Abstract
Demand for acute care is forecasted to grow in the United States. To meet this demand, nurse practitioners (NPs) are increasingly employed in acute care settings. Yet, there is concern about an adequate supply of acute care NPs given demand. Further, professional nursing organizations recommend aligning an NP's role with their education, certification, licensure, and practice. Given workforce constraints and the policy environment, little is known about how hospitals approach hiring NPs for acute care roles. The purpose of this study was to explore advanced practice provider (APP) directors’ approaches to hiring NPs within the context of alignment and describe factors that influence hiring decisions. We conducted semi-structured interviews with 17 APP directors in hospitals and health systems. Interviews were recorded, transcribed, and coded using an iterative, hybrid inductive and deductive method. Two themes emerged: (1) local factors that inform aligned hiring and (2) adaptive hiring responses to changing environments. Practices around hiring NPs varied across institutions influenced by organization and state policies and regulations, workforce availability, and institutional culture. Most APP directors recognized trends towards hiring aligned NPs for acute care roles. However, they also identified barriers to fully aligning their NP workforce and described adaptive strategies including hiring physician assistants, building relationships with APP schools, and leveraging hospital resources to develop the APP workforce to meet care delivery demands given the current NP workforce supply. Future research is needed to assess widespread practices around acute care NP alignment and the implications of alignment for patient and organizational outcomes.
There are nearly 35 million hospitalizations in the United States each year and demand for acute care will likely grow as the population ages and the prevalence of chronic diseases increases (Agency for Healthcare Research and Quality, 2021; Arora & Fried, 2020; VanOosteveen et al., 2015). To meet these demands, health systems are increasingly hiring advanced practice providers (APPs), especially nurse practitioners (NPs). Since 2010, the number of NPs working in hospital settings has more than doubled (Auerbach et al., 2020). Over the next decade, NPs are projected to be the fastest growing provider workforce, underscoring their potential to help meet rising demand for acute care services (Bureau of Labor Statistics, 2022).
The NP role originated in primary care settings before expanding into acute care. Education, policy, and regulations evolved to support these emerging NP roles. NPs receive focused education in specific patient populations guided by the Consensus Model for APRN Regulation, Licensure, Accreditation, Certification, and Education (the Consensus Model) which (1) defined APRN licensure, roles and population foci; (2) standardized education and certification; and (3) outlined a strategy to align education, certification, and licensure with practice roles (APRN Consensus Workgroup & National Council of State Boards of Nursing, 2008). Three of the six population foci align with acute care clinical practice that meets the care delivery needs of patients with changing, acute conditions (1) acute care adult/gerontology, (2) acute care pediatric, and (3) neonatal (National Organization of Nurse Practitioner Faculties, 2013). Aligned NP practice would result in NPs with expertise in these three population foci employed in roles caring for patients with acute and critical health care needs, which is often, but not exclusively, provided in hospital settings. Yet, 88% of the NP workforce have certifications that align with primary care (American Association of Nurse Practitioners, 2022). Therefore, the supply of acute care certified NPs is likely less than demand. In addition, since the introduction of the Consensus Model 15 years ago, few states have fully adopted the model, and hospitals’ implementation of aligned NP practice has been variable (Gigli et al., 2021; Hoyt et al., 2022; Kaplan & Klein, 2020; Martsolf et al., 2020; National Council of State Boards of Nursing, 2023).
This creates a tension for hospitals as they navigate hiring NPs to meet acute care demands when there is an abundance of primary care certified NPs. Professional nursing organizations recommend aligned NP practice, but most states lack regulations requiring it. Without regulatory mandates for aligned hiring, hospitals define their own criteria for hiring NPs (Hoyt et al., 2022; Kaplan & Klein, 2020). Hospital-based APP directors are well positioned to influence these hiring practices. However, little is known about their approach to hiring NPs for hospital roles, including how they view alignment of NPs for hospital roles and how state regulations inform hospital and health system hiring practices. The purpose of this study was to explore APP directors’ approaches to hiring NPs in hospital settings within the context of the Consensus Model and alignment and describe factors that influence their hiring decisions.
Method
Study Design
We performed a descriptive, observational, qualitative study of APP leaders in hospitals and health systems using semi-structured interviews to describe approaches to employing NPs in hospital settings. Data were analyzed using hybrid inductive and deductive coding (Fereday & Muir-Cochrane, 2006). The University of Pittsburgh Human Subjects Protection Office approved this study (STUDY19110294) before participant recruitment started. All participants provided informed consent.
Sample and Recruitment
We used snowball sampling to recruit APP directors who were involved in hospital and health system leadership of APPs. Our participants represented diverse disciplines in APP leadership roles (i.e., NPs and PAs), patient populations (e.g., children's hospitals, lifespan health systems), and geographic and state regulatory (scope-of-practice) environments. We contacted potential respondents via electronic mail and conducted all interviews using a web-based videoconferencing platform (Archibald et al., 2019).
Data Collection
We used a semi-structured interview guide to understand how hospitals and health systems approach hiring, onboarding, and retaining APPs to meet workforce needs. We developed the guide through iterative discussion among the investigators using existing theories of APP practice and regulation that informed our study conceptual framework. The conceptual framework included macro-, meso-, and micro-level factors (e.g., state scope-of-practice, work environment, NP characteristics) that influence APP care delivery and contribute to outcomes (Supplement A). In the context of this study, we sought to understand how factors in each level of the framework influenced APP directors’ approach as they considered the study outcome of interest, NP hiring decision. To refine the interview guide, we conducted two pilot interviews with non-study participants and made revisions for content and clarity based on their feedback. The final interview guide consisted of 15 questions. The full interview guide is available in the Supplemental Materials (Supplement B).
Interviews were conducted between October 2020 and May 2021. We conducted interviews until thematic saturation was reached, which we defined as the identification of no new themes after two consecutive interviews (Hamilton & Finley, 2019). Interviews were recorded and transcribed verbatim, and transcripts were stored in a secure, cloud-based platform (Graneheim & Lundman, 2004). Study team members deidentified transcripts and uploaded them into the NVivo software package (QRS International, Chadstone, VIC, Australia) for analysis.
Data Analysis
We used iterative, hybrid inductive and deductive coding to identify factors that influence practices related to hiring, onboarding, and retention of NPs in hospital roles (Hamilton & Finley, 2019). The codebook included thematic categories and subcategories, each with a unique definition and included code inclusion and exclusion criteria. Three researchers individually coded transcripts; the coders discussed and, through consensus, resolved discrepancies. The results are presented as a series of themes that are based on these codes and, for the purposes of this manuscript, focus on practices related to implementation of the Consensus Model, along with supportive quotes.
Results
Thematic saturation was reached after 17 interviews, with the 16th and 17th interviews adding no additional themes to the codebook. The final sample included 13 NPs and three PAs who served as APP directors within hospitals and health systems and one non-APP recruitment leader. These participants represented five children's hospitals, seven adult hospitals, and five lifespan hospitals and health systems. The hospitals and health systems were in three full, five reduced, and seven restricted state scope-of-practice environments. Two participants worked in health systems with multiple scope-of-practice environments. Interviews averaged 37 min in length.
Themes
Two overarching themes emerged from the interviews: (1) local factors that inform aligned hiring and (2) adaptive hiring responses to changing environments.
Local Factors that Inform Aligned-Hiring Decisions
Many factors influenced APP directors’ decisions regarding the extent to which they required NP alignment including being in a consensus state, local NP supply and substitutes, acute care NP inducements, and local culture.
Hiring in Consensus States
All interviewees reported being familiar with the Consensus Model. If there were clear state policies, those policies informed hiring approaches yet, most participants were from states without regulations on alignment (see Table 1). In Consensus Model states, APP directors simply needed to find acute care NPs without choice. In a state that adopted the Consensus Model, one APP director said, … early on [we] realized that we, I can’t put a primary care person in the inpatient side … there is no way to be nimble unless everybody's acute care on the hospital side.
Perspectives on Hiring Nurse Practitioners for Aligned Practice in Hospitals and Health Systems.

APP directors in states that had not fully implemented the Consensus Model demonstrated diverse perspectives on alignment. In many instances, the APP directors described the Consensus Model as ideal but not practical. Each developed, and modified with experience, a framework for how they would align NPs with roles that informed practice in their institution.
Local NP Supply and Substitutes
Participants described an uneven supply of acute care trained APPs across the country (see Table 2). Some interviewees identified a limited availability of acute care NPs. To meet care demands, APP directors in areas with a limited supply of acute care NPs described hiring primary care-trained NPs. Some accepted hospital experience as a registered nurse as an adequate substitute for formal acute care NP education. Further, APP directors discussed substitution of acute care NPs with PAs as a mechanism to diversify the workforce pipeline, increasing the available supply of APPs for hospital-based care roles. Notably, the generalist model of PA education and the ability for an institutions’ physicians to determine the PAs’ scope-of-practice supported hiring PAs. Interviewees also described the perception that, given complex state nursing regulations, PAs are “easier to supervise” than NPs. To mitigate perceived challenges navigating the NP regulatory environment, APP directors increasingly planned to hire PAs. Overall, APP directors reported, with a period of onboarding, perceptions that primary care-trained NPs and PAs provide equivalent care to acute care NPs. One APP director summarized these discussions: “side by side, given the same robust onboarding and orientation, six months later, you probably wouldn’t be able to tell the difference.”
Local Factors That Inform Aligned Hiring of Advanced Practice Providers in Hospitals and Health Systems.
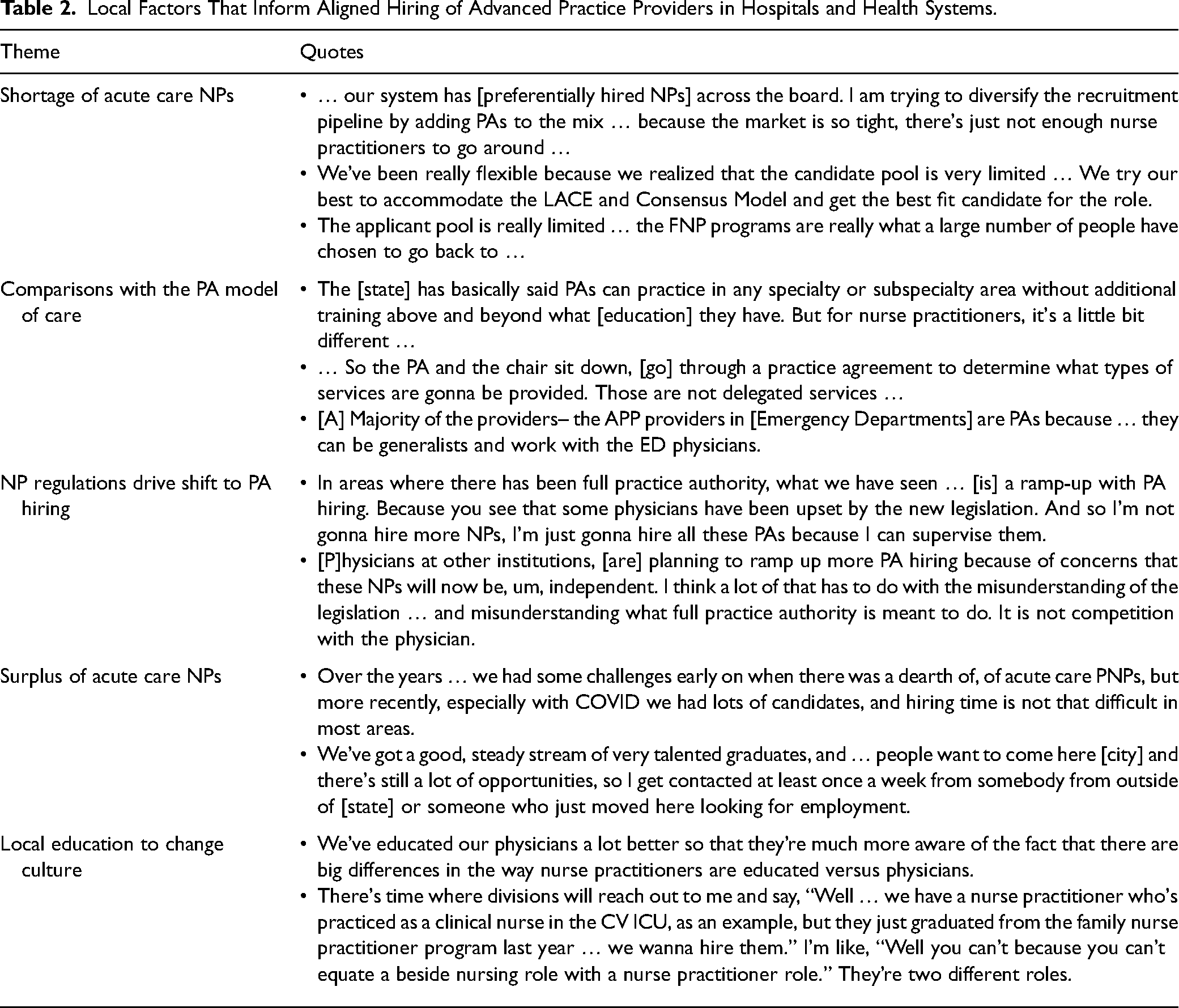
Acute Care NP Inducements
In other settings, APP directors had an adequate local supply of acute care NPs. Yet, these participants also acknowledged that nationally, there is dynamic and heterogeneous availability of the acute care NP workforce. To summarize the role of acute care NP supply in hiring practice, one APP director said, So, I think some organizations would be very hard pressed to draw that bright line and require an [acute care] certification [knowing] that they did not have a pipeline, but we’ve got a good … steady stream of, you know, very talented graduates …
Interviewees with adequate acute care NP staff described factors they felt increased the local availability of an acute care workforce. Several APP directors described being a “destination employer” with a combination of location (e.g., coastal, metropolitan area) and practice environment (i.e., formalized onboarding opportunities, full scope-of-practice) that were attractive to potential applicants. Others expressed gratitude to be situated in an area with an abundance of educational programs for acute care NPs and PAs that ensured a consistent pipeline of APP applicants. One APP director described how their institution identified a need for an acute care NP program and subsequently nurtured the development of a program, “… we really wrapped our arms around the acute care [NP] program here, … most of the lectures are given by people from our hospital, and we would also actively recruit from there, and actively provide the traineeships, practicums.”
Local Education to Change Culture
APP directors described their roles changing culture and providing education in their institutions to dispel beliefs that any NP is a qualified NP. One APP director said, “[physicians] are just so used to pulling a nurse off the floor and you train her and she's a nurse practitioner.” To achieve institutional change, APP directors described physicians’ need to understand, and support aligned hiring.
Adaptive Hiring Responses to Changing Environments
Hiring practices are continuously evolving in response to changing practice, educational, financial, and regulatory environments. Given these dynamics, to attain desired APP staffing levels, APP directors adopt strategies to support hiring to meet demand. As a result, APP directors often described approaches that included anticipatory planning and implementation of process changes to positively affect their ability to hire qualified APPs (see Table 3). Many APP directors recognized the limitations of graduate nursing education. One said, … I think the jobs have changed so much that even with [graduate education] it's just so not adequate to get people ready for where they are. And I do think it's impossible to totally prepare somebody for the diversity of [specialties].
Strategies Adopted by Hospitals and Health Systems’ Advanced Practice Provider Directors to Support Hiring in Response to Educational and Regulatory Environment Changes.

Abbreviations: BON = board of nursing; ICU = intensive care unit; NP = nurse practitioner; PA = physician assistant; PNP = pediatric nurse practitioner.
APP interviewees found the increasing reliance on online, distance education among NP programs particularly concerning. Many viewed a formal onboarding process as an important component of their hiring strategy to facilitate role transition.
Relationships with Stakeholders
APP directors highlighted how relationships with stakeholders informed hiring practices. To ensure an adequate acute care workforce, APP directors emphasized a need for relationships between institutions and schools that educate APPs. APP directors viewed clinical rotations as extended interviews through which they could screen and recruit APPs while in graduate school. Relationships with state boards of nursing were informative for APP directors when developing hiring policies. Yet, boards of nursing took different approaches to providing guidance. APP directors felt some state boards of nursing left interpretation of alignment to institutions while others were “overly prescriptive” and acted “beyond their legislative authority.” As scope-of-practice policies became less restrictive, some APP directors described receiving less guidance from boards of nursing. This was perceived as a challenge, shifting the onus for interpreting and adopting policies related to NP hiring practices solely to the institutions.
Changing Regulatory Environment
As states increasingly mandate alignment in acute care settings, many APP directors acknowledged there will be a future need to move their institution toward alignment. They are preparing for how that transition might impact their hospitals and health systems. For example, some interviewees were working to advise aspiring NPs to match their educational pursuits with their future career goals. Others discussed a practice change to hire only aligned NPs from a certain time onward. Despite the approach used to move towards alignment, they all acknowledged a need for time to adopt policies and grandfather current, misaligned employees.
In addition to mandates for alignment, APP directors anticipated changes to state scope-of-practice regulations and, in some cases, were implementing change in response to the recent passage of full practice authority legislation in their states. Most identified a need for institutional changes related to formal collaboration agreements and paperwork requirements as the primary difference associated with implementing new, less restrictive scope-of-practice regulations. There was a sense that modernization of rules would be beneficial but might not change practice in significant ways because of how hospital NP roles have grown despite “archaic” state regulatory environments.
Discussion
Through the perspective of APP directors, this study explores hospital practices related to hiring NPs for roles in acute care, including barriers and facilitators to hiring aligned NPs consistent with the Consensus Model. Participants identified acute care NP workforce availability, regulatory mandates, and institutional culture as essential elements informing APP hiring decisions. However, ambiguous guidance from boards of nursing and state regulatory changes were barriers to greater alignment of NPs. APP directors reported collaborating with stakeholders and the need for process change to improve aligned hiring.
The findings of this study reveal several insights with implications for NP education, practice, policy, and research. First, local availability of the acute care NP workforce influenced hiring practices around NP alignment. A majority of physicians stay in the geographic location where they complete their training (Boyle, 2021). While it is unclear if NPs have the same pattern, greater availability of local acute care NP education can facilitate hospitals aligned hiring of NPs and is one strategy to ensure future workforce growth. Second, respondents described the effectiveness of mandating an aligned NP workforce. As the nursing community pushes for greater nurse practitioner authority, policymakers considering these policy changes yield significant power regarding concurrent implementation of the Consensus Model. However, APP directors noted that while state mandates for alignment would have desired effects of an aligned workforce it could also have unintended consequences. For example, there were concerns about workforce availability given the relatively small acute care NP workforce compared to primary care NPs (HRSA Dashboard, 2018). As a result, educational capacity and availability of acute care programs would need to be considered if more states mandate alignment (Gigli et al., 2020). Further, policymakers should fund acute care NP programs when mandating alignment to support sustainability and growth of these educational pathways to aligned practice (American Association of Colleges of Nursing, 2023; HRSA, 2021). In addition, if policymakers pass legislation consistent with the Consensus Model, an adequate time frame to complete aligned, population-specific education is necessary to accommodate NPs whose education, certification, and licensure are currently misaligned with their roles, but who wish to continue their current practice. Finally, APP director perspectives diverged on the need for an aligned hospital NP workforce. Notably, many APP directors believed that after a period of onboarding, aligned and misaligned NPs or PAs had similar clinical practice and outcomes. However, to date, no studies examine outcomes associated with aligned or misaligned practice or PA substitution (Hoyt et al., 2022). This gap in empirical knowledge of the role of NP alignment on outcomes often results in APP directors using their gestalt, influenced by institutional culture and historical precedent, when making hiring decisions. Future research is needed to provide evidence of outcomes associated with NP alignment or substitution and should be a priority for funders given the projected workforce growth (Auerbach et al., 2020).
As the NP workforce grows, NPs will play a key and growing role in hospital care delivery (Auerbach et al., 2020). However, challenges in hiring to meet demand may prevent NPs from maximally contributing to hospital care delivery needs. Limiting regulatory barriers can significantly increase the effect of the NP workforce (Frogner et al., 2020). Importantly, hospital and health systems frequently impose additional regulations beyond state scope-of-practice (Bowman et al., 2022; Gigli et al., 2018; Pittman et al., 2020). While policies around alignment may complicate hiring and pose implementation challenges for APP directors, particularly in areas of limited supply, an aligned acute care NP should be better prepared to meet the acute care needs of hospital patients. In turn, aligned NPs would require less regulation of their practice by the hospital (Frogner et al., 2020). Aligned NPs then could be incentivized to seek out employers with less restrictive institutional policies and enjoy increased professional autonomy, drawing NPs to these positions and institutions. These types of positive regulatory changes support hiring needs and help achieve the full potential of the NP workforce.
Limitations
First, this study is qualitative; we describe hiring practices in a limited number of hospital settings. As such, our results may not generalize. However, we sought a diverse sample representing different professional backgrounds, hospital types and practice environments. Second, two members of the study team (KHG, JC) are acute care NPs who practice in hospital settings, and we acknowledge that this may have influenced our interpretation of the data and ensuing recommendations. In response, we sought thick description in data analysis to increase the internal reliability of our findings and collaborated with non-APP researchers (Morse, 2015).
Conclusion
This study examined APP directors’ approaches to hiring NPs. Most APP directors recognized trends towards hiring NPs whose education, certification, licensure, and practice aligned with their role. However, they also identified barriers to full implementation of aligned workforces and described adaptive strategies to meet care delivery demands given the current NP workforce supply. Future research is needed to assess widespread practices around acute care NP alignment and the implications for patient and organizational outcomes.
Supplemental Material
sj-docx-1-ppn-10.1177_15271544231204879 - Supplemental material for The Perspectives of Advanced Practice Provider Directors on Acute Care Nurse Practitioner Alignment and Hiring
Supplemental material, sj-docx-1-ppn-10.1177_15271544231204879 for The Perspectives of Advanced Practice Provider Directors on Acute Care Nurse Practitioner Alignment and Hiring by Kristin Hittle Gigli, Jackie Calhoun, Andrew M. Dierkes and Grant R. Martsolf in Policy, Politics, & Nursing Practice
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
