Abstract
The goal of this study was to analyze the effect of COVID-19 drugs and biologicals on hyperglycemia. A literature search with key terms, such as “COVID-19 drugs and hyperglycemia” and “COVID-19 vaccines and hyperglycemia,” was conducted using PubMed through September 2021. The CDC data were referenced for current COVID-19 profile and statistics. The NIH COVID-19 guidelines were referenced for updated treatment recommendations. Micromedex and UpToDate were used for drug and disease information. Current results suggested that corticosteroids (dexamethasone), remdesivir and antivirals (lopinavir and ritonavir) all have the potential to significantly raise blood glucose levels putting patients at elevated risk for severe complications. In contrary, hydroxychloroquine is associated with hypoglycemia, and tocilizumab decreases inflammation which is associated with improving glucose levels. Other anti-cytokine bioactive molecules are correlated with lower blood glucose in patients with and without diabetes mellitus. Ivermectin, used for mild COVID-19 disease, possesses the potential for lowering blood glucose. Covishield, Pfizer-BioNTech, and Moderna have all been associated with hyperglycemia after the first dose. Individualized /personalized patient care is required for diabetic mellitus patients with COVID-19 infection. Improper drug therapy aggravates hyperglycemic conditions and other comorbid conditions, leading to increased morbidity and mortality.
Dear Sir
Across significantly many evidence-based studies, the interrelationship between COVID-19 and diabetes mellitus (DM) is described as a bidirectional process. Studies have shown DM is an independent predictor of admission to the intensive care unit (ICU), requiring ventilation or mortality in COVID-19. 1 Hyperglycemia is common in the ICU resulting from stress-induced insulin resistance and increased glucose production. Viral-induced hyperglycemia usually persists because of inflammation and activation of the immune system. Table 1 summarizes the impact of pharmacotherapy and biologicals used in COVID-19 on blood glucose (BG) levels.
COVID-19 treatment impact on blood glucose.
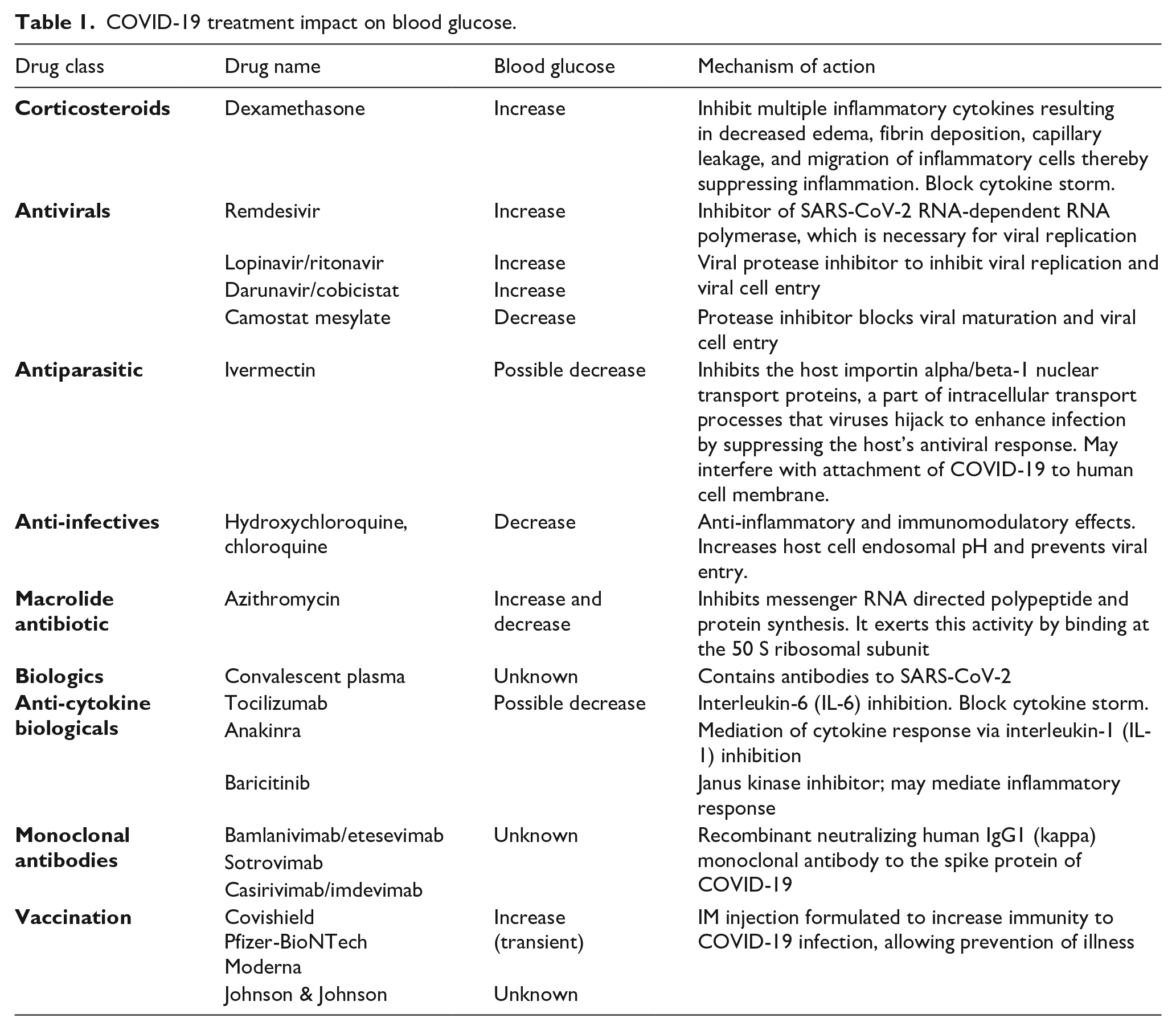
Corticosteroids are indicated for hospitalized COVID-19 patients requiring supplemental oxygen. Historically, corticosteroids are known to increase BG levels, but the benefit of anti-inflammatory treatment during active COVID-19 infection outweighs the risk of hyperglycemia.
Remdesivir, an antiviral, is FDA approved for COVID-19 and is commonly used in severe diseases requiring oxygen. 2 Remdesivir has been associated with elevated BG in COVID-19. Other antivirals (lopinavir/ritonavir, darunavir/cobicistat) are not recommended for hospitalized or non-hospitalized COVID-19 patients. 2 The use of these drugs in COVID-19 has been linked to elevated BG, but there is not enough evidence to evaluate health outcomes. Studies on camostat mesylate demonstrated decreased BG levels which may be a potential alternative antiviral option for DM patients; however, there is no current clinical evidence for use in COVID-19.
Oral therapy with the antiparasitic drug ivermectin is not recommended for use in COVID-19 due to insufficient data supporting efficacy. 2 Evidence has shown ivermectin may decrease BG levels.
Anti-infective and anti-inflammatory drugs (hydroxychloroquine, chloroquine) are not recommended in COVID-19. 2 Use of these drugs is associated with a decreased BG, which theoretically would suggest these drugs may be beneficial for DM patients at risk for contracting COVID-19. Hypoglycemia reportedly is a common adverse effect of hydroxychloroquine.
Azithromycin is not recommended for use in hospitalized and non-hospitalized COVID-19. 2 Evidence on the impact of hyperglycemia is lacking because of mixed study results. Since the use of this medication is not recommended in COVID-19, it is likely appropriate to avoid use in DM until further evidence is obtained.
Convalescent plasma is recommended for use in hospitalized COVID-19 without impaired immunity. 2 The impact of BG is unknown. Anti-cytokine biologicals used in severe COVID-19 treatment are tocilizumab, anakinra, and baricitinib. Evidence has shown each of the biologic therapies reduces BG in those with or without DM. 3 Monoclonal antibodies such as bamlanivimab/etesevimab, sotrovimab, and carisirivimab/imdevimab are indicated for mild to moderate COVID-19 in adults/pediatrics who are at high risk for progression to severe disease. 2 Data regarding the impact on BG is not available for these biologic agents. Common vaccinations like Covishield, Pfizer-BioNTech, and Moderna have some association with increasing BG post-vaccination, but the elevation is transient and usually lowers within 1–7 days.
In conclusion, COVID-19 can worsen DM by uncontrolled hyperglycemia, and DM patients are at an increased risk for severe COVID-19. Corticosteroids, antivirals, and vaccination have been reported to elevate BG. Alternatively, some biologics, anti-infectives, and antiparasitic drugs may reduce BG. This information may provide alternative drug recommendations in patients with uncontrolled BG who are at risk for diabetic-related complications. The risk/benefit ratio from the healthcare team should be applied to this patient population for COVID-19 therapeutic recommendations and prevention.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
