Abstract
Diabetes is a common comorbidity in patients hospitalized for an acute coronary syndrome event, and prevalence is increasing. Among patients hospitalized with acute myocardial infarction, diabetes can be an independent predictor of mortality and new cardiovascular events; both short- and long-term outcomes are worse for patients with diabetes relative to those without, and undiagnosed diabetes is associated with greater mortality. The impact of glycemic control on cardiovascular outcomes and the best approach to treat hyperglycemia upon hospital admission for acute coronary syndrome in patients with or without known diabetes remain open questions. This review assesses available evidence for hyperglycemia management at the time of admission for acute coronary syndrome and, thereafter, finds that (1) admission plasma glucose plays a role in predicting adverse events, especially in patients with unknown diabetes; (2) glycated haemoglobin is a likely predictor of events in patients with unknown diabetes; and (3) hypoglycemia at the time of acute myocardial infarction hospital admission is an important predictor for mortality in patients with and without diabetes. Whether glucose-targeted insulin and glucose infusion have advantages over glucose–insulin–potassium infusion remains controversial. Evidence for the effect of novel glucose-lowering agents used at the time of an acute cardiovascular event is limited and requires more dedicated studies.
Introduction
From 1990 to 2013, the estimated number of years of life lost due to diabetes has increased more than 50% globally, while over the same period, the total number of years of life lost due to any cause has decreased by approximately 16%. 1
The age-standardized incidence rate of first coronary heart disease (CHD) is significantly higher in patients with than in patients without type 2 diabetes.
2
Comorbidities such as chronic kidney disease (CKD) further increase the risk of cardiovascular disease (CVD) in patients with diabetes, with the prevalence of CHD being 31.6% in patients with non-albuminuric stage 3 CKD and 44.8% in those with albuminuric stage 3 CKD.
3
In men and women hospitalized with an acute myocardial infarction (AMI), diabetes is an important comorbidity.
4
Between 1999 and 2011, the prevalence of diabetes in patients with AMI, unstable angina (UA), heart failure (HF) or ischemic stroke has progressively increased.
5
Among patients undergoing percutaneous coronary intervention (PCI) for ST-segment elevation myocardial infarction (STEMI), 25% had a history of diabetes, almost 10% had previously undiagnosed diabetes, and 38.7% had pre-diabetes.
6
Among patients admitted to an intensive coronary care unit (ICU), 22% had a clinical diagnosis of diabetes. Compared with patients without diabetes, they are older, are more frequently female, have a worse coronary risk profile and have unfavourable clinical presentation.
7
Based on a US registry, nearly 7 out of 10 patients admitted to an ICU had dysglycemia, 38% had diabetes and 31% had impaired glucose tolerance (IGT).
8
The Organization to Assess Strategies for Ischemic Syndromes (OASIS) registry showed that among patients hospitalized with UA or non-Q-wave AMI, 21% had diabetes.
9
In this cohort, diabetes was an independent predictor of mortality [relative risk (RR) = 1.57; 95% confidence interval (CI) = 1.38–1.81;
Diabetes and IGT are strongly associated with CVD. Alterations in glucose metabolism are more prevalent in subjects with an acute CV event. The incidence of major CV events and death has progressively decreased in patients with diabetes between 1998 and 2014, yet a significant difference exists between patients with and without diabetes. 16 A similar trend has been observed in the United States.17,18 This reduction in CV morbidity and mortality is likely to be attributed, at least in part, to the increased use of safer glucose-lowering drugs as well as drugs to treat non-glycemic risk factors. However, the impact of glycemic control on CV outcomes and the best approach to treat hyperglycemia during and following an acute CV event remain a matter of debate. Even the latest Scientific Statement from the American Heart Association published in 2008 19 and recent guidelines on short- and long-term management of hyperglycemia after acute CV events 20 fail to address this specific topic. Due to this uncertainty, we have reviewed the available evidence in an attempt to assess the extent to which an evidence-based guide for the management of hyperglycemia at the time of an acute coronary syndrome (ACS) event can be generated.
Methods
A panel of Italian experts was convened to identify major questions related to the impact and treatment of hyperglycemia at the time of ACS. Five main questions were identified (vide infra) and a PubMed search was conducted to identify relevant studies published in English from 1975 through 2016 using Boolean search terms combined with the following terms for each of the following questions:
Question 1. Are admission glucose and glycated haemoglobin (HbA1c) predictors of short- and long-term mortality after ACS in patients with known or unknown diabetes mellitus? ‘type 2 diabetes’, ‘randomized controlled trial’, ‘fasting glucose’, ‘admission glucose’, ‘random glucose’, ‘mortality’, ‘acute coronary syndrome’, ‘myocardial infarction’ and ‘revascularization’.
Question 2. Is low blood glucose at admission a negative prognostic factor in patients with diabetes and ACS? all of the terms for Question 1, plus ‘hypoglycemia’ and ‘low blood glucose’.
Question 3. Does in-hospital appropriate glucose control with insulin improve short- and long-term prognosis in patients with diabetes and ACS? all of the terms for Question 1, plus ‘insulin’, ‘antidiabetic treatment’ and ‘oral antidiabetic agents’.
Question 4. Do glucose-lowering drugs other than insulin improve outcomes in the acute phase of ACS? all of the terms for Question 1, plus ‘insulin’, ‘antidiabetic treatment’ and ‘oral antidiabetic agents’.
Question 5. Which glucose-lowering medications should be used after hospitalization following ACS? all of the terms for Question 1, plus ‘post-acute phase’ and ‘long-term treatment’.
Considering the large number of articles published on the topic of ACS in patients either with or without diabetes, the search was focused on randomized controlled trials (RCT) only. The studies were assessed first by their titles, then by the abstract and followed by full text review. The relevant articles were assessed according to eligibility criteria: only RCTs were used because of their higher quality, better control, and replicability. Only human studies were used. Two of the authors (A.A. and S.G.) independently extracted data from eligible articles, recording demographics, trial characteristics and outcome data. This information was subsequently revised and discussed by all authors during a face-to-face meeting.
Results
Question 1: Are admission glucose and glycated haemoglobin predictors of short- and long-term mortality after ACS in patients with known or unknown diabetes mellitus?
In subjects with diabetes, anatomical and functional abnormalities affect the coronary circulation. As compared to subjects without diabetes, in those with diabetes, atherosclerotic plaques have larger necrotic cores, greater degree of inflammation, more ruptures and positive remodelling. 21 Along with coronary atherosclerotic lesions, subjects with diabetes often have coronary microvessel dysfunction yielding altered coronary autoregulation and impaired microvascular vasodilatory function. 22 Altogether these conditions may account for poorer outcome after STEMI. More controversial is the role of high glucose at admission of a person with diabetes, with some studies supporting a worse prognosis23–25 and others reporting no association.26–28 However, some studies have shown that admission hyperglycemia is a predictor of life-threatening complications and mortality in both individuals with and without known diabetes.29–31 If a worsening role of admission hyperglycemia may not be fully endorsed in diabetes, this has always been identified as a predictor of poor prognosis in patients with unknown diabetes.32–34 While the relationship between blood glucose levels and in-hospital mortality in patients with STEMI is linear in patients without diabetes,35,36 no association was reported with fasting glucose levels at admission in patients with diabetes and CHD, including STEMI and UA.37,38 Some evidence suggests that persistent hyperglycemia is a better indicator of prognosis than admission hyperglycemia. 39 Glycemic variability during the initial 48-h insulin/glucose infusion after a CV event was not associated with 1-year risk of death, re-infarction or stroke. 40 Peak glycemia in patients undergoing PCI was a predictor of early death in patients without diabetes though it affects long-term survival in patients with and without diabetes. 41 In a study of patients with STEMI undergoing PCI, admission glucose level was a predictor of 30-day mortality, but not late mortality, in both patients with and without diabetes. 42 Conversely, in patients with AMI, admission blood glucose was a predictor of long-term mortality regardless of diabetic status.34,43 However, normoglycemic patients with STEMI undergoing PCI generally have better outcomes than those with known diabetes or newly diagnosed diabetes in terms of in-hospital and long-term mortality. 6
Although IGT and newly diagnosed diabetes are associated with increased rates of major adverse CV events (MACE) and outcomes, 44 admission blood glucose seems to be a more accurate predictor of death than previous diabetes diagnosis. 45 Patients with STEMI undergoing PCI with overt or newly diagnosed diabetes have similar in-hospital and 3-year mortality, though mortality is lower in patients with pre-diabetes or no dysglycemia. 6 Postprandial hyperglycemia appears to be a predictive factor of event-free survival (CV death, non-fatal MI, non-fatal stroke, hospitalization for ACS or coronary revascularization planned after randomization) in patients with type 2 diabetes. 46 Patients with IGT or newly diagnosed diabetes following MI have an increased incidence of MACE with adverse outcomes. 44
Conversely, the role of HbA1c in predicting mortality after ACS remains uncertain. Two studies reported no association between HbA1c and prognosis.47,48 In other studies, an increase in HbA1c significantly reduced survival after AMI. In one study, it was shown that patients with newly detected diabetes and HbA1c ⩽ 7.0% had lower mortality (6.4%) than those with HbA1c > 7.0% (14.3%;
In conclusion, patients with some form of glucose intolerance are at higher risk of mortality after an ACS than those with normal glucose tolerance. Admission plasma glucose plays a role in predicting adverse events, especially in subjects with previously unknown diabetes. HbA1c might be a predictor of events in patients with previously unrecognized diabetes (Table 1). This epidemiologic association also recognizes a pathophysiologic plausibility as hyperglycemia may impact several processes that may be implicated in the worsening or protection at the time of a CV insult. High glucose can affect, for instance, autonomic nervous function as indicated by an inverse relationship between plasma glucose levels and baroreflex sensitivity 66 and the increase in heart rate along with QTc elongation under the condition of hyperglycemic clamp. 67 Hyperglycemia can increase levels of glucosamine in the endothelial cells with reduced endothelial nitric oxide (NO) synthase activity, 68 which may account for the inhibitory effect of hyperglycemia on flow-mediated vasodilation 69 and loss of ischemic preconditioning. 70 Hyperglycemia, also, through the activation of intracellular diacylglycerol, can contribute to activation of protein-kinase C and intracellular inflammatory response. 71 Finally, acute hyperglycemia can activate oxidative stress. 72
Cardiovascular outcomes in patients with type 2 diabetes.
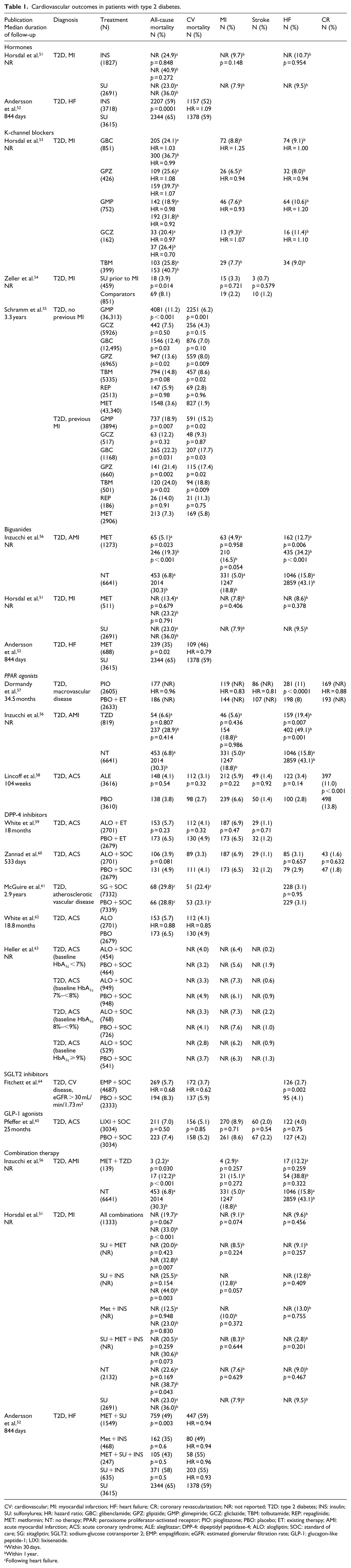
CV: cardiovascular; MI: myocardial infarction; HF: heart failure; CR: coronary revascularization; NR: not reported; T2D: type 2 diabetes; INS: insulin; SU: sulfonylurea; HR: hazard ratio; GBC: glibenclamide; GPZ: glipizide; GMP: glimepiride; GCZ: gliclazide; TBM: tolbutamide; REP: repaglinide; MET: metformin; NT: no therapy; PPAR: peroxisome proliferator-activated receptor; PIO: pioglitazone; PBO: placebo; ET: existing therapy; AMI: acute myocardial infarction; ACS: acute coronary syndrome; ALE: aleglitazar; DPP-4: dipeptidyl peptidase-4; ALO: alogliptin; SOC: standard of care; SG: sitagliptin; SGLT2: sodium-glucose cotransporter 2; EMP: empagliflozin; eGFR: estimated glomerular filtration rate; GLP-1: glucagon-like peptide-1; LIXI: lixisenatide.
Within 30 days.
Within 1 year.
Following heart failure.
Question 2: Is low blood glucose at admission a negative prognostic factor in patients with diabetes and ACS?
There is a concern that hypoglycemia occurring as a result of glucose-lowering therapy may be harmful for patients with AMI. In a study examining 30-day mortality rates in patients with AMI according to serum-glucose levels on admission, 30-day mortality rate was higher in those with the lowest and the highest glucose levels. 73 These results are in accordance with previously published data on patients with ACS and diabetes, underlying the poor prognosis associated with both hyperglycemia and hypoglycemia at admission. 74 Persistent hyperglycemia and hypoglycemia have also been associated with adverse prognosis in patients with AMI. 75 The same picture emerges in elderly patients (⩾65 years) with AMI: hyperglycemia and hypoglycemia at admission were associated with higher in-hospital and 3-year mortality. 76
Interestingly, while both admission and in-hospital hyperglycemia predicted 30-day death in patients with AMI, admission but not in-hospital hypoglycemia was predictive of 30-day survival. 77 In contrast, both in-hospital hyperglycemia and hypoglycemia were associated with increased risk of death during long-term follow-up in patients with HF following AMI. 78 Hypoglycemic episodes during hospitalization of patients with diabetes and AMI do not appear to be an independent risk factor for future morbidity. 79
Interestingly, increased mortality in patients with AMI appears to be limited to hypoglycemia that is unrelated rather than related to glucose-lowering therapy. 80
In conclusion, admission hypoglycemia may be an important predictor for mortality in patients with and without diabetes following AMI. The mechanisms through which hypoglycemia can contribute to worsening prognosis at the time of an acute CV event have been the matter of multiple studies. As recently reviewed by Rana et al., 81 putative pathological mechanisms linking hypoglycemia and adverse CV events include the development of a prothrombotic milieu and a rise in cytokines, vasoconstrictors, inflammatory markers, interleukins and free oxygen radicals. These changes can contribute reducing myocardial blood flow reserve and subsequent myocardial injury with a heightened risk of cardiac arrhythmias and sudden cardiac death.
Question 3: Does in-hospital appropriate glucose control with insulin improve short- and long-term prognosis in patients with diabetes and ACS?
It has been suggested that glucose, insulin, and potassium (GIK) therapy might prevent arrhythmia during myocardial ischemia through reduction of fatty acid levels and stimulation of potassium uptake, as well as of cellular transport and utilization of glucose. 82 Second, insulin therapy can effectively control blood glucose and prevent adverse outcomes associated with hyperglycemia. 83 Indeed, insulin exerts vasodilatory effects in the human circulatory system at physiological concentrations, inhibits platelet aggregation in response to multiple agonists by generating NO and cyclic guanosine-mono-phosphate and exerts direct inhibitory effects on mediators of inflammation in vivo. 84
Several clinical trials have investigated the effects of GIK therapy on post-ACS prognosis, but the results remain conflicting possibly due to the inclusion of patients with and without diabetes. The effect of GIK therapy in patients with and without diabetes has been determined in a meta-analysis of 33 randomized clinical trials. 85 GIK therapy significantly reduced myocardial injury and improved hemodynamic performance in patients without diabetes; on the contrary, glycemic control may be required during GIK therapy to elicit similar effects in patients with diabetes. GIK therapy improved myocardial salvage in patients with AMI and diabetes, but not in patients without diabetes. 86 In patients with suspected ACS without diabetes, GIK therapy reduced the composite endpoint of cardiac arrest or 1-year mortality, and of cardiac arrest, mortality, or HF hospitalization within 1 year. 87 In the CREATE-ECLA trial, GIK infusion had no beneficial effect on 30-day mortality in 20,201 STEMI patients, 88 and could have caused harm following a STEMI. 89 In patients with STEMI without HF, GIK therapy had no significant advantages in terms of number of deaths, revascularizations, and re-infarction at 1 year compared with conventional treatment. 90 Another study showed that patients without diabetes with STEMI may benefit from intravenous insulin infusions. 91 Furthermore, GIK had no advantage over conventional treatment in patients undergoing primary revascularization when considering myocardial function and viability.92–94
During GIK, however, glucose monitoring is not regularly performed and blood glucose levels may vary according to patient’s insulin sensitivity. On the contrary, insulin infusion should be adjusted to maintain plasma glucose levels at 90–140 mg/dL carefully avoiding hypoglycemia as suggested by the American Diabetes Association (Level of Evidence C). 19 Other studies have shown that, compared with routine glucose-lowering therapy, insulin-glucose infusion targeting plasma glucose levels between 126 and 196 mg/dL followed by multi-dose subcutaneous insulin reduces long-term (1 year and 3.4 years) mortality in patients with AMI and diabetes.95,96 The 20-year follow-up results of the first Diabetes Mellitus Insulin Glucose Infusion in Acute Myocardial Infarction (DIGAMI) study showed that intensified insulin-based glycemic control after AMI in patients with diabetes and hyperglycemia at admission had a positive effect on longevity. 97 Conversely, a study in which insulin/dextrose infusions were adjusted to target a blood glucose level of <180 mg/dL showed no reduction in mortality in patients with AMI and diabetes or hyperglycemia but did not rule out that better glycemic control may improve outcomes. 98 In the randomized BIOMarker Study to Identify the Acute Risk of a Coronary Syndrome–2 (BIOMArCS-2) Glucose Trial, patients (10% with diabetes) admitted for an ACS were randomized either to conventional or strict glucose control (glucose level 85–110 mg/dL from 6:00 a.m. to 10:59 p.m. and 85–139 mg/dL from 11:00 p.m. to 6:00 a.m.). There were no differences in both primary (high-sensitivity troponin T value 72 h after admission) and secondary endpoints (area under the curve of creatine kinase myocardial band, release and myocardial perfusion scintigraphy findings at 6-weeks follow-up) between the two treatment arms. 99 A meta-regression analysis of RCTs comparing intensive blood glucose control with a less intensive regimen showed limited benefit of intensive glycemic control in patients with type 2 diabetes with a MI, with a significant risk of serious hypoglycemia. 100
In conclusion, insulin and glucose infusions adjusted to a specific glucose target may have some advantages over GIK therapy, which appears to have a neutral effect on mortality after ACS; however, both may expose patients to an increased risk of hypoglycemia.
Question 4: Do glucose-lowering drugs other than insulin improve outcomes in the acute phase of ACS?
The most effective strategy for the treatment of patients with acute STEMI is reperfusion, to limit the size of the MI, preserve cardiac function, and reduce development of HF. However, the reperfusion procedure can cause myocardial injury. 101 Diabetes is a confounding factor in the treatment of patients following an acute CV event, and glucose-lowering therapy itself can promote or counteract cardioprotection. 101 Glucose normalization with or without insulin leads to better survival in patients with AMI and hyperglycemia. 102 Treatment with sitagliptin was shown to result in a lower risk of in-hospital complications and MACE at 30 days than other oral glucose-lowering therapies in patients with diabetes enrolled in the Acute Coronary Syndrome Israeli Survey. 103 Studies exploring the potential benefits of glucagon-like peptide-1 (GLP-1) receptor agonists in patients with STEMI have demonstrated an increase in myocardial salvage, reduction of the infarct size and improvements in left ventricular function with exenatide treatment.104–106 Conversely, use of metformin preceding the event was not associated with improvements in infarct size in patients with STEMI. 107
The DIGAMI 2 was performed to investigate long-term outcomes according to glucose-lowering regimens: patients received either insulin-based treatment, insulin during hospitalization followed by conventional glucose-lowering therapy or conventional therapy.
108
After a median of 4.1 years, mortality was 31%, with no difference in the three treatment groups. Compared with conventional treatment, insulin therapy was associated with a HR of 3.60 (95% CI = 1.24–10.50;
These results highlight the limited evidence on the effect of recently introduced glucose-lowering agents emphasizing the need for more dedicated studies to determine whether these novel forms of treatment are as effective or superior to insulin to control blood glucose in patients with diabetes and ACS. Preclinical studies have repeatedly demonstrated how dipeptidyl peptidase-4 (DPP-4) inhibitors, Glucagon-like peptide (GLP-1) receptor agonist and sodium-glucose cotransporter 2 (SGLT2) inhibitors can reduce the infarct size upon acute ischemia in rats110,111 and pigs. 112 Two large cardiovascular outcome trial (CVOT) have recruited patients with a recent (within 90 days) ACS. The first one assessed the effect of the DPP-4-inhibitor alogliptin 59 and the second one employed lixisenatide, 65 and both studies were neutral with respect of occurrence of three-point MACE. Smaller human studies suggest a potential beneficial effect of GLP-1 receptor agonists if administered at the time of an acute event. In STEMI subjects undergoing primary PCI, administration of exenatide at the time of reperfusion was found to increase myocardial salvage and to improve left ventricular function.104,106 Similar results were observed for liraglutide. 113 However, other investigators were unable to replicate these findings. 114
Question 5: Which glucose-lowering medications should be used after hospitalization following ACS?
Studies have shown that patients with diabetes have the same level of CV risk as non-diabetic patients with prior MI. This claims for a proactive treatment of the CV risk in patients with diabetes. 115 Because diabetic patients with a history of CV events are at an even greater CV risk, 116 an intensive management strategy is particularly important after the occurrence of a CV event. Germaine to this, a study showed that, in the general population, there was an increase in the incidence rate of treatment based on glucose-lowering medication within the first year following MI: this suggests that after an acute coronary event, there is an increased awareness of diabetes. 117
Various classes of glucose-lowering therapies have been evaluated for their use following hospitalization for acute MI with heterogeneous results, even within the same drug class (Table 1).51–65,115,117–121 In general, DPP-4-inhibitors showed improved glycemic control with no increase of the risk of CV events or HF outcomes as compared with placebo.59–63 Two of the recent cardiovascular outcome studies have been performed in diabetic patients with a recent ACS. The Examination of Cardiovascular Outcomes with Alogliptin versus Standard of Care (EXAMINE) trial tested the safety of alogliptin in type 2 diabetes patients with an ACS between 15 and 90 days before recruitment. A primary endpoint event occurred in 305 patients assigned to alogliptin (11.3%) and in 316 in those on placebo (11.8%;
The Evaluation of LIXisenatide in Acute coronary syndromes (ELIXA) trial demonstrated that the use of lixisenatide in patients with diabetes and a recent ACS (hospitalized for UA within the previous 180 days) did not affect CVD outcomes, with no increase in the risk of hospitalization for HF. 65
Six recent CV outcome studies, namely, the EMPA-REG Outcome trial, 123 the Liraglutide Effect and Action in Diabetes: Evaluation of CV Outcome Results (LEADER) trial, 124 the investigators in the Trial to Evaluate Cardiovascular and Other Long-Term Outcomes with Semaglutide in Subjects with Type 2 Diabetes (SUSTAIN-6), 125 the Canagliflozin Cardiovascular Assessment Study (CANVAS) Program, 126 the Dapagliflozin and Cardiovascular Outcomes in Type 2 Diabetes (DECLARE), 127 and the Albiglutide and CV outcomes in patients with type 2 diabetes and CVD (Harmony Outcomes), 128 have stirred a greater enthusiasm, as they showed superiority of empagliflozin, liraglutide, semaglutide, canagliflozin and albiglutide over placebo for the primary endpoint (CV death, non-fatal acute MI and non-fatal stroke). These studies recruited high-risk patients with type 2 diabetes. However, not all of the patients had already experienced a CV event and, if they did, the events were not as recent as in the EXAMINE or the ELIXA trials. In the EMPA-REG trial, 75% of patients had a history of CHD; in the LEADER trial, 31% had prior MI and 39% had prior coronary revascularization; in the SUSTAIN-6 trial, 60% had CHD and 32% had prior MI.
Metformin is considered cardioprotective, since treatment with this agent is associated with lower risk of mortality (compared with sulfonylurea or insulin therapy) in patients with diabetes and HF or MI, and with decreased risk of non-fatal MI or stroke in patients with diabetes and MI.52,109 Although some studies found no increased risk of adverse outcomes in patients receiving sulfonylurea before an index event,54,121 other studies found that patients with diabetes and MI on sulfonylurea at the time of admission for a CV event had higher CV risk as compared with those on metformin. 119 Finally, other studies have found no definite relationship between use of sulfonylureas and ischemic heart disease,51,118 although, compared with metformin, sulfonylureas may be associated with increased mortality and CV risk. 55
Differences in outcomes between the agents within the class have been reported. For instance, while the effect of rosiglitazone has been questioned due to a claimed increased CV risk in some but not all meta-analyses, the use of pioglitazone reduced the composite endpoint of all-cause mortality, non-fatal MI and stroke in patients with diabetes and a high risk of macrovascular events, 57 while no information is available with respect to its use in the early phase after ACS.
Discussion
In patients with STEMI, admission hyperglycemia is a strong predictor of short-term mortality in those without diabetes, while the relationship is not as clear in patients with diabetes. The prognostic value of HbA1c also remains unclear. Hypoglycemia at the time of admission is associated with higher short- and long-term mortality in patients with ACS, but this seems to be restricted to hypoglycemia not occurring as a result of glucose-lowering therapy.129,130 The role of hypoglycemia as a risk factor for death has led to the concept that there are three domains of glycemic control in the critically ill – hyperglycemia, hypoglycemia and glycemic variability – and that these must be addressed to optimize glycemic control. Interestingly, it appears that hypoglycemia per se, rather than drug-induced hypoglycemia, could play a role in increased mortality: decompensated cardiac failure is especially evident among hypoglycemic patients, as evidenced by low left ventricular ejection fraction and high NT-proBNP levels, and in those with elevated plasma alanine transferase suggesting significant hepatocyte injury. 131 Low pH values and high lactate concentrations may also explain hypoglycemia, since they reflect hypoperfusion, and hepatic dysfunction. 132
The effects of insulin on prognosis after ACS might be different in patients with versus without diabetes, as the former may benefit from insulin therapy if adequate glycemic control is ensured and hypoglycemia avoided. Because of the risk of hypoglycemia, other glucose-lowering agents could be considered (Table 2).62,133–137 In subjects with type 2 diabetes and a recent ACS, alogliptin, an inhibitor of DPP-4, was safe without the burden of hypoglycemia, though an increased risk of hospitalization for HF was observed in patients with no prior history for the condition. Similarly, lixisenatide, a GLP-1 receptor agonist, was safe in patients with diabetes and recent ACS. In patients with high CV events, the GLP-1 receptor agonists liraglutide and semaglutide, as well as the SGLT2 inhibitor empagliflozin, have shown significant reduction of CV risk.
Suggested glucose-lowering therapies during an acute coronary syndrome and after hospitalization.
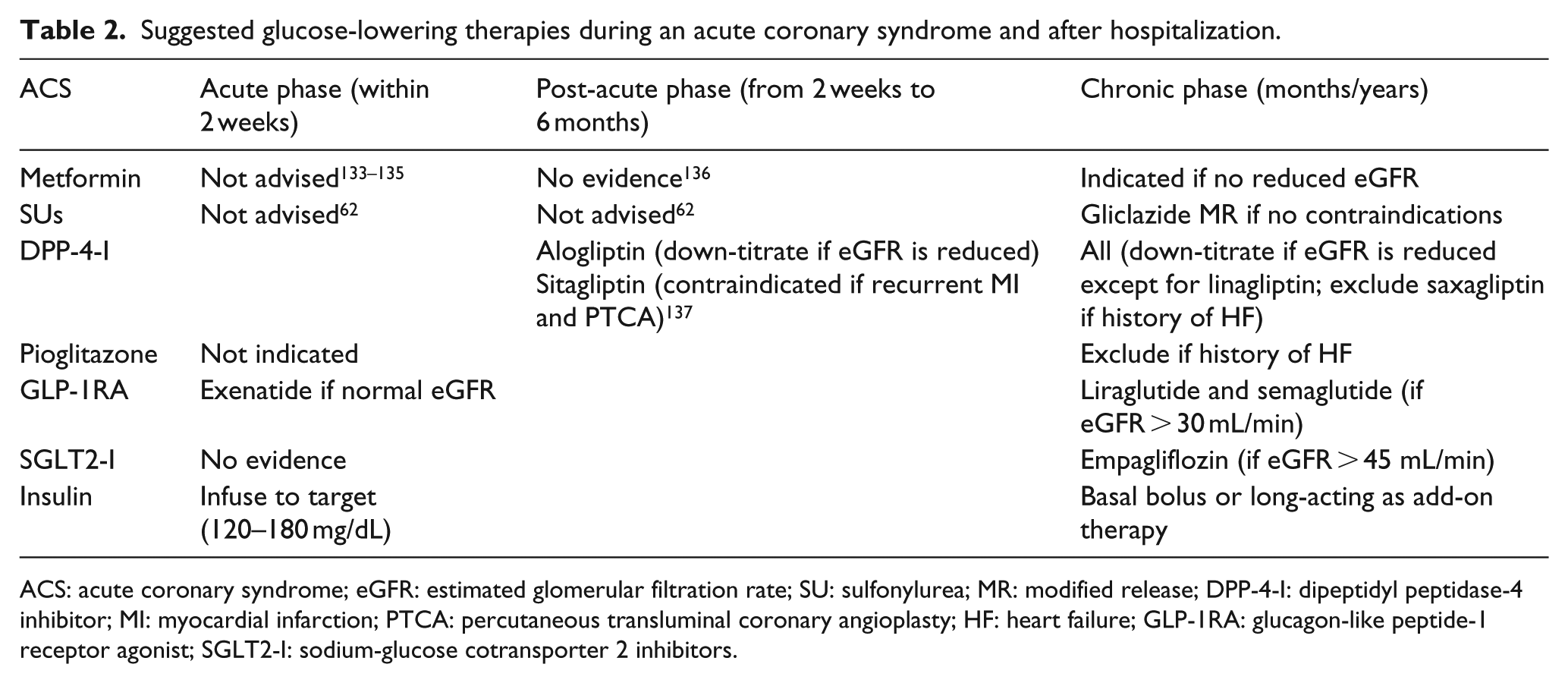
ACS: acute coronary syndrome; eGFR: estimated glomerular filtration rate; SU: sulfonylurea; MR: modified release; DPP-4-I: dipeptidyl peptidase-4 inhibitor; MI: myocardial infarction; PTCA: percutaneous transluminal coronary angioplasty; HF: heart failure; GLP-1RA: glucagon-like peptide-1 receptor agonist; SGLT2-I: sodium-glucose cotransporter 2 inhibitors.
In summary, how to treat hyperglycemia in patients with or without previously known diabetes at the time of hospital admission for ACS remains an open question. Insulin is the only treatment that has been evaluated in depth; however, results are conflicting and they differ with respect to diabetic versus non-diabetic hyperglycemia as well as in terms of short- versus long-term outcomes. In all cases, insulin use was associated with a significant increase in the risk of severe hypoglycemia, which should be avoided in these patients. Non-insulin therapies may sound attractive because of both the low risk of hypoglycemia and the effects that may potentially translate into CV protection at the time of an ACS. However, no studies have been performed to date with agents such as DPP-4-inhibitors, or SGLT2-inhibitors, and relatively few with GLP-1 receptor agonists at ACS presentation. The closest treatment to the time of an ACS is the one tested in EXAMINE (alogliptin) and ELIXA (lixisenatide). These agents have shown safety in highly vulnerable populations. CV protection as reported with empagliflozin, canagliflozin, dapagliflozin, liraglutide, semaglutide and albiglutide are of great value but they cannot be extrapolated to time of the occurrence of an ACS. In summary, there is an urgent need for studies exploring potential advantages of non-insulin treatments not associated with risk of hypoglycemia in patients with diabetes and ACS: in the meantime, a common-sense approach is proposed in Table 2. In the absence of such studies, we conclude that insulin should be used for admission hyperglycemia aiming at plasma glucose levels of 90–140 mg/dL, as also suggested by the American Diabetes Association, with careful avoidance of hypoglycemia.
In the earlier phase after ACS, alogliptin and lixisenatide have shown safety, and in those with high CV risk, empagliflozin, liraglutide and semaglutide may offer an opportunity for effective secondary CV prevention.
Key messages
Plasma glucose level at hospital admission for acute coronary syndrome (ACS) plays a role in predicting adverse events, especially in patients with previously unknown diabetes.
Admission hypoglycemia is an important predictor for mortality in patients with and without diabetes following acute myocardial infarction.
Insulin and glucose infusions aimed at specific glucose targets may reduce mortality after ACS while increasing the risk of hypoglycemia.
There is an urgent need for studies exploring potential advantages of non-insulin treatments not associated with a risk of hypoglycemia in patients with diabetes and ACS.
Footnotes
Acknowledgements
The authors would like to thank Cécile Duchesnes, PhD, and Georgii Filatov, of Springer Healthcare Communications, for providing medical writing assistance in the preparation of the outline and subsequent drafts of this manuscript.
Author contributions
A.A. and S.G. performed the preliminary literature search and analysis and identified the first version of the research questions. All authors revised and discussed the results of the preliminary search and contributed to the finalization of the research questions and of the relevant literature. All authors critically reviewed the manuscript drafts and approved the final version before submission.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: A.A. has received honoraria for advisory work and lectures from AstraZeneca, Boehringer Ingelheim, Bristol Myers Squibb, Eli Lilly, Bruno Farmaceutici, Amgen, Servier, Recordati, GlaxoSmithKline, Merck Sharp & Dohme, Novartis, Novo Nordisk, Sanofi and Takeda, and research support from Bristol Myers Squibb, Novartis, AstraZeneca and Novo Nordisk. E.B. has participated in advisory boards for Abbott, AstraZeneca, Boehringer Ingelheim, Bristol Myers Squibb, Bruno Farmaceutici, Janssen, Johnson & Johnson, Eli Lilly, Merck Sharp & Dohme, Novartis, Novo Nordisk, Roche, Sanofi, Servier and Takeda. He also received research grants from AstraZeneca, Genzyme, Menarini Diagnostics, Novo Nordisk, Roche and Takeda. A.C. has received consultancy or speaker fees from Abbott, AstraZeneca, Boehringer Ingelheim, Bruno Farmaceutici, Janssen, Eli Lilly, Merck Sharp & Dohme, Novartis, Novo Nordisk, Roche, Sanofi, Servier and Takeda. He also received research grants from Eli Lilly and Novo Nordisk. S.D.P. has received honoraria for advisory work and lectures from AstraZeneca, Boehringer Ingelheim, Bristol Myers Squibb, Eli Lilly, GI Dynamics Inc., GlaxoSmithKline, Hanmi Pharmaceuticals, Intarcia Therapeutics Inc, Janssen, Merck Sharp & Dohme, Novartis, Novo Nordisk, Roche Diagnostics Co., Sanofi and Takeda, and research support from Bristol Myers Squibb, Merck Sharp & Dohme, Novartis and Novo Nordisk. S.G. has participated in clinical research and scientific advisory boards, and served as a consultant or received honoraria for Abbott Diabetes Care, AstraZeneca, Boehringer Ingelheim, Bristol Myers Squibb, Eli Lilly, Janssen, Johnson & Johnson, Lifescan, Menarini, Merck Sharp & Dohme, Novartis, Novo Nordisk, Sanofi and Takeda. F.G. has received consultancy or speaker fees from Abbott, AstraZeneca, Boehringer Ingelheim, Eli Lilly, Merck Sharp & Dohme, Novo Nordisk, Roche Diabetes Care, Sanofi and Takeda; he also received research support from Eli Lilly, Takeda and Lifescan.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Medical writing assistance was funded by Ethos.
