Abstract
Introduction:
With the world population growing and aging, nonagenarians have become a distinct patient cohort with specific characteristics that render the prediction of outcomes essential. We aimed to investigate the specific characteristics of this patient’s cohort in a tertiary vascular center.
Materials and Methods:
Retrospective analysis was conducted for all consecutive patients 90 years and above referred or treated in the Department of Vascular Surgery between January 2017 and December 2022 for vascular pathologies. The main endpoint was to analyze the type of vascular services required for nonagenarians. Additional endpoints involved evaluation of treatment outcomes during the study period based on medical records. The analysis was patient-based.
Results:
A total of 148 nonagenarians were included in the study. In all, 71 (48%) of the patients underwent surgery, whereas 77 (52%) had conservative treatment. Most of the patients were referred for peripheral arterial (PAD; 56, 37.8%) and aortic-related (39, 26.4%) diseases. Other pathologies encountered involved acute limb ischemia (ALI; 25, 16.9%), carotid diseases (12, 8.1%), renal/dialysis-related consultations (8, 5.4%), and referrals from other departments (12, 5.4%). Urgent interventions were performed in 27% of the cases. Indications for surgery included PAD Rutherford Stages IV, V, and VI; symptomatic and ruptured aortic aneurysms; ALI Rutherford Stages I, IIa, and IIb; symptomatic and near total occlusion asymptomatic carotid disease; and dialysis-related procedures for patients with chronic renal failure on regular hemodialysis. Perioperative complications were experienced in 22 patients (14.9%), the 30-day reintervention rate was 7.4%, and 30-day mortality was 4.7%. The overall length of hospital stay for operated patients was a median of 8 nights.
Conclusion:
The proportion of nonagenarians in the population is growing and so is their referral to vascular surgery. Satisfactory short-term treatment outcomes can be achieved in this highly selected cohort of patients. Thirty-day mortality is higher in patients undergoing urgent procedures. Follow-up mortality was higher in the operated nonagenarians as compared with those who were treated conservatively. Careful patient selection and thorough preparation are crucial to enhance clinical outcomes. Further research on therapy outcomes of nonagenarians will enable physicians to make better evidence-based approaches to individual patients and should be encouraged.
Clinical Impact
The study highlights the growing need to manage vascular diseases in nonagenarians, emphasizing that age alone should not exclude patients from surgical interventions. By demonstrating acceptable short-term outcomes with careful patient selection, this research challenges the traditional bias against operating on the elderly. Clinicians should refine risk assessment and treatment plans, particularly when balancing surgical and conservative options. Comorbidities, rather than age, are key determinants of patient suitability, encouraging more individualized, evidence-based approaches in this expanding demographic.
Introduction
As the population is growing, the number of nonagenarians (≥90 years old) is anticipated to increase exponentially. In the European Union, the number of nonagenarians is expected to triple by 2080 (1 067 941 currently to 2 920 806). 1 Similarly, in the United States, people aged 80 years and older are estimated to reach 4.3% of the total population by 2050. 2 This increasing age expectancy will likely lead to an increase in surgical procedures in addition to health care–related costs. Vascular surgery is anticipated to record one of the highest projected demand growths by 2025 among all specialties, 3 and with such an aging population, the fragility of patients to different vascular diseases and interventions remains inadequately explored.
Due to significant advancements in endovascular procedures, the morbidity and mortality rates in the elderly population have considerably improved when compared with traditional open surgical interventions. 4 Despite improved perioperative outcomes with minimally invasive procedures, age remains an inherent risk factor, with nonagenarian patients considered high-risk patients. 5 However, despite the aging population, studies reporting on vascular disease prevalence and outcomes in this subset of patients remain scarce, with only some reports on the results of endovascular aneurysm repair (EVAR) in nonagenarians.6–9
As life expectancy is projected to increase worldwide, it is important to understand the association between nonagenarians and vascular diseases, report complications, and perioperative results. This will facilitate decision-making, allowing us to choose the best medical treatment for each patient. The aim of this study was to describe a single-center experience in the management of nonagenarian patients and their short-term outcomes.
Materials and Methods
Study Design
A retrospective study was conducted including all consecutive nonagenarian patients (90 years and older) undergoing either evaluation and treatment or hospitalization by the Department of Vascular Surgery in a high-volume tertiary center, between January 2017 and December 2022. Data were collected through available medical records and clinical reports. Patients were included if they received a vascular surgery–related medical consultation, primary vascular intervention or secondary to other departments’ operations, or hospitalization with conservative treatment and follow-up. Ethical committee approval was waived because of the retrospective design of the study with anonymized data analysis.
Study Population
Data collected included patient demographics, baseline characteristics, type of underlying vascular disease, intraoperative details, and postoperative outcomes. Baseline characteristics included coronary artery disease, congestive heart failure, hypertension, chronic kidney disease, dialysis, chronic obstructive pulmonary disease (COPD), diabetes mellitus, history of stroke, cancer, as well as estimated glomerular filtration rate (eGFR) and serum creatinine on admission. Intraoperative variables collected included type of anesthesia, total operative time, fluoroscopy time, radiation, and contrast dose. Postoperative outcomes involved intensive care and overall length of hospital stays, and 30-day outcomes including complications, reinterventions, and mortality. Postoperative complications included either medical (myocardial infarction [MI], respiratory insufficiency, dialysis, acute kidney injury [AKI], stroke) or surgical (access hematoma, infection, pseudoaneurysm, and wound dehiscence) complexities. Postoperative MI was defined as electrocardiographic changes or new elevation of troponin more than 3 times the upper level of reference range, intraoperatively or within 30 days after the procedure. 10 Acute kidney injury was based on eGFR evaluation 48 to 72 hours after the procedure, using the RIFLE criteria where AKI was defined as a drop in eGFR of at least 25%.11,12
The study cohort was categorized initially according to those who underwent surgical interventions and those who did not. Further analysis was continued by classifying patients according to underlying pathology into acute limb ischemia (ALI), peripheral arterial disease (PAD), aortic-related diseases (including aneurysms, dissections, intramural hematoma, and penetrating ulcer), carotid artery disease, and dialysis-related interventions. Both PAD and ALI were diagnosed and staged according to the Rutherford classification. 13 An additional category was created for patients who were referred for vascular intervention from other departments (Referrals), including access and vessel-related complications post-catheterization procedures.
Endpoints
The primary endpoint was to analyze the type of vascular services required for nonagenarians and to evaluate treatment outcomes during the study period based on medical records. Secondary endpoints included operative time and complications for those who required an intervention, as well as 30-day reintervention and mortality rates. The analysis was patient-based.
Statistics
Data were collected in a Microsoft Excel worksheet and analysis was performed using SPSS version 28.0 (IBM Corp, Armonk, New York). Continuous variables were tested for normality using the Kolmogorov-Smirnov test. Those with normal distributions were represented as mean±standard deviation (SD) and as median and interquartile range (IQR) if they did not. Categorical data were expressed in numbers and percentages. Student t-test and analysis of variance were used to analyze parametric continuous variables, whereas the Kruskal-Wallis test was used for nonparametric data. Pearson χ2 and Fisher exact tests were used for the analysis of categorical variables. A p value of <0.05 was used to determine statistical significance.
Results
General Cohort
One hundred and forty-eight patients were identified and included in the study, with a mean age of 92.7±2.4 years and a slight male predominance (52.7%) (Tables 1 and 2). A summary of the demographics and baseline characteristics can be found in Table 1.
Demographics and Baseline Characteristics of Study Patients.

Abbreviations: BMI, body mass index; CAD, coronary artery disease; CHF, congestive heart failure; CKD, chronic kidney disease; COPD, chronic obstructive pulmonary disease; Sr. Cr., serum creatinine; eGFR, estimated glomerular filtration rate; SAPT, single antiplatelet therapy; DAPT, dual antiplatelet therapy; DOAC, direct oral anticoagulation.
Surgical Versus Conserved Patients in Terms of Disease Classification and Their Outcomes.

Abbreviations: ICU, intensive care unit.
Bold text indicates significance (p<0.05)
A total of 71 (48%) patients required surgical repair. Indications included ALI (24, 33.8%), PAD (20, 28.2%), aortic diseases (7, 9.9%), dialysis-related (8, 11.3%), Referrals (8, 11.3%), and carotid diseases (4, 5.6%). Seventy-seven patients (52%) were managed conservatively, of which all presented with primary vascular diseases and no referrals from other departments.
Vascular Pathologies
PAD
The most frequent vascular pathology encountered was PAD, affecting 56 of the included patients (37.8%) (Tables 2 and 3). Ultimately, 20 (35.7%) required surgery, whereas 36 (64.3%) were treated conservatively. Indications for invasive treatment included ischemic rest pain (Rutherford IV; n=3) and tissue loss or gangrene (Rutherford V and VI; n=17). Treatment modalities included endovascular procedures in 15 patients, open surgeries in 3, and 2 hybrid repair where both open and endovascular means were used. A summary of the different diagnoses and treatment procedures performed is represented in Table 3.
Indications and Procedures for Operated Nonagenarians.

Abbreviations: AAA, abdominal aortic aneurysm; AIOD, aorto-iliac occlusive disease; ALI, acute limb ischemia; CFA, common femoral artery; CIA, common iliac artery; DCB, drug-coated balloon; DES, drug-eluting stent; EVAR, endovascular aneurysm repair; GSV, great saphenous vein; IBD, iliac branched device; ICA, internal carotid artery; IIA, internal iliac artery; IV, intravenous; LSA, left subclavian artery; PAD, peripheral arterial disease; PAU, penetrating aortic ulcer; PFA, profunda femoris artery; POBA, plain old balloon angioplasty; POPA, popliteal artery; PTA, percutaneous transluminal angioplasty; SFA, superficial femoral artery; TAA, thoracic aortic aneurysm; TEVAR, thoracic endovascular aortic repair.
Patients managed conservatively included 3 patients with Rutherford Stage 0, 17 with Rutherford Stages I to III, and 16 with tissue loss and/or ulcer Rutherford Stages IV to VI. In the latter group, 2 refused intervention and decided to go with conservative treatment. The remaining 14 patients were treated conservatively for ulcers that were dry, small-sized, and/or had no signs of inflammation. Reasons to go with conservative treatment for such patients included being bedbound, having chronic wounds and infections that were treated with topical measures and antibiotics, and/or receiving vacuum-assisted closure therapy with close follow-up.
Aortic
Thirty-nine patients presented with aortic diseases, with most of them being treated conservatively (n=32, 82.1%), and only 7 (17.9%) required an intervention. Indications for treatment included 5 infrarenal abdominal aortic aneurysms (AAA), 1 thoracic aortic aneurysm (TAA), and 1 penetrating aortic ulcer (PAU). Four patients were treated due to rupture (2 ruptured infrarenal AAAs, 1 contained ruptured juxtarenal PAU, and 1 ruptured TAA). One patient presented with infrarenal AAA and had associated aneurysmal 8 cm diameter iliac bifurcation. The patient initially presented with hematuria and when computed tomography (CT) was performed the aneurysm was diagnosed, and suspicion of a fistula was not ruled out. One patient presented with symptomatic infrarenal aneurysm of a maximum diameter of 60 mm and the last patient had an asymptomatic infrarenal AAA with a maximum diameter of 62 mm. Both were deemed at acceptable surgical risk for endovascular treatment as per their life expectancy, cardiopulmonary function, and multidisciplinary team consultation especially the anesthesia team.
Endovascular modalities were employed in 6 patients (5 EVAR and 1 thoracic endovascular aortic repair [TEVAR]), whereas only 1 patient underwent open aortic repair. The patient who had received open repair had a long history of deteriorating kidney functions and presented with a ruptured infrarenal AAA with high suspicion of infection based on CT appearance. He also had an accessory left renal artery of significant size just below the main left renal artery. Endovascular treatment was considered of high risk in terms of contrast-induced nephrotoxicity and infection. Open repair was performed in the form of an aorto-bi-iliac bypass with rifampin-soaked silver graft and omental flap closure.
Six of these patients received general anesthesia, whereas 1 had local anesthesia. All 6 patients who had endovascular procedures had percutaneous femoral access with closure using suture-mediated closure devices.
Thirty-two patients were managed conservatively; 18 presented with asymptomatic aortic aneurysms of a mean maximum diameter of 62.4±15.0 mm, 7 with PAU, 4 had endoleaks (3 type Ia and 1 type II), 2 with intramural hematoma type B one with maximum wall thickness of 5 mm and the other of 11 mm, and 1 with uncomplicated acute type B aortic dissection. Treatment was indicated in 9 patients as per the European Society for Vascular Surgery (ESVS) recommendations13,14 where intervention was refused in 8 (5 patients with aneurysms, 3 with endoleak Ia) and 1 infrarenal AAA of maximum diameter of 59 mm was treated conservatively due to advanced multiorgan disease of these 32 patients (5 patients with aneurysms, 3 with endoleak Ia) (Table 4). Patients with aortic aneurysms who were conservatively treated did not qualify for intervention in terms of symptomatology and aneurysm diameters and patients with PAUs were uncomplicated with no high rupture risk parameters.14,15
Nonoperated Nonagenarians.

Abbreviations: ICA, internal carotid artery.
Acute limb ischemia
Acute limb ischemia was present in 25 patients (16.9%), 24 of whom underwent invasive treatment. Four patients presented with Rutherford Stage I, 16 with Rutherford Stage IIa, and 4 patients with Rutherford Stage IIb. Eighteen patients underwent open surgical treatment, 5 had endovascular procedures, and 1 hybrid repair. The 1 patient who was treated conservatively had viable ischemia (Rutherford Class I) and was treated initially with anticoagulation to which he responded well. A summary of the different procedures performed can be found in Table 3.
Carotid
Twelve patients (8.1%) were evaluated due to carotid artery disease. Seven had asymptomatic internal carotid artery (ICA) lesions and 5 had symptomatic stenosis. Four patients (33.3%) underwent surgical repair, including 3 symptomatic stenosis and 1 asymptomatic near total occlusive lesion diagnosed in a patient with a previous history of Wernicke aphasia and transient ischemic attack 2 years ago. Carotid endarterectomy was implemented in all 4 cases, with 2 patients undergoing the eversion technique and 2 having bovine patch closure. All surgeries were performed under regional anesthesia in the form of cervical block with added local anesthesia when needed.
Asymptomatic patients included 1 near total occlusion of ICA (history of TIA with Wernicke aphasia 2 years prior), 1 restenosis of the left common carotid artery and ICA (stenosis 70%–80%) after previous surgical repair, 1 with 90% ICA stenosis, and 4 with <50% stenosis. The decision to conserve or treat asymptomatic patients was based on a multidisciplinary team that was formed of members from the departments of vascular surgery, neurology, interventional radiology, and anesthesia.
Dialysis
Eight patients (5.4%) were referred due to dialysis access consultations. All the presented patients had end-stage chronic renal disease on regular hemodialysis. All 8 patients had therapeutic procedures. The procedures performed included the placement of permanent hemodialysis catheters (n=6) and open surgical thrombectomy of access shunt (n=2). In the latter group, 1 patient received an additional bovine patchplasty due to juxta-anastomotic stenosis, and the other patient had additional resection of an aneurysmal vein segment.
Referrals
Eight patients (5.4%) were referred from other departments due to vascular access–related complications, of which all underwent surgical repair. Seven were following cardiac catheterization procedures and 1 was during a neurosurgical procedure. Five cases of access vessel injury presented with bleeding and 2 cases presented with access pseudoaneurysms. One case presented with limb ischemia and underwent angiography, which did not reveal stenosis but instead showed spasm of the infrainguinal vessels that were treated with heparinized saline and vasodilator agents.
The patients turned down, and the turndown rate of the whole cohort as well as for each disease category can be found in Table 5.
Turndown Rate.
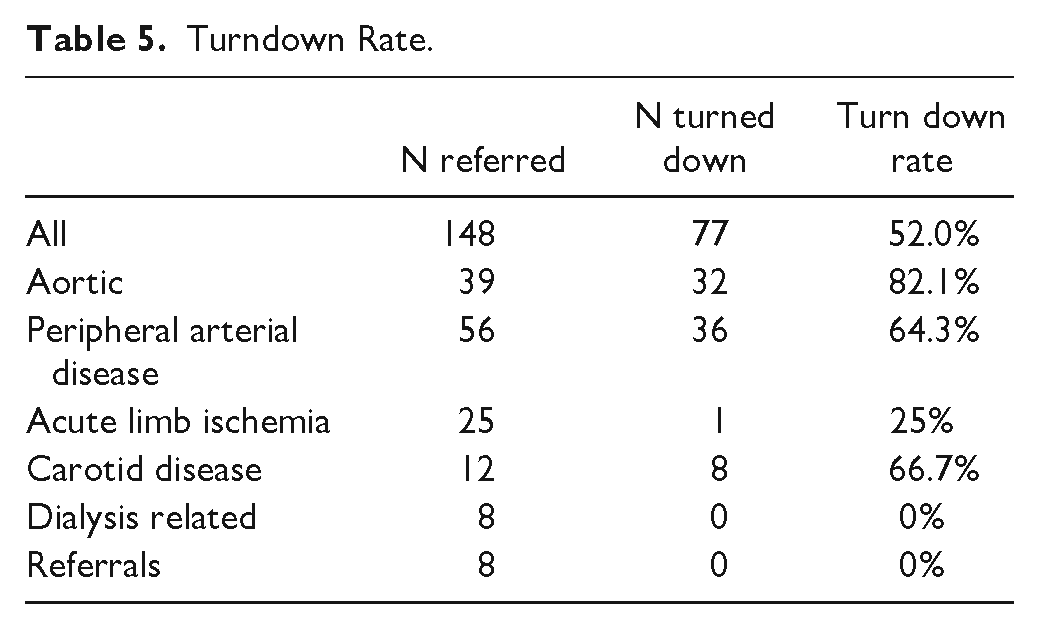
Postoperative Outcomes
The 30-day period recorded complications in 22 patients, 21 among the operated patients and 1 with a conservatively treated PAD patient who developed a urinary tract infection (Tables 3 and 6). Of the operated patients, 4 had access hematomas (2 ALI and 2 PAD), 3 (2 ALI and 1 PAD) were managed conservatively, and 1 (PAD) underwent hematoma evacuation. Three patients had wound dehiscence and 2 had femoral artery pseudoaneurysms. Two PAD and 2 ALI patients had reocclusion. One of the mentioned ALI patients who presented with reocclusion was recommended a major amputation; however, the patient ultimately refused and was discharged with wound management. One ALI patient developed postoperative compartmental syndrome. One PAD patient had a major stroke, and one aortic patient had an unfortunate aortic rupture. Two aortic patients had endoleak type Ia. One of them was an infrarenal aortic aneurysm and was treated with a Palmaz stent. The other patient had a ruptured TAA and received TEVAR with left subclavian artery stenting. His immediate postoperative CT scan showed an endoleak type Ia, but he refused further interventions. One PAD patient had increasing respiratory insufficiency, which was resolved conservatively with supportive measures, 1 presented with AKI following a short period of postoperative hypotension that resolved with fluids, and 1 presented with AKI and a rise in liver enzymes that was treated conservatively.
Operated Nonagenarians.

Abbreviations: ALI, acute limb ischemia; BMI, body mass index; PAD, peripheral arterial disease; ICU, intensive care unit.
The 30-day reintervention rate was 7.4% (n=11). One patient with a type Ia endoleak following an EVAR for a ruptured infrarenal AAA was treated with proximal extension with a Palmaz stent. Two patients had femoral hematoma evacuation and 2 with wound dehiscence had secondary sutures. The 2 femoral pseudoaneurysms were repaired surgically. Two PAD patients who had reocclusion underwent amputation (1 major and 1 minor). One ALI patient with reocclusion was reintervened with endovascular atherectomy and plain balloon angioplasty. The last patient was ALI and developed postoperative compartmental syndrome following revascularization and ultimately underwent a fasciotomy.
The 30-day mortality rate was 4.7% (n=7); 6 of which were operated, and 1 was conservatively treated and died because of multiorgan failure (PAD Rutherford V). One aortic patient died secondarily to respiratory and cardiac failure after open surgical repair of a ruptured infrarenal AAA. One patient with PAD died due to multiorgan failure secondary to sepsis. One referred patient died due to bleeding following injury to the femoral artery. Three patients presenting with ALI died; 1 due to acute coronary syndrome and AKI following revascularization, 1 following a major stroke with complete hemispheric infarction, and the third developed acute renal failure following recanalization of his popliteal artery occlusion. Reocclusion of the popliteal artery later occurred, and major amputation was recommended. However, the patient refused, and he ultimately died due to multiorgan failure.
When comparisons were made between urgent and nonurgent procedures, higher 30-day mortality was noted among the urgent patients (6, 15% vs 0; p=0.032). As for those who underwent open and endovascular procedures, no differences were found regarding intensive care unit (ICU) and hospital stay, operative details, 30-day and follow-up outcomes. Tables 7 and 8 illustrate the findings.
Comparing Urgent and Nonurgent Patients in Terms of Stay Period, Operative Details, and Outcomes.

Abbreviations: ICU, intensive care unit.
Comparing Patients Treated by Open and Endovascular Means in Terms of Stay Period, Operative Details, and Outcomes.

Abbreviations: ICU, intensive care unit.
Hospitalization and Follow-up
The median length of hospital stay was 8 nights (IQR 3–15), with patients who have had surgery requiring longer hospitalization times compared with the conservative cohort (9 nights, IQR 6–18 vs 6 nights, IQR 1–14; p=0.003). Operated patients also had longer IQR ICU stay which was statistically significant (p<0.001). Follow-up recorded a median of 19 days (IQR 8–122).
Discussion
Nonagenarians represent a significant proportion of our current societies, and their numbers are increasing with time. Due to increased experience with younger generations, improved medical and surgical technology, and enhanced lifestyles, the numbers are expected to rise widely.1–8,16 In addition, the life expectancy of nonagenarians at 90 and 95 years is calculated at around 4.8 and 3.6 years, respectively. 17 Consequently, the number of nonagenarians referred to vascular surgery centers is yet to rise. However, the benefits must be carefully weighed against the potential risks of planned medical therapy or surgery. The decision with conservative treatment has been the preferred management strategy for high-risk patients with multiple comorbidities. However, how to best manage each vascular pathology in this age group remains unanswered. Given that long-term follow-up remains a challenge, few studies have been published on vascular diseases in nonagenarians, and if age alone is sufficient to decide if a patient is a candidate for surgical treatment. Health care costs and benefit-risk relationships are therefore additional important aspects to be analyzed and studied to provide optimal management.18–20
Advancements in endovascular aortic repair have enabled surgeons to operate on high-risk patients who may not be suitable for open surgical repair. Nonagenarians might be considered high-risk patients because of advanced age. However, our group published a study of 349 cases of AAA repair in nonagenarians reported in the National Surgical Quality Improvement Program (NSQIP) from 2005 to 2010, comparing EVAR and open surgical repair (OSR), and the 30-day overall mortality was 3.8% after EVAR and 18.8% after OSR. 9 Furthermore, Prendes et al 8 conducted a retrospective analysis of the American College of Surgeons’ NSQIP database involving 12 267 patients, of whom 365 nonagenarian patients underwent EVAR and found that being nonagenarian with similar comorbidities to younger patients was not associated with higher 30-day mortality after EVAR.
In 2011, a study involved 176 patients with 102 women who underwent 196 procedures for various pathologies, including acute and chronic limb-threatening ischemia, aortic and popliteal aneurysms, and carotid stenosis. The overall morbidity and mortality rates were acceptable. 21 In addition, a retrospective study was published in 2021 which demonstrated how age was not an independent predictor of short-term 30-day mortality or major adverse events following endovascular aortic repair in nonagenarians. 8 The study included ruptured aneurysms and postoperative outcomes documented renal impairment and bleeding complications. However, when compared with non-nonagenarians, no significant differences were found. When considering EVAR for nonagenarians, age should not be the only factor in determining a decision for treatment, but appropriate timing and referring to the standard guidelines are mandatory. 22 Bruno et al 23 analyzed the outcomes of 7900 acutely admitted nonagenarians and octogenarians to the ICU. Nonagenarians demonstrated no higher 30-day mortality than octogenarians (27 vs 27%, respectively).
This was reported more than 20 years ago when KM Jain reported on 30-day and 24-month outcomes for ≥90-year-old patients undergoing various vascular procedures. 24 In terms of ICU stay, a study analyzing outcomes for nonagenarians acutely admitted to the ICU showed no differences between them and octogenarians in terms of ICU and 30-day mortality. 24 In short, this proves that there are other factors to consider before deciding on a surgical procedure for nonagenarians based on age, where comorbidities could have an equivalent or even superior role in determining the necessity of intervention. Conservative treatment has also been a therapeutic option for many nonagenarians presenting with vascular pathologies. It has achieved satisfactory outcomes in selected patients, yet the quality of life remains a concern.18–20
The present study analyzed the outcomes of operated and conservatively treated nonagenarians with different vascular pathologies and attempted to determine the possible correlation between age and complications. Many patients were treated conservatively (n=77; 52.0%). Cardiovascular risk factors were comparable across both cohorts; however, COPD was more common in the nonoperative group, indicating a probable selection of fit patients for operative procedures. Most operated nonagenarians presented with acute limb ischemia (n=24, 33.8%). Patients with urgent procedures had notably higher 30-day mortality that was of significance (15% vs 0%, p=0.032). In addition, follow-up mortality was significantly higher in the operated nonagenarians as compared with those who were treated conservatively (15.5% vs 0%; p=0.000). This highlights the importance of proper patient selection and thorough assessment for an individual-based treatment strategy and enhancing clinical outcomes. The median follow-up period was 19 days, but there were significant differences among patients with a maximum period recorded of 1785 days (>4 years). This indicates how challenging it is for nonagenarians to adhere to follow-up.
Nonagenarians are increasing and currently represent a significant category of the population. The need to provide optimal management is dependent not only on age but also on several other factors. Acceptable outcomes can be achieved. Nonagenarians perform well whether operated, conserved, and/or in ICU. Further studies are needed with a greater number of patients and regular follow-up with longer periods to address the outcomes of different vascular pathologies on such patients and what outcomes are expected.
Limitation of Study
This was a retrospective study that used analysis of previous medical records with all associated restrictions in data collection. Adherence to follow-up was very difficult for many nonagenarians. Although these patients tend to seek medical consultation when complications arise, this is unfortunately a subjective matter and cannot be used as the basis of follow-up. In addition, the study’s relatively small cohort size and the diversity of vascular pathologies contributed to a degree of heterogeneity that may limit the robustness of statistical analyses. While we identified trends within the data, these should be interpreted cautiously, and future studies with larger, more uniform populations with long-term follow-up will be essential to draw more definitive conclusions. Furthermore, additional studies are required to address the operative and nonoperative outcomes of different vascular pathologies, especially between genders.
Conclusion
The proportion of nonagenarians in the population is growing and so is their referral to vascular surgery. Satisfactory short-term treatment outcomes can be achieved in this highly selected cohort of patients. Thirty-day mortality is higher in patients undergoing urgent procedures. Follow-up mortality was higher in the operated nonagenarians as compared with those who were treated conservatively. Careful patient selection and thorough preparation are crucial to enhance clinical outcomes. Further research on therapy outcomes of nonagenarians will enable physicians to make better evidence-based approaches to individual patients and should be encouraged.
Footnotes
Abbreviations
AAA, abdominal aortic aneurysm; ALI, acute limb ischemia; AKI, acute kidney injury; BMI, body mass index; CAD, coronary artery disease; CHF, congestive heart failure; CKD, chronic kidney disease; COPD, chronic obstructive pulmonary disease; DM, diabetes mellitus; DR, department referrals; eGFR, estimated glomerular filtration rate; ESVS, European Society for Vascular Surgery; EVAR, endovascular aneurysm repair; ICA, internal carotid artery; LSA, left subclavian artery; MI, myocardial infarction; OSR, Open Surgical Repair; PAD, peripheral artery disease; PAU, penetrating aortic ulcer; RIFLE, Risk, Injury, and Failure; and Loss; and End-stage kidney disease; TAA, thoracic aortic aneurysm; TIA, Transient Ischemic Attack; TEVAR, thoracic endovascular aortic repair.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Was waived given the retrospective design of the study with anonymized retrospective data analysis.
