Abstract
Objectives
To demonstrate the power of integrating three theoretical perspectives (Mentalization Theory, Perceptual Control Theory and the Communicative Impact model), which jointly illuminate the communication challenges and opportunities faced by family carers of people with dementia. To point the way to how this framework informs the design and delivery of carer communication and interaction training.
Method
Conceptual synthesis based on a narrative review of relevant literature, supported by examples of family carers.
Results
We use the conceptual models to show how the capacity to mentalize (“holding mind in mind”) offers a greater sense of control over internal and external conflicts, with the result that they can be deescalated in pursuit of mutual goals.
Conclusions
The integrative conceptual framework presented here highlights specific psychological and relational mechanisms that can be targeted through carer training to enhance communication with a person living with dementia.
Introduction
In their recent systematic review of communication training interventions for carers of people living with dementia, Morris, Horne, McEvoy, and Williamson (2017) found that it is possible to improve carers’ knowledge of communication strategies and skills. However, only a minority of the reviewed studies found improvements in the wellbeing of carers or people living with dementia. Knowing that certain interventions are effective in improving knowledge and skills does not always translate to knowing how to improve wellbeing. One reason for this may be the absence, or limited efficacy, of theoretical models underpinning training interventions. Even where a training approach is effective for knowledge and skills development, the lack of adequate underpinning theory can prevent an understanding of the mechanisms through which beneficial effects are realized (Elvish, Lever, Johnstone, Cawley, & Keady, 2013; Popay et al., 2006). Consequently, it will be difficult to identify and justify potential routes towards improvements in training interventions, and also to distinguish in a principled way between which input is actually enhancing specific communication and interactive abilities, rather than only building general knowledge of potential strategies.
Where detailed conceptual models are presented (e.g. Haberstroh, Neumeyer, Krause, Franzmann, & Pantel, 2011), the primary skills-related focus tends to be quite narrow and cognitively superficial; for example, advice on eliminating distractions and delivering limited content information in short, simple sentences. While such strategies will certainly be helpful, they do not encompass important considerations that affect interactive success, such as the dynamics of relationships and the capacity to understand and accommodate the other person’s perspective. A recent systematic review indicated that in order to support carers with behaviour that challenges, emotional support for carers’ negative feelings and unmet psychological needs is important and could help maintain relational connections (Feast et al., 2016).
One of the most prevalent conceptual frameworks underpinning training interventions is person-centred care (Eggenberger, Heimerl, & Bennett, 2013; Morris et al., 2017). But even such approaches (Kitwood, 1997; Mitchell & Agnelli, 2015) could be considered limited if their vital emphasis upon treating people living with dementia as individuals with purpose and meaning is insufficiently underpinned by an understanding of what is required to achieve this aim (Brooker, 2003; Higgs & Gilleard, 2016). Additionally, person-centred theories have primarily been developed for professional rather than family care relationships (e.g. Brooker, 2003; McCormack & McCance, 2006) and thus do not accommodate the additional relational and emotional dynamics of the latter. They have been criticized as not taking into account the degree of “interdependencies and reciprocities” (Nolan, Ryan, Enderby, & Reid, 2002, p. 203), which are particularly nuanced in family relationships (Smebye & Kirkevold, 2013), and for positioning people living with dementia as passive recipients of care instead of active agents (Bartlett & O’Connor, 2007; Smebye & Kirkevold, 2013).
The development of effective communication training interventions requires a
conceptualization of how interaction fits into the emotional and cognitive landscape.
Associated guidance for carers on how to navigate and change this landscape should be
beneficial in helping them to improve the quality of their communication experience. This
article maps the broader context of interaction, by demonstrating the main determinants of
communication breakdown or challenge, and how they might be addressed in practice. Three
existing models are integrated:
The integrated framework outlined in this paper (Communication Empowerment Framework) has been developed to inform a communication and interaction training intervention known as Empowered Conversations, which is described in detail in a separate article. This framework emphasizes the importance of care partners trying to understand the perspective of the person they are caring for and indicates ways in which perspective-taking can be impaired. It demonstrates how carers can develop this understanding without losing sight of their own goals and responses. The framework indicates how communication can break down and ways in which it can be enhanced to support connected relationships. It specifies how conflicts can arise and indicates how they can be addressed. In this paper, challenges to communication and interaction are first detailed. Then, the three theoretical models that inform the framework are described and finally the Communication Empowerment framework is specified.
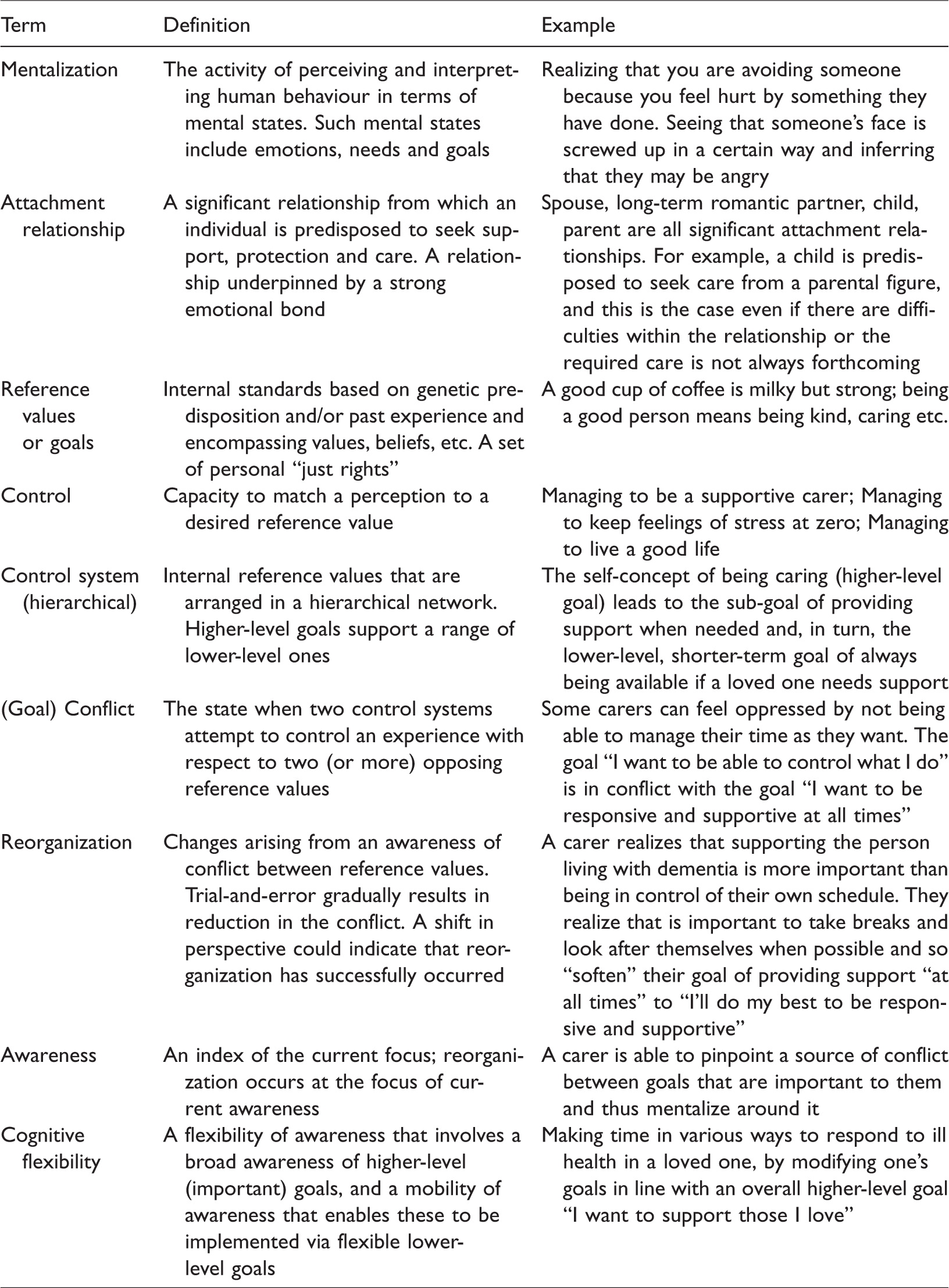
Key conceptual terms, marked in bold in the text, are defined in Table 1.
Glossary of key terms used.
Seven challenges for communication and interaction in the dementia context
Several factors potentially contribute to difficulties in communication between family
carers and people living with dementia, and it is these factors that need to be
accommodated and explained in the conceptual modelling that follows. Understanding change: Carers can have difficulties understanding
the changing internal world of a person living with dementia. As cognition is
compromised, it can impact not only on memory capacity, but also personality and,
directly or indirectly, the content and manner of a person’s communication (Pozzebon, Douglas, & Ames,
2016). Meanwhile, the person living with dementia is also trying to
navigate these changes and may attribute them to others, and the environment. This
in turn complicates the carer’s task in trying to sustain stability in the
relationship and in everyday activities. Language: Dementia often causes changes in the production and
comprehension of language (Bayles
& Tomoeda, 2014; Obler & De Santi, 2000; Watson, Aizawa, Savundranayagam, & Orange,
2012; Wray,
2016). Carers may have difficulty understanding a person living with
dementia, as their diminishing linguistic resources impede or reduce expression, or
lead to unconventional solutions for getting meaning across (Pozzebon et al., 2016; Wray, 2016). Breakdowns in communication can
result in either the person living with dementia or the carer getting frustrated,
bored or tired about not being able to communicate as they would like; for example,
when the carer needs to repeat things many times, or the person with dementia
repeats the same anecdotes. Theory of mind: There is evidence that some people living with
dementia experience difficulties with theory of mind, i.e. inferring others’ mental
states on the basis of immediately available information (e.g. facial expression or
tone of voice) (Bora, Eryavuz, Kayahan, Sungu, & Veznedaroglu, 2006; Bora, Walterfang, & Velakoulis,
2015; Heitz et al.,
2016). This can put strain on the relationship with a carer, who may feel
underappreciated and unheeded. Role changes and interpersonal dependence: Increased dependence,
along with cultural expectations, typically result in changes in the roles and
relationship dynamics between a person living with dementia and a family carer
(Butcher, Holkup, &
Buckwalter, 2001; Russell, 2001). In turn, relationship changes may lead to departures from
pre-existing communicative and interaction patterns. For example, a spouse or child
may feel increasingly cast in a parent role (Pozzebon et al., 2016). During this
transition, there may be considerable uncertainty about how to respond appropriately
in certain situations (Polk,
2005; Wray,
2014). Grief: Carers may also be experiencing a complex grief response
(Butcher et al., 2001)
as they observe the ongoing changes that the person living with dementia is
undergoing, and experience their own emotional and social responses associated with
the “loss” of the person to the disease (Pozzebon et al., 2016). People have varying
capacity for “adaptive coping”: the assimilation and acceptance of this change that
will enable “restoration of coherence to the narrative of [their] lives” (Schut & Stroebe, 1999, p.
202). Practical pressures, fatigue and social
isolation: For many carers, the sheer quantity of hours during which they
are responsible for a person living with dementia, which may extend to 24-7, make it
all but impossible to get the emotional and physical distance needed for reflecting
on how they are responding during interaction (Wray, 2016). Social encounters are often much
reduced, and it can be difficult for some carers to seek support, if they fear
stigmatization, or that others will not understand the nature and extent of their
challenges (Pozzebon et al.,
2016). Attachment: Close family carers have significant “
Overall conceptualization
The framework that is proposed here draws together aspects of three theoretical accounts of
how human beings negotiate their world and maintain psychological wellbeing. Mentalization
Theory relates to our perceptions about ourselves and others. PCT concerns the ways in which
The intention is to present general principles without being positivistic. Every person is different and so is every interactional event. There are many cultural differences too, that shape communicative episodes. For example, in westernized culture, dementia is generally viewed as a medical condition caused by disease, but in some cultures dementia is considered as a mental illness or a normal part of aging (Hinton, Franz, Yeo, & Levkoff, 2005; Narayan et al., 2015). There is also substantial evidence that the experience of being a family carer differs significantly across cultural groups (Napoles, Chadiha, Eversley, & Moreno-John, 2010). In ethnic minority groups, subcultures can develop that contradict the dominant narratives of diagnosis and care (Cohen, 1998; Ikels, 1998; Mahoney, Cloutterbuck, Neary, & Zhan, 2005; McLean, 2007). Therefore, culture can have an important, varied and complex impact on carer experience. The framework we propose is not intended to undermine specific religious frameworks or cultural norms, or treat carers or people with dementia as one homogenous group. While it does assume that people with dementia experience cognitive and perceptual changes that are not a normal part of aging, it is shaped to inform techniques and training interventions that can be used creatively to explore the meaning and implications of individuals’ religious and cultural frameworks.
Mentalization
Mentalization is “the imaginative mental activity that enables us to perceive and interpret human behaviour in terms of intentional mental states (e.g., needs, desires, feelings, beliefs, and goals…)” (Fonagy & Luyten, 2009, p. 1357). This “holding the mind in mind” (Allen, Fonagy, & Bateman, 2008, p. 3) begins with ourselves, but needs to extend to imagining the mental states of others. We do not have direct access to others’ mental states, so we are reliant on various indirect points of access. One is our experience of our own mental states. We are likely to make associations with states and behaviours that we have experienced ourselves. For example, if someone looks tearful, we may infer likely thoughts contributing to this emotional response with reference to what we think would lead us to a similar response, e.g. someone has just said something unkind, or an event has put them in mind of something sad. However, our own mental states are not always a reliable point of reference, for at least two reasons. Firstly, we do not necessarily understand ourselves very well, and therefore are compromised in making inferences about others (Allen et al., 2008). Secondly, we may have complex and inaccurate beliefs about the connections between our own mental states and external factors, built up over many years; these may then influence how we interpret the nature of, and reasons for, others’ states of mind.
A second point of access is our pre-existing models of the mind of the particular individual, based on knowing them for a long time, and experiencing them from our own (previous) role perspective. As roles, situations and personalities change in the course of dementia, it will become difficult to fully sustain these models, and attempting to do so may eclipse the cues indicating what the other person is actually communicating. If emotions are high, a carer will likely find it hard to slow their thinking down to evaluate the best approach in communication and care. This is because “mentalizing goes offline in the context of intense emotional arousal as the fight-or-flight response comes online” (Allen et al., 2008, pp. 133–134). At times of intense emotional arousal, patterns of brain functioning and responding can become more automatic and instinctive (Arnsten, Mathew, Ubriani, Taylor, & Li, 1999; Mayes, 2000). The threshold for switching from a mentalizing and flexible response to a more automatic response will vary between individuals (Mayes, 2000).
Consequently, it will be easier for a carer to work with the seven challenges for communication (section 2) if he or she has capacity for “good mentalizing”: an accurate and effective understanding of (a) his or her personally important goals and (b) the other person’s perspective that takes into account what is really important to them. As we shall see later, goals, rather than externalized behaviours, are crucial to understanding the dynamics of communication, and they are key to how mentalizing occurs. Research suggests that carers’ attempts to mentalize are worth the effort. A recent analysis of video data from nine people living with dementia highlighted that even when the carer could not understand the message that was being communicated, attempts to understand and empathize were appreciated (Alsawy, Tai, McEvoy, & Mansell, 2017).
A key influence on Mentalization Theory is attachment theory, according to which infants are biologically predisposed to form attachments to those who (to a greater or lesser extent) protect, soothe and look after them (Ainsworth, 1978; Ainsworth, Blehar, Waters, & Wall, 1978). Bowlby (1982) proposes that from such interactions with caregivers, individuals develop a mental representation of the self in relation to others, along with expectations about they should behave, and how others will behave, in social relationships. These constitute an important default for mentalizing, and thus, internal representations of attachment relationships influence interactions in adults across a range of contexts (Gleeson & Fitzgerald, 2014; Korver-Nieberg, Berry, Meijer, & Haan, 2014; Robles & Kane, 2014).
Significant attachment relationships shape our sense of identity or self (Fonagy, 1999; Pittman, Keiley, Kerpelman, & Vaughn, 2011; Shaver, Mikulincer, Sahdra, & Gross, 2016). In dementia care, long-established attachment relationships are disturbed: the child becomes the carer of the parent, or the wife shifts from intimate partner to a carer role. The significant relational changes experienced may challenge carers’ sense of their own identity (Butcher et al., 2001; Shaver & Mikulincer, 2007; Tuomola, Soon, Fisher, & Yap, 2016). Nolte et al. (2013) found that in young healthy adults, attachment-related stress interfered with the functioning of brain regions associated with mentalization more than other kinds of stress did. Thus, the loss of the ability to mentalize, mentioned above, may be particularly acute in family relationships, where the stress is commonly attachment-related.
An example of an attachment challenge that family carers may face is the conflict between
wanting the person to be “as they were”, yet having to deal with them “as they are”, that
is, with the cognitive, memory, communication and personality changes resulting from
dementia: “Seeing the person they had known for so long, who still was physically the same
person but in many other ways so different, was an incongruity that at times seemed
unreal” (Butcher et al., 2001,
p. 46). As noted in section 2, grief is a common response to caring for a person with
dementia (Pozzebon et al.,
2016). A recent study of family dementia carers found that the changes associated
with dementia were often experienced as threats to knowledge, personhood and closeness
(Ennis, Tai, McEvoy, & Mansell,
2017). These constitute multiple potential losses, and a capacity for adaptive
coping (Schut & Stroebe,
1999) is not guaranteed. Where adaptive coping is successful, the capacity to
mentalize means that it will often manifest as a recalibration of the carer’s assumptions
and priorities, as in An example of adaptive coping by a dementia carer.
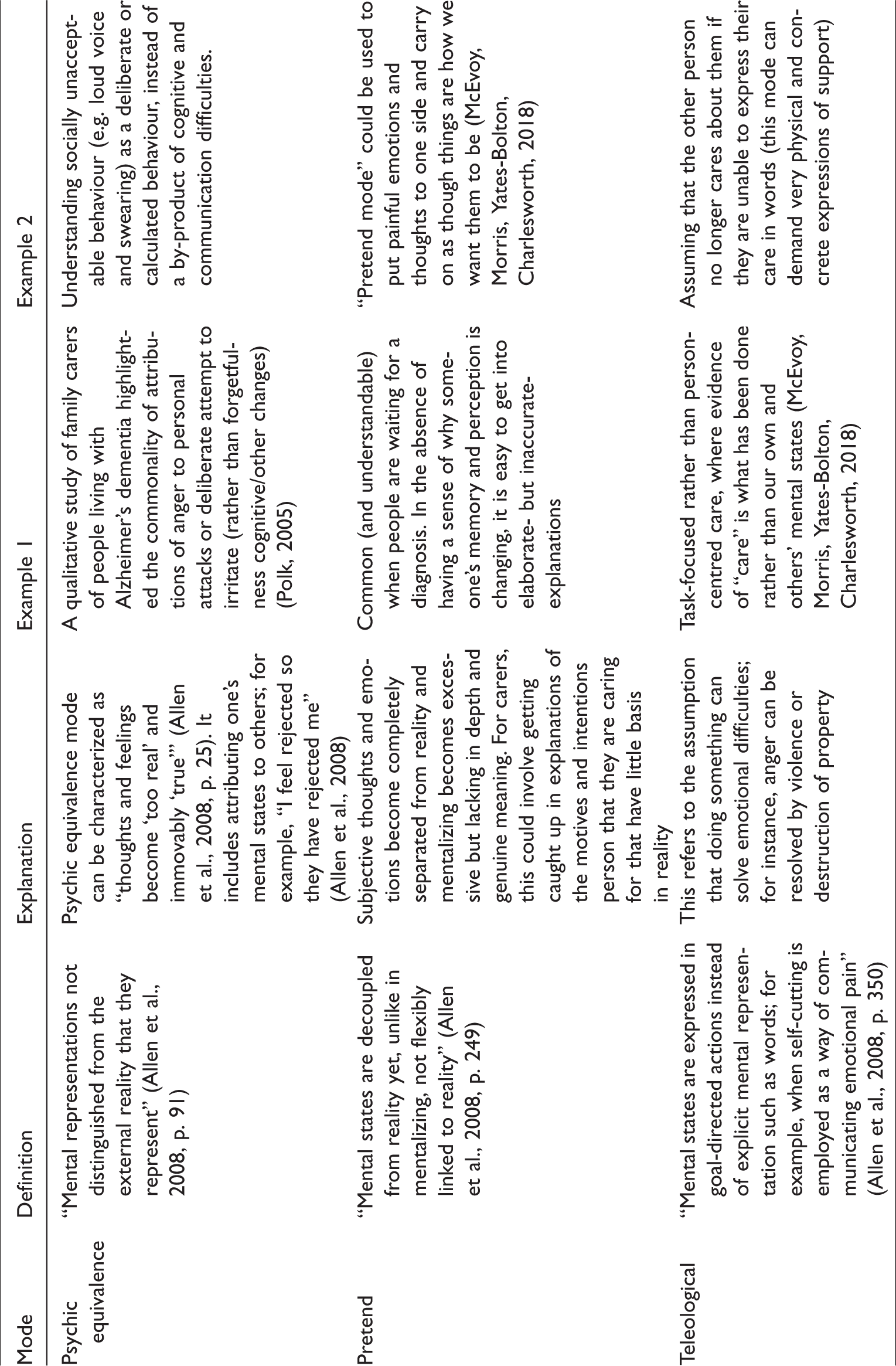
Certain detrimental “modes” can result from inadequate mentalization. In “psychic equivalence” mental states are experienced as external reality, e.g. because I feel angry, they intended to anger me (Allen et al., 2008, p. 25). In “pretend” mode, the mental state becomes detached from external reality, so that extensive mentalizing is needed to rationalize the feelings, e.g. explaining away dementia symptoms rather than facing the facts about their cause (Allen et al., 2008, p. 249). In “teleological” mode, mental states are externalized as actions, as with self-cutting to communicate emotional pain (Allen et al., 2008, p. 350). See Table 2 for more details of these mentalization modes.
Modes of experience when mentalization breaks down.

PCT and conflict
Where Mentalization Theory focuses on “modelling minds”, PCT relates more specifically to
the goals of those involved in interactions and how the individual engages externally. The
theory is based on the tenet that life, and thereby effective functioning, is a process of
Goals are conceptualized in a hierarchy, with the higher-levels, often associated with longer term values, setting the reference values for lower-levels (Powers, 1973). For example, the higher-level goal “be a good friend” sets the goal “keep in regular contact”, which could lead to actions such as texting friends, meeting regularly, etc. Higher-level references often represent longer term goals and values. Enduring conflict between higher-level references significantly contributes to loss of control and distress, as higher-level references specify a range of lower-level references (Alsawy et al., 2014; Kelly, Mansell, & Wood, 2011; Kelly et al., 2015).
The theory recognizes that since complete influence over events is rarely possible, the
way to sustain adequate control, and thus avoid conflict and distress, is to recognize and
adjust or abandon goals that cannot be achieved (Brandtstädter, 2009; Morris, Mansell, & McEvoy, 2016; Powers, 1973). This change happens
through a trial and error process termed reorganization (Powers, 1973). Full resolution of
internal conflict requires
People living with dementia may have a decreased capacity to rethink their situation, calibrate their goals appropriately, and act to achieve them, with the result that they experience reduced control (Moyle, 2010; Steeman et al., 2006). This leaves them vulnerable to their circumstances, making it vital that carers are able to manage any resulting externalized conflict, as explored in the next section.
Conflict and reduced Communicative Impact
Like PCT, Wray’s Communicative Impact model (Wray, 2016) identifies the achievement of personal goals as central to sustaining a sense of control over one’s life. Her model, however, specifically focuses on the role of communication in achieving these goals, and the “communicative impact” that a person’s interactive turns have in moulding their world as they want and need it to be. Much of the purpose of communication, in this view, is getting others to act as agents when it is not possible for the speaker to achieve change directly. Since people have multiple goals, communication is subtle. For example, a rude request to close a door may result in a closed door, but undermine the goal of sustaining a valued relationship. As a result, humans’ linguistic and non-verbal choices in communication are carefully tailored to navigate maximizing success on several fronts at once.
In dementia, communication is a significant casualty (Wray, 2018), with associated impact on the mental health of carers (Watson et al., 2012). The intricacies of effective communication, easily disturbed by changes in language patterns and relationships, are further undermined by the conflicts arising from unmet goals, as laid out in PCT. Interpersonal conflicts, such as arguments, expressions of frustration and anger, etc., can be conceptualized as external manifestations of internal conflict (Wray, 2016). Often, the failure to deploy communication effectively to achieve multiple, possibly contradictory, personal goals generates an emotional response (e.g. anger, stress or depression) that impedes effective mentalization.
Wray’s model offers specific insights into the problems that can occur when communicating
with a person living with dementia. One is a paradox that can arise between the desire to
treat a person living with dementia as “like me”, where the person’s behaviour as viewed
as bounded by normal social conventions, versus re-mentalizing, to see the person as “not
like me”, which accommodates any behaviour that would otherwise be upsetting or offensive
(Wray, 2013). The latter
option can protect the carer’s emotional state by neutralizing hurtful or annoying
behaviours. However, distancing like this could draw the carer into dehumanizing the
person with dementia. Wray argues that if the high-level goal of being a good person
conflicts with the high-level goal of self-protection through distancing, the carer may be
trapped in guilt and anxiety, leading to extreme stress. Wray proposes that if we once we
recognize how internal conflict can be the source of external conflict, “it becomes
possible to identify options for resolving conflict, which are not available if conflict
is located only in the external social space” (Wray, 2016, p. 117). Addressing conflicting goals.
Box 2 is an example of how awareness of internal conflicted goals can result in constructive attempts to meet the goals of all involved in the interaction. It was recounted by a carer at one of our Empowered Conversations training courses and has been fully anonymized and adapted to protect identities.
Towards supportive interventions in carer training: The Communication Empowerment framework
Carers may face many challenges, but they are also capable of identifying the positive aspects of their role (Brodaty & Donkin, 2009). Furthermore, people living with dementia can draw on considerable resources of resilience (Desai, Desai, McFadden, & Grossberg, 2016). One method for supporting both carers and people living with dementia is training for carers. Research indicates that the acquisition of knowledge and skills can support carer resilience and the maintenance of positive relationships with those cared for (Donnellan, Bennett, & Soulsby, 2015); for example, understanding how memory changes influence communication can enable more accurate mentalization. In particular, communication-focused training interventions can enhance perceived coping and control (Dias et al., 2015; Eggenberger et al., 2013; Harmell et al., 2011).
Jointly, the theories and models reviewed above offer new insights into how this can be achieved. In the Communication Empowerment framework, these theories are integrated; generating a means for emphasizing the importance of care partners trying to understand the perspective of the person they are caring for, while not losing sight of their own goals and experiences. This framework specifies how conflicts can arise and indicates how these can be addressed. It indicates other specific ways that communication can break down and be enhanced.
Training programmes need to provide techniques for responding to daily challenges that encourage the resolution of internal conflicts between higher-level goals, because this will increase the scope for control and thus promote resilience (Alsawy et al., 2014; Dias et al., 2015; Harmell et al., 2011; Morris et al., 2016). As noted above, reorganizing and resolving higher-level conflicts is also likely to improve communication, because it reduces the likelihood of external conflict. In turn, good relationships make it easier to spend time together and share activities, which people living with dementia identify as important to them (Alsawy et al., 2017). Carers benefit through the fulfilment of higher-level goals like creating joy and supporting the person living with dementia, commonly someone they have loved and known for a significant amount of time (Butcher et al., 2001; Russell, 2001). Raising awareness of higher-level goals thus exposes not only self-oriented priorities but also other-oriented ones, enabling a creative approach to working with conflicting goals (Morris et al., 2016).
Carers learn that even when an interaction features elements of conflict, such as
disagreement or verbal aggression, shared cooperative goals may underpin it. For example, it
is likely that both parties want to achieve lower-level goals (e.g. the successful eating of
a meal) alongside higher-level ones (e.g. sustaining calm and good humour). Drawing carers’
attention to the probability that any external conflict is not born of contradictory goals
but of different, perhaps misleading, ways of achieving aligned goals can be enough to help
the carer re-mentalize the situation to exploit the underlying harmony in their intentions.
Thus, even if there is conflict at one level of the The de-escalation of external conflict.
A key focus of the framework provided is recognizing how communicative behaviours on the part of the carer can unintentionally undermine the experience of control in the person they are caring for. For example, if the carer is aggressive, or unable to achieve basic communicative goals because of an internal conflict, the person living with dementia will have a reduced range of options for responding. Since enduring goal conflicts are likely to cause distress and stress (Gray et al., 2017; Kelly et al., 2015), helping carers to work around them is crucial.
Carers need to be supported in effective mentalizing, taking into account the current situation and not remaining in thrall to historical goals that can no longer apply. Mentalizing involves an integrated response to self and other and takes into account all perceptual data reasonably accurately, including the present situation, the likely perspective of the other person, and their own goals and emotional responses. “Great effort is required to attend to and reflect on mental states, especially when striving to hold multiple perspectives in mind in the midst of strong emotions” (Allen et al., 2008, p. 70).
It is also important to reassure carers that the temporary loss of mentalization is normal, since our attention fluctuates with context and mood. Thus, it is not a matter of having to sustain a highly deliberated perspective all the time, but of recognizing the risks of prolonged and intense loss of mentalization for precious interpersonal relationships. Ineffective mentalizing occurs when a particular mode (see Mentalization section) is used rigidly and inflexibly (Lemma, Target, & Fonagy, 2011; McEvoy, Eden, Morris & Mansell, 2016; Morris & Mansell, 2018). For example, if frustration becomes all-consuming, then it is likely to become difficult not to link it to the external reality (psychic equivalence mode – see Table 2), such as believing that the person with dementia is being deliberately annoying. If the teleological mode is entered, the carer may act on the emotion, by showing physical or verbal aggression (Asen & Fonagy, 2017a, 2017b). Although acknowledging anger is the first step, carers can be helped to recognize how, when anger is the dominant state, mentalizing becomes difficult and it is easy to lose perspective. That is, when people do things that they later regret and cause estrangement from those around them (Asen & Fonagy, 2017a). Particularly, potent forms of rigid control likely to affect carers include prolonged use of mentalization modes that enable emotional suppression. Rigid use of mentalization modes becomes problematic and distressing when this blocks the more important higher-level goals that are the truer reflection of the carer’s core intentions, such as commitment and care (Morris & Mansell, 2018).
Conclusion
We have shown how conflicts within and between people, with regard to their higher- and lower-level goals, are more or less inevitable, and that they are likely to result in emotional responses that shape the content and tone of communication. Since language is a window on our thoughts, it is very difficult fully to shield others from the emotive power behind our words and non-verbal signals. Carers of people living with dementia experience high levels of stress on account of their situation and the many conflicting goals they must deal with, including those that relate to their non-carer identities. They also often have a high level of commitment to maintaining connection with the person they are caring for.
Carers can be effectively supported by the opportunity to reflect on how these dynamics play out in their daily lives, and being helped to develop mentalization strategies that can give them the capacity to identify and then fulfil their own, and the others’, goals. We have described challenges that can affect communication between carers and people living with dementia. Responding creatively to these challenges and building on strengths and resilience can lead to more satisfying communication. This paper details specific psychological and relational mechanisms that can be targeted to enhance communication, the Communication Empowerment framework. This framework indicates (a) why it is important for both individuals in a conversation to feel that they have control and (b) how the carer can be equipped to recognize intra- and interpersonal goal conflicts and resolve them. Key elements that facilitate the resolution of internal and external conflicts include being able to recognize and express concerns (even if not always directly to the person with dementia), identify the source and nature of the conflict, engage with changes in emotion, and sustain an awareness of how thoughts and relationships are shifting.
For this reason, our training approach, Empowered Conversations, focuses on the above
elements, as a way of helping carers develop enhanced mentalization and facilitate
In summary, the key features of the Communication Empowerment framework enable it to generate direct practical implications. It supports care partners to “hold in mind” both their goals and the likely goals of the person they are caring for. It specifies ways in which communication can be impaired and related ways it can be enhanced; these include attention to emotion and non-verbal communication and the impact each of these can have on communication. Further, it delineates ways in which carers can be supported to identify and meet the important goals of all those involved in an interaction.
Footnotes
Acknowledgements
We thank Dr Margaret Garner for reviewing an earlier version of this manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This framework was developed as part of a project funded by the Big Lottery Fund (grant number 10010293441). This research was supported by an ESRC Impact Acceleration grant to Professor Alison Wray at Cardiff University.
![]()
![]()
![]()
