Abstract
Summary
Self-neglect, where adult individuals—for varying reasons—do not care for aspects of their health, wellbeing or home environment, involves significant risks and potential for harm. The importance of effective interprofessional and inter-agency collaboration in supporting people experiencing self-neglect is widely recognized, yet research and practice reviews attest to continuing challenges in collaborative working. This realist review integrates two sources of evidence, the international research literature and Safeguarding Adult Reviews (SARs) of practice cases in England, to theorize what mechanisms need to operate for effective inter-agency collaboration to support people experiencing self-neglect, and how context affects this. Searches in 2023–24 identified 41 studies and 273 SARs to inform the review, assessed on relevance and rigor.
Findings
The review identified four mutually reinforcing elements that underpin collaborative working: (1) Common framework provided by policies, procedures and interfaces; (2) Mutual understanding of each other's roles and the task; (3) Shared vision of the person and situation “in the round”; (4) Management and monitoring ensuring commitment, learning and resources. Each is discussed in light of the distinctive challenges of self-neglect, and a composite example constructed from the review sources is used to illustrate.
Applications
This review theorizes the elements needed for successful inter-agency and interprofessional collaboration in supporting people experiencing self-neglect. Its framework supports service leaders and researchers to consider how the mechanisms identified interact with the inter-agency context in which they unfold, and recognize the conditions needed for interventions to be effective.
Introduction
England's Department of Health and Social Care (DHSC) defines self-neglect as “cover[ing] a wide range of behaviour neglecting to care for one's personal hygiene, health or surroundings and includes behaviour such as hoarding” (2023, para. 14:17). Precisely how services operationalize this definition varies locally (Orr, 2023), just as it does between states in the USA (Dahl et al., 2020). Yet everywhere self-neglect poses consistent challenges: understanding why it occurs; balancing risk with the person's right to self-determination; and finding ways to engage where practitioner input may be unwelcome (Braye et al., 2014; Manthorpe et al., 2022). Social workers have a leading role in responding to self-neglect, but its complexity requires inter-agency collaboration. Yet self-neglect also exacerbates collaboration's “everyday” difficulties: divergent professional or organizational outlooks, lack of role clarity, power imbalance, or communication barriers (Wei et al., 2022). The stakes can be high. Severe self-neglect endangers life but the person often declines support, creating dilemmas for social care, health, police, housing, and other practitioners.
Braye et al.'s (2017) “seven literacies” framework comprises the key skills domains self-neglect requires of practitioners: legal, ethical, relational, emotional, knowledge, organizational, and decision-making literacies. Interprofessional collaboration is central to organizational literacy and underpins others such as decision-making literacy. Because self-neglecting individuals neglect self-care, they commonly do not or cannot themselves undertake the coordinating work typically expected of people to integrate the inputs they receive from different services. This puts more onus on social workers and other professions to coordinate proactively.
Safeguarding Adult Reviews (SARs) are statutory reviews, undertaken at local level, of cases raising concerns about how services “worked together to safeguard the adult” from abuse or neglect (Care Act, 2014, s. 44). SARs focusing on self-neglect, many led by social workers and nearly all considering social work among the agencies they reviewed, have repeatedly highlighted ongoing challenges to effective collaboration. Examples drawn from these SARs illustrate why collaboration matters (SAR numbering corresponds to Preston-Shoot's published index [see Methods], also accessible at Orr et al., 2023b):
Failures to coordinate care left people with brain injury-related self-neglect adrift within services. Support developed through a series of “disconnected” assessments rather than concerted planning (SAR 106). Practitioners met only to respond to crises rather than proactively addressing risks together (SARs 120, 338). Two of these men died by suicide, one by drug overdose. Slow or poorly understood information-sharing processes, inadequate IT records, or paucity of details characterized communication between services at crucial organizational interfaces, leaving people experiencing self-neglect at increased risk (SARs 121, 306, 379, 394). Care became bogged down in disputes over eligibility, with successive specialist services each finding reasons why a woman's complex mental health needs did not “fit” with them (SAR 366).
A “what works” scoping review of self-neglect by Martineau et al. (2021) touched on multi-agency working in self-neglect, pointing to the importance of strategic leadership in overcoming structural barriers, divisions between agencies, and lack of shared language. A series of reviews of self-neglect SARs (Preston-Shoot, 2016, 2017, 2020, 2021, 2023) catalogued a range of failings in collaboration and used systems analysis to propose improvements to practice. However, although close interprofessional collaboration is universally recommended in studies of self-neglect, to date no review has focused on overarching theorization of collaborative working, nor systematically integrated evidence from research studies and SARs. These are complementary resources. SARs are gray literature containing contextualized accounts of what happened in individual cases, and the resulting recommendations indicate what implicit theories safeguarding reviewers hold about what works. Research studies provide broader theorization that sheds light on SAR findings and processes, but can benefit from the testing-ground afforded by SARs’ practice-focused detail. Our review combined both sources to ask (1) what mechanisms are required for effective inter-agency collaboration supporting people in self-neglect to “work,” and (2) how context affects whether they do so. The resulting model provides a foundation for further theory testing and refinement (Table 1).
Acronyms used.

Methods
Realist review design
The study used modified realist review, following RAMESES (Realist And MEta-narrative Evidence Syntheses: Evolving Standards) quality standards (Wong et al., 2013), adjusted to incorporate SARs. Realist review focuses not only on what works, but for whom and under what conditions, and was therefore well suited to the complexity of self-neglect, where cases are diverse and desirable outcomes vary depending on the person's wishes. Realist review aims to produce theory to assist stakeholders in understanding how relevant mechanisms interact with contextual conditions and feed into outcomes. These Context-Mechanism-Outcome configurations (CMOcs) inform analysis and planning (Table 2; see also Pawson, 2006, pp. 21–25).
Brief definitions of key realist concepts.

The review was registered prospectively with the PROSPERO systematic reviews database (https://www.crd.york.ac.uk/PROSPERO/view/CRD42022329889).
Searching and inclusion criteria
Realist review considers both peer-reviewed research and gray literature (Pawson, 2006). This review proceeded along three parallel tracks, exploring: Strand 1. International research literature Strand 2. Publicly-available Safeguarding Adults Reviews Strand 3. Safeguarding Adults Board (SAB) self-neglect policies and procedures (published separately in Orr, 2023). SABs are statutory inter-agency bodies responsible for strategic oversight of adult safeguarding in their local area.
The three sources were iteratively compared and integrated, building on an initial framework based on informal literature scoping and discussion with SAB managers, and set out in the study protocol (Orr et al., 2024).
Strand 1. The databases AMED, British Nursing Index, CINAHL, ETHOS, Global Health, Medline, ProQuest Dissertations, PsycINFO, Social Care Online, SocIndex and Web of Science, were searched in January 2024 using the terms: Self-neglect AND Interprofessional Hoarding Multiprofessional Interagency Multiagency Collaborative “joint working” Partnership
The study stakeholders were consulted for additional literature (see “Stakeholder Involvement”).
Papers were double-screened against the inclusion criteria (Table 3), with any disagreements resolved through team discussion.
Inclusion criteria for Strand 1 review.

Two subsequent supplementary searches, going beyond a specific focus on self-neglect itself, were undertaken to deepen understanding of two mechanisms among those initially identified. These were selected as priorities, in consultation with stakeholders, because they have distinctive relevance in self-neglect:
assigning the role of assessing mental capacity among involved professionals (search terms: “mental capacity assessment” combined with terms listed above for interprofessional working). Several SARs highlighted practitioner uncertainty over who held responsibility for mental capacity assessment. A secondary search was undertaken because mental capacity assessment is often key in self-neglect practice. SARs’ contribution to informing inter-agency collaboration (search terms: “Safeguarding Adults Reviews”). SARs are themselves an intervention. Since SARs formed much of our evidence-base, a secondary search was undertaken into research on their strengths and weaknesses.
Resource and time constraints prevented further exploration of additional mechanisms.
Strand 2. SARs featuring self-neglect were identified from an index compiled in the Journal of Adult Protection, which contained 422 SARs at the start date of our review (Preston-Shoot, 2023). SARs were excluded where they were
published outside England (i.e., Scotland, Wales, Jersey). The Care Act 2014, which reclassified self-neglect as a safeguarding matter, applies only in England. The other jurisdictions have different legal frameworks. published before 2015, the year self-neglect was brought under safeguarding's remit. not found online, so that no unpublished (confidential) SARs from the index were analysed. thematic reviews which consider multiple cases, complicating extraction of individual case details.
Data extraction and quality appraisal
Two reviewers undertook data extraction for all research papers (Strand 1), resolving disagreements by discussion. High numbers of SARs made dual data extraction unfeasible (Strand 2), so reviewers jointly assessed 6 SARs to establish consistency before singly reviewing the others.
Realist reviews evaluate quality based on relevance and rigor. Research study relevance was ensured by applying the Strand 1 inclusion criteria; SAR relevance based on inclusion within Preston-Shoot's database. Research study rigor was assessed using the Critical Appraisal Skills Program Checklists (CASP, 2022) as appropriate. SARs, meanwhile, are case studies. The best provide fine-grained accounts, valuable for complementing and testing out broader-brush discussions found in the research literature (Yin, 2018). Many consulted carefully with the practitioners involved and all include multiprofessional perspectives, whereas the research predominantly features social worker views. However, not all SARs explain their analysis in depth, not necessarily as an oversight but to respect the privacy of those affected, which makes it difficult to assess rigor accurately. Existing quality criteria for SARs (SCIE, 2022) focus on the immediate, local needs of the commissioning SAB, not the needs of research evaluation, so were not used. This should be kept in mind when assessing the review findings.
Data extraction and appraisal are viewable (Orr et al., 2023a, 2023b).
Analysis and synthesis
The research was predominantly qualitative. What quantitative data was found did not directly address collaboration, so specific intervention models or comparators do not feature. Instead, the data extractions identified key factors perceived to shape relevant CMOcs. Data on the context of self-neglect services, theories used, and facilitators and barriers were extracted from the research studies and, through constant comparison and discussion, tentative CMOcs were derived. Data were extracted from the SARs on characteristics of the case, services involved, good and poor collaborative practice, and the recommendations, from which implicit theoretical assumptions informing the SAR analysis could be derived. Working iteratively and interpretively, the team refined CMO configurations, and developed propositions on what mechanisms potentially contribute to good collaborative working with self-neglect. These were initially expressed as 29 “if-then” statements (Orr et al., 2023c), which we found to be an accessible format to communicate CMOcs to stakeholders for their input: e.g., “IF feedback loops are put in place which work with, but are not undermined by, data sharing restrictions, THEN practitioners and community groups are less likely to give up on making referrals.” These 29 detailed statements were merged into a smaller number of overarching themes, and finally under 4 encompassing program theory (PT) statements, which set out how mechanisms are understood to contribute to outcomes.
Team and stakeholder involvement
Research team members brought to the review professional experience of practice in social work, nursing, clinical psychology and medicine (general practice), in the UK or Netherlands.
The review benefited from stakeholder input in several ways:
Researchers with lived experience: Two research team members brought lived experience of self-neglect. Each reviewed a small set of SARs and commented on the analysis. The study steering committee included two others with lived experience of self-neglect, two SAB Chairs, and three researchers with relevant expertise. Lived experience panel: A separate, six-member panel was recruited through participating services to bring direct and/or carer experiences of self-neglect. Two more individuals participated, asynchronously to facilitate their involvement. The research team liaised with five SABs through named Board members, who brought applied inter-agency perspectives.
Results
Figure 1 shows the screening process. In Strand 1, of 206 records initially screened for relevance, 61 underwent full-text review and 29 were retained for analysis. Stakeholders and post-search publication updates provided 4 more records; iterative secondary searching focused on two selected mechanisms (see section 2.2) brought 8 further records. The total number of research records synthesized was therefore 41.
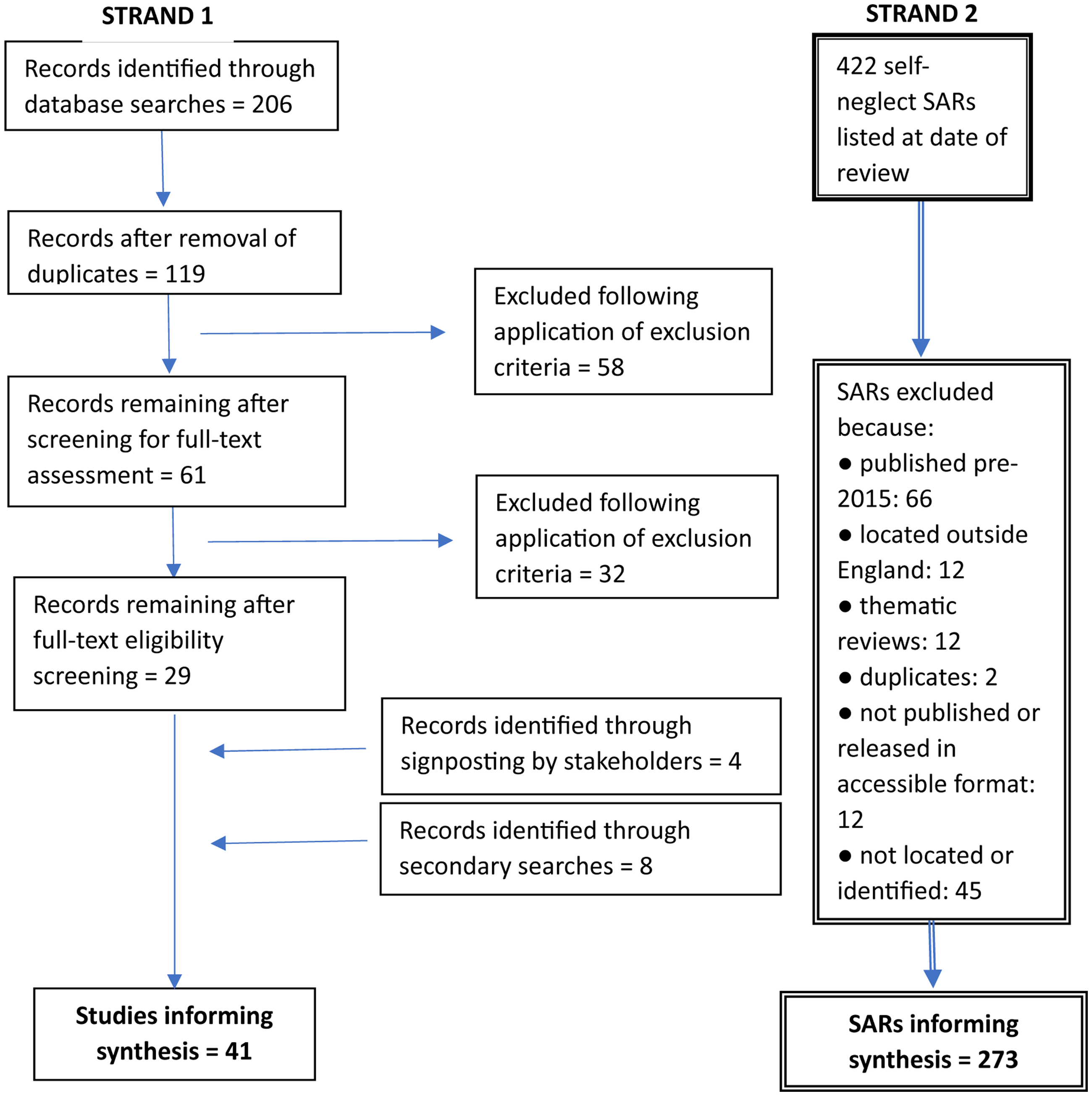
Flow diagram showing screening process.
In Strand 2, 149 SARs were excluded from the initial sample of 422, leaving 273 informing the synthesis.
Table 4 shows more details of included research studies. Most were from the UK.
Country and research type of studies included in the synthesis.

We developed four overarching PTs (Figure 2), under the headings of “Common framework provided by policies, procedures and interfaces,” “Mutual understanding of each other's roles and the task,” “Shared vision of the person and situation ‘in the round’,” and “Management and monitoring ensuring commitment, learning and resources.” These are mutually reinforcing and function iteratively: clear policies and protocols can enhance mutual understanding among practitioners; in turn this enables the different professionals to share perspectives and take a holistic approach; effective management and monitoring identify service gaps or support needed with these processes, whereupon leadership acts to revise protocols, raise team awareness or restructure interfaces. We present each PT in turn, the first three with illustrative worked examples of their application constructed from the literature.
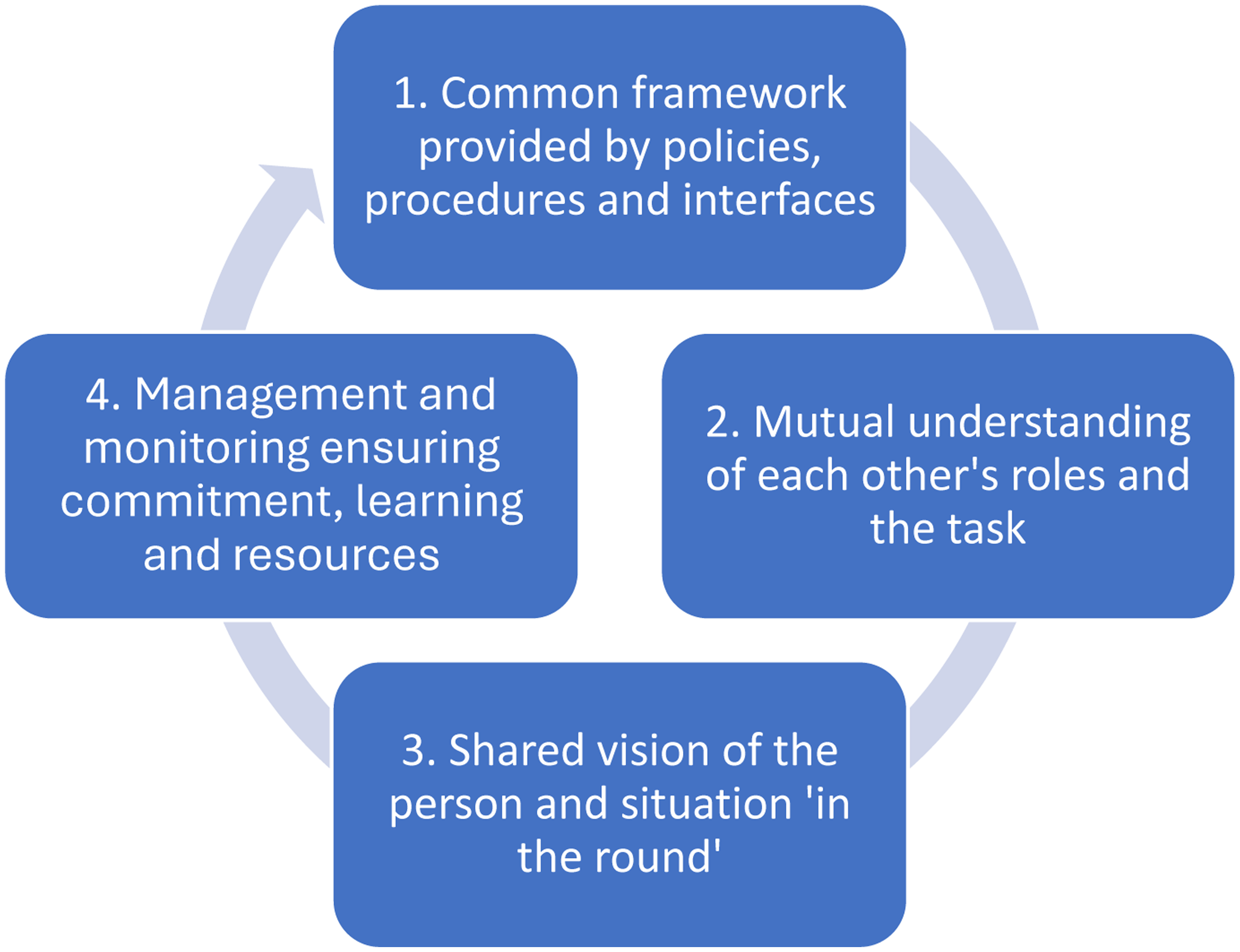
Key generative mechanisms within the realist review.
Mechanism 1: Common framework provided by policies, procedures and interfaces
PT: IF (a) clear pathways and systems are in place for practitioners to use and (b) practitioners show flexible adaptation to those systems’ limitations, THEN appropriate information and agreed actions flow between relevant agencies.
“Common reference-point” and “Balancing guidance with flexibility” were key elements within this mechanism.
Common reference-point: Several organizations may be involved with complex self-neglect, each with different priorities, mandates and demands on their resources. It may be unclear how far the person is actively choosing their situation and what the role of practitioners should therefore be. Some researchers argued that agreed self-neglect policies and/or procedures provide a framework for that discussion to take place between agencies, increasing clarity and confidence in responding, and providing a shared “overriding rationale for service provision” (Lauder et al., 2005, p. 195) which is otherwise lacking (Braye et al., 2011; D’Angelo et al., 2020). In the English context, bringing self-neglect within safeguarding's remit has apparently succeeded in providing impetus for inter-agency collaboration (Orr, 2023). North American research literature also identifies the value of inter-agency agreements, usually under municipal auspices (Bodryzlova et al., 2020; Bratiotis et al., 2019; Lacombe & Cossette, 2018).
Balancing guidance with flexibility: Procedures must be flexible because self-neglect presentations and needs vary widely, and involvement and support often need careful tailoring to be acceptable to the person (Lauder et al., 2005; SARs 131, 338). This avoids “over-proceduralisation” (Braye et al., 2014, p. 140) that can stifle responsiveness. Beyond specific self-neglect procedures, SARs also call for related protocols to improve agencies’ responsiveness to each other's concerns: formal escalation procedures for interprofessional challenge; structured timelines for responses; clarifying responsibilities during and after referral; and case closure protocols. This list indicates common failings: uncoordinated responses leading to stasis, or to vulnerable people left unsupported by gaps between services. Reliance on policies and procedures as a mechanism for resolving difficulties reflects SARs’ “procedural turn” (Preston-Shoot, 2017, p. 57). SAR 263, for example, recommends additional policies and procedures, despite having found that five existing ones were not being implemented or monitored. The existence of procedures does not itself trigger change: practitioners are not always aware of them (Brent, 2022), interpret them differently (Harris et al., 2023), can be confused by differing interpretations of protocols (e.g., SAR 291) or overlap between procedures in self-neglect and elsewhere such as mental health (SARs 250, 366), or IT system design can hinder the intended implementation of procedures (SARs 176, 392).
The following example illustrates how appropriate procedures may facilitate detection of self-neglect, but practitioner initiative is needed to adapt to procedures’ inevitable limitations: Context: Introducing a dedicated self-neglect policy raised practitioner awareness and prompted inter-agency referrals where practitioners had previously been unsure about whether and how to make them. However, SARs identified flaws in referral practices, including: (1) practitioners’ over-reliance on referring to personal contacts and services with which they are familiar, rather than following expected pathways (e.g., SAR 79); (2) practitioners relied more on phone calls and e-mails than on a formal notifications system when referring (e.g., SAR 322), raising concerns about tracking of cases. Mechanism: The SARs recommended systematizing regularized referrals by reinforcing procedures, and introducing escalation protocols so that disagreements are addressed directly rather than avoided. However, (1) where the relationship between agencies is characterized by mistrust and low confidence in the response to self-neglect, practitioners continue to avoid them or rely on other contacts (Mason & Evans, 2020). (2) Where practitioners rely predominantly on the formal notifications system, SARs urge them to follow up referral with back-up phone calls or e-mails, as this did more than the notifications to ensure referrals were accepted and appropriate action was taken (e.g., SARs 225, 306). Outcome: (1) Without targeted inter-agency work to improve understanding of referrals decision-making (SARs 127, 372), practice is resistant to change through the protocols. Conversely, collective feedback loops about responses to referrals, and consultation about and road-testing of protocols, facilitate their impact. (2) When seen across the range of SARs, relying on only formal systems or back-up contact appears insufficient; both formal procedures are to be used and reflexivity is required from practitioners about the limitations of referral notification systems and initiative in following up as needed.
Mechanism 2: Practitioners’ mutual understanding of other agencies and the task
PT: IF practitioners (a) understand each other and (b) put that understanding into effective action THEN assessment, planning and intervention are goal-directed and coherent.
“Knowing each other,” “Communication,” and “Ownership” were key elements within this mechanism.
Knowing each other: Practitioners need adequate working knowledge of each other's role with self-neglect, but also each other's disciplinary values and reasoning. When that reasoning is unclear, competing pressures to manage the risks of self-neglect while respecting the person's autonomy generate tensions between agencies when they prioritize different risks. Some studies documented interprofessional accusations of “withholding” involvement (Ariyo et al., 2021, p. 8; Aspinwall-Roberts et al., 2022). Mental health services have been accused of operating rigid, exclusionary assessment criteria (Mason & Evans, 2020, p. 674), social workers of using self-determination as a pretext to refuse support (Aspinwall-Roberts et al., 2022).
If these tensions arise they hamper interprofessional coordination. However, beyond noting that practitioners’ understanding of structural pressures such as budget cuts on fellow services favoured interprofessional trust (Mason & Evans, 2020, p. 674), the research suggests few remedies. SARs have rarely considered this mechanism. Some local multiagency procedures now incorporate pen-pictures of the professional roles most frequently involved with self-neglect, but these do not go into depth. Yet agencies should share guiding models such as trauma-informed practice or strengths-based approaches, and at least a basic awareness of the thinking behind each other's key models, otherwise input from one agency can work at cross-purposes to another. For example, SAR 403 notes how a housing provider's use of the Psychologically-Informed Environments model was undermined because other agencies were unaware of it.
Communication: Mutual knowledge and understanding is maintained only through clear written and verbal communication. SARs record instances of miscommunication in the process of referral, due to omitted details, or tentativeness in expressing concerns (SARs 224, 328). Self-neglect is prone to ambiguity, as it often follows safeguarding channels despite there being no third-party suspected of abuse or neglect (Harris et al., 2023); this can mean it fits poorly with standard referral forms. Confusion is exacerbated by tendencies to reproduce legal phrasing verbatim in forms (again hinting at overproceduralization), which can be lengthy or difficult to follow in day-to-day practice (SAR 176). A contrasting positive tool that assists shared understanding is the Clutter Rating Scale, a photo-based standardized assessment tool for hoarding, which has proven useful in enabling professionals to quickly communicate the severity of cases through widely-understood numerical ratings (SAR 422). A fourfold grading scale is also used to rate pressure ulcer severity in self-neglect affecting skin tissue (Manthorpe & Martineau, 2017a). However, effective communication of risks and severity across other areas of self-neglect is still limited by the lack of widely-understood and used objective rating scales.
Ownership: Mutual understanding and communication contribute to clear “ownership” and coordination of cases. SARs identify problems both of diffuse ownership, where multi-agency working itself increases risks because the involvement of other agencies leads to complacency and a “bystander effect” where practitioners assume others are dealing with risks (SARs 325, 337), and excessive ownership, where one agency dominates, leaving others poorly-informed (SAR 302). Properly joined-up working prevents agencies proceeding in isolation, and referrals being batted back and forth. Such “referral bouncing” can be common, particularly where there is “no neat fit along diagnostic lines” as with some complex mental health issues (SARs 248, 366). Undertaking joint assessments for cases falling between clear agency remits help resolve such disputes while enabling practitioners to learn from each other (SAR 108).
The following example illustrates the importance of mutual understanding through the example of ownership of mental capacity assessment, a recurring issue in self-neglect SARs: Context: Understanding of mental capacity and who should assess it is uneven. Although training is widely rolled-out, many practitioners find judging capacity daunting, particularly with self-neglect (Preston-Shoot, 2016). Consequently, they sometimes attempt to pass the task on to other professions, usually doctors or psychiatrists, influenced by the medical profession's high status or over-emphasis on the diagnostic test within capacity assessment, or to social workers, as perceived safeguarding specialists (SARs 172, 305; Jayes et al., 2017). Mechanism: Many SARs recommend further mental capacity training and case file audit. However, this is not always applied to the complexities of self-neglect, nor straightforward to transfer into practice (Aspinwall-Roberts et al., 2022; Preston-Shoot, 2021). Assessment templates may be: little more than itemized proformas listing principles of the MCA 2005 and the assessment criteria, rather than providing specific assessment strategies. (Ariyo et al., 2021, p. 11) Some practitioners perceive high stakes, fearing punishment if their assessments are seen to be wrong (Aspinwall-Roberts, 2019), and attempt to pass them on. Outcome: Training and resources may not correct erroneous assumptions that capacity assessment in self-neglect is the remit of specialists, not the person asking for the decision. While professional views on mental capacity may legitimately differ as capacity is time- and decision-specific, experiencing disagreement in practice can reinforce some practitioners’ sense that others are the “experts,” or arouse suspicions that professionals cynically find people to have capacity so that they can “abdicat[e] responsibility” (Aspinwall-Roberts et al., 2022, p. e4402). Moreover, anxieties around mental capacity can become the focus at the expense of seeing the situation holistically: [A] focus on capacity had not been helpful as the real issue was about managing the changes and transitions for Elizabeth. (SAR 317)
Mechanism 3: Shared vision of the person and situation in the round
PT: IF collectively practitioners can keep focus on the person and their situation “in the round” THEN support becomes more than the sum of its parts.
“Shared whole-picture view” and “Centering the individual” were key elements within this mechanism.
Shared whole-picture view: Practitioners working together must collectively “put the whole picture together” (SAR 106, p. 8). This means developing a holistic view, with shared hope for improvement, and together placing the person's perspective at the heart of planning. Otherwise, when time and space are not available, interprofessional work can easily settle into “reactive […] rather than reflective” (Preston-Shoot, 2016, p. 145), short-term management of immediate crises or “episodes” (SAR 417), losing sight of longer-term direction (SAR 225) and of unresolved issues underlying self-neglect (SAR 366) . These are clearer where collaboration combines complementary expertise instead of compartmentalizing perspectives, e.g., by jointly considering underlying patterns of brain injury, trauma or loss rather than focusing separately on individual agency priorities such as “drugs, drinking or homelessness” (SARs 106, 291). This extends to the expertise of involved family members or other close individuals (Holloway & Norman, 2022; Jones et al., 2020), whose input with self-neglect is often ignored (SARs 281, 305), or crowds out the person experiencing self-neglect (SARs 258, 322, 420).
Seeing the whole picture requires shared reflection, which is more likely in contexts where: time and opportunities are found for mutual discussion such as multidisciplinary meetings, consultations or supervision, resisting pressures for quick case closure (Anka et al., 2017; Braye et al., 2014); there is clear openness and interest in diverse practitioner perspectives being heard, regardless of status or seniority (Mason & Evans, 2020), and interprofessional wariness of (over-)identifying with a single, default position (Preston-Shoot, 2016); there is confidence about information-sharing, and access to specialist medical, psychological, legal, or other knowledge where needed (Holloway & Norman, 2022). Their absence provokes anxiety, inhibiting the professional curiosity constantly emphasized in SARs.
Centering the individual: Although the individual's perspective should be at the heart of safeguarding, it still easily becomes subsumed under the priorities of the sometimes-bewildering range of practitioners involved. Countering this encompasses very practical aspects, such as not discharging someone experiencing self-neglect from a service before considering reasons for nonresponse (SAR 283), and considering how professional language shapes interprofessional understanding, e.g., language such as “hunger strike” immediately frames refusal of food and drink as deliberate, leading self-neglect to be overlooked (SAR 364). Responding to the person's concerns is facilitated by taking time for relationship-building and close enquiry into the person's wishes, considering advocacy (Braye et al., 2014), and practitioners sometimes looking beyond (though not neglecting) what they might consider their primary role (Lauder et al., 2005). Closer involvement of people with lived experience in training for practitioners is one intervention suggested to facilitate this (Bodryzlova et al., 2020), though it remains uncommon in self-neglect.
An example shows the intersection between seeing the person and situation in the round, and collaborative working dynamics: Context: Not all practitioners are fully aware of the complex dynamics contributing to self-neglect, e.g., brain injury, alcohol dependence, criminal justice involvement and wariness of services. Stretched resources and lack of reflective spaces exacerbate challenges recognizing and addressing overlapping issues, potentially infecting interprofessional joint working with negative perceptions and consequent pessimism (Lauder et al., 2005; Mason & Evans, 2020). Mechanism: Uncertainties around information sharing between agencies hindered practitioners from seeing people experiencing self-neglect in the round. Information shared was inflected by agencies’ perceptions that emphasizing the severity of difficulties was necessary to meet thresholds for needs and increase the likelihood of accessing services (Mason & Evans, 2020, p. 673). For example, one man's history of problematic offending was emphasized in order to secure supported accommodation for him, but this had lasting effects on how he was seen and supported by practitioners (SAR 356). Practitioners need to be aware of how negative labels travel beyond their own agency and, if not counter-balanced, conceal the whole person: Improving the care for clients like Alan will require staff to have positive attitudes and beliefs about the response. Agencies need to believe that they should be working with such clients and that useful interventions are possible. If practitioners do not accept these two foundations, successful work is very unlikely. (SAR 357) Outcome: Despite good intentions, there were harmful effects because agencies receiving the referral saw the person primarily in terms of their “label” and the problems that implied. Combined with lingering perceptions of self-neglect as driven by “lifestyle choice” (Braye et al., 2014), this discouraged practitioners from seizing moments of openness to positive change and impeded person-centered collaborative working (SAR 356).
Mechanism 4: Management and monitoring ensuring commitment, learning and resources
PT: IF there is a clear strategy and monitoring from management and commissioning, THEN attention on and organizational learning from Mechanisms 1–3 are sustained.
Leadership, monitoring and support: Leadership is needed to embed the above mechanisms (Braye et al., 2014; Brent, 2022). Without management direction, the time, personnel and funds required are unavailable, and there is no consistent messaging to reinforce practitioner awareness and a culture of collaborative working on self-neglect. The ongoing reflexive monitoring of performance within and between agencies is a crucial management responsibility. SARs, which form much of the evidence-base for this review, or equivalent inquiries are key, as are the case file audits into mental capacity assessment, referral practices and other aspects of self-neglect work that they frequently recommend. SARs have limitations (see section 4.1), but these can be mitigated if the SABs that commission them set terms of reference carefully (Morgan, 2019; Preston-Shoot, 2021), as well as ensuring that resulting action plans are implemented. Practitioners can find the local processes of participating in the SAR to be a valuable learning process, though it also has potential to be anxiety-provoking and draining, so management support throughout is needed (O’Reardon, 2023). SARs can and do identify good practice, but largely focus on failings (Morgan, 2019) and, if used as the main learning tool, can encourage risk aversion and defensive practice (Manthorpe & Martineau, 2017b). Speculatively, the predominance of SARs in safeguarding training may even inadvertently exacerbate negative interprofessional perceptions. By highlighting instances of poor decision-making, they potentially prime practitioners to interpret judgements by the same profession that they disagree with as another, related instance of that service's characteristic failings.
Design and planning: Senior leadership can also contribute to establishing collaborative frameworks by building in effective multiagency linkage across organizational and specialism barriers when commissioning services (SAR 367). Good service design helps mitigate the limitations of “partnership working […] grafted onto old single-agency structures” (Preston-Shoot, 2018, p. 15); for example, self-neglect linked with multiple-exclusion homelessness commonly met inadequate responses because of services’ tendency to refer onwards for the ‘primary need’ (housing), rather than addressing complexity together (Harris et al., 2023).
Discussion
This review has proposed four mid-range PTs summarizing what is needed for successful collaborative working that supports people experiencing self-neglect to occur, and indicating why this is such a complex task. Primarily though not exclusively drawing on learning from the English experience, it identifies important generative mechanisms requiring consideration across all jurisdictions. These dynamics are not unique to, but are intensified with, self-neglect. We now reflect on what makes self-neglect distinctive in the demands of each mechanism, and what this review contributes to the knowledge-base.
First, the need for policies is more prominent in the literature on self-neglect than on many other health and social care challenges. This may be because self-neglect regularly brings together agencies that otherwise may not often work closely together, and requires them to work in concert to negotiate the individual's likely refusal of some or all input. This is a delicate task, which some agencies are more used to than others. Self-neglect policies in the UK and USA provided a reference-point for agencies to consider their responsibilities and mandate for collaboration; without them, practitioners have different views on thresholds, self-determination and their respective roles. This review has highlighted how, in turning policy into procedures, services have to balance the clarity for practice conferred by setting out defined pathways, against flexibility that takes account of how disparate the needs of self-neglecting individuals are. Self-neglect is an umbrella term capturing considerable diversity and consequently a range of responses might be considered; English national guidance declares that the suitability of a safeguarding response should be assessed on a “case-by-case basis” (DHSC, 2023). Procedures and guidance are therefore necessarily nuanced rather than prescriptive, leaving scope for interpretation (Orr, 2023) and challenging multi-agency cohesion. Practitioners value the sense of direction policies can provide, especially if they are less practised in sustained work in the face of ambivalence to encourage change (e.g., Fire & Rescue or Environmental Health, compared with social work). Inter-agency policies may need to take account of this difference. However, self-neglect remains difficult to proceduralize fully as self-neglecting individuals are often highly selective about which, if any, offered support they accept.
Second, interprofessional collaboration is universally advocated with self-neglect but is not always experienced on the ground as an unmitigated benefit. Practitioners sometimes choose to work alone instead of involving other services (Mason & Evans, 2020). Absent a context of mutual understanding and communication between agencies, extending “collaboration” potentially tangles support up in disputes and coordination difficulties. Clashes of professional models are a mainstay of the interprofessional working literature, but this review found that difficulties may arise as much from unawareness and knowledge of other professions’ models as from contradictions. Anxiety and uncertainty can be seen to spill over in practitioners’ attempts to pass on responsibility for mental capacity assessments, and in other common tensions.
Third, information about the self-neglecting person is often fragmented among different practitioners working to their own immediate remit, complicating the process of building a holistic picture that is understood and shared across professionals. In itself this is common, but the complexity of many self-neglect cases, and the likelihood that self-neglecting individuals may be unforthcoming with most practitioners, intensifies the challenge. Research has considered how individual services struggle to think and work in holistic and/or person- centered ways (Harris, 2022; Mason & Evans, 2020), but this has less often been analysed as a whole-system issue resulting from communication failings.
Fourth, the review confirms that safeguarding and agency leadership have an important role in clarifying complexity and setting priorities on self-neglect, by setting a consensual framework through the procedures they draft, but also in the support and follow-up offered. Monitoring and learning from self-neglect is complex because desired outcomes are not always clear: services want the person to be safe, but not at the expense of their wishes and self-determination. These dilemmas appear elsewhere in health and social care, but are often particularly sharp with self-neglect. As case studies, SARs are excellently suited to capture this complexity, but this review raised the question of what else is needed to complement them and ensure the evidence-base is balanced by a consolidated record (not just isolated examples) of successful practice.
The review has also identified gaps. Notably, it has flagged the need for research to go beyond identifying tensions that arise between agencies and explore practical measures with the potential to reduce them. SARs too tend to focus on failings in interprofessional communication without exploring what underpins these dynamics, as to do so in depth mostly goes beyond their scope. With few exceptions (Aspinwall-Roberts et al., 2022; Harris, 2022), social work perspectives are over-represented in research on interprofessional working with self-neglect; the field would benefit from complementary in-depth studies with other professions, and social work from the more holistic insights this would bring. Lastly but significantly, the review raises questions about spaces for the perspectives of people with lived experience of self-neglect. Practitioners are prominent in the research literature on collaborative working and are key voices in SARs, reflecting their knowledge of the day-to-day mechanisms of, and obstacles to, collaboration. People with lived experience have important insights into how that collaboration is constructed around (and sometimes without) them, which would enhance discussion and practice but feature only sporadically in the self-neglect evidence-base. Lived experience input to SAR processes is invited on the relatively rare occasions that the person remains alive, but it remains unclear how consistently people with lived experience feed into SAR quality assurance, SAB governance and training. SABs collect and report on satisfaction data with outcomes from people who have been safeguarded; however, participatory rather than consumer forms of involvement are seldom explicitly identified in reporting, though the research team knows anecdotally of stronger examples of representation at some SABs. Despite the undoubted challenges, as people who self-neglect are often wary of services, making lived experience perspectives on self-neglect more prominent would bring benefits to policy generation, training and monitoring. This might be considered a further PT for exploration, drawn from the study's lived experience input rather than the research or SARs.
Strengths and limitations
A strength of this review is the breadth of its sources. It answers Preston-Shoot's (2020) call to integrate research and SARs. Our stakeholders generously provided opportunities to check that our account resonated with lived and practice experience. The review's sources also bring limitations. The dominance of qualitative studies is unsurprising given the topic, but leaves the evidence reliant on practitioners’ stated perceptions of things such as the quality of referrals, without independent evaluation.
Evidence from the SARs provides only partial triangulation. Although they are an unparalleled repository of case studies rich in contextual details of practice and incorporating critical reflections from practitioners close to the case, SARs do not lend themselves to the usual academic standards of quality assessment. They have been critiqued as insufficiently cumulative for failing to build on earlier reviews or research, fostering defensive practice through their focus on failings, over-reliant on training and proceduralism as recommendations despite limited evidence of sustained efficacy, lacking a “gold standard” method, and too restricted in scope to analyse the micro-dynamics operating between professionals below the surface (Manthorpe & Martineau, 2017b; Preston-Shoot, 2020, 2017). Though SARs have undergone incremental improvements in response, these limitations cannot be casually dismissed. Our synthesis aimed to compensate some of these limitations, such as the lack of cumulative knowledge-building or the focus on practice failings, by reviewing the SARs in conjunction with the research-base. Challenges remained in that most of the SARs (and indeed, some of the research papers) from which our mid-range theory was constructed do not discuss theory explicitly, presenting an interpretive challenge (Pearson et al., 2015, p. 590) that inevitably increased the role of subjective judgement in this review.
Concentrating on interprofessional collaboration means the research considered in this review emphasis emphasized improvement in working together under existing conditions. SARs’ focus too is set in statutory guidance as learning for “individuals and organisations” (DHSC, 2023), and primarily explores local lessons. Arguably this understates the wider context of whether the necessary resources are in place to implement policy as intended. Collaborative working practices take place amidst a landscape of care where moves towards integrated working are tempered by countervailing realities of budgetary constraints, fragmentation and destabilizing reorganizations (Miller et al., 2021). Practitioners struggle to coordinate effectively with available resources (Hastings & Gannon, 2022) and an increasingly harsh tone in social policy has reduced opportunities to act preventively towards self-neglect. The sources reviewed, and therefore our synthesis, generally leave this macro-context under-explored beyond the immediate organizations concerned.
Conclusion
Theoretically driven synthesis of the research literature with SARs enables integration of contextualized case examples with studies that aim for greater generalization. Through this method we examined contexts and mechanisms that facilitate collaborative working to support people experiencing self-neglect, a particularly complex, challenging area. Although the current state of the evidence-base limits the practical recommendations for improvement that can be directly made, the suggested PTs support planning and reflection by identifying some of the conditions required for the effectiveness of training, procedures, practice and leadership. As social workers and allied services wrestle with growing demand for safeguarding and strained sector budgets, this synthesis points to some ways forward in refining and enhancing the contribution made by collaboration between professionals and organizations.
Footnotes
Ethical approval
Ethical approval was not required for this review as it involved only secondary analysis of publicly available texts.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the NIHR Health Services and Delivery Research Programme (NIHR 133885). The views expressed are those of the authors and not necessarily those of the NIHR or the Department of Health and Social Care.
Declarations of conflict of interest
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Orr co-authored some of the articles included in the review. Although other team members therefore reviewed these papers, it cannot be excluded that this indirectly influenced their evaluation. No other conflicts of interest have been identified.
Authors’ contributions
All authors contributed to the review and write-up. EW led the literature searches. EW and DO undertook screening. DO, EW, and CM carried out research study data extraction and appraisal. DO, CM, MN, EW, and NS undertook data extraction of the SARs. DO, CM, MN, NS, and EW contributed to the synthesis of the data. DO wrote the final manuscript with input and edits from HvM, EW, MN, and CM.
Acknowledgements
The Authors acknowledge the following people for their contribution to this article. Michael Preston-Shoot, Suzy Braye, Andrew Voyce and Michelle Lefevre made valuable comments on earlier drafts. We gratefully acknowledge the valuable input of the stakeholder groups named in the article methods, whose perspectives did much to improve the study, and the work of Reima Maglajlic in supporting the involvement of experts by lived experience. Responsibility for any errors remains our own.
Data availability statement
Repository: Realist review of collaborative working to support people experiencing self-neglect: data extraction summaries for (a) research studies; (b) SARs, ![]() . This project contains the following underlying data files: Collaborative working self-neglect realist review Research Studies Data Extraction Table Collaborative working self-neglect realist review SARs Data Extraction Table IF-THEN Statements expressing Program Theories.
. This project contains the following underlying data files: Collaborative working self-neglect realist review Research Studies Data Extraction Table Collaborative working self-neglect realist review SARs Data Extraction Table IF-THEN Statements expressing Program Theories.
The data extraction files (in .xlsx format) show the data extraction underpinning the analysis, for research studies and for SARs. The “IF-THEN Statements” file (in .pdf format) shows the intermediate steps of the analysis, prior to condensing into overarching program theories. This study is an analysis of policies which at the time of review were openly available at locations cited in the reference section. These data are available under the terms of the Creative Commons Zero “No rights reserved” data waiver (CC0 1.0 Public domain dedication).
Any other identifying information
The review was prospectively registered in the following databases:
ISRCTN Registry Number: ISRCTN16282284
PROSPERO Register Number: CRD42022329889
