Abstract
Summary
This article concerns interpreter-mediated Mental Health Act (MHA) (1983) assessments where either a signed or spoken language interpreter is required. It reports data from 132 Approved Mental Health Professionals (AMHPs) in England who have direct experience of such circumstances addressing expertise, training, readiness, and potential influences on the outcome when interpreters are involved. Quantitative data were collected by means of an online survey analyzed descriptively with additional open-ended qualitative responses analyzed thematically.
Findings
More interpreter-mediated MHA assessments were reported as occurring in hospital than in community settings. Although AMHPs were confident in their expertise, nearly two-thirds felt they were less effective when an interpreter was involved. The vast majority had received only minimal training on how to work with an interpreter. Recording of language and interpreter use in the assessment was revealed as inconsistent. Most AMHPs thought incorrectly that interpreters were subject to mandatory registration with assured minimum standards of qualification and expertise. Practical problems associated with the timeliness of access to interpreters and complexities of using telephone interpreters instead of face to face were raised. AMHPs expressed a wish for more training and guidance including expectations of the interpreter role.
Applications
Consistent standards of formal recording of interpreter use as part of annual monitoring of the MHA are required to understand any potential inequities of outcome resulting from language mediation. Joint training with interpreters is desirable with more specific guidance and resources for working AMHPs and interpreters to promote best practice.
Introduction and background
The Mental Health Act (UK Government, 1983), henceforth MHA, is a piece of legislation in England and Wales that allows for the formal assessment of a mentally ill person who might be a danger to themselves or others. Similar legislation and statutory guidance exist in many countries around the world (Fistein et al., 2009). Potential outcomes for an assessment conducted under the MHA might range from no admission, voluntary admission, to compulsory detention in a suitable psychiatric facility for assessment, treatment, protection, and care. In addition to a medical assessment, the Approved Mental Health Professional (AMHP) role explicitly requires the application of a social care perspective at the point of assessment. Their role ensures that options other than compulsory admission are investigated, the voice, and perspective of the person being assessed are taken into consideration, and their best interests are safeguarded (Campbell, 2010; DoH, 2015 para 14.34; Karban et al., 2021; NIMHE, 2008). Prior to the revisions to the Act in 2007, it was an exclusively social work role and today 95% of AMHPs are social work professionals (Skills for Care, 2022).
Central to the legislation (MHA, Section 13 1C (2)) and statutory guidance (DoH, 2015 para 14.49 p. 121) under which AMHPs act, is a fundamental instruction to ensure that individuals are assessed “in a suitable manner.” Originally this wording was an insertion into the MHA 1983 specifically at the instigation of the British Deaf Association (Jones, 1991, p. 48) and through a parliamentary lobbying group because of concerns that failure to assess Deaf people in British Sign Language (BSL) would result both in unjustified deprivation of liberty and/or failure to identify significant mental distress. However, the concern to ensure clear communication and understanding regardless of language use is common to all MHA assessments to this day, not just those that might involve Deaf BSL users. In Wales, for example, it also refers to the choice of assessment in Welsh or English. It is reasserted specifically in the current guidance (DoH, 2015, para 14.115–14.119 p.132). The meaning of suitable manner has been expanded to encompass a range of possible barriers to meaningful expression and comprehension between those being assessed and the assessors. This might include not interviewing when the person being assessed appears to be under the influence of alcohol or other substances or, for example, interviewing through a closed door or window (DoH, 2015, para 14.55 p. 122). However, an obvious potential impediment to being assessed in a suitable manner is when the professionals and the person being assessed do not share a common language. The inclusion of a signed or spoken language interpreter within any mental health process introduces an element of indirect communication and additional complexity to all (Costa & Briggs, 2014; Glickman & Crump, 2013; Searight & Armock, 2013).
It is unknown how many MHA assessments per year involve also a spoken or signed language interpreter nor how many people who undergo assessment are users of languages other than English. Despite reforms to improve data quality and reporting of MHA assessments, detentions, and outcomes (NHS Digital, 2017), language characteristics of the person assessed are not in the minimum data set, nor whether an interpreter was required in the assessment. Although individual AMHPs may record this information on their AMHP report forms, there is no mandatory requirement to upload language or interpreting data to NHS Digital in the same way as gender, age, and ethnicity, for example, is recorded in the minimum data set for purposes of annual monitoring (NHS Digital, 2022).
No substantive attention was given to the practice circumstance of interpreter-mediated MHA assessment in the Final Report of the Independent Review of the MHA (DHSC, 2018) or in its supporting documents (DHSC, 2019) other than a passing acknowledgment (p.57) of interpreters as reasonable adjustments in cases where a person is disabled, barriers faced (unspecified) for refugees and asylum seekers accessing therapeutic treatments (p. 91), as a potential issue in taking patients’ treatment views into account (p. 108) or a note that BSL provision at the point of emergency may be more costly but could result in better decision making at an earlier stage (p.114). We contrast these passing references with the strong contemporary emphasis on reversing disproportionate rates of detention and disparities in practice focused on what the independent review panel refer to as Black and Minority Ethnic (BAME) populations (Morgan et al., 2017; Weich et al., 2017). However, such a focus is not synonymous with inequalities in practice, outcome, or the promotion of autonomy that might arise through language mismatch between the assessor and potential patient. This is because attention to diversity in ethnic identity is not necessarily synonymous with a focus on diversity in language use. People from many different cultural backgrounds resident in England may be first language English users and many may not be. You cannot tell a person's language preference from ethnic identity data. Although cultural competence and cultural advocacy have been important features of the revisions to MHA (1983), issues arising from language use remain implied rather than explicit. This lack of attention is noteworthy given the increasing linguistic diversity of the UK overall (ONS, 2021) and the needs of migrants, refugees, and asylum seekers within the mental health system (Pollard & Howard, 2021; Uphoff et al., 2020). The Office of National Statistics (ONS, 2021) census data for England and Wales records that 4.1 million people (7.1%) of the overall population were proficient in English but did not speak it as their main language. Of the 5.1 million (8.9%) who did not report English as a main language, 17.1% (880,000) could not speak English well; 3.1% (161,000) could not speak English at all.
The current Code of Practice for England (Department of Health, 2015) strengthened existing guidance concerning the provision of interpreters, whether for signed or spoken languages, and responsibilities specifically with respect to deaf signers, yet no evidence exists about compliance, monitoring of quality of practice, outcomes, nor impact on rights and responsibilities of all parties involved. This is important to mitigate against the potential for illegal detention should the process be adversely impaired in situations where language mediation is required although there is no case law on this. The potential adverse implications of poorly executed interpreter-mediated practice in MHA assessments are of fundamental relevance to the principles of choice and autonomy, least restriction, therapeutic benefit, and the person as an individual that underpin the recent revisions to the MHA (DHSC, 2018). This is because well-executed interpreter-mediated assessments, in which both professionals and interpreters understand and know how to work together, have the potential to minimize barriers to expression and understanding (Napier et al., 2022; Tipton, 2016) and a fundamental human right under both the Equality Act 2010 and the UN Convention on the Rights of Disabled Persons.
The current AMHP competencies within the regulations (UK Govt, 2008) specifically include, “be able to communicate effectively with service users, relatives and carers when undertaking the AMHP role (Competence 4)” and “be able to promote the rights, dignity and self-determination of service users consistent with their own needs and wishes to enable them to contribute to the decisions made affecting their quality of life and liberty (Competence 1)”. Both competencies imply the provision of interpreting/translation when required.
A scoping review of evidence concerning interpreter-mediated MHA assessment and their statutory international equivalents revealed no quality evidence of good practice in this context (Rodriguez-Vicente et al., 2023). As previously discussed, no national evidence exists on the prevalence of interpreter-mediated MHA assessments nor the experience of AMHPs, interpreters, medical assessors, service users, or carers who have undergone MHA assessment via an interpreter. The INForMHAA (Interpreters For Mental Health Act Assessments) study was set up to address this evidence gap and collect data from a range of stakeholders with the aim of producing specific practice guidance and helpful resources for all parties. In this article, we present data from 132 AMHPs who completed an online survey all of whom had direct experience of interpreter-mediated MHA assessments in England.
Methods
The principal research question of the study overall is: How does interpreter mediation impact MHA Assessments and how can interpreter-mediated MHA Assessments be improved? In this first stage of data collection, the aim was to scope the range of experience of AMHPs undertaking MHA assessments with an interpreter and their view on training, competence, and any potential issues that might arise. A survey method was chosen with closed and open questions. These were derived from an initial online consultation with a small group of AMHPs, interpreters and service users, and carers prior to the application for the research grant that was awarded, and issues identified from a scoping review of interpreter-mediated practice in statutory assessments (this is the subject of a separate publication). The survey data would feed into the development of in-depth interviews to follow with AMPHs, service users and carers, interpreters, and AMHP and interpreter training providers which are reported elsewhere.
Following ethical approval, the study was advertised through AMHP research and training networks and via the study's bespoke website. Only qualified and currently approved AMHPs who worked in England with experience of having carried out an assessment with either a spoken or signed language interpreter (or both) were eligible to participate. (Those based in Wales were included if they carried out assessments in England). Data were collected through a three-month online survey (December 2021–February 2022) on the Qualtrics secure data collection platform. The survey used is available on request to the authors. Respondents could participate anonymously, only giving contact details should they wish to volunteer for the interview component of the research. No details of exactly where they worked were required other than at a regional level. Quantitative data were analyzed at a descriptive data level only with the support of SPSS. The many open-response comments were systematically grouped by question from which some overriding themes were derived. This approach was more akin to that of qualitative description rather than a wholly inductive thematic analysis (Kim et al., 2017; Neergaard et al., 2009). The qualitative elements of descriptive analysis are used to further illustrate the main results from the quantitative analysis, rather than being presented as a qualitative data set in their own right. Direct quotes included are intended to be illustrative; the participant identification number is in brackets.
Results
The sample
In total, 132 AMHPs completed the online survey, partially or fully (Table 1). This is 3.5% of the AMHPs in England whose total number is 3,800 (Skills for Care, 2022). It is considered a good number given the requirement that to participate AMHPs also needed to have direct experience of having carried out at least one MHA assessment with an interpreter.
Respondent characteristics.
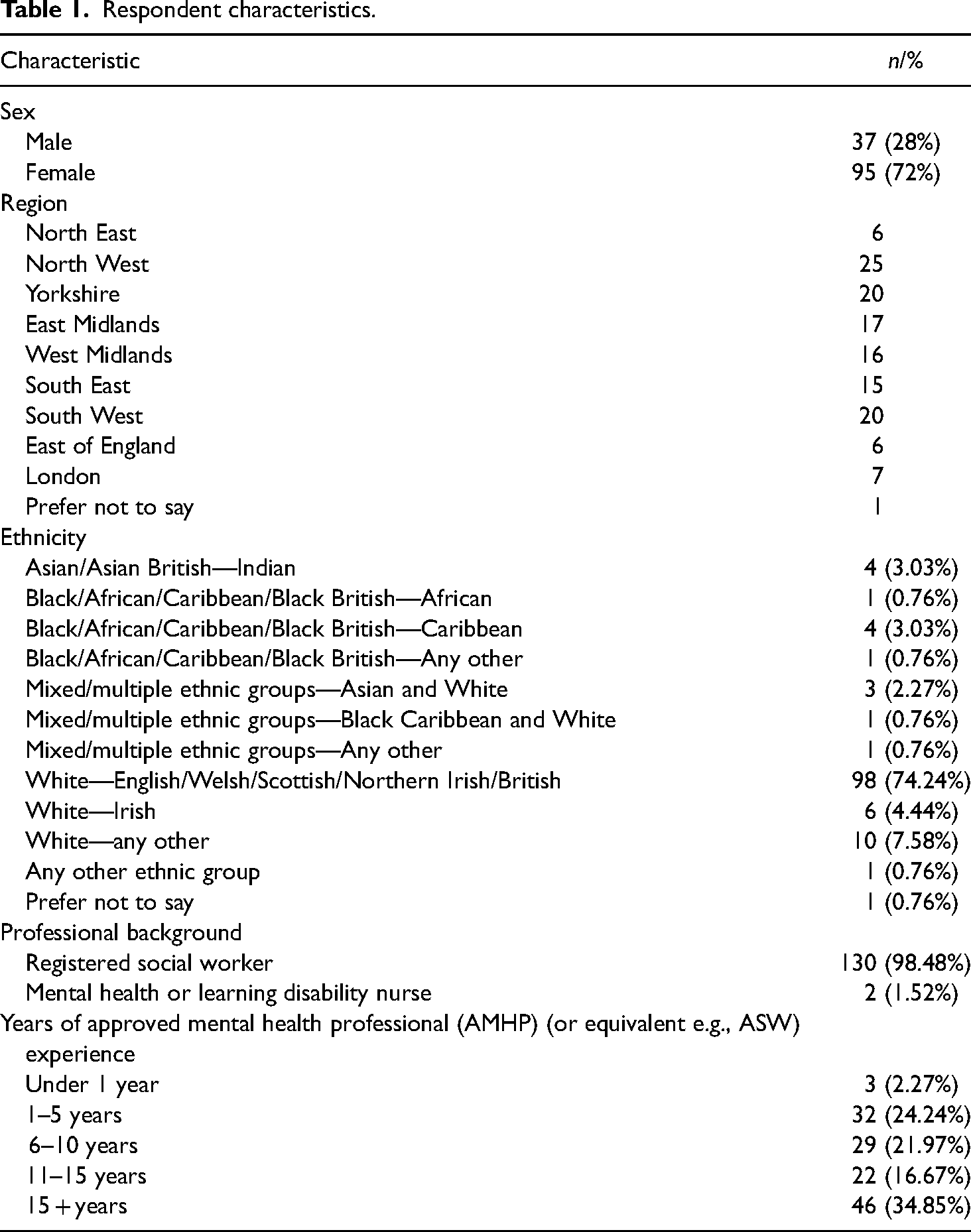
All but two participating AMHPs were social workers (the others being a mental health or learning disability nurse) which is consistent with national (England) figures of only 5% of AMHPs being drawn from professions other than social work (Skills for Care, 2022). All regions of England were represented but with fewer responses from London, the South East, and North East. The percentage of those who identified as being of an ethnicity that was Black, Asian, Mixed, or Minority Ethnic (12.2% (n = 15) is less than the national figures for AMHPs (20%) (Skills for Care, 2022). A higher percentage of women (72%; n = 95) than men (28%, n = 37) took part which is very close to the gender split in national figures for AMHPs of 74% female, 26% male (Skills for Care, 2022). There is a good spread of participants by number of years working as an AMHP, with over half (51.52%; n = 68) having 11 years or more experience as an AMHP. The national comparator is 56% of AMHPs who have 10 years or more experience (Skills for Care, 2022). National AMHP workforce data does not report any disability-related characteristics, however, the study's focus on signed languages as well as spoken languages prompted the collection of data on deafness in the sample. One identified as a Deaf BSL user and 5 more as hard of hearing/hearing impaired/hearing loss. National workforce data do not record the language characteristics of AMHPs. In this sample, 22 out of 132 (16.7%) described themselves as multilingual i.e., possessing a working knowledge of more than one language with three saying they have infrequently acted as an interpreter in an MHA assessment.
AMHPs in the sample very regularly carried out MHA assessments in the community and in hospital settings; their practice was current and therefore their views were a reflection of frequent and contemporary practice. In Table 2, the frequency of MHA assessments over the past 12-month period is contrasted with their frequency of assessments with an interpreter, in both hospital and community settings. Note, if a respondent said “none” they may have carried out interpreter-mediated assessments, just not in the past 12 months. Although assessments with an interpreter were far less frequent, some AMHPs had regular experience with them, be it more in a hospital than in a community setting.
Frequency of Mental Health Act (MHA) assessments in community and hospital settings, with and without interpreters over the previous 12 months (n = 132).
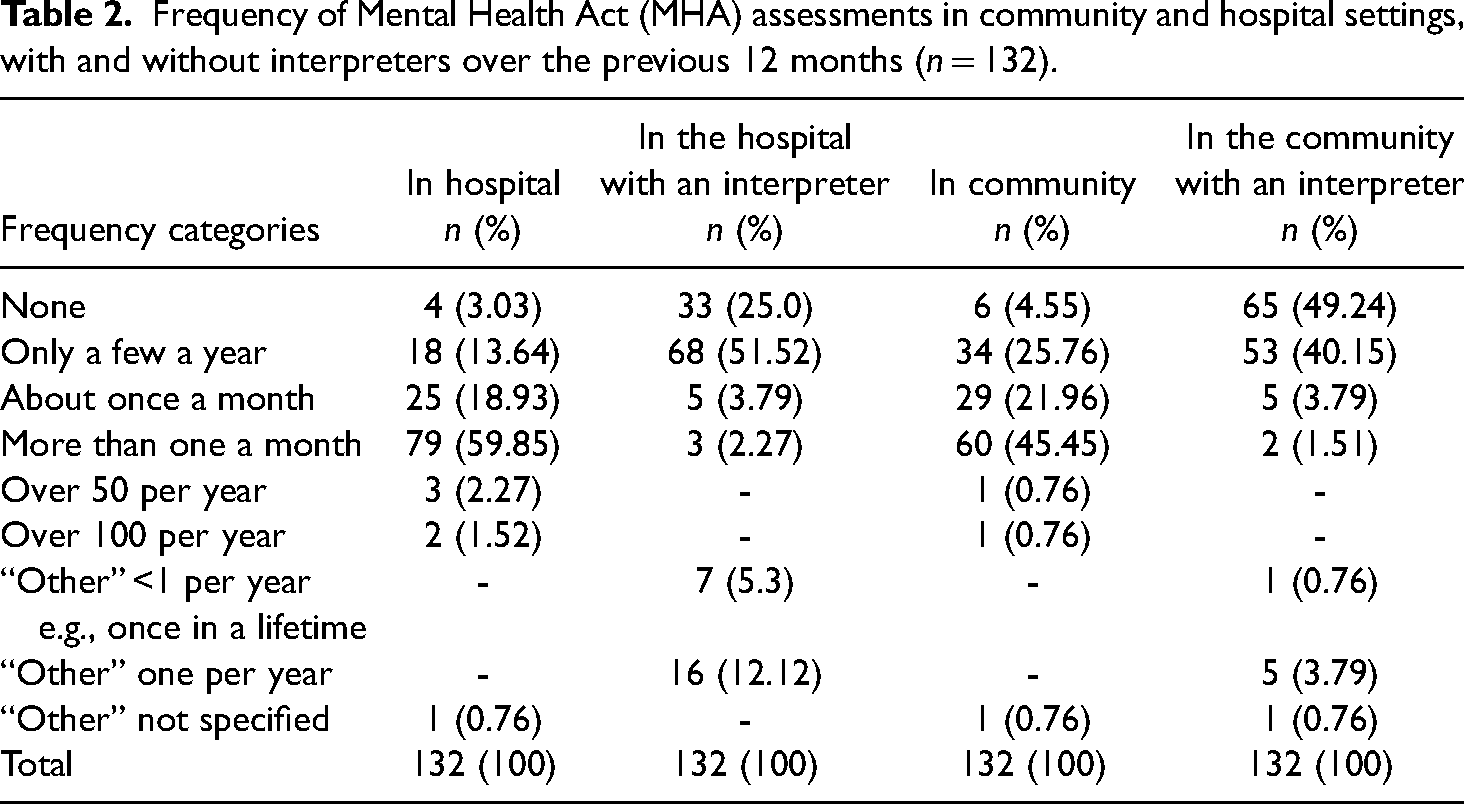
Most AMHPs had worked only with spoken language interpreters (n = 98; 74.2%) and one person exclusively with signed language interpreters. Thirty-one (23.5%) had worked with both spoken and signed language interpreters.
Theme one: Training and support
Given that MHA assessments using an interpreter were relatively infrequent, but nonetheless a recurring element of AMHP practice, respondents were asked about the training they had received in working with interpreters. Of the 121 who provided open-text answers, only nine could recall some specialist training as part of their course. In the case of seven of these, the training was part of a more general focus on the assessment of deaf people which included specialist input on how to work with a sign language interpreter. Since approval as an AMHP, 71.8% (n = 89) said they had not participated in any further training on working with interpreters. Furthermore, 58.9% (n = 73) said they had never received any joint training with interpreters (in any setting, not just with respect to MHA assessment). Nearly 60% (n = 67; 59.3%) concluded that their training had not adequality prepared them for working with interpreters whether in their AMHP role or otherwise. … on the one hand I do feel adequately prepared for working with interpreters and hadn't considered the issue to be an area of outstanding need prior to this questionnaire, however on the other hand the lack of specialist training in this area that this questionnaire has highlighted does seem like an area of practice that needs addressing. (25)
Many participants who had not received much training in working effectively with an interpreter in the MHA assessment situation explained that they had largely drawn on their personal or professional experience over time. This included their own family and personal experience of living as a multilingual or their other roles in social work. “Learning on the job” was a common response to being asked about training although there was also an awareness that this was not adequate. It was hard to spot where a potential difficulty might lie if you are just learning as you go along. I don't feel I have low competence in this area but I may of course be misguided and it would be useful to have some training or observation of my practice in this area to better assess my level of competence. (55)
The issues mentioned as those learned through experience included: needing to brief interpreters in advance that as an AMHP they wanted to hear any disordered language that a person might be using, rather than having it tidied up into something comprehensible; that it was not acceptable for an interpreter to summarize what someone had said, instead of interpreting it in full; ensuring that all parties, including doctors, speak directly to the person being assessed, not to the interpreter; not relying on family and friends to interpret that might compromise impartiality; ensuring that the interpreter fully understands the statutory nature of the MHA assessment through careful preparation and briefing with them. I think neither party, interpreter or AMHP, is fully prepared for this. I think interpreters don't always understand the process of MHA assessment or what it is for. They, therefore, don't always understand the information AMHPs need. This is not a criticism, as they cannot be expected to without training and support, but it can affect the assessment when they don't repeat what the person has said verbatim or include information such as tone and pitch and whether the speed is normal for that language. (88)
Although respondents were highly reflective and clearly many had a great deal of experience, there was also a sense from those who wrote additional responses that the expectation that you pick up as you go along how to work with an interpreter was not good enough given the gravity of the kinds of decisions that are made during MHA assessments. I am always anxious about this—I am making judgements about a person's civil liberties based on their presentation which is “filtered” through an interpreter so am I interpreting their situation accurately? (26)
Theme two: Practicalities of arranging for an interpreter
Asked how confident they felt about arranging for an interpreter in an adequate timescale for an MHA assessment, nearly one-third (n = 36; 31.3%) said “not at all confident.” This is not necessarily a reflection of whether in practical terms an AMHP knows how to book an interpreter, it is also a reflection of whether such a booking can be achieved in a timely manner. Either way, this has implications for the person being assessed. In the following, the AMHP describes how the competing priorities of ensuring high-quality interpreting and addressing with urgency a person's mental distress can create difficult decisions for AMHPs as responsible for the MHA assessment: There is a degree of urgency when a MHA [assessment] is called—we have to weigh this up against how proportionate it is to delay—it's crucial to make every effort with the resources available to make sure you understand the patient and they understand the situation—as far as language is concerned—phone interpretation is not perfect—it's also not always clear what is a language/communication issue and what is a symptom of mental health—I guess if I’m not satisfied how accurate the information is that I’m getting (to base a decision on), I have to weigh that and the delay involved in getting better information, against risk and urgency to arrive at a decision—detaining a person on basis of dubious information is a problem but so is holding a person and drawing out the process when person may need urgent mental health care under compulsion. (104)
Over half of the respondents (n = 59; 51.3%) said there were some languages that they found difficult to book interpreters for. Examples given included Russian, some Eastern European languages (Lithuanian, Romanian, Hungarian), some Chinese dialects, Vietnamese, Farsi, dialects of Kurdish, and some African languages, or as one respondent put it “anything out of the ordinary”. Furthermore, asked how easy they found it to source written or signed translations of information on Independent Mental Health Advocates (IMHA) in a timely manner, nearly three quarters (n = 85; 73.9%) responded “not very easy.” Other difficulties mentioned included potential restrictions that arose from which interpreting services the Local Authority and NHS Services had a contract with which could impede choice when a specialist was required, or an alternative interpreter needed to be sourced because of their pre-existing contact with the person being assessed.
Most respondents (n = 92; 80%) had worked with both face to face and remote interpreting (e.g., by telephone or more rarely video telephony), and 2 had only ever had experience of working with remote interpreters. Among the 21 (18.3%) who had only worked in face-to-face mode, there were some strongly expressed feelings that interpreters should be physically there for a MHA assessment to be effective, and that remote interpreting was not acceptable. This extended example, provided by one respondent in an open text answer begins to highlight the intersecting complexities and competing priorities faced by the AMHP in their role as the co-coordinator of the MHA assessment when an interpreter is also required. Some specific references to language, region, and culture have been deliberately excluded in this quotation to protect anonymity: I do not think the service I currently have access to is fit for purpose, especially over the phone, and often find that interpreter identified for assessment has not been trained in interpreting for MHA … At times I have had to use either family or one of the assessing doctors to interpret which is clearly not good practice. Interpreter familiar with the person had a tendency to offer her own opinions as she had known the man for many years and been involved in Mental Health Act assessments before. I did challenge her (and attempt to find an alternative interpreter). On balance the positives outweighed the negatives though as he was comfortable with her and a lot more willing to talk than he would have been with a stranger. His [cultural] background and the circumstances under which he was forced to leave his country led him to want to ask any new interpreter all about their personal history before being willing to accept their services as an interpreter. In the situation where the interpreter was a distant cousin (but within the very small [regional] community) I decided that with the individual and their families’ permission I would continue with the interpreter as there were no other speakers of that particular language available from the translation services the Local Authority contract with. I am unsure if in hindsight this was the right thing to do—I am not aware of any untoward consequences but even so … .” (24)
Theme three: Recording of interpreter use
The minimum data set for MHA statistics (NHS Digital, 2022) does not record what language an MHA assessment may have taken place in, whether an interpreter was used, nor the preferred or first language of the person assessed. There are no national comparative figures. On a local/regional basis, AMHPs may record this information on the AMHP report form but this form is designed on a local basis rather than there being a national template. Consequently, the consistency and comparability of recording with respect to interpreter use and the preferred language of the person assessed is unknown. Respondents were asked about whether they recorded when an interpreter was used in MHA assessments.
Of the 115 who replied, 100 said sometimes, 1 “always” and 14 “never.” This recording did not necessarily mean that the language used within the assessment would be recorded. As was pointed out in some of the free-text responses, AMHP report forms could be quite restrictive. Some might have a specific box to tick if an interpreter was used but recording which languages were left to the AMHP to add into another part of the form if they thought to do so. In some cases, AMHP report forms had a drop-down menu of languages that could be ticked but this might not cover all languages. Also, there was a difference between recording the language of the assessment and a person's preferred or first language. As some respondents pointed out the onus was on the AMHP to do this if they felt it important. Some recorded information about languages and interpreting in a section on interviewing in a suitable manner as the only place to put it. Others pointed out that a person's first or preferred language might be put in the AMHPs social circumstances report and recorded on the person's social care file.
Other potential recording pitfalls included the fact that the name of the interpreter used was not necessarily recorded which could mean the possibility of continuity for the person being assessed is taken away as the same interpreter could not be requested again. Equally, if the interpreter was not suitable there was no specific prompt to record this and to say should be avoided in the future. Once again it is at the discretion of the individual AMHP as a highly skilled professional and their personal practice whether any such information is recorded anywhere.
Theme four: Does an interpreter affect the process of assessment?
The presence or not of an interpreter was perceived to have a significant effect on the process of the MHA assessment. Nearly two-thirds (n = 71; 61.7%) when asked whether they “can/could carry out MHA Assessments through an interpreter with the same degree of effectiveness as in monolingual assessments?” replied “no.” As one respondent pointed out, however, “I am confident in my own assessment skills but find skills and experience of some interpreters problematic.”
Some of the effects on the process of a MHA assessment as mentioned in the open text comments included: A disruption the “flow” of an assessment if the AMHP and assessed person are unable to communicate directly, given how much an AMHP relies on linguistic and para-linguistic features of an individual's discourse as part of their MHA assessment of how mental ill health may be affecting them. I find it difficult to establish the true level of someone's mental crisis when communicating via a third party—never truly sure what has been relayed back to myself i.e., a literal translation can be given but the context of what is being said can often be missed. (36)
Asked whether subsequent to an MHA assessment they had ever realized that they should have had an interpreter when one had not been present, over one-third said yes (n = 42; 36.52%).
Theme five: Cultural advocates and language concordant support other than interpreters
The MHA Code of Practice to which AMHPs work in the execution of their role and duties (DoH, 2015, para 14.119 p. 133; para 22.67 p.236) states that cultural advocates may be present in addition to interpreters. A cultural advocate was defined in the survey as “advocates (i.e., a person who usually shares or understands a service user's ethnic and/or cultural background and who is able to help ensure their views and experiences are represented) or any other type of language concordant support (e.g., people who share the same language as the person being assessed e.g., legal intermediary, deaf relay interpreter)”. Respondents were asked if they had ever used a cultural advocate. Although 2 preferred not to say, nearly three-quarters (n = 86, 74.8%) said “no” they had never used one. Furthermore, 98 from 113 (86.7%) said they did not know how to arrange for a cultural advocate to attend a MHA assessment. It should be remembered that these results are in the context of AMHPs with specific experience in carrying out MHA assessments in circumstances where an interpreter is required, not in a general sample of AMHPs.
Theme six: Interpreter training, competence, and professionalism
In terms of direct practice with interpreters, 58 said that they “expect all interpreters to be registered with a regulator,” yet there is no national mandatory regulation of interpreters. There are voluntary registers such as the National Register of Public Sector Interpreters (NRPSI; https://www.nrpsi.org.uk/) and National Register of Communication Professionals with Deaf and Deafblind People (NRCPD https://www.nrcpd.org.uk) but there is no independent regulator of interpreters who set minimum standards of qualification, skills and experience, nor who monitor interpreting practice. While voluntary registration bodies have codes of conduct and minimum expectations of competence as well as examples of good practice (e.g., https://www.nrcpd.org.uk/code-of-conduct), interpreting is not a regulated profession, something of which these AMHPs were unaware. Only 82 AMHPs said they would “always check whether the interpreter is qualified and had any training in MHA assessments or mental health more generally.”
In total, 11 out of 115 respondents (9.6%) said they had made a complaint about an interpreter. Specific examples of cause for complaint offered in the open answers reflected three main issues:
(i) Organizational problems. These included the agency sending an interpreter who did not speak the language or dialect of the person being assessed; the interpreter being late without reason; the interpreter failing to attend but the agency still charging for their time; interpreting agency unable to supply an interpreter at the last minute and provided phone interpreting instead from someone who in the view of the AMHP appeared not to be listening or engaged anyway. More than one person mentioned that there was no mechanism for barring an interpreter from working if a complaint has been made because it is up to the agency who they send following an interpreter request. In fact, the name of the interpreter who was to be sent was often not shared in advance and so if an AMHP had reason to be concerned about an individual interpreter, they had no means of stopping this. The Local Authority or Trust having a specific contract with a specific agency meant it was not possible to book an interpreter outside of that contract and also did not assist this situation should it arise.
(ii) Lack of professionalism. It is interesting to note that the issues mentioned very much reflected key value issues for AMHPs from their own professional perspective. For example, the interpreter using stigmatizing language toward the person being assessed was mentioned. This did not necessarily refer to during the assessment itself but rather to the interpreter's conversations with the AMHP beforehand or afterwards and their choice of language to describe a person in mental distress. The interpreter not keeping professional boundaries and talking about their own mental health or their over-involvement in the life of the person being assessed was mentioned which was of concern given that boundaries are something very clearly emphasized in mental health work. Some examples concerned adult safeguarding issues that the AMHP identified such as a pre-existing relationship between the interpreter and person being assessed that was not declared and involved some financial dependency and an interpreter threatening a person being assessed on grounds of political differences: X [the person being assessed] was getting very agitated by interpreter's questions. I had suspicions based on negative comments pre-assessment that what we were asking wasn't being translated in the spirit it was meant—allowing for fact there isn't the equivalent in some languages for what we traditionally ask. X then barricaded themselves in to a room and family called to try de-escalate. Transpired interpreter from a different ethnic group in country of origin war zone and had been by their own admission threatening X with imprisonment which triggered very severe trauma responses (148)
In the case of the safeguarding concerns, these were reported by the AMHPs involved through the AMHP report form.
(iii) Poor interpreting skills/professional practice. From the AMHPs perspective feeling like they were not receiving the full range of communication and language displayed by the person being assessed was a key source of concern. This had different forms including, from a content perspective, being aware that the interpreter was only summarizing what the assessed person said rather than everything they communicated or how they communicated it. Boundaries were also mentioned again with regard to professional practice when it seemed that when informal introductions ended and the actual assessment began was not clear to either the AMHP or the person being assessed (which was their right to know). In a few instances, the problem was simply that the interpreter was not competent enough in the language of the person being assessed or in English to be able to translate what was being said.
Asked about best working practices with interpreters, AMHPs strongly promoted the notion that interpreters were part of the team 102 stating that they “always treat the interpreter as part of the team” and 87 that they “encourage interpreters to let me know if there are any problems understanding the language of the MHAA”. In total, 70.4% (n = 81) also said that they “always” engaged interpreters in briefing sessions prior to a MHA assessment although notably 2 said they never did and 6 only infrequently. In total, 71 agreed with the statement that “It is important for interpreters to share their thoughts about the interaction as part of the assessment process”. These comments on the inclusion of the interpreter in the team were meant more in the spirit of orientation to how people should work collectively. Nobody implied that being part of the team meant that the interpreter was part of the decision-making outcome of the assessment.
Theme seven: AMHPs ideas for additional training
In total, 99 out of 132 respondents gave written suggestions about what kind of training and in what form would be most helpful to them in the future about working with interpreters in MHA assessments. The idea of joint training for those who are working together was suggested, rather than AMHPs and interpreters being trained separately for MHA assessments. This extended to joint training involving doctors undertaking the medical recommendation component part of the assessment. However, as one participant emphasized, this was not just about practicalities or best inter-professional practices. It was also about jointly understanding what the least restrictive forms of joint working would be given the specific context of the MHA assessment in line with core values in how such an assessment should be carried out.
Specific aspects of joint practice from AMHPs’ point of view that were raised included exactly what an interpreter's role is and should be in a MHA assessment; whilst that of the AMHP and the doctor undertaking the medical recommendation are laid out in the code of practice, there was little guidance or agreed understanding on what the role of the interpreter was. For example, to what extent should an interpreter be providing additional cultural information and context? Other topics included how to brief interpreters, how much client related confidential information that should be shared in advance, and what to do if you are not happy during the MHA assessments with some aspect of the interpreting. The responsibility of the AMHP in supporting an interpreter in a stressful situation and debriefing with an interpreter was suggested.
Knowledge gaps were highlighted such as how you know whether an interpreter is qualified for mental health work and what exactly interpreter training consists of and how to access additional learning on cultural sensitivity and cultural competence if required. Two people specifically mentioned that they would like to understand more from the perspective of those being assessed about the impact of an interpreter during an assessment and what better practice would look like. Best communication practices were also mentioned as topics for training such as learning to use shorter sentences, avoiding euphemisms, keeping eye contact with the person assessed.
It was emphasized that training should be incremental, stretching from initial training as an AMHP and through top-up and refresher short courses. Furthermore, that training in translation and interpreting should be integrated into formal Continuing Professional Development, not left to the interest or initiative of individual AMHPs. The idea of experiential learning rather than just reading about issues was highlighted too with possibilities of online training and simulated practice mentioned. A guide to good AMHP practice when working with interpreters was also suggested.
Discussion
AMHPs are highly skilled, expertly trained professionals who carry out a significant role designed to promote appropriate assessment, treatment, and support of those whose mental illness puts them at a real risk of harm while protecting others and promoting universal human rights. Whilst interpreter-mediated MHA assessments are clearly not an everyday occurrence, the substantially large number of survey returns from those AMHPs with direct experience of these indicates it is not an infrequent practice issue. Furthermore, the overwhelming number and length of additional comments that were supplied in open-text responses is a clear indication that it is a topic that is of concern to AMHPs and one they would clearly welcome further training and exploration of in research. As previously discussed, the impacts of language diversity, rather than cultural and ethnic identity, have been hitherto mostly invisible in the discussion surrounding current reforms to the MHA and associated guidance. This endorsement by AMHPs of the importance of focussing on working with interpreters and its effects on the MHA assessment process is of itself an important finding.
In one sense, AMHP concerns that an interpreter may not be appropriately providing full communicative and linguistic access from their point of view is understandable. One of their roles is to gauge the extent to which the person being assessed understands exactly what is happening to them, whether a less restrictive alternative such as voluntary or informal admission might be possible, to protect the rights of the person being assessed and to clearly explain legally what is happening (DoH, 2015, para 14.42, p. 120). A great deal of the information an AMHP would need to make a judgment about the person being assessed comes from their observations of interpersonal interactions, the characteristics of a person's language, para-linguistic features of behavior associated with communication as well as the semantic content of what someone says in response. Indirect communication, such as that through a third-party interpreter, disrupts the AMHP's ability to gauge such features first hand. Hence concerns expressed in these data about the interpreter summarizing, rather than repeating exactly what was said, the suggestion of the need for “verbatim” translations, the importance of the AMHP being able to follow whatever side conversations may be happening between the interpreter and the person being assessed, and the worry that the interpreter may not be portraying the nature of the language being used. For example, if a person's language is disordered it may contain repetitive phrases, have an unusual intonation, and contain unexpected vocabulary choices or words/sounds/gestures that do not correspond to recognized language. If the interpreter tidies up this language or creates a coherent narrative for the AMHP to understand, this is at the loss of the AMHP's window in identifying tell-tale features of state of mind (Farooq & Fear, 2003).
However, some of the suggestions by AMHPs as to how interpreter practice may be improved perhaps betray a lack of understanding of how interpreters are trained and practice. For example, the request for “verbatim translation” in the sense of word-for-word equivalence between one language and the next is rarely used in interpreting practice. Interpreting implies making full sense of an utterance in a source language and conveying that in the target language in a way that is equivalent in that language; of itself a complex task (Bot, 2005; Gile, 2009; Hale, 1997). The French expression “il pleu des clous” would be rendered “it is raining cats and dogs”, not “it is raining nails” for example. It is the equivalence that is sought (Cambridge, 2012) not verbatim translation. However, ensuring that all points the AMHP is making are conveyed, not glossed over or generalized, is a reasonable request because the AMHP must satisfy themselves know that a person's rights have been explained, for example.
The recourse to the idea that an interpreter can disrupt the flow of an assessment is an interesting one and reflects well the idea that from the AMHP's perspective, the assessment does not progress as might usually be expected. However, without an interpreter, the MHA assessment would not be legal or practically possible. Therefore, the real question becomes what it might mean to grasp the disruption that interpreter-meditation brings and know how to work well with it. The fact that AMHPs in this survey could at one and the same time assert their high level of competence in carrying out a MHA assessment when an interpreter was present and simultaneously report that they felt less effective when an interpreter was used, is illustrative of this unresolved problem. It is a common misconception that working with an interpreter means working in exactly the same way as you always have but with the addition of an interpreter who sorts out the language barrier, what has been referred to as the “illusion of inclusion” (De Meulder & Haualand, 2021). The emerging question becomes: what would it mean to work differently within an interpreter-mediated assessment rather than how do you make accommodations because of the interpreter whilst essentially working in the same way? Survey respondents were starting to think about this in their many suggestions for training now and into the future.
Misperceptions by AMHPs about interpreters extended also into basic facts about the status of interpreters. Responses to the questions about regulation and training betrayed the fundamental lack of awareness that the profession of interpreting is not regulated in the same way that social work, medical, and allied health professions are regulated. Voluntary registration attempts to ensure professional conduct, standards of ethics, practice, and qualification of interpreters, as well as sanctions when appropriate, but practitioners are not legally bound by any form of regulation (Napier et al., 2022; Orlov, 2021). Research has shown that standards of qualification among spoken language interpreters are varied in comparison with much more consistent standards for qualification amongst sign language interpreters for example. Also, just because an agency is commissioned by a Local Authority or NHS Trust sends an interpreter when requested, this is no guarantee of their level of qualification or experience.
The delivery of specialist training for interpreters working in statutory mental health is ad hoc and not widely available and tends to be very brief. It is extremely rare to encounter any interpreter with mental health training at all. Most experts in this field have built up their experience over years of specialist practice (Skammeritz et al., 2019) and some voluntary registers such as that of NRCPD, for example, will enable an interpreter to specify their expertise. However, there is not a recognized qualification in mental health interpreting in the UK. From a safeguarding as well as a best practice point of view, these issues are important because interpreters, alongside AMHPs and doctors, are working in situations of extreme vulnerability and sensitivity. Although regular safeguarding protocols for escalation of concerns are in place as our survey data has demonstrated, the recourse to interpreter agencies and professional bodies in terms of consequences of safeguarding concerns is much less clear.
The survey results confirm our initial concerns about the lack of reliable data on how many people are assessed under the MHA through interpreters or indeed what their preferred or first language is. Additionally, systemic barriers to collecting these data effectively have been highlighted starting with the inconsistent nature of what is required to be recorded in the AMPH report form. The presence or not of an interpreter may be a required tick box or left to the AMHP to report in their open comments. The specific language used may be drawn down from a not necessarily complete list of possibilities or not even be asked for. The name and contact details of the interpreter used for purposes of future continuity of care appear to be discretionary. The lack of consistency in recording and the content of what is recorded is concerning because of its potential impact on the monitoring of quality in practice and the scale of need in terms of resources. The survey data hint at the lack of flexibility and availability of interpreters because of which specific interpreter agencies might have been commissioned. This is not a problem unique to interpreter-mediated MHA assessments but recognized more widely in health and social care commissioning strategy (NHS England, 2018). It is notable that in this respect, the apparent solution of using telephone or video interpreting to overcome availability barriers was questioned by survey respondents. During the Covid-19 pandemic, the easement that permitted remote, rather than in-person, MHA assessment (NHS, 2020; Vicary et al., 2020) has subsequently been deemed unlawful (Devon Partnership Trust judgment Case No: CO/2408/2020). Nonetheless, the practice of using a remote spoken language interpreter over the telephone, or a sign language interpreter by video link, continues with apparently little concern. The consideration here is not only to do with the effectiveness of this form of interpreting but also of how its disembodied or remote form might potentially add to the confusion, withdrawal, or distress of someone experiencing serious mental ill health.
The need for a safeguard of a person's rights is currently embodied under the MHA in two ways, the formal role of nearest relative (NR) and of the IMHA. Currently, the NR is determined through a hierarchical list defined under Section 26 of the MHA. They have a number of important rights and functions which are also formally defined (including requiring an MHA assessment to be made, the right to apply for admission [in the same way as an AMHP], rights to information and to object to a Section 3 or a Section 7). This role would be replaced by a new statutory one of a Nominated Person under the draft Bill. In addition, IMHAs are specially trained to represent and support detained patients, a provision extended to informal patients under the draft Bill. In the survey data, AMHPs acknowledge both roles but do not appear to make the additional step of the importance of being able properly to communicate with the NR who may also have the same language need. This is surprising given the safeguarding role that the NR holds. It is also ironic given the origin of the inclusion of the phrase “interview in a suitable manner” that the equivalent role of a language interpreter is not so defined under MHA in much the same way as these two roles have been and continue to be.
Limitations
This study was confined to AMHPs working in England and there was no requirement to triangulate information reported with records derived from AMHP report forms. However, a sub-sample of respondents has been followed up with in-depth semistructured interviews to understand more of their practice experience and this is the subject of a separate publication. Data from the perspective of interpreters is not included. However, interpreters have been surveyed and interviewed separately and this will be reported.
Conclusion
This is the first exploration of the experience of AMHPs in their conduct and experience of interpreter-mediated MHA assessments. It has confirmed the importance of this area of practice and the scope for further evidence-based guidance which the project overall will produce and make openly available.
Footnotes
Ethics
This study received ethical approval from the University of Manchester Research Ethics Committee (Ref. 12163).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by NIHR School for Social Care Research (Grant reference P 172). The views and opinions expressed therein are those of the authors and do not necessarily reflect those of the NIHR SSCR (grant number P172) or the Department of Health and Social Care.
Authors contributions
All authors contributed to the overall design of the study and all elements of its execution. SV, CH, and FE led the design of the survey instrument, and AY and FE on data analysis. NRV, RT, JN, SV, and AY wrote different parts of the final article with all authors contributing to editing and review. AY led the overall study.
Acknowledgements
The authors thank the many AMHPs who took the time to so diligently and extensively reply to our online survey.
