Abstract
Guidelines recommend aggressive goals for lipid and blood pressure reduction for high risk patients with diabetes mellitus and atherosclerotic coronary disease. However, it remains unclear how many patients achieve treatment goals versus the number of people merely placed on treatment. We conducted an observational study in an academic cardiology clinic. A total of 926 patients with atherosclerotic cardiovascular disease and concomitant diabetes mellitus met criteria. Mean age was 68.4 ± 10.2, 65.6% were male, and 86.8% were Caucasian. By the last visit a high percentage of patients were receiving recommended medications. Mean LDL-cholesterol achieved was 80.4 mg/dl with 40.9% reaching ≤ 70 mg/dl, and 61.7% reaching SBP ≤ 130 mmHg. Many patients with diabetes mellitus and atherosclerotic cardiovascular disease are prescribed recommended medications; however, few achieve guidelines-specified therapeutic goals for LDL-cholesterol and blood pressure. Studies evaluating performance improvement should include percentage of patients reaching treatment goals. Mechanisms underlying the treatment gap need to be identified and addressed.
Introduction
The association between diabetes mellitus and coronary heart disease risk is well appreciated.1,2 Diabetic patients who develop coronary heart disease experience higher rates of complications compared with non-diabetic patients suffering from coronary heart disease. 3 On the basis of these observations, the National Cholesterol Education Program (NCEP) Adult Treatment Panel (ATP III) recommended in 2004 to classify diabetics as a high risk group and to treat cholesterol aggressively. 4 The seventh report of the Joint National Committee on Prevention, Detection, and Evaluation of High Blood Pressure (JNC 7) recommends a blood pressure (BP) goal of 130/80 for patients with hypertension and diabetes. 5
The important role of abnormal cholesterol levels and development of coronary artery atherosclerosis is well established. In people with diabetes mellitus (DM), aggressive management of cholesterol is considered a central focus of preventing cardiovascular disease complications. Guidelines, which are supported by several studies,6–8 recommend that it is reasonable to attempt to achieve a level of low-density lipoprotein (LDL-C) less than 70 mg/dl for those diabetic patients with known cardiovascular disease. With both lipid and blood pressure goals, several issues remain to be addressed. To date, there has been relatively little attention devoted to practice management tools that may facilitate the translation of evidence -based medicine into common practice. Moreover, in spite of numerous quality initiatives9–11it remains unclear how well we are meeting the goals set by the guidelines in real-world practice for this high risk patient group. The purpose of this study was to determine how successfully guideline-derived treatment goals were met for outpatients with DM and concomitant coronary heart disease in an academic general cardiology practice with electronic medical record (EMR) and quarterly feedback to caregivers pertaining to quality metrics.
Methods
A retrospective, cross-sectional design was used to conduct the study. The Institutional Review Board approved the conduct of this study. Patients were included if they had a diagnosis of diabetes and concomitant atherosclerotic cardiovascular disease (defined as diagnosis of coronary artery disease, peripheral artery disease, renal artery disease or cerebral artery disease), and at least three visits to a general cardiologist in the practice between January 2004 and April 2009. To analyse changes between two time periods, patients were included if they had at least one visit between January 2004 and December 2007 and another visit between January 2008 and April 2009. The first clinic visit was designated as the ‘baseline’ visit and the second as the ‘follow-up’ visit. Patients were excluded if they were seen in only one of the specialised cardiac clinics including heart failure and transplant, device clinic, advanced lipid clinic, heart catheterisation and preoperative evaluation clinics.
Clinic setting
The general cardiology clinic structure is made up of fellows with supervising attending physicians divided into practice groups. In addition, attending cardiologists have independent clinic days where patients are seen without fellows or residents. The service is complemented by the nursing staff. Generally, medications are reconciled on each patient visit by the nurse using the computer workstation in examining rooms. Patients are encouraged to bring their medications to the clinic for verifying or confirming doses in case primary doctors have had reason to alter the dosage. Similarly, vital signs and pertinent labs are entered or interfaced into the computer system. Blood pressure is taken by the nurse, with the patient in the seated position after five minutes’ rest. If elevated, the blood pressure measurement is repeated later in the examination. Reported blood pressure values in this paper represent an average of two measures in the seated position.
Overall system performance of guideline quality measures are tracked and shared with each practice group on a quarterly basis. In addition to periodic group meetings, information and feedback are disseminated via electronic media and departmental conferences.
Data collection
Data in the EMR was collected through a combination of direct import from interfaced systems and manual entry. Because of the potential for error with manual entry, data that was outside of a realistic range was verified with original source documentation. Values were excluded from the analysis if an unrealistic value could not be verified from original documentation. Values for lipids and blood pressure were abstracted from baseline and follow-up visits.
Data analysis
Goals were established for LDL-C and BP measurements. In accordance with national guidelines, LDL-C goal was set at ≤ 70 mg/dl, systolic blood pressure (SBP) at ≤ 130 mmHg, and diastolic blood pressure (DBP) at ≤ 80 mmHg.4,5 Statistical analysis was performed with SPSS version 17.0 (SPSS Inc., Chicago, IL). Values of each measure for each patient were examined at baseline and at follow-up to determine whether goal achievement was met at either time point. Comparisons between baseline and end values were performed using the independent t-test, the paired sample t-test, and chi-square and multivariate logistic regression. The Wilcoxon Signed Rank test and Mann–Whitney U test were used for non-parametric data. Statistical tests were two-tailed. Values are expressed as mean values plus or minus standard deviations. A probability value of < 0.05 was considered significant. Mean doses of statins were computed by converting the individual doses of the various statins to the equivalent of atorvastatin according to their relative potency rates.12,13
Results
General
Baseline demographics and comorbidities are displayed in Table 1.There were a total of 926 patients with DM and concomitant atherosclerotic cardiovascular disease who met inclusion criteria. They included 607 males (65.6%) with a mean age at baseline of 68.4 ± 10.2 years (range 35–96). Other demographics included 86.8% Caucasians, 11.5% African Americans and other race 1.5%. The majority of patients (56%) were obese (BMI > 30 kg/m2). A high percentage of patients were prescribed recommended drug therapy at baseline, as follows, statins: 91.6%, anti-hypertensives: 88.4%, anti-platelet therapy: 92.9%, and beta blocker: 78.3%.
Baseline characteristics of study population at initial visit.
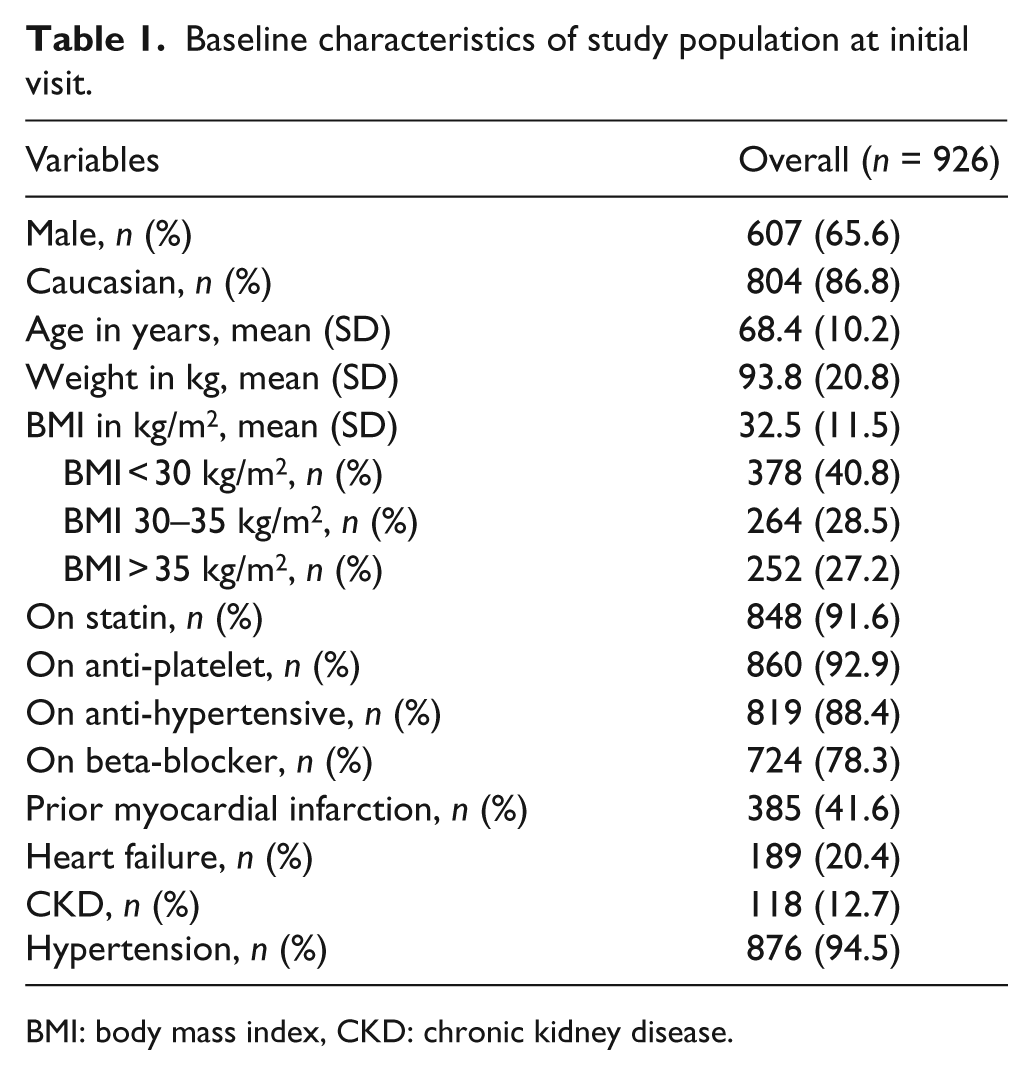
BMI: body mass index, CKD: chronic kidney disease.
Changes between baseline and follow-up visit
LDL-cholesterol
Baseline mean LDL-C was 82.4 ± 31.7 mg/dl and fell slightly to 80.4 ± 33.7 mg/dl at follow-up (p = 0.007). When analysed by gender, males had significant reductions in LDL-C, decreasing from 80.0 to 77.1 mg/dl (p = 0.004); female LDL-C was 87.1 ± 37.0 mg/dl at baseline and 86.6 ± 36.8 mg/dl at follow-up (p = NS). The percentage of patients achieving therapeutic LDL-C goals as per current guidelines is displayed in Figure 1. Specifically, the LDL-C goal of ≤ 70 mg/dl was met by 39.7% at baseline and 40.9% at follow-up. As per the guidelines, 4 195 (21%) met criteria for non-HDL cholesterol to be controlled as a secondary target. Among this subgroup with elevated triglycerides, 55.3% achieved the non-HDL target of 130 mg/dl and 12.4% reached 100 mg/dl at the follow-up visit. Among the entire sample, 79% reached the non-HDL target of 130 mg/dl and 49.5% reached 100 mg/dl (n = 776).
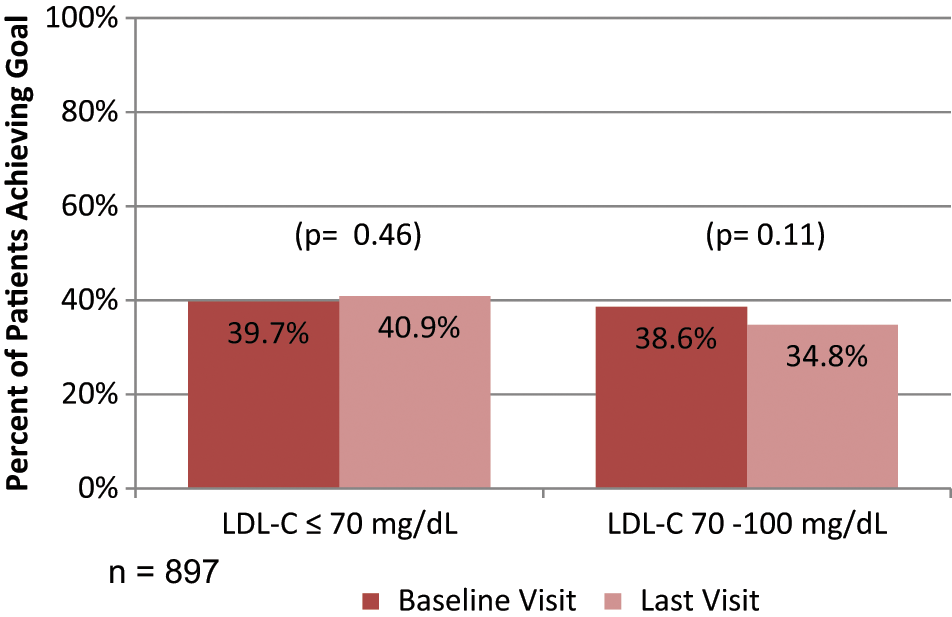
Percentage of patients achieving LDL-C goals at baseline and follow-up visits.
By the follow-up visit, 40.9% of patients were at the goal of LDL-C ≤ 70 mg/dl, while 81.4% achieved 100 mg/dl or lower. Table 2 shows differences between those patients who achieved and did not achieve the LDL-C goal at the end of the study. We sought to determine whether the mean dose of prescribed statins was correlated with achieving goal. Univariate analysis revealed that the mean dose was statistically higher among the group not at goal. The mean doses converted to equivalent of atorvastatin were 26.1 mg among the group at goal compared with 29.0 mg for those not at goal (p = 0.05). We were also interested in knowing whether being prescribed a relatively more potent statin was associated with reaching therapeutic goal. The analysis showed that 35.6% of those at goal received either rosuvastatin or atorvastatin compared with 39.9% of the group who did not reach therapeutic goal, although this difference was non-significant. There was no difference in the time to follow-up between those who did and did not achieve the therapeutic goal. After adjustment for baseline demographic/clinical characteristics, patients who were on a potent statin were significantly less likely to achieve LDL ≤ 70 (odds ratio – OR = 0.61, 95% confidence interval – CI = 0.40–0.92). No other factors were found to be statistically significant predictors of achieving outcome of LDL < 70 mg/dl. Figure 2 shows ORs for achievement of LDL-goal ≤ 70 mg/dl.
Achievement of LDL-C goal at last visit, by sociodemographic variables, HgA1C, weight, comorbidities and medications.
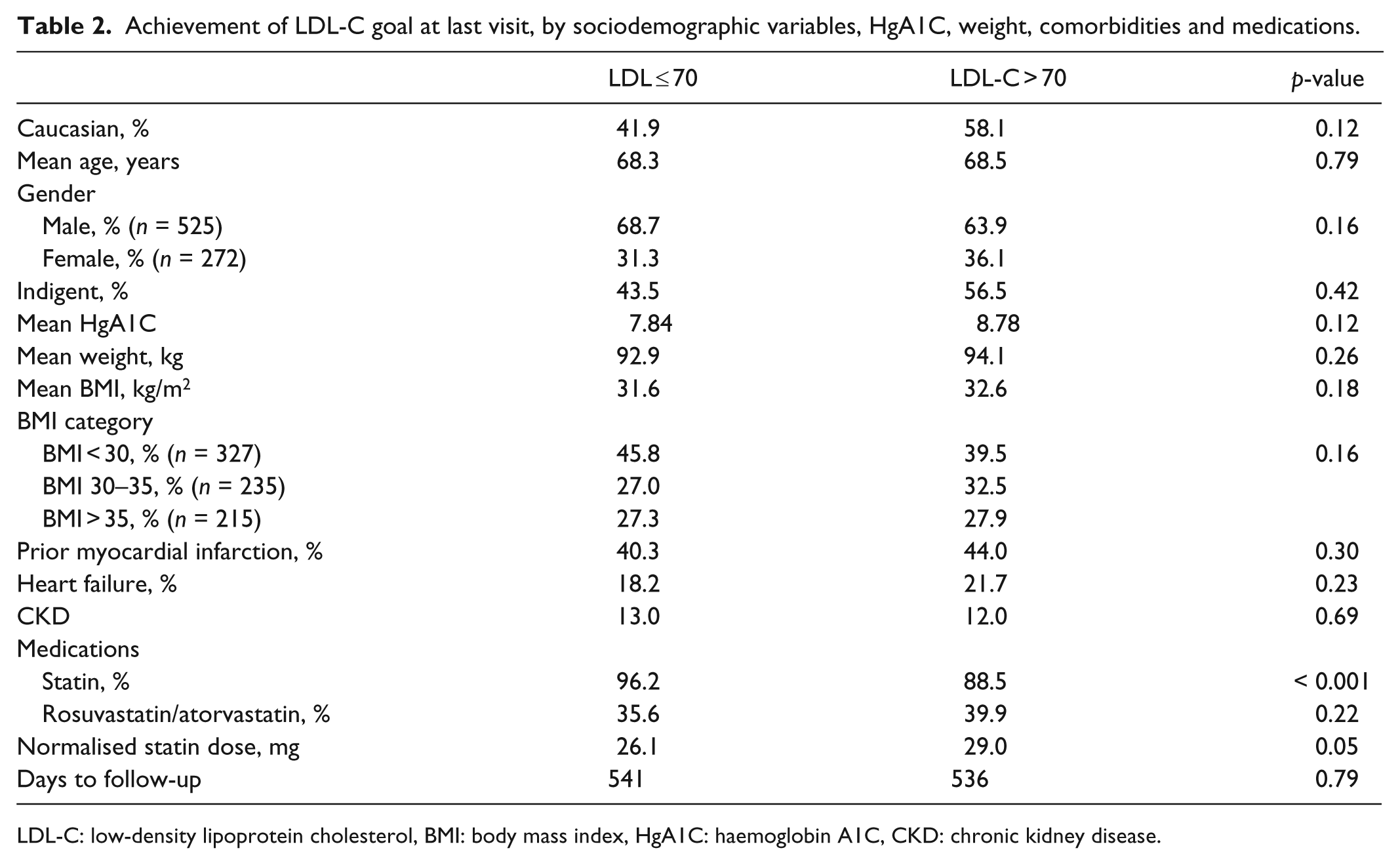
LDL-C: low-density lipoprotein cholesterol, BMI: body mass index, HgA1C: haemoglobin A1C, CKD: chronic kidney disease.
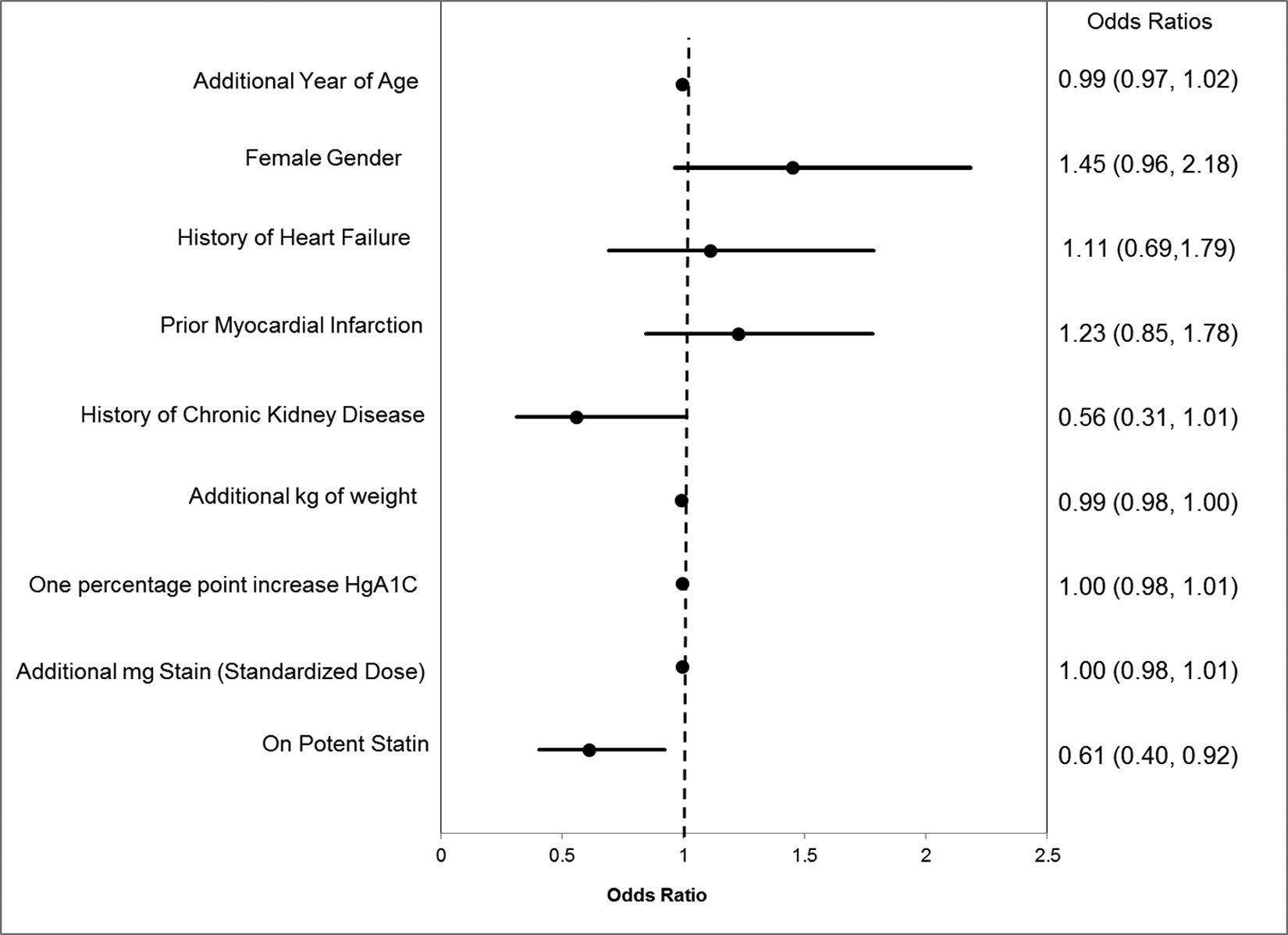
Factors associated with achievement of LDL-C goal ≤ 70 mg/dl. Point estimates are represented by points, and the 95% CIs are shown as bars.
Blood pressure
Baseline SBP was 129.1 ± 18.6 mmHg and 127.1 ± 18.6 mmHg (p < 0.001) at follow-up, and corresponding values for DBP were 67.8 ± 10.7 mmHg and 66.3 ± 9.6 mmHg (p < 0.001), respectively, at baseline and follow-up. Both males and females had significant reductions in SBP and DBP. Figure 3 shows the percentage of patients achieving BP goals at the baseline and last visits.
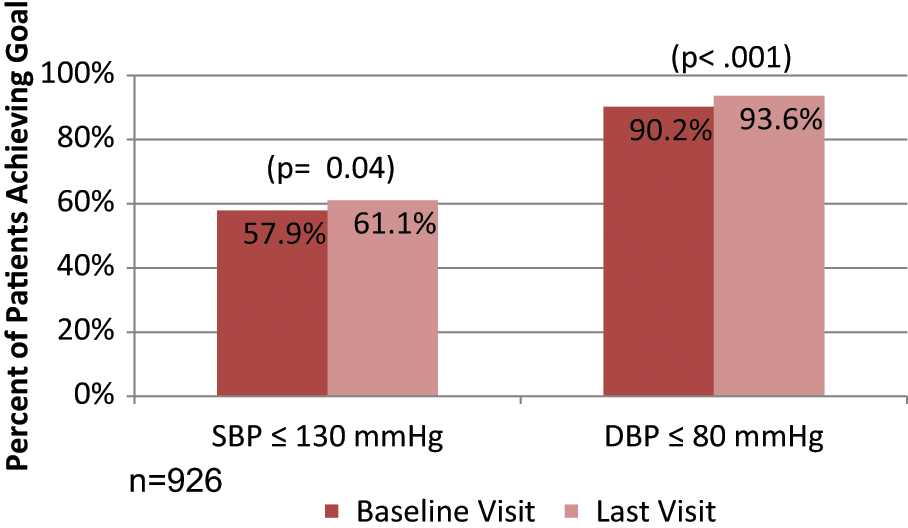
Percentage of patients achieving blood pressure goals at baseline and follow-up visits.
Table 3 shows differences between those patients who achieved and did not achieve SBP goals at the end of the study. Univariate analysis showed that those achieving goals were younger (67.7 years vs. 69.3 years, p = 0.02), and males were more likely than females to have achieved this goal (p < 0.001). Those achieving goal were less likely to be on anti-hypertensive therapy (83.1% vs. 89.1%, p = 0.01), and were less likely to have a history of hypertension (91.7% vs. 99.2%, p < 0.001). No significant differences were found between the two groups with respect to race, indigence status, weight, or BMI. Multivariate logistic regression was performed to determine factors independently associated with achievement of SBP goal ≤ 130 mmHg. Patients who were one year older (OR = 0.978, 95% CI = 0.963–0.992), female (OR = 0.676, 95% CI = 0.498–0.918,), and who had a history of hypertension (OR = 0.08, 95% CI = 0.023–0.275) were significantly less likely to achieve SBP ≤ 130. Figure 4 shows ORs for achievement of SBP goal ≤ 130 mmHg.
Achievement of SBP goal at last visit, by sociodemographic variables, weight and medications.
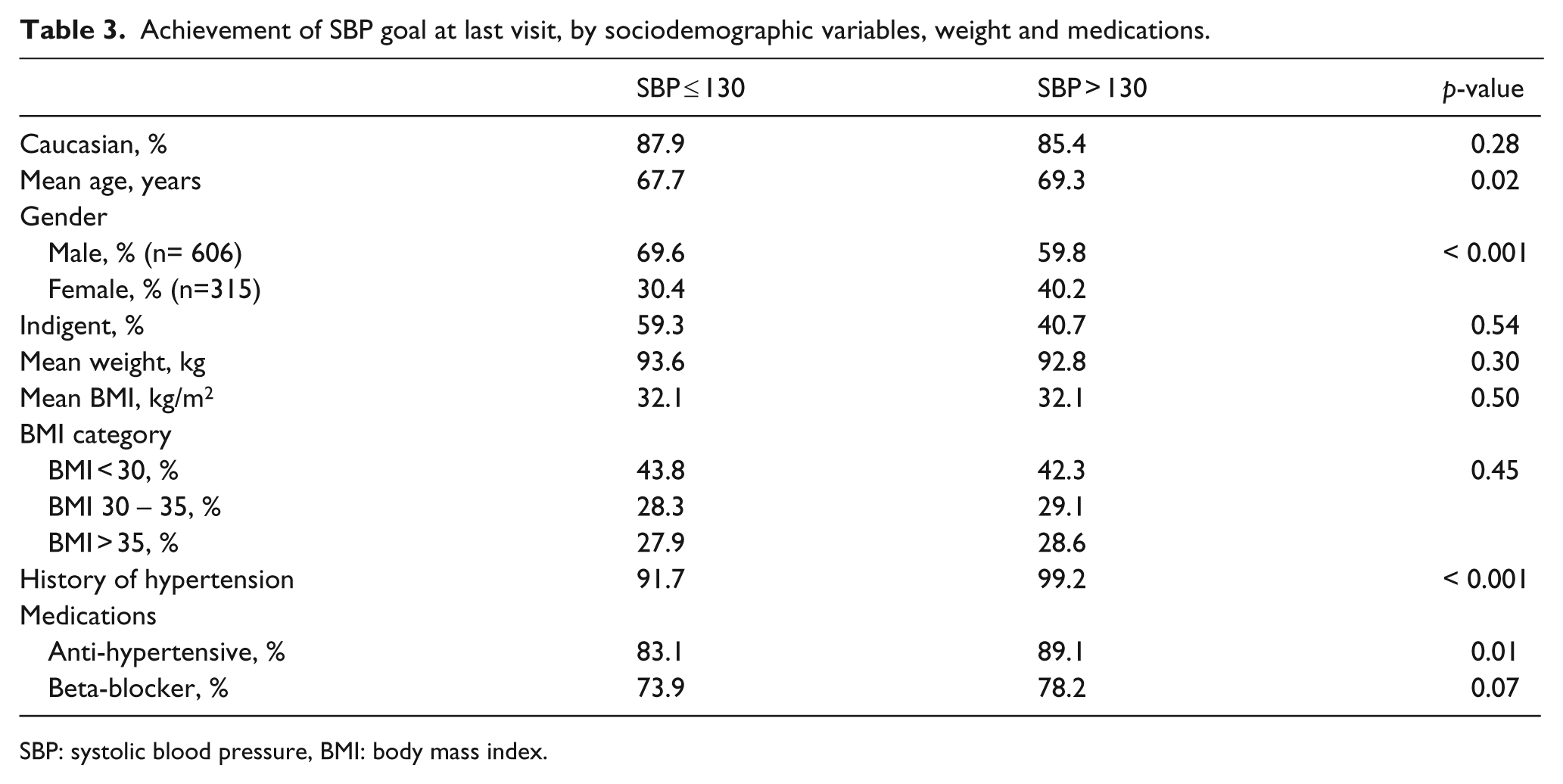
SBP: systolic blood pressure, BMI: body mass index.
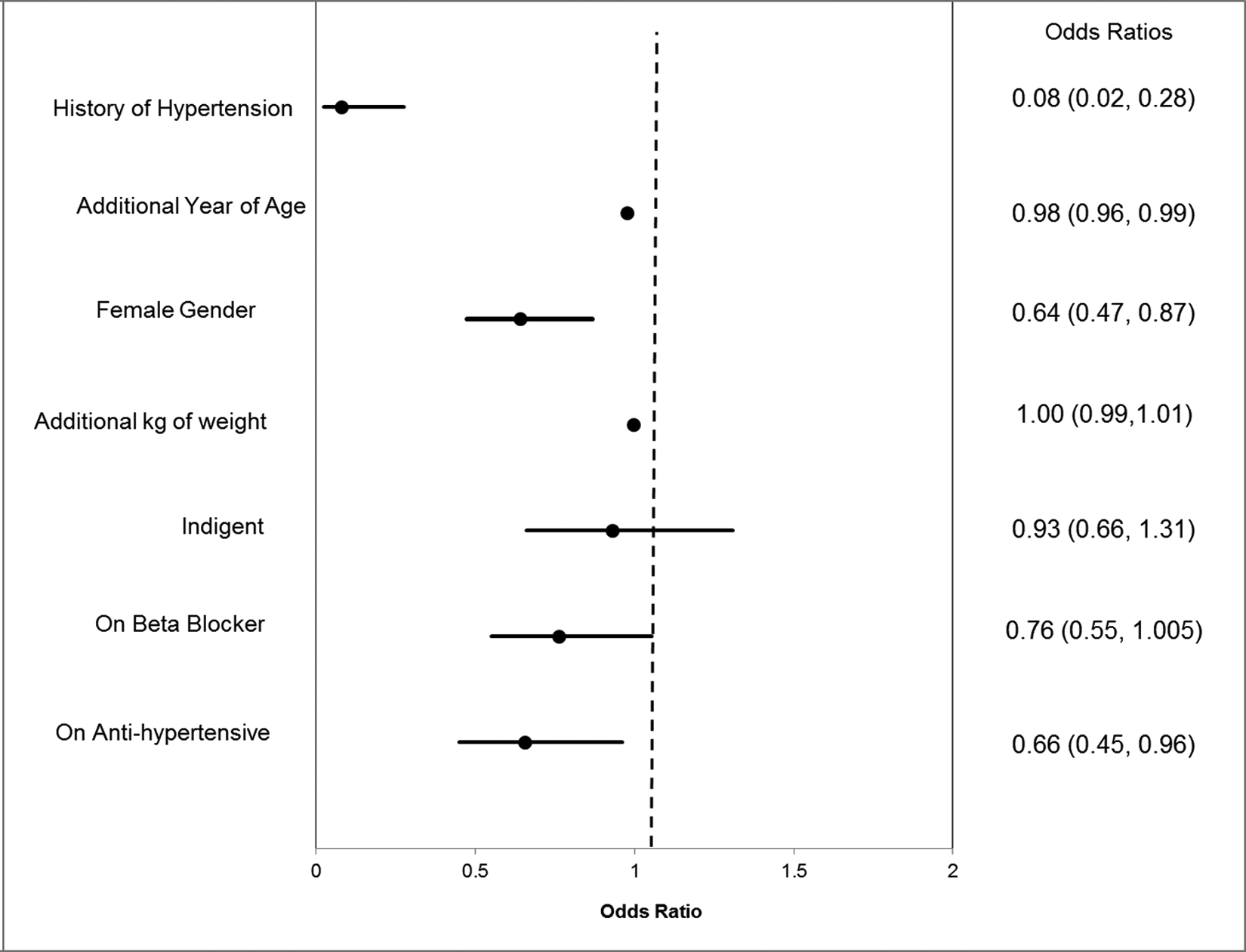
Factors associated with achievement of SBP goal ≤ 130 mmHg. Point estimates are represented by points, and the 95% CIs are shown as bars.
Discussion
Despite a very high percentage of patients receiving guideline-based drugs, with respect to achieving ATP III and JNC 7 target LDL-C and SBP goals, there was less success. The results show that our performance when measured in terms of percentage of patients actually treated to goal of LDL-C ≤ 70 mg/dl and the net increase in patients reaching blood pressure goal was modest. However, univariate analysis showed mean standardised dose of prescribed statins to be higher among the group not at goal, while multivariate analysis showed a negative association between patients being prescribed potent statins and their ability to achieve the lipid goal, both suggesting that there was attempt to treat more aggressively because of failure to achieve targets with lower doses or less potent statins.
Dyslipidaemia remains an important risk factor for both prevention and management of coronary heart disease.14–16Lipid lowering therapy has been shown to improve outcomes, including survival benefit in secondary prevention.17–19 Due to their safety profile, and proven efficacy in evidence-based medicine, statins have been prominently emphasised in both national and international guidelines for coronary heart disease management.4,20 The guidelines have recommended that the overall intensity of treatment be consistent with estimated cardiovascular risk of the individual: the higher the risk of cardiovascular event, the lower LDL goal of therapy according to the guidelines. People with DM are known to be at high risk for cardiovascular events and therefore the guidelines recommend treating diabetes as a coronary heart disease equivalent. 4 People with diabetes who already have known atherosclerotic cardiovascular disease are at extremely high risk and their goal for LDL-C management is set at 70 mg/dl or lower. Currently, there is very little data to suggest that the guidelines-recommended goal is met in this very high risk group of patients.
Comparison with literature
Despite the failure to meaningfully increase the percentage of patients at goal, with regard to the percentage of patients receiving treatment, the mean LDL and blood pressure values achieved, and the percentage of patients with an LDL ≤ 100 mg/dl, results were satisfactory and compare favourably with other reported studies. Randomised patients in the BARI 2D trial, 21 which was designed to test treatment strategies for patients with coronary artery disease and diabetes, achieved levels of medical therapy at the three-year follow-up visit similar to ours (aspirin: 94.2%, statin: 95.4%, beta-blocker: 87.9%, ACE or ARB: 92.0%), and patients achieved similar levels of cholesterol and blood pressure (LDL-C: 79 ± 25; systolic BP: 125.2 ± 15.3). In the ACCORD Lipid Study, which evaluated the effects of combination lipid therapy in type 2 diabetes, the investigators found that at the end of the study, approximately 86% of participants were still taking LDL lowering drugs. 22 The mean LDL-C attained was 80 mg/dl with 33% achieving LDL-C lower than 85 mg/dl.
Quality measures intended to narrow the gap between knowledge and actual practice, including collaborative initiatives and registries such as Get With The Guidelines 23 and other programmes,10,24 provide important information of continued performance improvement. However, previous reports have almost exclusively defined quality as percentage of subjects on therapy or the mean achieved LDL cholesterol. As our data shows, it is also important to track how well the guidelines-specified goal is attained. Failing to do so may risk masking important limitations which may have an impact on outcomes. Gagliardino et al. 25 compared metabolic monitoring and outcomes and coronary risk status in people with type 2 diabetes from Australia, France and Latin America, and found striking similarities regarding the low percentage of participants who achieved treatment goals. Data has been published regarding intensive medical therapy in patients participating in the COURAGE trial. 26 In that trial there were 766 patients with diabetes, and it was not published how many of them achieved the therapeutic goal of LDL-C ≤ 70 mg/dl. However, among the entire cohort of subjects, 46% achieved the goal with a mean LDL-C of 72 mg/dl. Physician compliance with the guidelines has been the subject of interest for a long time. Previous reports of low physician prescription rates of evidence-based medicine have resulted in several collaborative initiatives aimed at improving compliance. Recent reports have shown that these strategies have resulted in improvements in quality of care.24,27 However, these reports evaluated the proportion of patients prescribed medication but did not analyse how many achieved treatment goal.
For the high risk patient group, such as those with diabetes and concomitant coronary heart disease, it is important to ask whether we are treating to goal because of the strength of evidence for aggressive lipid reduction. Our study did not evaluate the mechanistic factors for failure to achieve goal, but we speculate the reasons may be multifactorial and may include physician inertia, adherence issues, patients who may be difficult to treat, failure to implement lifestyle changes, and inappropriate use of therapeutic substitutions.
Limitations
Our study is an observational study from one academic medical centre and as such the results may not be easily generalisable. Our institution is a major referral centre with a wide catchment area. For patients referred from communities far from us, their labs are usually drawn and run in their local communities and the results faxed to us. Manual entry of these results into our hospital computer system may lend itself to errors. Patients with comorbidities such as cancer or liver disease, or who were otherwise intolerant to statins, were not excluded, which may have confounded results, although we would have expected this to increase the number of people reaching goal. Next, we regret the fact that we currently have no outcomes data to report. Outcomes data will admittedly require longer time of follow-up, and it is our intention to evaluate the effect of our performance on outcomes. Another limitation is that we were unable to consistently determine individual compliance with prescribed medications during serial visits. We did not track patients receiving other lipid agents, such as fibrates or niacin, since during the study period physician use of these other medications had gone through fluctuations due to unfavourable or negative outcomes studies.
Summary
Similar to other investigators, our study shows that the majority of high risk patients with diabetes and coronary heart disease do receive recommended medications. When analysed in terms of drug prescription or mean targets achieved, one gets the impression that we are doing well. However, when examined from the perspective of percentage achieving guideline target, it is apparent that many do not achieve therapeutic goal. This has significant implications on further improving quality of care in patients at high risk. Efforts to evaluate mechanisms aimed at the overall system of care beyond the traditional hospital or individual physician–patient dynamics may be necessary to bring the benefit of evidence-based medicine to many patients.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest statement
The authors declare that there is no conflict of interest.
