoughts, feelings and behaviours interacted and maintained tinnitus distress (see Figure 3). When Liz heard Jane awake in the night, she felt sad about the thought of her daughter potentially being troubled by tinnitus, which “set alarm bells ringing”, provoking anxiety, a belief that “we’ve got to get rid of tinnitus”, and an urge to be with her daughter and instigate coping strategies. She would go to Jane’s room and initiate coping strategies, potentially spurring Jane’s worries that tinnitus is bad and that she cannot handle it alone, and therefore heightening Jane’s focus on tinnitus. Liz’s belief that “we’ve got to get rid of tinnitus” led her to cycle through multiple coping strategies, heightening Jane’s belief that she can’t get to sleep because of tinnitus, and fuelling distress. Jane’s distress further heightened Liz’s anxiety and desire to help, and spurred further attempted coping strategies, reinforcing Jane’s belief that tinnitus is intolerable, unfixable and she cannot face it alone. Interpersonal formulation of tinnitus distress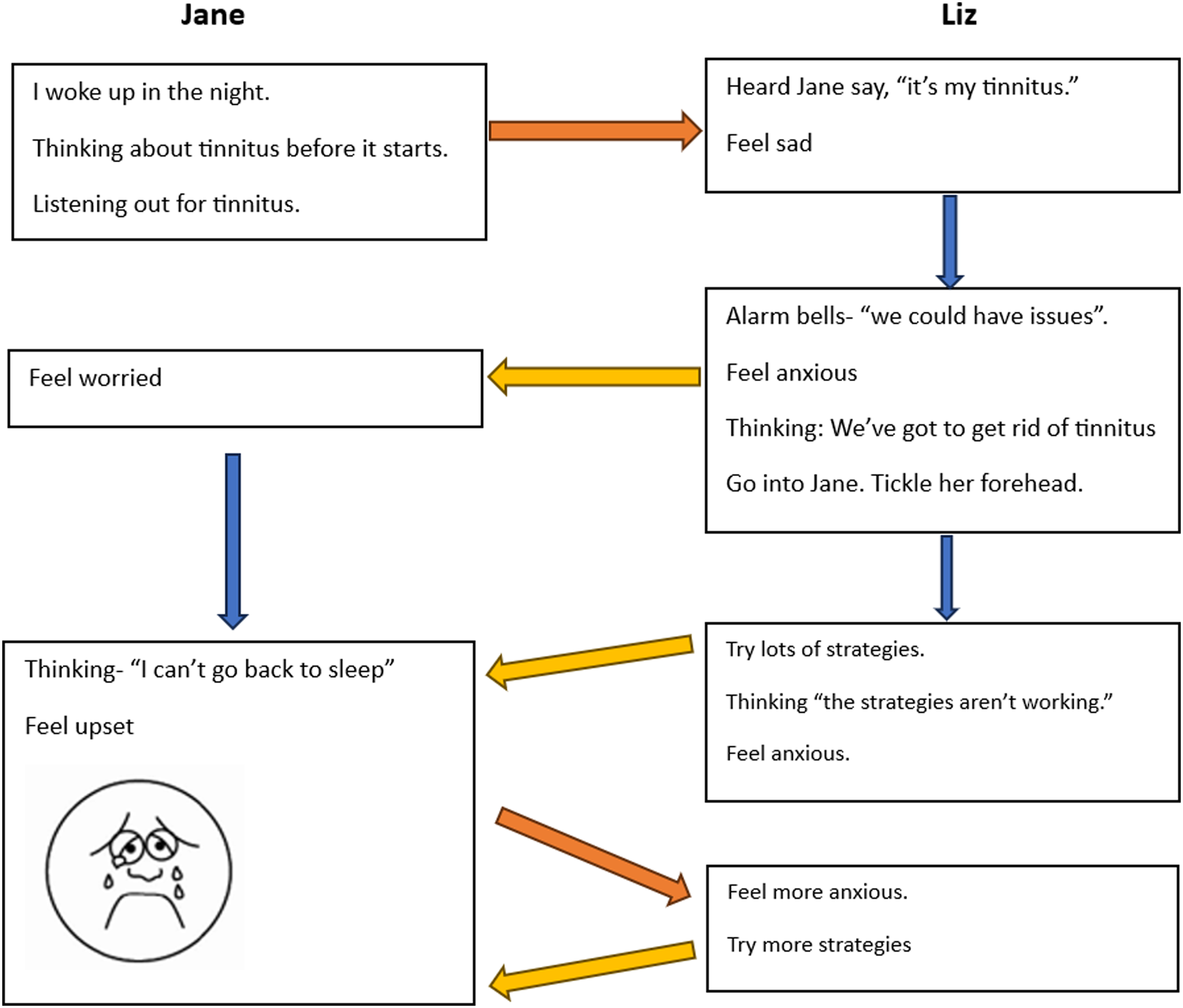
Course of Treatment and Assessment of Progress
Treatment Summary

Idiosyncratic measures were developed during an initial introductory meeting, then administered at the start of subsequent sessions. The first four sessions consisted of assessment. In session five-the first intervention session-a simplified vicious flower formulation was developed collaboratively (see Figure 4), identifying key maintenance mechanisms such as worry, hypervigilance, selective attention, negative thinking and safety-seeking behaviours. Liz recognised the possible role of her own anxiety about tinnitus in amplifying Jane’s anxiety, and resolved to stay calm if she heard Jane wake up in the night. The function of cycling through numerous ‘coping’ strategies was explored, pinpointing an underlying belief that “we’ve got to get rid of it”, which reinforced the sense that tinnitus could not be tolerated. Iterations of alternative perspectives were explored, moving from, “we’ve got to get rid of it”, to, “we’ve got to cope with it”, to, “I can cope with it”, to, “I can accept it”. Jane said that thinking, “I can accept/cope with it” would make her feel calmer than, “I’ve got to get rid of it”. Collaboratively developed vicious flower formulation. Black indicates behaviours or thoughts. Red indicates effects of thoughts or behaviours. Green indicates new alternative thoughts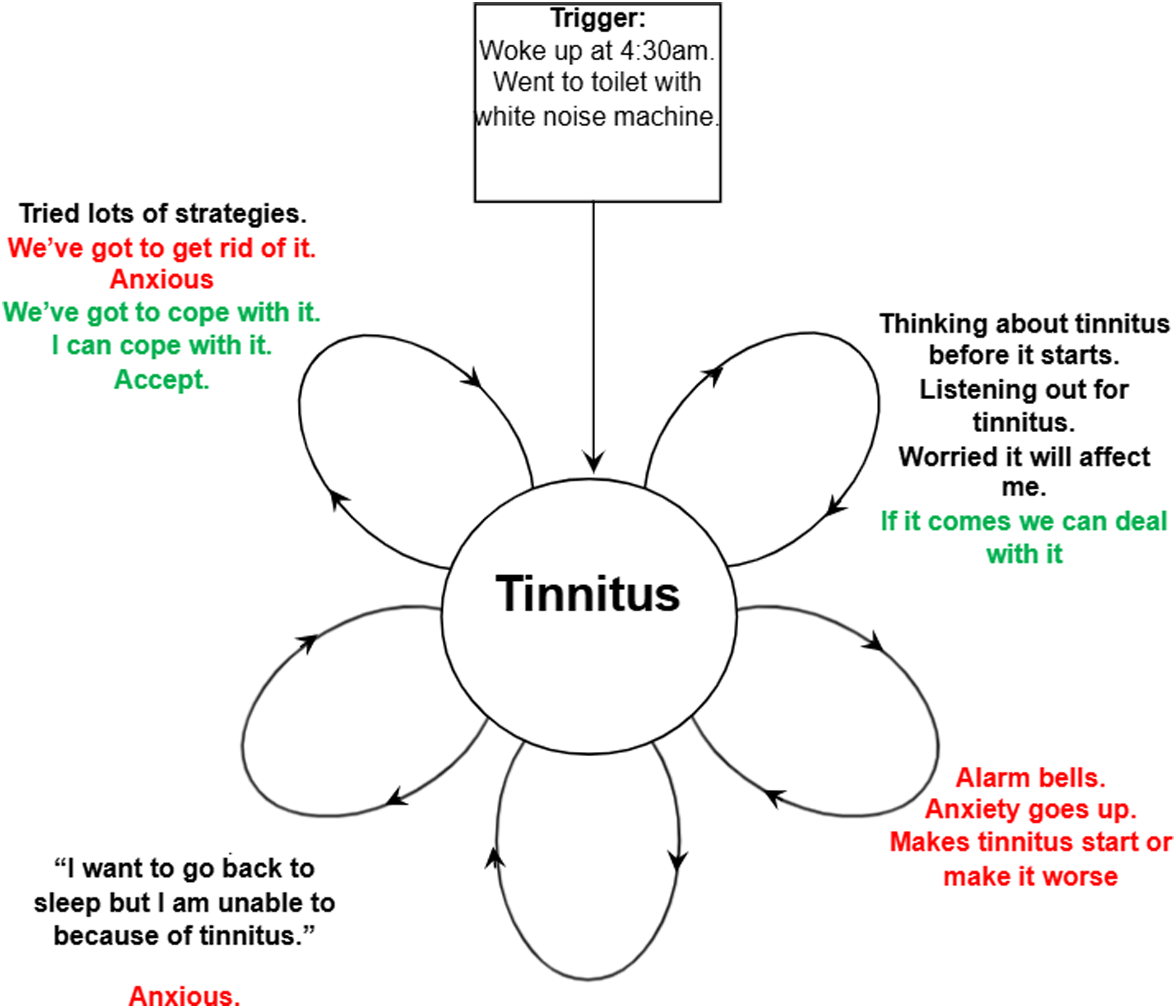
The following week, Jane and Liz described having implemented these changes in a similar situation. Liz said she recalled the formulation, thinking about “accepting” whatever comes, and conveying calm to Jane. Jane said she was not worrying about tinnitus, and that it did not start. The tinnitus measures dropped substantially. Re-visualising tinnitus to change its emotional meaning was introduced. Instead of viewing tinnitus as a horrible monster causing trouble and distress, Jane re-imagined tinnitus as the sound of a mongoose requesting food, as she had visited some mongooses that week (see Figure 5) or as the noise that Ant and Dec might hear in the jungle on the TV programme “I’m a celebrity, get me out of here”. Jane and Liz purchased several mongoose toys to facilitate re-imagining. The mongoose toy also served a sensory soothing function as Jane said their softness cultivated calm. Re-imagining tinnitus as a mongoose
In session seven, Jane said she had experienced tinnitus on two nights, possibly linked to hormone-related hot flushes. She said that although it was loud, it did not trouble her as much because she was thinking, “we can cope with this” rather than, “we’ve got to get rid of it”. In this session progressive muscle relaxation (PMR) was introduced. A recording and visual guide were provided to facilitate home practice.
Subsequent sessions focused on building Jane’s confidence and autonomy in using PMR, with Jane guiding in-session PMR practice. A side-by-side formulation was developed (see Figure 3) to conceptualise the circular causality (Cecchin, 1987) of anxiety, with Liz and Jane’s anxiety feeding into each other. A second side-by-side formulation (see Figure 6) was developed to underscore the difference when Liz resisted going to Jane’s room to soothe her, providing the opportunity to practise independent coping. Jane said she believed, “I’m OK I can do it by myself,” felt calm, and was able to implement strategies herself, leaving both Liz and Jane feeling happy and proud of Jane, and less worried about tinnitus. Interpersonal formulation supporting Jane’s autonomy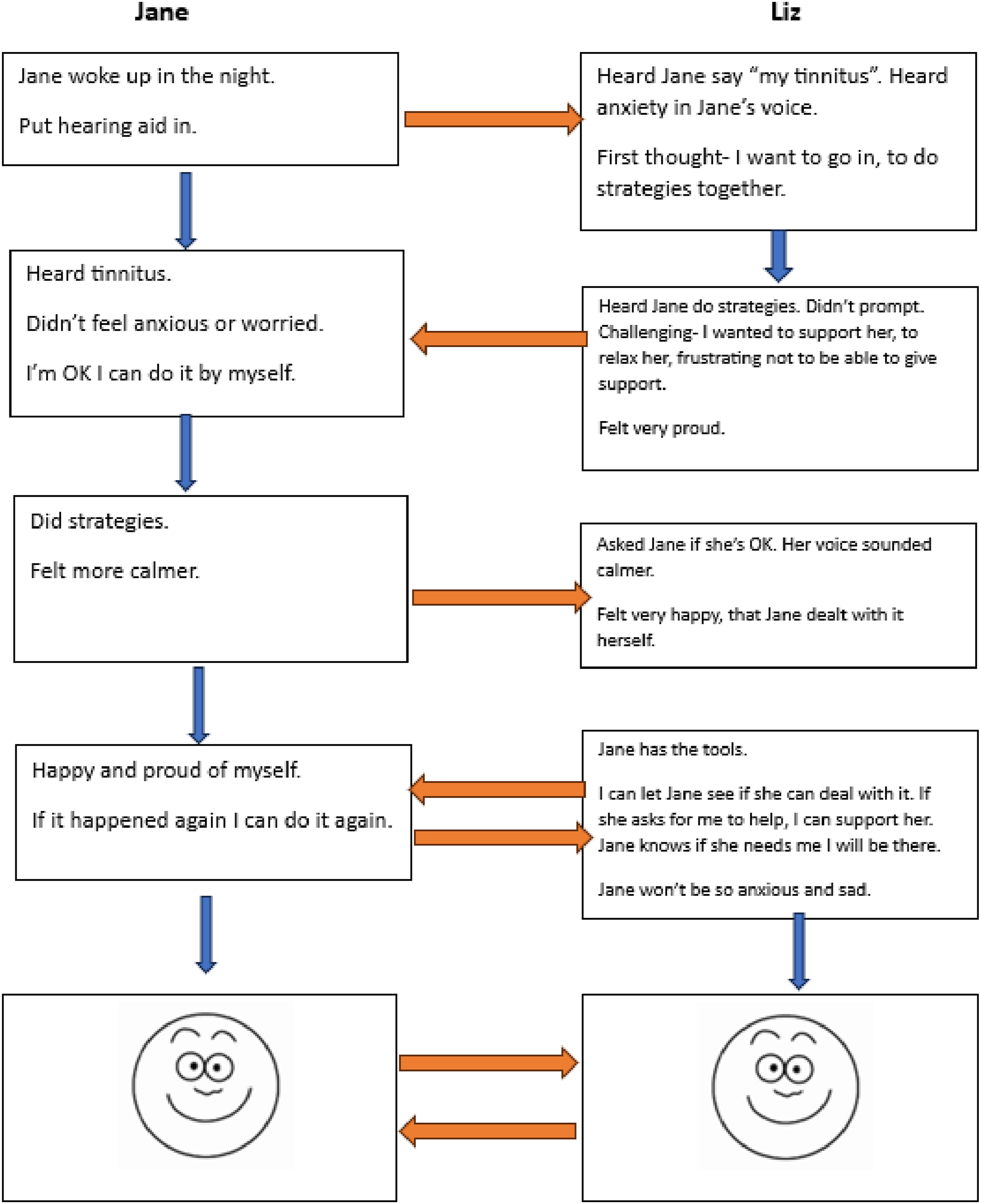
In session 10, Jane said hormone-related migraines had sparked tinnitus on the previous three days. However, she said her confidence in coping meant it did not bother her. In session 12, the therapist’s clinical supervisor (second author) attended the session to interview Jane and Liz about what they had learned during therapy. The supervisor, along with Jane’s father and brother, who also attended, served as outsider witnesses to Jane’s progress (White, 1998). Jane had prepared a visual presentation of the things she had learned.
Visual inspection indicated clear evidence of improvement in all tinnitus scores after intervention (see Figure 7). Data for each tinnitus measure, and composite measure. Dotted vertical lines indicate start of intervention. Horizontal dotted line indicates median. Solid lines indicate regression lines showing within-phase trends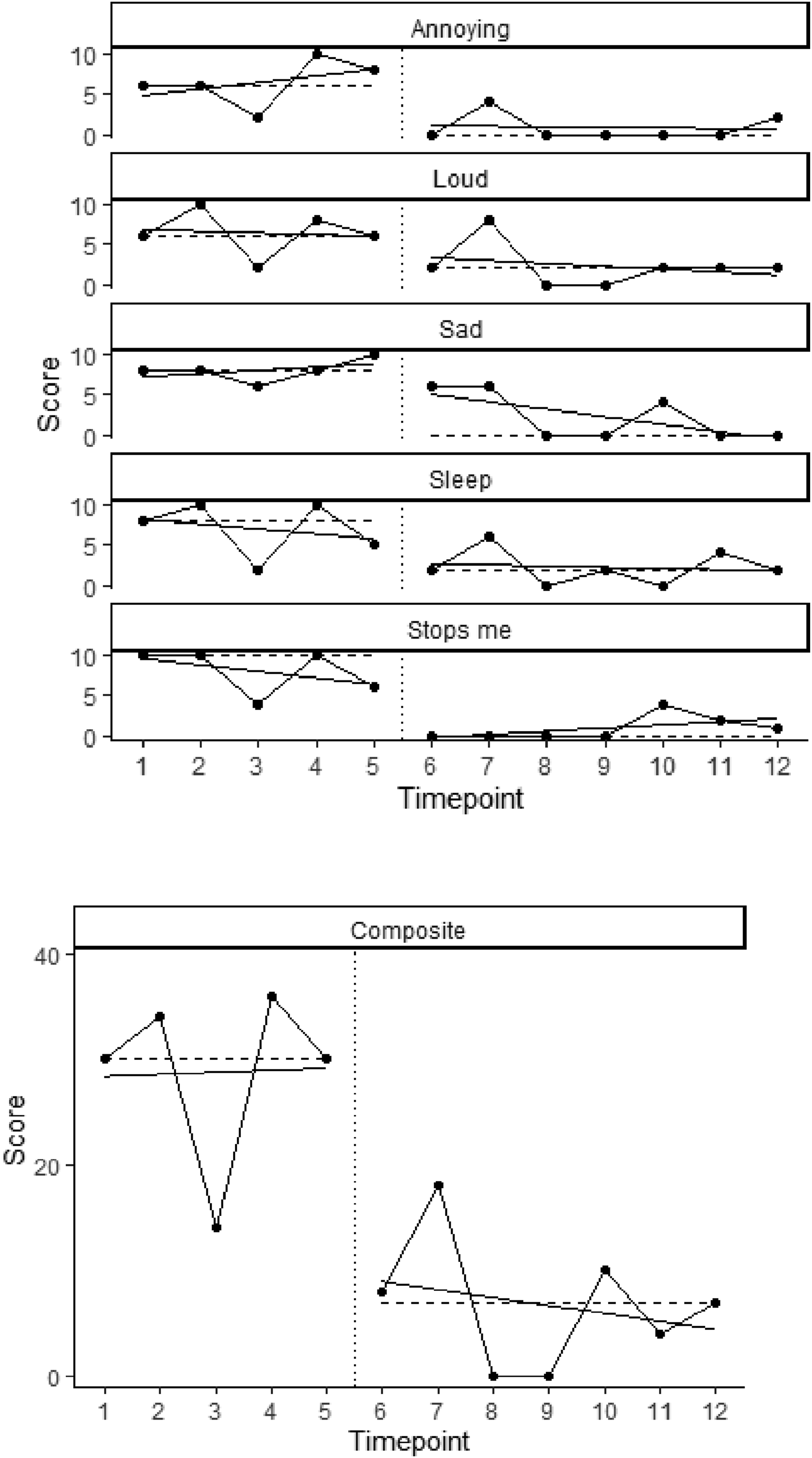
Results of SCED Analyses
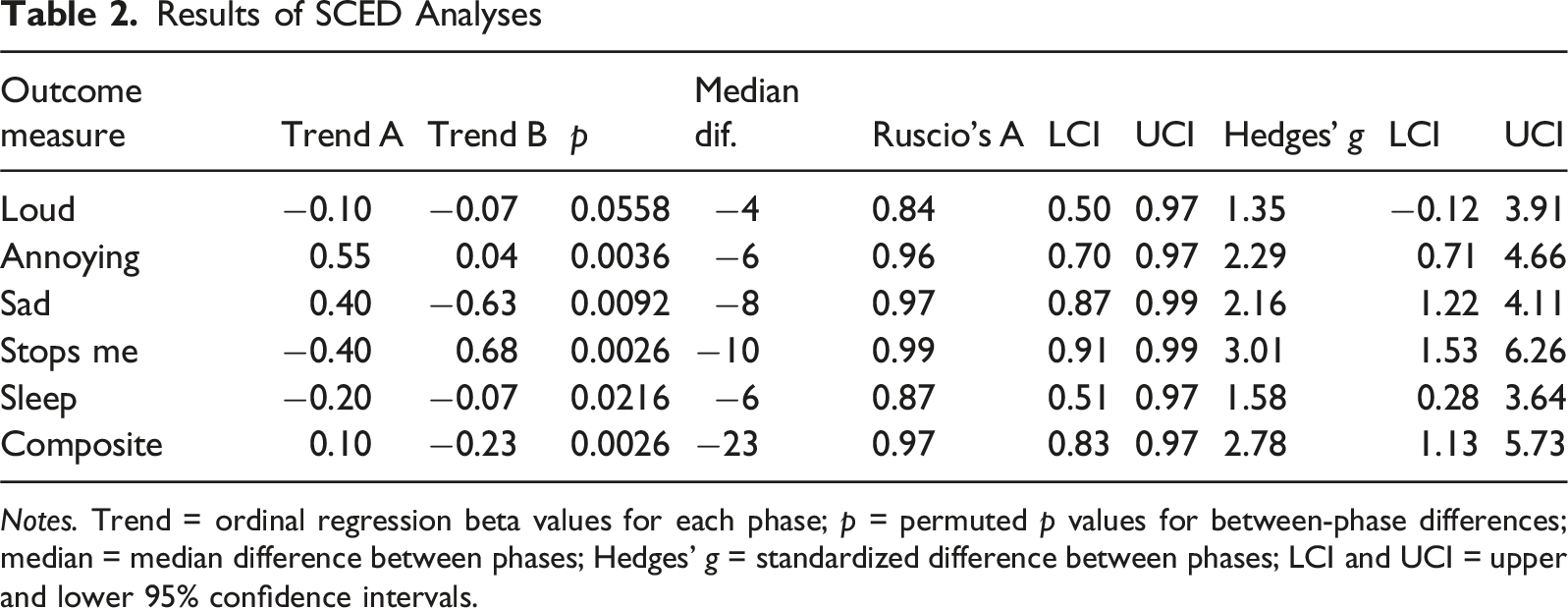
Notes. Trend = ordinal regression beta values for each phase; p = permuted p values for between-phase differences; median = median difference between phases; Hedges’ g = standardized difference between phases; LCI and UCI = upper and lower 95% confidence intervals.
Qualitative feedback from Jane and her family also indicated perceptions of positive change, which were attributed to the therapeutic intervention. Responding to questions guided by Elliott (2002) Client Change Interview Schedule, Jane and Liz reported feeling less anxious about tinnitus, and more confident in Jane’s ability to cope with tinnitus. Jane’s brother said he had noticed a generalised increase in Jane’s confidence, noting that Jane is no longer “just asking for Mum” but is instead “taking a moment to think… then realises she can do it herself”. Jane reported feeling more confident generally, particularly at college. Jane and Liz said these changes would not have happened naturally without therapy.
Jane said the most helpful intervention was reimagining tinnitus as a mongoose noise, while Liz noted a particularly helpful aspect was visual aids, such as images for PMR. Liz also said she is responding to tinnitus differently, namely worrying less and supporting Jane’s independent coping.
Complicating Factors
The quasi-experimental single case AB design meant all threats to validity could not be controlled. Initiation of the intervention coincided with Jane’s college term ending. Although the final measure indicated gains were maintained two weeks after college restarted, a single measure is inadequate to entirely discount the possibility that some improvement was related to a reduction in stress due to not attending college during the end of term holidays.
Tinnitus was also influenced by hormonal changes, to which Jane and Liz attributed tinnitus spikes in sessions four, seven and ten, notably separated by one month intervals. However, the length of the B phase (2.5 months) controlled for this to some extent-composite tinnitus scores in session seven and ten did not surpass the baseline median, while qualitative feedback emphasised therapy processes over biological processes.
Some tinnitus measures did not display a stable baseline. The ‘stops me doing’ measure indicated an improvement trend at baseline, which, taken in isolation, would preclude ruling out natural recovery. However, this measure showed a substantial, stable post-intervention improvement, with the largest effect size, and also aligned with the improvement seen on other scores, suggesting natural recovery was not accountable. Natural recovery was also ruled out in qualitative feedback. However, future studies could include a longer baseline.
It is known that people with LD exhibit greater social desirability bias in questionnaire responses than people without LDs (Langdon et al., 2010). Although the baseline controlled for this in isolation, measures were administered by the therapist who was not blind to the phase and expected treatment effects. In a more rigorous study, measures would be administered by a blinded researcher.
Measures were limited to five questions to reduce client burden. However, it would have been useful to measure cognitive change, to assess whether behavioural and emotional changes were cognitively mediated, or occurred independent of cognitive changes. Given parental thoughts, feelings and behaviours were a treatment target, and potentially causal factors in reduced tinnitus distress, future studies should measure these.
Access and Barriers to Care
Several adaptations were made to overcome barriers to care and facilitate access and engagement. Firstly, Jane’s fatigue and mobility issues meant she preferred sessions to be held online on Microsoft Teams. Visual aids were used to facilitate Jane’s understanding, recall and use of strategies, such as an image based PMR guide for reference, and the use of soft mongoose toys to aid the reimagining of tinnitus as a mongoose sound. Scaffolding was also used to support Jane’s learning of strategies. This consisted of repeated in-session practice initially guided by the therapist, then by Jane, and home practice initially supported by Liz, then led by Jane with prompts from Liz, then led by Jane without prompts.
In-session communication between Jane and the therapist was initially supported by Liz. However, it was hypothesised that Jane could communicate more independently, with less support from Liz. In order to give Jane time to autonomously think and communicate responses, Jane and Liz decided to Sellotape Liz’ mouth shut in latter sessions, which playfully empowered Jane to communicate more independently.
Follow-Up
Three follow-up measures were planned, at one month, three months and six months after the end of treatment. However, these were not completed as planned. The questionnaires were not returned, but informal feedback indicated progress was mostly maintained, with some challenges along the way.
Treatment Implications of the Case
This quasi-experimental single case study aimed to test the hypothesis that CBT would reduce tinnitus distress in a person with an LD. Quantitative and qualitative data supported this hypothesis. There were large, statistically significant reductions in self-reported tinnitus-related annoyance, sadness and sleep disturbance, and in tinnitus-related interference with desired activities. There was a non-significant trend decline in perceived loudness, reflecting meta-analytic findings (Andersson & Lyttkens, 1999) indicating psychological therapies have larger effects on tinnitus distress than on perceived loudness.
This is the first case study reporting adapted CBT treatment of tinnitus distress in a person with an LD, and as such offers valuable clinical implications. Although the AB design and integrated treatment package precludes strong causal inferences about specific active ingredients, session-by-session change and qualitative feedback support the hypothesis. The largest improvement occurred following session five, the first treatment session, which involved collaborative formulation of the role of worry, attention and Liz’s anxiety in Jane’s tinnitus distress. In the subsequent sessions Liz and Jane described the importance of Liz’s calmer approach in facilitating reduced tinnitus distress. Incorporating parental thoughts, feelings and behaviours as a treatment target was a novel aspect of this intervention compared with standard CBT for tinnitus. Liz noted that she was responding to Jane’s tinnitus differently—with less worry and anxiety—and began to support Jane’s self-efficacy in coping with tinnitus. Qualitative feedback indicated Jane perceived an increase in self-confidence that generalised beyond coping with tinnitus, a change that was also identified by other family members. The results offer tentative support to Jahoda et al. (2009) suggestion that involving carers in CBT work to support a service user’s autonomy and self-efficacy is particularly important in an LD context. A side-by side formulation (Halldorsson et al., 2019) may be a particularly useful method for developing a shared rationale for building autonomy. This is particularly important as initial steps towards autonomy and self-efficacy—the parent/carer stepping back—may appear aversive without a solid, shared rationale.
There was also a large improvement following session seven. Although this is partially attributable to hormonal change, which had seemingly driven a tinnitus rebound between session six and seven, Jane also attributed it to reframing tinnitus as a mongoose sound, with a mongoose toy used to facilitate this. Post-treatment, Jane highlighted this as the most helpful part of the intervention for her. Imagery interventions are a core component of CBT for tinnitus, although no dismantling studies have been conducted to test specific effects. It may have been particularly impactful in this case as it comprised both simplified cognitive restructuring and sensory soothing. The intervention seemingly altering cognitions about the perceived awfulness and intolerable nature of tinnitus and altered its emotional valence. This underscores the value of combining imagery interventions with tangible visuo-sensual aids for people with LD. Future research could use an ABACA design to examine the specificity of these interventions’ effects.
Recommendations to Clinicians and Students
This case study provides insights applicable to CBT treatment for tinnitus for people with LD, as well as for CBT work with people with LD more broadly.
Involving parents/carers in CBT for people with LD can be valuable in scaffolding skills development, as well as supporting autonomy and self-efficacy by stepping back (Jahoda et al., 2009). In the present case study, Liz’ role moved between the facilitator, co-clinician and co-client roles identified by Stallard, 2009. Liz’ role as a co-clinician, along with visual adaptations and repeated in-session practice, supported Jane’s understanding and use of strategies such as PMR. However, it was Liz’ role as a co-client, and the use of side-by-side formulations (Halldorsson et al., 2019), that helped conceptualise and alter interpersonal feedback loops contributing to the maintenance of anxiety and tinnitus. The conceptualisation and breaking of these feedback loops supported Jane’s development of autonomy and self-efficacy in her use of specific strategies. It also supported Liz’ understanding that stepping back to support self-efficacy was different to not caring. As such, it is recommended that coping and relaxation strategies are conceptualised as serving a dual function: both direct symptom alleviation, and the building of autonomy and self-efficacy. Using side-by-side formulations, and involving parents/carers as co-clients, may be crucial to the second function.
Using tangible visuo-sensual aids can support the use of imagery interventions for people with learning disabilities. These can also serve a dual function, providing both sensory soothing, as well as serving as anchors to recall and facilitate the use of more abstract imaginal strategies.
Developing idiosyncratic measures derived from validated questionnaires, and aligned with the service user’s goals and treatment foci, can provide a more user-friendly way of tracking progress. This may be particularly valuable when working with people with LD, as this minimises the burden presented by administration of longer psychometric questionnaires. However, it is also recommended that further work is carried out to develop a standardised measure of distress related to tinnitus for use with people with LD to compliment such bespoke and idiosyncratic measures of subjective distress.
Finally, it should be noted that, according to Jane’s mother, an earlier opportunity to receive treatment for tinnitus distress seven years earlier was missed when a mainstream child and adolescent mental health service declined to provide treatment due to Jane’s learning disability. Although the precise circumstances around that situation are unclear, it underscores the importance of training clinicians in adapting evidence-based interventions for people with learning disabilities and neurodiversity more broadly, to ensure that services are as accessible as possible (Rossiter & Holmes, 2013).
Footnotes
Acknowledgments
We would like to thank Jane and Liz (pseudonyms) for their hard work and engagement during treatment, and for their permission to publish this case study.
Ethical Considerations
Ethical approval was not required for this case study, as the intervention formed part of routine clinical practice.
Consent to Participate
Written informed consent was obtained from the patient and mother, including consent for publication. Identifying details have been altered to protect anonymity.
Author Contributions
JL conducted the clinical work described in this case study, which was closely supervised by HF, including the review of a session recording. JL conducted data analysis and visualisation, and wrote the first draft of the manuscript, which was reviewed by HF, who suggested revisions.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The clinical data that support the findings of this study are available from the corresponding author, upon reasonable request.
