Abstract
Keywords
Bereavement is a part of life. Nevertheless, some losses are so hurtful that the bereaved need professional help to cope with everyday life. In those circumstances, bereaved people’s needs may relate to a broad spectrum of life areas, from the spiritual (Silviken et al., 2015) and practical (Ross et al., 2021) to the economic (Fjær & Dyregrov, 2021) and psychosocial (Dyregrov et al., 2015). Unnatural deaths, as well as sudden and unexpected bereavement, risk affecting the bereaved person’s life and health in profound ways, and even the prospect of premature death looms larger (Djelantik et al., 2020; Kristensen et al., 2012; Song et al., 2010, 2019). The affected relations may include parents, children, siblings, extended family, partners and close friends (Bolton et al., 2016; Liu et al., 2019; Rostila et al., 2012; Templeton et al., 2018). Studies show that most of those bereaved by unnatural deaths report a need for professional help; however, many do not receive this help, and their own capacity to initiate it is impaired (Dyregrov, 2002; Peters et al., 2016; Pitman et al., 2017). The bereaved generally want the professionals to initiate contact (proactive help) and provide flexible help over time (Dyregrov et al., 2015; Dyregrov & Kristensen, 2021; Ligier et al., 2020; Wilson & Marshall, 2010). Early connection with support services generally results in positive experiences (McKinnon & Chonody, 2014), and outreach and proactive services have shown to improve the bereaved person’s likeliness to access help and support (Szumilas & Kutcher, 2011).
Drug-related deaths (DRDs) are unnatural deaths that tend to happen suddenly and unexpectedly (Titlestad, 2021). According to research, common experiences on such deaths include stigmatisation, complicated emotions and complex social relations (Dyregrov & Selseng, 2022; Titlestad et al., 2019), as well as struggles concerning meaning-making, shame and guilt (Titlestad et al., 2020a, 2020b). A study on DRD-bereaved parents in Norway found a high prevalence of complicated grief symptoms (Titlestad et al., 2021). In addition, a register-based study found a higher mortality rate among DRD-bereaved parents than with parents bereaved by other forms of death (Christiansen et al., 2020).
Internationally, the high number of DRDs is a significant public health issue (UN General Assembly, 2016). Since 1990, there has been a considerable increase in the number of people with drug problems worldwide (Degenhardt et al., 2018), and the number of deaths related to drug use has similarly increased (Murray et al., 2020). The World Health Organization (WHO; 2020, 2022) estimates that about 500,000 deaths annually are related to drug use, and about 182,000 of them are directly drug-induced. In the European Union countries, including Norway and Turkey, the annual toll of drug-induced deaths was estimated to amount to 5,800 in 2019 (EMCDDA, 2021). In Norway, an average of 275 individuals are annually registered as deceased by immediate drug-induced causes (Norwegian Institute of Public Health, 2021), and a total of at least 400 persons can be identified as deceased by both direct and indirect drug-related causes (including illness and drug-related violence and accidents). Thus, if we estimate that there can be eight close bereaved persons after each DRD, there will be 3,200 new bereaved in Norway each year, and about 60,000 persons can be defined as strongly impacted by a DRD in the last two decades. Based on the WHO estimates of total DRDs globally, the impact of DRDs affect four million bereaved people each year.
The few small studies concerning DRD-bereaved people’s encounters with professional services have found mixed experiences. In a UK study on drug- and alcohol-related deaths, the bereaved experienced fragmented encounters, but compassion and kindness from professionals mitigated feelings related to stigma (Walter et al., 2017). Another UK study found the experience of meeting a non-judgemental counsellor especially important for DRD-bereaved people (Cartwright, 2019). Of two small studies in Denmark, one reported a lack of help, understanding and support from professionals as common experiences (Biong & Thylstrup, 2016), while the other found that the bereaved were most satisfied with proactive help (Tjagvad et al., 2014). In a Norwegian study, only one of 14 DRD-bereaved parents received proactive help from professional services, and the experiences with help were generally mixed (Titlestad et al., 2020a, 2020b).
In sum, the studies investigating bereaved people’s needs and experiences with professional help after a DRD are small, mainly including participants with one or few relationships to the deceased (such as parents). However, together with research into help experiences after other forms of unnatural death, they do show the importance of the way professional services relate to the bereaved. This study is part of the END project, a sizeable Norwegian research project investigating DRD-bereaved people’s situations, experiences with help and how professional services relate to the bereaved. This article aims to provide knowledge on the needs for help that DRD-bereaved family members, close friends and partners have, the professional help that they have received, and on the variables related to participants’ satisfaction with the received help. Improvements in services will be suggested based on the findings.
Methods
In this study with a cross-sectional design, the reporting is guided by the STROBE Statement Checklist (Von Elm et al., 2007). All analyses were carried out using IBM SPSS Statistics Version 27.
Data collection
The data were collected through a survey answered by a sociodemographically and geographically heterogeneous convenience sample of DRD-bereaved family members and friends in Norway from February to December 2018. The recruitment strategy entailed information letters and cooperation with municipalities, hospital services, treatment centres and non-governmental organisations. In addition, recruitment was promoted through information letters to all Norwegian municipalities’ public email addresses, advertising in various media, information at conferences and snowball recruitment.
Participants
To be eligible, the participants had to be aged at least 18 years and to have lost a family member or close friend in a DRD more than three months before answering the survey. In total, 255 DRD-bereaved family members, partners and close friends participated in a survey completed on paper or digitally via Questback. Table 1 presents descriptive data of the sample, the reported relations to the deceased and the characteristics of the deceased.
Sample characteristics (n = 255) presented with (range), mean (sd) or n (%).

The vast majority of deaths the bereaved had experienced were sudden. The majority of the deceased died while actively using drugs (38%). A substantial group had died after relapse (22%) and after or during substance treatment or prison (21%), whereas 20% died in unclear or other circumstances. Drug use was known to the bereaved in almost all cases (95%), and in most cases, the deceased had started using drugs several years before the death.
Questionnaires and variables
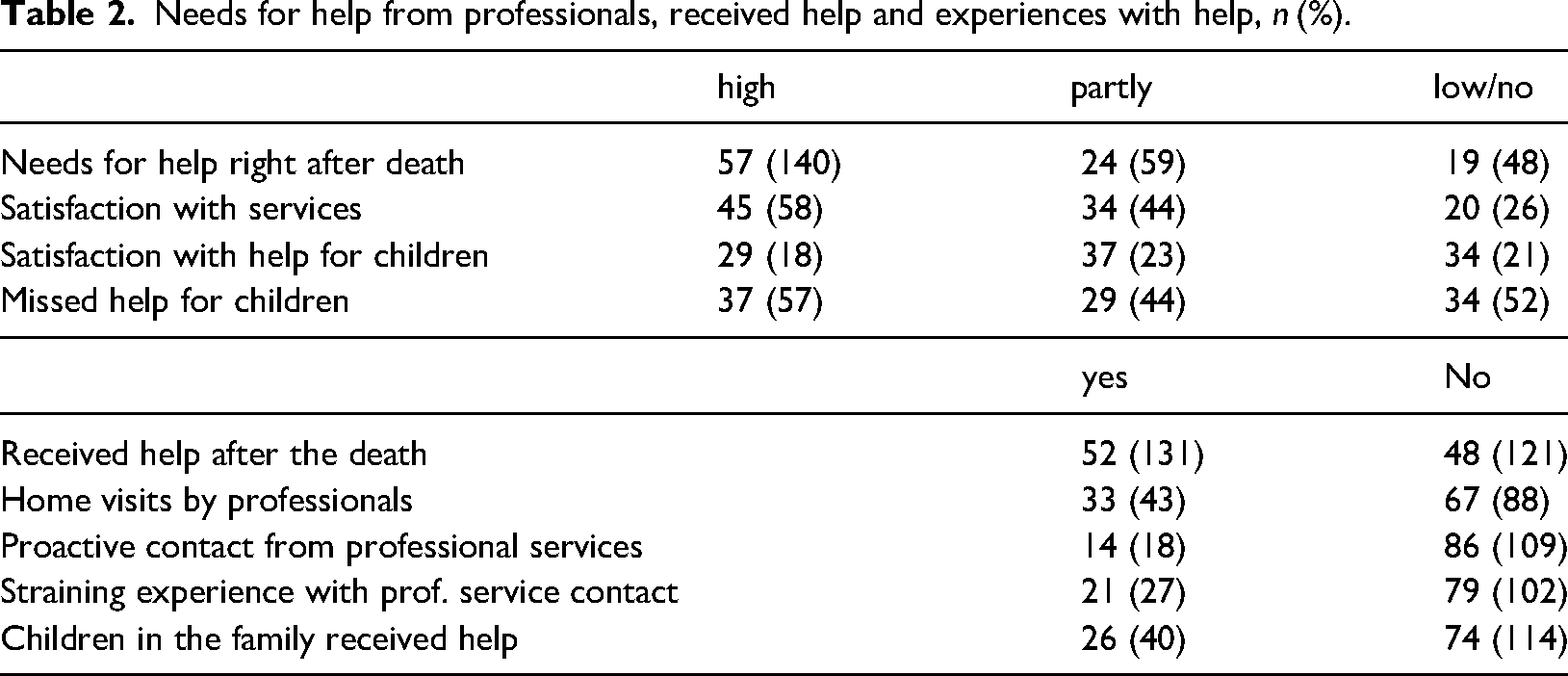
The survey consisted of 109 questions, and the data for this article included background variables and responses from three questionnaires in the survey. Some Likert items and nominal variables with more than two categories were collapsed because of statistical requirements, e.g., for the logistic regression analysis. In addition, some were collapsed in the frequency tables; for example, “high” and “very high” were collapsed into “high” in Table 2.
Needs for help from professionals, received help and experiences with help, n (%).
Assistance questionnaire
The assistance questionnaire (AQ-R), addressing bereaved people’s needs for help and received help, has been used in other studies with traumatised bereaved (Dyregrov, 2003; Wilson & Clark, 2005). It consists of 22 questions, 12 of which we used in this study. The response options are nominal, ordinal or 5-point Likert items. The respondents are asked whether they have received help (nominal), which services they have wanted and received help from (nominal, 12 options and free-text), whether proactive contact and home visits are included in the helping relationship (nominal), the degree of satisfaction with the help received (Likert item), whether contact was experienced as burdening (nominal), the need for help immediately after death (Likert item), ideal help duration (ordinal, five options and free-text), received help for children (nominal), satisfaction with help for children (Likert item) and wanted help for children (Likert item).
General self-efficacy scale, short form
Self-efficacy was measured using the generalised self-efficacy scale, short form (GSE-SF), which consists of five items, scoring 1–4 from “not at all true” to “exactly true”. The α-coefficient for the sample in this study was .834. One participant in the relevant analysis had missing values and was not included.
PG-13
Prolonged grief symptoms were measured using the diagnostic tool PG-13 (Prigerson & Maciejewski, N.D.). The measure consists of 11 5-point Likert items that score the frequency and intensity of distress symptoms related to bereavement, which are then summed continuously to reach a total score of 11–55. Higher scores mean more severe symptoms, and a preliminary cut-off for a diagnosis of prolonged grief is 35 or more (Pohlkamp et al., 2018). Five participants had more than 25% missing answers on this measure and were not included in the analysis, leaving 250. Nine participants had one missing value, and one participant had two, which constituted 0.4% of the total items. These were imputed based on the mean score of the participant’s reported inventory items. The α-coefficient for the sample was .898.
Statistical analyses
Frequency analyses were performed with variables related to the needs for help and received help for the whole sample. Next, we conducted chi-square analyses (χ²) for needs for help, received help and whether services initiated contact after the loss (proactive help) as dependent variables. The independent variables were sociodemographic characteristics, relation to the deceased (parent, partner or friend, sibling, etc.), temporal variables (age of the deceased and the bereaved at the time of death, time since loss, duration of the deceased’s drug use) and the circumstances (manner and context) of the death. Logistic regression analysis was used to see if any variables predicted participants’ ratings of high or low satisfaction with help controlled for confounding. See details for the logistic regression analysis in the supplementary file.
Ethical considerations
The END research project has been approved by the Norwegian Regional Committee for Medical and Health Research Ethics (reference no. 2017/2486/REK vest). When consenting to participate, all participants were informed in writing about the project’s aims. It was further explained that the data would be published in a non-identifiable manner and stored on the research server at the university (more details can be found on the END web page or ResearchGate).
Results
The needs for help and received help
Prolonged grief symptoms measured with PG-13 showed mean scores of 33.7 for participants bereaved within the last two years, 29.1 for those bereaved 2–5 years ago, and 25.0 for those bereaved >5 years ago.
Table 2 shows the answers of the bereaved concerning their reported need for help from professionals for their own sake and for children in the family. It also shows how many have received professional help, aspects of how the help was tailored, and their assessments of received help in terms of satisfaction and straining experiences.
Concerning the ideal duration of help, 20% reported 1–3 months, 36% stated 3–12 months, and 39% reported 12 months, or as long as needed. In addition, 10 (4%) participants were not sure, and one participant reported no need. Figure 1 shows the distribution of services from which participants received help, presented as a percentage of the total participants that had received help (n = 131). Most of those who received help did so from more than one service (M = 2.6). Figure 2 shows the services that participants missed help from as a percentage of the total sample who had responded on this item (n = 238).
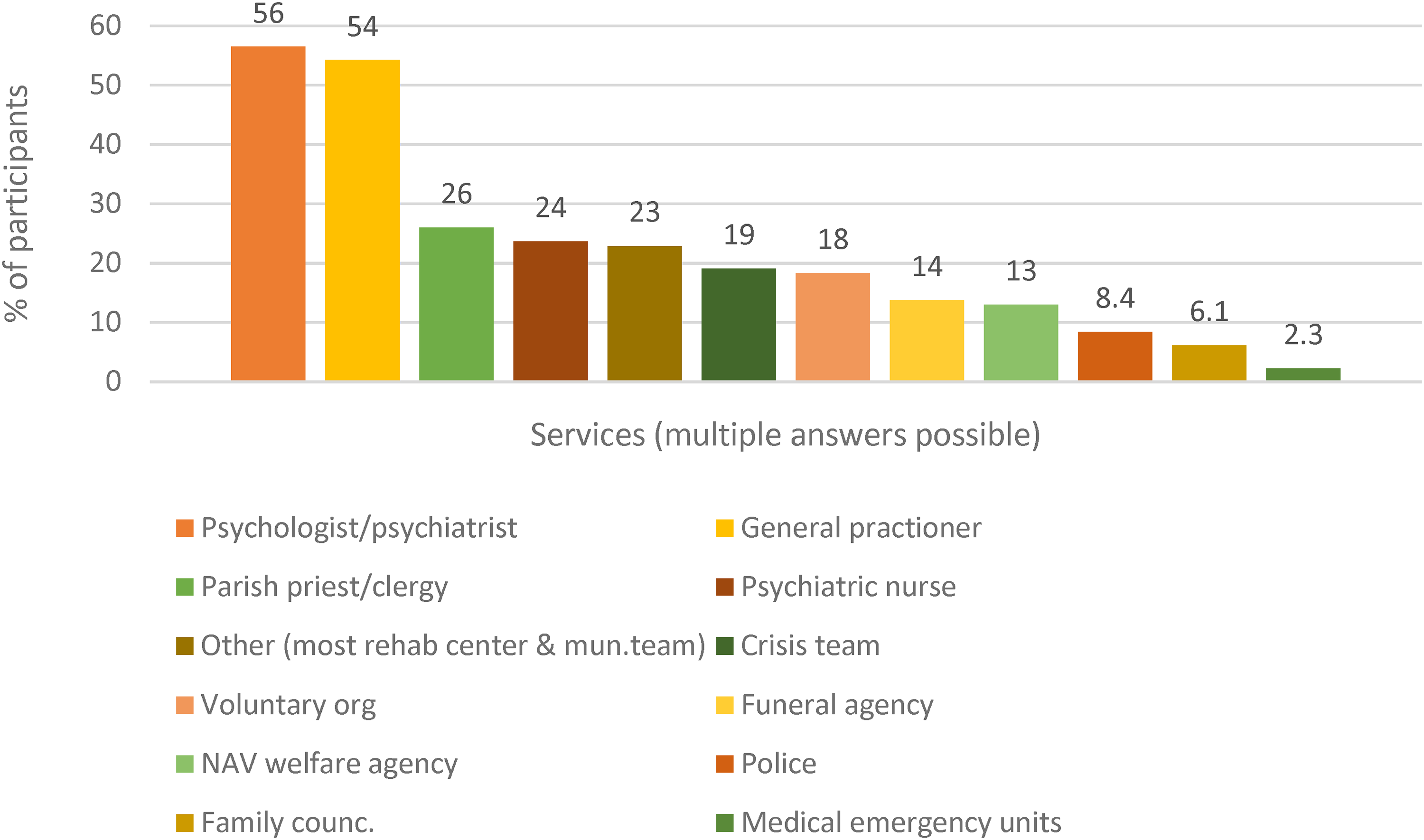
Received help after bereavement.
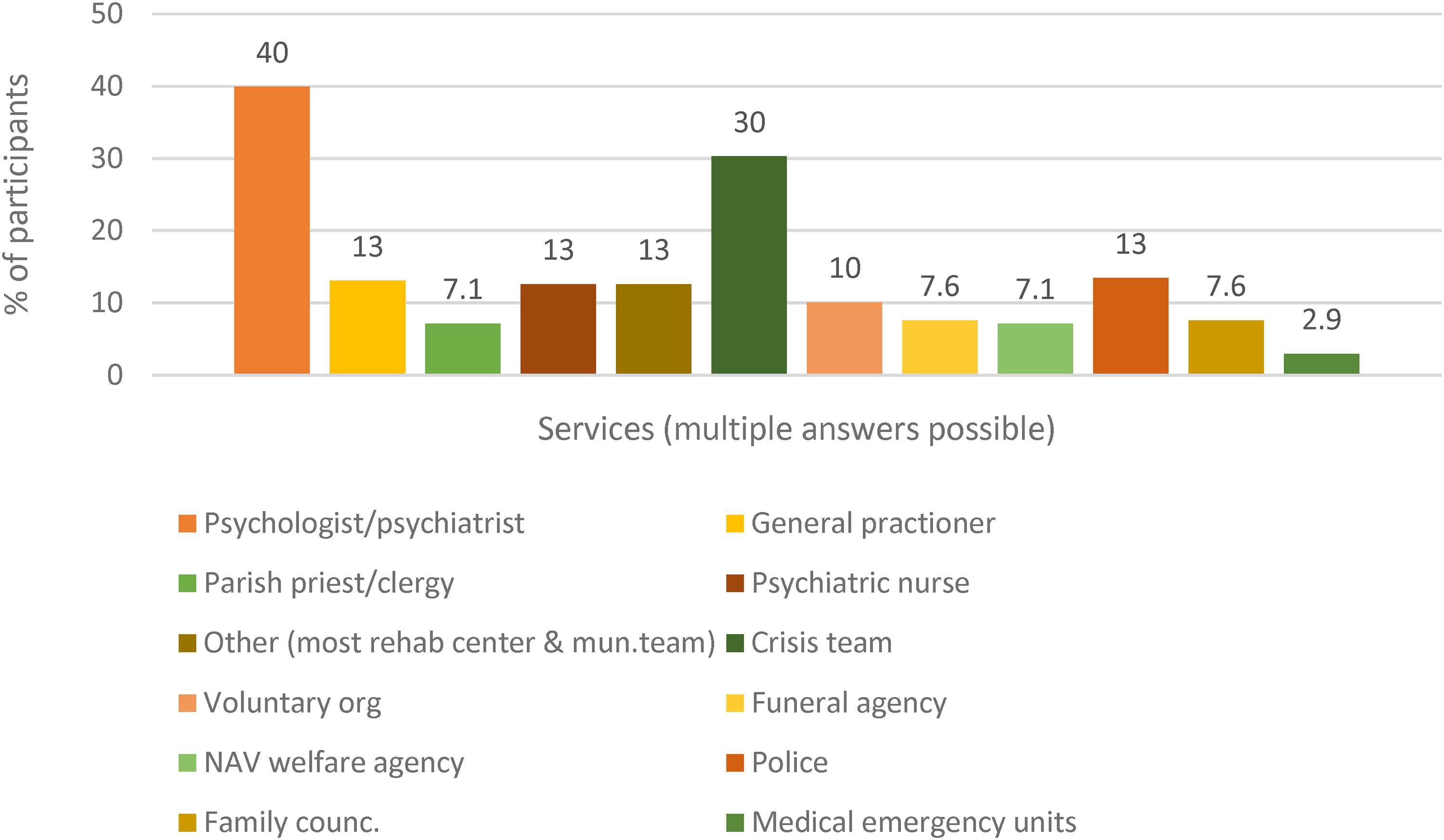
Missed contact with services after bereavement.
Variables associated with needs for help, received help and proactive help
The χ² analyses show that the needs for help are relatively evenly distributed between the different relations to the deceased. Only the variable of death by intentional or unintentional intoxication yielded a significant association to higher needs for help, compared with death by disease, accident, violence or uncertain manner (2, N = 245, χ² = 19.499, ϕc = .282, p < .001). The Cramer’s V (ϕc) of .282 suggests a medium correlation (Pallant, 2020). On the dependent variable of received help, we found a significant association between the needs for help and the level of received help (2, n = 247, χ² = 9.194, ϕc = .193, p = .01), which suggests a small to medium correlation. Relation to the deceased was also significantly associated with received help (4, n = 252, χ² = 15.458, ϕc = .248, p = .004), a medium correlation. The distribution of received help favours parents (adjusted residuals = 2.6) and disfavours the extended family (adjusted residuals = –3.0). The other relations showed minor deviations from the expected count. Being a parent was also significantly associated with the dependent variable of proactive contact from services (1, n = 127, χ² = 7.690, ϕ = .269, p = .006), a small to medium correlation (Table 3).
Needs for help, received help and proactive help. χ² analyses.
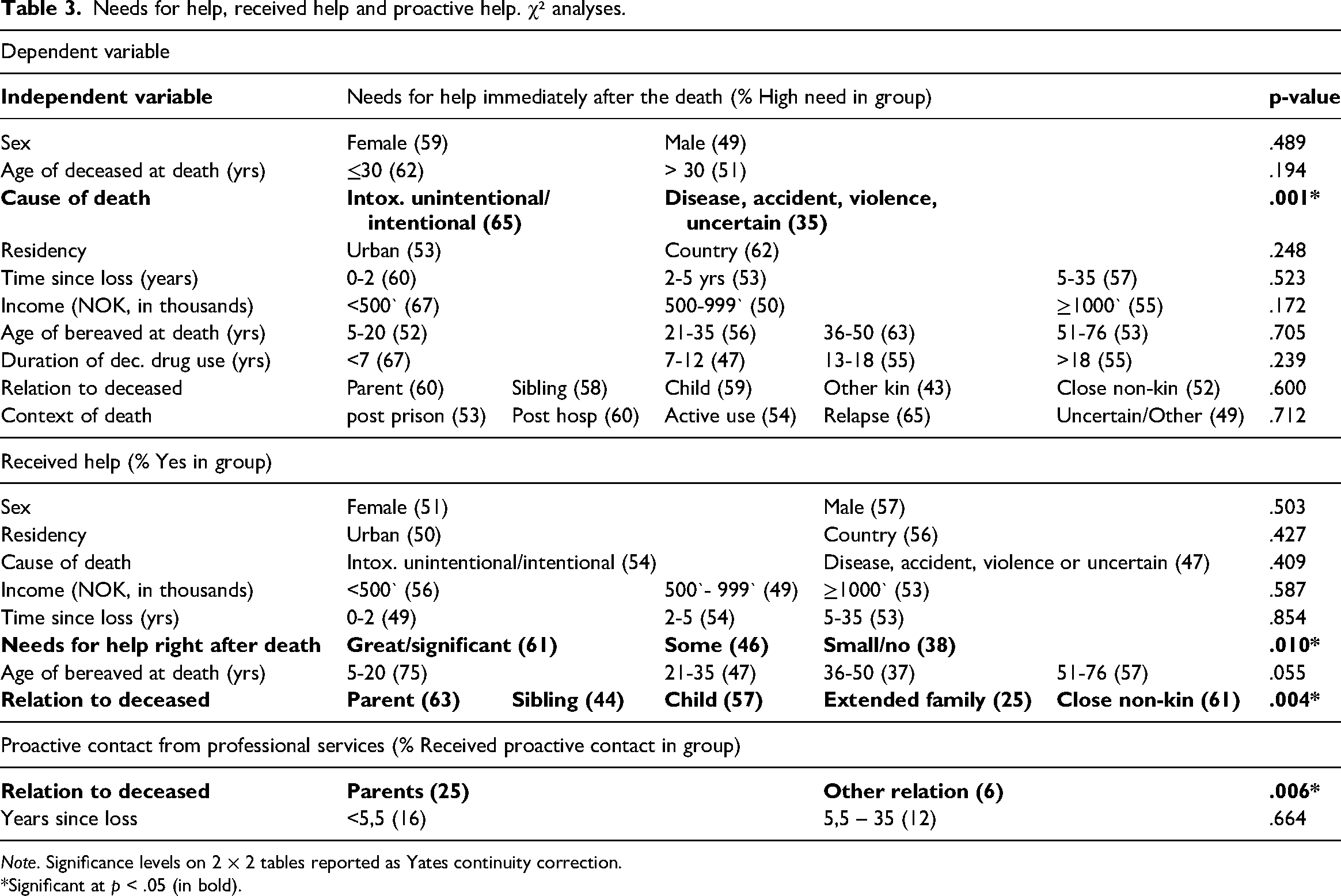
Note. Significance levels on 2 × 2 tables reported as Yates continuity correction.
*Significant at p < .05 (in bold).
Predictors to satisfaction with received help
The logistic regression model yielded five significant predictor variables at p < .05 and one interaction term at p < .10. The results show that a longer time since bereavement predicted higher satisfaction. Those of older age at the time of loss and those with higher self-efficacy were more likely to be satisfied with the help. Furthermore, if the bereaved received help from a crisis team or a psychologist/psychiatrist, they were also more likely to be satisfied with the help. On the interaction term psychologist/psychiatrist by age of bereaved at the time of death (p = .073), the analysis shows that having received help from a psychologist/psychiatrist predicts a higher likeliness for satisfaction with the help given younger age (Figure 3).
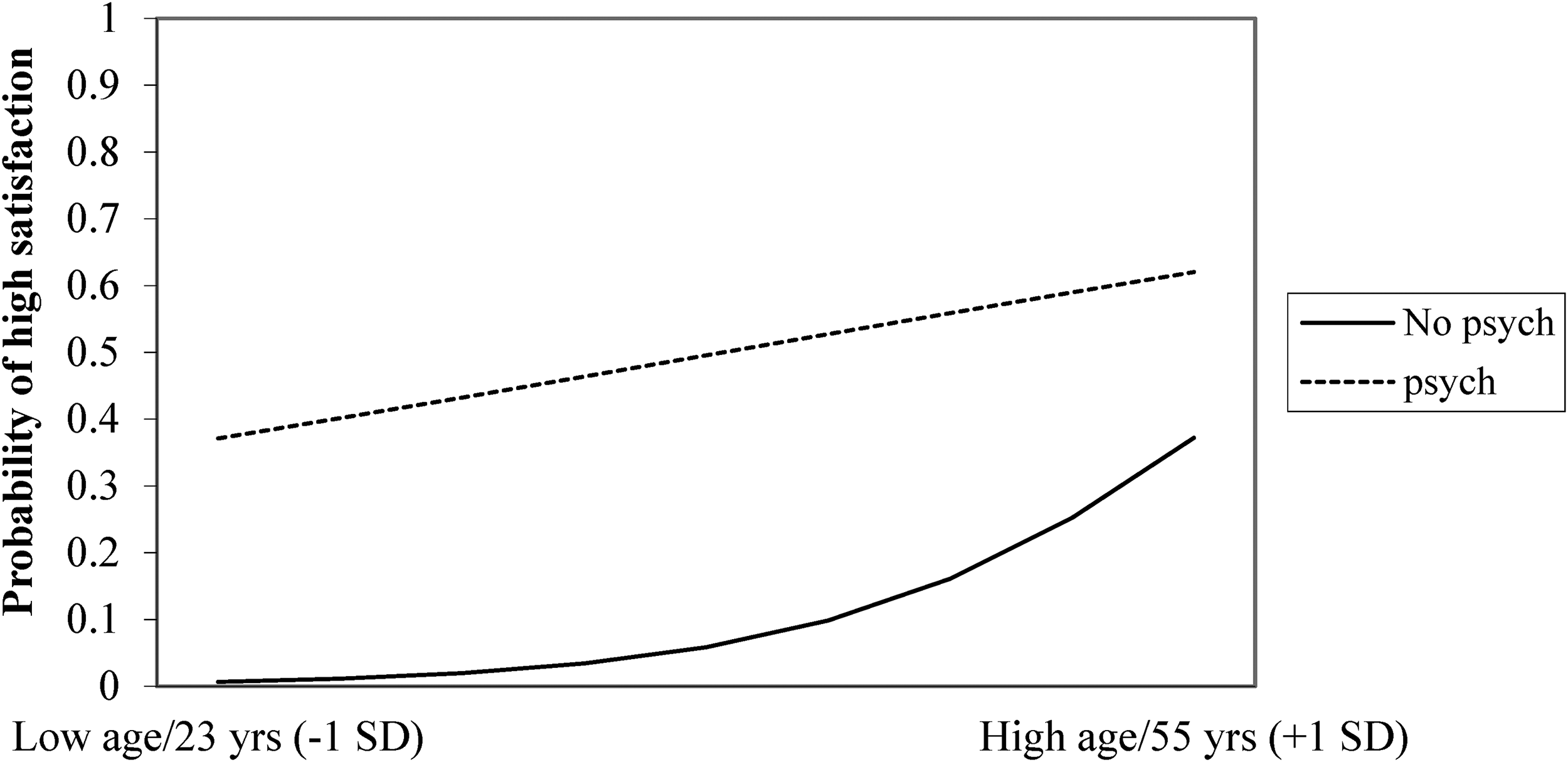
Interaction term psychologist/psychiatrist by age of bereaved at time of death.
Table 4 shows the odds ratios of the significant predictor variables associated with high satisfaction with help.
Final logistic regression-model for outcome high satisfaction with help (n = 124).a
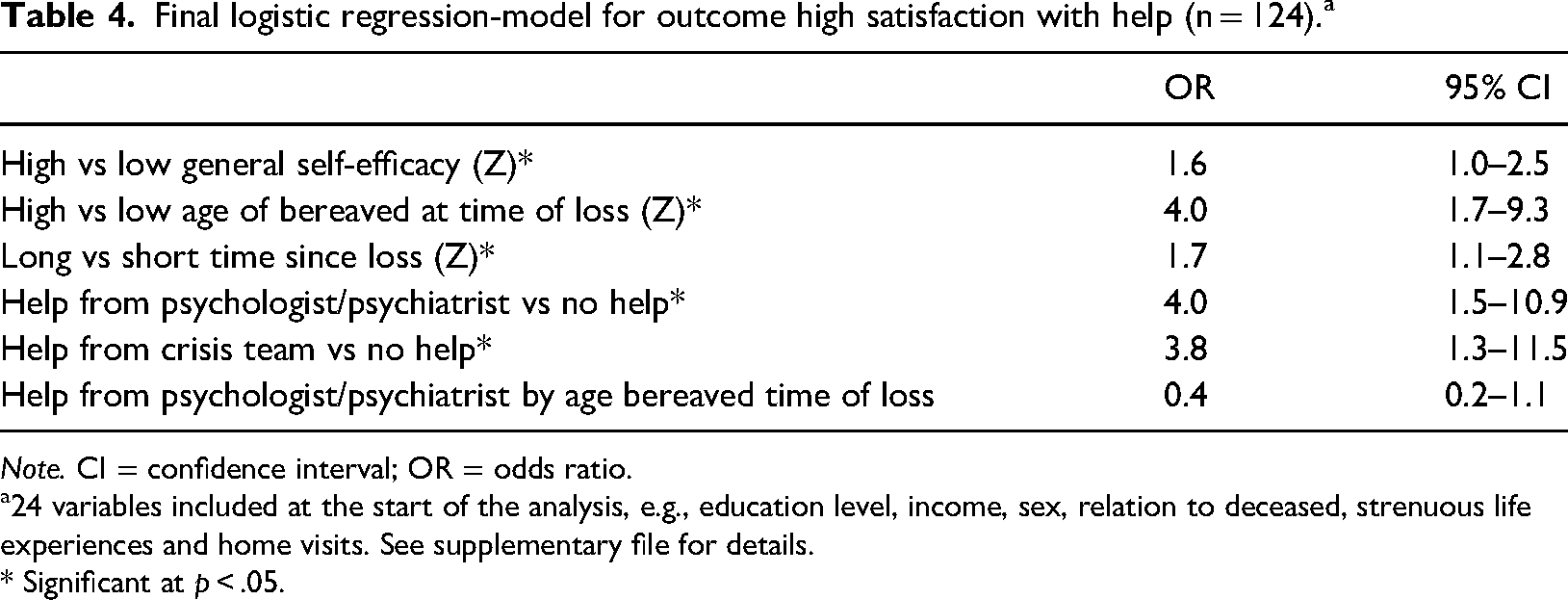
Note. CI = confidence interval; OR = odds ratio.
24 variables included at the start of the analysis, e.g., education level, income, sex, relation to deceased, strenuous life experiences and home visits. See supplementary file for details.
* Significant at p < .05.
Discussion
This article aimed to provide knowledge of which needs for help and received help from professional services were reported by DRD-bereaved family members, close friends and partners, and which variables were related to participants’ satisfaction with the help. Based on the findings, we suggest improvements in the services. Not only did most participants report a need for professional help after the death, but the mean scores of prolonged grief symptoms were high, in fact higher than in a study of Swedish parents who had lost an underage child within the last five years, comparing the same time since bereavement (Pohlkamp et al., 2019). Our sample is made up of heterogenous relations to the deceased, and as Titlestad and Dyregrov (2022) shows, there are group differences in mean scores in this sample depending on the relation. However, our sample’s overall mean score indicates that grief levels are generally high across different relations, thus showing a population exposed and vulnerable to complicated grief trajectories (Boelen & Lenferink, 2020).
About half of the participants had received help, and nearly half of them again were satisfied with the help. Parents and those who reported a high need for help received help significantly more often than others. The most important predictors for satisfaction with help were a higher age of the bereaved at the time of death, having received help from a psychologist/psychiatrist, or having received help from a crisis team. Many received help from psychologists/psychiatrists, few from crisis teams, and these help services were also missed the most. Help from a psychologist/psychiatrist tended to predict satisfaction better for the younger age group than the older. Few participants with children in the family reported that the children had received help. A majority lacked help for children, and less than one-third of participants were satisfied with the help provided for children. Based on these findings, we will discuss the manner of death, relationship to the deceased and age of participants, with similarities and differences in help needs and received help within the population. Moreover, we discuss the differences in satisfaction with services and suggestions for improved services.
Sudden and self-inflicted death predicts increased needs for help
Participants who were bereaved through intoxication with or without intention reported a higher need for help than those bereaved through disease, accident, violence or uncertain manner related to drugs. While all deaths within the first category were sudden and self-inflicted, the second category consisted of both sudden and expected, violent and non-violent, self-inflicted and other-inflicted deaths. The death’s suddenness can be one explanation for the difference in reported needs for help between these groups of the bereaved. There is considerable support in earlier research that sudden, unexpected and violent losses pose a higher risk for adverse health-related consequences for the bereaved (Djelantik et al., 2020; Kristensen et al., 2012).
The level at which self-infliction caused the death can be another part of the explanation. Self-infliction characterises both drug-induced deaths and suicides. In addition, the categories themselves overlap (EMCDDA, 2009). Although research findings differ on the consequences of suicide bereavement compared to other kinds of sudden and unexpected bereavement, experiences of stigmatisation and self-stigmatisation, meaning-making, shame and guilt seem to be more profoundly disturbing for many bereaved after suicidal deaths (Pitman et al., 2014; Shields et al., 2017; Wagner et al., 2021). These experiences are also documented in DRD bereavement, and the stigma and self-stigmatisation seem even more pronounced for those bereaved by such deaths (Dyregrov et al., 2020; Dyregrov & Selseng, 2022; Titlestad et al., 2019, 2020a, 2020b). Therefore, the suddenness, stigmatisation and level of self-infliction of the death can explain why this part of the population of DRD-bereaved people report a greater need for help.
Professional help is unequally distributed
There is an apparent discrepancy between reported needs for help and received help for participants: one-third of those who reported a need for help did not receive it. The discrepancy is higher for children, as only one-quarter of participants who had children in the family reported that they had received help. This discrepancy between the need for help and received help is higher than in other studies on traumatically bereaved populations in Norway (Dyregrov, 2002), especially compared to the follow-up after the terror attack in Norway on 22 July 2011, where 94% of the bereaved with different relations to the deceased received professional help (Dyregrov et al., 2015).
Our results show that reported needs for help did not differ significantly between relations to the deceased. A recent UK study also found that drug- and alcohol-related loss profoundly affected various relations to the deceased (Templeton et al., 2018). All these bereaved people needed recognition, and some needed more help than was available (Templeton et al., 2018). Furthermore, our results show differences in received help depending on the relation to the deceased, where parents received help significantly more often than did other relations. The difficulties for relations beyond the closest blood relatives in obtaining help parallels those recognised in the previously mentioned UK study (Templeton et al., 2018) and findings on other bereaved populations. In a study of psychosocial help to the bereaved after the 2011 terror attack in Norway where 77 people died, 25% of a sample of 67 bereaved reported rigidity in the professional services regarding who should and should not receive help (Dyregrov et al., 2015). Another study, based on interviews of bereaved friends after this attack, reported common experiences of not getting help or being acknowledged as bereaved (Johnsen & Tømmeraas, 2022). Thus, the experience of differing recognition of needs and access to help depending on relation to the deceased is a shared experience both for DRD-bereaved and other traumatically bereaved people.
The “grief hierarchy” following a death, which denotes the varying recognition and validation of grief and grief rituals depending on the relationship to the deceased (Robson & Walter, 2013), probably partly explains these differences. Which relative is contacted first after the death, which bereaved receive condolences, which bereaved organise and decide upon funeral arrangements and so on are informally and formally ordered in our culture (Cemetery Act, 1996 § 9-2; Robson & Walter, 2013). Extended family and friends do not have a prominent place in this order. A grief hierarchy provides predictability and order in circumstances of bereavement, but also creates barriers to recognising and acknowledging the help needs of the bereaved lower down in the hierarchy. Bereaved people’s call for help from a psychologist/psychiatrist may also suggest that the bereaved do not find help adequately accessible or that their wish for help is rejected. Access to help from these services is mostly available within the specialised health services, where the criteria for receiving help include a cost/benefit analysis based on referrals from other professionals in the primary health system (Norwegian Directorate of Health, 2015). Therefore, these services are not easily accessible. Bereaved people with needs for help may restrain themselves from seeking this help because of the notion that their relation to the deceased disenfranchises them from needing or seeking help, or they may be rejected if their needs are not considered severe enough. Thus, the finding that the needs for help are only partially met and that help is unequally distributed can be explained both by the grief hierarchy and the accessibility of services.
Help from some service providers predicts higher satisfaction
Those who received help from crisis teams or a psychologist/psychiatrist were more often satisfied with the help than those who received help from other services. These services were also those that participants missed the most. That help from a psychologist/psychiatrist was influential can be understood by the type of help these professionals provide and whether they have the tools to address and treat forms of complicated grief and posttraumatic stress. The term psychologist is used synonymously with psychotherapist in Norway (Lye, 2008). The academic profession of the therapist seems to be unimportant for the outcome of therapy (Fawcett & Crane, 2013; Simmons & Doherty, 1998). We can reasonably argue that the bereaved want competent professional help focusing on psychological and emotional needs. Thus, services that predict higher satisfaction with help and that participants want more of probably entail early help, flexible help and an emphasis on psychological and emotional needs –– which is in line with earlier findings on what kind of help the traumatically bereaved want (Dyregrov, 2002; Dyregrov & Kristensen, 2021).
That higher satisfaction is associated with help from specific services might be related to the finding that participants bereaved a long time ago were more likely to be satisfied with help than recently bereaved participants. As the funding of health and welfare services has increased in recent decades (Norwegian Ministry of Finance, 2021), it is unlikely that the finding is due to decreased access to and the quality of professional help. A more likely explanation is the change in the public discourse, which shows that expectations on health and welfare services have increased (Anvik et al., 2020). Psychosocial crisis teams did not exist 35 years ago (Dyregrov & Dyregrov, 2008), whereas they are now the norm in Norwegian municipalities. In addition, there is an increased awareness of and emphasis on emotional needs and therapeutic help (Madsen, 2017). The increased expectations are reflected in a national guideline from 2016 recommending proactive and flexible psychosocial professional help after crises, accidents and disasters (Norwegian Directorate of Health, 2016). Thus, satisfaction with services is likely influenced by the participants’ expectations, which again is influenced by the general public discourse and service organisation.
Special considerations should be paid to young bereaved
The bereaved person’s age at the time of death was related to satisfaction with services in that older age predicted higher satisfaction. Help from a psychologist/psychiatrist predicted satisfaction with help better for younger bereaved than older bereaved. A possible explanation for these findings is related to age-specific variables. Older age is generally associated with higher well-being and less emotional reactivity, suggesting that older persons’ emotion regulation capacities are generally better than those of younger persons (Charles & Luong, 2013; Urry & Gross, 2010). Rostila et al. (2012) found that the bereaved of younger age (18–39 years) had the highest increase in mortality risk associated with the death of a sibling, and suggested that this could be because of high stress levels, greater grief difficulties or fewer coping strategies among this group of bereaved people (Rostila et al., 2012). They also proposed that the finding could reflect the grief process in the family, where parents could be absorbed in their grief and unable to tend adequately to the bereaved sibling’s needs (Rostila et al., 2012). If the younger bereaved are less robust or receive less informal support, they may be more exposed to the adverse impacts of bereavement, which means they could need more or different help than older persons. There may also be cultural and context-bound explanations to lower levels of satisfaction of the younger bereaved, as emphasis on emotional needs and expectations of help from a therapist have become more acknowledged among new generations (Madsen, 2017). That younger persons are less satisfied with the help and that their satisfaction depends more on help from a psychologist/psychiatrist can thus be related to biological/developmental factors, family-related factors and changes in culture and expectations between generations.
Participants reported a low level of received help for children in the family. This can be understood in the broader context of Norwegian health services. Until recently, children as relatives/peers have lacked recognition in policy documents and services (Norwegian Ministry of Health and Care, 2009). A new law intended to ensure that health services recognise and include children as relatives was introduced in 2010 (Norwegian Directorate of Health, 2010), and in 2017 the law was extended to include a focus on children as bereaved people (Health Personnel Act, 1999 § 10b). Thus, the lack of help to children in our sample can at least partly be explained by the lack of recognition in policy documents until recently, which again is related to the general individual-centred focus within health services and the associated professions (Kalsås et al., 2020, p. 14; Ruud et al., 2015). Another explanation is probably professionals’ insecurity and lacking competence of helping bereaved children (Dyregrov & Dyregrov, 2013). Ruud et al. (2015) recommend that children and family be one of the main themes in all examinations and treatment within health services and that all services should include a child and family perspective. Dyregrov (2021) also recommends aid to families in creating open and direct communication between adults and children to help them cope and avoid the development of complicated grief reactions. Our findings show that the bereaved are lacking help for children and report low satisfaction, which suggests that an adequate child- and family-based perspective has been absent in the follow-up of the bereaved after a DRD.
Implications for practice and future research
The DRD-bereaved call for help from professional services. Services should routinely and proactively contact the bereaved and offer help if necessary. Based on our findings, we suggest that special considerations should be paid to younger age groups, especially children, and services probably need a family perspective in their follow-up to adequately reach them. The term “bereaved” should be defined broadly, including different family members, children, partners and close friends. Both psychological and biological closeness should be emphasised.
We need more knowledge of the DRD-bereaved who report a high need for help but do not receive it, and how relevant services can reach them. There is also a need for more research on bereaved people’s experiences of the helping relationships, where our results only provide a basic frame. In addition, more research is essential on how children can be acknowledged and helped in their own right and as part of help efforts for grief-stricken families. Finally, in these circumstances it is often necessary that different services organise help efforts flexibly but predictably in a situation where help needs vary over time (Norwegian Ministry of Health and Care, 2015). Further central questions concern approaches where different services can successfully include different relations, operate across sectoral boundaries and provide flexible, needs-based and broad-spectrum help over time within an acceptable cost/benefit frame.
Strengths and limitations
As far as we know, this study is the largest of DRD-bereaved family members, partners and friends. It is a strength that a considerable effort was made to recruit the broadest possible sample, both geographically and in sociodemographic terms. Strengthened validity and ethical consciousness have also been achieved by close cooperation with user representatives from the target population in study development and data collection. The survey was made available for those with less digital competence by including manual forms, reducing selection bias.
The cross-sectional design is not well suited for establishing causal relationships. In terms of the findings, we therefore argue for associations, not causality. As a non-probability sample, generalisations must be made cautiously. Selection bias may be present because of geographical overrepresentation from the south of Norway, skewed sex distribution in favour of females, which is often the case in studies on bereavement (see Boelen et al., 2016; Feigelman et al., 2009), and above average scores on socioeconomic variables (Statistics Norway, 2020). It is documented that low scores on socioeconomic variables are associated with higher risks of opioid-related overdoses (van Draanen et al., 2020), thus suggesting that a representative sample of DRD-bereaved people would also mirror this distribution. Since our sample reported average income and above-average education level compared to the general Norwegian population, the target population must probably cope with less psychosocial resources than our study sample.
There is a likelihood of recall bias because of the 35 years separating the different losses within the sample. This may especially influence the finding that time since loss predicts higher satisfaction with help. It is also important to note that the needs of bereaved children and adolescents are reported by adult family members, which may over- or understate their needs. Some participants were related to the same deceased, but the dataset did not contain sufficient information to identify dependent observations. Finally, it was not possible to fit a complete logistic regression model with all relevant variables because of inadequate data power, which we solved using “purposeful selection” (Hosmer et al., 2013). Confidence intervals in the results of this analysis are wide, primarily due to the low number of participants who had received help from a crisis team (n = 25).
Conclusion
This study shows that only a minority of those bereaved through a DRD received adequate help, and help for children was rare and perceived as unsatisfactory. Younger age groups and children need particular recognition, and a family perspective from services is essential for them to be reached adequately. When assessing the help needs of the DRD-bereaved, relations of both psychological and biological closeness should be recognised, including children, siblings, extended family members and close friends. Help efforts should be tailored according to established knowledge of help that bereaved populations deem effective. Every country must establish a foundation through legislation and guidelines that enables services to help and support the bereaved adequately. In Norway, this framework is established through the guideline for psychosocial measures in crises, accidents and disasters (Norwegian Directorate of Health, 2016).
Supplemental Material
sj-docx-1-nad-10.1177_14550725221125378 - Supplemental material for Needs for help and received help for those bereaved by a drug-related death: a cross-sectional study
Supplemental material, sj-docx-1-nad-10.1177_14550725221125378 for Needs for help and received help for those bereaved by a drug-related death: a cross-sectional study by Øyvind Reehorst Kalsås, Kristine Berg Titlestad, Kari Dyregrov and Lars Thore Fadnes in Nordic Studies on Alcohol and Drugs
Footnotes
Acknowledgements
We acknowledge the END project and the user representatives, for valuable inputs and interpretations concerning the findings. We also thank Associate Professor Lillian Bruland Selseng and Professor Sigurd Hystad for their respective help with study design and analyses.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by The Western Norway University of Applied Sciences and The Research Council of Norway
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
