Abstract
Introduction
Telemedicine services saw substantial surges in their use during the COVID-19 pandemic due to the lockdowns and characteristics of the pandemic. Therefore, the authors aimed to systematically review the telemedicine services provided during the COVID-19 pandemic and their potential applications.
Methods
The authors searched PubMed, Scopus, and Cochrane databases on September 14, 2021. Then, the retrieved records underwent two-step title/abstract and full-text screening processes, and the eligible articles were included for qualitative synthesis.
Results
The review of studies demonstrated that the telephone is listed 38 times, making it the most common technology used in telemedicine. Video conferencing is also mentioned in 29 articles, as well as other technologies: Mobile-health (n = 15), Virtual reality (n = 7). According to the findings of the present study, Tele-follow-up (n = 24), Tele-consulting (n = 20), Virtual visits (20), and Tele-monitoring (n = 18) were the most widely used telemedicine applications.
Conclusion
Telemedicine has been an effective approach to COVID-19 management. Telemedicine technology is going to play a key role in the future of health medicine, patient consultation, and many other extended applications of health care in remote rural locations.
Introduction
On March 2020, the World Health Organization (WHO), after the large expansion of SARS-CoV-2 infection, declared the coronavirus disease 2019 (COVID-19) outbreak as a public health emergency. 1 The extension rate of COVID-19 and its characteristics have highlighted the need for quick solutions. 2 To mitigate infection risk and the spread of the virus, various public health policies have been implemented, including the use of face coverings, social distancing mandates, closure of nonessential businesses and quarantine strategies.3–5 The healthcare systems also changed the way healthcare services were delivered to comply with these policies and prioritized social distancing as a substantial factor in slowing the spread of viruses.6–9 The healthcare systems have been confronted with challenges not only in treating COVID-19-afflicted cases but also in managing patients with other acute and chronic diseases.5,10 Therefore, the COVID-19 pandemic has significantly impacted the routine patient care workflow and health care resources.11,12 In this regard, health services have had to adapt and prioritize the safe delivery of care, limiting outpatient care. 13
As a result, there is a clear need for effective and innovative tools to address the continuum of care for patients with COVID-19 and others in need healthcare of service. 14 Telemedicine has been considered an ideal tool to manage these emergency and rapid regulatory changes. 15 Out of necessity, telemedicine and e-health platforms have been suggested as a main strategy for continuous patient care while mitigating the spread of viruses and conserving valuable healthcare resources.10,16
There are various definitions of telemedicine. The formal definition of telemedicine according to the WHO is the “delivery of healthcare services, where distance is a critical factor, by all healthcare professionals using information and communication technologies for the exchange of valid information for the diagnosis, treatment, and prevention of disease and injuries, research and evaluation, and for continuing education of health care providers (HCPs), all in the interest of advancing the health of individuals and their communities. 3 ”
During the COVID-19 pandemic era, telemedicine has become a key component in patient healthcare delivery. 5 The use of telemedicine technology brings essential benefits to improve access to quality and timely care while maintaining physical distancing, preventing disease, home COVID-19 screening and monitoring in epidemic conditions.17–19 Telemedicine offers great potential to provide services without the need for face-to-face contact and avoid exposure to respiratory secretions. 10 Telemedicine allows healthcare providers to focus more resources on pandemic usage and at the same time, continue caring for patients with chronic diseases who need follow-up and clinical intervention. 20 The use of telemedicine during the COVID-19 pandemic will help to decrease the time required to get a diagnosis and initiate treatment, quarantine or follow-up a patient.21,22 This technology uses electronic communication tools such as smartphones application or videoconferences. It allows clinicians to evaluate rapidly and detect patients with early signs of COVID-19 before they arrive at the emergency department. 21 Telemedicine is the best approach to avoid the inundation of hospitals with COVID-19 patients. 20 Through video calls, they determine which patients are at high risk and require an urgent referral and avoid overloading the healthcare system. 12
On the other hand, the benefits of using telemedicine technologies in epidemics allow helping patients with chronic diseases that are not infected with COVID-19 to receive medical attention without the risk of exposure to other patients in the hospital.16,7 Likewise, telemedicine technologies allow rapid consultation among specialists for medical decision-making in the face of COVID-19.12,23 This is an important achievement for rural areas. 12
Although the various applications and advantages of telemedicine hold promise for managing pandemic response, its adoption has limitations such as technological infrastructure, provider and patient education, quality of healthcare services, equipment costs, the privacy of sensitive patient data, legal issues and low motivation of providers.24,25 Establishing clear rules and regulations by governments and health organizations can contribute to avoiding misused telemedicine. Improving telemedicine infrastructure will facilitate a higher quality of care to a larger scale of patients. Furthermore, ethical considerations must be taken into account.26,27
Telemedicine technologies are tools specializing in the e-health sector. The solutions developed and functioned by these technologies contribute to the development of the health care system, patient care or clinical and epidemiological study in a wide range of uses. Telemedicine technologies’ activity is at the convergence of various disciplines (software engineering, space technologies, big data and data science, medicine and clinical operations, etc.) in an international environment and a start-up spirit. 24 During the current pandemic, the development of telemedicine applications using above mentioned technologies, increased as the healthcare system sought ways to improve access to safe and affordable care. Telemedicine applications provide remote healthcare delivery with the help of telecommunications technology. 28 This systematic review aimed to summarize the status related to the use of telemedicine technologies and applications and provide an overview of how these tools are being used to face the current COVID-19 pandemic.
Methods
Research question
In this comprehensive review, we are going to determine the telemedicine technologies and applications during the COVID-19 era by going through the available resources. To ensure the validity and reliability of results, this study adhered to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist. Considering the important role of the result of systematic reviews, the use of standard methodology has an effective role in confirming the study results. One of the standard methodology tools is the PRISMA checklist.
The PRISMA statement provides updated reporting guidance for systematic reviews that reflects advances in methods to identify, select, appraise, and synthesis studies. We anticipate that the PRISMA statement will benefit authors, editors, and peer reviewers of systematic reviews, and different users of reviews, including guideline developers, policy makers, healthcare providers, patients, and other stakeholders.
The aim of this study was to investigate telemedicine technologies and applications during the COVID-19 era. In this research, we sought answers to the following questions: 1- What kind of telemedicine technologies are used during the COVID-19 pandemic? 2- What are the applications for providing remote services during the COVID-19? 3- What are the advantages, disadvantages and impact of these technologies on the healthcare services for COVID-19?
Information sources
The authors systematically searched three widely used academic online search sources, including PubMed, Scopus, and Cochrane. We searched the medical subject heading (MeSH) database and looked upon similar studies to generate the keywords for COVID-19 and telemedicine.
Search strategy
The search was based on two search themes (COVID-19 and telemedicine) using the Boolean operator “OR.” The searches were combined by using the Boolean term “AND.” Alternative names for telemedicine, identified through various literature sources, as well as details on searching each database were added (Supplementary material 1). Search strategy for PubMed is mentioned in as an example: A. [COVID-19] OR [SARS-CoV-2] OR [SARS-CoV2] OR [Novel coronavirus] OR [2019-nCoV] B. [Telemedicine] OR [Tele-health] OR [Tele-care] OR [Tele-monitoring,] OR [Tele-consulting] C. [A] and [B]
Selection process
After downloading identified studies, the duplicate records were removed. Two investigators followed a two-phase screening process to determine the eligible results. They were aware, vigilant, educated and had PhD degree and did not have any conflict of interest. They also have expertise in reviewing articles and manuscripts and were a member of Pueblo’s reviewer database. First, they examined the title and abstract of the retrieved records and the ineligible studies were removed. Then, their full texts were evaluated based on their cohesion to the aim and inclusion/exclusion criteria and the eligible studies were included for qualitative synthesis.
Eligibility criteria
The authors included the original articles related to the research question from the initiation of the pandemic (December 2019) until September 14, 2021. Therefore, the exclusion criteria are as follows: 1) Non-original studies, including reviews, commentaries, opinions, or any studies with no original data, 2) Pure laboratory or animal studies not conducted on humans, 3) Case reports, 4) Ongoing projects (e.g., articles discussing the protocol of a future study), 5) Abstracts or conference abstracts, or no available full text.
Data collection process
Five investigators read the full texts of the eligible articles and extracted the data from the relevant included studies. We collected the following data from each study: A) the first author and country; B) results of identified telemedicine technologies, service receivers (Who? Which patients or staff?), their applications to provide healthcare services for COVID-19, and other findings to construct the results section. All included studies were English language and across all countries. Another independent investigator reviewed the extracted data and solved discrepancies and issues between the other investigators.
Risk of bias assessment
The results of Newcastle-Ottawa scale (NOS) risk of bias assessment.
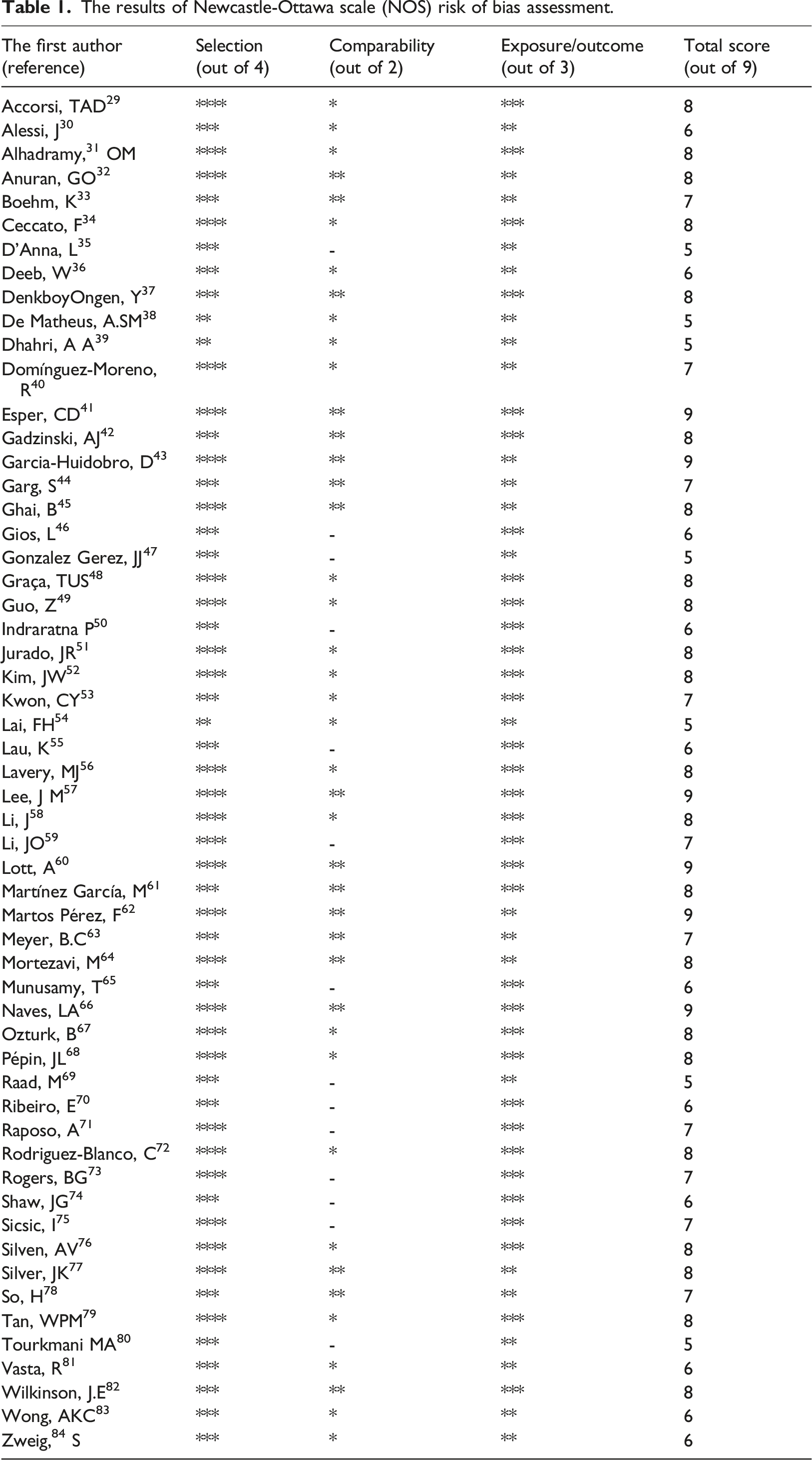
Informed consent
This article was a review one and we have not an informed consent.
Results
In this study, 2,053 documents were identified using a systematic search strategy. After an initial review of the retrieved articles, 1,459 duplicates were removed, and the titles and abstracts of the remaining sources were assessed. After applying the selection criteria, 538 articles were deleted in the two-phase screening process, and 56 articles met the inclusion criteria and were included in the final review (Figure 1). PRISMA flow diagram of the study’s selection process.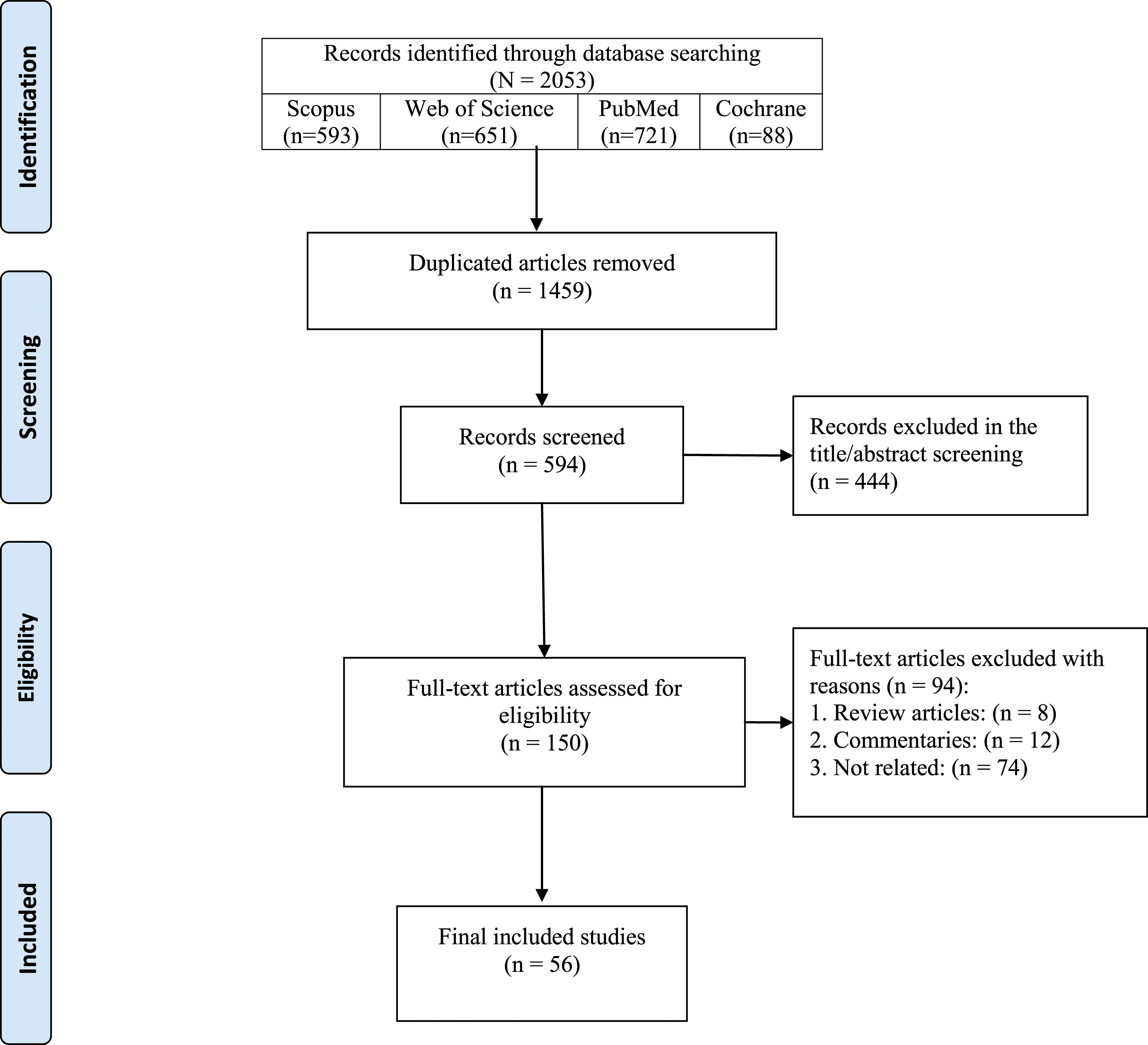
Identified telemedicine technologies and applications to provide healthcare services for COVID-19.
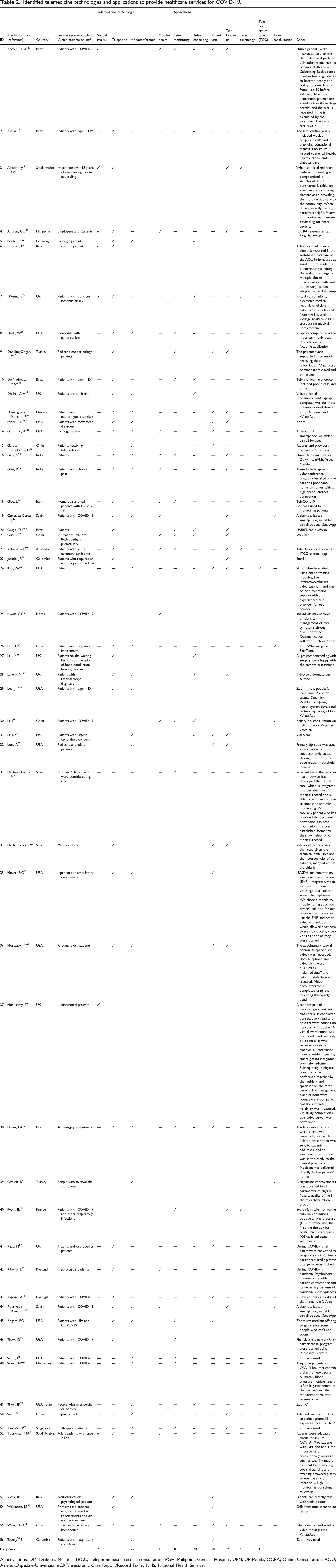
Abbreviations: DM: Diabetes Mellitus, TBCC; Telephone-based cardiac consultation, PGH; Philippine General Hospital, UPM; UP Manila, OCRA; Online Consultation, AOU; AziendaOspedale-Università, eCRF; electronic Case Report/Record Form, NHS; National Health Service.
Advantages, disadvantages, and impact identified technologies on the healthcare services for COVID-19.
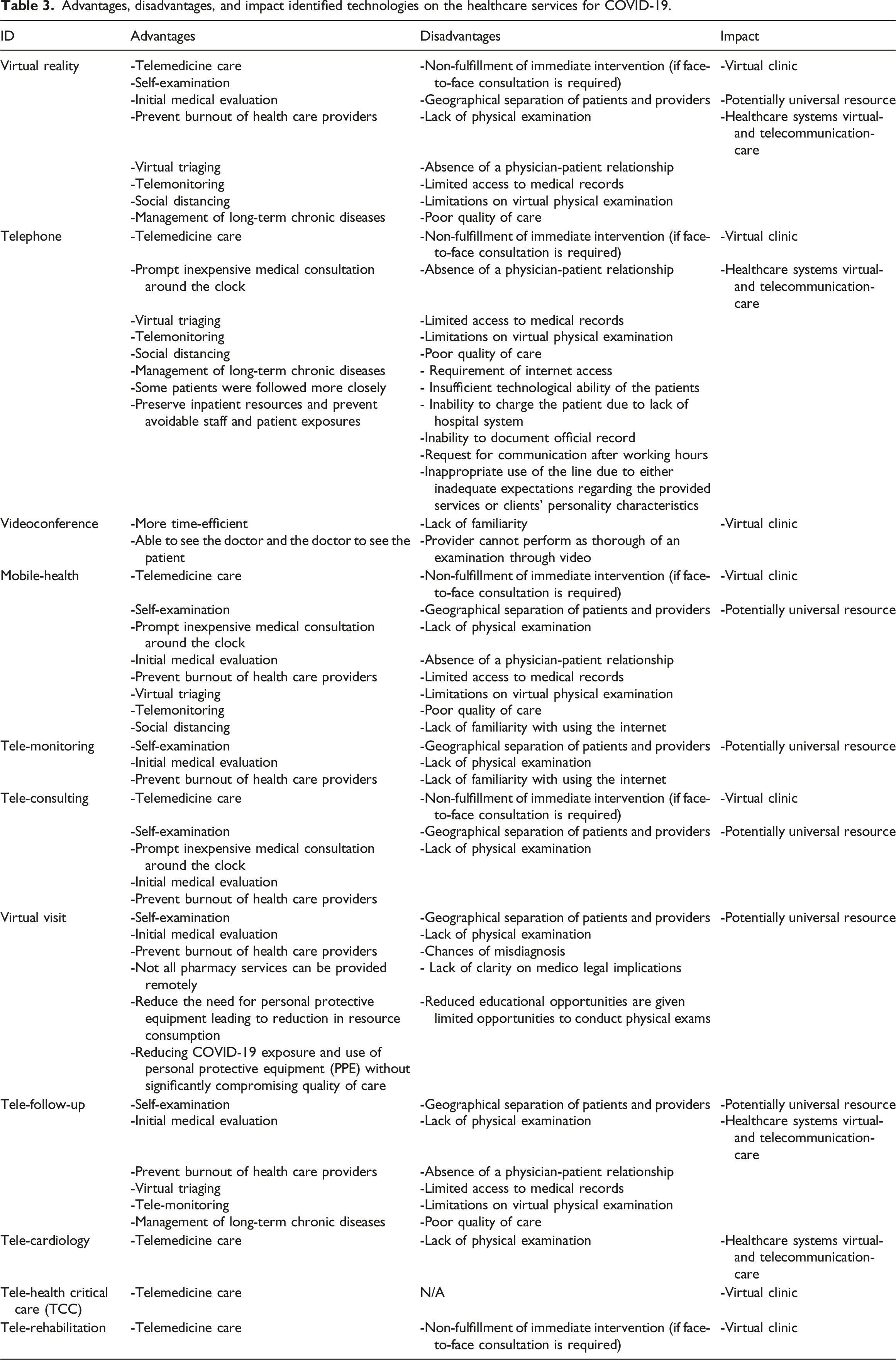
Telemedicine technologies, as well as the applications of these technologies, were reviewed. Studies in these articles have shown that the telephone is listed 38 times, making it the most common technology used in telemedicine. Video conferencing has also been mentioned in 29 articles (Figure 2). Percentage of studies that identified telemedicine technologies.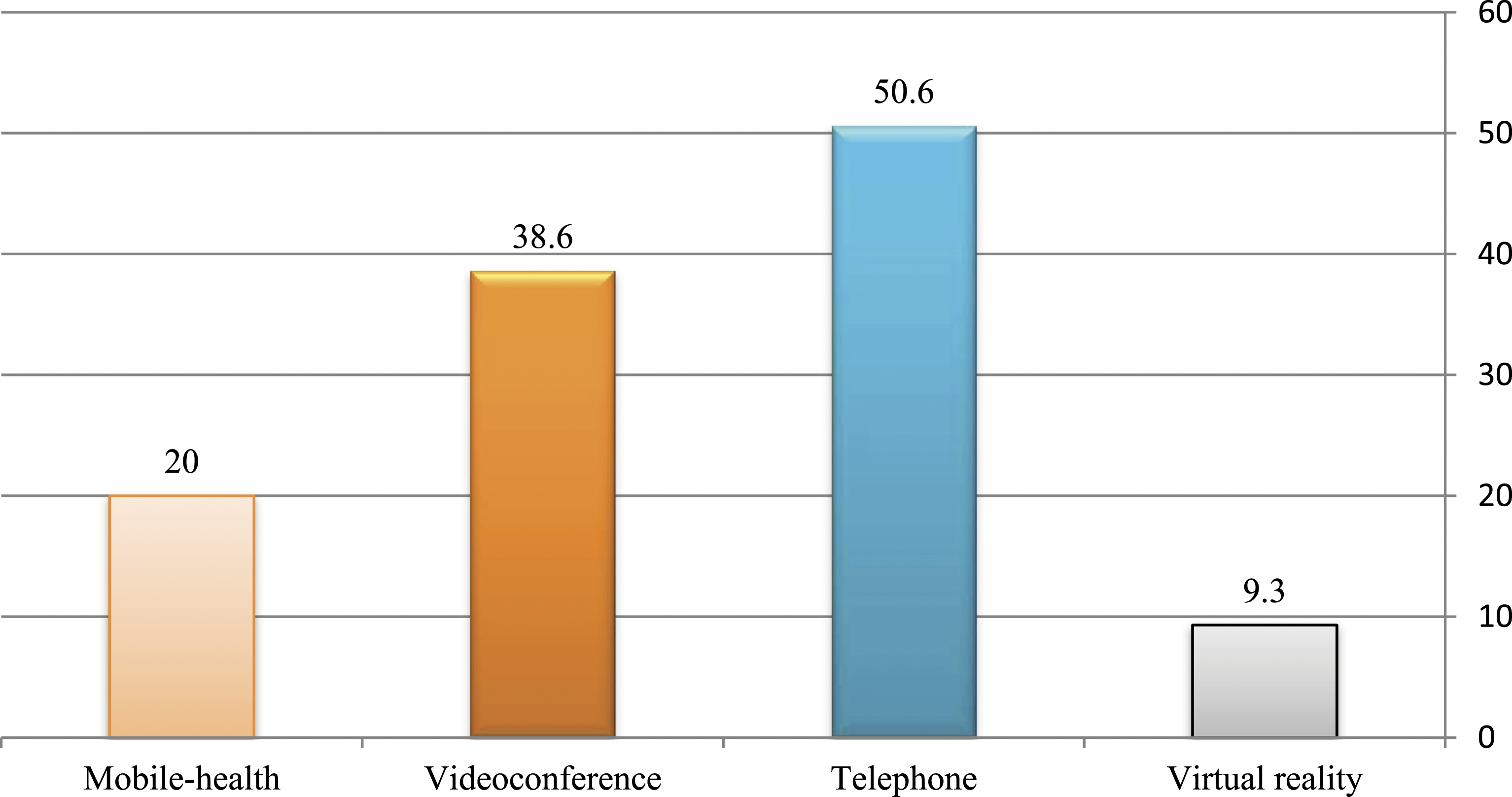
According to the findings of the present study, Tele-follow-up (n = 24), Tele-consulting (n = 20), Virtual visits (20), and Tele-monitoring (n = 18) were the most widely used telemedicine applications. The frequency of these applications is demonstrated in Figure 3. Percentage of studies that identified applications of telemedicine technologies.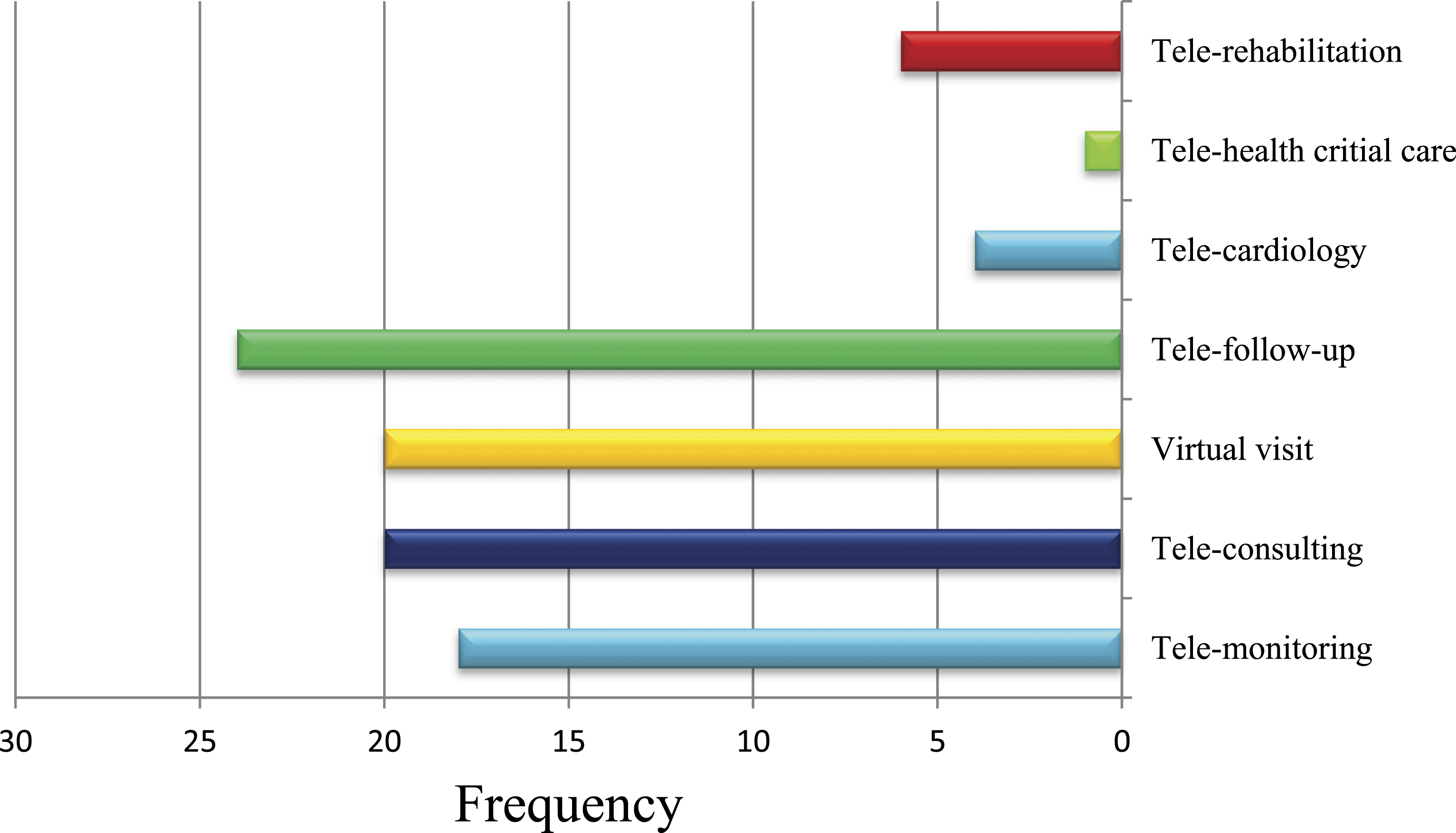
Most studies were related to the USA with 13, the UK with seven, Brazil with five, china with four, Spain with four and Italy with three articles. The rest of the selected articles were for countries Turkey, India, Colombia, and Portugal with two articles and the Philippines, Germany, Mexico, Chile, Korea, Australia, France, Singapore, and the Netherlands with one article.
Discussion
With the outbreak of the COVID-19 pandemic, the authors provide a comprehensive review of telemedicine and its applications and roles in the delivery of healthcare organizations. The present study, in which a total of 56 articles related to telemedicine solutions and applications are analyzed, indicates the application of telemedicine technology. This review has proved the high usage of telemedicine, especially during the COVID-19 pandemic, applications in Tele-follow-up, Tele-consulting, Virtual visits, as well as Tele-monitoring. Telephone, Video conferencing, Mobile-health and Virtual reality are the four main telemedicine technologies that are mentioned in the articles. The highest frequency of telemedicine services was through these four technologies. Also, since these technologies had been useful before accruing the COVID-19 pandemic, some of the articles suggested that the role and applications of these technologies will never diminish. Accordingly, this systematic review aimed to identify the telemedicine services provided and meaningful telemedicine applications through the COVID-19 pandemic.
Telemedicine technology holds great promise for patients during the pandemic duration. The most significant effect is provided to reduce potential exposure to SARS-CoV-2.85,86 Many people point out that telemedicine has existed in some way or another since the telephone was invented. 85 Telephone calls were the first method of connecting patients with HCPs at a distance, and it remains a crucial component of care in different situations. The telephone is now used in medical areas such as cardiology,35,50,87 dermatology, 56 mental health,36,54,78 rheumatology, 64 trauma and orthopedics, 69 neurologic disorders,40,81 urology,33,42 endocrine disorders34,39,57,65 to deliver improved treatment, follow up, consulting, monitoring and primary care to populations underserved by healthcare providers. It is often thought to be a way to reduce notably the expense of treating health problems such as diabetes type I and II, heart failure, and HIV which benefit from continuous observation of a patient’s condition38,50,73,80 Telephone calls deal with these problems in various areas, including performing cognitive or psychiatric assessments, consulting, drug therapies or social/lifestyle changes, primary care and remotely observing patients.50,54,82 The results of our study are consistent with the results of studies by Cervinoetla and Matthewson on the role of Telephone Triage before Attending Medical Office and telephone support service during the COVID-19 pandemic.88,89
Virtual Reality (VR) systems have modified communication in telemedicine devices, making them more immersive. In VR, physicians and their teams can now observe a 3D monitor when performing operations.87,90 The telehealth platform might use VR to simulate the patient’s data, and a graphical environment with video conferencing to streamline communication with a physician. 45 Specialists such as endocrinologists, cardiologists, infectious diseases, and neurosurgeons can answer electronically and educate about COVID-19, perform virtual examination and triage, virtual consulting, virtual monitoring and follow-up, and also patients can set up a virtual meeting with the physician.29,32,80 These virtual consultations can remove avoidable in-person referrals to specialists, reduce wait times for a specialist response, and avoid unnecessary travel.31,34 The results of our study are consistent with the results of a study by Ravi Pratap Singh et al., On the Significant applications of virtual reality for the COVID-19 pandemic. VR technology can reduce the face-to-face interaction of doctors with infected COVID-19 patients and avoid unnecessary travel. 91
Video conference technologies offer quick and simple methods of providing care remotely during the current pandemic. By employing video conferencing, physicians can educate groups of patients. Also, this enables medical teams to cooperate and hold video meetings on complex and urgent situations.64,73,75,76,84 Video conferencing was one of the most common technologies during the COVID-19 pandemic. Video conferencing is used in various situations, such as learning and videoconference and its role in teaching medical students and using this technology to maintain the education of residents, doctor-patient communication and communication between the medical team, Videoconference for clinical recommendations for treatment by the family of patients via providers during COVID‐19. In this regard, the results of the present study are in the same direction as previous studies such as Chick et al., and Matheson et al.92–94
Mobile-health let allows patients to count calories, record vital signs, record exercise, and control prescription doses and schedules, which are very useful and crucial for patient self-management and monitoring like hypertension, heart failure, diabetes and home-quarantined patients with COVID-19 during the pandemic. Mobile apps are also used for telehealth visits or electronic visits.44,46,50 Telemedicine application software companies utilize app connectivity and cloud technologies to grant real-time distant patient follow-up, monitoring, visiting and consulting. It saves time for both patients and physicians by monitoring health progress. 9 The telehealth apps and platforms ensure accurate patient record data. It helps pharmacies, customers, and prescribing physicians by delivering healthcare services more quickly.46,48,66 With an e-prescription feature, physicians can convey prescriptions with minor errors. It would help to save time while also improving linkage and customer satisfaction. 66 Thus Telemedicine via mobile health apps and tools, with the rise of digital devices and wearable and portable sensors, can help monitor and manage signs and symptoms. The results of the present study are consistent with Ming et al., and Lukas et al., studies on emerging telemedicine tools and the importance of health services through mobile apps.20,95
The wide variety of free software and platforms currently available, such as Zoom, WeChat, WhatsApp, Google Duo, WebEx, FaceTime, Redcap platform, Doxy.me platform, emails and also new software were introduced like e-CoVig, Microsoft Teams and TELEA tool; adequate lighting; good camera quality; and a good internet connection allow for the proper evaluation of patients.40,41,44,48,53,54,57,71,73–75,79,84 In current studies, Zoom was the most frequent application used mostly for Video-conference and virtual visits.36,40,41,43,54,53,57,71,73,77,79,84
As telemedicine is being used widely, preparing specific guidelines by worldwide institutions (e.g., WHO) might help HCPs and patients feel safe when using telemedicine. Moreover, developers should pay attention to data security and assure physicians and patients regarding their privacy. Despite the extent of the use of telemedicine, there are also opportunities to expand the area of applying this modern way of communication. For instance, providing specific platforms for each sub-specialty of medicine so that patients could communicate with their most appropriate healthcare provider as fast as they can. 96 Optimization of telemedicine could be summarized in the following domains: (1) safety: decreasing HCPs and patients’ exposure to infected cases and decreasing spread of COVID-19 for the so called “social distancing”; (2) effective: providing care not only for severely ill cases but also for all community with mild symptoms that require care to prevent delayed treatment and diagnosis, and even for decreasing stress and concern; (3) conservation: preventing waste of time, energy, and equipment; (4) timely: decreasing unwanted delays to prevent waste of time and energy of both HCPs and patients, also to decrease potential harms of delayed treatment; (5) patient-centered: to provide care based on patient’s needs and individual values; (6) balanced: same care quality for all individuals and avoid bias due to different socioeconomic status; (7) availability: infrastructures for delivering care and connectivity at both ends; (8) regulations: decreasing all restriction by governments also providing formal licenses for telemedicine implementation; (9) reporting: quality assurance mechanisms to report adverse events.21,96,97
Telemedicine, as a novel approach, is encountered various challenges. First, it is a primarily internet-based platform; thus, it would be difficult for people in developing countries to use telemedicine, as their internet access and quality are quite poor. Consequently, prioritizing expanding internet access worldwide to benefit from telemedicine should be considered. Physical examination is not applicable in telemedicine due to its virtual nature. Therefore, the quality of care in telemedicine is not the same as in-person care, especially for elderly patients that cannot use new technologies properly. Data privacy and security is another challenge due to the vulnerability of software platforms, which requires protective measures. Lack of regulations and legal obligations act as a barrier to limiting the extension of telemedicine Providers should prepare backgrounds of trust for patients, so that a wide range of people can turn to using telemedicine as their first choice when it comes to clinical issues. Specific benefits can be considered for physicians and HCPs to encourage them to utilize these platforms.
Conclusion
The current review discusses the telemedicine services provided and applications of available telemedicine technologies during the COVID-19 pandemic. The results indicate that telemedicine provides remote healthcare services and can help better control the disease. The study also determines the applications and frequency use of four main technologies used in the delivery services during the COVID-19 pandemic and their applications. As telemedicine technology further evolves with the expansion of the internet in rural areas, it will play a key role in the future of health medicine, patient consultation, and many other extended health care applications. The effectiveness of these telemedicine technologies as a critical topic can be investigated in upcoming research. Future research, particularly related to the implementation and compliance of telemedicine technologies during the non-emergency in delivering health services to support patients, will yield help.
Supplemental Material
Supplemental material - Telemedicine technologies and applications in the era of COVID-19 pandemic: A systematic review
Supplemental material for Telemedicine technologies and applications in the era of COVID-19 pandemic: A systematic review by Esmaeil Mehraeen, Seyed Ahmad Seyed Alinaghi, Mohammad Heydari, Amirali Karimi, Abdollah Mahdavi, Mehrnaz Mashoufi, Arezoo Sarmad, Peyman Mirghaderi, Ahmadreza Shamsabadi, Kowsar Qaderi, Pegah Mirzapour, Amirata Fakhfouri, Hadiseh Azadi Cheshmekabodi, Kimia Azad, Seyed Ali Bagheri Zargande, Shahram Oliaei, Parisa Yousefi Konjdar, Farzin Vahedi, Tayebeh Noori in Health Informatics Journal
Supplemental Material
Supplemental material - Telemedicine technologies and applications in the era of COVID-19 pandemic: A systematic review
Supplemental material for Telemedicine technologies and applications in the era of COVID-19 pandemic: A systematic review by Esmaeil Mehraeen, Seyed Ahmad Seyed Alinaghi, Mohammad Heydari, Amirali Karimi, Abdollah Mahdavi, Mehrnaz Mashoufi, Arezoo Sarmad, Peyman Mirghaderi, Ahmadreza Shamsabadi, Kowsar Qaderi, Pegah Mirzapour, Amirata Fakhfouri, Hadiseh Azadi Cheshmekabodi, Kimia Azad, Seyed Ali Bagheri Zargande, Shahram Oliaei, Parisa Yousefi Konjdar, Farzin Vahedi, Tayebeh Noori in Health Informatics Journal
Footnotes
Acknowledgements
The present study was extracted from the research project with research code IR-KH-1400-07-023 and ethics committee code IR.KHALUMS.REC.1400.007 entitled “A framework for implementing of telemedicine technology with COVID-19 pandemic approach in Emam Khomeini Hospital” conducted at Khalkhal University of Medical Sciences in 2020. We thank the statistical population and all the participants for taking the time to contribute to the study.
Author contributions
The conception and design of the study: Esmaeil Mehraeen and Tayebeh Noori. Methodology: Esmaeil Mehraeen, SeyedAhmad SeyedAlinaghi and Mohammad Heydari. Acquisition of data: Amirali Karimi, Esmaeil Mehraeen, Abdollah Mahdavi, Tayebeh Noori and Mehrnaz Mashoufi. Writing original draft preparation: Arezoo Sarmad, Peyman Mirghaderi, Ahmadreza Shamsabadi, Kowsar Qaderi, Pegah Mirzapour, Amirata Fakhfouri, Hadiseh Azadi Cheshmekabodi, Kimia Azad, Seyed Ali Bagheri Zargande, Shahram Oliaei, Parisa Yousefi Konjdar, and Farzin Vahedi. Writing—Review and Editing: SeyedAhmad SeyedAlinaghi and Amirali Karimi. Validation: Esmaeil Mehraeen, Mohammad Heydari and Tayebeh Noori.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Transparency statement
Tayebeh Noori affirms that this manuscript is an honest, accurate, and transparent account of the study being reported; that no important aspects of the study have been omitted; and that any discrepancies from the study as planned (and, if relevant, registered) have been explained.
Availability of data and material
The authors confirm that the data supporting the findings of this study are available within the article [and/or] its supplementary materials.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
