Abstract
Introduction:
To evaluate the influence of traditional risk factors of ischaemic heart disease and genetic factors to predict different types of acute coronary syndromes.
Materials and methods:
Five hundred and twenty-three patients with acute coronary syndromes (393 with ST elevation myocardial infarction (STEMI) and 130 with non-ST elevation myocardial infarction (NSTEMI)) comprised the study group. The control group consisted of 645 subjects free from symptoms of ischaemic heart disease and stroke. Genetic polymorphisms of
Results:
Patients with acute coronary syndromes more often had ID or II genotype than DD genotype of
Conclusions:
Genetic polymorphisms of
Introduction
The morbidity and mortality from cardiovascular diseases in Lithuania is one of the highest among the European Union member states. Ischaemic heart disease (IHD) and acute coronary syndromes (ACSs) comprise the largest portion of cardiovascular diseases.1,2 Epidemiological studies have confirmed that age, smoking, diabetes, dyslipidaemia, hypertension, obesity and gender are independent risk factors for atherosclerosis.3,4 The early detection of patients having a high risk of ACSs is a priority. Different ACS types such as ST elevation myocardial infarction (STEMI) and non-ST elevation myocardial infarction (NSTEMI) lead to a different clinical course of ACSs and outcomes and require different treatments.5,6 So far, there are no data on whether risk factors are different in particular ACS types. Also, great attention has been devoted to the evaluation of genetic variation of certain enzymatic systems, as a potential risk factor in the development of different ACS types. The renin–angiotensin–aldosterone system (RAAS) and the matrix metalloproteinases (MMPs) play a significant role in the pathogenesis of ACSs and the genetic polymorphism of enzymes of RAAS and various MMPs may affect the occurrence of ACSs.7–10 The activation of MMP and RAAS components is also regulated by genetic predisposition.7,8 This suggests that individuals carrying a higher activity allele of the certain gene have increased concentrations of the particular enzymes that play a crucial role in the atherosclerotic plaque instability and rupture, with consequent thrombus formation and the development of a greater extent of myocardial damage.
The aim of this study was to investigate genetic polymorphisms of several MMPs and angiotensin-converting enzymes (ACEs) mostly expected to play a significant role in the pathogenesis of ACSs if hypothesising that the different pathogenesis of the two conditions could be under the influence of the genotype along with traditional IHD risk factors.
Study population and methods
Subjects
Five hundred and twenty-three patients with ACS (393 with STEMI and 130 with NSTEMI) were enrolled into the study. All of them were admitted to the Department of Cardiology of the Lithuanian University of Health Sciences Hospital between 2007 and 2011. All the patients underwent coronary angiography, following percutaneous intervention of the culprit artery and conventional echocardiography.
Acute myocardial infarction (AMI) was defined according to the standard criteria based on clinical symptoms, ECG findings and cardiac enzyme abnormalities. 11 Family history, cardiovascular risk factors and current treatment were obtained from each patient using a standard questionnaire. Hypertension was defined as the presence of elevated systolic (≥ 140 mmHg) and/or diastolic (≥ 90 mmHg) blood pressure or the current use of antihypertensive drugs. A patient was considered as a smoker if he was smoking at the current time or had been a smoker in the past. Diabetes mellitus was identified when dietary treatment and/or medical therapy was required to control blood glucose levels. Dyslipidaemia was defined as serum total cholesterol levels of 5.2 mmol/L or more, low density cholesterol more than 2.6 mmol/L, and/or triglycerides equal to or more than 1.7 mmol/L or the use of statin medication. 12
The control group consisted of 645 subjects free from symptoms of IHD and stroke matching the study group design according to their age and gender. The control group consisted of subjects from a random sample of the Kaunas population screened within the international Health, Alcohol and Psychosocial factors In Eastern Europe (HAPPIE) project, the Countrywide Integrated Non-communicable Disease Intervention (CINDI) project and an international study, the Kaunas Healthy Ageing Study.
Written informed consent was obtained from all the patients, and the study protocol was approved by the Kaunas region ethics committee.
Genetic analysis
The DNA was extracted from the venous blood of patients using the Genomic DNA Purification Kit, according to the recommendations of the manufacturer. Aliquots of purified DNA were stored at –20°C until use in real time quantitative polymerase chain reaction (qPCR) analysis.
The determination of
Statistical analysis
All statistical analyses were conducted using the Software Package for Social Sciences (SPSS) version 19.0 (SPSS, Chicago, IL, USA).
Continuous variables were expressed as means ± standard deviations (SD) when normally distributed, and as medians (25th, 75th percentiles) when not normally distributed. Continuous variables were assessed using the unpaired Student’s
Results
Patients with ACS more frequently had arterial hypertension (
Comparison of IHD risk factors between ACS group and control group patients.

ACS: acute coronary syndrome; AH: arterial hypertension; BMI: body mass index; IHD: ischaemic heart disease; NSD: no statistical difference.
The distribution by gender, mean age and frequency of IHD risk factors, cholesterol level did not differ between the patients with STEMI and NSTEMI (Table 2). Heart rate (
Comparison of clinical characteristics of patients with STEMI and NSTEMI.
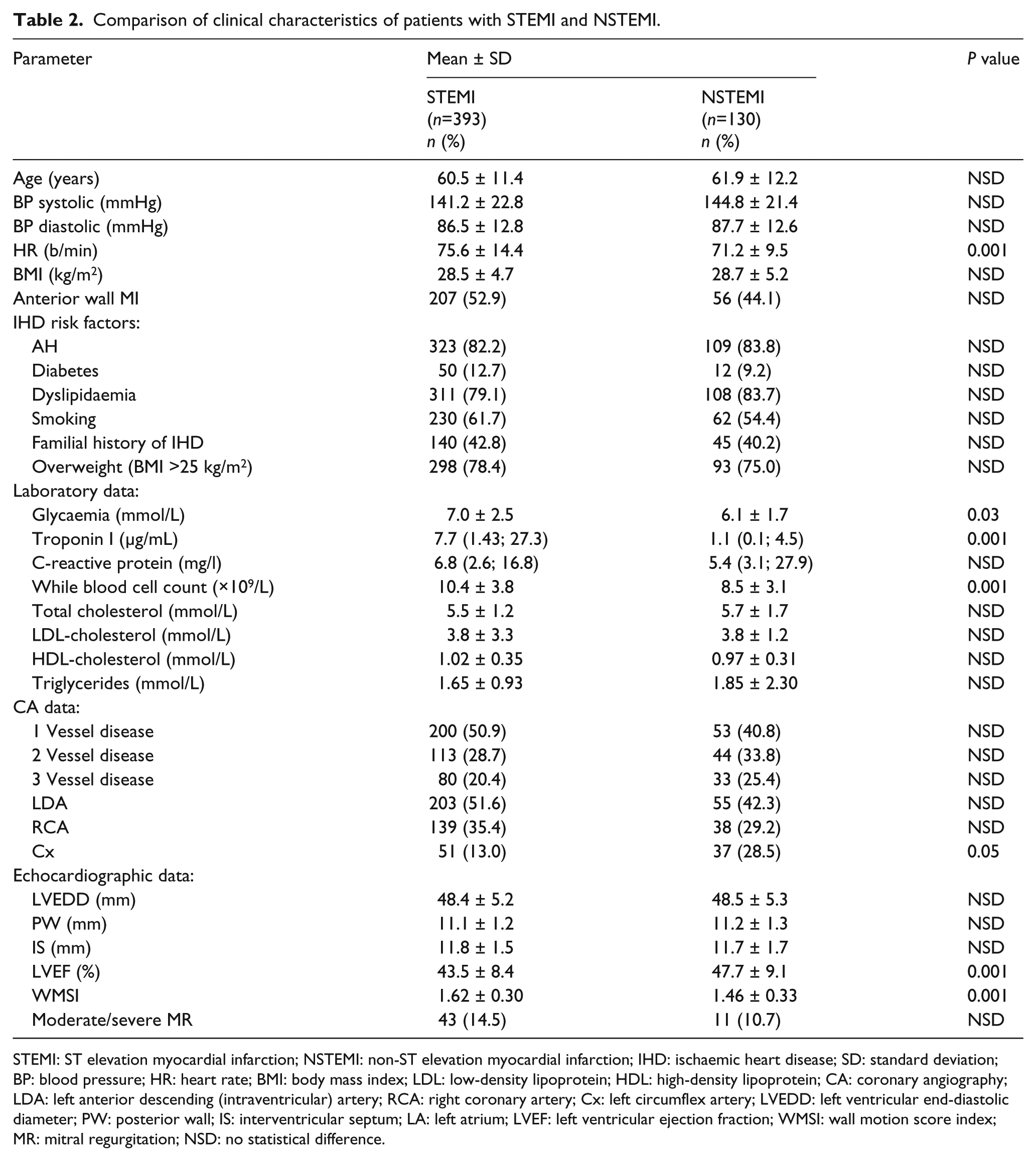
STEMI: ST elevation myocardial infarction; NSTEMI: non-ST elevation myocardial infarction; IHD: ischaemic heart disease; SD: standard deviation; BP: blood pressure; HR: heart rate; BMI: body mass index; LDL: low-density lipoprotein; HDL: high-density lipoprotein; CA: coronary angiography; LDA: left anterior descending (intraventricular) artery; RCA: right coronary artery; Cx: left circumflex artery; LVEDD: left ventricular end-diastolic diameter; PW: posterior wall; IS: interventricular septum; LA: left atrium; LVEF: left ventricular ejection fraction; WMSI: wall motion score index; MR: mitral regurgitation; NSD: no statistical difference.
Patients with ACS (STEMI or NSTEMI) had a higher frequency of ID genotype and lower frequency of DD genotype of
Comparison of

P<0.005 if comparing between STEMI and NSTEMI patients. ACE: angiotensin converting enzyme; ACS: acute coronary syndrome; STEMI: ST elevation myocardial infarction; NSTEMI: non-ST elevation myocardial infarction; I: insertion; D: deletion; MMP: matrix metalloproteinase; T: thymine; C: cytosine; A: adenine.
The genotypes of the MMPs are also presented in Table 3. The genotype distribution was in Hardy–Weinberg equilibrium. There were no differences in frequencies of
Multivariate logistic regression analysis revealed that smoking (
Univariate and multivariate logistic regression analysis to predict STEMI occurrence.

STEMI: ST elevation myocardial infarction; OR: odds ratio; CI: confidence interval; AH: arterial hypertension; MMP: matrix metalloproteinase; ACE: angiotensin-converting enzyme.
Independent predictors of NSTEMI development were as follows: smoking (
Univariate and multivariate logistic regression analysis to predict NSTEMI occurrence.

NSTEMI: non-ST elevation myocardial infarction; OR: odds ratio; CI: confidence interval; AH: arterial hypertension; MMP: matrix metalloproteinase; ACE: angiotensin-converting enzyme.
Discussion
The results of our study revealed that genetic polymorphisms of
The epidemiological studies revealed unquestionable risk factors of atherosclerosis and IHD such as smoking, diabetes mellitus, dyslipidaemia, arterial hypertension and physical inactivity.2–5 The exposure to different risk factors disrupts the endothelial function of a blood vessel, determining the beginning of the atherosclerotic process and formation of the atherosclerotic plaque. An inflammatory process regulates the process of atherosclerosis 16 and is the most important decisive factor of instability of an atherosclerotic plaque. 15 Data and results from the pathological, autopsy and angiographic studies revealed that plaque vulnerability, plaque morphology, thin fibrous cap, smaller lumen diameter account for the clinical presentation of myocardial infarction (MI).17,18
The results of our research confirm the influence of traditional risk factors on ACS occurrence. Patients with ACS more frequently were smokers and more frequently had arterial hypertension, diabetes mellitus and dyslipidaemia. Our study revealed that smoking, diabetes, dyslipidaemia and arterial hypertension increase the risk of STEMI development. However, diabetes mellitus has no associations with NSTEMI development while smoking, arterial hypertension and dyslipidaemia may be important in NSTEMI occurrence. The results of other researchers are quite contradictory. According to the data of Montalescot et al., patients with STEMI more frequently had arterial hypertension and diabetes mellitus than patients with NSTEMI while the patients with NSTEMI more frequently were smokers. 19 On the contrary, the results of Di Stefano et al. demonstrated that patients with STEMI more frequently have been smoking, and arterial hypertension has been more frequent for those who had NSTEMI. 20 Research by Ino et al. did not reveal any differences in IHD risk factors between the STEMI and NSTEMI patients at all. 21
The present study also demonstrated the differences in the basic clinical and biochemical parameters between STEMI and NSTEMI patients. Patients with STEMI had a higher heart rate and white blood cell count, higher levels of troponin I and glucose, as well as more severe heart dysfunction assessed than in patients with NSTEMI. This indicates that a higher activity of inflammation, more extensive myocardial necrosis and disbalance of glucose metabolism are more common in STEMI patients. Our results confirm the data of other studies reporting that the pathogenesis of STEMI is associated with a more active inflammation process and STEMI may lead to more extensive myocardial damage and necrosis.22–24 The research data of Di Stefano et al. demonstrated obvious differences in inflammation markers between patients with STEMI and NSTEMI. Patients with STEMI had a higher concentration of leukocytes and a higher activity of other markers of inflammation such as high sensitivity C-reactive protein, interleukin-6 and serum amyloid A. 20 The patients with NSTEMI had a lower concentration of leukocytes, and other inflammation markers were not increased at all. 20
Furthermore, in STEMI patients a more severe disturbance of glucose metabolism is present. According to our data, patients with STEMI had a higher level of glycaemia as compared to patients with NSTEMI at baseline and patients with STEMI also more frequently had diabetes in the past. Hyperglycaemia is a predictor of adverse outcomes in STEMI patients 25 as hyperglycaemia increases the amount of free fatty acids which may reduce vasodilation of small blood vessels, stimulate leukocyte adhesion and increase procoagulant action of thrombocytes, 26 and worsen myocardial perfusion and contractility. 27
Our results demonstrate that the concentration of troponin I at baseline is higher in STEMI patients than in NSTEMI patients. As we know, troponin I is the main marker of necrosis and death of myocytes during AMI and its level is an important predictor of a bad prognosis after AMI. 28 The results of other authors also show that a higher concentration of troponin I is detected in STEMI patients. An increased concentration of troponin I at the acute period of AMI not only reflects the size of the area of myocardial necrosis, but also demonstrates a higher probability of repeated ischaemic cardiac events and repeated hospitalisation because of ACS or a greater probability of death.29,30 According to the data of Di Stefano et al. the troponin I concentration correlates with the level of C-reactive protein in patients with STEMI suggesting that activation of the inflammatory system is closely related to the size of necrotic area of myocardium after MI. 20
According to the pathophysiological mechanisms of STEMI and NSTEMI that we ascribed earlier, we had a hypothesis that some genetic factors can also be important in the process of atherosclerosis and may cause the development of ACS. The results of our previous study confirmed that genetic polymorphism of the
Our results demonstrate that 5A5A and 5A6A genotypes of
In conclusion, smoking, diabetes, dyslipidaemia and arterial hypertension are undoubted risk factors for IHD and can cause STEMI and NSTEMI in which the metabolism of glucose is more important in STEMI pathogenesis rather than NSTEMI. Pathogenetic differences between STEMI and NSTEMI, different morphology of the atherosclerotic plaque and its rupture can be determined by genetic predisposition. The polymorphism of
Footnotes
Acknowledgements
All authors contributed equally to this work. The authors would like to thank all the participants in the research. They also thank the students and nursing staff at their hospital for their dedication to this study.
Declaration of conflicting interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
