Abstract
Military veterans in later adulthood are at increased risk for chronic posttraumatic stress disorder (PTSD), often characterized by cumulative trauma exposure, high levels of psychiatric and medical comorbidity, and prolonged symptom persistence. Although several evidence-based psychotherapies for PTSD are available, their effectiveness and clinical characteristics when implemented with older, non-active military veterans remain insufficiently synthesized. This integrative review aimed to examine psychotherapeutic interventions for PTSD in this population, focusing on intervention types, clinical outcomes, treatment acceptability, and strength of evidence. Following Preferred Reporting Items for Systematic Reviews and Meta-analysis Protocols guidelines, a comprehensive search was conducted in March 2024 across five electronic databases. Quantitative, qualitative, mixed-methods studies, and case studies published in English or Portuguese were eligible for inclusion. Of the 1,073 records identified, 23 studies met the inclusion criteria. Trauma-focused interventions were the most frequently studied, including prolonged exposure (PE), cognitive processing therapy (CPT), and exposure-based variants. Among studies with sufficient statistical reporting, trauma-focused therapies demonstrated the most consistent reductions in PTSD symptoms, with moderate to large effect sizes reported for PE, CPT, and multimodal motion-assisted memory desensitization and reconsolidation (3MDR). In contrast, relaxation-based and psychoeducational interventions were associated with smaller, inconsistent, or non-significant effects. Overall, findings support trauma-focused psychotherapies as the most robustly supported interventions for reducing PTSD symptoms in older, non-active military veterans. However, substantial heterogeneity in study design, outcome measurement, statistical reporting, and methodological quality limits comparability across studies and precludes quantitative synthesis, underscoring the need for more rigorous and standardized research to inform clinical decision-making in this aging veteran population.
Introduction
Many studies have revealed that during their military missions, veterans were frequently and severely exposed to a variety of war stressors, including seeing and moving corpses, witnessing or being the victim of grenades or mines, and witnessing or taking part in abusive violence against others. (Goldberg et al., 2016; Hyer et al., 1995; Maia & Morgado, 2019; Pless Kaiser et al., 2019). Such experiences are considered traumatic events and can contribute to the development of disorders such as PTSD (Cook et al., 2017; Goldberg et al., 2016; Hyer et al., 1995).
Defined as a mental health condition triggered by experiencing or witnessing traumatic events, PTSD manifests through a range of symptoms, including intrusive memories, avoidance, negative changes in mood and thinking, and heightened arousal (American Psychiatric Association, 2013). Among military veterans, the prevalence of PTSD varies across different conflicts and populations, with estimates ranging from 13.5% to 75% (Barros et al., 2022; Dursa et al., 2014; Goldberg et al., 2016; Shahmiri Barzoki et al., 2023). A meta-analysis of studies involving 4.945.897 veterans estimated the prevalence of PTSD at 23%. Additionally, a survey of Vietnam veterans found a lifetime prevalence of 16.9% for theater veterans aged at least 60 years (Goldberg et al., 2016). Furthermore, a survey of women Vietnam veterans reported a 20.1% prevalence of lifetime PTSD (Magruder et al., 2015).
A meta-analysis by Haagen et al. (2015) on the efficacy of recommended treatments for veterans with PTSD revealed that psychotherapeutic interventions, particularly Eye Movement desensitization and reprocessing (EMDR) therapy and cognitive processing therapy (CPT), showed significant positive effects in reducing PTSD symptoms. This study also highlighted that individual therapy formats delivered in outpatient settings were most commonly used and had favorable outcomes. Additionally, the analysis found that pretreatment PTSD symptom severity levels played a crucial role in predicting treatment gains, with an effect size of g = 1.12, indicating a substantial overall improvement in post-intervention symptoms (Haagen et al., 2015).
Despite the absence of global estimates regarding the size and characteristics of veteran populations, national-level data indicate that military veterans are disproportionately represented in older age groups. In the United States, nearly half of the veteran population is aged 65 years or older, with a substantial proportion having been exposed to major military conflicts such as the Vietnam War, the Gulf Wars, and earlier conflicts, including the Korean War and World War II (United States Census Bureau, 2023). Comparable demographic patterns have been documented in other countries, including Australia, New Zealand, and Canada, where a significant proportion of veterans also reside in later adulthood (Australian Bureau of Statistics, 2022; Barr & Young, 2024; Statistics Canada, 2022). This demographic reality has important clinical implications, as PTSD in military veterans often follows a chronic and evolving course across the lifespan. Empirical evidence suggests that older veterans with PTSD frequently present with cumulative trauma exposure, persistent symptomatology, and elevated psychiatric comorbidity, including depression, anxiety disorders, and substance use disorders (Baltjes et al., 2023; Moye et al., 2022). Rates of comorbidity are particularly high, with PTSD being associated with a three- to five-fold increased likelihood of major depressive disorder and substantial overlap with alcohol and substance misuse (Reisman, 2016). In addition, constructs such as moral injury have been proposed as relevant to understanding enduring psychological distress in veterans, potentially exacerbating PTSD symptom severity over time (Sadeh et al., 2017). Emerging research further indicates that aging-related life stressors, including retirement, loss of social roles, physical decline, and increased reflection on past experiences, may intensify trauma re-engagement and symptom expression in later life (Cook & Simiola, 2018; Kaiser et al., 2024). Together, this body of evidence underscores that PTSD in older military veterans is frequently characterized by chronicity, clinical complexity, and life-stage–specific challenges, warranting focused examination rather than assuming direct generalizability from younger or active-duty military samples.
The clinical profile associated with PTSD in older military veterans has important implications for treatment response and engagement. Evidence indicates that longstanding PTSD, particularly when accompanied by high levels of psychiatric comorbidity, is associated with greater symptom severity, functional impairment, and increased clinical complexity (Baltjes et al., 2023; Moye et al., 2022). Depression, substance use disorders, and anxiety frequently co-occur with PTSD in veteran populations and have been shown to compound symptom burden and complicate psychotherapeutic intervention (Reisman, 2016; Sadeh et al., 2017). In later adulthood, these challenges may be further intensified by age-related changes in physical health, cognitive functioning, and social context, which can influence treatment tolerance, adherence, and perceived relevance of therapy (Cook & Simiola, 2018). Emerging evidence suggests that aging-related processes, including trauma re-engagement in later life and shifts in identity and social roles, may shape how veterans experience and respond to psychotherapeutic interventions (Kaiser et al., 2024). Collectively, these factors suggest that treatment outcomes observed in younger or recently deployed military samples may not be directly transferable to older, non-active veterans with chronic PTSD, highlighting the need for careful synthesis of evidence that explicitly considers age, chronicity, and clinical complexity when evaluating intervention effectiveness.
That suggests that war conflicts dealt with by veterans extend into their daily lives long after the conflict has ended, as the enduring effects of PTSD can profoundly disrupt veterans’ social relationships, occupational functioning, and overall well-being, underscoring the urgent need for effective interventions and support mechanisms (Barros et al., 2022; Fulton et al., 2015; Maguen et al., 2020).
Given the pervasive impact of PTSD on the lives of military veterans, there is an extreme need for effective psychotherapeutic interventions (Haagen et al., 2015; Steenkamp et al., 2015). While conventional treatment modalities such as cognitive-behavioral therapy (CBT) and pharmacotherapy have demonstrated efficacy to varying extents, the veterans’ population requires different and more specific intervention approaches, due to the complex nature of PTSD and the characteristics of this population (Haagen et al., 2015; Shahmiri Barzoki et al., 2023).
When it comes to PTSD intervention, it is important to consider the existing guidelines based on scientific evidence (e.g., Courtois et al., 2017; Department of Veterans Affairs & Department of Defense [VA/DoD], 2023; National Institute for Health and Care Excellence [NICE], 2018; Phoenix Australia Centre for Posttraumatic Mental Health [Phoenix Australia], 2021), both for the general population and military veterans. Overall, CBT, CPT, EMDR, and Prolonged Exposure (PE) are strongly recommended for PTSD intervention (Courtois et al., 2017; NICE, 2018; Phoenix Australia, 2021; VA/DoD, 2023).
From a theoretical and clinical perspective, the psychotherapeutic interventions most used to treat PTSD target partially overlapping but distinct mechanisms of change. Trauma-focused exposure-based therapies, such as PE, primarily aim to reduce pathological fear responses through emotional processing and inhibitory learning by systematically confronting trauma-related memories and cues (Steenkamp et al., 2015). Cognitive-based interventions, including CPT, focus on modifying maladaptive trauma-related beliefs and appraisals through cognitive restructuring, thereby reducing negative alterations in cognition and mood (Haagen et al., 2015; Steenkamp et al., 2015). Other approaches, such as present-centered or non-trauma-focused interventions, emphasize coping with current life difficulties, problem-solving, and emotion regulation rather than direct trauma processing, and are generally associated with more modest symptom reductions (Steenkamp et al., 2015). In the context of older, non-active military veterans, age-related changes in physical health, cognitive flexibility, and tolerance for emotionally demanding interventions may further influence the acceptability and effectiveness of specific therapeutic mechanisms, underscoring the importance of examining how different approaches operate within this population.
Besides considering the different types of intervention, they must also be trauma-focused, because they are imperative to address the various manifestations of trauma and promote recovery of this population, given the multiple challenges they face (Goldberg et al., 2016; Haagen et al., 2015; VA/DoD, 2023). The meta-analysis by Haagen et al. (2015) is highly informative in this area; however, the literature shows more recent studies with potential relevance. Thus, it is essential to update current knowledge by mapping existing interventions, even if they do not present data on efficacy. By establishing the connection between research and clinical practice, this study aims to promote the quality of care and support provided to military veterans dealing with the enduring effects of trauma.
Objectives
The primary objective of this integrative review was to synthesize the existing evidence on psychotherapeutic interventions for posttraumatic stress disorder (PTSD) in older, non-active military veterans, with a particular focus on intervention effectiveness and clinical outcomes. Specifically, this review aimed at addressing the following overarching research question: Which psychotherapeutic interventions demonstrate the most consistent and clinically meaningful reductions in PTSD symptoms among older, non-active military veterans?
Secondary objectives were: (a) to map and categorize the types of psychotherapeutic interventions implemented with this population; (b) to describe key intervention characteristics, including treatment format, duration, outcome measures, follow-up assessments, and reported dropout rates; and (c) to critically appraise the strength and consistency of the available evidence, taking into account study design, methodological quality, and heterogeneity in outcome measurement.
This review explicitly distinguishes between the frequency with which interventions are studied and the strength of evidence supporting their effectiveness, providing a clinically meaningful synthesis to inform both research and practice among aging veteran populations.
Method
Protocol and Registration
We formulated our protocol according to the guidelines outlined in the Preferred Reporting Items for Systematic Reviews and Meta-analysis Protocols (PRISMA; Page et al., 2021). Our protocol was registered in the OSF.io platform (https://doi.org/10.17605/OSF.IO/TZSCM).
Eligibility Criteria
For this review, older, non-active military veterans were defined as individuals who had previously served in the armed forces and were no longer in active-duty service at the time of intervention, typically in later adulthood. This population includes veterans exposed to combat or other military-related traumatic events across different conflict eras.
The inclusion criteria were: (a) articles regarding one or more PTSD-focused intervention(s) with a sample of military veterans that used, at least, one validated, single-item, or multiple dimensions’ measures of PTSD; (b) papers in English and Portuguese; (c) quantitative, qualitative, mixed-method, and only-case studies; (d) no restrictions on minimum sample size or publication year. All types of PTSD-focused psychological interventions were included. No minimum limits were set for the sample size or year of publication.
Exclusion criteria were: (a) non-psychological interventions such as physical exercise or music therapy; (b) studies with a sample of military veterans mixed with active-duty military that did not report the differences in the results; (c) systematic reviews, scoping reviews, literature reviews, opinion pieces, and chapters of books.
Information Sources and Search Strategy
In March 2024, relevant studies were identified by three reviewers (T.G., B.S., and C.S.) through five electronic databases: Web of Science Core Collection, PubMed, PsycARTICLES, SciELO, and Scopus. The search terms were equal to all databases with the following search equation ((“veteran*” OR “soldier*” OR “militar*” OR “arm*” OR “marine*” OR “nav*” OR “air force*” OR “armed force*” OR “coast guard*” OR “seal*”) AND (“aging” OR “aged” OR “elderly” OR “older adult*” OR “senior*” OR “older person” OR “older people” OR “retired” OR “retirement” OR “not active” OR “reserve”) AND (“PTSD” OR “post-traumatic stress disorder*” OR “posttraumatic stress” OR “post-traumatic stress” OR “post traumatic stress” OR “post-traumatic” OR “posttraumatic” OR “post traumatic” OR “complex trauma” OR “CPTSD”) AND ("intervention*" OR "treatment*" OR “psych* treatment*” OR “psych* therap*” OR "therap*" OR “counseling”)). In addition to database searches, a bibliographic review of the identified papers and discussions with subject-matter experts were conducted, resulting in the discovery of two additional papers. The search strategy was restricted to “title and abstract” only. Five reviewers, A.M., T.G., B.S., C.S., and M.G., collaborated to develop the search equation, discussing and refining it as needed to address our research question better.
The inclusion of age- and retirement-related terms in the search strategy was intentional and aligned with the review’s primary aim to focus on older, non-active military veterans. This decision was grounded in evidence indicating that PTSD in later adulthood often presents with greater chronicity, higher comorbidity, and distinct clinical challenges when compared to younger or recently deployed populations. Restricting the search to this population was therefore considered methodologically appropriate to enhance clinical relevance and to avoid overgeneralization from studies conducted predominantly with younger or active-duty military samples.
Study Selection
We initially identified 1,073 records through electronic database searching. After removing duplicates (n = 589), 484 records remained for title and abstract screening. Following this screening stage, 444 records were excluded due to a lack of relevance. A total of 40 full-text articles were then assessed for eligibility. Of these, 21 studies met the inclusion criteria, while 19 were excluded for the following reasons: (a) wrong publication type (n = 5); (b) wrong outcome (n = 4); (c) lack of PTSD assessment (n = 3); (d) not psychotherapeutic interventions (n = 3); (e) full text not available (n = 2); (f) wrong population (n = 1); and (g) mixed active-duty and veteran samples without separate analyses (n = 1). References for the 21 eligible studies were manually analyzed, resulting in no additional studies. A total of two studies were identified through handsearch. In total, 1075 studies were identified in this review, of which 23 were considered eligible (Figure 1).
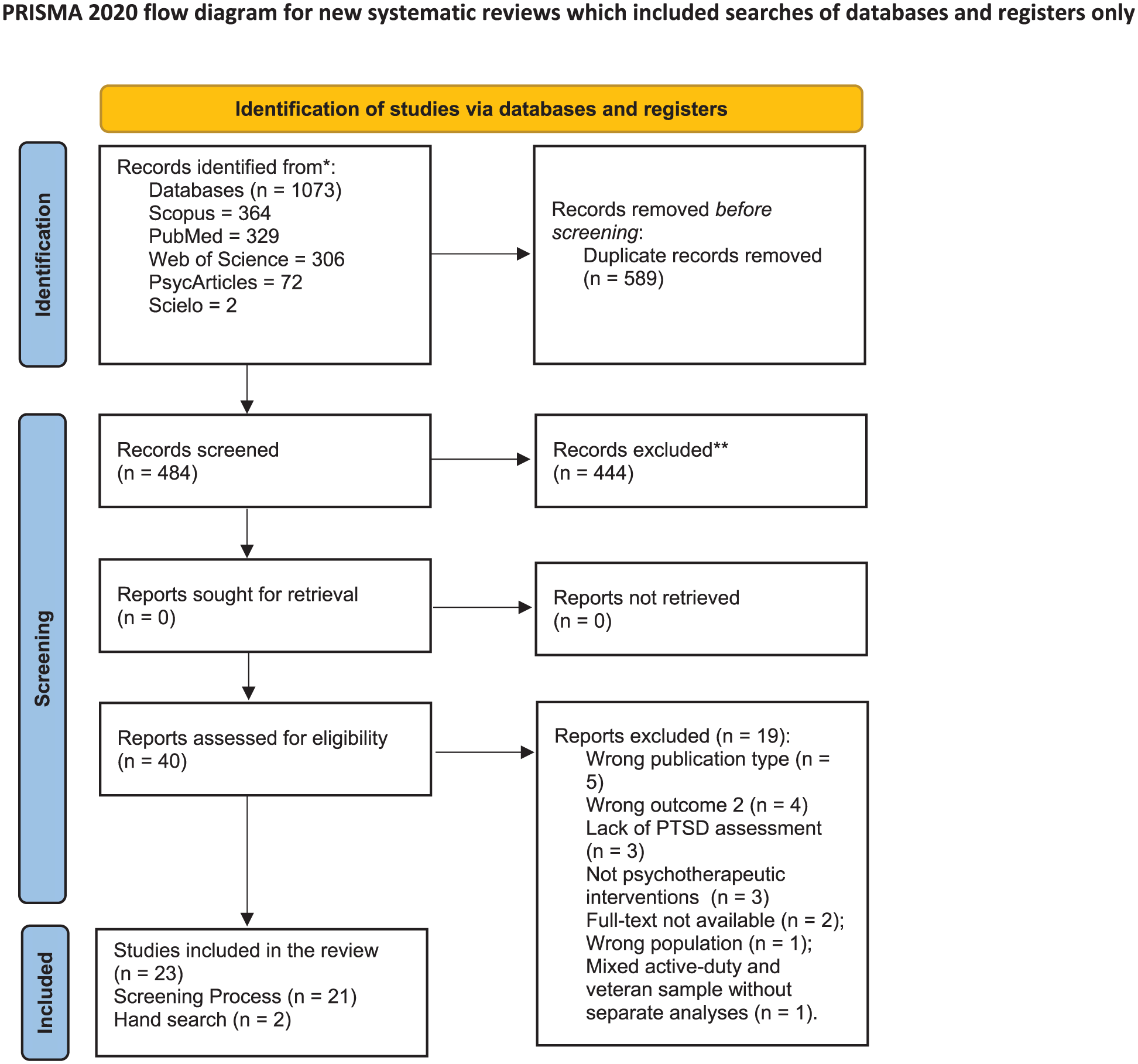
Flow diagram of the article selection.
Selection of Sources of Evidence
All records identified through database searching and handsearching were imported into Rayyan, a web-based systematic review management tool, for screening and deduplication. Duplicate records were removed prior to the screening process. Titles and abstracts were independently screened by two reviewers (T.G. and C.S.) to identify potentially eligible studies. Full-text articles of all records deemed potentially relevant were subsequently retrieved and independently assessed for eligibility by two reviewers (T.G. and B.S.), according to the predefined inclusion and exclusion criteria.
Any discrepancies or uncertainties regarding study eligibility were resolved through discussion and consensus between the reviewers. When necessary, the original full-text articles were re-examined to clarify methodological details. No automation tools were used for eligibility decisions beyond record management and screening support.
Data Extraction
Data extraction was conducted independently by two reviewers (T.G. and B.S.) using a standardized Excel-based data extraction form developed a priori. The form was piloted on a subset of included studies and refined as necessary to ensure consistency and completeness.
For each included study, the following information was extracted: author(s) and year of publication; study design; country; sample characteristics (including sample size and age range when reported); type of psychotherapeutic intervention; PTSD assessment instruments; presence or absence of a comparison group; outcome assessment points (pre-intervention, post-intervention, and follow-up); reported effectiveness outcomes; and dropout rates when available. Information regarding intervention structure (e.g., number and duration of sessions) was also extracted. The extracted data were cross-checked between reviewers, and any disagreements were resolved through consensus (Table 1).
List and Description of the Included Studies’ Characteristics.
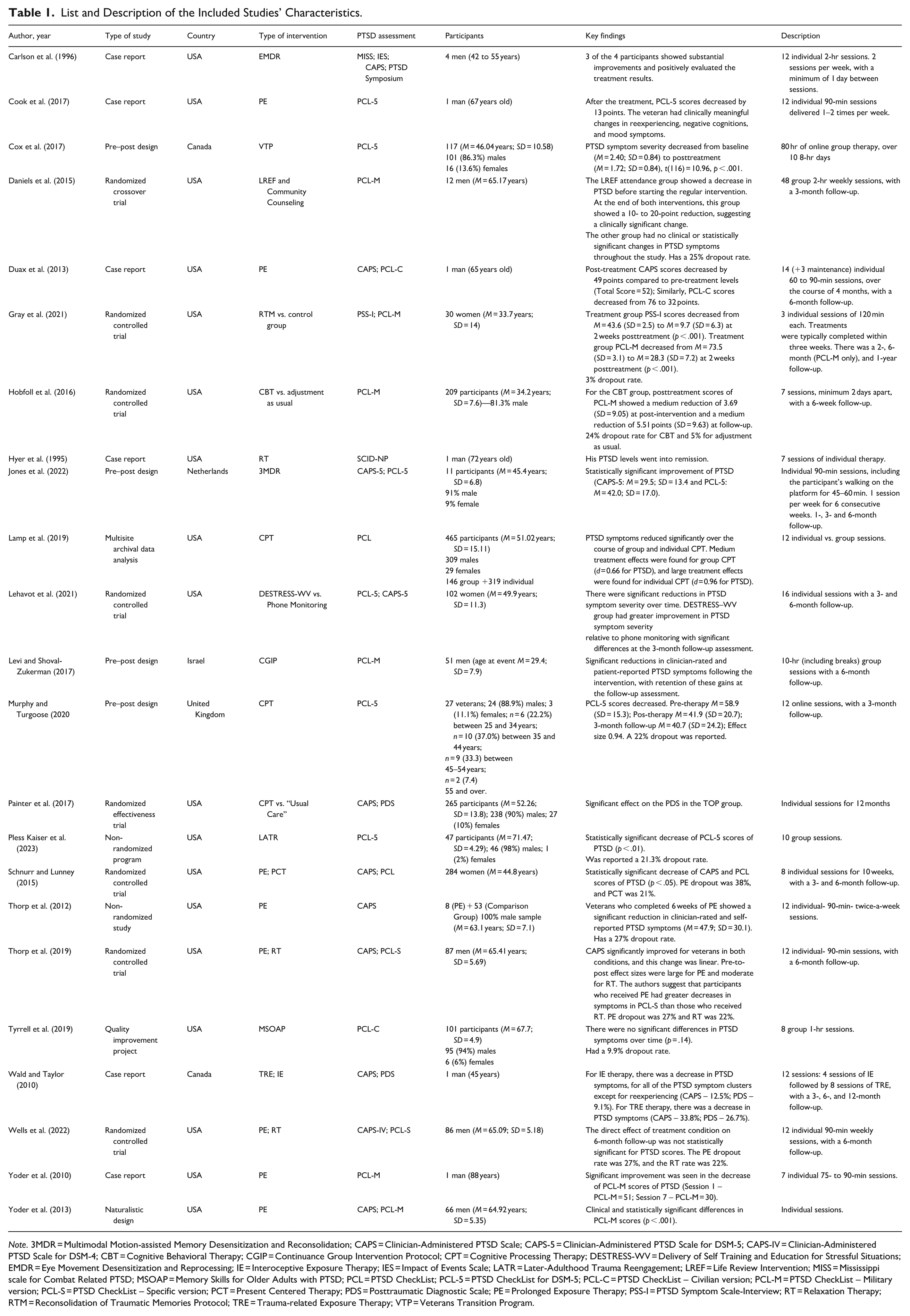
Note. 3MDR = Multimodal Motion-assisted Memory Desensitization and Reconsolidation; CAPS = Clinician-Administered PTSD Scale; CAPS-5 = Clinician-Administered PTSD Scale for DSM-5; CAPS-IV = Clinician-Administered PTSD Scale for DSM-4; CBT = Cognitive Behavioral Therapy; CGIP = Continuance Group Intervention Protocol; CPT = Cognitive Processing Therapy; DESTRESS-WV = Delivery of Self Training and Education for Stressful Situations; EMDR = Eye Movement Desensitization and Reprocessing; IE = Interoceptive Exposure Therapy; IES = Impact of Events Scale; LATR = Later-Adulthood Trauma Reengagement; LREF = Life Review Intervention; MISS = Mississippi scale for Combat Related PTSD; MSOAP = Memory Skills for Older Adults with PTSD; PCL = PTSD CheckList; PCL-5 = PTSD CheckList for DSM-5; PCL-C = PTSD CheckList – Civilian version; PCL-M = PTSD CheckList – Military version; PCL-S = PTSD CheckList – Specific version; PCT = Present Centered Therapy; PDS = Posttraumatic Diagnostic Scale; PE = Prolonged Exposure Therapy; PSS-I = PTSD Symptom Scale-Interview; RT = Relaxation Therapy; RTM = Reconsolidation of Traumatic Memories Protocol; TRE = Trauma-related Exposure Therapy; VTP = Veterans Transition Program.
Risk of Bias Selection
Risk of bias was assessed independently by two reviewers with expertise in trauma research and evidence synthesis (M.G. and T.G.). Randomized controlled trials (RCTs) were evaluated using the Cochrane Risk of Bias Tool 2 (RoB 2; Sterne et al., 2019), which assesses bias across five domains: (a) bias arising from the randomization process, (b) bias due to deviations from intended interventions, (c) bias due to missing outcome data, (d) bias in measurement of the outcome, and (e) bias in selection of the reported result. Overall risk of bias judgments followed the RoB 2 algorithmic guidance.
Non-randomized controlled studies and pre–post uncontrolled studies were assessed using the Risk of Bias Assessment Tool for Nonrandomized Studies (RoBANS; Kim et al., 2013), covering six domains: (a) selection of participants, (b) confounding variables, (c) measurement of exposure or intervention, (d) blinding of outcome assessment, (e) incomplete outcome data, and (f) selective outcome reporting. Overall judgments were derived in accordance with RoBANS guidance.
Each study was rated independently across all relevant domains of the respective tools. Discrepancies between reviewers were resolved through discussion and consensus, with consultation of the original study reports when necessary to clarify methodological details. Inter-rater agreement was high for both tools, with a Cohen’s kappa of .88 for RoB 2 assessments and .86 for RoBANS assessments, indicating excellent agreement. Risk of bias judgments were used to contextualize the interpretation of findings rather than to exclude studies from the synthesis.
Data Synthesis
Given the substantial heterogeneity in study designs, outcome measures, and reporting practices, a quantitative meta-analysis was not conducted. Instead, findings were synthesized using a narrative approach, supported by structured tables. Studies were grouped into discrete, non-overlapping categories based on the theoretical orientation of the psychotherapeutic intervention.
Within each category, results were summarized descriptively, with attention to consistency of findings, study design, sample size, statistical reporting, and treatment acceptability indicators such as dropout rates. Risk of bias assessments were used to contextualize the interpretation of findings rather than as criteria for study exclusion. The synthesis is presented in both narrative and tabular formats in the Results section.
Results
Studies Characteristics
This review included 23 studies involving a total of 2,030 individuals, with sample sizes ranging from 1 to 465 participants. Most studies (n = 20; 87%) were conducted in the United States (Carlson et al., 1996; Cook et al., 2017; Cox et al., 2017; Daniels et al., 2015; Duax et al., 2013; Gray et al., 2021; Hobfoll et al., 2016; Hyer et al., 1995; Lamp et al., 2019; Lehavot et al., 2021; Painter et al., 2017; Pless Kaiser et al., 2023; Schnurr & Lunney, 2015; Thorp et al., 2012, 2019; Tyrrell et al., 2019; Wald & Taylor, 2010; Wells et al., 2022; Yoder et al., 2010, 2013), two studies (8.7%) were conducted in Europe (Jones et al., 2022; Murphy & Turgoose, 2020), and one study (4.3%) in Asia (Levi & Shoval-Zukerman, 2017).
Of the 23 studies, 15 (65.2%) reported the mean age of participants, with an overall average of 51.3 years (SD ± 10.52). Regarding gender, 12 studies (52.2%) were conducted exclusively with male participants (Carlson et al., 1996; Cook et al., 2017; Daniels et al., 2015; Duax et al., 2013; Hyer et al., 1995; Levi & Shoval-Zukerman, 2017; Thorp et al., 2012, 2019; Wald & Taylor, 2010; Wells et al., 2022; Yoder et al., 2010, 2013), eight studies (34.8%) included both men and women (Cox et al., 2017; Hobfoll et al., 2016; Jones et al., 2022; Lamp et al., 2019; Murphy & Turgoose,2020; Painter et al., 2017; Pless Kaiser et al., 2023; Tyrrell et al., 2019), and three studies (13%) were conducted exclusively with women (Gray et al., 2021; Lehavot et al., 2021; Schnurr & Lunney, 2015).
Regarding study design, six studies (26.1%) were classified as RCTs (Gray et al., 2021; Hobfoll et al., 2016; Lehavot et al., 2021; Schnurr & Lunney, 2015; Thorp et al., 2019; Wells et al., 2022). Two studies (8.7%) used non-randomized controlled designs with a comparison group but without random allocation (Pless Kaiser et al., 2023; Thorp et al., 2012). The remaining 15 studies (65.2%) employed pre–post uncontrolled designs, including case-based studies, naturalistic designs, quality improvement projects, archival analyses, and other non-comparative approaches (Carlson et al., 1996; Cook et al., 2017; Daniels et al., 2015; Duax et al., 2013; Hyer et al., 1995; Lamp et al., 2019; Murphy & Turgoose, 2020; Painter et al., 2017; Tyrrell et al., 2019; Wald & Taylor, 2010; Yoder et al., 2010, 2013; Cox et al., 2017; Jones et al., 2022; Levi & Shoval-Zukerman, 2017).
With regard to intervention format, most studies (n = 17; 73.9%) implemented individual interventions (Carlson et al., 1996; Cook et al., 2017; Duax et al., 2013; Gray et al., 2021; Hobfoll et al., 2016; Hyer et al., 1995; Jones et al., 2022; Lehavot et al., 2021; Murphy & Turgoose, 2020; Painter et al., 2017; Schnurr & Lunney, 2015; Thorp et al., 2012, 2019; Wald & Taylor, 2010; Wells et al., 2022; Yoder et al., 2010, 2013), five studies (21.7%) used group interventions (Cox et al., 2017; Daniels et al., 2015; Pless Kaiser et al., 2023; Levi & Shoval-Zukerman, 2017; Tyrrell et al., 2019), and one study (4.3%) included and compared both individual and group formats (Lamp et al., 2019). All studies reported the number of intervention sessions.
Characteristics of Sources of Evidence
The 23 included studies were grouped according to the type of intervention provided: exposure therapies, relaxation therapies, cognitive reprocessing therapies, cognitive-behavioral therapies, trauma reengagement therapies, present-centered therapies, continuation group interventions, reconsolidation of traumatic memories (RTM), psychoeducation, and the Veterans Transition Program (VTP). Full details on authors, year of publication, study design, country, and setting, intervention type, PTSD assessment tools, participants, and key findings are summarized in Table 1.
Exposure Therapies
Nine studies evaluated 10 exposure-based interventions, including 8 on PE (Cook et al., 2017; Duax et al., 2013; Schnurr & Lunney, 2015; Thorp et al., 2012, 2019; Wells et al., 2022; Yoder et al., 2010, 2013), 1 on trauma-related exposure therapy (TRE; Wald & Taylor, 2010), and 1 on interoceptive exposure (IE; Wald & Taylor, 2010). All interventions were conducted in the United States and primarily delivered to male veterans (n = 8), with one study exclusively targeting women (Schnurr & Lunney, 2015).
Six of these studies used multiple instruments to assess PTSD symptoms (Duax et al., 2013; Schnurr & Lunney, 2015; Thorp et al., 2019; Wald & Taylor, 2010; Wells et al., 2022; Yoder et al., 2013). The tools applied included the CAPS (n = 6), PCL-S (n = 2), PCL-M (n = 2), CAPS-IV (n = 1), PCL (n = 1), PCL-C (n = 1), PCL-5 (n = 1), and PDS (n = 1) (Cook et al., 2017; Duax et al., 2013; Schnurr & Lunney, 2015; Thorp et al., 2012, 2019; Wald & Taylor, 2010; Wells et al., 2022; Yoder et al., 2010, 2013). All studies reported reduced PTSD symptoms from pre- to post-test, with five statistically significant improvements reported (Cook et al., 2017; Schnurr & Lunney, 2015; Thorp et al., 2012; Yoder et al., 2010, 2013). Wald and Taylor (2010) observed that IE reduced all PTSD symptom clusters except reexperiencing and that TRE further reduced symptoms across all clusters.
The number of PE sessions typically ranged from 7 to 15, with session durations between 60 and 90 min, and most often delivered once or twice a week. Maintenance sessions and follow-up assessments were also included (e.g., Duax et al., 2013; Schnurr & Lunney, 2015). For TRE and IE, Wald and Taylor (2010) implemented 12 sessions, including four IE sessions followed by eight TRE sessions, each lasting approximately 60 min. These interventions were generally moderate to high intensity and required consistent participant engagement over multiple weeks. Four studies reported dropout rates ranging from 20% to 38% (Schnurr & Lunney, 2015; Thorp et al., 2012, 2019; Wells et al., 2022), indicating potential challenges in retention for exposure-based interventions.
Relaxation Therapies
Three studies addressed relaxation interventions. Two studies (Thorp et al., 2019; Wells et al., 2022) compared the results of PE and Relaxation Therapy (RT), while another focused solely on RT (Hyer et al., 1995). These interventions were all US-based and were delivered to men with PTSD.
One of the studies used PCL-S and CAPS-IV to assess PTSD symptomatology (Wells et al., 2022), another study used CAPS and PCL-S (Thorp et al., 2019), and the other study used SCID-NP to assess PTSD scores (Hyer et al., 1995). Regarding pre-and post-test differences in PTSD scores, one study revealed significant differences (Hyer et al., 1995), another did not mention them (Thorp et al., 2019), and another reported that there were no significant differences (Wells et al., 2022). Two of the three studies that compared PE and RT results had a dropout rate of over 20% (Thorp et al., 2019; Wells et al., 2022). The other study did not mention a dropout rate (Hyer et al., 1995).
In terms of structure, the number of RT sessions varied across studies. Hyer et al. (1995) conducted seven individual sessions, although the duration of each session was not specified. In the trials by Thorp et al. (2019) and Wells et al. (2022), RT was delivered over 12 individual sessions, each lasting approximately 90 min. Sessions were typically conducted once a week over approximately 12 weeks. Despite this relatively intensive format, RT interventions were generally associated with smaller effect sizes but lower dropout rates when compared to PE, raising questions about their acceptability and clinical utility in this population.
Cognitive Reprocessing Therapies
Five studies addressed cognitive reprocessing interventions, including one study on EMDR, one on multimodal motion-assisted memory desensitization and reconsolidation (3MDR), and three on CPT (Carlson et al., 1996; Jones et al., 2022; Lamp et al., 2019; Murphy & Turgoose, 2020; Painter et al., 2017). Three studies were conducted in the United States (Carlson et al., 1996; Lamp et al., 2019; Painter et al., 2017), one in the Netherlands (Jones et al., 2022), and one in the United Kingdom (Murphy & Turgoose, 2020).
Four of the studies were delivered to both men and women (Jones et al., 2022; Lamp et al., 2019; Murphy & Turgoose, 2020; Painter et al., 2017), and one of them was exclusively delivered to men with PTSD (Carlson et al., 1996). In these studies, the instruments used to assess PTSD symptomatology were the PTSD Symptom Scale, MISS, IES, CAPS, PCL PCL-5 PCL-5, CAPS-5; and CAPS, PDS (Carlson et al., 1996; Lamp et al., 2019; Cox et al., 2017; Jones et al., 2022; Painter et al., 2017, respectively). All the studies reported clinically significant differences between the pre- and post-tests, with two studies (Jones et al., 2022; Lamp et al., 2019) also reporting statistically significant differences. Only one of the studies mentioned a dropout rate (22%; Murphy & Turgoose, 2020).
CPT was typically delivered over 12 sessions, each lasting between 50 and 60 min, and administered in either individual or group formats. Lamp et al. (2019) compared both modalities and found medium effect sizes for group CPT (d = 0.66) and large effect sizes for individual CPT (d = 0.96). In Murphy and Turgoose (2020), the 12 CPT sessions were conducted online and followed by a 3-month post-treatment assessment. The EMDR intervention (Carlson et al., 1996) was implemented through 12 individual sessions, each lasting 120 min, delivered twice weekly. The 3MDR protocol (Jones et al., 2022) involved six 90-min weekly sessions, combining virtual reality exposure with physical movement. This intervention reported significant reductions in PTSD symptoms, which were sustained at 1-, 3-, and 6-month follow-ups.
Cognitive Behavioral Therapies
Three studies (n = 1 Vets Prevail; n = 1 Life Review Intervention (LREF); n = 1 Delivery of self-training and education for stressful situations (DESTRESS-WV) addressed different cognitive-behavioral-based therapies (Daniels et al., 2015; Hobfoll et al., 2016; Lehavot et al., 2021). These interventions were all US-based, one was delivered exclusively to men (Daniels et al., 2015), one exclusively to women (Lehavot et al., 2021), and one to men and women (Hobfoll et al., 2016).
Two studies used PCL-M to assess PTSD symptomatology (Daniels et al., 2015; Hobfoll et al., 2016), while the remaining study used CAPS-5 and PCL-5 (Lehavot et al., 2021). All of the studies reported a decrease in PTSD symptomatology, but none reported whether this was statistically significant. Regarding the dropout rates, two of the three studies mentioned a dropout rate of 24% (Hobfoll et al., 2016) and 25% (Daniels et al., 2015).
The LREF was delivered over 48 weekly group sessions, each lasting 120 min, representing a long-term, high-intensity intervention. The DESTRESS-WV program consisted of 16 individual sessions, although the exact duration of each session was not specified. Follow-up assessments were conducted at 3 and 6 months after the intervention. The CBT intervention evaluated by Hobfoll et al. (2016) included seven individual sessions, delivered at least 2 days apart, and participants were followed up at 6 weeks. While none of these studies provided sufficient data to confirm statistical significance, all three interventions demonstrated potential for reducing PTSD symptoms in veteran populations.
Later-Adulthood Trauma Reengagement
One study (Pless Kaiser et al., 2023) addressed Later-Adulthood Trauma Reengagement (LATR). This intervention was US-based and delivered to a sample of men (n = 46) and women (n = 1) with PTSD. The instrument used to assess PTSD symptomatology was PCL-5, and significant differences between pre- and post-test were found. This study reported a dropout rate of 21.3%.
The intervention was structured as a 10-session group-based program, although the specific duration of each session was not detailed. The program targeted trauma re-engagement processes in later life, supporting the emotional processing of past wartime experiences in the context of aging. Despite limited evidence, this structured approach shows promising preliminary results for older veteran populations and warrants further empirical examination.
Psychoeducation
One study (Tyrrell et al., 2019) addressed an intervention program based on principles of psychoeducation, and it was called “Memory Skills for Older Adults with PTSD” (MSOAP). This intervention was US-based and delivered to a sample of men (n = 95) and women (n = 6) who had military-related PTSD. The instrument used to assess PTSD symptomatology was PCL-C, and no significant differences between pre- and post-test were found. This study mentioned a 9.9% dropout rate.
The program consisted of eight group sessions, each lasting approximately 60 min. The intervention was focused on enhancing memory and coping strategies through psychoeducational content rather than directly targeting trauma processing. While results did not demonstrate significant clinical change in PTSD symptoms, the relatively low dropout rate may indicate good acceptability and feasibility in older veteran populations.
Present-Centered Therapy
One study (Schnurr & Lunney, 2015) addressed present-centered therapy (PCT). This intervention was US-based and delivered to a sample of women (n = 284) with PTSD. The instruments used to assess PTSD symptomatology were CAPS and PCL, and significant differences between pre- and post-test were found. This study had a dropout rate of 21%.
The intervention consisted of eight individual sessions, delivered over 10 weeks, with each session lasting approximately 90 min. Follow-up assessments were conducted at 3 and 6 months post-treatment. PCT, while not explicitly trauma-focused, emphasizes current life problems and coping strategies and has demonstrated modest yet significant effects in clinical populations where trauma exposure is ongoing or where trauma-focused approaches may be contraindicated or declined.
Continuance Group Intervention Protocol
One study (Levi & Shoval-Zukerman, 2017) addressed a Continuance Group Intervention Protocol (CGIP). This intervention was developed in Israel and delivered to a sample of 51 with PTSD. The instrument used to assess PTSD symptomatology was PCL-M. The study reported statistically significant reductions in PTSD symptoms from pre- to post-intervention, with sustained improvements observed at the six-month follow-up. The study did not report any dropout rate.
The intervention was delivered in a group format of 10-hr sessions (including breaks), although the total number of sessions was not specified. The protocol focused on structured group engagement and emotional processing, aiming to reinforce psychological stability and coping in veterans. While the results are promising, the absence of dropout data and limited information on session frequency or duration per week constrain broader conclusions regarding feasibility and adherence.
RTM Therapies
One study (Gray et al., 2021) examined a RTM protocol. This intervention was US-based and delivered to a sample of 15 women with PTSD. The instruments used to assess PTSD symptomatology were PCL-M and PSS-I (PTSD Symptom Scale interview) and reported significant differences regarding both measures between pretest and posttreatment. This study mentioned a 3% dropout rate.
The intervention consisted of three individual sessions, each lasting approximately 120 min, and was typically completed within 3 weeks. Follow-up assessments were conducted 2 weeks after the initial assessment, with extended follow-ups at 6 months (PCL-M only) and 1 year. Despite the brief format, RTM showed strong short-term effects and high treatment retention. However, as evidence remains limited, further large-scale studies are needed to determine its long-term effectiveness and generalizability across populations.
Veterans Transition Program
One study (Cox et al., 2017) addressed the VTP. This intervention was based in Canada and delivered to a sample of 117 veterans with PTSD symptomatology, 101 males and 16 females. The instrument used to assess PTSD symptomatology was PCL-5, and reported statistically significant differences between pre- and post-test. This study did not mention any dropout rate.
The VTP consisted of an intensive 80-hr group program delivered over 10 consecutive days, comprising 8 hr of structured therapeutic activities daily. The intervention focused on psychological transition, identity reconstruction, and peer support in a group setting. Despite the high treatment intensity, results suggest meaningful clinical benefits. Nevertheless, the lack of dropout data and long-term follow-up limits the ability to draw broader conclusions about feasibility and sustained efficacy.
Frequency of the Identified Interventions
This subsection reports the frequency with which psychotherapeutic interventions were examined across the included studies and should not be interpreted as an indicator of the effectiveness of these interventions. Frequencies are presented at the study level, with each study counted once according to its primary intervention focus.
PE was the most frequently examined intervention, representing 29.6% of the included studies (n = 8). Relaxation-based interventions and CPT were each examined in 11.1% of studies (n = 3 each). Other interventions, including EMDR, 3MDR, PCT, psychoeducational approaches, LATR, and the VTP, were each represented in one or two studies.
The predominance of PE and other trauma-focused interventions likely reflects their longstanding presence in clinical guidelines and research agendas for PTSD rather than superiority in clinical outcomes per se. Conversely, several less frequently studied interventions may show promising effects but remain underrepresented due to their more recent development, narrower clinical scope, or limited dissemination within veteran health systems. Therefore, the frequency of investigation should be interpreted as an indicator of research attention rather than as evidence of comparative effectiveness, which is examined separately in subsequent sections.
Impact of the Identified Psychological Interventions on PTSD Symptoms Reduction
All 23 included studies reported reductions in PTSD symptoms from pre- to post-intervention assessments. However, the strength and interpretability of these findings varied substantially depending on the study design, statistical reporting, and methodological quality. Seventeen studies (73.9%) reported statistically significant symptom reductions. However, only seven studies (30.4%) provided sufficient statistical information, such as p-values or effect sizes, to allow explicit confirmation of statistical significance (Cox et al., 2017; Gray et al., 2021; Jones et al., 2022; Lamp et al., 2019; Pless Kaiser et al., 2023; Schnurr & Lunney, 2015; Yoder et al., 2013). Two studies explicitly reported no statistically significant effects (Tyrrell et al., 2019; Wells et al., 2022), while the remaining studies described symptom change without formal statistical testing.
Trauma-focused interventions, especially PE, CPT, and 3MDR, were associated with the most consistent reductions in PTSD symptoms across studies with higher methodological rigor. Among studies reporting effect sizes, these interventions demonstrated moderate to significant effects, including Cohen’s d values ranging from 0.66 to 1.90 (Jones et al., 2022; Lamp et al., 2019; Murphy & Turgoose, 2020; Yoder et al., 2013). Larger effect sizes were more frequently reported in RCTs and comparative designs (Gray et al., 2021; Schnurr & Lunney, 2015; Thorp et al., 2019), whereas non-randomized pre–post designs primarily provided evidence of within-group symptom change.
In contrast, non-trauma-focused interventions, including relaxation-based therapies and psychoeducational programs, were associated with smaller or non-significant reductions in PTSD symptoms when formally tested (Tyrrell et al., 2019; Wells et al., 2022). PCT demonstrated modest but statistically significant effects in a large RCT involving female veterans (Schnurr & Lunney, 2015), suggesting potential clinical utility for individuals who may not tolerate or prefer trauma-focused approaches.
Evidence from case studies and single-case reports was analyzed separately and is presented for illustrative purposes only. Across these studies, clinically meaningful reductions in PTSD symptoms were described following interventions such as PE, EMDR, RT, and trauma-related exposure approaches (Carlson et al., 1996; Cook et al., 2017; Duax et al., 2013; Hyer et al., 1995; Wald & Taylor, 2010; Yoder et al., 2010). These reports provided detailed qualitative accounts of symptom change and treatment feasibility in older veterans. However, they did not allow for statistical inference or comparative evaluation due to their inherent methodological limitations. Accordingly, case studies were excluded from the synthesis of intervention effectiveness and from any comparative assessment of the evidence strength.
Interpretation of the overall findings must also consider substantial heterogeneity in outcome measurement. Studies employed multiple versions of clinician-administered and self-report instruments, including CAPS and PCL variants with differing anchors and cut-off scores, which limits direct comparability across interventions (Cook et al., 2017; Thorp et al., 2019; Wells et al., 2022).
Follow-up assessments were reported in a minority of studies, with time points ranging from several weeks to 6 months (Jones et al., 2022; Murphy & Turgoose, 2020; Pless Kaiser et al., 2023; Schnurr & Lunney, 2015). Where follow-up data were available, maintenance of treatment gains was most consistently observed in structured trauma-focused interventions, although partial symptom return was reported in some cases (Wells et al., 2022).
Overall, while these findings support the effectiveness of several psychotherapeutic interventions for reducing PTSD symptoms among older, non-active military veterans, heterogeneity in study quality, outcome measurement, and reporting practices warrants cautious interpretation. Table 2 provides a comparative synthesis of intervention types, integrating study design, sample size, reported effectiveness, and treatment acceptability. Although effect sizes were extracted when available and are reported in the Supplemental Material, heterogeneity in study designs, outcome measures, and statistical reporting precluded their use as the primary basis for classifying the overall strength of evidence. The overall strength of evidence for each intervention was therefore qualitatively classified using an integrative approach that considered the number of independent studies, study design, consistency of findings, adequacy of statistical reporting, and approximate sample size (Table 2).
Comparative Summary of Psychotherapeutic Interventions for PTSD in Older, Non-Active Military Veterans.
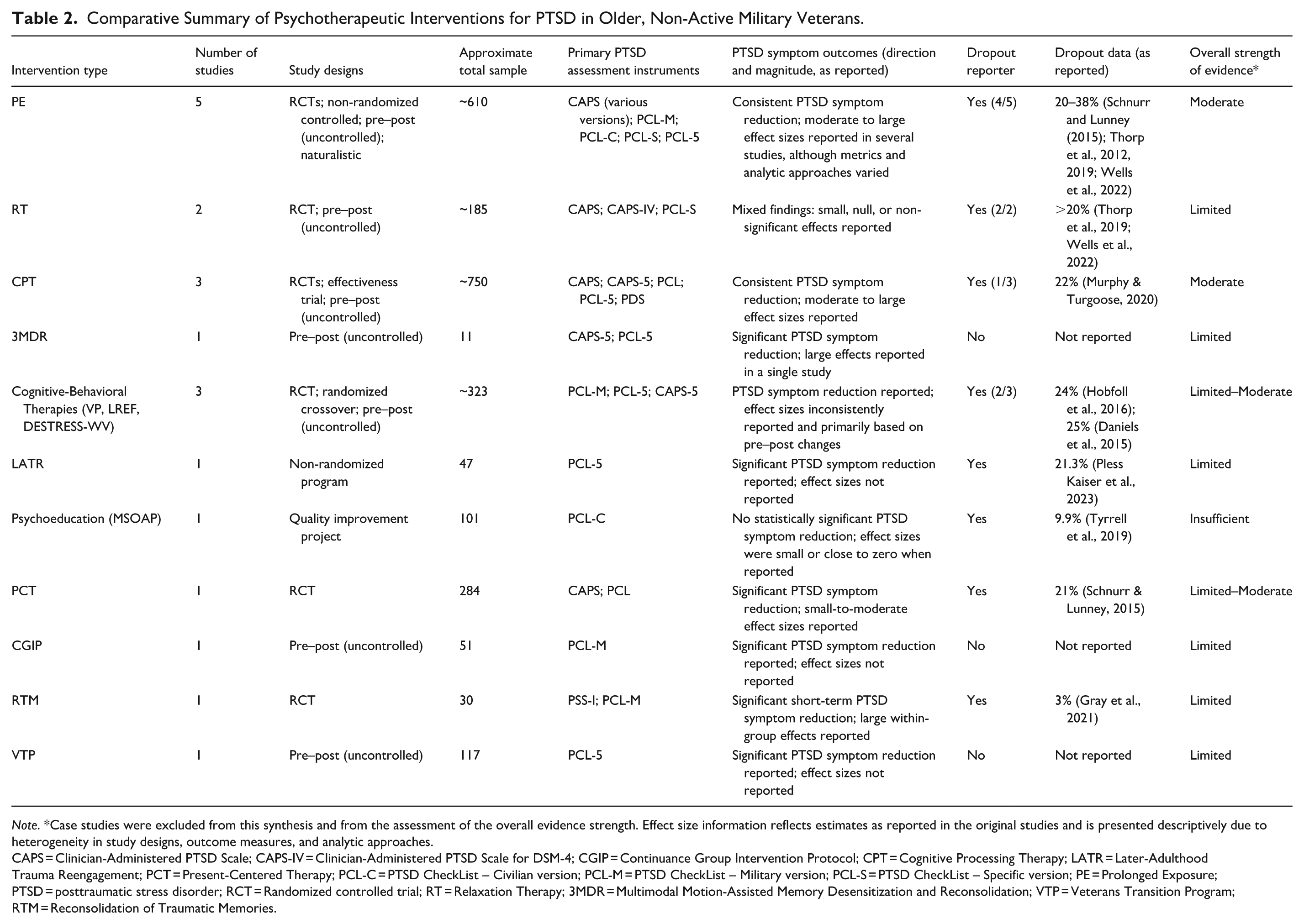
Note. *Case studies were excluded from this synthesis and from the assessment of the overall evidence strength. Effect size information reflects estimates as reported in the original studies and is presented descriptively due to heterogeneity in study designs, outcome measures, and analytic approaches.
CAPS = Clinician-Administered PTSD Scale; CAPS-IV = Clinician-Administered PTSD Scale for DSM-4; CGIP = Continuance Group Intervention Protocol; CPT = Cognitive Processing Therapy; LATR = Later-Adulthood Trauma Reengagement; PCT = Present-Centered Therapy; PCL-C = PTSD CheckList – Civilian version; PCL-M = PTSD CheckList – Military version; PCL-S = PTSD CheckList – Specific version; PE = Prolonged Exposure; PTSD = posttraumatic stress disorder; RCT = Randomized controlled trial; RT = Relaxation Therapy; 3MDR = Multimodal Motion-Assisted Memory Desensitization and Reconsolidation; VTP = Veterans Transition Program; RTM = Reconsolidation of Traumatic Memories.
Level of Bias of the Identified Psychological Interventions
Among the six RCTs included in this review (Table 3), four were judged to present some concerns regarding overall risk of bias (Gray et al., 2021; Hobfoll et al., 2016; Lehavot et al., 2021; Schnurr & Lunney, 2015), whereas two were classified as high risk of bias (Thorp et al., 2019; Wells et al., 2022). Regarding the randomization process, three trials were rated as low risk, as they provided adequate descriptions of sequence generation and demonstrated baseline equivalence between groups. In the remaining trials, insufficient reporting of allocation concealment procedures or the presence of baseline imbalances led to ratings of some concerns in this domain.
Risk of Bias Assessment of Randomized Controlled Trials Using the Cochrane Risk of Bias Tool 2 (RoB 2).
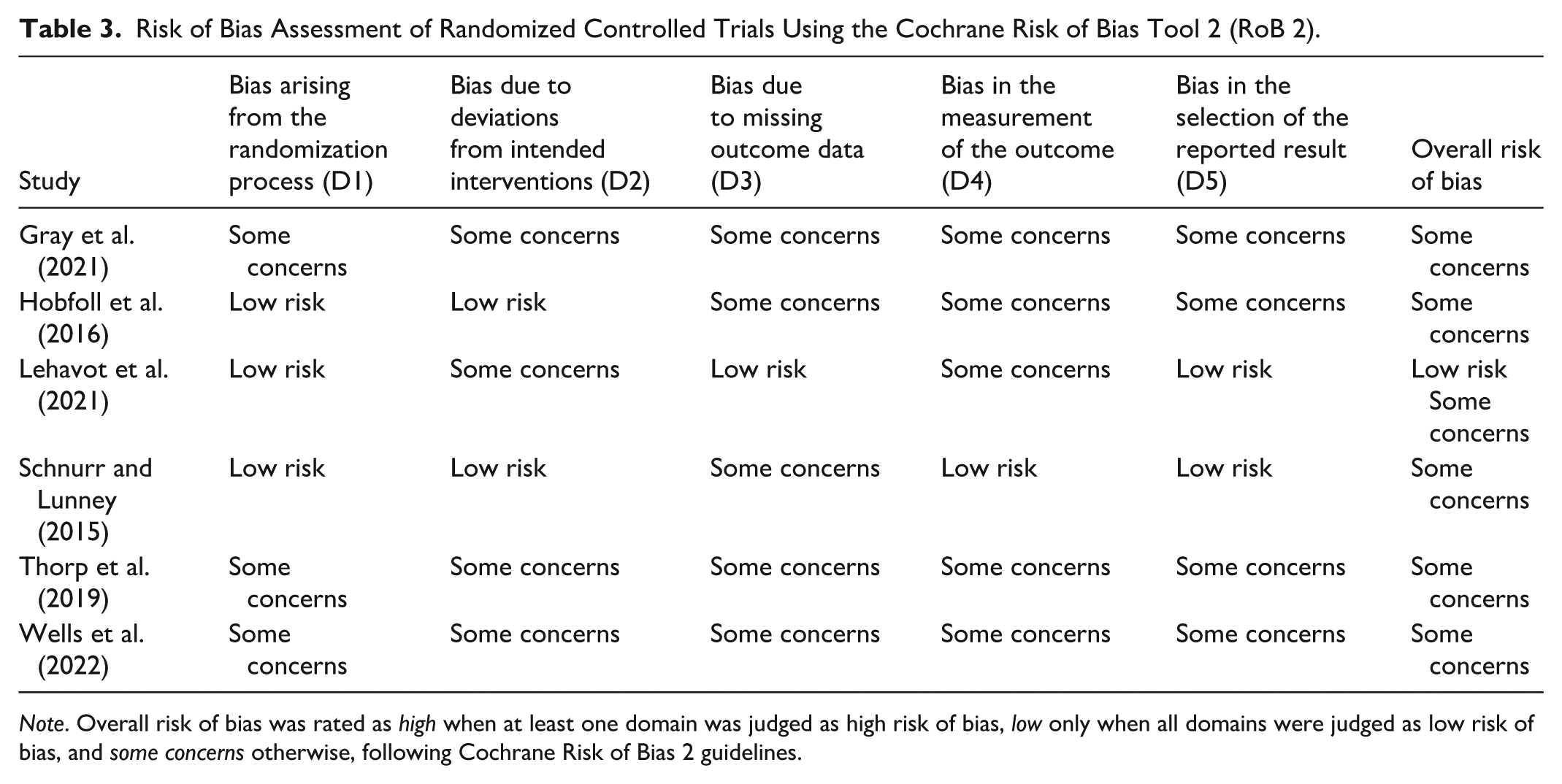
Note. Overall risk of bias was rated as high when at least one domain was judged as high risk of bias, low only when all domains were judged as low risk of bias, and some concerns otherwise, following Cochrane Risk of Bias 2 guidelines.
In the domain assessing deviations from intended interventions, most trials were rated as low risk. Although all studies necessarily employed open-label designs, the consistent use of intention-to-treat analyses, monitoring of treatment fidelity, and the absence of evidence for differential co-interventions supported favorable judgments in this domain. Missing outcome data emerged as a key source of bias. Two trials exhibited substantial attrition, particularly at follow-up assessments, and employed analytical strategies susceptible to bias, leading to judgments of high risk of bias for this domain and, consequently, at the overall level. In the remaining trials, although missing data were addressed analytically, differential dropout rates between intervention groups justified ratings of some concerns.
Regarding outcome measurement, trials relying on clinician-administered instruments conducted by independent and blinded assessors were rated as low risk. In contrast, studies that primarily relied on self-report measures without participant blinding were rated as presenting some concerns due to increased susceptibility to expectancy and reporting biases. Finally, in the domain of selection of the reported results, only a subset of trials reported preregistered protocols or clearly predefined analytic plans. The absence of preregistration or a priori outcome specification led to concerns in most trials. In accordance with RoB 2 guidance, the presence of some concerns in any single domain precluded an overall judgment of low risk of bias, even when all remaining domains were rated as low risk.
In contrast to the RCTs assessed with RoB 2, the evaluation of the 17 non-randomized and pre–post studies using RoBANS (Table 4) indicated a generally higher risk of bias. Most studies were judged to present a high risk of bias in participant selection, reflecting the frequent use of convenience samples, limited eligibility criteria, and the absence of appropriate comparison groups. The domain addressing confounding variables also emerged as a major limitation, as clinically relevant factors, such as psychiatric comorbidities, exposure to multiple trauma types, and concurrent psychological or pharmacological treatments, were rarely measured or systematically controlled.
Risk of Bias Assessment of Non-Randomized and Pre–Post Studies Using RoBANS.
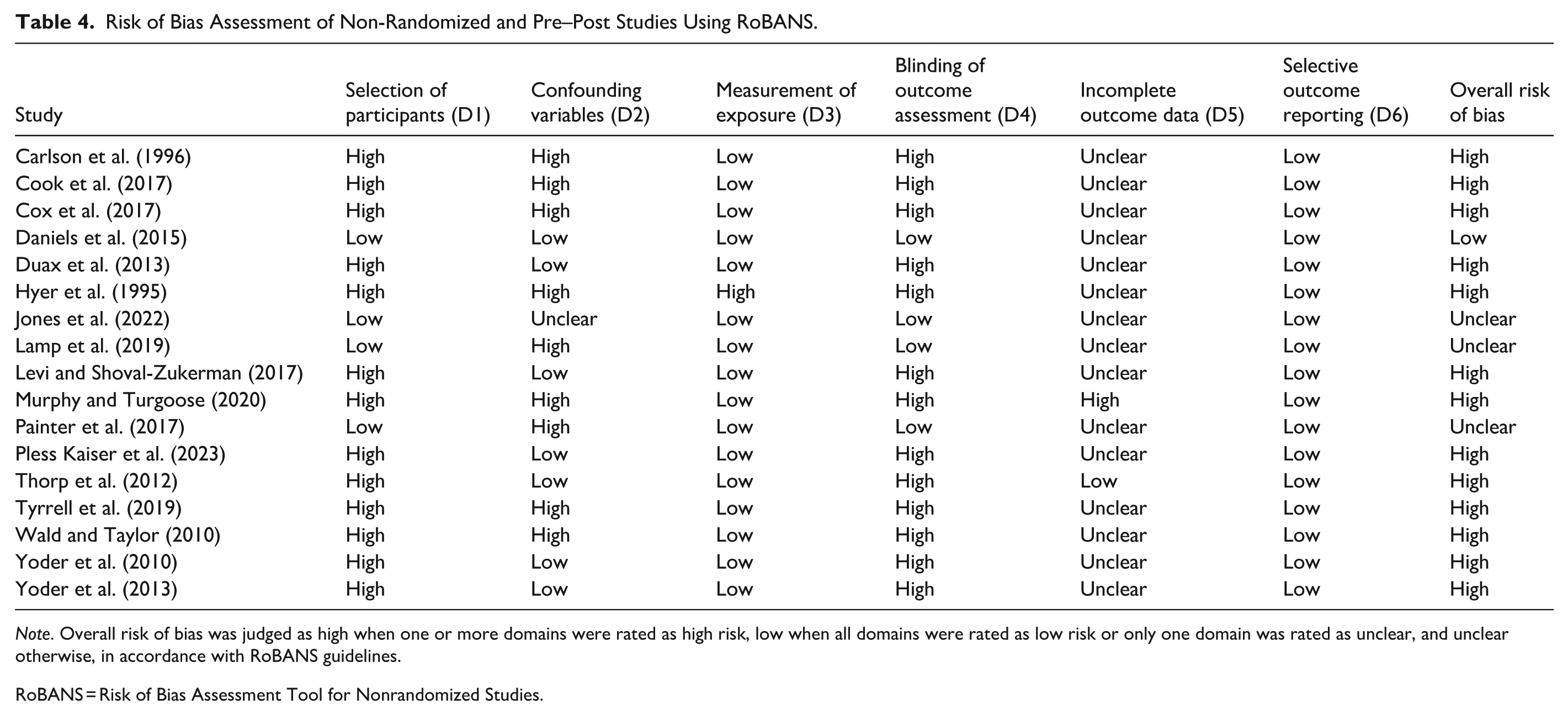
Note. Overall risk of bias was judged as high when one or more domains were rated as high risk, low when all domains were rated as low risk or only one domain was rated as unclear, and unclear otherwise, in accordance with RoBANS guidelines.
RoBANS = Risk of Bias Assessment Tool for Nonrandomized Studies.
In contrast, the measurement of exposure or intervention was generally rated as low risk, as most studies provided sufficiently detailed descriptions of the therapeutic protocols and their implementation. Greater variability was observed in the assessment of outcomes. Studies employing validated instruments and standardized assessment procedures tended to receive more favorable ratings, whereas studies relying exclusively on self-report measures without independent or blinded clinical assessment were rated as presenting a higher or unclear risk of bias in this domain.
The handling of incomplete outcome data represented an additional limitation. Several studies failed to report dropout rates or to describe strategies for managing missing data, resulting in high or unclear risk judgments for this domain. Selective outcome reporting was also identified as a recurrent concern, given the absence of preregistered protocols and incomplete reporting of statistical results in a substantial proportion of studies.
Taken together, the risk of bias assessment highlights substantial heterogeneity in the methodological quality of the available evidence. Although several psychotherapeutic interventions show promising effects for veterans with PTSD, limitations were particularly pronounced among non-randomized and pre–post studies, as well as among randomized trials with substantial attrition. These findings justify a cautious interpretation of effect estimates and provide essential context for the strength-of-evidence classifications.
Discussion
This integrative review identified 16 psychotherapeutic interventions across 23 studies involving 2,030 participants from 10 countries and 3 continents. Interventions were grouped into 10 categories according to their underlying theoretical models. To our knowledge, this is the first integrative review to focus specifically on psychotherapeutic interventions implemented with older, non-active military veterans diagnosed with PTSD. The primary aim was to identify and describe these interventions in terms of their structure, reported outcomes, including symptom reduction and dropout rates, and the strength of evidence supporting their effectiveness in this population.
Overall, exposure-based therapies emerged as the most frequently studied category. This predominance is consistent with the broader PTSD literature, which places strong emphasis on trauma-focused interventions supported by a substantial empirical base. Most interventions analyzed fell within this category, likely reflecting both accumulated scientific evidence and prevailing clinical practice patterns. The application of psychotherapeutic interventions in high-risk populations such as military veterans is marked by particular urgency and complexity, given repeated exposure to combat, death, and severe injury, often compounded by cumulative trauma and long-term symptom persistence (Goldberg et al., 2016; Shahmiri Barzoki et al., 2023).
The frequent implementation of exposure-based interventions, especially PE, reflects a clinical preference grounded in evidence demonstrating its effectiveness in reducing PTSD symptoms. Findings from this review are broadly consistent with previous studies supporting PE in veteran populations (Thorp et al., 2019; Wald & Taylor, 2010; Yoder et al., 2013). Interventions grounded in cognitive behavioral principles further underscore the relevance of addressing maladaptive trauma-related cognitions and avoidance behaviors (Daniels et al., 2015; Tyrrell et al., 2019). In contrast, less frequently studied interventions, including LATR, MSOAP, PCT, the CGIP, RTM, and the VTP, appear to reflect more recent developments or approaches tailored to specific clinical contexts. Their limited representation in the literature is more plausibly attributable to an early stage of empirical evaluation rather than a lack of therapeutic potential. Nevertheless, the available evidence remains insufficient to support robust conclusions regarding their comparative effectiveness.
Across the included studies, 17 reported statistically significant reductions in PTSD symptoms following intervention, spanning 11 distinct therapeutic approaches. However, only seven studies provided sufficient statistical detail to support robust inferences regarding effectiveness, underscoring persistent limitations in reporting practices. Overall, the pattern of findings is broadly consistent with international clinical guidelines, which recommend trauma-focused psychotherapies—particularly PE, CPT, EMDR, and CBT—as first-line treatments for PTSD (Courtois et al., 2017; NICE, 2018; Phoenix Australia, 2021; VA/DoD, 2023). At the same time, PCT is not uniformly recommended across guidelines, and relaxation-based interventions currently lack sufficient empirical support to justify recommendation as standalone treatments (Courtois et al., 2017; VA/DoD, 2023).
Importantly, inconsistencies were observed both across and within intervention categories. Two studies examining three interventions (PE, RT, and MSOAP) reported no statistically significant reductions in symptoms, while six additional studies involving seven therapies did not report whether pre–post differences reached statistical significance. Mixed findings were particularly evident for relaxation-based interventions, with some studies reporting symptom reductions and others reporting null effects (Wells et al., 2022). These discrepancies reinforce the importance of distinguishing between the frequency with which interventions are implemented and the strength of evidence supporting their effectiveness.
Treatment dropout represents a further critical issue. Fewer than half of the included studies reported dropout rates, limiting conclusions regarding acceptability and feasibility. Among those that did, dropout ranged from 3% to 38% across a range of interventions (Daniels et al., 2015; Gray et al., 2021; Hobfoll et al., 2016; Murphy & Turgoose, 2020; Pless Kaiser et al., 2023; Schnurr & Lunney, 2015; Thorp et al., 2012, 2019; Tyrrell et al., 2019; Wells et al., 2022). Prior research suggests that attrition may vary as a function of trauma type, with higher completion rates observed among veterans with combat-related PTSD compared to non-combat-related trauma (Miles & Thompson, 2016). These findings underscore the need to consider clinical complexity, comorbidity, and patient preferences when selecting and delivering interventions for older veterans.
Although substantial evidence supports the effectiveness of PE and CBT in reducing PTSD symptoms among older military veterans (Cook et al., 2017; Daniels et al., 2015; Duax et al., 2013; Hobfoll et al., 2016; Schnurr & Lunney, 2015; Thorp et al., 2012; Yoder et al., 2010), this does not preclude the potential value of less frequently studied interventions such as LATR and RTM. These approaches may be particularly relevant for specific subgroups or clinical contexts, especially when tailored to individual profiles and life-stage considerations. Continued research is therefore essential to expand the evidence base and support more nuanced, patient-centered clinical decision-making.
Despite the availability of validated interventions, several challenges persist in their application to veteran populations. These include limited treatment response for some individuals, high nonresponse rates, and the frequent presence of comorbid conditions such as traumatic brain injury and other medical or psychiatric disorders (Maguen et al., 2020; Steenkamp et al., 2015). Intervention timing, treatment completion, and modality have also been shown to influence outcomes (Steenkamp et al., 2015). Converging evidence suggests that treatment gains among veterans may be more modest than those observed in civilian populations, irrespective of baseline PTSD severity (Miles & Thompson, 2016).
The reliance on self-report measures to assess PTSD symptoms introduces additional interpretative challenges. Potential influences such as social desirability or symptom amplification related to access to services or benefits have been noted in the literature and may compromise outcome validity. These considerations highlight the importance of incorporating multimethod assessment strategies in future research.
Finally, the risk of bias assessment provides essential context for interpreting the findings of this review. Most RCTs were rated as presenting some concerns regarding risk of bias, primarily due to missing outcome data, reliance on self-report measures, and the absence of preregistered analytic plans. Two randomized trials were judged to be at high risk of bias, primarily due to substantial attrition at follow-up and limitations in handling missing data. In parallel, the majority of non-randomized and pre–post studies were classified as high risk of bias, particularly in domains related to participant selection and control of confounding variables. Taken together, these findings indicate that, although several psychotherapeutic interventions demonstrate promising effects for older veterans with PTSD, the current evidence base is constrained by methodological limitations that may inflate effect estimates or limit generalizability. Accordingly, strength-of-evidence classifications should be interpreted with caution. Future research would benefit from adequately powered randomized trials with improved retention strategies, standardized outcome assessment, and transparent preregistration of outcomes and analytic plans.
Limitations
This review has several limitations that should be considered when interpreting the findings. First, the literature search was conducted across five electronic databases (Scopus, PsycARTICLES, SciELO, PubMed, and Web of Science Core Collection). Although these databases cover a substantial proportion of the relevant literature in psychology and mental health, some eligible studies may not have been retrieved. In addition, only studies published in English or Portuguese were included, potentially excluding relevant evidence published in other languages.
Beyond the methodological constraints of the review process, important limitations were identified in the included primary studies. A significant limitation concerns the quality and consistency of statistical reporting. Many studies did not provide sufficient statistical information, such as effect sizes, confidence intervals, or detailed significance testing, thereby precluding quantitative synthesis and limiting robust comparisons across interventions. Consequently, conclusions regarding relative effectiveness must be interpreted with caution.
Another important limitation is the limited availability of follow-up data. Only a small subset of studies included follow-up assessments, restricting the evaluation of long-term treatment effects and the maintenance of symptom gains. Given the chronic and fluctuating nature of PTSD in older military veterans, the lack of longitudinal data represents a significant gap in the evidence base.
Dropout rates were also inconsistently reported across studies. Fewer than half of the included studies reported treatment attrition, limiting the assessment of intervention acceptability, feasibility, and adherence. This is particularly relevant in veteran populations, where clinical complexity, comorbidity, and treatment burden may substantially influence engagement and completion.
Substantial heterogeneity across studies further limits comparability. Included studies varied widely in design, sample size, intervention format, and outcome measures. The diversity and limited conceptual overlap of outcome instruments across studies precluded sensitivity analyses and systematic mapping of results to a standard metric. Consequently, it cannot be excluded that some observed differences between intervention types reflect, at least in part, measurement-related effects rather than actual differences in treatment efficacy, which constrains direct comparisons and has implications for the clinical interpretation of the findings. Many studies relied on pre–post designs without control groups, limiting internal validity and preventing causal inference. In addition, several studies relied exclusively on self-report measures to assess PTSD symptoms, which may be influenced by reporting biases, including social desirability or contextual factors related to access to services or benefits.
Finally, few studies systematically examined potential moderators of treatment outcome, such as trauma type, comorbid psychiatric or medical conditions, age-related factors, or demographic characteristics. The absence of moderator analyses limits our understanding of differential treatment responses and constrains the development of tailored, patient-centered interventions. Moreover, some interventions were evaluated in small samples, which may limit the generalizability of the findings to broader populations of older, non-active military veterans.
Clinical and Practical Implications
The findings of this review on psychotherapeutic interventions for military veterans with PTSD have several practical implications for clinical practice at different levels (see Table 5). The review synthesizes available psychotherapeutic intervention options, outlining their strengths and limitations to support clinical decision-making among mental health professionals. The identification of consistent evidence for the efficacy of trauma-focused therapies, such as CPT and PE, provides an empirical basis for treatment selection and prioritization. This evidence may assist clinicians in aligning intervention choices with approaches that are more likely to produce clinically meaningful outcomes for military veterans with PTSD.
Implications for Research, Practice, and Policy.

Future Research
Future studies should prioritize the implementation of methodologically robust, large-scale RCTs that directly compare the effectiveness of different psychotherapeutic interventions for military veterans with PTSD. Additionally, longitudinal studies are crucial for evaluating the durability of treatment effects over time. Further research should also explore the potential of integrating multiple therapeutic approaches to enhance clinical outcomes. It is essential to investigate demographic and contextual variables, such as age, gender, and cultural background, that impact treatment efficacy. Moreover, distinguishing between different trauma types (e.g., childhood trauma, combat-related trauma, and military sexual trauma) is critical to developing interventions that are sensitive to the specific characteristics and clinical needs of each subgroup. A more nuanced understanding of these factors will contribute to the development of personalized, targeted, and culturally competent interventions, thereby improving access to adequate care and overall mental health outcomes for veterans with PTSD.
Conclusion
This integrative review synthesized evidence from 23 studies involving 2,030 participants and provides an overview of the range of psychotherapeutic interventions implemented with older, non-active military veterans diagnosed with PTSD. The findings indicate that trauma-focused interventions, particularly exposure-based and cognitive behavioral approaches, dominate the existing literature and are supported by the most consistent evidence of symptom reduction (Table 6). Nevertheless, the predominance of these approaches reflects both clinical uptake and research focus, rather than unequivocal superiority across all outcomes and patient profiles.
Critical Findings of this Review.

Note. CGIP = Continuance Group Intervention Protocol; LATR = Later-Adulthood Trauma Reengagement; MSOAP = Memory Skills for Older Adults with PTSD; PCT = Present-Centered Therapy; PTSD = posttraumatic stress disorder; RT = Relaxation Therapy; RTM = Reconsolidation of Traumatic Memories.
Less frequently studied interventions, including later-adulthood trauma re-engagement and reconsolidation-based approaches, show preliminary promise and may be particularly relevant for specific subgroups of veterans or clinical contexts. However, the current evidence base remains limited, underscoring the need for further rigorous evaluation before broad clinical implementation.
Despite the availability of evidence-based psychotherapies, the review highlights persistent challenges in the treatment of PTSD among older veterans, including clinical complexity, comorbid conditions, variable treatment response, and substantial rates of nonresponse and dropout. These findings reinforce the importance of moving beyond one-size-fits-all models toward more flexible, patient-centered approaches that account for life-stage factors, comorbidity, and treatment tolerability.
Future research should prioritize methodologically robust designs, including adequately powered RCTs, standardized outcome measures, and more extended follow-up periods, to clarify the durability of treatment effects. Greater attention to moderators of treatment response will be essential to inform tailored intervention strategies and to optimize the quality of care for aging veteran populations living with PTSD.
Supplemental Material
sj-docx-1-tva-10.1177_15248380261433011 – Supplemental material for Psychotherapeutic Interventions for Older, Non-Active Military Veterans With PTSD: An Integrative Review of Types, Effectiveness, and Clinical Outcomes
Supplemental material, sj-docx-1-tva-10.1177_15248380261433011 for Psychotherapeutic Interventions for Older, Non-Active Military Veterans With PTSD: An Integrative Review of Types, Effectiveness, and Clinical Outcomes by Mariana Gonçalves, Tânia Gonçalves, Cristiana Santos, Bárbara Sousa and Ângela Maia in Trauma, Violence, & Abuse
Footnotes
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was conducted at the Psychology Research Centre (CIPsi/UM) School of Psychology, University of Minho, and supported by the Portuguese Ministry of National Defense and partially by the Foundation for Science and Technology (FCT; UID/01662: Centro de Investigação em Psicologia) through national funds. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
