Abstract
The growing role of the justice system in the care of individuals with mental illness has led to concerns about access to adequate and timely mental health services, particularly for persons with severe mental illness whose behaviors increase their risk of justice involvement. This study investigated the perceptions of people found not criminally responsible, their loved ones, peer support workers, and other mental health professionals and managers regarding access to effective and relevant mental health services. Semi-structured interviews and focus groups were conducted with 25 participants, and data analyses were carried out according using thematic analysis. The findings highlighted how past experiences of stigma, trauma, inefficiency, and discrimination within a hospital-centric system influenced service users’ and caregivers’ ability to seek and engage with care. Current access mechanisms, such as police intervention and emergency room visits, were described as unacceptable and often viewed as options of last resort. Consequently, service users frequently entered the healthcare system only when their needs had escalated in complexity, making them difficult to address within the scope of standard clinical practice. Implications for policy and service organization are discussed.
In many countries, the justice system plays an important role in leveraging access to care for people with mental illness (Jansman-Hart et al., 2011; Sheridan Rains et al., 2020). In Canada, this is particularly evident in cases where people are found not criminally responsible due to a mental disorder, meaning they committed a crime while “incapable of appreciating the nature and quality of the act […] or of knowing that it was wrong” (Canadian Criminal Code, 1992, section 16). While most people found not criminally responsible had prior contact with mental health services (Crocker et al., 2018), research highlights major service gaps, with many receiving only fragmented or inconsistent care in the year before their offense (Leclair et al., 2022a).
Using a verdict of not criminally responsible as a de facto diversion pathway carries significant consequences. Admission to forensic mental health services amplifies stigma (Markham, 2024; Vorstenbosch et al., 2025), creating enduring structural barriers to employment and housing (Salem et al., 2016). Forensic care is also costly, with treatment costs in Canada nearly five times higher than those of general mental health services (Jacobs et al., 2016). Some scholars argue that growing investments in forensic services divert funding from general mental healthcare, further restricting access (Seto et al., 2001).
The concern that mental healthcare systems often fail to meet the needs of individuals with severe mental illnesses is not unique to Canada; it is a global issue. The World Health Organization (WHO) reports that, worldwide, a significant portion of individuals requiring mental health services lack access to effective, affordable, and quality care. For instance, approximately 70% of people with psychosis in high-income countries do not receive mental health services (World Health Organization, 2021). In Canada, despite universal healthcare, many people with mental illness report unmet mental health needs (Corscadden et al., 2019). A recent review on access to care in Canada highlights that a primary obstacle is the lack of clear information about available services, limiting individuals’ ability to seek help (Moroz et al., 2020). Stigma is another major barrier, as actual or anticipated negative experiences within the healthcare system—such as discriminatory attitudes and therapeutic pessimism from providers—deter many from accessing care (Henderson et al., 2014).
These challenges are amplified for people with severe mental illness who are at risk of justice involvement, as they face the compounding effects of both psychiatric and criminal justice-related stigma (Roy et al., 2020b). As a result, this population experiences greater care disruption (Abbott et al., 2017) and stigma and discrimination from mental health workers (Vorstenbosch et al., 2025). For example, examining administrative health data of 1,014 people found not criminally responsible, Leclair and colleagues found that although 71% of individuals had at least one contact with mental health services in the year preceding their offense, fewer than half received consistent care. Many service users, for example, were discharged from psychiatric hospitalization without a follow-up appointment, resulting in significant gaps in therapeutic support and care continuity (Leclair et al., 2022a). Health services providers also report feeling pressured to use the criminal justice system as a lever to access specialized and integrated care for their clients (Roy et al., 2020a). This pressure is also felt by people in close support roles (friends, family members, or others) who are unable to access mental healthcare through other means (Larose-Hébert, 2020). This highlights the need to examine how and why the mental healthcare system fails to meet, in the community, the clinical needs of several people with severe mental illness and who display behaviors that are perceived as impulsive, disruptive, or aggressive.
Access to Care
Several models have been developed to conceptualize access to care, with differing perspectives on whether it is primarily a system attribute or a user-driven process. Donabedian (1973) viewed access as a property of healthcare resources that mediates the link between service availability and utilization. Penchansky and Thomas (1981) emphasized the “fit” between system characteristics (e.g., provider availability, service quality) and user needs. Synthesizing these perspectives, Lévesque et al. (2013) define access not merely as initial contact but as the ability to receive appropriate, timely, and continuous care. Their framework proposes that access results from the interaction between five healthcare system characteristics (approachability, acceptability, availability, affordability, and appropriateness) and five corresponding user abilities (ability to perceive, seek, reach, pay, and engage).
Approachability refers to the transparency of services and how easily they can be identified by those in need. It is shaped by service visibility, outreach, and health literacy. Users must also recognize their own health needs. Acceptability involves cultural, social, and professional norms that determine whether services are seen as appropriate or desirable. Discriminatory practices or a lack of culturally safe care can make services unacceptable, especially for marginalized groups, including those with justice involvement. Users’ ability to seek care is influenced by cultural beliefs, autonomy, and trust in the system. Availability refers to the physical and organizational accessibility of services, including location, hours, and appointment systems. Users’ ability to reach services depends on transportation, mobility, and social support. Affordability includes both direct (e.g., fees, medications) and indirect costs (e.g., time lost from work, travel expenses). The ability to pay includes financial resources and supports, such as paid sick leave. Finally, appropriateness refers to how well services meet users’ needs in terms of technical quality, relational care, coordination, and continuity. It also includes the system's capacity to address complex needs with specialized, trauma-informed, and culturally appropriate approaches. Users’ ability to engage in care depends on their knowledge of available services, social support, and empowerment in healthcare decisions. Lévesque et al.'s (2013) framework captures the entire user experience, including initial contact, sustained care, and the quality and adequacy of services received.
Objectives
This study examines perceptions and experiences of access to mental health services by people with severe mental illness and disruptive behaviors. Guided by Lévesque et al.'s (2013) framework, which conceptualizes access as the interaction between system characteristics and user abilities, this study includes perspectives of both mental health workers and decision-makers, who shape service availability and delivery, and service users and families, who navigate and experience these services.
Methods
Study Design and Positionality
We used a descriptive qualitative design, which seeks to provide a comprehensive summary of participants’ experiences using their own language with minimal researcher interpretation (Sandelowski, 2010). This design, often applied in health research (Neergard et al., 2009), captures experiences in everyday terms and is particularly suited to exploring complex service access issues. Our study was guided by the patient-centered model of access to care (Lévesque et al., 2013), which framed the interview guide (see Supplemental material) and informed the interpretation of the findings.
Our study was grounded in a constructivist epistemology, which acknowledges that knowledge is co-constructed between researchers and participants (Charmaz, 2006). This approach aligns with the descriptive qualitative design, emphasizing participants’ lived experiences while recognizing the influence of researchers’ interpretations in shaping findings. The constructivist perspective guided our data collection and analysis, ensuring that themes remained rooted in participants’ narratives while allowing space for contextual meaning-making.
Ethics approval was obtained from CIUSSS de l'Ouest-de-l'Île-de-Montréal, Université de Montréal, and Université du Québec en Outaouais. We report the findings following the Consolidated criteria for reporting qualitative research (COREQ; Tong et al., 2007).
First author positionality statement
I am a white, upper-class academic woman, dually trained in psychology and public health. I have conducted research in forensic mental health research for over 10 years and am affiliated at Philippe-Pinel Institute, a forensic mental health hospital. This institutional connection may have positioned me as an “insider” to some participants, particularly mental health workers. While my personal experiences with chronic illness have shaped my understanding of access to care, my experiences do not parallel the realities of those in secure care, who face loss of freedom and layers of stigma. I remain committed to approaching this work with humility.
Recruitment
Participants included service users who were found not criminally responsible in the prior 10 years, family caregivers of persons with justice involvement or found not criminally responsible, peer support workers, public/community health practitioners, and administrators/decision-makers. Service users were recruited from Philippe-Pinel Institute, Douglas Mental Health Institute, and a community organization that provides services and supervised housing for people found not criminally responsible. Philippe-Pinel Institute is the only forensic hospital in the province of Québec, Canada, and Douglas Institute is a large general mental health university hospital with dedicated forensic beds.
A researcher presented the research to service user committees and care teams. Potential participants either volunteered directly to the researcher or were approached by the care team to seek permission for the research team to contact them and present the project individually. Other participants were recruited via existing networks and emails to associations. Participants had to be over 18 years of age, able to hold a conversation in French or English, and–in the case of mental health workers and decision-makers–have been working for more than a year in their current role. Participants were purposely selected based on their ability to provide insights into different aspects of access to care, ensuring their contributions were relevant to the dimensions of access described by Lévesque et al. (2013) and reflected a variety of expertise.
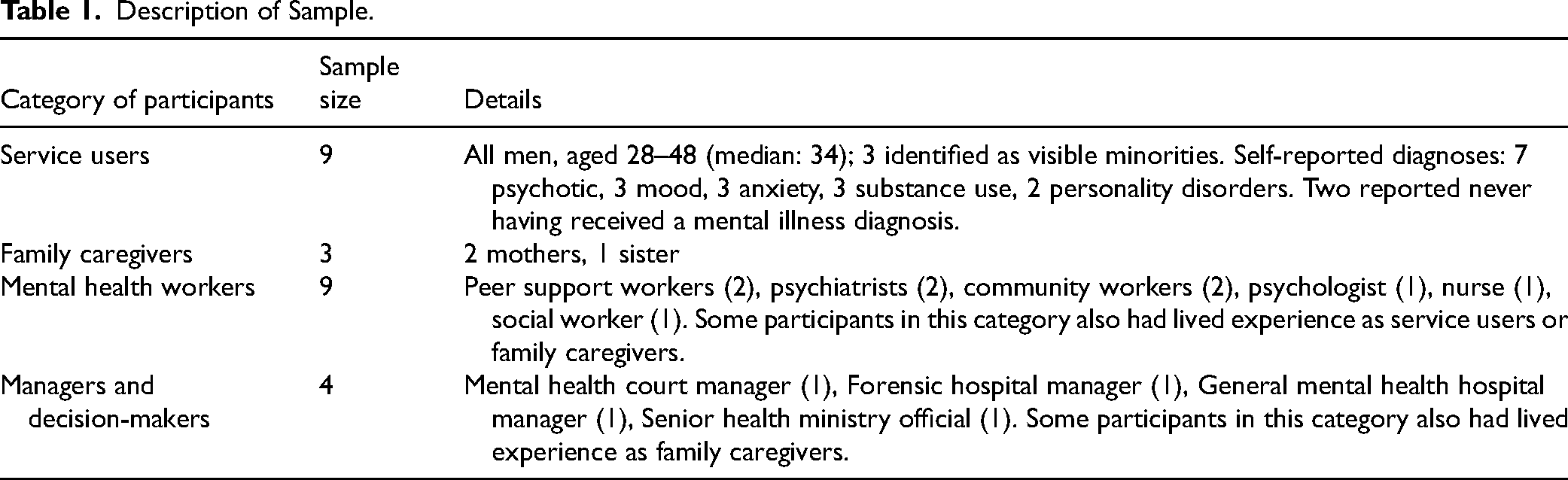
The sample size was determined using the information power model, which suggests that the number of participants should be guided by factors such as the study's aims, the specificity of the sample, the depth of dialogue generated during interviews, and the chosen analytical approach (Malterud et al., 2016). Given the study's objectives, the well-defined participant groups (people found not criminally responsible, their loved ones, and professionals working with them), the study's strong theoretical foundation, and the expertise of the interviewers in forensic mental health, we aimed for an estimated sample of 20 to 30 participants, including 8–10 service users. In total, 25 participants were interviewed (see Table 1 for sample description).
Description of Sample.
Data Collection
We used both one-to-one semi-structured interviews and focus groups to capture individual experiences and group dynamics. We used primarily focus groups with mental health workers and managers to construct shared and contrasting perspectives, identifying both convergences and divergences in their attitudes, beliefs, and experiences. Individual interviews were used for participants whose schedules conflicted with group sessions or who preferred a more private setting to share sensitive experiences. Participants had the choice of a focus group or a one-to-one interview. Notably, individual interviews were used with service users to give the time, space, and confidentiality to share their journey.
Individual semi-structured interviews (40–60 min) were conducted in private rooms at the hospitals or community organization. Questions included: “Can you tell me about the healthcare you received before coming here? How was your experience?” Three distinct 90-min focus groups on videoconference were held, moderated by the first author, with groups consisting of (1) mental health workers, (2) health and justice system managers, and (3) family caregivers, peer support workers, and community workers. Additionally, three individual semi-structured interviews were conducted with a senior decision-maker, a family caregiver, and a mental health worker. All interviews were recorded, transcribed, and assigned pseudonyms chosen by participants. All but two interviews were in French, and selected quotations were translated.
Data Analysis
After familiarizing ourselves with the data through transcription, relistening, and multiple readings, we applied thematic analysis as outlined by Paillé and Mucchielli (2012). Using inductive open coding, data from one-to-one interviews and focus groups were synthesized to develop low-inference themes (i.e., full sentences closely reflecting participants’ words with no or minimal interpretation). Two analysts independently coded a third (n = 8) of the transcripts, resolving discrepancies through consensus. Themes were reviewed for repetition, overlap, contradiction, and complementarity across participants and groups. After open coding, we classified these codes into the five dimensions of access from Lévesque et al.'s (2013) framework: approachability, acceptability, availability, affordability, and appropriateness. Thus, while the initial coding was inductive, the development of the thematic tree was structured by the theoretical framework through an iterative process discussed during author consensus meetings. Theoretical memos were written after each focus group or interview, as well as after each coding round. Memos were used to capture reflections on emerging patterns, document analytic decisions, and record insights that informed theme development (Paillé & Mucchielli, 2012). Reflexive team debriefings were held regularly to review the memos and discuss emerging findings.
Results
Thematic analysis identified six overarching themes reflecting barriers to accessing mental health care. These include (1) tensions in representations of access, highlighting the disconnect between service availability and meaningful care; (2) symptoms, denial, and fear, which prevent individuals from seeking help in the first episode of severe mental illness; (3) inadequate responses during high-risk periods, where crisis services are often unavailable or escalate distress; (4) hospitals as sites of trauma, stigma, and loss of dignity, where care is frequently perceived as punitive; (5) rigid and fragmented services, which limit access and disrupt continuity of care; and (6) limited evolution in mental health knowledge and practice, where outdated models, gaps in expertise, and overreliance on coercion hinder recovery-oriented care. Barriers are summarized in Figure 1.
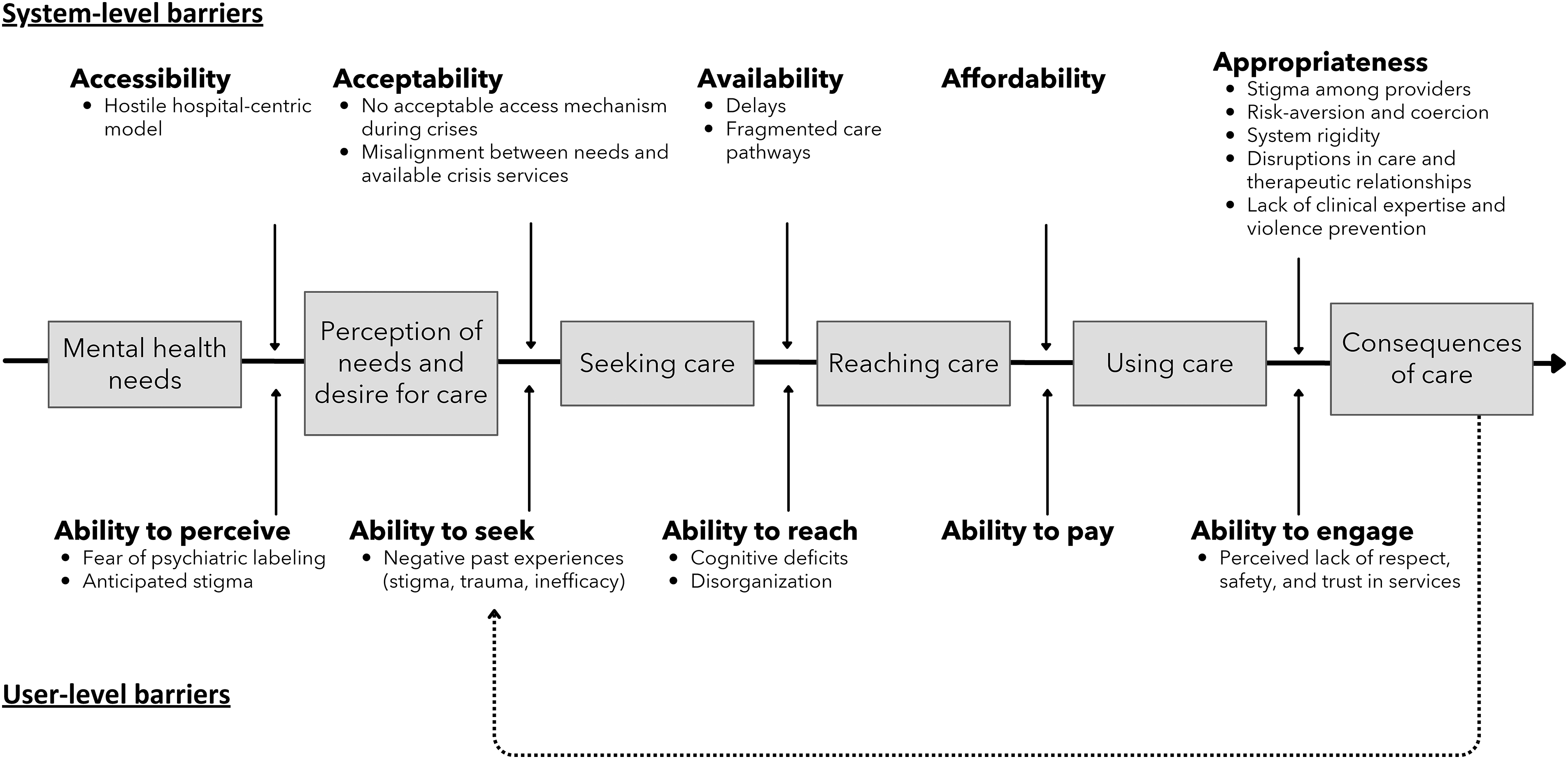
Systemic and User-Level Barriers to Accessing Care, Mapped to Lévesque et al.'s (2013) Patient-Centered Model.
Tensions in Representations of Access to Care
Although participants were not explicitly asked to define access, many did. Two conflicting perspectives emerged: access as initiating contact with services versus access as receiving the appropriate care.
Participants with lived experience dismissed the notion that access is merely about service availability: “Access to services is not just saying, ‘I’m opening an office with a silver plate, Doctor so-and-so here.’ That's not it.” (Pogo, peer support worker) Instead, they emphasized that access means “get[ting] the services they needed” (Fée clochette, mother).
In contrast, some professionals, particularly decision-makers, viewed access as time to initial contact. They rarely considered acceptability or appropriateness, shifting responsibility entirely to the service user: “There is no lack of access. […] What we have is that patients don't wish to consult, don't want to consult” (Steve, decision-maker). Because services are construed as widely available based on populational wait-time statistics, the fact that many people do not seek help is met with a sense of incomprehension, leading to frustration and impasse.
Symptoms, Denial, and Fear Creating Barriers in a First Episode
Many service users struggled to seek care due to a lack of insight, stigma, and fear of losing autonomy. Early symptoms were often unrecognized or dismissed, while concerns about being labeled “mentally ill” deterred help-seeking. Family members frequently noticed warning signs first but faced challenges in getting their loved one to engage with services. Additionally, fears of hospitalization and its long-term consequences reinforced avoidance of mental health care.
Lack of insight: “I didn’t think I was sick”
Service users identified active symptoms, substance use, and lack of insight as primary barriers to seeking care, preventing them from recognizing their need for care: “I didn’t think I was sick, I didn’t think I needed help” (Mario, service user). Instead, they described feeling that “I was exactly where I was supposed to be” (Swan, service user).
Loved ones often recognized the need for healthcare before service users did, but their attempts to intervene were not always effective: “Everyone was telling me that I wasn’t normal, but I really thought that they were the ones who weren’t normal” (Swan, service user). For others, the absence of family support during this period of denial made accessing care even more difficult: “[I did not have] family there to say, ‘We know Jack, we want to help him, we’re taking him to the hospital because he needs help.’ […] I didn’t have all that.” (Jack, service user)
Fear of Stigma and Autonomy Loss: “Getting a Kid to Set Foot on the Grounds of the Asylum…Good Luck”
Many participants avoided seeking mental health care due to stigma and fears of losing control over their lives. Some avoided treatment for fear of being labeled “mentally ill” or “being linked to a history of mental illness” (X, service user). Anticipating stigma, many preferred not to disclose their symptoms to professionals and loved ones: “It was difficult for me to talk about [hearing voices] because I didn’t feel secure. I was afraid to talk about it, afraid of being pushed away.” (Syndicat, service user)
For some, fear went beyond social stigma to concerns about coercion: “I wanted to get help. I wanted to receive care, but I found it upsetting to lose my freedom.” (Mario, service user). Participants worried about involuntary hospitalizations, loss of rights, and how a psychiatric record might “affect the life you lead outside”, including housing, jobs, “my hunting license, my driver's license” (X, service user).
Others emphasized that, compared to incarceration, hospitalization has no clear end date: “once you come here […] they try to keep you here” (Brandon, service user). In addition, they felt that “being around mad people, you feel like you’re going mad yourself (Ryan, service user).” These fears led some to seek alternative treatments, such as acupuncture or naturopathy, in an effort to avoid formal psychiatric services.
Inadequate Response During High-risk Periods
Participants highlighted that during a crisis, resources meant to provide immediate support were either unavailable or inappropriate. Attempts to seek help often resulted in delays, rejection, or responses that escalated rather than de-escalated distress. Many were reluctant to call the police, fearing it would lead to trauma rather than support.
Delayed Care Creating a Window of Risk: “This is Where We Put Ourselves at Risk, All of Us”
Service users and loved ones expressed frustration that care had been inaccessible until they had reached a breaking point: “As long as you’re not a threat to society or yourself, they send you back out [and] they tell you, ‘We’ll call you in three months to give you an appointment.’” (Sam, sister) This service gap between deteriorating health and intervention creates a “window where violent acts may occur” (Morpheus, psychiatrist).
Inaccessible Crisis Resources: “They Hung up on Him”
When people with mental illness or their families sought crisis services, they were often unavailable or inappropriate. A mother described how her son was “blacklisted” from a hotline: When he called the crisis center, after three minutes, they hung up the phone. Because he was “occupying the lines too much”. It doesn't work! In his anxiety and symptoms, he clearly says: “Can you be my rock for the next 15 minutes because I don't want to commit suicide?” What more do you have to say to ask for help? (Fée clochette, mother)
Fear and Avoidance of Police-based Responses: “No Safe Place to Call”
Loved ones hesitate to seek help during high-risk periods, fearing that doing so might endanger themselves, their relative, and their relationship. If we feel that our loved one is in crisis, really in trouble, at risk of acting out, there is no safe place to call without the police headlights coming on to the street […] without going to the emergency room for four hours and then coming back and not having more services.” (Brack, mother)
Many reported that calling the police felt inappropriate and dangerous, risking further trauma or victimization: “I did not want to send the police. It felt completely out of step to send the police to people who are in crisis and who are afraid” (Pito, peer support worker). For many, past negative experiences with emergency responses reinforced their reluctance to seek help, leading them to handle high-risk situations on their own rather than risk an inadequate or harmful intervention.
Hospitals as Sites of Trauma, Stigma, and Loss of Dignity
Rather than fostering recovery, many participants described hospital environments as distressing, restrictive, and dehumanizing—“an asylum” (Pogo, peer support worker). Service users reported that hospitalization itself often became a source of trauma, with rigid policies prioritizing risk management over well-being. Beyond the physical environment, interactions with healthcare professionals often felt cold and interrogative, reducing individuals to symptoms and compliance rather than recognizing their broader needs. Many experienced stigma, dismissal, and disbelief, further eroding trust in the system and reinforcing a sense of powerlessness and exclusion.
Hospital-induced Distress: “It Makes You Crazy Even if You’re Not Crazy to Begin With”
Service users described hospitals as overwhelming and restrictive, where constant noise, surveillance, and confinement worsened their mental health. Peer support workers suggested hospitalization itself often becomes a source of trauma. Participants attribute this harm to a risk-averse, rigid hospital culture, where risk management takes priority over well-being. A mother recounted the resistance she faced from staff when advocating for service users to engage in basic daily activities: It took me some real charm. We weren’t even leaving the institute… Just taking them from a secure floor […] to an environment where they could make some toasts, and everything was dangerous. (Fée clochette, mother)
Systemic Dehumanization: “Not Just a Person Who Has Symptoms”
Although some service users had a good relationship with specific mental health workers (especially in forensic mental health), nearly all shared that they experienced several healthcare interactions that felt cold, procedural, and interrogative—“like I’m at the police station” (Pogo, peer support worker), reducing people to their symptoms and treatment plans. Nobody talks to me like I'm a human… it's the interrogation: ‘Did you take your pills? How much? Did you eat? Did you sleep?’. (Pogo, peer support worker)
This narrow biomedical focus often neglects essential aspects of personhood, including emotional connection, spirituality, sexuality, and dignity. Some felt that treatment focused on superficial markers of clinical improvement rather than genuine quality of life: “They’ll medicate him until he smiles. Even if it's not an intelligent smile, he’ll have one.” (Sam, sister). Ultimately, this fixation on symptom control left service users questioning the purpose of treatment: “Insight is all well and good. But once it's done, what's left?” (Mario).
Dismissed and Discredited: “You’re Faking, get out”
Service users frequently reported feeling ignored, discredited, or treated with suspicion by healthcare professionals. Many described situations where they were denied care outright, reinforcing distrust in the system: I went to ten different hospitals. They’d say, ‘You’re fine, leave,’ and call the police. (Jack, service user) They didn’t trust what I was saying. I knew the pain wasn’t anxiety, but they kept telling me it was. (Syndicat, usager) Maybe because when you’re a professional, you’ve seen a lot of people. You start to understand that there are prototypes, different styles of people. They might see me as something I don’t necessarily want to be anymore. (Comeback Kid, service user)
Rigid and Fragmented Services
Despite the need for flexible, integrated care, participants described the mental health system as rigid, fragmented, and difficult to navigate. Services operate in silos, with strict eligibility criteria that exclude those with complex needs. Continuity of care is often disrupted, forcing service users to “start over” repeatedly. In some cases, judicial measures become the only pathway to treatment, highlighting the system's failure to provide accessible, coordinated care.
Fragmented and Arbitrary Access: “You'll Never Know Which Door to Knock On”
Participants emphasized how rigid program-based structures create barriers, often related to diagnoses, causing “a lot of suffering” (Jack, service user). For those who have complex histories, “in the end, they have so many diagnoses that there are no more programs for them” (Fée clochette, mother). As a result, accessing care did not felt like a structured process but rather a matter of “luck,” depending on the goodwill of a worker who “decides to take charge of the case” (Brack, mother).
Providers admitted that even they struggled to navigate the system, describing it as “pure hell” (Ophélie, social worker). You call one place, it's the wrong number. You call another place, you don't have the right postal code. […] If you knock on the wrong door, unfortunately, you'll never know which one to knock on. (Laure, manager)
Participants also described how the very symptoms (e.g., impairments, memory loss) make it difficult to access services designed for them: “The system doesn’t work because the person isn’t fit to receive that service” (Sam, sister). Examples of system rigidity include strict schedules, inflexibility regarding lateness, overreliance on technology for reminders, and inaccessible service locations. While many blamed the system's inflexibility, others framed the issue as a lack of patient engagement, citing challenges related to “what they are and the behaviors they have” (Steve, decision-maker). From this perspective, non-compliance, missed appointments, and difficulty following instructions were construed as service user limitations rather than system failures to accommodate diverse needs.
Disrupted Continuity of Care: “I Must Have Had 18 Psychiatrists in My Life, No Joke”
Service users emphasized the importance of “familiar faces” (Pogo, support worker), noting that frequent staff turnover disrupted engagement and trust: “I’m forced to tell my life story every time. When you change [team] often, it makes you shut down because you’re tired.” (Mario, service user) Mental health workers acknowledged how lack of relational continuity can lead to impersonal care: He becomes a number, this gentleman. You take over a file, you've never seen that patient. He was supposed to show up, he didn't… So you close the file. (Pearl, psychologist)
Criminalization as a Pathway to Care: “Let's Make This a Legal Issue”
Participants widely recognized that judicial measures often become a lever for access. It's so complicated to find the right path into the health system that we end up saying, ‘Let's make this a legal issue. At least there’ll be a first episode of care, and they can figure out where to send them after'” (Laure, manager)
However, this strategy was rarely effective. Because of the disconnect between the healthcare and justice systems (“driving on completely separate highways,” Le Délinquant, manager), those seeking care through the justice system often cycled through courts, police custody, and short-term interventions without sustained support.
Limited Evolution in Mental Health Knowledge and Practice
Despite advancements in mental health research, many participants felt that services remain anchored in outdated models, relying on rigid, institutionalized approaches rather than evidence-based recovery practices. The system prioritizes risk management over person-centered care, often defaulting to coercion due to gaps in clinical expertise—particularly in managing behavioral risks and violence prevention.
Outdated Knowledge and Reactive Approaches: “We're Just Health Professionals Here”
Participants described how mental health care continues to rely on traditional frameworks, prioritizing stability and compliance over autonomy and recovery. A key concern was the lack of clinical expertise in violence prevention and risk management in general mental health settings. Many workers felt unprepared to handle behavioral crises, particularly those related to aggression: “We're just health professionals here—we're not the police, and we're not prison guards either” (Morpheus, psychiatrist). Although risk assessment tools are widely used, there is little guidance on how to act on the findings, leaving clinicians without clear intervention strategies: “Ok, I have a rating—but what do I do after?” (Iris, nurse). The absence of specialized training in violence prevention and de-escalation not only contributes to reactive, coercive hospital-based practices but also shapes the inadequate crisis responses described in Theme 3. Without alternatives, services default to police interventions or forced treatment rather than proactive, recovery-oriented care.
Coercion as a Substitute for Expertise: “The Injection was Given, but at What Cost?”
Due to the lack of preventive and de-escalation strategies, coercion often becomes the default response to service users in distress. Many described the system as “custodial” (Mario, service user), where individuals have little say in their care and care is experienced as punitive rather than therapeutic. Even when service users understood why medication was necessary, the absence of communication deepened their sense of mistrust and disempowerment: “She didn't even tell me what it was. She just came in and kacha! in my leg with an injection.” (Brandon, usager)
Beyond individual experiences, participants noted that coercive measures often fail to produce lasting engagement, instead reinforcing a revolving-door cycle between hospitalization, legal intervention, and crisis-driven care. We bring back the patient, completely disorganized. He arrives at the ER for his injection, and I apologize for the term but - he stirs up shit, and the police becomes involved and so on. And whoop, we start another cycle. […] Yeah, the injection was given, but at what cost? (Le Délinquant, manager)
Beyond Control and Compliance: “Recovery is Possible for Everyone”
While models emphasizing recovery, strengths-based interventions, and harm reduction are increasingly recognized, participants described widespread reluctance to integrate recovery-based models into everyday clinical practice: “Recovery doesn’t come with the healthcare system—it's hard to make the two work together.” (Pito, peer support worker)
Some felt that recovery was seen as an unrealistic goal for those with complex needs, forensic backgrounds, or long-term institutionalization, reinforcing a static, custodial approach rather. Instead, they called for a shift toward recovery-oriented care that fosters autonomy and participation in society, rather than one that views service users as permanently institutionalized. I often hear, “Recovery is interesting, but not in tertiary care, not for institutionalized clients, not for the elderly.” It's as if it's not possible for everyone, while recovery is possible for everyone. (Didi, community worker)
Discussion
While the link between mental illness and violence is generally weak, system and policy factors—such as housing instability, poverty, and barriers to mental health care—can shape risk (Crocker et al., 2023). The findings of the present study illustrate how multiple dimensions of access (Lévesque et al., 2013) contribute to crisis-driven pathways into forensic care. Approachability was hindered by a lack of transparency regarding available services, leaving many service users and families uncertain about where to turn for help. Acceptability was compromised by stigma, coercion, and negative provider attitudes, making services undesirable or distressing to engage with. Availability gaps were evident in long wait times and the absence of crisis alternatives beyond police intervention. Affordability, while less frequently discussed, was a concern for some participants, particularly regarding the hidden costs of accessing care, such as time and transportation. Finally, appropriateness was a critical issue, with participants describing a system ill-equipped to meet their needs, particularly for those with complex conditions requiring coordinated, long-term, and trauma-informed care. While decision-makers emphasized service availability and individual responsibility, service users and families highlighted structural barriers, unacceptable access mechanisms, and the inadequacy of existing services to meet complex needs. This misalignment may contribute to policies that prioritize system efficiency over meaningful engagement, reinforcing the reliance on coercive and crisis-driven interventions rather than proactive, recovery-oriented care.
Consistent with past research (Jina-Pettersen, 2022), the findings reveal how stigma, trauma, inefficiency, and discrimination within a hospital-centric system limit access to care. Structural stigma, embedded in restrictive policies, risk-averse practices, and resource disparities (Corrigan et al., 2014; Livingston, 2020), creates systemic disadvantages that reduce service acceptability, leaving users and families to navigate fragmented services with minimal support. These systemic failures contribute to disengagement, reinforcing negative perceptions of mental health services and delaying help-seeking. These factors often make services unacceptable, prompting users and families to seek alternative, more compassionate strategies. Crisis services, such as police intervention or emergency rooms, are considered only when other strategies have failed and the person has experienced severe decompensation, by which point multiple crises—including relationship breakdowns and housing loss—may have already occurred (Larose-Hébert, 2020).
As a result, service users enter the healthcare system with highly complex needs that are challenging to address with current clinical and scientific knowledge and resources. The healthcare system's rigidity (e.g., fragmented program-based approaches, which multiples eligibility criteria, contributes to disengagement, and disrupts continuity of care) is ill-equipped to meet those needs. Participants described interactions with mental health services as dehumanizing and punitive, with risk management prioritized over person-centered care. The absence of relational continuity, shared decision-making, and proactive engagement strategies reflects a broader pattern of structural stigma within mental health services, contributing to distrust and disengagement. Coercive strategies, such as restraints, confinement, and mandatory treatment orders, are more likely to be used in this context, reinforcing the negative appraisal of services (Stanhope et al., 2009), reducing service user engagement (Brekke et al., 2023), exacerbating trauma and mental illness (Lohmann et al., 2024), and creating barriers to recovery (Aragonés-Calleja & Sánchez-Martínez, 2024).
Implications
Our findings highlight the need to reform crisis access mechanisms. Police involvement in mental health crises deters help seeking, heightens risk, and disrupts continuity of care by diverting people to emergency rooms outside their usual care setting (Saleh et al., 2018). Despite the creation of Crisis Intervention Teams, research shows they have not significantly reduced arrests and use of force, or improved crisis resolutions (Marcus & Stergiopoulos, 2022). Civilian mental health response teams offer a promising alternative by deploying trained crisis workers instead of police officers to de-escalate situations and connect individuals to care (Marcus & Stergiopoulos, 2022). These teams operate through partnerships between community organizations and health services, often incorporating peer support workers to improve engagement (see justmentalhealth.ca for a live repertoire of programs).
Addressing repeated negative interactions between service users and healthcare providers is also critical. Anti-stigma training should prioritize direct social contact with people with lived experience, as this approach has been shows to reduce stereotypes and improve adherence to recovery-oriented care (Knaak et al., 2016). However, meaningful organizational change requires organizational readiness for disruption and value alignment across partners (Sukhera & Knaak, 2022). A key strategy is the integration of lived experience in service design, delivery and evaluation (Mental Health Commission of Canada, 2015).
Shifting from hospital-centered to community-based care may reduce stigma and hostility for first-time mental health service users. The Trieste model, with its “Open door—No restraint” approach, offers a potential blueprint, emphasizing transdiagnostic, flexible, and family-centered care with minimal inpatient care (Sashidharan, 2022). It centers on 24/7 community mental health centers staffed by multidisciplinary teams working closely with general hospital psychiatric units, supported housing, and social enterprises (Mezzina, 2014). This model fosters strong therapeutic partnerships, empowerment, and social network enhancement, achieving an antipsychotic medication compliance rate of 75%, nearly double that of other systems (Palcic et al., 2011).
For service users with high and complex needs, mobile teams providing in-home support could offer the flexibility, responsiveness, and coordination needed. Implementing such teams could help prevent violence and reduce justice system involvement, provided they effectively identify at-risk individuals. One potential model is Forensic Assertive Community Treatment (FACT), which delivers intensive, multidisciplinary, community-based support for justice-involved individuals (Goulet et al., 2021). However, its current use is limited to those already involved with the justice system. Expanding such interventions based on service users’ needs rather than legal status is crucial. For those with lower needs, a navigator could greatly improve access and continuity of care. Nurse navigators, a model already common in chronic disease management, could be expanded to mental health care to provide personalized support in navigating complex systems, coordinating care, and improving service continuity. Navigators act as a single point of contact, reducing the burden on service users and their families.
Limitations
This study was conducted in two psychiatric hospital units—one forensic and one general—as well as in a community organization providing supervised housing. As a result, participants had relatively high levels of need and complex histories. It is possible that this focus may have limited the inclusion of perspectives from individuals with less complex needs. Another limitation is that all service users interviewed were men, which may not fully reflect gender-specific experiences. Women in forensic services are more likely to have prior emergency room visits (Leclair et al., 2022b), complex trauma histories (de Vogel et al., 2025), and greater suicidality (Nicholls et al., 2015). These differences may shape access, engagement, and interventions appropriateness. Future research should explore gender-specific barriers to inform tailored interventions.
Conclusion
Structural stigma against people with severe mental illness within the healthcare system creates and upholds significant barriers to accessing adequate care, recover, and thrive. This is especially true for people who have behaviors that are perceived as dangerous, disruptive, or violent and that are thus at risk of justice involvement and entry into the forensic mental health system. There is a need to transition towards community-based care and prioritize the lived experience of service users through evidence-based approaches. Reducing structural stigma in mental healthcare is a crucial step in decreasing the justice involvement of people with severe mental illness.
Supplemental Material
sj-docx-1-fmh-10.1177_14999013251353794 - Supplemental material for “No Safe Place to Call”: Perspectives and Experiences of Access to Mental Health Services by People Found not Criminally Responsible on Account of a Mental Disorder
Supplemental material, sj-docx-1-fmh-10.1177_14999013251353794 for “No Safe Place to Call”: Perspectives and Experiences of Access to Mental Health Services by People Found not Criminally Responsible on Account of a Mental Disorder by Marichelle Leclair, Laurence Roy, Jeanne Gobeil Langlois, Arianne Imbeault, Audrey-Anne Dumais Michaud and Anne G. Crocker in International Journal of Forensic Mental Health
Footnotes
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Support from the Canadian Institutes of Health Research as a Vanier doctoral fellowship for Leclair; support from the Social Sciences and Humanities Research Council of Canada as a doctoral fellowship for Imbeault and as a Canada Research Chair for Crocker; support from the Fonds de recherche du Québec as a salary award for Roy; Support from the International Centre for Comparative Criminology for data collection.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
