Abstract
Background
Subjective cognitive decline (SCD), defined as self-perceived cognitive worsening despite normal performance on standardized tests, is increasingly recognized as a potential early indicator of Alzheimer's disease and related dementias. Older adults with SCD face elevated dementia risk and may benefit from timely intervention or support. To guide such efforts, qualitative research is needed to understand how they experience and perceive cognitive changes in daily life.
Objective
This study aims to explore the daily life experiences of community-dwelling older adults with SCD, including how they respond to self-perceived cognitive changes, the impact on daily functioning and well-being, and their perceived factors associated with cognitive performance.
Methods
Using a qualitative descriptive approach, we conducted semi-structured interviews with 16 older adults who reported cognitive decline but showed no objective cognitive impairment. Transcripts were analyzed using thematic analysis to identify key themes related to lived cognitive experiences.
Results
Four major themes emerged: (1) cognitive changes manifesting in everyday tasks across domains such as memory, attention, and executive function; (2) active use of intentional internal and external strategies to manage these changes; (3) varied emotional responses and appraisals shaped by personal expectations and contextual factors; and (4) perceived risk (e.g., aging, stress, poor sleep) and protective factors (e.g., mental stimulation, social engagement) for cognitive function.
Conclusions
Participants with SCD reported cognitive changes that have influenced their daily activities, emotional well-being, and social interactions. Future research may consider person-centered strategies that support cognitive self-management and improve well-being among older adults with SCD.
Keywords
Introduction
Many older adults experience self-perceived worsening of cognitive function as they age. According to the Behavioral Risk Factor Surveillance System (BRFSS) survey, approximately 11% of U.S. adults aged 45 and older reported increased confusion or memory loss in the past year. 1 Importantly, even when cognitive performance remains within normal ranges on standardized tests, self-reported cognitive concerns—referred to as subjective cognitive decline (SCD) 2 —have been linked to an elevated risk of developing mild cognitive impairment (MCI) 3 and dementia. 4 Emerging research has also associated SCD with brain atrophy 5 and Alzheimer's disease (AD) biomarkers, such as beta-amyloid and tau accumulations. 6 As traditional cognitive assessments may be limited in capturing subtle changes in cognition, SCD is increasingly considered as a potential early indicator of AD and related dementias. To clarify the concept of SCD in the context of preclinical AD, the Subjective Cognitive Decline Initiative (SCD-I) working group proposed a research framework that includes two key criteria 2 : (1) a self-experienced and persistent decline in cognitive ability compared to a previously normal level, not explained by an acute event, and (2) performance within the normal range on standardized cognitive tests.
Over the past decade, research on SCD has expanded, primarily focusing on its epidemiological patterns and potential as a preclinical marker for cognitive impairment. However, limited attention has been paid to how individuals personally experience and navigate these early cognitive concerns. As a subjective phenomenon, SCD is shaped not only by cognitive changes themselves but also by individual, psychological, and socio-cultural contexts.7–9 Few studies have employed qualitative methods to explore how cognitive changes manifest in everyday life, and existing qualitative research has largely focused on individuals with diagnosed MCI or dementia.
Individuals with SCD often function independently, but may experience subtle cognitive lapses, such as not remembering the things they usually know or forgetting how to do the things they have always done,10,11 which may affect their confidence, daily routines, and well-being. 12 SCD offers a valuable window for early, preventive intervention before clinical impairment or dementia becomes evident. Understanding how older adults interpret and respond to these changes in the context of daily life is essential for developing person-centered interventions and support.
This study aims to explore the daily experiences of cognitive changes among community-dwelling older adults with SCD. Specifically, we seek to understand how they perceive and describe their cognitive changes, how their everyday lives and well-being are affected, how they manage these changes, and what contextual factors they believe influence their cognitive performance. By centering the voices of individuals with SCD, this study contributes to a more nuanced understanding of the subjective experience of early cognitive change and lays the foundation for providing supportive care and early intervention in future research.
Methods
To explore the daily experiences of cognitive changes in older adults with SCD, this study used a qualitative descriptive approach. 13
Participants
Older adults aged 50 or older, community-dwelling, English speaking, and meeting the criteria of SCD were eligible for this study. The following criteria were used to define SCD based on the SCD-I conceptual framework: 1) self-reported cognitive decline; 2) no objective cognitive deficits (Montreal Cognitive Assessment [MoCA] scores within normal range); 3) no diagnosis of dementia; 4) no significant functional impairment (Functional Activity Questionnaire [FAQ] < 9). Self-reported cognitive decline was determined if the participant endorsed the question, “Over the past several years or as getting older, have you experienced confusion or memory loss that is happening more often or is getting worse?”, which was adapted from the SCD assessment in the BRFSS survey. 14 The original question refers to a past 12-month timeframe, which is relatively too short to reflect the preclinical process of AD. To better capture the concept of “self-experienced persistent decline in cognitive capacity” as emphasized in the SCD-I framework, we expanded to participants who reported cognitive declines over the past several years or with aging.
Participants were purposively recruited in collaboration with the mPATH study (NCT05935241), an ongoing clinical trial conducted in Baltimore, Maryland. Recruitment strategies included community outreach, newspaper advertisements, and online platforms such as MyChart, Nextdoor, and Facebook. For the participants who enrolled in the mPATH study, data were collected in person, regardless of SCD status. We enrolled only those participants who met our study's inclusion criteria from the mPATH dataset. For the participants who did not enroll in the mPATH study due to ineligibility or not interested, recruitment was conducted separately. A research team member screened these individuals for eligibility for this study and, if interested and eligible, scheduled a virtual appointment for data collection using the same interview guide.
Eligible participants who met the SCD criteria were recruited sequentially until data saturation was reached, which was monitored concurrently with recruitment and analysis. Data saturation was determined based on both code saturation and meaning saturation, when no new codes, dimensions, nuances, or insights emerged from the data. 15 Although data collection for the mPATH study continued, interviews conducted after saturation were not included in this analysis.
Measures
Screening tools
MoCA is a brief cognitive screening tool widely used to detect mild cognitive impairment by assessing global cognitive function. 16 It covers multiple cognitive domains, including attention, executive function, memory, language, and orientation. The standard in-person version was administered during in-person data collection, while the telephone version (T-MoCA) was used for virtual data collection. Consistent with established cutoffs, scores >25 on the in-person MoCA 16 and >19 on the T-MoCA 17 were considered as cognitively intact.
FAQ is a questionnaire for evaluating the level of functional ability in performing daily activities, such as paying bills, shopping, and preparing meals. 18 A total score of < 9 is generally interpreted as indicating no significant functional impairment, supporting the absence of cognitive impairment or dementia. 18
Semi-structured interview guide
A semi-structured interview guide with open-ended questions was designed (Table 1) based on our research interests and a previous qualitative study investigating the impact of memory changes on daily life in older adults. 19 The interview guide was first piloted within the research team, reviewed by qualitative methodology experts, and was slightly adjusted after the first several interviews with participants. 20
Semi-structured interview guide.

Everyday cognition scale—short version (Ecog-12)
While there is no universally accepted measure for assessing SCD, Ecog scale 21 is a relatively widely-used self- or informant-report questionnaire that evaluates perceived changes in cognitive functioning during daily activities. The short-version, Ecog-12, 22 includes 12 questions related to common cognitive tasks such as remembering where objects are placed, navigating directions, and following conversations. Participants are asked to rate their current level of functioning compared to 10 years ago using a four-point scale: 1 = better or no change, 2 = occasionally worse, 3 = consistently a little worse, and 4 = consistently much worse. The total Ecog score is calculated by dividing the sum of completed item scores by the number of items completed, resulting in a score ranging from 1 to 4, with higher scores indicating greater subjective cognitive concerns. In this study, the Ecog-12 was administered after the qualitative interview or at a different data collection appointment, to avoid influencing participants’ responses during the interview.
Procedures
One-on-one interviews were conducted either in person, via Zoom, or by phone. Participants were interviewed as part of a broader qualitative study that explored various aspects of daily life, including sleep, cognition, physical activity, and technology use. For the present study, we focused on the portion of the interview related to cognition, which typically lasted between 10 and 20 minutes. The semi-structured interview guide (Table 1) was employed to ensure consistency across interviews while allowing flexibility for participants to share additional insights.
Data analysis
Thematic analysis was used to analyze the data, adhering to the six phases outlined by Braun and Clarke.23,24 All interviews were audio-recorded and transcribed verbatim. Analyses were conducted in Atlas.ti®, a qualitative data analysis software. To begin, we read the transcripts thoroughly to gain a comprehensive understanding of the content and re-read the cognitive section for interest of this study to get familiar with the data. In the second phase, we developed a preliminary codebook informed by the interview guide and initial readings of the data. Each code was defined, with descriptions and illustrative examples to ensure consistent application. As analysis progressed, the codebook was iteratively revised to reflect emerging insights, and new codes were added as needed. In the next phase, we sorted, compared, and grouped the codes using thematic networks to identify potential subthemes and overarching themes. During the fourth phase, these themes were reviewed and continuously refined through team discussions to make sure they reflected the data and captured meaningful patterns. We then finalized and named each theme. In the final phase, we synthesized the findings to develop a cohesive narrative that reflected participants’ experiences and perspectives on cognitive changes in the context of SCD. The analysis process is displayed in Figure 1.
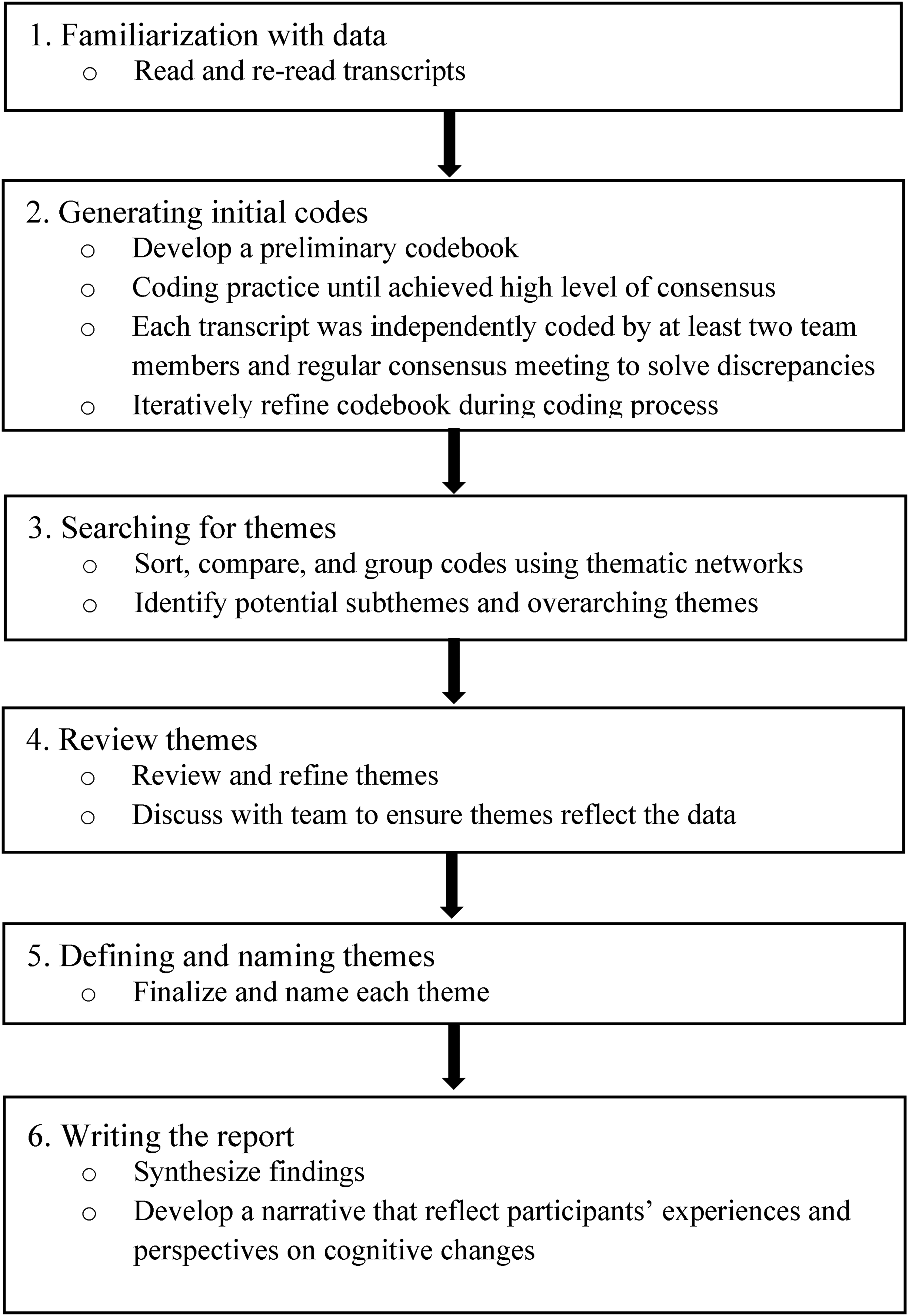
Adapted thematic analysis process (Braun & Clarke, 2006). 23
To enhance the methodological rigor of the study, we applied the criteria of credibility, dependability, confirmability, and transferability, as proposed by Guba and Lincoln 25 and expanded upon by Nowell et al. 24 To enhance credibility, the extent to which findings accurately reflect participants’ experiences and perspectives, we collaboratively reviewed the codebook and conducted practice coding sessions until a high level of consistency was achieved. Each transcript was independently coded by at least two team members (i.e., JH, YC, CW), followed by regular consensus meetings to resolve any discrepancies. In cases where disagreements persisted, additional researchers were consulted to reach a final consensus. Dependability, which refers to the stability and consistency of the research process over time, was established by maintaining detailed records of coding decisions, analytic memos, and the thematic development process. Confirmability defined as the degree to which findings are derived from the data rather than researcher bias, was strengthened through ongoing reflexive practice, including critical discussions about researcher assumptions and potential biases during team meetings. To support transferability and generalizability of the findings, we provided rich descriptions of the study context, sampling strategy, and participant characteristics, enabling readers to assess the applicability of our findings to other settings.
Results
Participant characteristics
A total of 16 participants were included in the final sample, and all 16 interviews were included in the analysis. This sample size is in the range of recommended sample sizes for qualitative studies.15,26,27 As shown in Table 2, the 16 participants had a mean age of 70.7 years (SD = 8.0), ranging from 52 to 83. Most of the participants were female (68.8%), White (62.5%), and had completed some college or higher education (81.3%). Additionally, 18.8% had a household income below 200% of the Maryland poverty level, and 31.3% were married. Participants had an average of 2.63 (SD = 1.26) chronic conditions. Nine participants (56.3%) reported a history of diagnosed depression or anxiety, and six (37.5%) were currently taking antidepressants. The average Ecog-12 score was 1.68 (SD = 0.53; range: 1.08–2.55), suggesting participants averagely endorsed functioning as between “no change” and “occasionally worse”, compared with 10 years ago.
Participant characteristics (n = 16).

SD: standard deviation.
Thematic analysis identified overarching themes and associated subthemes, which are summarized in Table 3 and described in detail below.
Summary of themes and representative quotations.
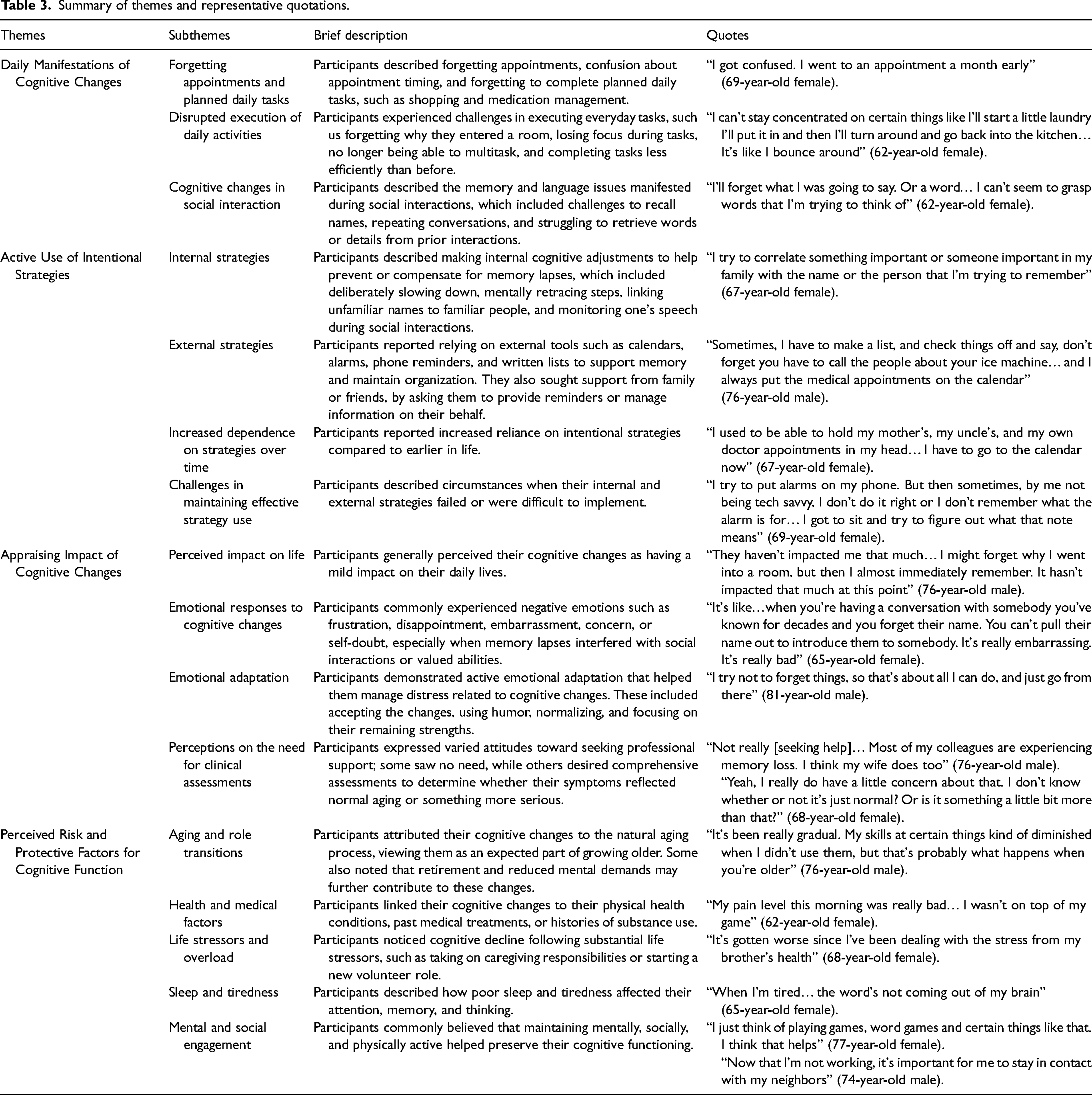
Theme 1: Daily manifestations of cognitive changes
Participants with SCD described their perceived declines in cognitive abilities and reported instances of these declines in their daily life experiences. These cognitive changes manifested across various aspects of daily life, from managing appointments and tasks to communication and social interaction. In turn, these cognitive changes affected their daily routines, reduced task efficiency, and hindered social engagement. We grouped them into three subthemes: 1) forgetting appointments and planned daily tasks, 2) disrupted execution of daily activities, and 3) cognitive changes in social interaction.
Forgetting appointments and planned daily tasks
Participants commonly reported forgetting appointments and to do planned daily tasks. They described this as a general tendency: “I think I forget to do things if I don't write it down” (77-year-old female) and “I had problems with keeping my appointments…” (67-year-old female). Participants also confused the timing of their appointments, arriving on the wrong day or even the wrong month. One participant shared, “If I don't put these appointments down, then I'll mess around. I'll either go the day before the appointment, or I'll go in the day after” (67-year-old female). Another added, “I got confused. I went to an appointment a month early” (69-year-old female).
Forgetfulness also occurs to other daily life tasks, such as forgetting to retrieve items from the dry cleaners or postponing shopping trips for days: “It might take me three or four days to remember to go to the store to get a certain item” (68-year-old male). Medication management was another concern, as expressed by one participant: “I feel like I'm not keeping up with stuff. Like, oh, did I take my medicine? Did I order my medicine? I could’ve sworn that I ordered it” (69-year-old female). This subtheme highlights forgetfulness as a key manifestation of cognitive changes perceived by participants with SCD.
Disrupted execution of daily activities
Participants described disruptions in performing everyday tasks due to changes in memory, attention, and cognitive control. A frequently mentioned experience was forgetting the reason for entering a room: “Sometimes I walk into the other room to get something, and I can't remember what it is” (83-year-old female). Participants might also experience a decline in performance in the daily tasks that they used to do well. For example, a participant once could do advanced calculus during his academic career reflected, “I'm really disappointed my ability to do math isn't the way it used to be… it's definitely gotten worse” (76-year-old male). Participants described struggles with remembering recipes or experiencing momentary disorientation in familiar environments: “Like I went away for a couple of weeks and when I came back home, I couldn't remember which way to turn the key in the door. You know, that's a natural thing. But I couldn't remember” (69-year-old female).
Participants also described difficulty maintaining focus on a single task, challenges with multitasking, and a reduced ability to complete tasks as efficiently as they once did. One explained, “I can't stay concentrated on certain things like I'll start a little laundry I'll put it in and then I'll turn around and go back into the kitchen…” (62-year-old female). Another reflected that “I can no longer really multitask. I was always a multitasker, and I could do 10 different things at one time and jump from one into the other and keep it all going. I can't do that anymore. It's hard enough for me to keep one thing going now [laughs]” (67-year-old female). This participant also shared a safety concern related to distraction while cooking: “I don't have the concentration that I used to have. I could make something, and then when I take it off the stove. I might forget to turn the stove off because I had it on a real low flame and I don't see it, and I'll forget. I've done that a couple times.” These challenges demonstrated how cognitive changes have impacted overall functioning in everyday activities and may even cause safety concerns.
Cognitive changes in social interaction
Participants described how memory and language issues manifested during conversations and social interactions. These experiences included challenges to recall names, repeating information, and struggling to retrieve details from prior interactions. One participant stated, “I have people that I haven't seen in quite a while, I have forgotten their names” (77-year-old female), while another observed, “It takes me longer to recall the name” (67-year-old female). Participants reported forgetting details of earlier conversations: “There was something that happened earlier in the day or something I said earlier in the day and they (friends or family) are trying to recall it. Sometimes I couldn't quite recall it all or not at all” (74-year-old male), and “Somebody will say, ‘Oh, they said this,’ and I have no recollection” (67-year-old female).
Language retrieval difficulties seemed to disrupt communication mid-sentence. One participant noted, “I’ll forget what I was going to say. Or a word… I can’t seem to grasp words that I’m trying to think of” (62-year-old female). Another described the experience of losing familiar words in the middle of a conversation: “And I think that the most prevalent thing in my mind is that things are on the tip of my tongue. It'll be like a super familiar word or phrase or name or place that I absolutely should know. And for whatever reason, I'm in the middle of a conversation and it's just gone, even though I know I should know it” (52-year-old female). These experiences illustrate how language and memory challenges can affect communication and social interactions among older adults, impacting their social relationships and engagement.
Theme 2: Active use of intentional strategies
When discussing cognitive changes, older adults with SCD consistently mentioned using various intentional strategies to help them remember and reduce the impact of cognitive decline. These strategies—both internal and external—were often integrated into everyday routines and adopted in response to increasing challenges in attention, memory, and organization. While participants commonly found these strategies helpful, some of them shared limitations or frustrations when strategies were inconsistently applied or failed to work as intended. This theme is organized into four subthemes: 1) internal strategies, 2) external strategies, 3) increased dependence on strategies over time, and 4) challenges in maintaining effective strategy use.
Internal strategies
Participants described making internal cognitive adjustments to help prevent or compensate for memory lapses at the moment. These self-regulatory strategies included deliberately slowing down, mentally retracing steps, and monitoring one's speech during social interactions. For example, one participant explained how she coped with forgetting the purpose of entering a room: “I just try to retract or keep thinking, thinking, thinking, and then it's been coming to me” (68-year-old female). Another participant shared how she purposely increased her self-monitoring during social interactions: “Before I start saying something, I'll start thinking, have I already said this? Or is this a question I've already asked?” (52-year-old female). Some participants also used internal memory cues to aid recall. One participant described linking unfamiliar names to familiar people in her life as a strategy: “I try to correlate something important or someone important in my family with the name or the person that I'm trying to remember” (67-year-old female). This subtheme highlights participants’ active self-regulation efforts to manage momentary memory challenges.
External strategies
External strategies were widely used to aid memory. Participants reported relying on external tools such as calendars, alarms, phone reminders, and written lists to support memory and maintain organization. For example, a participant mentioned, “I have to put everything in my phone, even the support moves” (68-year-old female). Another participant noted, “Sometimes, I have to make a list, and check things off and say, don’t forget you have to call the people about your ice machine… and I always put the medical appointments on the calendar” (76-year-old male).
Participants used environmental cues, such as wall calendars or placing items in visible locations. For example, “When I have to leave to go to work in the morning, I put whatever I need to take with me to go to work by the door, so that when I leave, I’ve got it all” (62-year-old female), and “I just write stuff down there [on the refrigerator]. That's helping out a little bit better because that's something that I actually see” (68-year-old male).
Participants also sought support from their social environment, by asking family or friends to provide reminders or manage information on their behalf. One participant described a typical scenario: “So I would say, can you just send me a text? Basketball game with the date and the time. And then, when I go home, I started putting reminders into my calendars” (68-year-old male). Another participant, despite having marked the appointments on her calendar, still sought reassurance: “Please don’t forget to call me and remind me as it gets closer, even though it's on the calendar” (62-year-old female). In some cases, participants delegated responsibility entirely, such as giving family member the event tickets and asking, “You hold the ticket … and always remind me” (69-year-old female).
In summary, participants used tools, environment cues, and support from others to aid memory and reduce the risk of lapses during daily activities and interactions.
Increased dependence on strategies over time
Participants noted that they relied on these strategies more than in the past. They contrasted their current habits with earlier stages of life when they could manage tasks without external support. One participant shared, “I used to be able to hold my mother's, my uncle's, and my own doctor appointments in my head… I have to go to the calendar now” (67-year-old female). Another observed, “I used to remember everything … now I write it down. And if I don’t bring that list with me, I forget something” (76-year-old male). This growing reliance was also reflected through more effortful planning: “I definitely spend more time organizing, preparing, being proactive, writing things down, texting myself” (52-year-old female).
Challenges in maintaining effective strategy use
While using these internal and external strategies to stay organized in their daily lives, participants described moments when their strategies failed or were difficult to implement. As an example of challenge in using internal strategies, participant described the difficulty of staying engaged in conversation while trying to retain a thought: “I wasn’t paying attention to what I was supposed to be paying attention to because a question pops into my mind and I was trying to remember it” (65-year-old female).
When using external strategies, forgetting to check calendars, misplacing lists, or relying on multiple tools sometimes led to confusion. Participants recalled that even though they put things on the calendar or set alarms, they could still forget. As one noted, “I put it on the calendar and it totally went out of my head…” (62-year-old female). Maintaining consistency in strategy use was also challenging, particularly when participants relied on multiple tools or forgot to bring them along. “I forgot to look at both calendars. So I just forgot about that appointment” (65-year-old female), and “Sometimes I’ll get outside, and I don’t have my shopping list” (81-year-old male).
Participants also described how fast-paced environments or multitasking disrupted their ability to implement strategies effectively. Competing demands could interrupt the moment of strategy use, leading to missed tasks. As one participant explained, “Before I go to put it in my calendar, I get a phone call and I forget all about putting the appointment in my calendar, and I missed an appointment” (68-year-old male).
Additionally, participants might also encounter challenges using technology-based tools. One participant explained, “I try to put alarms on my phone. But then sometimes, by me not being tech savvy, I don’t do it right, or I don’t remember what the alarm is for… I got to sit and try to figure out what that note means” (69-year-old female). This subtheme illustrates how cognitive lapses still occurred despite participants’ active use of internal and external strategies, particularly under conditions of distraction, multitasking, or technological difficulties.
Theme 3: Appraising impact of cognitive changes
Participants reflected on how their memory and cognitive changes influenced their daily lives and emotional well-being. Although most did not perceive these changes as having a significant impact on their lives overall, they expressed a range of negative emotions when cognitive lapses occurred, such as frustration, concern, or emotional discomfort. In response to these experiences, participants also demonstrated active emotional adaptation and expressed varied views on the need for clinical support. These appraisals appeared to be shaped by the perceived severity of symptoms, the extent to which daily life was affected, social contexts, and personal expectations regarding cognitive performance. Four subthemes emerged: 1) perceived impact on life, 2) emotional responses to cognitive changes, 3) emotional adaptation, and 4) perceptions on the need for clinical assessments.
Perceived impact on life
Participants generally perceived their cognitive changes as having mild impact on their daily lives. One participant shared, “They haven’t impacted me that much… I might forget why I went into a room, but then I almost immediately remember. It hasn’t impacted that much at this point” (76-year-old male). Similarly, others noted that the absence of serious consequences, such as missing important appointments or misplacing money, reassured them that their memory lapses were not yet problematic: “Not yet. You know, if I start misplacing money, or totally forgetting to get to a doctor's appointment, that would be a problem” (65-year-old female).
Participants cited their active use of intentional strategies and structured routines, which helped them minimize the impact of their cognitive changes. “It doesn’t impact my life because I’ve learned to proactively avoid that situation by writing things down, documenting things on the computer” (52-year-old female), and “I do the same thing every day, and you don’t forget that way” (81-year-old male). This subtheme reflects participants’ perceived level of concern and the degree to which cognitive changes affected their everyday lives, which was generally low due to absence of severe consequences and the use of compensatory strategies.
Emotional responses to cognitive changes
Emotional reactions to cognitive changes varied among the participants. Participants sometimes reported neutral emotional reactions to their cognitive changes. For instances, “If I don’t remember something, I just don’t remember. It doesn’t make me feel bad or anything” (77-year-old female).
However, participants also commonly experienced negative emotions such as frustration, disappointment, embarrassment, concern, or self-doubt, especially when memory lapses interfered with social interactions or valued abilities. “I don't like it. If I forget something major, I'd be upset with myself because I forgot it” (67-year-old female). Participants described the loss of cognitive skills they once prided themselves on: “I'm really disappointed my ability to do math isn't the way it used to be… I used to be very good at it when I was younger” (76-year-old male). They described social discomfort, such as forgetting the name of an old acquaintance: “It's really embarrassing. It's really bad” (65-year-old female) and repeating information in conversations: “It's frustrating because I start telling it [a story] and feel like [they are saying] ‘I’ve already heard you tell me this’” (62-year-old female). They also expressed mild concerns about their cognitive changes. One participant noted, “Mostly I'm just aware of it and there's a little bit of worry in the back of my mind” (74-year-old male). Another recognized, “Yeah, I really do have a little concern about that. I don't know whether or not it's just normal? Or is it something a little bit more than normal?” (68-year-old female).
Participants described emotional distress and diminished self-image related to their cognitive changes. One participant experiencing chronic pain on her foot, facing multiple health and life stressors, described feeling overwhelmed and diminished: “Sometimes it makes me feel inadequate… So, the memories, the not being able to do what I would normally want to do, not being able to do what my mind wants to do, put a change on who I am. I feel like I lost myself. My 100% feels like 25% compared to everybody else's” (69-year-old female). Another participant described persistent worry and hypervigilance: “I think I’m over-organized out of necessity because I worry that I’m going to forget something” (52-year-old female). For her, these concerns extended into social situations, where she became guarded and self-conscious: “Instead of just organically having a conversation, I’m kind of in my head wondering whether or not this is the right thing for me to say.” These reactions were possibly related to her high personal standards on herself and others: “I also think I have a higher expectation of other people, and I get irritated when other people aren't the same way.” This subtheme captures the emotional complexity surrounding cognitive lapses, ranging from neutrality to persistent strain, and highlights how such lapses can affect one's identity, confidence, and social engagement.
Emotional adaptation
While participants acknowledged experiencing negative emotional responses to cognitive changes, they also demonstrated active emotional adaptation that helped them manage distress. These included accepting the changes, using humor, normalizing, and focusing on their remaining strengths. One participant described a shift in her attitude over time—from defensiveness to acceptance: “I used to say, ‘I know you told me that.’ Now I just say, ‘You probably said it. I didn’t hear it right or I don’t remember’” (67-year-old female). Humor also served as a means of emotional relief, as another participant shared: “We just try to laugh at stuff, even if it's really not funny” (68-year-old female). Participants described similar memory lapses in their peers and felt this was normal for their age: “They (friends) are just as bad as I am” (68-year-old female). They focused on what they could still do: “I try not to forget things, so that's about all I can do, and just go from there” (81-year-old male). Cognitive changes were seen as a natural part of aging and were integrated into a broader understanding of life transitions: “It's just one of those things… I’m not concerned about it, and nobody else seems to be concerned about it, so I’m not too worried” (81-year-old female). This subtheme highlights how participants with SCD employed emotionally adaptive strategies to manage distress related to perceived cognitive changes.
Perceptions on the need for clinical assessments
Participants varied in their attitudes toward seeking professional support or assessments for their cognitive concerns. Some saw no need, viewing their experiences as typical for their age or comparable to those of peers. “Not really [seeking help]… Most of my colleagues are experiencing memory loss. I think my wife does too” (76-year-old male). Others felt their memory issues were not severe enough to warrant clinical support: “No, because I don’t think it's that bad” (81-year-old male). In contrast, a few participants expressed a desire for more thorough assessment. One participant described dissatisfaction with the standard cognitive screening during a Medicare visit: “To me, you can't really figure out by that little exercise. No, it's not enough” (68-year-old female). She expressed a need to obtain more comprehensive assessments to figure out her symptoms were part of normal aging or something more serious.
Theme 4: Perceived risk and protective factors for cognitive function
Older adults with SCD described a range of causes and contextual factors they believed influenced their cognitive performance. These perspectives reflected both long-term attributions—such as aging and health conditions—and short-term influences, such as stress and poor sleep. Participants also discussed factors they believed supported or enhanced cognitive functioning, particularly mental and social engagement. Five subthemes emerged: (1) aging and role transitions, (2) health and medical factors, (3) life stressors and overload, (4) sleep and tiredness, and (5) mental and social engagement.
Aging and role transitions
Participants viewed their cognitive changes as a natural consequence of aging. Forgetfulness and slowed processing were described as expected features of growing older: “I do believe it's come over time, but also I think it's part of the aging process that your mind starts to slow down” (74-year-old male). In addition to aging itself, participants noted that retirement and transitions away from mentally demanding roles might reduce their cognitive stimulation. One participant reflected, “It's been really gradual. My skills at certain things kind of diminished when I didn’t use them, but that's probably what happens when you’re older” (76-year-old male). Another participant affirmed, “Before, you're raising your family … now I'm retired. I don't have kids to take care of. So my brain is not engaged as much… I don't have to try to remember stuff” (62-year-old female). This subtheme captures participants’ conceptualization of cognitive changes as an inevitable and normal part of the aging process, understood through both biological aging and reduced cognitive stimulation.
Health and medical factors
Participants also attributed cognitive changes to physical health conditions, past medical treatments, or histories of substance use. Participants described their cognitive changes as linked to specific medical experiences, including chemotherapy, pain, and surgeries. One participant reflected on the lasting impact of cancer treatment: “Definitely with chemo…” (65-year-old female). However, she added that her husband, who hadn’t undergone chemotherapy, experienced similar memory lapses, implying that chemotherapy may not be the sole contributing factor. Participants pointed to chronic pain as interfering with focus and memory. One shared, “My pain level this morning was really bad… I wasn’t on top of my game” (62-year-old female). Participants also linked cognitive changes to substance use history and stated, “Now that I don’t do drugs anymore, my memory is not as strong” (67-year-old female).
Life stressors and overload
Participants reported noticing cognitive decline following substantial life stressors, such as taking on caregiving responsibilities or starting a new volunteer role. They described how heavy schedules, multitasking, and role overload appeared to negatively impact their cognitive performance. A participant reflected, “It's gotten worse since I’ve been dealing with the stress from my brother's health” (68-year-old female), while another observed slight improvement after stepping back from caregiving duties: “I probably got a little relief from all the stress” (67-year-old female). A participant who had recently taken on a demanding volunteer position noted, “I just got a lot more on my plate … a lot of times my job doesn’t end when I get home” (68-year-old male). Similarly, others described memory lapses when feeling overwhelmed by busy routines: “It usually happens when I got a lot going” (69-year-old female).
In addition to chronic stressors, participants identified acute pressure (e.g., rushing or multitasking) as contributing to momentary lapses in attention and recall. A participant described difficulty thinking clearly when getting multiple demands: “When I’m doing several things at once and more demands are placed… I can’t think that through” (74-year-old male). Others also noted a cognitive toll of rushing: “When I’m in a hurry, I find that I am more likely to just kind of ramble” (52-year-old female). This subtheme illustrates how participants with SCD perceived declines in cognitive performance during various stressful situations, including role overload, multitasking, and emotional strain.
Sleep and tiredness
Sleep quality and tiredness were identified as important factors on cognitive performance. Participants described how poor sleep negatively affected attention, memory, and thinking. Participants shared, “When I’m tired… the word's not coming out of my brain” (65-year-old female). They reflected on sluggish thinking: “If I don’t get a good night's sleep, I’ve got to play catch up… I feel like there's some confusion” (68-year-old male). They also shared how good sleep helped with memory: “When I sleep well… my memory—it's all much better” (76-year-old male).
Participants also noted that poor sleep and tiredness might affect their ability to function socially and physically, which might in turn impact cognitive performance. “When I’m very tired… the poor quality of my sleep keeps me from seeing people” (83-year-old female). They explained, “When I don’t sleep, I can’t walk… but when I get several days of sleep, I feel like I want to get out and do things” (76-year-old male).
Mental and social engagement
Participants commonly described the belief that staying mentally, socially, and physically active helped preserve their cognitive functioning. Their responses indicated specific activities and broader forms of engagement. Many participants reported regularly engaging in mentally stimulating activities, such as word games, puzzles, and reading, which they believed helped maintain memory and cognitive sharpness. As one participant shared, “I just think of playing games, word games and certain things like that. I think that helps” (77-year-old female). Another participant shared some specific games: “I try to do Wordle every day, and Connections, Strands, Crossword puzzles, and Shudoku. I’d like to think they are helpful” (65-year-old female). Some mentioned using mobile apps for brain games: “I have several apps on my smart phone, like finding words or stuff like that. I do that every day. That helps with memory” (68-year-old female). Reading was also perceived as beneficial. “I do a lot of reading—fiction and history of art… it keeps my mind busy and interested” (74-year-old male). For some, learning new skills was especially valuable: “I’m studying Morse code. I think studying helps a lot to keep my mind active and improve my memory” (76-year-old male).
Social engagement was also seen as beneficial for cognitive health. Participants believed that staying connected to others and involved in the world supported their overall well-being. As one participant shared, “The engagement with the world in general… that's one of the things that really keeps me alive and kicking.” Reflecting on past and present roles, he added, “Working on something I felt passionate about and helping people was very rewarding and enlivening. Now that I'm not working, it's important for me to stay in contact with my neighbors” (74-year-old male). Participants also described activities that supported emotional well-being and a sense of purpose, which they felt were beneficial overall. For example, one participant said, “I listen to a lot of music, which makes me much happier, and have conversations with people that I like” (81-year-old female), while another emphasized the importance of having small daily goals: “No matter how small it is, accomplish something” (74-year-old male).
Some emphasized the importance of staying active in multiple domains. “I think what can affect my thinking is being more active… I work part-time now, but if I were involved in more things, I think I could retain my memory better” (67-year-old female). Another participant concluded, “It's active—not just socially, but also physically. I think that helps a lot” (76-year-old male). This subtheme demonstrates how participants with SCD perceived mental and social engagement could be beneficial and important to their cognitive well-being.
Discussion
This study sought to enhance understanding of how older adults with SCD perceive and navigate cognitive changes in their daily lives. Through qualitative interviews, participants provided nuanced insights that informed four key themes: (1) daily manifestations of cognitive changes, (2) active use of intentional strategies, (3) appraising the impact of cognitive changes, and (4) perceived risk and protective factors for cognitive function.
Theme 1: Daily manifestations of cognitive changes
Older adults with SCD described declines across multiple domains of cognitive function, as evidenced by the challenges in everyday activities. Changes in memory were commonly reported. These include a decline in prospective memory, such as forgetting appointments, medications, or daily errands, indicating challenges in remembering to carry out intended actions. There might also be a decline in working memory, as participants forgot the purpose of entering a room or temporarily lost track of ongoing tasks might indicate. In addition, participants showed signs of episodic memory decline, particularly in recalling previous conversations or recent events. Participants described reduced attention and concentration, including difficulty focusing on a single task and diminished ability to multitask, which may also point to a decline in executive functioning, especially in planning, organization, and task management. Struggles with language, especially word-finding difficulties and “tip-of-the-tongue” experiences during conversations, were also reported. Participants described slower recall and occasional disorientation, which may suggest subtle changes in processing speed and visuospatial functioning.
These cognitive change symptoms reported by older adults with SCD also occurred in those with MCI, according to previous qualitative studies on MCI, such as forgetting daily events, difficulties in name and word finding, forgetting intentions after entering a room.28,29 This suggests that these cognitive symptoms can happen to both older adults with SCD and MCI. However, qualitative studies comparing cognitively unimpaired older adults with memory complaints and individuals with MCI have noted that the frequency and functional impact of memory problems are greater among those with MCI.19,30 In line with this observation, prior quantitative research suggests it may be the self-perceived consistency and progression of these cognitive changes that indicate elevated risk for further cognitive impairment. For instance, a prior study using the Ecog scale 3 found that older adults who consistently reported worsening on specific items were more likely to develop MCI. Similarly, another study 30 showed that cognitively intact individuals who perceived a progressive decline in memory exhibited greater amyloid-beta burden on positron emission tomography (PET) imaging than those without such concerns.
These subtle cognitive changes that individuals notice in their everyday lives may be hard to detect by neuropsychological cognitive tests. A systematic review of 167 quantitative studies 31 found that most did not detect significant differences between individuals with and without SCD on objective tests of global cognition, memory, attention, or language, although differences in global function and memory were more likely to be observed. Previous studies suggested that attention was fundamental for other cognitive functions, including memory, executive functioning, and language.32,33 Subtle decline in attention may be an early sign of cognitive decline, and individuals with SCD may retain sufficient attention to perform within normal ranges on cognitive tests—making early changes difficult to detect objectively.9,32 However, while prior qualitative research has largely focused on memory-related experiences,19,34,35 few studies have described declines in attention and executive functioning. Our findings provide more detailed insights into how such declines manifest in everyday contexts, contributing to a more comprehensive understanding of the experience of SCD.
Theme 2: Active use of intentional strategies
Consistent with previous qualitative studies on people with memory complaints or with MCI,19,35–37 our findings revealed that older adults with SCD actively employ a variety of compensatory strategies to manage perceived cognitive challenges in daily life. Participants described using internal strategies such as mentally retracing steps, monitoring their speech in social situations, and forming mnemonic associations to enhance recall. External aids—such as calendars, written lists, alarms, and environmental cues—were widely adopted and often embedded into daily routines. Participants utilized social support by requesting reminders from family and friends. These intentional efforts appeared comparable to those reported among individuals with MCI, according to the quotes and narratives in prior qualitative research.19,30
Expanding on previous findings, this study also found that older adults with SCD reported an increase in their reliance on such strategies over time. Participants contrasted their current dependence on reminders and external aids with earlier periods when such tools were unnecessary. Further, despite these intentional efforts, individuals reported challenges in implementing strategies consistently,such as forgetting to look at calendars, misplacing tools, or encountering difficulty with digital technologies. The increasing reliance on these aids and the cognitive lapses despite intentional management, may indicate progression in cognitive changes, which are often not well captured by current SCD measures. Current instruments21,38,39 tend to focus on the presence of cognitive complaints, but rarely assess the effort or burden involved in managing them—potentially overlooking an important dimension of SCD severity.
Importantly, while compensatory strategies can support autonomy and confidence, they may also introduce cognitive strain or emotional frustration, particularly when they fail or become burdensome. These findings suggest a need for supportive interventions that promote effective strategy use, while considering contextual barriers such as digital literacy, competing task demands, and the evolving nature of self-management needs in individuals with SCD. Tailoring these supports may improve quality of life and potentially delay functional decline.
Theme 3: Appraising the impact of cognitive changes
While the study participants reported that their cognitive changes had a low impact on their daily lives, they described experiencing negative emotions such as frustration, embarrassment, and worry, particularly in the moments when lapses occurred. These emotional responses appeared to be situational and transient, rather than persistent. In contrast, prior research has found that individuals with MCI often report more intense and persistent emotional distress, including feelings of depression, helplessness, and anxiety about the future.19,28,37,40 The uncertainty surrounding disease progression may be more pronounced in those with MCI, particularly for those who got a clinical diagnosis. 37 In our study, although participants expressed mild concern or uncertainty, wondering whether their symptoms were “normal,” participants regarded it as a part of normal aging and no need to seek clinical assessments.
Our findings also highlight a variability in how participants appraised the impact of their cognitive changes, which appeared to be influenced by personal and contextual factors. For example, participants normalized their symptoms as they observed similar memory lapses among their peers. Participants experiencing other health challenges or life stressors interpreted cognitive changes as part of a broader decline, which contributed to feelings of inadequacy or loss of identity. Similarly, participants with high personal standards or strong expectations of cognitive competence described heightened vigilance and self-consciousness in social situations. These findings suggest that psychological and social contexts play an important role in shaping how individuals interpret cognitive changes and perceive their significance.
Theme 4: Perceived risk and protective factors for cognitive function
Older adults with SCD perceived a range of factors as influencing their cognitive function. Consistent with prior quantitative research,41-44 they attributed cognitive changes to aging, physical health conditions (e.g., chronic pain), medical treatments (e.g., chemotherapy), and life stressors (e.g., caregiving responsibilities). Participants also described how their cognitive performance was worsened in stressful situations, especially under pressure or while multitasking. Participants also reported the effects of poor sleep and tiredness on cognitive performance, noting sharper thinking and better memory after restorative sleep. These observations align with existing evidence linking health conditions, 41 medical treatments, 42 chronic stress, 43 and sleep disturbances 44 to cognitive decline in older population.
Moreover, participants also identified modifiable factors they believed helped maintain or enhance their cognitive function, including mental stimulation, social engagement, and purposeful daily routines. These insights align with a growing body of research suggesting that cognitively and socially enriching activities may buffer against cognitive decline.45,46 Future research may examine whether addressing these risk and protective factors helps to mitigate SCD and prevent its progression to clinical cognitive impairment.
Strengths and limitations
This study has several strengths. It is among the first qualitative study to explore the daily life experiences of cognitive changes specifically in older adults with SCD. The qualitative approach extends beyond confirming the presence of cognitive complaints to examine how these changes manifest in real-world contexts, how individuals respond to them, and what meaning they assign to these experiences. Participants described variability in cognitive domains affected, the situational nature of lapses, and the subtle ways cognitive changes intersect with daily routines, emotional well-being, and social interactions. These dimensions are not fully captured by structured questionnaires or symptom checklists, which focus primarily on functional difficulty rather than the experiential processes. Also, previous qualitative studies have primarily focused on older adults with memory concerns only,19,35,36 we used the research criteria established by the SCD-I and included individuals who reported perceived decline across various cognitive domains, not limited to memory, to provide a broader view of SCD manifestations. Moreover, this study has identified novel insights such as challenges in compensatory strategy use, perceptions of the need for clinical assessment, and perceived factors on cognitive health.
Several limitations should be considered when interpreting these findings. First, although we used the MoCA to screen for objective cognitive impairment, this tool may not fully exclude MCI. In particular, the T-MoCA has demonstrated an accuracy of 0.72 in identifying MCI, lower than the in-person version. 17 Second, participants were recruited through convenience sampling via a clinical trial, and the sample was predominantly female and older than 65 years, which may limit the generalizability of the findings to males and younger adults with SCD. Third, although participants were encouraged to share openly, the interviews were relatively brief (10–20 min), which may have limited the depth and breadth of the narratives. Also, interviews were conducted using a mixed mode (phone, Zoom, and in-person), which may have affected the consistency of depth or comfort level across the participant responses. Lastly, because questions about cognitive changes were asked following a series of sleep-related questions, participants might have been more likely to consider sleep when answering the question about perceived influence factors of cognitive performance.
Implications for future research
Our qualitative findings underscore the complexity of interpreting SCD within AD research framework. On one hand, our findings support the SCD-I framework 2 that SCD may represent a stage when cognitive changes have begun to emerge, while intentional efforts are actively employed to compensate for the impacts. When considered alongside prior qualitative research,19,30 cognitive changes in SCD appeared to impact less on everyday functioning than those observed in MCI, but with no less compensatory efforts. These compensatory efforts may represent early manifestations of cognitive decline; however, they are challenging to assess and may mask the underlying cognitive impairment. Future qualitative research may directly compare the daily cognitive experiences of cognitively unimpaired older adults without SCD, those with SCD, and those with MCI, to better clarify similarities and differences in symptom patterns, compensatory processes, and functional impacts across the cognitive statuses. This may help refine the conceptual boundaries of SCD.
Meanwhile, our findings reinforce that SCD is a broad and heterogeneous construct shaped by diverse contextual factors. Participants described that physical and mental statuses, pain, substance use, and normative aging processes could influence their cognitive performance and potentially contribute to perceived cognitive changes. In many cases, SCD may arise from non-neurodegenerative sources and may not directly reflect AD pathology. 2 However, these factors may also co-occur with or contribute to underlying AD pathology. 9 For example, depression is a condition commonly co-occurs with SCD, which was also reported by half of our sample. A prior study 47 indicated that individuals with co-occurring SCD and depression had the highest risk of progressing to MCI or dementia compared with those with neither condition. From this perspective, SCD can still function as an indicator of increased vulnerability to cognitive impairment and warrant attention.
Our findings also indicate a role of personal and social contexts in shaping individuals’ awareness and appraisal of cognitive changes. A prior cross-sectional diagnostic study 48 suggested that a self-reported Ecog-12 score ≥ 1.36 may help distinguish cognitively unimpaired and cognitive impairment among general older adult populations. Our SCD sample had no evidence of objective cognitive impairment but reported a higher average Ecog-12 score (mean = 1.68). Although this observation requires confirmation in larger quantitative studies, it suggests mixed possibilities: individuals with SCD may experience subtle cognitive changes not detected by standard testing, and/or they may exhibit heightened awareness and monitoring of everyday cognitive functioning that may not necessarily reflect greater objective cognitive decline. While this study focused on participants’ subjective experiences of cognitive changes, future research may examine the discrepancies between self-reported cognitive concerns and study partner reports or objective behavioral observations to provide a more comprehensive understanding of how these concerns impact older adults’ daily lives.
Overall, research on SCD is still at a relatively early stage. There remains a critical need for continued research to understand the causes and mechanisms underlying SCD, to disentangle pathological and nonpathological pathways, and to examine protective and risk factors that influence the progression to objective cognitive impairment or dementia.
Implications for clinical practice
Individuals with SCD may seek medical advice because of concerns about changes in their cognitive functioning. Given the heterogeneity of SCD experiences, clinical evaluation may benefit from a person-centered approach that extends beyond standard neuropsychological testing. 9 Clinicians may pay attention to compensatory strategies, increased effort, and self-monitoring behaviors, which may provide important insights into early cognitive changes that are not captured by standardized tests. Evaluating the contextual factors (e.g., physical and mental well-being, social contexts) may be helpful to understand the potential contributors to the SCD and distinguish between situational influences and changes that warrant closer monitoring. Additionally, regular follow-up assessments may be particularly important to determine whether SCD resolves over time or shows signs of progression.
It is also important to evaluate how perceived cognitive changes impact individual's daily functioning and emotional well-being. Despite the absence of objective cognitive impairment, participants in this study described self-perceived cognitive changes that disrupted daily routines, reduced efficiency in completing tasks, and hindered communication and social interactions. Their emotional well-being, self-image, and social engagement seemed to be impacted. Negative emotional responses and unpleasant social encounters may, in turn, reduce confidence and impair daily functioning, 49 potentially creating a reinforcing feedback loop. These highlight the need for healthcare providers to offer supportive care for older adults with SCD, even when clinical assessments do not detect objective cognitive impairment. Rather than sending them home without guidance, providers may consider offering individualized guidance such as health education on mnemonic strategies, use of memory aids, and lifestyle modifications. Prior research50–52 has shown that such educational programs can significantly improve memory performance among individuals with SCD. Emotional regulation and cognitive coping strategies should also be incorporated, which may enhance psychological well-being, improve confidence, and ultimately support everyday functioning.
Conclusion
This study provides a nuanced understanding of the lived experiences of community-dwelling older adults with SCD. Participants described noticeable changes in multiple cognitive domains (e.g., attention, memory, language, and executive functioning), which were reflected in challenges with daily tasks and an increased reliance on intentional strategies. These experiences influenced their daily routines, emotional well-being, and social interactions. The findings also suggest SCD is a heterogeneous and contextually embedded phenomenon. There is a need for person-centered clinical evaluations that move beyond objective cognitive testing to incorporate contextual, emotional, and functional considerations. Future research should further elucidate the role of SCD in relation to underlying pathology and develop tailored support strategies that address the specific needs of older adults with SCD and promote their overall well-being.
Footnotes
Acknowledgements
JH was supported by the National Institute on Aging through fellowship F99AG088437.
Ethical considerations
This study was approved by the Ethics Committee of Johns Hopkins School of Medicine (IRB00440771 and IRB00396390). This research was conducted ethically in accordance with the World Medical Association Declaration of Helsinki.
Consent to participate
Informed consent was obtained from all participants before their participation.
Consent for publication
Not applicable.
Author contribution(s)
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute on Aging (R01AG080613), the Johns Hopkins School of Nursing 2023 Discovery and Innovation Fund, and the Johns Hopkins University Center for Equity in Aging 2023 Pilot Award.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
