Abstract
Dementia-related cognitive decline and ageing-related challenges impact social participation and relationships. Limited knowledge of dementia among family, friends and the public hinder support for interactions with those affected. Unmet social needs in community-living older adults with dementia remain underrecognized, despite their importance in healthy ageing and quality of life. This scoping review mapped existing evidence on unmet social needs of community-living older adults with dementia, including how these needs vary across dementia stages. We conducted a scoping review following Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) and Joanna Briggs Institute (JBI) guidelines. Four databases were searched (2000 –April 2025) in English, Portuguese and Mandarin, yielding 24 included articles. Seven themes of unmet social needs were identified: (i) participation in out-of-home activities, (ii) support for maintaining independence in daily life (iii) companionship, (iv) meaningful relationships, (v) respectful and dignified social interactions, (vi) emotional support, and (vii) social needs during the pandemic. Unmet social needs differed by dementia stage: in mild dementia, unmet social needs mostly relate to out-of-home activities, while in moderate and severe stages unmet social needs shifted towards daily activities, companionship and emotional support. Stigma emerged as a transversal influence shaping experiences of unmet social need across stages and contexts. Unmet social needs evolve across dementia stages and are influenced by relational, socio-cultural and structural factors. Future research should include more advanced stages, diverse populations, and strategies for addressing social needs from their own perspectives.
Keywords
Introduction
The World Health Organization's (WHO) Decade of Healthy Ageing defines “healthy aging” as “the process of developing and maintaining the functional ability that enables well-being in older age.” 1 Functional abilities encompass the capacity to meet one's basic needs; learn, grow, and make decisions; maintain mobility; contribute to society; and build and maintain relationships. The ability to engage in social activities and maintain interpersonal connections is therefore a fundamental component of healthy aging.
Drawing on the WHO decade of Healthy Ageing framework, 1 we conceptualize social needs as opportunities for social participation and engagement, including the ability to maintain meaningful interpersonal relationships and social activities. In addition, the Social Production Functions theory recognizes three core social needs2,3: affection, behavioral confirmation and status. Affection is defined as the need to give and receive love independent of personal abilities or resources. Behavioral confirmation refers to the need to feel that one's actions are ‘‘right’’ by oneself and others, and to have a sense of belonging with groups with shared values. Status relates to the need to distinguish oneself from others based on individual abilities, roles or resources. 2
Based on these frameworks, unmet social needs are operationalized as: i) constraints that limit engagement in social activities; ii) hinderances to the maintenance of interpersonal relationships; and/or iii) barriers to the fulfilment of the core social needs.
Dementia, a neurocognitive disorder affecting more than 55 million people worldwide, poses several challenges to social interaction and activities participation not only for people with dementia and their caregivers, but also for friends, wider social networks, and others within the care constellation.4,5 Dementia is characterized by a decline in cognitive functioning, with impairments in areas such as memory, language, and social cognition. 6 Behavioral and psychological symptoms of dementia (BPSD) like apathy, agitation and anxiety can further hinder social engagement.7,8 Literature suggests that older adults with dementia tend to report more unmet social needs than those without cognitive impairment. 9 During the mild stages of dementia, individuals can take part in community or social activities without help and may appear unimpaired to those who do not know them well. 10 In the moderate stage, signs and symptoms progress and become increasingly restricting. 10 In the severe stage, affected individuals may have complete dependence, inactivity, serious memory disturbances and physical signs. Consequently, maintaining social connections becomes increasingly difficult throughout the disease trajectory. In addition to cognitive decline, other aging-related factors further reduce social interaction. Retirement often leads to decreased daily contact with colleagues, while physical frailty and age-related health issues contribute to reduced mobility. 11 The loss of relatives, spouses, and close friends can further exacerbate social isolation, limiting opportunities to build new relationships.11,12
Studies focusing on community-living older adults with dementia highlight numerous unmet intrapersonal and interpersonal social needs, particularly related to daytime activities (e.g., social, work, leisure, learning activities), receiving company (e.g., social contact, contact with friends), and receiving help with psychological distress (e.g., agitation, needs for sympathy and support).13–16 Recognizing and addressing the unmet social needs of community-living older adults with dementia is crucial, as they are associated with a lower health-related quality of life and more symptoms of depression.13,14,17
Two main measures have been used to assess unmet needs among older adults with dementia. The Camberwell Assessment of Needs for the Elderly (CANE) is one of the most commonly used tools for identifying met and unmet needs among older adults. It comprises 24 areas related to the care recipient and two areas focused on the caregiver,16,18 covering areas such as social contact, accommodation, physical health, and access to information about their health condition. The CANE is typically administered by healthcare professionals and may not fully capture the subjective experiences of those living with dementia. Another widely used tool is the John Hopkins Dementia Care Needs Assessment (JHDCNA), which comprises seven areas related to the care recipient and six areas focused on the caregiver. The JHDCNA captures unmet social needs such as social engagement and interpersonal relationships within the Daily Activities domain, and it also addresses other areas including health care financing and general health care needs. Developed by clinical dementia care experts, the JHDCNA is clinician-administered, which may also limit the subjective inputs of those living with dementia. 14 Although qualitative methods such as interviews are also used to explore unmet needs among older adults with dementia, the majority of research in this area remains quantitative. 12
Previous reviews have mapped the evidence on the broader spectrum of unmet needs among older adults with dementia. A scoping review by Morrisby et al. 19 and a meta-analysis by Curnow et al., 20 identified needs in areas such as information, self-care, and peer support. However, none of the reviews19,20 focused specifically on unmet social needs. Furthermore, a large part of the existing literature is based on the perspectives of caregivers or healthcare professionals, rather than on older adults with dementia themselves.9,20–22 Although proxy reporting may be required in later stages of dementia due to reduced insight or capacity to complete questionnaires, dependence on proxy reports alone may fail to capture subjective social needs that are best understood from the perspective of older adults living with dementia. 21 Additionally, the current literature also does not provide clear insights on whether variations exist in unmet social needs across the stages of dementia.
To address these gaps, we conducted a scoping review to map the existing evidence and identify gaps in the literature about the unmet social needs of community-living older adults with dementia, considering their own perspectives. Our primary research question was: (1) “What are the unmet social needs of community-living older adults with dementia considering their perspective?”. The secondary research question was: (2) “How those unmet needs evolve along the stages of dementia?”
Methods
This review was conducted following the Joanna Briggs Institute (JBI) guidance for scoping reviews 23 and is reported by the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR). 24 Scoping reviews are a well-established method to identify key characteristics or factors of a given concept and research gaps.25,26 The protocol of this review was registered in the International Platform of Registered Systematic Review and Meta-analysis Protocols (https://inplasy.com/inplasy-2023-12-0082/).
The Population, Concept, Context (PCC) approach was used to outline inclusion and exclusion criteria (Table 1). Inclusion criteria consisted of primary peer-reviewed articles written in English, Portuguese or Chinese published from year 2000 onwards. The decision to focus on literature published in the past 25 years was to ensure relevance to today's context of care practices, social structures and cultural understandings of dementia, and align with the WHO's (2020) paradigm of healthy aging. 1 It is acknowledged that some unmet social needs identified in studies conducted during this period may reflect changes in social interactions, expectations, and care arrangements, which differed significantly before, during and after the COVID 19 pandemic. A prior literature review on the subjective needs of people with dementia 27 confirmed that most studies in which people with dementia were interviewed were conducted from year 2000 or later. All types of research approaches were considered. Unpublished studies and grey literature (e.g., reports and conference abstracts, books, documents) as well as systematic reviews or meta-analyses were excluded to ensure the scoping review provides an overview of available evidence based on peer-reviewed research. 26
Eligibility criteria according to the PCC approach.

Search strategy
A search strategy was devised with the assistance of an academic librarian. An initial search on PubMed was conducted to explore and identify relevant English-language search terms aligned with the research questions for use in the search strategy. The same derived search terms were applied in all database searches, using the same filters and date ranges. Search terms included “older people” OR elderly OR “old person” OR “older adults”, dementia OR Alzheimer OR “Neurocognitive disorder”, “social needs” OR leisure OR occupation OR interact* OR activit*, home OR community OR “community-living”. Four online databases (PubMed, Scopus, Web of Science, and Academic Search Complete) were initially searched on 11 December 2023. The scoping review was updated with a final search conducted on 22 April 2025, across all previously used databases, with the exception of Academic Search Complete, which was no longer accessible through the institutional database subscriptions at the time of the search. Hand-search of key authors and citations of included studies was conducted to ensure all relevant studies were included. The search was supplemented by conducting manual citation searching of relevant papers, which resulted in 1 paper 16 being added to the included studies. The full search strategy is provided in Supplemental Table 1.
Screening procedure
Following the JBI recommendations, the screening was performed in sequential steps. The proportion of screening conducted by each reviewer was further informed by the ‘Steps for Conducting a Scoping Review’. 28 Firstly, all search results were imported to Zotero, where the duplicate records were removed. Secondly, the first author (ST) conducted screening on all articles while the second author (MM) screened 20% of the articles. Where an abstract was unclear or its relevance was uncertain, it was added for full-text screening. Thirdly, full text was screened; the first author (ST) screened all articles while the second author (MM) independently screened 50% of the articles. For all three stages (title, abstract, and full text screening), both authors (ST and MM) discussed any disagreements to reach a consensus. Prior to the first stage, the first and second authors (ST and MM) performed a calibration exercise to ensure consistent application of the eligibility criteria. A random sample of 10% of titles and abstracts was independently screened by each reviewer. A high level of agreement (94.4%) above the recommended target of 90% was achieved between the two authors (ST and MM). All disagreements were solved through discussion between the first and second authors (ST and MM). Lastly, the reference list of all included articles was checked for additional relevant citations. If the full-text version of an article was inaccessible, the original authors were contacted. An additional screening of the reference list of a recent scoping review on ‘unmet care needs of older people’ 29 identified five papers that were added to the list of full texts screened.15,16,30–32 The inclusion and exclusion criteria applied during the three stages (title, abstract, and full text) were defined following JBI's recommendations for scoping reviews (Table 2). 23 All members of the review team are fluent in English. Additionally, the first author is also fluent in Mandarin, while the third, fourth and last authors are native Portuguese speakers.
Data extraction guidance sheet.
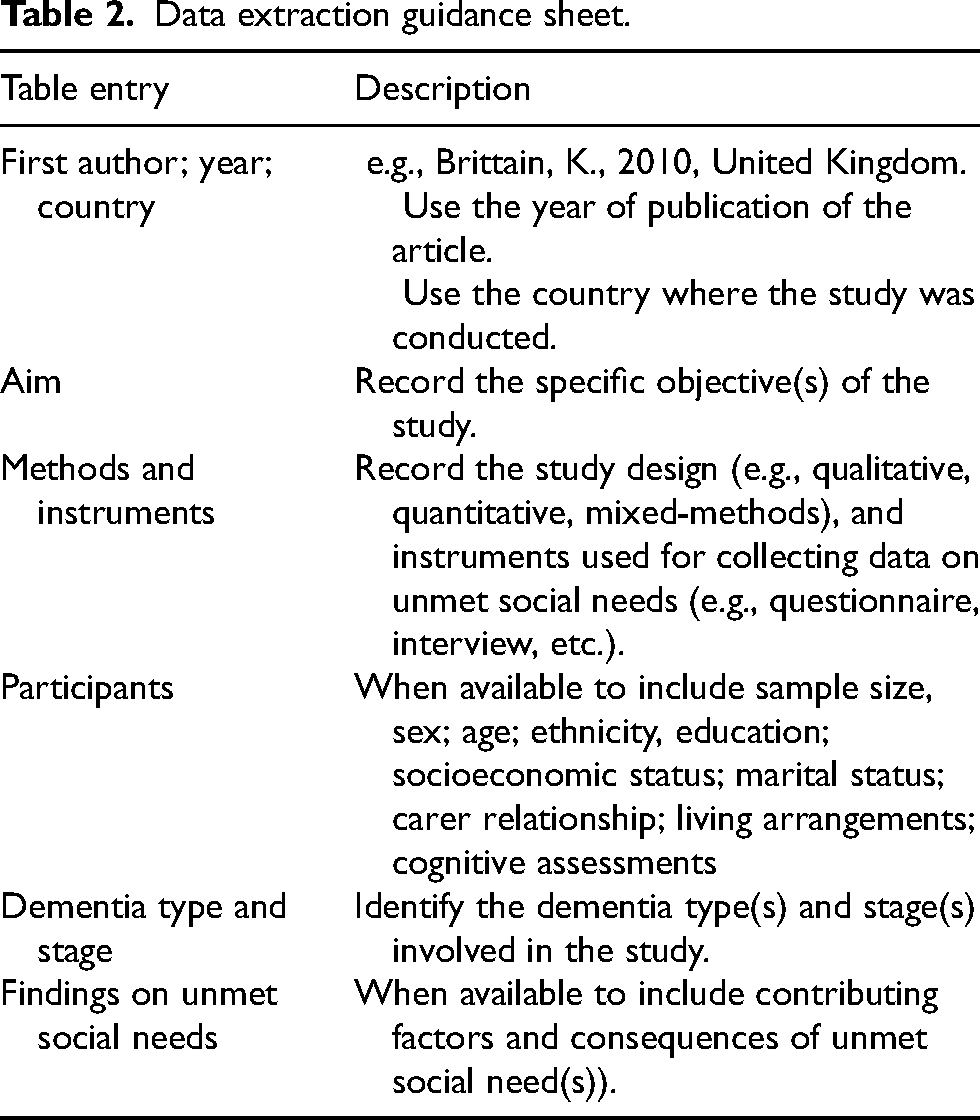

Data extraction
A spreadsheet for extraction was created using Microsoft Excel to retrieve data from the included studies. The first and second reviewers (ST and MM) each extracted data from 50% of the studies and cross-verified the data to ensure completeness and accuracy. Extracted data (where available) included: authors, year of publication and country; study aim(s), methods and instruments (study design, instruments used for collecting data on unmet social needs); participants (sample size, sex; age; ethnicity, education; socioeconomic status; marital status; carer relationship; living arrangements; cognitive assessments; dementia diagnosis method, type and stage); unmet social needs. The data extraction guidance sheet is provided in Table 2.
Data analysis
Data were analysed using descriptive statistics for study characteristics and thematic analysis was conducted on qualitative results following the six-stage approach recommended by Braun and Clarke. 33 Codes were developed inductively from the data, with themes generated from the reported experiences within the included studies through an iterative analytic process. The unit of analysis was the extracted qualitative data, which were coded sentence by sentence. The first reviewer (ST) familiarized with the data through repeated reading of the papers to gain a deep understanding of the content; systematically coded all relevant data in the papers; grouped related codes into potential themes; reviewed the themes against the entire coded data set; ensured themes were well-defined and finalized the themes; and presented the findings and themes according to the research questions. Throughout the process of thematic analysis, the first reviewer (ST) regularly shared and discussed the findings with the co-reviewers (LS, OR, and RMB). The final themes developed were discussed with the reviewers (LS, OR, and RMB) until a consensus was reached. A summary of the synthesized findings in a narrative form was provided. In line with the established guidelines,23,24 a quality rating of the studies and an assessment of the risk of bias were not conducted.
Results
The search yielded 5071 records as potential articles for inclusion. After removing duplicates, 3190 articles were screened based on their titles and abstracts. One article 16 was manually added through citation searching. After excluding irrelevant articles, 96 publications were retrieved for full-text assessment of eligibility. In total, 24 articles met the eligibility criteria and were included. The PRISMA-ScR flowchart detailing this process is presented in Figure 1. Detailed evidence regarding the included studies is presented in Table 3.
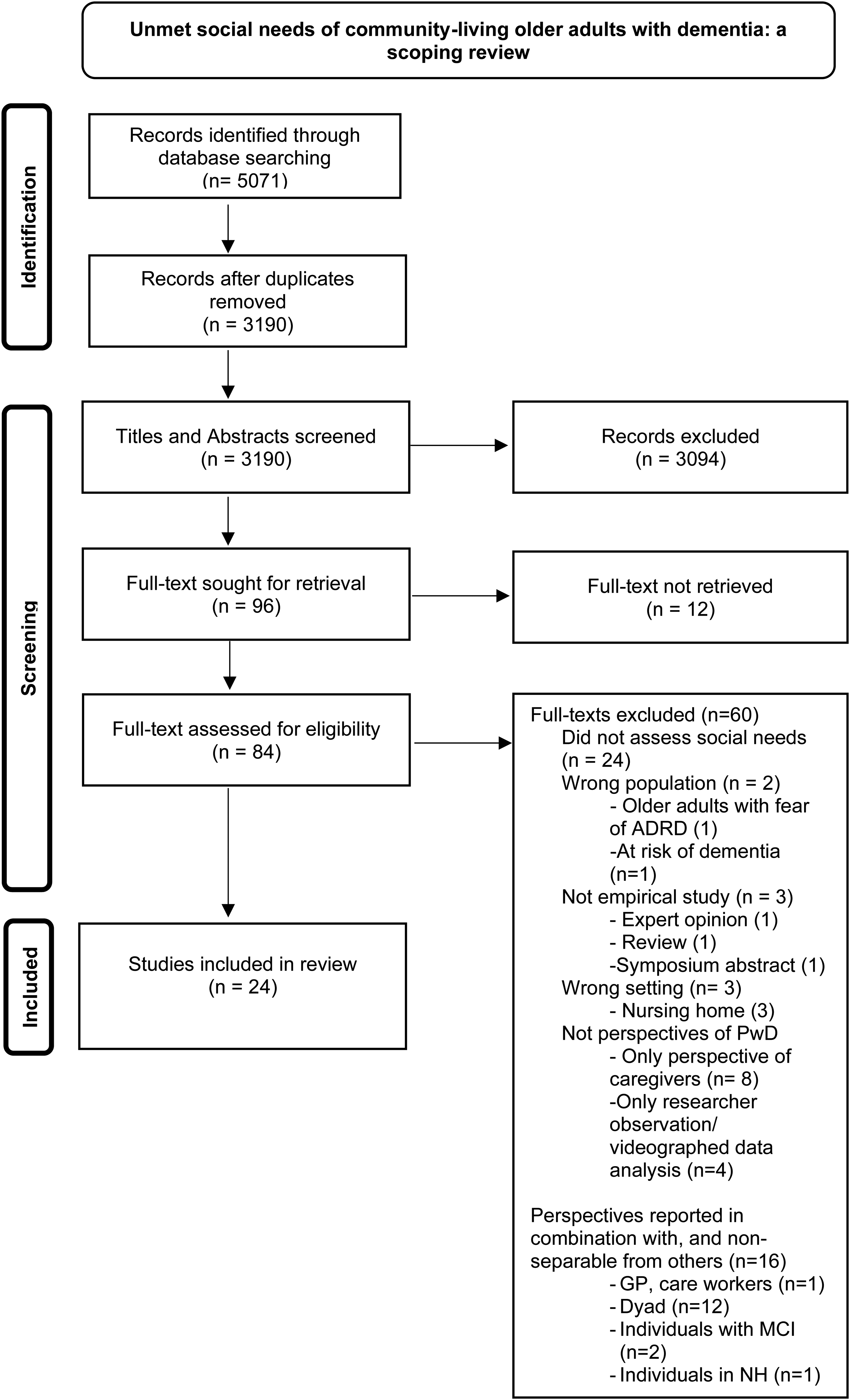
PRISMA 2020 flow diagram.
Summary of the included studies.
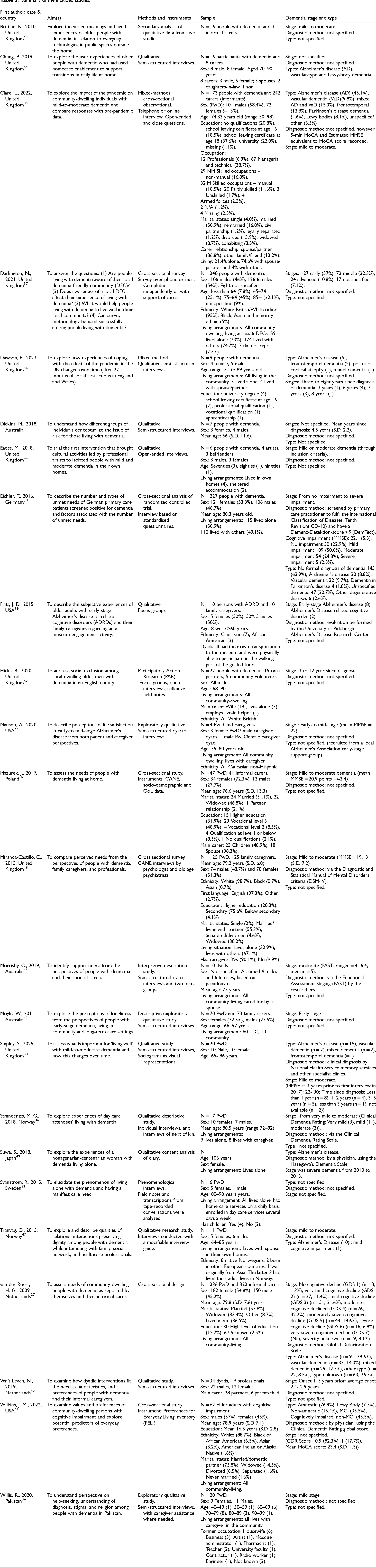
Overview of the included studies
The included studies were published between 2009 to 2025, of which 19 (79%) were published since 2015. Nine studies were conducted in the United Kingdom (37%), three in the United States of America (12.5%), three in Australia (12.5%), two in the Netherlands (8.3%), two in Norway (8.3%), and a study each (4.1%) in Sweden, Germany, Poland, Pakistan and Japan. Nineteen studies (75%) used qualitative methods and five used quantitative methods (25%).
The included studies reported information on 1382 older adults with dementia. Twenty studies (83%) recruited participants aged ≥ 65 years, except for four studies which included participants of an age range of 40–99 34 ; 50–98 35 ; 51–89 36 ; and younger than 64 years. 37 56% of participants were female. Three studies were part of the British IDEAL cohort study.35,36,38
The participants were in distinct dementia stages. Most studies involved participants who were in the earlier stages, with four specifically including participants in the mild stage34,39–41; ten studies included participants who were in mild to moderate stages.16,18,35,38,42–47 Two studies involved participants with moderate stage dementia,36,48 and one study included participants with severe-stage dementia. 49 Five studies spanned multiple stages from mild to severe-stage dementia.27,37,50–52 Two studies did not specify the dementia stage.53,54
In terms of diagnosis, 12 studies provided specific information, reporting on a range of dementia types, including Alzheimer's disease, vascular dementia, mixed Alzheimer's disease, dementia with Lewy bodies, Parkinson's disease dementia, and frontotemporal dementia. The remaining 12 studies did not specify the type of dementia.
Unmet social needs
Seven categories of unmet social needs were identified (Table 4), addressing the first research question. Each unmet social need is described in detail, based on the reported experiences from the included studies. The second research question aims to describe how unmet social needs vary across the dementia stages. Many studies did not include participants from a single stage of dementia, which limited our ability to draw stage-related trends. Variations across the stages of dementia are described based only on studies involving single stage participants (Table 4). In addition to stage-related patterns, the analysis also identified several cross-cutting influences that shaped how unmet social needs emerged and were experienced. Among these, stigma appears consistently as an embedded and transversal factor influencing social participation, help-seeking, and interpersonal relationships.
Main findings from included studies.
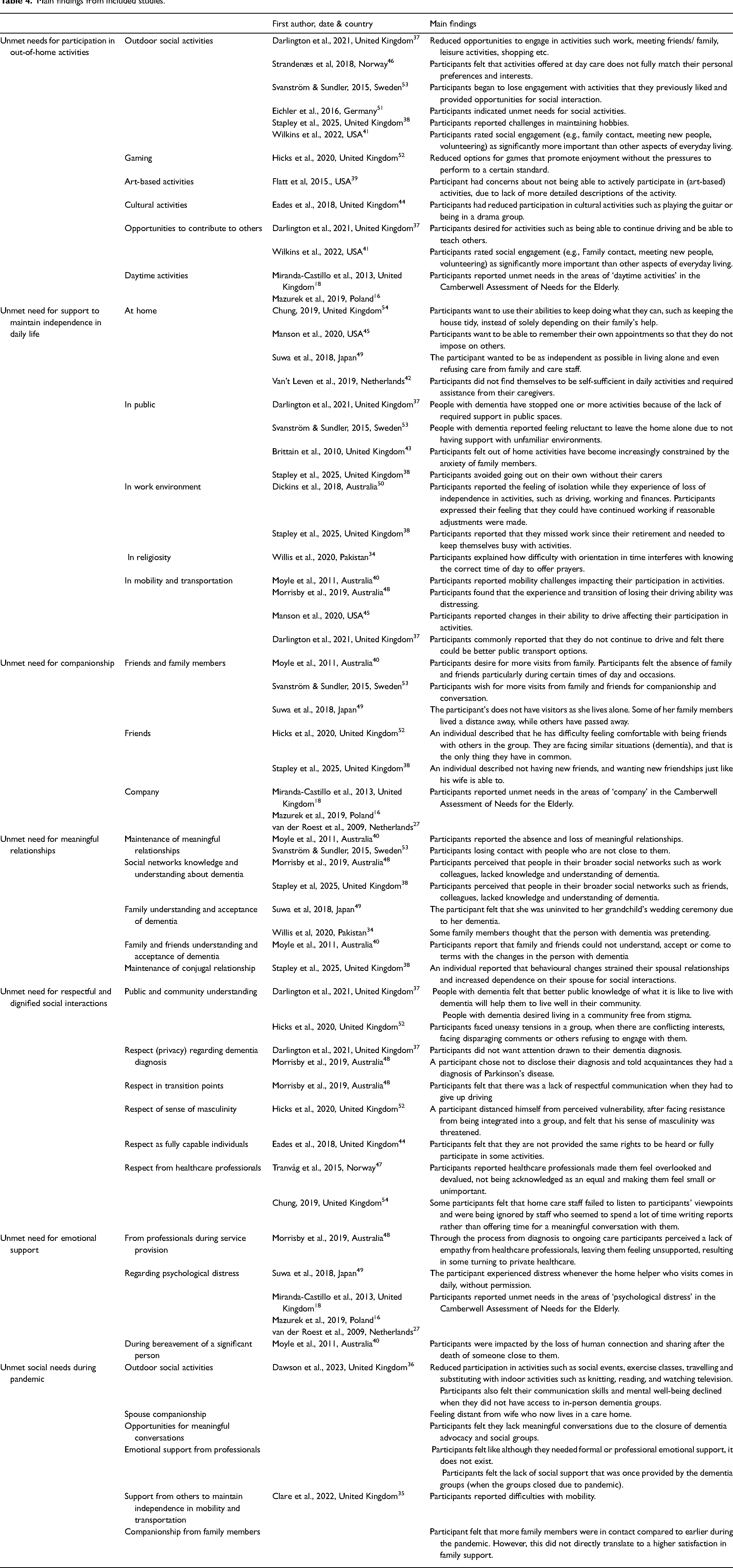
Unmet need for participation in out-of-home activities
The unmet need for participation in out-of-home activities was reported in eleven studies.16,18,37–39,41,44,46,51–53 It encompasses social, cultural, recreational, and outdoor activities such as meeting friends or family, attending events, or engaging in hobbies. These activities provide enjoyment, social connection, and a sense of purpose. This theme was described for the mild stage of dementia.39,41 Older adults with dementia desired art-based engagement; however, a lack of clear information about activities like museum visits was highlighted as a barrier to participation. 39 Using the Preferences for Everyday Living Inventory (PELI), Wilkins et al. 41 found that social engagement, including maintaining regular contact and volunteering, was highly valued yet often unfulfilled. This study's findings further revealed that social engagement was rated significantly more important than other everyday life domains, such as autonomous choice, personal growth, and maintaining a routine.
Studies which involved participants of mixed stages of dementia reported their desire to participate in out-of-home activities, yet barriers such as financial constraints and cognitive decline limit their involvement.37,46,51 Some participants reminisced about past cultural engagements or hobbies, which became challenging to maintain after dementia onset, a challenge further exacerbated by service and support closures during the COVID-19 pandemic.36,38,44 Among some older adults with dementia, activities that were once important, such as hobbies, engagement in clubs, and travelling, were described as becoming less meaningful and or enjoyable over time. 53 Performance pressures during gaming activities was found to discourage participation among individuals with dementia. 52 In two studies using the CANE instrument, ‘daytime activities’ was a significant unmet need - identified as the second most common unmet need in Miranda-Castillo et al. 18 (14.5%) and the third most common in Mazurek et al. 16 (25.5%).
Unmet need for support to maintain independence in daily life
Twelve studies reported on the unmet need for support to maintain independence in daily living.34,37,38,40,42,43,45,48–50,53,54 This theme was described for the mild34,40 moderate 48 and severe 49 stages of dementia. In the mild stage, Moyle et al. 40 reported that mobility challenges such as needing walkers or wheelchairs restricted their social participation. Willis et al. 34 found that participants placed importance on maintaining independence in cultural routines such as religious practices. In the moderate stage, Morrisby et al. 48 described how participants increasingly required support in daily activities due to reduced mobility and loss of driving privileges. Losing driving privileges was particularly distressing, especially when the decision was communicated by authorities or professionals in ways perceived as lacking sensitivity or respect. 48 In the severe stage, a case study by Suwa et al. 49 highlighted a participant's strong desire to live independently while living alone. Among studies which involved participants with mixed stages of dementia, needs for maintaining independence in daily life were identified across four areas: (i) their own homes, (ii) public spaces; (iii) workplaces, and (iv) mobility and transport. In their own homes, rather than solely relying on family support, many older adults with dementia wanted to continue engaging in household tasks to preserve their sense of self and purpose. Some resisted help when it was perceived as undermining their abilities, even if their families or carers felt it was necessary. 54 Others acknowledged the need for assistance with specific activities, such as using household devices or managing routines, which reflected a need for balance between autonomy and support.42,45 In public spaces, a lack of support in public environments led some older adults to stop going out entirely, or avoid being on their own in unfamiliar settings.37,38,53 Additionally, family members’ concerns about safety often resulted in restrictions on independent mobility, contributing to reduced social participation and feelings of isolation. 43 In workplaces, loss of employment was associated with a loss of identity and purpose.38,50 Some older adults with dementia felt they could have continued working if reasonable accommodations had been made, but instead faced abrupt restrictions following their diagnosis. 50 In mobility and transport, some individuals limit themselves to familiar routes when leaving their homes. 37
Unmet need for companionship
Eight studies reported the unmet need for companionship.16,18,27,38,40,49,52,53 This includes regular contact with family, friends, or social groups, even if the interactions were casual or not deeply personal. Individuals expressed a desire for more visits from family and friends, frequent conversations, and opportunities to engage socially to avoid feeling isolated. This theme was described for the mild stage 40 and severe 49 stage of dementia. In the mild stage, Moyle et al. 40 found that participants often felt the absence of regular interaction, especially during times such as holidays or nighttime. One participant described loneliness being most pronounced at night when not accompanied by his spouse. 40 In the severe stage, Suwa et al. 49 presented a case who described the emotional impact of living alone and having children who rarely visited. 49 Among studies which included individuals with mixed stages of dementia, the need for companionship was not limited to family members, and the presence of any visitor regardless of their relationship provided a sense of meaning and connection. 53 Some older adults with dementia felt isolated despite being part of dementia groups, suggesting that shared experiences of dementia did not necessarily lead to quality interactions. 52 An individual reported that he would like to make new friends, and compared himself to his wife who could. 38 In studies using the Camberwell Assessment of Need for the Elderly (CANE), the need for company was ranked the second 16 and third18,27 most commonly reported unmet need cited by 29.8%, 12.8% and 5.4% of participants respectively.
Unmet need for meaningful relationships
Six studies reported the unmet need for meaningful relationship.34,38,40,48,49,53 These studies highlighted the need for quality relationships that are emotionally fulfilling, which includes maintaining trusting and reciprocal relationships with close family, friends, and caregivers who are able to help the person living with dementia to feel understood, accepted and valued. This theme was described for the mild,34,40 moderate 48 and severe 49 stages of dementia. In the mild stage, Moyle et al. 40 reported that family members did not understand the cognitive changes associated with dementia, sometimes perceiving memory lapses as intentional, leading to feelings of guilt and frustration. Similarly, Willis et al. 34 found that family members were reported to suspect the older adult with dementia was “pretending” to forget, which strained family relations. In the moderate stage, participants felt that people in their broader social networks, such as colleagues, lacked an understanding of dementia, which contributed to feelings of being stigmatized. 48 In the severe stage, an individual expressed sadness at not being invited to a grandchild's wedding, interpreting that she was left out due to her condition. 49 Among studies involving participants with mixed stages of dementia, the perceived lack of empathy and understanding within families and friends often led to feelings of shame or being dismissed. 38 One individual reported behavioural changes having a negative effect on their spousal relationship, and being more dependent on their spouse for social interactions. 38 Others reported the lack of meaningful relationship due to the deterioration and challenges of maintaining close connections over time. 53
Unmet need for respectful and dignified social interaction
Six studies reported on the unmet need for respectful and dignified treatment.37,44,47,48,52,54 This includes unmet needs related to public knowledge and attitudes towards dementia, and the need to be treated with respect and dignity. The groups of people identified were families, friends, and broader social networks such as members of dementia support groups. Experiences reported include stigma, lack of understanding and acceptance, privacy of their diagnosis and difficulties in receiving the support they need. It includes situations where the person's voices and opinions were disregarded, leading to frustration and feeling undervalued. This theme was described for the moderate stage of dementia by one study, 48 which highlighted a lack of respectful communication during transitions, such as during the process of losing the driver's licence; participants also felt that there is still a stigma associated with dementia that led some to choose not to disclose their diagnosis. Among studies involving individuals with mixed stages of dementia, community dwelling individuals perceived that the public needs a better understanding of what is it like to live with dementia. 37 To avoid unwanted attention drawn to their diagnosis, some individuals choose to keep their diagnosis private. 37 In a group of men who attended a game-based social support program, one individual faced disparaging comments and social exclusion. 52 This lack of respect from the group made him feel that his sense of masculinity was under threat. 52 Another topic within this theme regards the perception that the right to be heard and capacity to participate fully in activities were not respected. 44 In their interactions with healthcare professionals, some participants felt that they were not acknowledged as an equal, resulting to them feeling overlooked and ignored.47,54
Unmet need for emotional support
Six studies reported on the unmet need for emotional support.16,18,27,40,48,49 This theme focuses on needs related to the emotional and psychological well-being of older adults with dementia. Individuals reported needs for emotional and psychological support to engage in social situations, and cope with psychological distress or bereavement. This includes formal sources of emotional support from professionals. This theme was described for the mild, 40 moderate 48 and severe 49 stages of dementia. In the mild stage, one participant described the loneliness experienced when reminiscing about shared experiences with a late loved one. 40 In the moderate stage, Morrisby et al. 48 reported a need for better emotional support during diagnosis and ongoing care. Some individuals perceived a lack of empathy from healthcare professionals, leaving them feeling dismissed or uncared for. One participant shared his disappointment with the memory clinic he attended, stating that some staff members “don't care”. 48 In the severe stage, a participant experienced emotional distress when caregiving routines were perceived as intrusive, particularly when an assigned home helper entered the home without permission. 49 In the studies involving individuals with mixed stages of dementia, psychological distress consistently emerged as the leading16,18 and third 27 unmet need assessed with the CANE, indicating the prevalence of emotional support as an unmet social need.
Unmet social needs during pandemic
Two studies reported unmet social needs that were related to the COVID-19 pandemic.35,36 Public health restrictions on social gatherings and the closure of community services led to increased social disconnection and isolation of older adults with dementia. Many individuals reported fewer opportunities for social interaction and meaningful conversation, contributing to feelings of isolation and decrease in emotional/psychological well-being. This theme was described for the mild stage of dementia by one study. 36 The participants described the closure of dementia advocacy and social groups as particularly impactful. These groups had previously offered companionship, shared experience and advisors. The loss of such social connections due to the closure of groups left many feeling increasingly isolated. An additional factor contributing to social isolation reported in Dawson's et al. 36 was the restriction of social gatherings beyond official guidelines, avoiding public places and events out of fear of harm to themselves or others. In place of group activities, some participants relied on solitary activities within the home such as knitting, reading, and watching television to remain occupied, although these did not fully replace the value of in-person connection. Over time, sustained isolation and lack of opportunities for social interactions led to marked declines in communication skills and mental well-being. As opportunities for social integration returned, several participants felt discomfort and frustrations when easing back into these social environments. Clare et al. 35 involved individuals in mixed stages of dementia. While some participants observed an increase in family contact during the pandemic, this did not translate into stronger sense of emotional support or connection. 35 In the same study, 39.3% reported difficulties in daily activities and 44.5% reported difficulties with mobility, both of which may limit their social participation.
Variation in unmet social needs across dementia stages
Most studies included participant across multiple stages of dementia without distinguishing the specific unmet social needs in each stage. Therefore, stage-specific observations could only be drawn from a small number of studies (Table 5).
Variation by stages.
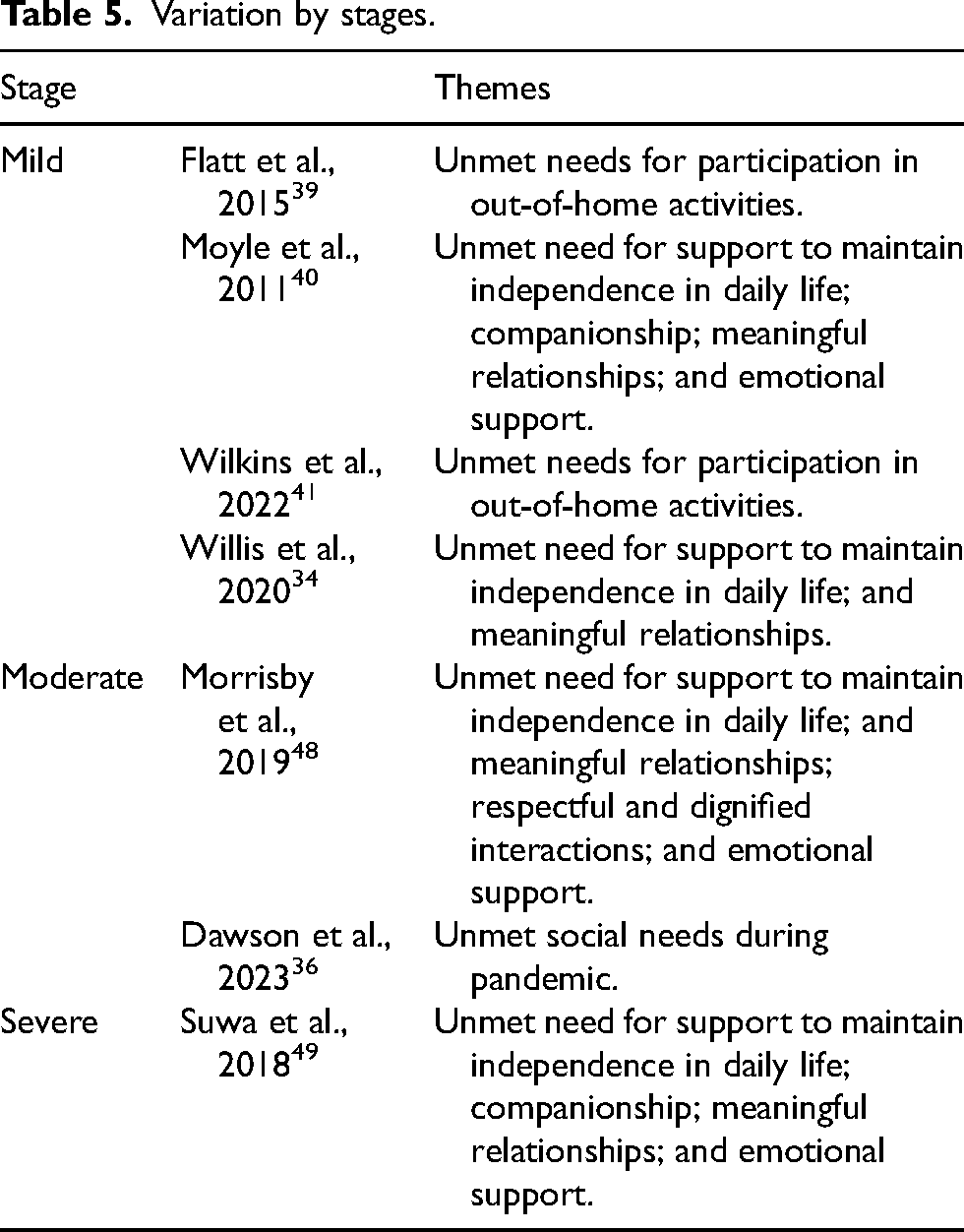
Results suggest that in the mild stage, unmet social needs tend to focus on maintaining activities and roles that reinforce personal identity, such as volunteering or community participation.39,41 Other unmet social needs observed include support for independence in daily life, companionship, meaningful relationships and emotional support.34,40 As dementia progresses into the moderate stage, unmet social needs shift towards navigating increasing dependence and dealing with role changes.36,48 Challenges related to acceptance from social networks emerge, along with more reliance on settings such as day centres, support groups, or home care services for social interactions.36,48 Emotional support remains essential in this stage. 48 In the severe stage, changes in communication ability and reduced confidence in social settings further contributed to unmet needs for companionship, meaningful relationships and emotional support. 49 These findings highlight a shift from actively seeking social engagement and autonomy in mild stages to requiring more supportive social interactions in the moderate and severe stages.
Beyond the life course trajectory of the older adult living with dementia, the family system's adaptation across the dementia stages also shapes unmet social needs. In the mild stages some families faced difficulties coming to terms with the condition, and even suspected the older adults to be “pretending” to forget.34,40 In the severe stages, role strains manifested in different ways ranging from overprotecting them and inevitably restrict their autonomy, to exclude them from family events. 49 Families also experience their own unmet social needs, such as emotional support, respite and guidance from both informal networks and formal services.
Stigma as a transversal influence on unmet social needs
Stigma was identified as an embedded factor shaping how unmet social needs emerged and were experienced across dementia stages, diverse cultural and national contexts. Older adults living with dementia reported feeling stigmatized, misunderstood or excluded37,40,48,49; as well as: ‘ignored by (healthcare) staff’, 54 ‘wanting their right to be heard’, 44 ‘negativity from family members’, 34 ‘overlooked or devalued’. 47 Studies reporting on stigma originated from diverse cultural contexts, including the United Kingdom, Australia, Norway, Pakistan and Japan, indicating that is a prevalent issue that transcends dementia stages and cultural contexts. Stigma was portrayed as a social experience that exacerbated unmet social needs. For instance, the fear of being judged or misunderstood led some individuals to withdraw from social interactions and hide their diagnosis, thereby further limiting opportunities for companionship, meaningful relationships and emotional support. This aligns with other literature showing that stigma towards dementia contributes to social exclusion, emotional withdrawal, reduced help-seeking and quality of relationships.55,56 This pattern leads to a vicious cycle where stigma contributes to isolation, and isolation in turn worsens stigma.57,58 Addressing stigma at the interpersonal, community and organizational socioecological levels is a necessary step in meeting the social needs of older people with dementia.
Discussion
This scoping review synthesised evidence on unmet social needs among community-living older adults with dementia, with attention to how these needs evolve across the dementia trajectory. Existing literature on social participation, social engagement, and psychosocial well-being in dementia has largely examined individual perspectives or interpersonal relationships as separate domains. This scoping review extends understanding by conceptualising unmet social needs as multidimensional and relational, shaped by dynamic interactions across individual, interpersonal, and community contexts. Applying a socioecological framework offers a multilevel perspective on how unmet social needs emerge, are shaped, and evolve. It underscores the importance of supports that spans the multiple levels rather than focusing on individual factors.
Multi-level influences on unmet social needs
While previous research has documented factors influencing social participation and engagement in dementia, it has generally examined these factors within a single domain, such as cognitive capabilities or caregiver characteristics, without considering how multiple levels interact to shape social experiences. Situating unmet social needs within a socioecological framework shifts the focus away from individual deficits toward modifiable relational, environmental, and structural influences. This perspective aligns with person-centred and rights-based approaches to dementia support, 59 which emphasise inclusion, participation, and social citizenship. From an intervention perspective, these findings suggest that targeting unmet social needs should extend beyond the individual to coordinate efforts across families, services, and communities. Figure 2 applies a socioecological lens to the unmet social needs reported in the scoping review, emphasizing their multilevel nature.
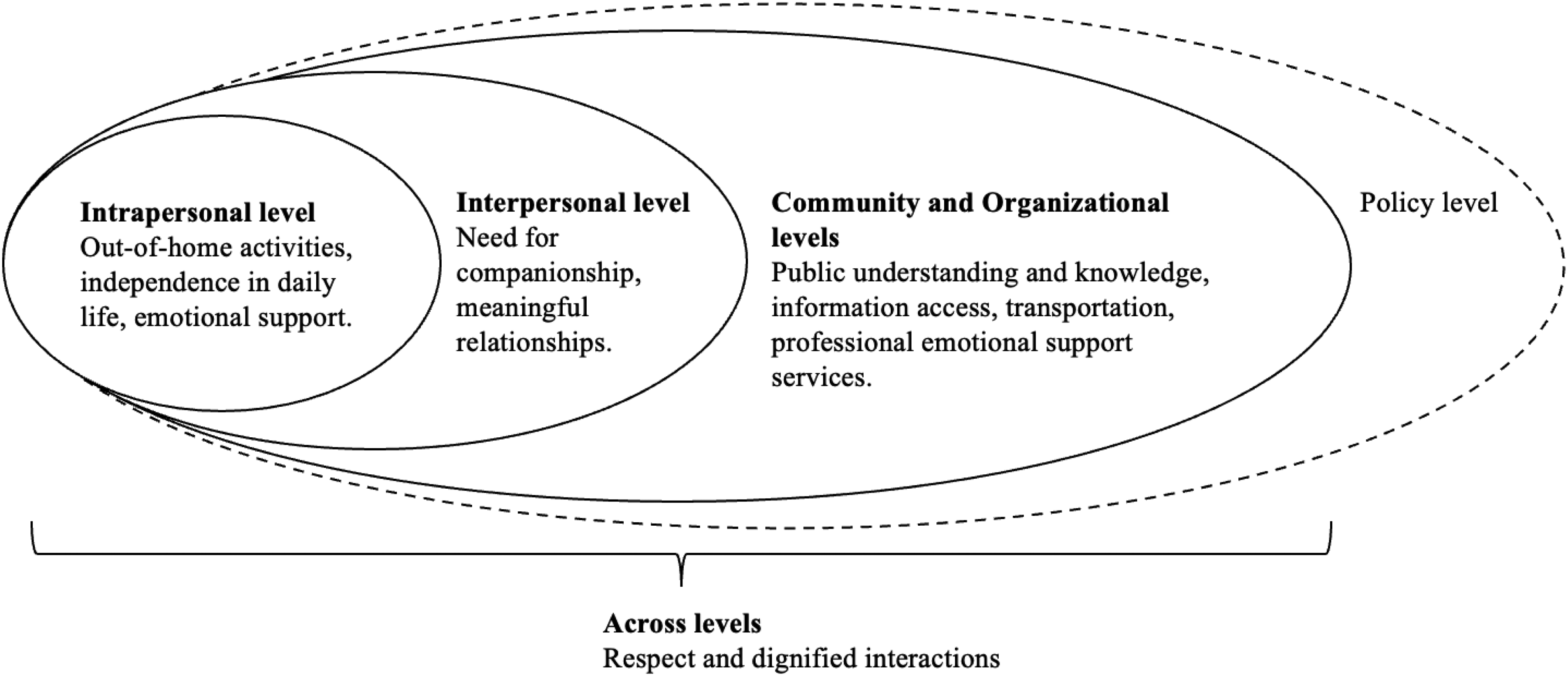
Unmet social needs across the socioecological levels.
Implications for stage-responsive social support in dementia care
Although dementia is clinically recognized as a progressive condition, research exploring the unmet social needs and participation of people living with dementia has rarely adopted a stage-sensitive perspective. This review highlights both the relevance of dementia stage in shaping unmet social needs and the limited empirical attention given to stage-specific experiences. Most included studies involved participants across multiple stages of dementia, which restricted detailed comparisons, underscoring a gap in the existing literature. Despite these limitations, the synthesis suggests patterns that align with frameworks describing social and identity changes in people living with dementia. As dementia evolves, there is a gradual transition from autonomy-oriented unmet social needs toward increasing reliance on supportive and inclusive social environments.
These findings underscore the importance of regularly reassessing unmet social needs across the dementia trajectory, and recognizing the dynamic nature of preferences and capacities. Stage-responsive interventions may support continued engagement in meaningful activities and roles in earlier stages, while prioritising emotionally supportive, inclusive, and dignity-preserving social environments in later stages.
Family coping as a contextual influence on unmet social needs
While caregivers, relatives and family members play a central role in shaping the social environments and opportunities of people living with dementia, family coping has rarely been examined as a contextual influence on unmet social needs. Existing research indicates that primary caregiver and family characteristics and behaviours can influence social participation outcomes.60,61 For example, partners of people living with dementia were considered as the most important social contact in reducing fear, and family members play key roles in initiating social activities. 60 Caregivers and family members who are socially active have been found to promote greater social participation among people living with dementia. 61 However, few studies explicitly explore how family adaptation, understanding, and coping processes shape the social experiences of people with dementia across stages.
Findings from this review suggest that family dynamics are closely intertwined with unmet social needs. In earlier stages, difficulties in family understanding and acceptance of the diagnosis sometimes led to misinterpretation of symptoms and strained relationships. 38 In later stages, role strain manifested through overprotection or exclusion from family activities, inadvertently limiting autonomy and social inclusion. 49 These patterns reinforce the view that unmet social needs are not solely a consequence of cognitive decline, but are also shaped by evolving family relationships and adaptive processes over time.
Literature has documented that caregiver needs and coping strategies vary across the stages of dementia, but are rarely examined in relation to the social participation and social needs of the person living with dementia. As a result, family coping is often treated as a static or background factor, limiting efforts to develop a more comprehensive understanding of unmet social needs. From an intervention perspective, these findings suggest that assessments and interventions aimed at addressing unmet social needs in dementia should incorporate caregiver, relatives and family coping and adaptation processes, recognising their potential to both support or constrain opportunities for social participation.
Gaps in research
Two main gaps were identified. First, scarcity of studies focusing on individuals in the moderate to severe stages of dementia. Including participants across all stages of dementia, in particular in the moderate and severe stage, is essential for developing a more comprehensive understanding of the unmet social needs experienced throughout the dementia journey.
Second, greater diversity in participant characteristics is needed. There is a significant imbalance in geographical and socioeconomic representation of participants. For instance, there is a lack of research from countries with more family-oriented traditions such as in Southern Europe, where government and public policies support family-integrated approaches. 62 The majority of included studies originate from higher-income and developed countries and lack exploration of how factors like community infrastructure and access to services may differ between urban and rural areas. It is equally important to include minority groups, which includes but is not limited to people with an immigrant background, sexual and gender diverse individuals, and individuals of diverse cultural backgrounds and social contexts. These populations may experience exclusions that affect their ability to have their social needs met. By actively engaging participants with a wide range of backgrounds, identities and lived experiences, future research can better capture the complexity and diversity of unmet social needs among older adults with dementia.
Limitations
This scoping review has some limitations. First, it excluded studies published before year 2000, in languages other than English, Portuguese and Mandarin, and grey literature or reports from key organizations. However, independent screening by two reviewers and adherence to the JBI and PRISMA-ScR guidelines sought to reduce bias. Second, this review did not explicitly include the exploration of solutions to unmet social needs as a research question, which may have limited the identification of studies addressing such solutions. Third, differences in unmet social needs across dementia subtypes were not examined in this review as it was not a predefined objective. The lack of dementia subtype reporting and diagnostically mixed populations further limited the feasibility of subtype specific analysis. Nonetheless, existing literature on social and behavioural changes in neurodegenerative conditions suggests that unmet social needs may vary by diagnosis. The limited attention to dementia subtypes in research on social needs likely reflects a widely recognised methodological challenges in dementia research, including difficulties in recruiting sufficiently large and diagnostically homogeneous samples, overlapping symptom profiles, and the inclusion of participants across mixed disease stages. Addressing these challenges in future research may support the development of more diagnosis sensitive and stage responsive approaches to social support.
Conclusion
This scoping review identified the following categories of unmet social needs: (i) participation in out-of-home activities, (ii) support for maintaining independence in daily life (iii) companionship, (iv) meaningful relationships, (v) respectful and dignified social interactions, (vi) emotional support, and (vii) social needs during the pandemic.
These needs evolve across dementia stages and are influenced by relational, socio-cultural, and structural contexts. The socioecological model provides a useful framework for understanding the multi-level factors that influence social needs. Future research should include a broader range of lived experiences, across all stages of dementia and reflecting diverse geographical, socioeconomic and cultural contexts. Greater inclusion of minority populations such as immigrants and sexual and gender diverse individuals is also essential. Strategies and approaches to addressing unmet social needs should be explored from the perspectives of older adults with dementia themselves.
Supplemental Material
sj-docx-1-alz-10.1177_13872877261442966 - Supplemental material for Unmet social needs of community-living older adults with dementia: A scoping review
Supplemental material, sj-docx-1-alz-10.1177_13872877261442966 for Unmet social needs of community-living older adults with dementia: A scoping review by Sunny Tan, Marine Markaryan, Óscar Ribeiro, Rita Maldonado Branco and Liliana Sousa in Journal of Alzheimer's Disease
Footnotes
Acknowledgements
The authors gratefully acknowledge the transformative agreement of University of Aveiro with Fundação para a Ciência e a Tecnologia (FCT) and B-On, supporting the publication of this article.
Ethical considerations
As this study is a scoping review and did not involve data collection with participants, ethical approval was not required.
Consent to participate
Not applicable
Consent for publication
Not applicable
Author contribution(s)
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the European Union's Horizon Europe under the Marie Skłodowska-Curie Actions’ Doctoral Networks, HORIZON-MSCA-2021-DN-01–01, proposal number 101072827.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Data are available upon request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
