Abstract
We investigated the reasons why the transition from paper to electronically formatted records during patient handover between ambulance crews and emergency department staff in a North East England Emergency Department has not always been viewed positively. Interviews with seven paramedics and three emergency department staff were conducted in addition to observations of 74 ambulance staff during 37 handovers in the emergency department. In just over half of the handovers (20), paramedics found it necessary to provide written information to aid emergency department staff, in addition to that recorded electronically. There were a number of issues that impeded the ready utilisation of electronic records in this context. The major factors identified as contributing to this were the choice of system architecture, the design of user interfaces, and the procurement process used by the National Health Service. We have made some suggestions about how the system could evolve from one focused on providing management information to one that also supports operational needs.
Keywords
Introduction and background
Healthcare provision in the United Kingdom is organised through a set of largely autonomous agencies and hence involves frequent exchange of information about patients. The North East Ambulance Service, NHS Foundation Trust (NEAS) has adopted an electronic Patient Report Form (ePRF) as the primary record of patient care. The ePRF is used to record details relating to ambulance call-outs and to share this information with emergency department (ED) staff in receiving hospitals. Introducing the electronic record involved replacing an A3-size paper form (the Patient Report Form (PRF)) with a digital equivalent (ePRF) and was completed in 2012.1,2
The ePRF (or PRF) is completed by the ambulance paramedics as their official record for an incident, providing a report from their perspective, together with their observations of a patient’s clinical condition, medication administered, etc., in a structured and legible format. The ePRF also has other uses: it provides ED staff with confirmation of what was reported to them verbally at patient handover, can assist NEAS management in planning service improvements, and can provide evidence in response to complaints or investigations about patient treatment and outcomes in ambulance and/or hospital settings.
From other work we have undertaken, it became evident that the ePRF was not always viewed positively by either the crews or ED staff. Therefore, our research question for the work described in this article is, ‘What factors constrain the effectiveness of electronic information transfer through use of the ePRF, and how might they be resolved?’
In the rest of this section, we outline the background regarding provision of information at handover from ambulance crews to ED staff within the NEAS area, and conflicts that arise from its use and design.
Transferring patient information
The decision to dispatch an ambulance to an incident is taken by a dispatcher based on the information gathered by a call handler, both of whom are based in the NEAS control centre. Initial information related to the incident, as provided by the caller, can be passed to the ambulance crew via their Mobile Data Terminal (MDT). The crew is required to use their ruggedised laptop computer, called a Toughbook (issued to them by NEAS), together with the initial and incident information, to create an ePRF. The ePRF contains fields for entering mandatory and/or optional information such as incident observations, treatment details, medication administered, health condition data, and the means of optionally attaching electrocardiographic (ECG) recordings. The crew is required to complete an ePRF, even when the incident does not require the patient to be taken to an ED.
If the decision is taken to transfer the patient to an ED, the ED staff at the designated hospital can view the initial information provided by the caller on the pre-alerting screen installed in the ED by NEAS, so that they have an idea of what to expect. However, the patient’s situation, as reported to the call handler by the caller, will depend upon the caller’s interpretation and so may sometimes be inaccurate. ED staff can only view the incident information, as provided by the paramedic, after the ePRF has been uploaded, that is, after patient handover. 3
On arrival at the ED, the patient is usually registered at reception and the ambulance crew then waits for a nurse in order to initiate a verbal handover. This consists of a summary of the patient’s condition and immediate needs, followed by more detailed information about observations and any treatment given prior to handover. The nurse is then required to sign the ePRF, confirming that a detailed handover has occurred. Ideally, this will also indicate that the ePRF is finalised, with all the mandatory fields having been completed en route to the ED.
Once finalised, the ePRF is uploaded to the NEAS database, either via a wireless connection or by attaching it to the docking station provided in every ED by NEAS for this purpose. After this step, all appropriately authorised ED staff can access it via the Webviewer tool, using a smart card issued by NEAS together with their password. This process is consistent with the system developed by the East Midlands Ambulance Service which was the first National Health Service (NHS) Ambulance Trust to implement an ePRF. 4 Prior to adoption of the ePRF, a paper PRF would be completed manually on the way to the ED or on arrival and then signed by the nurse. The PRF is still available as a backup mechanism.
The ePRF finalisation process does not always run smoothly. Paramedics may not have time or opportunity to complete the ePRF in advance of arrival and so, after handover, may need to go back to the vehicle to complete the ePRF. During this time, the only updated information available to the ED staff is that provided during the verbal handover. However, uploading of the ePRF and therefore ED access to critical new information may be delayed due to a variety of factors.
Other ‘information stakeholders’
As indicated above, the ePRF system described here was adapted by NEAS from an existing system3,4 which was designed largely from the perspective of intra-agency information recording and analysis. However, the ePRF also supports current and potential inter-agency information transfer, and, indeed, the ePRF information is useful to others besides the ED staff. These include the following:
NEAS and hospital management teams, providing data about ambulance use such as numbers of patients being conveyed to ED via the ambulance service, reasons for their conveyance, the workload on NEAS, and the consequent workload on ED occasioned by the ambulance service. Information of this sort aids both management teams in audits, categorisation of ambulance and ED users, planning for improved service utilisation, and so on. Hence, this kind of information empowers management in performing managerial, administrative, and operational tasks, making resource decisions based on documented usage, and therefore (hopefully) developing sound estimations of future need.
Patients, who can have greater confidence about receiving appropriate treatment, based upon knowledge that information within the ePRF may improve both ambulance and hospital services, while also ensuring that their health status and other personal information is only being accessed by authorised relevant health providers. Greater sharing of ePRF information may prompt health personnel to view the patient as a whole, therefore enabling both patient and health professionals to take a holistic perspective of appropriate treatment options.
Other hospital departments/wards, which could be notified when their regular patients have been admitted to the ED and the reasons for this.
Technology adoption and human factors
Information and Communication Technology (ICT) systems, both within and among the National Health Service (NHS) health providers, are complex, heterogeneous, and autonomous.5–7 ICT designers and implementers face challenges in the healthcare domain, arising from multiple users with multiple needs, pre-existing clinical and management systems, and the use of technologies of variable sophistication. The complexity means that various literatures relating to the ways that people interact with and use computer systems, such as interaction design, human–computer interaction (HCI), and computer-supported cooperative working (CSCW), among others, each illuminate various facets of functionality. In this article, these literatures each provide insights suggesting how the identified constraints on the effectiveness of the ePRF during patient handover might be remedied.8–15
The literature on diffusion of innovation is also helpful in considering factors that affect the uptake of the ePRF. According to Rogers 16 and Greenhalgh et al., 17 adoption rates for different innovations in healthcare vary among individuals and organisations. They note that the adoption of an innovation is more likely to occur if it possesses some specific characteristics. For the ePRF, particularly relevant ones include the following:
Relevant advantage, so that potential users can envisage clear benefits from its adoption;
Compatibility, by which the innovation is compatible with the norms, needs, and values of the adopter;
Complexity, whereby it is perceived as being easy to embrace and use;
Trialability, meaning that users can experiment with its use;
Observability, in the sense that the benefits can be clearly perceived by potential users;
Reinvention, through which users can configure it to meet their requirements and needs (closely related to the HCI concept of appropriation 18 ).
As we will demonstrate, because the adoption of the ePRF was motivated largely by the needs of a single agency (NEAS), few of these characteristics have really been achieved in this system. We suggest that only relatively small changes are needed to improve the situation although we recognise it cannot be assumed that action will be taken to resolve the identified usability and adoption problems, especially since this is an outsourced system transferring information between two distinct organisations. 1
Method
We used a mix of interviews and observation to investigate our research question. 19 Interviews were held with paramedics and ED nurses. The interviews with paramedics were conducted on different dates and time slots between September 2014 and October 2014 at Durham University in accordance with the preferences of the paramedics. However, the interviews with nurses were conducted within the ED as per the agreement with the Hospital’s Trust and the ED Manager. Semi-structured pilot interviews were carried out to test the interview schedule. All interview participants were provided with study information sheets approved by the NHS Health Research Authority and all participants signed consent forms to indicate their agreement to participate and to be audio-recorded where appropriate. All recordings were transcribed by the first author to ensure confidentiality.
A total of 37 observations were made of the ED patient handover process performed at the relevant Hospital Trust over a range of shifts encompassing days and times of the week regularly associated with both high and low ED usage. Observations took place in four consecutive days in January 2016. This included two night shifts and two morning shifts. The observations were of ambulance crews, usually consisting of a paramedic, together with an advanced technician and/or an emergency care support worker, at the receiving bay in ED. Each observation session was 4 h long, with the first author being positioned in the receiving bay at the ED, sitting adjacent to the docking station and the monitoring pre-alerting screen. This position made it possible to both observe the complete handover process and ask some clarifying questions when handover had been completed, without causing any interruption to the process. This also made it possible for ambulance crew to ask questions about the research and to engage in brief conversations about the ePRF with the observer.
The data collected from interviews and observations were manually analysed on a thematic basis by extracting keywords, shared views, common ideas, and issues raised by the majority of participants and identifying within these any emergent themes relevant to the participants’ immediate experiences. These emergent themes were later reviewed again using models and concepts from the literature on CSCW and HCI.
We also studied relevant documentation about the design and implementation of the ePRF. 20 Although material about the ePRF was scarce, information was found online, in addition to that provided by NEAS, and some was found in reports, including management documentation describing the purpose of the system and the time frames for its implementation. Among other things, this material helped with framing questions for the interviews.
Conduct of the study
Face-to-face interviews were conducted with seven paramedics working for NEAS and with three ED nurses working for a North East Hospital Foundation Trust which provides tertiary care services. In total, 37 handovers were also observed, each with two members of the ambulance crew. NEAS participants had experience ranging from 6 to 20 years. The three ED nursing staff had experience ranging from 1 to 20 years. Table 1 displays details of the data collection and its location and numbers of participants for each group.
Research participants in the study.
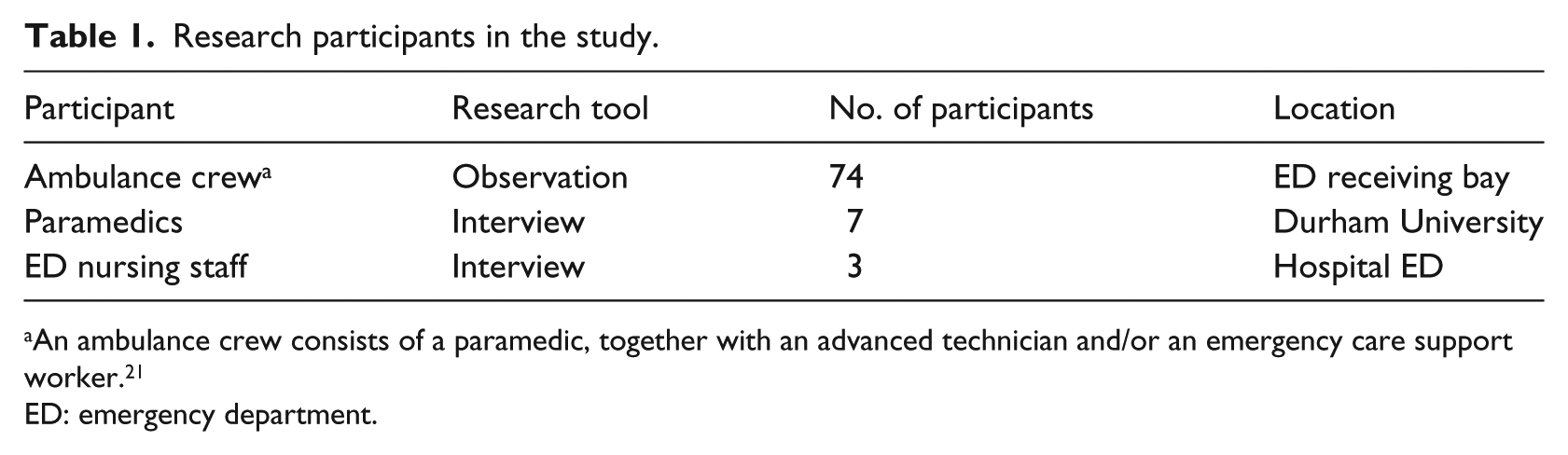
An ambulance crew consists of a paramedic, together with an advanced technician and/or an emergency care support worker. 21
ED: emergency department.
Results
We report on the combined interview and observational results from the perspectives of the paramedics and ED staff.
Issues identified by the paramedics
During observations of handover, 57 per cent (21) ambulance crews stated that they preferred using the ePRF; however, they still had mixed views about the benefits it provided, largely related to its realisation. The combined observation and the interview data revealed the following:
All paramedics considered it time consuming to complete.
The ePRF has more fields than the PRF, some of which require information that paramedics feel they are not trained to assess.
There was a lack of training for required information input.
The PRF format is concise and highlights the most important information categories, whereas the ePRF is subdivided into multiple pages on the Toughbook screen; navigation between these occasionally causes important information to be ‘lost in the detail’.
Some paramedics viewed it as having the role of a legal medical document and being too detailed.
The observation data, brief conversations with paramedics during observations, and the interview data together indicated that there are several key issues that affect finalising the ePRF after verbal handover, potentially delaying the availability of the crew for the next incident callout.
Ease of Data Entry. The journey time from the incident location to the ED, if short, may not be long enough for the ambulance crew to record incident data regardless of the incident type or the record format. On longer journeys, data field navigation can affect the speed with which ambulance officers perform data entry and influence whether they can complete it en route to the ED. Observations indicated that the type of record being used typically did not affect the period of time a paramedic spent between arriving at the receiving bay and leaving the patient in a cubicle under the care of ED staff. However, the record type did have a substantial effect on the amount of time taken to finalise the record before the crew could depart from the ED to the next assignment. Using a PRF, the crew could leave more or less immediately once they had a signature, as the concise fields in the paper form are easy to complete, but the hierarchical structure of the ePRF requires additional navigation time for completing data entry. Both the interviews and our observations indicated that, on average, a paramedic needed around 20 min to complete the ePRF after the ED nurse had signed it off in an ED cubicle.
Connection Availability. If the Toughbook cannot be connected to the NEAS server, paramedics face the challenge of finding a way to connect their Toughbook to the system to download a patient’s initial information and/or upload the finalised ePRF. In addition, when a Toughbook needs to be rebooted to help establish connectivity, there is a risk that ‘saved’ data are lost, meaning that patient information has to be re-entered.
Job Type. Another influence upon data entry speed is the ‘Job Type’. When patient treatment needs are relatively simple (termed a ‘Green Job’), the paramedic is likely to complete entry of the data en route to the ED. In life-threatening trauma events (‘Red Job’), however, the patient usually requires extensive and/or intensive care and data entry may not be possible until after the patient has been transferred into ED care. One paramedic reported that in complex ‘outlier’ Red Jobs, data entry could take as much as 3 h when using the ePRF requiring the crew and the ambulance to remain at the ED to upload the ePRF after ED staff have signed it off. In contrast, the same paramedic indicated that in similar situations completing the PRF would only take around 5–10 min.
Technical Issues. The other factor extending the time needed to finalise the ePRF compared to the PRF was computer-related technical issues other than connectivity. Paramedics sometimes encounter slow responses, running out of battery, frozen screens, or physical damage to the Toughbook due to mishaps, requiring them to find a workaround while under pressure. Workarounds were employed in some 20 of the 37 handovers that were observed (over half). A variety of different workarounds were employed, including writing on small pieces of paper (seven occasions), writing on the back of a printed ECG (seven occasions), writing on a glove (five occasions), and using a PRF (three occasions). In a few cases, more than one workaround was used at the same time (such as writing on an ECG and also on a small piece of paper or, in one case, writing on a napkin).
The form of workaround used would depend upon when problems occurred, for example, whether during transport to the ED or upon arrival. The complexity of the case and/or the likely consequences of lost time for both the current patient and the next patient needing urgent ambulance attendance also affect the type of workaround adopted. The workarounds noted above preserve the integrity of the immediate care encounter and ensure timely clinical actions; however, they potentially result in incomplete records through missed data fields or illegible handwriting, both of which undermine the ePRF’s usefulness as a legal document and management tool.
Paramedics also have mixed views about the Toughbook laptop itself. The Toughbook, at present, is mainly used to record information and is subject to the abovementioned problems which often cause frustration and require extra time to address. On the other hand, it can provide support by enabling paramedics’ access to limited additional online information. This information is currently restricted to primarily care pathways and guidelines issued by the Joint Royal Colleges Ambulance Liaison Committee, pharmaceutical information within the British National Formulary, and guidance on information to be recorded via ATMIST (a handover tool defined as Age of patient, Time of incident, Mechanism of injury, Injuries suspected, vital Signs, Treatment administered).22,23 The limited information access also caused frustration, with interviewees noting that they would value access to information about local care guidelines, specific individual patient needs, and patient history with the ambulance service. This is because paramedics decide whether the patient needs to be conveyed to an ED, taken home, or released at the scene after stabilisation, while also taking into account the patient or carer’s wishes. 24 Having such additional information would enable them to make better decisions about whether or not to convey the patient to ED.
Issues identified by the ED staff
As noted, the interviews conducted with ED staff were shorter and involved fewer staff.
5. Rapid Access to Patient Information. On patient arrival, ED staff would like accurate and fast access to information about the patient. Staff rely heavily on verbal information from the paramedics and/or the patient since, until an ePRF is finalised and uploaded, the only other information available to them is the initial information provided by the call maker. As noted earlier, this represents the call maker’s perception of the incident and is often inaccurate. One ED interviewee suggested that access to accurate information could be improved by generating a paper printout of the ePRF on arrival even though it may be incomplete at that point in time.
6. Information Availability. The usefulness and the amount of information provided on handover depend partly upon the individual paramedic’s knowledge, skill, and time constraints; thus, the ED staff can be overloaded with information or lack key knowledge. ED staff would like to have a system that, first, conveys key elements of incident information to them before patient arrival or handover and, second, facilitates access to any other health information that may be available about that particular patient.
7. Accessibility. Prior to the ePRF, ownership of the paper PRF and the data it contained was shared between NEAS and the ED. Upon ambulance arrival, paramedics simply gave ED staff a copy of the PRF, thus giving all ED staff instant access to patients’ incident information. The ePRF system however limits formal information access rights to those few ED staff authorised by NEAS to use the Webviewer tool. Most ED staff therefore do not use either the Webviewer or the ePRF; in fact, of the three staff members interviewed, two stated that they had never seen an ePRF. Even those ED staff authorised to access the ePRF usually do not do so; they prefer to spend additional time with patients rather than accessing information that has already been delivered to them verbally.
Overall, the paper PRF is considered to be more convenient for ED staff than the ePRF, though both formats reinforce verbal handover information. The ePRF is also viewed as being a NEAS project, with ED staff having no sense of ownership.
Analysis
Having identified and described seven issues that are considered to impede the process of handover, and hence that create barriers to the utilisation of the ePRF, we now examine each of these in more detail. Table 2 provides a summary of these and highlights the fact that, while there is some overlap of issues for NEAS and ED clinical staff, the immediate concerns of the two clinical groups are quite different.
Summary of issues identified by participants as affecting the effective utilisation of the ePRF.
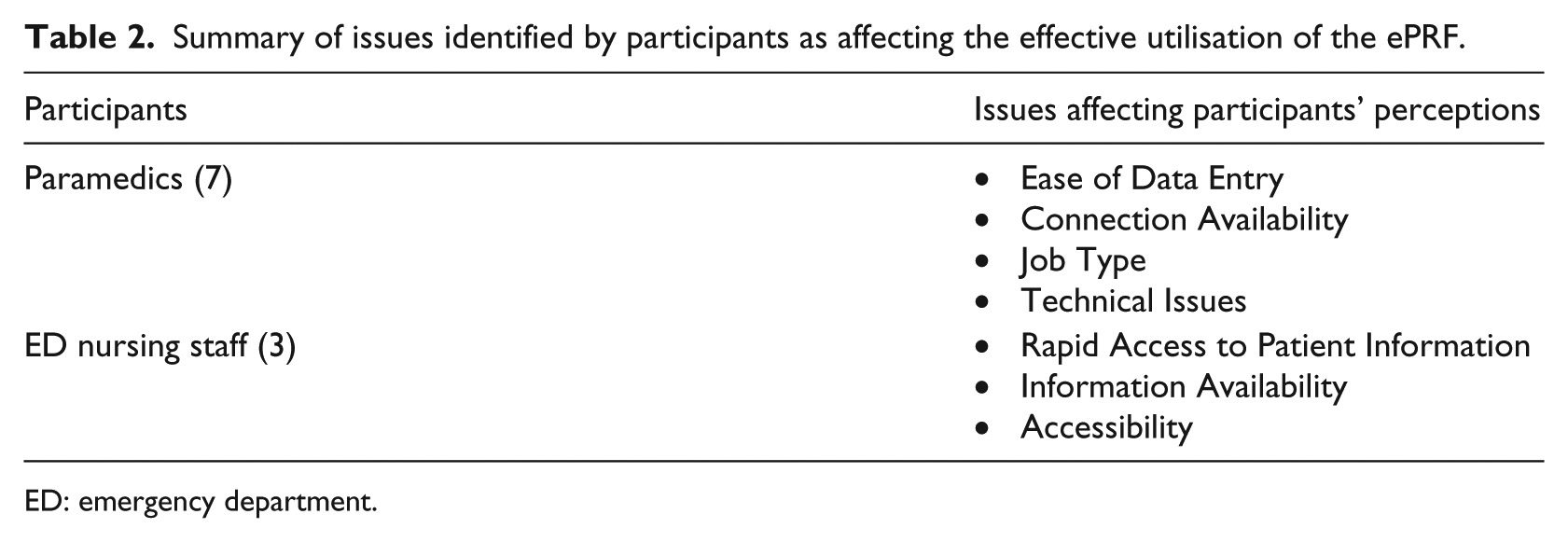
ED: emergency department.
In order to identify the higher level concerns that underlie the immediate issues, for each one we have sought to answer the following questions:
What is the immediate cause of the issue?
Does the issue arise as an identifiable consequence of specific choices or decisions?
Are there ways in which its effects could be removed or ameliorated, whether through the use of technology or other changes?
In doing so, we have also tried to classify the nature of the barrier using the categories from Rogers 16 and Greenhalgh et al. 17 and hence to consider whether the issue might be converted from being a barrier to forming a benefit or advantage.
Ease of Data Entry. Data entry needs to be undertaken regardless of record format. The issue here is the additional time required for data entry in the ePRF compared to the PRF. The cause of this is the navigational challenge stemming from the limited size of the Toughbook screen, requiring that the ePRF be made up of a set of screen-sized pages. The ePRF is structured using a set of tabs, with each tab having up to two further levels of sub-tab, requiring navigation up and down. In contrast, the PRF is contained on a single A3 sheet, and navigation around this is limited to spatial positioning of boxes on a fixed and known grid. Complicating factors are that extra fields have been introduced in the ePRF (requiring more tabs), and some fields have been made mandatory. Essentially, this is an unavoidable consequence of employing an electronic format. While A3-size flexible screens may be available in the future, they are currently not an option in this context. In addition, while including the additional and mandatory fields was obviously viewed as an opportunity from the perspective of those commissioning the system, they are concerned with enhancing data collection rather than meeting operational needs, and require further navigation. The problem stems from a perception of increased ‘complexity’ with additional navigation viewed from the perspective of the paramedics, although clearly the benefits are recognised. The issue cannot be eliminated with the current technology. Two opportunities for amelioration are to provide users with a choice of navigational models and introduce different navigation structures for red/green jobs, perhaps by providing a different set of tabs for green jobs, thus reducing the required interaction. However, using different structures might potentially add to the cognitive load already placed upon the user.
Paramedics did identify some related opportunities related to the use of the Toughbook. These included providing additional information or guidelines for treatment and adding a facility for spell checking and auto-correction; including these might improve the acceptability of the ePRF in terms of ‘relative advantage’.
2. Connection Availability. Connectivity is obviously a necessity for any information transfer to occur. The (non-technical) connectivity problem here relates to the system design. The primary cause is that the Toughbook needs to be connected to the remote NEAS server rather than directly to an ED facility (which is likely to be adjacent) so data flow from the ambulance to NEAS Headquarters and only then are they available to the ED, an unnecessary interposition. This data flow appears to be a consequence of focusing upon the needs of NEAS management and therefore treating this as a database system rather than as a system for transferring operational information. As such, it represents a ‘compatibility’ barrier for the actual users who are concerned with the needs of the patient at the ED, not the completeness of the records making up the NEAS database. Changing the information flow so that it flows from the ambulance directly to the ED and then to the NEAS database would improve all connections and be simpler to use.
The current information flow structure can be viewed as a fundamental design flaw which stems from prioritising an administrative need over an operational need. The system, as a whole, needs to be (or at least thought of as being) a real-time ‘command and control’ system rather than as a database system. Doing so would probably also assist with improving the ‘observability’ benefits of using the ePRF.
3. Job Type. The impact of job type as an issue around data entry was raised only by paramedics. The cause would appear to be that the design of the ePRF focuses upon its role as a means of collecting and recording data, rather than the role of the data itself, and the way that the user interacts with the system. This is probably a further consequence of the focus placed upon recording data rather than upon its operational use.
Currently, users are presented with an unnecessarily inflexible system that creates (perhaps unnecessary) ‘complexity’ and lacks scope for ‘trialability’. We have suggested one simple way of reducing navigational burden by providing two separate interfaces in our analysis of item 1 above. However, it may be that there would be more value in allowing paramedics greater freedom to organise data entry in a more task-related manner to fit the needs of different jobs. As long as all of the required fields are completed and the needs of both the ED and NEAS management are satisfied, the way this occurs could be left to the preferences of the paramedics rather than be imposed upon them.
4. Technical Issues. From the descriptions provided by the paramedics, these appear to relate to the performance of the underlying operating system. We lack detailed information about the examples of such incidents as frozen windows, cited by the interviewees, and so can only speculate about this one. However, the cause seems to be the use of a commercial operating system (Windows)
3
that was designed for general-purpose office and home use. This means that system housekeeping may not be under the control of the users. This choice is probably a consequence of NHS procurement processes, and probably also of available developer skills. A more robust platform such as Linux might well address this problem, but would require quite extensive re-development.
Overall, it is surprising that a general-purpose operating system was used in this role, suggesting that lessons from the London Ambulance Service fiasco 25 in the early 1990s may no longer be a part of collective memory.
5. Rapid Access to Patient Information. This issue was one of those identified by the ED staff and concerns delays in being able to access the ePRF after arrival. The cause of this is the same as that discussed in Issue 2 above namely, the system requires that data be sent to NEAS before it can be relayed to the ED. As before, this is a consequence of designing this system as a database management system (DBMS) rather than a ‘command and control’ system handling operational data. As a result, both priorities and system architecture are ill-suited to the range of roles the ePRF has. The primary means of eradication would be to upload the data directly to the ED as already suggested for Issue 2. The suggestion from ED staff of making some form of printout available may also help reduce the risk of errors arising from over-reliance upon verbal handover.
In many ways, this mirrors the connectivity issue identified by the paramedics and, again, if addressed would assist with providing ‘observability’ for the benefits of using electronic information transfer.
6. Information Availability. The primary concern here is with providing appropriate information to the ED both in advance of patient arrival and at handover. The cause of the concern is that ED staff do not wish to be making potentially inappropriate preparations or treatments based upon the information from the original call. This is again a consequence of information currently needing to be routed to NEAS before it is provided to the ED. It is further complicated by the verbal interaction between the caller and the NEAS call handler, which involves providing information within a stressful situation and the various issues identified above. Until arrival at ED and the start of handover, the best knowledge about the patient is that possessed by the paramedics. The issue might be ameliorated by streaming key fields from the ePRF to the ED (including any changes).
7. Accessibility. Once again, this issue was raised by the ED staff. The cause of the problem is the addition of a role-based access control (RBAC) model to the system as a mechanism to ensure data protection for the information in the NEAS database. This appears to be a consequence of the records being treated as confidential personal data that has become the responsibility of NEAS and for which system governance requires that suitable protection be provided. Data protection is indeed an important issue, but the use of RBAC may be an inappropriate overhead within a context such as an ED, where the focus needs to be upon the patient rather than on the data. In particular, decisions about who should have access to critical patient information, and how this should be protected, should really be the responsibility of the ED, not of other agencies.
Perhaps understandably, the emphasis upon data rather than operational issues is a big factor here. The main barrier is really one of ‘compatibility’ with NEAS seeing the key need as data protection, while the ED is concerned with patient treatment.
Some of the factors affecting these information transfers are the social and human interactions between the two parties, the availability of structured protocols to help manage this process, the level of terminology used to convey information, and the nature of the information transferred and needed.26–29
Even with more accurate information transfer, there appears to be no path for integrating the information from an ePRF into other hospital records, not least because only a limited number of ED staff have access rights. This leads to fragmentation of patient information. In contrast, a paper PRF can be attached to ED patient records, facilitating access to the data by all ED staff, ward staff, and staff in other departments.
Again, this highlights the limitations of designing such a system around a database architectural style. The barriers introduced include both ‘relevant advantage’ and also ‘compatibility’.
Summary of factors
In the above analysis, the causes explain why the different stakeholders (paramedics and ED staff) see particular issues as being barriers to adoption and effective utilisation, while the consequences identify the reason why these arise. Our concern here is therefore with elucidating the key factors that emerge from the consequences. There are three of these:
The system architecture. While the system needs to support operational decisions, particularly those made by ED staff, it has been designed around a central database architectural model. Data entry, access, and so on are then subordinate to the creation of an accurate database record. Fundamentally, the system architecture is unsuited to the purpose. [Issues 2, 3, 5, and 6]
The user interface. This is related to the system architecture, in that it would appear that the use of the system, ranging from data entry to clinical use of the information in ED, is constrained by the database context. Ensuring data integrity is the major goal rather than ensuring data availability. [Issues 1, 3, 6, and 7]
System procurement. This has clearly been based upon the requirements of one group of stakeholders (NEAS management) rather than the shared concerns of the different stakeholders and potential stakeholders, such as other hospital departments. The choice of a centralised database architecture itself largely stems from this. [Issues 1, 2, 3, 4, 5, 6, and 7]
In the next section, we discuss these factors and the lessons they provide.
Discussion
The move from a paper PRF to an ePRF has the potential to enhance the experiences of all of the stakeholders involved in handover at the ED, and as such, its adoption was a sound move on the part of NEAS. It can assist with improving communications between NEAS and the receiving locations, assist with selection of an appropriate health service pathway to alleviate pressure on scarce resources, and improve reporting of information about patients. Unfortunately, due to the factors identified in the preceding section, this potential has yet to be fully achieved.
We should also observe that both the literature and this study identify the handover process as being problematic, and it is one in which the people involved may react differently and have separate perspectives arising from cultural, organisational, and individual characteristics.26,30 These differing reactions and perspectives can create communication gaps that may accrue throughout the care process with potentially serious impact upon patient safety or treatment appropriateness.28,31 That said, although we observed that the use of the ePRF could and sometimes did create additional stress, many paramedics did prefer using it, as against the PRF, while at the same time still wishing to see improvements.
In the rest of this section, we consider what lessons could usefully be learned from the impact of these three factors, and discuss how it might be possible to reduce or remove some of the barriers that they create for the handover process.
The system architecture
As we noted, the choice of a centralised database architecture stems from the focus upon the needs of one stakeholder (NEAS management). Such an architectural form is inherently unsuited to the needs of a complex environment such as the ED in a hospital and the interactions that this involves. Consequently, while the use of a database to support the processes involved in handover is indeed appropriate, not least as a means of ensuring that multiple copies of patient information are not in use concurrently, it should not be the ‘controlling’ element.
This raises three questions:
(a) What might be a more suitable architectural form?
(b) Can the present architecture be modified to meet the needs of all stakeholders?
(c) What design process might have created a better architecture?
Given that the role of the system is one of information management and communication, and that many of the stakeholders will access this information remotely, the answer to the first question could be provided through the adoption of a client–server architecture, where the different stakeholders have separate client roles. Such a choice would also provide scope to answer our second question, since it would be possible to retain the existing database as a central element of the server (and therefore preserve data integrity).
We can answer the third question by observing that this procurement could well have been an exercise in co-design, involving participants from all of the stakeholders. However, not only was this lacking between the agencies concerned, it also seems to have been lacking within organisations including NEAS itself. We noted two examples of this: NEAS did not involve either its own paramedics or other agencies in the design and implementation of the ePRF; and within the hospital there are no existing mechanisms to aid with sharing patient information from the ED with other departments.
Although there is a strong sense here of an ‘opportunity missed’, there seems no reason to believe that it could not be remedied, providing that some shared overarching motivation could be found. We return to this point later.
The user interface
In their current form, the interfaces provided for both paramedics and ED staff are focused upon the structure of the data, rather than upon its immediate role as a source of knowledge about the condition of the patient. It would perhaps be better to view the process of handover as a ‘case conference’ related to the patient – where the barriers to sharing knowledge need to be overcome in the interests of the patient. 32
If we take that view, then the user interface(s) to the system can be considered as having two main roles:
(a) Data entry by the paramedics;
(b) Sharing of information during handover.
For data entry, it is impossible to avoid some segmentation of the ePRF since it needs to be mapped onto a small screen. One approach may be to provide different structures for ‘red’ and ‘green’ jobs. These could have slightly different interface structures, or the hierarchy of tabs could ensure that common information is entered first. Doing so would also provide ambulance crews with an element of choice about how the task was performed. It could also be accompanied by a ‘validate’ button to allow them to check whether all of the key elements were complete, giving a sense of control over their actions that might help with finding better ways to perform this task (appropriation). 18 Furthermore, user-activated facilities such as a spell checker could also be provided.
The information transfer during patient handover clearly needs to be improved so that it is seen to assist ED staff, rather than forming an administrative overhead. Relatively simple steps that could be used to address this include using a different mechanism for ‘signing’, removing joint signing as a mandatory action, and possibly providing a printed copy of the ePRF for ED staff. Overall, this really needs to be designed as a shared work task, and as noted earlier, responsibility for managing access control should be assigned to the ED staff.
System procurement
It can be argued that all of the problems identified in our analysis stem from failures in the procurement process. However, we should note that these are essentially systemic ones of the NHS and its organisation, rather than some specific failure on the part of NEAS.
The key problem is that for system developments such as this, with effects spanning across multiple agencies, there is no one NHS agency with both a holistic view of the procurement package and process and the authority needed to influence it. The current constitution of the NHS fragments responsibility and militates against collaborative developments, promoting procurement through a single agency.
Factors needed for success
Here we briefly return to the earlier discussion of the key factors identified by both Greenhalgh et al. 17 and also Rogers 16 as influencing adoption of technical innovations, examine their relevance to this study, and consider how our suggestions might affect them.
Relevant advantage. Paramedics showed some ambivalence about the benefits of the system, while ED staff tended to view it as an impediment to effective work practices. However, improvements to the user interface and to the handover process could probably largely remove this particular barrier.
Compatibility with the norms, needs, and values of the adopter. This was probably achieved for NEAS management but less so for the ED staff. However, an improved and shared handover process, together with the transfer of responsibility for access control to ED, should help achieve compatibility for all users.
Complexity in use. The main impediment here is that of data entry. Greater attention to the ideas of Interaction Design 33 should be able to reduce the negative aspects of this.
Trialability. The need to follow well-established procedures means that this is unlikely to be a key factor for a system such as the ePRF.
Observability. Apart from NEAS management and some of the paramedics, the ePRF is not perceived to be conferring any benefits to its users. Again, a more shared approach to management of information transfer during handover and to some aspects of data entry could widen its acceptability among the stakeholders.
Reinvention. The need to follow procedures probably limits scope for this. However, there is scope to provide paramedics with more choice and control about how they perform the task of data entry.
Arguably, where these do form a barrier to adoption, the underlying cause is one of a lack of a collaborative culture for implementing and introducing new technology.
Limitations of the study
The two factors that we consider most likely to affect the validity of the findings from our study are concerned with the way that the study was conducted, and with our analysis of the results.
With regard to how the study was conducted, we would observe the following:
In the period since we made our observations, the ePRF has been updated to a newer version. Since the changes are largely concerned with the user interface, it appears unlikely that this change would make any difference to the issues that we discuss in this article.
We were only able to interview three ED nurses. One had much more experience than the other two and acted as the main source of information for many topics. So it is possible that this may have introduced some bias and that some issues may have been missed. However, the responses from the interviews do triangulate well with our observations made at handover (and obtained over a number of sessions).
Our observations were conducted in a single ED. Since the interface provided by NEAS is standard across EDs, we have no reason to consider that the experiences from this department were not representative of others.
Our analysis of the results, being largely qualitative, is vulnerable to inconsistent interpretation of the interview responses and the notes from observations. Again though, we were able to address this by the use of triangulation between the sources. Our suggestions about the possible improvements that might be made inevitably involve an element of extrapolation regarding the technological issues. However, we would also argue that the problem identified with system procurement is indeed systemic and that a major value of this study is to illustrate the consequences for the procurement of software systems, of whatever form, that can arise from adopting this approach.
Conclusion
Returning to our original research question, regarding the factors that limit the effectiveness of electronic information transfer in the context of handover, we have identified two such factors that are ‘technical’ in nature: an unsuitable system architecture and poor design of the user interfaces for both paramedics and ED staff. A third factor concerns how such systems are procured.
These factors are, of course, entwined and, as we have argued, many aspects of the technical factors can be viewed as stemming from the way that procurement of such systems is organised within the NHS. However, we should also acknowledge that federal systems, such as the NHS, do present inherent challenges to procuring IT systems that can be used to maximum effect across and between agencies.
To end on a positive note, there seems to be good scope for this system to evolve in the future from a management-facing record system to one that can also provide useful operational support. Achieving this mainly requires a different perspective regarding its role rather than widespread and expensive technical changes.
Footnotes
Acknowledgements
The authors would like to thank the staff of the NEAS, and Graham McClelland in particular, for their cooperation and help with this study. They would also like to thank staff and management of the ED that allowed them to observe handovers and answer questions during busy work periods. The study has obtained ethical approval from Durham University, NHS Health Research Authority (Protocol No. ESC2/2013/20).
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
