Abstract
Introduction
Better understanding of patient experience is an important driver for service improvements and can act as a lever for system change. In the United Kingdom, the patient experience is now a central issue for the National Health Service Commissioning Board, clinical commissioning groups and the providers they commission from. Traditionally, dementia care in the United Kingdom has focused predominantly on the individual experience of those with late onset dementia, while the voice of those with young onset dementia has been, comparatively, unheard. This study aims to improve the understanding of the personal experience of younger people undergoing investigation for dementia.
Methods
A modified Delphi approach was undertaken with 18 younger people with dementia and 18 supporters of people with young onset dementia. Questions were informed by a scoping review of the literature (O’Malley, M., Carter, J., Stamou, V., Lafontaine, J., & Parkes, J. (2019a). Receiving a diagnosis of young onset dementia: A scoping review of lived experiences.
Results
Twenty-seven of these statements were rated as absolutely essential or very important and included (1) for the general practitioner to identify dementia in younger people, (2) clinicians should be compassionate, empathic and respectful during the assessment and particularly sensitive when providing information about a diagnosis, and (3) remembering that receiving the diagnosis is a lot to absorb for a person with dementia and their supporter. Statistical analyses found no difference in the scoring patterns between younger people with dementia and supporters, suggesting similar shared experiences during the diagnostic process.
Conclusion
Understanding the uniquely personal experience of young people going through the process of diagnosis for dementia is essential to provide person-centred, needs-led, and cost-effective services. Patient’s values and experiences should be used to support and guide clinical decision-making.
Introduction
The prominence of the ‘patient experience’ as the fourth of five domains in the National Health service (NHS) Outcomes Framework (NHS Digital, 2019) highlights that the patient experience has become a central issue for the NHS Commissioning Board, clinical commissioning groups and the providers they commission from. A better understanding of patient experience can drive service improvements and act as a lever for system change, but at an individual level, it is crucial to provide health care which is person-centred and meets emotional and physical needs. The King’s Fund in 2011 (Robert et al., 2011b) documented that providing the right care the first time around and reducing multiple assessments improves the patient experience in the NHS and avoids unnecessary expenditure. Delivering exceptional patient experience requires the optimising of staff interactions with patients and families and support for staff through ongoing education, training and development.
People with young onset dementia (YOD) face inequity across the dementia pathway compared to those with late onset dementia. This includes taking longer to get an accurate and specific diagnosis, a lack of age appropriate services and a lack of support to meet their unique needs (Rodda & Carter, 2016; Svanberg et al., 2011; Van Vliet et al., 2013). Capturing what matters to younger adults diagnosed with dementia undergoing assessment for dementia is currently lacking (O’Malley et al., 2019a). International research shows that for these young people, aged below 65 years, receiving a confirmed and accurate diagnosis of dementia can be a long and daunting process, taking on average up to 4 years in the Netherlands (Van Vliet et al., 2013; Vernooij-Dassen, 2006) and 4.7 years in Australia (Draper et al., 2016). Compared with late onset dementia (dementia diagnosed over the age of 65 years), the presentations of YOD are likely to be of rare cause disorders, and the common dementias (such as Alzheimer’s disease) frequently present with atypical symptoms (such as visual loss as seen in Alzheimer’s disease variant of posterior cortical atrophy) rather than with memory loss as the first symptom (Harding et al., 2018; Rosness et al., 2016; Vieira et al., 2013).
The increased frequency of symptoms, other than memory loss, upon first presentation tends to result in misdiagnoses, such as psychiatric disorders, depression or other neurological illness (Vieira et al., 2013). Even when presentations include complaints about memory loss, the lack of YOD awareness amongst some healthcare professionals can result in a late detection of red flag symptoms and an under recognition that dementia could be the underlying cause of the symptoms. This period is coupled with feelings of uncertainty for families and a delay in accessing suitable support (Williams et al., 2001). Timely and accurate diagnoses as well as increased awareness of YOD amongst healthcare professionals would help mitigate these issues (Millenaar et al., 2016; Sansoni et al., 2016).
Qualitative studies involving younger people with dementia (YPD) have illuminated how personal and individual the diagnostic journey is (Rabanal et al., 2018; Roach et al., 2016; Wawrziczny et al., 2016). A recent literature review (O’Malley et al., 2019a) has highlighted that delays in diagnosis can be attributed to the initial delays in accessing help by the younger person and the misattribution of symptoms by the clinician. The review also illuminated how reactions to the diagnosis can range from feelings of reassurance (in that their symptoms are now explained) to shock and destabilisation. In addition, the review emphasised how unique the impact of receiving a diagnosis is to each family affected, and how vital the role of the clinician in communicating the diagnosis.
Although a body of research has emphasised qualitative aspects of the experience of diagnosis for young people with dementia (O’Malley et al., 2019a), no research to date has employed a quantitative method aimed at generating and collating the important aspects of the individual experience during the referral, assessment and diagnosis of dementia in a younger adult.
The present study forms part of the evidence for ongoing research conducted by the authors, aimed at improving the quality of diagnosis for YPD (UCL, 2016). The design of the study is a modified Delphi approach in which people living with YOD and their supporters living in England were consulted. In order to further inform this under-researched field, the Delphi process described here was modified to suit the needs of our participants. The findings will provide unique tenets for a code of best practice against which services can be benchmarked.
Method
Study design
Steering group
The decision to conduct a Delphi study with people living with YOD and their family supporters came from a meeting with the Angela Project’s steering group committee. The Angela Project study design originally included a Delphi study with clinical experts in diagnosis of YOD. Re-evaluation by the research team and steering group committee about the study aims concluded that balance must be provided by additional consultation with experts by experience to understand their personal views about the experience of diagnosis. This led to the current Delphi study format, which has been appropriately adapted to accommodate the unique needs of this specific group.
Public and patient involvement group
In line with the CO-researcher INvolvement and Engagement in Dementia Model (Swarbrick et al., 2016), the Patient and Public Involvement (PPI) group for our study was an integral part of the project. The Angela Project’s PPI group was involved from the beginning through to the dissemination phase of the project (Oliver et al., 2020).
Literature review
An in-depth literature review (O’Malley et al., 2019a) was conducted to provide focus for the questions and the modified Delphi study design. The review identified eight qualitative research studies which highlighted the key diagnostic concerns for those with YOD as a theme or finding. The review clearly indicated that there was a need for a study specifically focusing on the diagnostic journey.
Delphi method
The Delphi method is particularly useful in situations where existing literature is incomplete and inconsistent (Hasson et al., 2000; Keeney et al., 2006). It involves a structured process of collecting information on a specific subject or problem from a panel of experts through a series of questionnaires. The approach allows anonymised individuals to freely express their opinions, reconsider them in the light of collective opinions from the whole group and initiate a narrowing of the range of opinions with each round to gain consensus. As the study focused on an under-studied area, involving a group whose voices are often not heard, we undertook a qualitative first round to capture the experiences and views of our participants (Iqbal & Pipon-Young, 2009; Van Der Steen et al., 2014). Whilst there are shared experiences across individuals and families during the diagnostic journey, receiving a diagnosis of dementia is a unique experience. With this in mind, we modified the Delphi method to include all statements in the final list (including those where consensus was not reached) with their corresponding descriptive statistics to ensure all views were reported and not discarded. In addition, we also offered an e-Delphi option to enable our participants to complete the process online to suit their personal circumstance.
In the present study, the Delphi process to determine what constitutes a good diagnostic experience for YPD involved four steps: (1) formation of the expert panels, (2) survey development informed by a literature search, (3) data collection and analysis and (4) guidelines development.
Sample selection
Participants’ demographic table.
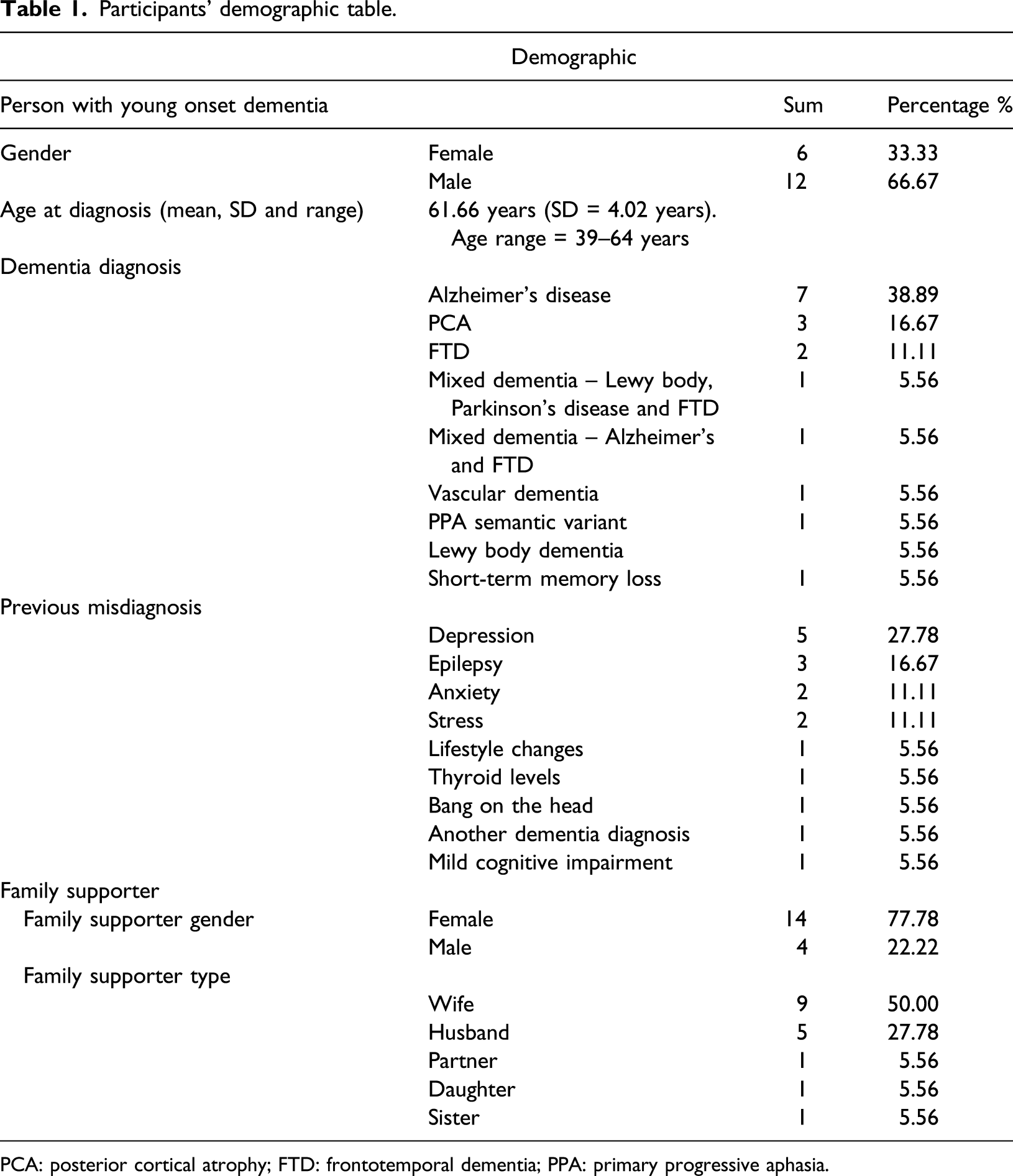
PCA: posterior cortical atrophy; FTD: frontotemporal dementia; PPA: primary progressive aphasia.
Survey development
Open-ended questions for Round 1 of the Delphi related to the personal experience of participants about referral, assessment and diagnosis of dementia (see Supplemental Appendix 1 for the questions presented in Round 1) and were co-designed with YPD and family supporters who were members of the PPI panel.
The PPI group were asked to comment and revise the wording of open ending questions for Round 1, and provided feedback on how user-friendly and legible the questionnaires were for both Rounds 1 and 2.
Analysis framework
Full list of statements and the supporting raw data quote from the participants with young onset dementia and the family supporters, following Round 1 of the Delphi and in preparation for Round 2.

PCA: posterior cortical atrophy; YOD: young onset dementia; SPECT: single photon emission computed tomography; MRI: magnetic resonance imaging; GP: general practitioner.
Round 1
The analysis framework for Round 1 consisted of 4 stages.
Stage 1
The first stage focused on the researchers’ familiarisation with the qualitative responses from our participants and involved. The researchers read through all reports from the participants and where appropriate grouped the exact quotes from that reported similar topics. Quotes were revised and rewritten to develop a summary short title (please see Supplemental Appendixes 2 and 3 for the short titles), and a longer detailed title, for clarity and legibility and a second checker read through the statements and prepared feedback. Only the detailed longer titles are included in the main body of this article. Finally, the second checker and researcher attended a ‘statement workshop’ where statements were grouped and collapsed as appropriate.
Following this Stage 1 process, there were 224 statements in total. One hundred statements were from people with dementia and 124 statements were from supporters.
Stage 2
Two of the researchers collated similar statements per question across the two groups of YPD and supporters, further reducing the statements to 81 in total. These were next itemised as originating either from both people with dementia and supporters or separately from people with dementia or supporters.
Stage 3
Similar statements were further reduced by looking at similarities across the whole dataset. Doing this reduced the list of Delphi statements to a final list of 29. See Table 2 for the final list of statements and the supporting quotes from YPD and family supporters.
Stage 4
Statements were organised according to three headings; referral, assessment and diagnosis of YOD. Consultation with the project PPI members, between February 2017 and December 2019, provided guidance on how best to present the statements to participants in the final round. This consultation included the presentation of the rating scale, font type and size and wording of the statements.
Round 2
In the final round (Round 2) of the Delphi, participants were asked to rate the importance of the 29 statements using a 7- point Likert scale, with points on the scale representing whether statements were not at all important, low importance, slightly important, neutral, moderately important, very important or absolutely essential. In Round 2, we also wanted to explore whether there were any statistically significant differences in the Likert scale ratings between those with YOD versus family supporters.
Ethics
The Angela Project was approved by the Health Research Authority in England and by the South Central Berkshire Research Ethics Committee (REC ref.: 17/SC/0296).
Findings
Thirty-six participants, 18 people diagnosed with YOD and 18 family supporters were recruited between February 2018 and July 2018. See Figure 1 below which shows the geographical locations of the participants. Geographical spread of participants who took part in the Delphi study. This image was produced by the research team using Maptitude 2019 (Calibre Corporation).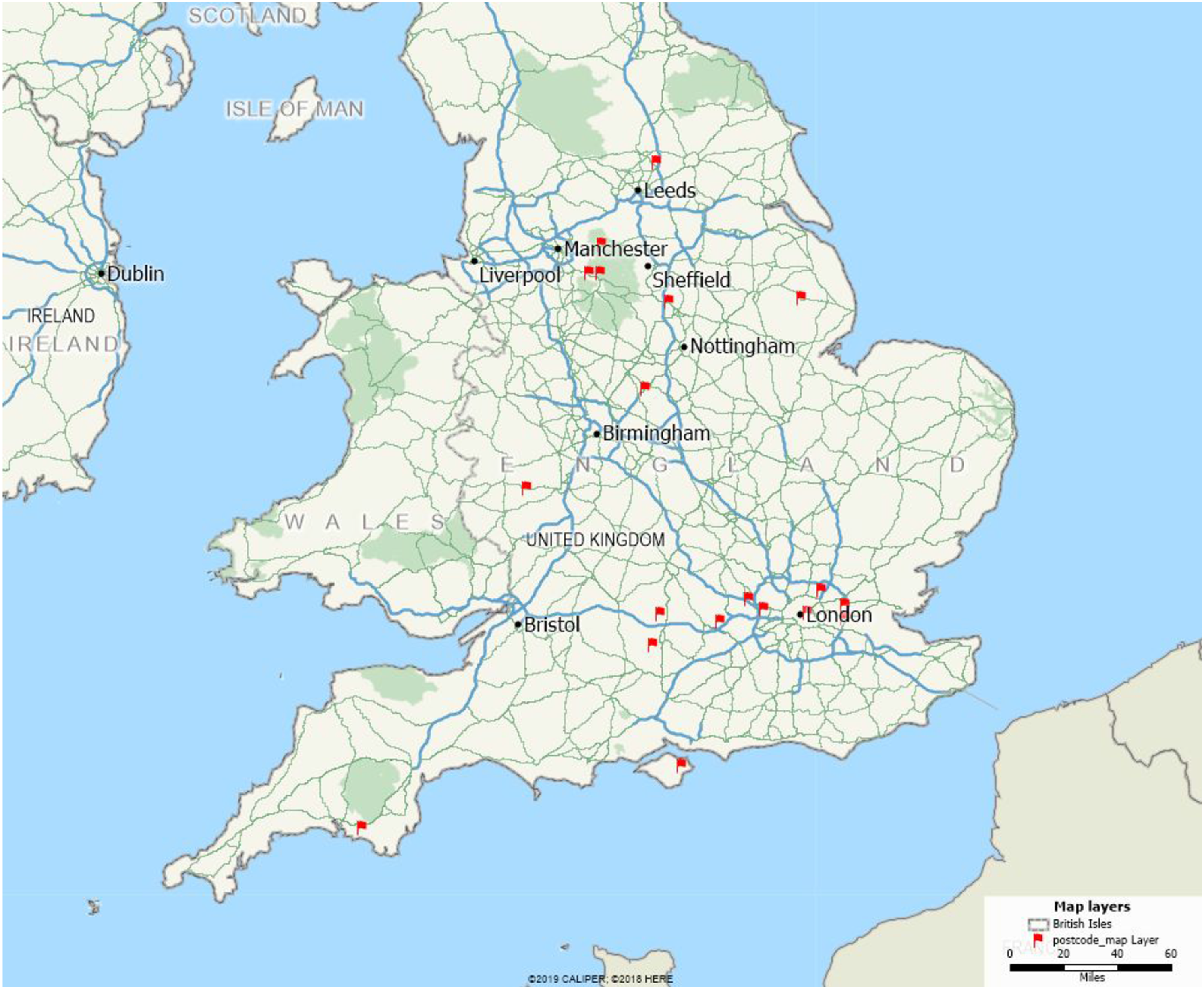
Location
Two rounds of a modified Delphi process resulted in 29 key statements related to referral, assessment and diagnosis of which 27 were rated by participants as absolutely essential or very important. Please see Table 2 for the full list of 29 of statements that were organised following the analysis framework of Round 1 of the modified Delphi and the supporting raw data quote from the participants with YOD and the family supporters.
Statistical analyses
In addition to the rich qualitative data to support the formation of each statement, we wanted to explore whether there were any significant differences in the ratings given by those with YOD versus family supporters following Round 2. The distributions of the ratings for all 29 statements were non-normal; therefore, a non-parametric test (Mann–Whitney test) was used for the analysis. Statistical significance was tested at the 5% level throughout.
Full list of the statements, inter-quartile range, median score and results of the Mann–Whitney test that compared ratings between people with dementia and family supporters.
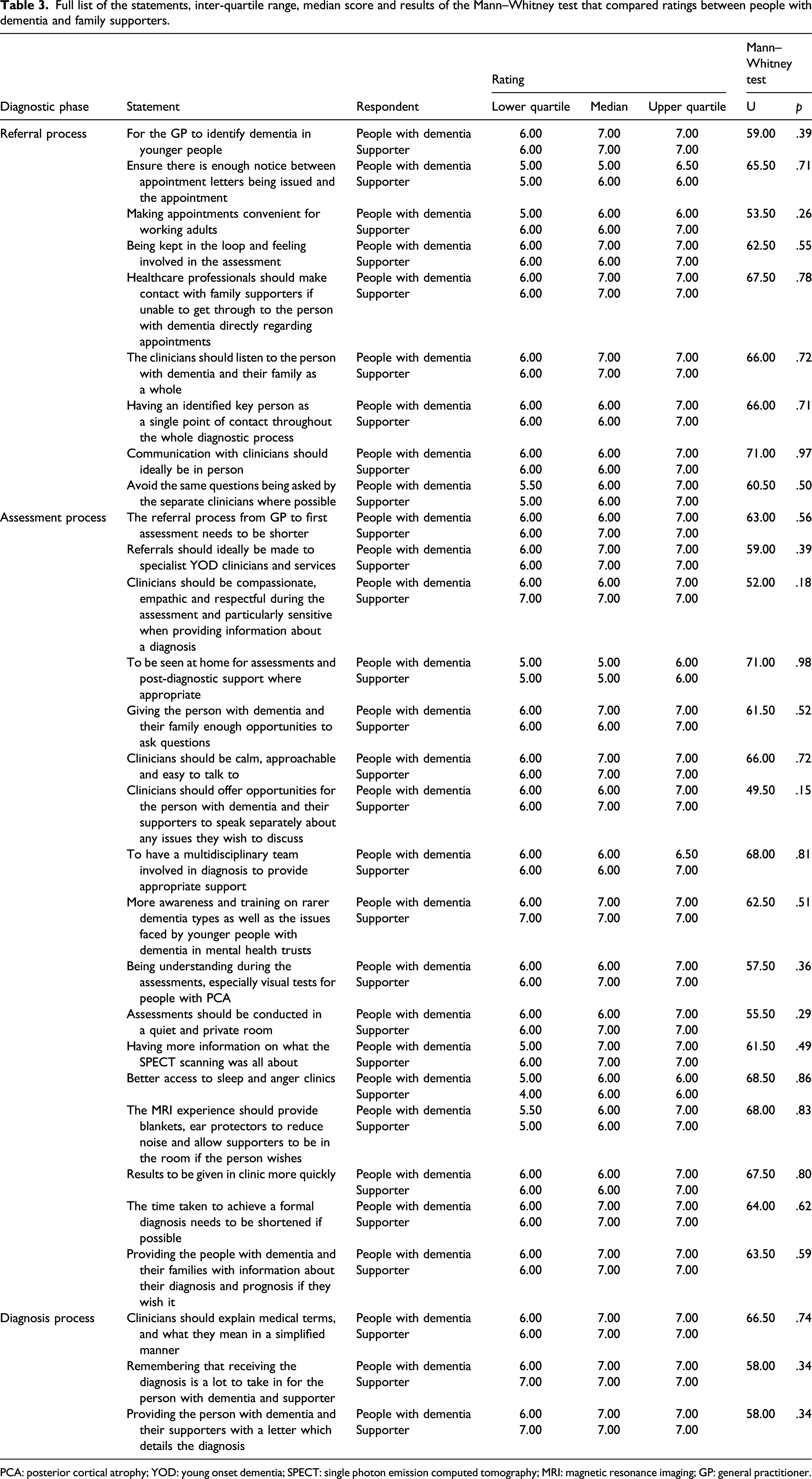
PCA: posterior cortical atrophy; YOD: young onset dementia; SPECT: single photon emission computed tomography; MRI: magnetic resonance imaging; GP: general practitioner.
The statement ‘Ensure there is enough notice between appointment letters being issued and the appointment’ only reached a moderate importance consensus level for people with dementia and ‘To be seen at home for assessments and post-diagnostic support where appropriate’ only reached moderate importance consensus level for both people with dementia and family supporters.
Statistics
There were no statistically significant differences between statements expressed by the people with dementia and their supporters. There was a ceiling effect which effectively decreased the sensitivity of the scale since most of the median ratings were 7 (Absolutely essential), with the lowest median rating being 5 (Moderately important). However, this does show a high degree of agreement that the statements extracted were considered important to all participants. Paired analysis of the ratings of people with dementia and their supporter also did not show any statistically significant differences in ratings for any of the statements.
Agreement between those diagnosed with dementia and supporters
Following the ratings made for each statement in Round 2, scores were available for 10 dyads who participated in this round. Paired tests (Wilcoxon tests) on data from people with dementia/supporter dyads also showed no statistically significant differences between the scores of YPD and their supporters on statements, with the exception of the statement ‘Making appointments convenient for working adults’ where there was a statistically significant difference between the responses of people with dementia compared to their supporters, with the supporters generally reporting this as having higher importance (related-samples Wilcoxon test, test statistic = 15,
Percentage agreement
Level of agreement (percentage) on statements between the 10 dyads that completed all rounds of the Delphi.

PCA: posterior cortical atrophy; YOD: young onset dementia; SPECT: single photon emission computed tomography; MRI: magnetic resonance imaging; GP: general practitioner.
It is important to note that the percentage agreement between dyad findings do not take into account the agreement that would be expected purely by chance. High levels of agreement do not mean high levels of importance of that statement (just that most pairs of people with dementia gave the same score for that statement as their supporter). Note that there were no statistical differences between the paired scores for all but one of the statements, so low percentages do not suggest that people with dementia scored differently overall to their supporters (the differences were in both directions; sometimes people with dementia scored higher than supporters, sometimes the other way round).
Discussion
In this study, young people with dementia and their supporters have highlighted key components of the referral, assessment and diagnosis that they deem to be absolutely essential or very important for informing best practice based on their own personal experience.
People with YOD expressed concern about inequity in waiting times in receiving a diagnosis and access to necessary investigations, as highlighted in the present study’s final list of 29 statements. Research has shown people with YOD can wait 4 years (Van Vliet et al., 2013) for diagnosis, and that in England, only 45.9% of those predicted to have a diagnosis of YOD have a recorded diagnosis compared to those over 65 where the recorded diagnosis rate is 68% (Public Health England, 2020)
In general practice, delays may be due to general practitioners (GPs) not considering the possibility of dementia in younger people and because the rarer types of dementia that are more common in younger people are harder to recognise and have symptoms that overlap with those of common psychiatric disorders such as depression. This explanation is consistent with the reports of misdiagnosis by the participants in the current study, whereby 15 of the 18 individuals reported a diagnosis of another condition before receiving a confirmed diagnosis of dementia. Once someone is referred to a specialist setting, there can be further delays due to a lack of specialist clinicians and limited access to the often, complex investigations required to diagnose YOD. This means a longer period of having to cope with unexplained symptoms and no support, for both the person with dementia and their family.
Healthcare research has established that involving individuals in shared decision-making by encouraging active participation and enhanced communication, can provide individuals with more control over their care, improves the ability to make informed choices and allows them to participate knowledgeably in treatment decisions (De Wilde et al., 2017; Elwyn et al., 2010). Shared decision-making in dementia care is a relatively new concept (Mariani, 2019) and has more often been implemented in terms of care planning and end-of-life care (Gjerberg et al., 2015), though more recently research is exploring shared decision-making during the diagnostic process (De Wilde et al., 2017). As captured in our statements, patient–clinician conversations during the workup require sensitivity, and care should be taken when delivering updates on ongoing assessments and when delivering diagnoses.
Evidence suggests that improving the patient experience is linked to improvement in performance and systems within clinical practice (Schlesinger et al., 2015) but equally as important it increases individual autonomy and empowerment to maintain independence (Stamou et al., 2020). The results presented here support this view by clearly demonstrating that while both the efficiency and practicalities of the diagnostic process were important, participants equally valued feeling listened to, informed and supported.
Of note, rapid referral to specialists, early identification of presenting symptoms by GPs, convenient appointment times especially for working adults are in-line with known ‘pinch points’ in current care pathways for YPD which result in delays in referral (O’Malley et al., 2019a, 2019b; Van Vliet et al., 2011). Clinicians taking time to gather the views of important informants and listening to the whole family, overlaps with good practice guidance for clinicians in assessment and history taking, particularly where the person with dementia may lack insight into their difficulties or the presentation is non-amnestic and harder to recognise (Harding et al., 2018; O’Malley et al., 2019b). YPD endorsed the value of having an identified key person as a single point of contact throughout the whole diagnostic process. Although, this approach to case management is enshrined in the National Institute for Clinical Excellence dementia guideline (National Institute for Health and Clinical Excellence, 2018), the necessity for specialist skills in the case management role specifically relevant to YPD are usually not acknowledged. For example having skills and knowledge to facilitate access to information about YOD and rare forms of dementia, to communicate the diagnosis to young children and to facilitate access to specialist advice and support about young onset specific needs, for example employment, mortgage and financial obligations and future financial planning, guidance on this role is available (Hussey & Hayo, 2019).
The communication skills of the clinician and the feeling of being listened to and heard by those with expertise in diagnosis formed the focus of most statements in relation to the assessment stage of the process. Sensitivity about the impact of the information because of the ‘lack of narrative’ for dementia at a young age and making time for questions with follow-up summary information were particularly valued in terms of the way diagnosis was relayed. Getting a diagnosis in working age can significantly disrupt the normal life events, particularly when the person faces increasing disability, dependency and mortality (Clemerson et al., 2013; Pipon-Young et al., 2012). At the point of diagnosis, there would be an opportunity for the clinician to have a conversation with the person about the impact of the diagnosis on the changes they may be faced with, and how they might adjust (Roach et al., 2008). However, these conversations would need to be considered in a person-centred and individual way as they may not be appropriate for some individuals.
The clinician’s use of language, avoiding the use of medical jargon and adopting a calm manner in a private environment were all also valued. This mirrors findings in a recently published scoping review that highlighted how the impact of a diagnosis on the patient and their supporter was heavily influenced by the language used by the clinicians (O’Malley et al., 2019a, 2019b).
Several generic frameworks have attempted to capture what matters most to patients (Robert et al., 2011a) in terms of improving individual experience, and the statements identified here show significant overlap with their core tenets, often identified as relational and functional aspects. Most research in the field of patient experience has focused upon the relational aspects of care (feeling informed, listened to) but interestingly in our study, the majority of statements preferentially related to functional aspects of care (i.e. the process). This may reflect previous research which demonstrates that those with YOD often see up to five different consultants before diagnosis and care pathways can be chaotic (Carter et al., 2018). Our own research which identifies the core features of YOD services which are perceived positively (Stamou et al., 2020) demonstrates that positive post-diagnostic services may collectively create an enabling-protective circle that supports YPD to re-establish and maintain a positive identity in the face of YOD.
It could be argued that many of the individual statements reported by YPD and family member/supporters simply represent good practice in all-age dementia assessment. However, statements related to knowledge base of rare dementias, GP recognition of early symptoms, shortening the time to diagnosis and explanation of specialist investigations, arguably reflect the reality of current shortfalls in services for those with YOD (Murrells et al., 2013). Additionally, the value of the statements here is that they provide insight into the multidimensional aspects of individual experience ranging from ‘relational’ aspects of care, such as feeling informed, listened to, communication styles, to ‘functional’ aspects of care, such as the practicalities of the process and how this can guide shared decision-making, deliver a more person-centred experience and increase individual autonomy.
Interestingly, there were no significant differences in the opinions expressed by YPD or family/supporters, although it is recognised that this may often not be the case. This might be explained in the current study by the low number of participants with dementia subtypes more commonly associated with reduced insight such as frontotemporal dementias.
The statements derived from this Delphi study offer the potential to identify shortfalls in current services and improve the quality of services to better meet the needs of YPD and families.
Strengths and limitations
Although we recruited a broad geographical spread of participants, only individuals living in England took part in the study. Diagnostic experiences from the rest of the United Kingdom were therefore not captured and were beyond the scope of the current study. Future research should aim to include those living in Wales, Scotland and Northern Ireland to explore whether the statements and key reports are consistent with the experiences of those living in the rest of the United Kingdom and whether additional statements should be considered for other regions.
A modified Delphi methodology was adopted to refine the statements viewed as being crucial during the diagnostic period. Consensus was not the prime aim of this article rather it was to capture absolutely essential and very important aspects of the process of diagnosis for young people with dementia. We have presented the full list of statements to ensure that all views are captured, and statements were not excluded because they represented a minority view. The limited number of participants means that the study may have missed important lived experiences of younger people undergoing assessment for dementia and may not be truly representative. It was also a small sample for statistical analysis and may have not had sufficient power to identify small to moderate differences. However, the population of individuals who participated came from across the whole of England (see Figure 1 for the geographical spread) and were recruited through both NHS services for YPD, as well as third sector organisations and therefore could be considered representative.
How people with dementia experience their condition depends on their own complex biographies and relationships as well as the behaviour of those they encounter during the diagnostic process. Everyone’s experience of receiving a diagnosis of dementia is unique, so practitioners and clinicians should use our findings as guidance but continue to listen to the views of their own patients in their specific setting and be alert to expressed differences.
Implications and implementation
The qualitatively rich reports made by our participants highlighted key aspects of the referral, assessment and diagnosis of dementia that should be considered by healthcare organisations as important to the individual experience and hence delivery of good care. Good experience is generally considered a multidimensional concept dependent on functional (process), transactional (‘being care for’) and relational (‘being care about’) aspects of care. Several approaches to measurement of these aspects of care are available and future work is necessary to assess how these can inform a strategic approach to improve the experience for young people with dementia and their families/supporters.
Conclusion
In this article, we have presented the findings from a unique and innovative modified Delphi deliberately designed to capture the perspectives of YPD and their carers as ‘experts’ of their experiences. The study provides insight into the complex interpersonal aspects of care that matter to YPD, alongside transactional and functional aspects that are necessary to improve individual experience.
Supplemental Material
Supplemental_material – Supplemental Material for Receiving a diagnosis of young onset dementia: Evidence-based statements to inform best practice
Supplemental Material, Supplemental_material for Receiving a diagnosis of young onset dementia: Evidence-based statements to inform best practice by Mary O’Malley, Jacqueline Parkes, Jackie Campbell, Vasileios Stamou, Jenny LaFontaine, Jan R Oyebode and Janet Carter in Dementia
Footnotes
Acknowledgements
The research team acknowledges the support of the National Institute for Health Research Clinical Research Network (NIHR CRN). The research team would also like to thank all the NHS sites and third sector organisations, which facilitated the recruitment of participants to the study. Special thanks go to the Angela Project’s Public and Patient Involvement (PPI) group and Steering Committee for their helpful suggestions through the project.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Alzheimer’s Society (AS-PG 15b-034).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
