Abstract
We previously performed Monte Carlo simulations of magnetically focused proton beams shaped by a single quadrapole magnet and thereby created narrow elongated beams with superior dose delivery characteristics (compared to collimated beams) suitable for targets of similar geometry. The present study seeks to experimentally validate these simulations using a focusing magnet consisting of 24 segments of samarium cobalt permanent magnetic material adhered into a hollow cylinder. Proton beams with properties relevant to clinical radiosurgery applications were delivered through the magnet to a water tank containing a diode detector or radiochromic film. Dose profiles were analyzed and compared with analogous Monte Carlo simulations. The focused beams produced elongated beam spots with high elliptical symmetry, indicative of magnet quality. Experimental data showed good agreement with simulations, affirming the utility of Monte Carlo simulations as a tool to model the inherent complexity of a magnetic focusing system. Compared to target-matched unfocused simulations, focused beams showed larger peak to entrance ratios (26% to 38%) and focused simulations showed a two-fold increase in beam delivery efficiency. These advantages can be attributed to the magnetic acceleration of protons in the transverse plane that tends to counteract the particle outscatter that leads to degradation of peak to entrance performance in small field proton beams. Our results have important clinical implications and suggest rare earth focusing magnet assemblies are feasible and could reduce skin dose and beam number while delivering enhanced dose to narrow elongated targets (eg, in and around the spinal cord) in less time compared to collimated beams.
Introduction
The current delivery method of choice for proton radiosurgery is passive collimation, which can deliver small beams with a sharp penumbra. However, because lateral particle equilibrium breaks down for small fields, beam broadening due to multiple Coulomb scattering tends to reduce the effectiveness of protons to a greater extent than for larger fields. Magnetic focusing can potentially reduce this particle outscatter that tends to degrade peak to entrance performance and thus improve treatment dose rate and efficacy for proton small fields. Moreover, for narrow and elongated planning target volumes, a single quadrapole focusing magnet could potentially be used. 1
We recently reported results from Monte Carlo simulations of magnetically focused proton beams shaped by a single focusing magnet at proton energies relevant to radiosurgery applications (100, 125, and 150 MeV) and compared their properties with passively collimated beams shaped by an elliptical collimator. 1 Both beams produced narrow elongated transverse dose profiles at Bragg depth (monoenergetic cases) and over the spread out Bragg peak (SOBP; modulated cases). Compared to the collimated beams, the magnetically focused beams showed superior dose distribution properties: monoenergetic focused beams showed larger peak to entrance ratios, and smaller entrance dose, integral dose, estimated therapeutic ratios, penumbra volumes, and vertical lateral penumbras at Bragg depth. In addition, 100 MeV modulated focused beams showed an increase in central peak to entrance dose ratio, and smaller vertical profile lateral penumbras over the range of the SOBP plateau. The clinically relevant advantages can be attributed to the preferential directional acceleration of protons due to the magnetic field. 1
In the previous work, 1 the focused beams were simulated using magnet parameters that were chosen to mimic k = 3 (quadrapole) Halbach cylinders. Such cylinders consist of sections of directionally magnetized material arranged to produce a high magnetic field inside a cylindrical cavity but with negligible field outside. 2 In this article, we present data from proton beams shaped by actual prototype quadrapole Halbach cylinders that were constructed from rare earth permanent magnet materials. Data was collected at energies and treatment nozzle configurations used in radiosurgery cases at our institution. This data was also compared to additional Monte Carlo computer simulations. Because the prototype magnets were manufactured to have specifications similar to the simulated magnets of the previous work, the present study provides experimental verification of the feasibility and potential clinical utility of the use of such magnets suggested by the previous simulations.
Materials and Methods
Quadrapole Halbach Cylinders
Focusing magnets were designed using Maxwell electromagnetic field simulation software (Ansoft Inc, Canonsburg, Pennsylvania) in conjunction with a vendor with extensive experience in the development and manufacture of rare earth magnetic materials and systems (Electron Energy Corporation, Landisville, Pennsylvania). The same vendor manufactured two prototype magnets consisting of 24 segments of Sm2Co17 permanent magnetic material adhered into a hollow cylinder (inner diameter (ID) 20 mm, outer diameter (OD) 150 mm, axial length 150 mm; Figure 1A). The material was chosen for its radiation hardness and has an energy product of 219 kJ/m3 and a coercive force of 803 kA/m. The assemblies produce quadrapole magnetic fields inside the cylindrical cavity with a magnitude of 1.5 T at the poles and a radial gradient of 150 T/m. The maximum field magnitude (which occurs in vicinity of the poles) in planes parallel to and at 3 and 10 cm from the end surface of the magnet are ~85 and 2 mT, respectively. A nonmagnetic stainless steel case consisting of a sleeve (ID 150 mm, OD 155 mm, length 40 mm) and 2 end caps (ID 48 mm, OD 155 mm, thickness 15 mm) provides structural support to the assembly. Because the end caps also determine the minimum axial separation between the magnets and other magnetic objects, they provide a safety function by limiting the potentially very large forces between magnet fringe fields and object. Polycarbonate safety cases, which extend 15 mm from the end caps, were constructed to further limit this distance and are equipped with removable covers that prevent physical access to the magnet core when not in use (Figure 1B). Finally, a track system was constructed to precisely and securely position the focusing magnets in the beamline of the Gantry 1 treatment room at Loma Linda University Medical Center (Figures 1C and 2).

Prototype magnetic assemblies. A, Focusing magnets consist of 24 segments of uniformly magnetized Sm2Co17 material adhered into a cylinder and encased in nonmagnetic stainless steel. B, Lexan safety/mounting case surrounding magnet. C, Magnet positioned in mounting track upstream from a water tank containing EBT2 radiochromic film.
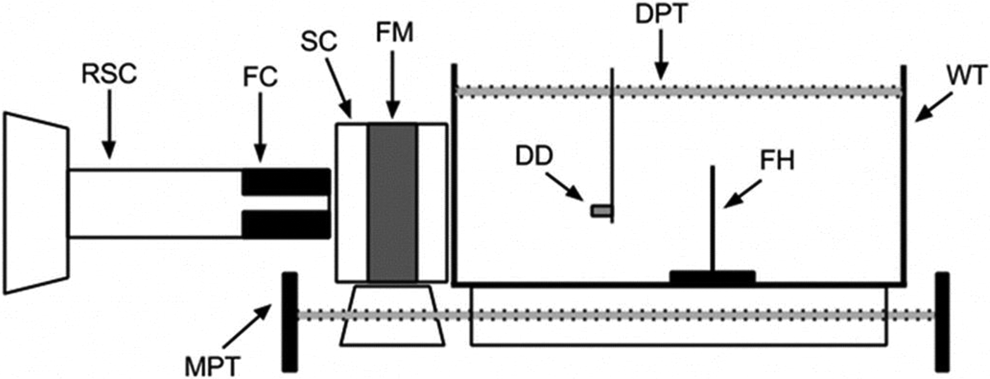
Schematic of experimental setup showing radiosurgery cone (RSC) with final collimator (FC), focusing magnet (FM) inside its safety case (SC) mounted on the magnet positioning track (MPT), water tank (WT) sitting above the MPT and containing either the diode detector (DD) mounted on its servo motor controlled detector positioning track (DPT) or a film holder (FH) containing radiochromic film.
Proton Beam Experiment Parameters
A schematic of the experimental setup used to collect proton data is shown in Figure 2. A single focusing magnet was mounted on its positioning track and placed between one of two radiosurgery cones (a clinical cone or experimental functional cone, each containing a collimator) and water tank such that the magnet safety case was touching both the cone upstream and tank downstream. This made the distance between the magnet proper and the cone 32 mm (clinical cone) or 18 mm (experimental cone) and between the tank 32 mm (both cones), and these are the smallest distances possible in our setup. With this setup, we investigated focusing beams of varying energy, modulation, and initial beam diameter, all chosen to be clinically relevant to radiosurgical applications. Modulated and unmodulated protons were delivered at 127, 157, and 186 MeV. At our facility, beams of the former 2 energies are delivered using a single scatterer, whereas the latter uses a double scattering system. 3,4 Modulated beams produced SOBP plateaus of 15 or 30 mm. Immediately upstream of the magnet, the beams were collimated to either 15, 12, or 8 mm diameter. Finally, longitudinal depth and transverse dose distributions were measured in the water tank using a PTW proton diode detector (Freiburg, Germany) and radiochromic film, respectively (see below). In addition to the focused beams described thus far, data was also collected for 127 MeV, 15 mm initial diameter unfocused (ie, collimated only) beams. This data were acquired and compared with the associated focused beams with the only difference being the absence of the magnet from the beamline.
Diode Detector (Depth Dose)
As focused beam spots are narrow and have a steep transverse dose gradient, a detector with high spatial resolution was necessary to avoid partial volume effects. Therefore, depth dose profiles were measured using a p-type silicon diode chamber (PTW PR60020 Dosimetry Diode PR) in the water tank positioned by a servo motor controlled track developed in-house (Figure 2). The diode has a single cylindrical sensitive volume with a cross-sectional area of 1 mm2 and a thickness of 20 mm, and a water-equivalent window thickness of 1.33 mm. 1 Data was acquired with the diode axis parallel to the proton beam with beam delivered to each diode position for 20 s.
Radiochromic Film (Transverse Profiles)
To obtain transverse dose profiles, 3.5” × 2” pieces of Gafchromic EBT2 radiochromic films (Advanced Materials Group, Wayne, New Jersey) were placed in custom-designed holders along the beam axis (Figure 1C) at 3 depths in the water tank representing entrance, mid-range region proximal to the Bragg peak, and Bragg depth/center of modulation (COM) dose positions for each energy/modulation (see Figures 1C and 2). Films were irradiated for 165 to 310 seconds depending on beam parameters producing beam spots with maximum doses ranging from 280 to 1300 cGy. Additional 2” × 5” pieces of films were also exposed at reference doses (RDs) ranging from 200 to 1200 cGy. All films were scanned in the same orientation in 48 bit red/blue/green (RGB) format at 72 dots per inch (dpi) using an Epson 10000XL flatbed scanner. Dose maps were created with Film QA Pro software (Ashland Inc, Wayne, New Jersey) based on the red channel response rescaled by the reference films using a rational linear function fit to previously exposed calibration films. 5 Cross-sectional profiles of the dose maps were obtained using Film QA Pro. The data was normalized based on the maximum dose map value, or in the single case shown in Figure 3, by the maximum simulation dose value.
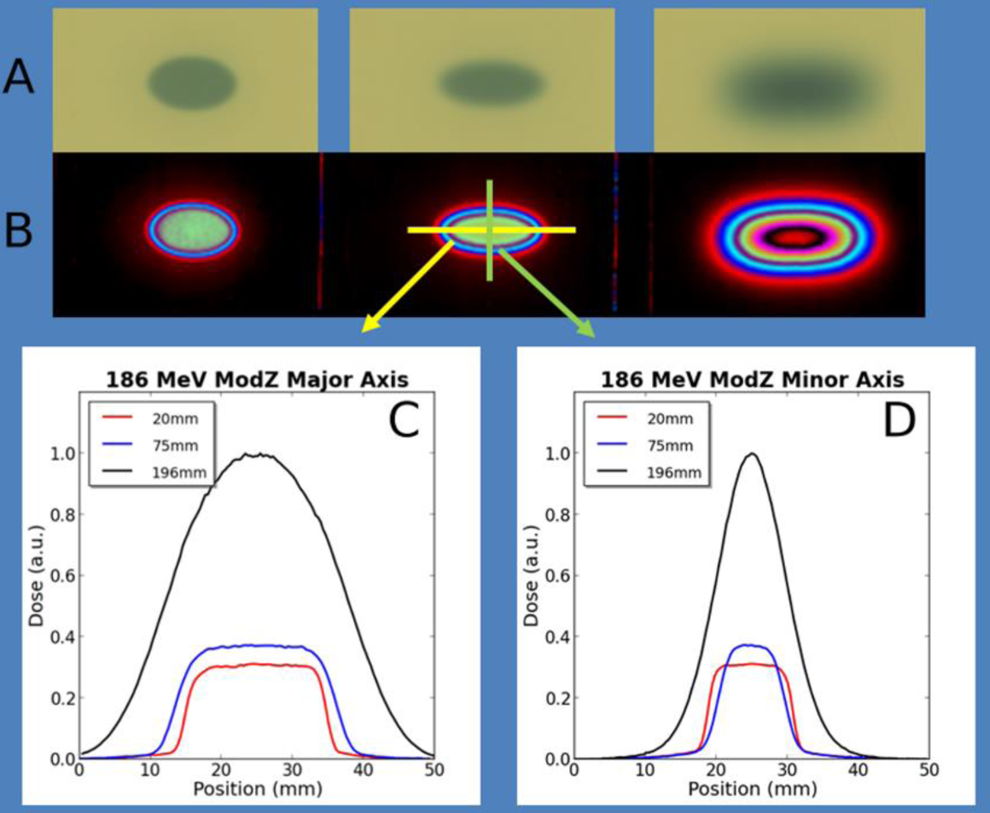
Beam spot symmetry. Beam spots (A) and (B) associated dose contours for successive exposed EBT2 film placed at 20, 75, and 196 mm (Bragg depth) depth in the water tank for an 186 MeV unmodulated proton beam with an 15 mm initial diameter. Major (C) and (D) minor diameter cross-sectional dose profiles (wrt to arrows) across the beam spots.
Monte Carlo Simulations
Monte Carlo computer simulations were performed with in-house software utilizing the Geant4 v9.5p01 toolkit. 6,7 Proton transport and interaction through the Gantry 1 treatment room beamline of the James M Slater Proton Treatment and Research Center was modeled similarly as described in Wroe et al. 8 However, similar to that described in McAuley et al, 1 a single quadrapole magnet was placed immediately upstream from the water phantom where dose was scored. The parameters of the magnet field and geometry were identical to those given in McAuley et al 1 (1.5 T at poles, 20 mm in diameter, and 40 mm in length) and the energies, phantom to magnet separation, etc. were modeled to match the analogous experiment setups for the proton data collection described above. Total dose was detected and scored in a terminal voxelized water phantom. Along the beam axis, the water phantom dimensions were either 160 mm (for 127 and 157 MeV beams) or 210 mm (186 MeV beams) and 100 × 100 mm in the transverse plane, and the voxel size was 0.25 × 0.25 × 0.25 mm. Longitudinal depth dose or transverse cross-sectional dose profiles from simulation data were calculated using in-house software.
Dose Profile Comparisons
Depth profiles were normalized with respect to dose at Bragg depth or COM of the SOBP, and transverse dose profiles were normalized by maximum dose for experimental and simulation data. Peak to entrance ratios were calculated as the ratio of maximum dose (unmodulated data) or dose at COM (modulated data) to dose at 10 mm water equivalent depth (WED). The R50 and R90 dose values were calculated from data points by linear interpolation. Simulation cross profiles were center-aligned with film diode cross profiles for analysis with full width at half maximum (FWHM) and full width at 90% maximum (FW90M) dose calculated for comparison.
Focused Experimental Versus Elliptically Collimated Simulated Beams
To better match the 90% RD contour line for the focused elongated beam spots at Bragg depth/COM and thereby provide a more suitable comparison with dose distribution properties for collimated beams, elliptically shaped collimated (ESC) beams were simulated and compared with focused diode data. Using an iterative process, the major (minor) axis FW90M diameters of ESC beams were compared with the FW90M diameters of the focused beams until they matched within 0.4 mm (0.2 mm). The final diameters of the elliptical collimators used were major (minor) axis diameter of 20 mm (4.5 mm) for unmodulated beams, and 25 mm (6 mm) for 15 and 30 mm modulated beams.
Results
Magnetically focused beams showed elongated beam spots with high elliptical symmetry. Figure 3 shows beam spots and associated dose distributions in exposed film placed at successive depths in the water tank. The high symmetry suggests focusing aberrations due to fringe fields of the magnetic assemblies or deviations from a pure quadrapole field are negligible for the experimental conditions. The absence of the latter is indicative of magnet quality.
Properties of depth dose profiles for diode and simulation data from 127, 157, and 186 MeV focused beams are shown in Table 1. Transverse dose profile properties for EBT2 film and simulation data from focused beams of each of these energies are shown in Tables 2, 3, and 4. Figures 4 and 5 show plots comparing the experimental and simulation data.

Dose profile comparison, 127 MeV. Relative dose profiles are compared with Geant4 simulation data for 127 MeV protons with an initial beam diameter of 15 mm. Each column contains data from unmodulated beams (panels A to D), beams of 15 mm modulation (E to H), or beams of 30 mm modulation (I to L). Depth dose profiles are shown in the top row for each modulation (A, E, and I) and compare data measured with the diode detector (red circles) and Geant4 simulations (solid black line). Corresponding transverse dose profiles are shown in the columns below (B to D, F to H, and J to L) and compare EBT2 film data with simulation data. Transverse profiles taken along the major and minor axes of the elliptical beam spots are plotted using black and red lines, respectively. Finally, transverse profile data from successively deeper depths in the water tank are presented as you move down each column, with the actual water equivalent depth (WED) designated in the title of each panel. G4Maj/G4Min, Geant4 simulation data along major/minor axis; FilmMaj/FilmMin, EBT2 film data along major/minor axis.
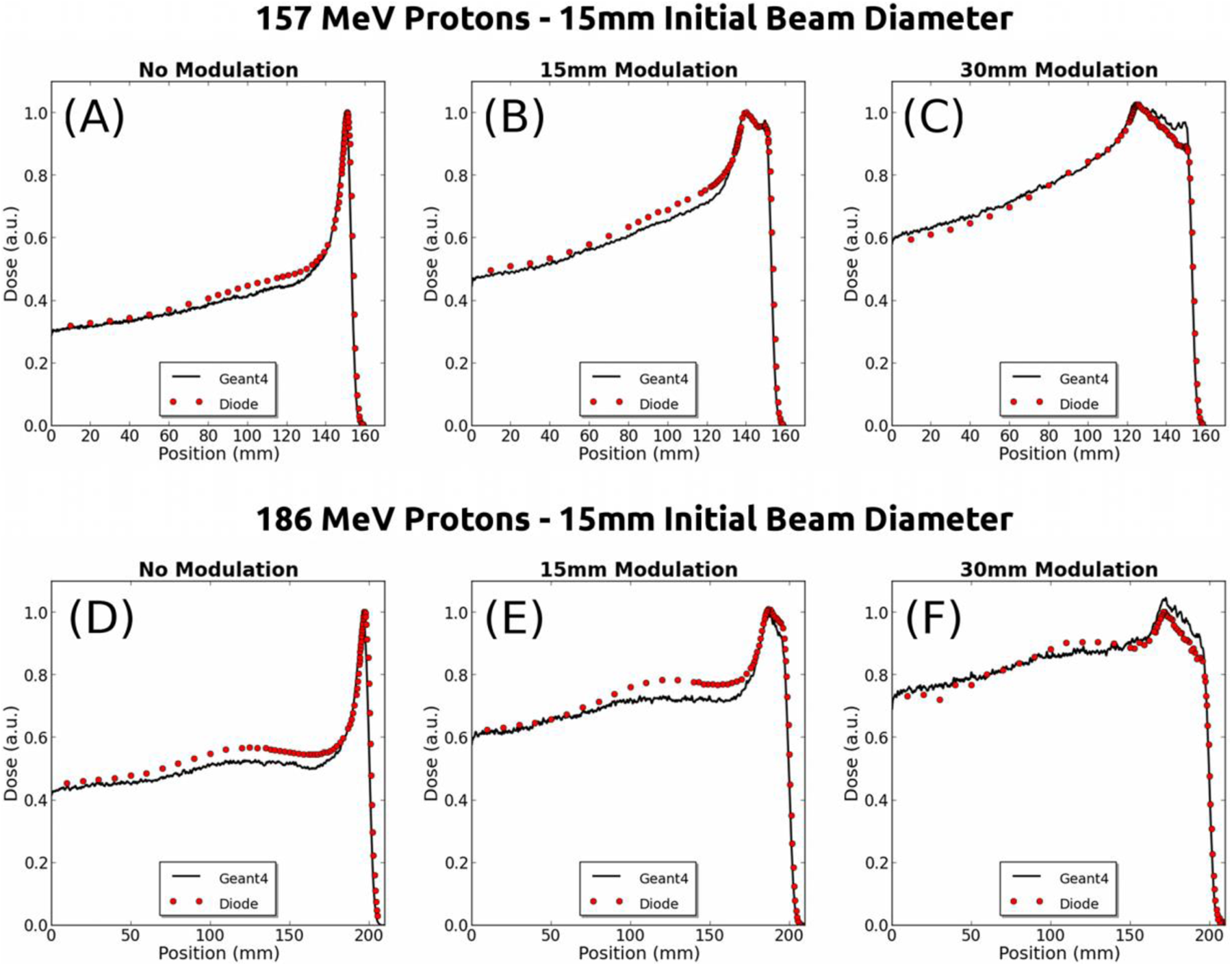
Depth dose profile comparison, 157 and 186 MeV. Depth dose profiles from diode data (red circles) are compared with Geant4 simulation data (solid black lines) for 157 MeV (panels A to C) and 186 MeV (D to F) protons with an initial beam diameter of 15 mm. Each column contains data from unmodulated beams (A and D), beams of 15 mm modulation (B and E), or beams of 30 mm modulation (C and F).

Focused versus unfocused 127 MeV beams. Depth dose profiles are shown of beams with an initial diameter of 15 mm. Each column contains data from unmodulated beams (A and D), beams of 15 mm modulation (B and E), or beams of 30 mm modulation (C and F). A to C, Diode data for focused beams (red circles) are compared to unfocused beams (ie, no magnet in beam line (black circles)) and Geant4 simulation data for collimated beams shaped by an elliptical collimator (blue solid line). (A to C) are plotted mutually normalized to dose at Bragg depth/center of modulation to reveal the superior peak to entrance dose properties of the focused beams. To compare the efficiencies of dose delivery, (D), (E), and (F) show simulations of focused, circularly collimated, and elliptically collimated beams without the normalization of (A), (B), and (C). Compared to elliptically collimated, the simulated focused beams are ~2× more efficient.
Depth Dose Profile Data for 127, 157, and 186 MeV Focused Beams.
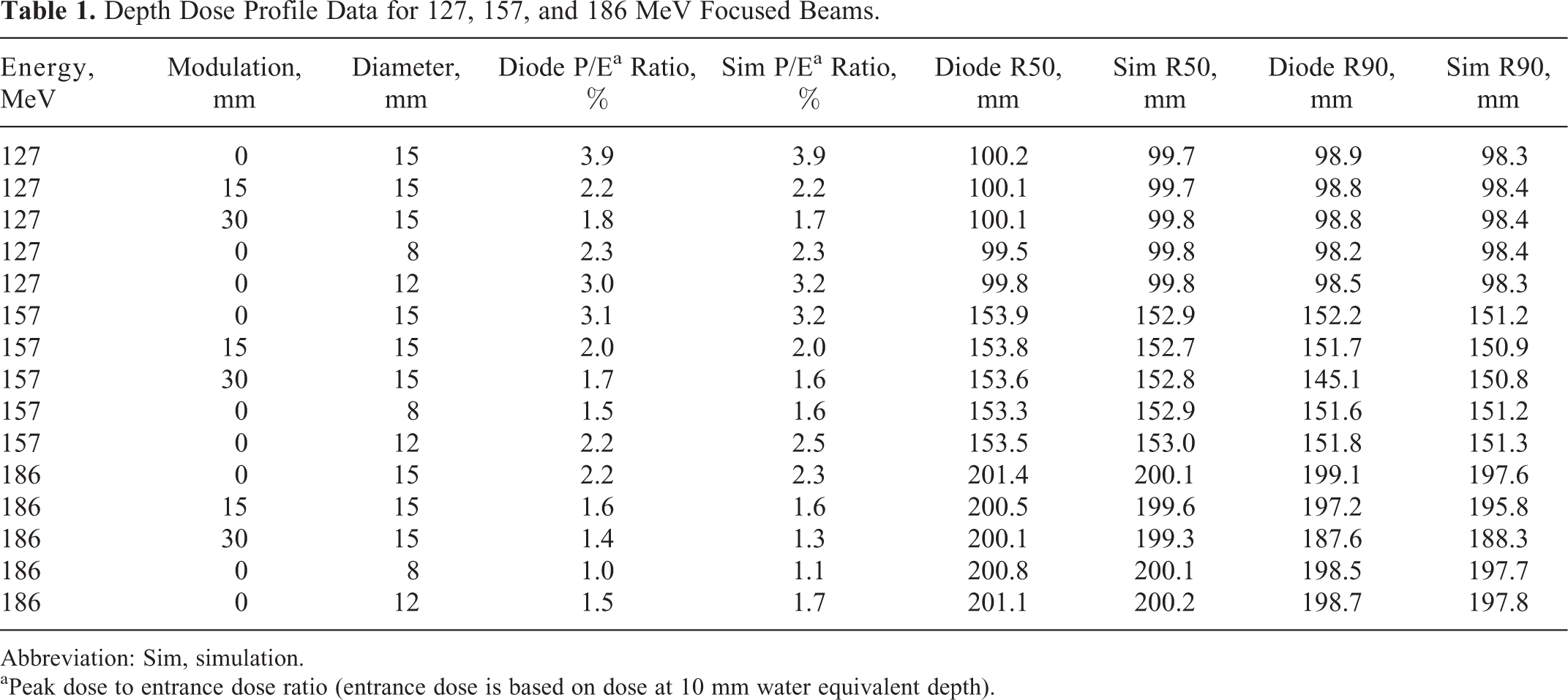
Abbreviation: Sim, simulation.
aPeak dose to entrance dose ratio (entrance dose is based on dose at 10 mm water equivalent depth).
Cross Profile Full Widths for Film and Simulation Data for 127 MeV Focused Beams.
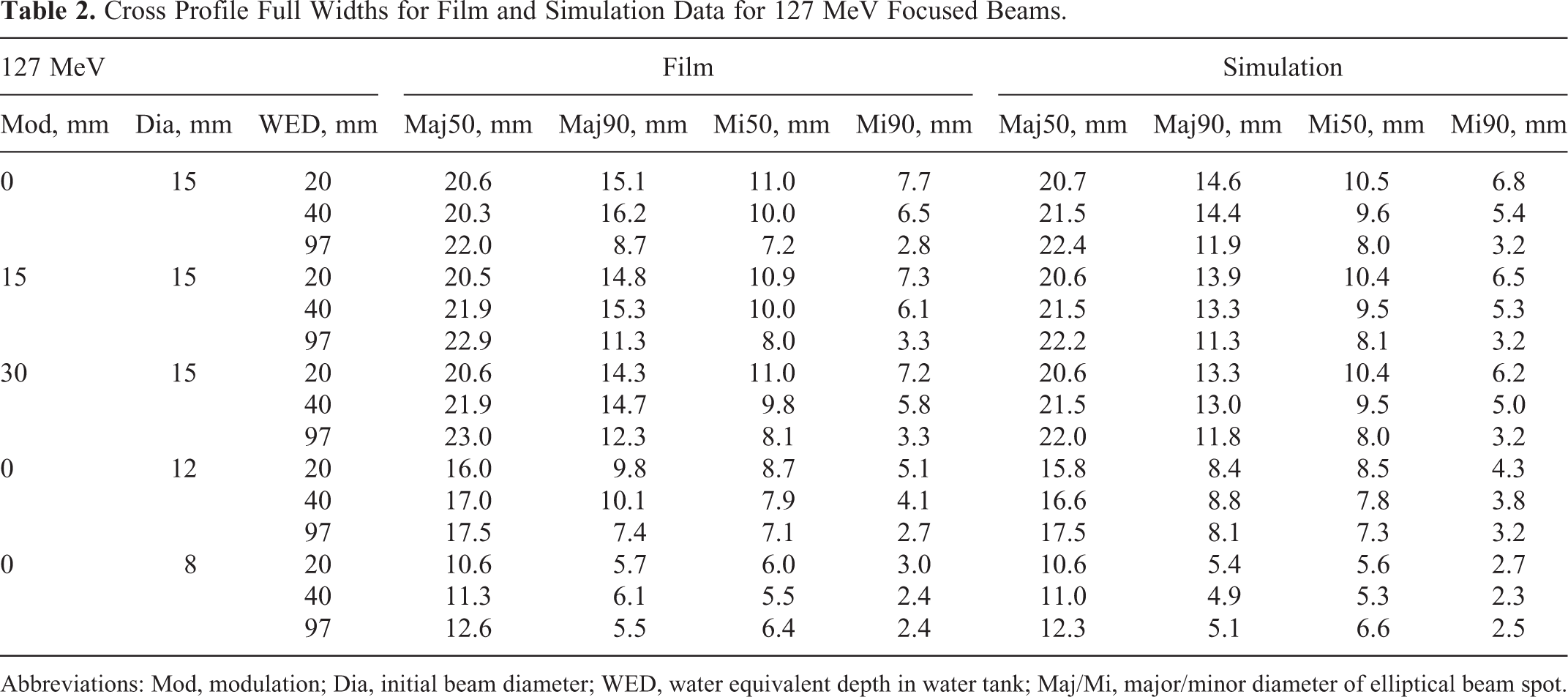
Abbreviations: Mod, modulation; Dia, initial beam diameter; WED, water equivalent depth in water tank; Maj/Mi, major/minor diameter of elliptical beam spot.
Cross Profile Full Widths for Film and Simulation Data for 157 MeV Focused Beams.

Abbreviations: Mod, modulation; Dia, initial beam diameter; WED, water equivalent depth in water tank; Maj/Mi, major/minor diameter of elliptical beam spot.
Cross Profile Full Widths for Film and Simulation Data for 186 MeV Focused Beams.

Abbreviations: Mod, modulation; Dia, initial beam diameter; WED, water equivalent depth in water tank; Maj/Mi, major/minor diameter of elliptical beam spot.
Peak to entrance dose ratios for diode and simulation data agreed within a few tenths of a percentage in absolute value for all energies, modulations, and diameters (Table 1). The average percent difference of diode versus simulation ratios was 3.6% for all diameters, and was 1.9% for 15 mm beams. R50 values agreed within 0.5 mm (0.3 mm average) for 127 MeV beams, within 1.1 mm (0.8 mm average) for 157 MeV beams, and 1.3 mm (0.9 mm average) for 186 MeV beams. R90 values agreed within 0.6 mm (0.3 mm average) for 127 MeV beams and 1.5 mm (1.1 mm average) for 186 MeV beams. R90 values differed within 1.0 mm (0.7 mm average) for 157 MeV with the exception of the 15 mm initial diameter 30 mm modulated beam (see Figure 5C) where divergence between experimental and simulation data in the distal SOBP plateau causes a R90 discrepancy of 5.7 mm. With this exception, the overall average discrepancies of R50 and R90 values are 0.7 and 1.0 mm, respectively, and R50 and R90 percentage differences between diode data and simulations are always less than 0.8%. Finally, it is worthy of notice that peak to entrance ratios, R50 values, and R90 values agree more closely between experimental data and simulations for lower energy, and R90 values also better agree for smaller diameter beams.
Tables 2 to 4 reveal that at Bragg depth/COM, major axis FWHM ranged from ~12.5 to 26 mm, while minor axis FWHM ranged from ~6.5 to 11 mm, depending on energy and modulation. The FW90M values at these depths ranged from ~5.5 to 12.5 mm and ~2.5 to 4.5 mm along the major and minor axes, respectively. The 127 MeV 15 mm transverse dose profiles shown in Figure 4D-L are typical of all focused beam energies and diameters as a whole in that film and simulation data generally agree better for minor than for major axis profiles, and minor axis profiles are more symmetric and better agree mid-range and at Bragg depth/COM. In addition, profiles are generally less symmetric near the top of the profile and occasionally an asymmetry results in an atypically large difference between film and simulation (eg, Figure 4L). Finally, film profiles tend to be slightly wider than simulation profiles, especially for higher dose values and at entrance and mid-range WED. These features are consistent with the quantitative data given in Tables 2 to 4. For example, the average differences (and standard deviation [SD]) between all experimental and simulated minor axis FWHM and FW90M profiles are 0.20 (0.18) and 0.76 mm (0.57 mm), respectively, whereas the major axis full width averages (and SDs) are larger: 0.63 (0.52) for FWHM and 1.36 mm (0.51 mm) for FW90M. That FW90M average differences are larger than FWHM width differences is consistent with a greater asymmetry and generally wider film profiles for higher dose values. There are two instances where major axis FW90M differences are greater than 3 SD above the average (3.2 and 3.3 mm). However, all of the 43 remaining cases in this category fall within 1.3 SD (2.0 mm) and the former 2 cases clearly involve anomalies in the film data (eg, asymmetry). Minor axis FWHM, FW90M average differences (SD) for entrance dose (ie, 20 mm WED) are, respectively, 0.38 (0.16) and 1.05 mm (0.40 mm). These values are larger than corresponding values for mid-range and Bragg/COM depths: 0.22 (0.22) and 0.42 mm (0.32 mm), respectively. Finally, a careful examination of Tables 2, 3, and 4 reveals that film full widths (both FWHM and FW90M) are larger than 71% of their counterpart simulation widths overall (0.73 mm average; 0.52 mm SD), and entrance and mid-range full widths are larger 84% of the time (0.73 mm average; 0.51 mm SD). The generally good agreement of depth dose data acquired by the diode detector and cross dose profile data obtained by EBT2 affirms the utility of the Monte Carlo simulations as a tool to investigate competing putative magnetic system designs and their resulting dose distributions in silica, and thus inform final design decisions.
Examination of Table 1 and Figures 4 and 5 also reveals that peak to entrance ratios tend to decrease with modulation as well as with energy. This is expected and can be explained because the extent of Coulomb scattering increases with energy (particle range) and modulation, and the extent of focusing decreases with energy for a given magnet. Also noteworthy in the 157 and 186 MeV depth dose profiles (Figure 5) are the decreasing slopes of the plateaus of the SOBPs of the modulated beams. This feature is essentially absent in the 127 MeV beams (Figure 4; see Discussion). Finally, Figure 5 also reveals a convex inflection in dose at mid-range depths for 157 and (especially) 186 MeV focused beams. This feature is apparently enhanced for the smaller diameter 8 and 12 mm beams of these energies (see Figure 7), and barely visible for 8 mm 127 MeV beams (see Figure 7A). Its origin can be explained by mid-range protons accelerated toward the beam axis in the presence of both increased outscatter due to the greater range of the higher energy protons and lateral particle equilibrium breakdown present for the smaller beams (see Discussion).

Depth dose comparison by initial beam diameter. A to C, Depth dose profiles for 127, 157, and 186 MeV protons within initial beam diameters of 8, 12, and 15 mm are compared for unmodulated focused beams. D, Profiles for simulations for focused 186 MeV beams of 8 mm initial diameter comparing magnets with gradients of 120 T/m (red trace) and 150 T/m (used everywhere else in this study). See text for details.
Diode depth dose data for 127 MeV 15 mm initial beam diameter unfocused beams are listed in Table 5 and compared with 127 MeV 15 mm diameter focused beams in Figure 6. Compared to unfocused beams, peak to entrance depth dose ratios were 11%, 14%, and 12% larger for 0, 15, and 30 mm modulated beams, respectively (compare Tables 1 and 5). However, when compared to the simulations of elliptically collimated unfocused beams (see Discussion), depth dose ratios were, respectively, 38%, 29%, and 26% larger (Figure 6A-C; compare Tables 1 and 5). Figure 6D-F shows simulation data for focused, unfocused (ie, circularly collimated), and elliptically collimated beams normalized per particle. Based on this simulation data, the expected gain in efficiency for the focused beams is ~2× greater than the elliptically collimated beams. These results suggest that the use of rare earth magnet assemblies could reduce skin dose and beam number while delivering enhanced dose to narrow elongated targets in less time than collimated beams.
Depth Dose Profile Data for 127 MeV Collimated Beams.

aPeak dose to entrance dose ratio (entrance dose is based on dose at 10 mm water equivalent depth).
bDimension of elliptically shaped collimator along major/minor axes.
Figure 7A-C displays depth dose profiles from diode data of focused beams of initial diameters 8, 12, and 15 mm plotted on the same axis for each energy (127, 157, and 186 MeV) for comparison. The degradation of the peak to entrance performance with increasing energy and decreasing diameter is apparent and expected. However, the simulation data shown in Figure 7D reveal that peak to entrance ratios can be improved by an appropriate choice of magnet and setup parameters: simulations of 186 MeV 8 mm beams, a magnet of 0.65 T, and a bore of 5 mm yield an approximately 10% larger peak to entrance ratio (however, see Discussion).
Discussion
A primary clinical goal overarching this project was to create narrow elongated proton beams of elliptical cross-section with superior dose delivery characteristics compared to current proton radiosurgery delivery modalities (eg, collimated beams). Such beams could find application in novel proton functional and standard radiosurgery treatments in or in close proximity to critical structures such as the spinal cord. Previous computer simulations suggested that focusing magnets made of rare earth permanent magnetic materials could produce beams with the desired properties. 1 In the present work, experiments with actual prototype magnets were performed using energies and modulations relevant to clinical radiosurgery applications. The focused beams produced narrow elongated beam spots of high symmetry. Dose distributions from the focused beams were in good agreement with analogous Monte Carlo simulations. Compared to unfocused beams and target-matched unfocused simulations, the focused beams showed larger peak to entrance ratios, and target-matched focused simulations showed more efficient per-particle dose delivery. These advantages in dose distribution properties and efficiency can be attributed to the acceleration of protons in the transverse plane due to the magnetic field. In addition, while entrance dose increased in the focused beams with decreasing initial beam diameter, simulations of focusing magnets with appropriately chosen parameters (ie, pole field strength and cylinder diameter) produced beams with improved ratios.
Both our previous simulations and those performed in the present study consisted of proton beams focused by a single idealized magnetic cylinder, that is, no fringe field and perfect quadrapole fields. 1 Theoretical K = 3 (quadrapole) Halbach cylinders consist of material with a magnetization that continuously varies over 3 full cycles around the circumference of the inner cavity and has a zero axial component. 2 The prototype magnets used in the present study, however, were constructed from 24 wedge-shaped segments of uniform magnetization. This discrete approximation as well as imperfections in the manufacturing process would be expected to result in aberrations from a pure quadrapole field and deviations from elliptical shape and spot/or asymmetry, and additional asymmetries could also be introduced from finite fringe fields. 9,10 For example, instead of elliptical beam cross-sections, large higher order multipole components (sextupole, octupole, etc) would tend to produce obvious spoked or star-shaped cross-sections. 9 However, such features were absent in our results, and our magnetically focused beams showed beam spots with high elliptical symmetry. Under the present experimental conditions (eg, a range of energies relevant to radiosurgery) the effects from magnet fringe fields, manufacturing defects, or higher order multipoles appear to be negligible. Therefore, these results suggest that rare earth magnetic assemblies similar to our prototypes can be practically manufactured at a sufficient level of quality to produce elongated spots of high symmetry for radiosurgery energies and applications.
Such magnets can currently be manufactured to suitable clinical specifications for costs of the order of thousands of dollars. In addition, because the prototype focusing magnets are constructed using permanent magnet material and are of Halbach design, no power or cryogenic coolants are needed for their operation nor are high fields present along with the requisite shielding. Not only is this important for cost reduction and safety, but it simplifies the incorporation of the magnets into a cone that could easily mount on the terminal end of common existing hardware, for example, in place of the aperture in a standard proton treatment nozzle. Thus, the key results of the present research suggest that use of rare earth magnetic assemblies is a feasible and inexpensive method to produce narrow elongated beams with reduced particle outscatter that tends to degrade the peak to entrance performance of small field proton beams.
The extent of the magnet focusing effect depends on several parameters, including particle energy, displacement and divergence, magnet parameters (eg, field strength and effective length), and particle drift space. In addition, as protons enter tissue, Coulomb scattering and energy deposition due to electromagnetic and nuclear interactions involving primary and secondary particles determine the dose deposition in and outside of target as a function of tissue composition and beam properties. Finally, most clinically useful beams utilize a spectrum of energies to produce a SOBP to cover a therapeutic target, and treatment beams are generally optimized based on target size and depth. Because of this complexity, the best choice of parameters in a magnet focusing system may not be intuitively obvious. In addition, these complicated interactions cannot be practically modeled analytically, and such analyses become the purview of Monte Carlo simulations. It is therefore an important result that the Monte Carlo simulations in the current study show good agreement with experimental data. Such simulations provide a priori guidance to magnet system design, potentially reducing cost and effort in the development of useful magnet focusing systems.
Peak to entrance depth dose ratios for diode data from focused beams were 11% to 14% larger (as a function of modulation) than diode data from unfocused beams of the same initial diameter (15 mm). This can be attributed to the focusing effect. However, it is important to note that the experimental unfocused collimated beams produced circular not elongated beam spots. Therefore, a more relevant comparison with the elongated focused beams requires a narrow elongated shaped collimator, such as the elliptical collimator simulated in our previous Monte Carlo studies. 1 Because particle outscatter tends to increase with narrower fields, the advantages in dose distribution under such an improved and more clinically relevant comparison are expected to be greater. Simulation data using such an elliptical collimator, where the 90% RD contours were matched at Bragg depth/COM with focused beams, produced peak to entrance ratios 26% to 38% larger for the focused beams. In addition, since the narrow collimators reduce particles from the beam, the focused simulated beams were ~2-fold more efficient in that fewer particles were needed to achieve the same dose. These results are similar to the 31% to 47% larger ratios and ~1.5× efficiency gains we reported previously for simulated focused beams. 1 Because of the good agreement between our Monte Carlo experiments and diode data, similar results are expected for experimental elliptically collimated beams. These results suggest that focused beams could reduce skin dose and beam number while delivering enhanced dose to narrow elongated targets in less time than collimated beams.
It can be seen from Figure 5 that depth dose profiles from experimental diode data as well as simulations show a decreasing slope in the SOBP plateau of the 157 and 186 MeV modulated beams. However, the slopes of the plateaus are relatively flat or only slightly decreasing in the 127 MeV modulated beams (Figure 4). Although the treatment nozzle setup for 127 MeV beams uniquely includes a ridge filter (several thin steel wires perpendicular to the beam designed to reduce jaggedness of the plateau), the down slope is best explained by increased scattering (due to longer particle range) and decreased focusing (due to energy). The sloped plateau is not generally a desirable clinical feature. However, the modulation wheels used in our treatment nozzle were optimized for passive and not actively focused beams, and we showed in previous simulations 1 that changing the modulation weighting could change sloped plateaus into flat plateaus. In addition, increasing the relative contribution of higher energy components while decreasing contribution of middle components that contribute to the convex inflection in dose seen in the present study could have an additional benefit in further increasing the peak to entrance ratios of the modulated focused beams and merits further study.
The dose distributions resulting from focused beams are affected by magnetic forces and multiple Coulomb scattering, and both phenomena depend on energy and beam diameter. The focusing power (ie, focal length) of quadrapole magnets depends on proton kinetic energy (see Equation 2 in McAuley et al 1 ) and the magnetic force experienced by a proton inside the magnet’s cavity is proportional to its radial distance from the magnet axis. 10 Therefore, the average force on a proton inside the magnet is proportional to the maximum radius of the beam, and the extent of focusing decreases as beam diameter decreases. In addition, higher proton energies have both higher momentum and greater penetration depth. Increased particle range implies more scattering events that tend to increase beam broadening. On the other hand, Coulomb deflections are smaller because of the higher momentum. Finally, net outscatter increases for smaller diameter beams as lateral particle equilibrium begins to break down. The interplay between scattering and focusing is perhaps most effectively illustrated in the present study by the convex inflection that, while invisible in the 127 MeV protons, becomes increasingly pronounced in the 157 and 186 MeV beams. The fact that focusing is actually greater for 127 MeV protons suggests that this feature results from the increased scattering away of protons that “reveal” the presence of the focused protons. Similar to the sloped plateaus discussed previously, the mid-range “bump” in dose would not generally be desirable. However, as also mentioned earlier, this could possibly be remedied by adjusting the modulation weighting. On the other hand, unlike the single magnet focusing performed in the present study that results in single-plane focusing, in multimagnet focusing, additional magnets would defocus proton away from the beam axis and thus tend to reduce the swelling in mid-range dose.
In the present study, we used a single prototype magnet for proton beams with 3 different initial beam diameters and 3 energies currently used in clinical radiosurgery applications at our institution and the range of penetration depths of protons with these nominal energies differs by up to 10 cm (eg, see Figure 7). Therefore it follows from the discussion immediately above, the relative extents of the focusing effect and multiple Coulomb scattering are weighted differently for each experimental case considered in this study. This is illustrated in peak to entrance ratios that decrease with energy and modulation (Figures 4 and 5) and beam diameter (Figure 7), and the aforementioned sloping SOBP plateaus and swelling of mid-range dose (Figures 5 and 7). However, by adjusting magnet, modulation, and setup parameters for each energy/modulation and diameter case, it may be possible to optimize the dose distribution properties for a given application. For example, Figure 7D shows how a smaller magnet gradient can lead to an improved peak to entrance ratio. In addition, because the reduced gradient was achieved using a magnet with a smaller bore and magnetic pole strength (5 mm and 0.6 T, respectively), less magnetic material is necessary and the resulting magnet would be smaller, lighter, and less expensive to manufacture. On the other hand, a smaller gradient would lead to wider and less elongated beam spots, which may not be desirable for a given treatment plan. Further study regarding the optimization of magnetic system parameters for specific cases relevant to potential radiosurgical treatments is warranted.
A single quadrapole magnet focuses in one plane longitudinal to the particle beam but defocuses in the other perpendicular plane. In this project, we exploited this property by using a single magnet to shape the beam to match narrow and elongated targets (eg, the spinal cord). However, radiosurgery targets such as metastases of the brain, liver, or lung are small and nominally spherical. To achieve more symmetrical beams spots, quadrapole magnetic focusing requires the use of at least two magnets in series, and stigmatic focusing requires 3 or 4 magnets. 9,10 The dose advantages observed in this study can be attributed to the acceleration of protons in the transverse plane that tends to counteract Coulomb scattering. This focusing effect is present when using more than one magnet, and similar dose and efficiency advantages are expected when focusing to symmetrical clinical targets. Because Bragg depth degradation due to particle outscatter tends to increase with decreasing field size, a multiple magnet system should be particularly beneficial to small spherical functional, stereotactic radiosurgery, and stereotactic body radiation therapy targets, and is the subject of ongoing research.
Conclusion
The magnetically focused beams produced by our prototype magnets produced elongated beam spots with high elliptical symmetry. Compared to target-matched unfocused simulations, the focused beams showed larger peak to entrance ratios and more efficient per-particle dose delivery. These advantages in dose distribution and efficiency can be attributed to the magnetic acceleration of protons in the transverse plane due that tends to counteract the particle outscatter that leads to reduced peak to entrance performance especially in small field proton beams. Taken together, our clinically relevant results suggest that rare earth magnetic assemblies are feasible and could reduce skin dose, the number of treatment beams required to achieve a suitable conformity index, and spare normal tissue and organs at risk while delivering enhanced dose to narrow elongated targets at an increased dose rate than collimated beams. Knowledge gained from the present study will inform the design of a prototype treatment cone that incorporates similar focusing magnets for irradiations of elongated as well as nominally spherical small volume radiosurgery targets.
Footnotes
Acknowledgments
We gratefully acknowledge time and expertise afforded by the Loma Linda University Medical Center James M. Slater Proton Therapy and Research Center accelerator team, Samuel Barnes, Anthony Teran, and Bob Jones, and the staff and engineers of Electron Energy Corporation.
Abbreviations
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research and/or authorship of this article: This project was sponsored by funding from the Department of Defense (DOD W81XWH-BAA-10 -1).
