Abstract
Objective:
The objective was to explore experiences of older adults who completed a 12-week telehealth-delivered multidisciplinary lifestyle intervention (MLI) and examine factors influencing continued use of MLI practices.
Methods:
We used thematic analysis to identify patterns in open-ended, postintervention survey responses in a randomized trial of telehealth-delivered MLI, including yoga, music therapy, cognitive training, and nutrition.
Results:
Participants (mean age 63) were predominantly female (82%) and white (77%). They reported high satisfaction with the telehealth-delivered format and content. Key themes included enrollment motivation, delivery preferences, session content feedback, facilitators of long-term behavior change, and implementation suggestions. All participants indicated a high likelihood of continuing lifestyle changes beyond the intervention period, with nutritional (86%) and cognitive training (64%) being most endorsed.
Conclusion:
Telehealth-delivered MLI was acceptable and well-received among neurologically at-risk older adults. Participant insights can inform more engaging and sustainable lifestyle programs to promote brain health and support healthy aging.
Keywords
Background
Neurological disorders among older adults are highly prevalent and costly.1,2 The prevention of major neurological disorders is an urgent need in a rapidly aging society. Recent research suggests multidisciplinary lifestyle interventions (MLI) as a promising route for preventing and slowing the progression of neurological disorders. 3 However, bringing MLI into clinical practice requires making it accessible and scalable. Telehealth has emerged as a widely used means of providing outpatient neurological care. Several studies show that telehealth is well received by patients and neurologists alike.4–7 Telehealth approaches can address structural barriers to in-person care by enabling participation among older adults with limited mobility, transportation constraints, or caregiving responsibilities. Therefore, telehealth-delivered (online) platforms provide an ideal technology for delivering MLI at the scale necessary to meet the demographic challenges and achieve American Academy of Neurology (AAN)’s national brain health vision by 2050. 8
This population-level scalability of telehealth-delivered MLI was recently demonstrated in a randomized controlled trial of ≥6,000 community-dwelling older adults in Australia with modifiable dementia risk factors. 9 As telehealth MLI delivery becomes more accessible and accepted, understanding older adults’ experiences is crucial to facilitating its integration into clinical practice. We have developed an MLI program that includes practices with evidence of effectively preventing or treating neurological disorders, specifically yoga, music therapy, cognitive training, and diet and nutrition.10–17
We aimed to understand the experience of older adults with the telehealth-delivered MLI program and its influences on the continuation of MLI practices. We hope these insights are used to improve the delivery and content of future telehealth interventions. By learning which practices participants are likely to continue, clinicians and researchers can better support patients and participants in making and maintaining lifestyle changes. Ultimately, effective telehealth-delivered MLIs could become a scalable tool for promoting healthy aging across diverse clinical settings.
Methods
STUDY DESIGN
This qualitative substudy was conducted within the intervention arm of the open-label Multidisciplinary Lifestyle Interventions for Neurological Disorders during the Silent (MINDS) phase randomized controlled trial (ClinicalTrials.gov: NCT05984056). The parent trial evaluates the feasibility and effectiveness of a 12-week telehealth-delivered multidisciplinary lifestyle intervention (MLI) for adults ≥50 years at risk for neurological disorders (dementia, stroke, Parkinson’s disease, epilepsy) based on validated risk factors (Fig. 1, Table 1). The MINDS study protocol and participant selection criteria were previously published. 18
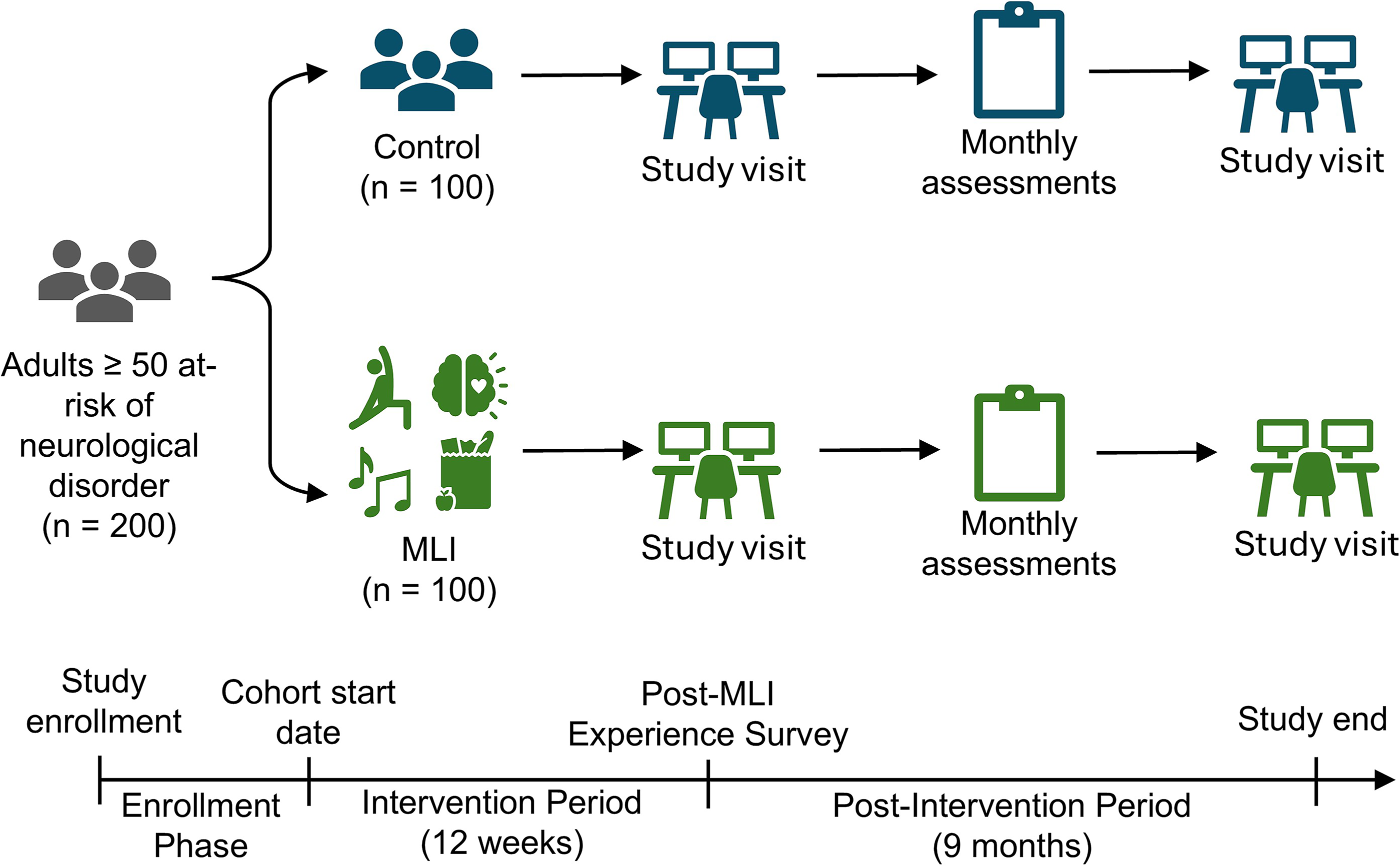
MINDS Study Protocol. Note the three phases for the study participants randomized to MLI, which include enrollment phase, intervention period, and postintervention period. The post-MLI Experience Survey is administered at the 12-week mark. Other study assessments include a 3-month study visit, health-related surveys, and a 12-month study visit. MINDS, Multidisciplinary Lifestyle Interventions for Neurological Disorders during the Silent; MLI, multidisciplinary lifestyle intervention.
Neurological Disorder Risk Factors and the Number of Participants with post-MLI Survey Responses for Each

Fazekas F, Chawluk J, Alavi A, Hurtig H, Zimmerman R. MR signal abnormalities at 1.5 T in Alzheimer’s dementia and normal aging. American Journal of Roentgenology. 1987;149 (2):351–356; doi: 10.2214/ajr.149.2.351.
Busch RM, Hogue O, Postle AF, Floden DP. Automated detection of cognitive impairment in clinical practice. J Neurol. 2024;271 (8):5187–5196; doi: 10.1007/s00415-024–12444-8.
Schoenberg M, Dawson K, Duff K, Patton D, Scott J, Adams R. Test performance and classification statistics for the Rey Auditory Verbal Learning Test in selected clinical samples. Archives of Clinical Neuropsychology. 2006;21 (7):693–703; doi: 10.1016/j.acn.2006.06.010.
Brumm MC, Pierz KA, Lafontant DE, et al. Updated Percentiles for the University of Pennsylvania Smell Identification Test in Adults 50 Years of Age and Older. Neurology. 2023;100 (16):e1691–e1701; doi: 10.1212/WNL.0000000000207077.
MLI, multidisciplinary lifestyle intervention; MRI, magnetic resonance imaging; EEG, electroencephalogram; BACH, Brief Assessment of Cognitive Health; RAVLT, Rey Auditory Verbal Learning Test; UPSIT, University of Pennsylvania Smell Identification Test.
This analysis addressed two questions: (1) What was the participant experience with the intervention, and how could it be improved? and (2) What influenced participants’ likelihood of continuing MLI practices postintervention? Control participants who did not receive telehealth-delivered MLI were not included. We employed an inductive, thematic analytic approach within a constructivist research paradigm to explore participant experiences with the MLI and their reported likelihood of continuing its practices postintervention.
The study was approved by the Cleveland Clinic Institutional Review Board (IRB #22-941). All participants provided written informed consent. This article was prepared in alignment with the Standards for Reporting Qualitative Research guidelines (full checklist in Supplementary Materials). 19
STUDY POPULATION AND SETTING
Participants were drawn from the first five cohorts of the intervention (telehealth-delivered MLI) arm conducted between August 3, 2023, and July 4, 2024. This timepoint was selected to capture a range of experiences, maintain a manageable dataset, and inform imminent studies of lifestyle interventions. The MLI comprised yoga, music therapy, cognitive training, and diet/nutrition education, delivered in weekly 2-hour group sessions (5–10 participants) over 12 weeks (Table 2). Our target sample size was 20 participants, consistent with guidance suggesting this is generally sufficient to achieve thematic saturation.20,21
DATA COLLECTION
Postintervention surveys were administered electronically via REDCap.22,23 The survey included open-ended, finite choice, and Likert-scale questions about expectations, preferred delivery mode, enthusiasm for continuing practices, and overall feedback (full survey in Supplementary Materials).
Telehealth-Delivered MLI Session Overview by Week
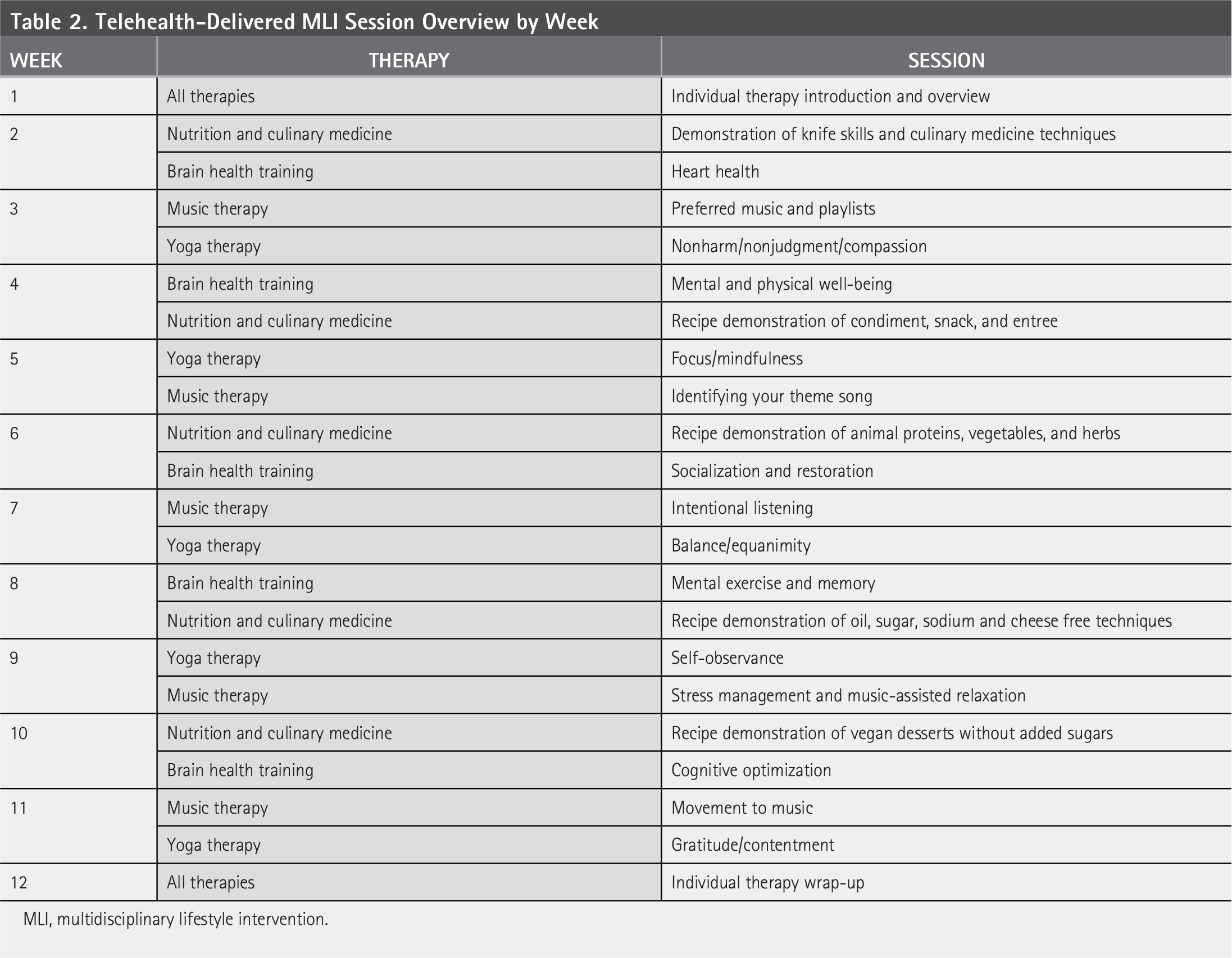
MLI, multidisciplinary lifestyle intervention.
DATA ANALYSIS
Between July 18 and October 31, 2024, we analyzed open-ended responses using thematic analysis, identifying patterns through initial coding and theme development. 24 We chose thematic analysis for its flexibility and suitability for survey responses of varying depth and for interpreting experiences relevant to intervention sustainability. 24
Two coders (S.T. and M.Z.) independently generated initial codes based on the open survey responses. One of the coders (S.T.) was the MINDS study data scientist and trained in thematic coding by the other coder (M.Z.), a qualitative research expert. A third team member (L.S.), with extensive qualitative and implementation research experience, reviewed and reconciled any coding conflicts. The team met biweekly to refine themes.
Results
PARTICIPANT CHARACTERISTICS
Of 31 eligible participants who completed all MLI sessions, 22 (71%) completed the postintervention survey and were included in the analysis. Survey participants were predominantly female (n = 18, 82%), white (n = 17, 77%), and non-Hispanic (n = 17, 77%), with a mean age of 63 years (Q1–Q3: 59–71) at enrollment. They were highly educated, averaging 16.7 years of education (Q1–Q3: 16–18). Demographic characteristics closely matched the full eligible sample, including nonresponders [mean age 63 years (Q1–Q3: 59–71); female (n = 25, 81%), white (n = 25, 81%), and non-Hispanic (n = 23, 74%)].
FINITE FEEDBACK
We asked finite choice and Likert-scale questions (1 = extremely unlikely, 10 = extremely likely) to assess participants’ overall experience and likelihood of continuing MLI practices. For “How likely are you to recommend a similar 12-week telehealth-delivered lifestyle intervention to a loved one in your age group?”, participants gave a median score of 10 (Q1–Q3: 8–10), with 18 (82%) rating 8–10 (Fig. 2A). For “How likely are you to continue some or all of these lifestyle modifications for one year or longer?”, participants gave a median score of 9 (Q1–Q3: 8–10), with the same proportion rating 8–10; no participants indicated a low likelihood (Fig. 2B).
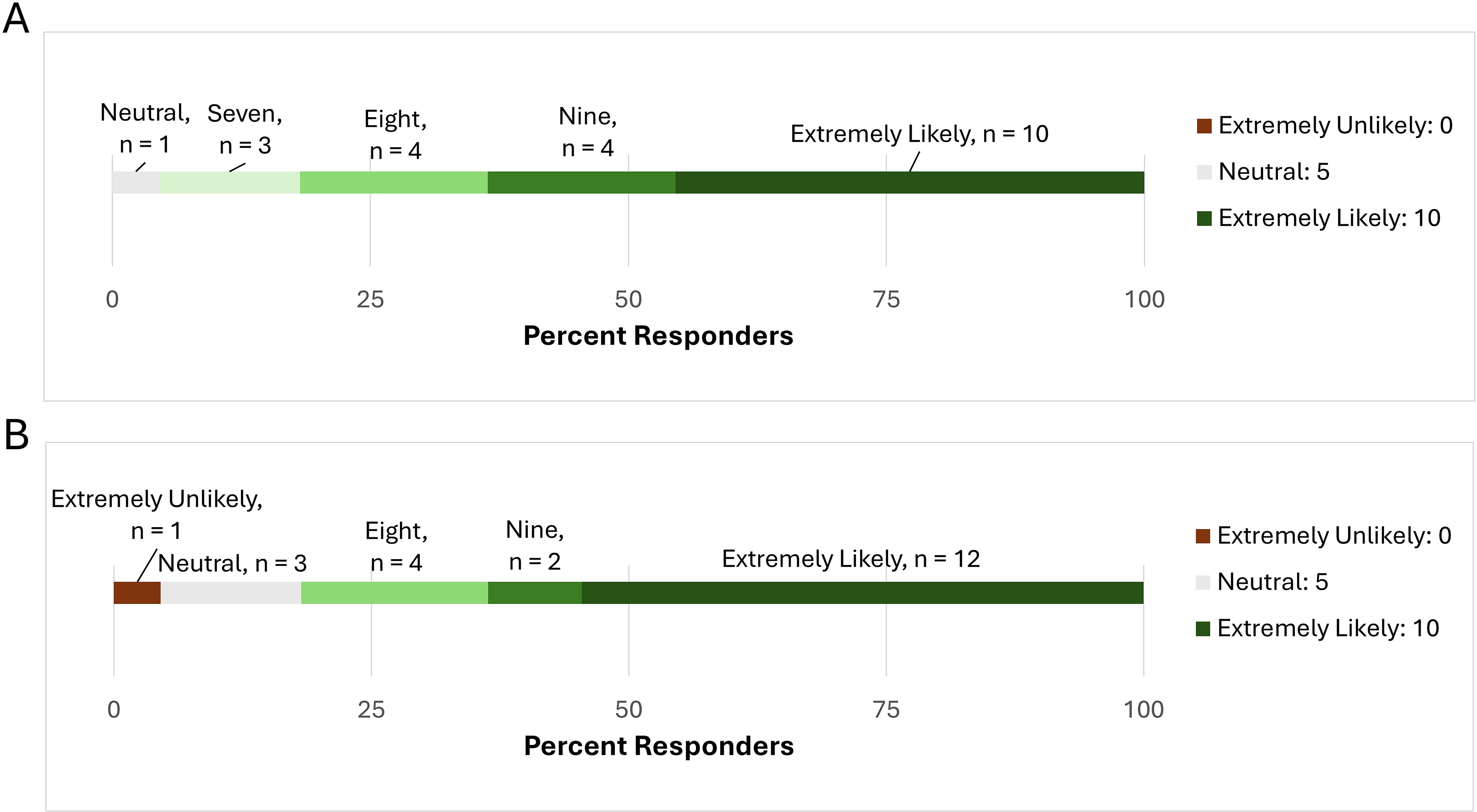
Participant likelihood to recommend the MLI program and to continue MLI practices. Percent of participants selecting a particular value on the Likert scale (ranging from 0: Extremely Unlikely to 10: Extremely Likely, with 5 as the neutral option) is shown for the questions. Counts for each response provided in annotations, and legend for the color scheme distinguishing between the response values is on the right.
When asked which components they would likely continue long term (multiple selections allowed), most participants chose nutrition (n = 19; 86%), followed by cognitive skills (n = 14; 64%), yoga (n = 11; 50%), and music therapy (n = 8; 36%). Six participants (27%) selected all four interventions; four (18%) selected cognitive skills and nutrition; and four (18%) selected nutrition alone (Fig. 3).
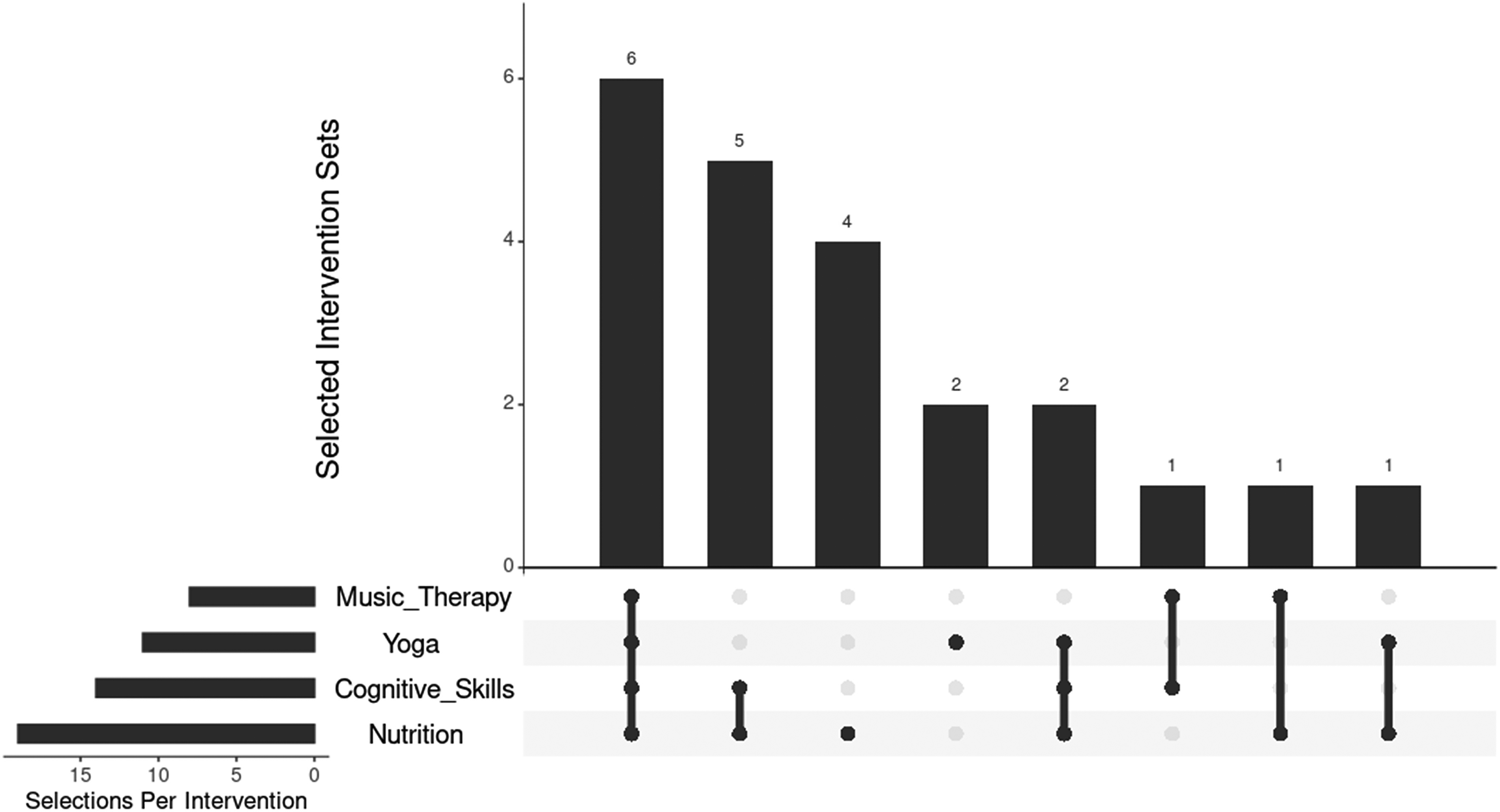
MLI practices participants report they are likely to continue long-term. Participant counts for the multiselection question “Which of the 4 interventions are you most likely to continue for the long-term?” are shown. Counts for each individual domain are shown in horizontal bar charts in the bottom left-hand corner. Counts for every combination of responses shown in vertical bar charts with the domains included in each set below the bars. MLI, multidisciplinary lifestyle intervention.
THEMATIC FINDINGS
We identified themes specific to each of the three phases of the study timeline (Fig. 4). “Study enrollment motivation” was the sole theme for the study enrollment phase. We defined two themes for the MINDS intervention phase: “timing and format of intervention delivery” and “session content feedback.” The former included two subthemes of “time commitment” and “format of delivery: telehealth-delivered vs. in-person trade-offs.” For the postintervention study phase, we defined two themes: “facilitators for lifestyle change implementation” and “suggestions for lifestyle change implementation.” Themes and representative quotations are provided in Table 3.
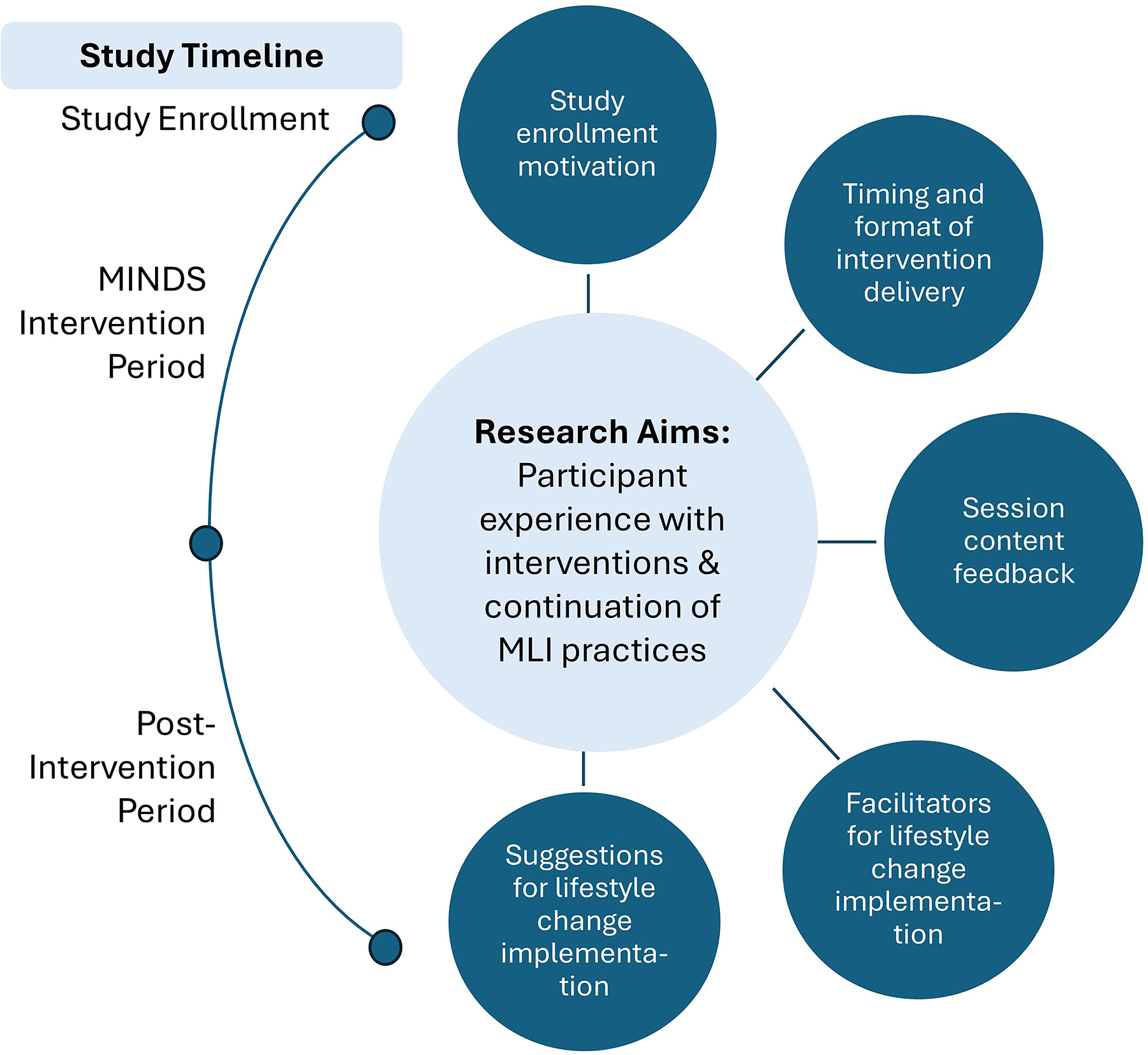
Summary figure of general thematic analysis of final themes. The themes all radiate out from our central research aims. The study timeline on the left shows how the themes group into each study phase. Study enrollment refers to the period of recruitment and enrollment of participants into the study. The MINDS intervention period starts with the first intervention session and lasts 12 weeks. The postintervention period refers to any time after the 12-week mark. MINDS, Multidisciplinary Lifestyle Interventions for Neurological Disorders during the Silent.
Themes with Corresponding Code and Example Quotes
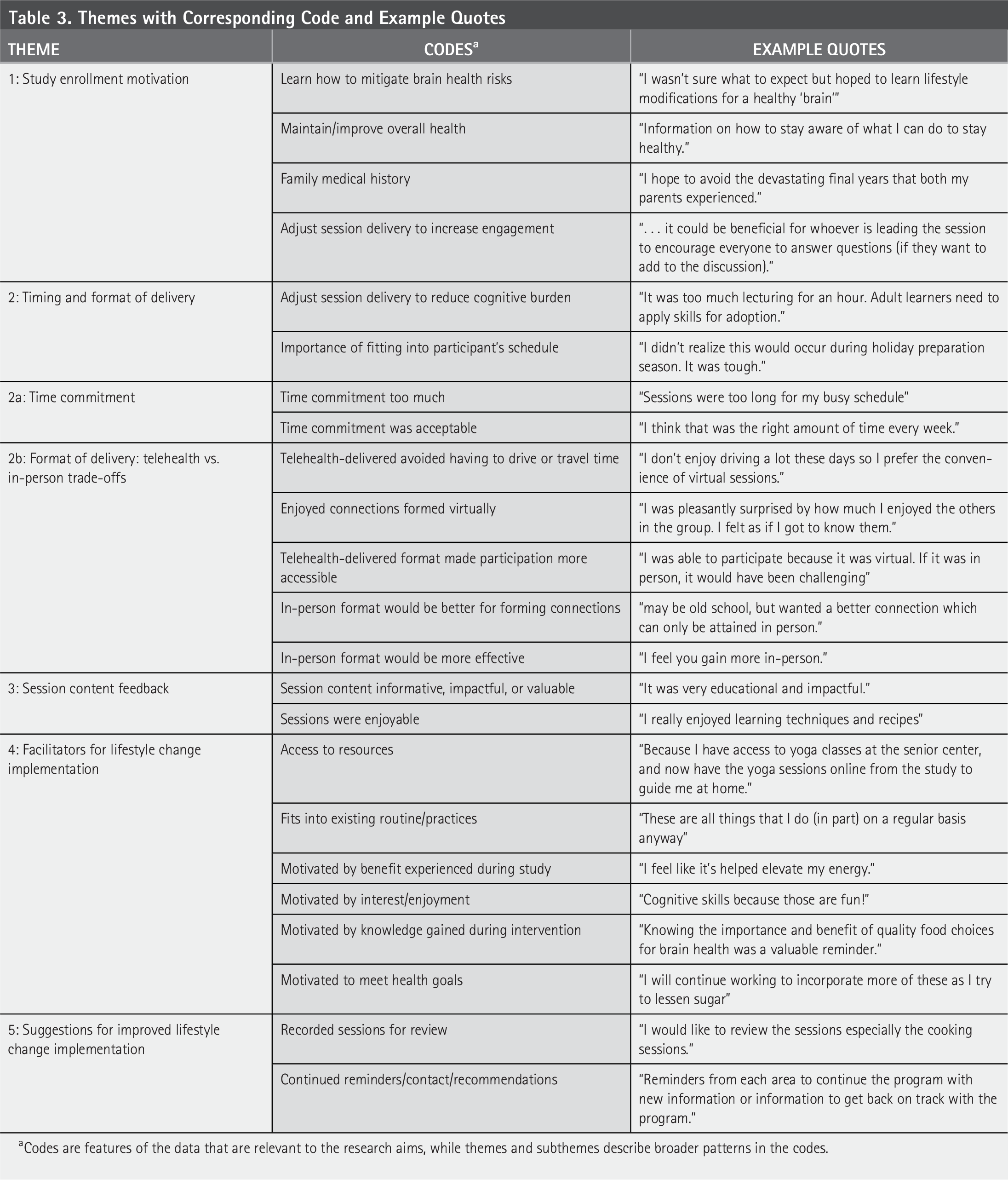
Codes are features of the data that are relevant to the research aims, while themes and subthemes describe broader patterns in the codes.
Study enrollment motivation
Although the survey did not explicitly ask about enrollment reasons, participants described motivations that contextualized their expectations for MLI sessions. Some sought strategies to support brain health, such as reducing the risk of stroke or dementia: “I hoped to learn healthy habits to help me delay any onset of a stroke or dementia.” Others joined to maintain or improve overall health, or because of family medical history. One participant noted, “I hope to avoid the devastating final years that both my parents experienced.”
Timing and format of intervention delivery
Participants discussed how timing and format influenced engagement and accessibility. Some suggested more prompts from session leads, a chat feature, or greater emphasis on skill application to reduce cognitive burden. Others noted that scheduling mattered and avoiding “supper time zone” or busy periods like “holiday preparation season” helped participation.
Time commitment
Opinions varied: some found the weekly two-hour sessions too demanding, while others considered the commitment reasonable.
Format of delivery: Telehealth-delivered vs. in-person trade-offs
When asked about delivery preference, 82% (n = 18) chose virtual. Participants highlighted connections only possible with the telehealth-delivered format, with one participant saying they “enjoyed meeting people from other areas around the country.” One participant felt in-person meetings, at least for kickoff and closing sessions, would foster deeper relationships. Participants frequently cited the convenience of avoiding travel. One noted that in-person sessions “would add so much time and aggravation.” For those living far from the study site, telehealth-delivered delivery made participation feasible. Some participants suggested that an in-person format would be more effective for specific aspects of the intervention, like yoga or culinary teaching. Other participants generally felt that in-person sessions would allow for greater focus and effectiveness.
Session content feedback
Participants described the session content as informative, valuable, and enjoyable. One highlighted “knife skills, yoga, music therapy, and brain exercises” as especially useful, while another found the program “very educational and impactful.” Others emphasized enjoyment, with one calling it a “wonderful experience” and noting they “will miss the weekly telehealth-delivered interventions with the Cleveland Clinic staff.” Feedback on specific improvements varied, including demonstrating all yoga poses, offering more electronic resources, and providing guidance on shopping for foods related to the nutrition lectures.
Facilitators for lifestyle change implementation
For the postintervention period, the first theme we defined related to factors that facilitate the continued implementation of MLI changes. Some participants highlighted access to resources outside of the study that would allow them to continue certain aspects of the MLI practices, like “access to yoga classes at the senior center,” as well as resources from the study itself, including the online yoga sessions, diet checklist, and study guidebook. Some participants indicated they would continue practices that fit into their existing routine or activities they had been working on prior to the start of the study.
While not explicitly asked about motivations for continuing intervention practices, some participants indicated they were motivated to continue due to the benefits of the lifestyle practices that they experienced during the intervention phase. For example, one participant specified, “Regular use of mindfulness apps has been helpful for my sleep and breathing exercises have helped me deal with stressful situations.” Other participants were motivated to continue the practices they were interested in or enjoyed. For example, one participant mentioned, “I love cooking so nutrition is easy.”
Some participants reported being motivated by knowledge gained during the intervention. For instance, one participant said they would continue the nutrition and diet practices they learned because “the importance and benefit of quality food choices for brain health was a valuable reminder.” Other participants alluded to learning about multidisciplinary approaches as key. For example, one participant selected that they will likely continue all four intervention domains long-term and explained each “serve individual purposes to help my body feel and move better.” Finally, some participants indicated that they were motivated to continue practicing MLI to meet health goals, including reducing sugar intake and medications.
Suggestions for improved lifestyle change implementation
Participants were asked directly what would be helpful in continuing the MLI practices. Some participants specified that having recorded sessions of the intervention to review moving forward would be helpful. Others suggested continued reminders, contact, or recommendations after the intervention phase. Another spoke specifically to more personalized recommendations as useful moving forward, suggesting “additional yoga recommendations as skill levels improve.”
Discussion
In this qualitative study of neurologically at-risk older adults, we explored experiences with a 12-week, telehealth-delivered MLI program. Participants reported positive experiences and high likelihood of continuing lifestyle changes, suggesting strong receptivity to telehealth delivery of an MLI to improve brain health. Our findings contribute to a growing body of evidence demonstrating that telehealth platforms can effectively deliver behavior-based preventive care to aging populations, overcoming barriers of distance, mobility, and scheduling that often limit participation in in-person programs.4,5,7,9,25,26
Furthermore, our study offers critical insights into older adults’ preferences that could be incorporated in future clinical practice and studies to improve satisfaction and engagement with telehealth-delivered MLI. By examining participants’ perspectives on accessibility, engagement, and adherence within a telehealth framework, this study adds needed qualitative evidence on virtual health delivery in neurologically at-risk populations.
Participants described multiple benefits of telehealth delivery, including convenience, accessibility, and the ability to connect with geographically diverse peers. While most participants preferred fully telehealth-delivered sessions, some felt in-person contact could foster stronger connections. Participants also suggested that at least one in-person session could be helpful for hands-on components like yoga or culinary coaching. These perspectives support a hybrid model that maintains the accessibility of delivery while offering optional in-person touchpoints to enhance engagement with MLI programs involving physical activities, an approach increasingly recommended in telehealth design for older adults. 27 Participant feedback on intervention content and delivery included appreciating access to experts and an enjoyable and engaging experience, similar to a telehealth-delivered lifestyle intervention study in chronic pain management. 28
Our study identified multiple facilitators of long-term adherence, including access to resources/infrastructure, positive view of physical changes, and positive opinions about the intervention content, supported by the literature on use of lifestyle interventions for weight-loss. 29 In addition, we found that inherent enjoyment of practices as well as the adaptability of practices to participants’ existing routines are important facilitators. General self-management skills and personalized recommendations could contribute to increased facilitation in future applications of MLI in clinical care.28,30 These themes align with prior research on telehealth-based behavioral interventions showing that reinforcement through digital materials, structured follow-up, and personalized recommendations enhances long-term adherence. 31
The use of lifestyle interventions in nonneurological specialties like cardiology is well-established. 32 A 2024 systematic review found that group-based internet lifestyle interventions offer a scalable, cost-effective option that effectively improves smoking cessation, physical activity, and obesity outcomes. 33 However, MLI’s use in neurological care is a nascent field, and therefore, it is crucial to learn if synchronous (live, healthcare provider-led) telehealth-delivered MLI programs can provide long-term change in brain health promoting lifestyle. The participants in our study, at the end of 12 weeks, found the experience rewarding enough that most of them were highly likely to recommend a similar program to their loved ones.
The MLI program also made a subjective benefit to the participants’ sense of well-being and improved knowledge, given their enthusiastic endorsement of goals to continue one or more lifestyle changes for a year or longer. Dietary and nutritional changes followed by cognitive training were most likely to be pursued long-term (86% and 64% of participants, respectively). The continued use of music therapy-based changes was least likely among our sample. The reasons for lower preference for one versus other lifestyle interventions were not investigated here but may need further study, especially given that NIH has launched the Sound Health Initiative to stimulate the use of music-based intervention for brain disorders of aging. 34
With national research organizations increasingly funding MLI and cognitive training studies aimed at improving brain health and AAN’s related call to action, lifestyle interventions are increasingly promoted by healthcare organizations and getting incorporated into neurological care programs.35–40 In such an environment, it is crucial to understand the target population’s perspective of MLI and its mode of delivery. We found that participants enrolled in the MLI program due to personal health concerns, including a family history of neurological disorders and individual risk factors identified during recruitment. The awareness of the latter, such as white matter disease, likely motivated participation, consistent with prior research in nonneurological specialties. 29
Although our study did not specifically assess telehealth-delivered MLI enrollment strategies, our findings suggest that designing recruitment materials that emphasize actionable health benefits and patient-specific risk factors could enhance study enrollment in future telehealth-based MLI programs and encourage lifestyle changes as part of clinical care.
LIMITATIONS
One major limitation of this study is that we only surveyed individuals who chose to participate in an MLI program, which may have inflated positive feedback. Some eligible individuals with neurological disorder risk factors declined participation, potentially due to the time commitment required or a lower inherent interest in MLI. Such factors could limit broader adoption in clinical settings. In addition, the MINDS sample was composed primarily of highly educated, higher-socioeconomic status (SES) participants with access to resources such as time, reliable internet, and digital devices. This profile may not reflect the broader population, particularly individuals from disadvantaged backgrounds. Consistent with prior literature on the SES-linked “digital divide” in health technology adoption,41,42 these participants may have had more favorable experiences with telehealth-delivered MLI than those with fewer resources.
Nonetheless, our goal was to analyze and learn from the experience of those who were able to enroll and complete telehealth-delivered MLI. A recent scoping review of telehealth-delivered lifestyle interventions for individuals with low SES identified barriers such as technology access and digital literacy, as well as facilitators including personalized recommendations and regular reminders. 43 In alignment with those findings, several participants in our study suggested these same strategies, indicating their potential utility across diverse socioeconomic groups. Active recruitment and technology support may be additional strategies for engaging participants and patients with increased socioeconomic deprivation. 43
Despite these limitations, our results have important implications for future telehealth studies and clinical programs promoting brain health. Incorporating participant-driven feedback can improve lifestyle intervention program design, particularly in session delivery, resource availability, and follow-up support. Offering flexible scheduling, hybrid formats, and tailored resources could enhance recipients’ engagement and adherence. These findings can play a critical role in starting our journey toward accomplishing the aims of the AAN’s Brain Health Initiative 8 and advance the role of telehealth in neurological preventive care.
Conclusions
We found that the neurologically at-risk older adults’ experiences of a telehealth-delivered MLI intervention were overall positive. In addition, these individuals indicated that some or all lifestyle changes learnt and incorporated into their daily routines during the 12-week program were likely to be continued long-term. Based on their feedback, we believe that telehealth-delivered MLI to older adults is both feasible and effective in engaging its recipients. Finally, the participants provided valuable insights on how to improve the design and administration of future telehealth-based lifestyle intervention programs that allow us to reduce the burden of neurological disorders and achieve optimal brain health.
Trial Registration
The associated MLI clinical trial was registered with ClinicalTrials.gov (ID NCT05984056, submitted 2023-08-02).
Authors’ Contributions
S.T., M.Z., and V.P. contributed to the study concept and design; data analysis and interpretation; and drafting and revising the article, including medical writing for content. S.T. and A.L. had major roles in data acquisition. A.L. and L.G. contributed to article drafting and revision and data acquisition. I.P., M.A., S.K., S.D., K.A., A.S., G.S., J.P., P.B., R.W., and H.W. made major contributions to data acquisition. S.D., K.A., J.P., and L.S. contributed to the study concept and design. L.S. contributed to study design, data analysis and interpretation, and article revision. V.P. also participated in drafting the article and provided overall supervision. All authors reviewed the article.
Footnotes
Acknowledgments
The authors thank Vonita Burke, Johanna Goldfarb, Valerie Williams, Judi Bar, and Sally Sherwin for their contributions to the design and delivery of the yoga portion of the intervention, as well as Debbie Bates and Katie Platz for their design and delivery of the music therapy portion of the intervention.
Author Disclosure Statement
The authors declare that they have no competing interests.
Funding Information
Data Sharing Statement
The sharing of anonymized participant-level data and statistical code from the study will be considered based on a reasonable request from a qualified investigator for rigorous scientific inquiry.
Supplemental Material
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
