Abstract
Objectives:
The objective of this scoping review is to examine the extent, range, and nature of literature targeting health-care professionals on the prevalence and outcome of intimate partner violence (IPV)-related traumatic brain injury (TBI). The purpose is to gain an understanding of prevalence, investigate screening tool use, generate IPV/TBI-specific support recommendations, and identify suggestions for future research.
Method:
The review was guided by Arksey and O’Malley’s five stages for conducting a scoping review. A comprehensive search of nine databases revealed 1,739 articles. In total, 42 published research papers that focused specifically on TBI secondary to IPV were included in the study.
Synthesis:
The literature reports inconsistencies in prevalence rates from IPV-related TBI. There are no current standardized screening practices in use, though the literature calls for a specialized tool. Frontline professionals would benefit from education on signs and symptoms of IPV-related TBI. Empirical studies are needed to generate reliable data on prevalence, experience, and needs of brain-injured survivors of TBI.
Conclusions:
Findings from this study demonstrate the need for the development of an IPV-sensitive screening tool, more accurate data on prevalence, an interprofessional approach to care, and raised awareness and education on the diffuse symptoms of IPV-related TBI.
Traumatic brain injury (TBI) is a serious consequence of intimate partner violence (IPV) that is often overlooked or misdiagnosed (Corrigan, Wolfe, Mysiw, Jackson, & Bogner, 2003; St. Ivany & Schminkey, 2016). IPV-related TBI can have debilitating long-term effects on a survivor’s overall function and independence and may masquerade as a number of other physical, social, and mental health issues, preventing survivors from receiving appropriate intervention by health and community professionals (Iverson & Pagoda, 2015; Kwako et al., 2011). Research and guidance for professionals working in this community is limited, despite the resounding call throughout the literature for increased awareness of this population across diverse fields of practice, study, and sites of triage.
IPV encompasses physical, sexual, and emotional abuse, and controlling behaviors, inflicted by an intimate partner (World Health Organization [WHO], 2016). While sex workers are often excluded from this group, there are many shared experiences of violent encounters linked to intimate relationships between women exposed to IPV and sex workers (Baumann et al., 2018; Farley, Banks, Ackerman, & Golding, 2018), as such, we have chosen to include sex workers in this review. The WHO estimates one in three women throughout the world will experience IPV in their lifetime (WHO, 2017). According to recent Canadian statistics, rates of self-reported spousal violence range from 4% to 8% across provinces (Statistics Canada, 2016). It is estimated that 42% of women survivors experience injury as a result of IPV (Statistics Canada, 2016). The most common injuries are from battery to the face, head, and neck, a pattern of violence leaving survivors vulnerable to TBI (Sheridan & Nash, 2007).
TBI is defined as “an alteration in brain function or other evidence of brain pathology, caused by an external force” such as a blow or injury to the head, severe rotation of the neck, and acceleration/deceleration movement (Menon, Schwab, Wright, & Maas, 2010, p. 1638). Classifications of severity are typically assessed through tests measuring loss of consciousness, post-traumatic amnesia, and postincident deficits. It is a leading cause of disability worldwide and is more prevalent than breast cancer, spinal cord injury, HIV/AIDS, and multiple sclerosis combined (Haag et al., 2016). While brain injury caused by lack of oxygen through strangulation is technically classified as anoxic or hypoxic injury, resultant challenges closely resemble TBI and both conditions are treated in the same manner (Cullen & Weisz, 2011). As such, we, along with others, have chosen to include IPV-related strangulation injuries (Campbell et al., 2018; Kwako et al., 2011; St. Ivany & Schminkey, 2016; Valera & Kucyi, 2017; Valera et al., 2018).
TBI as a consequence of injuries in football, hockey, soccer, and military service are areas of increasing interest (Schneuer et al., 2018; St. Ivany & Schminkey, 2016; Zetterberg et al., 2018). Public awareness of the concussion crisis in sports and the military has increased, including the long-term effects of a condition found in athletes with a history of repeated brain trauma called chronic traumatic encephalopathy (CTE). However, notwithstanding the mechanism of injury, symptom sequelae, and prognosis of CTE being comparable, IPV-related TBI remains understudied, despite indications of increased prevalence rates (Goldin, Haag, & Trott, 2016; Kwako et al., 2011; St. Ivany & Schminkey, 2016; Valera et al., 2018).
Exposure to TBI through IPV tends to be long term in nature. Women are often exposed to repeated violent encounters before calling police, go through numerous attempts before permanently leaving an abuser, and are at the highest risk of being murdered when attempting to leave or report (Banks, 2007; Car, 2000). Repeated trauma to the head can cause brain tissue degeneration resulting in fatigue, depression and mood changes, memory loss, confusion, aggression, impaired judgment, and difficulty with everyday tasks and can lead to dementia and other chronic health conditions (Langlois, Rutland-Brown, & Wald, 2006). Women exposed to IPV are twice as likely to experience depression, and nearly twice as likely to have alcohol use disorders, compared to women who have not experienced IPV (WHO, 2017).
It is difficult to estimate the impact of this issue and provide appropriate care for survivors without adequate means to measure and understand the relationship between IPV and TBI. Whereas there are distinct bodies of literature examining IPV and TBI, respectively, relatively few studies directly address the correlation between them. While there are some excellent existing literature reviews exploring the link between IPV and TBI, which are informative and relevant in nature and content, they did not use systematic data collection nor do they cover the full scope of the literature available (Banks, 2007; Kwako et al., 2011; Murray, Lundgren, Olson, & Hunnicutt, 2016; St. Ivany & Schminkey, 2016). Since the last literature reviews available, there have been numerous additional studies published on IPV-related TBI. Therefore, we undertook this scoping review with the following objectives: (a) determine how the literature understands the relationship of IPV and TBI, (b) summarize prevalence of IPV-related TBI as reported in current literature, (c) determine what screening tools are being used to identify TBI in IPV survivors, (d) develop IPV/TBI support recommendations for health-care professionals and support personnel, and (e) identify suggestions for future research.
Method
Scoping review methodology (Arksey & O’Malley, 2005; Levac, Colquhoun, & O’Brien, 2010) is used to collect all relevant studies and determine whether a full systematic review is warranted when the scope of existing literature is known to be limited. The systematic nature of this approach to sampling ensures that the search is repeatable and comprehensive, while identifying gaps in knowledge and areas of future study (Arksey & O’Malley, 2005). Although the authors acknowledge that IPV takes many forms and affects other related populations, the study focused on IPV-related TBI in women, addressing a previously identified need to highlight gender differences and complications unique to women and TBI (Haag et al., 2016).
The study followed five major steps of scoping review as outlined by Levac, Colquhoun, and O’Brien (2010): (a) identify the research question, (b) identify relevant studies, (c) select studies, (d) chart data, and (e) collate, summarize, and report the results. Our preliminary search for data was guided by the following research question: To what extent does health-care literature recognize the correlative relationship of TBI and IPV?
The search strategy was designed in consultation with an expert librarian. Nine major health science databases were searched: OVID Medline, Cochrane, CINAHL, EBSCO, Embase, ASSIA, PsycINFO, Scopus, and Web of Science. To qualify for inclusion, each article was required to be peer reviewed, available in English, and explicitly address the intersection of TBI and IPV. In an effort to draw all relevant literature, our search was delimited by time frame. Articles selected corresponded with a paired combination of the following two key word categories:
domestic violence, spousal abuse, intimate partner violence (IPV), interpersonal violence, battered women, intimate violence,
traumatic brain injury (TBI), concussion, head injury, post-concussion syndrome, strangulation, choking, face injury, neck injury
An additional manual search was conducted from the reference lists of each included study. The research team developed specific inclusion and exclusion criteria and a three-stage process was completed to identify all relevant articles. In the first stage, two researchers independently completed an initial title review and articles were included based on appropriateness of the title. In the case consensus could not be reached, a third author was consulted and/or it was included in the abstract review. Articles were primarily excluded because they (a) lacked relevance to TBI and IPV, (b) focused on children, (c) addressed IPV or TBI as distinct or unrelated, or (d) emphasized the perpetrator role. Once the title review was completed, an abstract review was done following the same procedures, and then, full consideration of each remaining article, to determine final suitability for inclusion.
Results
The initial search returned 1,739 articles and, with the addition of a hand search by three authors, 42 articles were included in the final sample. Three researchers independently extracted data and compared findings to ensure consistency, using a charting form to organize key variables. The extracted data were then organized into the following four key domains: (a) estimates of prevalence, (b) screening tools and identification procedures for IPV-related TBI, (c) recommendations for health-care professionals, and (d) recommendations for future research. The results provided below are organized into these domains for clarity of reporting. Article summaries reporting original research are listed in Table 1. Literature reviews, editorials, and invited commentary are reported in Table 2.
Data Chart Original Research.
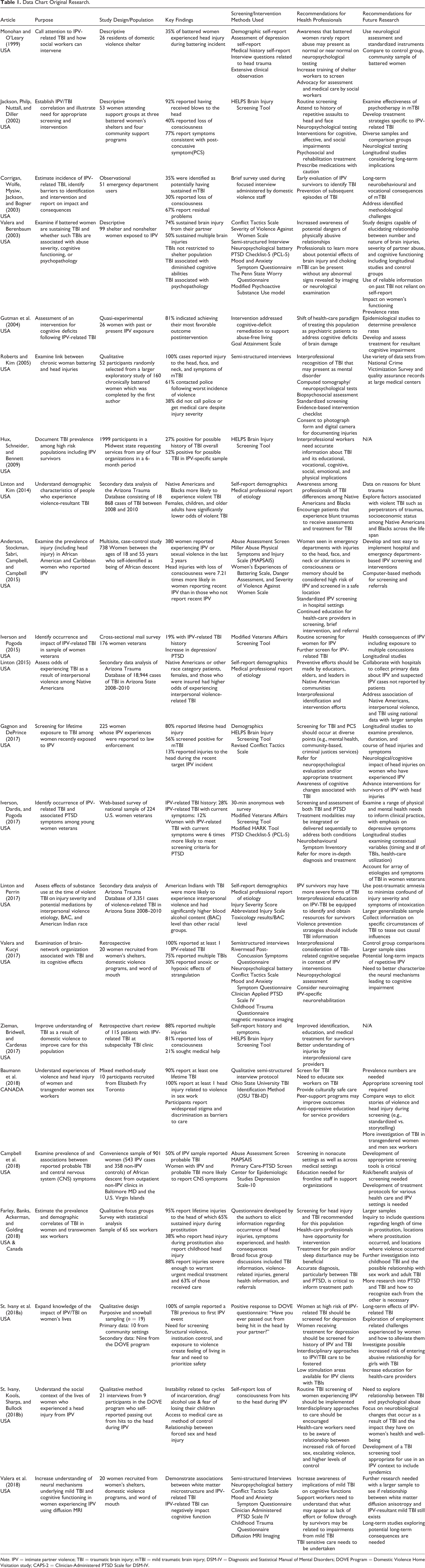
Note. IPV = intimate partner violence; TBI = traumatic brain injury; mTBI = mild traumatic brain injury; DSM-IV = Diagnostic and Statistical Manual of Mental Disorders; DOVE Program = Domestic Violence Home Visitation study; CAPS-2 = Clinician-Administered PTSD Scale for DSM-IV.
Data Chart Review Articles.
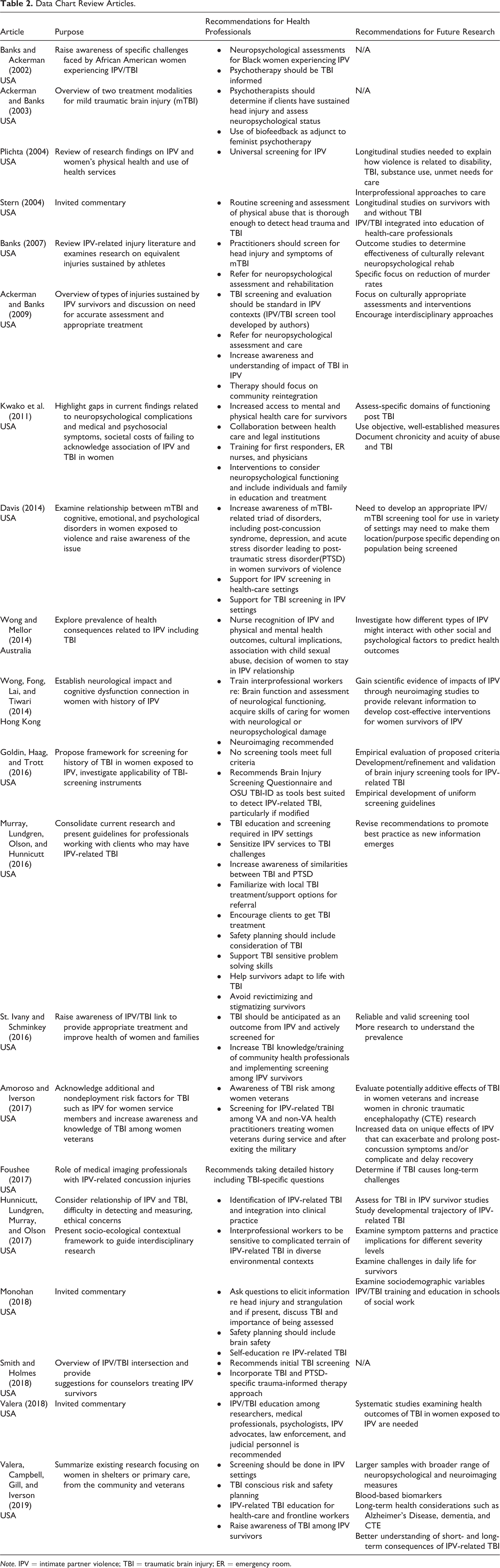

Note. IPV = intimate partner violence; TBI = traumatic brain injury; ER = emergency room.
Estimates and Reports of Prevalence
Empirical studies reported original prevalence data figures of IPV-related TBI ranging from 19% (Iverson, Dardis, & Pogoda, 2017) to 75% (Valera et al., 2018) and as high as 100% in studies that included only survivors who reported injuries to the head (Roberts & Kim, 2005; St. Ivany et al., 2018a), itemized by study in Table 1. Diagnostic criteria for TBI-related IPV focused on positive history of physical blows to the head, face, and neck, altered or lost consciousness, TBI symptom sequelae, or a combination of these elements. For example, in one study, 100% of the respondents were positive for both history and lasting TBI symptoms (Roberts & Kim, 2005), while another study reported 92% of respondents had a positive history of blows to the head with 40% losing consciousness (Jackson, Philp, Nuttal, & Diller, 2002). In both cases, a TBI diagnosis was inferred. Studies also referred to IPV-related TBI by a number of different words including TBI, mild TBI, head injury, and concussion, so a positive screen may be named in different ways based on different criteria. History of physical violence to the head, face, and neck was found in anywhere from 35% to 100% (Monohan & O’Leary, 1999; Roberts & Kim, 2005) of respondents in this sample. Estimates of lost consciousness during episodes of physical violence were reported to range from 30% to 81% (Corrigan et al., 2003). One study distinguished between single and multiple episodes of violence resulting in TBI, 100% and 75%, respectively, with strangulation in 25% of these cases (Valera & Kucyi, 2017). Population types included shelter populations (Gutman et al., 2004; Jackson et al., 2002; Monohan & O’Leary, 1999; Roberts & Kim, 2005; Valera & Berenbaum, 2003; Valera & Kucyi, 2017), emergency department and hospital users (Corrigan et al., 2003), survivors in contact with law enforcement (Gagnon & DePrince, 2017), women seeking services in non-IPV specific health-care clinics (Anderson, Stockman, Sabri, Campbell, & Campbell, 2015; Campbell et al., 2018), sex workers (Baumann et al., 2018; Farley et al., 2018), and veterans (Iverson et al., 2017; Iverson & Pogoda, 2015). Many studies recruited for participants who were undiagnosed but suspected of TBI, some selected only on history of IPV, and others were included based on known TBI diagnosis, which may contribute to the variance of reported rates of prevalence.
A number of nonsystematic literature reviews and editorials were also included. Most reported statistics from empirical studies mentioned above. One study combined empirical data and extrapolations from studies concluding that 30–74% of women exposed to IPV and reporting to emergency departments may have an undiagnosed TBI (Kwako et al., 2011).
Screening Tools and Identification Procedures for IPV-Related TBI
While there are currently no validated tools designed specifically to detect IPV-related TBI, two have been developed by researchers (Ackerman & Banks, 2002; Valera & Berenbaum, 2003), and the HELPS tool has been adapted for use in an IPV context. A recent study examining existing TBI screening tools found that the Ohio State University TBI-Identification Method (OSU-TBI-ID) and the Brain Injury Screening Questionnaire were the two most adaptable for this specialized population as they met the following criteria set out by the authors: (1) include prompts relevant to the events that can result in TBI in this population; (2) allow for safe and private endorsement of an event; (3) offer ease of administration by IPV knowledgeable staff without the need for special training in TBI. (Goldin et al., 2016, pp. 2–3)
Recommendations for Frontline Professionals
The onus of screening, assessment, and triage for IPV largely falls on frontline professionals in health-care and community contexts. As early screening and intervention can lead to improved outcomes, routine screening for TBI when IPV is disclosed or suspected was encouraged by a number of authors (Ackerman & Banks, 2009; Amoroso & Iverson, 2017; Baumann et al., 2018; Campbell et al., 2018; Corrigan et al., 2003; Davis, 2014; Farley et al., 2018; Iverson et al., 2017; Iverson & Pagoda, 2015; Jackson et al., 2002; Monohan & O’Leary, 1999; Murray et al., 2016; Smith & Holmes, 2018; Stern, 2004; St. Ivany, Kools, Sharps,& Bullock, 2018b; Zieman et al., 2017). Some authors also emphasized the need for increased training for workers around identification of TBI in IPV survivors and its effects (Ackerman & Banks, 2009; Anderson et al., 2015; Baumann et al., 2018; Farley et al., 2018; Hux et al., 2009; Kwako et al., 2011; Linton & Perrin, 2017; Wong, Fong, Lai, & Tiwari, 2014). Recommendations for training included administering standardized assessments, responding to positive screens, differentiating TBI symptoms from related comorbidities, and neurological from psychiatric.
Several studies advocated for improved awareness of the intricacies of this unique population (Amoroso & Iverson, 2017; Hunnicutt, Lundgren, Murray, & Olson, 2017; Hux et al., 2009; Linton & Kim, 2014; Monohan & O’Leary, 1999; Roberts & Kim, 2005; Stern, 2004; St. Ivany & Schminkey, 2016; Valera & Berenbaum, 2003; Valera & Kucyi, 2017; Wong & Mellor, 2014; Zieman et al., 2016). Examples included awareness of IPV and its associated dangers, IPV survivors rarely reporting without being asked, and IPV-related TBI presenting as mental health and/or addictions issues. Even when neuropsychological testing is completed appropriately, it is possible survivors with IPV-related TBI may present as normal or near normal (Monohan & O’Leary, 1999; Valera & Berenbaum, 2003). Support approaches should include referral for assessment and/or external programs for clients who screen positive or are suspected of TBI (Banks, 2007; Campbell et al., 2018; Iverson & Pogoda, 2015; Jackson et al., 2002).
Some authors cited the need for health professionals to support safety planning in an effort to reduce subsequent and repetitive assaults that may have a cumulative effect on the brain (Corrigan et al., 2003; Jackson et al., 2002; Banks, 2007). Suggestions for practice included provision of transportation vouchers to aid women in finding emergency shelter and support and keeping emergency hospital or security staff in view and/or accessible at all times (Roberts & Kim, 2005). Health professionals are encouraged to maintain quality documentation and use an interprofessional approach, providing services for community reintegration and follow-up counseling in a healthy and safe atmosphere (Banks, 2007; Davis, 2014; Murray et al., 2016; Roberts & Kim, 2005; Sheridan & Nash, 2007; St. Ivany & Schminkey, 2016). Authors indicated that workers should gain competence in addressing the physical, cognitive, and psychosocial factors that may influence the experience, function, and recovery of IPV-related TBI rather than focusing purely on a medical model (Davis, 2014; Farley et al., 2018; Gutman et al., 2004; Jackson et al., 2002; Murray et al., 2016; Roberts & Kim, 2005; St. Ivany et al., 2018a).
Health-care professionals who suspect or are aware of IPV should anticipate a TBI outcome, remaining cognizant that survivors tend to report psychosomatic symptoms of abuse such as headaches, fatigue, nausea, memory issues, cognitive changes, or dizziness rather than the violence itself (Monohan & O’Leary, 1999; St. Ivany & Schminkey, 2016; St. Ivany et al., 2018a, 2018b; Valera et al., 2018). Physical symptoms include headaches, fatigue, sleep disturbances, vertigo, and pain, while cognitive symptoms affect attention, concentration, and executive functioning, suggesting interventions should serve to strengthen the capacity of the survivor to process and interpret information (Corrigan et al., 2003; Jackson et al., 2002; Murray et al., 2016; Valera & Berenbaum, 2003; Valera et al., 2018).
Some studies noted that health professionals should seek education on patterns of brain function and dysfunction, as medical treatment and intervention for TBI may be different and more varied than a psychiatric disorder (Banks, 2007; Farley et al., 2018; Gagnon & DePrince, 2017; Gutman et al., 2004; Roberts & Kim, 2005; Valera & Kucyi, 2017; Valera et al., 2018; Zieman et al., 2017). Recommended psychosocial interventions included providing support and reassurance to survivors and facilitating development of important skills such as problem-solving, self-esteem, and coping strategies (Banks, 2007). The need to reduce the experience of isolation and for education on available resources was also emphasized (Jackson et al., 2002; St. Ivany & Schminkey, 2016). Other educational topics identified included information on the effects of head injuries, monitoring worsening symptoms, and encouraging health-promoting behaviors (Corrigan et al., 2003; Jackson et al., 2002; Murray et al., 2016).
Recommendations for Future Research
The literature highlighted key recommendations for future research that would advance this field of study while also improving frontline approaches to care. Many authors cited the need to establish a reliable, valid, and standardized screening tool to identify TBI in survivors of IPV (Anderson et al., 2015; Baumann et al., 2018; Campbell et al., 2018; Corrigan et al., 2003; Davis, 2014; Goldin et al., 2016; Iverson & Pogoda, 2015; Kwako et al., 2011; Monohan & O’Leary, 1999; St. Ivany & Schminkey, 2016; St. Ivany et al., 2018b; Valera & Berenbaum, 2003). A population-specific tool may inform triage and eventual outcomes for survivors while also contributing more accurate estimates of prevalence to the literature (Davis, 2014). A few studies demonstrated the potential value of neuroimaging in research and diagnosis of IPV-related TBI (Valera & Kucyi, 2017; Valera et al., 2018; Wong et al., 2014). Several called for research on the long-term effects of IPV-related TBI (Amoroso & Iverson, 2017; Corrigan et al., 2003; Foushee, 2017; Gagnon & DePrince, 2017; Hunnicutt et al., 2017; Iverson et al., 2017; Kwako et al., 2011; Plichta, 2004; Stern, 2004; St. Ivany et al., 2018a; Valera & Berenbaum, 2003; Valera et al., 2018; Wong & Mellor, 2014). Evaluation of effectiveness of specific interventions in this population to guide practice was also discussed (Banks, 2007; Baumann et al., 2018; Gutman et al., 2004; Jackson et al., 2002; Wong & Mellor, 2014).
The literature called for researchers to address methodological problems including sample size, population, and generalizability. Authors specifically noted the need for larger population samples and/or inclusion of control groups (Farley et al., 2018; Linton, 2015; Linton & Perrin, 2017; Monohan & O’Leary,1999; Roberts & Kim, 2005; Valera & Berenbaum, 2003; Valera et al., 2018), longitudinal studies (Gagnon & DePrince, 2017; Iverson et al., 2017; Stern, 2004; Wong & Mellor, 2014; Valera et al., 2018), and more reliable information on past incidences of IPV-related TBI than self-report (Linton, 2015; Valera & Berenbaum, 2003).
Further epidemiological study into the incidence of IPV-related TBI was recommended (Baumann et al., 2018; Gagnon & DePrince, 2017; Gutman et al., 2004; St. Ivany & Schminkey, 2016). Documentation of the chronicity and acuity of these injuries is needed (Amoroso & Iverson, 2017; Farley et al., 2018; Foushee, 2017; Gagnon & DePrince, 2017; Hunnicutt et al., 2017; Iverson et al., 2017; Kwako et al., 2011; Linton & Perrin, 2017; St. Ivany et al., 2018a, 2018b; Valera et al., 2018; Wong et al., 2014), as well as inquiry into the causal influences and reasons for blunt trauma (Linton & Kim, 2014). A few authors noted a possible relationship between childhood TBI and subsequent involvement in violent relationships, suggesting further research may provide insight into prevention as well as treatment (Farley et al., 2018; St. Ivany et al., 2018a). A final key recommendation is to increase research grant money to enable future study of IPV-related TBI (Gutman et al., 2004; Roberts & Kim, 2005).
Discussion
The 42 articles sampled in this study provide an excellent foundational understanding of IPV-related TBI. However, with only 22 empirical studies, most of which gathered American data with limited sample size and diversity, the need for a broader understanding and exploration into these intersecting conditions is apparent. Professionals in a number of diverse fields including medicine, occupational therapy, radiological science, and psychotherapy have called attention to this issue and unilaterally agreed that increased awareness and understanding of this population are paramount. Further investigation into prevalence, long-term implications for women’s health and social integration, IPV/TBI-specific interventions, and approaches to prevention are all warranted, particularly with respect to cultural and geographical diversity.
Challenging knowledge synthesis, this field of study is plagued by the abundance of terms for both TBI and IPV used in various contexts, functionally referring to the same group of survivors. Even in this targeted effort to collect all that is known on the topic, extensive hand searching was necessary to account for differences in terminology across time periods and fields of study that would have otherwise been excluded or missed entirely. Professionals and the public are similarly unlikely to have shared language to identify IPV-related TBI or find what limited resources exist. This gap in knowledge and understanding leaves women at risk of continued violence and ongoing exposure to increased physical and psychological trauma as health-care practitioners are without clear protocols, service providers are without a dedicated screening tool, and support personnel remain unaware of the unique challenges faced by brain-injured women survivors of IPV. Further action by researchers and direct service providers, combined with increased social awareness, is critical to developing effective supports.
The limited amount of literature may be due to the sensitive nature of IPV. Survivors may be reluctant to disclose violence due to stigma and fear of retribution making locating this population very difficult. Complicating the issue further, the long-term effects of TBI itself may hinder a survivor’s awareness and insight into her own deficits, preventing her from seeking help or being capable of leaving an abusive situation independently, thereby remaining vulnerable to repeat and/or chronic violence. It is important to note that allowing TBI to go undetected in IPV survivors increases the probability of cumulative effects of repeated injury to the head, face, and neck (Banks, 2007; Campbell et al., 2018; Davis, 2014). Violence-related TBI has poorer outcomes than nonviolence-related TBI (Kim, Colantonio, Dawson, & Bayley, 2013), and repeated injury further compounds negative outcomes making it critical to identify and support survivors at the earliest possible point of contact.
Raising awareness and challenging outdated assumptions among health-care practitioners and society at large around who is likely to suffer a head injury, how that injury will present, and the considerable risk for IPV-related TBI may lead to improved outcomes for women survivors. Even when a woman presents with an obvious injury to the head, face, or neck and is suspected of being involved in IPV, a TBI diagnosis is often not made (Banks, 2007). One explanation offered is that emergency departments are simply not aware that survivors of IPV are at great risk of TBI (Jackson et al., 2002). They tend to see brain injury in young men as a result of high-risk behaviors. Additionally, IPV/TBI survivors may initially present with addiction and/or mental health issues rather than an obvious trauma, as they are nearly twice as likely to have challenges with alcohol use and self-medication with drugs, potentially masking TBI symptoms (WHO, 2017). Professionals are urged not to wrongfully assume that a person presenting with symptoms such as headaches, depression, agitation, and suicidal behavior is suffering from mental illness and requires psychiatric medication (Campbell et al., 2018; Car, 2000; Farley et al., 2018; Smith & Holmes, 2018). In fact, medication carries its own risks in TBI populations, as survivors can be particularly vulnerable to side effects (Jackson et al., 2002). Awareness of this comorbidity can improve screening and avoid misdiagnosis.
Interprofessional workers providing direct services to IPV survivors across the care continuum and researchers are encouraged to advocate for the needs of this vulnerable population. Health-care costs can be prohibitive, and preventing women from gaining access to services and financial dependency is often a mechanism of control for abusers. Increased financial assistance through social programming may encourage or enable more survivors to seek adequate health care (Banks, 2007; Car, 2000). Frontline workers are often the first line of contact for women exposed to IPV and are well positioned to combat the socially derived culture of shame and blame often associated with both IPV and TBI. Advocating for the development of supports sensitive to this population could substantially contribute to improved service provision, reduction of stigma and isolation, and overall progress in psychosocial outcomes.
Screening and assessment remain a priority in the advancement of this field of research and practice. While a number of screening tools were used, discussed, and recommended in this review, development and validation of a specific tool is recommended as a primary directive in future research. An effective tool should take into account unique aspects of this population such as the role of sex and/or gender (e.g., hormones and/or expectations around childcare and employment), impact of socially derived stigma and shame, chronicity and form of violence, implications for personal safety, and contexts of structural violence and intersectional marginalization (Corrigan et al., 2003; Goldin et al., 2016; Iverson & Pogoda, 2015; St. Ivany & Schminkey, 2016; St. Ivany et al., 2018a, 2018b; Valera & Berenbaum, 2003). Additionally, emerging data suggest not enough is currently known about the associated risks and benefits of screening for TBI within an IPV context (Campbell et al., 2018). Current investigation by the authors of this review also revealed the potential risk of increased vulnerability to manipulative partners and potentially non-TBI sensitive legal and child welfare systems. As formal diagnosis is difficult to achieve without expensive testing largely inaccessible to IPV survivors and little-to-no supports for them exist, the immediate benefit of formal TBI identification is not to be assumed. We concur with Campbell and colleagues’ (2018) recommendation that further investigation into the benefits and risks of screening take place, including extensive discussion with survivors, to determine best practices.
Until standardized screening protocols have been implemented, a first step toward identifying TBI in women survivors of IPV may be in simply recognizing a cluster of diffuse symptoms with no originating incident reported, as the survivor may be unwilling to disclose. This review suggests that women exposed to IPV are unlikely or unable to report violence to health-care workers without being directly asked (Campbell et al., 2018; Foushee, 2017; Monohan & O’Leary, 1999; St. Ivany et al., 2018b). Professionals may elucidate a more complete history of trauma by asking if there was ever a time when a patient felt she should have sought medical treatment for head injury but did not (Monohan & O’Leary, 1999; St. Ivany et al., 2018b). It is recommended to bear in mind that many survivors may appear as “normal” leading to the exclusion of a TBI diagnosis (Monohan & O’Leary, 1999; Valera & Berenbaum, 2003). Until we have a more nuanced understanding of the issues at hand, it may be useful to adopt a default suspicion of TBI in the presence of a history of IPV, particularly when coupled with mental health and addictions comorbidities. Specific questions or lines of questioning for frontline use are suggested (Foushee, 2017; Gagnon & DePrince, 2017; Smith & Holmes, 2018).
In addition to documenting the symptoms and experiences of survivors, a few authors have emphasized the value of incorporating more verifiable information from imaging and medical professionals about IPV-related TBI and its effects (Linton & Perrin, 2017; Valera & Berenbaum, 2003; Wong et al., 2014). They, and others, note the challenge in achieving such documentation given the expense required to obtain them, the nature of IPV episodes, and the lack of reporting by survivors. However, by establishing and raising awareness of a physiological basis for the sometimes diffuse somatosensory and emotional symptoms experienced by people with IPV-related TBI, we may minimize stigma and further improve disclosure rates. Empirical studies are needed to generate reliable data on the prevalence, experience, and needs of brain-injured survivors of IPV to be used in health care and community settings and inform policy decisions. As nearly all current data were gathered in the United States, there is particular need for original studies situated in contrasting social, political, and economic contexts, and, in specific, from within a public health-care model. It is possible a publicly funded system of health care and social supports for women survivors of IPV and TBI may be able to develop and implement protocols more quickly and efficiently than one that is not.
Finally, in order to address barriers to adequate health care and support, broader knowledge of currently unexamined contexts is needed. As few authors explore the intersectional complexities experienced by women IPV/TBI survivors of diverse cultural/ethnic backgrounds (Anderson et al., 2015; Campbell et al., 2018; Linton, 2015; Linton & Kim, 2014; Linton & Perin, 2017; Oden, 2000) and fluid gender identities (Baumann et al., 2018; Farley et al., 2018), further research considering the implications of the layers of marginalization experienced by these women is critical. Additionally, capturing this issue beyond shelter populations and emergency rooms is needed and should include police offices, courthouses, mental health centers, or family counseling centers, as well as the dentist office and eye doctor, all of which are important sites of triage for this population (Roberts & Kim, 2005).
An unexpected outcome of this review was the identification of articles calling attention to the importance of the dentistry profession in the detection of IPV survivors and advocating for vigilance in head injury screening, although the potential for TBI was not discussed (Arosarena, Fritsch, Hseuh, Aynehchi, & Haug, 2009; Gwinn, McClane, Shanel-Hogan, & Strack, 2004; Lincoln & Lincoln, 2010; Mishra, 2012; Nelms, Gutmann, Soloman, Dewald, & Campbell, 2009). Dentists routinely examine the head, face, neck, and mouth (HFNM) and may be able to detect physiological signs of IPV, including strangulation, potentially invisible on other medical exams (Arosarena et al., 2009; Lincoln & Lincoln, 2010). Dentists and dental assistants have a unique opportunity for early identification of survivors of IPV seeking routine treatment (Gwinn et al., 2004). Furthermore, forensic odontologists play a significant role in the investigation of violence and abuse and are cited as appropriate multidisciplinary leaders in the training of dentistry in the detection of HFNM injuries (Gwinn et al., 2004; Lincoln & Lincoln, 2010). This review also returned one article outlining a similar role for ophthalmologists detecting injuries to the eye that indicate violence to the head, face, and neck (Beck, Freitag, & Singer, 1996). As these professions emerge as stakeholders in IPV/TBI survivors care, more investigation into best practices is needed.
Conclusion
This review was conducted to update and continue the discussion on the link between IPV and TBI, systematically capturing and synthesizing all of the available current literature exploring this intersection. We also seek to amend the interprofessional approach recommended by the literature by highlighting unique roles and perspectives in this developing field of study. More research is needed including exploration of head injuries and mental health disorder outcomes, efficacy of neuropsychological assessment, strategies for access to appropriate care, establishing premorbid functioning, and the role of dentistry and ophthalmology in identification of IPV-related TBI. Other frontiers for future work include determining what is understood about IPV/TBI among frontline workers in nonmedical settings, motivations/deterrents for disclosure, and strategies for fostering interprofessional alliances in support of survivors across community and health-care settings.
Research generating accurate prevalence figures may lead to a greater understanding of the impact of this issue and inform approaches to detection and care, leading to fewer overall repeated episodes of IPV, appropriate medical intervention, and ongoing support. While development and/or validation of a TBI screening tool, sensitive to the IPV context is critical, further research into the risks and benefits of screening should be undertaken. Cross-sector collaboration is essential to develop appropriate processes and programming for this unique population. It is our hope that with increased research and awareness, fewer women will be at risk of TBI as a result of IPV.
Key Findings
IPV can cause brain injury resulting in fatigue, depression, memory loss, confusion, impaired judgment, and difficulty with tasks that may impair ability to leave an abuser. Presenting with an obvious injury to the head, face, or neck, and suspected IPV does not always lead to a TBI diagnosis. Survivors of IPV-related TBI may initially present with addiction and/or mental health issues rather than an obvious trauma potentially masking TBI symptoms. Disclosure is a key step in the care of this population. Women survivors of IPV are unlikely to report violence to frontline workers unless directly asked. A wide range of prevalence estimates are published based on diverse samples. It is critical that IPV survivors with TBI are identified and supported at the earliest possible point of contact to avoid repetitive trauma to the brain and related outcomes.
Implications for Practice, Policy, and Research
Professionals offering direct services to women survivors of IPV (e.g., police, health care, counseling, shelter staff) should adopt a default suspicion of brain injury in the presence of a history of intimate violence, particularly when coupled with diffuse physical symptoms, somatic complaints, and/or mental health and addictions comorbidities. TBI-specific IPV supports may improve psychosocial outcomes. Investigation into the benefits and risks of screening for IPV-related TBI is needed. Development and/or validation of a TBI screening tool for an IPV context is critical. Empirical studies using larger sample sizes and diverse populations are needed.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The current study was directly supported by funds from the Women’s College Hospital Women’s Xchange Grant program and the Canadian Institutes of Health Research. Neither organization had any practical role in the study whatsoever. Halina (Lin) Haag was also supported by a doctoral fellowship from the Social Sciences and Humanities Research Council of Canada and the Ontario Women's Health Scholar Award from the Ontario Ministry of Health and Long-Term Care and Dr. Angela Colantonio was supported by a research chair in Gender, Work and Health from the Canadian Institutes of Health Research Institute of Gender and Health (grant no. CGW-126580).
