Abstract
This study investigates differences in attitudes towards, and experiences with, online electronic health records between cancer patients and patients with other conditions, highlighting what is characteristic to cancer patients. A national patient survey on online access to electronic health records was conducted, where cancer patients were compared with all other respondents. Overall, 2587 patients completed the survey (response rate 0.61%). A total of 347 respondents (13.4%) indicated that they suffered from cancer. Results showed that cancer patients are less likely than other patients to use online electronic health records due to general interest (p < 0.001), but more likely for getting an overview of their health history (p = 0.001) and to prepare for visits (p < 0.001). Moreover, cancer patients rate benefits of accessing their electronic health records online higher than other patients and see larger positive effects regarding improved communication with and involvement in healthcare.
Introduction
Healthcare has undergone a number of major changes in recent years, partly due to advances in electronic health (eHealth) technologies. 1 It is increasingly recognized that patients can participate more actively in decisions regarding their own care when they have access to relevant information.2,3 A lot of effort has been put into the development of new eHealth technologies to promote patient participation, enhancing information-sharing and communication with patients4,5 and improving health outcomes.5,6 An example of this type of service is to provide patients with online access to their electronic health records (EHRs). 7
The overall goal of patient accessible EHRs is to improve communication between healthcare professionals and patients, ultimately increasing patients’ engagement in care and improving shared decision-making between professionals and patients. 7 Two well-known examples of large-scale EHR systems are OpenNotes in the United States2,8 and MyUHN Patient Portal in Canada. 9 A similar service was launched in 2012 in Sweden, when the regional healthcare authority in Region Uppsala (county council) gave all citizens over 18 years of age online access to their EHR through the eHealth service ‘Journalen’. The service was eventually launched as a national system in Sweden. It is accessible through a national patient portal and provides means to access all health record information from all public and private healthcare providers patients have visited independent of which medical record keeping system the healthcare providers use. 10 Currently, when patients access Journalen, they find a variety of types of clinical content, including medical notes, a list of prescribed medications, lab results, medical alerts, diagnosis, maternity care records, referrals and vaccinations (see Figure 1).
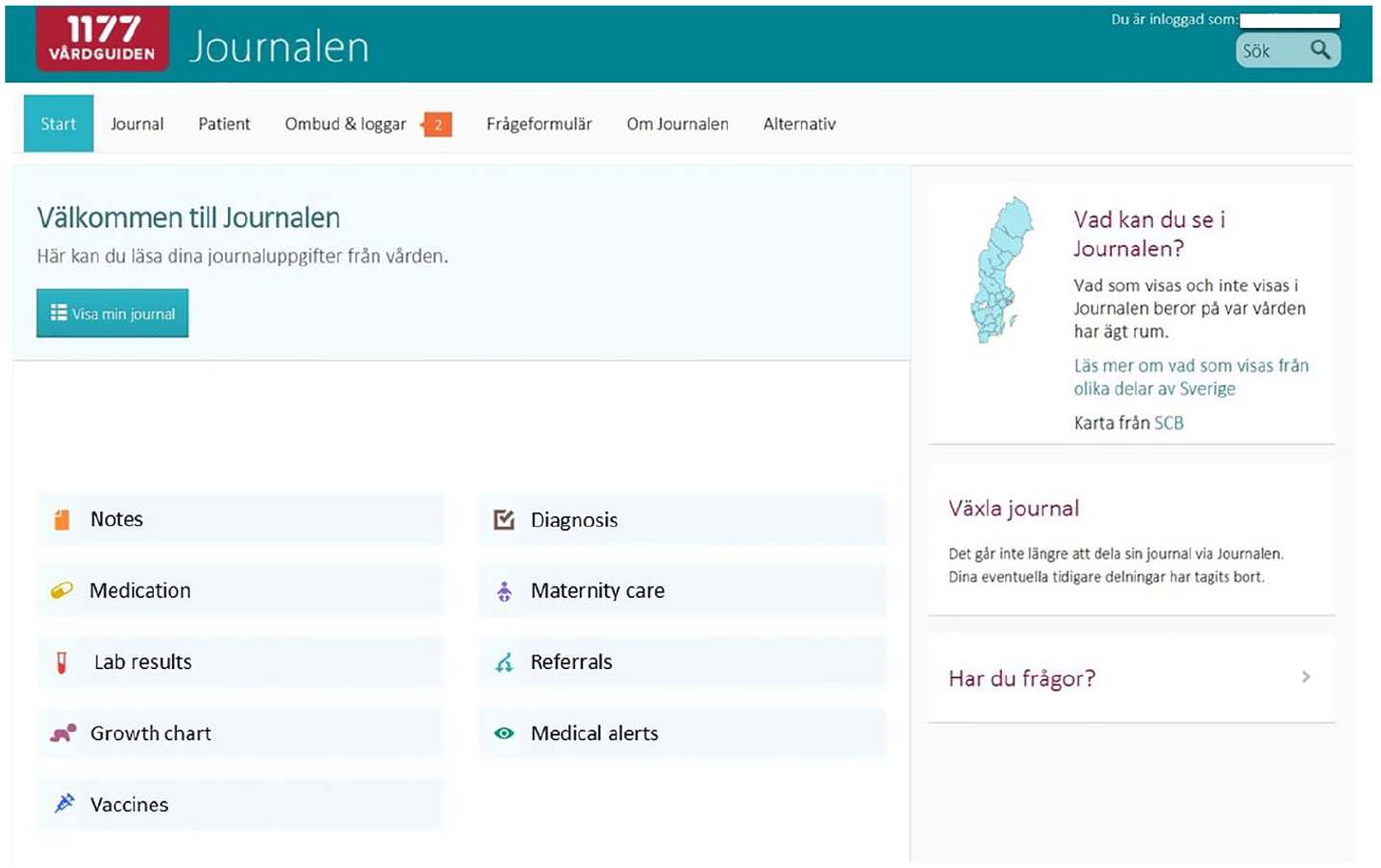
The eHealth service Journalen after login, showing the functions and information available (partially translated).
Although the Journalen interface is identical for all users, there are some differences in how much information each healthcare provider gives access to. Available information depends on if patients have received care from a public or private healthcare provider. With public providers, the available information depends on whether Journalen has already been implemented in a specific county council. Some private healthcare providers give their patients access to their EHR, even if the local county has not implemented Journalen. However, it is also possible that a local county council has implemented Journalen, but specific private healthcare providers in the area do not give access to their medical notes. All 21 regions in Sweden give patients access to medical notes from the EHRs (from all healthcare professions and all connected healthcare providers that have agreed to give access, both public and private). However, access to for example test results (17 of 21) is still not implemented in all regions.
Moreover, the implementation process of Journalen has been long and fraught with issues necessitating changes in legislation and research to allay a series of concerns raised, especially, by clinicians. Healthcare professionals have been worried that online access to EHRs would increase their workload and cause confusion and anxiety with patients if they misinterpret or fail to understand the contents of the record. This was considered particularly problematic if patients access their records during weekends and evenings, when no staff is available at healthcare units to answer patients’ questions or deal with their concerns.11,12
Some healthcare professionals have also raised a concern that patients might misuse the information – attempt to diagnose themselves or decline beneficial treatment because they have misunderstood the content of the record. These concerns are not unique to Swedish clinicians. Similar reactions have been reported from other countries, including the United States and the United Kingdom. 13 Moreover, the impact of providing access to information on the patient’s level of anxiety, especially for oncology patients, has been debated by clinicians. 14 While some opine that patients may experience anxiety when accessing test results independently without a professional present in the situation, others argue that waiting for results is a more significant source of anxiety.14,15 There is evidence that full access to healthcare records increase satisfaction with the process of care without increasing anxiety in patients with newly diagnosed cancer. 16 Wass and Vimarlund 17 suggest that online access to EHRs plays a role in increasing patient involvement by (1) fostering a balanced relationship between patients and healthcare professionals and (2) improving access to information. Comparable studies from within the OpenNotes initiative have shown that physicians and patients experienced relational benefits when medical notes were shared. 18 Furthermore, Bell et al. 19 have shown that access to EHRs can forge stronger partnerships with healthcare professionals and increase patient satisfaction with doctor–patient communication. 20 A study by Esch et al. 20 have also shown that access to notes improved adherence to medical advice and self-care. Patients also described how they felt empowered or reassured when accessing their EHRs. 20 Another recent study from the OpenNotes initiative reported a higher degree of participation in shared decision-making among those patients who read their clinical notes online. 3 Similar results have been reported in the work of Vermeir et al. 21 Others, including Ross and Lin 22 and Wright et al., 23 suggest that online access to EHRs can improve adherence to medical advice.
In addition to research on the effects of consulting EHRs, there is a relatively large number of studies on how patients access their EHRs online and their attitudes to the prospective introduction of such eHealth services.24–28 There is also some earlier research on cancer patients and their use of online EHRs.29,30,15 However, to the best of our knowledge, there is no comparative research on how online EHRs are perceived and used depending on whether you are seriously ill (e.g. diagnosed with cancer) or have other chronic conditions such as, high blood pressure and diabetes. Studying and comparing the experiences and attitudes of different patient groups in relation to online EHRs can provide us with useful insights into how eHealth solutions can support specific groups of patients in their contact with healthcare. Moreover, understanding cancer patients’ perceptions of the usefulness of and benefits of online EHRs is important because of the large size of the group. Over 60,000 people in Sweden are diagnosed with cancer each year and it is estimated that one in three persons will be diagnosed with cancer during their lifetime. 31 Studying differences in attitudes and preferred usage between cancer patients and other patient groups is also relevant from the perspective of the ongoing debate about the effects on anxiety for cancer patients in particular. 14
The aim of this study is to address the lack of comparative research and shed light on differences in attitudes towards, effects of, and experiences with online EHRs between cancer patients and other patient groups. The broader goal of this research is to increase our understanding of aspects of online EHRs that are important for patients with serious diagnoses and explicate patients’ perspective to a question that has been primarily discussed by healthcare professionals.
The remainder of this article is organized as follows. First, a description of the research approach is given, followed by a presentation of the main findings. A discussion and conclusions of the findings are given in the last section of the article.
Method
This study is based on data from an online national patient survey distributed to users of Journalen through a link available on the login page of the service. The respondents were informed about the purpose of the study as well as presented a standard consent they were required to accept before starting the survey. The survey, which focussed on attitudes towards and experiences with using Journalen, was approved by the Regional Ethical Review Board in Uppsala, Sweden (EPN 2017/045).
The survey included 24 questions with a combination of Likert-type scale items and multiple-choice items. Some of the questions also contained a free text in which the respondent could comment on the question. The questionnaire was developed based on a literature review and other studies performed in Sweden related to Journalen.15,32,33
The literature review helped to identify unexplored areas related to online EHRs. The literature review resulted in the following areas:
Attitudes and reactions
Access to and usage of information
Effects on contact with healthcare
Information content
Security and privacy
Personal health information
Demographics
Seven questions related to the areas 1, 2, 3, 4, and 6 have been analysed in this study. Six of these questions, relating to category 1–4 were all in 5-point Likert-type scales. Area 6, on personal health information (multiple-choice), included a question on which categories of conditions the respondents identified themselves with if any. The respondents could choose between the alternatives; cancer, mental health, diabetic, high blood pressure and other. The specific diagnoses cancer, diabetes and high blood pressure were chosen as they are the most common chronic conditions in Sweden. Mental health was included to address the ongoing debate in Sweden on whether psychiatric records should be made available and whether this patient group can benefit from accessing the EHRs or not. A total of 347 respondents, which constitutes 13.4% out of the 2587 respondents who answered the survey, indicated that they suffered from cancer. Figure 2 provides a breakdown of the conditions indicated by the respondents. This article focusses on the cancer patients’ answers and their relation to answers from all other respondents. Since the survey did not include any questions related to for example type or stage of cancer, these aspects have not been taken into account in the analysis. The same is true for comorbidity – combinations like cancer and mental health issues have not been considered here. Overall results of the survey, as well as a more detailed account of the analysis and data collection procedures, have been published in the work of Moll et al. 34
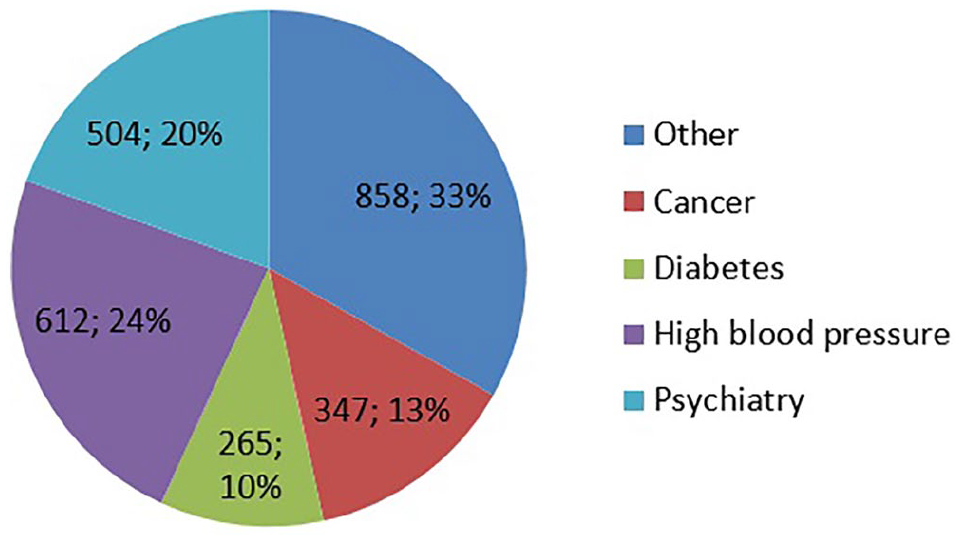
The distribution of respondents over disease groups.
The data were analysed using descriptive statistics. The Mann–Whitney U-tests were used for detecting group-wise differences between answers to Likert-type scale questions from cancer patients and other respondents. Thus, the multiple-choice question on personal health information was used as a grouping variable. The Likert-type scale alternatives (strongly agree, agree, neutral, disagree, strongly disagree) were converted to a numerical scale 1–5 before the analysis. No free text responses have been analysed. SPSS 25 was used for all calculations.
Results
General attitudes
The Figure 3 shows that the vast majority of both the cancer patients and the group consisting of all other respondents are positive towards the reform that gave patients online access to their EHR in Journalen (‘question a’). The same holds true for ‘question b’: ‘I believe that access to “Journalen” is good for me’. The Mann–Whitney tests show a significant difference between the two groups for ‘question a’ about Journalen as a reform (U = 354,988, p = 0.008), with cancer patients (mean = 4.86, SD = 0.46) being more positive towards the reform than other patients (mean = 4.77, SD = 0.63). No significant differences were found between cancer patients (mean = 4.86, SD = 0.50) and other patients (mean = 4.84, SD = 0.54) regarding ‘question b’ (U = 369,998, p = 0.76).
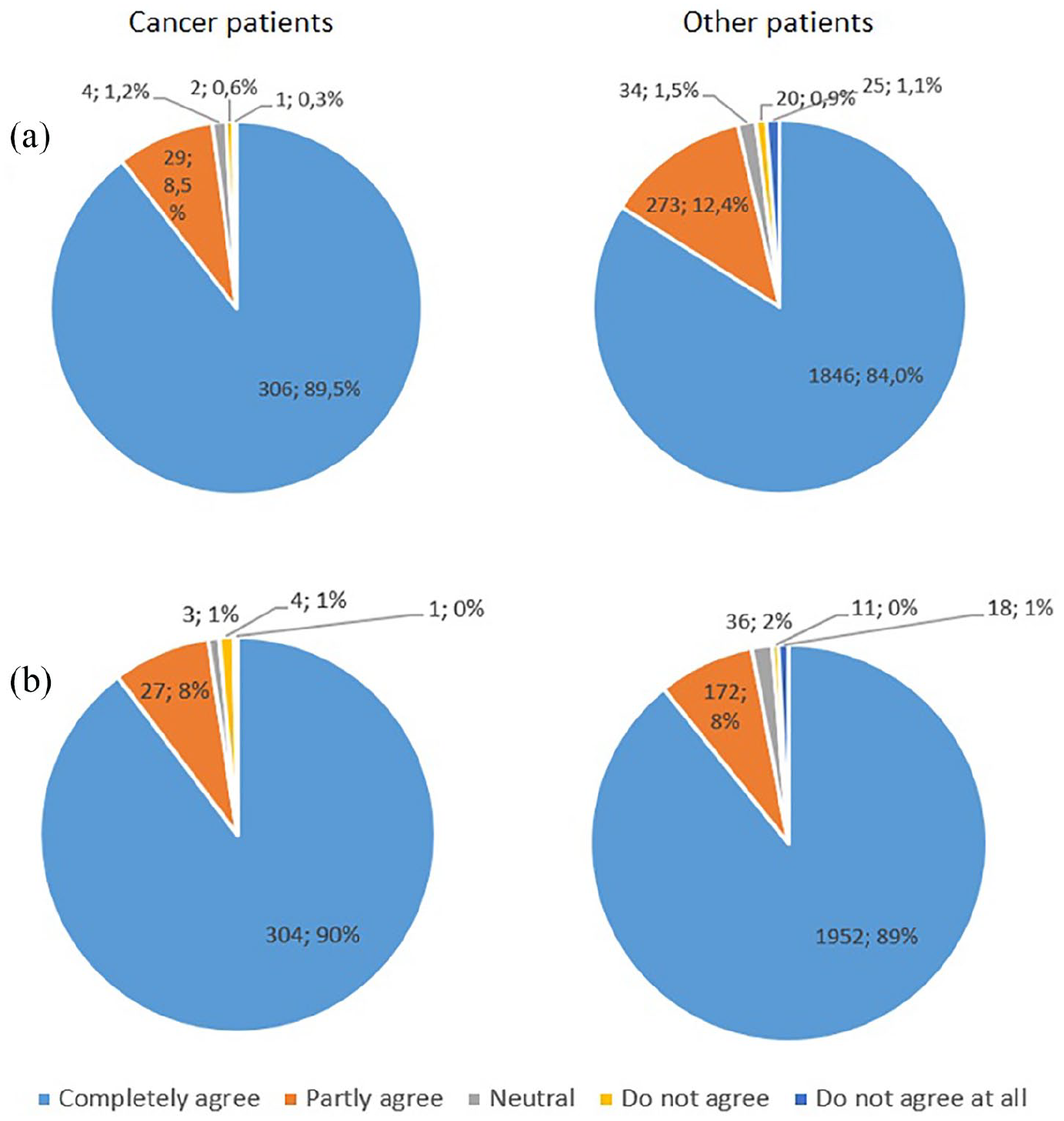
Compilation of responses to the questions: (a) ‘I believe that access to medical records online is generally a good reform’ and (b) ‘I believe that access to “Journalen” is good for me’.
Accessing patient information
When it comes to reasons for using Journalen, several statistically significant differences were found between answers from respondents belonging to the group of cancer patients and others. The Table 1 shows items with statistically significant differences. The results show that cancer patients are less likely than other patients to use Journalen due to general interest (p < 0.001), but more likely than other patients to use the service to get an overview of their health history (p = 0.001), to follow-up on visits (p = 0.039), to prepare visits (p < 0.001) and to become more involved in their care (p < 0.001).
Answers to the question ‘Why do you use Journalen?’ from cancer patients and all other patients, respectively.
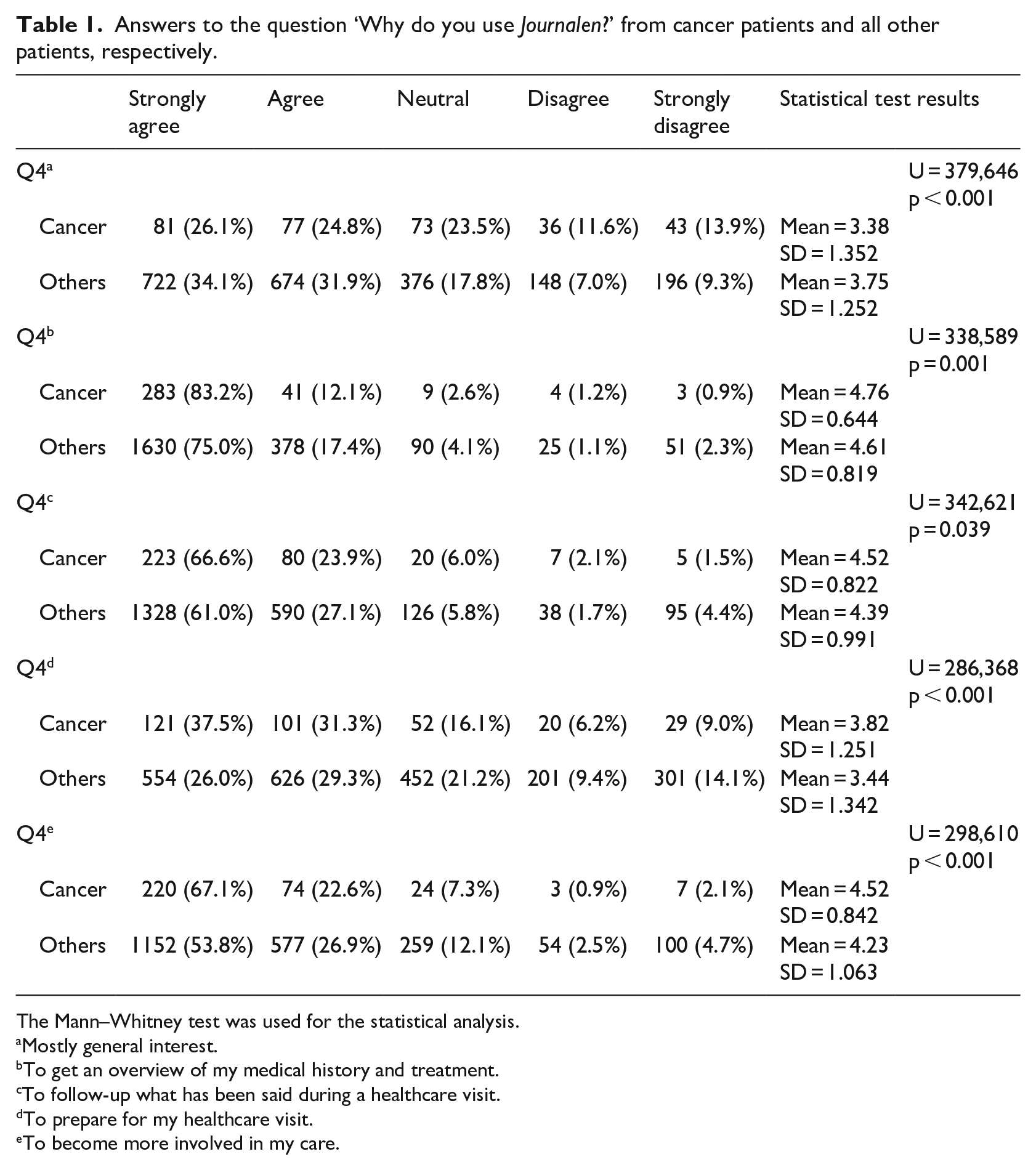
The Mann–Whitney test was used for the statistical analysis.
Mostly general interest.
To get an overview of my medical history and treatment.
To follow-up what has been said during a healthcare visit.
To prepare for my healthcare visit.
To become more involved in my care.
There were also several statistically significant differences in the perceived importance of being able to access patient information in Journalen (Table 2). The results show that cancer patients are more inclined to consider that Journalen improves communication with medical staff (p = 0.009), that it improves the understanding of the condition (p = 0.008), makes the patient feel more informed (p = 0.023), improves the possibility for self-care (p = 0.024) and improves the possibility to actively participate in decisions (p = 0.042), than other patients.
Answers to the question ‘How important is it for you to be able to access patient information?’ from cancer patients and all other patients, respectively.
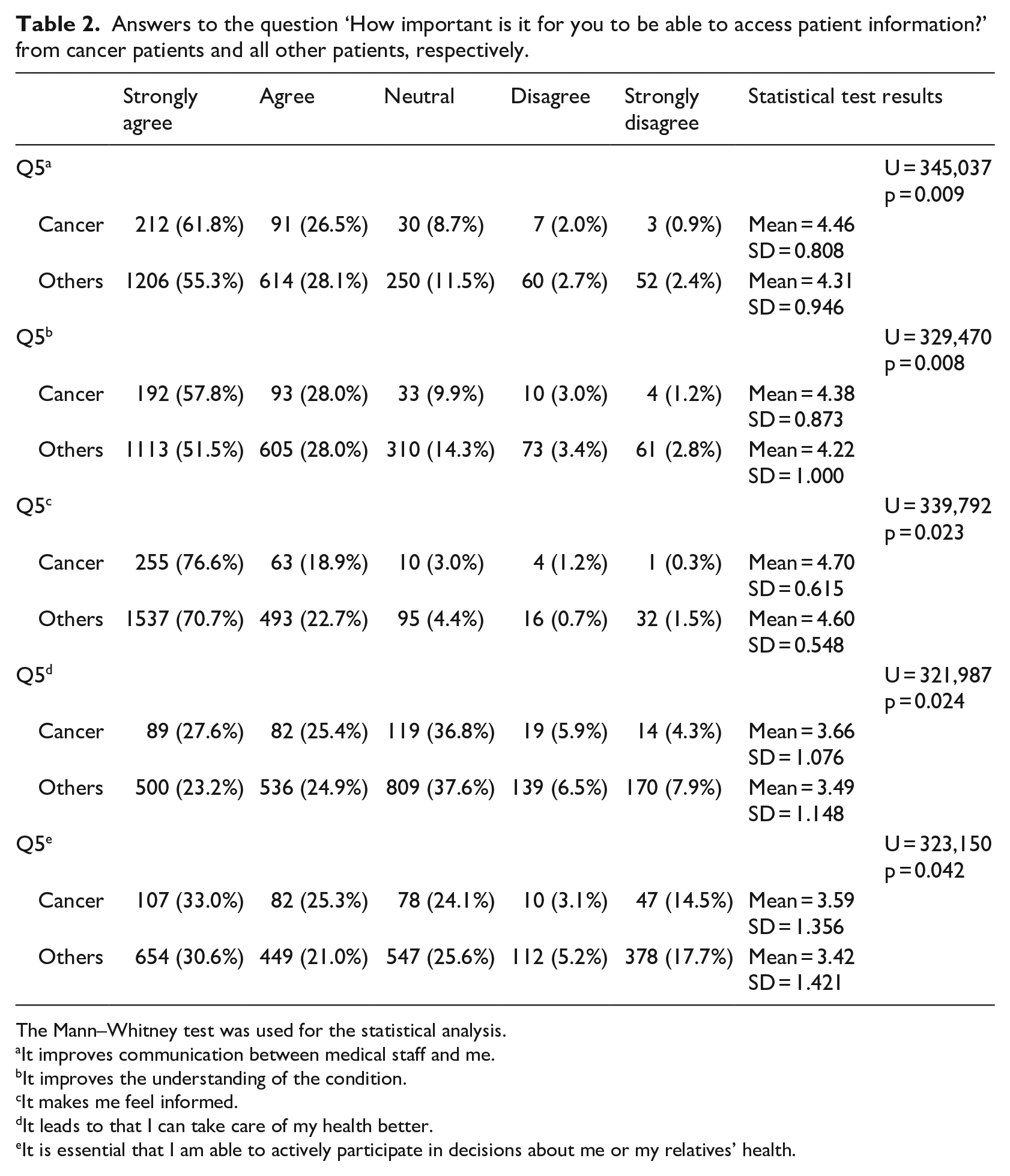
The Mann–Whitney test was used for the statistical analysis.
It improves communication between medical staff and me.
It improves the understanding of the condition.
It makes me feel informed.
It leads to that I can take care of my health better.
It is essential that I am able to actively participate in decisions about me or my relatives’ health.
The respondents were also asked to rate how important they found different types of information and functions available in Journalen. Table 3 shows five items with statistically significant differences. Cancer patients rated the following information types and functions significantly lower than other patients did: overview of immunizations (p = 0.017), psychiatry record information (p < 0.001), ability to block access to certain information (p = 0.009), ability to see the log list (p = 0.001) and the possibility to access and manage services for children (p < 0.001). No information type or function was found for which cancer patients gave a significantly higher rating.
Answers to the question ‘How important is it for you to have access the following information which is wholly or partly based on information contained in “Journalen”?’ from cancer patients and all other patients, respectively.
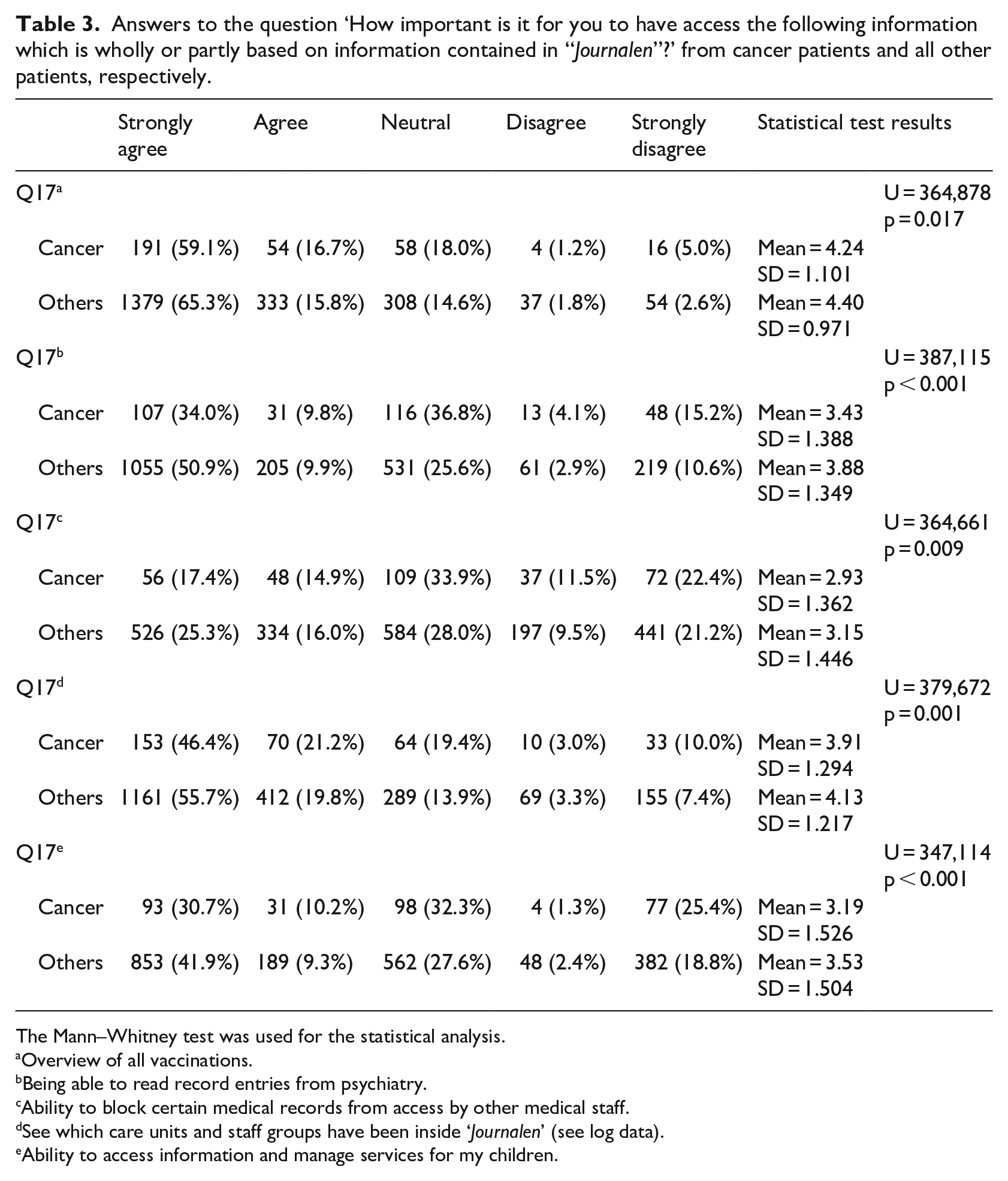
The Mann–Whitney test was used for the statistical analysis.
Overview of all vaccinations.
Being able to read record entries from psychiatry.
Ability to block certain medical records from access by other medical staff.
See which care units and staff groups have been inside ‘Journalen’ (see log data).
Ability to access information and manage services for my children.
Involvement and communication
For questions pertaining to the relationship with healthcare and communication with healthcare professionals, significant differences were found for all items (Table 4, Q7). Cancer patients were inclined to see a positive effect on their relationship with healthcare as a consequence of being able to access information in Journalen (p < 0.001). Even though the ratings for items regarding communication about Journalen are generally low, cancer patients gave significantly higher ratings for all items in this category (p < 0.001 in all cases). The difference between cancer patients and all other patients is the highest when it comes to discussing the content of Journalen with healthcare professionals (e.g. during visits to healthcare).
Answers to the questions ‘To what extent do you agree with the following statements regarding your relationship with healthcare?’ (Q7) and ‘How important is “Journalen” to make you feel that you are involved in your own care?’ (Q16) from cancer patients and all other patients, respectively.
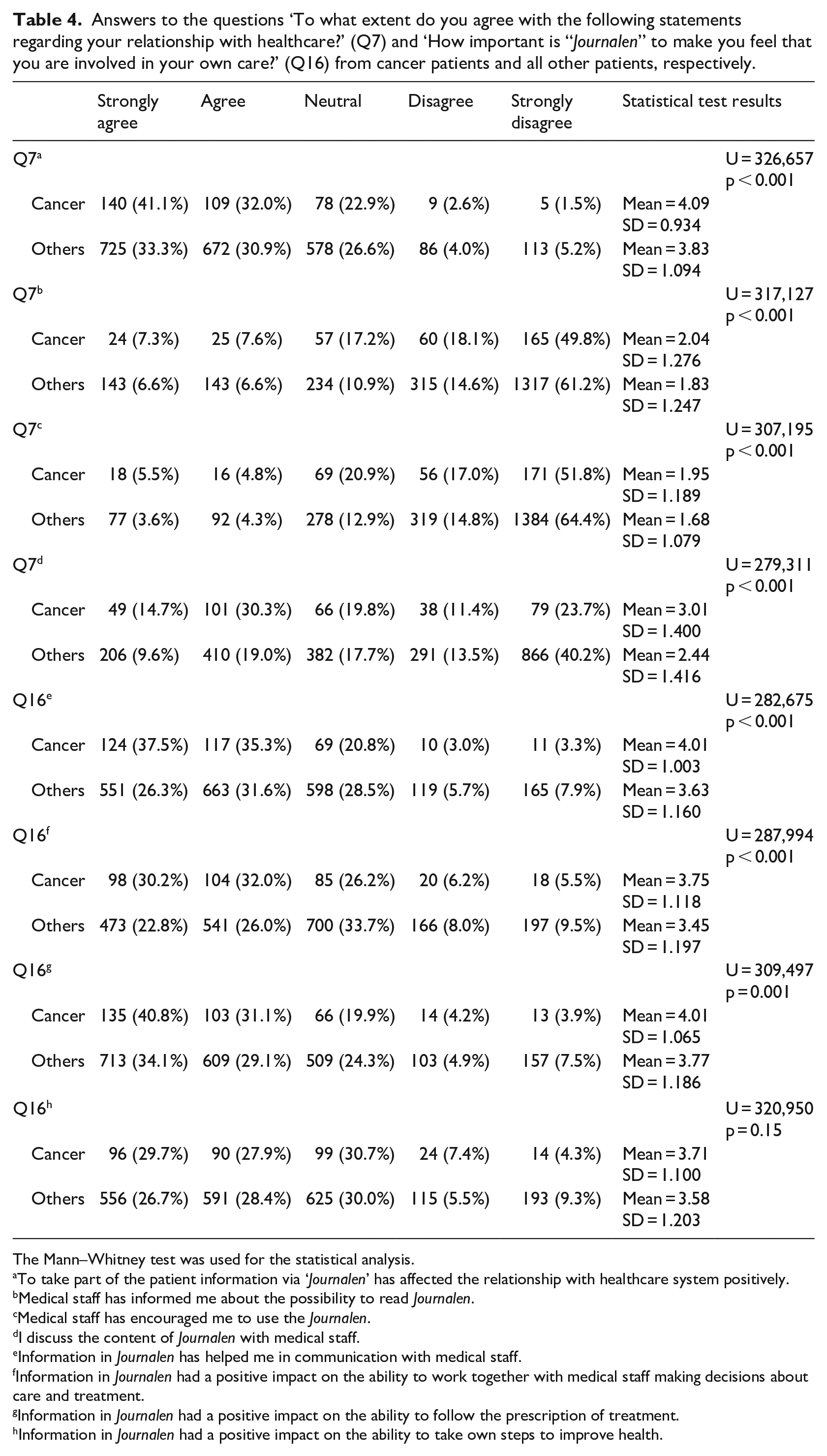
The Mann–Whitney test was used for the statistical analysis.
To take part of the patient information via ‘Journalen’ has affected the relationship with healthcare system positively.
Medical staff has informed me about the possibility to read Journalen.
Medical staff has encouraged me to use the Journalen.
I discuss the content of Journalen with medical staff.
Information in Journalen has helped me in communication with medical staff.
Information in Journalen had a positive impact on the ability to work together with medical staff making decisions about care and treatment.
Information in Journalen had a positive impact on the ability to follow the prescription of treatment.
Information in Journalen had a positive impact on the ability to take own steps to improve health.
Significant differences were also found regarding the involvement in care (Table 4, Q16). Cancer patients rated significantly higher the benefits of Journalen as an aid for communicating with medical staff (p < 0.001), the ability to engage in shared decision-making (p < 0.001) and the ability to follow prescriptions of treatment (p = 0.001). No significant difference was found regarding the perceived ability to engage in self-care (p = 0.15). In the latter case, however, there is still a tendency of higher ratings with cancer patients.
Discussion
The purpose of this study was to compare the attitudes towards, experiences with and identified potentials of the Swedish patient accessible EHR Journalen between cancer patients and other patients. This article is a part of a much needed follow-up of the effects of the patient’s access to their EHR several years after the launch of Journalen. The national patient survey yielded an array of interesting findings highlighting clear differences between cancer patients and other patients in several different respects. Even though there is an increasing number of studies focussing on the use of patient accessible EHR in oncology care, there are, to the best of our knowledge, no comparative studies of the kind reported in this article. The explicit comparisons made, helps in highlighting for example what aspects of the patient accessible EHR that are of most importance for this particular group of patients, whose use of the system has been up for debate – both in Sweden and abroad – for a long time. Below, results from the various aspects covered in the survey are more thoroughly discussed.
The vast majority of both cancer patients and others are positive towards the opportunity to consult their health records online through the eHealth service Journalen and perceive it as important for themselves. However, not wholly unexpectedly, the cancer patients differ from all other patients in how they perceive Journalen as an instrument for managing and coping with their specific condition. Earlier studies have shown that general interest and curiosity are major motivators for patients to read their EHR. 13 Simultaneously, there is evidence that cancer patients might have somewhat different preferences. 15 The present analysis shows that this is the case. Unlike other patients, whose primary motivation for using Journalen is general interest and curiosity, the results show that cancer patients are more likely to use the eHealth service to get an overview of their health history, to follow-up on visits and to prepare for upcoming visits. The findings also suggest that cancer patients can be expected to be more likely to benefit more from using eHealth services than other patients in terms of improved communication with healthcare professionals 20 and improved understanding of their condition.13,15 At the same time, the specific features valued most (e.g. access to health history) by the respondents of this study are linked to information with implications to shared decision-making and the ability to follow prescriptions of treatment.7,35 This is in line with the earlier studies on OpenNotes2,3 with similar conclusions. However, in comparison with earlier studies, the present analysis shows that even if all patients scored high, the cancer patients valued these features to a greater extent than the others.
Another observation that can be made on the basis of the analysis is that cancer patients consider to a greater extent that their relationship with healthcare professionals improves as a consequence of being able to access their EHRs. A possible explanation is that, patients who feel an increased participation in decisions as a result of being able to access information also develop a more positive view of their relationship with healthcare professionals. Hence, engaging patients through online EHR may provide opportunities to strengthen care partnerships between patients and healthcare professionals. 13 Moreover, the ratings for the items related to improved communication with healthcare professionals were generally low within all patient groups whereas cancer patients gave significantly higher ratings. Previous research15,36 has also reported improved communication as an important perceived outcome of having access to information from the EHR, a finding that this study confirms with a larger group of cancer patients, and simultaneously shows a previously unreported significant difference in this respect to other patients. Furthermore, the present findings add to the earlier observations that cancer patients seem to be more keen to discuss the content of Journalen with healthcare professionals (e.g. during healthcare visits) and perceive that Journalen has had a positive impact on collaboration between patients and professionals. However, as the vast majority of the patients have not been encouraged by the healthcare professionals to use the eHealth service Journalen there is room for highlighting the collaborative potential of the service for professionals. The potential significance of communicative and collaborative benefits for cancer patients is underlined by the fact that no statistically significant differences were found between the patient groups in their self-perceived ability to engage in self-care.
Furthermore, with regard to the importance of information and functions available in Journalen, there were no significant differences between cancer patients and other patients that indicated that certain types of information would be more important for cancer patients. However, cancer patients rated certain types of information as less important, including immunizations, psychiatry record information and information about which healthcare professionals had accessed their medical record, the so called log list. This could be expected assuming that their primary concern is their cancer and directly related information, not other issues.
The findings of this study contribute to the understanding of differences in perceptions and use of information in EHRs between patient groups. The study presented in this article is also one of the first that consider long-term effects of patient accessible EHRs for specific patient groups in Sweden, as well as in Europe – in this case cancer patients. The study reports perceptions of Journalen 5 years after it was originally launched and is hence an important complement to earlier studies (including an interview study with cancer patients in Region Uppsala reported in the work of Rexhepi et al. 15 ), which were conducted within a year after launch. The results are also relevant to the ongoing debate among healthcare professionals about the effects of providing access to Journalen for this particular group of patients 14 by providing new insights from the perspective of patients. Many physicians are still concerned regarding cancer patients’ access to EHR due to the possibility of adverse effects of learning about serious diagnoses online without the presence of a qualified healthcare professional.12,14 A recently published survey study among oncology professionals also showed that a majority of the respondents believed that the notes were more confusing than helpful to their patients. 37 The new results presented in this article show that cancer patients see pronounced benefits of accessing online EHRs when it comes to involvement and communication with healthcare – benefits that are significantly less pronounced for other groups of patients. The fact that the surveyed cancer patients articulated specific rather than general reasons for accessing their EHR suggests that they tend to know what they are doing rather than accidentally stumbling on information they were not looking for. This being said, it is possible that a noteworthy problem regarding patients’ use of online EHRs and shared decision-making is that patients’ access to their notes is not integrated in the patient meeting. For example, most patients have not discussed Journalen with their healthcare providers or been encouraged by healthcare professionals to use the eHealth service. One possible reason can be the above mentioned concerns. Moreover, a possible positive outcome of this study could be that the results would persuade oncology professionals to start a conversation with their patients about EHR and explore the possibilities already identified by the patients. The present survey did not address the question of anxiety directly, but there are no specific reasons to doubt that the results of an earlier interview study with Swedish cancer patients 15 conducted 1 year after the launch of Journalen would not hold. According to these findings, several interviewees reported that they preferred to get bad news about their disease online so that they could prepare themselves for the meeting with their physician. At the same time, however, it is important to keep in mind that a small group of patients both in the present material and in earlier studies 15 have expressed anxiety – a finding that further underlines the importance that healthcare professionals discuss EHR use together with their patients.
Limitations of the study
This study has some limitations that need to be taken into account when interpreting the results. First, the fact that only the persons who have logged in to Journalen at least once had a possibility to participate in the survey is a possible source of a positive bias. Second, access to information from Journalen is to some extent dependent on where the patient has received care. In this study, we have not made county-wise comparisons and hence, not accounted for the specific types of information that the different respondents could get access to in Journalen. Our assumption is that the effect of the availability of information is similar for cancer patients and other respondents.
Another limitation with this study stems from the fact that all cancer patients were grouped together in the analysis, regardless of the stage of cancer or possible comorbidity. It is, for example, reasonable to believe that a patient’s information behaviour changes as the disease progresses. It is unclear how comorbidity could factor in, and in future research this aspect will be considered in the study design and analysis. These limitations aside, the results still provide some valuable and clear indications.
Conclusion and future work
One of the recent innovations to promote patient engagement is allowing patients to access their EHRs online. Our analysis shows that patients using a specific patient accessible EHR service Journalen are generally positive towards such an opportunity. Compared to other groups, cancer patients tend to use Journalen for the specific purposes of getting an overview of health history, to follow-up on visits and to prepare for upcoming visits rather than for general interest. They also consider that they benefit more from using the eHealth service than other patient groups in terms of improved understanding of the condition and increased participation in making decisions. The ratings for the items related to improved communication with healthcare professionals were generally low within all patient groups; however, cancer patients gave significantly higher ratings than all other respondents. Overall, the results indicate that cancer patients have more specific reasons related to managing and understanding their own disease and can be expected to be a group that benefits from increasing empowerment and involvement in care. The findings point towards the potential usefulness of an increased dialogue between oncology professionals and cancer patients on how to relate to Journalen and use patient accessible EHRs as a part of communication and collaboration between patients and professionals.
As for future research, the next step is to elaborate the present and earlier findings 15 in an in-depth qualitative study with cancer patients. Qualitative data are especially crucial for increasing our knowledge about how patient accessible EHRs have affected communication and patient involvement in practice when several years have passed after the initial launch of the systems. Further research with oncology professionals is also needed to elaborate the understanding of the limits and possibilities to develop the role of the patient accessible EHR in oncology care.
Footnotes
Acknowledgements
The authors would like to thank the colleagues in the national DOME (Development of Online Medical records and E-health services) consortium who participated in the data collection. We would also like to thank INERA and Evry for distributing the survey through the national patient portal.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
