Abstract
Summary
An interview study was conducted with persons receiving home care services and personal assistance in Sweden (13 individuals, 25 interviews) with the aim to analyze their experiences of managing personal and intimate care. The analytical approach was guided by phenomenologically informed research and Erving Goffman's theoretical work on self-presentation and social life as it differs in frontstage and backstage settings.
Findings
A reflected approach to the complex challenges associated with becoming and being a person in need of personal and intimate care was revealed. This involved continuous adaptations and attuning to organizational and relational conditions of formal home care. Being a recipient of personal and intimate care does not mean being passive. It entails relating to and sustaining the care relation, where even choosing to accept suboptimal conditions is an act of agency. The recipients’ private homes were hybridized, transformed both into a waiting room, with the recipient on standby and into a workplace. The homes thus partly lost their character as a backstage realm where one could avoid the gaze of others. This also led to a hybridization of the personal sphere, in the form of marginal scope for true privacy, necessitating strategies for protecting one's own space.
Applications
It is important both to acknowledge the intrusive nature of personal and intimate care, which results in extensive hybridization of the home and personal sphere and to recognize care recipients’ agency in the relationship that care establishes.
Introduction
Sweden, as a welfare state, has a long tradition of providing social care and support to its citizens in their own homes through formal home care, either through home care services (HCS) or disability services (DS). Most persons who receive formal home care need support with personal and intimate care (National Board of Health and Well-being (NBHW), 2020), that is, help with eating, showering, getting dressed, and personal hygiene. Earlier studies have depicted the intimate and personal care situation as sensitive and challenging for care recipients as well as care providers (Conder & Mirfin-Veitch, 2008; Kalman & Andersson, 2014; Kwan et al., 2019).
A previous study on formal home care showed how staff used a variety of communicative and relational strategies to get to know care recipients, their needs, and preferences and to build a good working relationship. The quality of the care relation was seen as key to managing situations in which the provision of personal and intimate care could be experienced as non-invasive, thus safeguarding integrity and self-determination (Andersson et al., 2022). However, little is known about the strategies care recipients use to manage and relate to such care. To shed light on care recipients’ perspectives, interviews were conducted with recipients of Swedish formal home care. The aim was to explore and analyze their experiences of managing personal and intimate care.
Swedish context of formal home care
In Sweden, the services provided by formal home care, HCS, and DS, respectively, are to be guided by principles such as autonomy, integrity, and self-determination. The provision of HCS is regulated by the Social Services Act (SFS 2001:453), henceforth referred to using the Swedish abbreviation SoL. SoL authorizes social services (e.g., municipal support including financial benefits, HCS, housing, addiction, and dependence treatment) for all citizens, that is, anyone who cannot meet their own needs or have them met in other ways. The aim of SoL is to ensure that all individuals have a reasonable standard of living. HCS offers support through targeted interventions, for example, receiving support with personal hygiene and getting dressed, meals, or medication. In between these HCS visits, the care recipient is on her own. Because HCS's interventions are scheduled based on organizational conditions, a recipient of HCS often encounters several different care workers (NBHW, 2020).
In addition to SoL, people with considerable disabilities have the right to DS according to the Act concerning Support and Service for Persons with Certain Functional Impairments (SFS 1993:387), henceforth referred to using the Swedish abbreviation LSS. Support based on LSS is more extensive in scope than SoL, as disability services are to promote equal living conditions and full participation in society and ensure a good standard of living. One of these services is personal assistance, which entails personalized support for persons with considerable and permanent disabilities if they are considered to need support with basic needs and are under 66 years of age when applying. Basic needs include personal hygiene, meals, dressing and undressing, communication with others, or other help that requires extensive knowledge about the person with functional impairment. Personal assistance builds on the right to have a personal assistant (PA) present several hours a day to provide support in everyday life. When LSS was introduced in 1994, the right to personal assistance was heavily influenced by the independent living ideology (Andersen et al., 2014; Askheim, 2008).
During recent decades, however, formal home care has experienced several rationalizations and austerity policies (e.g., Andersson & Kvist, 2015; Norberg, 2019). This has led to increased pressure on care workers and PAs as well as a general decrease in the level of support to care recipients. The result is a widened gap between policy and practice (Altermark & Nilsson, 2018; Andersson & Kvist, 2015), at the expense of care recipients’ ability to partake in society as citizens (Bylund, 2022).
Research overview and theoretical point of departure
Care recipients’ private homes create a setting for care provision that differs significantly from institutional settings such as hospitals, residential facilities, or nursing homes, where most of the previous research has been performed (e.g., Clark, 2009; Inoue et al., 2006; Wilson et al., 2009). The home is more than a physical space. It is a place of privacy that is fundamental to the experiences of everyday life, and a base for everyday routines (Goffman, 1959/1990; Scott, 2009), providing familiarity and comfort. Regarding in-home care, England and Dyck (2011) described the home as being actively co-constituted through negotiations of micro-practices in care recipients’ everyday lives.
In a study of intimate and personal care in formal home care, accounts of what this comprised revealed a broad range of perceptions and actions on the part of recipients as well as providers of care (Ahnlund et al., 2022). Apart from support with personal hygiene, the interviewees included intrusions into different modalities of care recipients’ personal spheres. These modalities were temporal, spatial, and relational. The experience of intrusion was mitigated when care workers were on-time, meaning that the timing of care work was both satisfactory in relation to care recipients’ needs and on schedule. The importance of timing became especially evident when intrusions were made off-time, in relation to both the schedule and entrance to different parts of the physical home, as demarcated by exterior and interior thresholds (Ahnlund et al., 2022; cf. England & Dyck, 2011, pp. 211, 217). The relational aspects of care were further highlighted in how care staff related to the home as a private space and arena for the individual's ongoing everyday life.
However, care recipients’ private sphere was not confined to the home. The experience of intrusion was also heightened when support needs were exposed in public and at social events, as it challenged one's self-presentation and the possibility to maintain dignity. The way in which support is performed and how the care provider relates to the situational and relational context at hand determine whether the support truly facilitates participation in the event (Ahnlund et al., 2022; cf. Scott, 2009). This can be read in light of Goffman's theoretical work on “self-presentations” and “impression management” (1959/1990, 1967/2005), which describes interaction rituals occurring in “encounters between social actors” working to “establish a common definition of the situation” (Scott, 2009, p. 26). Goffman (1959/1990, pp. 97–101) stressed the difference between being/acting frontstage, in the gaze of others, and backstage, in privacy “behind the curtains.”
An often-overlooked aspect of the support provided by a PA concerns the periods of standby, the periods in between when the PA is present and available to provide support if/when needs arise (Egard, 2018). Standby represents a passive state for the PA, however, not a proper rest as the person is ready to act (Egard, 2018, p. 75), which in turn is a prerequisite for a functioning everyday life for many care recipients.
Another kind of public exposure surfaces when one is applying for service from the welfare system and an assessment, or reassessment, of needs is performed. In these situations, one is expected to prove that one is both “worthy” of support and fulfills the stated criteria. The challenge of having to present oneself as needing support with tasks that most persons want to manage on their own has been well-documented (e.g., Hultman et al., 2017; Järkestig Berggren et al., 2021).
Interactional care practices are framed and shaped by organizational norms and rules, which entail the risk that the recipient's life may take on some institutional characteristics, for example, that inflexible organizational routines and practices will constrain the individual's ability to have real influence in everyday life (cf. Harnett, 2010).
In a study of recipients’ views on the quality of care and care satisfaction in Swedish HCS, all but one respondent described (re-)occurring problems and their strategies for dealing with them—despite their overall expressed satisfaction (Westerberg et al., 2017). In most cases, the problems were attributed to work conditions, work organization, and a lack of other resources in the eldercare organization. Among these care recipients, the two most common strategies were trivialization, that is, downplaying problems and/or their own needs, and adaptation. A third strategy, which was used least often, was to express dissatisfaction. The authors concluded that what in reality is being assessed in care quality assessments may reflect care recipients’ understanding of work conditions and organizational issues rather than the quality of care (Westerberg et al., 2017).
Kittay (2019) argued for the importance of recognizing the agency inherent in being a care recipient, stressing that “to be receptive to care can itself be an affective affirmation of a willingness to be helped and to embrace the relationship that care establishes.” She labeled this “the completion of care” (Kittay, 2019, p. 186).
Methods and materials
As part of a larger study exploring intimate and personal care in formal home care, the present study is based on semi-structured iterated (1–2) individual interviews with care recipients in formal home care, that is, receiving personal assistance or HCS. The interviews were conducted in 2019 and 2020, most of them as personal meetings; however, due to the spread of the coronavirus, the later interviews were conducted face to face via video-link or by phone. In the recruitment process, it was explicitly stated that we hoped to achieve breadth and variation in the number of years receiving services as well as in participants’ gender, ethnicity, and age.
The recruitment process included going through directors of formal home care in two larger cities in Sweden. When consent was given by the directors, staff were informed and asked to distribute information letters to care recipients. To safeguard confidentiality, staff were asked to distribute information letters only to clients who they believed could participate in interviews on their own. To ensure voluntary participation and anonymity, a prepaid envelope was attached to the consent form. The recruitment process was also supported by a respondent, who handed out information letters in his/her wide network.
Three of the authors conducted a total of 25 interviews with 13 individuals: seven recipients (six women, one man) of home care services (RCWs) and six persons (three women, three men) receiving support from personal assistants (RPAs). The age interval among recipients varied (RCWs: 39–92; RPAs: 40–66). All interviews except four were recorded (mean duration 44 min, range 12–94 min) (Table 1).
A brief description of the interviewee.
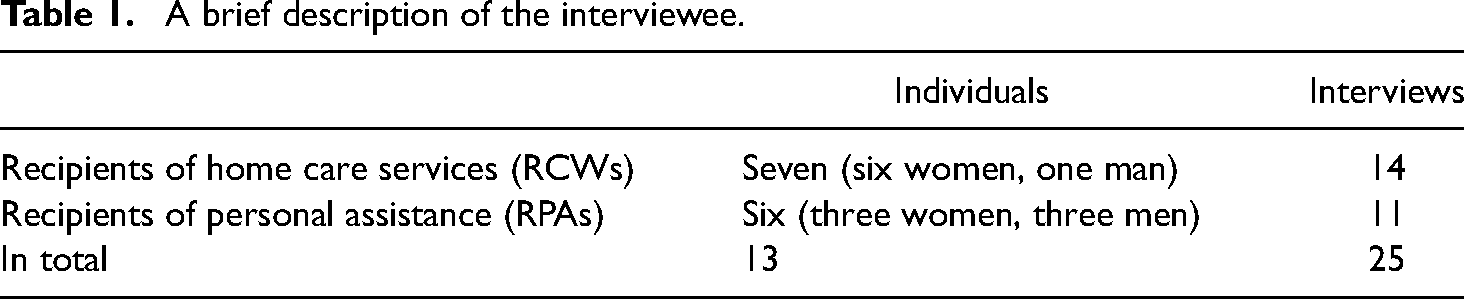
Informed consent was obtained in writing and then repeated orally at each interview. To ensure confidentiality, all personal data are stored in a safety vault, following the rules at Umeå University. The interviewees have been given pseudonyms in the transcripts.
Analysis
With a commitment to understanding the participants’ perspectives, ample space was given to their own reflections on their agential experiences. Though the interviews were semi-structured, they were also dialogical in nature. During and in connection with the interviews, fieldnotes were taken. The transcribed interviews were read through by all four researchers separately and then discussed, along with the fieldnotes, within the group of researchers. Our analysis was partly inductive and partly guided by earlier theorizing and phenomenologically informed research (cf. Goffman, 1959/1990, 1967/2005; Scott, 2009; Smith et al., 2009; Thornquist, 2021). The modalities of their experiences were interpreted in light of their respective contexts and their positions in care relations. In iterative rounds of readings, critical, typical, or otherwise qualitatively salient situations were highlighted. Anonymized quotes that illuminate such experiences have been chosen. To ensure that the authentic meaning of the verbatim quotes was captured, the translation of the quotes was thoroughly discussed.
Results
Formal home care gives care recipients opportunities to live a life that would otherwise not be available. However, there is also a challenging journey associated with becoming and adjusting to being a care recipient. Adapting to the organizational and relational conditions of being a care recipient included a far-reaching agency in handling one's role in the care relation. The respondents’ homes, which are the primary location of support, were shown to take on a hybrid character, in that care interventions change the privacy of backstage to frontstage. In addition, this hybridization does not only concern the home as a space but also the spatial and temporal dimensions of a lived personal sphere—at home, at work, and in public.
Adjusting and attuning to being a care recipient
Most of the interviewees had a long experience of receiving personal and intimate care, whereas for some it was more temporary, following, for example, a hip fracture. Those who needed temporary care were satisfied with receiving HCS while rehabilitating from a disease or accident, but they also described relief when considering a future when they would no longer need HCS. They had all adjusted to receiving care in their homes, which sometimes included having their preconceived notions challenged: It's worked really well! […] It was so interesting because there were girls from different countries and talking to them has always been interesting. It was Chile and Nigeria, and all sorts, about four of them. I got used to them, and I’ve read in the papers that there is a huge staff turnover, but that hasn’t been the case with the help that I received. (RCW4, Martha)
However, for interviewees receiving personal and intimate care more permanently, it was shown to involve some conscious choices about how to deal with the long-term situation of being a care recipient.
“It was hard in the beginning”: a career as care recipient
Speaking at various lengths and with different emphases, several interviewees described their “journey” to becoming a person who receives intimate care. For some, this journey had begun quite abruptly, for example, following a brain injury, whereas others were faced with a gradual albeit steady decline in abilities due to disease progression. This journey might be seen as a kind of career in managing the loss of independence and the at times increasing need for personal and intimate care. Several resolutely summarized their learning experience of becoming a care recipient, describing it both as a challenge and as “a fact of life” that also involves a conscious decision to try to not dwell on one's more independent days.
For Margret, it has often been very hard to accept her need for intimate care, especially when receiving support from her closest family: If it was embarrassing for me, it was just as embarrassing for them. […] No, at times [the close family] fared poorly. […] I once said: ‘I don’t want to have to go through these kinds of situations.’ […] We had crossed a boundary, somehow. […] There are limits, there are things one should be spared. (8 sec silence) Much to my regret, the two people who are closest to me had to go through this. (RPA2 Margret)
Sandra described some of the challenges she experienced while adjusting to the thought of becoming a recipient of formal home care. This included having to acknowledge, describe, and expose her vulnerable and most dependent side, the side that was experienced as being least related to herself and her agency. To deal with everyday life and work, Sandra eventually realized she had to go through the emotional labor of applying for HCS: It was a bit tricky […] to apply for home care services because then you have to turn your life upside-down […] bring out the difficulties […] When I was younger I got to a point where I didn’t want to take part in the procedure of applying for support. […] but with time I also realized that I have to do this in order to get the support I need, so I can live the life I want to live. I’m thinking that I have home care services because it will make my everyday life easier, so [I ask myself] ‘what do I need to do to make that possible?’, sort of. (RCW7 Sandra)
Using similar words, most of the interviewees described the effort it had taken to accept their need for support with personal and intimate care. Once the effort of acknowledging one's needs for support has been dealt with, and the right to support has been approved by the municipality, a new part of the journey takes place where one needs to repeatedly describe and explain one's vulnerable and dependent side every time a new care worker or PA arrives.
To make his support truly function, Robert needs to regularly instruct and educate new PAs even in the smallest details, for example, what is an appropriate bite size for him to chew—and consider what is an appropriate size in relation to different kinds of food. When discussing the precariousness of having progressive neurological disease, the need for increasing and comprehensive support, and having to reveal his life and impairments in full detail in his ongoing efforts to make support function adequately, Robert shrugged his shoulders and said: “I don’t allow myself to think about it, it only makes things harder […] If I put energy into that, then everything would go to hell” (RPA3 Robert).
Another journey was presented by Anne, who had HCS but whose need for comprehensive support qualified her for receiving support from a PA. With HCS, she encountered (too) many different care workers, as these interventions are scheduled and based on organizational conditions (cf. NBHW, 2020). For Anne, the irregularity in who would come and when led to a considerable lack of consistency and a heightened feeling of being exposed and vulnerable: For a while, I felt like: ‘Is it half the people in town who’ve been helping me in my apartment?’ That's how it was with home care services. As if everybody had been here, at my place. That's not nice, because then you start feeling bad about it. (RPA6 Anne)
She described how she values her independence and has a need for solitude and therefore had been reluctant to apply for personal assistance, as that would mean having a person present several hours a day. After the process of getting approval for personal assistance, which takes quite some time (Hultman et al., 2017), the next challenge was to truly absorb the fact that she was allowed to choose how she wanted to live and make use of her support. This meant taking command of her days and weeks in new ways compared to when she was dependent on HCS arriving at certain predefined points in time: [With HCS] You have to go to the loo at a certain time, otherwise, it doesn’t work. To try to pee as a matter of routine – it's almost like everything in your body shuts down and gets locked. And when buying food, you were expected to be quick about it. Then they don’t want to run over time because it will affect the next person. It was so stressful; I was so stressed! The job was stressful, my whole life was like a timetable. All I thought was ‘Oh, this is so tough.’ It took me a long time [with personal assistance] to realize that I could buy groceries when I wanted to. (RPA6 Anne)
Anne further explains that, for those receiving personal assistance, it takes some adjustment to realize that they actually are at the helm and do not need to give in to an assistant's more or less subtle attempts to take over: For example, if a person wants to go out for a walk even though it's windy or raining, some assistants might try to cancel that walk, asking questions like: ‘Do you really want to go out in this weather?’ etc. Then this person must be clear and explicit about what she wants – that it's just a matter of getting dressed for the outdoors. (RPA6 Anne)
Having been dependent on the restraining organizational conditions imposed by HCS, Anne reflects on how she previously had adjusted to not being in control of her day and now, with personal assistance, has gradually explored her ability to insist on self-determination.
Attuning to organizational conditions
For those receiving HCS, attuning to organizational conditions included the experience of having to be in a state of readiness for quite some time, while waiting for the care workers to arrive. Because the care workers’ working schedules could change from day to day, when new care recipients were added or unexpected things happened, they could arrive early, on time or late. The RCWs explained the late arrival of the HCS with reference to the care workers’ work conditions (cf. Westerberg et al., 2017). For some, waiting for support, a seemingly passive state, meant being on standby, a stressful state of readiness, such as when Martha waited for help with showering: “I was always prepared” (RCW4 Martha).
There was further a duality in the “ready-and-prepared” waiting mode—the dull and tiresome side of it, on the one hand, and the professed agency of being someone who can deal with it, on the other: That's what's so annoying about HCS, the times! One day they might arrive at eight, the next at nine, and then the very next at ten. I don’t care so much, but for the other elderly… Those with insulin and such. That's why they arrive [at such different times] because to me it doesn’t matter when they arrive, and I’ve told them so. (RCW2 Christine)
As we can see, Christine expressed her agency by showing solidarity with the other RCWs’ more extensive or medical needs as well as with the burdened staff. Like several other interviewees, she considered herself to be “lucky” in comparison with other care recipients, as she could speak for herself and to some extent negotiate the conditions of care. However, Christine's agency also represents another form of adapting to organizational conditions: first to put up resistance then surrender and adapt to the situation at hand. She would like to see standards applied but knows they will not always be met: I think that it's best if [not more than] two or three persons are involved in my shower schedule. Of course, if the other care recipients are in a really bad way and need help using the toilet, then they [the care workers] can’t keep it at that. But regarding showering, I do think they ought to try. (RCW2 Christine)
Ruth (RCW1), who described herself as a “night owl” who enjoys staying up late, had tried to arrange for the HCS to visit her as late as possible. Still, her narrative revealed compliance by adapting her activities to the organizational conditions, for example, going to bed before 8 p.m. Another example of adaptation, and surrender, was how Ethel (who has a PA during the day and support from HCS at night) at first told the care manager that she did not want male care workers (RPA1 Ethel). However, she later retracted her statement because “you get used to it if they know the routine.” If a male care worker from the night shift arrives, she might still ask if the other care worker is a woman and if the woman could help her instead. If this is not the case, “then it is what it is” (RPA1 Ethel).
Lilian, however, gave two examples of her putting up resistance, without surrendering to the crossing of what she felt were clearly expressed boundaries: I get help showering twice a week, and I have told them that no man gets to help me with showering. Once they sent a man, but I threw him out. […] Not long ago I almost threw somebody out. She was unpleasant when she was about to help me shower. She stood there and told me this and that, but I want to do what I can, don’t I? And then she told me she couldn’t be here all day – then I got angry. I told her that ‘if this doesn’t suit you, the door is over there! (RCW3 Lilian)
Thus, adapting and surrendering might have limits if a person's resistance is strong enough.
Attuning to relational conditions
The interviewees described how they attune to relational conditions through preparation, for example, by finding out in advance which care worker will be arriving or whether there will be a new care worker. Not knowing who is coming can be particularly stressful, and Margret described how she had felt when she had HCS and needed to wait for help to get up and take a shower: Each morning I’d take a deep breath in bed: ‘Now, what will this day be like?’, I thought, ‘who's coming? Who will help me take a shower? Will it be someone with the right grip, or someone who's nervous and wary?’ [I have] wobbly legs and such, that makes for situations where I have to work hard. […] I’ve become an expert at reading people. You notice that kind of thing very quickly, whether this will be a good shower or not, that is, good within citation marks. (RPA2 Margret)
Helen described another way of being prepared when she knew a new care worker would come. At first, she would ask around, for example, ask other care workers if they thought the new one would be suitable for her—mainly to avoid having to “dismiss” the person the very first time they met. In a second step, she would interview the person to get a sense of him/her: “If I don’t get along with people, I can’t let them in” (RCW6 Helen). She, like several other interviewees, talked about “personal chemistry,” that is, a sense of a “natural” connection, and an almost immediate sense of being comfortable with each other. However, the expression also includes aspects of adapting to the other person.
Several of the interviewees described themselves as being able to handle the care and adapt to a variety of caregivers. This entailed being flexible regarding the relational conditions of receiving care, making efforts and using their skills when relating to the care workers or PA, and as Margret related, adapting to the situation: But I know that I’m quite good at adjusting […] if need be, I can fix it. […] I need to handle my assistants every day and to do that you need some sensitivity and some active interest. (RPA2 Margret) Well, at times it feels like you’re about to burst – you know when it feels tough to get support from that person. Then you try to analyse yourself: ‘Is it really as bad as that, or is there something else that makes me lose my composure?’ (RPA5 Edward)
Owning a space of one's own
With formal home care, the care recipients’ homes took on a “hybrid” character (cf. Ahnlund et al., 2022), manifested in different adaptations for care workers and PAs. The care work, along with the adaptations, results in transgressions of both the physical and personal space. To own a place and space of one's own becomes a challenge.
One's home as a site for care
The hybrid character of homes was manifested in different ways, for example, by having lists posted on the walls to guide the care workers and PAs in how and when to do certain tasks. Even though Ethel (RPA1) and her assistant “M” have their common routines, M has also posted a written timetable on the wall to help potential substitutes see when insulin needs to be administered and what tasks the staff must assume responsibility for. Other adaptations might be to accept a portable toilet next to one's bed at night or to change the living room into a bedroom.
A deliberate adaptation of one's home to meet the needs of different PAs was another kind of hybridization, chosen by some care recipients. This was done to establish good working conditions for, and relations with, those working in one's home. There might be an assigned chair in the kitchen and/or living room, places for storage of the PA's clothes or food for the day, or similar customizations. Such choices were common among RPAs, although seldom as explicit as in the excerpt below: [the interviewer has made a remark on an infrared heating device in the living room] I have an assistant who is sensitive to cold, therefore we [also] have maximum heat in the car […] And on the other side, I have a fan for the assistant who sweats as soon as the temperature goes above 0 °C (a short laugh). (RPA4 Peter)
Another kind of hybrid character is illustrated by a narrative describing the inconvenience created when one of the PAs used personal protective equipment, for example, latex gloves, throughout his/her hours at Anne's home (note—this was pre-COVID19): Then there was somebody who wore gloves from the moment she entered until she left. […] You know the kind…Latex! That felt a bit… ‘Do you think it's as dirty as that at my place?’ (RPA6 Anne)
The practice of wearing gloves throughout the work shift created a demeaning depiction of Anne and her home, which is an extension of herself, as being filthy. This hurt her.
Owning one's space also means having one's home respected as a living space, where the person who lives there has the right to decide how it is decorated and equipped—something most persons would consider self-evident. Sandra, however, reported that gaining the respect of the care workers in her home has been quite a struggle: Then I’ve had the feeling that they forget about me. Maybe someone enters the apartment, not really thinking that this is the place where I live, sort of. I've had a cohabitee for four years now, and that became a minor concern like: ‘oh, now there's another person’ – that they had to think about this as a home. That we have decided to have our stuff here and there. It makes me a bit upset at times when I feel that a person has not really been listening when I’ve told him/her how I want it to be. That knives are supposed to be there and so on – all the things that make it work in the long run, for them [as well]. (RCW7 Sandra)
As Sandra aptly pointed out, the way in which this home has been planned and equipped to be well-functioning is the result of the joint deliberation of the two people who live there.
Being backstage and/or frontstage
Having support with personal and intimate care entails having the boundaries of one's personal and private life transgressed. Especially the RPAs reflect on what strains they experience due to having a person present for extended periods of the day: Sitting at home is quite nice, but now there's always some person there, in your sitting room. So, you have to think about not expressing yourself too – you have to think before you speak. […] At night I have support on call. Then they go home to sleep, and I can call them. You do feel you can breathe freely after they’ve left. You get to be on your own and just have peace and quiet. (RPA4 Peter)
Relaxing in one's private home means, in Goffman's terminology, to be backstage, relaxing one's public character and being “free” from the gaze of others (1959/1990). This contrasts with being frontstage, for example, having guests, which often includes feeling the need to be or make oneself and one's home presentable. Peter continued to describe his feeling about having a PA from morning to night: I like them to be themselves, even when working, and not have to feel that they’re… prepared and waiting for me to say something, to ask them to do something. Just take it easy and be in the situation as it is. The assistants do have an impact on someone else's living environment. […] Generally speaking, I think they should act as if they were at home. (RPA4 Peter)
The quotes illustrate another aspect of having “guests,” being frontstage, as the PA crosses a boundary that might be seen as both intimate and personal (cf. Ahnlund et al., 2022). Peter described yearning for the PA to be relaxed and not on edge, but at the same time prepared to give support when needed, on standby (cf. Egard, 2018).
Anne (RPA6) described how she has adjusted to having a PA present a large part of the day, despite her appreciation of being on her own. For her, lying awake in bed during the night represents her own secluded and appreciated space: “At night I don’t have help, and because I’m a night person that works well” (RPA6 Anne).
The strains for those in need of support at night, for example, with turning over in bed, meant never really being backstage, that is, not being able to have the nights as a space of one's own. Robert described being impatient with care workers who do not consider that he is asleep and wants to retain the silence and darkness of the night, who turn on the lights and greet him without lowering their voices: “Oh, but things like that can make you totally crazy!” (RPA3 Robert). He further described the feeling of losing his warm and secluded space and being exposed: And when there's someone new, and they rip off your quilt… that drives me crazy as well, because then you’re lying in a warm cosy bed and someone pulls the quilt, then you’re lying there completely sprawling. They can turn me over in bed anyway. (RPA3 Robert)
Protecting a space of one’s own: preserving integrity
Robert's example of having his nights interrupted also illustrates a far-reaching loss of one's personal and private sphere. A related disturbance might be when one is interrupted and brought out of one's “mind space” or working mode. Anne (RPA6) described her experience of having a PA who had an overly caring attitude, almost as if Anne were a child. When Anne was deeply involved in a working task, the assistant might suddenly turn up at her side and in a hushed voice ask her whether she needed to go to the toilet. Anne would politely explain: “You don’t need to ask me; I’ll tell you when I need to.” An occasion when Anne almost “went crazy” was in a meeting at her workplace, when the same assistant leaned over her shoulder and asked: “Is it good for you now, does it feel good?” (Anne RPA6). Anne concluded that even though she has PAs taking part in her everyday life, frontstage as well as backstage, this is not a matter of them interacting with her all the time.
Having support in public places meant a demanding frontstage setting. Such situations strain one's ability to maintain personal integrity, and some of the RPAs reflected on how receiving support with meals in public is especially sensitive: I’d rather not go to a restaurant with a new assistant, whereas I know when I have M [a personal assistant] it will be much better, no spilling on my shirt […] He or she [the PA] is supposed to be somebody who works well in the context, not like a fly on the wall, I want someone who takes part in the conversation. […] That's important. My friends won’t have a very good time if there's someone who is completely out of place, and whom they notice does a poor job feeding me. They shouldn’t have to think about that, because I have an assistant: ‘How can we help NN?’. That's not the way it's supposed to be. (RPA3 Robert)
This challenge at social events can be read in light of Goffman's theoretical work on the presentation of the self (1959/1990). For Robert, like for many others, it is important that the assistant functions as a smooth team member who adapts to the different conditions of his personal life; this improves his social ability and preserves his dignity even in a frontstage setting (cf. Goffman, 1959/1990, pp. 77–78). Support that is not appropriate or that functions poorly affects and might disrupt the social event. A smooth reflective dialogue among friends [relatives, colleagues] might tolerate a disruption or two, but if the support becomes a constant worry among the other participants, it will undermine the social aspects of the event for all participants, including the recipient of support (cf. Scott, 2009, pp. 101–111).
Discussion
The present study has explored and analyzed care recipients’ experiences of managing personal and intimate care in Swedish formal home care. Our analysis revealed a deliberate and reflected approach to the complex challenges associated with becoming and being a recipient of personal and intimate care. Besides having to accept the need for support with things most people want to do by themselves in private, this meant continuous adaptation and attuning to the organizational and relational conditions of formal home care.
Applying for support, revealing one's needs and personal preferences, and explaining private parts of one's life are often experienced as vulnerable and humiliating situations (cf. Bylund, 2022; Hultman et al., 2017). Further, being a care recipient entails a continuous negotiation with oneself, reflecting on one's own needs and current health/disability situation and accepting that one is a person in need of support within the limited organizational framework afforded by the social welfare system (cf. Norberg, 2019).
As with the relational work performed by care workers and PAs (cf. Andersson et al., 2022; Guldvik et al., 2014), the care recipients also deliberated on their own relational work in this respect. Relational work concerns one's role in the family, at work, in one's social network and in relation to the different care workers and PAs who support one's everyday needs. Recipients of formal home care put a great deal of effort into the care relation by being socially responsive and stepping into the role of being a “fairly reasonable” care recipient when responding to the care workers’ and PAs’ differences, expectations, and organizational conditions (cf. England & Dyck, 2011; see also Scott, 2009). Their agency as care recipients also included strategies for putting up resistance to the shortcomings of organizational conditions and/or non-responsive care workers. However, this often resulted in situations in which one nevertheless chose to “surrender and adapt” (cf. Andersson & Kvist, 2015; Harnett, 2010).
Being a recipient of personal and intimate care does not mean being passive, but actively relating to and sustaining the care relation, where even choosing to accept suboptimal conditions constitutes an act of agency. For example, choosing an agential position in relation to the working conditions of care workers and PAs as well as other care recipients’ needs, and disregarding their own inconveniences, can be seen as an act of solidarity (cf. Westerberg et al., 2017). This also serves as a presentation of oneself as a flexible and capable person (cf. Goffman, 1959/1990).
The hybridization of the care recipients’ homes was apparent and partly out of their control. Different parts of the home's character as frontstage (kitchen, living room) or backstage (bedroom, bathroom) changed with care interventions, even with the mere arrival of the care worker/PA (cf. Ahnlund et al., 2022). The “normal” spatial order of frontstage and backstage in the home (Scott, 2009) transforms, where backstage might become semi-frontstage and a form of public area, as described by the woman who felt as if everybody had been at her place, supporting her with personal and intimate care.
The hybridization also includes a lived personal sphere that has both spatial and temporal dimensions. The temporal dimension of the hybridization became apparent, for example, when care workers arrive unexpectedly, off-time, due to unexpected changes in their workload. This has radical effects on care recipients’ daily life and affects the private/public character of their homes. For recipients of HCS, temporal hybridization might concern waiting for the care worker to appear, being on standby and prepared, where the home transforms toward being a waiting room for care to be carried out in before one can begin other activities. For recipients of personal assistance, the hybridization entails having a PA in a standby position and managing the gaze and presence of the assistant when relaxing backstage or immersing oneself in one's own thoughts.
The private homes of care recipients thus partly lose their character of being a backstage realm where one can relax from the gaze of others (cf. Goffman, 1959/1990), which leads to a marginal room for true privacy in time and space. Support in public represents a demanding frontstage setting, which challenges possibilities to maintain one's personal integrity and preserve dignity. Strategies to protect the personal and private sphere become a necessity.
Limitations of the study
We strived to recruit interviewees who could participate on their own, our goal being to ensure confidentiality. But this also meant that we interviewed persons who describe themselves as being lucky—lucky because they can speak for themselves. Our findings can still be regarded as representative of a larger group of care recipients, as our informants have articulated important reflections on the experience of being in the position of a care recipient.
Conclusions
It is important for social welfare services, in education and in-house training, to acknowledge the intrusive nature of personal and intimate care, which results in extensive hybridization of the home and personal sphere. It is also crucial to recognize the agency inherent in being a care recipient—having an active role in the relationship that care establishes.
Footnotes
Ethics
Ethical approval for this project was given by the Regional Ethical Review Board in Umeå (Reg. No. 2018/363-31).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the Kamprad Family Foundation for Entrepreneurship, Research & Charity (grant number 20180140).
Author contributions
All authors contributed to developing the interview guide. VL, HK, and KA conducted the interviews. PA coded the texts. All authors reviewed coding for major themes. VL and HK conducted the in-depth analysis of coded materials and wrote the manuscript with input by PA and KA. HK led the overall study.
Acknowledgements
We thank all the interviewees for sharing their experiences and valuable perspectives with our team of researchers.
