Abstract
This study identified the readiness factors that may create challenges in the use of telemedicine among patients in northern Louisiana with cancer. To identify these readiness factors, the team of investigators developed 19 survey questions that were provided to the patients or to their caregivers. The team collected responses from 147 respondents from rural and urban residential backgrounds. These responses were used to identify the individuals’ readiness for utilising telemedicine through factor analysis, Cronbach’s alpha reliability test, analysis of variance and ordinary least squares regression. The analysis results indicated that the favourable factor (positive readiness item) had a mean value of 3.47, whereas the unfavourable factor (negative readiness item) had a mean value of 2.76. Cronbach’s alpha reliability test provided an alpha value of 0.79. Overall, our study indicated a positive attitude towards the use of telemedicine in northern Louisiana.
Introduction
LeRouge and Garfield 1 indicated that a critical need exists to bolster telemedicine throughout the United States. However, this need may only be fulfilled if the challenges involved in implementing telemedicine can be clearly identified. There is a lack of formal analysis of the appropriateness of the use of telemedicine during the prevailing circumstances, 2 and its adoption among clinicians is slow.3,4 The American Telemedicine Association (ATA), whose global advocacy promotes the use of telemedicine, reports that telemedicine is a highly valued growth component of health services in the United States. According to the ATA, the telemedicine market is growing rapidly with both public and private insurers covering payments for telemedicine just as they do for in-person services, citing several prominent studies that demonstrate its cost-effectiveness over in-person services. 2
In the coming years, technologic advancement, patient and physician technology adeptness, the shortage of providers, telemedicine successes and financial incentives are likely to make telemedicine a substantial channel for healthcare delivery.5,6 The rural populations stand to benefit from care delivery through telemedicine with improved cost efficiency, better access and greater compliance. 7
This study examines the acceptability of telemedicine that considers the perceptions of patients from rural and urban regions of northern Louisiana. The study also hypothesises that patient readiness is affected by such perceptions. This exploratory research aims to answer the following question: ‘What is the extent of patient readiness for the use of telemedicine services and what are the perceptions (positive and negative) that must be addressed?’ Specifically, we focus on patient readiness for the use of telemedicine in clinical specialty consults. A combination of parameters from the Technology Acceptance Model (TAM) 8 and the Fit between Individuals, Task and Technology framework (FITT) 9 (Figure 1) was applied in this study to the data collected using the survey instrument.
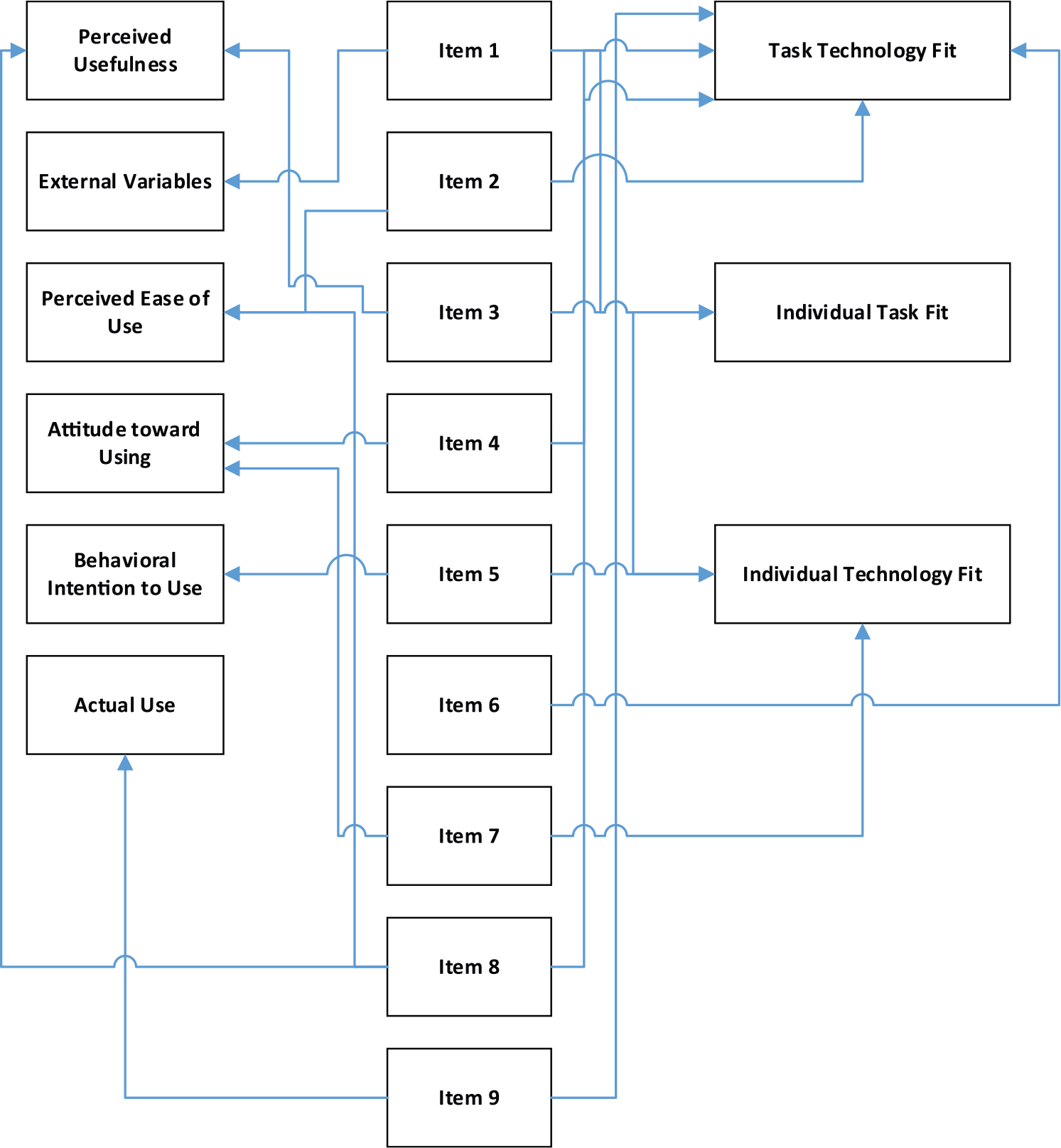
Integration of FITT and TAM frameworks using the survey instrument.
Literature review
The role of telemedicine clinical oncology practices has been evolving in many regions of the United States, thereby providing supportive care including pain assessment, nutrition and patient education. 10 Although physicians may treat patients with many diagnoses that usually require physical exams and diagnostic tests, 11 a clear indication exists regarding the need for additional technology to support these processes. Wootton 12 conducted a qualitative study to assess the value of telemedicine in the management of five common chronic diseases (chronic obstructive pulmonary disease (COPD), asthma, diabetes, heart disease and high blood pressure) and concluded that the value of telemedicine in managing chronic diseases is not substantial. In contrast, Cusack et al. 13 listed the various benefits of telemedicine with many different types of cases and suggested that the benefits outweighed the implementation costs. Recent studies have shown that a telemedicine system may aid the delivery of neuro-oncology, chemotherapy, stroke treatment and other time-sensitive treatments safely and effectively, with high levels of patient satisfaction and improved patient monitoring, adherence and knowledge.14,15
The consensual concerns expressed by physicians call for policy makers, academia, patient advocacy groups and private-sector organisations to create partnerships to rapidly test, evaluate, deploy and pay for new care models that use telemedicine. 16 State-by-state licensure and encumbrances imposed by some states impede the adoption of telemedicine. Telemedicine provides a much-needed union of integrated care through the combination of technology, business and clinical processes. 17 However, the use of telemedicine should be optimised to improve patient-centred outcomes at the population level with proper integration of telemedicine with the existing care delivery system resulting in better provider–patient and provider–provider relationships.18,19
In addition to the well-perceived potential benefits of telemedicine, the prior studies demonstrated that telemedicine utilisation results in better healthcare access and quality at lower costs.10,11 For treatments such as chemotherapy that require regular case reviews, telemedicine may be a simple and efficient approach that is cost-effective, safe and associated with good outcomes. 7 Although the observational studies conducted by Jhaveri et al. 20 found that outcomes were favourable for telemedicine compared to face-to-face care delivery, the patient satisfaction element of telemedicine requires further exploration. 21 Highly important to the creation of the collaborative partnership necessary for successful implementation of telemedicine is the establishment of strong relationships between the physician and the remote clinician (nurse/medical assistant) as well as the remote patient. 22
In many states, simultaneous video and audio consultation only constitute the use of telemedicine. Beyond the real-time remote patient consultations, telemedicine should also comprise the remote monitoring of patients’ vital signs and conditions, the storage and forwarding of diagnostics and analysis, and the provision of specialised patient care services. Additional guidelines and standards from the ATA such as clinical guidelines for telepathology may enhance the widespread adoption of telemedicine. 23 From the FITT perspective, the successful adoption of telemedicine depends on its ability to provide the right information to the right individuals at the right time. 24
Study overview
In this study, we analysed the data by combining elements from two of the well-known theoretical models. TAM analyses the technology acceptance by the individual, the technology and the management and implementation contexts, and explains the adoption by healthcare professionals. FITT analyses the technology adoption in clinical settings based on the fit between the object attributes of the individuals, technology and clinical tasks by including individual-task, individual-technology and task-technology. The investigators examine the patient readiness for telemedicine use or the diffusion of technology by combining the attributes from the TAM and FITT frameworks. The data collection reflects the patient and physician perceptions regarding usage rather than the actual use of the technology. 25
Based on the literature review, the investigators developed the survey instrument and conducted the survey among a representative sample of patients from the rural and urban population in and around Shreveport, Louisiana. Whereas the general goal of the survey was to identify the readiness of patients in terms of positive and negative perceptions of telemedicine use, the specific aims of this instrument with respect to the oncology practice in northern Louisiana were as follows:
Identify the perceptions regarding telemedicine use between individuals of different genders;
Identify the perceptions regarding telemedicine use between individuals of different education levels;
Identify the perceptions regarding telemedicine use between individuals of different ethnic groups;
Identify the perceptions regarding telemedicine use between individuals of different household income levels.
The investigators obtained 147 responses as detailed in Table 1. The sampling method used was convenience sampling, based on the clinics that were willing to participate in the study. The survey instrument consisted of two sections: (a) patient perspectives and (b) patient demographics. Perception questions (based on psychometric analysis) required a 5-point Likert-scale response (1 = strongly disagree through 5 = strongly agree) that would help analyse the responses by fitting them into a statistical model to assess the required readiness factors.
Demographic characteristics of the sample.
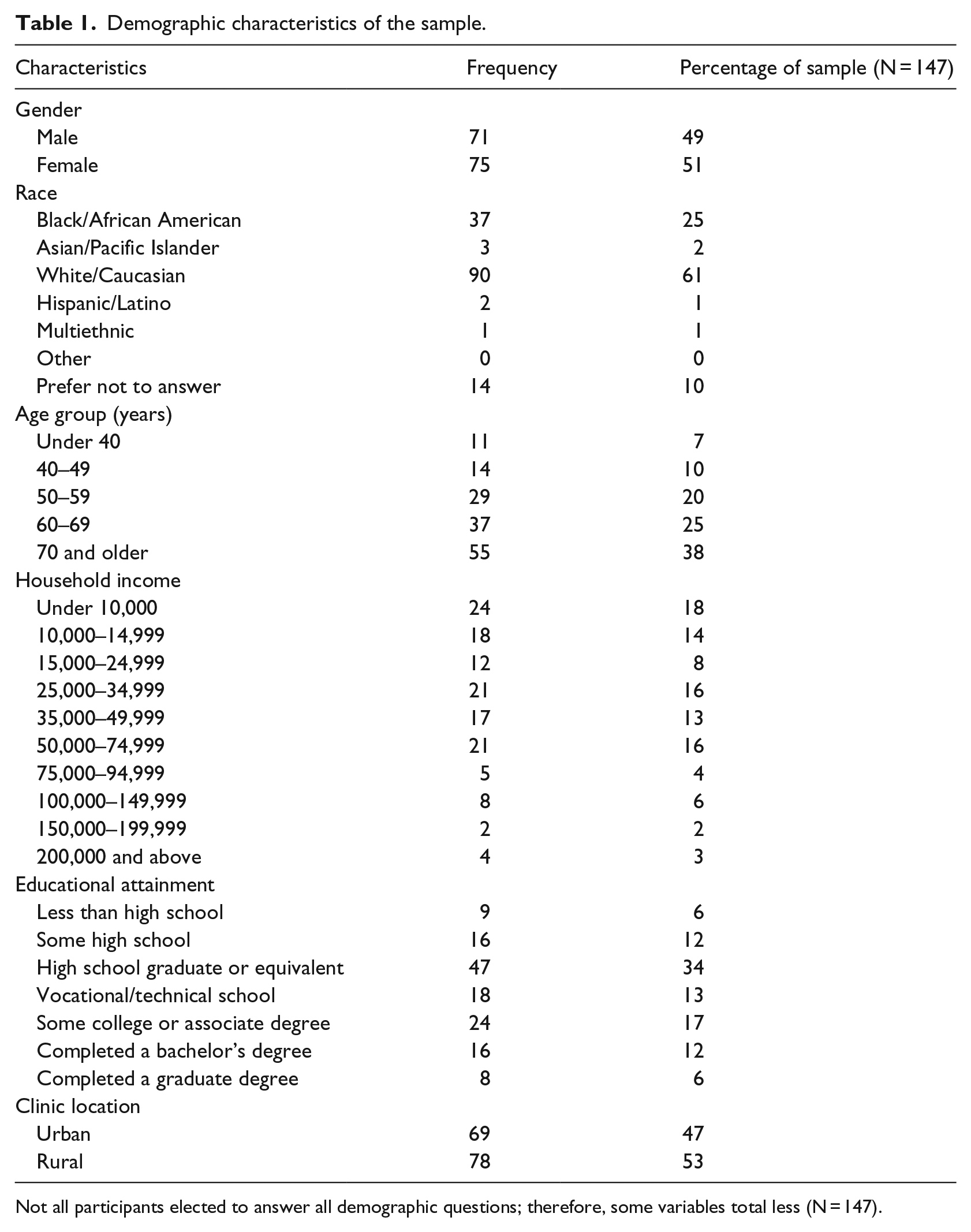
Not all participants elected to answer all demographic questions; therefore, some variables total less (N = 147).
Methods
The survey instrument was developed through a mix of questions with proper negation that were randomly sequenced to minimise the potential ceiling effects in data collection. After coding (and recoding with reverse scale for negatively worded questions) the survey responses, the investigators performed both descriptive and inferential statistical analyses on the model parameters, using IBM SPSS 22. They performed statistical analyses (correlation, exploratory factor analysis and alpha analysis) to evaluate the reliability, convergent validity and discriminant validity of the responses. The responses were tested based on the models to measure the readiness of the patients to use telemedicine and to identify the barriers for telemedicine utilisation from the patient perspective.
Analysis was performed on each of the response variables to obtain the descriptive statistics, central tendency and response pattern. Considering the Likert-scale responses as ordinal, a correlation bivariate analysis was performed to determine the direction and strength of the linear relationships between the responses. Combining the concepts of the theoretical TAM and FITT frameworks, the responses were grouped into positive and negative readiness indicators. The positive readiness indicators were the perceptions regarding benefits (travel cost savings, less waiting time), motivation (better feedback, quicker response time), compatibility and relative advantage (easier accessibility and better availability of specialists) in using telemedicine. The negative readiness indicators were the perceptions concerning anxiety (suboptimal comprehension, decreased communication) and complexity (complicated technology).
The analysis was performed starting with factor analysis to reduce the components to a single dimension and to compute the corresponding weighted factor scores (weighted readiness scales). For the weighted factor scores, we used the following computation:

where
Additionally, we performed analysis of variance (ANOVA) on weighted factor scores based on different demographic categories: gender, income group, education level and ethnic group. The hypotheses are given below, with a significance level of 0.05:
Finally, we performed ordinary least squares (OLS) regression analyses to estimate the influence of the demographic factors such as ethnicity, age and income on weighted factor scores (readiness scales).
Survey development integrating FITT and TAM models
The survey instrument developed by the investigators integrates both FITT and TAM models. Here, Item 1 targets external variables from the TAM model by including gasoline cost and distance from the clinic and the Task-Technology fit from the FITT model. Item 2 identifies the ability of the patient to understand the physician through telemedicine, thereby covering ‘perceived ease of use’ from the TAM model and the Task-Technology fit of the FITT model. Item 3 inquires about the physician ability to understand the patient, thereby indicating the ‘perceived usefulness’ criteria from TAM and the Individual-Task fit from FITT. Item 4 tests the patient attitude towards using telemedicine from TAM and the Task-Technology fit from FITT. Item 5 focusses on ‘behavioural intention to use’ from TAM and the Individual-Technology fit from FITT because it inquires about the possibility of improving feedback through telemedicine. A focus on the reduction in response time is indicated in Item 6 using telemedicine, thereby covering ‘perceived usefulness’ from TAM and the Task-Technology fit from FITT. The investigators determined whether telemedicine was too complicated through Item 7, which covers ‘perceived ease of use’ from TAM and the Individual-Technology fit from FITT. Item 8 targets the ‘perceived usefulness’ from TAM and the Task-Technology fit from FITT because it probes whether the individual would be interested in using telemedicine rather than driving to a bigger city. Finally, Item 9 focusses on the ‘actual use’ criteria of TAM and the Task-Technology fit from FITT.
Results
The results gathered indicated that the patients were reasonably ready to use telemedicine and needed more exposure, education and opportunity to utilise the telemedicine services effectively. Nevertheless, telemedicine services are not commonly offered by physicians in many areas in the United States due to barriers such as licensure, reimbursements, liability and privacy rules.4,5
Factor analysis and ANOVA on weighted factor scores
The factor analysis results from SPSS are shown in Table 2. Principal component analysis was used for the extraction method, and components with eigenvalues greater or equal to 1 were selected as the principal components. Furthermore, the orthogonal rotation method Varimax was used as the rotation method, which helps identify the best dimension to explain total variance.
Factor analysis – principal component results and total variance explained.
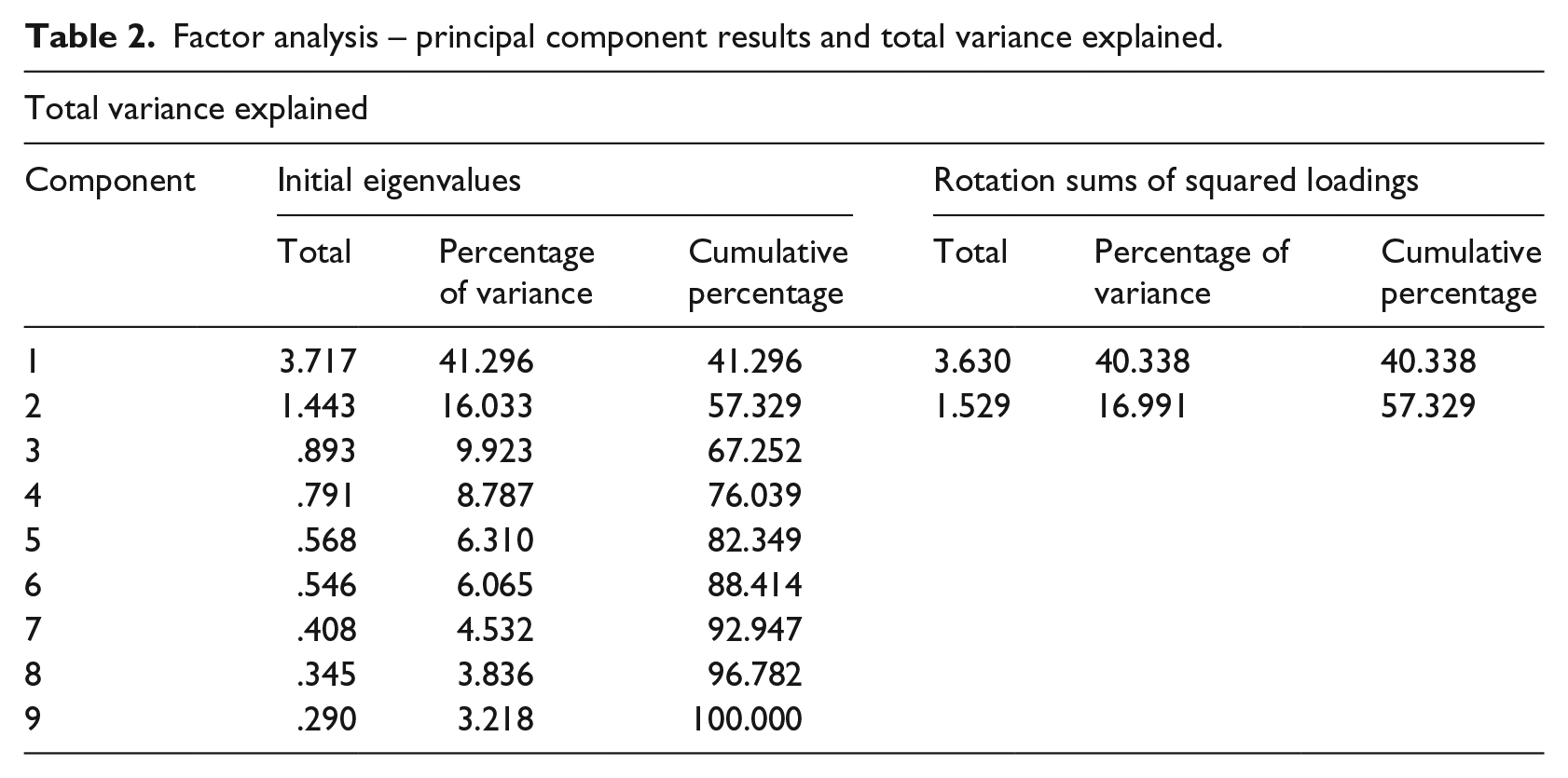
Component 1 had an eigenvalue of 3.717 and Component 2 had an eigenvalue of 1.443. Together they explained 57.33 per cent of the total variance (Table 2). Loadings for each component showed the correlation relationship between the item and its corresponding component. Because the investigators re-coded using a reverse scale for negatively worded questions with the first component explaining the majority of the variance, the items should be reduced to a single-dimension scale. High scores represented positive readiness towards telemedicine, whereas low scores represented negative readiness towards telemedicine. Weighted factor scores were calculated by multiplying loadings with item scores.
High-loading values (Tables 3 and 4) for Item 1 (Cost Savings), Item 4 (Less Waiting), Item 5 (Better Feedback), Item 6 (Quicker Response Time), Item 8 (Easier Accessibility) and Item 9 (Better Specialist) indicated a positive correlation between the benefits, motivation, compatibility and relative advantage in using telemedicine and the total factor scores. Favourable factors contributed positively and highly towards higher weighted factor scores (readiness scores).
Readiness in terms of benefits, motivation and relative advantage.
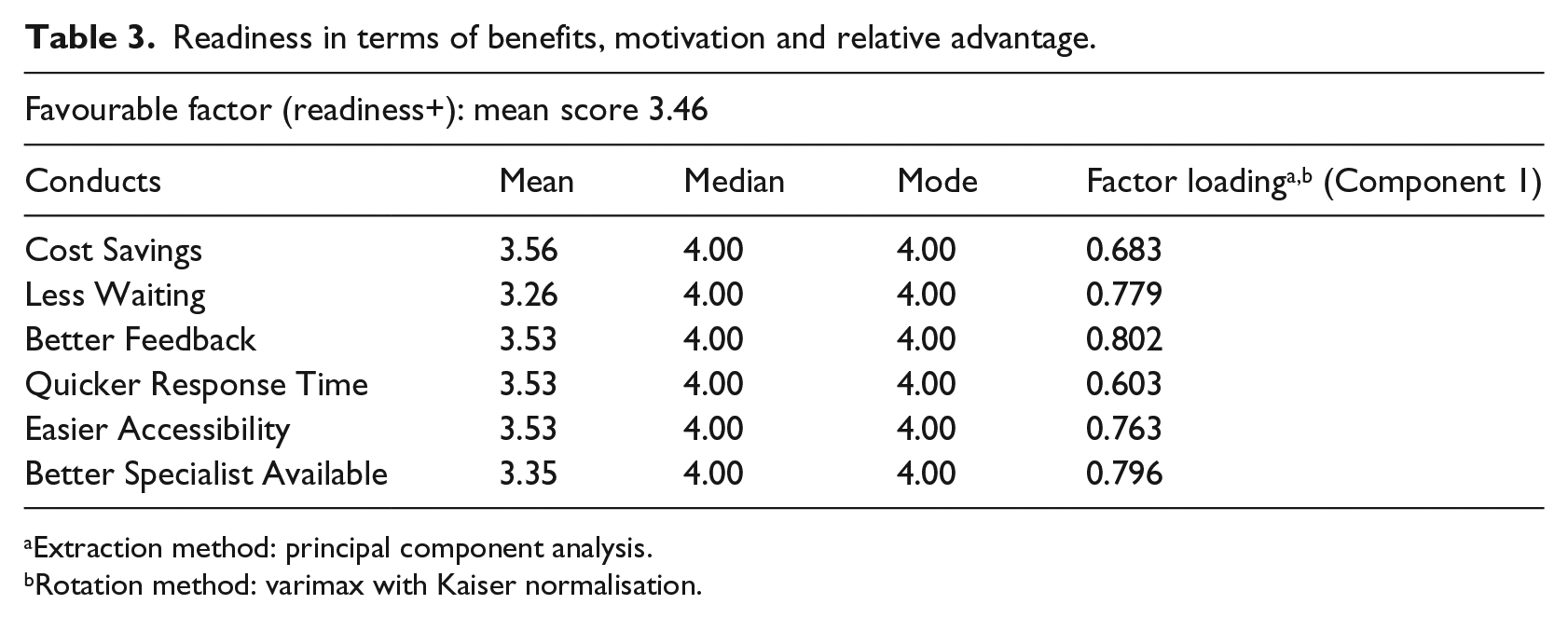
Extraction method: principal component analysis.
Rotation method: varimax with Kaiser normalisation.
Readiness in terms of communication factor based on comprehension, communication and technology.
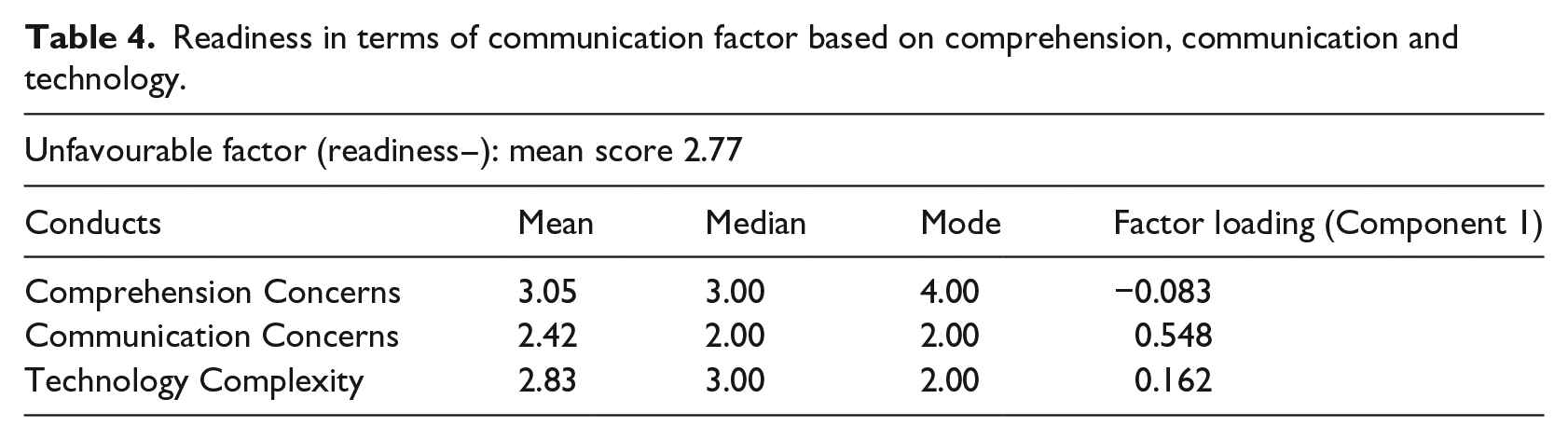
In contrast, Item 2 (Comprehension Concerns) and Item 7 (Technology Complexity) loaded slightly on Component 1, indicating anxiety and complexity, which are interpreted as unfavourable factors that affect negatively towards telemedicine readiness.
Item 5 had the highest loading among all the favourable factors and was therefore considered the salient item. The context of Item 5 is ‘I feel telemedicine can improve patient feedback regarding the side effects of therapy’. Alternatively, Items 2 and 7 contributed nearly equally to the unfavourable factor.
The instrument was validated using ANOVA. Performing ANOVA on weighted factor scores allowed the investigators to identify the significance of the individual demographic variables to the response items listed in the survey. The purpose of performing regression is to identify the standardised coefficients that determine the relative importance between the different demographic variables from the survey. Factor analysis is used to reduce the data dimension to uni-dimension. Reducing the data into uni-dimension aided in calculating the weighted factor scores. Additionally, Cronbach’s alpha coefficient was calculated to test the reliability of the instrument.
ANOVA on weighted factor scores instead of raw data would be more effective. We performed ANOVA to test the hypotheses targeting gender, income, education and ethnic groups independently. Table 5 shows the ANOVA results.
ANOVA hypothesis tests on gender, income, education and ethnic groups.
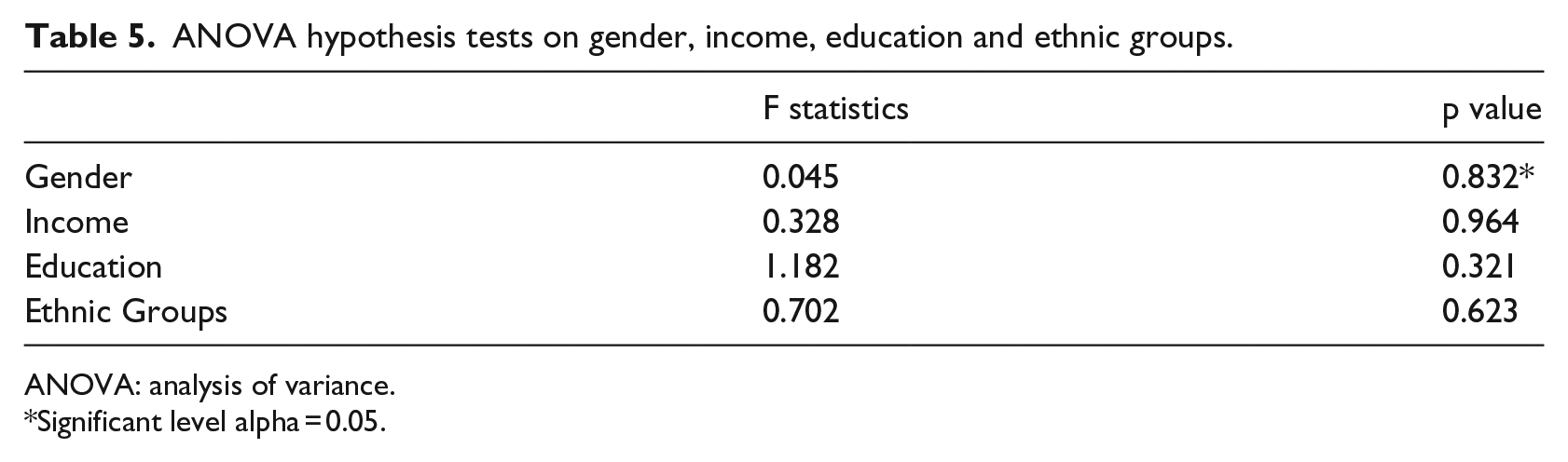
ANOVA: analysis of variance.
Significant level alpha = 0.05.
All the p values of testing on favourable factor scores were greater than 0.05, which indicates that the investigators should not reject any of the null hypotheses and should conclude that no significant difference existed between gender, income levels, education levels and ethnic groups towards the weighted favourable factors. People of different genders, income levels, education levels and ethnic groups showed similar attitudes towards telemedicine readiness.
Descriptive statistics and OLS regression analysis
Favourable factors (readiness+) (mean = 3.47, value >3 is towards agreement with positive perceptions) indicate that the patients agreed with the perceived benefits, motivation and relative advantage. Unfavourable factors (readiness−) (mean = 2.76, value <3 is towards disagreement with negative perceptions) indicate that patients did not tend to agree with the negative perceptions such as communication problems, comprehension concerns and technologic complexity. The details of the individual components are illustrated in Tables 3 and 4. According to these tables, we measured the readiness factor as 0.69 (favourable minus unfavourable factor mean values, that is, 3.46 − 2.77).
A bivariate analysis of Pearson’s correlation (two-tailed) showed significant correlations at the 0.05 level among the items in the scales. Both readiness scales had reasonably acceptable results for the measure of scale reliability. Cronbach’s alpha coefficient of 0.840 (alpha > 0.70) for the six items in the favourable factors suggests that the items had relatively high internal consistency. However, the alpha coefficient for the three items in the unfavourable factor scale was only 0.476 (alpha < 0.70). This finding suggests that the items did not have high internal consistency, which could have been due to the phrasing of one of the questions indicating negative perceptions in the reverse direction.
We were able to draw some inferences from the OLS regression analysis on weighted factor scores based on age, household income, ethnicity and education, which could only explain approximately 6 per cent of the variance in readiness (R2 = 0.0532, F = 0.59, sig = 0.8193 at 0.05). A standard beta coefficient was calculated to compare the relative importance between parameters. Table 6 shows that none of the parameters were significant to the model, which signifies that this model may only be used in descriptive analysis rather than prediction analysis.
Ordinary least square regression result and standardised parameters.
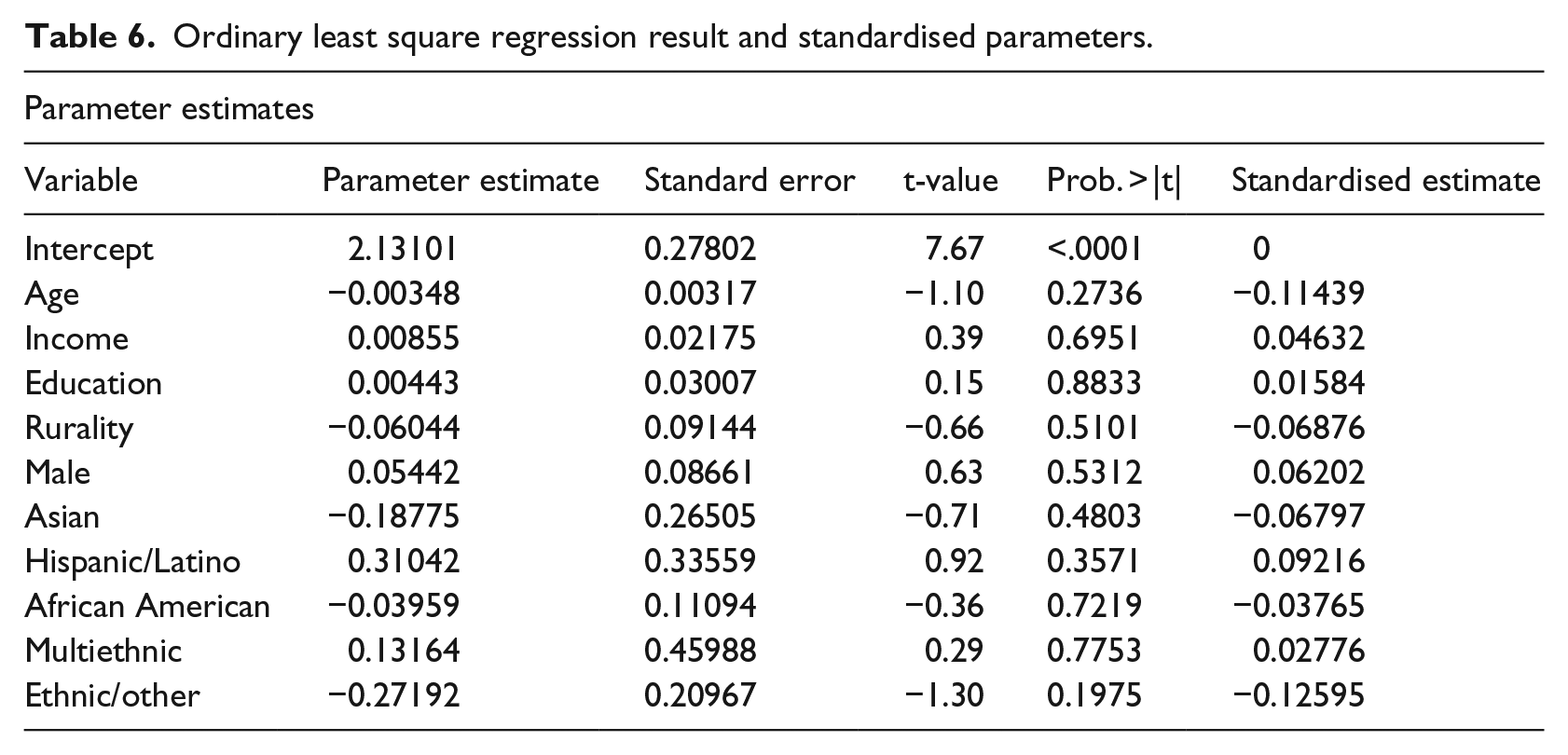
A negative linear relationship trend (standard coefficient: −0.11439) tended to exist between age and agreement. That is, as age increased, item agreement declined. For example, for Item 3, ‘I think that the doctor will be able to understand me through telemedicine video’, a steady decline was observed in agreement from the under-40 age group (73%) to the 70 and over age group (50%). Similarly, in responding to Item 4, ‘I would prefer to see a physician sooner though telemedicine than wait to see a physician in-person’, 82 per cent of participants under age 40 agreed with the statement, whereas only 46 per cent of the 70 and over age group agreed.
The results of the household income variable displayed a sporadic pattern of responses. Moreover, it showed a positive correlation with factor scores (standard coefficient 0.04632), which signified that the greater the household income, the greater the readiness towards telemedicine. No significant differences were found.
Overall, the education variable suggested that those who completed a graduate degree were more polarised, tending to agree with the use of telemedicine at a higher percentage than individuals with lower education levels (standard coefficient 0.01584). For example, in responding to Item 3, of those who completed a graduate degree, 63 per cent agreed with the statement, ‘I think that the doctor will be able to understand me through telemedicine video’, whereas 13 per cent disagreed. For the same item, only 44 per cent of those who completed less than high school agreed with the statement, whereas 44 per cent disagreed. A similar pattern was seen for Item 6, ‘I feel telemedicine can reduce physician response time’, for which 88 per cent of those who completed a graduate degree agreed with the statement and 0 per cent disagreed compared to those who completed less than high school for which 50 per cent agreed and 25 per cent disagreed.
The results for males and females were consistent across the items. Males indicated a higher inclination towards the use of telemedicine than females (standard coefficient 0.06202). The only deviations in agreement (greater than 10 percentage points) occurred with Items 7 and 8. Females (36%) were more likely than males (22%) to agree that the idea of telemedicine sounded too complicated (Item 7). Additionally, males (68%) were more likely than women (58%) to agree that they would prefer to see a specialist via telemedicine rather than go to a big city (Item 8). No significant differences were found (Tables 7 and 8).
Likert-scale analysis of questions related to proximity.
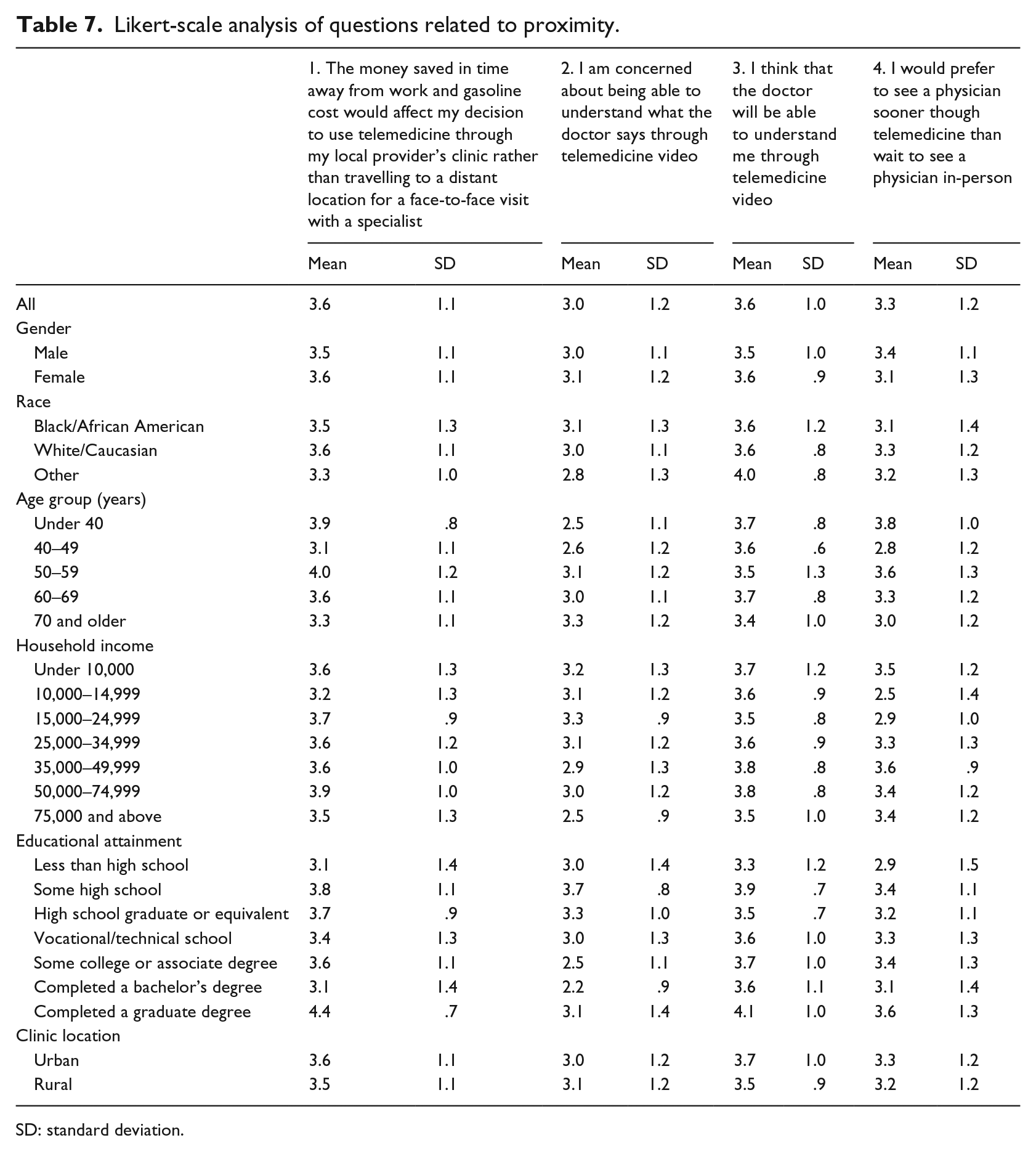
SD: standard deviation.
Likert-scale analysis of questions related to likeability of telemedicine.
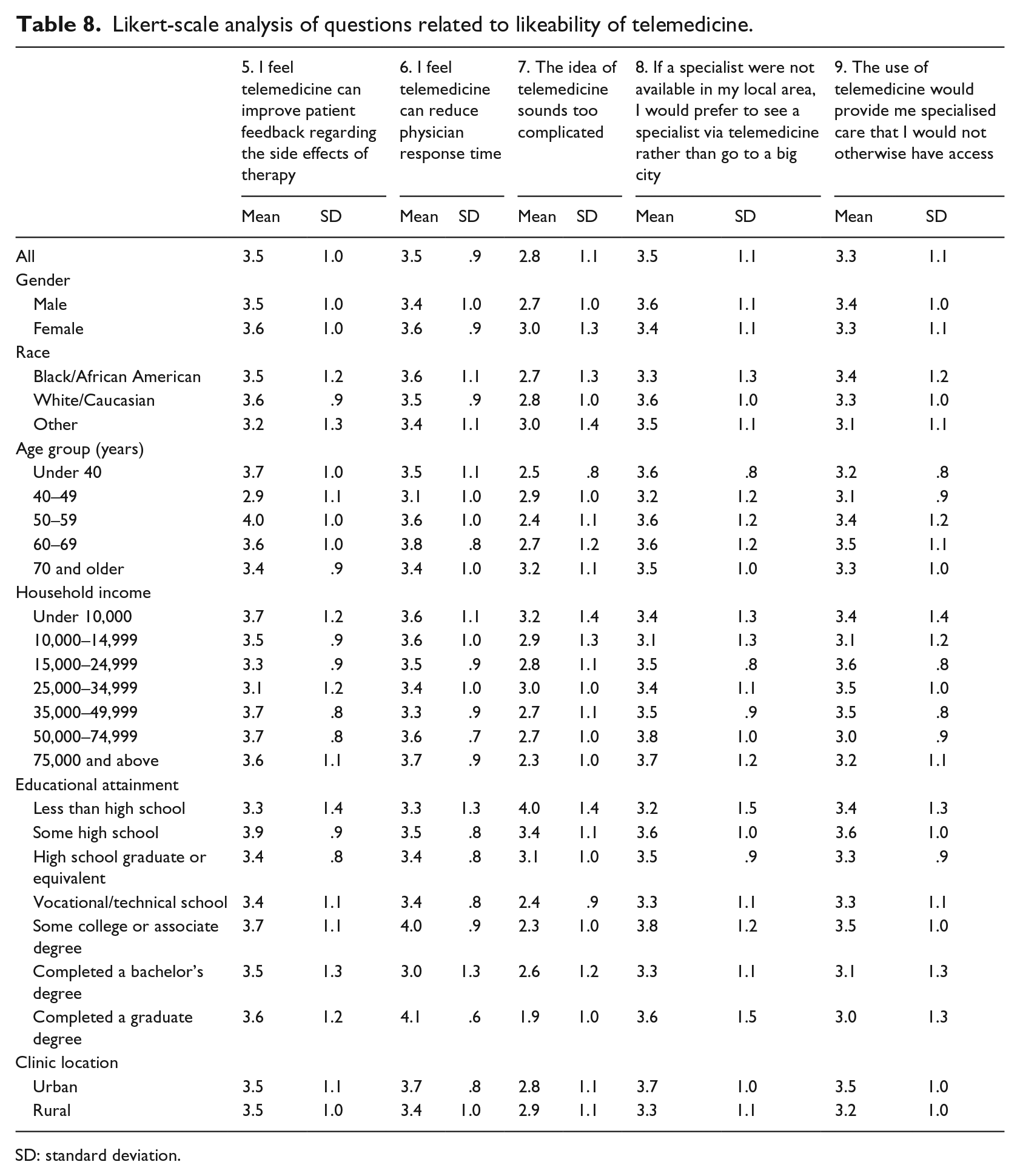
SD: standard deviation.
Across ethnicity, African Americans and Caucasians displayed a consistent pattern of responses with few exceptions. For example, 49 per cent of African Americans compared to 38 per cent of Caucasian participants agreed with Item 2: ‘I am concerned about being able to understand what the doctor says through telemedicine video’. Conversely, Caucasian participants (66%) were more likely to agree with Item 8, ‘If a specialist were not available in my local area, I would prefer to see a specialist via telemedicine rather than go to a big city’, than African-American participants (54%). African-American participants also disagreed with Items 1, 3, 4, 5, 7 and 8 at least 10 per cent more frequently than did Caucasian respondents. No significant differences were found.
The response patterns of the rural and urban participants were very similar with most items agreed and disagreed upon at a similar rate. Rurality showed a negative correlation with the weighted factor scores (standard coefficient: −0.06876), which indicates that individuals from rural areas had a higher tendency to reject telemedicine. The only exceptions were the responses to Item 3, ‘I think that the doctor will be able to understand me through telemedicine video’, and Item 8, ‘If a specialist were not available in my local area, I would prefer to see a specialist via telemedicine rather than go to a big city’. For Item 3, 69 per cent of the urban sample agreed with the statement compared to 58 per cent of the rural sample. Similarly, 70 per cent of the urban sample agreed with Item 8 compared to 57 per cent of the rural sample. No significant differences were found.
Participants tended to agree with the survey items, indicating a positive association with telemedicine. For example, 61 per cent of the sample agreed with Item 1, ‘The money saved in time away from work and gasoline cost would affect my decision to use telemedicine through my local provider’s clinic rather than travelling to a distant location for a face-to-face visit with a specialist’, whereas only 18 per cent of the sample disagreed with the item. Similarly, over 60 per cent of the sample agreed with Item 3, ‘I think that the doctor will be able to understand me through telemedicine video’, and Item 8, ‘If a specialist were not available in my local area, I would prefer to see a specialist via telemedicine rather than go to a big city’.
Discussion
The readiness factor of 0.69 (values may vary from −4 to +4) indicates that the patients had positive perceptions towards the use of telemedicine in northern Louisiana. However, the relatively moderate scores (preferred score is closer to +4 with readiness+ closer to 5, herein 3.46 and with readiness− closer to 1, herein approximately 2.76) suggest that prospective patients need some motivation to elevate their readiness levels. This requires all the stakeholders in the healthcare community such as policy makers, providers, payers and patients to identify the determinants 6 of successful telemedicine utilisation.
Demonstration of a positive perception is vital to the applicability of telemedicine that is both cost-effective and less resource intensive, while increasing access to healthcare for remote patients. 26 This study examined the patient readiness for the use of telemedicine based on the attributes of objects and dimensions of TAM and FITT frameworks. According to the postulates of the model, the perceived benefits and motivational factors significantly influence the intention to use telemedicine among patients across the demographic characteristics. Therefore, telemedicine access encompassing uniformity and a simplified patient approach will result in user-friendly utilisation that is cost-effective for patients. 7
Perceived benefits appear to represent the most significant factor influencing the patients to use telemedicine. Reduced anxiety and complexity concerns enhance the utilisation of telemedicine. Patients show only moderate concerns about inadequate communication, anxiety and technologic complexity. Telemedicine may reduce the need for in-person referrals and allow patients to access care without a face-to-face visit with a specialist. The lack of trial-ability of teleconsultations limits the confidence that patients need to subscribe to telemedicine services. However, before implementing telemedicine services, a need exists to conduct a formal analysis to identify the patients, conditions, economic concerns and clinician preferences that will benefit the utilisation and render services efficiently and effectively.3,13 Telemedicine usage is also affected by protected health information (PHI) security concerns. Compliance of telemedicine use with the Health Insurance Portability and Accountability Act (HIPAA) has unique, significant security challenges that call for apposite implantation of the technology. 27 Given the present circumstances, some literature indicates that the Affordable Care Act is likely to increase the use of telemedicine in many areas such as for remote consultations, gap service coverage, emergency services, mandated services and multisite group chart rounds. 28 Many patients are also likely to use telemedicine services using video calls from personal devices such as tablets, phones or computers that meet the technologic requirements. 29
This study suggests that the patients were ready, but not very well informed and trained. Moreover, they required greater motivation through education, observations and trial-ability with better human–computer interaction (HCI) through the Clinical User-Experience Evaluation (CUE). 30 The well-planned implementation of a telemedicine system enhances the geographical access of the care providers and the efficient use of their time while reducing the barriers to effective patient interaction. To stimulate the rapid adoption of telemedicine, efforts are needed to remove the barriers identified in this study by adopting an optimum strategy for efficient and effective utilisation of telemedicine services. Our observations indicate that a healthcare delivery system should demonstrate to the amenable patients the compatibility and equivalence of telemedicine with in-person visits through better trainability and observability.18,31
Limitations of the study
The investigators identified three main limitations of this study: (a) the survey respondents were mainly from an oncology practice, (b) the survey items did not include some technical components such as the type of devices the respondents would be more comfortable using and (c) a nation-wide or international survey may be required to further ascertain the results gathered from the investigation. Further research conducted within this project will attempt to overcome some of these limitations.
In addition to this, one of the contributions of the study is the development of a survey instrument that covers the aspects included in the TAM and FITT frameworks. This feature is illustrated in Figure 1. Because the survey was employed using respondents who happened to be predominantly patients, it did not cover the actual use factor of the TAM framework to the extent we would have preferred. The actual use criteria will be thoroughly tested in the next phase of the study in which we intend to survey the physicians regarding their perceptions of telemedicine uses. Additionally, this study is limited only to the perceptions of patient motivation and readiness among non-users of telemedicine, which calls for further exploration into patient satisfaction, outcomes, safety, efficacy and other quality measures that help the triple aim of enhanced care, better health and lower cost of the health system. 32
Planned future study
The investigators plan on advancing this study to explore the contextual utilisation of telemedicine to determine how the effectiveness and efficiency of telemedicine usage vary with time, place and specific services in a diverse population. This endeavour aids in the more effective implementation of telemedicine following pertinent healthcare regulations with a flexible and integrated care delivery system that is patient-centric and fosters innovation. 18 Additionally, the investigators also plan to survey the physicians regarding their perceptions of telemedicine usage and the application of the Innovation Diffusion Model (IDM). 33 The investigators involved in the study also wish to use this instrument in a non-oncology practice and in a different part of the United States to identify trends in the perception of telemedicine use. Incorporating telemedicine as part of the standard of care depends on human factors, technology and economics. This study suggests that a need exists for improvements in the human factors to positively influence health economics through telemedicine use. The needs, gaps and challenges of the current landscape must be addressed through proper patient engagement.34,35 Future studies should select diverse samples from multiple communities so that variations in the readiness to use telemedicine may be better portrayed. Additionally, personal characteristics such as the need for care, motivation and knowledge about telemedicine should be simultaneously considered in the investigation.
Conclusion
To conclude, the investigators succeeded in fulfilling the aforementioned specific aims of the study. The analysed results indicated a positive trend towards the perception of telemedicine use among the respondents involved in the study. According to our study, Cronbach’s alpha reliability test provided an alpha value of 0.79, which approximates 0.8 and could be considered as good. The factor analysis indicated a uni-dimensional scaling because the first component explained the majority of the total variance. The first component explained 40 per cent of the total variance from which we could compute the weighted factor scores. The ANOVA tests based on the weighted factor scores showed that no significant difference was detected among the groups of gender, household income, education, ethnicity and rurality. The ordinary least squares regression showed no significant predictors towards weighted factor scores with an R2 value of 0.06. However, this study requires further probing due to the aforementioned limitations.
Overall, the study indicates that the positive inclination towards the use of telemedicine for the study sample was based on perceived benefits, motivation and relative advantage, whereas the negative inclination of the subjects was due to communication problems, comprehension concerns and technologic complexity.
Footnotes
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
