Abstract
Purpose:
Acute lower limb ischemia (ALI) is a sudden decrease in arterial limb perfusion due to an arterial blockage, threatening limb and life. Catheter-directed thrombolysis (CDT) is a minimally invasive procedure to remove such obstructions. However, approximately one-third of patients endure a re-occlusion after successful CDT. This study aimed to investigate the short- and long-term outcomes of CDT for early (<1 year) and late (>1 year) re-occlusions.
Material and Methods:
This retrospective multicenter study reviewed patients from 2 medical centers with an acute arterial re-occlusion of the lower limb after successful CDT between December 1996 and April 2021. The primary endpoints were angiographic success, defined as thrombus dissolution over 95% with outflow to at least 1 crural artery, and clinical success, defined as a score of ≥1 on the Rutherford scale for assessing changes in clinical status. Secondary endpoints included bleeding complications, patency, amputation, and mortality. Kaplan-Meier analyses were used to estimate patency, survival, and freedom from amputation.
Results:
Seventy-seven cases were included, with 52 early re-occlusions (<1 year) and 25 late re-occlusions (>1 year). The median time to re-occlusion since the last CDT treatment was 4 months in the early re-occlusion group and 24 months in the late re-occlusion group. Angiographic success was achieved in 73% of early and 64% of late re-occlusions. Clinical success rates were 80.8% for the early and 80.0% of the late re-occlusion cases. Major bleeding occurred in 2% of the early and 8% of the late re-occlusion group. Patients were followed up until symptoms or signs of limb ischemia were resolved, with a median follow-up time of 15 months for the early and 22 months for the late re-occlusion group. During follow-up, secondary re-occlusions were observed in 59.6% of the early and 44% in the late group. Cumulative amputation rates at 1, 5, and 8 years were 36%, 36%, and 52% for early and 18%, 30%, and 30% for the late re-occlusions, respectively.
Conclusion:
In our experience, CDT is an effective short-term revascularization strategy for the majority of patients with both early and late re-occlusions. Long-term results are limited by secondary re-occlusions and limb loss.
Clinical Impact
Catheter-directed thrombolysis (CDT) is a well-established treatment for acute lower limb ischemia (ALI). Re-occlusions after successful treatment are, however, observed in almost a third of the patients. Yet, the outcomes of CDT for re-occlusions for patients who were previously treated with CDT are not well known. This study showed that CDT is effective in achieving revascularization in cases of early and late re-occlusion after treatment for ALI, but the risk for further re-occlusions is high. Future studies should focus on maintaining patency after successful CDT for ALI.
Keywords
Introduction
Catheter-directed thrombolysis (CDT) is an effective treatment for patients with acute lower limb ischemia (ALI).1,2 This endovascular revascularization technique is the choice of treatment for Rutherford class II ALI, as it has equal outcomes to surgery. 3 The main advantages of CDT include lysis of thrombi in small peripheral vessels and the minimally invasive nature of the procedure, without the need for surgery or anesthesia. 2 Despite its advantages, up to 29% of patients suffer from re-occlusions after successful CDT.4,5 Re-occlusions can be classified as early, within 1 year, or late, after 1 year, with a majority of cases observed within the initial year following revascularization. 5 While multiple studies have investigated the outcomes of CDT in primary ALI, 2,6,7 there remains a notable absence of evidence concerning the effectiveness of CDT for recurrent ALI at varying onset times. The limited research on re-occlusions in the context of modern endovascular treatment further adds uncertainty to the potential benefit of CDT for patients with recurrent episodes of ALI. This study, therefore, aims to provide an overview of the short- and long-term outcomes of CDT in patients with early (within 1 year after initial revascularization) and late (more than 1 year after initial revascularization) acute re-occlusion, to identify and describe the factors contributing to the success of CDT in these patients. It was hypothesized that outcomes of CDT for re-occlusions, especially those occurring early, would result in poorer outcomes compared to initial events.
Methods
Study Design Data Collection
All patients with ALI of native arteries or bypass grafts treated with CDT between December 1996 and April 2021 at Dijklander Hospital (DLZ) and Amsterdam University Medical Centers (AUMC) were included in this retrospective multicenter study if they were previously treated with CDT in one of the hospitals. All patients were treated in intensive care units at AUMC Location AMC, whereas those at AUMC Location VUmc were treated in a hospital ward. The Ethics Committee of the hospitals approved the study protocol, and the study was performed in accordance with the Declaration of Helsinki.
Eligible patients were identified through a systematic selection of diagnostic codes for peripheral arterial occlusion, treatment codes for thrombolysis, and equipment codes for thrombolysis for cross-checking. ALI was defined as a potentially threatening sudden decrease in arterial perfusion to the limb, requiring urgent management within 2 weeks of symptom onset. 3 Clinical data from patients were retrieved and analyzed according to a predetermined case report. The data were prospectively entered into an electronic database using Castor EDC (Castor Electronic Data Capture platform, Clwlt BV, Amsterdam, I.C., Netherlands, 2018), but the analysis of the case records was conducted retrospectively. For this study, all ALI patients who were treated with CDT for re-occlusions were identified from this database. Re-occlusions were defined as a recurrent life-threatening sudden decrease in arterial perfusion of the limb requiring urgent evaluation and management within 2 weeks of symptom onset. Patients were included if both the initial and subsequent re-occlusion events were treated at 1 of the 2 designated medical centers. Follow-up data included surveillance imaging studies, loss of patency with or without interventions, amputations, and mortality. Patients were excluded if the thromboembolic occlusion was a complication caused by an intervention and/or if the occlusion was trauma induced.
Indication for Thrombolytic Therapy
In both hospitals, CDT was the treatment of choice for patients with Rutherford I and II ALI, unless contraindicated. Absolute contraindications for thrombolysis included active internal bleeding, recent (<10 days) surgery or trauma, manifest ulcus pepticum or gastrointestinal bleeding (<1 month), esophagus varices, recent cerebrovascular accident (< 3 months), intracerebral tumor, aneurysm of arteriovenous malformation, a trauma with organ lesions and or multiple hematomas, recent cardiopulmonary resuscitation (<1 month), thrombocytopenia, thrombocytopathy, and coagulation deficiency.
Thrombolysis Protocol
Depending on the urgency of the situation and the requirement for detailed anatomical information, patients received either a Duplex ultrasound or CT-angiography (CTA) to diagnose ALI and determine the exact localization of the occlusion. During thrombolytic treatment, all antithrombotic and antiplatelet agents were discontinued except for acetylsalicylic acid.
Following ultrasound-guided puncture and sheath insertion, usually a Cragg-McNamara catheter (Micro Therapeutics Inc., Irvine, CA) was placed intra-arterially in the distal segment of the thrombus. Upon successful catheter positioning, patients treated with Urokinase (UK; Medacinase Urokinase, Medac, Hamburg, Germany) received a UK bolus of 250,000 international units (IU) or 500,000 IU followed by the continuous infusion of 50,000 (low dose group) or 100,000 IU/h (high dose group). Heparin was administered through the side port of the sheath by a continuous intra-arterial infusion of 4,800 (low dose) or 9,600 (high dose) IU/24 h to prevent peri-catheter clotting. To detect accidental systemic doses, the APTT was measured.
Between 2004 and 2011, all patients presenting with ALI were treated using a low-dose urokinase protocol. Based on a nationwide survey on thrombolysis, which revealed that most Dutch hospitals used high-dose protocols, the low-dose urokinase protocol was replaced with a high-dose protocol in 2011. However, concerns about the safety and effectiveness of high-dose urokinase arose due to the high incidence of major bleeding events, despite comparable success rates to the low-dose protocol. As a result, the high-dose protocol was replaced by a low-dose protocol once again in 2013.
In 2018, urokinase manufacturer supply problems prompted a switch to alteplase (rt-PA). This rt-PA regimen can, according to Ebben et al, 6 be categorized as a low-dose protocol. In both hospitals, CDT with rt-PA started with a 2.5 or 5.0 mg rt-PA bolus, followed by a continuous infusion of 0.5 or 1 mg/hr for 24 hours and 0.5 mg/hr rt-PA after 24 hours. Additionally, a continuous dose of 4800 IU/24 hours heparin was infused through the side port of the sheath. CDT was stopped in cases of low fibrinogen levels (< 0.5 g/L), major bleeding, lack of further progress observed on arteriography, or completion of lysis.
Control angiographies were performed every 24 hours or earlier. If the obstructive thrombus had been successfully lysed, an endovascular (e.g., percutaneous transluminal angioplasty [PTA] with or without stenting) or surgical procedure (e.g., endarterectomy, bypass) was performed to treat culprit lesion and/or improve inflow or outflow. After successful thrombolysis, low-molecular-weight heparin at therapeutic dose was initiated, followed by either coumarins with a target INR range of 2.0–3.5 or direct oral anticoagulants. Given the elevated risk of stroke and valve thrombosis in patients with mechanical heart valves, a target INR between 2.5 and 3.5 was maintained, while for the remaining patients, a target INR range of 2.0–3.0 was pursued.
Laboratory Test Measurements
Hemoglobin, thrombocytes, APTT, prothrombin time (PT) measured as INR (normal range 0.80–1.20), and fibrinogen (normal range 2–4 g/L) were regularly determined before and during thrombolysis. A detailed description of the corrections implemented in the thrombolytic protocol in response to fibrinogen levels has been described in a prior publication. 7
Follow-up
Patients were monitored for varying periods post-procedure. The initial routine follow-up visit was typically scheduled for 1 month post-procedure. Subsequent follow-up visits were arranged at different intervals until patients no longer exhibited symptoms or signs of critical limb ischemia. These visits routinely comprised physical examinations. For symptomatic patients, ankle-brachial index (ABI), toe pressure measurements, and ultrasound evaluations were performed. Based on the clinical circumstances, additional elective, urgent, and emergency follow-up visits and admissions were arranged, and the need for angiography was evaluated to ensure comprehensive monitoring.
Endpoints
Cases were categorized based on time to re-occlusion, either as early (within 1 year after initial revascularization) or late (more than 1 year after initial revascularization) re-occlusion. The primary endpoints were angiographic success and clinical success for each case of re-occlusion. Angiographic success after CDT was defined as is dissolution of the thrombus >95% with outflow to at least one crural artery. Clinical success was defined as a score of +1 or higher on the Rutherford recommended scale for gauging changes in clinical status. 8 The secondary endpoints included the incidence of minor and major amputations, death, minor- and major bleeding complications, additional interventions, patency of the treated native artery or conduit during follow-up, the first major adverse limb events (MALE), and the first major adverse cardiac events (MACE) during follow-up. Amputations performed through the tarsometatarsal joint or below were defined as minor, and those proximal to this joint as major. Bleeding was classified as minor if no invasive (surgical- or endovascular) interventions were necessary and as major if it was an intra- or retroperitoneal bleeding, intracranial bleeding, or when blood transfusion or invasive interventions were required and/or for which thrombolytic treatment needed to be interrupted. MALE was defined as ALI, major limb amputation, and the need for surgical or endovascular revascularization in the same limb. MACE was defined as cardiac arrest, myocardial infarction (MI), heart failure, or death unless clearly noncardiac.
Statistical Analysis
Normality of continuous variables was assessed using the Shapiro-Wilk test. Normally distributed continuous variables were presented as mean ± standard deviation (SD), while nonnormally distributed variables were presented as median with interquartile range (IQR). Categorical variables were presented as numbers and percentages. The following outcomes were analyzed by means of Kaplan-Meier estimates with standard error: patency, freedom from amputation, and survival rates. Statistical analyses were performed using SPSS Statistics 28 software (IBM, Armonk, NY).
Results
During the inclusion period, 443 patients treated with CDT for ALI were identified, of whom 58 patients had re-occlusions (Figure 1). A total of 116 re-occlusion cases occurred in these 58 patients, of which 39 cases were excluded because of surgical or conservative treatment. Among the 77 cases included, 52 were early re-occlusions and 25 were late re-occlusions that were treated with CDT. The total cohort had a mean age of 68±10 years, with a majority of patients being male (64.9%). Additionally, a significant proportion of cases (68.9%) experienced re-occlusion of a prosthetic bypass graft, resulting in ALI Rutherford grade IIA (Table 1). Patient characteristics and details of the occlusions are shown in Table 1. The overall etiology of ischemia was arterial thrombosis in 85.7% and arterial embolus in 14.3% of cases (Table 1). In the majority of cases, patients suffered from re-occlusion of a prosthetic femoropopliteal bypass. Most patients used anticoagulation at presentation (Table 1).
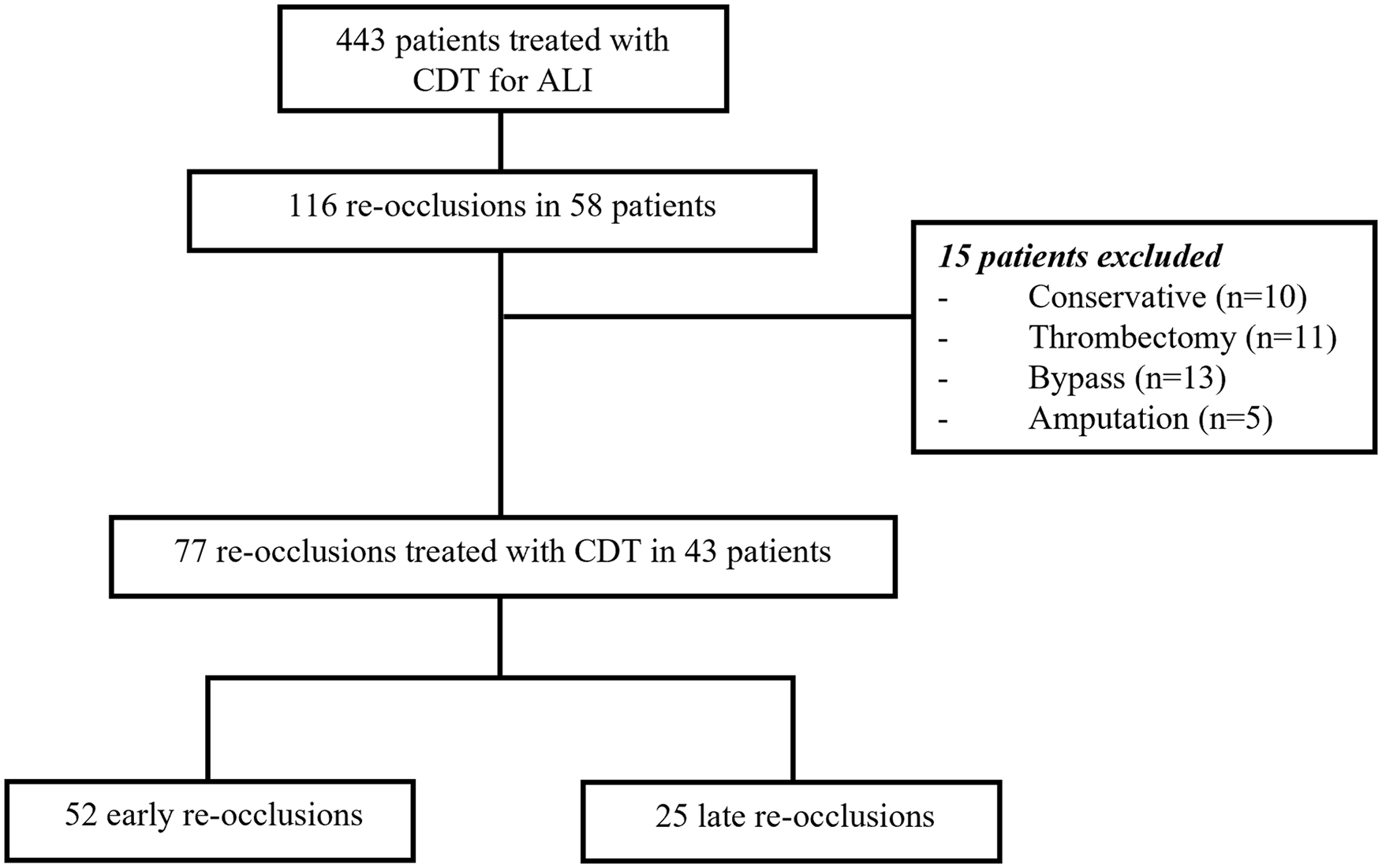
Ex- and included cases; values presented are cases.
Baseline Characteristics & Occlusion Details.
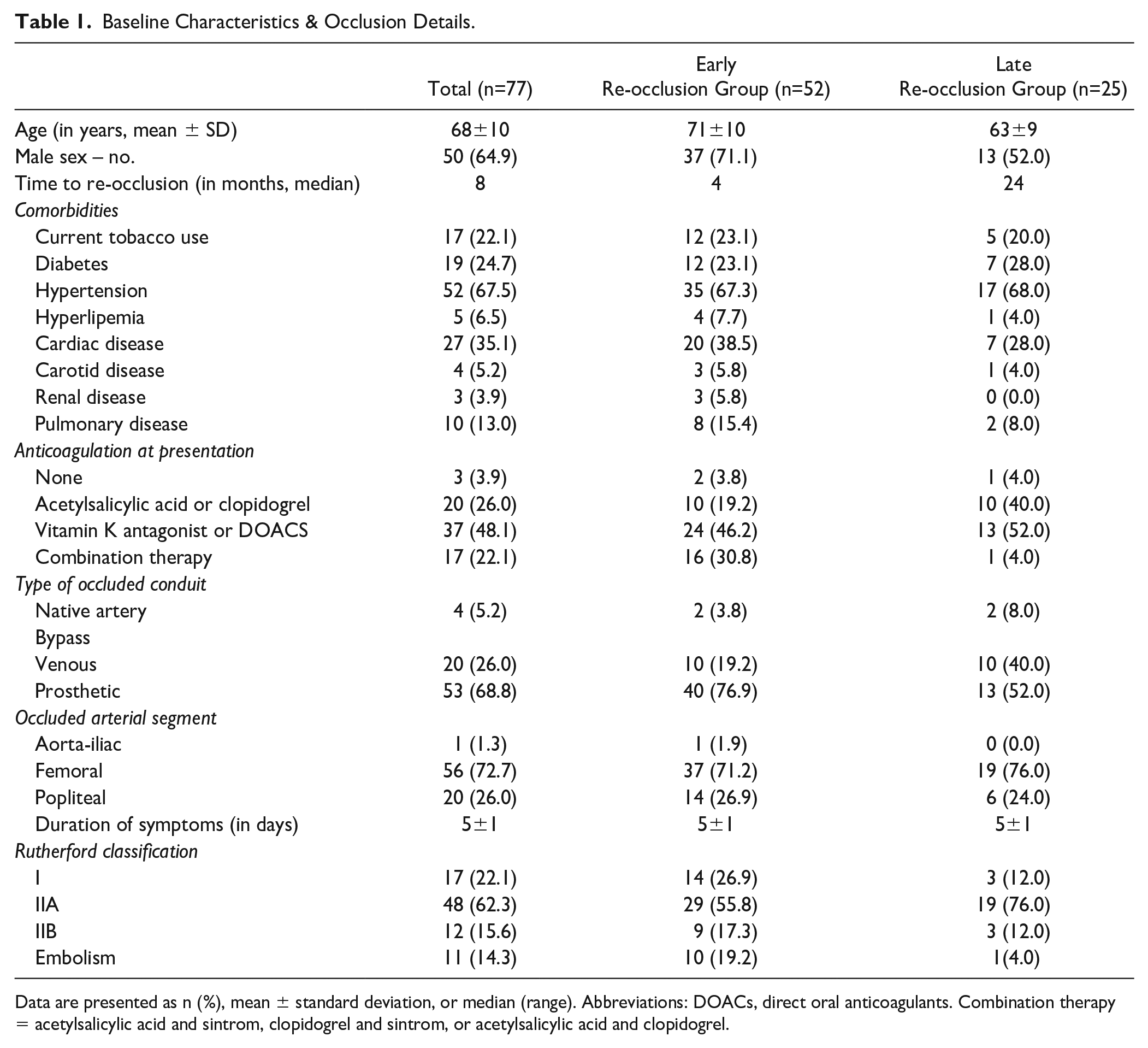
Data are presented as n (%), mean ± standard deviation, or median (range). Abbreviations: DOACs, direct oral anticoagulants. Combination therapy = acetylsalicylic acid and sintrom, clopidogrel and sintrom, or acetylsalicylic acid and clopidogrel.
Early Re-occlusion Group
The treatment characteristics and short-term outcomes of both groups are summarized in Table 2. The median time to re-occlusion since the last CDT treatment was 4 months (IQR=7). In the early re-occlusion group, clinical improvement was observed in 80.8% of cases, and angiographic success was achieved in 73.1% of cases. Adjunctive procedures were used in 63.5% of cases, including percutaneous mechanical thrombectomy (PMT) in 5 cases (guiding catheter [n=4] or AngioJet [n=1]). In cases in which patency could not be restored by endovascular means, additional surgical interventions were performed, including thromboembolectomy (n=9), bypass surgery (n=2), and amputations (n=3). In four cases, the surgical intervention was not successful, and amputation was needed. The most prevalent postoperative complications in the early re-occlusion group were minor bleeding, occurring in 25% of cases. Major hemorrhagic complications occurred in 1.9% (n=1) of the group. One patient died within 30 days after CDT due to heart failure. At discharge, acetylsalicylic acid or clopidogrel was prescribed in 7 cases, a vitamin K antagonist or direct oral anticoagulants (DOAC) in 27 cases, and a combination therapy in 18 cases.
Treatment Characteristics.
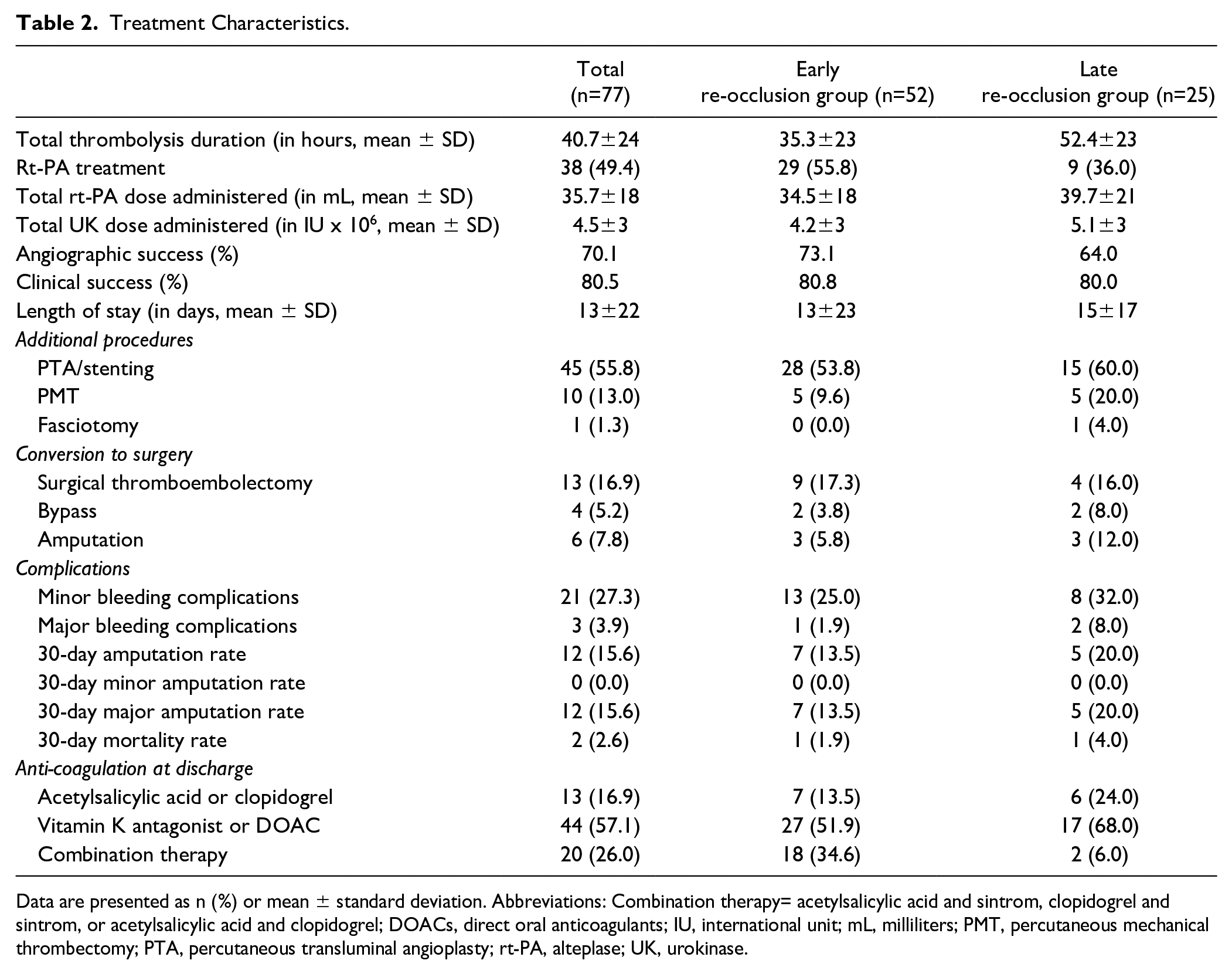
Data are presented as n (%) or mean ± standard deviation. Abbreviations: Combination therapy= acetylsalicylic acid and sintrom, clopidogrel and sintrom, or acetylsalicylic acid and clopidogrel; DOACs, direct oral anticoagulants; IU, international unit; mL, milliliters; PMT, percutaneous mechanical thrombectomy; PTA, percutaneous transluminal angioplasty; rt-PA, alteplase; UK, urokinase.
The median follow-up period for the early re-occlusion group was 15 months (IQR=38). During follow-up, a secondary re-occlusion was observed in 59.6% (n=31) of the early re-occlusion group. Freedom from secondary re-occlusion rates at 1, 5, and 8 years were 36.6±8%, 19.1±8%, and 19.1±8% for the early re-occlusion group (Figure 2). Freedom from amputation rates in the early re-occlusion group were 63.4±7%, 63.4±7%, and 47.6±14% at 1, 5, and 8 years, respectively (Figure 3). Survival rates were 97.9±2%, 59.8±11%, and 38.1±11% at 1, 5, and 8 years for patients with early re-occlusions (Figure 4). At 5 years follow-up, the incidence of MALE and MACE in the early re-occlusion group were 59.6% (n=31) and 13.5% (n=7) (Table 3).
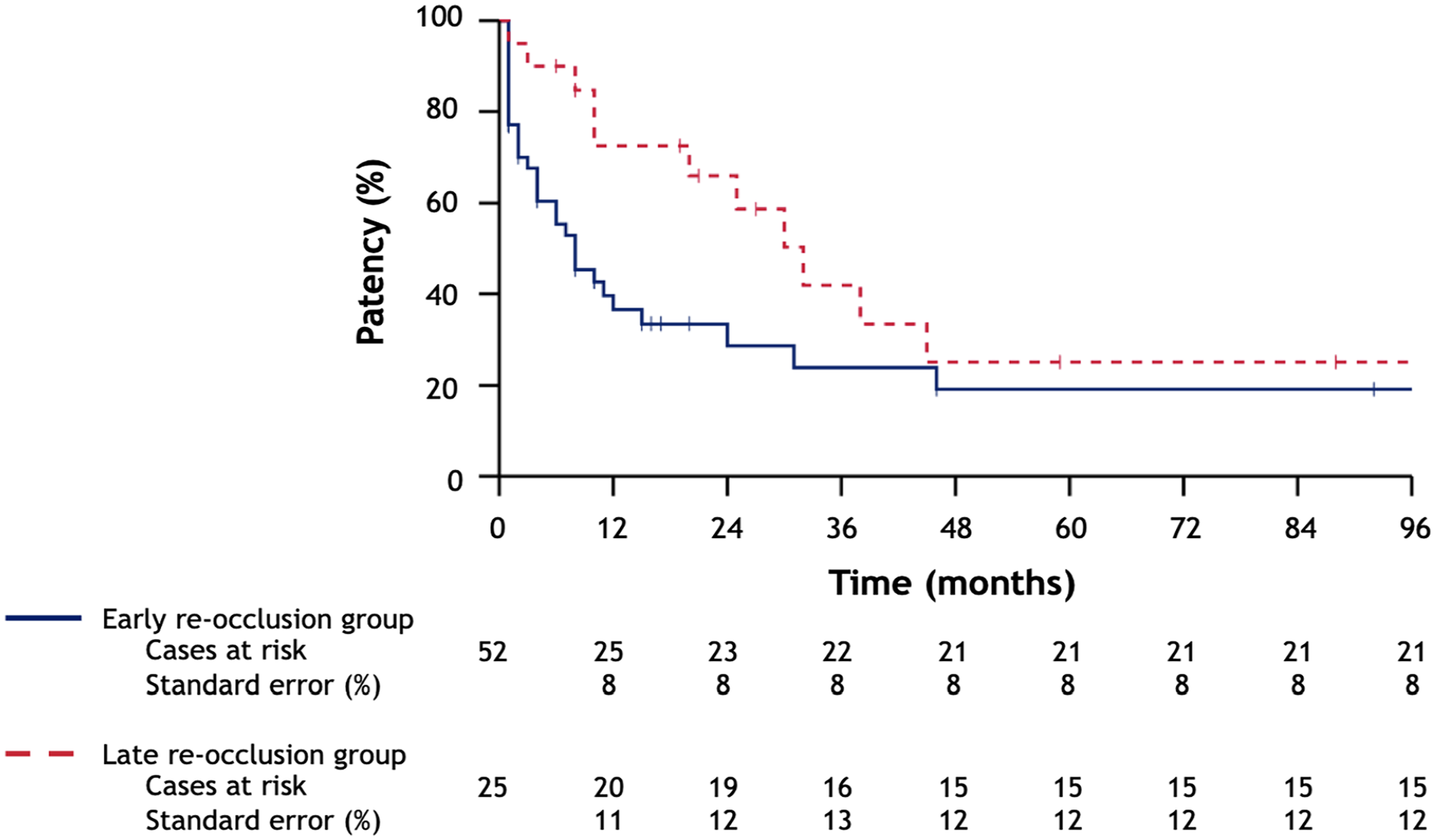
Kaplan-Meier survival curves—primary patency after CDT for patients that endured early or late re-occlusions; values are presented in cases.
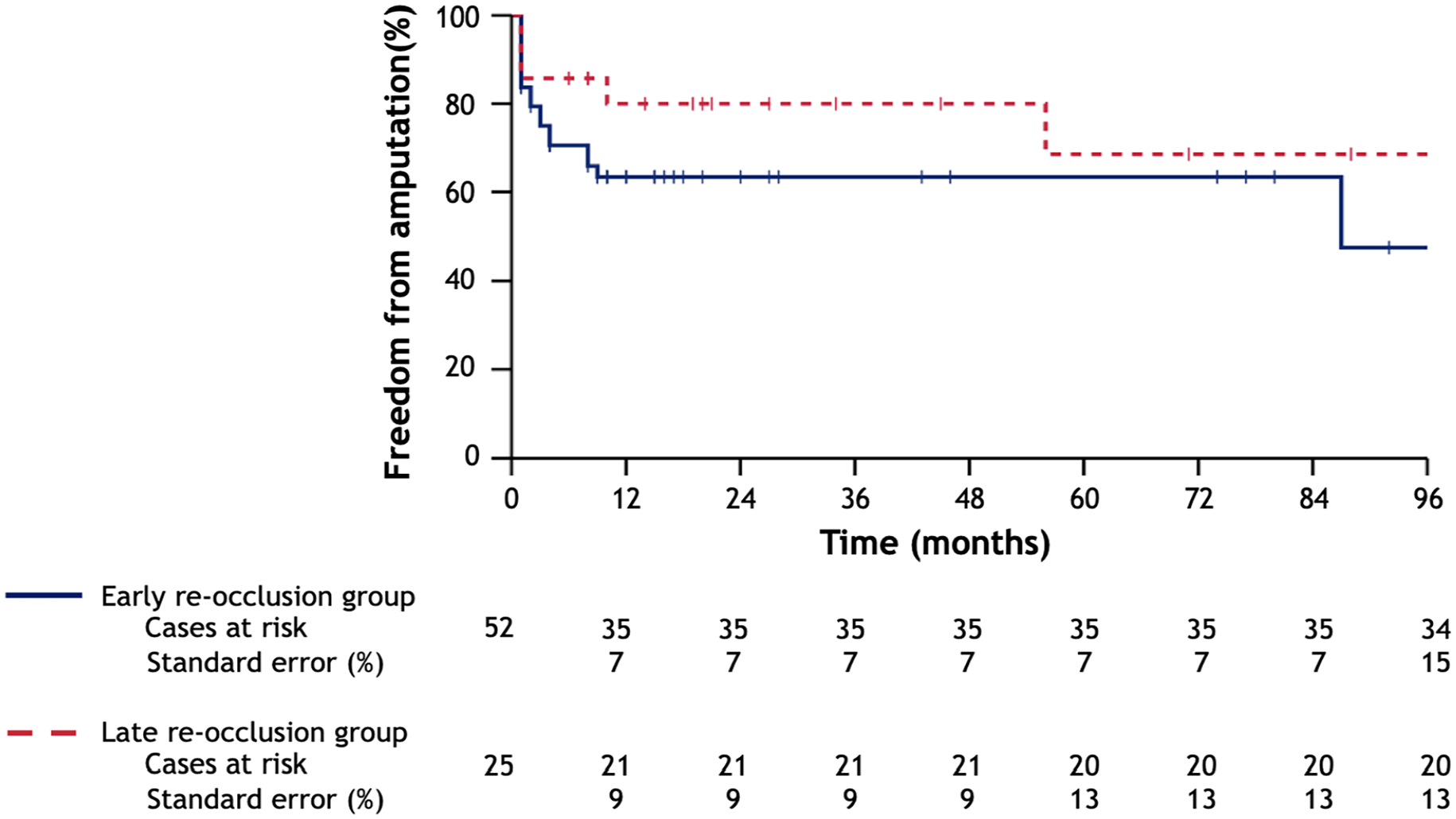
Kaplan-Meier survival curves—freedom from amputation after thrombolysis of patients that endured early or late re-occlusions; values are presented in cases.
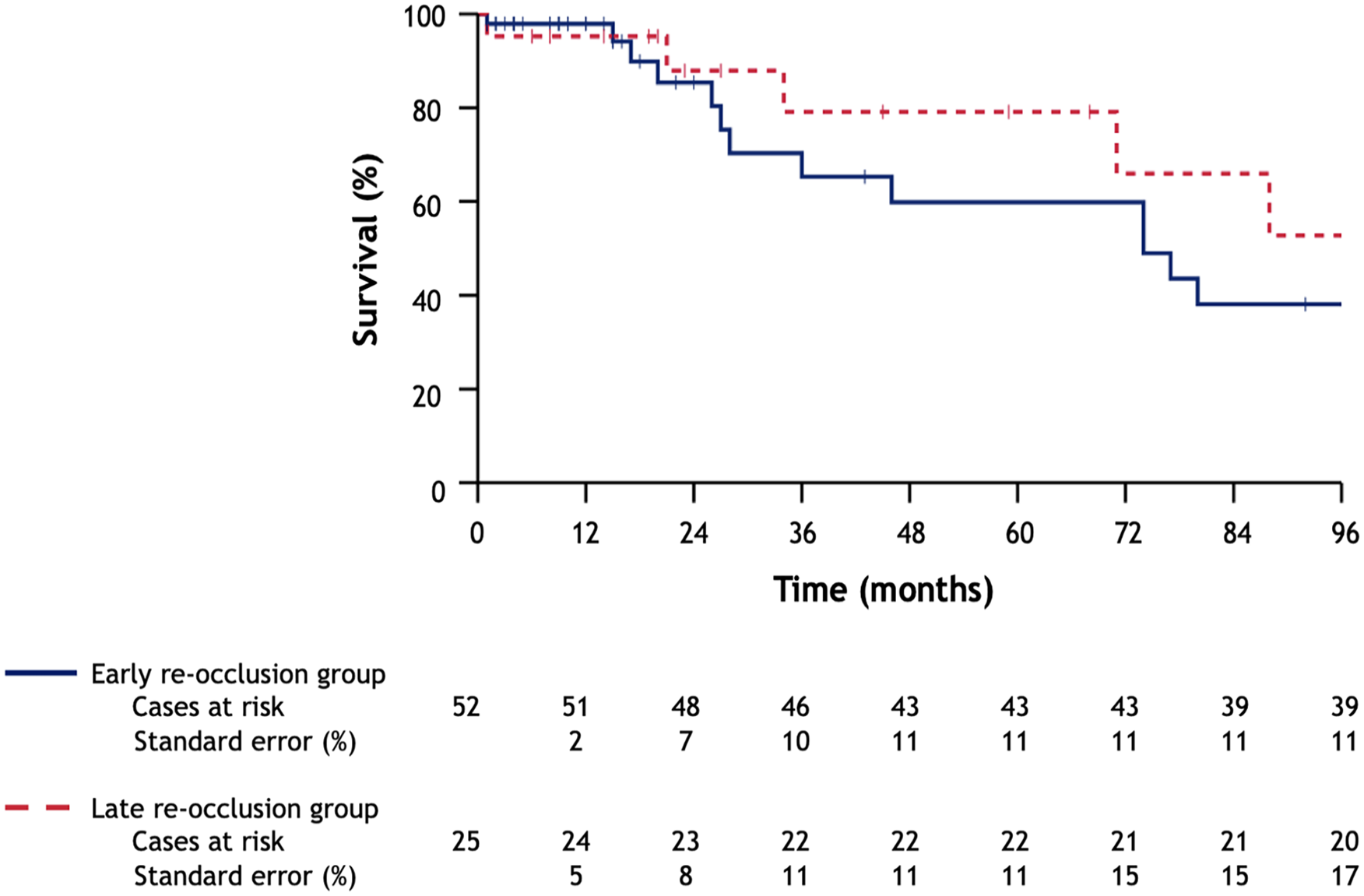
Kaplan-Meier survival curves—survival of patients that endured early or late re-occlusions; values are presented in cases.
MALE and MACE at 5 Years Follow-up.
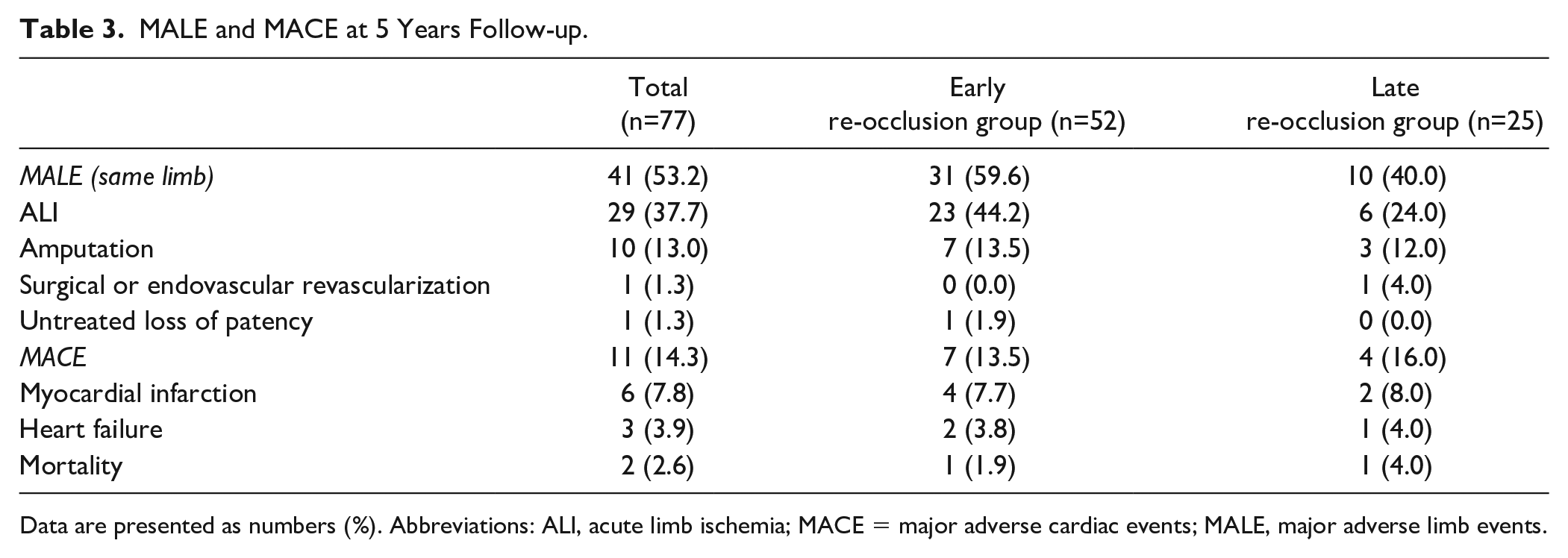
Data are presented as numbers (%). Abbreviations: ALI, acute limb ischemia; MACE = major adverse cardiac events; MALE, major adverse limb events.
Late Re-occlusion Group
The median time to re-occlusion since the last CDT treatment was 24 months (IQR=29) (Table 2). In the late re-occlusion group, clinical success was observed in 80% of cases, and angiographic success was achieved in 64% of cases (Table 2). Adjunctive procedures were used in 84% of cases. PMTs were performed in 5 cases using a guiding catheter. Additional surgical interventions were required in cases where patency could not be restored by endovascular means (thromboembolectomy in n=4, bypass surgery in n=2, and amputation in n=3). In two cases where thromboembolectomy was unsuccessful, a secondary surgical intervention, amputation, was needed. The most prevalent post-CDT complication in the late re-occlusion group was minor bleeding, occurring in 32.0% of cases. Major hemorrhagic complications occurred in 8.0% (n=2) of cases. One patient died within 30 days after discharge to home due to unknown reasons. At discharge, acetylsalicylic acid or clopidogrel was prescribed in 6 cases, a vitamin K antagonist or DOAC in 17 cases, and a combination therapy in 2 cases.
The median follow-up time for the late re-occlusion group was 22 (IQR=63) months. A second re-occlusion was observed in 44.0% (n=11) of the late re-occlusion group during follow-up. Freedom from secondary re-occlusion rates at 1, 5, and 8 years were 72.6±11%, 25.1±12%, and 25.1±12% for the late re-occlusion group (Figure 2). Freedom from amputation rates in the late re-occlusion group were 80.0±7%, 68.6±13%, and 68.6±13% at 1, 5, and 8 years, respectively (Figure 3). Survival rates were 95.2±4%, 79.1±11%, and 52.7±17% at 1, 5 and 8 years for the late re-occlusion group (Figure 4). The incidence of MALE and MACE at 5 years follow-up were 40.0% (n=10) and 16.0% (n=4) in the late re-occlusion group (Table 3).
Discussion
Our findings indicate that CDT is an effective revascularization method for both early and late re-occlusions of ALI, achieving a clinical success rate of 80%. Despite the high initial clinical success rate for early re-occlusions, 55% of cases endured a secondary re-occlusion within 1 year.
In this study, the efficacy of CDT was evaluated based on angiographic and clinical success rates. Clinical success was determined by the relief of acute limb ischemia symptoms. For patients presenting with acute-onset claudication, the Rutherford classification for chronic peripheral artery disease (PAD) was employed. 9 Current literature uses a variety of criteria to assess clinical success or failure, focusing on the extent to which a patient’s clinical status changes following endovascular treatments. To distill these criteria into meaningful measures and ensure their precise and consistent application, there is a pressing need for a standardized core outcome set (COS). Implementing a COS, grounded in evidence, will significantly improve the uniformity and comparability of outcome reporting for ALI.
In this study, it was hypothesized that re-occlusions, especially those occurring early, would result in poorer outcomes compared to initial events. Interestingly, our findings indicate that the short-term outcomes of these re-occlusions are comparable to those observed with initial CDT treatments.4,8 Nevertheless, only moderate success rates were observed in the late re-occlusion group, which may be partly explained by the higher proportion of occluded vein grafts among the late re-occlusion group. CDT has been shown to be more effective for occluded prosthetic grafts than for vein grafts.9,10 This non-normal distribution of this study’s data, largely attributed to limited patient cohorts, impeded further comparative analyses. In this cohort, the most common cause of failure following CDT was incomplete lysis, observed in 10 early and 6 late re-occlusion cases. Furthermore, residual stenosis was the cause of CDT failure in 4 cases (2 early and 2 late re-occlusions), and in 2 cases CDT had to be discontinued due to bleeding complications (one early and one late re-occlusions). In order to strengthen the interpretation of the present findings, future studies should explore the influence of diverse patient-level covariables on the outcomes of CDT for re-occlusions. Understanding these variables would help personalize treatment strategies to improve long-term outcomes.
Despite the high angiographic success rate of CDT and notwithstanding the meticulous treatment of culprit lesions, the observed long-term patency rates after re-occlusions are disappointing. The patency rates found in this study were considerably lower than the secondary patency rates reported in studies on primary CDT treatment for ALI. For instance, Grip et al reported a secondary patency rate of 75% at 5 years follow-up, 1 and another study showed a secondary patency rate of 65% at 5 years follow-up following CDT for occluded bypass grafts. 11 As is known for this patient group, the patients from this cohort also suffered from many comorbidities, with 20% of patients unable to quit smoking. The considerable loss of patency in this cohort was, however, not accompanied by an equivalent increase in amputation rates. An aggressive treatment strategy was opted for these re-occlusions, offering CDT or surgery, even after several occlusions. This approach might have had a beneficial effect on the freedom from amputation rates, as the amputation rates in our cohort were lower than those found in other studies.1,12 Nonetheless, more than 30% of patients suffered amputation within 5 years, indicating long-term results in this patient group need improvement. It is important to note that the long-term outcome of CDT has been closely associated with co-morbidities, while limb salvage may be more dependent on the success of the initial treatment and the severity of ischemia. 13
In the European Society for Vascular Surgery (ESVS) guidelines, CDT is not recommended for patients with not-immediately-threatened limb ischemia (Rutherford I). Prior to the dissemination of the ESVS guidelines, the thrombolysis protocol utilized in this investigation included patients with Rutherford I and II for the administration of CDT as a treatment approach. It’s essential to emphasize that the recommendation within the ESVS guidelines, based on insights from 2 cited papers, might not align with modern-day practices given the substantial advancements in CDT since to the original trials. A recent meta-analysis and systematic review highlighted that while thrombolytic intervention in Rutherford I ALI achieves high angiographic success, it is also associated with a substantial risk of mortality and poor long-term outcomes. 14 Whether this overrides the immediate benefits of CDT remains to be determined.
The ESVS guidelines recommend considering long-term anticoagulation after endovascular treatment of a prosthetic bypass occlusion. A study conducted by Vakhitov et al determined that the lack of anticoagulant or antiplatelet medication was independently associated with the occurrence of re-occlusions. 5 Furthermore, antiplatelet therapy or anticoagulants are recommended for re-occlusions after previous revascularization to reduce cardiovascular events following CDT, though no specific preference on type of antithrombotic therapy has been established. 11 In line with this finding, the vast majority of our patients received anticoagulation, and some patients received single antiplatelet therapy.
While thrombolytic treatment has improved over the last 2 decades, the risk of hemorrhage remains high in the literature. Systemic heparinization and prolonged duration of treatment were previously linked to an increased bleeding risk. 3 The ESVS guidelines recommend against the use of concomitant systemic heparinization to reduce the bleeding risk during CDT. 3 As a result, all patients of this study received subtherapeutic doses of heparin through the arterial sheath, solely to prevent peri-catheter thrombosis. This approach, along with the use of low to moderate doses of thrombolytics, resulted in a relatively low incidence of major bleeding complications in this cohort. However, minor bleeding complications in this study were relatively high compared to other studies.4,7 Minor bleeding complications can, however, easily be managed by noninvasive interventions. It should also be noted that the number of patients included in this study is small. Thus, the incidences of bleeding complications should be interpreted with caution.
Strengths & Limitations
The main strength of this study is the long-term follow-up time, which allowed us to investigate the real-world outcomes of CDT for early and late re-occlusions in ALI. Furthermore, a complete database was utilized with a low number of missing values. However, this study has some limitations, including its retrospective design, the small number of patients included due to the patient group’s specific inclusion criteria, and the inclusion of patients was limited to cases in which the first and subsequent re-occlusion occurred in 1 of the 2 medical centers. This was specifically done to ensure accurate information on previous CDT treatment. A small number of patients were included more than once in this study, as some had multiple re-occlusions; each case of re-occlusion was analyzed separately. Due to the retrospective nature of this study and the extended inclusion period, inevitable changes were made to the protocols based on emerging literature, leading to differences in thrombolytic dosage regimens and follow-up visits. Future prospective cohort studies should aim to standardize follow-up protocols and treatment regimens to minimize these variabilities and improve the consistency and reliability of the outcomes. Notably, the primary objective of this study was not to compare early versus late re-occlusions. Instead, the study aimed to offer an overview of the outcomes of CDT for re-occlusions occurring at 2 time intervals during the follow-up period. Due to the small sample size, it is not feasible to provide p-values for each variable, as the statistical power would be insufficient to draw reliable conclusions. Future research with larger sample sizes is necessary to explore these influential factors comprehensively. The outcomes derived from this study hold the potential to serve as a benchmark for guiding future research endeavors in the field. Moreover, these findings carry considerable relevance for patients and physicians engaged in the decision-making process concerning CDT for ALI re-occlusions.
Conclusion
This study showed that CDT can be performed to revascularize patients with both early and late re-occlusions, achieving angiographic and clinical success comparable to CDT for first occlusions. Long-term outcomes, however, are limited by secondary re-occlusions and limb loss. Therefore, future studies should focus on maintaining patency after successful CDT for ALI.
Footnotes
Author Contributions
SO, SD, AH, and VJ wrote the manuscript. SO, SD, AW, AH, KY, and VJ critically revised the manuscript, and all authors approved the final version of the manuscript.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: One of the authors of this article is the editor-in-chief of the journal. To avoid a conflict of interest, an alternate member of the Editorial Board handled this submission.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Prior presentations
None.
