Abstract
While regular physical-activity (PA) is beneficial, multimorbid individuals at increased dementia risk may exhibit reduced PA levels. Thus, a more comprehensive understanding of mediating factors responsible for inactivity in this population is needed. This study investigated the impact of a multimodal intervention on PA changes at 24-month follow-up and associated mediating factors among community-dwelling patients aged 60-77, with increased dementia risk determined by the CAIDE Dementia Risk Score. Of 1030 participants recruited, 819 completed the assessment. Thus, a generalized estimating equations model initially assessed differences in PA over 24 months, followed by a tree analysis identifying mediating factors influencing PA changes post-intervention. While no significant effect on regular PA was found during the follow-up (P = .674), subgroup analysis revealed improved self-efficacy (P = .000) associated with increased engagement in PA. Incorporating self-efficacy elements into future strategies is crucial for promoting PA among individuals with multimorbidity and at increased dementia risk.
Significance Statement
This manuscript uses a unique methodology to study factors contributing to inactivity in older adults with multimorbidity and at increased dementia risk. Our approach identifies specific mediating factors including self-efficacy and subgroups within the population with shared characteristics related to desired health behaviour (physical activity). This information can help target interventions more effectively, improving physical activity promotion, guiding policies, and resource allocation in public health.
Introduction
As the world’s population ages, the prevalence of dementia is increasing. 1 It is estimated that there will be a global increment of 57.4 million cases of dementia in 2019 to 152.8 million cases in 2050. 2 Indeed, the growth in the number of persons living with dementia represents a primary worldwide challenge because of its physical, psychological and economic repercussions. 3 Together with its global prevalence and impact, the absence of a cure and treatment for dementia highlights the relevance of prevention as an effective way to reduce dementia implications. 1 Therefore, currently, both scientific research and global health strategies have focused on dementia prevention efforts by addressing modifiable risk factors, including physical inactivity.4,5 Approximately 40% of dementia cases worldwide can be linked to modifiable risk factors. 6 Likewise, multimorbidity has a robust association with mild cognitive impairment and subsequent dementia. 7 Particularly, older adults with cardiovascular, sensory impairment and neuropsychiatric multimorbidity are affected. 8 Thus, by recognizing and targeting modifiable and associated risk factors for dementia, key elements are highlighted for primary prevention strategies and dementia incidence reduction. 4
Multimodal interventions that target modifiable risk factors show promise in preventing cognitive decline. Notable European studies such as The Finnish Geriatric Intervention Study to Prevent Cognitive Impairment and Disability (FINGER), 9 the French Multimodal Alzheimer Preventive Trial (MAPT), 10 and Dutch Prevention of Dementia by Intensive Vascular Care (PreDIVA) 11 have demonstrated the efficacy of such approaches. The FINGER Trial, 9 lasting two years, displayed significant cognitive improvements among at-risk older adults through lifestyle interventions. Similarly, the 3-year MAPT Trial 10 displayed positive cognitive effects despite not meeting its primary goal. Lastly, the 6-year PreDIVA Study 11 revealed a reduction in dementia incidence among individuals with untreated hypertension who adhered to treatment. These trials highlight the potential of targeting modifiable risk factors to reduce dementia risk.
Within these interventions, physical activity (PA) is consistently included as a crucial component, with the aim of mitigating various dementia risk factors, promoting brain health and enhancing overall well-being. 4 Long-term engagement in PA has been linked to cognitive benefits, improved physical functioning, and mental health, reducing dementia risk and delaying dementia progression.12,13 Moreover, a strong correlation exists between PA and reduced non-communicable diseases (NCDs) and decreased mortality risk linked to multimorbidity. 14 In order to achieve those health benefits, the World Health Organization (WHO) recommends a minimum of 150 min/per week of moderate-intensity aerobic PA for older adults. 15
Despite PA benefits, the effectiveness of PA in delaying cognitive decline is not yet fully established, 4 especially considering the challenges of engaging and maintaining adherence among older adults.16,17 Evidence shows that in Germany, less than 150 minutes of PA per week is reported by 65% of individuals aged 65 or older, indicating a shortfall in meeting WHO recommendation. 18 Similarly, adherence to WHO PA recommendations was found to be less than a third among older adults with multimorbidity. 19 Such a considerable absence of adherence to recommended PA may contribute to worsening multimorbidity or other adverse health outcomes. 19
Given the extensive incidence of low PA levels in older adults with multimorbidity and increased dementia risk, understanding the mediating factors influencing PA engagement within multimodal interventions is essential. Additionally, investigating the impact of multimodal interventions on PA changes can provide valuable insights into their effectiveness. 20 Potential mediating factors influencing engagement in PA interventions among older adults with multimorbidity and at increased dementia risk, as proposed by the socioecological model, encompass both individual and environmental factors.21,22 Notably, recurring barriers often hinder PA participation among people with multimorbidity, including physical barriers (e.g. pain and fatigue), psychological constraints (depression, anxiety, fear of falling, extrinsic motivation, feelings of isolation, knowledge about the condition), and financial limitations. 20 While previous literature provide some evidence, regarding mediating factors for regular PA in persons with multimorbidity, prior research presents a limitation by studying PA mediating factors without considering possible high-risk subgroups. 23 Decision tree analysis plays an essential role in public health research by analysing the intricate interactions across outcomes and mediating factors, identifying high-risk subgroups to implement preventive measures and interventions. 24 Thus, decision trees enable the identification of distinct subgroups within the population that have common and distinguishable characteristics, either barriers or facilitators (mediating factors), to the desired health-related behaviour. 19 Therefore, this methodology holds great significance in targeting interventions towards specific groups and fostering the adoption of healthy behaviours, like PA; facilitating as well the efficient prediction, and design of population-based health promotion interventions. 24 Over the past years, decision tree analysis has been applied in various public health settings with different populations. 25 However, to our knowledge, limited research has specifically explored the application of decision trees aiming to understand mediating factors for PA among individuals with multimorbidity and at increased dementia risk. 26
Our primary aim is to investigate the impact of one multimodal intervention, the AgeWell study, on PA behaviour at 24-month follow-up, aiming to elucidate changes in PA after participation. Additionally, we aim to integrate decision tree analysis to understand the mediating factors influencing changes in PA at the 24-month follow-up among older adults with multimorbidity and increased dementia risk, identifying as well high-risk subgroups. These objectives will not only provide significant insights into the challenges and opportunities for promoting PA in older adults with multimorbidity and dementia risk but also offer a solid foundation for the design of future interventions and public health policies targeting this vulnerable demographic group.
Methods
Study Design
The AgeWell.de study is the first cluster-randomized, controlled trial in Germany to evaluate the effectiveness of a multicomponent intervention aimed at preventing cognitive decline in older adults with multimorbidity and at increased dementia risk. 27 The intervention for the experimental group encompassed a diverse range of content, including PA enhancement, which consisted of a standardized training program with home exercises (strengthening and flexibility/balance exercises) to be performed twice a week. Additionally, individualized goals for aerobic exercise were set, targeting 3 to 5 times per week. Meanwhile, the control group received general practitioner treatment as usual and general health advice covering the components of the intervention. The primary outcome measure was cognitive function, with secondary outcomes including mental and physical health assessments. The AgeWell.de trial is registered in the German Clinical Trials Register (DRKS; trial identifier: DRKS00013555).
Participants
The study included community-dwelling patients aged between 60 and 77 years old and at increased risk of dementia, as determined by the CAIDE Dementia Risk Score (Cardiovascular Risk Factors, Aging, and Incidence of Dementia). 28 Participants were included in the study based on a CAIDE Dementia Risk Score of ≥9. Furthermore, the prediction of dementia risk was determined using a sensitivity of .77 and a specificity of .63 at a cut-off point of ≥9. 28 The CAIDE assessment comprises various factors, including age, education, gender, blood pressure, body mass index, total cholesterol, and physical activity. This approach ensured that individuals already diagnosed with dementia or mild cognitive impairment at the study’s outset were not included, as the CAIDE Dementia Risk Score was specifically developed to assess dementia risk in individuals without clinical dementia or mild cognitive impairment at the time of evaluation. Eligible participants for AgeWell.de were screened at general practitioner (GP) practices. Exclusion criteria encompassed the diagnosis or suspicion of dementia by GP, health conditions that could impede safe participation in the intervention as determined by GP, significant loss of vision, hearing, or insufficient ability to speak or read German, severe mobility impairment and concurrent participation in any other intervention trial. For additional information regarding the diagnostic criteria and procedures employed in this study, readers are encouraged to consult the AgeWell study protocol, 29 which provides a comprehensive overview of the methodology and assessment procedures.
Between June 2018 and October 2019, enrolled GP practices recruited eligible participants (n = 1030) from five study sites. Among them, n = 487 participants were randomized to the intervention group, while n = 543 participants were randomized to the control group. For the intention-to-treat analysis, n = 819 (79.5%) participants (intervention/control: n = 378/441) completed the 24-month assessment between July 2020 and January 2022. Dropout rates were n = 109 (22.4%) in the intervention group and n = 102 (18.8%) in the control group. Due to the COVID-19 pandemic and associated restrictions on personal contact, there were delays in the follow-up assessments, resulting in a mean duration of M = 25.6 months (SD: 2.8) between the baseline and follow-up interviews. The participant flow is illustrated in detail in Figure 1. Participant flowchart for random assignment in the AgeWell.de study.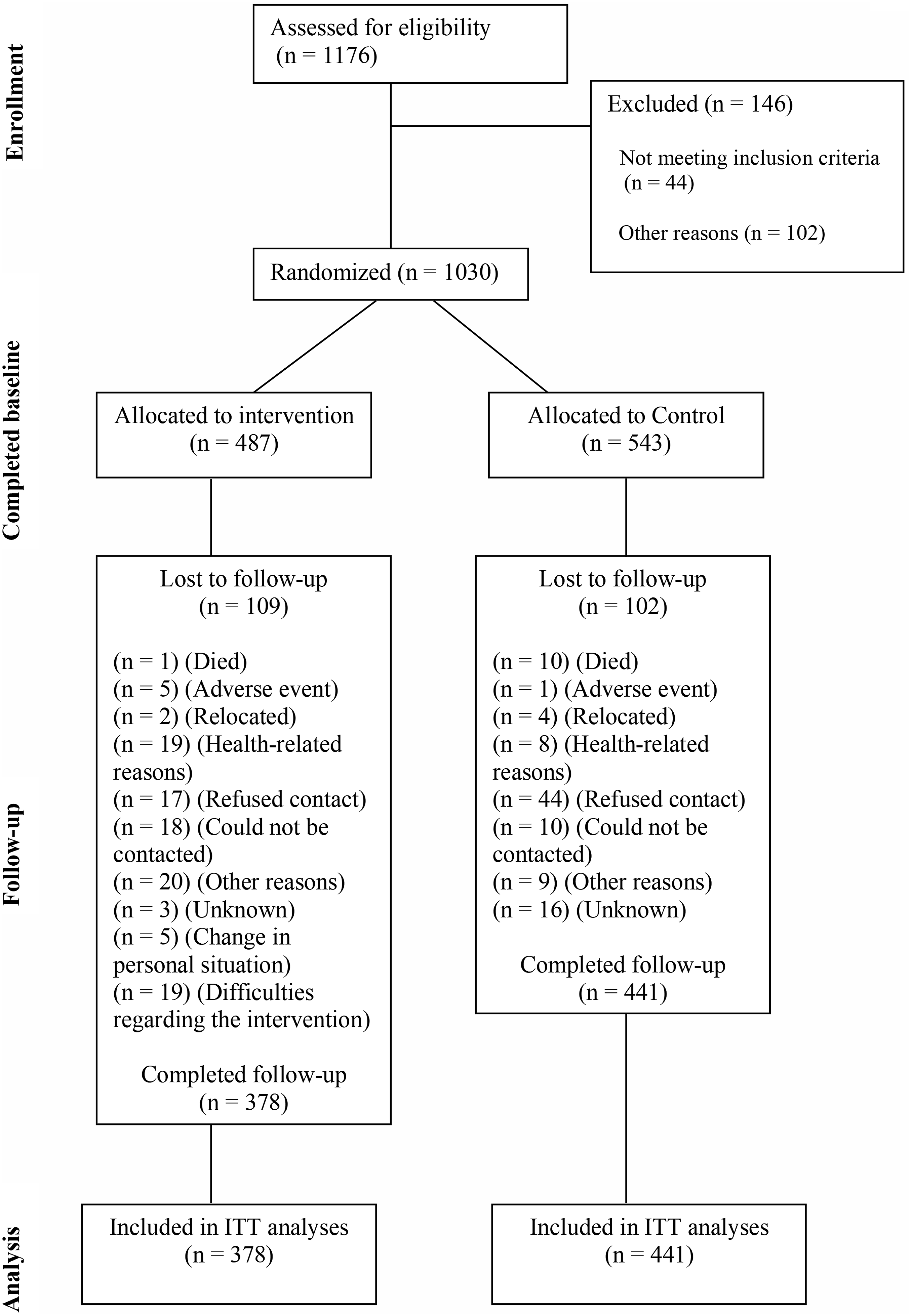
Data Collection
Data collection consisted of self-reported, structured face-to-face interviews and standardized questionnaires implemented at baseline and follow-up by GPs. The different relevant study variables and measurement tools used are presented below.
Dependent Variable
We administrated a self-developed questionnaire adapted from Lippke et al. 30 to evaluate “regular PA”. Participants were inquired about their recent participation in regular PA (≥2 days per week for 30 minutes), and their responses were recorded as a dichotomous variable yes or no. This reference value (regular PA = ≥2 days per week for 30 minutes) was chosen as a benchmark, given that regular weekly aerobic PA is linked to significant benefits on several health outcomes. 15
Taking into account that one of our aims was to identify factors associated with changes in PA engagement at follow-up, the variable “regular PA engagement” was transformed in four PA states (changes): (1) Physically active at baseline and follow-up; (2) Physically active at baseline, became inactive at follow-up; (3) Physically inactive at baseline, became regularly active at follow-up; and (4) Absence of regular PA both at baseline and follow-up.
Independent Variables
GPs provided sociodemographic (age, sex, living with a partner, education) and participant’s medical conditions information. Other factors were measured through questionnaires, which included the following variables: Cognitive status (Montreal Cognitive Assessment (MoCA)); 31 Depressive symptoms (Geriatric Depression Scale (GDS)); 32 Performance in activities of daily living (Barthel-Index); 33 and Health-related quality of life (EQ-5D-5 L). 34 In addition, participant’s health behaviours, such as alcohol consumption per day (g/day), were assessed. Participants were also asked about their current smoking status, with response options of yes or no.
Furthermore, participants self-efficacy for PA was evaluated using the health-specific self-efficacy scale proposed by Schwarzer and Renner, 35 which assessed how confident they felt to be physically active when: they were worried and had a problem, when they felt sad, tense, tired, and busy. The available response choices were (1) Very uncertain; (2) Rather uncertain; (3) Almost certain; and (5) very certain.
Social support measurements were obtained using the Lubben Social Network Scale/LSNS-6. Finally, the living area variable was examined and categorized into four classes based on population density: small urban area, with a population between 50,000 and 100,000; medium-sized urban area, with a population between 100,000 and 250,000; metropolitan urban area, with a population between 250,000 and 1.5 million; and large metropolitan urban areas, with a population above 1.5 million. 36
In order to identify whether there had been changes after the intervention, quantitative and qualitative independent variables were transformed into new variables. Quantitative variables (cognitive status, depression, social isolation, degree of independence, quality of life, alcohol consumption, and self-efficacy for PA) were transformed by computing the post-pre score difference. As for the qualitative variables with dichotomous yes/no responses, they were transformed into variables representing four states. For instance, the variable mobility difficulties was categorized into these four states: (1) Mobility difficulties at baseline, mobility difficulties at follow-up; (2) Mobility difficulties at baseline, no mobility difficulties at follow-up; (3) No mobility difficulties at baseline, mobility difficulties at follow-up; and (4) No mobility difficulties at baseline, no mobility difficulties at follow-up. The same transformation was applied to the variables smoker and GPs diagnoses (type 2 diabetes, hypertension, coronary heart disease, myocardial infarction, visual and hearing difficulties). Conversely, variables such as sex, age, living with a partner, educational level, and living area remained unchanged and were utilized in their baseline form.
Statistical Data Analysis
Descriptive statistics were used for the baseline characteristics of participants. Moreover, to assess between groups differences in PA engagement outcome at 24 months follow-up, a generalized estimating equations model was performed from a repeated measures binary logistic model. Finally, a decision tree analysis was conducted to identify mediating factors associated with changes in PA state after the intervention. Using a decision tree model, the probability of different variables in determining changes in regular PA engagement was estimated. This process allowed us to prioritize those factors that could be addressed to promote changes in regular PA practice (as shown in Figure 2). Statistical tests such as Pearson’s chi-square identified significant differences between subgroups, with a P-value < .05 considered significant. Analysis was done using IBM Statistical Package and Services Solutions (SPSS) version 25 (IBM Corp, Armonk, NY, USA). Framework analysis employed for recognising factors mediating regular PA changes.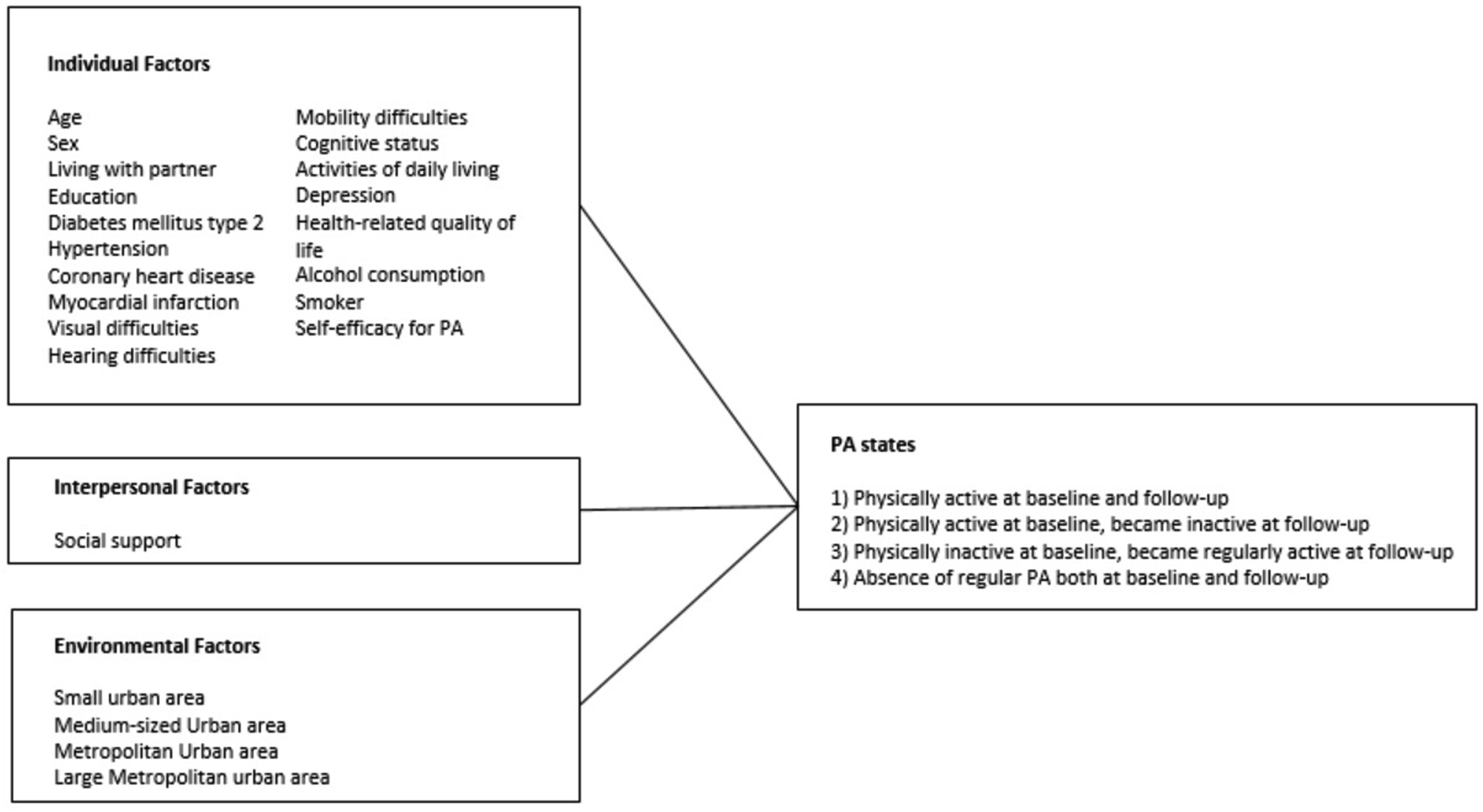
Ethics
The study was approved by the responsible ethics committees of the coordinating centre (Ethics Committee of the Medical Faculty of the University of Leipzig; ethical vote number: 369/17-ek) and of all participating study sites. Participants provided written informed consent to participate.
Results
Baseline Characteristics
Baseline Characteristics of AgeWell.de Study Participants.
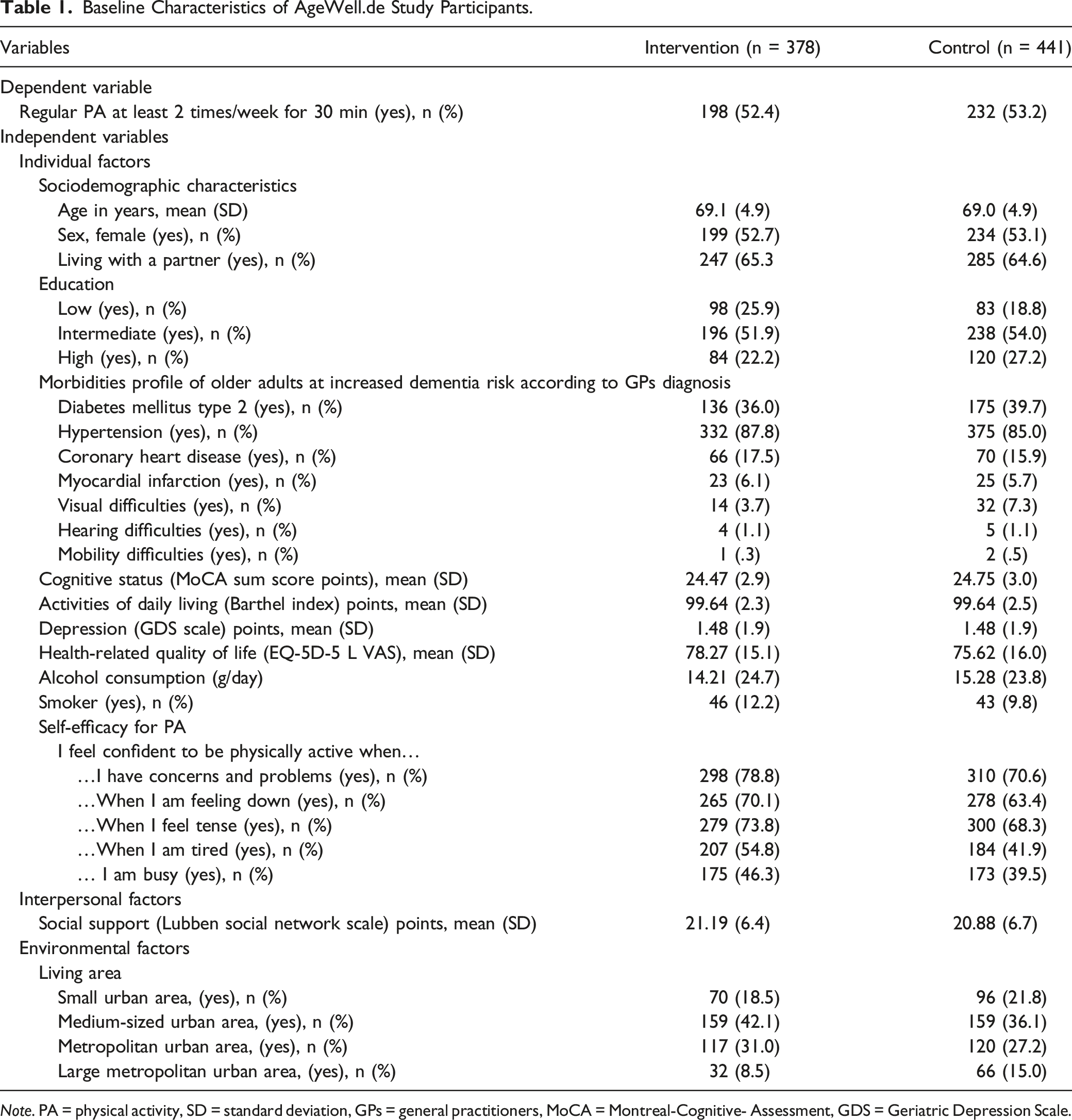
Note. PA = physical activity, SD = standard deviation, GPs = general practitioners, MoCA = Montreal-Cognitive- Assessment, GDS = Geriatric Depression Scale.
Between-Group Differences in PA Engagement at 24 Months Follow-Up
A generalized estimating equations model was conducted based on a repeated measures binary logistic model, in which it was identified that there were no significant differences between the control and the experimental group. Results showed a P-value equal to .674.
Although there were no significant differences between groups, some changes in PA behaviour were found. Figure 3 provides a description of the four different PA states (changes) that resulted from baseline to follow-up between-groups. Particularly, while 52.7% of the participants in the intervention group became physically active after the intervention, only 47.3% of the control group were able to make this transition at follow-up. Also, a greater absence of PA can be observed in the control group after the intervention (56.4%), in contrast to the intervention group (43.6%). Between-groups changes in PA states from baseline to follow-up.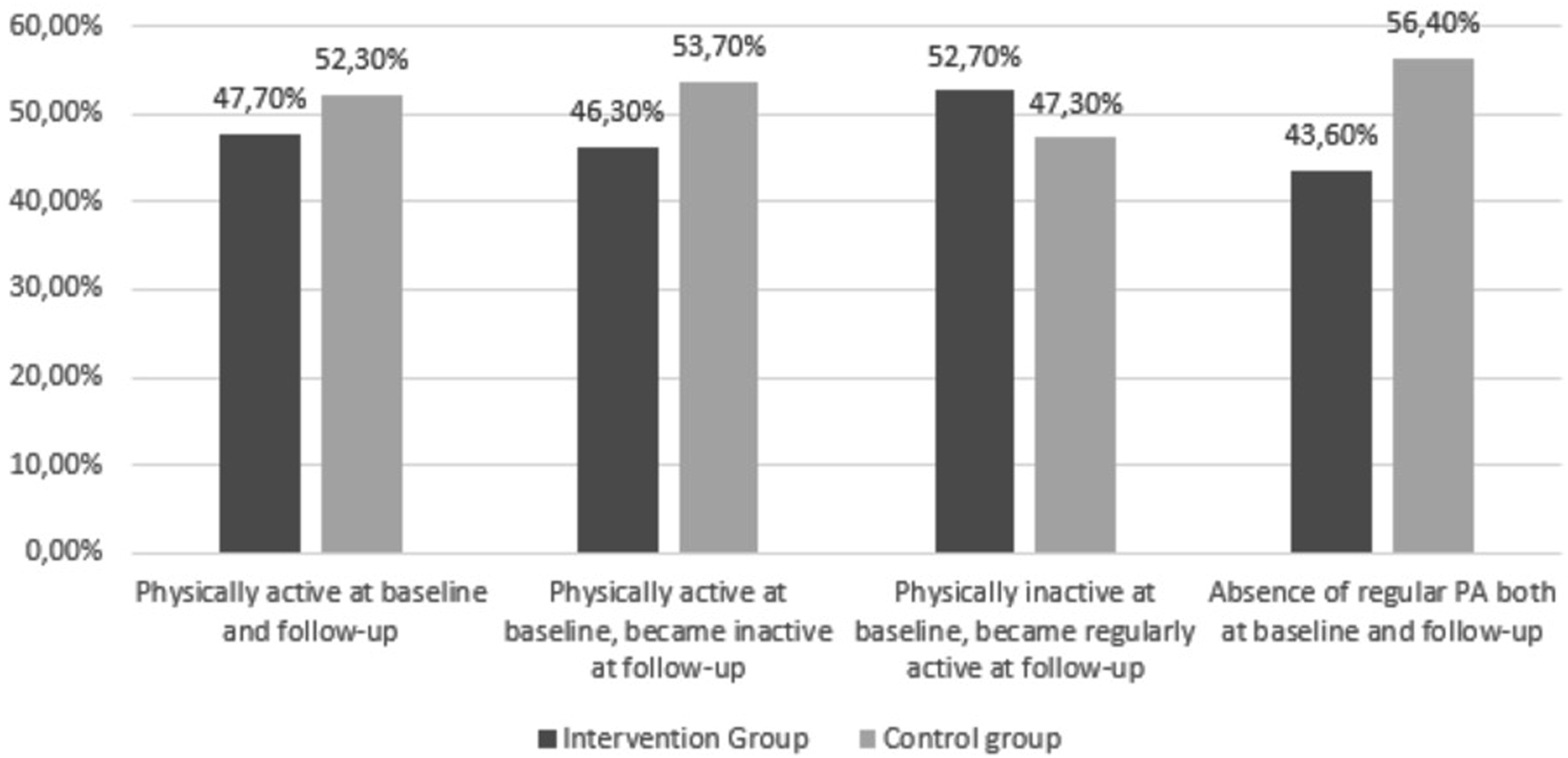
Outcomes of Decision Trees Analysis
Mediating Factors for Changes in PA States
A decision tree analysis was conducted to recognise mediating factors associated with previous changes in PA states between baseline and follow-up. We employed decision trees as a method to dissect the intricate relationships between various factors and their impact on PA bahaviour. Decision trees serve as a visual representation to understand these relationships more intuitively. The process begins by examining the entirety of the dataset, similar to starting at the root of a tree. Subsequently, the algorithm divides the dataset into smaller subsets based on the most influential factors affecting PA. This segmentation continues recursively, forming a tree-like structure. Each terminal node of the tree represents a distinct subgroup of individuals with similar characteristics. By exploring the branches from the root to the terminal nodes, we can identify the primary mediating factors influencing PA patterns.
According to our analyisis, illustrated in Figure 3, the model identified that the most influential variable impacting changes in PA was the difference in self-efficacy scores (P < .001). This finding suggests that variations in self-efficacy scores between baseline and follow-up influenced the likelihood of engaging in PA. Additionally, as illustrated in Figure 4, the model categorized the difference in self-efficacy scores into five distinct groups: Node (1) score difference equal or less than −6 points; Node (2) score difference between −6 and −1 points; Node (3) score difference between −1 and 0 points; Node (4) score difference between 0 and 5 points; Node (5) score difference greater than 5 points. Notably, positive scores indicated an increase in self-efficacy, whereas negative scores indicated a decrease in self-efficacy at follow-up. Decision tree analysis: Mediating factors associated with PA changes at follow-up.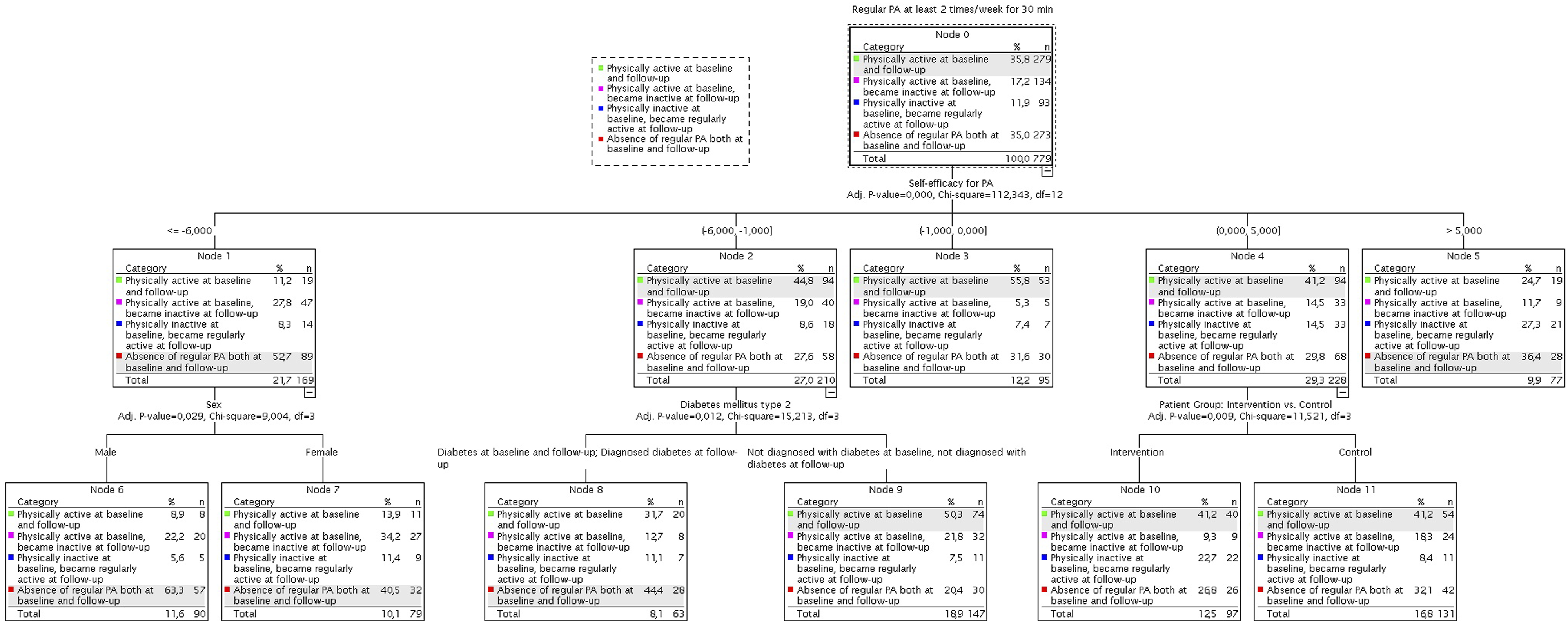
Nodes 1, 2, and 3 indicated a decrease in the probability of transitioning from physical inactivity at baseline to becoming physically active at follow-up among individuals with a negative difference in self-efficacy scores ranging from ≤-6 to 0 points (as indicated by the blue square in Figure 4). For instance, in node 1, this probability dropped from 11.9% to 8.3%; in node 2, the probability went from 11.9% to 8.6%; and node 3 declined from 11.9% to 7.4%. On the contrary, nodes 4 and 5 showed that individuals who increased scores from 0 to ≥5 points on the self-efficacy scale raised their likelihood of transitioning to a state of regular PA during follow-up after being inactive at baseline. For example, the probability at node 4 increased from 11.9% to 14.5% and in node 5 raised to 27.3%.
Moreover, the findings in nodes 6 and 7 revealed a significant association between gender and a negative difference of ≤6 points in self-efficacy scores (P = .0029). For instance, men experiencing a decline in their self-efficacy scores by ≤ -6 points increased their probability of absence of regular PA both at baseline and follow-up (PA state indicated by red square in Figure 4). This probability increased from 52.7% to 63.3%. On the contrary, despite having the same negative difference in their self-efficacy scores, women decreased this probability from 52.7% to 40.5%.
Furthermore, node 8 highlights that individuals with diabetes and a self-efficacy score difference ranging from −6 to 1 point showed an increased likelihood of absence of regular PA, both at baseline and at later follow-up (PA state indicated by red square in Figure 4). This probability increased from 27.6% to 44.4%. In comparison, node 9 indicated that those not diagnosed with this disease reduced this probability from 27.6% to 20.4%.
Finally, nodes 10 and 11 showed a significant relationship between an increase in self-efficacy scores (between 0 and 5 points) and the condition of the participants, either belonging to the control or intervention groups (P = .009). In Node 10, participants within the intervention group who experienced a self-efficacy score increase of 0 to 5 points at follow-up were observed to have an augmented probability of transitioning from physical inactivity at baseline to regular activity at follow-up (as indicated by the blue square in Figure 3). This probability increased from 14.5% to 22.7%. Conversely, in node 11, participants from the control group demonstrated a decrease in this probability from 14.5% to 8.4%.
In summary, the results of the decision tree analysis reveal that the difference in self-efficacy scores was the most influential variable in changes in physical activity states between baseline and follow-up. The probability of engaging in physical activity varied significantly based on the difference in self-efficacy scores, indicating an increased likelihood of regular physical activity participation with higher self-efficacy scores. Furthermore, significant associations were observed between gender and the presence of diabetes with changes in self-efficacy and physical activity participation. Additionally, a significant relationship was identified between the increase in self-efficacy scores and the participants’ condition, with a notable increase in the probability of transitioning to regular physical activity in the experimental group compared to the control group. These findings underscore the importance of self-efficacy in promoting physical activity and suggest that interventions aimed at improving self-efficacy may be effective in fostering more active behaviors in the studied population.
Mediating Factors for PA Engagement at Follow-Up
Additionally, we examined potential mediating factors influencing regular PA at follow-up. Thus, a second decision tree analysis was conducted, including just the dichotomous dependent variable “regular PA engagement ≥2 days/week for at least 30min"; yes/no at follow-up. The results of this analysis, as shown in Figure 5, reaffirmed self-efficacy as a significant determinant for regular PA engagement (P = .019). Decision tree analysis for regular PA engagement at follow-up.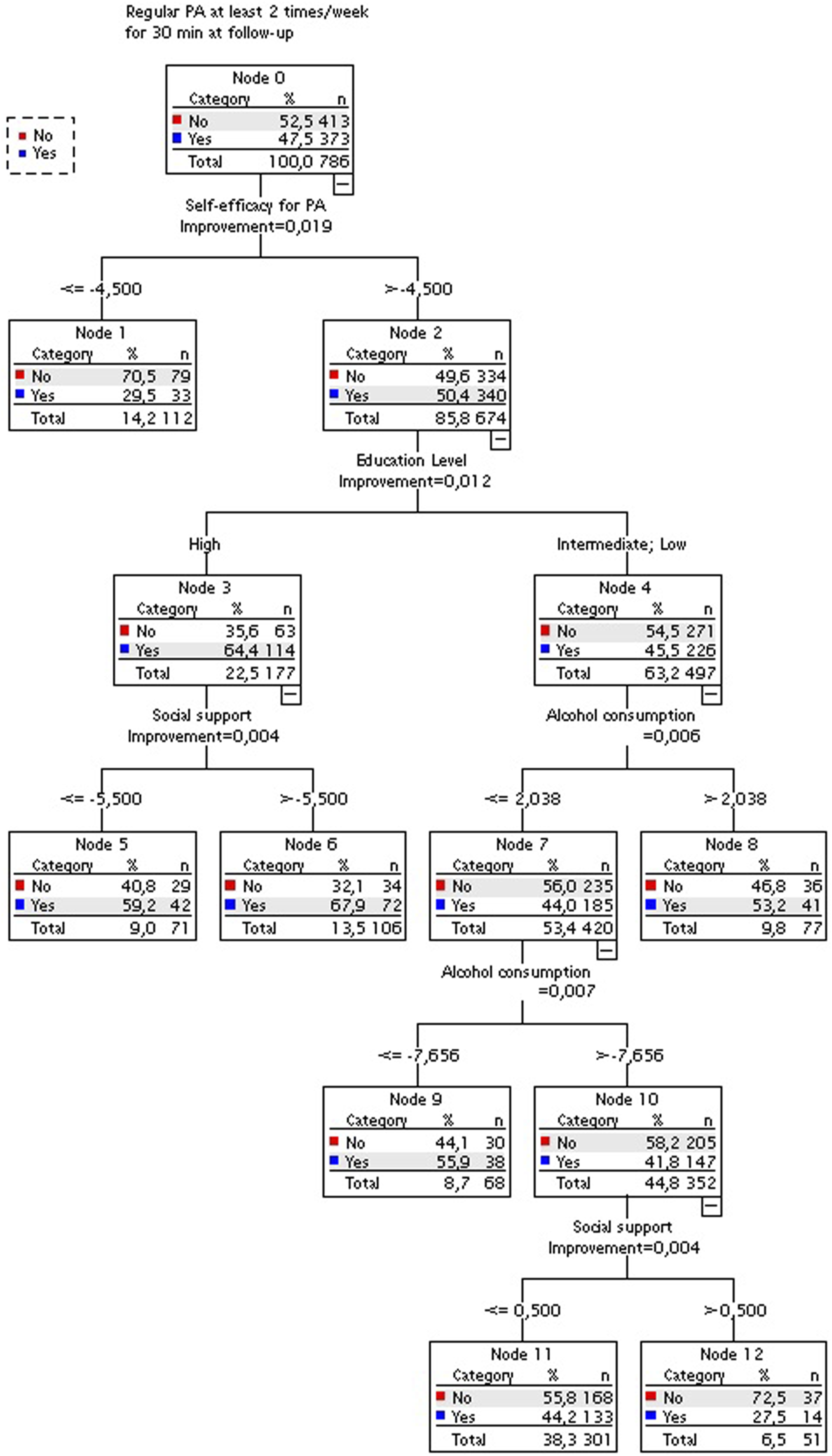
Results from this tree analysis revealed (see Figure 5) that a negative difference between baseline and follow-up of ≤ -4.50 points on the self-efficacy scale decreases the probability of regular PA at follow-up. This probability went from 47.5% to 29.5%. In contrast, when participants increased score differences by more than −4.5 points on the self-efficacy scale, their chances of doing PA regularly at follow-up increased. The probability rose from 47.5% to 50.4%.
In the same way, individuals who scored differences above −4.5 points on the self-efficacy scale in the follow-up and reported a high education level demonstrated an increased probability of engaging regularly in PA. This percentage went from 50.4% to 64.4%. Nonetheless, in the case of individuals with a high level of education, if they scored a difference of ≤ -5.5 points in their social support scores, their likelihood of engaging in PA regularly in the follow-up period decreased. The probability went from 64.4% to 59.2%.
In contrast, those with an intermediate to low educational level exhibited a reduction in their probability of engaging regularly in PA at follow-up. This went from 50.4% to 45.5%. Within this group of participants who scored differences above −4.5 points on the self-efficacy scale and had a low level of education, alcohol consumption emerged as a significant variable (P = .006). Those who increased their consumption (>2.03 g per day) at follow-up were less likely to not engage in PA regularly after the intervention. This probability was reduced from 54.5% to 46.8%. On the other hand, those who decreased their alcohol consumption by −7.6 g increased their probability of doing PA regularly at follow-up. This probability changed from 44.0% to 55.9%. On the other hand, those who increased their consumption by more than −7.6 g per day decreased their likelihood of PA from 44.0% to 41.8%.
Discussion
Main Findings
In the initial analysis, the present study did not find any significant effect on PA engagement during the 24-month follow-up period. However, looking in more detail through decision trees analysis, the likelihood of regularly engaging in PA increased during the follow-up period within specific subgroups. Particularly, individuals with increased self-efficacy at follow-up raised their probability of engaging regularly in PA after the intervention. Thus, self-efficacy was identified as the most important mediating factor associated with the likelihood of changes in PA participation at follow-up. In addition, other characteristics of participants mediated the probability of regular PA at follow-up associated with self-efficacy, including gender, presence of diabetes, being in the treatment group, educational level, social isolation, and alcohol consumption. A more detailed discussion of these sub-groups is presented below.
Self-Efficacy
The decision tree analysis identified among all the factors examined that the most important mediating factor associated with changes in regular PA participation at 24-month follow-up was the change in self-efficacy scores. These findings are consistent with those reported in previous literature. 37 For instance, self-efficacy was related to PA engagement and adherence in asymptomatic and older adults with chronic diseases, including recovered individuals of cardiovascular disease and survival in chronic obstructive pulmonary disease.37,38 Moreover, according to 2- to 5-year follow-up study in which PA was promoted, self-efficacy has been shown to be crucial in the long-term maintenance of PA. 39 Of note, the relationship between PA and self-efficacy is not unidirectional and can be influenced by other factors, such as physical and mental health, social environment, and individual limitations. 37 However, in general, it has been found that there is a positive association between self-efficacy and PA in older adults.
Self-efficacy refers to a person’s belief in his or her ability to achieve certain tasks or goals. 40 In the context of PA, self-efficacy relates to the confidence a person has in his or her ability to participate in and maintain regular PA. 41 Thus, self-efficacy may play a crucial role in exercise behaviours as older adults with higher self-efficacy perceive that they can overcome the barriers and challenges associated with PA, increasing their motivation and likelihood to participate in it. 41 According to Bandura’s theory, confidence in personal ability influences choices and effort devoted to PA behaviour. 40
In this way, it is necessary to address psychological key components, such as self-efficacy, to design effective programs promoting PA engagement and adherence. 41 To our knowledge, there is a limited amount of research on PA interventions for patients with multimorbidity and at increased dementia risk, focusing on improving self-efficacy in PA. Thus, self-efficacy enhancement strategies may be useful in interventions to increase PA engagement and adherence among this particular population.
Self-Efficacy and Gender
Another variable that mediated regular PA engagement in our study was gender. The results of the decision tree model showed that being male was a risk factor for physical inactivity as long as there was a decrease in self-efficacy. In particular, it was found that males with a decrease in self-efficacy scores were more likely to not participate in regular PA, both at baseline and at subsequent follow-up. These results are consistent with previous literature, 42 particularly coinciding with differences between PA determinants according to gender. One study reported that intention and habit are key to short- and long-term factors influencing PA in both genders. 43 However, differences were found in the role of self-efficacy, emphasizing that attitude towards PA was important for men while planning was crucial for women. 43 However, it is important to acknowledge the complexity of the relationship between attitude and planning in the context of PA. While our initial discussion highlighted the importance of attitude for men and planning for women, it is recognized that these factors may not operate independently. 43 Indeed, positive attitudes towards PA may enhance motivation for planning, suggesting a more complex relationship between attitudes and planning across genders. 43 In another study, 44 investigating gender differences in psychosocial factors related to PA during a lifestyle change intervention, it was found that men received more social support for PA, but women increased their exercise plans more. While there were differences in the importance of planning between genders, these were not consistent across all analyses. Self-efficacy was a strong predictor of behaviour change, and pre-intervention social support was important for both genders. Women showed greater use and effects of action planning, possibly linked to their social roles and responsibilities. Overall, the findings suggest that men and women may not differ in socio-cognitive variables generally, but rather in those related to their social roles. Interventions could benefit by supporting women more in behaviour change planning and by facilitating their ability to activate social support sources. Furthermore, existing literature has indicated gender differences in psychological resilience among older adults. 45 Given that women tend to report lower levels of psychological resilience compared to men, it is conceivable that this disparity could also contribute to differences in self-efficacy. 46 Lower resilience levels among older women might influence their confidence in engaging in PA and planning their exercise routines effectively. 47 Therefore, attitudes towards PA and psychological resilience could certainly be underlying factors contributing to the observed gender differences in self-efficacy. 48 Future research could explore these aspects further to provide a more comprehensive understanding of the mechanisms driving gender disparities in self-efficacy among older adults. These gender differences have implications for the development of future gender-specific PA interventions, as also stated in previous studies. 43
Self-Efficacy and Type 2 Diabetes
It was also found that a decrease in self-efficacy in combination with a diagnosis of type 2 diabetes was a risk factor for physical inactivity. In other words, if participants had this diagnosis before or after the intervention and a decrease in their self-efficacy scores, they were more likely to have no change in their physical inactivity behaviour. Previous studies also show that the diagnosis of type 2 diabetes was a risk factor for inactivity. 49 Therefore, developing tailored guidelines for PA and self-efficacy enhancement aimed at this population is also essential.
Self-Efficacy in the Experimental Group vs. Control Group
Increases in self-efficacy at follow-up and intervention group participants experiencing an increase in self-efficacy between baseline and follow-up were more likely to present a higher probability of transitioning from being physically inactive at baseline to physically active in the follow-up, unlike the control group. Thus, as has also been shown in other studies, 50 multicomponent programs should aim at integrating PA, cognitive and social activities, providing knowledge, tools, and skills that may enable participants to increase self-efficacy and feel more confident in engaging in regular, long-term PA.
Self-Efficacy, Educational Level, Social Support, and Alcohol Consumption
Additionally, high educational level accompanied by increased self-efficacy at follow-up increased the likelihood of regular PA in the follow-up. Comparing these findings with recent literature, various studies showed a positive correlation between educational level and PA participation in older adults.51,52 A person’s education can influence his or her behaviour and attitudes toward healthy lifestyle behaviours.53,54 Older adults with higher levels of education tend to have a better understanding of the health benefits of PA and a greater awareness of how to maintain a healthy lifestyle. 53 In addition, education can provide them with the skills and knowledge needed to participate in PA safely and effectively. 53 These findings highlight the importance of education and self-efficacy as facilitating factors to promote an active lifestyle in older adults with multimorbidity and at increased dementia risk.
It is worth noting that for this population with increased self-efficacy and a high level of education, a decrease in social support at follow-up was a risk factor for not engaging in regular PA. Thus, these results highlight that social support was a relevant mediator for PA in people with higher education and multimorbidity. We did not find studies showing direct correlations between high educational levels, decreased social support and PA engagement. In general, studies reported that a high level of education was associated positively with social support as it offers greater opportunities for social interaction and access to broader social networks. 55 However, each population group is different. Perhaps there are certain additional key aspects to consider when individuals are multimorbid and at increased dementia risk. For instance, although individuals may have a higher level of education and self-efficacy when they suffer from multimorbidity, they may experience changes in their social environment and support, which could affect their probability of engaging in PA. Hence, social support might be also an essential factor to consider when planning PA promotion strategies for persons with multimorbidity and at increased dementia risk.
Finally, low educational level and alcohol consumption were also risk factors, as these factors reduced the likelihood of regular PA in follow-up. These findings are in accordance with the literature, as it has been found that low educational levels and alcohol consumption are associated with low PA levels. 56 This may be due to unfavourable socioeconomic factors, social and cultural norms that normalize alcohol consumption and hinder access to resources, knowledge, and skills needed to initiate and maintain PA behaviour. 57 Programs aimed at increasing self-efficacy among low-educated older adults should consider the challenges and limitations inherent to this population sub-group. Such programs could incorporate components and strategies that guarantee access to resources, support, knowledge, and skill building.
Strengths and Limitations
One of the strengths of this study lies in the utilization of decision tree analysis. This approach facilitated examine complex interactions among mediating factors for PA engagement during the follow-up period and identified high-risk subgroups. The classification of the population based on these findings will contribute to the effective targeting and design of future interventions targeted at high-risk groups for dementia. The study has recognized various limitations, highlighting the need to interpret the findings carefully. Firstly, larger sample sizes are necessary to ensure more robust and reliable results. Furthermore, the exact amount of PA undertaken by individuals is unknown, as only the receipt of the multimodal intervention is documented. Lastly, the sample was rather selective - based on the inclusion criteria alone, an increased number of participants were probably physically inactive (physical inactivity is also a component of the CAIDE score, and criteria such as body-mass-index (BMI) > 30, which also correlates strongly with inactivity). Therefore, the results can only be generalized to a limited extent.
Conclusion
The study sample did not exhibit any significant impact on PA effect following the intervention. However, certain subgroups showed an increased likelihood of adopting regular PA during the follow-up period. Notably, participants who experienced an improvement in their self-efficacy scores at follow-up had a higher probability of enhancing their regular PA, mainly if they were initially physically inactive. These observations suggest that intervention programs successfully enhancing self-efficacy are more likely to promote regular PA. Therefore, self-efficacy remains a crucial aspect to consider and evaluate in future intervention studies targeting older adults with multimorbidity and at increased dementia risk. Efforts should be focused on individualizing interventions, particularly for men, individuals with type 2 diabetes, those with low social support, those with intermediate or low education, and those with higher alcohol consumption.
Footnotes
Acknowledgments
Members of the AgeWell.de study group: Principal Investigator: Steffi G. Riedel-Heller; Co-Principal Investigators: Wolfgang Hoffmann, Jochen Gensichen, Walter E. Haefeli, Hanna Kaduszkiewicz, Hans-Helmut König, Thomas Frese, David Czock, Jochen René Thyrian; Members of the study team: Franziska Berg, Andrea Bischhoff, Christian Brettschneider; Mandy Claus, Juliane Döhring, Alexander Eßer, Corinna Gräble, Stephanie Hingst, Caroline Jung-Sievers, Kerstin Klauer-Tiedtke, Kerstin Krebs-Hein, Flora Kühne, Sebastian Lange, Paula Liegert, Dagmar Lochmann, Tobias Luck, Silke Mamone, Andreas Meid, Michael Metzner, Lydia Neubert, Anke Oey, Susanne Röhr, Franziska-Antonia Zora Samos, Karin Schumacher, Theresa Terstegen, Sandy Thieme, Svetlana Usacheva, Lars Wamsiedler, Tanja Wehran, Marina Weißenborn, Ines Winkler, Isabel Zöllinger, Andrea Zülke, Ina Zwingmann. Additionally, we would like to extend our acknowledgments to Julian Tamayo for his statistical guidance in the decision trees analysis. His expertise and insights greatly contributed to the rigor and accuracy of our study.
Author Contributions
Conceptualization, J.G., W.H., H.K., H.-H.K., J.R.T., B.W., and S.G.R.-H.; Data curation, M.I.C., and B.W.; Formal analysis, M.I.C.; Funding acquisition, J.G., W.H., H.K., H.-H.K., J.R.T., B.W., and S.G.R.-H.; Investigation, M.I.C., A.Z., M.L., C.B., A.B., E.S.K., and J.D.; Methodology, M.I.C. and J.R.T.; Project administration, W.H., H.K., H.-H.K., J.R.T., B.W., and S.G.R.-H.; Resources, J.G., W.H., H.K., H.-H.K., J.R.T., and S.G.R.-H.; Supervision, A.Z., M.L., T.F., J.G., W.H., H.K., H.-H.K., J.R.T., B.W., and S.G.R.-H.; Validation, W.H., H.K., T.F., J.G., J.R.T., B.W., and S.G.R.-H.; Visualization, M.I.C. Writing—original draft, M.I.C.; Writing—review and editing, E.S.K., A.B., M.W., J.G., M.L., A.Z., W.H., H.K., C.E., R.P.K., J.D., C.B., H.-H.K., B.W., J.R.T., S.G.R.-H. All authors have read and agreed to the published version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This publication is part of the study “AgeWell.de – a multi-centric cluster-randomized controlled prevention trial in primary care” and was funded by the German Federal Ministry for Education and Research (BMBF; grants: 01GL1704A, 01GL1704B, 01GL1704C, 01GL1704D, 01GL1704E, 01GL1704F).
Ethical Statement
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
