Abstract
Patients with borderline personality disorder (BPD) are overrepresented in compulsory inpatient care for suicide-protective reasons. Still, much evidence indicates negative effects of such care, including increased suicide risk. Clinical guidelines are contradictory, leaving clinicians with difficult ethical dilemmas when deciding on compulsory care. In this study, we analyse the arguments most commonly used in favour of compulsory care of BPD patients, to find out in what situations such care is ethically justified. The aim is to guide clinicians when deciding on compulsory care for BPD patients and reduce the use of potentially harmful care. The arguments analysed are (a) the patients lack decision competence, (b) the patients lack authenticity, (c) compulsory care saves the patient from suicide, (d) compulsory care safeguards against litigation, complaints, or doctor's anxiety, (e) compulsory care is a practical solution in emergencies, and (f) it is better for the caregiver to ‘err on the safe side’. We conclude that compulsory care is not ethically justified in most cases unless the clinician has probable reason to believe that the patient lacks decision capacity by suffering from a severe mental co-morbidity and stands to benefit from such care.
Introduction
Borderline personality disorder (BPD) is a psychiatric diagnosis in the DSM V, 1 which describes a set of personality traits that cause significant suffering and dysfunctionality for the patient. BPD can be understood as a developmental disorder with consistently fluctuating symptoms from early adulthood and on through life. Patients with BPD often display difficulties regulating and containing negative emotions that commonly arise when interacting with other people or facing everyday adversities. The difficulties often entail rapid mood shifts, interpersonal problems, and dysfunctional coping strategies – like using suicidality and other forms of self-harm behaviour to handle negative emotions and emotionally challenging situations. Other symptoms are a shifting sense of identity, shifting future plans, and a chronic sense of inner emptiness. When in distress, BPD patients can also experience transient dissociative symptoms, which mimic those of psychosis.1,2
Considering the BPD patients’ emotional instability and suicidality, one may ask if there are reasonable grounds for questioning compulsory care for patients with BPD. After all, it seems intuitively like the right thing to do when the patient is in crisis and risks harming themself.
However, here we will argue, primarily from an ethical perspective, that it is in the BPD patient's best interest for the doctors to be more restrictive with compulsory care than is the case in many psychiatric clinics today. The ethical analysis will include both consequentialist considerations of beneficence and harm reduction and deontological considerations based on respect for autonomy.
BPD patients are generally considered to have the mental capacity to decide about the care offered, even though this capacity has been debated when it comes to situations of increased suicide risk.3–7 From an ethical point of view, the lack of such capacity is arguably a requirement for treating a person under compulsory care. 8 At least, the presence of decision-making capacity makes compulsory care more difficult to defend since such care would go against the principle of autonomy and constitute hard, rather than soft, paternalism. Hard paternalism means that a decision-competent patient is treated against their will but in their best interest, regarding the care decision in question. Conversely, soft paternalism implies such care when the patient is decision-incompetent. 8 We will develop these points further below.
Because of their frequent suicidal behaviour and relentless crises, BPD patients are often admitted – voluntarily or compulsorily – to inpatient care and are overrepresented among younger adults in such care both in Sweden and other Western countries.9–13 However, the collected experience from the last decades points to no, or negative, effects of such suicide-protective measures. The negative effects of inpatient care for BPD patients include an increase in suicidal behaviour (independent of pre-admission suicide risk), an increase in regressive behaviour, and a loss of skill in how to handle negative emotions and crises by oneself.2,13–17 Consequently, many clinical guidelines advise against inpatient care and overtaking patient autonomy, like compulsory care. 14 Even so, inpatient compulsory care is still frequently used for patients with BPD, mostly young women, with acute suicidality being the main reason for doing so.10,11 This is supported by some clinical recommendations on how to handle suicidal patients. 18
Based on the above, care providers are confronted with difficult choices and trade-offs when deciding on compulsory care for BPD patients. Firstly, these patients do not respond positively to compulsory or voluntary admittance to the hospital, and yet such action is frequently taken.9–13 Secondly, the clinical guidelines seem contradictory when it comes to handling BPD patients in suicidal situations, leaving the care provider with little decisional support.15,18 Thirdly, the patient's mental capacity to decide on the care offered has been debated in situations with increased suicide risk.3–7 Our paper aims to shed some light on these matters and provide clinicians with better guidance when deciding on compulsory care of BPD patients.
We will address some commonly used arguments5,19–21 that have been used in defence of compulsory care (Figure 1) through the looking glass of medico-ethical principlism, which maintains that healthcare decisions should be beneficial to the patient, not do harm, respect a decision-competent patient's autonomy, and that equal cases should be treated equally. 8
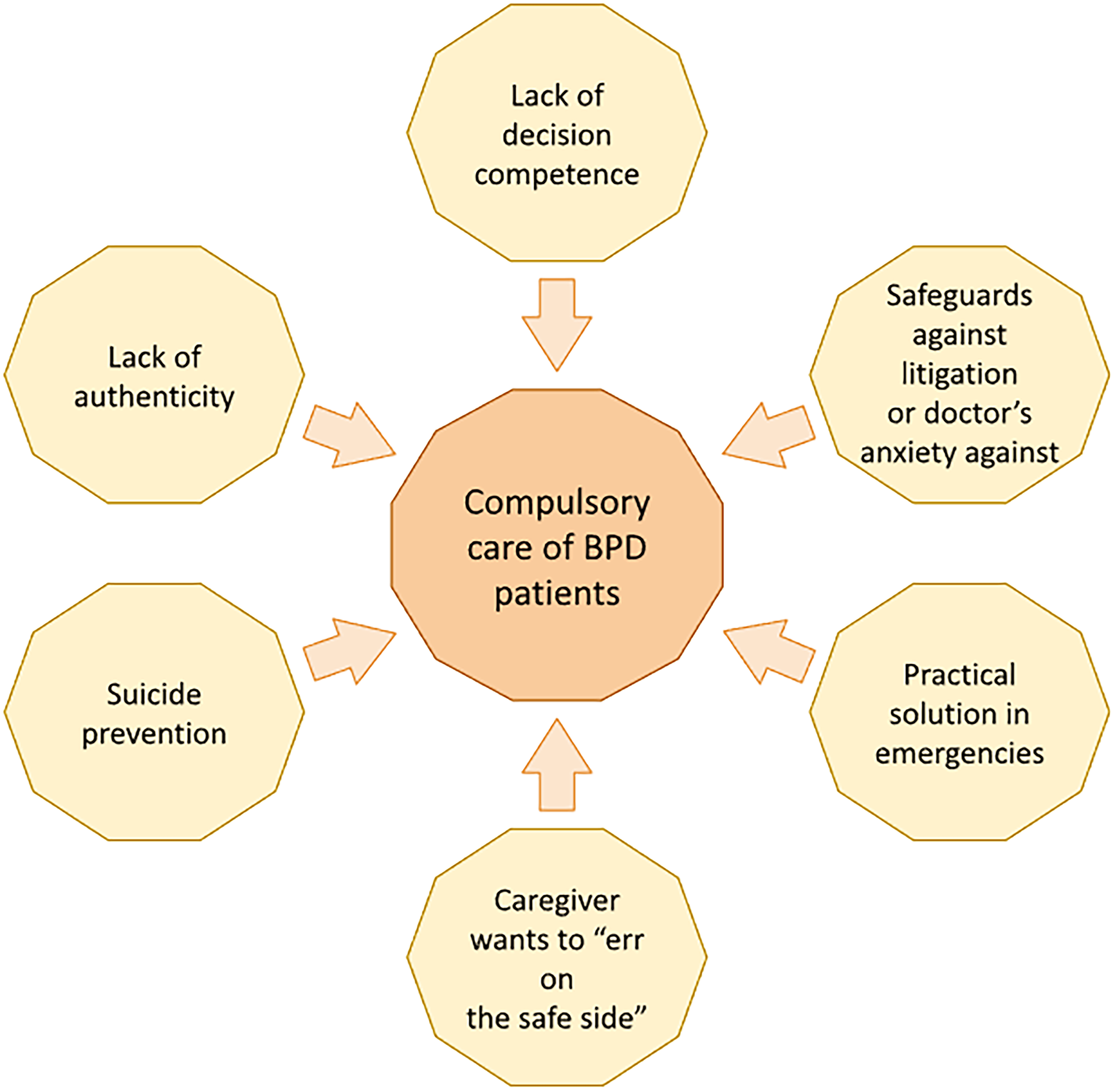
Arguments used in defence of compulsory care of BPD patients. BPD: borderline personality disorder.
Lack of decision competence justifies compulsory care
One argument proposed in defence of compulsory care of BPD patients is that these patients lack decision competence, at least, in situations when they are upset and have suicidal thoughts. According to the principles of biomedical ethics, as described by Beauchamp and Childress, 8 the patient's consent to or refusal of treatment should be respected when informed, voluntary, and autonomous. A prerequisite for being autonomous is being decision-competent. Conversely, forcing the patient into care is only ethically justified when the patient is decision-incompetent to decide about the care offered. 8 The legislation on compulsory care differs between countries and not all countries have decision incompetence as a prerequisite for treating a patient against their will. However, some countries do, like the Mental Capacity Act of England and Wales. 22
Decision competence in clinical practice
Decision competence comprises the ability to formulate a preference, understand information, appreciate one's situation, reason around the likely consequences of one's decision, and reach a decision in light of what one wants to achieve. 23 This ability is usually tested with the ‘MacArthur Competence Assessment Tool – Treatment’, MacCAT-T. 24 The patient is to be assumed to have decision competence unless the care provider can prove otherwise.5,22 Also, the assessment should be independent of the patient's decision and the consequences of that decision.19,22
BPD patient's decision competence
If the BPD patient is assessed as decision-incompetent to consent to care, then compulsory care could be ethically justified, at least provided that the care in question is in the patient's best interest. On the one hand, some argue that BPD patients in crisis can be interpreted as decision-incompetent because their emotional state makes them disregard risks, thereby compromising their ability to use and weigh information.5,19,20,25 Others point to the BPD patients’ neurocognitive aberrations from normative functioning, like risky decision-making, impaired empathy, and reduced mentalisation abilities, 26 when arguing for the patients’ decision incompetence. On the other hand, the limited empirical evidence so far points to BPD patients being mostly decision-competent, as measured by using the MacCAT-T – even during crises.3,4,24 This resonates with the collected body of clinical experience, describing BPD patients as competent and cognitively intact agents who can learn skills on how to handle their emotional crises constructively with the right guidance.2,3,27,28
Conclusion
Taken together, studies and clinical experience of BPD patients’ decision competence so far give us reason to believe that they should generally be assessed as decision-competent even if in an upset state. Of course, there could be exceptions, e.g., if affected by some co-morbid state that affects their cognitive abilities in a significant way. We conclude that the argument of decision incompetence lacks empirical support.
Lack of authenticity justifies compulsory care
Rather than the ability to cognitively understand, process, and make a decision on the information given, the crux of the matter seems to be whether the BPD patient's desires underpinning their decisions are autonomous, especially if those desires are self-destructive.5,29 Non-autonomous desires, not aligned with the person's continuous psychological identity, are called inauthentic. 30 Hence, one could argue that the self-destructive BPD patient's lack of authenticity in their decision-making justifies compulsory care.
Authenticity in clinical practice
The Mental Capacity Act of England and Wales does not explicitly mention authenticity as a condition for being autonomous, but by stating that the patient must be able to ‘use and weigh’ relevant information about care options, some have made the interpretation that patients, whose weighing of information could be affected by their underlying disorder, are not autonomous because their priorities are not authentic, i.e. not really their own.5,22,29 This element of the MCA seems to have caused interpretative difficulties and disagreements, like in a case when the patient with a long-term eating disorder had cognitive decision capacity but their self-destructive desire was considered pathological and hence non-autonomous. 29 This could be seen as an example of how a lack of authenticity is used as a motive for compulsory care of self-destructive psychiatric patients – maybe, because it is intuitively difficult to accept that self-destructive decisions can be authentic. At the same time, the MCA states that a person should not be treated as lacking autonomy just because their decision is ‘unwise’. 22
In clinical practice, however, the latter seems only to apply to non-psychiatric patients. When, for example, a decision-competent cancer patient refuses life-saving treatment their authenticity is rarely disputed – even if one could argue that they could have desired differently had they not had cancer – but when a decision-competent psychiatric patient refuses life-saving care their authenticity is often questioned because, without their mental disorder, they would have desired differently – or so it is argued. Some have interpreted this as a form of discrimination against psychiatric patients. 29
The authenticity of BPD patients
Having an unstable sense of identity is one of the core symptoms of BPD. 1 It has been argued that BPD patients lack a temporally coherent and overarching identity since their narrative of self is fragmented and compartmentalised. 31 One explanation could be the BPD patient's intense emotional reactions to adversities, which narrow their perspective on themselves and the world to the absolute present, cutting them off from past and future projections of self. Another explanation is their dichotomous shifts in how they perceive themselves and the world, depending on mood and context, and their ability to transform themselves in a chameleonic way to fit into social settings and feel accepted by others. These shifts in narrative identity, with corresponding changes in future plans and zest for life, can fluctuate within the same day.1,2,26,31
Difficulties and risks of using the authenticity concept in clinical practice
Considering the above, one could maintain that BPD patients are chronically inauthentic, or – since nobody can be chronically inauthentic, by definition –, that their lack of a continuous narrative identity, or a ‘core self’, is the very nature of their authentic selves. This makes the concept of authenticity difficult to use for BPD patients – what psychologically continuous beliefs and desires are the assessing psychiatrist going to refer to? This problem may not be confined to BPD patients, since, generally, people's narrative identities can change – more or less – over time. 32 Therefore, it is difficult to use the concept of authenticity in clinical practice. This notion is supported by previous work, criticising the use of authenticity in healthcare – not least because there is no reliable and objective way of assessing authenticity. 30 This assessment problem conveys a risk that the psychiatrist presumes that the BPD patient's authentic desires are aligned with what the psychiatrist thinks is best for them. That would open up for hard paternalism, meaning that the care provider overrides the wishes of a decision-competent patient in their best interest and thereby disrespects the patient's right to autonomy.8,30
Of course, one can contend that hard paternalism is justified when BPD patients are displaying suicidal behaviour – we will discuss this in the next section – but that does not need to involve authenticity. Even though it has been argued otherwise, there is no strong support for saying that a desire must be inauthentic just because it is self-destructive, because the person chooses to disregard risks, or the person is upset.30,33 If so, only calm, constructive, and prudent people's desires would be considered authentic.
Conclusion
To sum up, on the face of it, a lack of authenticity may seem like a reasonable motive for compulsory care – that the person is acting out of character and therefore non-autonomously. But, again, the concept is vague and difficult to use in clinical practice, risking arbitrary interpretations and hard paternalism. Also, one core feature of BPD is having a chronically unstable sense of identity, and this makes the authenticity concept even more difficult, not to say impossible, to use. Our conclusion is therefore that the argument of lacking authenticity is too weak to justify the use of compulsory care for BPD patients.
Compulsory care saves the patient from suicide
As mentioned above, some may argue that it is justified to apply hard paternalism to BPD patients to save them from committing suicide.
Suicide prevention by compulsory admissions
Compulsory hospitalisation has not been shown to have a suicide-protective effect on BPD patients in any controlled studies. Conversely, the pooled empirical experience from several decades has indicated negative effects, like an increase in suicidal behaviour and loss of self-caring abilities, when BPD patients are hospitalised for suicide-protective reasons2,13,15,34 or when treated under compulsory care. 35 These negative effects seem to show after around three days of compulsory admission. 21 Compulsory hospital stays shorter than 3 days have not shown either positive or negative effects.15,21 Nonetheless, one RCT study of BPD patients indicated that psychiatric crisis service utilisation by itself, including emergency room visits and previous inpatient treatment, conveys an increased risk for suicide attempts. 13 This could imply that even very short contact with emergency and inpatient settings can confer an increased suicide risk for BPD patients.
Suicide prevention by short compulsory admissions
Some could argue that since there is limited proof of very short compulsory stays causing harm, the care provider should play safe and detain the patient at least for a few days. But this would be an ‘appeal to ignorance’ logical fallacy: Just because there is limited proof that very short compulsory stays cause harm, the collected evidence does not give us reason to believe that short compulsory stays are beneficial or non-harmful. Also, disrespecting the BPD patient's autonomy comes with a cost, e.g. by decreasing their already low self-reliance, reinforcing their actively passive solution methods, and depriving them of learning skills on how to manage their emotional crises autonomously in the future.2,13,15,27,34 Moreover, disrespecting someone's autonomy is in itself an ethical cost. These costs cannot be disregarded when there is no support the action is compensated by a surpassing positive outcome.
Value of suicide risk assessments
Another problem with this argument is that the tools used to assess suicidality have poor to no clinical value for the individual and can lead to faulty prioritising of who should be admitted to hospital care.36–39 Suicide risk assessment tools have a low short-term positive predictive value (PPV), referring to the proportion of patients identified as high-risk who die by suicide. Even if hypothetically optimal tests with 95% sensitivity and 95% specificity existed, the PPV would be around 1% since suicides occur rarely. One of the best tests today, the Columbia-Suicide Severity Rating Scale screen, has a short-term PPV of 0,2%, meaning that out of 500 patients assessed with high risk, only one will commit suicide in the near future. Therefore, it can be maintained, balancing respect for autonomy with possible beneficence, that clinicians do not have the tools to predict suicide with enough accuracy on an individual level to justify, for example, compulsory interventions. 39 Especially, since the use of compulsory inpatient care may confer an increased suicide risk by itself, sustaining years after discharge – a claim that will be discussed in more detail below.39,40 Instead, it has been argued that clinical measures should be based on the patient's needs, irrespective of perceived suicide risk. 36
Suicide prevention by compulsory admission in cases of co-morbidity
BPD patients in crises are commonly assessed as having additional diagnoses, such as depression, which are used to justify compulsory inpatient care when they are considered suicidal. 6 Of course, the patient could suffer from a comorbid state that is best treated in a hospital but if the main purpose of doing so is to reduce suicide risk the intervention can still be questioned. Psychiatric inpatient care has thus far not shown suicide-protective effects in controlled studies (such studies are difficult to perform), even if there is some evidence to support that it may do so for some patients, e.g. elderly male patients.41,42 From clinical experience, one could hypothesise that these could be patients with melancholic depression, who are not capable of participating in outpatient care and can be successfully treated in the hospital. Still, a meta-analysis of studies from all over the world over the past 60 years, concluded that psychiatric hospitalisation seems to confer a higher suicide risk than any other known factor, with an association between psychiatric hospitalisation and suicide that is statistically stronger than the association between smoking and lung cancer. 43 The suicide risk can be elevated for years after discharge. Even if it is difficult to prove causality and a large part of the association could be a result of patient selection, it has been argued that the strong association, repeatedly observed by different researchers over time and in different places, together with weak association with suicide risk at admission, a dose–response relationship between the amount of hospital care and suicide, significant variations in suicidality between clinics, and accounts of psychological harm from coercion and confirmed feelings of helplessness during admissions, could suggest a certain causal association between psychiatric hospitalisation and suicide. Or, at least, that hospitalisation does not seem to be an effective tool to prevent suicide.17,39,40,42–45 This is supported by a recent study, indicating an association between post-discharge suicide attempts and perceived coercion during admission – even after adjustments for co-variates. 46 Also, some studies have indicated that the intervention of keeping patients behind locked doors in the hospital, compared with open doors, be it BPD patients or others, does not decrease suicidality and may even increase suicidal behaviour.15,47,48 In summary, there is reason to question the idea that coercively admitting patients to the hospital has a suicide-protective effect for patients in general.49,50 This also speaks against using compulsory care if the main purpose is to prevent suicide.
Conclusion
Taken together, this intuitively appealing motive for using compulsory care on BPD patients to prevent suicide lacks empirical support. The cost of depriving the patient of their right to autonomy does not seem to be compensated by a larger consequential benefit. Therefore, we find that the argument must be rejected.
Compulsory care safeguards against litigation, complaints, or doctor's anxiety
Some may claim that compulsory care should be justified as a means to safeguard doctors against anxiety, conflicts, and medico-legal repercussions – clinical measures which go under the name ‘defensive medicine’. 51 If such measures are not taken, doctors will suffer, patients will be disappointed, and society's trust in psychiatry could decrease – or so it could be argued by the doctors who practise defensive medicine.
Defensive medicine in the treatment of BPD patients
Studies have indicated that a majority of mental health providers have made clinical decisions, like applying compulsory care, that were not in the BPD patients’ best interest but, instead, to protect themselves from conflicts or criticism52,53 One explanation could be that, in medicine and society, there are strongly held and generally accepted beliefs that suicide is almost always the tragic consequence of a treatable mental disorder, 54 which means that acutely suicidal patients should be hospitalised – by force if needed – to reduce suicide risk. 18 Even though research and clinical experience give us good reason to question those beliefs, as argued above,2,13,14,17,37,40,55,56 they still influence clinical guidelines on how to treat suicidal patients 57 and affect how supervising authorities assess complaints and medical culpability post-suicide. 18 These circumstances could explain why many doctors practice defensive medicine to protect themselves from litigation and blame.51,52,54
Psycho-social circumstances underpinning the motive
The argument is understandable from a psychological point of view. When a society embraces certain beliefs as truths, it may take a large amount of evidence and support from respected authority figures to change those beliefs. For a single person to act against generally accepted ideas takes courage and conviction. These phenomena can be explained by people's tendencies to social conformity and following established routines (so-called path dependency), adjusting their beliefs to the group (the so-called bandwagon fallacy), and resistance to changing opinions.58–62 Analogously to these social phenomena, if the medical society, supervising authorities, and the patients, hold that certain ideas and practices are right, it is difficult for single doctors to practice against the norm and thereby risk litigation – even if the norm-b
Psycho-social circumstances can be changed
On the other hand, the clinical norms, regarding the use of compulsory care for self-harming BPD patients, seem to differ significantly between psychiatric clinics.10,11,21 Hence, it seems reasonable to assume that switching from one norm to another could be possible. One can hypothesise as follows: once a new practice is embraced by a critical number of doctors in a clinic, the clinical norm can change rapidly. Then, the new practice may also get accepted by the local supervising authorities, patients, and relatives, and the need for compulsory care as a defensive measure against litigation could decrease.
The motive from an ethical viewpoint
Even if the argument is psychologically understandable, according to medico-ethical principles, one should only exercise compulsory care for the sake of the patient and when the patient is decision-incompetent. 8 We have argued in this article that neither of these conditions is fulfilled for this patient group.
Conclusion
This motive is foremost an expedient one, putting the doctor's interests before the patient's, which is not compatible with medico-ethical principlism and the principle of using compulsory care in the patient's best interest. 8 Hence, the argument is rejected.
Compulsory care as a practical solution in emergencies
When BPD patients enter the emergency room, they are usually in crisis; emotionally upset and oftentimes ambivalent about the care offered.2,63 Suicidal communication and self-harm behaviour (including self-cutting or intoxication with or without suicidal intent) are common.13,15 If the patient is assessed as decision-incompetent, then compulsory care may of course apply, provided it is in the patient's best interest. 29 But even if that is not the case, it can be challenging for the doctor to handle the emotionally charged situation without admitting the patient involuntarily under the Mental Health Act. 20 Hence, compulsory care could be considered justified as a practical solution in emergencies.
Emergency room situations
The situation pictured above tries to show how chaotic and unnerving it can be for the doctors in the emergency room to handle suicidal BPD patients. In the aftermath, one can criticise the use of compulsory care when used as a practical solution, but it is probably understandable for those who have worked in psychiatric emergency units: stress levels are usually high, you have limited time for each patient, you risk criticism and litigation if the patient self-harms under your ‘watch’, there may be assertive relatives or authority figures who demand you to forcibly admit the patient, the patients sometimes indicate they want to be forcibly admitted, you may feel uncertain of the diagnosis, and if you sway the patient into accepting voluntary admission, they may change their mind later during the night and you are back to square one. 20
Response to the emergency-related motives
As understandable as it may be that doctors apply low-threshold use of compulsory care in the emergency room, the question remains whether it is ethically defensible when the patient is predominantly decision-competent and compulsory care is not in the patient's best interest. If we look at the paragraph above and address the problems described in emergency units, we can respond as follows: high-stress levels and extra workload for the doctors in the emergency unit are, for obvious reasons, not sufficient arguments for ethically justifying compulsory care. Compulsory care as a means to handle fear of litigation, doctor's anxiety, and complaints from other stakeholders, was rejected in the former section. Compulsory care on the BPD patient's request, as a form of ‘Ulysses contract’, has been argued not to justify compulsory care 56 – this will be explained further below. The suicidality argument has been rebutted previously in this text. This leaves us with the argument of diagnostic uncertainty to justify the practical low-threshold use of compulsory care.
Diagnostic uncertainty as a motive for compulsory care
As described in the Introduction, the burden of proof lies on the doctor when assessing the patient as decision-incompetent to decide on the care offered.5,8,19 This entails that, if there is uncertainty about whether the patient is decision-incompetent, the patient should be assessed as decision-competent until proven otherwise.5,19
However, there could also be uncertainty about whether the patient suffers from some additional mental disorder, which could require psychiatric hospitalisation. For example, if a patient lacks a diagnosis from before and displays high levels of emotional distress, perhaps even violent or erratic behaviour, it could be difficult for the on-call doctor to dismiss a comorbid psychotic disorder. In such cases, decision competence may be difficult to assess and there could be a reason to assume decision incompetence since psychotic patients usually present with a higher degree of decision incompetence, compared with BPD patients. 3 Combined, these diagnostic uncertainties and the patient's precarious behaviour may leave the doctor with probable reason to believe that the patient lacks the capacity to decide on their care and should benefit from compulsory hospitalisation to treat the condition. Under such premises, the care harmonises with medico-ethical principlism. 8 Therefore, short-term (e.g. overnight) compulsory care for observation and retrieval of more information seems ethically justified in those situations – even if it later turns out that the patient is indeed decision-competent.
Compulsory care on the BPD patient's request, as a form of ‘Ulysses contract’
Sometimes BPD patients communicate suicidality or acute distress to their environment, which brings them to the psychiatric emergency unit. However, once there, the patient sends mixed signals to the care provider: that they may harm themselves if not admitted to the hospital but at the same time that they will not accept voluntary admission because they cannot trust themselves. This could be compared to a form of ‘Ulysses contract’ or advance statement, in that the patient requests compulsory admission to prevent themselves from giving in to near-future suicidal impulses.20,56 In a previous normative study, 56 arguments in favour of compulsory care on the BPD patient's request were scrutinised but rejected since this form of compulsory care could neither be justified from a clinical, legal, nor ethical perspective. The reasons being, for example, that BPD patients are mostly decision-competent and therefore should have the right to reject the care offered at any time, that the concept of authenticity is too vague to be used in the clinic and could open up for hard paternalism (as argued above in this text), that the patients do not benefit from such care, and that the concept lacks legal support – especially when it comes to coercive measures on a decision-competent BPD patient who no longer wishes compulsory detention. 56
The risk of extinction bursts
In addition to the situations described above, there is the problem with so-called extinction bursts, which we will now explain. BPD patients sometimes expect the doctor to subject them to compulsory care when they express suicidal thoughts and may take comfort in having the burden of self-responsibility lifted off their shoulders. 21 Unfortunately, this alleviation of autonomy seems to reinforce the BPD patient's suicidal behaviour, as explained previously.2,13,34 When the doctor avoids reinforcing the suicidal behaviour, for example by refraining from using compulsory care, the patient may react with a temporary escalation in suicidal communication and suicidal behaviours – before the suicidal behaviour decreases, or, in the best case, is extinguished. This phenomenon is known as ‘extinction bursts’ and is not uncommon for patients with self-harm behaviour. 17 Still, in our experience, it sometimes causes anxiety among emergency room staff and some doctors resort to ‘giving’ the patient compulsory care just to avoid an extinction burst on their shift. As a consequence, one could argue that the risk of extinction bursts justifies the use of compulsory care. Yet, since that handling is associated with reinforcement of suicidal behaviour, there is probable reason to believe it means doing the patient a disservice. A better option could be to inform the patient of why compulsory care is avoided and offer, for example, voluntary overnight admission or telephone support at home. Even if that would lead to an extinction burst, the patient has not been rejected care and, after the temporary burst, in our experience, the patient usually accepts voluntary care alternatives. 17
Conclusion
In summary, generally, compulsory care as a practical solution in emergencies does not comply with the medico-ethical principles of beneficence, non-maleficence, and respecting the decision-competent patient's autonomy. 8 Having said that, there could be situations when the patient's behaviour makes it difficult to dismiss a severe psychiatric condition, like a psychotic state, and there is probable reason to believe that the patient lacks decision competence. In such situations, we conclude that short-term compulsory care can be ethically justified to evaluate the condition and reassess the patient's decision capacity.
Compulsory care is justified when the caregiver wants to ‘err on the safe side’
Above, we described a situation in which the BPD patient behaves so erratically that the on-call doctor may have probable reason to believe that they are decision-incompetent and in need of hospitalisation. Consequently, short-term compulsory care for further observation could be justified. From this conclusion, some may extrapolate that all diagnostic uncertainties in the psychiatric evaluation of suicidal or violent patients should be taken as a pretext to forcibly admit the patient, because, as doctors sometimes say, ‘it is better to err on the safe side’. 25 If hospitalisation is the safe alternative in such situations, then compulsory care could be ethically justified.
Using the precautionary principle as a justification for compulsory care
The idea of ‘erring on the safe side’ can be tied to the precautionary principle. The basic idea of the precautionary principle is that measures against a possible hazard should be taken even if the existence of such a hazard lacks solid scientific support. A stronger definition says that actions that may produce severe harm should not be undertaken unless it has been shown that they do not impose too serious risks. However, this principle does not mean that action should never be taken when there are risks involved. Instead, it includes balancing the risks of both taking and not taking a precautionary action; there is only a ‘safe option’ if it carries no risks whatsoever – and that is rarely the case in reality. But then, doctors wanting to err on the safe side may equate ‘safe’ with ‘the least risky’ side. If compulsory care is to be justified by the precautionary principle, then the benefits of using such care must outweigh the risks of not doing so, even if we, in line with the precautionary principle, put more weight on negative outcomes than benefits.64,65
Balancing risks with benefits when using compulsory care for BPD patients
The risks involved when deciding on compulsory care for BPD patients, could, for example, be death by suicide, harm to others, and the risk of missing a severe condition that requires inpatient treatment. We will address these risks one by one below and evaluate, using the precautionary principle, whether they can be used in favour of compulsory care.
Compulsory care as a precaution against suicide
Further up in this text, we have elaborated on the lack of empirical support for compulsory care having suicide preventive effects for BPD patients. Having said that, BPD patients still carry an increased suicide risk, and, as of yet, no treatment option can reduce that risk completely. In other words, there is no ‘safe’ option when it comes to suicide risk in BPD patients, only a statistically less risky one. What we know is that the evidence points to lower suicide risk when BPD patients are treated as agents and hospitalisation is avoided, and that seems to include very short hospital stays – even if there is less evidence supporting the latter claim.2,6,13,14 On the other hand, no controlled data support the opposite – that compulsory inpatient care or hospitalisation, in general, has suicide-preventive effects for these patients.13,15 Therefore, the argument that compulsory care can be used as a precautionary measure to prevent suicide does not hold water. If anything, erring on the safe side would entail avoiding compulsory admission or, at least, not detaining the patient for longer than a day or two.2,13,15,21
Compulsory care as a precaution against harm to others
Just as arresting a person can temporarily decrease the risk of the person causing harm, so can detention by compulsory care. Still, this measure does not comply with the medico-ethical principle that compulsory care should primarily be given in the patient's best interests – not in the best interests of others. 8 The long-term negative consequences of using psychiatry as an extra-judicial form of prison probably exceed the short-term benefits of locking potentially violent patients up in hospitals. Unless, of course, the violence is secondary to a severe mental condition that can successfully be treated in the hospital – but this is not the case for BPD patients, as argued above. In addition, using psychiatry as a corrective institution could decrease society's trust in psychiatry and deter patients from seeking mental health care when in need. This is certainly a risk too, invoked by using compulsory care. Balancing risks and benefits, compulsory care should not be used as a precautionary measure to prevent harm to others.
Compulsory care as a precaution when there is diagnostic uncertainty
In the emergency room, in which there is limited time for observation of the condition, there is a risk that the on-call doctor misses a severe co-morbidity that could have justified compulsory care, like melancholic depression or psychosis. Still, the behaviour of BPD patients in crisis is usually not typical for the symptoms of psychotic or melancholically depressed patients. BPD patients in crisis rarely display the psychomotor inhibition and excessive feelings of guilt of a typical melancholically depressed patient, and their dissociative – psychotic-like – symptoms are more transient, cohesive and figurative than those of a typical psychotic patient. 1 Correspondingly, severely depressed or psychotic patients rarely display the common symptoms of a BPD patient in crisis: presenting themselves as helpless and incompetent, regressive body language (e.g. sitting in a foetal position, face buried between their knees (the author's own experience)), assigning blame to others, active passivity (e.g. communicating need of help and at the same time not cooperating when the help is offered), acting out physically when not receiving the help they want, distractable and context-dependent symptoms.2,6,20 To sum it up, in most cases, there should be little room for diagnostic uncertainty if the on-call doctor is familiar with the typical symptomatology of different psychiatric disorders. Still, there is a tendency for doctors to diagnose an additional severe disorder to legitimise the use of compulsory treatment and thereby avoid the moral dilemma of potentially causing harm by forcibly detaining the patient.66,67 In such cases, a purported diagnostic uncertainty does not compensate for the previously described negative effects of detaining BPD patients under compulsory care.
Conclusion
When balancing the risks and benefits of detaining the BPD patient as a precautionary measure, most evidence so far indicates that the probable negative effects exceed the positive effects, even if one can never guarantee the outcome for a single patient. Compulsory care of a decision-competent patient also implies violating their right to autonomy – something that is rarely mentioned when debating the use of compulsory care. Overriding a person's autonomy is inherently undesirable, and perhaps especially so for BPD patients, whose symptoms can be compounded by such care. The point is this: there is no safe side to err on since all alternatives have possible negative outcomes (risks) and positive ones (benefits) in this context. And, as we have argued, there is scarce support to suggest that the risk-benefit ratio is, in general, poorer if one abstains from compulsory care than if one exercises it, quite the contrary. In summary, when looking at the use of compulsory care through the lens of the precautionary principle, it is difficult to find situations when it is justified.
Concluding remarks
Our normative analysis concludes that compulsory care of BPD patients is not ethically justified in most cases – unless there is probable reason to believe that the patient is decision-incompetent, e.g. due to a severe co-morbid disorder, and stands to gain from such care. In the latter case, the doctor's decision does not conflict with medico-ethical principles of respecting the patient's autonomy, giving beneficial care and avoiding causing harm to the patient. 8
Resistance to change
Still, we believe that there will be resistance to decreasing the use of compulsory care for suicidal BPD patients. It is difficult to change work practices that have been around for a long time and have strong emotional support.61,62,68 The idea of saving the patient by hospitalising them and overtaking their autonomy may feel intuitively right: the doctors feel as if they are ‘doing something’, showing their competence and power to save people. Also, the idea ‘better to do too much than too little’ is deeply rooted in doctors’ work routines – taught from generation to generation of doctors. 69 In contrast, transferring responsibility to the patient, intervening less, and medicalising less, could make the doctors feel weak and incompetent to save the patient's life. These challenges must be faced when trying to change the current work practice in a more autonomy-emphasising and evidence-based direction.62,68,70 Still, it is not difficult to conceive of how doctors may resist such change, not least because emotionally charged opinions tend to become reinforced and defended when challenged – even when faced with the strongest of arguments.61,68
Instead of compulsory care, other measures can be taken
BPD patients may not respond well to decreasing their autonomy but other interventions can be more helpful to them. For example, supporting their agency and active participation when planning for their care; offering telephone support in the evenings when they are in crisis; short voluntary hospital stays (1–3 days with pre-determined discharge date) when they seek help to stabilise their emotions (instead of self-harming); providing evidence-based psychotherapies in an outpatient setting; and involving relatives and informing them on how to best treat the patient.2,15,21 Considering the different views on how suicidal patients should be handled, the rationale for avoiding compulsory care should be documented in the patient's medical records – an action that is informative to both the patient and other caregivers and decreases the risk of medico-legal repercussions.
Advance statements, joint crisis plans, and self-referred brief admissions are all interventions that have been tried for patients with BPD.71–74 Theoretically, these measures may sound palatable, since they intend to increase the patient's agency, increase therapeutical alliance, decrease self-harm behaviour, and decrease the need for compulsory care. So far, however, such interventions have not been shown to decrease the amount of inpatient care, self-harm episodes, suicide attempts, deaths, or compulsory care.71,72 On the other hand, patients have felt validated and content with such interventions.73,74
There is always a risk, when working with BPD patients, that interventions done with the best intentions do not entail the expected consequences. Hospitalisation in itself seems to have ‘toxic’ properties for these patients, particularly during longer or involuntary stays, and should be used with caution.2,15,34 The patient (and the doctor) may have an idea that hospitalisation provides a safe space where the patient can regain their emotional balance in a safe environment. That may be true but has little evidential support. When the patient learns that the best way of handling their suicidal crises is to hand over the responsibility for regulating their emotions to others, the result seems to be an increase in regressive and self-harm behaviour rather than the opposite.2,21,34 Still, voluntary short admissions according to a crisis or treatment plan could be beneficial to a limited extent, i.e. if not used too often so that hospitalisation becomes an alternative to learning how to manage crises on their own.2,15 As Westling et al. have shown, 71 self-referred brief admissions could decrease the amount of compulsory care for some patients. In summary, BPD patients seem to appreciate being involved in forming their treatment plans, and considering the above, it could be beneficial if the plan includes a provision to offer short voluntary admissions on the patient's demand if other means to regulate the patient's crisis have failed. However, such a provision should be followed up after some time to check if the use of hospital admissions has had the effect intended.
Lastly, even if there is much to do on a ward or in an emergency unit, doctors and nurses must be given time to explain to the patient why compulsory care is not a good solution and why other alternatives can be better. BPD patients are very sensitive to rejection, and many suffer from low self-esteem and feelings of helplessness. Therefore, it is important to validate their feelings while still treating them as competent agents and maintaining best practices.2,15 In our experience, respectful treatment, even if the patient is discontent with the doctor's decision, is very helpful when helping BPD patients learn new, and more constructive ways, of dealing with crises than being forcibly hospitalised.
Footnotes
Acknowledgements
We thank the consultant psychiatrists and psychiatric residents at Norra Stockholms Psykiatri (Psychiatry of Northern Stockholm), St Görans Hospital, who shared their personal experiences of working with BPD patients and provided relevant aspects to the content.
We also express our gratitude to Dr Lukas J. Meier, who contributed valuable comments on the manuscript. All remaining weaknesses are the full responsibility of the authors.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data availability statement
Data sharing not applicable to this article as no datasets were generated or analysed during the current study.
