Abstract
Introduction
Dementia is a complex, debilitating brain disorder that causes a progressive decline in memory, communication, cognition, and eventually, the ability to carry out simple everyday tasks (Sehar et al., 2022). Approximately 900,000 people in the UK are estimated to have dementia, the prevalence of which is due to increase exponentially as the population ages (Wittenberg et al., 2019). With the increasing prevalence of dementia, the number of carers needed to support persons with dementia in their daily activities is also on the rise. Informal (unpaid) carers, predominantly family members, form the backbone of dementia care, providing essential support valued at approximately £13.9 billion annually in the UK (Wittenberg et al., 2019). Despite their critical role in caregiving, the health and well-being of family carers often go unaddressed. It is well-documented that family carers have poorer mental and physical health than non-carers (Richardson et al., 2013), highlighting the need for targeted strategies to address these health disparities.
A healthy diet or better diet quality, defined as a higher intake of fruits, vegetables, fish, and whole grains, is widely recognised as a cornerstone of good physical and mental health, reducing the risk of chronic diseases and supporting overall well-being (Afshin et al., 2019; Guasch-Ferré & Willett, 2021; Jaron & Galal, 2009; Laraia, 2013; Owen & Corfe, 2017; Slawson et al., 2013). However, research focussing on the dietary behaviours of carers of persons with dementia remains limited, despite evidence suggesting that carers are particularly vulnerable to malnutrition and suboptimal dietary patterns. Previous studies demonstrate that carers exhibit ‘at risk’ dietary behaviours such as increased reliance on coffee for energy (Tsapanou et al., 2024), inadequate intake of fruit and vegetables (Bailey et al., 2019) and susceptibility to both undernutrition (Rullier et al., 2014; Tombini et al., 2016), and over-nutrition, for example, obesity (Carpenter et al., 2020; Vitaliano et al., 1996). Nevertheless, to our knowledge, no studies have examined the quality of carers’ diets, which may offer more meaningful insights into multidimensional dietary behaviours, which are more informative for health outcomes than isolated measures of certain nutrients (Hu, 2002).
Moreover, while previous studies suggest that family carers are at risk of poor dietary health, there is a lack of contextual understanding of how caregiving stressors and constraints contribute to these behaviours. For example, family carers of persons with dementia face unique challenges that may influence diet quality, including the physical and emotional demands of caregiving, financial pressures, and changes in meal preparation routines due to the altered eating behaviours and appetites of the person with dementia (Cipriani et al., 2016; Kasper et al., 2015; Walker-Clarke et al., 2022). Caregiving often requires carers to prioritise the nutritional needs of their loved ones over their own, leading to compromised dietary behaviours (Uemura & Hirakawa, 2020). In a recent study, Mole et al. (2021) explored family carers’ experiences of providing nutritional care for persons with dementia and noted that carers reported sacrificing their own nutrition to meet the needs of the person they cared for. However, to what extent this impacts the carers’ overall diet quality remains underexplored. In this context, the primary aim of this study was to pilot a mixed-methods approach to provide a more comprehensive understanding of the dietary behaviours of family carers of persons with dementia.
Methods
Study Design
A convergent conceptual framework was developed to address the research question ‘What is the impact of caring for a person with dementia on dietary quality of informal carers?’ The framework was developed around three constructs: (1) Quantitative assessment of diet quality, measured using validated tools. (2) Qualitative exploration of how caring for a person with dementia influences dietary behaviours. (3) Integration of datasets to identify patterns or divergences within the sample population.
Pragmatism is the philosophical perspective most commonly associated with mixed-methods research designs (Creswell & Clark, 2017) and this worldview was adopted by the authors, acknowledging the problem-based nature of the research goal. This study utilised a concurrent mixed-methods design using an online survey to capture quantitative data on dietary intake and food security, and semi-structured interviews to capture qualitative data on the influence of caring on dietary behaviours in a subset of survey respondents.
Participants and Recruitment
Participants voluntarily took part in the study that was advertised on social media and shared through dementia and caring organisations. Inclusion criteria were UK-based primary, informal carers (≥18 years of age), responsible for providing daily nutritional care to a community-dwelling family member (≥65 years of age), with a confirmed diagnosis of dementia. Participants were not required to reside with the care recipient to avoid limiting the recruitment pool and ensuring that a variety of familial relationships could be explored. Exclusion criteria were carers with medical dietary restrictions or requirements. As this was an exploratory study to gather preliminary insights, 30 carers were recruited for the online survey which is in-line with the recommendations due to the pilot nature of this study (Johanson & Brooks, 2010), 10 of whom were then invited to participate in an interview. A purposive sampling method for the interviews was used with the intention of obtaining a balance in terms of carer sex, relationships, and living arrangements. Informed consent was obtained from all participants before their involvement in the survey and interview; the study was approved by the Health and Life Sciences Academic Integrity and Ethics Committee (#21672).
Quantitative Component
A self-completed online survey was distributed using QuestionPro (©2024) from March – September 2024. The survey collected participant demographic information such as age, self-reported BMI, postcode, employment status, education, relationship to the person with dementia, hours of support provided per day, length of caring for the person with dementia and the person with dementia's age at diagnosis. The survey included validated questionnaires on diet quality and food insecurity. Participants then completed an online dietary assessment tool accessed via an embedded link in the survey and entering personalised login credentials.
Diet Quality
The Mediterranean Diet Adherence Screener (MEDAS) is a widely used tool for evaluating overall diet quality by assessing adherence to the Mediterranean diet which has been associated with reduced disease risk (Miller et al., 2020). It consists of 14 items that measure key components of the diet, such as the intake of fruits, vegetables, olive oil, fish, legumes, nuts, and wine, while also considering the moderation of certain foods like red meat, sugary baked goods or drinks, and dairy products and preference of certain foods such as olive oil as a main source of fat and vegetable protein or white meat over red meat. Each item is scored as 0 or 1, with a maximum score of 14, where higher scores reflect better adherence and higher diet quality; with low adherence, ≤5; moderate to fair adherence, 6–9; good or very good adherence ≥10 (Martínez-González et al., 2012).
Food Insecurity
The Food Insecurity Experience Scale (FIES), developed by the United Nations Food and Agriculture Organization (UN FAO), provides a globally comparable measure of the severity of food insecurity. It comprises eight questions that assess respondents’ self-reported challenges in accessing adequate food. Based on the number of affirmative responses, individuals are classified into one of four categories: food secure, mildly food insecure, moderately food insecure, or severely food insecure. These classifications represent distinct points along the continuum of food security that can be compared to the UK population (Pool & Dooris, 2022).
Dietary Intake
Intake24, a validated (Foster et al., 2019), self-completed 24-h recall system that allows users to report all foods and beverages consumed in the previous 24 hours was used to capture participants’ dietary intake. It prompts participants to provide detailed information on portion sizes and preparation methods, using visual aids for accuracy. Foods within the system are linked to the Nutrient Databank and all data are automatically coded so that nutrient intake can be estimated. Intake24 is currently being piloted in the Scottish Health Survey and is the dietary assessment method for the National Diet and Nutrition Survey (NDNS) Rolling Programme.
Qualitative Component
Semi-structured, one-to-one interviews were conducted to capture information related to the influence of caring on dietary behaviours (n = 10) using a moderator guide developed by the research team referencing previous research interested in dietary behaviours of carers (Lindeza et al., 2024; Rullier et al., 2014; Uemura & Hirakawa, 2020). Ten interviews were thought likely to be sufficient to reach data saturation, particularly given the purposive nature of participant selection The interview explored the carers’ knowledge and perceptions of a healthy diet, perceived and actual barriers to healthy eating; and finally, factors that might facilitate and encourage healthy eating as a response to caring for a person with dementia (Supplemental File 1). The interviews were conducted online over Microsoft Teams due to participants’ diverse regional distribution (Saarijärvi & Bratt, 2021). Interviews were transcribed real-time using the in-built function on Microsoft Teams and then checked for accuracy against the audio recordings.
Data Analysis
Quantitative data was analysed using Jamovi (Version 2.4.8). Descriptive statistics are reported as means (± standard deviations) for continuous data unless otherwise stated. For categorical data, percentages and frequencies were calculated.
Qualitative interview responses were analysed using reflexive thematic analysis, engaging in researcher reflexivity to acknowledge biases, and collaboratively identifying patterns that captured the lived experiences and dietary behaviours of family carers of persons with dementia. (Braun et al., 2023). The data analysis was conducted iteratively and followed the six stages of reflexive thematic analysis: (a) familiarisation; (b) coding; (c) generating initial themes; (d) developing and reviewing themes; (e) refining, defining, and naming themes; and (f) writing up (Braun & Clarke, 2006) facilitated using NVivo 12 software (QSR International). MS familiarised himself with the data and led the coding and generation of initial themes. Ongoing iterative discussions were held within the research team to develop and refine the named themes, thereby reducing potential researcher bias.
Quantitative and qualitative findings were then integrated in the analysis through side-by-side examination of the data sets as a whole, to facilitate understanding of macro-level comparisons and contrasts between the data sets (Creswell & Clark, 2017).
Results
Survey Findings
Participant Demographics
Characteristics of Survey Respondents (n = 30)
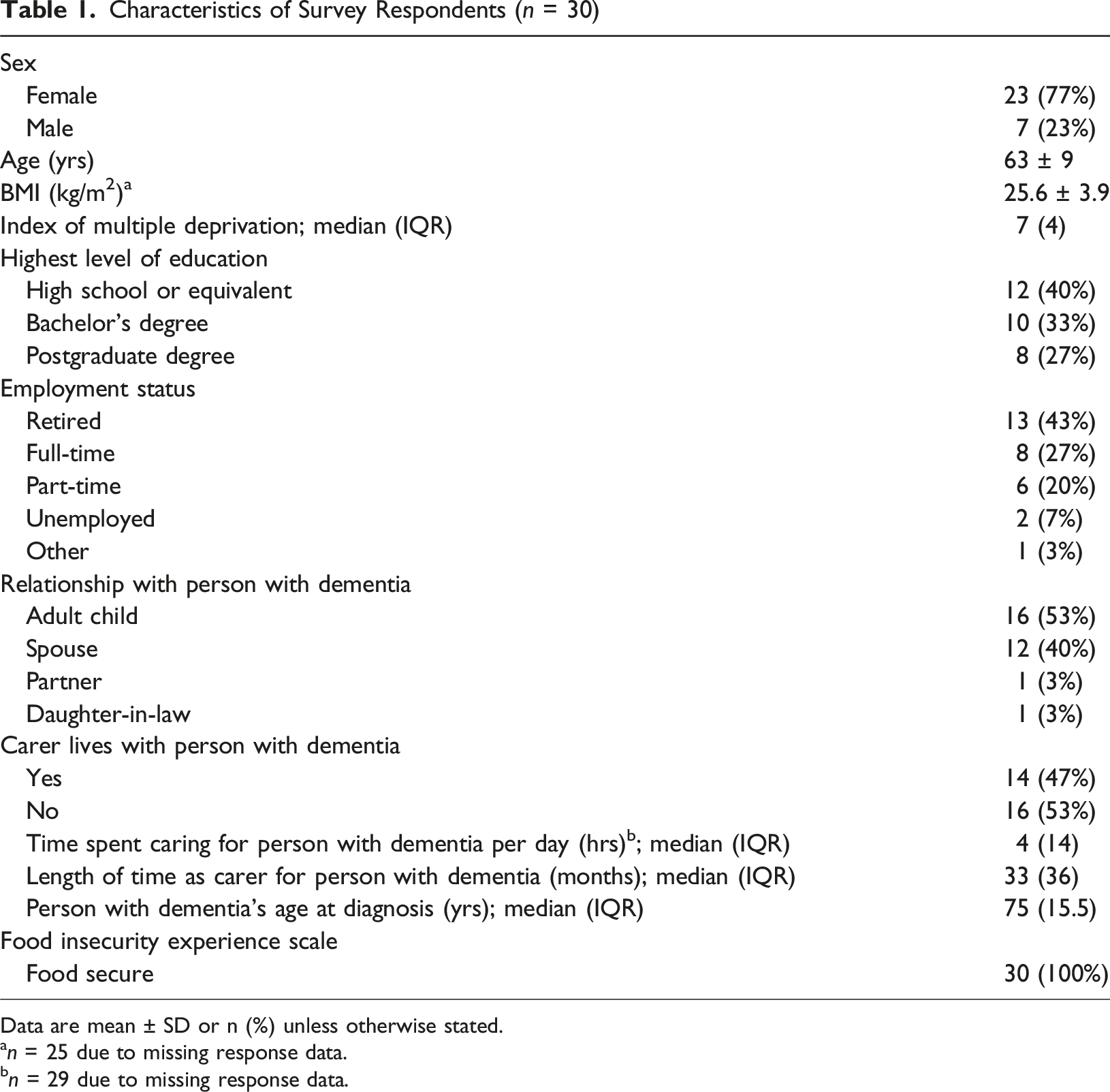
Data are mean ± SD or n (%) unless otherwise stated.
an = 25 due to missing response data.
bn = 29 due to missing response data.
Diet Quality
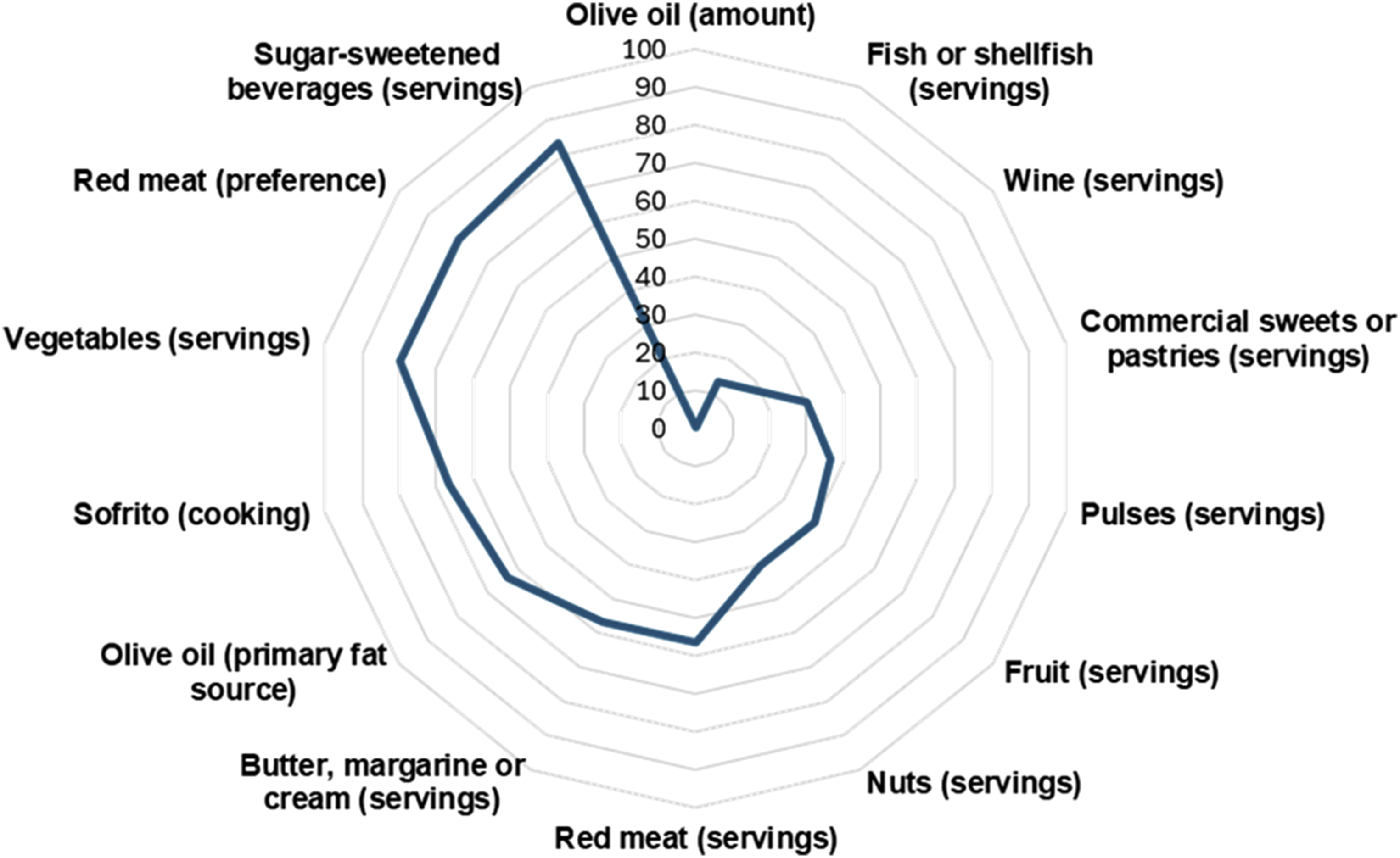
The mean MEDAS score was 6.6 ± 2.06 (range 3−11) arbitrary units, as shown in Figure 1. Thirty percent of family carers reported low adherence, 60% fair adherence and 10% high adherence to the Mediterranean dietary pattern. A radar chart is shown in Figure 2 to visualise which MEDAS components were least/most likely to be achieved. Scores were plotted as a percentage of carers who scored points for each of the individual components. Individual, Mean, and Standard Deviation of Mediterranean Diet Adherence Screener (MEDAS) Questionnaire Score (Arbitrary Units) of Carers (n = 30). The Maximum Possible Score is 14 if all Components are Achieved Radar Chart of the Percentage of Carers (n = 30) Who Scored for Each of the 14 Mediterranean Diet Adherence Screener (MEDAS) Items. A Score of One Indicates Healthy Dietary Patterns in Line With the Mediterranean Diet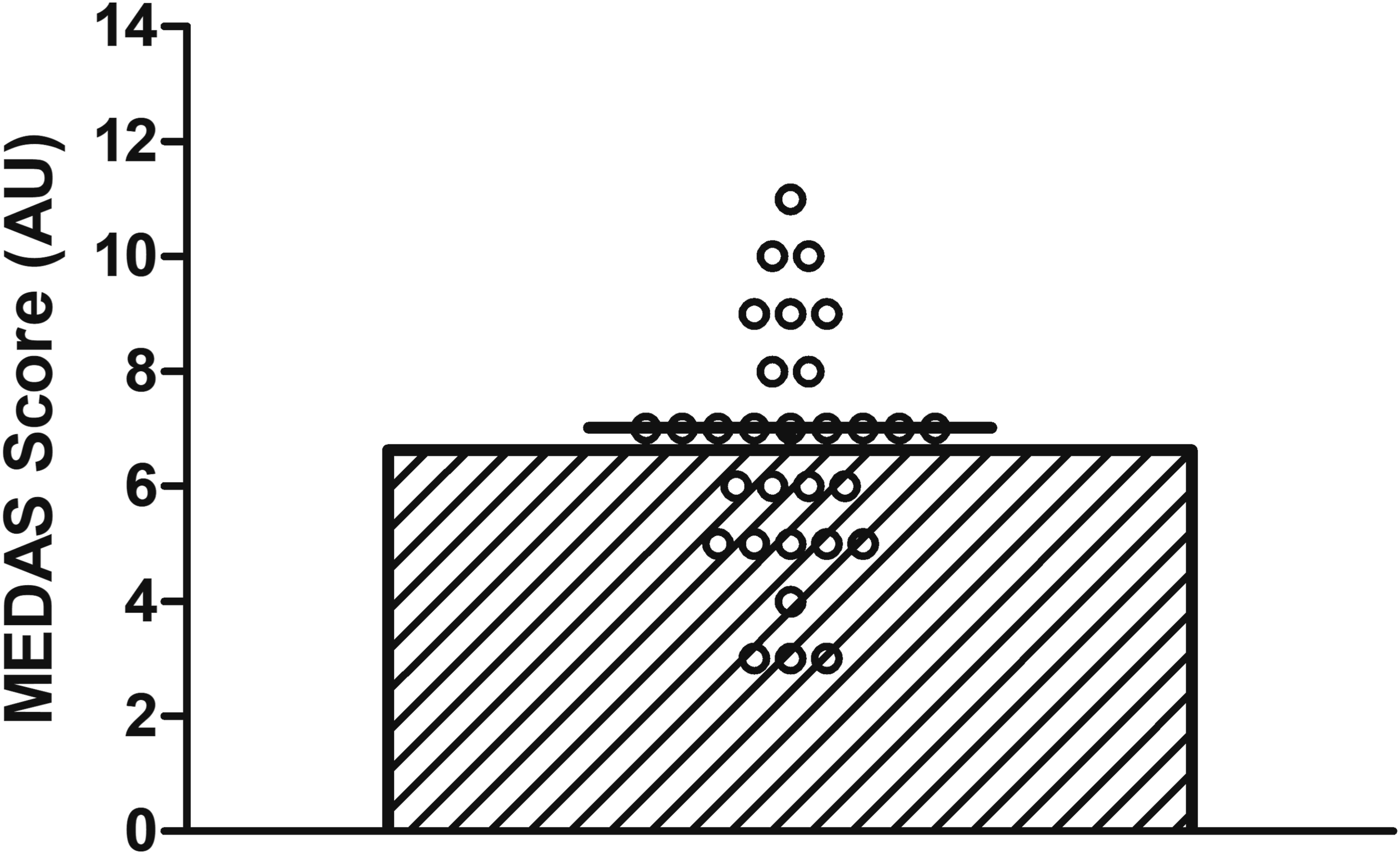
Dietary Intake
Dietary Intake Based on 24-H Dietary Recall Using Intake24
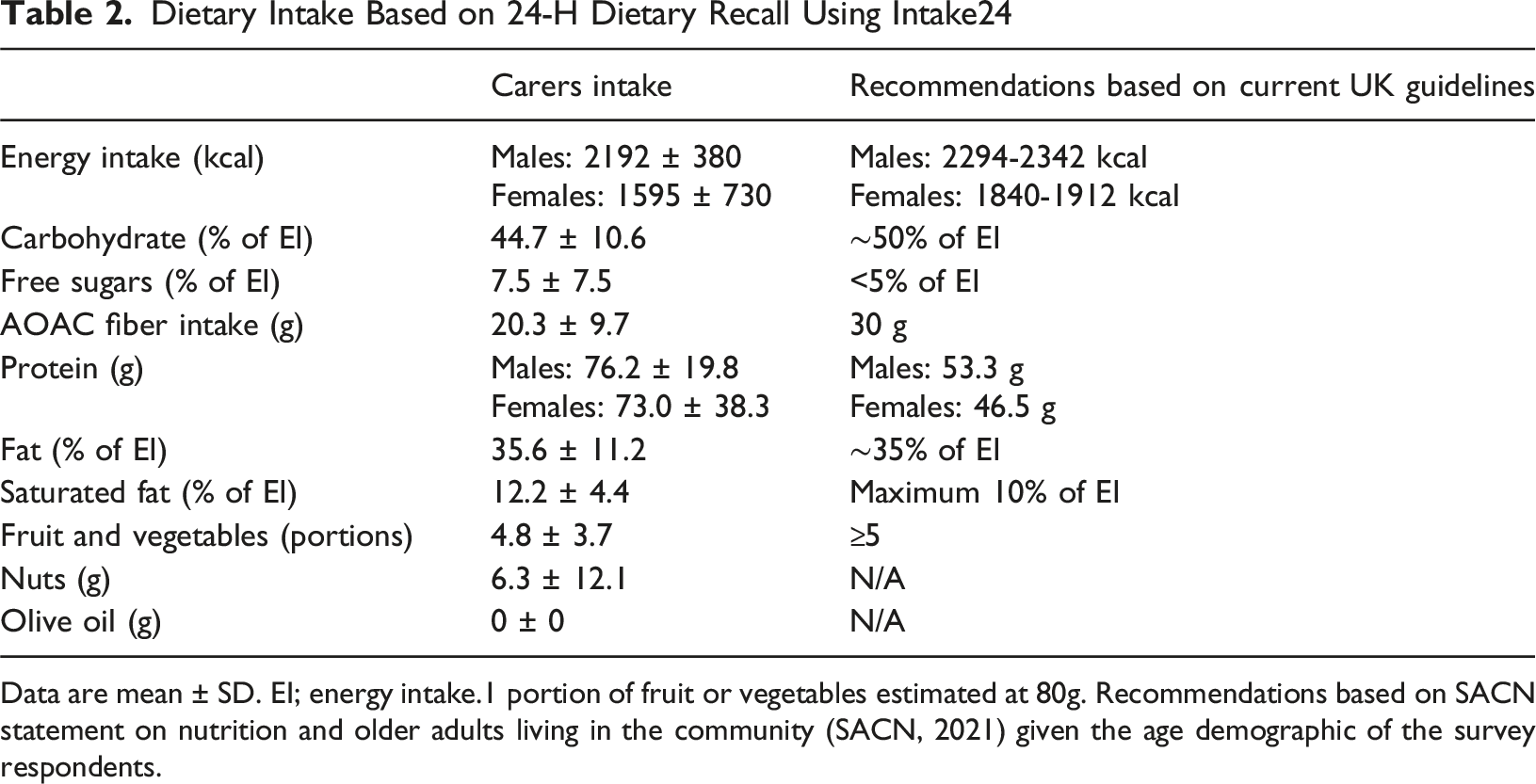
Data are mean ± SD. EI; energy intake.1 portion of fruit or vegetables estimated at 80g. Recommendations based on SACN statement on nutrition and older adults living in the community (SACN, 2021) given the age demographic of the survey respondents.
Qualitative Findings
Ten carers (6 female and 4 male) who completed the survey participated in one-to-one interviews which lasted between 32 and 64 minutes.
The analysis of the interview data created two main themes, with subthemes. The first theme, ‘A lot on our plates’ represents how the day-to-day and practical aspects of caregiving impact on the diets of family carers. The second theme ‘Shifting p(a)lates’ represents the specific impact caring for someone with dementia has on diet and nutrition overall.
Theme 1 - A Lot on Our Plates
It is well established that providing care for a person with an illness or a disability can impact the physical and mental well-being of the person providing care. Participants discussed the impact of caregiving on their own diets. This included how they changed their eating patterns to meet the needs of the person they were caring for, the emotional and physical impact of caregiving, and how dealing with their own health problems further exacerbates their diets and nutrition.
Changing Routines and Food Availability
Participants recognised that providing care for a family member with dementia impacted on the food choices they made, as well as their eating patterns. Tiredness due to balancing caring with other responsibilities, as well as a desire to ensure that the nutritional needs of the person with dementia were met, resulted in their own preferences and routines being overlooked as they attempted to fit in with the likes and routines of the person they cared for. This was particularly prominent in situations where the carer lived in the same household as the person with dementia. But rather than be bothered with cooking two meals I would make the spaghetti bolognese and I’d have some as well. (Husband, Age 69, live-in carer)
This often resulted in participants reporting less flexibility in their eating habits, as well as routine eating, which removes some of the enjoyment and social aspect of eating rituals. So, one of one of my observations, I think this is true of most people with dementia, but certainly true of my wife, is that regularity is quite key. So, I’d say that one of the things that’s happened because of my caring role, is that we’re eating meals at a more sort of regular time. So, we’re having breakfast at the same time, lunch at the same time, evening meal at round about the same time. Whereas in the past, I think particularly with the evening meal, there might have been a bigger flexibility. (Husband, Age 69, live-in carer)
Dietary behaviours are influenced by commensality and participation in social groups, where shared rituals around food become part of the social experience. Historical or current attitudes to nutrition and food appeared to be a good predictor of how well the carer was able to maintain a healthy lifestyle despite the other potential factors from their caring role that could influence their diet. I’m very mindful of what we eat. I am. I am, I am. Have done … watched my weight for donkey’s years. (Wife, Age 62, live-in carer)
When family carers lived in a different household from the person living with dementia, there was a focus on ensuring the person with dementia was eating but trying to avoid eating themselves to prevent them from overeating or making poorer dietary choices whilst balancing two households. It would be awful to live with her and have to... Oh, God. No. Oh, yeah. Oh, dear me. Yeah. It would be awful. Yeah. Trying to balance my own diet and health needs with hers. It just can't. They just. God knows how I would manage that. (Daughter, Age 54, Live-out carer)
Another commonly cited approach was family carers missing meals all together. I might miss food or not eat so much. Perhaps, like yesterday I went around early in the morning. I ended up not eating many breakfast wise, but that’s as likely to be because I'm busy at work than anything else, I suppose. (Daughter, Age 58, Live-out carer)
However, some participants acknowledged the benefits of routine eating to support them to maintain the energy required for caregiving. A healthy diet for me would be eating regularly. Because when I’m tired, I will just have one pile of crap in the evening and eat nothing in between. So regular eating is the key for me. (Daughter, Age 54, Live-out carer)
Changes in routine and flexibility around eating for the person with dementia have indirect impacts on the diets of carers, by removing some of the spontaneity around food for them. This is particularly true for those who live with their care partner, who have to adapt to encourage regular mealtimes for their family member.
Emotional Eating (Disordered Eating)
Many of the participants spoke about the difficulties of caring for a person living with dementia. High levels of stress and the emotional toll of caring for a loved one could lead carers to using eating or alcohol consumption as a coping mechanism. I’m frustrated or, you know, if, if, if [person with dementia] is having a confused moment and it’s very stressful you know, to, to join her in having some ice cream or, you know, to have a few glasses of wine is, you know, I would, I would go that way. Whereas if I didn’t have that, you know, those stressor moments. Then I might not have done that. (Husband, Age 69, Live-in carer)
This can result in carers recognising their poor nutritional choices and feeling guilty about comfort eating. You’d be pissed off and resentful that you’ve spent your whole day doing something. She appreciates it. She can’t help it. But you know what I mean. So, I would just think, stuff it. I’m having [chocolate bar]. I’m going to buy five donuts from the [supermarket] on the way home. Donuts are a bad habit as well. There’s a theme. And just eat that, and it makes you feel better for about 1.5 seconds after you’ve finished, and then you just feel disgusting. (Daughter, Age 54, Live-out carer)
The emotional impact of caring can lead to disordered eating or drinking habits, including comfort eating, binge eating and consumption of alcohol.
Family Carers’ General Health and Morbidities
The general health of carers, as well as their own morbidities impacted on their ability to manage their diets and nutrition as well as their ability to provide care. They were very aware of trying to maintain their own health to allow them to continue to provide care for their loved one, particularly when they were a spouse or partner of the person with dementia, and cognizant of the impact of age-related illnesses. I think the main thing to do is to eat what you enjoy and try not to get overweight. Because you still want to keep your mobility and try to avoid any of the obvious things from being overweight, just getting arthritis or diabetes, if you can avoid it. (Husband, Age 80, Live-in carer).
This is often challenging, and increased tiredness and lower mood can impact the motivation to maintain a healthy diet. If you have a poorer diet, it affects how you’re feeling. It can affect your mood; you can become low. You can put on weight. You can become lethargic, loss of energy. Patience, I imagine, would change. You have to be on top of the game to think ahead to what he’s going to do all the time. I’m up three or four times in a night because he’s off wandering. (Wife, Age 62, Live-in carer)
Further, feelings of helplessness around health, as participants aged, were evident. Some participants stated that maintaining a healthy diet would no longer benefit them, and the priority was to use food as sustenance to have enough energy to get through the day. The idea of eating healthily at this stage in my life is ridiculous. I mean, focussing on a healthy diet at our stage of life becomes something which is totally unnecessary. Food becomes much less of, how do I say it, it's a less important part of the day, it’s something you’ve just got to get out of the way. (Husband, Age 80, Live-in carer).
However, there were instances where the physical toll of caregiving was impacting the health of the family carer and exacerbating underlying health problems. I’ve got post-concussion headaches and stuff like that. I keep forgetting things, and post-traumatic stress and… post-traumatic stress and fibromyalgia, chronic fatigue. But it’s difficult to decide which bit is down to the dementia caring and which bit is down to my condition. (Husband, Age 58, Live-in carer).
Overall, the health, situation and impact of caring for a loved one with dementia impacts the diets and nutrition of family carers. While there are some positive impacts, family carers reported having so much ‘on their plates’ due to caring, and prioritising the needs of their family member often meant that the carers’ health, diet and nutrition were not prioritised.
Theme 2 - Shifting P(a)lates
As well as the impact of general caregiving on the diets and nutrition of participants, they also reported specific impacts related to how dementia affects the loved one they are caring for.
Evolving Palates
A common symptom of dementia is a change in response to certain tastes and textures of food. This means that foods or drinks that a person living with dementia enjoyed pre-diagnosis or earlier in their diagnosis become dislikes and can cause stress and distress responses when served. Most often this means moving towards a preference for ‘bland’ and ‘sweet’ foods. Some carers reported compromising their diets or omitting foods to accommodate their family members’ evolving palates or abilities to eat certain foods. “I used to eat a lot more fish, for example, and I’m eating much less fish than I used to eat. My wife doesn't. She doesn’t like the texture of fish. And especially oily fish. Now, I used to really enjoy mackerel and sardines and things like that, and huge kippers, kippers are one of my favourite things, and she can't stand them. So, there’s quite a few things we just don’t buy anymore, which we would previously have bought. So, I end up omitting certain things.” (Husband, Age 80, Live-in carer).
Additionally, the shift to more sweet foods resulted in increased availability of things like chocolate, cakes, and sweets in the household, and often social outings would centre around going to get some cake. I mean, we never really ate sweets or chocolate much as a family. But he’s desperate to have chocolate. He must have chocolate every day. And, you know, I don’t eat much chocolate. But you know, I buy chocolate for him all the time. (Female partner, Age 75, Live-out carer).
This not only increases the temptation for family carers, but also a need to join the person with dementia eating cake to connect socially, when they would not have previously. So we go for a drive, and then we always end up getting cake. So, whether I want it or not, because I know she’s not eating as well, and so I want her to eat and therefore I end up eating with her (Husband, Age 80, Live-in carer).
Although family carers recognised that the increase in sweet foods had negative implications for their own health, the majority agreed that this was necessary to ensure that the person with dementia had sufficient calories as concerns over them not eating at all were greater than not eating the ‘correct’ food. So she was, she was then, and she was eating a lot of sweet stuff. But then she's been put on some tablets and so I'm not sure it’s good or bad, but her, her desire to eat lots of sweet stuff has gone since then. But at least that was some calories. (Daughter, Age 58, Live-out carer).
The evolving palates of people with dementia has an indirect impact on the people who care for them in terms of social behaviours, food availability and concern over the wellbeing of the individual with dementia.
Challenges of Food-Related Tasks
Some carers reported challenges faced with shopping and preparing foods due to their family member’s condition. As dementia progresses and care needs increase, getting time to go to for the food shopping can be a challenge as the person may not be able to stay alone in the house. I think sometimes shopping is a bit of a problem because, you know, I’m leaving him for maybe about an hour or something, but I try to do that while he’s sleeping in the morning. I mean, I do leave him on his own. And he’s been okay up to now, but I know that could change anytime, I suppose. (Wife, Age 75, Live-in carer).
This can mean the shopping trip is rushed and stressful while worrying about the person with dementia at home. This could result in forgetting items and opting for the convenient option over the healthy option when deciding what to buy. Participants also spoke about the challenges related to going shopping with the person they are caring for, resulting in the focus being on making sure their family member is well and safe and not being able to focus on the task of shopping. If I would do the shopping myself, it would take me 10 minutes. But when you’ve got to get mum in and out of the car and then we shuffle around and then every time you speak to her….They can’t walk and talk at the same time quite often. So, yeah. God, it takes ages. Absolutely ages. And when she gets in there, it’s completely overwhelming for her. But she wants to keep going. I’ll come away from the shops and I haven’t bought anything for myself. So not only do I not buy it then I’ve not got energy left to cook it. (Daughter, Age 54, Live-out carer)
However, some family carers did discuss how they have adapted their shopping habits to their situation to remove the stress of going to the shops, by having shopping delivered or using click and collect services. My bugbear is doing the weekly shop. With [person with dementia] it’s a nightmare. So, because he will forget what you’ve picked. Well, I just don’t want to go there. So, my … What I have learned thanks to COVID is I do click and collect at [supermarket]. So, I do everything online. (Wife, Age 62, Live-in carer
When it came to preparing food, family carers reported having to adapt their approach as well. There were many reasons for this, including to meet the abilities of the person with dementia so they can maintain independence in feeding themselves. … becoming less able to cut up his food. So, I tend to kind of make things that stick together, if you know what I mean? You know, like mince and potatoes and that kind of stuff that he can, you know, maybe manage with a spork or something. (Wife, Age 75, Live-in carer).
Further, the changes in taste and abilities to communicate can have an impact on how the family carer prepares food. … she can make very pointed and very personal comments to me about stuff I cook sometimes, you overcook this, when she’s never said anything before. So, I’ve had to change how I cook things more or less. (Husband, Age 58, Live-in carer). I never did any cooking, ever. It was never something which my mother expected us to do, and it was never something which my wife expected me to do. So, I’m afraid that this whole new idea of managing the household is a new experience. (Husband, Age 80, Live-in carer). … because I wasn’t in charge of the cooking and the shopping. I paid very little interest to it. So, so, so long as food was tasty. That was the only you know, that was the only sort of measure I applied to the food that I ate. Is it tasty or is it not tasty? Whereas now I apply an additional measure, which is it actually doing me and my wife good? (Husband, Age 69, Live-in carer).
Discussion
This study is the first to explore the factors that influence the dietary behaviours of carers of persons with dementia in conjunction with self-reported dietary intake. The results indicated that family carers of persons with dementia fail to meet current dietary recommendations for saturated fat, sugar, fibre, and fruit and vegetables but had a moderate diet quality. They were food secure, however, the findings from the semi-structured interviews demonstrated that caring for a person with dementia could influence their own dietary behaviours, beyond financial reasons.
The findings of the current study are in line with existing evidence that being a carer can result in negligence of one’s own health-promoting (including dietary) behaviours (Bailey et al., 2019; Gallant & Connell, 1998). In contrast, Uemura and Hirakawa (2020) found that some family carers of persons with dementia placed a high priority on healthy food choices, including limiting sugar intake, to remain in good health. While this be related to cultural differences between studies, a limitation of that study is it reported self-perceived dietary habits. Here we report that carers’ diets were high in saturated fats and free sugars and low in fruit and vegetable and fibre intake which was corroborated by their overall diet quality demonstrating a higher intake of red meat, commercial sweets and pastries, and a lower intake of fruit and pulses, as shown in Figure 2, when compared to the healthy Mediterranean dietary pattern. This was despite those interviewed having clear knowledge of what constitutes a healthy diet with most referencing the “importance of fruit and vegetables”, indicating a knowledge-behaviour gap, with the qualitative interviews suggesting that other factors such as historical and current attitudes to nutrition and motivations to eating healthy potentially playing a more important role in their dietary behaviours in line with the findings of others (Bloom et al., 2017; Eglseer et al., 2025). Therefore, providing nutritional information to family carers of persons with dementia is unlikely to be an effective way to initiate behaviour change and instead any education may want to place emphasis on the importance of diet for providing effective care and staying healthy and support that addresses both the demands of caregiving and the shifting nutritional needs of their loved ones.
It is important to acknowledge that this does not necessarily reflect poorer dietary behaviours in carers compared to the general UK population, in which only ∼13% and ∼28% of adults meet free sugar and 5-A-Day recommendations, respectively (SACN, 2021). Moreover, their MEDAS diet quality score was comparable to large-scale study in the UK population (Shannon et al., 2023). However, the findings of the qualitative interviews highlight some additional barriers to healthy eating directly related to their role as a carer of a person with dementia. For example, changes in eating behaviours, diet, and appetite frequently occur in dementia, with cravings and preference for sweet foods being a prominent and commonly reported feature (Fostinelli et al., 2020; Ikeda et al., 2002). Family carers have previously reported feeling guilt regarding the nutritional value of the food provided (such as discretionary and convenience foods), whilst still wanting to ensure the person with dementia is eating and enjoying food (Mole et al., 2021). In the current study this meant carers were more likely to buy and have access to these foods (e.g., cakes and biscuits), which were also offered in support groups creating additional temptations, whereby ease and access to foods are linked to their intake (Blechert et al., 2016; Maas et al., 2012). Moreover, carers reported omitting certain foods to accommodate the person with dementia's preferences, including foods that they knew were important for their overall health such as fish and vegetables, affecting their overall dietary quality.
Additionally, carers reported challenges with shopping, preparing food, and changing roles consistent with the findings of others (Hogan et al., 2004; Papachristou et al., 2013). However, the current study adds to our understanding of how these factors can specifically impact on the carers’ own dietary behaviours, for example by limiting their time and energy to devote to mealtime tasks and changing the foods they eat to maintain their loved one’s independence. On the other hand, this change in roles was viewed as a positive for one carer, giving them a chance to develop an interest in nutrition and shape improved dietary behaviours. The qualitative interviews also indicated that the impact of this was dependent on the stage of dementia and the family carers’ living and employment status. Co-residing with the person with dementia appeared to be associated with more significant dietary compromises in our qualitative data. Additional demographic factors may also have influenced the dietary behaviours observed. For example, older carers may face age-related changes in appetite, energy needs, or comorbidities that affect eating patterns (Roberts & Rosenberg, 2006). Similarly, socioeconomic status and education influence dietary behaviours, with lower levels often linked to poorer diet quality due to limited resources, food access, and nutrition knowledge (Darmon & Drewnowski, 2008). Therefore, demographic variables, such as age, education level, employment status, and living situation, interact with caregiving demands to shape dietary decisions in complex ways. However, due to its exploratory nature this study had a small sample size and was underpowered to explore these factors in detail. Moreover, as shown in Table 1 most of the participants were well educated and from less deprived areas, limiting the applicability of our findings to more diverse or underserved populations. Future research should assess dietary behaviours and the influence of caring in a larger and more diverse sample of family carers of persons with dementia.
Another subtheme ‘emotional eating’ centred around family carers turning to food and alcohol for comfort. Tangelo and colleagues (2018) assessed family carers of persons with dementia unmet needs and also found that they reported eating unhealthy foods to treat or comfort themselves when they felt stressed. Moreover, previous studies have shown that family cares may be more likely to engage in harmful alcohol consumption (Bailey et al., 2019; Denham et al., 2020). Given that caring for someone with dementia can be a particularly demanding and distressing role for the family carer (Feast et al., 2016), potential interventions should address the cognitive and emotional aspects of caregiving stress to support healthier dietary behaviours. For example, enhancing self-efficacy through behavioural interventions has been shown to significantly reduce emotional eating behaviours in family carers (MacDougall & Steffen, 2017).
Practical Implications
The findings of this study highlight the need for practical, flexible, and personalised approaches to support the nutritional well-being of family carers of persons with dementia that address time constraints, emotional stress, and role changes experienced by carers. Evidence suggests that tailored interventions, such as digital health interventions can lead to meaningful improvements in emotional self-regulation strategies in carers (Zhai et al., 2023). Additional strategies may include grocery and/or meal delivery services (Zhu & An, 2013), embedded nutrition support for carers within dementia care pathway and community services (Gitlin et al., 2006). Additionally, healthy food provisions and peer-support networks in carer support services could promote healthier dietary patterns (Moore et al., 2019). These approaches should be adaptable to diverse caregiving situations and consider demographic factors and intervention accessibility.
Strengths and Limitations
Despite this study benefitting from a mixed-methods design providing an in depth understanding of the dietary behaviours of family carers of persons with dementia, the current study has limitations that warrant discussion. Firstly, the sample size (n = 30 for the survey; n = 10 for interviews), while appropriate for an exploratory, mixed-methods design, limits the statistical power and may affect the generalisability of findings. Moreover, recruitment through social media and carer organisations may have resulted in a sample of more health-conscious or digitally connected individuals, potentially introducing selection bias. Furthermore, despite using a validated 24-h dietary recall, assessment of dietary intake is subject to misreporting (Poslusna et al., 2009), which should be taken into consideration when interpreting the quantitative findings. The macro-level convergent analysis approach means that individual-level qualitative observations were not paired with quantitative findings, limiting the ability to compare MEDAS scores with demographic characteristics. Finally, the cross-sectional design of the study limits our understanding of how dietary behaviours evolve with changes in caregiving demands or dementia progression, warranting additional longitudinal studies.
Conclusion
In summary, this study highlights the complex interplay between caregiving responsibilities and the dietary behaviours of family carers of persons with dementia. Despite moderate diet quality comparable to the general UK population, carers frequently failed to meet recommendations for saturated fat, sugar, fibre, and fruit and vegetable intake, reflecting a knowledge-behaviour gap potentially influenced by the stress and demands of providing care. Key barriers included limited time and energy, adjustments to fit persons with dementia's needs, and the accessibility of discretionary foods, which often led to compromises in dietary quality. Emotional eating was identified as a significant coping mechanism, emphasising the need for interventions that address the cognitive and emotional stressors of caregiving. To better support family carers of persons with dementia, future research should explore how dietary behaviours evolve with caregiving demands, investigate the demographic and psychological factors influencing emotional eating, and develop personalised dietary interventions that address practical, cognitive, and emotional challenges to improve carer well-being.
Supplemental Material
Supplemental Material - Having Their Cake and Eating it Too: An Exploratory Mixed-Methods Study on the Dietary Behaviours of Family Carers of Persons With Dementia
Supplemental Material for Having Their Cake and Eating it Too: An Exploratory Mixed-Methods Study on the Dietary Behaviours of Family Carers of Persons With Dementia by Michael Smith, Natalie Dickinson, Nicholas Sculthorpe, Louise Ritchie, and Rachel Kimble in Dementia
Footnotes
Acknowledgements
We would like to acknowledge Join Dementia Research and various carer and dementia organisations for their assistance in participant recruitment. Our sincere thanks also go to the participants for generously sharing their time and insights, making this research possible.
Ethical Statements
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by an Institutional Dementia Seedcorn Funding grant made possible through the generosity of The RS MacDonald Trust, Alzheimer Scotland, and The University of the West of Scotland (GA-02551).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data will be made available upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
