Abstract
Aims
To summarize methods used to account for antihyperglycemic medication changes in randomized controlled trials evaluating the effect of dietary and physical activity interventions on glycemia among adults with diabetes.
Methods
Using studies included in two recently published systematic reviews of randomized controlled trials examining the glycemic effects of dietary and physical activity interventions, we evaluated how each study accounted for antihyperglycemic medication changes. Data were analyzed using summary statistics, stratified by the type of intervention studied, and each was assigned a score from 0 to 6 reflecting the strength of medication controls employed.
Results
We evaluated 22 physical activity focused and 27 dietary focused articles. Our scoring system yielded a mean concurrent medication adjustment score of 3.9/6 for the physical activity studies and a score of 1.7/6 (p < 0.001) for the dietary studies.
Conclusions
We found that randomized controlled trials included in recent systematic reviews of physical activity and dietary interventions did not robustly account or control for changes in antihyperglycemic medications, with physical activity interventions doing so more robustly than dietary interventions. This is a threat to the validity of study findings, as observed glycemic changes may in fact be attributable to imbalances in concurrent medication adjustments between groups.
Background
Randomized controlled trials (RCTs) evaluating the effectiveness of antihyperglycemic medications often employ standardized protocols for handling other antihyperglycemic medications during the study. These protocols allow researchers to attribute observed changes in glycemia to the agent under study. 1 They may include restricting the changes that clinicians can make to study participants’ medication regimens, providing stringent stepwise protocols by which medication up-titration must proceed, and/or conducting a priori prespecified subgroup analyses that exclude patients who had changes to their medication regimens during the study. These measures are important to provide concrete evidence that the observed changes in glycemia are, in fact, attributable to the intervention under study and not due to concurrent changes to other medications that have similar impacts on the outcome of interest.
RCTs testing the impact of changes in diet quality and physical activity levels on glycemia, however, are not bound by requirements from regulatory bodies like Health Canada, 2 and therefore they may not plan as stringent measures for dealing with concomitant changes in patient medications during the trial. Therefore, patients may have significant changes in their antihyperglycemic medication regimen concurrent with the intervention under study. The effects of dietary and physical activity interventions may work synergistically with concurrent antihyperglycemic medication changes, making it difficult to determine which factor produced the largest effect. There is not a clear standard for investigators to adhere to for accounting for these changes in dietary and physical activity interventions. Our objective was to summarize the methods used to account for concurrent medication changes in recent RCTs evaluating the effect of dietary and physical activity interventions on glycemia among adults with diabetes.
Methods
We found two of the most recent published systematic reviews of RCTs examining the effects of dietary and physical activity interventions (separately) on glycemia among adults with diabetes.3,4 We located the full-text manuscripts for all included primary studies in each of these systematic reviews (n = 28 for dietary studies, n = 37 physical activity studies). Studies were excluded from our analysis if they did not measure and report A1C at both baseline and following the intervention resulting in 27 dietary intervention studies and 22 physical activity intervention studies. We then reviewed each manuscript in detail, extracting data pertinent to our research question - how antihyperglycemic medication changes were accounted for or tracked in the study. This question was broken down into five unique questions including: Were antihyperglycemic medications assessed at baseline? Were changes in antihyperglycemic medication restricted? Were changes in antihyperglycemic medications reported? Was a standard protocol for antihyperglycemic medication adjustment used? Was a sensitivity analysis conducted to examine the effectiveness among those who did not have any concurrent medication changes?
We then created a scoring system, the concurrent medication adjustment score, reflecting the strength of medication controls employed by each study. Scores could range from 0 (weakest) to 6 (strongest) as follows:
Box 1: Concurrent medication adjustment score.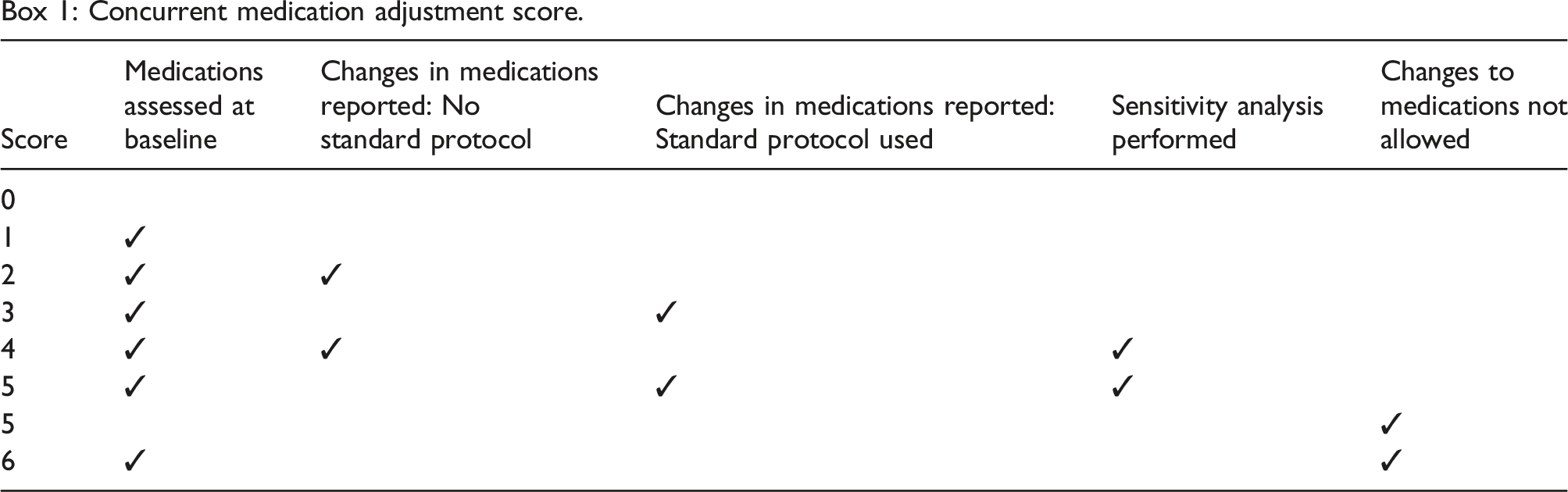
Data extraction was performed in duplicate by two independent reviewers (DBC & TD), with discrepancies resolved by the principal investigator (DJTC). Data were analyzed using summary statistics, stratified by the type of intervention under study (physical activity or diet). We then assessed differences in mean concurrent medication adjustment score between the two types of interventions, using the Student’s t-test.
Results
From the review focused on physical activity interventions, 4 we extracted data from 22 studies that had the necessary information to answer our research questions. We also extracted data from 27 studies from the review focused on dietary interventions 5 (Supplementary material).
Among the 22 physical activity interventions, our scoring system yielded three studies with zero points, one with one point, four with two points, two with four points, four with five points, and eight with six points, where a higher score indicates more robust controls for concurrent medication adjustment (Figure 1). The mean concurrent medication adjustment score for these studies was 3.9/6 points. Concurrent antihyperglycemic medication controls used in physical activity and dietary intervention studies.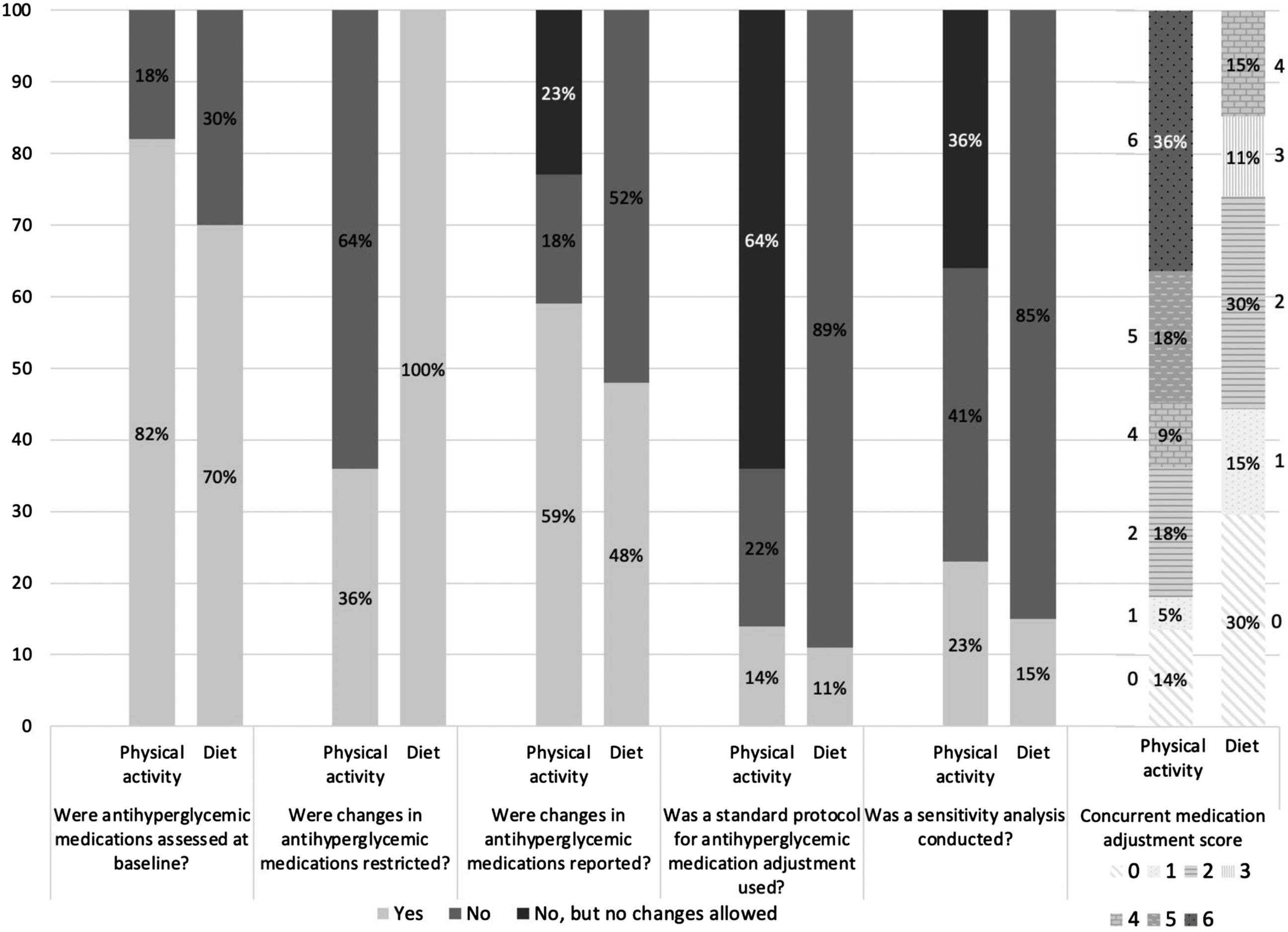
With respect to the studies focused on dietary interventions, our scoring system yielded eight studies with zero points, four with one point, eight with two points, three with three points, and four with four points (Figure 1). The average concurrent medication adjustment score for the 27 dietary studies was 1.7/6 points.
A t-test comparing mean concurrent medication adjustment scores between the physical activity and dietary interventions indicated that physical activity interventions were more likely to use stronger measures to account for concurrent medication changes than studies of dietary interventions (p = <0.0001).
Conclusions
There remains a tremendous amount of heterogeneity in how RCTs of dietary and physical activity interventions address potential concurrent changes in antihyperglycemic medications. We found that RCTs included in recent systematic reviews of physical activity and dietary interventions did not robustly account or control for concomitant changes in antihyperglycemic medication regimens. However, it appears that physical activity interventions accounted for such changes in a more robust manner than did dietary interventions. This may be due to the fact that physical activity interventions may be more likely to result in hypoglycemia than most dietary interventions, making tracking changes in antihyperglycemic medications more important in these studies.
Allowing concurrent medication changes without accounting for these in study design is a threat to the validity of RCT findings, as observed glycemic changes may in fact be attributable to imbalances in concurrent medication adjustments between groups, particularly insulin initiation or titration. This review highlights the need to create standardized protocols and guidelines for addressing concurrent medication adjustment in future RCTs of dietary and physical activity interventions for glycemia. Our novel concurrent medication adjustment score may be a starting point for considering how adjustments could be considered or graded in future RCT protocols. 5
Limitations of the present study include: use of prior conducted systematic reviews and availability of data: investigators used only what was available in the published manuscript and did not have access to investigator brochures and standard operating procedures that were unpublished.
Supplemental Material
Supplemental Material - Accounting for concurrent antihyperglycemic medication changes in dietary and physical activity interventions: A focused literature review
Supplemental Material for Accounting for concurrent antihyperglycemic medication changes in dietary and physical activity interventions: A focused literature review by Dennis B Campbell, Dana Lee Olstad, Teagan Donald and David JT Campbell in Diabetes and Vascular Disease Research
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
