Abstract
Single-dose preoperative stereotactic body radiotherapy is a novel radiotherapy technique for the early-stage breast cancer, and the treatment response pattern of this technique needs to be investigated on a quantitative basis. In this work, dynamic contrast-enhanced magnetic resonance imaging and diffusion-weighted magnetic resonance imaging were used to study the treatment response pattern in a unique cohort of patients with early-stage breast cancer treated with preoperative radiation. Fifteen female qualified patients received single-dose preoperative radiotherapy with 1 of the 3 prescription doses: 15 Gy, 18 Gy, and 21 Gy. Magnetic resonance imaging scans including both diffusion-weighted magnetic resonance imaging and dynamic contrast-enhanced magnetic resonance imaging were acquired before radiotherapy for planning and after radiotherapy but before surgical resection. In diffusion-weighted magnetic resonance imaging, the regional averaged apparent diffusion coefficient was calculated. In dynamic contrast-enhanced magnetic resonance imaging, quantitative parameters
Keywords
Introduction
Breast cancer is a major cause of cancer death in women in most Western countries. Statistics shows that 1 (12.5%) of 8 women will be affected by breast cancer during her lifetime. Radiation therapy plays an important role in breast cancer treatment. Currently, breast-conserving treatment consisting of lumpectomy followed by 3 to 6 weeks of daily external beam radiation therapy (RT) is a standard treatment option. Studies have proved that this approach significantly decreases the local recurrence rate in women receiving conservative surgery. 1,2 However, some women electing to receive breast conserving surgery are not able to complete the recommended RT due to financial concerns or distance to the nearest treatment facility. 3 As a result, partial breast radiation therapy (PBI) was developed to decrease the treatment burden for patients. In early studies, PBI technique has been demonstrated to have efficacy comparable to historical controls. 4,5 Several techniques exist for delivery of partial breast treatment but may require additional equipment or specialized training. 6 Given the fact that most modern radiotherapy centers are able to deliver stereotactic and intensity-modulated radiotherapy, 7 –9 external beam partial breast irradiation might be a viable option. However, preliminary data have suggested higher rates of suboptimal cosmesis, possibly related to the large volumes of normal breast tissue treated. 10,11 Compared to postoperative PBI, preoperative radiotherapy has been shown to reduce treatment volumes significantly. 12,13 In addition, preoperative treatment provides an opportunity to evaluate pre- and postradiation imaging in order to better understand radiation response and potentially identify the functional imaging biomarkers that can be used as prognostic and predictive tools. 14 As a result, in consideration of all mentioned issues simultaneously, we developed a novel clinical trial evaluating the use of a highly conformal preoperative stereotactic body radiotherapy (SBRT) approach with the single-fraction delivery, and we utilized dynamic contrast-enhanced magnetic resonance imaging (DCE-MRI) and diffusion-weighted magnetic resonance imaging (DW-MRI) for the radiation response investigation
A typical DCE-MRI involves a serial acquisition of T1-weighted magnetic resonance (MR) images of region of interest (ROI) before and after the intravenous injection of a low molecular, T1-shortening paramagnetic compound as the contrast agent (CA), and the evolution curve of CA concentration as a function of time can be acquired from the signal intensities of sampled images. As convenient and robust analysis metrics, semiquantitative parameters including initial area under the MR signal evolution curve (iAUC), variance of enhancement slope, and early contrast uptake have been frequently used in fast DCE-MRI analysis.
15
–18
In quantitative analysis, biological parameters depicting microvascularity permeability, tissue perfusion, and extracellular volume fraction can be derived by fitting the CA concentration evolution curves into an appropriate pharmacokinetic model with certain pathological assumptions. In earlier assessment studies, relationship between the change in a lesion’s pharmacokinetic parameters and the pattern of tumor vasculature integrity change following drug treatment and chemotherapy has been shown.
19
–21
Compared with DCE-MRI, DW-MRI utilizes the natural sensitivity of MR to motion. The thermally induced random motion of water molecules is described as self-diffusion or Brownian motion. The water diffusion rate can be described by a logarithmic parameter apparent diffusion coefficient (ADC), which is derived quantitatively from 2 sets of diffusion-weighting strength in the pulse sequence in aspect of pulse amplitude, duration, and spacing of a diffusion gradient, jointly expressed as a “
Although this new single-dose preoperative breast radiotherapy treatment is promising, its treatment response pattern needs to be further investigated on a quantitative basis. In this study, DCE-MRI and DW-MRI were firstly used to assess the response of the new single-dose preoperative radiotherapy treatment scheme in breast cancer. The semiquantitative parameter iAUC and the quantitative tissue permeability parameters from the classic compartment pharmacokinetic models were investigated in DCE-MRI analysis, and in DW-MRI analysis, ADC was chosen as the biomarker to assess radiation-induced changes. Our primary objective was to assess the relative changes in selected parameters after radiation treatment. Our secondary objective was to investigate the potential linear relationship between parameter changes and delivered radiation dose.
Materials and Methods
Patients
Fifteen patients were involved in this Institutional Review Board-approved study (Table 1). Each patient was required to have a complete history and biopsy-proven invasive/infiltrating or in situ breast carcinoma. For each patient, the gross tumor volume (GTV) was delineated based on magnetic resonance imaging (MRI) and generally has a volume of less than 1 cm3. The prescription dose was delivered in a single fraction using intensity-modulated RT. The MRI scans were acquired about 1 week before and 1 week after radiotherapy. All patients underwent surgical tumor resection within 10 days of radiotherapy using standard surgical procedure.
Patient History and Treatment Information.
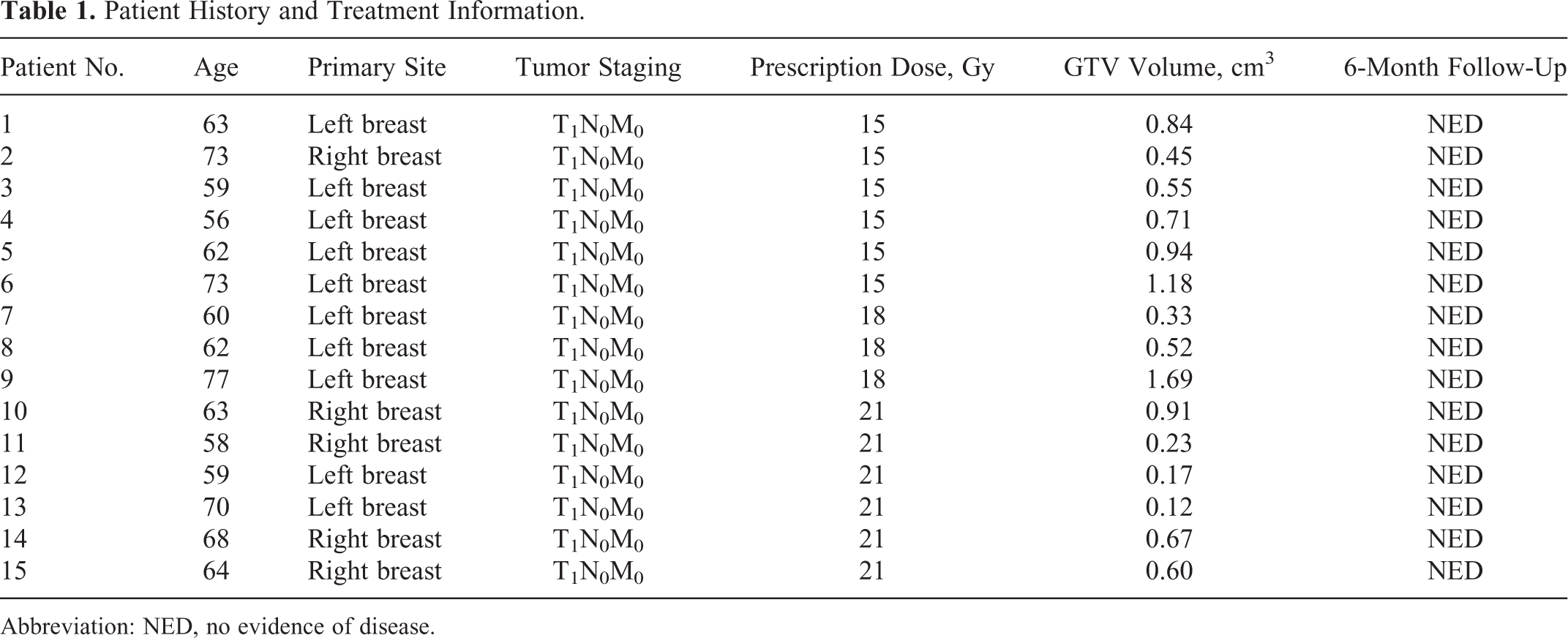
Abbreviation: NED, no evidence of disease.
Image Acquisition
All MRI scans were acquired with patients’ in the prone position on a 1.5-T clinical scanner (GE Healthcare, Milwaukee, Wisconsin) using a standard 4-channel breast coil. The imaging protocol included T1- and T2-weighted imaging, DW-MRI, and DCE-MRI. In this work, DCE-MRI data acquired were used for tumor delineation and radiotherapy planning and as such demands high spatial resolution with adequate fat saturation. A balanced choice between high spatial resolution and high temporal resolution was made. 20 In DCE-MRI, 2 T1 calibration scans using dual flip angles 5° and 15° were acquired first to get the T1 value before CA injection. 26 The CA gadopentetate dimeglumine (Magnevist; Schering, Berlin, Germany/Bayer, Whippany, New Jersey) was intravenously administered by power injection with a dose of 0.1 mmol/kg bodyweight at 2 mL/s flow rate. The DCE-MRI scans were acquired in the sagittal plane with 1 pre-enhanced and 6 postenhanced series using a T1-weighted fast 3D Spoiled Gradient Echo (SPGR) dynamic sequence (repetition time [TR] = 6 ms, echo time [TE] = 2.9 ms, field of view = 24 × 24 cm2, matrix size = 256 × 256, slice thickness = 3.4 mm, no averages). One preinjection volume and 6 postinjection volumes were acquired in each scan, and the temporal resolution was about 1 minute.
The DW-MRI scans were acquired in the sagittal plane using a spin-echo Echo Planar Imaging (EPI) sequence (TR = 3125 ms, TE = 77 ms, field of view = 30 × 30 cm2, matrix size = 256 × 256, slice thickness = 5 mm, 4 averages). The diffusion-sensitized gradient encoding with a diffusion weighting factor of
Analysis of DCE-MRI
The posttreatment scans were rigidly registered to the pretreatment scans using a feature-based algorithm using the mutual information of the chosen points’ location information.
27
The T1 values before CA administration, T10, and T1 values at 6 time point after CA administration, T1(t1-6), were derived from the signal ratio of scans with dual flip angles. The change in longitudinal relaxation rate

where

In Equation 2,
The CA concentration evolution in the blood plasma

In the Equation 3,

Equation 4 was used to resolve 2 unknown variables (
The GTV, clinical target volume (CTV), and planning target volume (PTV) were selected as ROI for analysis. The values for iAUC6min,
Analysis of DW-MRI
Given the fact that the DW-MRI images were inherently aligned with the DCE-MRI images by sharing the same coordinate of each scan, the posttreatment DW-MRI images were registered to the pretreatment images with the DCE-MRI registration information. Based on the DW-MRI images, the ADC value is calculated by Equation 5:

Statistical Analysis
Statistical analysis was performed using the commericial software referred to as SPSS program (SPSS Software Products, Chicago, Illinois). The Wilcoxon signed-rank test was used to assess the relative changes in iAUC6min,
Results
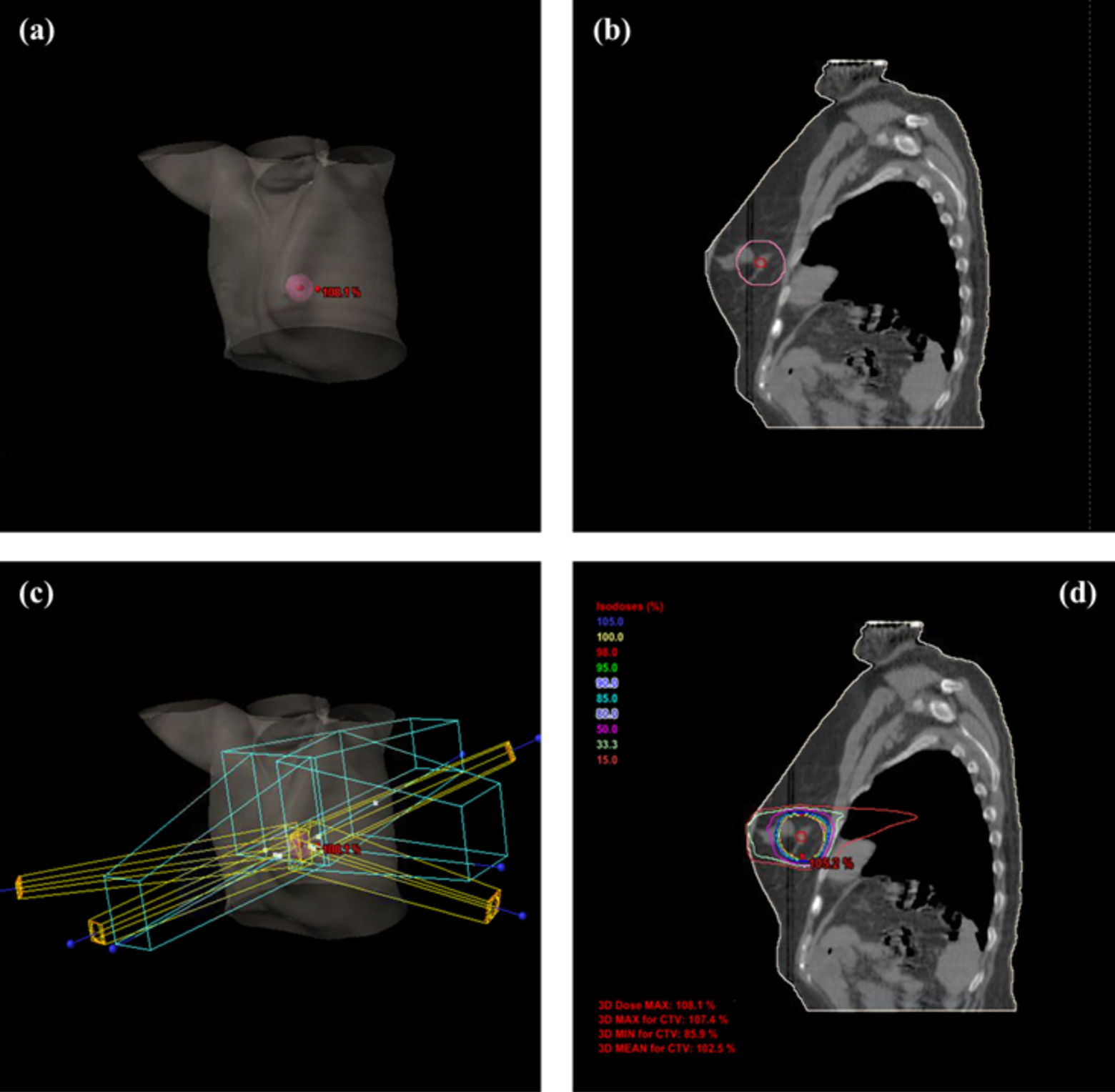
All the patients received radiotherapy as planned. Figure 1 shows the radiotherapy from a selected patient. The GTV (0.71 cm3) and PTV (35.37 cm3) are displayed in red and pink, respectively. Figure 2 shows the same patient’s paired DW-MRI and DCE-MRI images. Figure 3A presents the same patient’s preinjection T1 map (T10) at the pretreatment scan day. The 3D mean value of the CTV (indicated by the red contour) T10 was 689.1 ± 56.2 ms. Figure 3B shows the AIF, CTV CA concentration measurement, and its fitting. The measured CA curve was successfully fitted by the Tofts model (

Treatment plan from a selected patient. A, GTV (red, 0.71 cm3) and PTV (pink, 35.37 cm3) shown in 3D body; (B) GTV and PTV shown in a selected slice of CT; (C) field arrangement in 3D body; and (D) dose distribution within a selected slice of X-ray computed tomography (CT). GTV indicates gross tumor volume; PTV, planning target volume.
MR images from a selected patient. A, Pretreatment DCE-MRI of a selected temporal frame; (B) posttreatment DCE-MRI of the same temporal frame as (A); (C) pretreatment DW-MRI; and (D) posttreatment DW-MRI. All pretreatment and posttreatment images are registered. MR indicates magnetic resonance; DCE-MRI, dynamic contrast-enhanced magnetic resonance imaging; DW-MRI, diffusion-weighted magnetic resonance imaging.
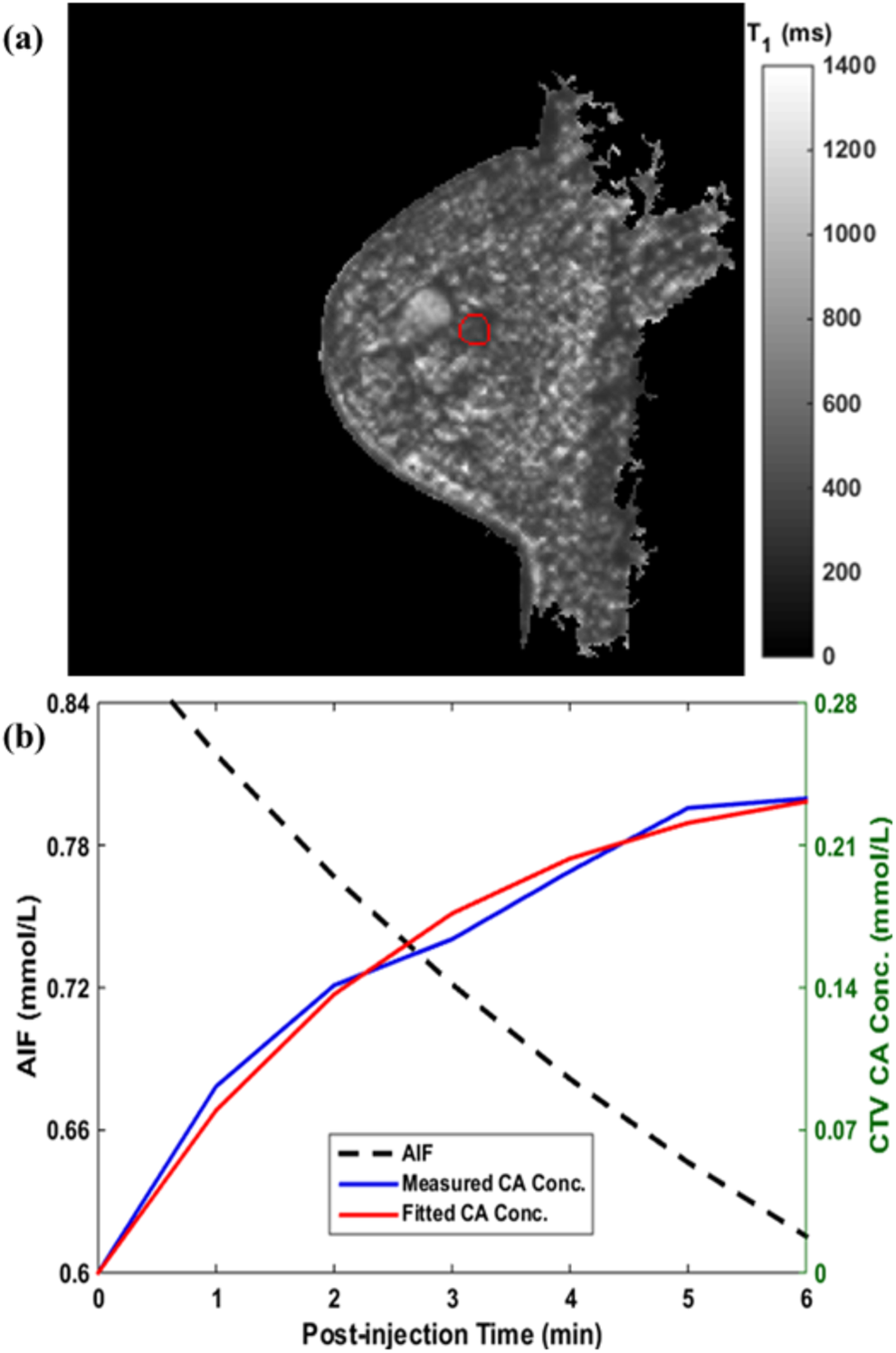
Pretreatment scan analysis. A, Preinjection T10 map and (B) AIF (black), CTV CA concentration measurement (blue) and its fitting (red) in pharmacokinetic analysis. AIF indicates arterial input function; CTV, clinical target volume; CA, contrast agent.
Table 2 presents the 15 patients’ average values of the investigated parameters at different ROIs measured before and after radiotherapy. As shown in Table 2, the semiquantitative iAUC significantly increased in PTV (
The Parameters’ Average Value Before and After Radiotherapy.

Abbreviations: PTV, planning target volume; RT, radiotherapy; CTV, clinical target volume; GTV, gross tumor volume; rADC, regional apparent diffusion coefficient; iAUC, initial area under the concentration curve.
aStatistically significant (
To investigate the potential parameter changes’ linear dependence on the treatment dose, we then performed correlation tests on each parameter in different ROIs. Table 3 includes the relative changes of each parameter after radiotherapy with 15 Gy, 18 Gy, and 21 Gy prescription dose, Pearson correlation coefficients, and significance
Correlation Test Results Between Parameter Changes and Radiation Doses.

Abbreviations: PTV, planning target volume; CTV, clinical target volume; GTV, gross tumor volume; rADC, regional apparent diffusion coefficient; iAUC, initial area under the concentration curve.
aStatistically significant (

Linear correlation tests of PTV parameters’ changes and treatment dose. A, iAUC6min; (B)
Discussion
As the first study investigating single-dose preoperative breast SBRT with quantitative MR imaging technique, we used DW-MRI and DCE-MRI for the assessment of a novel breast radiotherapy treatment scheme. In general, the results showed that the model-free iAUC6min and model-based
In this study, the rADC results are interesting. The measured water ADC is often considered to be dominated by the fraction of intracellular water. Due to the existence of organelles, the extracellular water has been estimated to diffuse with the rate constant 2 to 3 times larger than the corresponding rate of intracellular water. 39 The increased ADC has been associated with reduced cell density and restricting barriers of cell membrance induced by radiation cell killing. 20 As a result, the slight decrease in rADC in this study may suggest suboptimal therapeutic effects of this new treament scheme. It shall be noted that the potential linear correlation of rADC change in Table 3 shows that rADC increased in all ROIs after radiotherapy when the treatment dose was 21 Gy. This suggests that rADC change had a different trend depending on the treatment dose, and there could be a potential dose threshold that determines the trend of rADC change.
The results of correlation analysis demonstrated that a linear relationship might be feasible to describe the relationship between the radiotherapy dose and the relative parameter changes in most substudies. This suggests that as the preoperative radiation dose goes up, the surrogate biomarkers may have larger changes. If the linear correlation held valid, it implied that radiation-induced changes in biomarkers could be potentially predicted with a given radiation dose. This finding may be valuable to future work on dosage optimization of breast single-dose preoperative radiotherapy.
There are several limitations in the present study. First, the simple 2-compartment based Tofts model may not be the optimal one to describe the biological environment of breast tumors. In addition, the linear relationship between CA concentration and longitudinal relaxation change assumes the sufficiently fast water exchange from EIS to EES, yet the assumption is not always guaranteed.
40
A second limitation is the failure of nonlinear model fitting for quantitative GTV DCE-MRI analysis for certain patients. A fitting is justified as unsucessful if the obtained parameter violates the model assumption (
Conclusion
As the first study investigating a new single-dose breast SBRT with quantitative MRI technique, the initial results suggest that the MR quatitiative parameters could potentially be used as radiation response biomarkers. A linear relationship between the radiotherapy dose and the relative parameter changes was observed in various MR quatitiative parameters. The results might provide valuable references for future research on this new single-dose breast radiotherapy. Further work exploring and validating these biomarkers to optimize breast radiation treatment assessment is expected.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was partially supported by grants from the National Institutes of Health grant K12HD043446 - Building Interdisciplinary Research Careers in Women's Health (JH) and Varian Medical Systems (JH).
