Abstract
Background and Aims:
The incidence of olecranon fractures is rising. Displaced fractures are usually operated either by tension band wiring or plate fixation. The aim of this review is to evaluate the best current evidence on the management of displaced olecranon fractures.
Materials and Methods:
Randomized controlled trials were systematically gathered in May 2018 from CENTRAL, MEDLINE, Embase, CINAHL, Scopus, and PEDro databases. The methodological quality of articles was assessed according to the Cochrane Collaboration’s domain-based framework. Prospero database registration number: CRD42018096650.
Results:
Of 1518 identified records, finally, 5 were relevant. Four trials were found on tension band wiring: two compared tension band wiring with plate fixation (n = 108), one compared plate fixation with an olecranon memory connector (n = 40), and one trial compared tension band wiring with a modified tension band wiring called Cable Pin System (n = 62). In addition, one trial compared operative and conservative treatment in elderly (n = 19). The risk of bias was considered low in two and high in three of the trials. The follow-up time was 5–36 months, and outcome measures varied from patient-rated and physician-rated measures to radiological outcomes. In the analysis, there was no difference between tension band wiring and plate fixation. The data were insufficient for further quantitative analysis.
Conclusion:
No differences were found in clinical or patient-rated outcome measures between the two most frequent fixation methods (tension band wiring and plate fixation) of displaced olecranon fractures. Current data are not sufficient to evaluate other treatment methods; however, conservative treatment might serve as an option for selected patients in the elderly population.
Keywords
Introduction
The incidence of olecranon fractures, especially in the elderly, is rising (1, 2). Displaced fractures have traditionally been treated operatively to re-establish the congruency of the ulnar joint-surface and to re-attach the triceps tendon (3). The most frequent operative methods for fixation of a displaced fracture are tension band wiring (TBW) and plate fixation (PF). According to previous observational studies, both of these methods seem to achieve adequate union and functioning but are also associated with high rates of re-operations due to operative complications and removal of the prominent metalwork after fracture union (4, 5). As relying on observational, mainly retrospective studies, previous reviews and a meta-analysis (3, 5) have shown a lack of level I/II evidence to support one implant over another. In a Cochrane review of randomized controlled trials (RCTs) from 2014 authors stated that no sufficient evidence based on randomized, controlled trials yet existed (6).
In addition to these two main fixation options (TBW and PF), also other operative techniques and instruments have been suggested. Furthermore, based on data from small retrospective series in the elderly, it seems that conservative treatment could provide a good functional outcome with a low complication burden in this population (7, 8). In this review, we aim to evaluate the current evidence of the treatment of displaced olecranon fractures based on randomized controlled studies.
Materials and Methods
Search Criteria
Inclusion criteria for this review were based on PICOS framework (population, intervention, comparison, outcome, and studies) as follows:
Population: Adults (>18 years) with acute, traumatic, and displaced olecranon fracture excluding multiple and open fractures and fractures associated with malignancy.
Intervention: Operative treatment using TBW or PF.
Comparison: Any other treatment (also TBW or PF when not used as intervention).
Outcome: any outcome.
Studies: RCTs and if under five, controlled studies with at least 10 participants in any language with English abstract excluding conference proceedings, theses, reviews, case studies, and so on.
Search Methods for Identification of Studies
The CENTRAL (Cochrane Central Register of Controlled Trials), MEDLINE, Embase, CINAHL (Cumulative Index to Nursing and Allied Health Literature), PEDro (Physiotherapy Evidence Database), and Scopus databases were searched in May 2018 unrestricted by date. Search clauses for each database are shown in Table 1. To avoid missing relevant studies, use of limits was restricted and further selection was conducted manually. The references of identified studies were also checked for relevancy.
Search clauses.

Study Selection and Methodological Quality Assessment
After saving all identified records to citation manager EndNote software (X7.2; Thomson Reuters, New York, NY, United States), two authors (I.R. and K.L.) performed a crude exclusion of irrelevant records, duplicates, clear conference proceedings, theses, reviews, posters and expert opinions based on titles (Figure 1). Two independent reviewers (I.R. and A.M.) screened all the remaining 81 records based on titles and abstracts, and then screened the full texts of the selected potentially relevant studies. The same independent reviewers also rated the methodological quality of the included five trials (Table 2). Disagreements between reviewers were resolved by consensus or by a third reviewer (K.L.).
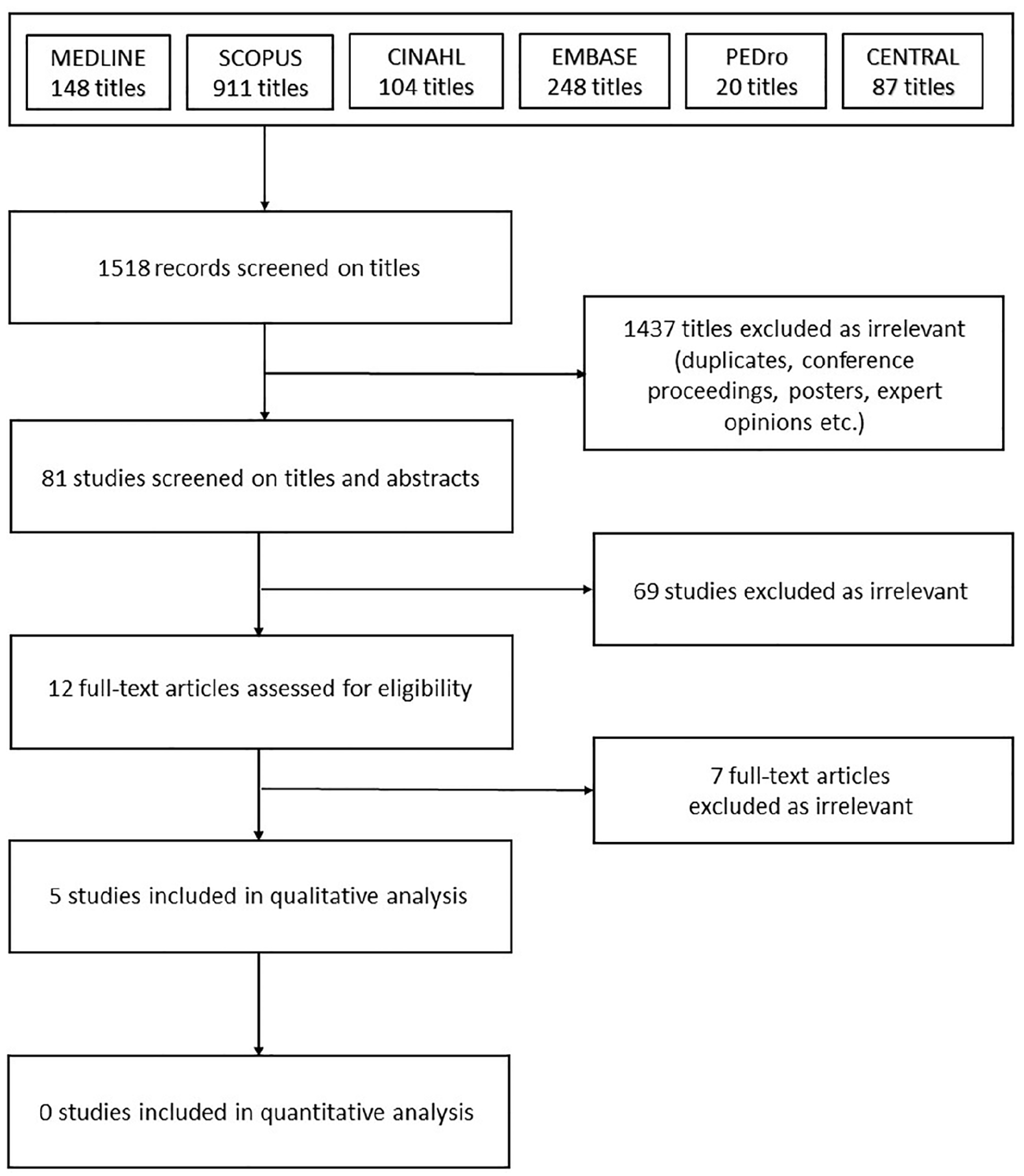
Flow chart of the search process.
Risk-of-bias.
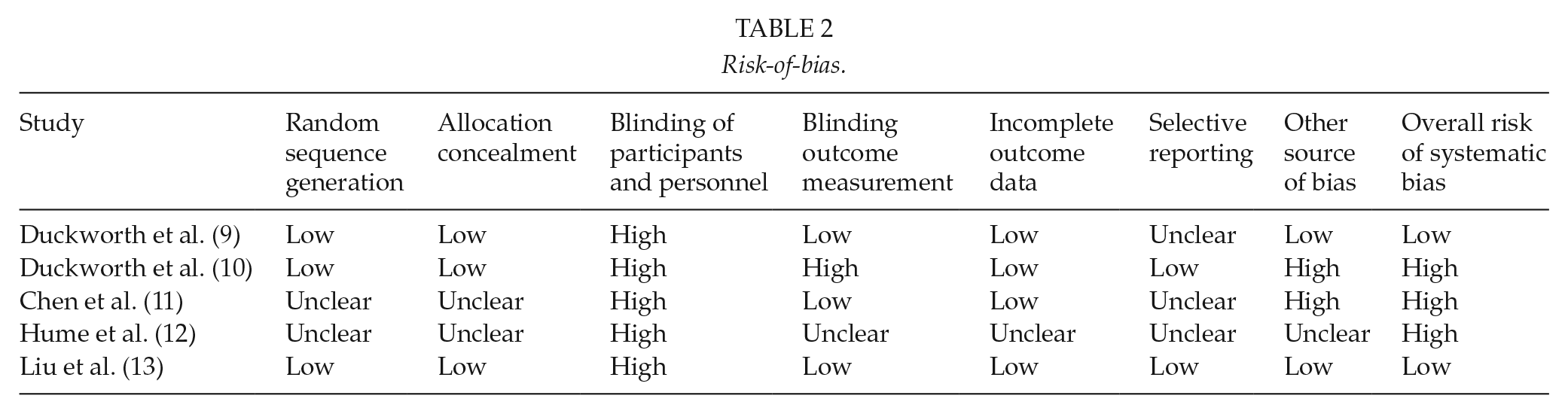
Data were extracted from included studies using a standardized form based on recommendations in the Cochrane Handbook for Systematic Reviews of Interventions, Version 5.1.0 (14). The methodological quality was assessed according to the Cochrane Collaboration’s domain-based evaluation framework (14). Following main domains were assessed: (1) selection bias (randomized sequence generation and allocation concealment), (2) performance bias (blinding of participants and personnel), (3) detection bias (blinding of outcome assessment), (4) attrition bias (incomplete outcome data, for example, due to dropouts), (5) reporting bias (selective reporting), and (6) other sources of bias. The scores for each bias domain and the final score of risk of systematic bias were graded as low, high, or unclear risk (14). The registration number of this review (Prospero database) is CRD42018096650.
Treatment Methods Included to the Study
TBW
In traditional TBW, two parallel Kirschner wires are inserted in a longitudinal direction from the proximal fragment of the olecranon extra-articularly, into the ulna more distally. The wires can be placed through the anterior cortex or straight down the shaft of the ulna. A transverse tunnel is drilled in the ulnar shaft about 4 cm distal to the fracture site, and then a flexible cerclage wire (usually 1.0 or 1.2 mm) is passed through the tunnel and posterior to the two Kirschner wires in a figure of eight. The wire is tensioned, and all wire ends trimmed and buried into the triceps tendon (9).
PF
In PF, the fracture is reduced and a pre-contoured dorsal proximal ulnar plate is applied. Aiming for a stabile construct, the plate is fixated with screws (9).
Outcome Measures
Any patient-reported, physician-reported, or other clinical or radiological outcome measures with indicators of mobility and complications were included. Mainly used scores were “the Disabilities of the Arm, Shoulder and Hand” (DASH) questionnaire (15, 16) which is a patient-rated outcome measure (PROM) with a sum score 0–100 (0 = no, 100 = severe disability), and two physician-based measures, “the Mayo Elbow performance score” (MEPS) (17) (5 = worst, 100 = best: pain = 0–45, range of motion = 5–20, stability = 0–10, and functions = 0–25) and “Broberg and Morrey score” (B&M) (18, 19) (0–100, 0 = worst, 100 = best: range of motion = 0–40, strength = 0–20, stability = 0–5, and pain = 0–35).
Statistical Analysis
A meta-analysis was inapplicable due to the dissimilarities of the included RCTs. The effect sizes of the outcomes of the included studies could not be calculated either, because baseline values were not reported. Analysis of studies was reported by absolute numbers with percents and mean values with standard deviations.
Results
Of the 1518 records identified in the search, 5 were finally considered relevant for analysis (Figure 1) (9–13). The pooled patient population of these RCTs involved 229 patients (Table 3): 85 in TBW, 75 in PF, 61 in different operations, and 8 in conservative treatment group (9–13). The size of study populations varied from 19 (11 cases vs 8 controls) (10) to 67 (34 cases vs 33 controls) (9). The types of the fractures were classified according to Mayo (20, 21) (Table 3). The duration of follow-up ranged from about 5 months (13) to 3 years (11) (Table 3). Three studies compared TBW to PF (9, 12) or to modified technique of TBW: Cable Pin System (CPS) (13). One study compared PF to olecranon memory connector (OMC) (11), and one study compared operative treatment to conservative treatment (10). The risk of bias was considered high in three of the five trials (Table 2) (9, 11, 12). A meta-analysis was not applicable due to lacking baseline values and differing outcome measures.
Descriptive characteristics of the included studies.
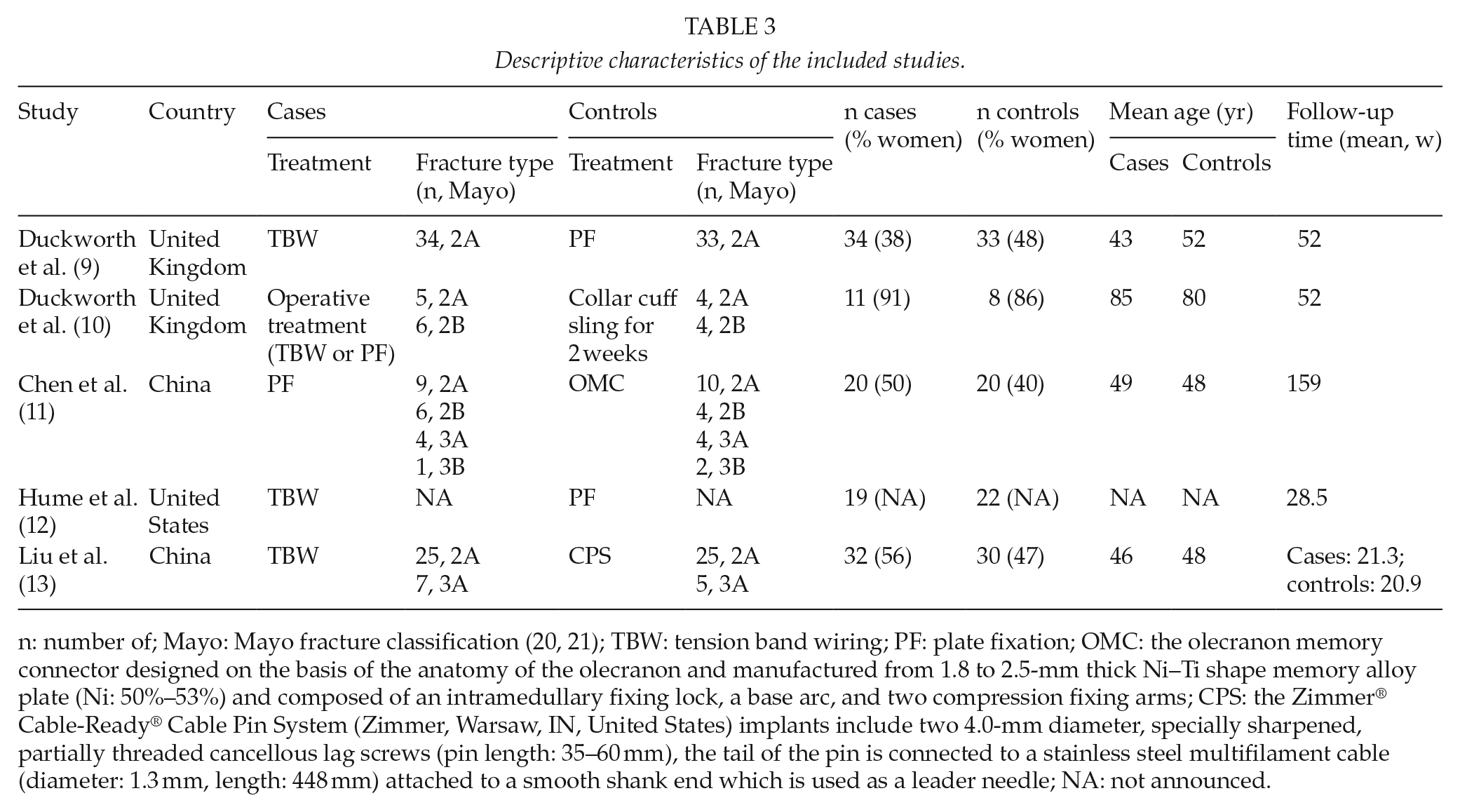
n: number of; Mayo: Mayo fracture classification (20, 21); TBW: tension band wiring; PF: plate fixation; OMC: the olecranon memory connector designed on the basis of the anatomy of the olecranon and manufactured from 1.8 to 2.5-mm thick Ni–Ti shape memory alloy plate (Ni: 50%–53%) and composed of an intramedullary fixing lock, a base arc, and two compression fixing arms; CPS: the Zimmer® Cable-Ready® Cable Pin System (Zimmer, Warsaw, IN, United States) implants include two 4.0-mm diameter, specially sharpened, partially threaded cancellous lag screws (pin length: 35–60 mm), the tail of the pin is connected to a stainless steel multifilament cable (diameter: 1.3 mm, length: 448 mm) attached to a smooth shank end which is used as a leader needle; NA: not announced.
Outcome Scores
Overall, all included studies showed a good prognosis despite of the chosen treatment (Table 4). When different operative techniques were compared (9, 11–13), there were no statistically significant between-group differences in patient-rated scores (DASH) (9, 11) or in the range of motion (9, 11, 12). Physician-rated scores (B&M or MEPS) were statistically similar when comparing TBW and PF (9), but had a statistically significant difference in the studies comparing PF to OMC (11) and TBW to CPS (13). In both studies, the result of MEPS was better in the control group (OMC or CPS) with a 7%–8% between-group difference and a highly overlapping standard deviation (11, 13). Fracture healing time was rated in one study (13), and was reported to be shorter in CPS than in TBW group (about a 1-week’s mean difference). The results of one study comparing TBW and PF (12) favored PF in clinical and radiographic results, when assessed in three categories: good/fair/poor.
Main outcomes of the included studies.
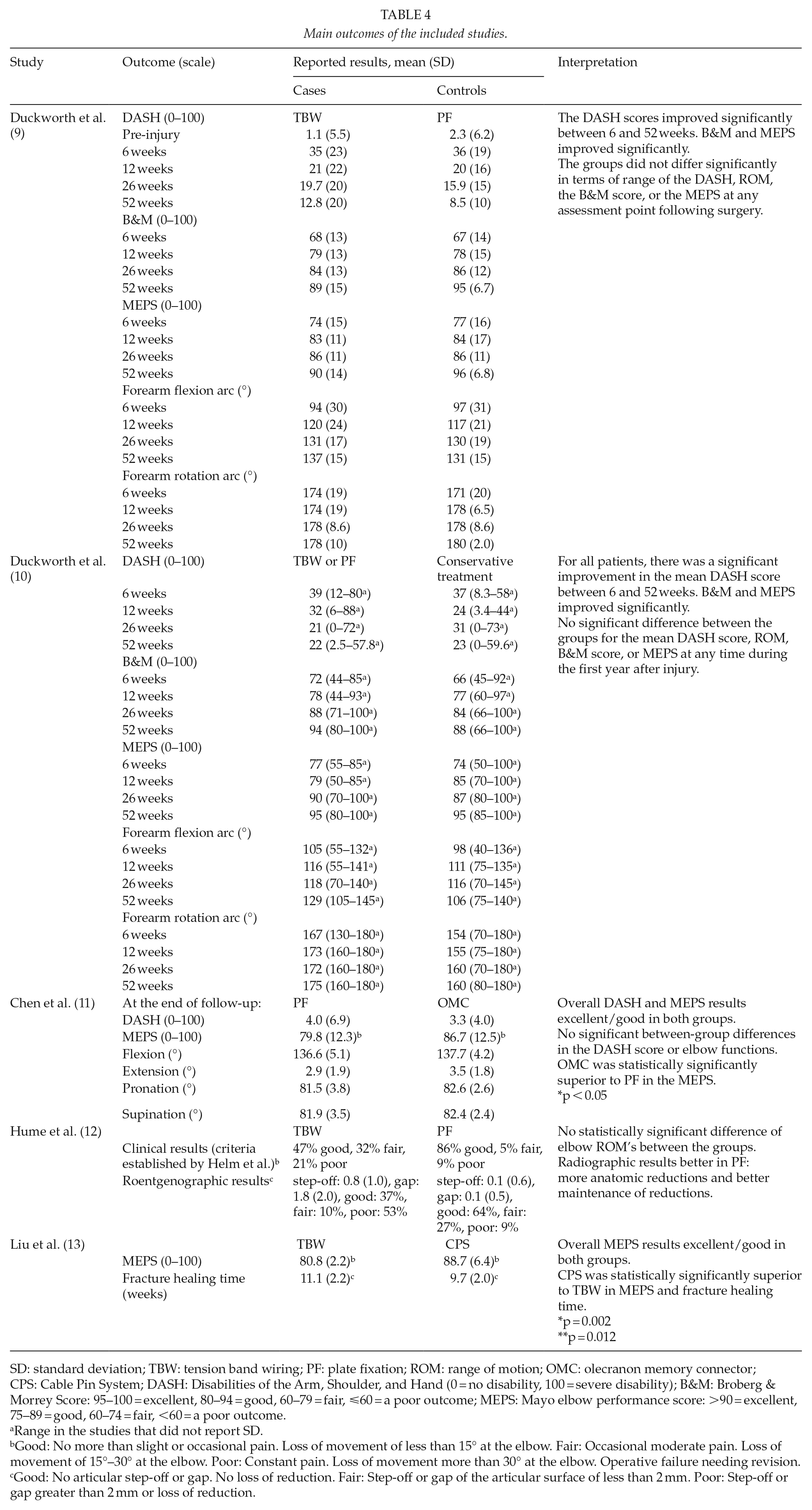
SD: standard deviation; TBW: tension band wiring; PF: plate fixation; ROM: range of motion; OMC: olecranon memory connector; CPS: Cable Pin System; DASH: Disabilities of the Arm, Shoulder, and Hand (0 = no disability, 100 = severe disability); B&M: Broberg & Morrey Score: 95–100 = excellent, 80–94 = good, 60–79 = fair, ⩽60 = a poor outcome; MEPS: Mayo elbow performance score: >90 = excellent, 75–89 = good, 60–74 = fair, <60 = a poor outcome.
Range in the studies that did not report SD.
Good: No more than slight or occasional pain. Loss of movement of less than 15° at the elbow. Fair: Occasional moderate pain. Loss of movement of 15°–30° at the elbow. Poor: Constant pain. Loss of movement more than 30° at the elbow. Operative failure needing revision.
Good: No articular step-off or gap. No loss of reduction. Fair: Step-off or gap of the articular surface of less than 2 mm. Poor: Step-off or gap greater than 2 mm or loss of reduction.
When comparing operative and conservative treatment (a collar cuff sling for 2 weeks) in elderly, there were no between-group differences in patient- or physician-based outcome evaluations or range of motion (10).
Re-Operations and Complications
In comparison of complication rates, re-operations in TBW groups due to prominent metalwork varied from 16% to 50% across studies reaching 27% (23 of 85) of all participants in TBW groups (9, 12, 13) (Table 5). In PF groups, removal rates were lower. Some plates had to be removed because of prominence (9, 10), and one study reported 22% removal rate (9). Infection rates varied from 0% to 14% (9–13). Loss of reduction was more common in TBW groups than in control treatments (9, 10, 12, 13). The study comparing operative and conservative treatment in elderly was interrupted because of the high complication rate in operative group (10).
Complications reported in studies.
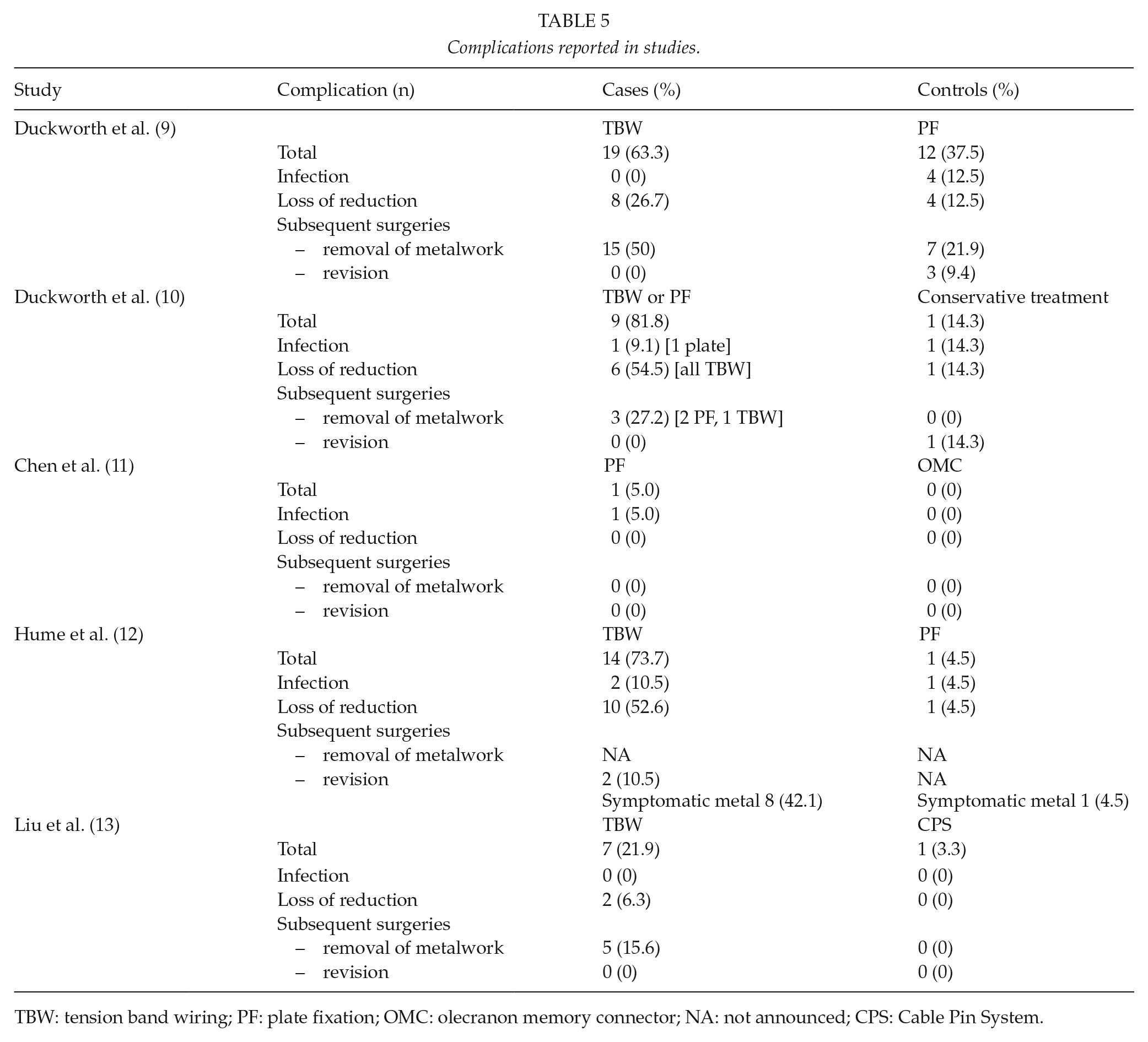
TBW: tension band wiring; PF: plate fixation; OMC: olecranon memory connector; NA: not announced; CPS: Cable Pin System.
Discussion
The four main findings of our systematic review of RCTs on displaced olecranon fractures were (1) the lack of high-quality evidence, (2) a good prognosis with all studied treatment options, (3) rather high complication rates after operations, and (4) small and clinically non-significant difference or no difference at all in the outcomes between the studied treatment options. Unfortunately, current evidence did not enable us to pool the results for a more accurate meta-analysis.
Our results are highly comparable with the only one previous systematic review of RCTs on operative treatment of olecranon fractures, where the search was performed in September 2014 (6). In contrary to this previous Cochrane review, we excluded high-bias-risk quasi-RCTs. In addition, we focused on displaced fractures with a long-term follow-up, and to studies comparing either PF or TBW to other treatment options. Three studies were included in both systematic reviews. Two recent studies, both from one study group in the United Kingdom published in 2017, enabled us to include conservative treatment option into the current review.
As in 2014 (6), all studies are small (19–67 participants), and have inadequately reported blinding of clinicians and participants, possibly influencing the patient- and physician-reported outcome measures. Each of our five RCTs evaluated either differing treatments (TBW vs PF, PF vs OMC, TBW vs CPS, or operation vs conservative treatment), or when comparing same treatments (TBW vs PF in two studies), the outcome measures were not comparable: validated questionnaires and range of motion in one, and combined clinical results in the other. Even if the authors of the previous review (6) stated that weaknesses of the included high-bias-risk studies highly affected the reliability of their conclusions, they wanted to help clinicians with a quantitative evaluation. As studies included in our and in the previous review did not have any baseline measurements before the treatment, the comparison of between-group differences is based on the follow-up measurements only, and has a higher risk of bias than when comparing the change of baseline values between two groups. In our study, we did not compensate the lack of meta-analysis with other types of quantitative reporting.
Based on our results, current evidence, or lack of evidence, does not support changing treatment practices in working-age patient populations. Comparably to earlier data, there were no significant differences between operative treatment methods, usually TBW, PF, or their modifications in adults with displaced olecranon fractures (4,22,23). Both methods, TBW and PF, achieve adequate union and elbow function but are associated with high rate of re-operations because of infections or removal of the prominent metal devices after fracture union. Authors of one study concluded that modification of TBW (CPS) was better than standard TBW (13), and authors of another study concluded that a novel invention resembling TBW (OMC) was superior to locking PF (11). In both studies, the between-group differences in the follow-up values were under 10% with highly overlapping standard deviation. Positive results with OMC were reported by the designers of this technique, and their findings should be confirmed before implementing OMC to clinical practice. The clinical relevance concerning the reported superiority of PF in radiological outcomes in one included study remains questionable since there were no acceptable limits reported. In addition, radiological results were not compared to the functions (12). Compared to earlier reviews, we were able to include more recent RCTs and conservative treatment to our review.
We found two new studies after the review in 2014. One low-bias-risk study compared PF and TBW, and found similar patient-rated outcomes and clinical functions after both operation techniques (9). The other new study was planned to compare conservative and operative treatment in the elderly (10). This study questions the treatment paradigm of displaced olecranon fractures and is in line with previous retrospective studies showing no patient- or physician-rated benefit of operative treatment over conservative treatment. The study was prematurely discontinued after only 19 participants due to complications in the operative treatment arm. Reconstruction of articular surface is important in the active elbow loading working-age population. However, conservative treatment may yield satisfactory outcomes in daily activities, and may be considered as a potential treatment in the elderly population.
In all studies, complications after operative treatment were common, especially after TBW. The soft tissue coverage of the olecranon is very thin, and operative hardware (wires, plates, screws, or pins) are prone to cause problems under the skin. Hardware prominence remained the most common adverse effect in this review frequently leading to re-operations, and assessing and reporting of complications is recommended also in future RCTs.
We acknowledge that our study had several limitations. In a wide systematic review as ours, the results always depend on the search clauses and used databases. Even if we kept the search wide, and if we assume that these five studies reflect this patient population, we only have information of some outcome measures. While the evidence is still limited, results may change after high-quality, low-bias-risk studies. The short-term outcome was not in the scope of this review, and we consider that long-term outcome is more important when choosing treatment options. To obtain more definite conclusions, meta-analysis on only low-bias-risk RCTs would be needed; however, this is not possible based on current studies. Despite the weaknesses, this review is the first update of reviewing RCTs after year 2014 (6). Previously, the most frequently used method of care for olecranon fractures was operative treatment. However, the proportion of conservative treatment is increasing among low demand patients, and therefore, we feel that this review is a valuable addition to the previous literature.
In conclusion, the evidence is insufficient to draw robust conclusions on the clinical superiority of one treatment over another. The current literature supports standard fixation methods (TBW and PF) on displaced olecranon fractures in adults. In the elderly population, conservative treatment may be a potential treatment option to avoid unnecessary operations and complications.
Footnotes
Authors’ Contributions
All authors have substantially contributed in designing the study, and acquiring, analyzing, and interpreting the data. All authors have also participated in drafting the article and revising it critically for important intellectual content. All authors have given their final approval of the submitted version of the article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
