Abstract
Objectives
The use of empathy during clinical practice is paramount to delivering quality patient care and is important for understanding patient concerns at both the cognitive and affective levels. This study sought to determine how and when physicians self-report the use of empathy when interacting with their patients.
Methods
A cross-sectional survey of 76 physicians working in a large urban hospital was conducted in August of 2017. Physicians were asked a series of questions with Likert scale responses as well as asked to respond to open-ended questions.
Results
All physicians self-report that they always (69%) or usually (29.3%) use empathic statements when engaging with patients. 93.1% of physicians believe that their colleagues always (20.7%) or usually (69%) use empathic statements when communicating with patients. Nearly one-third of physicians (33%) indicated that using the words “I understand” denotes an empathic statement. Although 36% of physicians reported that they would like to receive more training or assistance about how and when to use empathy during clinical practice.
Significance of Results
Despite the self-reported prevalent use of empathic statements, one-third of physicians indicate a desire for more training in what empathy means and when it should be used in a clinical setting. Additionally, nearly one-third of physicians in this study reported using responses that patients may not perceive as being empathic, even when intended to be empathic. This suggests that many physicians feel uncertain about a clinical skill they believe should be used in most, if not all, encounters.
Keywords
Introduction
Physicians cannot and should not take on the suffering of each of their patients; however, they ought to express empathy. Although empathy has been defined in many ways, it is in essence physician recognition of the patient's experiences, concerns, and perspective, combined with the physician's communication of compassion and an intention to help. Empathy is distinguishable from sympathy and compassion because in showing empathy one acknowledges the other person's suffering. To be sympathetic entails feeling what the other person actually feels, while compassion involves taking steps to alleviate the suffering of another. Empathy requires a physician to recognize a patient's situation, concerns, and perspective, without experiencing the patient's suffering.1,2 The use of empathy during clinical practice is paramount to delivering high quality patient care and is important for understanding patient concerns at both the cognitive and affective levels.3–10
Physician use of empathy is associated with better patient and family experiences, higher patient satisfaction, increased patient compliance, improved patient safety, increased trust, enhanced communication, decreased medical malpractice claims, and reduced anxiety.3–12 Although some physicians have expressed concern that the use of empathy may increase the duration of patient visits, empathy has been associated with reduced visit duration.13,14 Conversely, a lack of empathy may adversely impact a patient's treatment course or impede communication about prognosis.15–17 Communication skills training curricula, such as VitalTalk, exist to train physicians on how to use empathy. Institutional decisions about whether to invest in communication skills training may depend on perceptions of the local physician workforce and their needs and experiences. This study sought to obtain a single institution snapshot of physician perceptions of their own use of empathy, their colleagues’ use of empathy, their experiences with empathy training in the past, and need for further training. This objective of this study was to determine physician perceptions of their own use of empathy and their colleagues use of empathy when interacting with their patients and whether physicians have received training and whether they would be open to engaging in training about what empathy means and when empathy should be used in the healthcare setting. Although many studies focus on patient perceptions of physician empathy, few studies have sought to determine physician's own perceptions of the use of empathy during clinical practice.
Methods
A cross-sectional survey of physicians working within a large multispecialty academic health care network in a Midwestern metropolis was conducted during July and August of 2017 to determine how and when physicians’ own perceptions about the use empathy when interacting with their patients and whether physicians’ believe their colleagues use empathy during clinical practice.
Survey design
An extensive literature review was conducted on physician use of empathy during clinical practice. The survey was designed based on the relevant literature and was reviewed for face validity by experts in empathy research including professors, clinicians, and clinical researchers. The survey was pretested for content validity with practicing physicians.
For the purposes of this study, empathy was defined as “Physician recognition of the patient's experiences, concerns, and perspective, combined with the physicians’ communication of compassion and an intention to help.” The survey indicated this definition prior to posing the survey questions.
In order to measure physician use of empathy when interacting with their patients, the survey included questions that asked the physician to use a Likert scale to indicate whether they: (1) use empathic statements when engaging with patients and whether the use of empathic statements helps them better communicate with patients, have a better bedside manner, and feel that their patients care more about them; (2) whether they believe that their colleagues use empathic statements when communicating with patients; and (3) whether they have received training about what empathy means and when empathy should be used in a healthcare setting and whether they would like to receive more training or assistance about how and when to use empathy during clinical practice. These statements were based on the physician's perceptions of their own use of empathy and their colleagues use of empathy. Additionally, the survey asked respondents to identify words or statements as well as behaviors that they believe are empathic. These open-ended questions included no prompts and allowed respondents to list multiple words, statements, or behaviors. The Universities Institutional Review Board approved this study.
Survey sample
A list of physicians practicing at an academic health center was obtained through a publicly available source. The list included 798 physicians who met the inclusion criteria of being a practicing physician. Non-practicing or retired physicians were excluded from this study. Using a random number generator, 250 physicians were randomly selected to receive the survey.
Survey administration
Surveys were distributed in two waves approximately one month apart. The first wave of the surveys was sent via campus mail in July of 2017. The second wave of the survey was sent via email in August of 2017. The second wave provided a link to REDCap, an electronic survey platform. Study participants were not offered an incentive for participation. Each survey contained a subject identification number which allowed the tracking of non-respondents. All data for this study were entered and stored in REDCap.
Statistical analysis
Descriptive statistics were performed in order to determine physicians’ self-reported use of empathy during clinical practice, physicians’ self-reported perceptions of their colleagues’ use of empathy during clinical practice, and education and training in the use of empathy during clinical practice. Descriptive statistics are shown as relative frequencies and percentages from the total sample size. All analyses were preformed using SAS version 9.4 (SAS Institute, Cary, NC).
Results
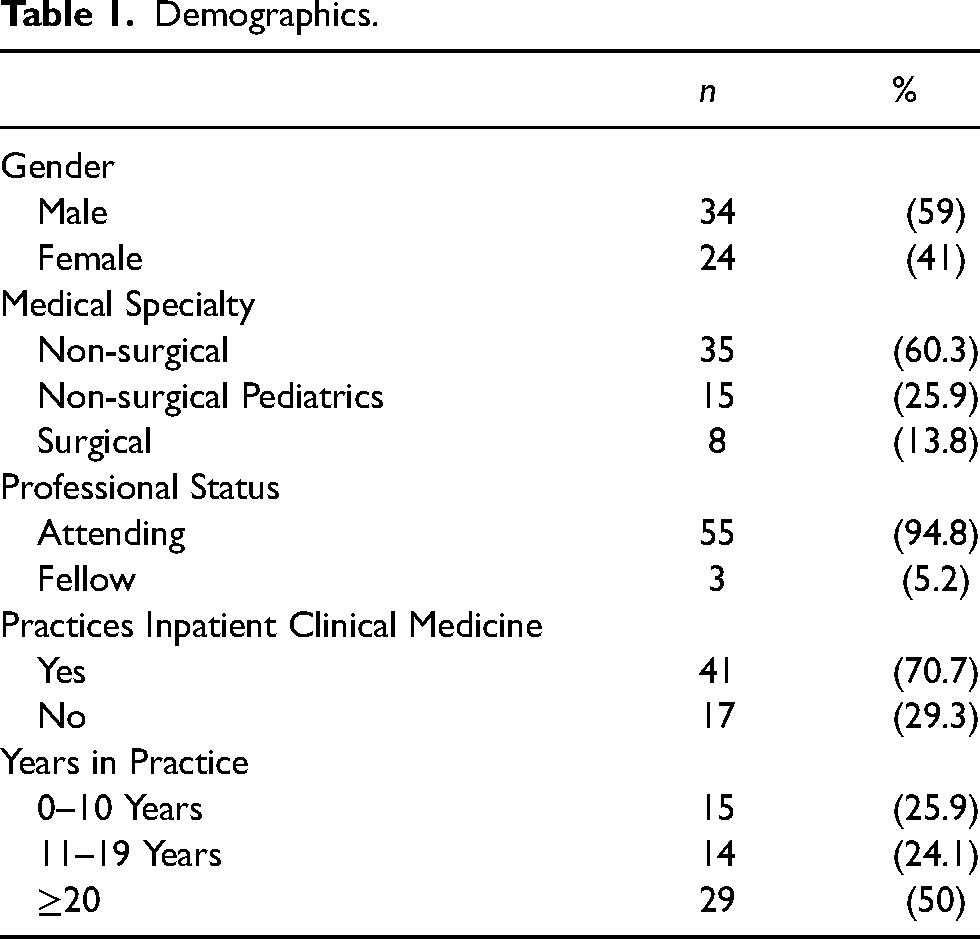
In total, n = 58 physicians completed the survey questionnaire. Survey respondents represented a diverse population of physicians and included 59% male respondents (Table 1). The majority of physicians’ specialties was non-surgical 60%, 26% of physicians were non-surgical pediatrics, and 14% practiced in a surgical specialty; 71% practiced inpatient clinical medicine. Half of physician respondents indicated they have practiced medicine for greater than 20 years, while 24% indicated they have practiced for 11–19 years, and 26% practiced for 10 years or less. There were no statistical differences between physician's years in practice, gender, and age in physician self-reported use of empathy during clinical practice.
Demographics.
All physicians self-report that they always (69%) or usually (29.3%) use empathic statements when engaging with patients (Table 2); 93% of physicians believe that their colleagues always (20.7%) or usually (69%) use empathic statements when communicating with patients; 100% of physicians believe that using empathic statements helps their patients feel that they care about them and 98% of physicians believe that empathic statements help them have a better bedside manner (Table 2). Nearly one-third of physicians (33%) indicated that using the words “I understand” denotes an empathic statement (Table 3). Nearly 60% of physicians identified body language as being an important part of expressing empathy (Table 4); 39% of physicians report that they have not received training about what empathy means and when it should be used in a clinical setting (Table 5); 36% of physicians’ reported that they would like to receive more training or assistance about how and when to use empathy during clinical practice (Table 5).
Physician use of empathy during clinical practice.
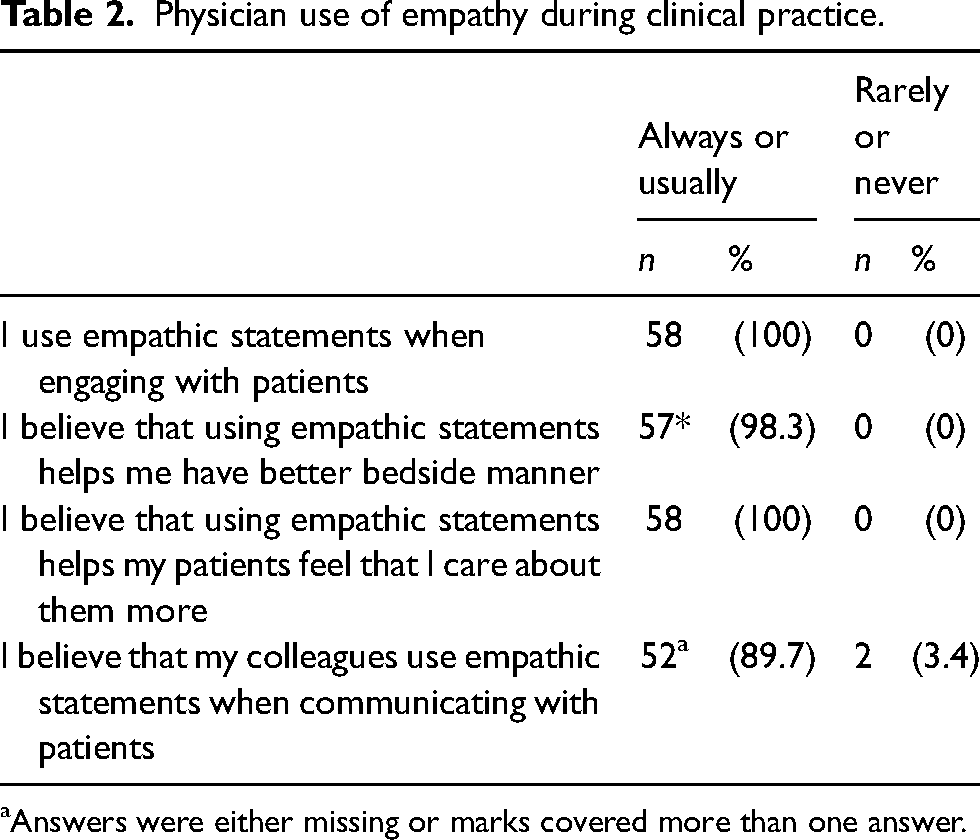
Answers were either missing or marks covered more than one answer.
Words and statements physicians identified as empathic.
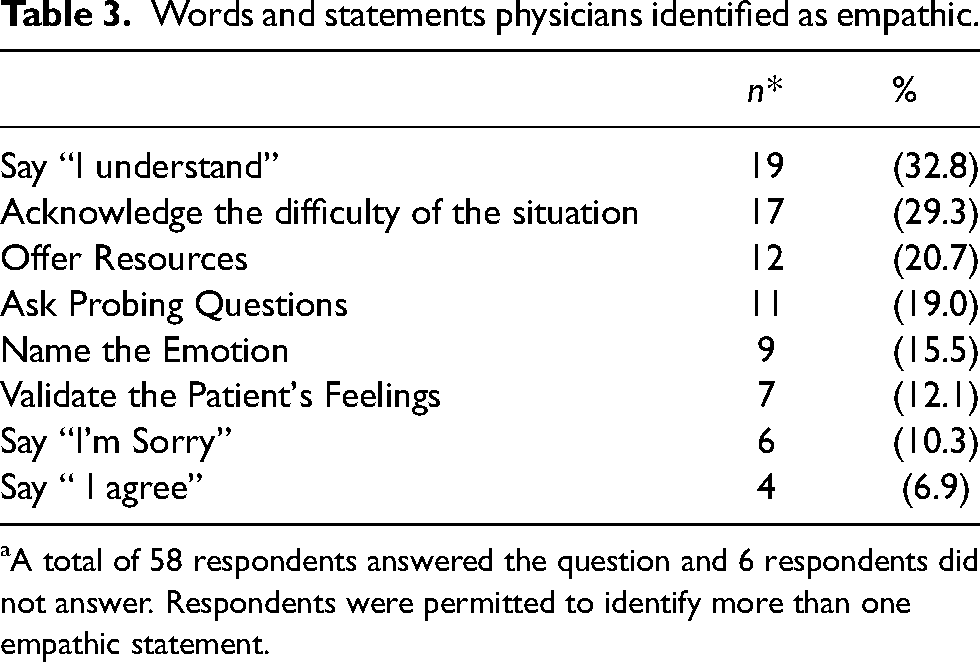

A total of 58 respondents answered the question and 6 respondents did not answer. Respondents were permitted to identify more than one empathic statement.
Physician identified empathic behaviors.

A total of 58 respondents complete the question and 7 respondents did not answer. Respondents were able to identify more than one type of empathic behavior.
Empathy training.

1 missing response.
Discussion
All physicians in this study believe that they always or usually use empathic statements when engaging with their patients and almost all physicians believe that their colleagues use empathic statements. Although this study did not verify the actual use of empathic statements during clinical encounters, the results of this study confirm that physicians believe they use empathy in almost all encounters, making it a skill that can have a potentially wide-ranging impact on an individual physician's patients. Despite the self-reported prevalent use of empathic statements, one-third of physicians indicates a desire for more training in what empathy means and when it should be used in a clinical setting. This suggests that one-third of physicians feel uncertain about a clinical skill they believe should be used in most, if not all, encounters. The desire for more training found in this study is in alignment with The National Academy of Sciences and other organizations that have called for widespread and mandatory communication skills training. 18 Communication skills training with the use of simulated patients has been shown to be effective for increasing clinician capacity for empathy in communication, including responding to patient emotions and allowing for silence when patients are responding to serious news. 19 Physicians have also rated the value of such training to be high. 20 Based on these findings, physician's may be open to the opportunity to engage in empathy training courses. This is important to health care systems that are interested in improving the quality of the patient–provider relationship.
When asked about communicating with patients, nearly half of physicians in this study reported using responses that patients may not perceive as being empathic, even when intended to be empathic, such as “I understand”. For example, telling a dying patient “I understand what you are going through” may be intended as empathic but may not be perceived by the patient as empathic because it is not possible for the physician to actually understand what the dying patient is experiencing. This finding aligns with other studies which have found that physicians’ perceived use of empathy does not align with their patients’ perception of the physicians’ use of empathy. 21
Although most physicians report having received past training about empathy, this study did not assess the type of training physicians have received in the past, so it is unclear whether respondents received training that incorporated feedback on skills formation, which may be the most critical element of education about empathic communication. Medical education curricula may include content that educates trainees about knowledge, attitudes, and skills related to empathy. The fact that one-third of physicians indicated that they need more training on the clinical use of empathy suggests a possible need for greater emphasis on skills practice and feedback during training. Additionally, this study clearly demonstrates that physicians have adopted an attitude about empathy that recognizes the importance of it in clinical practice, which may reflect both their education and practice experiences.
This study has several limitations. First, it does not measure whether physicians’ self-reported use of empathy is concordant with their actual use of empathy during clinical practice. Second, this study was only conducted in one institution which may limit generalizability. Third, this study did not measure whether physician self-reported use of empathy correlates with the patient perception of the physician's empathy. Past research has demonstrated that physician self-assessments of their communication skill level does not correlate with patient assessments. However, physicians may have the internal experience of empathy without conveying empathy to the patient in a meaningful way, which may further confound physician self-assessment. This is supported by studies which have found that the use of empathy during clinical practice varies between gender and physician specialty. 22
This study gives a sense of what comes to mind for physicians when they think of empathic responses. Although this study does not actually illustrate whether a physician has the skill to respond empathically in a real scenario, this study samples physicians’ metacognition about empathy, that is, how the physician thinks about empathy. It is possible that while some of the physicians in this study did not have the reflective ability to think about how they use empathy, or could not label or generalize a definition of empathy, they may have the skill set to employ empathy during clinical practice. This study illustrates the desire among physicians to gain a better metacognitive understanding of empathy. Greater confidence and ability to express empathy may lead to more empathic behavior in the clinical setting. Further training, such as VitalTalk would provide physicians with the skill set necessary to better employ the use of empathy in clinical practice.
Conclusions
In summation, the results of this study are important because they show that physicians value the use of empathy during clinical practice and believe that they are using empathy. Furthermore, this study shows that many physicians are open to the potential of having further empathy training. As empathy has been shown to improve patient outcomes and lead to higher quality care, knowing that physicians value the use of empathy and are willing to engage in further training provides opportunities for health systems to provide empathy training to physicians in order to benefit clinical practice and improve patient care.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
