Abstract
This paper presents a study of heat-setting treatment on tubular polydioxanone stents which can be used as intestinal implants. Two PDO monofilaments with linear densities of 100 ± 2 and 150 ± 2 tex respectively were used for producing a set of weft-knitted tubular stents using a small-diameter, circular weft knitting machine. The heat-setting treatment was used for the stents to restore a tubular shape. The physical, mechanical and thermal properties of the stents were examined before and after the heat-setting treatment. The results of mechanical testing illustrated that the prototype stents in this work could achieve higher radial forces than Wall stents and Z stents on the market. The heat setting with temperature of 80℃ and time of 5 min were found to be more appropriate for the stents. In conclusion, the stents were successfully developed and have potential application for the treatment of intestinal stenosis or obstruction.
Introduction
Intestinal obstruction and stenosis appear in 7–29% of colorectal cancer patients in clinical [1]. Metal self-expanding stent has been used for the treatment ofstenosis and obstruction of bowel and vessels for three decades [2,3]. Biodegradable stents have been demonstrated to be another option to treat obstruction and stenosis previously [4,5]. The major advantages of biodegradable stents different from other kinds of stents are that they can prevent serious long-term complications and do not require removal, thus avoiding further surgeries and potential morbidity [6–8]. The most frequently used biodegradable polymers for stents arealiphatic polyesters, such as polylactic acid, poly(L-lactide), poly (lactic-co-glycolicacid) and polydioxanone (PDO) [9]. Compared to other polymers, PDO offers a number of advantages, such as good flexibility and elasticity, appropriate absorption rate, suitable biocompatibility, and minimal inflammatory response [6,10–12].
As shown in Figure 1, the biodegradable intestinal stents mainly give mechanical support of obstructed intestines which can restore intestinal lumen and waste flow smoothly. After knitting, the tubular PDO stents were easily deformed and the tubes collapsed because they could not withstand the residual tension within the knitted structure induced by the knitting process. Heat setting is a thermal process often performed using dry heat or steam which stabilises the dimensions of thermoplastic yarns, monofilaments or fabrics to achieve dimensional stability, mechanical properties and temperature resistance. PDO is a kind of biomedical polymer that cannot be treated at high temperature because its glass transition temperature and melting temperature are only around –10–5℃ and 105–115℃, respectively. Therefore, heat-setting at lower temperatures under a vacuum environment is better to retain its original properties.
The diagram of placement process and mechanical function of intestine stents. (a) The cross-section of the deflated balloon catheter and closed stent inserted into the narrowed intestine. (b) A balloon inflated, expanding the stent and compressing the tumor to restore the lumen size of the intestine, the stent can be adhesive to the intestinal mucosa. The compressed tumor and stent-widened intestine; IP is the intestinal pressure because of the solid feces and movements of intestine, and IAP is the intra-abdominal pressure concealed within the abdominal cavity [5].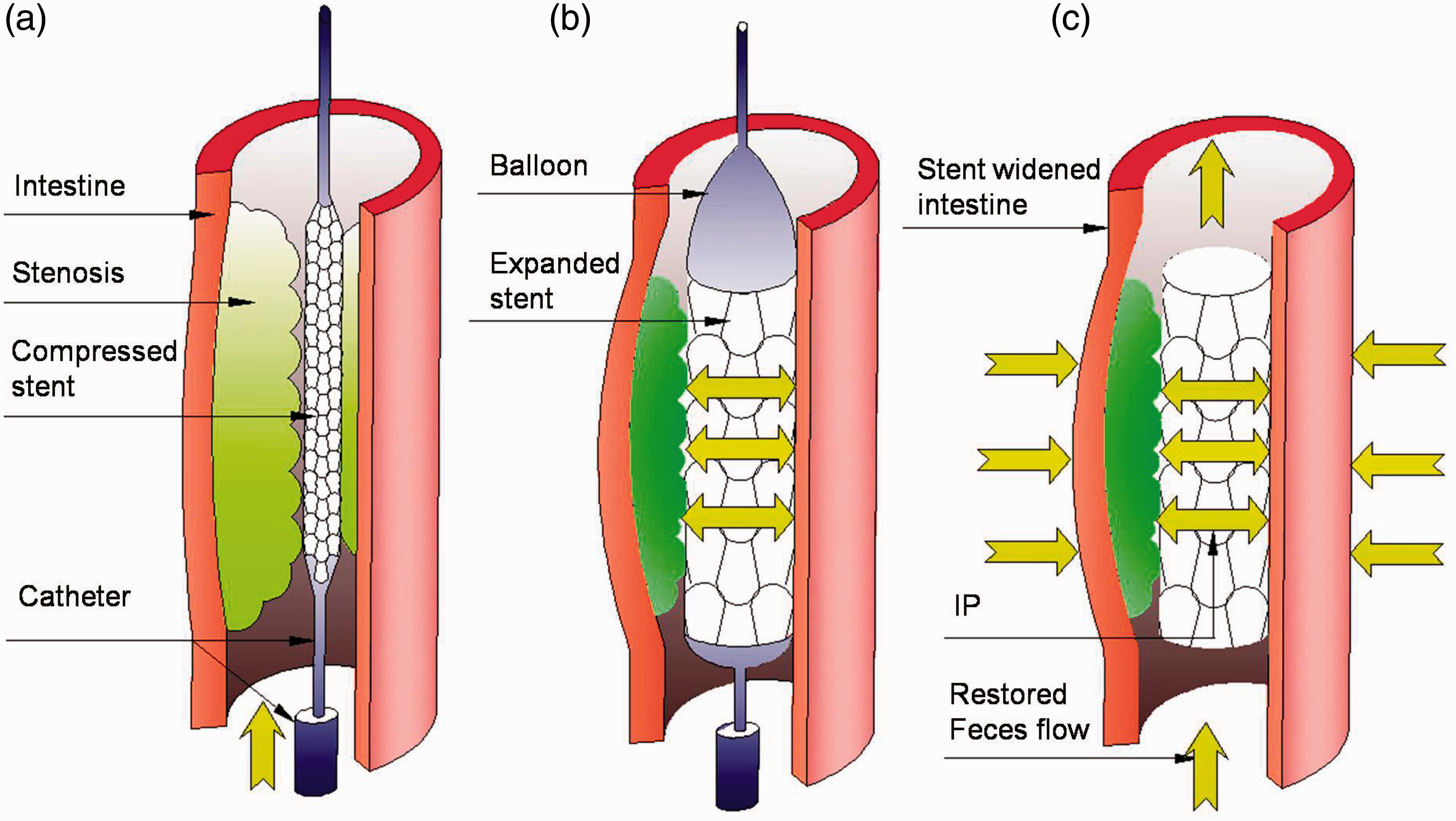
The aim of this work is to investigate heat-setting effects on physical and mechanical properties of prototyped PDO stents made from weft-knitting technology for the treatment of intestinal stenosis. First, a set of stents was knitted on a small diameter, circular weft knitting machine using PDO biodegradable monofilament. Subsequently, the stent was heat-set in order to restore a tubular shape to the stents. Finally, the mechanical properties of the stents were characterized, and their thermal stability following a heat-setting process was evaluated.
Material and methodologies
Material
PDO polymer synthesized using a conventional bulk ring-opening polymerization method was purchased from Samyang Co., Korea. The PDO monofilament was produced by an extrusion process immediately followed by a drawing process to create a self-reinforced structure (Horcon Ltd. Co., China). Two PDO monofilaments with linear densities of 100 ± 2 and 150 ± 2 tex were produced because these were the most suitable for the gauge of the weft-knitting machine.
Fabrication of the weft-knitted PDO stent
Physical parameters of the weft-knitted stent samples.

Heat-setting
A vacuum oven (DZF-6020, Yiheng Co., Ltd. China) was used to create vacuum heat-setting to the stent under a vacuum environment: 80 ± 5 kPa. According to the previous studies, the reported effective heat-setting temperature (Teff) is 54℃ [14]. Usually, for the heat-setting treatment, 2–15 s can induce thermoplastic relaxation and configuration at the molecular level of textile fiber. Our pilot experiments showed that 5 min can induce the inner molecular stresses of PDO monofilament adjusted to a new and lower level of energy [15]. In the present work, four sets of stents were mounted on a 20 ± 2 mm diameter cylinder and placed under vacuum at different heat-setting parameters, i.e. temperatures: 60, 70, 80 and 90℃, for 5 min to determine the optimum heat-setting conditions. Photographs of the collapsed stents and the circular cross-section stents after heat-setting are shown in Figure 2.
Photos of a stent before and after heat-setting and PU coating on the inner surface of stent, (a) and (b,c) are photos of a stent before and after heat-setting.
Characterization
Mechanical properties of PDO monofilaments
In accordance with British standard BS EN 13895:2003, the tensile properties of the prepared monofilaments were measured using an Instron-4411 tensile testing machine. Under the same testing conditions, each monofilament was tested 20 times to obtain reliable average data. A pre-tension was applied to the monofilament to maintain the standard test condition for all samples. The pretension on the monofilament was set at 0.5 ± 0.05 cN/tex, the gauge length was 500 ± 10 mm and the testing speed was 8 ± 0.1 mm/s. The tests were conducted under a standard textile testing environment: 20 ± 2℃, relative humidity 65 ± 2%.


Mechanical properties of the PDO stents
The stents are designed to provide mechanical support within obstructed intestines to restore the intestinal lumen and allow smooth waste flow. Therefore, it is important to investigate the mechanical properties of stents. During this treatment, the stent must withstand two principle forces, a radial force (RF) and a circumferential force (CF) [5]. We previously reported the method of measurement of RF and CF according to BS EN ISO 25539: 2009. The purpose of the RF test is to determine the force exerted by a stent on the vessel in the deployed state during expansion and compression of the testing device [12,13]. The device was installed on an Instron model 4411 testing machine set with the following conditions: head speed: 5 mm/min, full scale: 500 cN; testing conditions: room temperature 20 ± 2℃, relative humidity 65 ± 2%. The radial force was defined as the force required to reduce the stent diameter by 50%.
The CF is a stent-expanding force designed to simulate the force exerted by solid wastes as it passes through the intestine. In vivo, the stent can be expanded by the function of intra-intestinal pressure and solid feces because of the movements of the intestine within human body, so that the stent must have appropriate CF against expanding force. According to ISO 7198, a new device was installed to an Instron-4411 model testing machine for testing CF of PDO stents. Samples were tested at 20 ± 2℃ and relative humidity 65 ± 2% with the CF applied at a head speed of 5 mm/min, maximum load 5 kN. Each mechanical measurement was repeated five times.
Wide angle X-ray diffraction
The internal crystalline structure of the PDO monofilament was examined via WAXD (Regaku 9 KW SmartLAB) using a Cu Kα source. A two-dimensional X-ray diffraction pattern was obtained using a Regaku X-ray diffractometer with nickel-filtered Cu Kα1 radiation with the following settings: DP Max 22,550 PC, Cu, Kα, wave length 0.154 nm, range 5–60°. Each measurement was repeated three times. The equation for the degree of crystallization is as follows
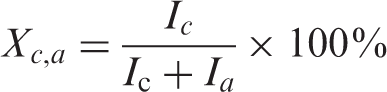
Differential scanning calorimeter
In order to understand the changes in the thermal properties and crystallization of the samples at different temperatures during heat-setting of the PDOs, a thermal history was derived using a differential scanning calorimeter (Perkin–Elmer DSC-2). All the tests were conducted under a nitrogen atmosphere. Indium and zinc standards were used for calibration. The sample (100 ± 2 tex) weight was 8 ± 0.2 mg and the samples were placed in aluminium pans. The temperature program, including heating and cooling process, was set in the range –30℃ and 150℃ at the rate of 10℃ per minute. The DSC endothermic peak was obtained during the heating process of temperature program, while the exothermic curve was tested during the cooling process. Each measurement was repeated three times.
Results and discussion
Mechanical properties of PDO monofilaments
In order to compare the mechanical properties of the PDO monofilament with other available commercial monofilaments, the polypropylene and polyester were chosen and their mechanical properties were tested. The tensile testing results of the three monofilaments of same linear density are given in Table 2. Their tensile curves are shown in Figure 3(a). The tensile strain (X axis) and tenacity (Y axis) for the three kinds of monofilaments were calculated using equations (1) and (2), respectively. The maximum tensile strength of the PDO was much higher than the PET and shows that the PDO monofilament had a much better tensile property. PDO, therefore, could be more suitable for intestinal stents in terms of its mechanical property. As shown in Figure 2(b), the tensile strength decreased and the modulus of PDO increased slightly as the heat-setting temperature changed from 80 to 90℃. A reduction in the tensile strength and increase in modulus of the PDO monofilament may reduce the CF and diameter deformation recovery of stents, respectively. Therefore, a higher heat-setting temperature should be avoided.
Tensile curves for PDO, PET and PP: (a) the maximum tensile strength of PDO is much higher than PP and PET showing PDO had a better tensile property; (b) mechanical changes in PDO before and after heat-setting. Under the same testing conditions, each monofilament was tested 20 times to obtain reliable average data. Tensile properties of four monofilaments used. Note: All samples were subjected to a pre-tension of 0.5 ± 0.1 cN/tex to remove the residual internal stress to maintain the standard test condition for the samples.

Mechanical properties of the PDO stents
The RFs for the two types of stents prepared viz. single jersey stents and plated stitch stents were compared with the commercially available Wall stent and Z-stent [16]. As shown in Figure 4(a), the RF of the single jersey stents and the plated stitch stents were higher than the other two commercial stents. Of these, the RF value of the plated stitch stents was higher than that of the single jersey stents. These stents with high mechanical performance properties should be developed for patients diagnosed of serious obstruction or stenosis in larger bowel. The weft-knitted stent is composed of knitted loops. The weft-knitted structure of stents can be unraveled when it endures higher circumferential expanding force. Unraveling means that a yarn has become separated or departed from a fabric structure [17]. For the weft-knitted stents, the weft-knitted loops are destructed and the PDO monofilament is then separated from the stents under higher CF. The unraveling problem is often found among the knitting fabrics, especially for single jersey of weft-knitted fabric due to the one yarn system only [15]. The CF value was collected before loops raveling while conducting the CF test. The three CF curves for the three kinds of stents prepared are shown in Figure 4(b). The CF value of the two single jersey stents was lower than the value of the plated stitch stent.
Radial force and circumferential force comparison, the radial forces of two prototyped biodegradable stents were much higher than the other two commercial stents, 0.12 and 0.18 cN/cm2 at 50% of compression; the radial force values for the plating stitch stents were higher than single jersey stents.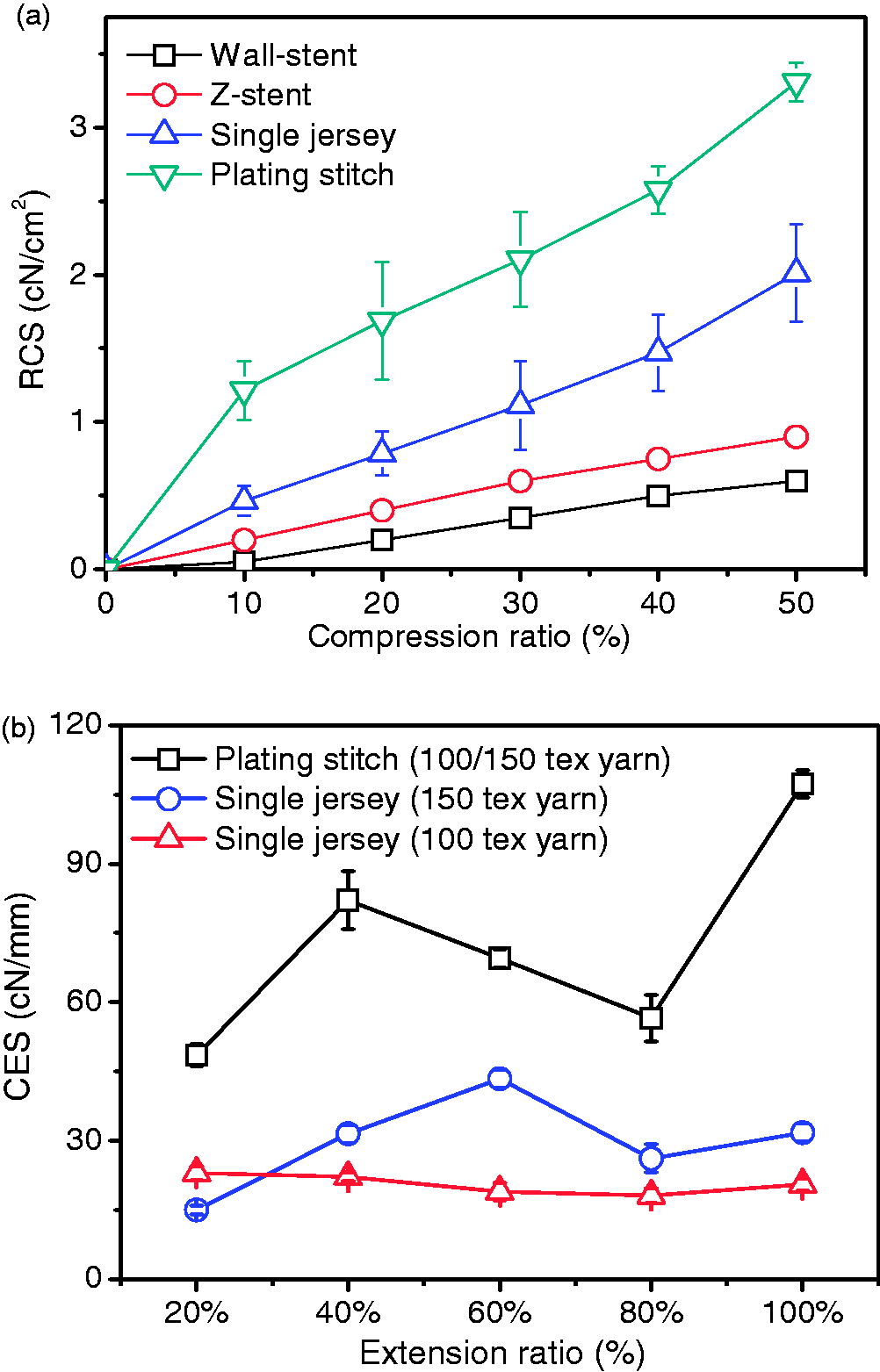
Thermal characterization of PDO monofilaments
As shown in Table 3, the RF of the stents increased as the heat-setting temperature was increased. The diameter of the stent reached a maximum of 93.3% at 80℃ due to the removal of the residual internal tension within the PDO monofilament. In order to investigate the temperature impact on the mechanical properties and molecular structure of the PDO monofilament and its stents, wide angle X-ray diffraction (XRD) (Figure 5) and differential scanning (DSC) (Figure 6) calorimeter were used.
WAXD pattern of PDO before and after heat-setting; the crystalline peak of PDO (2θ = 21.8°) was clearly observed, which was unchanged when the heating temperature changed a lot from 60 to 90℃. DSC patterns of PDO before and after heat-setting, (a) the DSC pattern of the endothermic process; (b) the DSC pattern of the exothermic process. Mechanical properties of the samples before and after heat-setting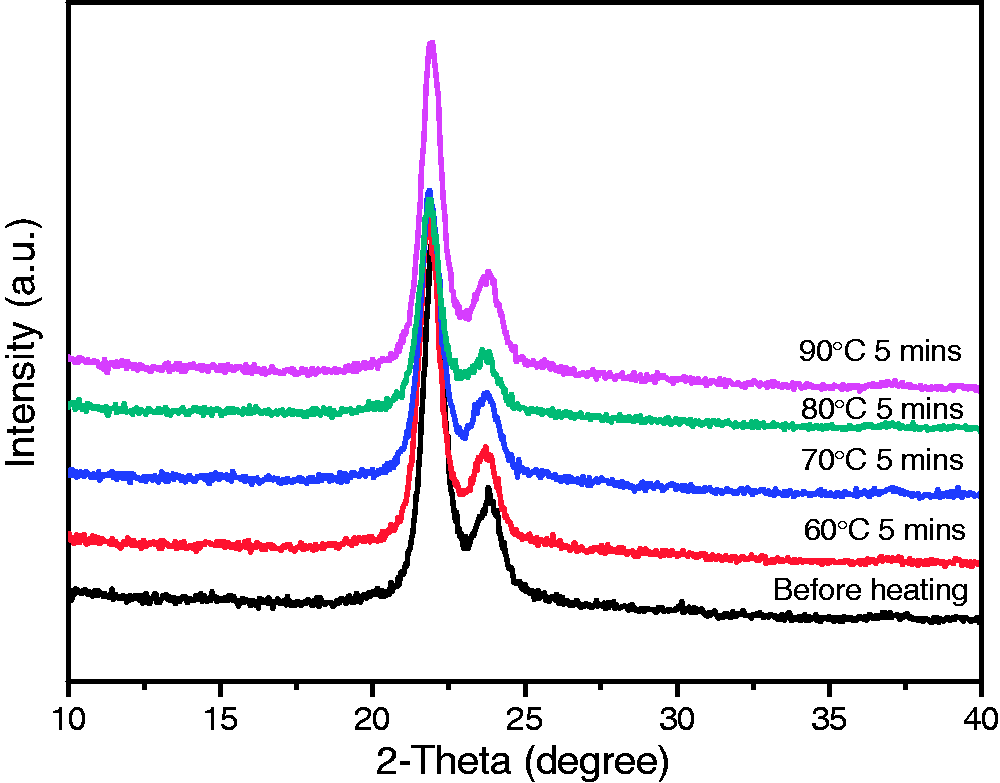


Figure 5 shows the change in intensity, height and width of two strong reflection peaks (110) and (200) at the angles of (21.8°) and (23.7°) in the WAXD pattern of PDO before and after heat-setting, respectively. These peaks were assigned on the basis of the orthorhombic unit cell structure of PDO crystals [18]. Few new peaks were observed during this heating process; only the intensity of peaks declined or increased in the heating temperature from 60 to 90℃. The results showed that the crystallinity degree of PDO increased slightly when the heat-setting temperature increased from 60 to 80℃. The reason is that the molecular orientation degree of PDO monofilament increased under the beginning of the heat-setting process. However, when the heat-setting temperature increased to 90℃ the crystallinity degree decreased to 67.6 ± 0.9 which is even lower than the polymer before heat-setting. This is because 90℃ is closed to the melting temperature of PDO polymer (105℃).
In the DSC thermograms, the melting temperature (Tm) and crystallization temperature (Tc) of PDO were similar as the reported temperature [18,19]. As shown in Figure 6, the high endothermic peak was induced by the molten phase content of crystallites during the process of drawing and heat-setting treatment. This happens because of the mobility of the chain segments, which are necessary to promote the recovery of the enthalpy. The Tm of the sample was closed before and after heat-setting. Hence, the crystal structure and size remain stable during the heat-setting process. The Tc of PDO was slightly lower after heating, which demonstrates that the interaction force between the molecules decreased while the molecular mobility of the polymer increased under high temperature. Based on the analysis above, few differences of these samples after heat-setting at different temperatures were found in the thermal characterization. We may conclude that the temperature of 80℃ and time of 5 min are appropriate for the heat-setting process of PDO intestinal stents.
Conclusions
In this work, a kind of biodegradable stent made from weft-knitting technology was developed and its heat-setting treatment was discussed. The RFs that the single jersey stents and plated stitch stents could withstand were higher than those for the two other commercially available stents tested. Furthermore, the CF value of the two single jersey stents was lower than the value of the plated stitch stent. The results of thermal characterization demonstrated that the crystal structure and size remain stable during the heat-setting process. The XRD results demonstrated that the interaction force between the molecules decreased while the molecular mobility of the polymer increased under high temperature. According to the characterization results for the crystallization and mechanical properties of the PDO monofilament and its stents before and after heat-setting, a temperature of 80℃ and a heat setting time of 5 min were preferable for the heat-setting parameters of PDO stents. In conclusion, the stents were successfully developed and have potential application for the treatment of intestinal stenosis or obstruction.
Footnotes
Acknowledgements
We would like to thank Prof. David Kaplan and Prof. Xiaoqin Wang from Tufts University for their kind instructions on this writing.
Declaration of Conflicting Interests
Declaration of Conflicting Interests The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The project was funded by State Key Laboratory for Modification of Chemical Fibers and Polymer Materials—Donghua University with project code LK1421. We would like to thank the support of Guangdong Provincial Department of Science and Technology through the Guangdong–Hong Kong International Textile Bioengineering Joint Research Center with project code 2012B091000143 and Guangzhou Science and Technology Program with project codes 2014J4100237.
