Abstract
Close interpersonal relationships represent both a key context for the genesis of complex trauma and a positive modifiable factor in recovery following trauma exposure. Furthermore, symptoms of individual trauma affect the family system and partners, supporting the need for systemic approaches in trauma recovery. This review sought to systematically identify and synthesise current approaches to involving the family or relational partners in trauma recovery, including an evaluation of their effectiveness on a range of individual and systemic outcomes. Eligible articles were published between January 2013 and October 2024, in English, and evaluated an intervention aimed at improving mental health or relational outcomes of trauma, where a family member or ally attended at least one session with the trauma-affected individual. Screening of an initial 3,169 articles identified a total of 41 eligible studies evaluating 32 different family-inclusive or relational approaches to trauma recovery. Data were narratively synthesised based on the characteristics of the study, population and intervention characteristics and the efficacy of each intervention on improving individual and systemic outcomes. Results suggest a generally positive impact of family-inclusion in trauma treatment paradigms, independent of intervention duration, theoretical underpinning, service setting or to the training or discipline of the provider. Practice recommendations are provided regarding different approaches based on the age and specific needs of the trauma-affected individual. Overall, the review supports family-inclusive and relational intervention frameworks that integrate well-established systemic practices in conceptualising the trauma experience as a shared experience and a shared recovery pathway.
Introduction
Family-inclusive and relational treatment approaches broaden the focus on individual outcomes to include the wider family, relational and caregiving system (Foster et al., 2016). Such approaches span a continuum, ranging from interventions in which a family member or relational partner participates in one or more sessions to support an individual’s treatment, to fully systemic family interventions in which the family system itself is the primary unit of change. Established evidence demonstrates that family-inclusive practices across this continuum play a key role in promoting mental health outcomes for all age groups with a mental illness and associated trauma (Foster et al., 2016; Poon et al., 2019). In this light, evidence-based frameworks, policies and practice guidelines are increasingly advocating for a greater uptake of both family member participation and systemic family interventions (hereafter referred to under the umbrella term of ‘family-inclusive and relational interventions’). This review seeks to add value through synthesising contemporary trauma recovery approaches that include a family member or relational partner to address the key question of whether family involvement contributes to better outcomes for those who have experienced trauma.
Trauma reflects a rupture or loss of connection to oneself, our family and world following exposure to events that exceed a human’s capacity to cope and make sense of the experience (van der Kolk, 2014). The spectrum of traumatising events spans singular exposure (e.g. serious accidents, isolated threats to safety, war-related combat, exposure to community violence) through to prolonged, relationship-based ‘complex’ trauma (e.g. violence or abuse within relationships of dependence). Posttraumatic stress disorder (PTSD; American Psychiatric Association, 2022) or complex PTSD are disorders directly linked to trauma exposure. Furthermore, untreated posttraumatic symptoms or impairments resulting from childhood trauma within the parent–child dyad are disproportionately associated with later complex presentations, such as affective, anxiety, dissociative, addictive disorders and borderline personality disorder (Ford & Courtois, 2021; Lewis et al., 2021). Beyond a diagnostic lens, the impacts of trauma are pervasive and systemic, affecting thought, capacity for self-efficacy and self-leadership and importantly, trust in others (Campbell & Renshaw, 2018).
Interpersonal relationships represent both a key context for the genesis of complex trauma and a positive modifiable factor in recovery following trauma exposure (Marshall & Kuijer, 2017). Under optimal circumstances, an individual’s relational bonds can provide the context within which healing can be achieved through caregiving, meaning-making and social support (Calhoun et al., 2022). Conversely, interpersonal trauma exposure (Logue et al., 2024), PTSD symptoms (Brown & Welc, 2025) and affective, anxiety and behavioural symptoms (Kamali et al., 2024) are associated with lower levels of perceived social support. Furthermore, post-traumatic growth theory suggests that supportive relationships can be strengthened following traumatic events through self-disclosure and discourse, the co-construction of new trauma narratives and their meaning in relation to others (Purol & Chopik, 2024). Trauma-affected children or young people also benefit from caregiver support during treatment (Clark & Nadeem, 2023).
The potential benefits of supportive relationships in trauma recovery are juxtaposed with well-established evidence demonstrating the secondary and systemic effects of individual trauma on the family system and relational partners (Russin & Stein, 2022). For example, PTSD is one of the mental health difficulties most strongly associated with relationship distress (Whisman et al., 2000). Systematic reviews and meta-analyses show a consistent and strong association between PTSD and a range of family problems, including mental health difficulties in partners and children (Lambert et al., 2014; Monson et al., 2022; Russin & Stein, 2022) and negative developmental outcomes for children of trauma-affected parents (Lambert et al., 2014; van Ee et al., 2016). Family members supporting trauma-affected individuals experience cumulative demands, including secondary/vicarious traumatisation, caregiver burden and ambiguous loss (i.e. the sense that they have ‘lost’ their loved one, despite their continued physical presence; Monson et al., 2022). Furthermore, evidence suggests that conflictual relationships (i.e. conflict in social networks), when combined with low levels of instrumental support, may be associated with harsh parenting practices among adults facing adversity (Marra et al., 2009). Multiple members in a family may be also affected by shared trauma, such as family violence or intergenerational or cultural trauma (O’Neill et al., 2018). This can be further compounded by trauma-symptomology (e.g. lowered perceptions of self-efficacy and less effective coping) leading to more frequent support-seeking behaviour and increased demands on supports, who may not always be well-equipped (Calhoun et al., 2022). Therefore, while supportive relationships can be protective, such protective influence is not unconditional and depends on the quality, stability and capacity of relational supports. Together, these processes can create a bidirectional impact of the trauma on family relationships.
While existing individualised, evidence-based treatments are highly efficacious for improving PTSD and common comorbid symptoms (Watkins et al., 2018), some fall short of improving couple and family functioning (Suomi et al., 2019) thereby lacking the moderating influence of couple/family functioning on individual trauma treatment (Meis et al., 2010). Furthermore, most intervention frameworks neglect the fact that relationships may be traumatised, and not just individuals. Thus, recognising the relational impact of trauma and the healing potential of positive relationships highlights the need for systemic approaches, as evidenced by successful family-inclusive practices in other mental health contexts (Foster et al., 2016; Poon et al., 2019). Work is continuing to bridge this gap by applying family therapy models to trauma-affected families (Dalton et al., 2013; Kerig & Alexander, 2012; Kiser et al., 2010), as well as integrating family intervention into individualised treatments (Thompson-Hollands et al., 2021). This could support those recovering from trauma and their families by modifying unhelpful relational patterns resulting from trauma-exposure and mobilising the family’s strengths and resources. Practice calls for evidence-based and systemic approaches to trauma recovery that consider both the needs of the trauma-affected individual and their relational partners (i.e. a family-inclusive and relational approach to trauma recovery).
Given these findings and the desire of many trauma-affected individuals to include their families and relational partners in treatment (Figley & Figley, 2009), it is timely to review the contemporary, published evidence on family-inclusive and relational interventions to trauma recovery. The present review aims to address this need by identifying current approaches to involving the family or relational partners in trauma recovery, including an evaluation of their effectiveness on a range of individual and systemic outcomes.
Methods
Review Methodology
This review followed a rapid systematic review methodology using a condensed process allowing a timely knowledge transfer to policy and practice, conducted in accordance with the Cochrane Rapid Review methodological guidelines (Garritty et al., 2020). The reporting of the methodology and results was guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA; Page et al., 2021).
Search Strategy
Four databases (Cochrane, Embase, Medline and PsycINFO) were systematically searched on October 24, 2023, with an additional search on 4th October 2024. Search results were restricted to peer reviewed articles published within the last 10 years (2013–2024) to ensure a contemporary review of the evidence. Search terms relating to trauma (e.g. trauma* OR ‘posttraumatic stress’ OR ‘post-traumatic stress’ OR ‘post traumatic stress’ OR PTSD), intervention or treatment (e.g. therap* and recover*) and relational (e.g. famil* and carer*) constructs were used with MeSH headings. Review articles were hand-searched to identify additional relevant studies for inclusion.
Study Eligibility
Study eligibility was established in accordance with the Population, Intervention, Comparator, Outcome and Study (PICOS) design framework (Bramer et al., 2018); Supplemental Table 1). Studies were included if they evaluated an intervention aiming to improve mental health or relational outcomes of trauma and involved the client and at least one family member or ally in at least one session. Studies focusing on intimate partner relationships were excluded, given these have been reviewed extensively elsewhere (Suomi et al., 2019). Similarly, dyadic parent–child trauma interventions were excluded unless they went beyond the dyad to include more than one caregiver or sibling/s. Only articles published in English and over the last 10 years were considered (i.e. published in 2013 or later).
Study Screening and Selection
The systematic search identified 4,388 records. All records were imported into Endnote (2013), and duplicates were removed resulting in 3,169 unique records. Covidence (Veritas Health Innovation, 2020) was used for all data screening and record management. Screening at title/abstract was done by two reviewers (ZC, AV) and 25% of records were double screened. A total 223 records remained at full-text level, screened by ZC and AV against inclusion criteria; again 25% of records were doubled screened. Full-text search resulted in 36 articles subjected to data extraction. Using the snowballing method, a further six studies were identified, of which five studies met inclusion criteria resulting in 41 articles included in this review. At both levels, disagreements were resolved through conferencing. See Figure 1 for a PRISMA diagram.
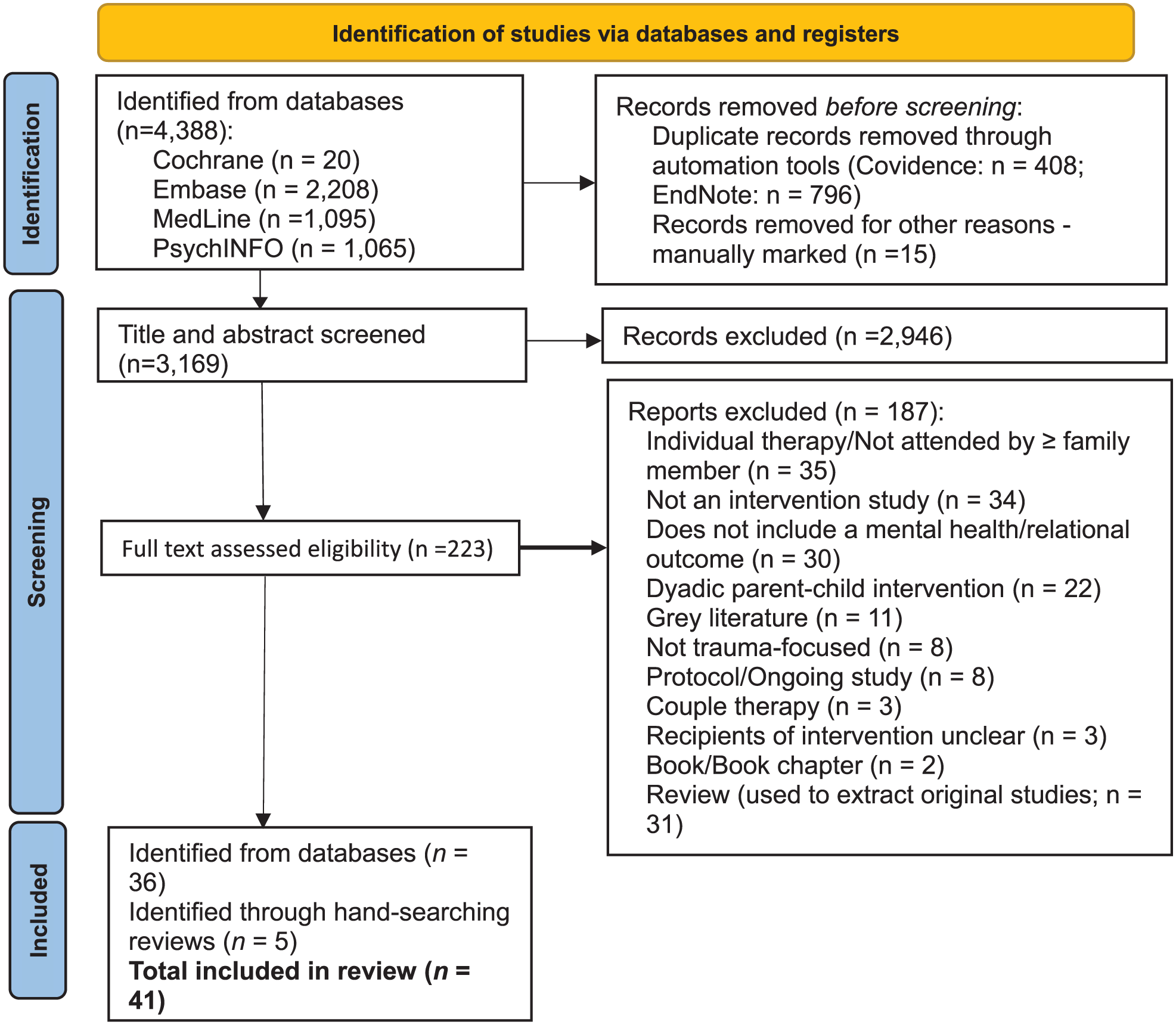
PRISMA chart of article identification process.
Data Extraction, Synthesis and Analysis
Data Extraction
Data were extracted by two reviewers (ZC, AV) using standard tables, with one charting data and the second verifying information. Disagreements were resolved through discussion. Interventions were grouped by age of the traumatised client, that is, children/youth and adults (see Table 1). Additional detail can be found in Supplemental Table 2.
Study Details, Quality of the Evidence and Outcomes of Family-Inclusive Approaches to Trauma Recovery.
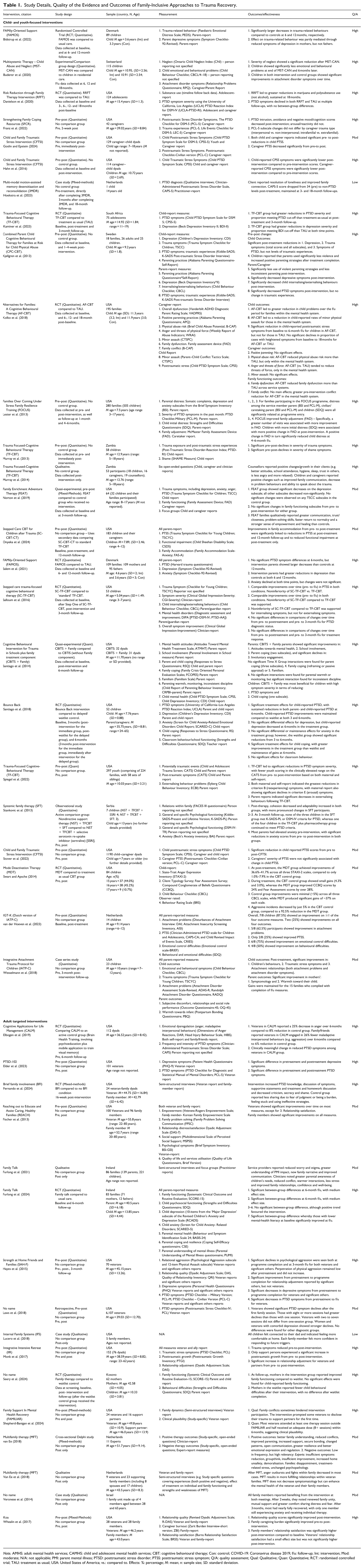
Note. AMHS: adult mental health services; CAMHS: child and adolescent mental health services; CBT: cognitive behavioural therapy; Con: control; COVID-19: Coronavirus disease 2019; f/u: follow-up; Int: intervention; Mod: moderate; N/A: not applicable; PMI: parent mental illness; PTSD: posttraumatic stress disorder; PTSS: posttraumatic stress symptom; Q/A: quality assessment; Qual: Qualitative; Quan: Quantitative; RCT: randomised controlled trial; TAU: treatment as usual; USA: United States of America; vs.: compared to. Effects: %: percentage; M: mean; n: sample size; SD: standard deviation.
Synthesis
Results were narratively synthesised (i.e. descriptive synthesis) following recommendations by Garritty et al. (2021) as data heterogeneity prohibited meta-analysis. Data was synthesised according to the study characteristics (i.e. country of origin, methodological diversity and longitudinal follow-up), quality assessment, population characteristics (i.e. sample size, target populations and trauma subtype), intervention characteristics (i.e. interventions targeting children/youth [under 18 years] or adults [18 years and above], number of sessions, delivery details and theoretical approach) and individual and systemic outcomes.
Risk of Bias Assessment
The Quality Assessment for Diverse Studies tool (QuADS; Harrison et al., 2021)) was used to appraise study quality and risk of bias. The QuADS assesses methodological quality for mixed- or multi-method studies and has demonstrated high validity and reliability allowing for comparison of heterogenous study designs. The QuADS scores 13 items on a 4-point rating scale (i.e. 0 = low, 1 =low-moderate, 2 =moderate-high and 3 =high). For overall study quality appraisal, the items were summed and converted to percentages out of a total score of 39, following cut-off points applied in an earlier scoping review (Orr et al., 2021): <60% (low-quality), 60% to 80% (moderate-quality) and >80% (high-quality).
Results
Summary of Search Results
After eliminating duplicates, the systematic search yielded a total of 3,169 records. Of these, 2,798 were excluded after reviewing their titles and abstracts (n = 2,946) and full texts (n = 187). Screening achieved an inter-rater reliability (IRR) of 94% with a Cohen’s Kappa statistic (κ) of 0.81 for titles and abstracts, and an IRR of 98% with a Cohen’s Kappa statistic (κ) of 0.94 for full-texts. A total of 41 published primary studies met all inclusion criteria and were narratively synthesised. Figure 1 (PRISMA) details the results at each level and reasons for exclusion.
Characteristics of Included Studies
Country of Origin
Most studies were conducted in the United States (n = 25) followed by the Netherlands (n = 4), Denmark, Zambia, Ireland (each n = 2), Israel, Kosovo, Serbia, South Africa, Sweden and Switzerland (each n = 1).
Methodological Diversity
Included studies covered a range of study designs, with the majority applying quantitative research methods (n = 30), followed by mixed-methods (n = 6) and qualitative studies (n = 5). Of the quantitative studies, 16 studies followed a single group pre–post study design, 10 employed a randomised controlled trial, 2 used an experimental (two-arm) study design and 2 followed a case series/case study design. One study utilised a quasi-experimental (two-arm) design, and one study used observational research methods. Methods of data collection used for qualitative studies included semi-structured interviews, focus groups and subjective questionnaires containing open-ended questions. One qualitative study employed a case study design. Of the mixed-methods studies, two were single arm, pre–post study designs, one was a cross-sectional Delphi study, one was a case study, one was a randomised controlled trial, while another was a quasi-experimental (two-arm) study design.
Sample Size
Sample descriptions were inconsistent, referring to individuals (children, adolescents, caregivers, veterans), families, dyads or broader groups (veterans with family members, ‘experts’). Nine studies specified child/youth numbers averaging 56.93 participants (SD = 35.50; range 1 to 124). Five adult-focused studies averaged 1,276 participants (SD = 2,415.58; range 42 to 6,107). Twenty studies reported dyads/families, ranging from 1 family to 1,190 dyads (M = 115.10; SD = 251.25).
Longitudinal Follow-Up
Pre–post-intervention assessments were most common (n = 20), with 14 studies including additional follow-up assessments. The follow-up periods varied from 1 month to 18 months. Seven studies included only one data collection point (i.e. post-intervention only).
Quality Assessment
Overall quality of included studies was high (60.98%, n = 25), followed by moderate (34.15%, n = 14) and low quality (4.88%, n = 2). Table 1 displays the quality assessment rating for each individual study (see also Supplemental Figure 1 for a visual representation of study quality).
Population Characteristics
Intervention details including target population characteristics, trauma subtype, theoretical approaches, session length and delivery details can be found in Supplemental Table 2 and are briefly summarised below.
Target Populations and Trauma Subtype
Most interventions targeted one of three groups: families exposed to a traumatic event/s (n = 13), those affected by child abuse/neglect (n = 9) and veteran families (n = 12). Others addressed paediatric cancer survivorship (Bidstrup et al., 2022; Salem et al., 2021), adolescent substance misuse as a coping mechanism for trauma-related symptoms (Danielson et al., 2020), attachment trauma (van der Hoeven et al., 2023; Wesselmann et al., 2018) and parent mental illness, including PTSD (Furlong et al., 2021, 2024).
Trama subtype was categorised as either ‘non-interpersonal’ (i.e. accidents, natural disasters, life-threatening illness) or ‘interpersonal’ (i.e. relational or prolonged abuse or extrafamilial interpersonal trauma including war-related combat). Among child/youth interventions, 61% (n = 11) addressed interpersonal trauma, eight supported both trauma subtypes and four targeted non-interpersonal trauma/s. One study was uncategorised. Twelve child/youth interventions addressed trauma arising from intrafamilial abuse, with 75% restricting family involvement to non-offending caregivers or adult family members (including one study whereby adolescents selected a caregiver or family member to participate; participation was presumed to involve non-offending caregivers (Swart & Apsche, 2014). Three child/youth interventions explicitly included offending caregivers, and these were limited to contexts of physical abuse or neglect (Buderer et al., 2020; Kjellgren et al., 2013; Kolko et al., 2018).
Conversely, 59% of adult-focused interventions targeted interpersonal extrafamilial trauma, mainly war-related (n = 10). Another addressed both interpersonal and non-interpersonal trauma types, and two involved PTSD without specifying trauma subtype (Furlong et al., 2021, 2024). No adult-focused interventions included offending family members.
Intervention Characteristics
Child/Youth or Adult Interventions
Interventions primarily supported families where a child or youth needed support (n = 24), with the average age of children or youth being 10.38 years (SD = 3.47; three studies did not provide enough data to calculate the average age of their sample). The remaining 17 studies reported on interventions focused on families where an adult required support, with an average age of 44.52 years (SD = 5.47; four studies did not provide enough data to calculate the average age of their sample). Table 1 (and Supplemental Table 2) orders the display of interventions based on the age of the trauma-affected family member.
Number of Sessions
Child and youth interventions ranged from 1 to 4 sessions to weekly sessions over 6 to 8 months (M = 12; Mdn = 10). Four studies reported sessions numbers as case-dependent, and one did not report them. Adult-focused interventions ranged from 3 to 10 sessions (M = 7; Mdn = 8). One study reported case-dependent sessions, and three did not specify numbers, describing delivery instead as a 4-day or 14-day intensive programme.
Delivery Details (Provider and Setting)
Interventions were delivered by mental health clinicians (n = 19), trained providers (n = 11), postgraduate student providers (n = 2), social workers (n = 3) or lay counsellors (n = 4). Four studies did not specify the provider. Most were delivered in-person at a health centre (n = 23), others used blended (e.g. in-person/online or clinic/home; n = = 5), in-home (n = 4), school (n = 2), outdoor (n = 1) or video-only teleconference (n = 2) formats. Delivery setting was unspecified in five studies.
Theoretical Approach
Detail on the intervention theoretical approaches are provided in Supplemental Table 2. Among child- and youth-focused interventions, two distinct models of family involvement were evident. Fifteen studies evaluated interventions designed as systemic family interventions, in which the family unit or the parent–child relationship constituted the unit of change. In contrast, nine studies evaluated interventions that involved family member participation, whereby a family member (e.g. non-offending caregiver) attended one or more sessions in support of the child’s treatment, typically to receive psychoeducation about trauma-symptoms.
Most child- and youth-focused interventions were grounded in cognitive behavioural therapy (CBT; n = 11), including seven evaluations of trauma-focused CBT. Three studies applied explicitly systemic or family-centred models, while others combined CBT with systemic principles, and mode deactivation therapy. Three other studies applied novel approaches (Hoekstra et al., 2023; Norton et al., 2019; Wesselmann et al., 2018).
Most adult-focused interventions were systemic in nature, with the couple or family relationship serving as the primary unit of change (n = 14). Conversely, three adult-focused interventions involved family-member participation limited to psychoeducation about trauma symptoms. Adult-focused interventions, particularly for veterans (n = 10), drew from psychoeducation, systemic models, multifamily therapy and behaviour or cognition-based models. One study used administrative data only (Laws et al., 2018). Among non-veteran families, five studies applied systemic, narrative or CBT-informed models.
Outcomes
Table 1 presents study outcomes, detailing the specific measures, informants and the effectiveness of each intervention in enhancing both individual and systemic outcomes. A summary of this data is also provided below.
Who Reported Outcomes?
Most studies used a multi-informant approach including a mixture of child/youth, caregiver and/or practitioner-completed measures (n = 21). Thirteen studies relied exclusively on adult-caregiver/parent-report, three studies used practitioner-reports and two studies child/youth reports only.
Effectiveness of Interventions for Individual Outcomes
PTSD symptoms were the most frequently reported individual outcome (n = 25), followed by general mental health or distress (n = 20) and emotional/behavioural problems (n = 9). Systemic outcomes were reported in 15 studies, including family functioning (n = 9), relationship quality (n = 6), parenting practices (n = 6), attachment symptoms (n = 4) and social support (n = 1). Further detail can be found in Table 1.
Child Trauma Symptoms
Eighteen studies assessed child PTSD symptoms with consistent pre- to post- intervention improvements across family-inclusive interventions. Five evaluated trauma-focused CBT (Kaminer et al., 2023; Murray et al., 2013, 2014; Spiegel et al., 2022), all reporting significant symptom reduction, with one study demonstrating sustained reductions at the 3-month follow-up assessment (Kaminer et al., 2023). A stepped-care version of trauma-focused CBT showed comparable effectiveness, with reductions maintained over time when measured at 3-month follow-up (Salloum et al., 2014). One study linked the reduction in child trauma symptomology to reductions in family accommodation (i.e. behaviours intended to relieve immediate distress but negatively reinforce and perpetuate symptomology over time), which were maintained at 12 months (Onyeka et al., 2024).
Some studies found similar improvements but lacked a control group design or longitudinal follow-up. Sustained benefits were found in six studies with follow-up periods ranging from 3 months (Danielson et al., 2020; Norton et al., 2019; Wesselmann et al., 2018) to 6 months (Lester et al., 2013; Santiago et al., 2014; Santiago et al., 2018). However, Danielson et al. (2020) found that short-term improvements at 3 months were not maintained at 18 months, with noninferiority over usual care (non-family-inclusive intervention). One case study reported diagnostic remission at 18 months (Hoekstra et al., 2023), while an RCT showed parent-reported ‘trauma-related behaviours’ improved significantly, sustained at 6- and 12-month follow-up (Bidstrup et al., 2022).
Child Internalising and Externalising Behaviours
Nine studies assessed the child’s internalising and/or externalising behaviours. All studies demonstrated significant improvements in internalising symptoms post-intervention. All but one (Salloum et al., 2016) also showed significant improvements in externalising symptoms. Five studies compared improvements in internalising and externalising symptoms with a control group. Furthermore, most studies included a longitudinal follow-up (n = 5), reporting sustained improvements in internalising and externalising symptoms, with follow-up assessments ranging from 1- to 4-week post-intervention (Kjellgren et al., 2013), 3 months (Salloum et al., 2016; Wesselmann et al., 2018) and 6 months (Buderer et al., 2020; Furlong et al., 2024).
Child Mental Health and Related Outcomes
Nine studies reported improvements in child mental health, including reductions in depression (Kaminer et al., 2023; Kjellgren et al., 2013; Santiago et al., 2018), anxiety and coping (Santiago et al., 2018), distress (Lester et al., 2013), anger and fear (Swart & Apsche, 2014), shame (Murray et al., 2013), psychological functioning (Stankovic et al., 2013) and trauma-related substance misuse (Danielson et al., 2020). Furlong et al. (2024) found no significant group differences in depression or anxiety compared to usual care, although a positive trend favoured the family-inclusive intervention. Four studies used active control groups. Five showed sustained improvements at follow-ups ranging from 1 week (Kjellgren et al., 2013) to 18 months (Danielson et al., 2020).
Adult PTSD Symptoms
All five studies evaluating adult PTSD symptoms focused on military/veteran families and reported significant improvements following family-inclusive interventions. However, only one included a control group (Elbogen et al., 2019), and just two assessed outcomes longitudinally – at 3 months (Hayes et al., 2015) and 6 months (Elbogen et al., 2019).
Adult Mental Health and Related Outcomes
Ten studies assessed adult mental health or related outcomes, predominantly depression (n = 4). Other outcomes included coping and resilience (Furlong et al., 2024), emotion dysregulation (Elbogen et al., 2019), mental health attitudes (Santiago et al., 2014), quality of life (Fischer et al., 2018) and caregiver burnout (Whealin et al., 2017).
Five studies focused on military/veteran families, though most studies lacked control groups and/or longitudinal follow-up. Elbogen et al. (2019) reported greater and sustained improvements in emotion regulation at 6 months compared to an active control. Hayes et al. (2015) found reductions in depressive symptoms for both veterans and their partners, maintained at 3 months.
Among parents, five studies reported improved mental health outcomes post-intervention, with follow-up ranging from 1 week (Kjellgren et al., 2013) to 12 months (Bidstrup et al., 2022). However, only two studies included a control group (Bidstrup et al., 2022; Santiago et al., 2014). Bidstrup et al. (2022) found reduced maternal depression partly mediated reductions in children’s trauma-related behaviours.
Efficacy of Interventions for Systemic Outcomes
Systemic outcomes included family functioning (n = 9), parenting practices and attachment (n = 9) and relationship satisfaction, quality and adjustment (n = 6). Other relationship outcomes included relational aggression (Hayes et al., 2015) and social support (Fischer et al., 2018).
Family Functioning
Nine studies focused on family functioning (Furlong et al., 2024; Norton et al., 2019; Seery et al., 2024), adjustment (Lester et al., 2013), coping (Santiago et al., 2014), relationships (Stankovic et al., 2013), problem solving and empowerment (Fischer et al., 2018) and dysfunction or conflict (Kolko et al., 2018). Improvements in family functioning were found in four studies (Fischer et al., 2018; Furlong et al., 2024; Lester et al., 2013; Seery et al., 2024), including control group comparison (Seery et al., 2024) or a 6-month follow-up (Furlong et al., 2024). Norton et al. (2019), however, found no significant change in family functioning at 3-month follow-up. Kolko et al. (2018) reported significant, sustained reductions in family dysfunction (but not conflict) at 6-, 12- and 18-month follow-ups. Stankovic et al. (2013) found improvements in family relationships in a controlled trial, while no significant improvements were found for family coping at 6-month follow-up (Santiago et al., 2014).
Parenting Practices and Attachment
Six studies assessed parenting outcomes, practices (Kjellgren et al., 2013; Kolko et al., 2018), warmth (Santiago et al., 2014; Wesselmann et al., 2018), monitoring and inconsistent discipline (Santiago et al., 2014), neglect (Buderer et al., 2020) and physical abuse or use of force (Kolko et al., 2018). Findings were mixed; one study showed improvements post-intervention (Kjellgren et al., 2013), while another found no differences to treatment-as-usual at 6-, 12- and 18-month follow-ups (Kolko et al., 2018). Parental warmth improved in one within-group study at 3-month follow-up (Wesselmann et al., 2018), but not at 6 months when compared to a control group (Santiago et al., 2014). Reductions in parental anger and threats of force were observed but not significant (Kolko et al., 2018). Neglect and physical abuse risk showed significant declines in two controlled studies, sustained over 18 months (Buderer et al., 2020; Kolko et al., 2018). Three studies examined attachment outcomes. Two reported within-group reductions in attachment problems either at post-intervention (van der Hoeven et al., 2023) or at 3-month follow-up (Wesselmann et al., 2018), while one found similar improvements across intervention and control groups at 18-month follow-up (Buderer et al., 2020).
General Relationship Outcomes
Four studies, all military/veteran families, measured various relationship outcomes including relationship satisfaction (Fischer et al., 2018; Whealin et al., 2017), quality (Hayes et al., 2015; Whealin et al., 2017), adjustment (Monk et al., 2017), relational aggression (Hayes et al., 2015) and perceived social support (Fischer et al., 2018). Three studies demonstrated within-group, pre- and post-intervention improvements of relationship adjustment (Monk et al., 2017), relational aggression (Hayes et al., 2015) and social support (Fischer et al., 2018). However, three studies found significant within-group pre- and post-intervention improvements to relationship quality and satisfaction as reported by the veteran’s relational partner or family member/s, but not by the veterans themselves (Fischer et al., 2018; Hayes et al., 2015; Whealin et al., 2017). Of note, none of the mentioned studies involved a control group comparison and only one included a longitudinal follow-up of up to 3 months (Hayes et al., 2015).
Discussion
This review identified current approaches to involving the family or relational partners in trauma recovery, narratively evaluating target populations, intervention designs and effects on individual and systemic outcomes. Findings support the positive influence of family inclusion in treating child and adult mental health for trauma-affected individuals. Of 41 studies, most involved children or youth (n = 24) or adult veterans (n = 12). Despite methodological heterogeneity, effectiveness did not appear linked to intervention duration, service setting or provider background, suggesting an independent positive impact of family inclusion in trauma treatment.
Child and Youth-Focused Interventions
There is consistent evidence of immediate improvement in child PTSD, trauma-related symptoms, internalising/externalising problems and general mental health; sustained in half of the studies. Theoretical approaches varied, but most used cognitive behavioural methods, particularly trauma-focused CBT (standard or stepped care; Kaminer et al., 2023; Murray et al., 2013, 2014; Salloum et al., 2016; Spiegel et al., 2022), often combined with systemic principles. Thus, findings support the integration of well-established individual therapeutic approaches with systemic principles for trauma-affected children and youth.
Despite most child- and youth-focused interventions being considered underpinned by systemic principles (i.e. interventions positioned the family system or parent–child relationship as the primary unit of change), only one in four child and youth-focused studies assessed systemic outcomes. Of these, the studies revealed mixed findings with half demonstrating either improvements (Kjellgren et al., 2013; Kolko et al., 2018; Lester et al., 2013; Stankovic et al., 2013) or no change (Buderer et al., 2020; Norton et al., 2019; Santiago et al., 2014). Given the systemic nature of family-inclusive interventions, future research needs to prioritise relational outcomes, such as family communication, connection and problem-solving.
Adult-Focused Interventions
Across diverse theoretical approaches, adult-focused family-inclusive interventions improved individual PTSD symptoms in all identified studies, adding to previous research on benefits of family-inclusive approaches for anxiety and depression (Vossler et al., 2024). Importantly, most adult interventions were systemic in nature, with the couple or family positioned as the primary unit of change rather than involving family members solely in support of an individual’s treatment. However, evidence for complex trauma recovery in adults is scarce, likely due to the predominance of research focused on dyadic intimate partner interventions (e.g. Liebman et al., 2020; Suomi et al., 2019), which were excluded from the present review. Furthermore, all systemic outcomes were in military/veteran families, yielding mixed findings. Some found relational improvements (Fischer et al., 2018; Hayes et al., 2015; Monk et al., 2017), while others found that benefits were limited to family members and not the veterans themselves (Fischer et al., 2018; Hayes et al., 2015; Whealin et al., 2017). Only four studies examined adult-focused systemic outcomes of family-inclusive interventions among non-veteran families (Franz et al., 2022; Furlong et al., 2024; Furlong et al., 2021; Veronese et al., 2014), highlighting a major evidence gap.
These findings suggest that current knowledge is limited to children or veterans affected by trauma and their families, largely neglecting the broader adult mental health space. Research addressing this space has predominately been focused on intimate partner relationships (Suomi et al., 2019). This is surprising, given the wealth of evidence on the successful inclusion of families and carers in adult treatment of other serious mental health concerns, including depression and schizophrenia (Foster et al., 2016).
Strengths, Limitations and Future Research Directions
Most studies received high quality ratings, providing confidence in the validity and reliability of findings for shaping clinical practice and policy decisions on family-inclusion in trauma recovery. Twelve studies included were RCTs, but heterogeneity in design across all studies limited cross-programme comparisons. Future research needs to favour randomised controlled designs including validated instruments to capture relevant outcomes. Furthermore, less than half of the studies included follow-up data (n = 18), limiting evidence on sustained effects. Retaining multiple family members in research is challenging; thus, research investment fostering long-term engagement of multiple family members is essential to evaluate the sustained effectiveness of family-inclusive and relational trauma interventions. Insights from participating family members are essential to ensure improvements are maintained.
Finally, most studies were from the United States or Europe (88%). While the remaining few studies still demonstrated effectiveness, for example, in Zambia (Murray et al., 2013, 2014) and Israel (Veronese et al., 2014), the concentration of participants from Westernised countries limits generalisability. For example, cultural differences in stigma or family structure and support suggest the need for culturally-adapted models (Gopalkrishnan, 2018; O'Mahony & Donnelly, 2007), especially in collectivist contexts where family-inclusive interventions may be particularly effective (Gopalkrishnan, 2018).
Implications for Practice
Trauma recovery can be effective when individuals are treated within their family context. Both child/youth interventions and adult interventions appear to be feasible for frontline services (i.e. eight sessions for children and six sessions for adults), and effectiveness across various settings (e.g. homes, community centres or schools) offers flexibility for implementation. Provider qualifications did not appear to significantly influence outcomes, suggesting that delivery can involve a range of practitioners trained in systemic approaches. Systemic training appears essential to support formulation of trauma within relational contexts and to guide safe and responsive family involvement. Alongside this, ongoing evaluation and adaptation based on family feedback may further support quality and acceptability of care.
At the same time, the current evidence base only supports the inclusion of offending caregivers within child/youth focused interventions addressing physical abuse or neglect, delivered within structured models designed to prioritise child safety. No comparable evidence was found to support inclusion of offending caregivers in cases of intrafamilial sexual abuse, nor in adult-focused interventions. In addition, available studies provide limited guidance for practice in contexts involving child welfare or juvenile justice system involvement, family separation or removal of offending or victimised family members. A more developed evidence base is needed to understand the effectiveness, boundaries and ethical application in contexts where safety considerations necessitate restricted or modified family involvement. Until more detailed and systematic research is available, family-inclusive approaches should not be assumed to be universally appropriate and must be guided by statutory requirements, safeguarding frameworks and ongoing risk assessment.
From a practice perspective, family-inclusive models may be considered where they align with clinical goals, client preferences and safety considerations, and where appropriate training, supervision and practice structures are in place to support family perspectives within treatment planning and delivery. Future investment should prioritise rigorous evaluation and implementation research to clarify under what conditions family-inclusive trauma approaches yield the most meaningful and sustained benefit, in order to inform future policy and funding decisions.
Conclusion
Trauma treatment is effective via intervention frameworks that integrate established individualised interventions with systemic practices conceptualising the trauma experience as a shared experience and a shared recovery pathway. Future investments in refining this evidence across developmental and socio-cultural contexts are needed, together with service system collaboration in implementation of family inclusive approaches to trauma care.
Summary of Critical Findings
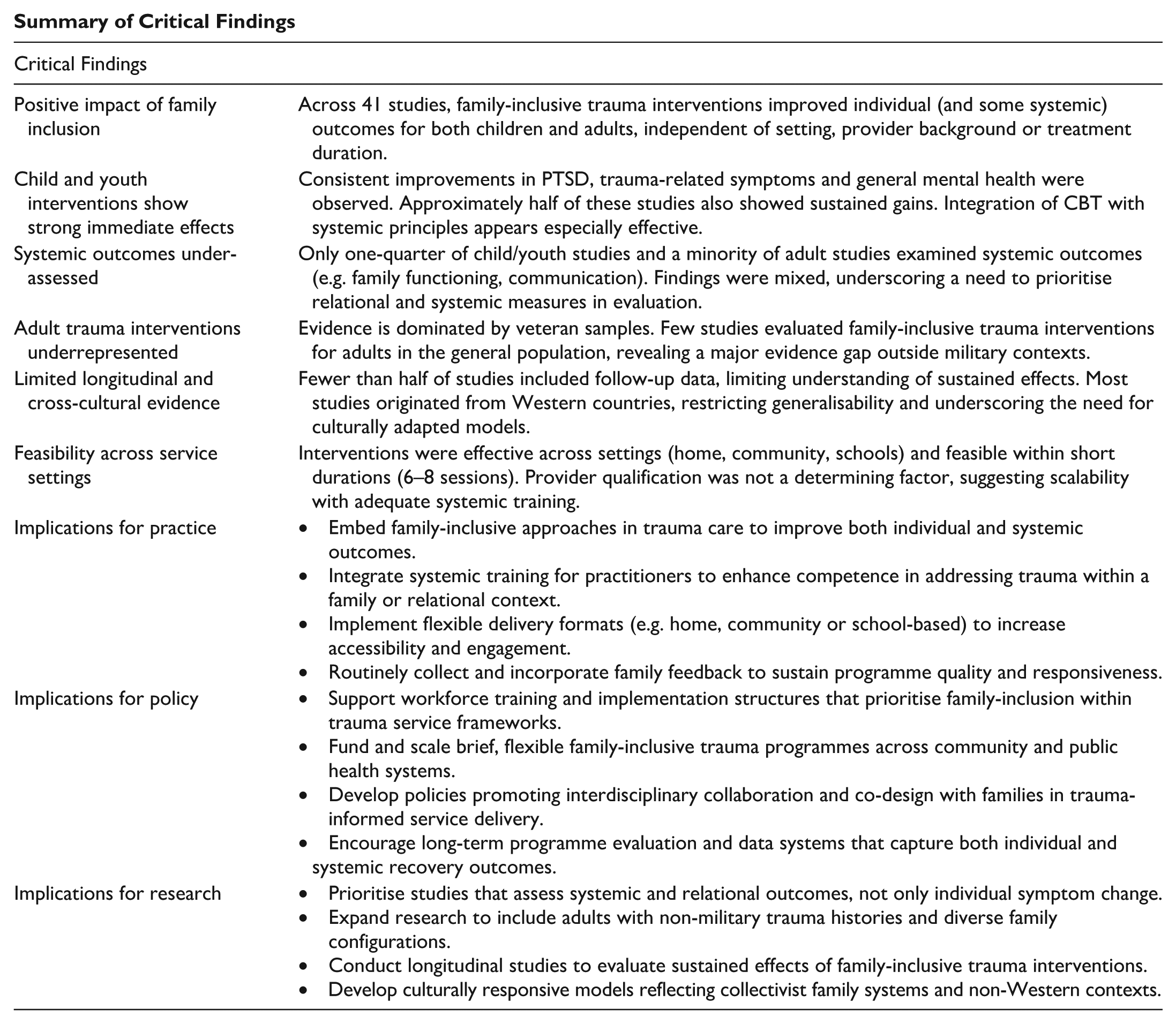
Supplemental Material
sj-docx-1-tva-10.1177_15248380261429511 – Supplemental material for Family-Inclusive and Relational Approaches to Trauma Recovery: Literature Review and Narrative Synthesis
Supplemental material, sj-docx-1-tva-10.1177_15248380261429511 for Family-Inclusive and Relational Approaches to Trauma Recovery: Literature Review and Narrative Synthesis by Zoe C. G. Cloud, An Vuong, Nicolas Barrington, Nella Charles, Jennifer McIntosh and Sandra Kuntsche in Trauma, Violence, & Abuse
Supplemental Material
sj-docx-2-tva-10.1177_15248380261429511 – Supplemental material for Family-Inclusive and Relational Approaches to Trauma Recovery: Literature Review and Narrative Synthesis
Supplemental material, sj-docx-2-tva-10.1177_15248380261429511 for Family-Inclusive and Relational Approaches to Trauma Recovery: Literature Review and Narrative Synthesis by Zoe C. G. Cloud, An Vuong, Nicolas Barrington, Nella Charles, Jennifer McIntosh and Sandra Kuntsche in Trauma, Violence, & Abuse
Supplemental Material
sj-docx-3-tva-10.1177_15248380261429511 – Supplemental material for Family-Inclusive and Relational Approaches to Trauma Recovery: Literature Review and Narrative Synthesis
Supplemental material, sj-docx-3-tva-10.1177_15248380261429511 for Family-Inclusive and Relational Approaches to Trauma Recovery: Literature Review and Narrative Synthesis by Zoe C. G. Cloud, An Vuong, Nicolas Barrington, Nella Charles, Jennifer McIntosh and Sandra Kuntsche in Trauma, Violence, & Abuse
Footnotes
Acknowledgements
The authorship team would like to thank the Department of Health, Victorian Government for their thoughtful contributions to the conceptualisation of this review.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by the Department of Health, Victorian Government, Australia.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
