Abstract
Aims:
To assess the relationship between time in range (TIR), extrapolated from self-monitoring of blood glucose (SMBG) measures, and adverse perinatal outcomes in pregnant women with type 1 diabetes (T1D).
Methods:
A retrospective cohort study was conducted, including singleton pregnancies that began antenatal care before 20 weeks of gestation and delivered live newborns without malformations between 2010 and 2019. Glycemic data from SMBG were categorized into TIR (63–140 mg/dL or 3.5–7.8 mmol/L), based on guidelines for real-time continuous glucose monitoring. Extrapolated TIR (eTIR) was defined as the proportion of time spent within the target range and categorized into three intervals: eTIR <50%, eTIR 50%–70%, and eTIR >70%. Clinical characteristics and obstetric outcomes were compared across these intervals. Multivariate logistic regression was used to evaluate the prediction of adverse outcomes, including preeclampsia, nephropathy, cesarean section, preterm birth, macrosomia, large for gestational age (LGA), small for gestational age (SGA), 5-minute Apgar score <7, shoulder dystocia, neonatal respiratory distress, neonatal hypoglycemia, and neonatal intensive care unit (NICU) admission.
Results:
Data from 140 pregnancies were analyzed. Of these, 20% had eTIR <50%, 53.6% had eTIR 50%–70%, and 26.4% had eTIR >70%. Women with eTIR 50%–70% and eTIR >70% were less likely to experience preterm birth (OR: 0.271; 95% CI: 0.094–0.786 and OR: 0.219; 95% CI: 0.058–0.826), neonatal respiratory distress (OR: 0.341; 95% CI: 0.124–0.936 and OR: 0.122; 95% CI: 0.029–0.516), and LGA infants (OR: 0.246; 95% CI: 0.084–0.719 and OR: 0.115; 95% CI: 0.028–0.469) compared with women with eTIR <50%.
Conclusions:
Higher eTIR values were associated with a reduced risk of preterm birth, neonatal respiratory distress, and LGA infants. For pregnant women with T1D, achieving an eTIR above 50% was sufficient to decrease the risk of these adverse outcomes, highlighting the importance of glucose control even in challenging circumstances.
Keywords
Introduction
Diabetes is one of the main medical conditions that complicate women’s health during pregnancy, and women with type 1 diabetes (T1D) have worse outcomes when compared with pregnant women without the disease.1–4 The risk of a large for gestational age (LGA) infant is approximately 50%, and these children in adulthood have a predisposition to obesity, type 2 diabetes, and cardiovascular disease.2,5,6 However, achieving ideal glycemic levels to reduce the risks of adverse outcomes during pregnancy remains one of the greatest challenges, especially in the population using complex insulin therapy regimens.4,6 Self-monitoring of blood glucose (SMBG) and glycated hemoglobin (HbA1C) levels are usually used to measure and monitor glycemic levels, despite they do not capture daily glucose fluctuations.4,7–10 On the contrary, continuous glucose monitoring system (CGMS) offers the potential to measure interstitial glucose continuously and provides detailed data of how glycemic patterns and glucose variability may influence pregnancy outcomes.3,7,11,12 Across pregnancy, the goal is to spend more time within glucose target levels, called time in range (TIR) and less time above and below range, besides reducing glycemic variability.8,11 Currently, the American Diabetes Association (ADA) recommends achieving more than 70% of TIR (63–140 mg/dL or 3.5–7.8 mmol/L), less than 25% of time above range (TAR) and less than 5% of time below range (TBR).11,13 Two of the main studies about CGMS and TIR in pregnant population with T1D showed an association between lower TIR and LGA infants, and glycemic targets achieved only at the end of the second trimester to third trimester.3,6 Nonetheless, CGMS is not an option guaranteed by health insurance and public health systems in general, and SMBG remains the main method for monitoring blood glucose levels in most patients with T1D.10,12 Therefore, this study aimed to assess the association between TIR extrapolated from SMBG (eTIR) and adverse perinatal outcomes in pregnant patients with T1D.
Materials and Methods
Study design and participant population
A retrospective cohort study was performed of women with T1D who received prenatal care and delivered at a tertiary hospital (Hospital das Clinicas da Faculdade de Medicina da Universidade de São Paulo [HC-FMUSP]), between 2010 and 2019, in Brazil. Included patients had a singleton pregnancy and available glucose profile data (a minimum of 70% of the glucose data, for at least 1 week in each trimester) as well as obstetric outcomes recorded in medical records. Patients with fetal malformations, pregnancy loss before 20 weeks of gestation, or who began antenatal care after 20 weeks of gestation were excluded. This study was approved by the Institutional Ethics and Research Committee of our hospital (approval number: 60202122.5.0000.0068).
Diabetes management
In accordance with our institutional protocol, 14 all patients attended antenatal visits every 1 to 2 weeks. These women performed daily SMBG, taking seven measurements per day (before and 1 h after breakfast, lunch, dinner, and overnight 3 AM). The target glucose levels set as follows: fasting glucose below 95 mg/dL (5.3 mmol/L), premeal and overnight glucose below 100 mg/dL (5.5 mmol/L), and postmeal glucose below 140 mg/dL (7.8 mmol/L). Throughout the pregnancy, the medical team monitored capillary blood glucose levels, reinforced dietary guidelines, and adjusted insulin doses to meet glycemic targets. HbA1c levels were measured at the start of antenatal care and in each trimester. Delivery was planned between 37 and 40 weeks of gestation, provided there were no maternal or fetal complications.
Glycemic data
Glycemic data obtained through SMBG during antenatal care were recorded in Microsoft Access software. Extrapolated TIR (eTIR) was defined as the proportion of time a patient spent within the target glucose range for pregnancy (63–140 mg/dL or 3.5–7.8 mmol/L). It was calculated as follows: (number of readings within target range/total number of readings) × 100 = eTIR. The data were retrospectively categorized into three groups: eTIR <50%, eTIR50-70%, and eTIR >70%. All available glycemic data from patient records were considered.
Obstetric and neonatal variables
Both physical and electronic medical records were reviewed. LGA and small for gestational age (SGA) were defined as birth weights above the 90th percentile and below the 10th percentile, respectively, for the neonate’s gestational age and sex, based on the Fenton growth chart. 15 The following data were collected for each patient: maternal age, duration of diabetes, ethnicity, parity, prepregnancy body mass index (BMI), weight gain during pregnancy, history of hypertension or nephropathy, preeclampsia, worsening or onset of nephropathy, use of an insulin pump and mode of delivery. Neonatal health outcomes were also recorded, including gestational age at birth, preterm delivery (<37 weeks), birthweight, macrosomia (>4000 g), sex, shoulder dystocia, hypoglycemia, respiratory distress, and admission to the neonatal intensive care unit (NICU) for more than 24 h.
Statistical analysis
Patients were divided into three groups: eTIR <50%, eTIR 50%–70%, and eTIR >70%. Data are presented as absolute and relative frequencies or as means (standard deviations). Categorical independent variables were analyzed using the chi-squared or Fisher’s exact tests. The non-parametric Mann–Whitney U test was used to compare groups for quantitative independent variables that did not have a normal distribution. The prediction for adverse obstetric and neonatal outcomes was studied using multivariate logistic regression, including clinical and laboratory variables for each outcome of interest: preeclampsia, worsening or new onset nephropathy, cesarean section, preterm birth, macrosomia, LGA infant, SGA infant, 5 min Apgar score <7, shoulder dystocia, neonatal respiratory distress, neonatal hypoglycemia, and NICU admission. For this analysis, we included the three categories of eTIR (eTIR <50%, eTIR 50%–70% and eTIR >70%) as independent variables, along with clinical factors that could be associated with each outcome. A significance level of 5% (P < 0.05) was considered statistically significant. All analyses were conducted using Statistical Package for the Social Sciences (SPSS) version 29.0 for Windows (Armonk, NY: IBM Corp).
Data and resource availability
The datasets analyzed in the current study are available from the corresponding author upon reasonable request.
Results
Between 2010 and 2019, 140 pregnant women with T1D were included with at least 1 week episode with more than 70% of the glucose profile per trimester. The dataset comprised a total of 142,997 glycemic records. Women were divided according to time spent within the target range, into three categories: 28 (20.0%) in the eTIR <50% group, 75 (53.6%) in the eTIR 50%–70% group, and 37 (26.4%) in the eTIR >70% group (Fig. 1). There were no significant differences in maternal characteristics, except for the HbA1C in the second and third trimester between eTIR <50% vs. eTIR >70% groups (P = 0.002 and P = 0.005, respectively) (Table 1). Approximately 30% of the patients in the eTIR >70% used insulin pumps, with no significant difference among groups. In relation to maternal and neonatal outcomes (Table 2), there was a statistically significant difference in preterm birth and respiratory distress, both were more prevalent in the eTIR <50% group, showing a positive linear association across progressive eTIR categories. Prematurity was mainly related to premature rupture of ovular membranes (11%), preterm labor (29%), and fetal distress (26%), with an average gestational age at birth of 35 weeks. In the eTIR <50% group, 7.1% and 57.1% of the women presented SGA and LGA infants, respectively. On the other hand, almost 22% of women had SGA infants in the eTIR >70% group.
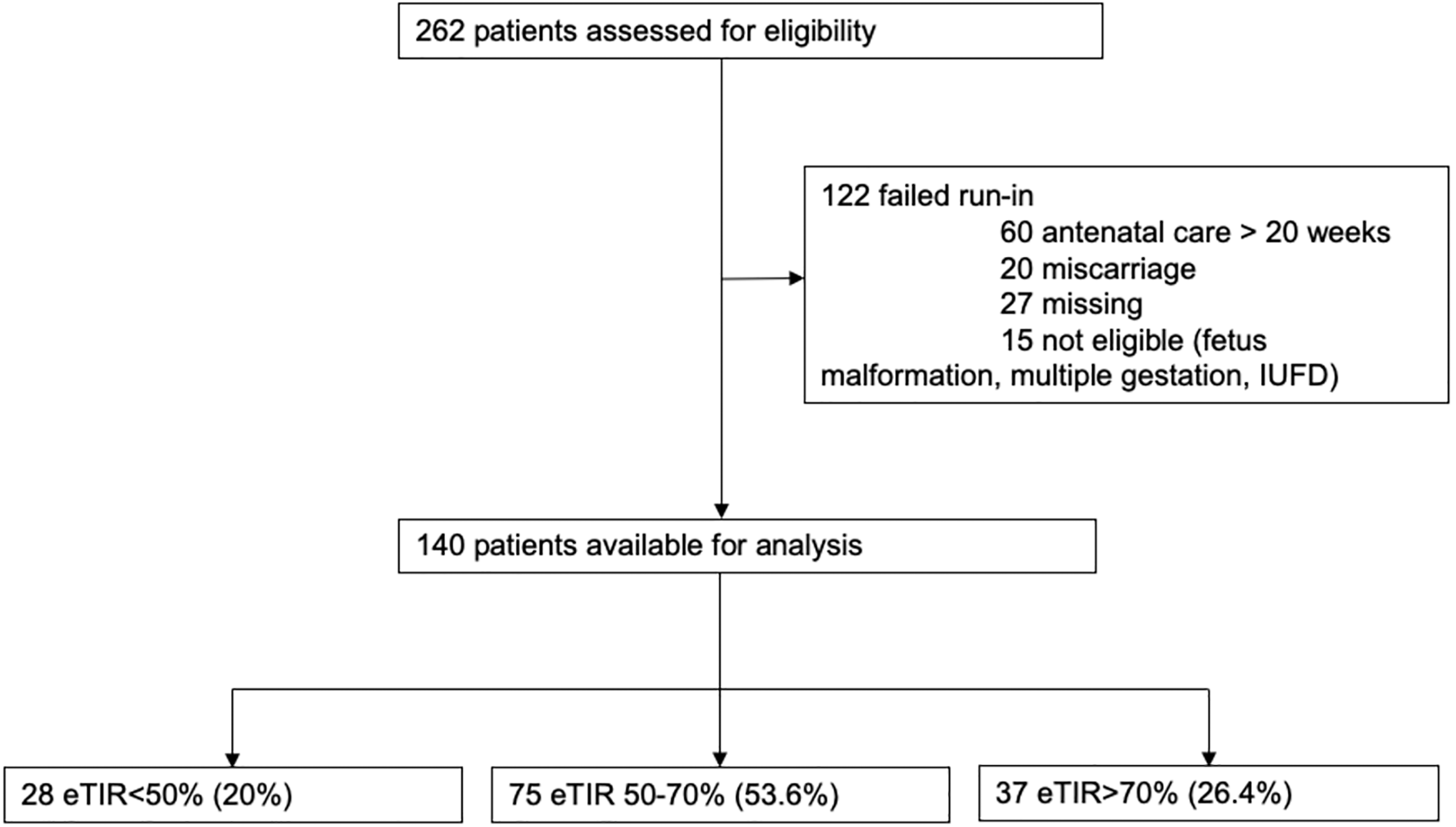
Flowchart of participant selection. IUFD, intrauterine fetal death; SGA, small for gestational age; AGA, adequate for gestational age; LGA, large for gestational age; eTIR, extrapolated time in range.
Baseline Characteristics of Pregnant Women with Type 1 Diabetes According to Extrapolated Time in Range Intervals Groups
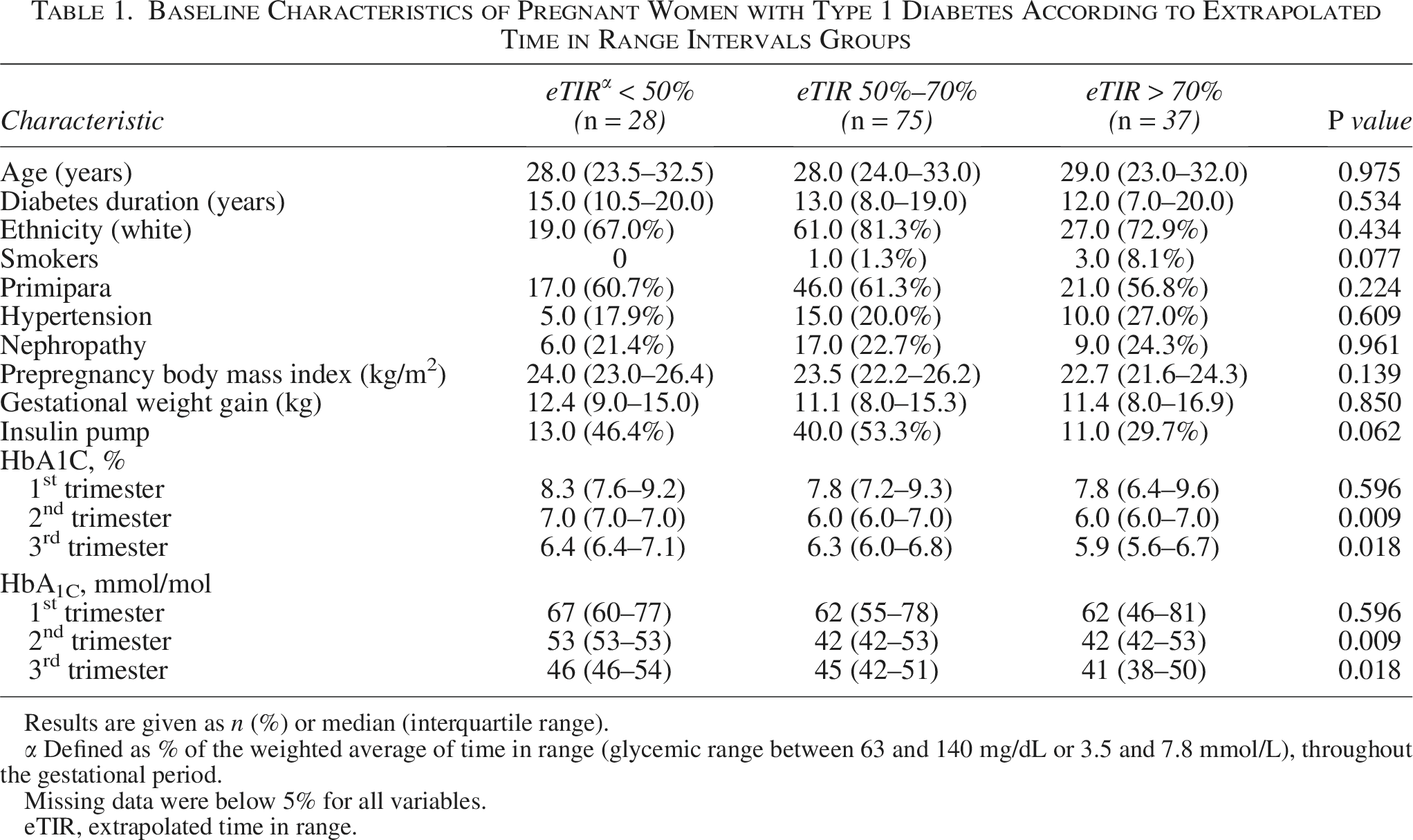
Results are given as n (%) or median (interquartile range).
α Defined as % of the weighted average of time in range (glycemic range between 63 and 140 mg/dL or 3.5 and 7.8 mmol/L), throughout the gestational period.
Missing data were below 5% for all variables.
eTIR, extrapolated time in range.
Maternal and Neonatal Outcomes in Pregnant Women with Type 1 Diabetes According to Extrapolated Time in Range Intervals Groups
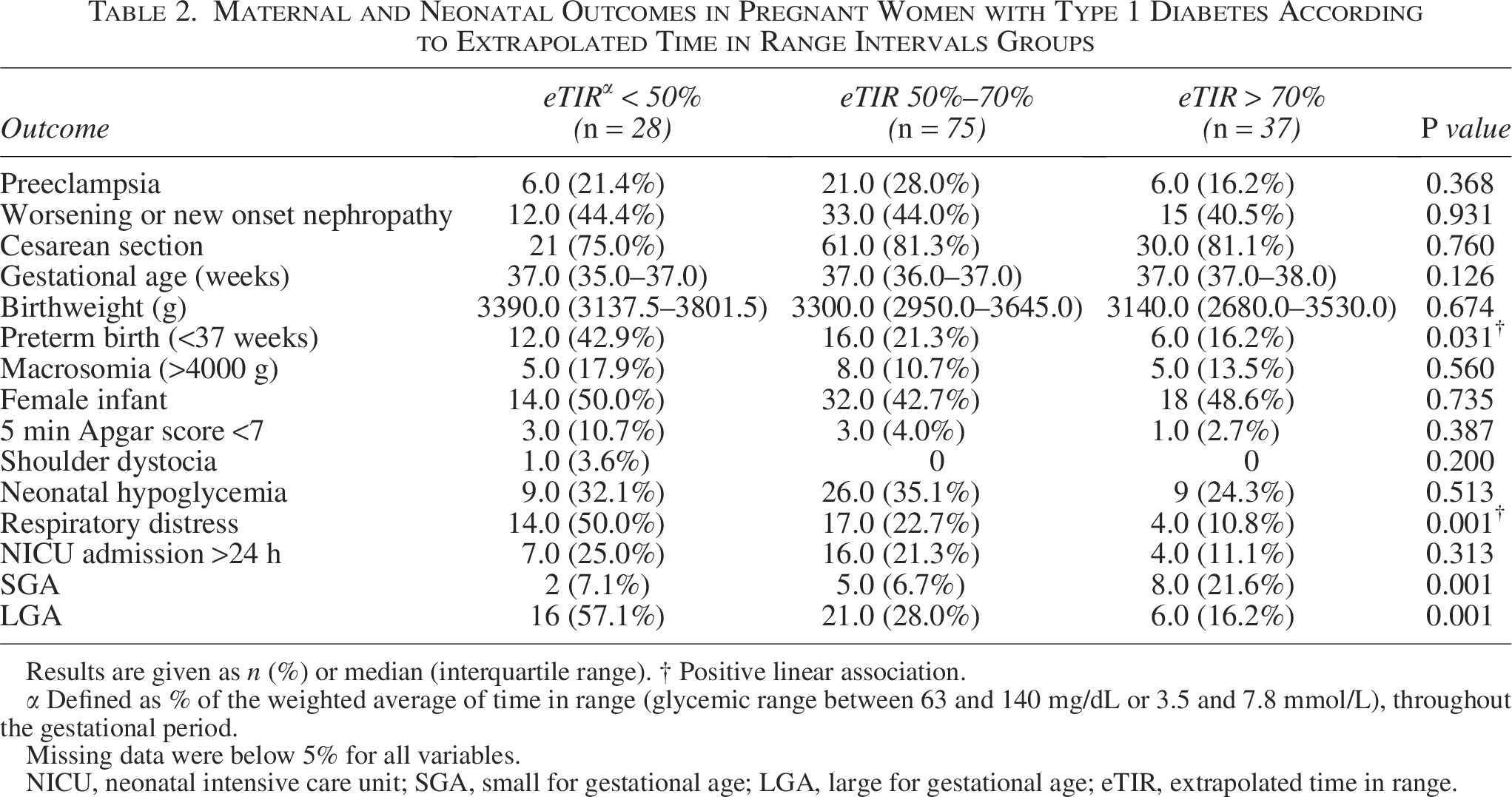
Results are given as n (%) or median (interquartile range). † Positive linear association.
α Defined as % of the weighted average of time in range (glycemic range between 63 and 140 mg/dL or 3.5 and 7.8 mmol/L), throughout the gestational period.
Missing data were below 5% for all variables.
NICU, neonatal intensive care unit; SGA, small for gestational age; LGA, large for gestational age; eTIR, extrapolated time in range.
For premature birth, there was a significant linear association (P = 0.018), with a higher frequency of prematurity as lower the eTIR category, but no significant difference was identified between groups after Bonferroni adjustment. At multivariate analysis and logistic regression, eTIR was an independent risk factor for this event. Compared with pregnant women with eTIR <50%, eTIR 50%–70% was associated with a reduction of 73% in prematurity (OR: 0.271; 95% CI: 0.094–0.786) and eTIR >70% was associated with a reduction of 78% in this event (OR: 0.219; 95% CI: 0.058–0.826) (Table 3).
Multivariate Logistic Regression Analysis of Predictor Variables for Preterm Birth, Neonatal Respiratory Distress, Small for Gestational Age Infant, and Large for Gestational Age Infant in Pregnancies Complicated by Type 1 Diabetes
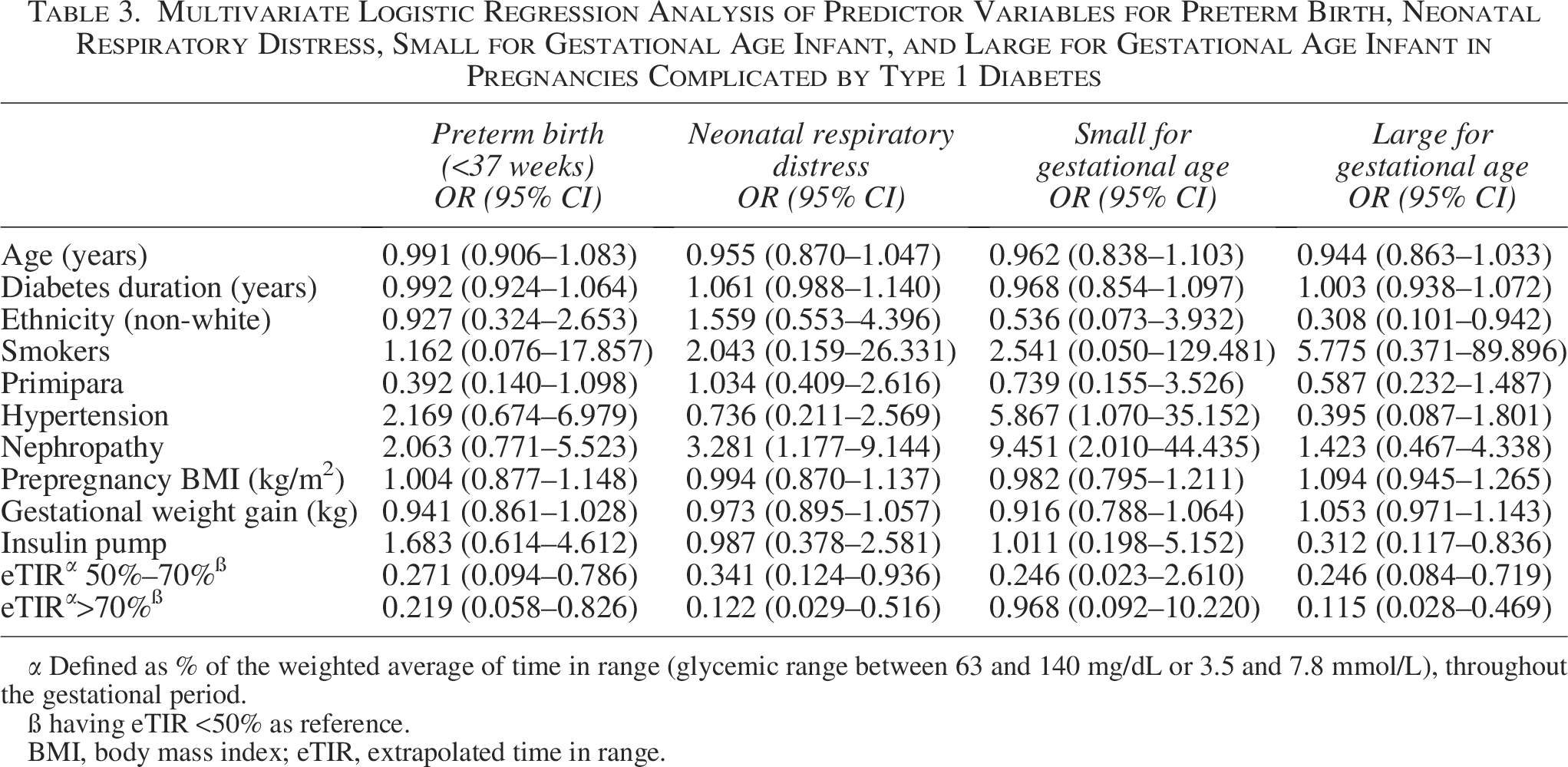

α Defined as % of the weighted average of time in range (glycemic range between 63 and 140 mg/dL or 3.5 and 7.8 mmol/L), throughout the gestational period.
ß having eTIR <50% as reference.
BMI, body mass index; eTIR, extrapolated time in range.
Neonatal respiratory distress also showed a significant linear association (P < 0.001) with higher rates as lower the eTIR category and, in the pairwise comparison, it was more prevalent in the eTIR <50% group than in the eTIR 50%–70% group (50.0% vs. 22.7%, P = 0.021) and the eTIR >70% group (50.0% vs. 10.8%, P = 0.001). However, no significant difference was identified between the eTIR 50%–70% and eTIR >70% groups after Bonferroni adjustment. At multivariate analysis and logistic regression, eTIR and a history of previous nephropathy were independently associated with the outcome of neonatal respiratory distress (Table 3). The presence of nephropathy was associated with higher rates of this outcome by 3.28 times (OR: 3.28; 95% CI: 1.117–9.144). With regard to eTIR, when compared with pregnant women who had an eTIR <50%, those who had an eTIR 50%–70% had an association with a 66% lower risk of neonatal respiratory distress (OR: 0.341; 95% CI: 0.124–0.936), and those who had eTIR >70% were associated with 88% lower risk of this outcome (OR: 0.122; 95% CI: 0.029–0.516).
For the outcome of SGA infants there was no statistically significant difference between groups in the pairwise evaluation after Bonferroni adjustment. SGA outcome was independently associated with the history of hypertension and nephropathy, using adequate for gestational age (AGA) infants as a reference. Extrapolated TIR was not associated with SGA in the logistic regression (Table 3). Nonetheless, a history of hypertension was associated with a 5.86-fold increased risk of SGA (OR: 5.867; 95% CI: 1.070–35.152) and the history of nephropathy was associated with a 9-fold increased risk of this outcome (OR: 9.451; 95% CI: 2.010–44.435).
Finally, regarding LGA infants, there was a statistically higher frequency within the eTIR <50% group than in the eTIR 50%–70% group (57.1% vs. 28.0%, P = 0.018) and eTIR >70% (57.1% vs. 16.2%, P = 0.002), with no significant difference between the last two groups in the adjusted pairwise comparison. At multivariate analysis and logistic regression, using the group of AGA infants as a reference, the eTIR, ethnicity, and the use of insulin pump were independent factors for the outcome (Table 3). Non-White pregnant women had a 69% lower chance of LGA infants (OR: 0.308; 95% CI: 0.101–0.942). Patients who used insulin pump had a 69% lower chance of this outcome (OR: 0.312; 95% CI: 0.117–0.836). Compared with those with eTIR <50%, those who remained with eTIR 50%–70% presented a 75% lower rate of LGA infants (OR: 0.246; 95% CI: 0.084–0.719), as well who remained with eTIR >70% that presented an 89% lower frequency of this outcome (OR: 0.115; 95% CI: 0.028–0.469).
Discussion
Despite the great focus in the literature about the importance of TIR on the risk of excessive fetal growth, it is known that hyperglycemia during pregnancy is also associated with other perinatal complications. Our study is one of the first to investigate the association between eTIR intervals and the occurrence of other outcomes, such as prematurity and neonatal respiratory distress, complications that are typically associated with T1D during pregnancy.
Prematurity was present in 24% of our sample, being consistent with other studies in the literature that presented prematurity rates of 28%–38%.3,7 Increased eTIR has proven to be associated with lower rates of prematurity, with rates reduced more than 70% when patients achieved eTIR above 50%. In Sobhani et al.’s 16 retrospective cohort study, they found that TIR was linked to perinatal outcomes in 91 pregnant women with T1D using CGMS. Overall, 32% of the sample evolved with preterm birth, with a mean gestational age at birth of 35 weeks, 41% spontaneously and 59% associated with other causes, mainly preeclampsia. TIR remained between 37% and 47% in patients with this outcome. Moreover, it was observed that a 5% increase in TIR in the 12th and 20th week was associated with a 60% and 27% reduction in the risk of prematurity, respectively (OR: 0.40; 95% CI: 0.20–0.79 and OR: 0.73; 95% CI: 0.61–0.87, respectively). Our study showed that eTIR above 50% was associated with a reduced risk of prematurity by more than 70%, which could lead us to believe that even slightly better TIR intervals would be enough to improve certain perinatal conditions.
Along with prematurity, neonatal respiratory distress was also associated with eTIR, in addition to a history of previous nephropathy. Our rate of neonatal respiratory distress was 25%, mainly within the group of LGA and SGA fetuses. Again, it is noted in our results that eTIR intervals above 50% already was association with a significant reduction in this outcome. In our study, no significant association was observed between eTIR and other obstetric outcomes, such as preeclampsia, admission of the newborn to the NICU, and neonatal hypoglycemia. In contrast, Fishel et al. 17 compared obstetric and neonatal outcomes in 78 pregnant women with pregestational diabetes with TIR ≤ or >70%. All pregnant women used CGMS, and the main outcomes evaluated were LGA fetus, admission to NICU, use of intravenous glucose, neonatal respiratory distress, and hypertensive syndromes during pregnancy. Newborns of pregnant women with TIR ≤70% were more susceptible to admission to NICU (P = 0.035), receiving intravenous glucose (P = 0.005), presenting neonatal respiratory distress (P = 0.012), and developing hypertensive syndromes (P = 0.04). The association between preeclampsia and TIR was also observed by Sobhani et al., 16 with preeclampsia occurring in 29% of their sample, a frequency similar to our study (23.7%). In addition, they reported a 45% reduction (OR: 0.55; 95% CI: 0.30–0.99) in the likelihood of this outcome for every 5% increase in TIR at the 12th week.
In our results, there was no association between SGA and eTIR, but a history of chronic arterial hypertension and/or previous nephropathy were strong factors associated with the outcome, being present in 20% to 25% of the patients. Elucidating the worsening of nephropathy remains a challenge, since objective criteria are not clearly defined, making it very difficult to differentiate between the diagnosis of preeclampsia or worsening of previous nephropathy within this population. 18 In a meta-analysis conducted by Relph et al., 19 including 56 cohort studies with 12,819 pregnant women with diabetes, the presence of nephropathy increased the outcome of preeclampsia by 10 times (OR: 10.76; 95% CI: 6.43–17.99), by 4.5 times the risk of prematurity before 37 weeks (OR: 4.48; 95% CI: 3.40–5.92), and by 16 times the risk of SGA infants (OR: 16.89; 95% CI: 7.07–40.37). Interestingly, it was observed that when eTIR is within the desired glycemic range (≥70%), there was an increased frequency of SGA infants. This may suggest that once the hyperglycemia factor for excessive fetal growth is eliminated, placental factors and those related to pre-existing vasculopathy become more prominent, limiting fetal growth.20,21 In a cohort study carried out by Bacon et al., 21 157 pregnant women with T1D from the CONCEPTT study were analyzed for birth weight and placental function, based on angiogenic factors—placental growth factor (PlGF) and soluble fms tyrosine kinase type 1 (sFlt-1). It was observed that patients with low PlGF (<100 pg/mL) or high sFlt-1/PlGF ratio (>85) and suboptimal glycemic control with TAR > 30% (≥140 mg/dL) or HbA1C > 6.5% had newborns with lower birth weights and, despite not presenting criteria for growth restriction or SGA fetus, still presented potential fetal growth restriction, suggesting that additional obstetric surveillance may be useful in pregnant women with inadequate glycemic control (TAR > 30% or HbA1C > 6.5%) even with apparently normal fetal growth, since this may indicate deficient placental function.
The use of insulin pump was identified as a protective factor for LGA infants, with a 69% reduction in patients using the device. Secondary analyses, both from the Swedish study and the CONCEPTT study indicated that use of insulin pump did not affect LGA outcomes.22,23 However, the latter study revealed higher rates of hypertensive syndromes, neonatal hypoglycemia, and NICU admissions among users of the device. The association between TIR and LGA infants is well-established, where TIR acts as a predictor for this outcome. The two main studies involving pregnant women with T1D and the association of TIR measured by CGMS showed that these patients tend to increase their TIR as pregnancy progresses, thereby decreasing the likelihood of LGA infants.3,7 Our group had previously demonstrated that eTIR from SMBG measurements was associated with a reduction of LGA infants by 2.3% (OR: 0.977; 95% CI: 0.955–0.998) for every 1% increase in eTIR in the third trimester, and for every 1% increase in extrapolated TAR during the third trimester, the risk of having an LGA infant increased by 4.6% (OR: 1.046; 95% CI: 1.018–1.075). 24 In the present study, eTIR >50% was associated with a 75% reduction in the incidence of LGA infant.
Our study has both strengths and limitations. Firstly, the retrospective design limited data collection to what was already available in both physical and electronic medical records. In addition, glucose excursions during the first hour postprandially and overnight were not captured by the eTIR used, which limits direct comparisons. It is possible that a greater proportion of patients in the present cohort achieved an eTIR above 70% than it would be observed in a population using CGM (without automated insulin delivery).
One of the key strengths of our study is its focus on multiple obstetric outcomes beyond fetal weight. This is particularly significant because, while other studies have validated TIR extrapolated from SMGB measurements in both pregnant and non-pregnant populations, they primarily focused on LGA infants in pregnant women. In addition, our findings may help patients understand that even suboptimal TIR levels, below the recommended 70%, could already provide benefits in terms of obstetric outcomes, even when based on extrapolated SMBG data. Furthermore, our study includes a substantial number of patients from a single center, all of whom were managed by a cohesive team of obstetricians with extensive experience in caring for pregnant women with diabetes.
Conclusions
Considering the well-established link between TIR measured by CGMS and the occurrence of LGA infants, we aimed to adapt this concept to our local context and evaluate TIR data measured by SMBG and its impact on other perinatal outcomes. According to our findings, it is observed that when eTIR exceeds 50%, there is already an association with reduced rates of prematurity, neonatal respiratory distress, and LGA infants. This suggests that this threshold may be sufficient to reduce adverse perinatal outcomes, particularly to women facing challenges to achieve TIR above 70%.
Authors’ Contributions
E.A.M.S.: Conceptualization, data curation, methodology, writing—original draft; T.A.Z.: Software, data curation; C.F.P.: Resources, data curation; R.P.V.F.: Validation, writing—review and editing; Supervision; R.A.C.: Methodology, formal analysis, writing—review and editing.
Footnotes
Funding Information
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit-sectors.
Authors’ Relationships and Activities
The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Disclosure Statement
None.
