Abstract
Objective:
The objective of this study was to examine the short- and midterm outcomes of catheter-directed thrombolysis (CDT) for acute lower limb ischemia (ALI), classes Rutherford 1 and 2, with specific attention to functional outcome.
Methods:
This retrospective study included patients with ALI treated with CDT from 2 vascular centers between May 2018 and April 2021. Cases were analyzed in groups according to the Rutherford (1 and 2) classification. The primary endpoint was functional outcome during follow-up, assessed by Rutherford’s chronic limb ischemia classification. Functional outcomes over time were analyzed by generalized estimating equations. Kaplan-Meier analysis was used to estimate reintervention, amputation, survival, and reintervention-free survival rates.
Results:
Two hundred cases were included (Rutherford 1, n = 51; Rutherford 2, n = 149). Total median treatment duration was 27 hours in the Rutherford 1 group and 39 hours in the Rutherford 2 group (P= 0.120). Initial clinical success was high (Rutherford 1, 82% vs Rutherford 2, 89%; P= 0.253). Complications were comparable between the 2 groups: major bleeding 8% vs 10% (P= 0.634), major amputation 4% vs 7% (P= 0.603), and mortality 6% vs 6% (P= 0.967). Median follow-up was 32 months (0-63 months). During follow-up, there was a high number of reinterventions (43%) and amputations (20%) in patients with Rutherford 1 limb ischemia, which was comparable to patients with Rutherford 2 limb ischemia. Fifty-six percent of the patients with Rutherford 1 limb ischemia reaching 2 years of follow-up were asymptomatic, 20% had mild and 16% had moderate to severe claudication. Initial clinical success following CDT and not immediately threatened ischemia at presentation are associated with improved functional outcomes during follow-up (P < 0.001 and P= 0.009, respectively).
Conclusions:
In our cohort, CDT was effective in reestablishing arterial flow for not immediately threatened ALI. Patients with Rutherford 1 limb ischemia who receive CDT had a more favorable functional outcome than patients with more severe limb ischemia (Rutherford 2). However, reinterventions were required frequently, and there was a substantial risk of complications.
Clinical Impact
Acute lower limb ischemia (ALI) does not immediately jeopardize limb survival in patients with Rutherford 1 limb ischemia but can induce disabling claudication. In such patients, catheter-directed thrombolysis (CDT) is often performed to improve functional outcome. However, previous reports warned about the complications of CDT, and so far, mid- and long-term functional outcomes have not been reported. This study, in which a large cohort of patients with ALI was included, demonstrates a high technical success of CDT for not immediately threatened ALI with more favorable functional outcomes when compared with those with threatened limbs. Nevertheless, major complications pose a serious risk, and the need for reinterventions in the long term is high.
Keywords
Introduction
Acute lower limb ischemia (ALI is a challenging vascular emergency. In patients with threatened limbs, classified as Rutherford 2a (R2a) or Rutherford 2b (R2b), prompt treatment is important to increase the chance of saving the patients’ limb. 1
In patients with not immediately threatened limbs, classified as Rutherford 1 (R1), both patients and physicians are faced with a dilemma. The survival of the limb is not immediately threatened, but disabling claudication can severely hamper the patient’s quality of life. Although the European Society for Vascular Surgery guidelines recommend against catheter-directed thrombolysis (CDT) for R1 ALI, it is commonly performed in such patients. 1 Conservative treatment is suggested by guidelines as the initial approach for such patients but may lead to residual invalidating claudication despite exercise therapy. The rationale behind treating CDT in R1 patients with CDT is to dissolve fresh thrombus and subsequently treat the culprit lesion, which can be short and relatively easy to treat with standard endovascular techniques. A recently published meta-analysis on the outcomes of CDT for R1 ALI revealed high angiographic success and a low amputation and mortality rate at 30 days. However, long-term patency was low. 2 Unfortunately, functional outcome was not assessed. The aim of this study was to report on the outcomes of CDT for patients with not immediately (R1) and threatened (R2a and R2b) limbs with special emphasis on functional outcome.
Methods
Study design and patients
This retrospective observational study was approved by the local institutional review board, and the study was performed in accordance with the Declaration of Helsinki. The opt-out method was followed in accordance with Dutch civil procedure. Patient were informed of the study and could opt out by using the response form.
All patients with ALI of native arteries or bypass grafts distal to the aortic bifurcation referred to the Department of Vascular Surgery of the Amsterdam University Medical Centers (locations VUmc and AMC) and the Dijklander Hospital, Hoorn, Netherlands, between May 2018 and April 2021 and treated with CDT were included. CDT was the preferred treatment for patients with Rutherford 1 and 2a ALI, unless contraindicated. In accordance with the European Society for Vascular Surgery guidelines, we categorized occlusions in patients with symptoms lasting <14 days as acute, whereas patients presenting with symptoms persisting for 14 days or more were considered nonacute and thus excluded. 1 Contraindications for thrombolysis were a recent (<1 year) cerebrovascular event, active bleeding diathesis, recent (≤10 days) gastrointestinal bleeding, intracranial trauma, and/or neurosurgery within the last 3 months. CDT was performed in selected Rutherford 2b patients with mild sensory loss and muscle weakness. Patients with insufficient documentation and those who presented with a thromboembolic occlusion caused by trauma or iatrogenic injury were excluded.
Data from clinical and outpatient records, radiology reports, and surgeons’ and nurses’ reports were collected by 3 investigators (SD, SO, and BT) and entered into the electronic data-capture platform Castor EDC (Castor Electronic Data Capture platform, CLWLT BV, Amsterdam, Netherlands). Baseline characteristics included age, sex, medical history, degree of ischemia categorized by the Rutherford classification, 3 and pre-and postprocedural thrombolytic therapy. Follow-up data comprised all surveillance outpatient clinic visits including clinical examination, reinterventions, amputations, and mortality.
Intervention
The lytic agent of choice was recombinant tissue plasminogen activator (rtPA; Actylise, Boehringer Ingelheim, Ingelheim, Germany). Catheter placement was performed under local anesthesia. In both hospitals, CDT with rtPA started with a 2.5- or 5.0-mg rtPA bolus, followed by continuous infusion of 1 mg/h rtPA for 24 hours and 0.5 mg/h rtPA after 24 hours. Additionally, a continuous dose of 4800 IU/24 h of heparin was infused through the side port of the sheath to prevent pericatheter clotting. CDT was discontinued in case of low fibrinogen levels (<0.5 g/L), major bleeding, when lysis was complete, or when no further progress was observed at angiography. After successful thrombolysis, an endovascular (ie, percutaneous transluminal angioplasty [PTA] with or without stenting) or surgical procedure (ie, endarterectomy or bypass) was performed to treat culprit lesion(s) and/or improve inflow or outflow. A detailed description of the procedure was provided in a previous publication. 4
Laboratory test measurements
Hemoglobin concentration, thrombocyte count, activated partial thromboplastin time, prothrombin time x(PT) measured as international normalized ratio (normal range, 0.80-1.20), and fibrinogen concentration (normal range, 2-4 g/L) were regularly determined before and during thrombolysis. A detailed description of the corrections implemented in the thrombolytic protocol in response to fibrinogen concentrations was provided in a prior publication. 4
Follow-up
Patients were observed for varying periods. Most patients underwent the first routine follow-up visit at 1 month after the procedure. Subsequent follow-up visits were scheduled at different intervals until patients no longer exhibited symptoms or signs of critical limb ischemia. These visits routinely comprised physical examinations, and for symptomatic patients, ankle-brachial index determinations, toe pressure measurements, and ultrasound evaluations were performed. Based on the clinical circumstances, additional elective, urgent, and emergency follow-up visits and admissions were arranged, and the need for angiography was evaluated.
Endpoints and definitions
According to Rutherford’s recommended clinical categories of ALI, patients were divided into 2 groups based on the degree of ischemia at admission: R1 and R2a/2b. 3 The primary endpoint was functional outcome during follow-up assessed by Rutherford’s recommended clinical categories of chronic limb ischemia. 3 Secondary endpoints included clinical success according to Rutherford’s recommended scale for gauging changes in clinical status (defined as a score of +1 or higher), 3 angiographic success (defined as dissolution of the thrombus >95% with outflow to at least one crural artery), and the occurrence of bleeding complications. The definition of minor bleeding entails no invasive (surgical or endovascular) interventions, whereas major bleeding involves intra- or retroperitoneal bleeding, intracranial bleeding, or the need for blood transfusion or surgical interventions resulting in the interruption or cessation of CDT.
Statistical analysis
Continuous variables were presented as mean ± SD for normally distributed data or median and interquartile ranges for non–normally distributed data. As appropriate, group differences were determined by Student’s t test or Mann-Whitney U test. Categorical data were presented by frequency and percentages, and a χ2 test followed by post hoc analyses was used to compare the differences between groups. The reintervention, amputation, survival, and amputation-free survival rates were analyzed by the Kaplan-Meier method. The functional outcome data were repeated measures obtained from the 2 degree-of-ischemia groups during follow-up. To arrive at a precise inference, the impact of thrombolysis on the 2 subgroups was examined statistically using generalized estimating equations based on multinomial distribution. A P value of <0.05 (2-sided) was considered statistically significant. Statistical analyses were performed using SPSS Statistics 20 software (IBM Corp, Armonk, NY).
Results
During the study period, we identified 277 patients with ALI. Of these, 77 were excluded due to treatment with surgical or conservative methods. Among the remaining 200 patients treated with CDT, 51 were classified as R1 and 149 as R2 (Figure 1). Most patients were male (n = 138; 69%), and the mean age of the total cohort was 69 ± 10 years. The patient and occlusion characteristics are shown in Table 1. No differences in baseline characteristics were found between groups, except for the longer duration of ischemic symptoms (7 vs 3 days; P = 0.000) and fewer instances of prior ipsilateral thromboembolectomy in the R1 group (4 vs 30 cases; P = 0.044).
Patient baseline and occlusion characteristics.
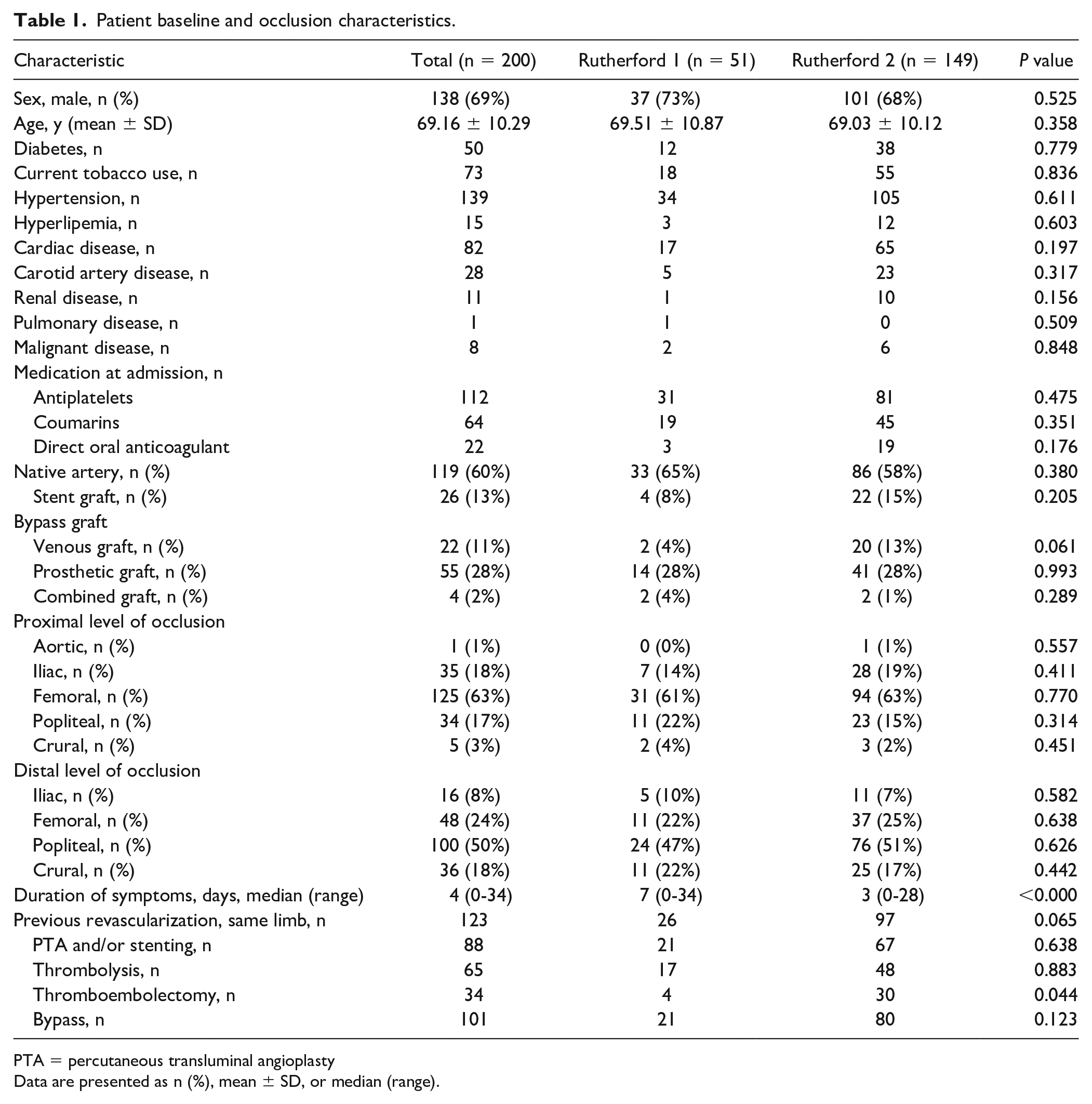
PTA = percutaneous transluminal angioplasty
Data are presented as n (%), mean ± SD, or median (range).
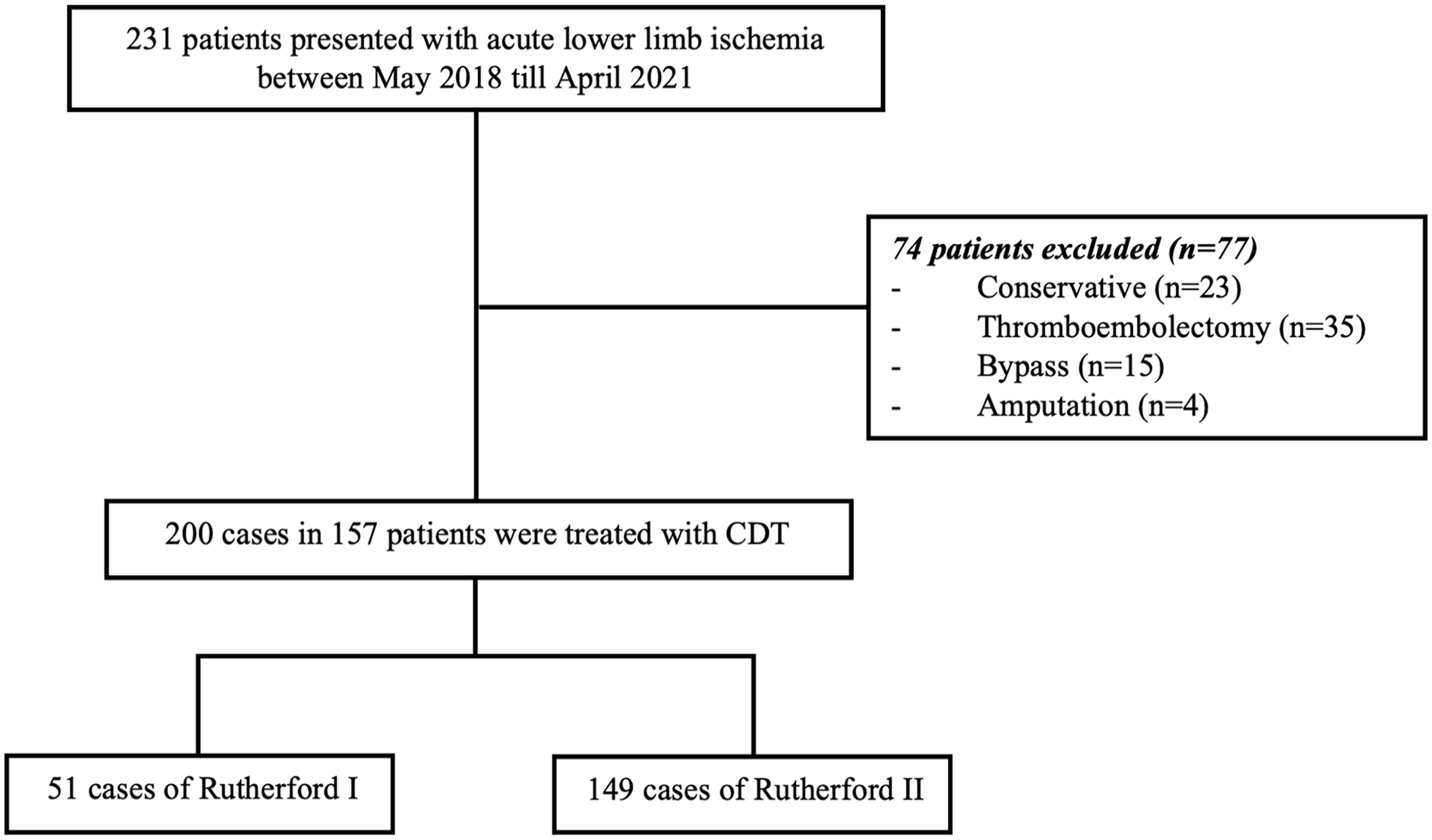
Flowchart of included and excluded cases.
Short-term outcomes
Treatment characteristics of all groups are shown in Table 2. The median (range) treatment duration was 26.7 hours (3-88 hours) in the R1 group and 39.4 hours (2-120 hours) in the R2 group (P = 0.120), and the median rtPA dose administered was 29.1 mg (3.8-188.8 mg) and 33.5 mg (6.2-226.2 mg), respectively (P = 0.246). Angiographic success rates in the R1 and R2 groups were 78% (n = 40) and 74% (n = 111), respectively (P = 0.573). Clinical success following CDT was 82% (n = 42) in the R1 group and 89% (n = 132) in the R2 group (P = 0.253). In 64% of patients (n = 128), adjunctive procedures were used, including percutaneous mechanical thrombectomy in 5 patients (guiding catheter [n = 4] or AngioJet [n = 1; Boston Scientific, Boston, MA]). In patients in whom patency could not be restored by endovascular means, additional surgical interventions were performed (eg, thromboembolectomy in 12, bypass surgery in 3, and amputation in 14). Two patients (1%) with thrombosed popliteal artery aneurysms were included, both of whom had previously diagnosed bilateral popliteal artery aneurysms and were under close observation. One patient responded successfully to thrombolysis and subsequently received elective open surgical repair with a synthetic graft. The thrombolytic treatment in the other patient was complicated by acute intracerebral hemorrhage, necessitating a shift to palliative care due to poor prognosis.
Treatment characteristics.
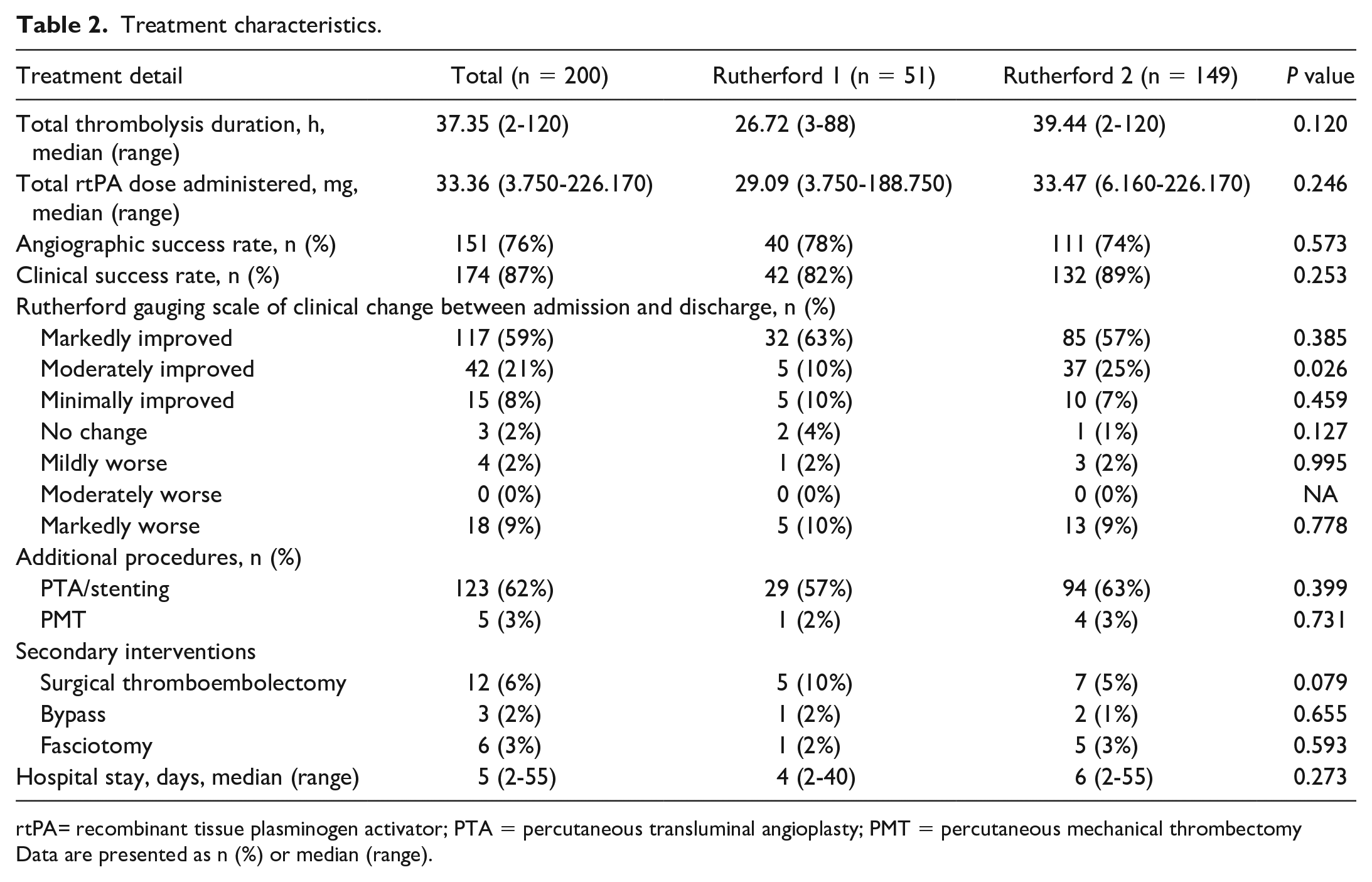
rtPA= recombinant tissue plasminogen activator; PTA = percutaneous transluminal angioplasty; PMT = percutaneous mechanical thrombectomy
Data are presented as n (%) or median (range).
Table 3 provides an overview of all periprocedural complications. Bleeding complications occurred in 82 patients (41%), of which 10% were classified as major bleeds. The 30-day mortality rate was 6% (n = 12) and was similar in both groups (P = 0.967). The cause of death was intracranial bleeding in 3 patients, heart failure in 2 patients, multiorgan failure and sepsis in 3 patients, and retroperitoneal bleeding in 1 patients, and the cause of death could not be determined in 2 patients. One patient died of end-stage pancreatic adenocarcinoma 2 weeks after discharge.
Complications.
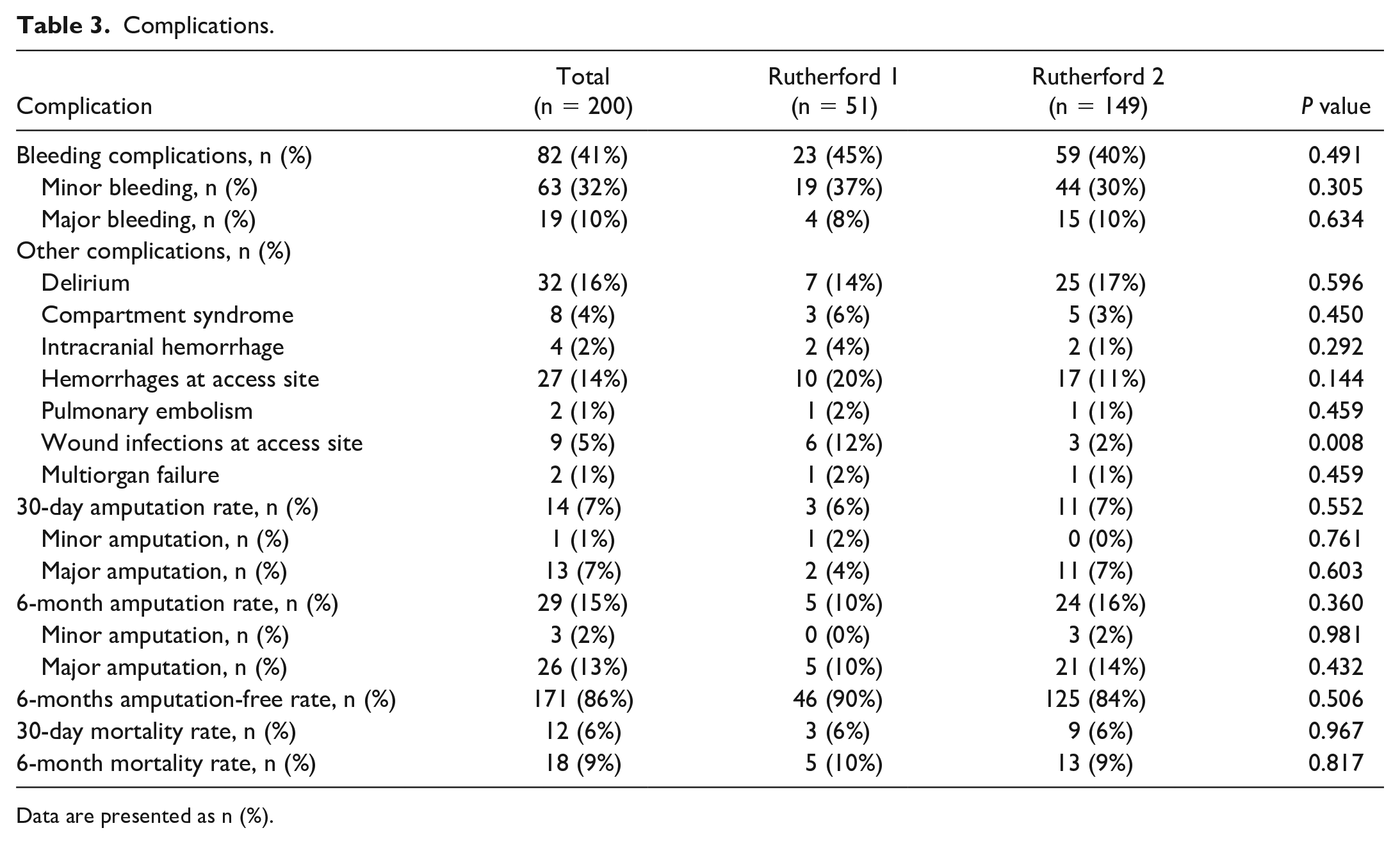
Data are presented as n (%).
Midterm outcomes
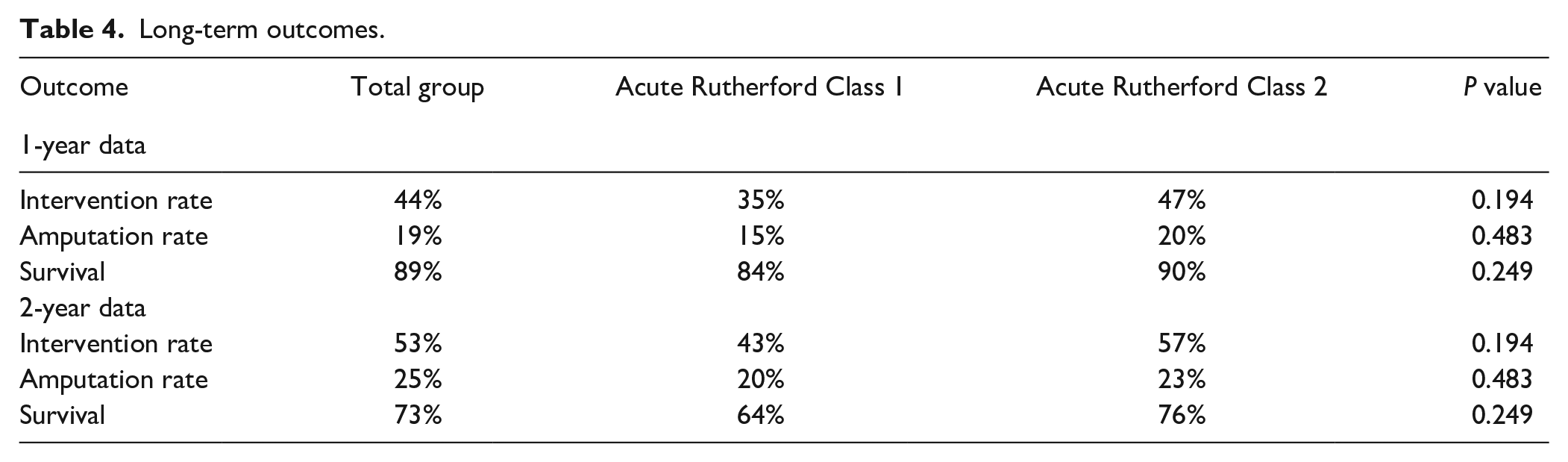
The overall median length of follow-up was 32 months (range, 0-63 months) and was similar for all degrees of ischemia, 31 months (0-61 months) in the R1 group and 32 months (0-63 months) in the R2 group (P = 0.742). The overall reintervention rates after restored patency were 44% and 53% at 1- and 3-year follow-ups, respectively. For the R1 group, the reintervention rates at 1- and 3-year follow-ups were 35% and 43%, respectively, and did not differ from the R2 group (P = 0.194 and P = 0.194; Table 4). The amputation rates at 1- and 3-year follow-ups, respectively, were 15% and 20% for the R1 group and 20% and 23% for the R2 group (P = 0.483 and P = 0. 483; Table 4). The survival rates at 1- and 3-year follow-ups, respectively, were 84% and 64% for the R1 group and 90% and 76% for the R2 group (P = 0.249 and P = 0.249; Table 4). The overall reintervention-free survival rates were 51% and 39% at 1 and 3 years, respectively. The reintervention-free survival rates at 1 and 3 years were 51% and 46%, respectively, for the R1 group and 50% and 36%, respectively, for the R2 group. Analysis of the reintervention-free survival rates in relation to the degree of ischemia revealed similar results for both groups (P = 0.427; Figure 2).
Long-term outcomes.
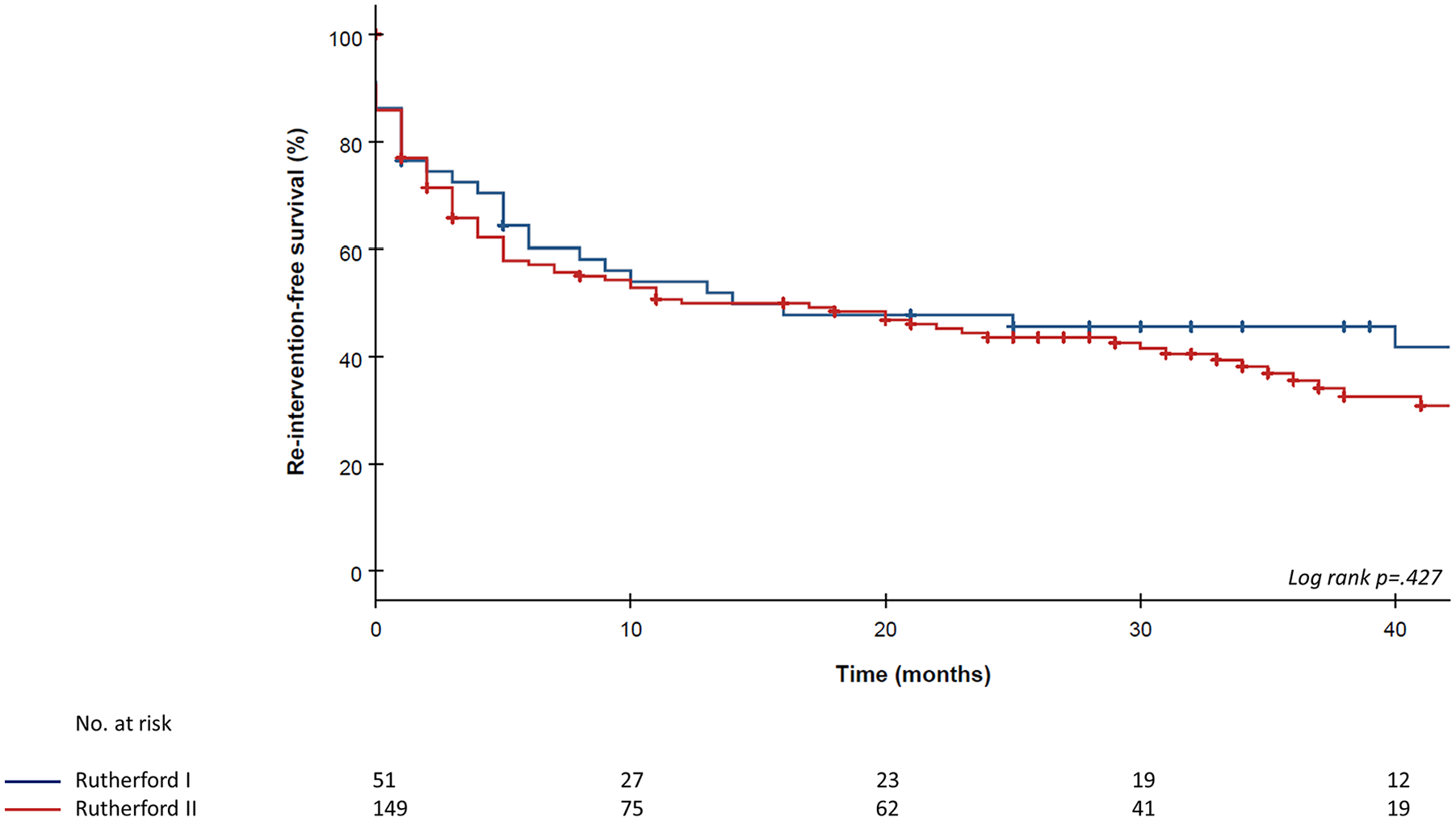
Kaplan-Meier survival curves. Reintervention-free survival after catheter-directed thrombolysis comparing subgroups depending on the degree of ischemia graded by the Rutherford’s acute lower limb classification.
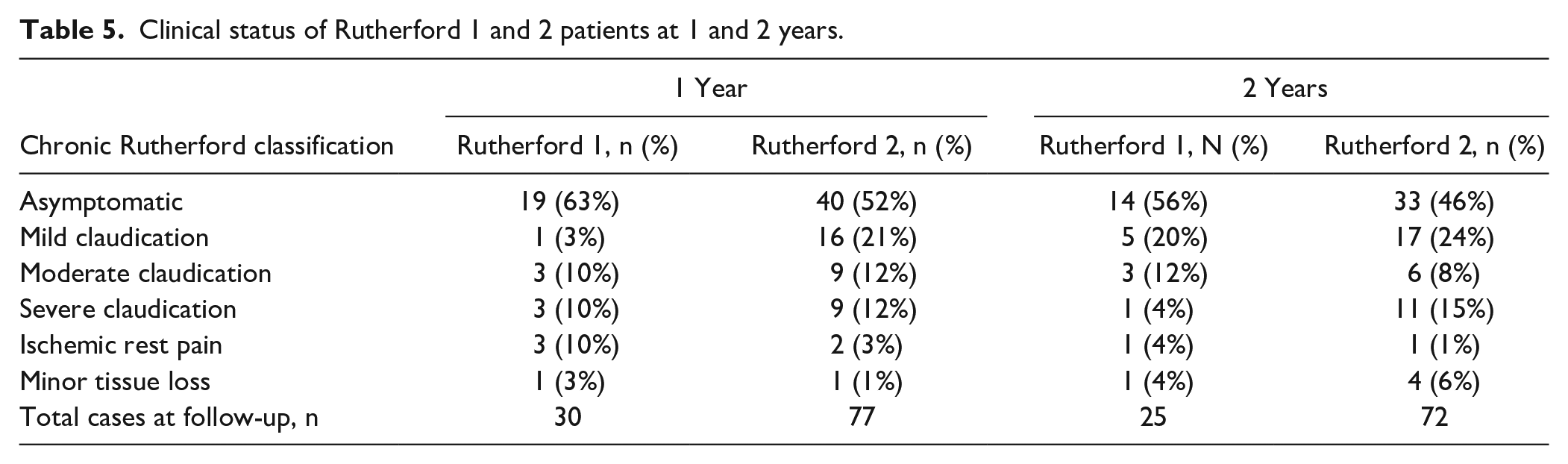
Clinical symptoms of 131 patients could be graded by the Rutherford’s 6-category chronic limb ischemia classification system to evaluate potential changes in functional outcome during follow-up. At 2 years, 47 patients (36%) were asymptomatic, 22 patients (17%) had mild claudication, 21 patients (16%) had moderate to severe claudication, and 7 patients (5%) had ischemic rest pain to minor tissue loss (Table 5).
Clinical status of Rutherford 1 and 2 patients at 1 and 2 years.
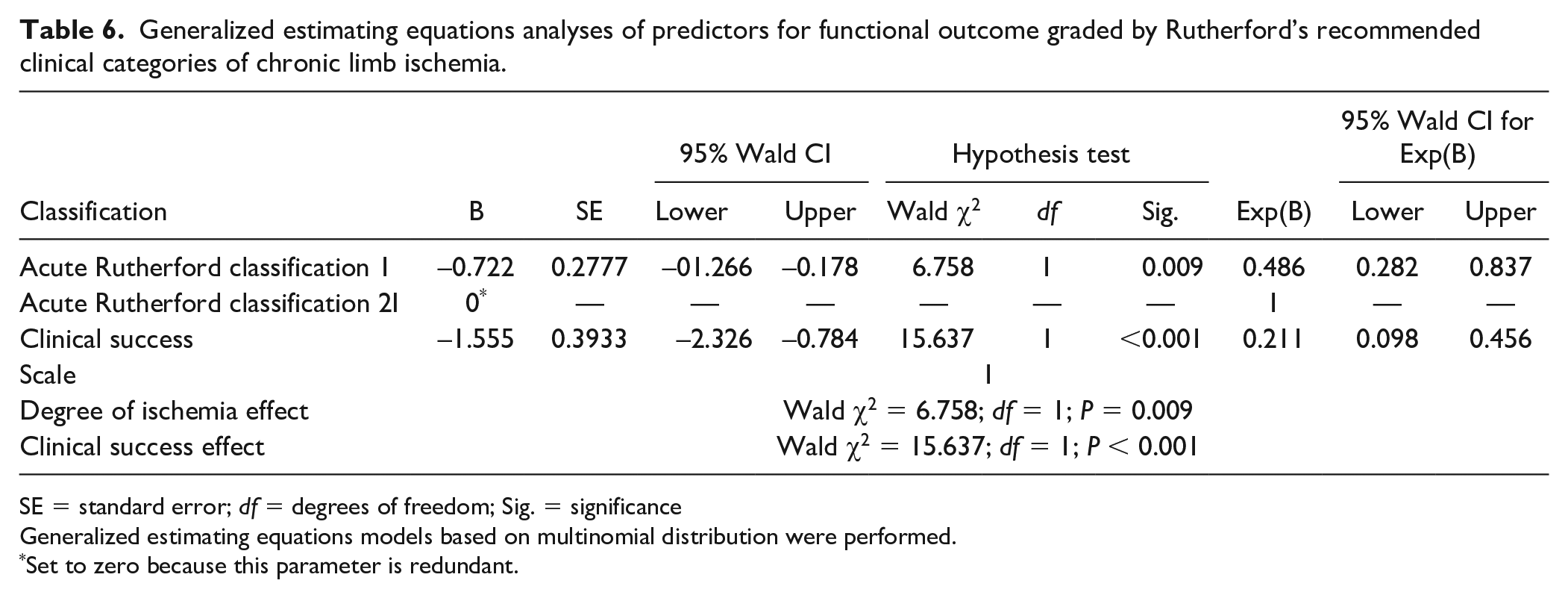
According to the results of generalized estimating equation analyses presented in Table 6, initial clinical success following CDT and not immediately threatened ischemia at presentation are associated with improved functional outcomes during follow-up (P < 0.001 and P = 0.009, respectively).
Generalized estimating equations analyses of predictors for functional outcome graded by Rutherford’s recommended clinical categories of chronic limb ischemia.
SE = standard error; df = degrees of freedom; Sig. = significance
Generalized estimating equations models based on multinomial distribution were performed.
Set to zero because this parameter is redundant.
Discussion
This study shows that the use of CDT is equally effective in reestablishing arterial flow for not immediately threatening (R1) ALI and more advanced ischemia (R2). The functional outcome for R1 patients during follow-up was better than for R2 patients. At the same time, overall treatment outcome and risk of complications during admission and follow-up are not more favorable for R1 patients than for R2 patients with ALI.
It was anticipated that not immediately threatened limbs, due to milder ischemia, would respond more favorably to CDT than those with more profound ischemia. However, angiographic and clinical success rates of R1 and R2 following CDT were equivalent, which is in line with previously published studies.2,5 Despite successful revascularization, the overall long-term outcomes after initial CDT were somewhat disappointing. Roughly 20% of treated patients required amputation at 1-year follow-up. This is in line with other studies and may be explained by the inclusion of patients with extensive peripheral arterial disease with or without previous bypass surgery and possible limited outflow to the foot. 6
The lower ischemia grade of R1 patients did not significantly reduce thrombolytic treatment durations or doses, nor did it result in a lower bleeding risk. Major bleeding is a well-known risk of CDT and was not lower than that reported in previous literature. 5 To reduce the risk of bleeding, a protocol using subtherapeutic doses of heparin and a relatively low dose of thrombolytic agents has been implemented. However, the optimal dosage of thrombolytic agents remains unknown due to the absence of comparative studies. Notably, predicting the risk of bleeding remains a challenging task. 7
In our cohort study, it was observed that patients experienced a substantial burden of severe comorbidities, which led to numerous complications. Among these, the in-hospital mortality rate was high (6%). It is noteworthy that besides hemorrhages, most of the reported deaths resulted from cardiopulmonary complications or cancer. Regrettably, these comorbidities also pose a significant risk during follow-up. 8 Interestingly, the subset of patients (4%) who underwent concurrent treatment for an underlying malignancy exhibited similar outcomes following thrombolytic treatment when compared with those without cancer, with an amputation-free survival rate of 75% at 3-year follow-up.
Our study reveals that thrombolysis holds clinical advantages for patients with not immediately threatened limb ischemia in the mid and long term; however, this benefit must be weighed against the risk of life-threatening complications. Therefore, several authors recommended initial conservative treatment.9-12 Mokete and Earnshaw suggested that conservative treatment for not immediately threatened ischemia resulted in more favorable outcomes. 11 In a small prospective cohort study, 8 patients were admitted for observation while being anticoagulated and were all discharged home without additional intervention. Only 2 patients needed surgical intervention for debilitating claudication during the follow-up period of 18 months. The value of conservative treatment also has been investigated by Kulezic and Acosta, who observed a high amputation-free survival in R1 patients (12 of 15; 80%) compared with the overall group (86 of 161; 53%). 13 Despite the small number of patients included, these studies suggest that initial conservative management can be worthwhile, especially for mild ALI without significant functional impairment. More data on outcome in conservatively treated patients are urgently needed. Unfortunately, inadequate documentation and adherence to follow-up procedures among these patients often hinder comprehensive analysis.
In this study, we used Rutherford’s chronic limb ischemia classification, which incorporated clinical symptoms with objective findings. 3 This allowed us to quantify the contributions of both restoration of useful limb function and relief of ischemic symptoms during follow-up. The severity of limb ischemia at presentation seems to significantly influence the functional outcome following thrombolytic treatment. Although it might be intuitive to assume that patients with a more severe degree of ischemia would experience a poorer long-term outcome, the differences observed in this study should be interpreted with caution because functional status does not stratify other endpoints nor weight them according to importance.
The median follow-up period in our series was 32 months, and for more definitive conclusions, one undoubtedly needs a longer follow-up period. The relatively short follow-up duration may be explained by the fact that some patients who are doing well are less likely to return for clinical follow-up. Because we only included patients who presented after 2018, the limited timeframe available for midterm follow-up may be another possible explanation. It is worth noting that long-term outcomes seemed to be more related to comorbidity, whereas limb salvage may be more related to the severity of ischemia and initial treatment success. 14 To mitigate any potential observer bias, 3 assessors independently scored the Rutherford classification based on the self-reported symptoms and physical examination documented in the hospital records. Although it is likely that the applied revascularization strategy was influenced by the severity of ischemia, the choice and timing of revascularization ultimately were determined by the treating physician. The distinction between degrees of ischemia can be challenging at times, which may have contributed to some misclassification. The effect of this misclassification on treatment decisions and outcomes remains unknown. Detailed information on the length of the lysis catheter and run-off characteristics was not consistently reported for each patient and therefore could not be uniformly included in our study. Given the relatively low incidence of not immediately threatened ALI, a multicenter cooperation with larger and more homogeneous cohorts is recommended to identify the influential risk factors affecting the outcomes of CDT. Another weakness in this study is the study design, which was retrospective; the chart review, however, was performed prospectively.
Conclusion
This study shows that CDT may serve as an effective first-line approach for not immediately threatened (R1) ALI with a more favorable functional outcome compared with those with threatened limbs. Nonetheless, when comparing R1 patients with those with more severe ALI (R2), there is no significant advantage in terms of overall treatment outcomes and amputation risk. These results question the optimal treatment approach for R1 ALI. Additional research is required to provide more conclusive evidence.
Footnotes
Acknowledgements
The authors thank statistician S. van Dieren from the Department of Surgery for her advice regarding statistical analysis.
Author Contributions
SD, AH, VJ, and KY wrote the manuscript; SD, SO, BT, AW, AH, VJ, and KY critically revised the manuscript, and all authors approved the final version of the manuscript.
Declaration of Conflicting Interests
The authors declare the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: One of the authors of this article is the editor-in-chief of this journal. To avoid a conflict of interest, an alternate member of the Editorial Board handled this submission.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
