Abstract
Dementia is a progressive condition that can affect memory, thinking and communication in different ways. As a person’s communication patterns and needs change over time, care partners may need to adapt their approaches to continue supporting meaningful interactions and connection. Education to enhance the confidence and competence of care partners is therefore essential. This study evaluated an online first-year university unit designed to improve communication knowledge and skills in the context of dementia care. Using a pre-post survey design, the study integrated quantitative and qualitative data to assess changes in participants’ self-rated communication knowledge and confidence, as well as perceived impacts on practice. Quantitative measures revealed significant improvements in all assessed domains, with p-values <.001 and effect sizes ranging from moderate to very large (Glass’s Δ = 0.57–1.51). Qualitative findings supported these outcomes, with participants reporting enhanced communication practices, more person-centred care approaches, and greater knowledge sharing. These results highlight the value of targeted, dementia-specific education in fostering meaningful changes in communication and care delivery. The study also outlines practical implications for research and practice.
Background
Dementia is a neurological condition that involves progressive changes in cognition (Barber, 2020). It can affect memory, orientation, language, thinking, behaviour, and everyday functioning (Sabat, 2018; World Health Organisation, 2023). Changes in communication are a common feature, including difficulties in information processing, verbal expression, coherence, and fluency (Banovic et al., 2018; O’Brien et al., 2018). The nature and extent of these changes differ from person to person and vary depending on the type and stage of dementia (Banovic et al., 2018; Bourgeois & Hickey, 2009; Pepper & Dening, 2023b; van Manen et al., 2021). For example, in the early stages of Alzheimer’s disease – the most common form of dementia – an individual may experience subtle difficulty in word-finding and understanding complex language structures (Savundranayagam & Orange, 2014). As the condition progresses, there are often more noticeable changes in attention span, topic maintenance, information retrieval and conversation flow (Bourgeois & Hickey, 2009; Wray, 2020).
Such changes in cognitive-linguistic functioning affect how individuals feel able to participate in everyday interactions, and increasing effort is required to sustain meaningful engagement (Dooley & Walshe, 2019; Moyle, 2023). This can cause anxiety, embarrassment, frustration, or distress for some people living with dementia (Hamilton, 2019; Wray, 2020). Difficulties in understanding and expression may also affect confidence, self-esteem, and social participation (Alsawy et al., 2019; Nickbakht et al., 2023). All of these factors can shape emotional wellbeing, relationships, quality of care, and overall quality of life for people living with dementia (Downs & Collins, 2015; Machiels et al., 2017; Moyle, 2023). It is critical that interactions with people living with dementia are strengths-based, individualised, and focused on factors they have identified that help them live well.
Just as it is challenging for people living with dementia, it can also be difficult for formal and informal care partners, including families, carers, nurses, healthcare professionals, and others providing care or support, to ensure a positive experience for everyone involved. As communication patterns and needs change over time, care partners play a vital role in interpreting verbal and non-verbal cues and adapting strategies to better understand and respond to each person’s needs (Dooley & Walshe, 2019). This can be a demanding task, especially when there are changed behaviours due to unmet needs (Nguyen et al., 2022; Pepper & Dening, 2023a). Communication difficulties can contribute to care partners’ stress, burnout, and strain in relationships (Karg et al., 2018; Morris et al., 2021; Roberts et al., 2022; Watson et al., 2012).
Despite these challenges, people living with dementia and their care partners can be supported to achieve positive outcomes. In the earlier stages of common dementias, many communication abilities remain largely intact, such as pronunciation, grammar, oral reading, comprehension of familiar written texts, and contributing to conversations (Bourgeois & Hickey, 2009; Wray, 2020). As the condition becomes more advanced, even when verbal communication becomes limited or is no longer possible, people living with dementia often retain the ability to express and interpret feelings and respond non-verbally to sensory stimuli (Bourgeois & Hickey, 2009; Cornish, 2017; Evans-Roberts & Turnbull, 2011). This suggests that with the right support and encouragement, it is possible for people living with dementia to continue to connect with others and co-construct positive interactional experiences (Brandão et al., 2024).
For care partners, acquiring dementia-specific communication skills enhances interactions with people living with dementia (Wray, 2020). Understanding the person’s abilities and knowing how to apply facilitative, strengths-based strategies enable care partners to adopt a more therapeutic person-centred approach, thereby improving communication (Brandão et al., 2024). Recognising the value of meaningful interactions also encourages care partners to engage in more supportive practices, such as being attentive listeners or validating feelings to foster a sense of being heard and valued (Alsawy et al., 2019). Exploring ways to connect with the person living with dementia, both physically and emotionally, allows care partners to show respect for their dignity as individuals with unique identities, feelings, and thoughts (Pulsford & Thompson, 2020; Wray, 2020).
For the above reasons, it is crucial to offer effective educational programs that enhance the confidence and competence of care partners in fostering meaningful engagement with people living with dementia and responding appropriately to their changing abilities and needs. A number of stand-alone educational programs have been developed and evaluated, primarily focusing on discrete aspects of communication, such as verbal and non-verbal skills, or techniques for responding to changed behaviours (Nguyen et al., 2019). Other studies on dementia care and communication have typically evaluated education or training within broader healthcare disciplines (Dahlke et al., 2024; Williams & Daley, 2021), rather than within programs dedicated specifically to dementia. This paper reports on the evaluation of a dementia-specific communication unit (the DCU) - an online first-year university unit designed to improve communication knowledge and skills in dementia care through comprehensive and rich content. This unit is part of a university degree program aiming to develop specialised knowledge in dementia care, alongside education on the biology and pathology of dementia, care principles, therapeutic approaches, post-diagnostic supports and services, and cultural safety. The findings of this study are expected to contribute to the existing evidence on the impact of educational efforts in dementia care and to inform the design and delivery of interventions to enhance the communication competence of care partners of people living with dementia.
Methods
The DCU
This single-semester unit was developed and refined based on literature about dementia-specific education programs and the needs of families and carers of people living with dementia. The DCU integrates both theory and skill-building to maximise effective communication in dementia care settings. It is designed to equip learners with knowledge about dementia-related changes in communication, factors affecting communication experiences in dementia care, and strategies to enhance communication outcomes in various situations. It encourages learners to create a more supportive and inclusive environment where the person is respected and offered opportunities and choices for interaction. It also enables learners to understand the lived experiences of people with dementia and to see from their perspective when communicating with them. Firsthand accounts, such as published personal narratives, memoirs, and videos featuring people living with dementia and their care partners, are integrated into learning materials where appropriate. This helps ensure that their voices are heard and provides authentic contexts for discussion and reflection. Delivered online, the unit provides many opportunities to engage with the contents and interact with others, including video lectures, readings, scenario-based discussions on discussion boards, guided reflections, automated formative quizzes, and web-conferencing tutorials. Learners are advised that the unit will require approximately 130 hours of learning in total. The content structure of the DCU is presented in Figure 1. DCU’s content structure and learning activities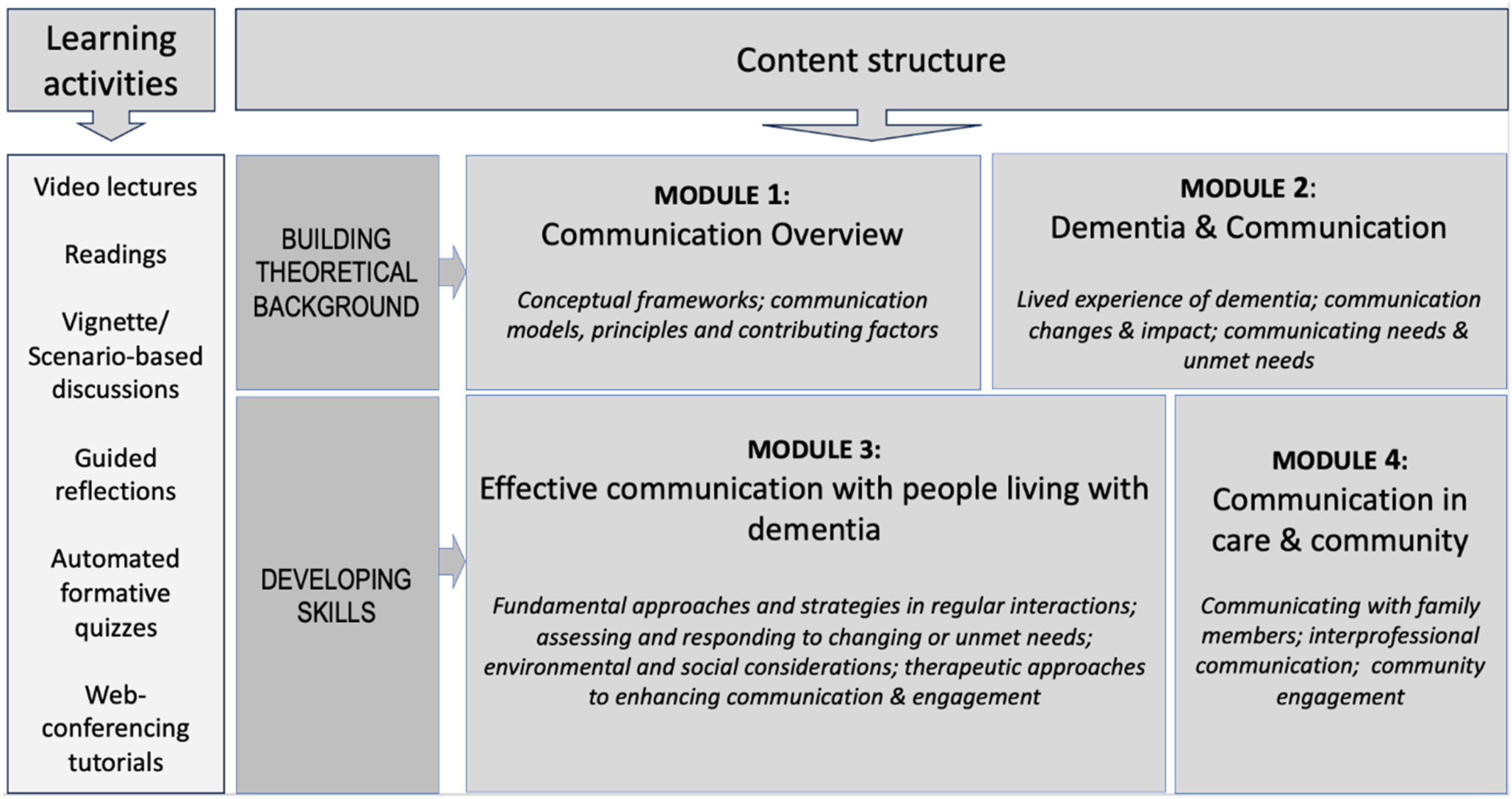
Study Design and Participants
A pre-post survey design was used in this evaluation study to identify potential changes in self-rated knowledge and confidence in communicating with people living with dementia. Participants were recruited from learners undertaking the DCU in February – May of both 2023 and 2024. All enrolees were invited to participate in the study via an email invitation with a link to the Participant Information Sheet. It was made clear that participation was voluntary and involved completion of an anonymous online survey at the commencement (orientation week) and completion (week 13) of the unit. The study received ethics approval from the University of Tasmania Human Research Ethics Committee (Ethics approval reference number: H0028597).
Outcome Measures and Data Analysis
The key outcomes are participants’ self-rated knowledge and confidence in communicating with people living with dementia. These two outcomes were measured using a questionnaire developed by the authors, based on literature review and research about carers’ communication experiences and needs. Both pre- and post-surveys included demographic questions and 15 self-rated questions about various aspects of dementia-specific communication knowledge (on a 5-point Likert knowledge scale from 1 = Very poor to 5 = Very good) and confidence in performing different communication skills (on a 5-point Likert confidence scale from 1 = Not at all confident to 5 = Extremely confident). The post-survey had an additional set of questions about perceived impacts of the DCU on participants’ general knowledge, confidence, and current or future practice regarding dementia-specific communication. These questions were either closed-ended (on a 5-point Likert rating scale from 1 = Not at all to 5 = To a very large extent) or open-ended.
Guided by a convergent mixed-methods approach (Creswell & Plano Clark, 2018), the quantitative and qualitative data collected from the survey were analysed separately and then integrated during interpretation to provide complementary insights into the unit’s impact. The quantitative results indicated the size and direction of changes in knowledge and confidence, while the qualitative data provided contextual detail not otherwise available, such as how these changes occurred and how they influenced participants’ communication and care practices. Both descriptive statistics and inferential statistics were employed to analyse the quantitative data (via SPSS version 26). Descriptive statistics (e.g. percentage, mean, standard deviation) were used to present demographic data, self-rated knowledge and confidence of participants, as well as perceived impacts of the DCU. Inferential statistics, including Student’s t-tests and Welch’s t-tests, were conducted to determine if there was a significant difference in participants’ self-rated knowledge and confidence before and after the educational program. The magnitude of the effect size was determined using Glass’s delta. Participants’ textual responses to the open-ended questions were imported into Nvivo (version 14) and thematic analysis (Braun & Clarke, 2019) was used to analyse this qualitative data. Codes were initially developed to capture key ideas, which were then organized into themes based on their relationships. The final themes were reviewed and refined by the team to ensure relevance and clarity. These themes are described in the findings with illustrative participant quotes, including reference to participant ID, role in dementia care, and years of caring experience (e.g. P26_Residential Carer_2y).
Findings
Participant Description
Demographic Description of the Participants
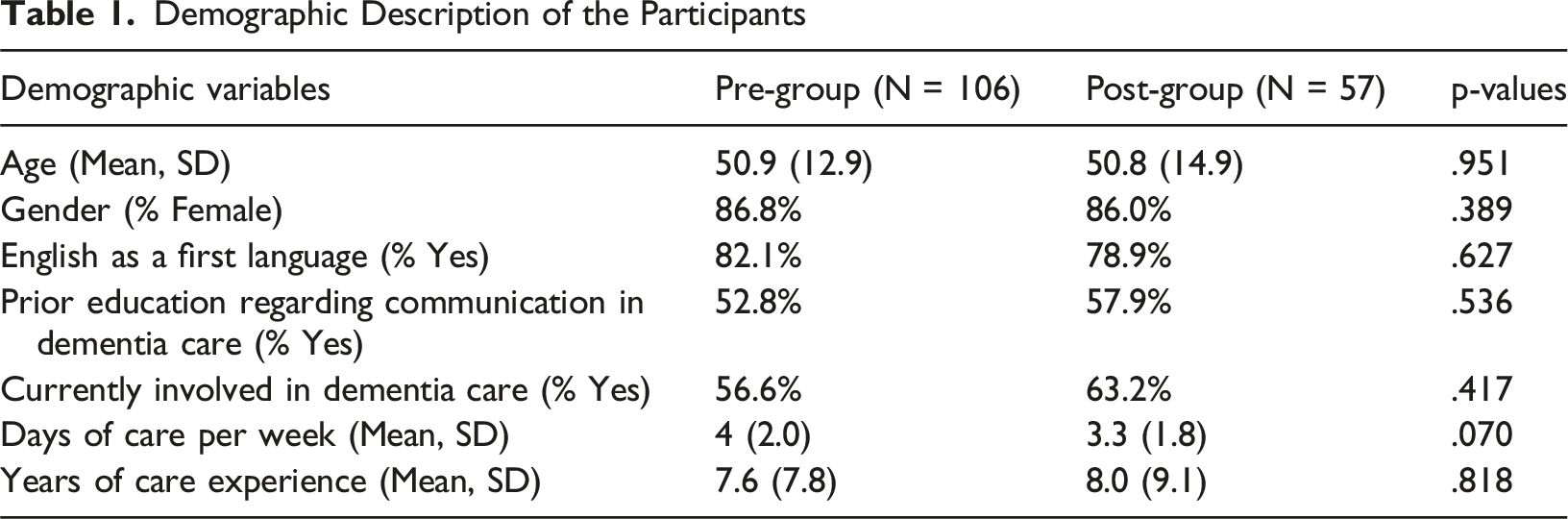
Quantitative and qualitative findings of this evaluation study are presented under the key outcomes: self-rated communication knowledge and confidence; and perceived impacts of the DCU.
Self-Rated Communication Knowledge and Confidence
T-Test Results of Self-Rated Communication Knowledge
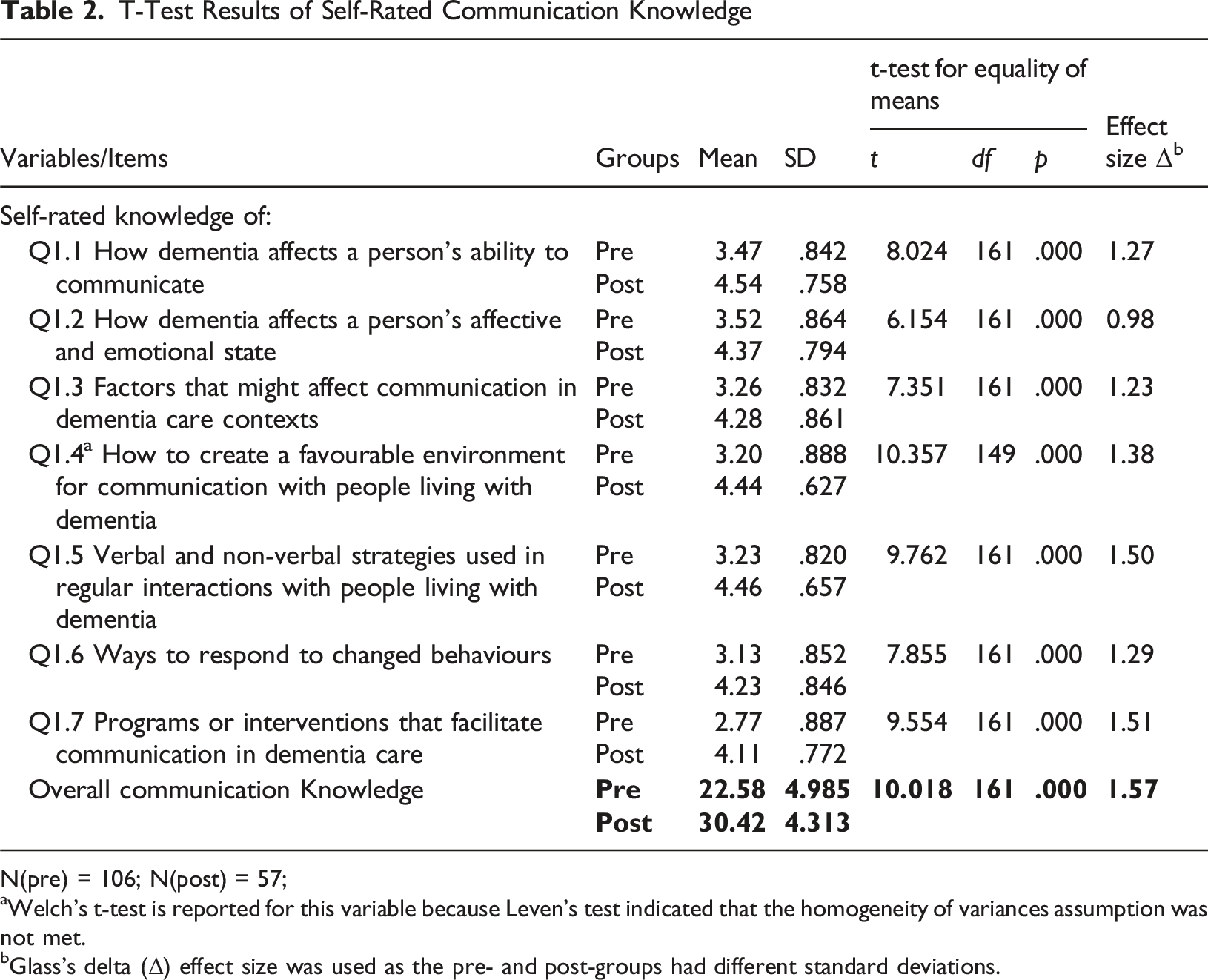
N(pre) = 106; N(post) = 57;
aWelch’s t-test is reported for this variable because Leven’s test indicated that the homogeneity of variances assumption was not met.
bGlass’s delta (Δ) effect size was used as the pre- and post-groups had different standard deviations.
T-Test Results Regarding Self-Rated Communication Confidence
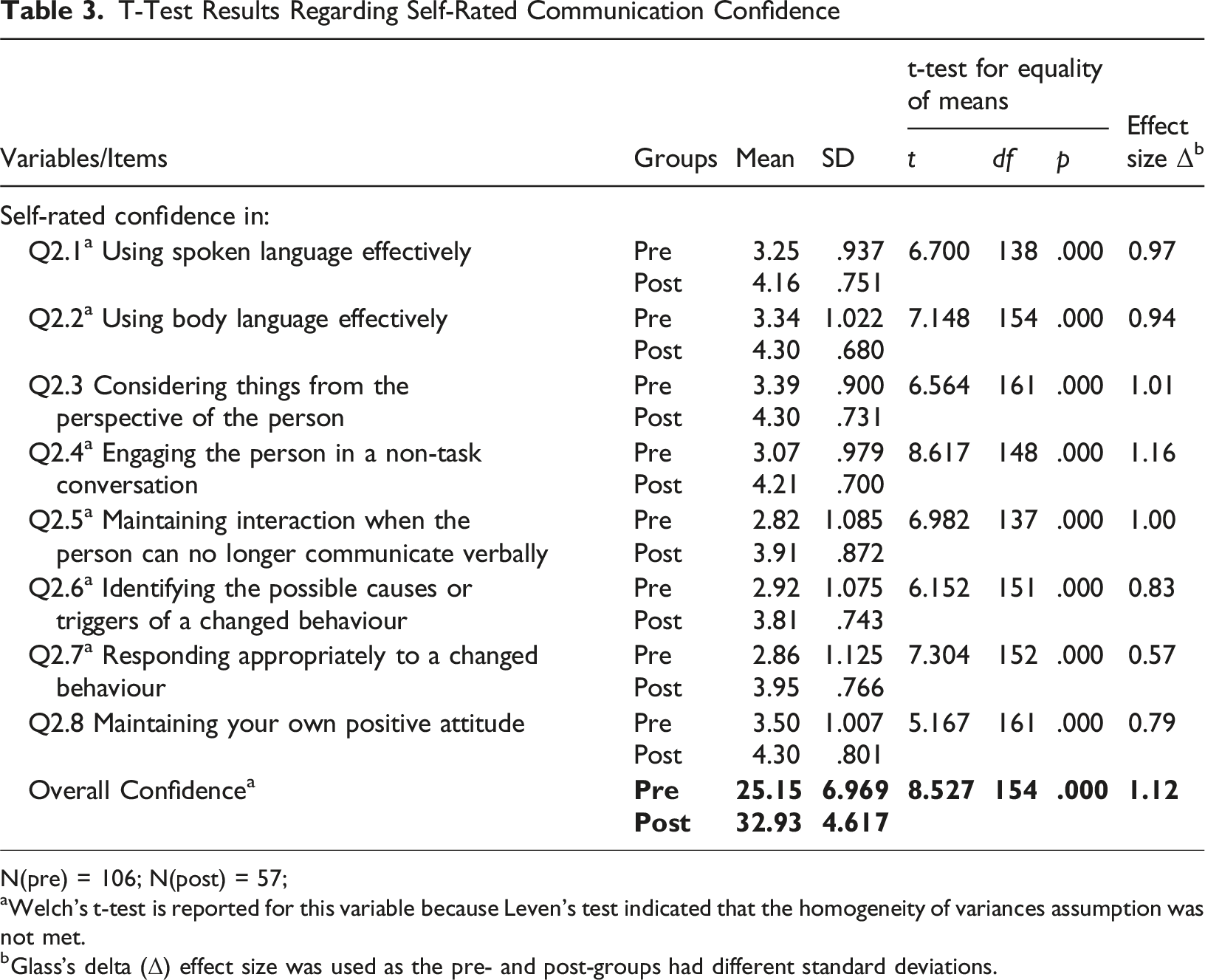
N(pre) = 106; N(post) = 57;
aWelch’s t-test is reported for this variable because Leven’s test indicated that the homogeneity of variances assumption was not met.
bGlass’s delta (Δ) effect size was used as the pre- and post-groups had different standard deviations.
Self-rated communication knowledge scores were significantly different between the two groups across all seven aspects of dementia-specific communication, with all p values less than .001 and t-values ranging from 6.154 to 10.357 (Table 2). Glass’s delta effect sizes were large to very large (0.98–1.51), indicating the substantial impact of the DCU on participants’ perceived knowledge. The variable with the lowest rating in both groups and the highest effect size was knowledge of interventions that facilitate communication in dementia care.
Similarly, regarding self-rated confidence scores, significant differences were found across all eight communication skills (p < .001; t = 5.167 – 8.617), with the post-group consistently reporting higher confidence than the pre-group (Table 3). Glass’s delta effect sizes ranged from 0.57 to 1.16, reflecting a moderate effect for one skill (Q2.7_Responding appropriately to a changed behaviour), and large to very large effects for the remaining skills. These results indicate a strong overall impact of the DCU on participants’ communication confidence. The items with the lowest confidence ratings of both groups included: identifying causes of changed behaviours, responding appropriately to changed behaviours, and maintaining interaction when the person no longer could communicate verbally.
Perceived Impacts of the DCU
Perceived Impacts on Communication Knowledge and Confidence
With regards to participants’ perceived impacts of the DCU, the results demonstrated strong positive outcomes for a vast majority of the post-group (n = 57; Figure 2). A significant proportion of participants (93.0%) reported that the unit increased their general knowledge of communication in dementia care to a large or very large extent. The unit also had a positive impact on participants’ confidence, with 86.0% reporting their general confidence in communicating with people living with dementia increased to a large or very large extent. Results of perceived impacts of the DCU unit (n = 57)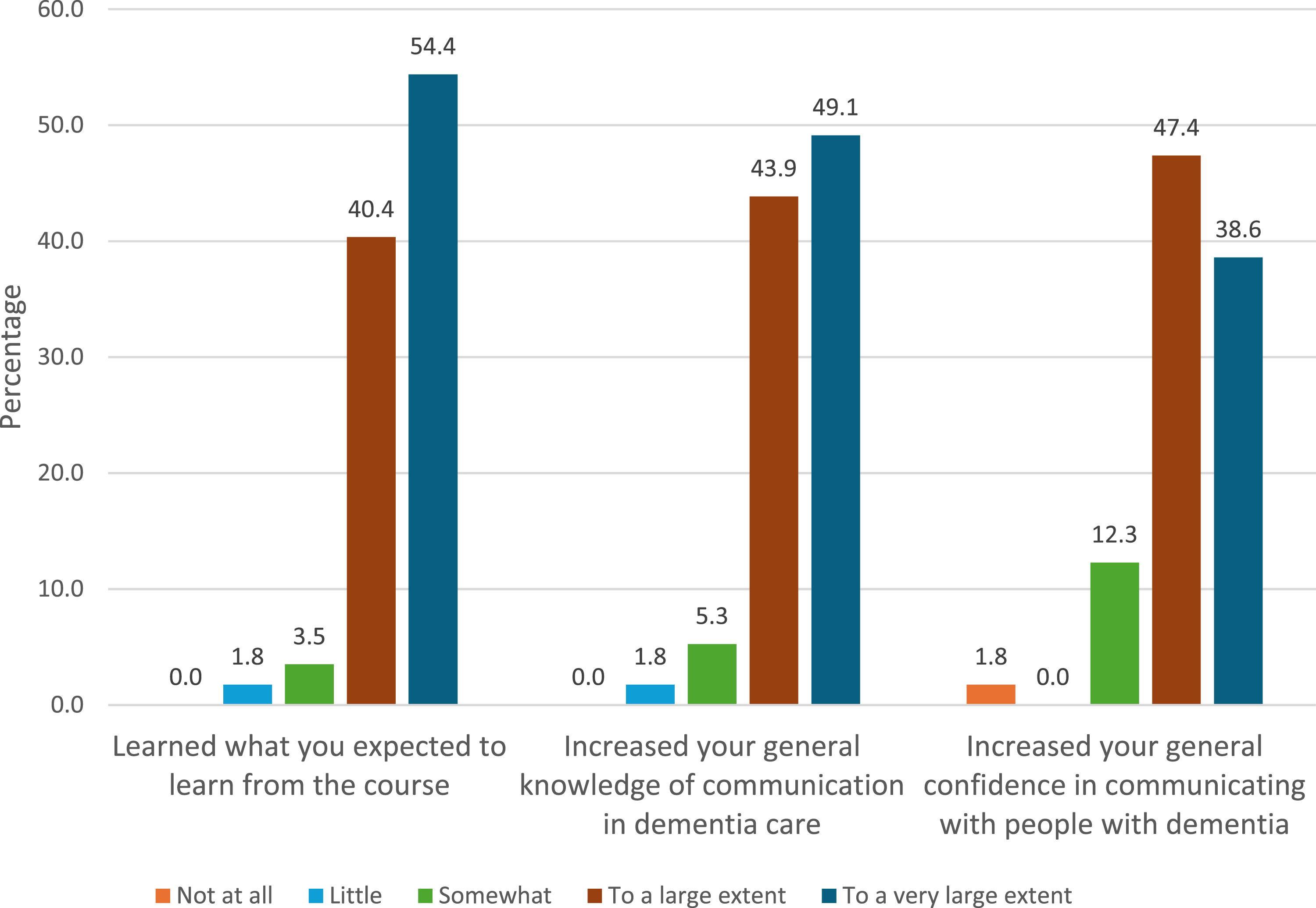
Additionally, an overwhelming 94.8% indicated that they learned what they expected to learn from the unit to a large or very large extent, suggesting a close alignment between the unit content and learners’ expectations. Responding to the open-ended question about topics to address further in the unit, some participants suggested more in-depth exploration, and more practical examples, of interactions with individuals no longer able to communicate verbally, and assessment of potential triggers and appropriate responses to changed behaviours.
Perceived Impacts on Current and Future Practice
In terms of the DCU’s impacts on participants’ current and future practice, qualitative data revealed encouraging outcomes under three key themes: improved communication practice, enhanced care delivery, and increased capacity for knowledge sharing.
Improved Communication Practice
Many participants reported that the unit improved their ability to engage with people living with dementia and others in the care settings, enabling them to “implement different strategies” (P13_Community Care Worker_3y) for more effective communication. I am certain that my interactions are much more positive now having done this unit. I know that I can make a difference and know that I can help make people living with dementia feel more safe and less anxious about what is happening. (P33_Physiotherapist_36y) I can now communicate better with the residents at the RACF I work at. I can also facilitate better communication between the residents and my co-workers, or specialists that visit. (P26_Residential Carer_2y)
Participants particularly highlighted greater awareness of the various factors that influence communication in dementia care, including both environmental and individual aspects. Being more attuned to these influencing factors allowed them to adjust their approaches to improve communication outcomes. I came to understand the importance of adapting my communication approach when interacting with individuals living with dementia. This involves tailoring my methods to suit the specific environment, such as addressing background noise from the TV. (P52_Lifestyle Assistant_7y) I will be more thoughtful about how I communicate with people living with dementia… My tone, language and body language will be tailored to suit the situation. (P16_Volunteer Carer_2y) This unit has reminded me of the importance of empathy, patience, and the importance of recognising and meeting the psychological needs of people living with dementia. (P56_Family Carer_4y)
Another prominent impact was a reported increase in participants’ confidence when interacting with people living with dementia, which aligned with the quantitative findings. “I now have the confidence to engage in communication” (P24_Famiy Carer_2y) or “This subject has enhanced my skills and confidence to the next level” (P01_Family Carer_2y) were comments that echoed among participants after completing the unit. They particularly reported higher self-assurance in their ability to use person-centred communication strategies and respond to the emotions of the person with dementia. I’m more confident to implement some strategies (verbal, paraverbal and non-verbal) in my practice when I work with people living with dementia, with person centred principles. (P46_Aged Care Assessment Clinician_6y) I feel much more confident about how to understand the distress and anxiety of people I encounter who are living with dementia. (P32)
Overall, equipped with a broader repertoire of communication strategies, enhanced awareness of influencing factors, and increased confidence, participants reported being empowered to communicate more effectively in dementia care settings. Such positive changes in communication practice were believed to not only enhance day-to-day interactions but also build the foundation for the provision of quality care.
Enhanced Care Delivery
Participants noted improvement in their delivery of care as a result of the unit completion. One notable aspect was their enhanced ability to recognize and address unmet needs of people living with dementia. Some participants reported being more able to recognise subtle cues or expressions that might indicate underlying issues, and this allowed them to respond more promptly and proactively to needs that may have otherwise gone unnoticed and/or unmet. I respond more appropriately to unmet needs now that I know what an expression of them may look like. I am constantly on the lookout for needs that may be going unmet. I provide better care and hopefully I'm improving the quality of life for those I am working to support daily. (P26_Residential carer_2y)
The knowledge and skills gained from the DCU also reportedly helped participants in developing better care plans. “My care plans will be better”, Participant 11 (Case Manager_2y) expressed. This could be attributed to their better understanding of the person living with dementia, as explained by some participants. Having more knowledge and awareness of the difficulties people living with dementia might have with communication helps me to take better care of my clients. (P55_Homecare Social Support Worker_2y) I am better now at seeing from their perspective more than I was. (P33_Physiotherapist_36y)
Expanding on this, other participants highlighted how the DCU reinforced the importance of seeing the person behind the condition or “recognising the individual and personal narrative” (P52_Lifestyle Assistant_7y), which is integral to the delivery of empathetic and individualised care. I see the person for what they really are, beyond the dementia and what they were before. There’s so much I have learnt from them by just listening and engaging in conversations with them. (P16_Volunteer Carer_2y)
All of this could be expected to help foster a better understanding of the person, a heightened commitment to meeting individual needs, and hence a more compassionate person-centred approach to dementia care.
Increased Capacity for Knowledge Sharing
In addition to the DCU’s perceived impacts on communication and care practices, many participants expressed greater confidence in sharing what they had learnt with colleagues or those providing care and support for people living with dementia. Comments like “I will pass the knowledge and skills on to my colleagues” (P46_Aged care Assessment Clinician_6y), or “share this information with my colleagues to improve overall practice at our facility” (P17_Registered Nurse_14y) showed participants’ willingness to contribute to a culture of continuous learning for improved practice. Elaborating on this, some participants felt better equipped to discuss a communication situation or passing on useful materials. I think I can explain better to other people why a situation is happening and help them understand the behaviours. (P08) I feel that I am now better able to source information on communication techniques and share these resources with my colleagues. (P28_Residential Carer_15y)
Learnings from the unit seemed to have expanded participants’ role beyond caregiving, enabling them to become a champion for more effective communication and care, both within their organisations and in the wider community. The following comment illustrates this readiness for knowledge sharing across care and support networks around people living with dementia. I feel empowered to educate my colleagues and others involved in the care of people with dementia, including community groups, regarding effective communication with people living with the condition. I have been inspired to develop and support programs that facilitate opportunity for inclusion and contribution, as well as communication and social connection, for people living with dementia in our local community. (P48_Community Support Worker_6y)
Discussion
This paper demonstrates the impact of the DCU, a dementia-specific communication unit, embedded within a larger university program on dementia care. Notably, participants reported significant improvements across all areas of knowledge and skills related to communicating with people living with dementia. This suggests that the DCU effectively supports the acquisition of key aspects of communication competence in dementia care. These findings on improved knowledge and confidence accord with a wide range of studies worldwide that have demonstrated the positive impacts of education and training in enhancing care-partners’ communication competence in this care context (e.g. see reviews by Carrier et al., 2023; Nguyen et al., 2019).
It was found that the knowledge gained from the DCU had been translated into day-to-day communication practice of those directly involved in the care and support of people living with dementia. Participants particularly highlighted their improved ability to adapt communication strategies and respond sensitively to the emotions of people living with dementia. These skills are essential for facilitating meaningful engagement and promoting understanding (Alsawy et al., 2019; Pepper & Dening, 2023b), which can foster trust and strengthen relationships. This is especially important in dementia care settings where communication can be affected by cognitive-linguistic changes, emotional responses, and other factors such as sensory or perceptual changes (Coleman & Asiri, 2020; Hamilton, 2019; Wray, 2020).
As a result of greater attention to non-verbal cues and communication strategies, participants also reported a shift in their care practices towards a more individualised and empathetic approach. They described becoming more proactive in responding to subtle cues of needs and viewing the individual as a person, rather than focusing solely on symptoms. These changes align with the broader person-centred principles widely promoted to optimise communication and dementia care (Coleman & Asiri, 2020; Downs & Collins, 2015; Fazio et al., 2017). Although the unit primarily focused on enhancing communication, its impact on care practice, as demonstrated in this study, reflects the interdependence between communication and care in dementia settings. This relationship is well established in the literature, with positive interactions recognised as an essential component of effective person-centred dementia care (James & Gibbons, 2019; Kitwood, 1997; O’Rourke et al., 2022). These findings further highlight the significance of communication competence in ensuring quality care and ultimately improving wellbeing outcomes (Dampney-Jay, 2015; Perkins et al., 2022).
Another important finding was that learnings from the DCU not only enhanced participants’ knowledge and practice, but also expanded their roles and scope of influence. Participants reported that the unit empowered them to take on more active roles in sharing knowledge among colleagues, families, and the wider community. This emerging role as advocates for best practices demonstrates the broader impact of educational interventions like this unit, extending beyond the individual learner. This finding underscores the pivotal role of dementia-focused education and training in “driving and transforming practice change” (Surr et al., 2023, p. 2).
The DCU was designed to foster deep and meaningful learning by integrating theory with practice and using multimodal delivery strategies, which is in line with evidence-based approaches to effective dementia education (Moehead et al., 2020; Phillipson et al., 2016; Surr et al., 2017, 2023). Notably, scenario-based discussions and reflective practice played a crucial role in bridging theory and practice. These discussions enabled participants to situate their learning within the practical realities of dementia care, drawing on personal experiences and diverse perspectives to co-construct knowledge and strengthen their ability to respond appropriately to people living with dementia. This approach reflects the principles of Situated Learning Theory (Lave & Wenger, 1991; O’Brien & Battista, 2020), which highlights the importance of learning within authentic contexts and through social interaction. The real-world scenarios allowed participants to see the applicability of their learning, an essential feature of effective dementia education (Rasmussen et al., 2023). Furthermore, interactive peer-to-peer learning in supportive environments, such as these online discussions, is especially valuable in programs designed to build dementia skills and knowledge (Cobbett et al., 2016; Gulline et al., 2025; Norris, 2024).
Reflective practice was another key component that may have contributed to the DCU’s overall impact. Through structured reflections on their observations and experiences in dementia contexts, participants were encouraged to move beyond surface-level engagement to critically evaluate interactions, identify areas for growth, and adapt approaches for better outcomes. By placing critical reflection at the heart of the learning process, the unit’s pedagogy aligns well with Transformative Learning Theory (Mezirow, 1991, 2018). This theory posits that when learners reassess their existing beliefs and assumptions, they are better positioned to make informed positive changes. Reflective practice is therefore considered vital in healthcare educational programs (Mantzourani et al., 2019; Weller-Newton & Drummond-Young, 2023), and especially in dementia-specific communication interventions (O’Rourke et al., 2022).
Although the DCU effectively addressed a significant need by providing communication education tailored to dementia care settings, the findings also highlight areas for further development, particularly in supporting care partners to assess and respond to changed behaviours. While this topic was included in the unit, more structured and detailed guidance could enhance learners’ confidence and competence in navigating these often-distressing situations (Dookhy & Daly, 2021; Duxbury et al., 2013). Additional emphasis on strategies for engaging with individuals who are non-verbal or have limited verbal communication would also benefit care partners. In addition, considering the current lack of direct involvement of people with lived experience, the unit could be further enhanced by engaging individuals living with dementia in the co-design of its content. Addressing these areas in future iterations or expansions of the unit will help ensure care partners are well equipped to meet the complex and evolving communication needs of people living with dementia.
Overall, the study demonstrates that learnings from the DCU led to improvements in communication practice, care delivery, and knowledge sharing. It reinforces the importance of integrating practical communication strategies with a broader understanding of the lived experience of dementia, and highlights the need for multimodal, context-specific, and reflective approaches to education. The findings contribute to the growing body of evidence supporting the value of educational programs for care partners of people living with dementia, particularly those focused on communication (Nguyen et al., 2019, 2022; Perkins et al., 2022). In particular, the study demonstrates the impact of an educational offering situated within a broader program dedicated to dementia care. The use of a pre- and post-survey design, combining both quantitative and qualitative data, strengthened the findings by capturing changes over time and offering rich insights into the unit’s impact. While the results are promising, they should be interpreted with some caution given limitations such as the absence of a control group, and reliance on self-reported data. Due to the study’s scope and resource constraints, the design focused on assessing short-term changes in participants’ communication knowledge, confidence, and practice. Future research could incorporate comparison groups or longer-term follow-up to enhance the robustness of the evidence.
Recent reforms in the Australian aged care system, such as the new rights-based Aged Care Act (Australian Government, 2024) and strengthened Aged Care Quality standards (Aged Care Quality and Safety Commission, 2025) emphasise the need to understand and respond to the communication needs and preferences of people receiving care. The National Dementia Action Plan expressly identifies this need for people living with dementia (Australian Government Department of Health and Aged Care, 2024). Effective communication strategies, particularly for people living with dementia, are fundamental to meeting this reform agenda, and courses such as the DCU support the development of these skills in care partners. The unit aligns with the National Dementia Education and Training Standards Framework (Dementia Training Australia, 2024), particularly Domain 7: Communication and Connection, which emphasises understanding the impact of cognitive changes on communication and developing skills to enhance interactions and relationships. Communication is also integral to other domains, such as Domain 4: Person-Centred Care and Domain 11: Behaviour, highlighting its relevance to difference aspects of dementia care. By strengthening communication competencies, the unit supports learners in providing person-centred, relationship-focused care that enhances the quality of life of people living with dementia.
Conclusion
This study demonstrated a significant increase in participants’ communication knowledge and confidence following the DCU, along with reported improvements in their communication practices, care approaches, and knowledge sharing. These findings highlight the value of targeted education in dementia-specific communication, suggesting that well-designed educational interventions can have a strong positive impact, both for participants and more broadly. In particular, the results support educational interventions that develop person-centred communication knowledge and skills, grounded in a broader understanding of the lived experience of people living with dementia, and delivered through varied, context-specific and reflective methods. Future research should build on this work by exploring long-term impacts not only on care partners’ communication and care practices, but also on wellbeing outcomes for both care partners and people living with dementia.
Footnotes
Ethical Considerations
The study received ethics approval from the University’s Human Research Ethics Committee (H0028597).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
